LEPTOSPIROSIS: AN EMERGING HEALTH PROBLEM IN THAILAND
|
|
|
- Gabriella Gibbs
- 5 years ago
- Views:
Transcription
1 LEPTOSPIROSIS IN THAILAND LEPTOSPIROSIS: AN EMERGING HEALTH PROBLEM IN THAILAND W Tangkanakul 1, HL Smits 2, S Jatanasen 1 and DA Ashford 4 1 Bureau of General Communicable Diseases, Department of Disease Control (DDC), Ministry of Public Health (MOPH), Nonthaburi, Thailand; 2 KIT Biomedical Research, Royal Tropical Institute/ Koninklijk Instituut voor de Tropen (KIT), Amsterdam, The Netherlands; 3 National Center for Infectious Diseases, Center for Disease Control and Prevention (CDC), USA Abstract. Leptospirosis is an emerging health problem in Thailand, with dramatic increases in reported incidence since The annual number of reported leptospirosis cases increased from 398 cases in 1996 to 14,285 cases in In 2001, 2002, and 2003, the number of reported cases decreased, but still remained high at 10,217, 6,864, and 4,958 cases, respectively. The epidemiological characteristics of leptospirosis in Thailand include a peak incidence in September and October in association with the rainy season. A vast majority of the cases (90%) were reported in the Northeast region. The case fatality rate was as high as 4.4%, having a predominant association with male farmers aged 15 to 45 years. Outpatient cases were approximately 9 times more common than admitted cases, with an apparent recent shift in the pattern of infecting serovars among reservoir animals and humans. INTRODUCTION Thailand is situated in Southeast Asia from 5º 30 to 21º North latitude and from 97º 30 to 105º East longitude. The country is divided into 4 geographical regions: North, Central, South, and Northeast. There are three seasons in Thailand: cool, from November to February, hot, from March to May, and a rainy season from June to October. The average minimum temperature is 20ºC and the average maximum temperature is 37ºC. Thailand receives an average annual rainfall of about 1,700 mm or 252 billion m 3. Half of the country, mostly in the North and the Northeast, has fewer than 80 rain-days per annum. Leptospirosis is a zoonotic infection caused by pathogenic spirochetes of the genus Leptospira (Faine, 1998; Tappero et al, 1998; Levett, 2001). Risk groups include veterinarians, cattle, rice, and sugarcane farmers, military personnel, meat workers, sewage workers, and garbage collectors. In addition, recreational activities are Correspondence: Dr Waraluk Tangkanakul, Bureau of General Communicable Diseases, Department of Disease Control, Ministry of Public Health, Nonthaburi 10100, Thailand. Tel: 66 (0) ; Fax: 66 (0) Waraluk@health.moph.go.th increasingly recognized as risk factors for leptospirosis, with outbreaks being reported among swimmers, white water rafters, triathletes, and adventure athletes (Jackson et al, 1993; CDC, 1998). Outbreaks of leptospirosis have been associated with conditions of flooding (Sanders et al, 1999). This paper describes the epidemiological patterns of leptospirosis in Thailand and a recent increase in cases in Thailand. Reasons for the increased cases are discussed. Strategies for the assessment and control of leptospirosis are suggested. EPIDEMIOLOGICAL PATTERNS Leptospirosis in Thailand, Leptospirosis was first reported in Thailand in 1942 by Yunibandhu et al (1943). In 1972, leptospirosis was included as one of the 58 reportable infectious diseases under the National Passive Surveillance System. Reported leptospirosis cases are based on the clinical case definition of the WHO. Information was collected on a standard case report form and reported to the Ministry of Public Health (MOPH). From 1972 to 1988, 10 to 20 leptospirosis cases were reported annually in Thailand. Be- Vol 36 No. 2 March
2 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH Number of cases 16,000 14,000 12,000 10,000 8,000 6,000 4,000 2, Leptospirosis Source: Disease notification report. Ministry of Public Health, Thailand. Fig 1 Reported cases of leptospirosis by year in Thailand from 1990 to tween 1982 and 1994, the number of cases ranged from 55 to 272 cases per year (Fig 1) and represented an annual incidence rate of approximately 0.3/100,000 population (MOPH, Thailand; Tangkanakul et al, 1998). From 1991 to 1995, around 34% of the cases were reported from the Northeast region. The disease showed a seasonal fluctuation with most of the cases occurring between June and December. The peak incidence was observed in October. Most leptospirosis cases were seen among farmers aged years, with a male to female ratio of nearly 30:1 in some areas (Tangkanakul et al, 1998). Common reported symptoms included fever, myalgia, headache, conjunctival suffusion, and meningism (Tangkanakul, 2000). The most common serious complications reported were jaundice and renal impairment. Case-fatality rates were around 10%. In early serological studies of leptospirosis patients, Icterrohaemorrhagiae and Bataviae had the greatest serologic reactivity by MAT (Yunibandhu, 1943; Adthamsoontorn et al, 1960; Sundharagiati et al, 1964; Charoonruangrit and Bunpacknavig, 1964; Bunnag et al, 1965; Nimmanitya et al, 1984). A serologic study comparing patients presenting with acute fever of unknown origin (FUO) suggested that leptospirosis represented between 20 and 40% of FUO cases in rural and urban hospitals (Bunnag et al, 1965; Jatinandana et al, 1971; Nimmanitya et al, 1984; Heisey et al, 1988; Sundharagiati et al, 1996). Bataviae and Pyrogenes represented the serovars with the highest immunoreactivity by MAT in those studies (Sundharagiati et al,1996; Heisey et al, 1988). In addition, seroprevalence studies of the general population performed in the early 1960 s suggested a general seroprevalence of 28% in 71 provinces (Sundharagiati et al, 1964). Various serosurveys performed in the 1960 s indicated that Bataviae, Icterohaemorrhagiae and Grippotyphosa had the greatest serologic reactivity by MAT in normal people (Adthamsoontorn et al, 1960; Charoonruangrit et al, 1964; Sundharagiati et al, 1964; Tangkanakul, 2000). During the 1960s, some animal surveys were performed in order to help identify potential reservoirs for infection in Thailand. Rodent seroprevalence was estimated to be approximately 10% to 50% and leptospiral infections were found to be uncommon in house mice (Sundharagiati et al, 1969). In other studies, cultured leptospires from rat kidney tissue (Rattus. norvegicus) yielded an overall prevalence of 66%, suggesting that serosurveys may have been underestimating the prevalence in rodents (Sundharagiati et al, 1965). Serotyping of isolates showed that the serovars most common in rodents were Autumnalis, Bataviae, Javanica and Hebdomadis. These studies concluded that rodents were important reservoirs and sources of infections. However studies of seroprevalence in dogs captured in Bangkok showed a seroprevalence of 43%. In 8.1% of the dogs, leptospires (Bataviae, Javanica, and Ballico) could be isolated (Sundharagiati et al, 1965). Leptospirosis in Thailand: Data from disease notification reports indicated a drastically increase in leptospirosis cases between 1995 and 2003, with a peak in The number increased from 143 cases reported in 1995, to 398 in 1996, 2,331 cases in 1997, 6,080 cases in 1999, 14,285 cases in 2000, 10,217 cases in 2001, 6,864 in 2002 and 4,958 cases in 2003 (Fig 1). This was an increase in the incidence rate from less than 0.3 per 100,000 in 1995 to 23.7 in 2000, with a drop in subsequent years. There were 266 deaths reported in 1999 for a case fatality rate (CFR) of 4.4%, 362 deaths in 2000 for a CFR of 2.7%, 171 deaths in 2001 for a CFR of 1.7%, 95 deaths in 2002 for a CRF of 1.4%, and 82 death in 2003 for a CRF of 1.7 %. The male to female case ratio was 9:1 in 1995, 7:1 in 1996, 9:1 in 1997, 6:1 in 1998 to Vol 36 No. 2 March 2005
3 LEPTOSPIROSIS IN THAILAND and 3:1 in (MOPH, Thailand; Tangkanakul et al, 1998). As noted in the past, the peak incidence of leptospirosis still occurred in September to October each year (Fig 2). Leptospirosis cases were seen in all age groups except in children younger than 5 years of age. A peak was observed in the age group 25 to 54 years, accounting for 80% of all cases. Each year, most cases were farmers ( %) aged more than 15 years. The average inpatient to outpatient case ratio during was approximately 9:1. Pulmonary hemorrhage was observed as a major cause of death (Panaphut et al, 2002). The epidemic began after flooding in 1996 in the Nong Bunnak district, Nakhon Ratchasima Province in the Northeast (Sthonsaowapak, 1997). In 1997, it expanded to 16 out of 19 provinces in the Northeast region. The epidemic extended to the North and the Central. By 1997 the epidemic had expanded to 37 provinces, continuing to spread to 57 provinces in 1998, and to 64 provinces in 1999 (Tangkanakul et al, 1998). In the year 2000, provinces adjacent to Cambodia and the Central regions showed a leptospirosis morbidity rate of more than 50 per 100,000 inhabitants (Fig 3). High morbidity provinces were situated in the lower part of the Northeast, near the Cambodian border (Fig 3). Provinces with low morbidity were in the upper part, near the border with the Laos People s Democratic Republic. The average total rainfall in the lower part (1,000-1,500 mm per year) was less than in the upper part (1,400-2,000 mm per year). The many tributaries of the Shi and Nam Moon rivers divide large areas of the lower part. These areas are flooded during the rainy season, but are very dry during the rest of the year. The areas in the upper part are along Mekong River in the North. Cases 4,000 3,000 2,000 1,000 0 Jan Feb Mar Apr May June July Aug Sep Oct Nov Dec mean Source: Disease notification report. Ministry of Public Health, Thailand. Fig 2 Distribution of Leptospirosis cases by month in Thailand from 1996 to Source: Disease notification report. Ministry of Public Health, Thailand. (*)=Nakhon Ratchasima Province Fig 3 Morbidity rate of leptospirosis by province, Northeast, Thailand between 1996 and Vol 36 No. 2 March
