University of Groningen
|
|
|
- Bertina Walsh
- 6 years ago
- Views:
Transcription
1 University of Groningen Implant decontamination during surgical peri-implantitis treatment de Waal, Yvonne; Raghoebar, Gerry; Slater, J.J.R.; Meijer, Hendrikus; Winkel, Edwin; van Winkelhoff, Arie Jan Published in: Journal of Clinical Periodontology IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document Version Publisher's PDF, also known as Version of record Publication date: 2012 Link to publication in University of Groningen/UMCG research database Citation for published version (APA): de Waal, Y. C. M., Raghoebar, G. M., Slater, J. J. R., Meijer, H., Winkel, E. G., & Winkelhoff, A. J. V. (2012). Implant decontamination during surgical peri-implantitis treatment: a randomized, double-blind, placebo-controlled trial. Journal of Clinical Periodontology, 40(2), Copyright Other than for strictly personal use, it is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), unless the work is under an open content license (like Creative Commons). Take-down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from the University of Groningen/UMCG research database (Pure): For technical reasons the number of authors shown on this cover page is limited to 10 maximum. Download date:
2 J Clin Periodontol 2013; 40: doi: /jcpe Implant decontamination during surgical peri-implantitis treatment: a randomized, double-blind, placebo-controlled trial Yvonne C. M. de Waal 1, Gerry M. Raghoebar 2, James J. R. Huddleston Slater 1,2, Henny J. A. Meijer 1,2, Edwin G. Winkel 1 and Arie Jan van Winkelhoff 1,3 1 Center for Dentistry and Oral Hygiene, University Medical Center Groningen, University of Groningen, Groningen, The Netherlands; 2 Department of Oral and Maxillofacial Surgery, University Medical Center Groningen, University of Groningen, Groningen, The Netherlands; 3 Department of Medical and Oral Microbiology, University Medical Center Groningen, University of Groningen, Groningen, The Netherlands de Waal YCM, Raghoebar GM, Huddleston Slater JJR, Meijer HJA, Winkel EG, Jan van Winkelhoff A. Implant decontamination during surgical peri-implantitis treatment: a randomized, double-blind, placebo-controlled trial. J Clin Periodontol 2013; 40: doi: /jcpe Abstract Aim: The objective of this randomized, double-blind, placebo-controlled trial was to study the effect of implant surface decontamination with chlorhexidine (CHX)/ cetylpyridinium chloride (CPC) on microbiological and clinical parameters. Material & Methods: Thirty patients (79 implants) with peri-implantitis were treated with resective surgical treatment consisting of apically re-positioned flap, bone recontouring and surface debridement and decontamination. Patients were randomly allocated to decontamination with 0.12% CHX % CPC (test-group) or a placebo-solution (without CHX/CPC, placebo-group). Microbiological parameters were recorded during surgery; clinical and radiographical parameters were recorded before (pre-) treatment (baseline), and at 3, 6 and 12 months after treatment. Results: Nine implants in two patients in the placebo-group were lost due to severe persisting peri-implantitis. Both decontamination procedures resulted in significant reductions of bacterial load on the implant surface, but the test-group showed a significantly greater reduction than the placebo-group (log versus log , p = 0.006). Multilevel analysis showed no differences between both groups in the effect of the intervention on bleeding, suppuration, probing pocket depth and radiographical bone loss over time. Conclusion: Implant surface decontamination with 0.12% CHX % CPC in resective surgical treatment of peri-implantitis leads to a greater immediate suppression of anaerobic bacteria on the implant surface than a placebo-solution, but does not lead to superior clinical results. The long-term microbiological effect remains unknown. Key words: cetylpyridinium chloride; chlorhexidine; decontamination; microbiology; peri-implantitis; resective surgery Accepted for publication 1 October 2012 Conflict of interest and source of funding statement The authors declare that they have no conflict of interest. The test- and placebo-solutions were provided for free by Dentaid SL (Cerdanyola, Spain). 186 The principal objectives for treatment of peri-implantitis are resolution of inflammation and preservation of supporting bone. If non-surgical therapy does not resolve the inflammatory lesion, access flap surgery is recommended (Lindhe & Meyle 2008). Surgical access to the peri-implantitis lesion allows for proper removal of granulation tissue and exposes the implant surface for debridement and decontamination. The clinical effects of access surgery combined with surface debridement
3 Implant surface decontamination 187 and decontamination have been investigated in only a few studies (Leonhardt et al. 2003, Maximo et al. 2009, Heitz-Mayfield et al. 2012). Three other studies have evaluated resective surgical procedures, for example, apically re-positioned flap, bone re-contouring and/or implantoplasty, combined with debridement and decontamination of the implant surface (Romeo et al. 2005, Deppe et al. 2007, Serino & Turri 2011). Most of these studies included adjunctive systemic antibiotic therapy in their treatment protocol. Different protocols, materials and chemical compounds for decontamination of the implant surface have been used, including 10% hydrogen peroxide (Leonhardt et al. 2003), teflon curettes and abrasive sodium carbonate air-powder (Maximo et al. 2009), titanium coated curettes and surgical gauzes soaked in saline (Heitz- Mayfield et al. 2012), metronidazole gel and a tetracycline hydrochloride solution (Romeo et al. 2005), air-powder abrasive alone or in combination with CO 2 laser irradiation (Deppe et al. 2007) and an ultrasonic instrument and rotating rubber cup under chlorhexidine (CHX) irrigation (Serino & Turri 2011). Due to the wide variation in materials and procedures that have been described for the treatment of periimplantitis, it is difficult to discriminate between effective and ineffective (components of) interventions. Therefore, it has been suggested that it may be necessary to start assessing simple interventions using a double-blind study design before gradually testing more complex treatments (Esposito et al. 2012). Future studies should compare two treatment protocols that differentiate only on one component of the intervention. So far, only two randomized controlled trials, comparing different protocols for debridement and decontamination of the implant surface and combined surgical treatment of peri-implantitis, were published (Romeo et al. 2005, Schwarz et al. 2011). Modification of surface topography (implantoplasty) when combined with resective surgery seems to positively influence implant survival and clinical parameters such as peri-implant pocket depth, suppuration and sulcus bleeding (Romeo et al. 2005). In the second randomized controlled trial, implantoplasty was used as an adjunct to regenerative surgical procedures (Schwarz et al. 2011, 2012). The method of surface debridement and decontamination (Er:YAG laser versus plastic curets + cotton pellets + sterile saline) did not significantly impact the clinical outcomes, neither after 6 months nor after 2 years. Unfortunately, in both studies, the microbiological effects of the surface modification/ decontamination procedures were not assessed. As peri-implantitis is an infectious disease (Lindhe & Meyle 2008, Zitzmann & Berglundh 2008), it seems logical to focus on anti-infective measures. The screw-shaped design of implants and the various implant surface modifications may limit the effect of mechanical debridement of implant surfaces and may advocate the use of additional therapies, such as antibiotics or antiseptics. An in vivo study showed that the antiseptics chlorhexidine, sodium hypochlorite, hydrogen peroxide, essential oils and citric acid may have some beneficial effect in reducing the bacterial load on titanium surfaces and may improve peri-implantitis therapy (Gosau et al. 2010). CHX has broad antibacterial activity and, for periodontal diseases, has welldocumented clinical efficacy and plaque-reducing capabilities [for reviews see: (Addy 1986, Jones 1997)]. The objective of this study was to study the microbiological, clinical and radiographical effect of implant surface decontamination by a CHX/ cetylpyridinium chloride (CPC) solution in comparison to a placebosolution in resective surgical treatment of peri-implantitis. It was hypothesized that no differences would exist in reduction of counts of anaerobic bacteria on the implant surface between the two decontamination procedures. Material and Methods Participants Participants were consecutively recruited from patients referred for treatment of peri-implantitis to the University Medical Center Groningen, the Netherlands. Written informed consent was obtained from all participants before entering the trial. Inclusion- and exclusion criteria are depicted in Fig. 1. Peri-implantitis was defined as bleeding and/or suppuration on probing combined with a peri-implant probing pocket depth (PPD) 5 mm and bone loss 2 mm. The study took place between October 2009 and September The study has been conducted in full accordance with the World Medical Association Declaration of Helsinki (version 2008) and was approved by the Institutional Review Board of the University Medical Center Groningen, the Netherlands (METc ). US National Institutes of Health clinical trial registration was done at www. ClinicalTrials.gov (NCT ). The CONSORT guidelines for reporting a clinical trial were followed (Moher et al. 2010, Schulz et al. 2010, Cairo et al. 2012). Trial design This study is a randomized, doubleblind and placebo-controlled trial evaluating the microbiological, clinical and radiographical outcomes of resective surgical treatment of periimplantitis combined with decontamination of the implant surface using 0.12% CHX % CPC or a placebo-solution. Follow-up time was 12 months. Patients were randomly assigned to either the test- or placebo-group using a one-to-one allocation ratio. Randomization Fifteen notes with the words solution A and 15 notes with solution B were put into 30 identical, sequentially numbered, non-transparent envelopes according to a computer generated randomization list with a permuted block design (fixed block sizes of four). No stratification was performed. All envelopes were irreversibly sealed, only to be opened by the surgical assistant during the surgical procedure. According to the information on the note, the surgical assistant prepared a syringe with either solution A or solution B and was unaware of the composition of the solution. This information was stored and kept by an independent person not involved in the study. The placebo-solution was matched to the CHX-solution for taste, smell, colour and viscosity, ensuring blinding of the assistant, the surgeon, the patient and the investigator to treatment allocation.
