Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen
|
|
|
- Jessie Parker
- 5 years ago
- Views:
Transcription
1 University of Groningen Peri-implant infections de Waal, Yvonne IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document Version Publisher's PDF, also known as Version of record Publication date: 2015 Link to publication in University of Groningen/UMCG research database Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen Copyright Other than for strictly personal use, it is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), unless the work is under an open content license (like Creative Commons). Take-down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from the University of Groningen/UMCG research database (Pure): For technical reasons the number of authors shown on this cover page is limited to 10 maximum. Download date:
2 Prognostic indicators for surgical peri-implantitis treatment Y.C.M. de Waal G.M. Raghoebar H.J.A. Meijer E.G. Winkel A.J. van Winkelhoff Edited version of: Clinical Oral Implants Research 2015; 1-9. doi: /clr [Epub ahead of print]
3 Abstract Objectives Objective of this study was to identify prognostic indicators for the outcome of resective peri-implantitis treatment, by an analysis of the pooled data of two previously conducted randomized controlled trials. Material and methods Data of 74 patients with peri-implantitis (187 implants) who had received resective surgical treatment were available. Primary outcome variable was failure of peri-implantitis treatment after 12 months. Multilevel univariable and multiple logistic regression analyses were performed to evaluate the effect of various potentially prognostic indicators on the primary outcome. CHAPTER 8 Results Peri-implantitis treatment was unsuccessful in 106 implants (57%) and 48 patients (67%) after 12 months. In the multiple regression analysis the variables order of inclusion (p = 0.016) and mean bone loss at baseline (p = 0.030) were significant prognostic indicators for treatment failure. To eliminate the effect of order of inclusion, post-hoc analyses were carried out in a subgroup of patients. The univariable post-hoc analysis showed a significant association for smoking (p = 0.015), maximum pocket depth at baseline (p = 0.073), mean bone loss at baseline (p = 0.003) and presence of plaque (p = 0.100). In the multiple regression post-hoc analysis only the variables smoking (p = 0.044) and mean bone loss (p = 0.043) remained statistically significant. Conclusions The outcome of surgical peri-implantitis treatment is influenced by the experience of the surgical team with the surgical procedure. The observed learning effect has consequences for clinical practice and for conducting and interpreting clinical trials on peri-implantitis treatment. Other prognostic indicators are amount of peri-implant bone loss at baseline and smoking, and to a lesser extent, probing pocket depth at baseline and presence of plaque during follow-up. Early diagnosis of peri-implantitis and control of behavioral factors are crucial in achieving peri-implantitis treatment success. 154
4 Introduction Peri-implantitis is an infectious disease that resides in the mucosa surrounding dental implants and also affects the supporting bone (Lindhe et al. 2008). It is a common biological complication following implant therapy. The frequency of peri-implantitis on patient level ranges from 6 to 47% (mean 18.8%, 95% CI [16.8, 20.8]) and on implant level from 2 to 37% (mean 9.6%, 95% CI [8.8, 10.4]) after a mean observation period of approximately 10 years (Atieh et al. 2013). Higher prevalence figures are reported for smokers and patients with a history of periodontitis and with increasing implant function time (Atieh et al. 2013, De Waal et al. 2013b). Plaque has been identified as a major risk factor for development of peri-implantitis (Heitz-Mayfield 2008), which explains the observation that participation in a supportive maintenance program results in lower prevalence of peri-implantitis (Atieh et al. 2013). Once peri-implantitis has been diagnosed, it is essential to initiate a prompt curative intervention in order to resolve the inflammatory lesion and prevent further bone loss. Although some initial peri-implantitis lesions might be effectively treated by nonsurgical treatment alone, more advanced peri-implantitis lesions require additional surgical intervention to achieve disease resolution (Lindhe et al. 2008). As of yet, the most effective intervention for treatment of peri-implantitis has not been identified and there is no validated treatment protocol available (Esposito et al. 2012). It might be hypothesized that those patients who are at high risk for development of peri-implantitis, also run a higher risk for failure of peri-implantitis treatment once the disease has been diagnosed. Establishing such risk profiles for peri-implantitis treatment could expedite improvement of treatment protocols, assist in selection of the most effective individual treatment and could allow for optimal information and motivation of patients. Furthermore, it could be helpful in clinical decision making and would enable clinicians to estimate the chances on a successful treatment. The available evidence for the factor smoking as potential prognostic indicator for peri-implantitis treatment is limited and conflicting. From a large retrospective study it was suggested that smoking and smoking dose might be associated with failure of peri-implantitis treatment (Charalampakis et al. 2011), but this was not substantiated in prospective studies (Serino & Turri 2011, Heitz-Mayfield et al. 2012). The evidence on poor oral hygiene and history of periodontitis as potential prognostic indicators is scarce and available from only one retrospective study evaluating different treatment strategies with different follow-up periods (Lagervall & Jansson 2013). Other factors that have been suggested to influence results of peri-implantitis treatment include early disease development (Charalampakis et al. 2011), implant bone loss of more than 1/3 of the length of the implant (Lagervall & Jansson 2013), non-acceptable compliance (Lagervall & Jansson 2013), bone defect configuration (Schwarz et al. 2011), implant surface characteristics (Roccuzzo et al. 2011), amount of initial bone loss (Serino & Turri 2011), initial presence of pus (Thierbach & Eger 2013) and participation in a maintenance program (Serino et al. 2014). However, the evidence on all these factors is limited due to the small number of studies and small study groups. The problem of small study groups can be overcome by pooling data of multiple Prognostic indicators 155