4 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH Serologic data from outbreak investigations in the late 1990s indicate that Bratislava, Sejroe and Pyrogenes have become the most common serovars (Chaifoo et al, 1998; Arjkien, 2000; Boonyod et al, 2001; Tangkanakul et al, 2002). This indicates a shift from the historical MAT data, which showed the predominant serovars as Icterohameorrhagiae and Bataviae (Yunibandhu, 1943; Adthamsoontorn et al, 1960; Charoonruangrit et al, 1964; Sundharagiati et al, 1964; Bonnag et al, 1965; Nimmanitya et al, 1984). During the spring of 1998, an outbreak of febrile illness occurred in the Kosum Phisai district, Maha Sarakam Province in Northeast Thailand after flooding (Ratanasang et al, 2001). A serosurvey using slide microscopic reaction (H.S leptospira antigen, Sanofi Pasteur) was conducted among 245 asymptomatic farmers and agricultural workers aged 15 to 65 years. The overall prevalence rate was 13.5% (male = 13.9% (22/158), female = 12.7% (11/87). The highest prevalence rate was found in the age group (28.6 %), followed by the age group (25%) (Ratanasang et al, 2002). This overall prevalence rate was higher than that found in normal male military personnel in Khon Kaen in the Northeast (8.13%; 30/369). The most frequent detected serovar by MAT in military personnel was Bratislava (Phulsuksombati et al, 2001a). In 1998, a matched case-control study was conducted in Nakhon Ratchasima with the aim of identifying risk factors among rice field workers (Tangkanakul et al, 2000a). The results indicated that wading through stagnant water (OR 4.9, 95%CI ), applying fertilizer in wet fields for more than 6 hours a day (OR 3.4, 95%CI ), plowing in wet fields for more than 6 hours a day (OR 3.5, 95%CI ), and pulling seedlings in wet fields for more than 6 hours a day (OR 3.1, 95%CI ) were risk factors. Plowing, pulling seedlings and fertilizing activities were associated with a greater risk of skin cuts and abrasions than other rice farming activities. The seroprevalence rate in agricultural workers involved in high-risk activities was 42.9% (30/70) (Tangkanakul et al, 2000b). In 1999, an outbreak in the Buri Ram Province in the Northeast among villagers involved in pond cleaning was investigated. The villagers had been engaged in pulling reeds and water hyacinths from the water. Of 104 persons suspected of having leptospirosis, anti-leptospiral antibodies were detected in 43 (41%). The wearing of long pants or skirts during the pond-cleaning activities was found to be protective (OR 0.2; 95%CI ), whereas the presence of more than two wounds on the body was found to be a risk factor (OR 3.9; 95%CI ) (Phraisuwan et al, 2002). Rodents have long been associated with leptospirosis in Thailand. In 1998, an assessment of rodent populations in Nakhon Ratchasima revealed a ten times greater density of rats in an epidemic subdistrict (1 rat/80 m 2 ) than in a nonepidemic subdistrict (1 rat/800 m 2 ). The isolation rate from the rat kidneys using EMJH medium (n = 218) in Nong Bunnak (epidemic subdistrict) was 5.5%. All positive rats were Bandicota indica. All rats (n = 132) from Nong Yang (non-epidemic subdistrict) were found to be uninfected. Monoclonal antibody testing indicated that 11 were serogroup Autumnalis and one Pomona (Tangkanakul et al, 2002; Phulsuksombat et al, 1999). From June 1999 to September 2000, 989 rodents were captured from 4 epidemic provinces (Buri Ram, Surin, Khon Kaen and Kalasin) in the Northeast; 321 rodents were captured from a non-epidemic province (Nakhon Phanom) in the Northeast. Leptospires were isolated from rat kidney using EMJH medium. In the epidemic provinces, Leptospires were isolated from 7 out of 9 species of rodents (Rattus norvegicus (36.7%, 92/251), Bandicota indica (13.1%, 24/ 183), Rattus losea (7.7%, 5/65), Rattus rattus (7.1%, 9/126), Rattus argentiventer (6.2%, 6/97), Bandicota savilei (6.0%, 3/50), and Rattus exulans (1.0%, 2/199). In the non-epidemic province, Leptospires were found in 4 of 9 species, including Rattus norvegicus (62.5%, 35/56), Bandicota indica (14.6 %, 12/82), Rattus losea (16.7%, 1/6), and Rattus rattus (1.7%, 1/58). Mus cervicolor and Mus calori were not found to be reservoirs of leptospirosis (Phulsuksombati et al, 2001b). The prevalence of leptospires in rodents in the epidemic provinces and the non-epidemic 284 Vol 36 No. 2 March 2005
5 LEPTOSPIROSIS IN THAILAND province was 14.3% (141/989) and 15.3% (49/ 321) respectively. The isolation rate from rice field rats was 9.0% (47/521) and 9.5% (14/148) in the epidemic and non-epidemic provinces, respectively, whereas from house rats the prevalence was 20.1% (94/468) and 20.2 (35/173) in the epidemic and non-epidemic provinces, respectively. The total infection rate of leptospirosis in rodents was 14.5% (190/1310). Leptospiral isolates were identified from a panel of 26 standard antisera from a cross agglutination absorption test (CAAT) at the WHO/FAO Leptospirosis Reference Laboratory, Brisbane, Australia. Rattus norvegicus was the major reservoir of serogroup Pyrogenes, whereas Bandicota indica was infected with Autumnalis, Bataviae, Pyrogenes, Javanica and Australis serogroups. Our study failed to find a difference in the total population of rodents between the epidemic and non-epidemic provinces (Phulsuksombati et al, 2001b). Serosurveys among a variety of other animals species during 1999 did not find any significant difference in seroprevalence between the 4 epidemic provinces (Buri Ram, Surin, Khon Kaen, Kalasin in the Northeast) and a non-epidemic province (Nakhon Phanom in the Northeast). The prevalence of antibodies found using MAT in epidemic provinces was 77.2% (179/232) in cattle, 86.1% (155/180) in buffalo, and 60.4% (58/96) in swine. The prevalence of leptospiral antibodies in the non-epidemic province was 69.85% (90/129) in cattle, 82.2% (88/107) in buffalo and 62.5% (40/64) in swine. In cattle and buffalo, seroreactivity was observed mainly with serogroups Sarmin, Ranarum, Sejroe and Castellonis. In swine, reactivity mainly was observed with serovars Sarmin, Ranarum, Bratislava and Pomona (Suwancharoen et al, 2000). DISCUSSION Leptospirosis was first reported in Thailand 62 years ago. The incidence has dramatically increased since 1996, with a peak in During this period, leptospirosis showed the same seasonal variations, and affected the same highrisk groups, mostly agricultural workers, affected before the onset of the epidemic. There are areas that deserve attention, such as: 1) the center of the epidemic is in the Northeast, 2) the ratio of male to female cases decreased, 3) a shift in the predominant infecting serovars, and 4) a change in the most common complications. Reported leptospirosis cases were based on the initial clinical diagnoses of the physicians. Variation in the experience and awareness of the physicians regarding leptospirosis can lead to case ascertainment bias in both over- (false positive) and under- (false negative) diagnosis. Due to the protean nature of the disease, leptospirosis cases in Thailand can present and be reported as FUO or scrub typhus. In Thailand, the morbidity rate of FUO cases has increased from 239 in 2000 to 434 per 100,000 population in During , around 48% of reported FUO cases in Thailand were reported from the Northeast. Half of the FUO reported cases were farmers. The number of reported scrub typhus cases increased, with 1,210, 2,604, 1,969, 2,597, 3,914, 5,090 and 4,120 reported cases from 1996 to 2002, respectively (Tangkanakul and Ratanasang, 2003). Most causes of fever of unknown origin, such as leptospirosis, can not be identified, due to the limitation of laboratory diagnosis. Thus, the actual incidence of leptospirosis is not yet fully known. It cannot be said with any certainty whether the recent decrease in the number of cases marks the end of the epidemic or whether the epidemic is still expanding. The cause and trigger factors of the epidemic are still unknown. The most likely reasons for the epidemic are: 1) climatological and ecological conditions in the Northeast, favor the transmission of the disease during the rainy season, 2) the changing ecology and epidemiology of domestic animals and changes in the agricultural practices in the Northeast, 3) increase in rodent density resulting in an increased risk of infection, 4) physicians and villagers have increased their awareness and ability to recognize the disease and seek health care, and an increase in the availability of laboratory testing, 5) the increase may be due to an associated shift in the predominant infecting serovars. The serological data indicating the change in circulating serovar, however, must be interpreted with cau- Vol 36 No. 2 March