4 188 de Waal et al. Intervention Presence of 1 endosseous dental implant with clinical and radiographical signs of peri-implantitis (peri-implantitis defined as: bleeding and/or suppuration on probing, peri-implant probing pocket depth 5 mm and bone loss 2 mm); Implant function time 2 years. Medical and general contra-indications for the surgical procedures; A history of radiotherapy to the head and neck region; Pregnancy and lactation; Insuline-dependent diabetes; Use of antibiotics during the last 3 months; Incapability to perform basal oral hygiene measures due to physical or mental disorders; Active, uncontrolled periodontal infections of the natural dentition (PPD > 5 mm); Implants with bone loss exceeding 2/3 of the length of the implant or implants with bone loss beyond any transverse openings in hollow implants; Implant mobility; Implants at which no position could be identified where proper probing measurements could be performed; Previous surgical treatment of the peri-implantitis lesions. Fig. 1. Inclusion- and exclusion criteria. Before the surgical procedure, all patients received extensive oral hygiene instructions and mechanical debridement of implants, suprastructures and remaining dentition. Patients were all surgically treated by one experienced oral- and maxillofacial surgeon (GR). Suprastructures were removed if reasonably possible (in all but eight patients). Incisions were made using a surgical blade (no. 15) under local anaesthesia. Flaps were designed to allow optimal access to the periimplant bone defect for granulation tissue removal and debridement and decontamination of the implant surface. Vertical releasing incisions extending into the alveolar mucosa were placed at the mesial and distal aspects of the horizontal incision. Full thickness mucoperiosteal flaps were raised buccally and lingually. Granulation tissue was removed using curettes (Gracey; Hu-Friedy, Chicago, IL, USA). Bone re-contouring, aimed at eliminating angular bony defects, was performed using a rotating round bur under saline irrigation. The implant surface was mechanically cleaned using surgical gauzes soaked in saline. After mechanical debridement, patients were randomly allocated to either the placebo- or the test-group. After treatment allocation, the implant surface was rinsed for 1 min with 0.12% CHX % CPC without alcohol (Perioaid; Dentaid SL, Cerdanyola, Spain) (test-group) or with the placebo-solution (placebo-group). Test- and placebo-solutions were prepared and distributed by Dentaid SL. The placebo-solution contained the same ingredients as the test-solution, except for CHX and CPC. Care was taken to continuously cover the implant surface with the solution. This was achieved by continuous irrigation and refreshment of the solution using a syringe with a 22 gauge needle to ensure penetration into deep bony defects. Subsequently, the implant surface was rinsed with abundant amounts of sterile saline for 1 min. Suprastructures were re-positioned and mucosal flaps were apically positioned and firmly sutured (Vicryl Plus 3-0; Ethicon Inc., Somerville, NJ, USA). For both placebo- and test-group, surgery was followed by 2 weeks of mouth rinsing with 0.12% CHX % CPC without alcohol (Perioaid; Dentaid SL) two times daily during 30 s. Sutures were removed after 2 weeks. During follow-up examinations, patients were re-instructed in oral hygiene measures and implants and teeth were cleaned as necessary. Follow-up visits were scheduled after 3 (T 3 ), 6 (T 6 )and12(t 12 )months. Outcomes Primary outcome The primary outcome variable was the difference in anaerobic bacterial load of the implant surface before and after mechanical and chemical debridement and decontamination. After flap deflection and granulation tissue removal, a sample was obtained from the implant surface by rubbing a sterilized brush (Microbrush International, Grafton, WI, USA) across the implant surface (T pre ). A second sample was obtained after mechanical debridement and rinsing of the implant surface with the test- or placebo-solution and saline (T post ). The top part of the brush was cut-off and collected in a vial containing reduced transport fluid (Syed & Loesche 1972). Separate samples were obtained from every implant presenting peri-implantitis. All microbiological samples were processed within 24 h as described by Van Winkelhoff et al. (1985) and Van Steenbergen et al. (1986). Total anaerobic bacterial load and presence and numbers of the putative periodontal pathogens Aggregatibacter actinomycetemcomitans, Porphyromonas gingivalis, Prevotella intermedia, Tannerella forsythia, Fusobacterium nucleatum, Parvimonas micra and Campylobacter rectus were determined by laboratory technicianswhowereblindtotreatmentallocation. Secondary outcomes Secondary outcome parameters were presence of plaque (% sites plaque), bleeding on probing (% sites BoP), suppuration on probing (% sites
5 Implant surface decontamination 189 SoP), mean PPD and mean radiographical marginal bone loss. Measurements were performed before (pre-) treatment (baseline, T 0 ) and at 3, 6 and 12 months after surgery (T 3, T 6 and T 12 ) by one and the same experienced examiner (YDW) who was blind to treatment allocation. Presence of plaque was assessed (present/absent) at four sites per implant (mesial, buccal, distal and lingual) by running a probe across the marginal surface of the implant/ suprastructure. Peri-implant pocket probing was performed at four sites per implant using a pressure sensitive probe (probe force of 0.25 N; KerrHawe Click Probe, Bioggo, Switzerland). PPD was scored to the nearest millimetre. Up to 30 s after pocket probing, the presence or absence of bleeding and suppuration were assessed. Reproducibility of probing pocket depth measurements was assessed by evaluating 20 implants in eight subjects on two separate occasions, 1 week apart and calculating the linear weighted kappa (j) value. Intra-oral radiographs were obtained using an aiming device and the long cone paralleling technique. Care was taken to position the film parallel to the long axis of the implant. Due to anatomical restrictions, in nine fully edentulous patients (16 implants) no intra-oral radiographs could be obtained without pain or major distortion of the image. In these patients, orthopantomograms were taken. All radiographs were digital. Measurements were performed using Adobe Photoshop (version ; Adobe Systems Incorporated, San Jose, CA, USA). The radiographs were calibrated using the known dimensions of the implant as reference values. A horizontal line was drawn through the shoulder of the implant and the distance from this line to the first bone-to-implant contact was measured at the mesial and distal site. Bone loss was assessed with regard to the position at which the bone is normally positioned, taking into account the different implant types and brands. Reproducibility of radiographical examinations was assessed by evaluating radiographical images of 20 implants (10 intra-oral radiographs and 10 orthopantomograms) twice with a 1-week interval. Intra-class correlation coefficients were calculated for both categories of radiographs. Statistical methods Sample size calculation From the literature, no data were available for estimating the effect size. However, the microbiological effect of rinsing the dental implant surface with a CHX-solution versus rinsing with a placebo-solution