5 prospective studies and perform a meta-analysis. However, heterogeneity among study designs very often restricts the possibility of a meta-analysis. Recently, two randomized controlled trials on resective surgical treatment of peri-implantitis were published, with almost identical study protocols (De Waal et al. 2013a, De Waal et al. 2014). The aim of the present study was to identify indicators that are prognostic for the outcome of resective surgical peri-implantitis treatment, by carrying out an analysis of the pooled data of these two previously conducted studies. Material and methods CHAPTER 8 This study was an analysis of the pooled datasets of two previously conducted randomized, double-blind, controlled trials evaluating the clinical, radiographic and microbiological outcomes of resective surgical treatment of peri-implantitis combined with mechanical debridement and chemical decontamination of the implant surface (De Waal et al. 2013a, De Waal et al. 2014). The research protocols of both studies were identical except for the method of chemical decontamination of the implant surface. The two studies were performed consecutively. Intervention Participants were consecutively recruited from patients referred for diagnosis and treatment of peri-implantitis to the University Medical Center Groningen, the Netherlands. Written informed consent was obtained from all participants before entering the study. The studies were approved by the Institutional Review Board of the University Medical Center Groningen (METc and METc ) and registered at ClinicalTrials.gov (NCT and NCT ). Peri-implantitis was defined as bleeding and/or suppuration on probing combined with a peri-implant probing pocket depth (PPD) 5 mm and bone loss 2 mm. Patients were all surgically treated by one and the same oral and maxillofacial surgeon (G.R.). Full thickness mucoperiosteal flaps were raised buccally and lingually. Granulation tissue was removed using curettes (Gracey, Hu-Friedy, Chicago, IL, USA). Bone recontouring, aimed at eliminating angular bony defects, was performed using a rotating round bur under saline irrigation. The implant surfaces were mechanically cleaned using sterile surgical gauzes soaked in saline. After mechanical debridement, the implant surfaces were rinsed for 1 min with a placebo solution (De Waal et al. 2013a) 0.12% chlorhexidine (CHX) % cetylpyridinium chloride (CPC) (De Waal et al. 2013a, De Waal et al. 2014) or a 2% chlorhexidine solution (De Waal et al. 2014). Subsequently, the implant surfaces were rinsed with abundant amounts of sterile saline for 1 min. Suprastructures were repositioned (if necessary) and mucosal flaps were apically positioned and firmly sutured (Vicryl Plus, Ethicon Inc., Somerville, NJ, USA). For all patients, surgery was followed by two weeks of mouth rinsing with 0.12% CHX % CPC without alcohol (PerioAid, Dentaid SL, Cerdanyola, Spain) two times daily during 30 s. Sutures were removed after two weeks. During follow-up examinations, patients were re-instructed in oral hygiene measures and implants, and teeth 156
6 were cleaned as necessary. Use of topical or systemic antibiotic treatment was not part of the treatment protocol. Follow-up visits were scheduled after 3, 6, and 12 months (T 3, T 6 and T 12 ). At baseline (T 0 ) and during follow-up visits radiographs and microbiological samples were taken and clinical measurements were performed by one and the same examiner (Y.W.). Presence of plaque was assessed (present/absent) at four sites per implant (mesial, buccal, distal and lingual) by running a probe across the marginal surface of the implant/suprastructure. Peri-implant pocket probing was performed at four sites per implant using a pressure sensitive probe (probe force of 0.25 N; KerrHawe Click Probe, Bioggo, Switzerland). PPD was scored to the nearest millimeter. Up to 30 s after pocket probing, the presence or absence of bleeding and suppuration were assessed. The width of keratinized mucosa was assessed at the mid-buccal position of the implant. Outcomes Primary outcome The primary outcome of the present study was failure of peri-implantitis treatment after 12 months. Clinical and radiographic data collected during the last follow-up visit were combined to produce this outcome. Treatment was considered a failure if one or more of the following criteria were met: absence of the implant; progressive bone loss 1 mm during follow-up (between T 3 and T 12 ), on the mesial and/or distal side of the implant as assessed on radiographs; presence of suppuration on probing; bleeding on probing on 3 or 4 sites per implant; probing pocket depth of 5 mm in combination with bleeding; Prognostic indicators Success was defined as the inverse of failure. Predictors Data on the following potential predictors were collected: Patient characteristics (measured on patient level): Age at surgery; Gender; Daily medication intake; Use of systemic antibiotics during follow-up; Smoking; History of periodontitis; Dental status (fully edentulous versus partially edentulous); Number of implants with peri-implantitis; Order of inclusion (order in which patients were consecutively included and treated). Clinical characteristics (measured on implant level): Removal of suprastructure during surgery; 157