6 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH tion. The analyses have been based on MAT data, which is unable to identify specific serovars responsible for infection, but rather represents a pattern of cross-reactivity among serovars represented in the testing panel. The high seroprevalence rates in the humans and animals observed in the early days of leptospirosis in Thailand may suggest that leptospirosis always has been a potential, but until recent years unrecognized and underreported, health problem. To improve the surveillance data on leptospirosis in Thailand, laboratory confirmation of leptospirosis is essential. In recent years, a latex agglutination assay produced in Thailand has been implemented and is presently available at various sites at the district level (Naigowit et al, 2001). A confirmatory evaluation of the screening assay, however, is still needed to assess the validity of the test in hospital and field studies. Systematic evaluation of the current surveillance system is needed in order to ascertain current reporting practices among health care providers, to estimate the true burden of disease by laboratory confirmation, and to review the ability of the surveillance system to truly reflect the incidence of disease. Confirmation of cases and epidemiological investigations linking outbreaks to sources of infection preferably should be done by MAT. MAT confirmation is limited to the National Institute of Health (NIH), Bangkok, and several regional laboratories, each serving provinces. The Thai MAT incorporates 16 common serovars in its battery for the regional laboratory center and 23 serogroups for the NIH laboratory. Patterns of utilization of MAT confirmation among suspected leptospirosis cases in Thailand are presently unknown, and a reliable method of linking laboratory confirmation with epidemiological information is not currently in place. Recent animal serosurveys conducted in an attempt to determine an animal reservoir have yielded mixed results, and as yet a plausible animal reservoir has not been identified. An encompassing effort to obtain serovar information from likely animal reservoirs, determined on the basis of regional epidemiologic information, is needed to address this issue. Identification of matching serovars, from both culture-confirmed human cases and prospective infecting animal reservoirs, is the most reliable method for identifying potential reservoirs, and a focused attempt to identify such a linkage is needed in Thailand. A number of interventions were implemented in order to reduce the incidence of leptospirosis among rice farmers in the Northeast. These included advising the use of boots and gloves during farming work, and large rat extermination campaigns. Boots have been provided to local rice farmers for barrier protection, however, the effectiveness of this campaign has yet to be evaluated. Despite these interventions, the number of reported cases in the Northeast has not seemed to decrease. There are several possible reasons for this, they include the ineffectiveness of the implemented interventions, noncompliance with barrier protection methods, misguided eradication of animals other than the true reservoir, and as an artefact of changing reporting practices. The economic impact of leptospirosis in Thailand, and the potential cost to benefit ratio of interventions have been incompletely analyzed, and the overall economic impact of leptospirosis has not yet been studied in great detail. Based on estimates of costs made in a community hospital, the medical care cost for a mild case is 1,800 baht (US$50) per case; for more severe cases, which require hemodialysis, the cost increases to 10,000 baht (US$278) (Sthonsaowapak, 1997). The economic impact on an individual, related to medical and nonmedical costs, was 2,790 (US$ 70.50)-24,700 baht (US$ ) per case. Such a loss excluded the cost incurred by the public (Pornsiripongse et al, 2001). Other costs, such as the loss of workdays and cost of transportation for patients to and from clinical care are not included in this estimate. For successful control, the passive surveillance system should be strengthened, and strategies for active surveillance in animals and humans should be developed and implemented. This surveillance should include improved techniques for culturing and identifying serovars infecting humans and animals. Through the iden- 286 Vol 36 No. 2 March 2005
7 LEPTOSPIROSIS IN THAILAND tification of risk factors and identification of infecting animal reservoirs, effective methods of prevention and control may be designed. Control measures could include the escalation of barrier protection measures, vaccination and treatment of livestock, control of animals serving as infecting reservoirs, and increased sanitation measures. Ideally, these measures should also undergo thorough cost-effectiveness analysis. Education programs to alert people to avoidable and modifiable risk factors are in place and should be continued aggressively. ACKNOWLEDGEMENTS We would like to thank Drs Supamit Chunsuttiwat, Vinai Vuttivirojana, Kumnuan Ungchusak and Sirisak Warintrawat, Ministry of Public Health, Thailand for their valuable support on the leptospirosis problem. The authors also would like to express our sincere thanks to Drs Sandra Bragg and James Joseph Sejvars, Center for Disease Control and Prevention for their kind assistance. REFERENCES Adthamsoontorn L, Boonyaplika P, Sundharagiati B. Leptospirosis in Pitsanuloke Province. Vejasarn Med J 1960; 9: Arjkien W. Leptospirosis in northern Thailand. Monthly Epidemiol Surveill Rep 2000; 31: Boonyod D, Tanjatham S, Luppanakul P, Kiatvitchukul C, Jittawikul. Leptospira in patient sera in the lower north. Health Sci 2001; 10: Bunnag D, Jaroonyesama N, Harinsuta C. A clinical study of leptospirosis. J Med Assoc Thai 1965; 48: CDC. Update: leptospirosis and unexplained acute febrile illness among athletes participating in triathlons Illinois and Wisconsin, MMWR 1998; 47: Chaifoo W, Tharmapornpilas P, Limpaiboon R, Bragg S, Aye T. Clinical study for finding leptospirosis definition at Udon Thani Hospital, Udon Thani, and October Reg 6/2 Med J 1998; 6: Charoonruangrit S, Boonpacknavig S. Leptospirosis at Chulalongkorn hospital. J Med Assoc Thai 1964; 47: Faine S. Leptospirosis. In: Hausler WJJr, Sussman M, eds. Topley and Wilson s microbiology and microbial infections. 9 th ed. London: Arnold, 1998: Heisey GB, Nimmanita S, Karnchanachetanee C. et al. Epidemiology and characterization of leptospirosis at an urban and provincial site in Thailand. Southeast Asian J Trop Med Health 1988; 19: Jackson LA, Kaufmann AF, William G, et al. Outbreak of leptospirosis associated with swimming. Pediatr Infect Dis J 1993; 12: Jatinandana S. A study of fever of unknown origin in Northeast Thailand. In : Report of The First International Seminar of the SEATO Medical Research Laboratory, Bangkok, February 1971: Levett P. Leptospirosis. Clin Microbiol Rev 2001; 14: Naigowit P, Luepaktra O, Yasang S, Biklang M, Warachit P. Development of a screening test for serodiagnosis of leptospirosis. Intern Med J 2001; 17: 1-5. Nimmanitya S, Thisyakorn U, Ningsanonda C. Leptospirosis in Children. Bull Dept Med Sci 1984; 9: Panaphut T, Domrongkitchaiporn S, Thinkamrop B. Prognostic factors of death in leptospirosis: a prospective study in Khon Kaen, Thailand. Int J Infect Dis 2002; 6: Phraisuwan P, Spotts Whitney EA, Tharmaphornpilas P, et al. Leptospirosis: skin wounds and control strategies, Thailand, Emerg Infect Dis 2002; 8: Phulsuksombati D, Tangkanakul W, Sangjun N, Kingnate D, Khoprasert Y, Hamarit K. Isolation of leptospirosis from wild rodent in Thailand, Health Sci 1999; 8: Phulsuksombati D, Sangjun N, Tangkanakul W, Sudsaward Y, Chumchat P. Prevalence of leptospiral antibody in military recruits, Khon Kaen, RTA Med J 2001a; 54: Phulsuksombati D, Sangjun N, Khoprasert Y, Kingnate D, Tangkanakul W. Leptospires in rodent, northeastern region Health Sci 2001b; 10: Pornsiripongse S, Muangkliang R, Usuparat P et al. Knowledge about leptospirosis among high risk group. Health Sci 2001; 10: Ratanasang P, Tangkanakul W, Namrit S, Kaewhanam B. Prevalence of leptospiral antibody in agricultural group, Kosumpisai district, Mahasarakam province, Health Sci 2001; 10: Ratanasang P, Tangkanakul W, Namrit S, Kaewhanam Vol 36 No. 2 March
8 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH B. Leptospirosis outbreak in Kosumpisai district, Mahasarakam Province, Health Sci 2002; 11: Sanders EJ, Rigua-Perez JG, Smits HL, et al. Increase in leptospirosis in dengue-negative patients, after a hurricane in Puerto Rico, Am J Trop Med Hyg 1999; 61: Sthonsaowapak T. Leptospirosis investigation Nongbunnak district, Nakhon Ratchasrima province, J Northeastern Reg Epidemiol 1997; 2: Sundharagiati B, Harinasuta C. Studies on leptospirosis in Thailand [A review]. J Med Assoc Thai 1964; 47: Sundharagiati B, Harinsuta C, Pholpothi T. Leptospirosis in rats. J Med Assoc Thai 1965; 48: Sundharagiati B, Potha U, Pholpothi T, Naebnien K, Intarakao C. Leptospirosis in rats of thirty one provinces: A study of 3,658 rats (eleven species) J Dept Med Serv 1969; 18: Sundharagiati B, Kasemsuvan P, Harinsuta C, Potha U. Leptospirosis as a cause of pyrexia of unknown origin in Thailand. Ann Trop Med Parasitol 1996; 60: Suwancharoen D, Indrakamhang P, Neramitmansook P, Tangkanakul W. Serological survey of leptospiral antibody in livestock in 5 northeastern provinces. J Thai Vet Med Assoc 2000; 51: Tangkanakul W, Kingnate D. Leptospirosis epidemic in northeastern provinces of Thailand, 1997 [A review]. Health Sci 1998; 7: Tangkanakul W. Epidemiology and clinical manifestation of leptospirosis in Thailand [A review]. J Northeastern Reg Epidemiol 2000; 5: Tangkanakul W, Tharmaphornpilas P, Plikaylis BD, et al. Risk factors associated with leptospirosis infection in northeastern Thailand, Am J Trop Med Hyg 2000a; 63: Tangkanakul W, Naigowit P, Smithsuwan P, Kaewmalang P, Khoprasert Y, Phulsuksombati D. Prevalence of asymtomatic leptospirosis infection among high risk group Health Sci 2000b; 9: Tangkanakul W, Hinjoy S, Smithsuwan P, Phulsuksombati D, Choomkasien P. Leptospira serovar in humans and animals, Nakhon Ratchasima. Monthly Epidemiol Surveill Rep 2002; 33: Tangkanakul W, Ratanasang P. Epidemiology of noticeable rodent-borne diseases in 506 report. J Health Sci 2003; 12: Tappero J, Ashford DA, Perkins BA. Leptospirosis. In: Mandell GL, Bennett JE, Dolin R, eds. Principles and practice of infectious diseases. 5 th ed. New York: Churchill Livingstone; 1998: Yunibandhu J. First report of Weil s disease in Thailand. J Med Assoc Thai 1943; 26: Vol 36 No. 2 March 2005
