Randomized, prospective, clinical evaluation of prosthodontic modalities for mandibular implant overdenture treatment
|
|
|
- Dwight Todd
- 6 years ago
- Views:
Transcription
1 Randomized, prospective, clinical evaluation of prosthodontic modalities for mandibular implant overdenture treatment David R. Burns, DMD, a John W. Unger, DDS, b James P. Coffey, DDS, MS, c Thomas C. Waldrop, DDS, MS, d and Ronald K. Elswick, Jr, PhD e Virginia Commonwealth University, Richmond, Va Statement of problem. Mandibular implant overdentures provide improved treatment outcome than conventional denture therapy, but there is controversy as to which overdenture treatment is the best choice. Purpose. This study evaluated 3 different mandibular implant overdenture treatments with respect to prosthesis retention and stability, tissue response, patient satisfaction and preference, and complications to determine treatment outcomes. Material and methods. In a prospective, randomized clinical trial, using a crossover design, 30 subjects (mean age, 58.9; 63% male) received 4 implants in the anterior mandible. For each subject, 3 different overdenture attachment types were fabricated and/or fitted to the implants. These included a 4-implant bar attachment fitted to all 4 implants, a 2-implant bar attachment, and 2 independent ball attachments. Subjects were randomly assigned to 1 of 6 possible treatment sequences and received all 3 attachment types each for approximately 1 year. Data were collected at baseline, and at 6 and 12 months for treatment types. Denture retention and stability and parameters of soft tissue response were recorded. Complications were documented and questionnaires were used to identify subject masticatory ability, denture complaints, and preferences. Data were analyzed to determine statistical equivalence among the 3 different treatments using the Schuirmann s two one-sided test (TOST) procedure, and the Wilcoxon-Mann-Whitney TOST procedure (α=.05). Results. Force gauge prosthesis retention measurements showed that the 3 treatment types were t statistically equivalent, with the 4-implant bar demonstrating the greatest retention. Criterion-based retention scores were statistically equivalent for all treatments. Both the force gauge and criterion-based prosthesis stability measurements were statistically equivalent among all 3 treatment types. Analysis of all other multiple criterion-based scoring systems indicated the majority of these variables demonstrated equivalence. Where equivalence was t identified, the most favorable responses were typically found with the O-ring treatment, and the least favorable with the 4-implant bar treatment. From the small percentage of treatment visits demonstrating mir complications, single treatment presented with greater complications than the others. For the treatment preference among subjects, 52% selected the independent ball attachment, 32% the 4-implant bar, and 16% the 2-implant bar (P=.10). Conclusions. The 2-implant independent treatment used in this study provided equivalent or more favorable treatment outcomes for most measured parameters relative to the more complex and costly 2- and 4-implant bar attachments. The 4-implant bar treatment provided greater prosthesis retention than the other treatment types in this study, but after experience with all systems, subjects were more satisfied with and preferred the independent implant treatment. (J Prosthet Dent 2011;106:12-22) Supported by grant #R01 DE12204 from The National Institute of Dental and Craniofacial Research. a Professor, Department of Prosthodontics, School of Dentistry. b Professor and Chair, Department of Prosthodontics, School of Dentistry. c Associate Professor, Department of Prosthodontics, School of Dentistry. d Professor and Program Director, Department of Periodontics, School of Dentistry. e Professor, Department of Biostatistics, School of Medicine.