7 Use of surgical dressing; Presence of Aggregatibacter actinomycetemcomitans and/or Porphyromonas gingivalis in the oral cavity at baseline (measured on patient level); Presence of pus at baseline; Probing pocket depth (PPD) at baseline: highest value per implant (maximum PPD) and mean of four measurements per implant (mean PPD); Bone loss at baseline: highest value per implant (maximum bone loss) and mean of mesial and distal measurement per implant (mean bone loss); Bone defect configuration at baseline: angle between bone and implant in apical half of bone defect, lowest value of mesial and distal measurement; Presence of plaque at any moment during follow-up: yes/no and mean percentage of sites with plaque; Presence of keratinized mucosa at T 3. CHAPTER 8 Implant characteristics (measured on implant level): Implant function time: time between 2 nd stage surgery and peri-implantitis surgery; Implant location: fully edentulous jaw versus partially edentulous jaw, maxilla versus mandibula, anterior region versus posterior region; Previous bone augmentation; Implant placement procedure: one-stage versus two-stage procedure; Implant length; Implant surface roughness: smooth/machined surface versus minimally/moderately rough versus rough. Since it was shown that the method of surface decontamination did not have a significant effect on treatment outcome parameters (De Waal et al. 2013a, De Waal et al. 2014), this factor was not included in the present analysis. Statistical analysis To take into account the hierarchical structure of the data a two-level hierarchical random intercepts model was chosen, with two levels of analysis being implant-level and patient-level. Multilevel univariable logistic (logit) regression analyses were performed separately for all potential prognostic indicators with our primary outcome measure, i.e. failure of peri-implantitis treatment at 12 months after treatment. Parameters were estimated using the second order penalized quasi-likelihood (PQL) estimation procedure. The linearity of the associations of continuous variables with the outcome was examined by dividing the data into quartiles. Variables that did not show a continuous relationship were dichotomized or categorized, depending on the observed data structure. Variables with a statistically significant association with the outcome (p 0.10) were selected for the multilevel multiple logistic (logit) regression analysis. Collinearity and multicollinearity between the selected variables were assessed by determining correlation coefficients and variance inflation factors (VIF). From variables that were strongly correlated (correlation coefficient > 0.70 or VIF > 5) only the variable that was most strongly associated with the outcome as observed from the univariable analyses was selected for the multiple regression analysis. 158
8 Multilevel models were analyzed using MLwiN version 2.12 (Centre for Multilevel Modeling, University of Bristol, Bristol, UK). For descriptive data and collinearity diagnostics Graphpad Prism 5 for Windows (version 5.04, Graphpad Software, San Diego, CA, USA) and IBM SPSS Statistics 22 (version , IMB, Armonk, NY, USA) were used. Results The complete datasets of two randomized controlled trials were available for the current analysis (De Waal et al. 2013a, De Waal et al. 2014). A total of 74 patients presenting a total of 187 implants with peri-implantitis were previously included and had been treated according to the study protocols (respectively 30 patients with 79 implants in the first study and 44 patients with 108 implants in the second study). Two patients had their implant removed between T 3 and T 6 because of implant fracture and were excluded from the current analysis. The remaining patients attended all follow-up visits and no patient was lost to follow-up. Therefore, the current analysis is based on data from 72 patients and a total of 185 implants. Patient and implant characteristics are depicted in Table 1. Five patients had one or more implants removed during follow-up because of persisting peri-implantitis. These implants were classified as failures (14 implants). An additional 92 implant were classified as failures based on the previously stated criteria on bone loss, suppuration, bleeding on probing, and/or probing pocket depth. In total, 106 implants (57%) in 48 patients (67%) showed failure of peri-implantitis treatment at T 12. Prognostic indicators Prognostic indicators Some of the continuous variables showed no linear association with the primary outcome and were either dichotomized (age, number of implants with peri-implantitis, mean plaque percentage after surgery, implant function time and implant length) or categorized (angle of bone defect). The results from the univariable and multiple regression analyses are presented in Table 1. Univariable analysis showed a significant association between the outcome for the potential prognostic indicators smoking, order of inclusion, maximum pocket depth at baseline, mean bone loss at baseline, presence of plaque after surgery, mean plaque percentage after surgery, implant length and implant surface roughness (p 0.10). In the multiple regression analysis only the variables order of inclusion and mean bone loss at baseline were significant prognostic indicators for failure of peri-implantitis treatment (p < 0.05). Post hoc analysis Since order of inclusion was the strongest prognostic indicator for the primary outcome, the relationship between this variable and the outcome was examined in more detail. Implants were divided into deciles according to the order of inclusion and corresponding success percentages were calculated. The success percentages are graphically depicted in Figure 1, which may be interpreted as a graphical representation of the learning curve of the treatment team. 159
9 Table 1. Univariable and multivariable associations with failure of peri-implantitis treatment after one year (study 1 and 2 combined) Variable n (%) Univariable regression analysis Multiple regression analysis OR 95% CI p* OR 95% CI p Patient characteristics Age < 60 years # 32 (44) 60 years 40 (56) Gender Female # 50 (69) Male 22 (31) Daily medication intake 37 (51) Smoking 24 (33) History of periodontitis 32 (44) Dental status Fully edentulous # 39 (54) Partially edentulous 33 (46) # implant with peri-implantitis < 4 implants # 50 (69) 4 implants 22 (31) Order of inclusion (range) ** Treatment / clinical characteristics Removal of suprastructure during surgery 116 (63) Use of surgical dressing 138 (75) Presence of Aa and/or Pg in the oral cavity at baseline 43 (23) Presence of pus at baseline 91 (49) Maximum pocket depth at baseline (mm; mean (SD)) 6.5 (1.6) Mean bone loss at baseline (mm; mean (SD)) 4.0 (1.8) ** Angle of bone defect at baseline 37.5º # 55 (30) > 37.5º and < 52.5º 63 (34) º 67 (36) Presence of plaque after surgery 114 (62) Mean plaque percentage after surgery < 25% # 117 (63) 25% 68 (37) Presence of keratinized mucosa after surgery 112 (61) Implant characteristics Implant function time < 6 years # 93 (50) 6 years 92 (50) Implant location Fully edentulous jaw # 144 (78) Partially edentulous jaw 41 (22) Mandibula # 84 (45) Maxilla 101 (55) Anterior region # 96 (52) Posterior region 89 (48) Implant placed in bone augmented site 76 (41) Implant placement procedure Two stage procedure # 100 (54) One stage procedure 85 (46) Implant length < 13 mm # 81 (44) 13 mm 104 (56) Implant surface roughness Smooth 9 (5) Minimally/moderately rough # 145 (78) Rough 31 (17) # Reference category * Variables with a univariable p value 0.10 were selected for multiple regression analysis ** Statistically significant p < 0.05