Leptospirosis as a public health concern New Caledonia as a case study
 Leptospirosis as a public health concern New Caledonia as a case study Eric D Ortenzio Infectious Diseases Epidemiology Unit Institut Pasteur of New Caledonia Leptospirosis: an emerging public health problem
Leptospirosis as a public health concern New Caledonia as a case study Eric D Ortenzio Infectious Diseases Epidemiology Unit Institut Pasteur of New Caledonia Leptospirosis: an emerging public health problem
Global Alert & Response (GAR) Leptospirosis. Global Alert & Response (GAR)
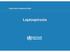 Leptospirosis Leptospirosis, a zoonotic and environmental disease a zoonotic and environmental disease Bacteria hosted in animals' kidneys for months/years Environment contaminated by urine (weeks/months)
Leptospirosis Leptospirosis, a zoonotic and environmental disease a zoonotic and environmental disease Bacteria hosted in animals' kidneys for months/years Environment contaminated by urine (weeks/months)
Malaria Risk Areas in Thailand Border
 Malaria Risk Areas in Thailand Border Natthawut Kaewpitoon PhD*, **, Ryan A Loyd MD***, Soraya J Kaewpitoon MD**, ***, Ratana Rujirakul MEd** * Faculty of Public Health, Vongchavalitkul University, Nakhon
Malaria Risk Areas in Thailand Border Natthawut Kaewpitoon PhD*, **, Ryan A Loyd MD***, Soraya J Kaewpitoon MD**, ***, Ratana Rujirakul MEd** * Faculty of Public Health, Vongchavalitkul University, Nakhon
Leptospirose in de Lage Landen
 Leptospirose in de Lage Landen 72 STE EDITIE GENEESKUNDIGE DAGEN VAN ANTWERPEN Marjan Van Esbroeck referentielaboratorium ITG Antwerpen Wim Flipse - Agentschap Zorg en Gezondheid Leptospira species Order
Leptospirose in de Lage Landen 72 STE EDITIE GENEESKUNDIGE DAGEN VAN ANTWERPEN Marjan Van Esbroeck referentielaboratorium ITG Antwerpen Wim Flipse - Agentschap Zorg en Gezondheid Leptospira species Order
Protect & Prevent: A Quick Guide to Canine Leptospirosis
 Protect & Prevent: A Quick Guide to Canine Leptospirosis To Prevent and Protect First Learn and Discern Leptospirosis is a geographically widespread disease which affects many animal species including
Protect & Prevent: A Quick Guide to Canine Leptospirosis To Prevent and Protect First Learn and Discern Leptospirosis is a geographically widespread disease which affects many animal species including
LEPTOSPIRA SPP Date of document: July 2004
 LEPTOSPIRA SPP Date of document: July 2004 1.- INTRODUCCIÓN The Leptospira genus is a member of the Leptospiraceae family, Spirochaetales order. The classification of the leptospiras is very complex and
LEPTOSPIRA SPP Date of document: July 2004 1.- INTRODUCCIÓN The Leptospira genus is a member of the Leptospiraceae family, Spirochaetales order. The classification of the leptospiras is very complex and
Field application of Lepto lateral flow for rapid diagnosis of leptospirosis
 Journal of Medical Microbiology (2003), 52, 897 901 DOI 10.1099/jmm.0.05064-0 Field application of Lepto lateral flow for rapid diagnosis of leptospirosis S. C. Sehgal, P. Vijayachari, A. P. Sugunan and
Journal of Medical Microbiology (2003), 52, 897 901 DOI 10.1099/jmm.0.05064-0 Field application of Lepto lateral flow for rapid diagnosis of leptospirosis S. C. Sehgal, P. Vijayachari, A. P. Sugunan and
Management of Leptospirosis Outbreaks. Irmingarda P. Gueco, MD, FPCP, FPSN, MBA
 Management of Leptospirosis Outbreaks Irmingarda P. Gueco, MD, FPCP, FPSN, MBA Objective : To discuss the handling of Leptospirosis outbreaks with specific reference to Philippine experience. Outline :
Management of Leptospirosis Outbreaks Irmingarda P. Gueco, MD, FPCP, FPSN, MBA Objective : To discuss the handling of Leptospirosis outbreaks with specific reference to Philippine experience. Outline :
PROVINCIAL RISK MAPS FOR HIGHEST TENDENCY RANKING EPIDEMIOLOGICAL SURVEILLANCE DISEASES IN AYUTTHAYA PROVINCE, THAILAND
 PROVINCIAL RISK MAPS FOR HIGHEST TENDENCY RANKING EPIDEMIOLOGICAL SURVEILLANCE DISEASES IN AYUTTHAYA PROVINCE, THAILAND Soutthanome KEOLA, Mitsuharu TOKUNAGA Space Technology Applications and Research
PROVINCIAL RISK MAPS FOR HIGHEST TENDENCY RANKING EPIDEMIOLOGICAL SURVEILLANCE DISEASES IN AYUTTHAYA PROVINCE, THAILAND Soutthanome KEOLA, Mitsuharu TOKUNAGA Space Technology Applications and Research
ªí À Õß ª µ ª πø å æàõ àæ π ÿå ÿ :
 «µ«æ å ªï Ë 30 Ë 3, 2543 25 π æπ åµâπ ªí À Õß ª µ ª πø å æàõ àæ π ÿå ÿ : π Ÿµ º ß» «ß ÿ«å * Õ æ ÿ «ß å ƒµ** Abstract Duangjai Suwanchareon* Annop Kunavongkrit** AN OUTBREAK OF LEPTOSPIROSIS IN A SWINE
«µ«æ å ªï Ë 30 Ë 3, 2543 25 π æπ åµâπ ªí À Õß ª µ ª πø å æàõ àæ π ÿå ÿ : π Ÿµ º ß» «ß ÿ«å * Õ æ ÿ «ß å ƒµ** Abstract Duangjai Suwanchareon* Annop Kunavongkrit** AN OUTBREAK OF LEPTOSPIROSIS IN A SWINE
Dengue Surveillance and Response in Thailand
 Dengue Surveillance and Response in Thailand Dr.Sopon Iamsirithaworn, MD, MPH, PhD Office of Disease Prevention and Control 1, Department of Disease Control, Ministry of Public Health, Thailand 1 April
Dengue Surveillance and Response in Thailand Dr.Sopon Iamsirithaworn, MD, MPH, PhD Office of Disease Prevention and Control 1, Department of Disease Control, Ministry of Public Health, Thailand 1 April
Assessment of Distribution Leptospira Spp. In Surface Waters of Guilan Province
 American-Eurasian Journal of Scientific Research 3 (2): 147-152, 2008 ISSN 1818-6785 IDOSI Publications, 2008 Assessment of Distribution Leptospira Spp. In Surface Waters of Guilan Province 1 2 3 4 K.
American-Eurasian Journal of Scientific Research 3 (2): 147-152, 2008 ISSN 1818-6785 IDOSI Publications, 2008 Assessment of Distribution Leptospira Spp. In Surface Waters of Guilan Province 1 2 3 4 K.
Leptospirosis and its complex ecology
 Department of Medicine Clinical Research Unit Project Zoonotic Diseases Swiss TPH Winter Symposium 2018 One Health: Zoonoses Control in Humans and Animals Taking Stock and Future Priorities Leptospirosis
Department of Medicine Clinical Research Unit Project Zoonotic Diseases Swiss TPH Winter Symposium 2018 One Health: Zoonoses Control in Humans and Animals Taking Stock and Future Priorities Leptospirosis
Network for Prevention and Control of Leptospirosis in Asia
 Network for Prevention and Control of Leptospirosis in Asia JUN FUJII, SHIN-ICHI YOSHIDA Kyushu University, Japan XIAO-KUI GUO Shanghai Jiao Tong University, China SUBHASH C SEHGAL WHO Collaborating Centre
Network for Prevention and Control of Leptospirosis in Asia JUN FUJII, SHIN-ICHI YOSHIDA Kyushu University, Japan XIAO-KUI GUO Shanghai Jiao Tong University, China SUBHASH C SEHGAL WHO Collaborating Centre
ENDEMIC MALARIA IN FOUR VILLAGES IN ATTAPEU PROVINCE, LAO PDR
 ENDEMIC MALARIA IN FOUR VILLAGES IN ATTAPEU PROVINCE, LAO PDR R Phetsouvanh 1, I Vythilingam 2, B Sivadong 1, S Lokman Hakim 2, ST Chan 2 and S Phompida 1 1 Center for Malaria, Parasitology and Entomology,
ENDEMIC MALARIA IN FOUR VILLAGES IN ATTAPEU PROVINCE, LAO PDR R Phetsouvanh 1, I Vythilingam 2, B Sivadong 1, S Lokman Hakim 2, ST Chan 2 and S Phompida 1 1 Center for Malaria, Parasitology and Entomology,
Seroprevalence of Tetanus Antibody in the Thai Population: A National Survey
 ASIAN PACIFIC JOURNAL OF ALLERGY AND IMMUNOLOGY (2007) 25: 219-223 Seroprevalence of Tetanus Antibody in the Thai Population: A National Survey Pantipa Chatchatee 1, Susheera Chatproedprai 1, Porpit Warinsathien
ASIAN PACIFIC JOURNAL OF ALLERGY AND IMMUNOLOGY (2007) 25: 219-223 Seroprevalence of Tetanus Antibody in the Thai Population: A National Survey Pantipa Chatchatee 1, Susheera Chatproedprai 1, Porpit Warinsathien
SHORT REPORT Acute Q fever in northern Queensland: variation in incidence related to rainfall and geographical location
 Epidemiol. Infect. (213), 141, 134 138. f Cambridge University Press 212 doi:1.117/s952688121495 SHORT REPORT Acute Q fever in northern Queensland: variation in incidence related to rainfall and geographical
Epidemiol. Infect. (213), 141, 134 138. f Cambridge University Press 212 doi:1.117/s952688121495 SHORT REPORT Acute Q fever in northern Queensland: variation in incidence related to rainfall and geographical
Emergence of chikungunya in Moonlapamok and Khong Districts, Champassak Province, the Lao People s Democratic Republic, May to September 2012
 Outbreak Investigation Report Emergence of chikungunya in Moonlapamok and Khong Districts, Champassak Province, the Lao People s Democratic Republic, May to September 2012 Chanthavy Soulaphy, a Phouthone
Outbreak Investigation Report Emergence of chikungunya in Moonlapamok and Khong Districts, Champassak Province, the Lao People s Democratic Republic, May to September 2012 Chanthavy Soulaphy, a Phouthone
Downloaded from ismj.bpums.ac.ir at 11: on Friday February 22nd 2019
 ELISA (outbreak) (LDS) (DST) (IHA) (Weil's disease) (Outbreak) (Outbreak) ۀ SERION-ELISA Classic Leptospira Institut Virion / Serion GmbH Leptospira interrogans L. copenhagenil L. icterohaemorrhagiae L.