was expected to be large. To detect a difference of 1 standard deviation (assumed to be unknown and equal) between both groups under the null hypothesis that both group means were 0.0, with a significance level (a) of 0.05 and a power (b) of 80% using a two-sided two-sample t-test, required group sample sizes of 15 (G*Power Version 3.1.0; University of Kiel, Kiel, Germany). As no compensation for patient withdrawal or losses to follow-up was required (data regarding primary outcome variable was collected during surgical treatment), a sample size of 30 patients was chosen (15 per group). Statistical analysis Total anaerobic bacterial load at baseline (T pre ) was distributed normally after logarithmic transformation. To compare outcomes between placebo- and test-group, linear regression analysis was performed. Baseline values and implant surface roughness were included in the regression model. For comparison of within-group differences in detection frequency of single bacterial species between T pre and T post, the McNemar test was used. Betweengroup differences at T post were analysed using the Fisher s exact test. As the primary outcome variable is a measure of the local effect of decontamination, the implant (and not the patient) was taken as the statistical unit, despite the fact that multiple implants were present per patient. To correct for the within patient dependency, multilevel modelling was used to determine the effect of the intervention over time (test-group versus placebo-group) on the secondary outcome variables. A multilevel hierarchical three-level structure was chosen with three levels of analysis being timing of follow-up measurements (level 1), implant (level 2) and patient (level 3). Baseline values of BoP, SoP, PPD and marginal bone loss (continuous variables), smoking, dental status and history of periodontitis (dichotomous variables) and implant surface roughness (categorical variable) were a priori identified as potential confounders. For each outcome variable two analyses were performed (Twisk 2006). With the crude analysis the effect of the intervention over time was determined, while controlling for baseline value and time. Since follow-up was conducted at irregularly spaced time intervals and not completely similar for each patient, time was included in the crude model (Ridgers et al. 2007). In the adjusted analysis, the potential confounders smoking, dental status, history of periodontitis and implant surface roughness were additionally included in the model. Descriptive data and data regarding the primary outcome variable were analysed using PASW Statistics 18 (version ; SPSS inc., Chicago, IL, USA). Multilevel models were analysed using MLwiN version 2.12 (Centre for Multilevel Modeling, University of Bristol, Bristol, UK). Results The flow of the participants throughout the different phases of the study is depicted in Fig. 2. Eligible patients were recruited from October 2009 to September 2010 and were followed 3, 6 and 12 months after the surgical procedure. The baseline demographic patient and implant characteristics are reported in Table 1. Thirty patients with a total of 79 implants with peri-implantitis were included. Primary outcome The log-transformed mean anaerobic bacterial load of the culture positive implants for the placebo- and testgroup before and after debridement and decontamination of the implant surface are depicted in Table 2. Sixty of the 79 sampled implant surfaces appeared culture positive after exposure and removal of granulation tissue (T pre ). In both groups, the decontamination procedure resulted
6 190 de Waal et al. Assessed for eligibility (n = 55) Excluded (n = 25) Not meeting inclusion criteria (n = 20) Declined to participate (n = 5) Randomized (n = 30) Allocated to placebo-group (n = 15 subjects, 48 implants) Received allocated intervention (n = 15) Did not receive allocated intervention (n = 0) Allocated to test-group (CHX) (n = 15 subjects, 31 implants) Received allocated intervention (n = 15) Did not receive allocated intervention (n = 0) Lost to follow-up (n = 0) Discontinued intervention (n = 3 subjects, 10 implants) Lost to follow-up (n = 0) Discontinued intervention (n = 0) 1 subject/1 implant: implant fracture between surgery and T 3 1 subject/7 implants: all implants removed after T 6 due to persisting peri-implantitis 1 subject/2 implants: 2 out of 3 implants removed after T 6 due to persisting periimplantitis Analysed for primary and secondary outcomes, intention to treat analysis (n = 15 subjects, 48 implants) Analysed for primary and secondary outcomes, intention to treat analysis (n = 15 subjects, 31 implants) Fig. 2. Flow-diagram. in a significant reduction of the bacterial load on the implant surface, although the test-group showed a significantly greater reduction than the placebo-group ( versus , p = 0.006). The number of implants culture positive for the selected periodontal pathogens before and after decontamination are depicted in Table 3. A. actinomycetemcomitans was not detected on any of the implant surfaces. Both decontamination procedures resulted in reduction below detection level of P. gingivalis and P. intermedia and in significant reductions in detection frequencies of T. forsythia, F. nucleatum, P. micra and C. rectus. No differences were observed between both groups. Secondary outcomes One implant (machined surface; Nobel Biocare AG, Zu rich, Switzerland) in one patient (with no other implants affected by periimplantitis) was lost due to implant fracture between surgery and T 3.No signs of fracture were present during the surgical procedure. Nine implants in two patients from the placebogroup had to be removed between T 6 and T 12 due to severe persisting periimplantitis. One patient lost all seven treated implants (Nobel Biocare, Ti-Unite surface) and discontinued the study. The other patient lost 2 of 3 treated implants (Straumann AG, Basel, Switzerland, TPS surface), but continued the study with the remaining implant. No implants were lost in
7 Implant surface decontamination 191 Table 1. Baseline demographic characteristics of included subjects/implants Characteristics Placebo Test Number of patients Age [years; mean (SD)] 61.5 (10.0) 59.4 (14.0) Gender; M (male), F (female) M 5, F 10 M 5, F 10 Smoking; n subjects (%) Never (or quit smoking before implant 7 (46.7) 8 (53.3) placement) Former (quit smoking after implant 1 (6.7) 3 (20.0) placement) Current 7 (46.7) 4 (26.7) History of periodontitis; n subjects (%) 5 (33.3) 6 (40.0) Dental status; n subjects (%) Fully edentulous 9 (60.0) 10* (66.7) Partially edentulous 6 (40.0) 5 (33.3) Total number of implants (range) 63 (2 10) 58 (1 10) Number of implants presenting 48 (1 7) 31 (1 5) peri-implantitis (range) Time in function [years; mean (SD)] 8.6 (5.5) 9.2 (3.8) Implant surface; n implants (%) Nobel Biocare Machined surface 1 (2.1) 4 (12.9) Porous anodized surface, TiUnite 21 (43.8) 6 (19.4) Straumann Titanium plasma-sprayed, TPS 5 (10.4) 0 (0) Sandblasted large grit acid-etched, SLA 4 (8.3) 14 (45.2) Sandblasted large grit acid-etched, SLActive 10 (20.8) 1 (3.2) IMZ Titanium plasma-sprayed 7 (14.6) 2 (6.5) Astra Tech Fluoride-modified titanium dioxide grit-blasted, Osseospeed the test-group. The patients from both groups attended all follow-up visits and no patient was lost to follow-up. Descriptive statistics of the clinical and radiographical outcomes