10 Figure 1. Learning curve of the surgical team % success of peri-implantitus treatment n th decile of treated implants Figure 2. Success percentage of peri-implantitis treatment related to mean amount of bone loss at baseline (only study 2). Prognostic indicators % success of peri-implantitus treatment n = 26 n = 56 n = 21 n = 4 mean bone loss 161
11 Figure 3. Success percentage of peri-implantitis treatment related to mean amount of bone loss at baseline for non-smokers and smokers (only study 2). % success of peri-implantitus treatment non-smokers smokers n = 19 n = 7 n = 38 n = 18 n = 11 n = 14 CHAPTER 8 mean bone loss An increase in success percentage and a flattening of the learning curve was observed after treatment of about 40% of the implants. The highly significant effect of the variable order of inclusion on the outcome of peri-implantitis treatment might have blurred possible important effects of other potential prognostic indicators. Therefore, additional univariable and multiple regression analyses were carried out including only the patients from the second study, i.e. 107 implants in 43 patients. In this group, peri-implantitis treatment was unsuccessful in 26 of these 43 patients (60%) and in 46 of the 107 implants (43%). Patient and implant characteristics and the results from the additional multilevel univariable and multiple logistic regression analyses are presented in Table 2. The variable order of inclusion no longer appeared to be statistically significant (p = 0.26). Variables that did show a significant univariable association with the primary outcome were smoking, maximum pocket depth at baseline, mean bone loss at baseline and presence of plaque (p 0.10). In the multiple regression analysis only the predictors smoking and mean bone loss remained statistically significant (p < 0.05). The success percentages in different categories of bone loss and smoking are graphically depicted in Figure 2 and 3. Discussion The present study was initiated with the aim to identify potential risk indicators for poor outcome of peri-implantitis treatment. It was shown that order of inclusion, mean amount of bone loss at baseline and smoking are strong prognostic indicators for the outcome of resective surgical peri-implantitis treatment. Less strong prognostic indicators were maximum pocket depth at baseline and presence of plaque during follow-up. 162
12 Table 2. Univariable and multivariable associations with failure of peri-implantitis treatment after one year (only study 2) Variable n (%) Univariable regression analysis Multiple regression analysis OR 95% CI p* OR 95% CI p Patient characteristics Age < 60 years # 21 (49) 60 years 22 (51) Gender Female # 30 (70) Male 13 (30) Daily medication intake 22 (51) Smoking 13 (30) ** History of periodontitis 19 (44) Dental status Fully edentulous # 21 (49) Partially edentulous 22 (51) # implant with peri-implantitis < 4 implants # 30 (70) 4 implants 13 (30) Order of inclusion (range) Treatment / clinical characteristics Removal of suprastructure during surgery 77 (72) Use of surgical dressing 69 (65) Presence of Aa and/or Pg in the oral 30 (28) cavity at baseline Presence of pus at baseline 57 (53) Maximum pocket depth at baseline 6.0 (1.1) (mm; mean (SD)) Mean bone loss at baseline 4.1 (1.6) ** (mm; mean (SD)) Angle of bone defect at baseline 37.5º # 29 (27) > 37.5º and < 52.5º 35 (33) º 43 (40) Presence of plaque after surgery 56 (52) Mean plaque percentage after surgery < 25% # 73 (68) 25% 34 (32) Presence of keratinized mucosa after 70 (65) surgery Implant characteristics Implant function time < 6 years # 61 (57) 6 years 46 (43) Implant location Fully edentulous jaw # 77 (72) Partially edentulous jaw 30 (28) Mandibula # 50 (47) Maxilla 57 (53) Anterior region # 50 (47) Posterior region 57 (53) Implant placed in bone augmented site 40 (37) Implant placement procedure Two stage procedure # 60 (56) One stage procedure 47 (44) Implant length < 13 mm # 44 (41) 13 mm 63 (59) Implant surface roughness Smooth 5 (5) Minimally/moderately rough # 85 ( Rough 17 (16) # Reference category * Variables with a univariable p value 0.10 were selected for multiple regression analysis ** Statistically significant p < 0.05
13 CHAPTER 8 All patients included in the present study were treated by the same surgical team. This team has great experience in oral- and maxillofacial surgery, including implant dentistry, but the experience with the specific resective surgical peri-implantitis treatment was relatively limited prior to the start of the study. The variable order of inclusion was included in the current analysis to explore a possible learning effect of the surgical team with the specific procedure. This variable appeared to be a strong prognostic indicator for the outcome of peri-implantitis treatment. The first treated patients showed significantly higher failure rates than the patients that were treated later in the study. This holds true even when other factors such as amount of bone loss and probing pocket depth at baseline are taken into account, as can be observed from the multiple regression analysis. This learning effect or phenomenon of improvements in performance over time when adopting a new technique is well-known in medicine, psychology and engineering (Ramsay et al. 2000, Ramsay et al. 2002). Factors that influence individual learning curves include: experience and type of people in the surgical team, facilities provided by the institution, individual patient and clinical characteristics in the population undergoing the procedure and characteristics of the surgeon such as attitude, natural abilities, capacity for acquiring new skills and previous experience (Cook et al. 2004). As learning effects are present in many surgical procedures, including implant dentistry (Geckili et al. 2014), they form an obstacle to undertaking and interpreting clinical trials (Cook et al. 2004). It is therefore important to statistically consider learning effects in clinical studies (Ramsay et al. 2000). This has been done in the present study by carrying out a post-hoc analysis including only patients that were treated after fading of the learning effect. The amount of bone loss was the only statistically significant prognostic indicator in both the first evaluation as well as the post-hoc evaluation. Increasing amounts of bone loss at baseline were associated with decreasing success percentages. Specifically smokers with peri-implant bone loss exceeding 5 mm were extremely difficult to treat successfully, resulting in a success percentage of only 32%. The factor bone loss has been identified by others as a determining factor for peri-implantitis treatment outcome. Serino & Turri (2011) found that the proportion of implants that showed healthy peri-implant conditions following resective peri-implantitis treatment was higher for those with minor initial bone loss (2 4 mm bone loss as assessed during surgery) compared to implants with bone loss of 5 mm (74% vs. 40%). The retrospective study of Lagervall & Jansson (2013) showed that implants with bone loss exceeding 1/3 of the length of the implant were significantly associated with failure of peri-implantitis treatment. Amount of bone loss and pocket depth at baseline can be seen as representatives for disease severity. Implants with large amounts of bone loss and with deep peri-implant pockets are generally associated with large inflammatory lesions. If the bone and attachment loss have occurred in a relatively short period of time, the disease process may be viewed as an aggressive or rapidly progressing form of peri-implantitis. In line with what seems to be true for treatment of aggressive and chronic periodontitis (Teughels et al. 2014), aggressive peri-implantitis might be more difficult to threat than slowly progressing peri-implantitis. In implants with large amounts of bone loss a substantial part of the rough, screw-shaped implant surface becomes exposed to the oral environment and is covered with a biofilm. In these 164
14 cases, complete biofilm removal, by the surgeon during surgery and by the patient after surgery, might be more difficult to achieve than in cases with only minor bone loss and mainly smooth surfaces to be cleaned. In addition, the unfavorable configurations with regard to neighboring teeth that can develop as a result of substantial bone loss (angular defects and deflecting gingival/mucosal margin) might hinder proper cleaning of the implant and may hamper treatment success. Early diagnosis of peri-implantitis seems crucial for achieving a successful peri-implantitis treatment outcome. Two out of the three major risk factors for development of peri-implantitis (Heitz- Mayfield 2008), were also identified as prognostic indicators for peri-implantitis treatment outcome, being smoking and, to a lesser extent, presence of plaque. A history of periodontitis could not be identified as prognostic indicator, which might be due to the fact that a substantial proportion of patients was fully edentulous and data on history of periodontitis was mainly based on self-reported information. Smoking, a known risk factor for peri-implantitis (Heitz-Mayfield 2008), is also a major risk factor for periodontitis (Bergström 2006). It has been shown that smoking negatively influences periodontitis treatment outcomes (Bergström 2006, Labriola et al. 2005) and that smoking cessation results in better treatment results (Chambrone et al. 2013). The results of the present study are in line with this observation and the findings of Charalampakis et al. (2011), who also showed an association between smoking and poor peri-implantitis treatment outcomes. Although this association could not be established in prospective studies up to now (Serino & Turri 2011, Heitz-Mayfield et al. 2012), it seems advisable to encourage smokers with peri-implantitis to abandon smoking as part of their peri-implantitis treatment strategy. The variable presence of plaque after surgery was not statistically significant (p = 0.11 in multiple regression analysis), but may still be considered a relevant prognostic indicator for peri-implantitis treatment. Patients with plaque at their implants at any moment during the follow-up period (at T 3, T 6 and T 12 ) showed higher failure rates than patients with good oral hygiene, which is in line with observations made by others (Lagervall & Jansson 2013). A high standard of oral hygiene and participation in a recall system seem important, both for prevention of peri-implant disease (Anner et al. 2010, Costa et al. 2012) as well as maintenance of stable peri-implant conditions after periimplantitis surgery (Serino et al. 2014). In conclusion, the present study is an analysis of the pooled data of two previously conducted studies. The data sets of the two studies could be meaningfully combined because the research protocols were almost identical, patient groups were similar and treatments were performed by the same surgical team. The outcome of a surgical peri-implantitis treatment is most significantly influenced by the amount of experience of the surgical team with that specific procedure. The observed learning effect has consequences for clinical practice and for conducting and interpreting clinical trials on treatment of peri-implantitis. Other factors that influence the treatment outcome are amount of peri-implant bone loss at baseline and smoking, and to a lesser extent, probing pocket depth at baseline and presence of plaque during follow-up. Early diagnosis of peri-implantitis and control of behavioral factors are crucial in achieving peri-implantitis treatment success. Prognostic indicators 165