ELISA (outbreak) (LDS) (DST) (IHA) (Weil's disease) (Outbreak) (Outbreak) ۀ SERION-ELISA Classic Leptospira Institut Virion / Serion GmbH Leptospira interrogans L. copenhagenil L. icterohaemorrhagiae L.
Study of Leptospirosis outbreak in Sri Lanka. In Kurunagala District -2008
 Study of Leptospirosis outbreak in Sri Lanka In Kurunagala District -2008 22.05.2009, Pubuduni Weerakoon, Research Assistant, Real-Time Biosurveillance Program Introduction In the year 2008 bringing forth
Study of Leptospirosis outbreak in Sri Lanka In Kurunagala District -2008 22.05.2009, Pubuduni Weerakoon, Research Assistant, Real-Time Biosurveillance Program Introduction In the year 2008 bringing forth
Research Article Leptospirosis in Vellore: A Clinical and Serological Study
 Microbiology, Article ID 643940, 5 pages http://dx.doi.org/10.1155/2014/643940 Research Article Leptospirosis in Vellore: A Clinical and Serological Study G. Vimala, 1 A. Mary Josephine Rani, 1 and V.
Microbiology, Article ID 643940, 5 pages http://dx.doi.org/10.1155/2014/643940 Research Article Leptospirosis in Vellore: A Clinical and Serological Study G. Vimala, 1 A. Mary Josephine Rani, 1 and V.
Dengue Haemorrhagic Fever in Thailand
 By Wiwat Rojanapithayakorn Office of Dengue Control, Department of Communicable Diseases Control, Ministry of Public Health, Thailand Abstract Dengue haemorrhagic fever was first reported in Thailand in
By Wiwat Rojanapithayakorn Office of Dengue Control, Department of Communicable Diseases Control, Ministry of Public Health, Thailand Abstract Dengue haemorrhagic fever was first reported in Thailand in
Studies and interventions in Animals
 Studies and interventions in Animals NZ-based Projects and Perspectives Peter Wilson, Cord Heuer, Jackie Benschop Julie Collins-Emerson and Emilie Vallée This presentation Leptospirosis Research Group
Studies and interventions in Animals NZ-based Projects and Perspectives Peter Wilson, Cord Heuer, Jackie Benschop Julie Collins-Emerson and Emilie Vallée This presentation Leptospirosis Research Group
Navigating vaccine introduction: a guide for decision-makers JAPANESE ENCEPHALITIS (JE) Module 1. Does my country need JE vaccine?
 Navigating vaccine introduction: a guide for decision-makers JAPANESE ENCEPHALITIS (JE) Module 1 Does my country need JE vaccine? 1 about this guide Japanese encephalitis (JE), a viral infection of the
Navigating vaccine introduction: a guide for decision-makers JAPANESE ENCEPHALITIS (JE) Module 1 Does my country need JE vaccine? 1 about this guide Japanese encephalitis (JE), a viral infection of the
Analysis of Hospital-Based Sentinel Surveillance Data on Leptospirosis in Sri Lanka,
 Jpn. J. Infect. Dis., 65, 157-161, 2012 Original Article Analysis of Hospital-Based Sentinel Surveillance Data on Leptospirosis in Sri Lanka, 2005 2008 Chandika D. Gamage 1, Jagath Amarasekera 2, Paba
Jpn. J. Infect. Dis., 65, 157-161, 2012 Original Article Analysis of Hospital-Based Sentinel Surveillance Data on Leptospirosis in Sri Lanka, 2005 2008 Chandika D. Gamage 1, Jagath Amarasekera 2, Paba
FMD Control Initiatives in Bangladesh
 FMD Control Initiatives in Bangladesh Dr. Md. Mohsin Ali Dr. Md. Ainul Haque Department of Livestock Services, Bangladesh Country Profile In Short Bangladesh is a Republic of South Asia It is bordered
FMD Control Initiatives in Bangladesh Dr. Md. Mohsin Ali Dr. Md. Ainul Haque Department of Livestock Services, Bangladesh Country Profile In Short Bangladesh is a Republic of South Asia It is bordered
Department of Medical Microbiology, Faculty of Medicine, University of Malaya, Malaysia; 2
 SEROPREVALENCE OF RICKETSIAL ANTIBODIES AMONG URBAN MALAYSIANS ANTIBODY PREVALENCE OF ORIENTIA TSUTSUGAMUSHI, RICKETTSIA TYPHI AND TT118 SPOTTED FEVER GROUP RICKETTSIAE AMONG MALAYSIAN BLOOD DONORS AND
SEROPREVALENCE OF RICKETSIAL ANTIBODIES AMONG URBAN MALAYSIANS ANTIBODY PREVALENCE OF ORIENTIA TSUTSUGAMUSHI, RICKETTSIA TYPHI AND TT118 SPOTTED FEVER GROUP RICKETTSIAE AMONG MALAYSIAN BLOOD DONORS AND
Update on the Dengue situation in the Western Pacific Region
 Dengue Situation Update Number 537 27 February Update on the Dengue situation in the Western Pacific Region Northern Hemisphere Cambodia As of 2 February, a total of 132 suspected dengue cases have been
Dengue Situation Update Number 537 27 February Update on the Dengue situation in the Western Pacific Region Northern Hemisphere Cambodia As of 2 February, a total of 132 suspected dengue cases have been
Global Leptospirosis Environmental Action Network
 Global Leptospirosis Environmental Action Network Leptospirosis as a global threat for both animals and humans: The GLEAN Story Claudia Munoz-Zanzi Division of Epidemiology and Community Health School
Global Leptospirosis Environmental Action Network Leptospirosis as a global threat for both animals and humans: The GLEAN Story Claudia Munoz-Zanzi Division of Epidemiology and Community Health School
Case report in Republic of Korea. Dong-Kun Yang Senior researcher Lab. of rabies in viral disease division of QIA
 Case report in Republic of Korea Dong-Kun Yang Senior researcher Lab. of rabies in viral disease division of QIA Contents 1. Epidemiological situation of rabies 2. Current control program in wildlife 3.
Case report in Republic of Korea Dong-Kun Yang Senior researcher Lab. of rabies in viral disease division of QIA Contents 1. Epidemiological situation of rabies 2. Current control program in wildlife 3.
Q Fever among Dairy Cattle in Chiang Mai Province, Thailand, 2012: A Preliminary Study
 Q Fever among Dairy Cattle in Chiang Mai Province, Thailand, 2012: A Preliminary Study Pranee Rodtian 1, *, Nuamjit M 1, Srijan M 2, Opaschaitat P 3, Ekgatat M 3 1 Fifth Regional Livestock Office, Chiang
Q Fever among Dairy Cattle in Chiang Mai Province, Thailand, 2012: A Preliminary Study Pranee Rodtian 1, *, Nuamjit M 1, Srijan M 2, Opaschaitat P 3, Ekgatat M 3 1 Fifth Regional Livestock Office, Chiang
Doxycycline versus Azithromycin for the Treatment of Leptospirosis and Scrub typhus. ACCEPTED
 AAC Accepts, published online ahead of print on 16 July 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.00508-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 16 July 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.00508-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
Leptospirosis - a global disease but a local phenomenon
 Leptospirosis - a global disease but a local phenomenon Jackie Benschop, Julie Collins-Emerson, Neville Haack, Shaan Mocke, Juan Sanhueza, Yuni Yupiana, Jenny Weston, Cord Heuer and Peter Wilson. 22 and
Leptospirosis - a global disease but a local phenomenon Jackie Benschop, Julie Collins-Emerson, Neville Haack, Shaan Mocke, Juan Sanhueza, Yuni Yupiana, Jenny Weston, Cord Heuer and Peter Wilson. 22 and
Rift Valley Fever RVF. Enhancing Safe Inter-Regional Livestock Trade Dubai, United Arab Emirates June 13-16, 2011
 Rift Valley Fever RVF Enhancing Safe Inter-Regional Livestock Trade Dubai, United Arab Emirates June 13-16, 2011 Definition Rift valley fever (RVF) is an acute febrile arthropod-borne zoonotic disease.
Rift Valley Fever RVF Enhancing Safe Inter-Regional Livestock Trade Dubai, United Arab Emirates June 13-16, 2011 Definition Rift valley fever (RVF) is an acute febrile arthropod-borne zoonotic disease.