at baseline and at different follow-up visits are depicted in Table 4. Data are reported at implant level and, in more detail, on different sites per implant. Intraexaminer reproducibility of clinical measurements was good as indicated by a linear weighted kappa (j) value of Intra-class correlation coefficients were 0.99 and 0.96 for radiographical measurements on intra-oral 0 (0) 2 (6.5) Dentsply Friadent Grit-blasted acid-etched, Friadent plus 0 (0) 2 (6.5) Type of restoration; n implants involved (%) Single crown 4 (8.3) 2 (6.5) Fixed partial denture 4 (8.3) 1 (3.2) Fixed full denture 7 (14.5) 6 (19.4) Overdenture 33 (68.8) 22 (71.0) Screw- or cement-retained restoration; n implants involved (%) Screw-retained 44 (91.7) 28 (90.3) Cement-retained 4 (8.3) 3 (9.7) Implants placed in maxilla or mandible; n implants (%) Maxilla 24 (50.0) 20 (64.5) Mandible 24 (50.0) 11 (35.5) *3 were partially edentulous at the time of implant placement. radiographs and orthopantomograms, respectively, indicating very good intra-examiner reproducibility. Clinical improvements occurred in both the test- and placebo-group, as indicated by the reduction in percentage of sites with BoP and/or SoP and reduction in mean PPD. However, at T 12 almost all implants still showed at least one site with BoP (95.7%) and a substantial number of implants showed signs of suppuration (nine implants in test-group, six of remaining implants in placebo-group). The results from the multilevel modelling analysis regarding the effect of the intervention on BoP, SoP, PPD and radiographical marginal bone loss across time are shown in Table 5. No significant differences were observed between both groups for all investigated secondary parameters, both in the crude and adjusted model. Smoking, dental status (fully versus partially edentulous), history of periodontitis and implant surface roughness are confounders to the crude model. Discussion To our knowledge, this is the first randomized, double-blind, placebocontrolled trial evaluating the microbiological, clinical and radiographical effect of an implant surface decontamination procedure combined with resective surgical treatment of periimplantitis. The results of this study indicate that decontaminating the implant surface with 0.12% CHX % CPC leads to a greater reduction of the anaerobic bacterial load on the implant surface than using a placebo-solution. Therefore, the null hypothesis of no difference can be rejected. However, this greater reduction in bacterial load did not lead to superior clinical or radiographical results over a period of 12 months. These findings are consistent with Schwarz et al. (2011, 2012) who did not find an impact of the method of surface debridement and decontamination on the clinical outcomes following combined surgical therapy of advanced peri-implantitis lesions. It was suggested that the long-term stability of the clinical outcomes may be influence by factors other than the method of surface debridement and decontamination. Chlorhexidine is considered the gold standard for oral antiseptics (Addy 1986, Jones 1997). It has been widely used and extensively tested and has a broad spectrum of antibacterial activity including grampositive and gram-negative bacteria (Jones 1997). From the literature, no comparable studies are available evaluating the immediate microbiological effect of an antiseptic agent on a genuine peri-implantitis-associated biofilm. However, an in vivo study showed that chlorhexidine, among other antiseptics such as sodium hypochlorite, hydrogen peroxide,
8 192 de Waal et al. Table 2. Log-transformed mean bacterial anaerobic counts (SD) of culture positive implants for the placebo- and test-group before (T pre ) and after (T post ) debridement and decontamination of the implant surface N = 60* Placebo 5.54 (1.23) [35] Test 5.46 (1.13) [25] Total anaerobic bacterial load logtransformed mean (SD) T pre T post Difference 2.77 (2.37) [21] 1.25 (2.11) [7] essential oils and citric acid, may have some beneficial effect in reducing the bacterial load on titanium surfaces and may improve peri-implantitis therapy (Gosau et al. 2010). The antibacterial mode of action is based on the ability of the cationic CHX-molecule to rapidly get attracted by the negatively charged bacterial cell surface (R olla & Melsen 1975). Upon interaction, the integrity of the bacterial cell membrane is altered, which leads to leakage and eventually to destruction of the cell (Russell 1986). CHX does not distinguish between bacterial and non-bacterial proteins found in 2.77 (2.12) 4.21 (1.89) b (95% CI) p-value 1.57 ( 2.68 to 0.46) *Implants with baseline values of 0 excluded from analysis. Linear regression analysis, adjusted for baseline values and implant surface roughness. Statistically significant difference. [n], number of culture positive implants. Table 3. Number of culture positive implants of selected periodontal pathogens and mean (SD) percentage of total anaerobic bacterial load on culture positive implants for the placebo- and test-group before (T pre ) and after (T post ) debridement and decontamination of the implant surface N = 60* Placebo (n = 35) Test (n = 25) T pre T post T pre T post Aa n % Pg n % 63.0 (32.2) 31.0 (36.6) Pi n % 2.5 (0.7) 6.0 Tf n 13 3 [1] 7 1 [1] % 9.9 (17.0) 10.0 (9.2) 4.7 (3.3) 2.0 Fn n 20 6 [1] 19 3 [1] % 9.0 (9.9) 16.7 (19.9) 12.7 (13.1) 32.7 (30.1) Pm n % 12.8 (9.8) 30.8 (33.8) 19.1 (11.9) 24.0 (24.3) Cr n [1] % 7.5 (7.7) 22.0 (14.1) 11.8 (9.8) 4.0 *Implants with baseline values of 0 excluded from analysis. Significant change from baseline p < 0.05 (McNemar test). There were no significant differences between both groups after debridement and decontamination (Fisher s exact test). Aa, Aggregatibacter actinomycetemcomitans; Pg, Porphyromonas gingivalis; Pi, Prevotella intermedia; Tf, Tannerella forsythia; Fn, Fusobacterium nucleatum; Pm, Parvimonas micra; Cr, Campylobacter rectus; [n], number of implants culture negative at baseline but culture positive after decontamination. mature plaque (Jones 1997). Therefore, to remove extraneous protein and thereby optimize the effectiveness of the CHX-solution, we first mechanically cleaned the implant surface using gauzes soaked in saline. Furthermore, to optimize the penetration on rough implant surfaces, at sites away from application and in deep bony defects, a rinse was chosen as mode of application rather than a gel. One of the main advantages of CHX is its property of substantivity, which leads to prolonged activity (Addy 1986, Kuyyakanond & Quesnel 1992). However, in vitro studies have shown that CHX can be highly cytotoxic on fibroblasts, endothelial and osteoblastic cells (Babich et al. 1995, Cabral & Fernandes 2007, Giannelli et al. 2008). The cell damaged induced by CHX is concentration and time-dependent and might negatively interfere with the early healing phase of oral diseases (Giannelli et al. 2008). To minimize any possible negative side effects of CHX, it was decided to rinse the implant surface and wound area with copious amounts of saline immediately after CHX-rinsing. As a consequence, by washing out the wound area, the potential benefits resulting from CHX-substantivity may have also diminished. The commercially available CHXsolution used in this study also contained CPC as active ingredient. CPC is a cationic agent and has a broad antimicrobial spectrum with bactericidal effect