2 July Clinical Implications The 2-implant independent mandibular implant overdenture treatment is preferred by patients to the bar attachment treatments. This preference occurs despite greater prosthesis retention with the 4-implant bar. The benefits of implant-retained/ supported mandibular implant overdenture (IOD) treatment relative to conventional mandibular denture treatment have been well documented. 1-9 Half of all conventional mandibular dentures demonstrate problems with prosthesis stability and retention, with retention being the single most important deficiency reported. 10 Feine et al 11 and Thomason et al 12 stated that for the edentulous mandible, a 2-implant overdenture treatment should be the standard of care relative to conventional denture treatment. Enhanced prosthesis retention and stability have been identified as perhaps the most important factors for producing more favorable mandibular IOD treatment outcome and improved patient satisfaction. 2,10,13 Mandibular IOD prosthesis retention, stability, and support are provided by both the mucosa and implants. As increasing numbers of implants are used, it is possible they will assume a greater role with treatment outcome, particularly involving prosthesis support. 14 However, more implants may t translate to improved prosthesis retention and/or stability, and subsequent treatment outcome may be relatively unaltered, 14 other than a slight increased risk from additional treatment and added expense. Zarb and Schmitt 15 and Visser et al 16 indicated that successful IOD treatment outcome can be achieved regardless of the number of implants used, but this concept remains controversial. 14 Two implants have been considered the minimum necessary for mandibular IOD treatment 1,15 and can be used either with independent, unsplinted attachments or splinted together using a cast metal bar and a bar-clip attachment. 17 Four implants splinted with 3 interconnecting bar and bar-clip attachments is ather treatment alternative. With a lack of consensus regarding the number of implants necessary for mandibular implant overdenture treatment, the best choice of an attachment mechanism between the implants and denture base also remains controversial. 14,18 Wismeijer et al 19 studied 110 mandibular IOD patients, who received either 2 implants with a ball attachment, 2 implants with an interconnecting bar, or 4 implants splinted with 3 bars. Treatment outcome was measured using patient questionnaires. Nearly all subjects were satisfied with treatment after 16 months, and statistical difference was found among the 3 treatment strategies. The authors concluded that the 2-implant ball attachment treatment was a good choice, but the need for additional clinical trials was emphasized. Mau et al 20 conducted a randomized study to evaluate 2-versus 4-implant bar attachments. The authors found a higher rate of complication for the 4-implant design, but in terms of treatment efficacy, both methodologies were the same after 5 years of service. Using 3-dimensional finite-element analysis, Meijer et al 21 studied bone stress in the anterior mandible surrounding implants when either 2 or 4 implants were used for IOD treatment. The authors concluded that when the occlusal load was distributed over increasing numbers of implants, there was reduction in the principal bone stresses surrounding the individual implants. Timmerman et al 22 reported that after 8 years, subjects from their study were more satisfied with a 2-implant single bar treatment than either 2 independent implants with ball attachments or 4 implants with 3 bars. They suggested that patient satisfaction was linked to prosthesis retention and stability, and t the number of implants used. Cune et al 23 measured patient satisfaction using a crossover design, where 18 subjects received 2 implants, and then in a randomized order, received magnetic, bar-clip, or ball attachments, each for a 3-month period. Questionnaires were used to register complaints, satisfaction, and preference. The authors reported that after subjects experienced all treatments, 1 subject preferred the magnetic attachment, 7 preferred the ball attachment, and 10 preferred the bar-clip. Walton et al 24 evaluated time and cost factors associated with IOD. Sixty-four subjects received 2 mandibular implants and either a bar with 2 clips or 2 ball attachments. The authors found that subjects were equally satisfied with their treatments, but 84% of subjects with the ball attachment required at least 1 repair versus 20% for the bar-clip attachment. They concluded that because of the lower rate of repair, the bar-clip design was a better choice. However, Watson et al 25 stated that all IOD attachments required significant post insertion maintenance, but there were advantages to using independent implant attachments relative to bar attachment designs. The free-standing attachments required less space within a denture base; they were easier for a patient to keep clean; the initial prosthodontic treatment was less involved and more ecomical to perform; and routine maintenance, such as denture relines, was easier to manage. Gotfredsen and Holm 26 studied maintenance requirements for both ball and bar attachments over a
3 14 Volume 106 Issue 1 5-year period. They found that during the first year, there were significantly more complications requiring repairs with the bar group relative to the ball group. After the first year, there was significant difference between the 2 groups. Naert et al 17 compared prosthodontic treatment and subject satisfaction with splinted versus unsplinted 2-implant mandibular IODs in 36 subjects over a 10-year period. The authors found that at year 10, the ball attachment provided better prosthesis retention and patient satisfaction, with fewer soft tissue complications relative to bar or magnetic attachment designs. The bar attachment negatively influenced the opposing maxillary denture in terms of comfort and stability. Stoker et al 27 provided a cost analysis of initial treatment and aftercare expenses associated with 3 mandibular IOD treatments over an 8-year period. The authors compared a 4-implant bar, a 2-implant bar, and a 2-implant ball attachment. They found that aftercare patient