Evaluation of Early Aberration Reporting System for Dengue Outbreak Detection in Thailand
 Evaluation of Early Aberration Reporting System for Dengue Outbreak Detection in Thailand Supharerk Thawillarp 1, *, Carlos Castillo-Salgado 2, Harold P. Lehmann 1 1 Division of Health Sciences Informatics,
Evaluation of Early Aberration Reporting System for Dengue Outbreak Detection in Thailand Supharerk Thawillarp 1, *, Carlos Castillo-Salgado 2, Harold P. Lehmann 1 1 Division of Health Sciences Informatics,
A REVIEW OF DENGUE FEVER INCIDENCE IN KOTA BHARU, KELANTAN, MALAYSIA DURING THE YEARS
 DENGUE FEVER INCIDENCE IN KOTA BAARU, MALAYSIA A REVIEW OF DENGUE FEVER INCIDENCE IN KOTA BHARU, KELANTAN, MALAYSIA DURING THE YEARS 1998-2003 Narwani Hussin 1, Jesni Jaafar 1, Nyi Nyi Naing 1, Hamzah
DENGUE FEVER INCIDENCE IN KOTA BAARU, MALAYSIA A REVIEW OF DENGUE FEVER INCIDENCE IN KOTA BHARU, KELANTAN, MALAYSIA DURING THE YEARS 1998-2003 Narwani Hussin 1, Jesni Jaafar 1, Nyi Nyi Naing 1, Hamzah
Epidemiology of Lassa Fever
 Epidemiology of Lassa Fever Njideka E. Kanu Department of Community Medicine, University of Medical Sciences, Ondo A lecture delivered at the Academic Seminar of University of Medical Sciences, Ondo, 14
Epidemiology of Lassa Fever Njideka E. Kanu Department of Community Medicine, University of Medical Sciences, Ondo A lecture delivered at the Academic Seminar of University of Medical Sciences, Ondo, 14
Outbreak Investigation:
 Outbreak Investigation: Principles & Practice Panithee Thammawijaya, MD PhD Bureau of Epidemiology A Call for Help On 16 May 2005, Bureau of Epidemiology (BoE) received a notification call from a northern
Outbreak Investigation: Principles & Practice Panithee Thammawijaya, MD PhD Bureau of Epidemiology A Call for Help On 16 May 2005, Bureau of Epidemiology (BoE) received a notification call from a northern
Emerging Infectious Disease Categories (NIAID) 1 of 3
 Emerging Diseases Emerging Infectious Disease Categories (NIAID) 1 of 3 Category A Priority Pathogens Category A pathogens are those organisms/biological agents that pose the highest risk to national security
Emerging Diseases Emerging Infectious Disease Categories (NIAID) 1 of 3 Category A Priority Pathogens Category A pathogens are those organisms/biological agents that pose the highest risk to national security
Health advice for travelers
 Health advice for travelers Welcome to Thailand Every year millions of tourists set Thailand as one of their favorite destinations. The information provided here will help you come up with appropriate
Health advice for travelers Welcome to Thailand Every year millions of tourists set Thailand as one of their favorite destinations. The information provided here will help you come up with appropriate
ORIGINAL ARTICLE. SEROPREVALENCE OF DENGUE IN TERTIARY CARE CENTRE AT LUCKNOW Shipra Singhal 1, Krati R. Varshney 2, Vineeta Mittal 3, Y. I. Singh 4.
 SEROPREVALENCE OF DENGUE IN TERTIARY CARE CENTRE AT LUCKNOW Shipra Singhal 1, Krati R. Varshney 2, Vineeta Mittal 3, Y. I. Singh 4. 1. Junior Resident, Department of Microbiology, Era s Lucknow Medical
SEROPREVALENCE OF DENGUE IN TERTIARY CARE CENTRE AT LUCKNOW Shipra Singhal 1, Krati R. Varshney 2, Vineeta Mittal 3, Y. I. Singh 4. 1. Junior Resident, Department of Microbiology, Era s Lucknow Medical
Global and National Trends in Vaccine Preventable Diseases. Dr Brenda Corcoran National Immunisation Office.
 Global and National Trends in Vaccine Preventable Diseases Dr Brenda Corcoran National Immunisation Office Global mortality 2008 Children under 5 years of age 1.5 million deaths due to vaccine preventable
Global and National Trends in Vaccine Preventable Diseases Dr Brenda Corcoran National Immunisation Office Global mortality 2008 Children under 5 years of age 1.5 million deaths due to vaccine preventable
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Culex larvae found collecting in standing water Image by CDC/James Gathany - License: Public Domain. Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County Culex larvae found collecting in standing water Image by CDC/James Gathany - License: Public Domain. Maricopa County Department of Public Health Office of Epidemiology
Economic Impacts of Porcine Reproductive and Respiratory Syndrome (PRRS) Outbreak in Vietnam Pig Production
 Tropical Agricultural Research Vol. 23 (2): 152 159 (2012) Economic Impacts of Porcine Reproductive and Respiratory Syndrome (PRRS) Outbreak in Vietnam Pig Production H. Zhang * and H. Kono 1 Department
Tropical Agricultural Research Vol. 23 (2): 152 159 (2012) Economic Impacts of Porcine Reproductive and Respiratory Syndrome (PRRS) Outbreak in Vietnam Pig Production H. Zhang * and H. Kono 1 Department
Application of recombinant Leptospiral outer membrane protein in ELISA-based serodiagnosis. Thareerat Kalambaheti
 Application of recombinant Leptospiral outer membrane protein in ELISA-based serodiagnosis Thareerat Kalambaheti 1 Background to study Leptospirosis : Caused by bacteria of the genus Leptospira Humans
Application of recombinant Leptospiral outer membrane protein in ELISA-based serodiagnosis Thareerat Kalambaheti 1 Background to study Leptospirosis : Caused by bacteria of the genus Leptospira Humans
Profile on TADs in Japan
 Profile on TADs in Japan Country Report Tatsumi Okura Deputy Director, Animal Health Division, Food Safety and Consumer Affairs Bureau, Ministry of Agriculture, Forestry and Fisheries, Japan Coordination
Profile on TADs in Japan Country Report Tatsumi Okura Deputy Director, Animal Health Division, Food Safety and Consumer Affairs Bureau, Ministry of Agriculture, Forestry and Fisheries, Japan Coordination
OIE Situation Report for Highly Pathogenic Avian Influenza
 OIE Situation Report for Highly Pathogenic Avian Influenza Latest update: 28/02/2018 The epidemiology of avian influenza is complex. The virus constantly evolves and the behavior of each new subtype (and
OIE Situation Report for Highly Pathogenic Avian Influenza Latest update: 28/02/2018 The epidemiology of avian influenza is complex. The virus constantly evolves and the behavior of each new subtype (and
Trichinosis Table of Contents
 Subsection: Trichinosis Page 1 of 9 Trichinosis Table of Contents Trichinosis Trichinosis (Trichinellosis) Fact Sheet Investigation of Trichinosis Surveillance Case Report (CDC 54.7) Subsection: Trichinosis
Subsection: Trichinosis Page 1 of 9 Trichinosis Table of Contents Trichinosis Trichinosis (Trichinellosis) Fact Sheet Investigation of Trichinosis Surveillance Case Report (CDC 54.7) Subsection: Trichinosis
Update on the dengue situation in the Western Pacific Region
 Dengue Situation Update 448 23 September 214 Update on the dengue situation in the Western Pacific Region Northern Hemisphere Japan As of September 22, Ministry of Health, Labour and Welfare (MHLW), Japan,
Dengue Situation Update 448 23 September 214 Update on the dengue situation in the Western Pacific Region Northern Hemisphere Japan As of September 22, Ministry of Health, Labour and Welfare (MHLW), Japan,
Leptospirosis a zoonotic disease with global impact
 Leptospirosis a zoonotic disease with global impact Richard Zuerner BVF Sveriges lantbruksuniversitet Leptospirosis One of the most common zoonotic diseases known World wide distribution Disease incidence
Leptospirosis a zoonotic disease with global impact Richard Zuerner BVF Sveriges lantbruksuniversitet Leptospirosis One of the most common zoonotic diseases known World wide distribution Disease incidence
Translated version CONTINGENCY PLAN DENGUE FEVER PREVENTION AND RESPONSE IN HOCHIMINH CITY IN 2012
 VIETNAM RED CROSS SOCIETY Hochiminh Chapter Hochiminh City, 20 June 2011 CONTINGENCY PLAN DENGUE FEVER PREVENTION AND RESPONSE IN HOCHIMINH CITY IN 2012 I. Background Following the guideline of Vietnam
VIETNAM RED CROSS SOCIETY Hochiminh Chapter Hochiminh City, 20 June 2011 CONTINGENCY PLAN DENGUE FEVER PREVENTION AND RESPONSE IN HOCHIMINH CITY IN 2012 I. Background Following the guideline of Vietnam
Summary of current outbreak in Guinea, Liberia and Sierra Leone
 ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
Hepatitis E Vaccine Clinical Experience. Mrigendra P. Shrestha
 Hepatitis E Vaccine Clinical Experience Mrigendra P. Shrestha 1 Hepatitis E in Nepal 2 Hepatitis E in Nepal Most common type of acute viral hepatitis Occurs in annual rainy season outbreaks Responsible
Hepatitis E Vaccine Clinical Experience Mrigendra P. Shrestha 1 Hepatitis E in Nepal 2 Hepatitis E in Nepal Most common type of acute viral hepatitis Occurs in annual rainy season outbreaks Responsible
SECTOR ASSESMENT (SUMMARY): HEALTH
 Greater Mekong Subregion Health Security Project RRP REG-48118-002 SECTOR ASSESMENT (SUMMARY): HEALTH A. Sector Performance, Problems, and Opportunities 1. The governments of Cambodia, the Lao PDR, Myanmar,
Greater Mekong Subregion Health Security Project RRP REG-48118-002 SECTOR ASSESMENT (SUMMARY): HEALTH A. Sector Performance, Problems, and Opportunities 1. The governments of Cambodia, the Lao PDR, Myanmar,
Usa Thisyakorn and Chule Thisyakorn
 CHILDHOOD DENGUE DISEASES: A TWENTY YEARS PROSPECTIVE STUDY Usa Thisyakorn and Chule Thisyakorn Department of Pediatrics, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand Abstract. Dengue
CHILDHOOD DENGUE DISEASES: A TWENTY YEARS PROSPECTIVE STUDY Usa Thisyakorn and Chule Thisyakorn Department of Pediatrics, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand Abstract. Dengue
Epidemiology of HAV, HDV and HEV in Belgium
 Epidemiology of HAV, HDV and HEV in Belgium Prof. Dr. Steven Van Gucht National Reference Centre of Hepatitis Viruses B, C, D and E Viral Diseases Scientific Institute of Public Health (WIV-ISP) Brussels
Epidemiology of HAV, HDV and HEV in Belgium Prof. Dr. Steven Van Gucht National Reference Centre of Hepatitis Viruses B, C, D and E Viral Diseases Scientific Institute of Public Health (WIV-ISP) Brussels
Middle East respiratory syndrome coronavirus (MERS-CoV) and Avian Influenza A (H7N9) update
 30 August 2013 Middle East respiratory syndrome coronavirus (MERS-CoV) and Avian Influenza A (H7N9) update Alert and Response Operations International Health Regulations, Alert and Response and Epidemic
30 August 2013 Middle East respiratory syndrome coronavirus (MERS-CoV) and Avian Influenza A (H7N9) update Alert and Response Operations International Health Regulations, Alert and Response and Epidemic
4.3.9 Pandemic Disease
 4.3.9 Pandemic Disease This section describes the location and extent, range of magnitude, past occurrence, future occurrence, and vulnerability assessment for the pandemic disease hazard for Armstrong
4.3.9 Pandemic Disease This section describes the location and extent, range of magnitude, past occurrence, future occurrence, and vulnerability assessment for the pandemic disease hazard for Armstrong
Rift Valley Fever. What is Rift Valley Fever?