on gram-positive pathogens and yeast in particular (Pitten & Kramer 2001). CPC has a strong immediate bactericidal effect, but lower residual effect compared with CHX (Pitten & Kramer 1999). It has been shown that the non-alcoholic formulation of 0.12% CHX % CPC is an equally effective anti-plaque and anti-inflammatory agent as the 0.2% CHX mouthrinse with alcohol (Quirynen et al. 2001). In addition, Herrera et al. (2003) showed that the re-formulation and addition of 0.05% CPC to 0.12% CHX products may not only compensate for the absence of alcohol but may rather increase the in vitro and in vivo antimicrobial activity. Both CHX + alcohol and CHX + CPC showed high antimicrobial activity to 20 bacterial species, including periodontal pathogens. In this study, microbiological samples were collected using sterilized microbrushes. These were small enough to reach the areas between implant threads, but robust enough to allow rubbing of the implant surface. As the local and immediate microbiological effect of the decontamination procedure was evaluated, data were analysed on implant level. Microbiological parameters were not assessed over time. The clinical and radiographical data were analysed using a multi-level model. By using multilevel modelling, a correction is made for the difference in number of
9 Table 4. Descriptive statistics of clinical and radiographical parameters N = 79 Placebo Test T 0 (n = 48) T 3 (n = 47) T 6 (n = 47) T 12 (n = 38) T 0 (n = 31) T 3 (n = 31) T 6 (n = 31) T 12 (n = 31) Plaque % of sites (SD) 17.7 (26.3) 17.6 (22.7) 28.7 (28.5) 15.8 (17.8) 9.7 (30.1) 17.7 (27.5) 18.6 (24.1) 12.9 (19.2) % of implants (n) 41.7 (20) 46.8 (22) 66.0 (31) 50.0 (19) 9.7 (3) 35.5 (11) 48.4 (15) 38.7 (12) BoP % of sites (SD) 79.7 (28.1) 62.6 (33.3) 60.1 (32.0) 57.2 (29.0) 80.4 (26.5) 69.4 (27.9) 54.0 (36.6) 60.5 (30.1) % of implants (n) 95.8 (46) 91.5 (43) 91.5 (43) 94.7 (36) 96.8 (30) 96.8 (30) 80.6 (25) 96.8 (30) SoP % of sites (SD) 14.6 (25.2) 1.6 (6.2) 4.4 (11.2) 5.9 (14.7) 31.7 (31.6) 0.8 (4.5) 5.6 (12.4) 14.5 (28.0) % of implants (n) 31.3 (15) 6.4 (3) 14.9 (7) 15.8 (6) 64.5 (20) 3.2 (1) 19.4 (6) 29.0 (9) PPD Mean (SD) 5.5 (1.4) 4.0 (1.3) 4.1 (1.4) 3.7 (0.8) 6.6 (1.6) 4.2 (1.5) 4.0 (1.5) 4.3 (2.1) PPD 5 mm % of sites (SD) 75.2 (26.1) 26.2 (31.6) 29.6 (35.0) 17.1 (24.0) 88.2 (18.4) 39.5 (36.4) 33.1 (31.9) 33.9 (39.0) % of implants (n) 100 (48) 51.1 (24) 55.3 (26) 47.4 (17) 100 (31) 64.5 (20) 67.7 (21) 54.8 (17) PPD 6 mm % of sites (SD) 49.0 (33.8) 16.5 (29.0) 14.4 (30.0) 7.2 (19.2) 57.0 (33.5) 21.8 (34.0) 17.7 (30.4) 20.2 (35.0) % of implants (n) 81.3 (39) 31.9 (15) 25.6 (12) 15.8 (6) 87.1 (27) 35.5 (11) 32.3 (10) 32.3 (10) PPD 5 mm + % of sites (SD) 70.0 (30.4) 23.6 (30.9) 25.4 (34.1) 15.8 (23.6) 80.1 (23.0) 36.3 (32.8) 23.4 (30.9) 29.0 (37.1) BoP/SoP (same site) % of implants (n) 95.8 (46) 46.8 (22) 48.9 (23) 42.1 (16) 100 (31) 64.5 (20) 48.4 (15) 48.4 (15) PPD 6 mm + % of sites (SD) 46.9 (33.7) 16.0 (29.1) 14.4 (30.0) 7.2 (19.2) 54.6 (33.7) 19.4 (30.1) 14.5 (27.2) 17.7 (34.3) BoP/SoP (same site) % of implants (n) 81.3 (39) 29.8 (14) 25.5 (12) 15.8 (6) 87.1 (27) 35.5 (11) 32.3 (10) 25.8 (8) Marginal bone loss Mean (SD) 3.6 (1.9) 4.0 (2.0) 4.3 (2.2) 3.9 (2.0) 4.3 (2.1) 4.7 (2.2) 4.9 (2.4) 5.0 (2.5) BoP, bleeding on probing; SoP, suppuration on probing; PPD, probing pocket depth. Implant surface decontamination 193 implants per patient and the dependency of the observations within each patient and over time. As multilevel modelling is very flexible in handling missing data points, all longitudinal data could be used despite some incomplete patient records (e.g. implants that were removed during the follow-up period) (Twisk & de Vente 2002). Due to practical and anatomical limitations, radiographs could not be standardized. In addition, in many fully edentulous subjects intra-oral radiographs could not be obtained and had to be replaced by orthopantomographs. However, despite these limitations, intra-examiner reproducibility was very good both for intra-oral radiographs and orthopantomographs (intra-class correlation coefficients were 0.99 and 0.96 respectively). No significant differences were seen between the test- and placebogroup over 12 months of observation in BoP, SoP, PPD and marginal bone loss. Although both groups showed improved clinical parameters as a result of treatment, complete resolution of inflammation (i.e. health) was almost never achieved. Sixty-six of the 69 implants present at T 12 showed at least one site with BoP and 15 implants additionally showed suppuration (representing either periimplant mucositis or peri-implantitis). If the criteria for treatment failure were to be defined according to the inclusion criteria used in this study (residual pockets 5 mm associated with bleeding and/or suppuration) treatment was only successful for 11 (38%) subjects and 38 (49%) implants. Increasing the threshold to pockets 6 mm associated with bleeding and/or suppuration results in treatment success for 17 (59%) subjects and 55 (71%) implants. These results are somewhat less than the 2- year follow-up results described by Serino & Turri (2011), who used more or less a comparable surgical approach (apically re-positioned flap, bone re-contouring and mechanical cleansing of the implant surface under CHX irrigation). Two years after treatment, 77% of the subjects and 75% of the implants showed no pockets 6 mm associated with bleeding/ suppuration. A possible explanation for the difference between both studies is the fact that in the latter study, all patients received adjunctive systemic
10 194 de Waal et al. Table 5. Average differences in BoP, SoP, PPD and radiographical marginal bone loss between placebo- and test-group over three follow-up measurements (3, 6 and 12 months) from baseline Outcome variable Crude model* p-value Adjusted model p-value b (95% CI) b (95% CI) % Sites BoP 0.34 ( to 15.61) ( to 9.05) % Sites SoP 0.08 ( 5.36 to 5.52) ( to 2.72) Mean PPD 0.26 ( 1.13 to 0.62) ( 1.40 to 0.41) Mean marginal bone loss 0.01 ( 0.35 to 0.38) ( 0.27 to 0.48) Note: The reference category for intervention effect is the placebo-group. The regression coefficients (b) indicate the average differences in secondary outcomes between placebo- and test-group over the three follow-up measurements (3, 6 and 12 months) from baseline. BoP, bleeding on probing; SoP, suppuration on probing; PPD, probing pocket depth; 95% CI, 95% confidence interval. *Adjusted for baseline value and time. Adjusted for baseline value, time, smoking, dental status, history of periodontitis and implant surface roughness. antibiotic therapy (clindamycine). However, one could think of many other factors that may influence treatment results (e.g. patient factors such as smoking, plaque levels, periodontitis and dental status, implant factors, treatment factors) making a direct comparison between this study and other studies difficult. Therefore, more randomized controlled trials are needed, each focusing on one aspect of the treatment protocol at a time. This study shows that implant surface decontamination with 0.12% CHX % CPC in resective surgical treatment of peri-implantitis leads to greater suppression of anaerobic bacteria on the implant surface than a placebo-solution. However, this does not translate to better clinical or radiographical outcomes of the intervention. References Addy, M. (1986) Chlorhexidine compared with other locally delivered antimicrobials. A short review. Journal of Clinical Periodontology 13, Babich, H., Wurzburger, B. J., Rubin, Y. L., Sinensky, M. C. & Blau, L. (1995) An in vitro study on the cytotoxicity of chlorhexidine digluconate to human gingival cells. Cell Biology and Toxicology 11, Cabral, C. T. & Fernandes, M. H. (2007) In vitro comparison of chlorhexidine and povidoneiodine on the long-term proliferation and functional activity of human alveolar bone cells. Clinical Oral Investigations 11, Cairo, F., Sanz, I., Matesanz, P., Nieri, M. & Pagliaro, U. (2012) Quality of reporting of randomized clinical trials in implant dentistry. A systematic review on critical aspects in design, outcome assessment and clinical relevance. Journal of Clinical Periodontology 39 (Suppl. 