15 Conflict of interest and source of funding statement The study was financed by the University Medical Center Groningen. Co-authors E.G. Winkel and A.J. van Winkelhoff have stock ownership in Dentaid BeNeLux B.V. via their company LabOral International B.V. CHAPTER 8 166
16 References Anner R., Grossmann Y., Anner Y. & Levin L. (2010) Smoking, diabetes mellitus, periodontitis, and supportive periodontal treatment as factors associated with dental implant survival: a long-term retrospective evaluation of patients followed for up to 10 years. Implant Dentistry 19, Atieh M.A., Alsabeeha N.H., Faggion Jr. C.M. & Duncan W.J. (2013) The frequency of peri-implant diseases: a systematic review and meta-analysis. Journal of Periodontology 84, Bergström J. (2006) Periodontitis and smoking: an evidence-based appraisal. Journal of Evidencebased Dental Practice 6, Clinical Periodontology 40, Esposito M., Grusovin M.G. & Worthington H.V. (2012) Interventions for replacing missing teeth: treatment of peri-implantitis. Cochrane Database of Systematic Reviews (Online) 1, CD Geckili O., Bilhan H., Geckili E., Cilingir A., Mumcu E. & Bural C. (2014) Evaluation of possible prognostic factors for the success, survival, and failure of dental implants. Implant Dentistry 23, Heitz-Mayfield L.J., Salvi G.E., Mombelli A., Faddy M., Lang N.P. & Implant Complication Research Group. (2012) Anti-infective surgical therapy of periimplantitis. A 12-month prospective clinical study. Clinical Oral Implants Research 23, Chambrone L., Preshaw P.M., Rosa E.F., Heasman P.A., Romito G.A., Pannuti C.M. & Tu Y.K. (2013) Effects of smoking cessation on the outcomes of nonsurgical periodontal therapy: a systematic review and individual patient data meta-analysis. Journal of Clinical Periodontology 40, Charalampakis G., Rabe P., Leonhardt Å. & Dahlén G. (2011) A follow-up study of peri-implantitis cases after treatment. Journal of Clinical Periodontology 38, Cook J.A., Ramsay C.R. & Fayers P. (2004) Statistical evaluation of learning curve effects in surgical trials. Clinical Trials 1, Costa F.O., Takenaka-Martinez S., Cota L.O., Ferreira S.D., Silva G.L. & Costa J.E. (2012) Peri-implant disease in subjects with and without preventive maintenance: a 5-year follow-up. Journal of Clinical Periodontology 39, De Waal Y.C., Raghoebar G.M., Meijer H.J., Winkel E.G. & Van Winkelhoff A.J. (2014) Implant decontamination with 2% chlorhexidine during surgical peri-implantitis treatment: a randomized, doubleblind, controlled trial. Clinical Oral Implants Research [Epub ahead of print] De Waal Y.C., Raghoebar G.M., Huddleston Slater J.J., Meijer H.J., Winkel E.G. & Van Winkelhoff A.J. (2013a) Implant decontamination during surgical peri-implantitis treatment: a randomized, doubleblind, placebo-controlled trial. Journal of Clinical Periodontology 40, De Waal Y.C., Van Winkelhoff A.J., Meijer H.J., Raghoebar G.M. & Winkel E.G. (2013b) Differences in peri-implant conditions between fully and partially edentulous subjects: a systematic review. Journal of Heitz-Mayfield L.J. (2008) Peri-implant diseases: diagnosis and risk indicators. Journal of Clinical Periodontology 35, Labriola A., Needleman I. & Moles D.R. (2005) Systematic review of the effect of smoking on nonsurgical periodontal therapy. Periodontology , Lagervall M. & Jansson L.E. (2013) Treatment outcome in patients with peri-implantitis in a periodontal clinic: a retrospective study. Journal of Periodontology 84, Lindhe J., Meyle J. & Group D of European Workshop on Periodontology. (2008) Peri-implant diseases: Consensus Report of the Sixth European Workshop on Periodontology. Journal of Clinical Periodontology 35, Ramsay C.R., Wallace S.A., Garthwaite P.H., Monk A.F., Russell I.T. & Grant A.M. (2002) Assessing the learning curve effect in health technologies. Lessons from the nonclinical literature. International Journal of Technology Assessment in Health Care 18, Ramsay C.R., Grant A.M., Wallace S.A., Garthwaite P.H., Monk A.F. & Russell I.T. (2000) Assessment of the learning curve in health technologies. A systematic review. International Journal of Technology Assessment in Health Care 16, Roccuzzo M., Bonino F., Bonino L. & Dalmasso P. (2011) Surgical therapy of peri-implantitis lesions by means of a bovine-derived xenograft: comparative results of a prospective study on two different implant surfaces. Journal of Clinical Periodontology 38, Schwarz F., Sahm N., Iglhaut G. & Becker J. (2011) Impact of the method of surface debridement and Prognostic indicators 167
17 decontamination on the clinical outcome following combined surgical therapy of peri-implantitis: a randomized controlled clinical study. Journal of Clinical Periodontology 38, Serino G., Turri A. & Lang N.P. (2014) Maintenance therapy in patients following the surgical treatment of peri-implantitis: a 5-year follow-up study. Clinical Oral Implants Research [Epub ahead of print] Serino G. & Turri A. (2011) Outcome of surgical treatment of peri-implantitis: results from a 2-year prospective clinical study in humans. Clinical Oral Implants Research 22, Teughels W., Dhondt R., Dekeyser C. & Quirynen M. (2014) Treatment of aggressive periodontitis. Periodontology , CHAPTER 8 Thierbach R. & Eger T. (2013) Clinical outcome of a nonsurgical and surgical treatment protocol in different types of peri-implantitis: a case series. Quintessence International 44,
18 169 Prognostic indicators
19
University of Groningen
 University of Groningen Implant decontamination during surgical peri-implantitis treatment de Waal, Yvonne; Raghoebar, Gerry; Slater, J.J.R.; Meijer, Hendrikus; Winkel, Edwin; van Winkelhoff, Arie Jan
University of Groningen Implant decontamination during surgical peri-implantitis treatment de Waal, Yvonne; Raghoebar, Gerry; Slater, J.J.R.; Meijer, Hendrikus; Winkel, Edwin; van Winkelhoff, Arie Jan
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
The International Journal of Periodontics & Restorative Dentistry
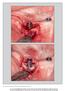 The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Porous titanium granules in the treatment of peri-implant osseous defects a 7-year follow-up study
 Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease?