 Rift Valley Fever What is Rift Valley Fever? Rift Valley fever (RVF) is a peracute or acute insect-borne disease of man and animals, historically restricted to Africa. An outbreak of RVF in animals frequently
Rift Valley Fever What is Rift Valley Fever? Rift Valley fever (RVF) is a peracute or acute insect-borne disease of man and animals, historically restricted to Africa. An outbreak of RVF in animals frequently
Dengue Stephen J. Thomas, MD Director, Viral Diseases Branch Walter Reed Army Institute of Research (WRAIR) 14 AUG 2012
 Dengue Stephen J. Thomas, MD Director, Viral Diseases Branch Walter Reed Army Institute of Research (WRAIR) 14 AUG 2012 Dengue Lecture Outline Dengue Virus Dengue Epidemiology Military Significance Clinical
Dengue Stephen J. Thomas, MD Director, Viral Diseases Branch Walter Reed Army Institute of Research (WRAIR) 14 AUG 2012 Dengue Lecture Outline Dengue Virus Dengue Epidemiology Military Significance Clinical
Clinical and serological evaluation of leptospirosis in Puducherry, India
 Original Article Clinical and serological evaluation of leptospirosis in Puducherry, India Smita B. Shekatkar, Belgode N. Harish, Godfred A. Menezes and Subhash C. Parija Department of Microbiology, Jawaharlal
Original Article Clinical and serological evaluation of leptospirosis in Puducherry, India Smita B. Shekatkar, Belgode N. Harish, Godfred A. Menezes and Subhash C. Parija Department of Microbiology, Jawaharlal
Dark field Microscopy an important conventional technique for the early diagnosis of Leptospirosis
 ISSN: 2319-7706 Volume 4 Number 6 (2015) pp. 718-722 http://www.ijcmas.com Original Research Article Dark field Microscopy an important conventional technique for the early diagnosis of Leptospirosis N.
ISSN: 2319-7706 Volume 4 Number 6 (2015) pp. 718-722 http://www.ijcmas.com Original Research Article Dark field Microscopy an important conventional technique for the early diagnosis of Leptospirosis N.
DENGUE WITH CENTRAL NERVOUS SYSTEM INVOLVEMENT
 DENGUE WITH CENTRAL NERVOUS SYSTEM INVOLVEMENT Usa Thisyakorn and Chule Thisyakorn Department of Pediatrics, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand Abstract. Dengue has spread
DENGUE WITH CENTRAL NERVOUS SYSTEM INVOLVEMENT Usa Thisyakorn and Chule Thisyakorn Department of Pediatrics, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand Abstract. Dengue has spread
Hand, Foot, and Mouth Disease Situation Update. Hand, Foot, and Mouth Disease surveillance summary
 Hand, Foot, and Mouth Disease Situation Update 24 February 215 Hand, Foot, and Mouth Disease surveillance summary This surveillance summary includes information from countries where transmission of Hand,
Hand, Foot, and Mouth Disease Situation Update 24 February 215 Hand, Foot, and Mouth Disease surveillance summary This surveillance summary includes information from countries where transmission of Hand,
BULLETIN. World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 8 January 2006 ISSN
 BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 8 January
BULLETIN World Health Organization Regional Office for the Western Pacific Expanded Programme on Immunization World Health Organization, Western Pacific Regional Office, Manila, Philippines Issue 8 January
Impacts of Climate Change on Dengue Haemorrhagic Fever Cases in Banjarbaru Municipal, South Kalimantan During the Year
 Impacts of Climate Change on Dengue Haemorrhagic Fever Cases in Banjarbaru Municipal, South Kalimantan During the Year 2005-2010 TIEN ZUBAIDAH * ABSTRACT Environment is one of instrumental factor in the
Impacts of Climate Change on Dengue Haemorrhagic Fever Cases in Banjarbaru Municipal, South Kalimantan During the Year 2005-2010 TIEN ZUBAIDAH * ABSTRACT Environment is one of instrumental factor in the
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
Acute Kidney Injury Due To Leptospirosis-A Cohort Study
 Advances in Bioresearch Adv. Biores., Vol 8 (1) January 2017: 182 187 2017 Society of Education, India Print ISSN 0976 4585; Online ISSN 2277 1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
Advances in Bioresearch Adv. Biores., Vol 8 (1) January 2017: 182 187 2017 Society of Education, India Print ISSN 0976 4585; Online ISSN 2277 1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
Alberta Health and Wellness Public Health Disease Under Surveillance Management Guidelines March 2011
 March 2011 Histoplasmosis Case Definition Confirmed Case Clinical illness [1] with laboratory confirmation of infection: Isolation of Histoplasma capsulatum from an appropriate clinical specimen (tissue
March 2011 Histoplasmosis Case Definition Confirmed Case Clinical illness [1] with laboratory confirmation of infection: Isolation of Histoplasma capsulatum from an appropriate clinical specimen (tissue
Dengue Fever & Dengue Hemorrhagic Fever Annual Reports to WHO
 Dengue Virus Member of the genus Flavivirus Transmitted by the Aedes mosquito; mosquito => human cycle 4 serotypes: DENV1, 2, 3, and 4 Homotypic immunity is long lasting Heterotypic immunity is short lived
Dengue Virus Member of the genus Flavivirus Transmitted by the Aedes mosquito; mosquito => human cycle 4 serotypes: DENV1, 2, 3, and 4 Homotypic immunity is long lasting Heterotypic immunity is short lived
February Emerging Infectious Diseases: The Global Picture
 Emerging Infectious Diseases: The Global Picture Breaches in species barrier: emerging infections in humans Infection Animal linked Year infection to transmission first reported Ebola virus Bats 1976 HIV-1
Emerging Infectious Diseases: The Global Picture Breaches in species barrier: emerging infections in humans Infection Animal linked Year infection to transmission first reported Ebola virus Bats 1976 HIV-1
Are 10-year booster doses of yellow fever vaccine necessary? Peter Teitelbaum, MD Committee to Advise on Tropical Medicine and Travel (CATMAT)
 Are 10-year booster doses of yellow fever vaccine necessary? Peter Teitelbaum, MD Committee to Advise on Tropical Medicine and Travel (CATMAT) Disclosure of Potential for Conflict of Interest Peter Teitelbaum,
Are 10-year booster doses of yellow fever vaccine necessary? Peter Teitelbaum, MD Committee to Advise on Tropical Medicine and Travel (CATMAT) Disclosure of Potential for Conflict of Interest Peter Teitelbaum,
Southeast Asia and China FMD Campaign
 Southeast Asia and China FMD Campaign Ronello C. Abila SEACFMD Regional Coordinator OIE Sub-Regional Representative for SE Asia OUTLINE SEACFMD Campaign FMD Status Risk factors The new SEACFMD Roadmap
Southeast Asia and China FMD Campaign Ronello C. Abila SEACFMD Regional Coordinator OIE Sub-Regional Representative for SE Asia OUTLINE SEACFMD Campaign FMD Status Risk factors The new SEACFMD Roadmap
CDC Cooperative Agreement Influenza Surveillance Review Project Period(Sep 2004-Sep 2011)
 CDC Cooperative Agreement Influenza Surveillance Review Project Period(Sep 2004-Sep 2011) National Institute of Health Department of Medical Sciences, Bureau of Epidemiology Department of Disease Control,
CDC Cooperative Agreement Influenza Surveillance Review Project Period(Sep 2004-Sep 2011) National Institute of Health Department of Medical Sciences, Bureau of Epidemiology Department of Disease Control,
Seroprevalence and Recent Trends of Dengue in a Rural Area in South India
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 36-41 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.005
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 36-41 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.005
OIE Situation Report for Avian Influenza
 OIE Situation Report for Avian Influenza Latest update: 25/01/2018 The epidemiology of avian influenza is complex. The virus constantly evolves and the behavior of each new subtype (and strains within
OIE Situation Report for Avian Influenza Latest update: 25/01/2018 The epidemiology of avian influenza is complex. The virus constantly evolves and the behavior of each new subtype (and strains within
Influenza and the Poultry Link
 Influenza and the Poultry Link Hemagglutinin Neuraminidase Type A Influenza Surface Antigens Subtype Surface Antigens Hemagglutinin 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 human equine swine Neuraminidase
Influenza and the Poultry Link Hemagglutinin Neuraminidase Type A Influenza Surface Antigens Subtype Surface Antigens Hemagglutinin 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 human equine swine Neuraminidase
Forecasting Dengue Hemorrhagic Fever Cases Using Time Series in East Java Province, Indonesia
 Forecasting Dengue Hemorrhagic Fever Cases Using Time Series in East Java Province, Indonesia Hasirun 1, Windhu P 2, Chatarina U. W 3, Avie Sri Harivianti 4 Department of Epidemiologi 1,3, Department of
Forecasting Dengue Hemorrhagic Fever Cases Using Time Series in East Java Province, Indonesia Hasirun 1, Windhu P 2, Chatarina U. W 3, Avie Sri Harivianti 4 Department of Epidemiologi 1,3, Department of
Live Poultry Markets in Bangkok Metropolitan, Thailand: A Survey of H5 & H7 Prevalence in Bird and Worker s vaccination and knowledge
 Live Poultry Markets in Bangkok Metropolitan, Thailand: A Survey of H5 & H7 Prevalence in Bird and Worker s vaccination and knowledge Prabda Praphasiri, DrPH, PhD 29 August 2016 Thailand MOPH U.S. CDC
Live Poultry Markets in Bangkok Metropolitan, Thailand: A Survey of H5 & H7 Prevalence in Bird and Worker s vaccination and knowledge Prabda Praphasiri, DrPH, PhD 29 August 2016 Thailand MOPH U.S. CDC
Western Pacific Regional Office of the World Health Organization WPRO Dengue Situation Update, 2 October 2013 Recent Cumulative No.