12), Deppe, H., Horch, H. H. & Neff, A. (2007) Conventional versus CO 2 laser-assisted treatment of peri-implant defects with the concomitant use of pure-phase beta-tricalcium phosphate: a 5-year clinical report. The International Journal of Oral & Maxillofacial Implants 22, Esposito, M., Grusovin, M. G. & Worthington, H. V. (2012) Interventions for replacing missing teeth: treatment of peri-implantitis. Cochrane Database of Systematic Reviews 1, CD doi: / CD pub5. Giannelli, M., Chellini, F., Margheri, M., Tonelli, P. & Tani, A. (2008) Effect of chlorhexidine digluconate on different cell types: a molecular and ultrastructural investigation. Toxicology In Vitro: An International Journal Published in Association with BIBRA 22, Gosau, M., Hahnel, S., Schwarz, F., Gerlach, T., Reichert, T. E. & B urgers, R. (2010) Effect of six different peri-implantitis disinfection methods on in vivo human oral biofilm. Clinical Oral Implants Research 21, Heitz-Mayfield, L. J., Salvi, G. E., Mombelli, A., Faddy, M., Lang, N. P. & Implant Complication Research Group (2012) Anti-infective surgical therapy of peri-implantitis. A 12-month prospective clinical study. Clinical Oral Implants Research 23, Herrera, D., Roldan, S., Santacruz, I., Santos, S., Masdevall, M. & Sanz, M. (2003) Differences in antimicrobial activity of four commercial 0.12% chlorhexidine mouthrinse formulations: an in vitro contact test and salivary bacterial counts study. Journal of Clinical Periodontology 30, Jones, C. G. (1997) Chlorhexidine: is it still the gold standard? Periodontology , Kuyyakanond, T. & Quesnel, L. B. (1992) The mechanism of action of chlorhexidine. FEMS Microbiology Letters 79, Leonhardt, A., Dahlen, G. & Renvert, S. (2003) Five-year clinical, microbiological, and radiological outcome following treatment of periimplantitis in man. Journal of Periodontology 74, Lindhe, J., Meyle, J. & Group D of European Workshop on Periodontology (2008) Periimplant diseases: Consensus Report of the Sixth European Workshop on Periodontology. Journal of Clinical Periodontology 35, Maximo, M. B., de Mendoncßa, A. C., Renata, Santos. V., Figueiredo, L. C., Feres, M. & Duarte, P. M. (2009) Short-term clinical and microbiological evaluations of peri-implant diseases before and after mechanical anti-infective therapies. Clinical Oral Implants Research 20, Moher, D., Hopewell, S., Schulz, K. F., Montori, V., Gotzsche, P. C., Devereaux, P. J., Elbourne, D., Egger, M., Altman, D. G. & Consolidated Standards of Reporting Trials Group (2010) CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. Journal of Clinical Epidemiology 63, e1 e37. Pitten, F. A. & Kramer, A. (1999) Antimicrobial efficacy of antiseptic mouthrinse solutions. European Journal of Clinical Pharmacology 55, Pitten, F. A. & Kramer, A. (2001) Efficacy of cetylpyridinium chloride used as oropharyngeal antiseptic. Arzneimittel-Forschung 51, Quirynen, M., Avontroodt, P., Peeters, W., Pauwels, M., Coucke, W. & van Steenberghe, D. (2001) Effect of different chlorhexidine formulations in mouthrinses on de novo plaque formation. Journal of Clinical Periodontology 28, Ridgers, N. D., Stratton, G., Fairclough, S. J. & Twisk, J. W. (2007) Long-term effects of a playground markings and physical structures on children s recess physical activity levels. Preventive Medicine 44, R olla, G. & Melsen, B. (1975) On the mechanism of the plaque inhibition by chlorhexidine. Journal of Dental Research 54, Spec No. B, B57 B62. Romeo, E., Ghisolfi, M., Murgolo, N., Chiapasco, M., Lops, D. & Vogel, G. (2005) Therapy of peri-implantitis with resective surgery. A 3-year clinical trial on rough screw-shaped oral implants. Part I: clinical outcome. Clinical Oral Implants Research 16, Russell, A. D. (1986) Chlorhexidine: antibacterial action and bacterial resistance. Infection 14, Schulz, K. F., Altman, D. G., Moher, D. & CONSORT Group (2010) CONSORT 2010 Statement: Updated guidelines for reporting parallel group randomised trials. Journal of Clinical Epidemiology 63, Schwarz, F., John, G., Mainusch, S., Sahm, N. & Becker, J. (2012) Combined surgical therapy of peri-implantitis evaluating two methods of surface debridement and decontamination. A two-year clinical follow up report. Journal of Clinical Periodontology 39, Schwarz, F., Sahm, N., Iglhaut, G. & Becker, J. (2011) Impact of the method of surface debridement and decontamination on the clinical outcome following combined surgical therapy of peri-implantitis: a randomized controlled clinical study. Journal of Clinical Periodontology 38, Serino, G. & Turri, A. (2011) Outcome of surgical treatment of peri-implantitis: results from a 2-year prospective clinical study in humans. Clinical Oral Implants Research 22, Syed, S. A. & Loesche, W. J. (1972) Survival of human dental plaque flora in various transport media. Applied Microbiology 24, Twisk, J. & de Vente, W. (2002) Attrition in longitudinal studies. How to deal with missing data. Journal of Clinical Epidemiology 55, Twisk, J. W. R. (2006) Applied multilevel analysis, pp Cambridge: Cambridge University Press.
11 Implant surface decontamination 195 Van Steenbergen, M. J., van Winkelhoff, A. J., van der Mispel, L., van der Velden, U., Abbas, F. & de Graaff, J. (1986) Comparison of two selective media for Actinobacillus actinomycetemcomitans. Journal of Clinical Microbiology 24, Van Winkelhoff, A. J., van Steenbergen, T. J., Kippuw, N. & De Graaff, J. (1985) Further characterization of Bacteroides endodontalis, an asaccharolytic black-pigmented Bacteroides species from the oral cavity. Journal of Clinical Microbiology 22, Zitzmann, N. U. & Berglundh, T. (2008) Definition and prevalence of peri-implant diseases. Journal of Clinical Periodontology 35, Address: Yvonne de Waal Center for Dentistry and Oral Hygiene University Medical Center Groningen Antonius Deusinglaan AV Groningen The Netherlands y.c.m.de.waal@umcg.nl Clinical Relevance Scientific rationale for study: The method of surface debridement and decontamination might influence the outcome of surgical treatment of peri-implantitis. However, limited evidence exists as to which method should be used. Principal findings: Implant surface decontamination with chlorhexidine/ cetylpyridinium chloride during resective surgical treatment of peri-implantitis leads to greater bacterial reduction, but similar clinical results compared with decontamination with a placebo-solution. Practical implications: Chlorhexidine/cetylpyridinium chloride might be useful for decontamination of the implant surface during surgical treatment of peri-implantitis, but it fails to improve clinical results significantly.
Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen
![Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen](/thumbs/82/86452679.jpg) University of Groningen Peri-implant infections de Waal, Yvonne IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Peri-implant infections de Waal, Yvonne IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
The International Journal of Periodontics & Restorative Dentistry
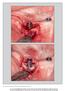 The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis
 Journal of Dental Research, Dental Clinics, Dental Prospects Original Article Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis Zeinab
Journal of Dental Research, Dental Clinics, Dental Prospects Original Article Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis Zeinab
Frank Schwarz *, Andrea Schmucker and Jürgen Becker
 Schwarz et al. International Journal of Implant Dentistry (2015) 1:22 DOI 10.1186/s40729-015-0023-1 REVIEW Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis
Schwarz et al. International Journal of Implant Dentistry (2015) 1:22 DOI 10.1186/s40729-015-0023-1 REVIEW Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis
Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study
 Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment
 The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
Key words: Peri- implant Mucositis, Peri- implantitis, Peri- implant Diseases, Treatment
 PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
Show biofilm the red card
 Show biofilm the red card BIOFILM-ERASER 1 A NEW APPLICATION Effective treatment for periodontal and peri-implant inflammation Periodontitis and peri-implantitis are bacterial inflammations with similar
Show biofilm the red card BIOFILM-ERASER 1 A NEW APPLICATION Effective treatment for periodontal and peri-implant inflammation Periodontitis and peri-implantitis are bacterial inflammations with similar
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS
 Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS Guidelines for use of antibiotics in periodontal therapy 1. The clinical
Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS Guidelines for use of antibiotics in periodontal therapy 1. The clinical
Citation for published version (APA): Otten, M. P. T. (2011). Oral Biofilm as a Reservoir for Antimicrobials Groningen: University of Groningen
 University of Groningen Oral Biofilm as a Reservoir for Antimicrobials Otten, Marieke Petronella Theodora IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Oral Biofilm as a Reservoir for Antimicrobials Otten, Marieke Petronella Theodora IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
What s new for the clinician? Summaries of and excerpts from recently published papers
 http://dx.doi.org/10.17159/2519-0105/2017/v72no8a8 < 387 What s new for the clinician? Summaries of and excerpts from recently published papers SADJ September 2017, Vol 72 no 8 p387- p391 Compiled and
http://dx.doi.org/10.17159/2519-0105/2017/v72no8a8 < 387 What s new for the clinician? Summaries of and excerpts from recently published papers SADJ September 2017, Vol 72 no 8 p387- p391 Compiled and
Treatment Concepts for PERI-IMPLANTITIS
 Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Antimicrobial Treatment for Advanced Periodontal Disease
 Antimicrobial Treatment for Advanced Periodontal Disease James S. Kohner, DDS DISCLOSURES December 15, 2011 Editor's Note: This author's case report is based on the work of Jorgen Slots, DDS, DMD, PhD,
Antimicrobial Treatment for Advanced Periodontal Disease James S. Kohner, DDS DISCLOSURES December 15, 2011 Editor's Note: This author's case report is based on the work of Jorgen Slots, DDS, DMD, PhD,
Porous titanium granules in the treatment of peri-implant osseous defects a 7-year follow-up study
 Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Periodontitis & Implants
 Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Maintenance in the Periodontally Compromised Patient. Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club
 Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Clinical outcomes following surgical treatment of peri-implantitis at grafted and non-grafted implant sites: a retrospective analysis
 Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
University of Groningen. Restorative dentistry done digitally Schepke, Ulf
 University of Groningen Restorative dentistry done digitally Schepke, Ulf IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Restorative dentistry done digitally Schepke, Ulf IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Volume 2 Issue
 Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
TwinLight TM Periodontal Treatment. Tomaž Lipoglavšek, DMD
 TwinLight TM Periodontal Treatment Tomaž Lipoglavšek, DMD REVIEW OF THE LITERATURE 2 The available evidence consistently shows that therapies intended to arrest and control periodontitis depend primarily
TwinLight TM Periodontal Treatment Tomaž Lipoglavšek, DMD REVIEW OF THE LITERATURE 2 The available evidence consistently shows that therapies intended to arrest and control periodontitis depend primarily
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions
 Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Effect of temperature change of 0.2% chlorhexidine rinse on matured human plaque: an in vivo study.
 ISSN: 2278 0211 (Online) Effect of temperature change of 0.2% chlorhexidine rinse on matured human plaque: an in vivo study. Dr. Yashika Jain Senior Lecturer, Institution: SGT Dental College & Hospital,
ISSN: 2278 0211 (Online) Effect of temperature change of 0.2% chlorhexidine rinse on matured human plaque: an in vivo study. Dr. Yashika Jain Senior Lecturer, Institution: SGT Dental College & Hospital,
Immediate loading in heavy smokers
 case report Immediate loading in heavy smokers Dr Dr Branislav Fatori & Dr Inge Schmitz, Germany Today, numerous implant systems and many modifications thereof are available on the market, and it may be
case report Immediate loading in heavy smokers Dr Dr Branislav Fatori & Dr Inge Schmitz, Germany Today, numerous implant systems and many modifications thereof are available on the market, and it may be
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Illustrations by Carole Fumat.
 www.acteongroup.com To visualize our channel: www.youtube.com/user/acteonsatelec (1) Mombelli A, et al. The epidemiology of peri-implantitis. Clinical Oral Implants Research 23 (Oct 2012): 67-76 (2) European
www.acteongroup.com To visualize our channel: www.youtube.com/user/acteonsatelec (1) Mombelli A, et al. The epidemiology of peri-implantitis. Clinical Oral Implants Research 23 (Oct 2012): 67-76 (2) European
The inhibitory effects of different mouthwash brands on the zone of inhibition of. Micrococcus luteus and Escherichia coli
 The inhibitory effects of different mouthwash brands on the zone of inhibition of Micrococcus luteus and Escherichia coli George Kendros Bio 2290 Section 001 TM Gray 2013 04 10 Abstract The use of mouthwash
The inhibitory effects of different mouthwash brands on the zone of inhibition of Micrococcus luteus and Escherichia coli George Kendros Bio 2290 Section 001 TM Gray 2013 04 10 Abstract The use of mouthwash
The Microbial Etiology and Pathogenesis of Peri-Implantitis
 The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
Very small abutment head easy and secure handling. Ankylos. The SmartFix concept. Prosthetic solution on angled implants
 Very small abutment head easy and secure handling Ankylos The SmartFix concept Prosthetic solution on angled implants Stable prosthetic fit The area supporting the prosthesis is extended distally by the
Very small abutment head easy and secure handling Ankylos The SmartFix concept Prosthetic solution on angled implants Stable prosthetic fit The area supporting the prosthesis is extended distally by the
Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014
 Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014 Tooth Replacement treatment options and benefits Identify Existing Patients
Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014 Tooth Replacement treatment options and benefits Identify Existing Patients
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Citation for published version (APA): Schortinghuis, J. (2004). Ultrasound stimulation of mandibular bone defect healing s.n.