 C L I N I C A L Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease? Johan Hartshorne 1 A critical appraisal of a systematic review: A. Monje, L. Aranda, K.T. Diaz,
C L I N I C A L Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease? Johan Hartshorne 1 A critical appraisal of a systematic review: A. Monje, L. Aranda, K.T. Diaz,
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Periodontitis & Implants
 Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
University of Groningen. BNP and NT-proBNP in heart failure Hogenhuis, Jochem
 University of Groningen BNP and NT-proBNP in heart failure Hogenhuis, Jochem IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen BNP and NT-proBNP in heart failure Hogenhuis, Jochem IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
University of Groningen. Immediate dental implant placement in the aesthetic zone Slagter, Kirsten
 University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta
 Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
University of Groningen. Soft tissue development in the esthetic zone Patil, Ratnadeep Chandrakant
 University of Groningen Soft tissue development in the esthetic zone Patil, Ratnadeep Chandrakant IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Soft tissue development in the esthetic zone Patil, Ratnadeep Chandrakant IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Retrospective analysis of periimplantitis therapy
 Retrospective analysis of periimplantitis therapy of 158 implants Abstract Objective Jörg-Ulf Wiegner, a Hermann Klinsmann a & Toralf Kömmling b a Private practice, Saalfeld, Germany b Private practice,
Retrospective analysis of periimplantitis therapy of 158 implants Abstract Objective Jörg-Ulf Wiegner, a Hermann Klinsmann a & Toralf Kömmling b a Private practice, Saalfeld, Germany b Private practice,
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Citation for published version (APA): Otten, M. P. T. (2011). Oral Biofilm as a Reservoir for Antimicrobials Groningen: University of Groningen
 University of Groningen Oral Biofilm as a Reservoir for Antimicrobials Otten, Marieke Petronella Theodora IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Oral Biofilm as a Reservoir for Antimicrobials Otten, Marieke Petronella Theodora IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Clinical outcomes following surgical treatment of peri-implantitis at grafted and non-grafted implant sites: a retrospective analysis
 Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Treatment Concepts for PERI-IMPLANTITIS
 Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
University of Groningen. Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella
 University of Groningen Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Interrelationship between Periodontitis and Peri-Implantitis: Myth or Reality?
 REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study
 Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
The notable success of dental implants. Relationship Between Smoking and Bleeding on Probing RESEARCH
 RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
PERIODONTAL CASE PRESENTATION - 1
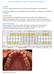 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
University of Groningen. Restorative dentistry done digitally Schepke, Ulf
 University of Groningen Restorative dentistry done digitally Schepke, Ulf IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Restorative dentistry done digitally Schepke, Ulf IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Citation for published version (APA): Schortinghuis, J. (2004). Ultrasound stimulation of mandibular bone defect healing s.n.
 University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Citation for published version (APA): Ebbes, P. (2004). Latent instrumental variables: a new approach to solve for endogeneity s.n.
 University of Groningen Latent instrumental variables Ebbes, P. IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Latent instrumental variables Ebbes, P. IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Frank Schwarz *, Andrea Schmucker and Jürgen Becker
 Schwarz et al. International Journal of Implant Dentistry (2015) 1:22 DOI 10.1186/s40729-015-0023-1 REVIEW Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis
Schwarz et al. International Journal of Implant Dentistry (2015) 1:22 DOI 10.1186/s40729-015-0023-1 REVIEW Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
The International Journal of Periodontics & Restorative Dentistry
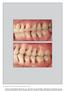 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr.
 Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Periodontal Treatment Guide
 Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Key words: Peri- implant Mucositis, Peri- implantitis, Peri- implant Diseases, Treatment
 PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions
 Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Improving quality of care for patients with ovarian and endometrial cancer Eggink, Florine
 University of Groningen Improving quality of care for patients with ovarian and endometrial cancer Eggink, Florine IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Improving quality of care for patients with ovarian and endometrial cancer Eggink, Florine IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Outcome of dental implants in patients with a history of periodontitis
 Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
University of Groningen. Real-world influenza vaccine effectiveness Darvishian, Maryam
 University of Groningen Real-world influenza vaccine effectiveness Darvishian, Maryam IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
University of Groningen Real-world influenza vaccine effectiveness Darvishian, Maryam IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
European Federation of Periodontology
 The 1999 classification system was the first to recognise the need to classify gingival diseases and conditions, but there were many flaws in its approach. It did not define health and the description
The 1999 classification system was the first to recognise the need to classify gingival diseases and conditions, but there were many flaws in its approach. It did not define health and the description
Principles of Periodontal Instrumentation. Periodontology I - 4th year 23/2/2012 Dr. Murad Shaqman
 Principles of Periodontal Instrumentation Periodontology I - 4th year 23/2/2012 Dr. Murad Shaqman Outline Classification of periodontal instruments General principles of instrumentation Principles of scaling
Principles of Periodontal Instrumentation Periodontology I - 4th year 23/2/2012 Dr. Murad Shaqman Outline Classification of periodontal instruments General principles of instrumentation Principles of scaling
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera
 Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series
 Rima Jaiswal et al Case Report 10.5005/jp-journals-10012-1146 Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series 1 Rima Jaiswal, 2 S Mahantesha, 3 S Ashwini ABSTRACT Introduction:
Rima Jaiswal et al Case Report 10.5005/jp-journals-10012-1146 Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series 1 Rima Jaiswal, 2 S Mahantesha, 3 S Ashwini ABSTRACT Introduction:
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature
 The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Introduction to Periodontal and Implant Surgery
 Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Introduction to Periodontal and Implant Surgery Professor Jon B. Suzuki, DDS, PhD, MBA Temple University Professor of Microbiology and Immunology (Med) Professor of Periodontology and Oral Implantology
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran
 Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Flapless Dental Implantation using Cortex Implants
 Flapless Dental Implantation using Cortex Implants By Dr. Meir Mamraev DMD LLB W e P r o v e I t E v e r y D a y The following case study discusses the flapless implant surgery approach using the Cortex
Flapless Dental Implantation using Cortex Implants By Dr. Meir Mamraev DMD LLB W e P r o v e I t E v e r y D a y The following case study discusses the flapless implant surgery approach using the Cortex
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
The Microbial Etiology and Pathogenesis of Peri-Implantitis
 The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
The International Journal of Periodontics & Restorative Dentistry
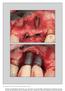 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
J. A. H. Lindeboom, J. W. H. Frenken, P. Valkenburg & H. P. van den Akker. Introduction. Abstract
 The role of preoperative prophylactic antibiotic administration in periapical endodontic surgery: a randomized, prospective double-blind placebo-controlled study J. A. H. Lindeboom, J. W. H. Frenken, P.
The role of preoperative prophylactic antibiotic administration in periapical endodontic surgery: a randomized, prospective double-blind placebo-controlled study J. A. H. Lindeboom, J. W. H. Frenken, P.
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Implantology without Periodontology is like Yin without Yang.
 Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna
 University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
Referral of Patients. to the. Community Dental Referral Service. Hillingdon
 Referral of Patients to the Community Dental Referral Service In Hillingdon June 2012 1 Contents Page Background 3 Best use of Resources 3 Process for Referral 3-4 Acceptance Criteria for Specialist Treatment
Referral of Patients to the Community Dental Referral Service In Hillingdon June 2012 1 Contents Page Background 3 Best use of Resources 3 Process for Referral 3-4 Acceptance Criteria for Specialist Treatment
PERI-IMPLANTITIS A PROBLEM.
 PERI-IMPLANTITIS A PROBLEM. Infections around implants are stubborn. What can help? What doesn t? How can infections be prevented? Geistlich News 02 2014 5 Illustration: Büro Haeberli How prevalent is
PERI-IMPLANTITIS A PROBLEM. Infections around implants are stubborn. What can help? What doesn t? How can infections be prevented? Geistlich News 02 2014 5 Illustration: Büro Haeberli How prevalent is
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
Complex Exodontia. Jone Kim, DDS, MS
 Complex Exodontia Jone Kim, DDS, MS Diplomate, American Board of Oral & Maxillofacial Surgery Lecturer, UCLA School of Dentistry, Dept. of Oral & Maxillofacial Surgery Principle of Complex Exodontia Principle
Complex Exodontia Jone Kim, DDS, MS Diplomate, American Board of Oral & Maxillofacial Surgery Lecturer, UCLA School of Dentistry, Dept. of Oral & Maxillofacial Surgery Principle of Complex Exodontia Principle
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Peri-implantitis. Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
 Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1002/JPER.16-0350 2017 WORLD WORKSHOP Peri-implantitis Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1002/JPER.16-0350 2017 WORLD WORKSHOP Peri-implantitis Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
University of Groningen. Diminished ovarian reserve and adverse reproductive outcomes de Carvalho Honorato, Talita
 University of Groningen Diminished ovarian reserve and adverse reproductive outcomes de Carvalho Honorato, Talita IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Diminished ovarian reserve and adverse reproductive outcomes de Carvalho Honorato, Talita IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Immediate Implants: New Opportunities and Contraindications
 Immediate Implants: New Opportunities and Contraindications Immediate implants are becoming more common and the goal of every immediate implant is to place an implant that is just as healthy with the same
Immediate Implants: New Opportunities and Contraindications Immediate implants are becoming more common and the goal of every immediate implant is to place an implant that is just as healthy with the same
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis
 Journal of Dental Research, Dental Clinics, Dental Prospects Original Article Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis Zeinab
Journal of Dental Research, Dental Clinics, Dental Prospects Original Article Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis Zeinab
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
An intriguing case of gingival enlargement associated with generalised aggressive periodontitis
 CLINICAL REPORT 295 Ajay Mahajan, Jaya Dixit, Umesh Verma An intriguing case of gingival enlargement associated with generalised aggressive periodontitis KEY WORDS antimicrobial therapy, clinical findings,
CLINICAL REPORT 295 Ajay Mahajan, Jaya Dixit, Umesh Verma An intriguing case of gingival enlargement associated with generalised aggressive periodontitis KEY WORDS antimicrobial therapy, clinical findings,
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment
 The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