 Western Pacific Regional Office of the World Health Organization WPRO Dengue Situation Update, 2 October 2013 http://www.wpro.who.int/emerging_diseases/denguesituationupdates/en/index.html Regional dengue
Western Pacific Regional Office of the World Health Organization WPRO Dengue Situation Update, 2 October 2013 http://www.wpro.who.int/emerging_diseases/denguesituationupdates/en/index.html Regional dengue
A Study on Common Etiologies of Acute Febrile Illness Detectable by Microbiological Tests in a Tertiary Care Hospital
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 7 (2016) pp. 670-674 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.507.076
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 7 (2016) pp. 670-674 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.507.076
Trends of Pandemics in the 21 st Century
 Trends of Pandemics in the 21 st Century 1 H5N1 influenza, Hong Kong, 1997: 18 human infections/6 deaths 500 450 400 350 300 250 200 150 100 50 0 #H5N1 #sampled Parks Live domesticated foul markets Source:
Trends of Pandemics in the 21 st Century 1 H5N1 influenza, Hong Kong, 1997: 18 human infections/6 deaths 500 450 400 350 300 250 200 150 100 50 0 #H5N1 #sampled Parks Live domesticated foul markets Source:
Studies and interventions in animals: Ecoepidemiology of leptospirosis in urban slums
 Studies and interventions in animals: Ecoepidemiology of leptospirosis in urban slums International Workshop of the /FIOCRUZ 5 th GLEAN Meeting November 10, 2015, Rio de Janeiro F Costa, E Wunder, DS Olveira,
Studies and interventions in animals: Ecoepidemiology of leptospirosis in urban slums International Workshop of the /FIOCRUZ 5 th GLEAN Meeting November 10, 2015, Rio de Janeiro F Costa, E Wunder, DS Olveira,
LEPTOSPIROSIS: Working with beef cattle
 INFORMATION SHEET LEPTOSPIROSIS: Working with beef cattle This fact sheet provides information about the risk of leptospirosis infection in people working with beef cattle. KEY POINTS > > Leptospirosis
INFORMATION SHEET LEPTOSPIROSIS: Working with beef cattle This fact sheet provides information about the risk of leptospirosis infection in people working with beef cattle. KEY POINTS > > Leptospirosis
Diarrhoeal disease outbreak investigation in Guadalcanal and Honiara Provinces, September November 2008
 Diarrhoeal disease outbreak investigation in Guadalcanal and Honiara Provinces, September November 2008 This article is an outcome of the field epidemiology or Data for Decision Making (DDM) training undertaken
Diarrhoeal disease outbreak investigation in Guadalcanal and Honiara Provinces, September November 2008 This article is an outcome of the field epidemiology or Data for Decision Making (DDM) training undertaken
The Royal Veterinary College. The Swiss Federal Veterinary Office
 The Royal Veterinary College The Swiss Federal Veterinary Office Schweiz. Arch. Tierheilk. 2008 Vector-borne viral disease of ruminants 24 known serotypes, member of genus Orbivirus Transmitted by midges
The Royal Veterinary College The Swiss Federal Veterinary Office Schweiz. Arch. Tierheilk. 2008 Vector-borne viral disease of ruminants 24 known serotypes, member of genus Orbivirus Transmitted by midges
Assessment of Water, Sanitation, and Hygiene Interventions in Response to an Outbreak of Typhoid Fever in Neno District, Malawi
 Assessment of Water, Sanitation, and Hygiene Interventions in Response to an Outbreak of Typhoid Fever in Neno District, Malawi Sarah D. Bennett, MD, MPH Lieutenant, U.S. Public Health Service April 13,
Assessment of Water, Sanitation, and Hygiene Interventions in Response to an Outbreak of Typhoid Fever in Neno District, Malawi Sarah D. Bennett, MD, MPH Lieutenant, U.S. Public Health Service April 13,
Rift Valley Fever in Saudi Arabia Current Status. Presented by: Bayoumi, F. A. Director of Animal Health Branch Ministry of Agriculture, KSA
 Rift Valley Fever in Saudi Arabia Current Status Presented by: Bayoumi, F. A. Director of Animal Health Branch Ministry of Agriculture, KSA History of the 2000 outbreak In September, 2000 an epizootic
Rift Valley Fever in Saudi Arabia Current Status Presented by: Bayoumi, F. A. Director of Animal Health Branch Ministry of Agriculture, KSA History of the 2000 outbreak In September, 2000 an epizootic
CHOLERA UPDATES in Indonesia
 CHOLERA UPDATES in Indonesia Musal Kadim MD Gastrohepatology Division, Child Health Department, University of Indonesia Indonesian Pediatric Society Cholera epidemiology update History 7 cholera pandemics
CHOLERA UPDATES in Indonesia Musal Kadim MD Gastrohepatology Division, Child Health Department, University of Indonesia Indonesian Pediatric Society Cholera epidemiology update History 7 cholera pandemics
Zika Virus. Centers for Disease Control and Prevention
 Centers for Disease Control and Prevention Zika Virus Ingrid Rabe Medical Epidemiologist Arboviral Diseases Branch Centers for Disease Control and Prevention February 1, 2016 Zika Virus Single stranded
Centers for Disease Control and Prevention Zika Virus Ingrid Rabe Medical Epidemiologist Arboviral Diseases Branch Centers for Disease Control and Prevention February 1, 2016 Zika Virus Single stranded
Auchara Tangsathapornpong 1, Churairat Puriburt 2 and Pornumpa Bunjoungmanee 1
 EPIDEMIOLOGY OF DENGUE AT THAMMASAT UNIVERSITY HOSPITAL DURING 2006-2015 Auchara Tangsathapornpong 1, Churairat Puriburt 2 and Pornumpa Bunjoungmanee 1 1 Department of Pediatrics, Faculty of Medicine,
EPIDEMIOLOGY OF DENGUE AT THAMMASAT UNIVERSITY HOSPITAL DURING 2006-2015 Auchara Tangsathapornpong 1, Churairat Puriburt 2 and Pornumpa Bunjoungmanee 1 1 Department of Pediatrics, Faculty of Medicine,
Deterministic Factors of Thai Cassava Prices: Multi-Uses of Cassava from Food, Feed, and Fuel Affecting on Thai Cassava Price Volatility
 ISSN 2413-0877 Volume 3 (2016) 12-16 ICoA Conference Proceedings, 7 9 November 2015 Deterministic Factors of Thai Cassava Prices: Multi-Uses of Cassava from Food, Feed, and Fuel Affecting on Thai Cassava
ISSN 2413-0877 Volume 3 (2016) 12-16 ICoA Conference Proceedings, 7 9 November 2015 Deterministic Factors of Thai Cassava Prices: Multi-Uses of Cassava from Food, Feed, and Fuel Affecting on Thai Cassava
2.3 Invasive Group A Streptococcal Disease
 2.3 Invasive Group A Streptococcal Disease Summary Total number of cases, 2015 = 107 Crude incidence rate, 2015 = 2.3 per 100,000 population Notifications In 2015, 107 cases of invasive group A streptococcal
2.3 Invasive Group A Streptococcal Disease Summary Total number of cases, 2015 = 107 Crude incidence rate, 2015 = 2.3 per 100,000 population Notifications In 2015, 107 cases of invasive group A streptococcal
Epidemiologic and Clinical Features of Measles and Rubella in a Rural Area in China
 ORIGINAL ARTICLE Epidemiologic and Clinical Features of Measles and Rubella in a Rural Area in China Youwang Yan* Health Bureau of Jingzhou District, Jingzhou City, Hubei Province, People s Republic of
ORIGINAL ARTICLE Epidemiologic and Clinical Features of Measles and Rubella in a Rural Area in China Youwang Yan* Health Bureau of Jingzhou District, Jingzhou City, Hubei Province, People s Republic of
AVIAN INFLUENZA (A/H5N1) SITUATION IN VIETNAM, National Institute of Hygiene and Epidemiology
 AVIAN INFLUENZA (A/H5N1) SITUATION IN VIETNAM, 2003-2005 National Institute of Hygiene and Epidemiology General Information Area: 332,600 km2 Provinces: 64 Districts: 668 Communes/wards: 10,732 Population:
AVIAN INFLUENZA (A/H5N1) SITUATION IN VIETNAM, 2003-2005 National Institute of Hygiene and Epidemiology General Information Area: 332,600 km2 Provinces: 64 Districts: 668 Communes/wards: 10,732 Population:
Control of DHF Outbreak in Cambodia, 1998
 By Ngan Chantha, P. Guyant, S. Hoyer National Malaria Centre, 372 Monivong Boulevard, Phnom Penh, Cambodia Abstract In January 1998, an unprecedented dry-season outbreak of dengue haemorrhagic fever (DHF)
By Ngan Chantha, P. Guyant, S. Hoyer National Malaria Centre, 372 Monivong Boulevard, Phnom Penh, Cambodia Abstract In January 1998, an unprecedented dry-season outbreak of dengue haemorrhagic fever (DHF)