 University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters
 Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters REVIEWED PAPER Most patients visiting dental surgeries suffer from various types of periodontopathies. Since
Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters REVIEWED PAPER Most patients visiting dental surgeries suffer from various types of periodontopathies. Since
Kerry Hyland-Lepicek, RDH
 The Oravital System: A Paradigm Shift in the Treatment of Periodontal Disease There is substantial evidence indicating that most forms of periodontal disease are specific infections caused by an overgrowth
The Oravital System: A Paradigm Shift in the Treatment of Periodontal Disease There is substantial evidence indicating that most forms of periodontal disease are specific infections caused by an overgrowth
NEW 12-MONTH CLINICAL STUDY RESULTS
 NEW 12-MONTH CLINICAL STUDY RESULTS March 30, 2015 Dear Oxyfresh Professional: We are thrilled to share with you the exciting results of a NEW 12-month, double blind clinical study published in the International
NEW 12-MONTH CLINICAL STUDY RESULTS March 30, 2015 Dear Oxyfresh Professional: We are thrilled to share with you the exciting results of a NEW 12-month, double blind clinical study published in the International
Probiotics In Gingivitis Management: A Randomized Clinical Trial. Jordi Espadaler, PhD. Director of Innovation
 Probiotics In Gingivitis Management: A Randomized Clinical Trial Jordi Espadaler, PhD. Director of Innovation espadaler@ab-biotics.com Improving oral care Mechanical plaque removal, brushing and rinsing
Probiotics In Gingivitis Management: A Randomized Clinical Trial Jordi Espadaler, PhD. Director of Innovation espadaler@ab-biotics.com Improving oral care Mechanical plaque removal, brushing and rinsing
Implantology without Periodontology is like Yin without Yang.
 Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
PERIODONTAL CASE PRESENTATION - 1
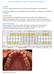 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Detection of predominant subgingival periopathogens around submerged and non submerged hydroxy apatite implants
 [Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
[Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Principles of endodontic surgery
 Principles of endodontic surgery Note: the doctor said that this lecture mainly contain notes, so we should study it from the book for further information (chapter 18) principles of endodontic surgery.
Principles of endodontic surgery Note: the doctor said that this lecture mainly contain notes, so we should study it from the book for further information (chapter 18) principles of endodontic surgery.
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
ARESTIN (minocycline hcl) subgingival powder
 ARESTIN (minocycline hcl) subgingival powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
ARESTIN (minocycline hcl) subgingival powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr.
 Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
University of Groningen. Soft tissue development in the esthetic zone Patil, Ratnadeep Chandrakant
 University of Groningen Soft tissue development in the esthetic zone Patil, Ratnadeep Chandrakant IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Soft tissue development in the esthetic zone Patil, Ratnadeep Chandrakant IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
Periodontal (Gum) Disease
 Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Interest in and studies on osseointegration
 CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 485 Bacterial Biofilm Morphology on a Failing Implant with an Oxidized Surface: A Scanning Electron Microscope Study Massimo Simion, MD,
The International Journal of Periodontics & Restorative Dentistry 485 Bacterial Biofilm Morphology on a Failing Implant with an Oxidized Surface: A Scanning Electron Microscope Study Massimo Simion, MD,
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Case Report Peri-Implant Bone Loss and Peri-Implantitis: A Report of Three Cases and Review of the Literature
 Hindawi Publishing Corporation Case Reports in Dentistry Volume 2016, Article ID 2491714, 8 pages http://dx.doi.org/10.1155/2016/2491714 Case Report Peri-Implant Bone Loss and Peri-Implantitis: A Report
Hindawi Publishing Corporation Case Reports in Dentistry Volume 2016, Article ID 2491714, 8 pages http://dx.doi.org/10.1155/2016/2491714 Case Report Peri-Implant Bone Loss and Peri-Implantitis: A Report
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Interventions for replacing missing teeth: treatment of peri-implantitis (Review)
 A-PDF Watermark DEMO: Purchase from www.a-pdf.com to remove the watermark Interventions for replacing missing teeth: treatment of periimplantitis (Review) Esposito M, Grusovin MG, Worthington HV This is
A-PDF Watermark DEMO: Purchase from www.a-pdf.com to remove the watermark Interventions for replacing missing teeth: treatment of periimplantitis (Review) Esposito M, Grusovin MG, Worthington HV This is
University of Groningen
 University of Groningen Maxillary overdentures supported by four or six implants in the anterior region Slot, Wim; Raghoebar, Gerry; Cune, Marco; Vissink, Arjan; Meijer, Hendrikus Published in: Journal
University of Groningen Maxillary overdentures supported by four or six implants in the anterior region Slot, Wim; Raghoebar, Gerry; Cune, Marco; Vissink, Arjan; Meijer, Hendrikus Published in: Journal
Overview of Periodontics for the General Practicioner
 Overview of Periodontics for the General Practicioner Nashville Area Dental Continuing Education August 27, 2008 Phillip D. Woods, DDS, MPH Commander, USPHS BOP National Periodontal Consultant Diplomate,
Overview of Periodontics for the General Practicioner Nashville Area Dental Continuing Education August 27, 2008 Phillip D. Woods, DDS, MPH Commander, USPHS BOP National Periodontal Consultant Diplomate,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
Microbiological effects of an antiseptic mouthrinse in irradiated cancer patients
 Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.17234 http://dx.doi.org/doi:10.4317/medoral.17234 Microbiological effects of an antiseptic mouthrinse in irradiated cancer
Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.17234 http://dx.doi.org/doi:10.4317/medoral.17234 Microbiological effects of an antiseptic mouthrinse in irradiated cancer
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
The notable success of dental implants. Relationship Between Smoking and Bleeding on Probing RESEARCH
 RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
14/09/15. Assessment of Periodontal Disease. Outline. Why is Periodontal assessment needed? The Basics of Periodontal assessment
 Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
Assessment of Periodontal Disease Dr Wendy Turner Outline Why is Periodontal assessment needed? The Basics of Periodontal assessment Probing: Basic Periodontal Examination for adults and children. Detailed
PERI-IMPLANTITIS A PROBLEM.
 PERI-IMPLANTITIS A PROBLEM. Infections around implants are stubborn. What can help? What doesn t? How can infections be prevented? Geistlich News 02 2014 5 Illustration: Büro Haeberli How prevalent is
PERI-IMPLANTITIS A PROBLEM. Infections around implants are stubborn. What can help? What doesn t? How can infections be prevented? Geistlich News 02 2014 5 Illustration: Büro Haeberli How prevalent is
Periodontal Treatment Guide
 Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera
 Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93.
 Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
J. A. H. Lindeboom, J. W. H. Frenken, P. Valkenburg & H. P. van den Akker. Introduction. Abstract
 The role of preoperative prophylactic antibiotic administration in periapical endodontic surgery: a randomized, prospective double-blind placebo-controlled study J. A. H. Lindeboom, J. W. H. Frenken, P.
The role of preoperative prophylactic antibiotic administration in periapical endodontic surgery: a randomized, prospective double-blind placebo-controlled study J. A. H. Lindeboom, J. W. H. Frenken, P.
Immediate fixed teeth a treatment concept for edentulous patients
 52 Maxillary rehabilitation using the All-on-4 concept Immediate fixed teeth a treatment concept for edentulous patients DR DUSAN VASILJEVIC AND VLADAN VASILJEVIC, FRIEDEBURG, GERMANY The number of edentulous
52 Maxillary rehabilitation using the All-on-4 concept Immediate fixed teeth a treatment concept for edentulous patients DR DUSAN VASILJEVIC AND VLADAN VASILJEVIC, FRIEDEBURG, GERMANY The number of edentulous
University of Groningen. Immediate dental implant placement in the aesthetic zone Slagter, Kirsten
 University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Retrospective analysis of periimplantitis therapy
 Retrospective analysis of periimplantitis therapy of 158 implants Abstract Objective Jörg-Ulf Wiegner, a Hermann Klinsmann a & Toralf Kömmling b a Private practice, Saalfeld, Germany b Private practice,
Retrospective analysis of periimplantitis therapy of 158 implants Abstract Objective Jörg-Ulf Wiegner, a Hermann Klinsmann a & Toralf Kömmling b a Private practice, Saalfeld, Germany b Private practice,
Core build-up using post systems
 Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
FACULTY OF HEALTH SCIENCES INSTITUTE OF CLINICAL DENTISTRY
 Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