expenses were comparable for all treatments, but initial costs represented 75% of the total costs, and were significantly higher for the 4-implant treatment relative to the 2-implant varieties. The hypothesis of this study was that clinical treatment outcomes using measured parameters to define prosthesis performance and patient satisfaction/preference for the various mandibular IOD treatment modalities were equivalent. If the hypothesis were supported, it would imply that a 2-independent implant treatment option might be preferred because the more costly and complex treatment involving additional implants and bar splinting would provide similar treatment outcomes to those using less costly and simpler solutions. MATERIAL AND METHODS This study was a prospective, randomized clinical trial, using a crossover design to prospectively test the statistical equivalence among the 3 different mandibular IOD treatments. In contrast to the typical clinical trial, in which the intent is to demonstrate the superiority of one treatment over ather, the goal of this study was to demonstrate equivalence among the 3 treatment types. Preliminary data were gathered during a previous study and were used for the statistical power analysis. 1,2 Equivalence testing with dental clinical trials was described in a previous study. 28 It was determined that 30 subjects were required to provide appropriate statistical power, and additionally, allow for a potential 25% subject dropout over the course of the study. Prospective subjects were all patients of record at Virginia Commonwealth University School of Dentistry, and all had conventional complete denture experience for at least one year. Inclusion criteria included adult patient, male or female, at least 1 year of previous conventional complete denture treatment history, willingness to accept the conditions of the study and freely provide informed consent, ability to participate for at least 6 years, ability to understand and respond to self-reporting measurement scales used in the study, a minimum of 20- mm interarch distance at the estimated occlusal vertical dimension, bone quality of 1 or 2 according to the Lekholm and Zarb criteria, 29 and adequate bone quantity to minimally accommodate 4 (3.75mm diameter) implants (Brånemark; Nobel Biocare USA, Yorba Linda, Calif ) anterior to the mental foramen bilaterally. Exclusion criteria included administrative or physical considerations that would seriously affect the surgical procedure or constitute a hindrance for a 6-year involvement, history of drug or alcohol abuse, excessive smoking (1+ pack/day), uncontrolled systemic disease, inability to undergo mir oral surgery because of health or personal reasons, irradiated surgical site, unrealistic expectations of the prosthodontic treatment outcome, psychological or psychiatric conditions that could influence the subject s reaction to treatment, acute or chronic temporomandibular disorder (TMD) problems, pregnancy, class II jaw relationship, and after informed consent, conventional dental treatment as the treatment of choice. Selected subjects were required to provide written informed consent. The study was approved and continuously monitored by an internal Institutional Review Board and an external National Institutes of Health, Data and Safety Monitoring Board. Eighty-seven potential subjects were screened and of these, 51 were excluded due to failure to meet inclusion criteria or willingness to sign the informed consent. Thirty-six subjects were enrolled and provided informed consent. Six of these subjects dropped out for various reasons after enrollment, but before implant placement. Thirty subjects provided pretreatment demographic information. After implant placement and during the course of the investigation, 3 subjects were discontinued from the study and therefore provided postintervention data. One was removed because of compliance concerns regarding prosthesis use. This subject was diagsed with Alzheimer s disease and was unable to communicate effectively as to his treatment satisfaction, complications, and preferences. The second subject was unable to continue because of his wife s chronic illness and inability to return for data collection. A third subject died due to a ruptured coronary aneurysm. Demographic data for enrolled subjects with postintervention data are presented in Table I. Four implants (Brånemark Nobel Biocare USA) were placed anterior to the mental foramen bilaterally in the mandible of each subject using conventional 2-stage surgical techniques. 30 All subjects received 3.75 mm diameter implants, but implant length varied for each subject to provide the most favorable treatment progsis. A presurgical trial denture was fabricated and used to produce a surgical implant guide for each sub-
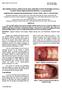
4 July Table I. Demographic summary (n=27) Enrolled with Postintervention Data Male Female ject. Implants were allowed to integrate for 4 to 6 months. After healing, all implants were required to show evidence of implant mobility, radiographic periimplant radiolucency, or pain. 31 Two implants failed during the course of the investigation by becoming mobile during the integration phase. These implants were retreated and were successful thereafter. Upon successful integration of 4 implants, soft tissue height measurements were made and standard abutments (Nobel Biocare USA) were selected for each implant. Mandibular bar attachment kits (Overdenture Kit, with gold bar; Nobel Biocare USA) were used to fabricate the 2-implant and 4-implant bar attachments. The 2-implant O-ring attachment (Ball Attachment; Nobel Biocare USA) was selected for each subject. The mandibular IOD definitive cast impression was made with the completed 4-implant bar positioned intraorally. Subsequently, the completed mandibular IOD had space allocated in the denture base to accommodate the 4-implant bar, the largest of the treatment types to be tested. Definitive denture Frequency (%) 17 (63%) 10 (37%) Mean (SE) Subject age 58.9 (1.87) Maxillary Mandibular Maxillary Mandibular Mean (SE) Years Edentulous 9.8 (2.08) 6.8 (1.85) Mean (SE) Years with Current Denture 2.1 (0.77) 1.1 (0.18) treatment was completed in both arches using a flat occlusal plane and 0-degree teeth. A crossover design was used in this investigation; each subject received all 3 attachment systems over the course of the trial. Specifically, a 4-period (12 month duration/period), a 6-sequence (A-B-C-C; A-C-B-B; B-A-C-C; B-C-A-A; C-A-B-B; C-B-A-A), and a 3-treatment crossover experimental design was used. Each of the subjects was randomly assigned to 1 of 6 treatment sequence groups according to a randomization schedule generated by the biostatistician investigator. The 3 implant overdenture treatments consisted of (), an independent O-ring attachment using 2 implants, (), a bar attachment using 2 implants, or (), a bar attachment using 4 implants. The purpose of the fourth period was to allow for testing of an equal carryover effect on the crossover design by repeating the third period data collection for an additional 12 months. During this fourth period, the direct effects of the treatments were estimated more efficiently because they were t confounded with carryover influence. The respective denture bases were fitted and adjusted to the alveolar tissues. Space previously created in the tissue surface of the mandibular denture to correspond with the attachment permitted easy access and orientation for placement of all bar clips or O-ring housings within the denture base, regardless of the treatment type being used. These retentive elements were positioned on their corresponding implant components and secured within the denture base using autopolymerizing acrylic resin (Perm Reline and Repair Resin; The Hygienic Corp, Akron, Ohio), while the prosthesis was accurately and simultaneously positioned on the supporting alveolar tissues (Fig. 1). Resilient lining material (TruSoft; HJ Bosworth, Skokie, ll) was used to provisionally fill the open denture base space t being used when the treatment was t being tested (Fig. 2). Final prosthesis occlusal adjustment was completed after the addition of the attachment mechanism. For standardization, the clips used with all bar attachments were arbitrarily adjusted before installation to 10±0.1 N of retentive quality. This was done by placing each clip on a section of the gold bar material used in this investigation and removing it using a push/pull force gauge (Chatillon 5 kg push/pull force measurement gauge; Hunter Products, Bridgewater, NJ). Crimping adjustments to each clip were accomplished as necessary until the proper retentive force measurement was achieved. In addition to screening demographic and implant integration information, the clinical conditions associated with each subject s preexisting dentures were evaluated and recorded after both preimplant and postimplant placement surgery using each investigative parameter. Thereafter, subjects received the appropriate treatment at approximately 12-month intervals in response to their specific randomized treatment sequence schedule. During this time, denture adjustments were accom-
5 16 Volume 106 Issue 1 1 Space allocated in denture base to accommodate all 3 treatment modalities. attachment were positioned into denture base with autopolymerizing acrylic resin. 2 Provisional denture reline material used to fill open denture base space when t all implants were used. Note imprint of healing abutments in provisional reline material for implants t used for treatment. plished as needed. O-ring replacement (), bar clip replacement (), or adjustment () was completed on an asneeded basis, and the clips were recalibrated when this was done. Data were independently and concurrently recorded by 3 prosthodontic coinvestigators. To address measurement reliability, 2 the observations from the 3 raters were averaged to create a single observation. Data were collected at 6 and 12 months after placement of each attachment system. After 12 months of monitoring and data collection for the first overdenture attachment treatment, all subjects was recalled and their particular attachment system was replaced with the next, as defined by the subject s randomized treatment sequence group. After monitoring and data collection for ather 12 months, the third and final attachment system was placed, and the same monitoring and data collection protocol was followed. This final treatment was sustained for an identical fourth 12-month period of data collection. Subjects were included in the data analysis regardless of outcome during the clinical trial, following the intent to treat principle. All post-implant data were included in the data analysis. Throughout the investigation, the following data collection standardized procedures were uniformly followed: The push/pull force gauge (Chatillon 5 kg) was used to quantitatively measure denture retention and stability. With prostheses in place, subjects sat upright in a dental chair. To measure retention, the pull end of the force gauge was connected to a 15-cm long, 18 gauge orthodontic wire (Great Lakes Orthodontics, Tonawanda, NY) with the ends of the wire bent into a hook. The hook was positioned under the mid-labial flange of the IOD, and the force gauge was pulled vertically upward until denture retention was lost and the prosthesis moved vertically. This force was measured in newtons (N) and recorded. For stability, the push end of the gauge was positioned in the gingival embrasure area of the canine denture tooth on the right side of the prosthesis. The gauge was pushed horizontally against the denture. The force (up to a maximum of 20 N) necessary to destabilize and dislodge a denture was measured and recorded. In addition to this objective analysis, each subject s mandibular denture was evaluated for denture retention and stability with the criteria scoring system previously reported. 1 Examiners independently observed a subject s IOD and recorded the numbered criteria that best described the denture retention and stability. The retention criterion was defined as a score from 0 to 3 with 0 = retention, 1 = minimal retention, 2 = moderate retention, and 3 = good retention. Similarly, the stability criterion was defined as a score from 0 to 2 with 0 = stability, 1 = some stability, and 2 = sufficient stability. The condition of the prosthesissupporting oral mucosa and perimplant health were assessed using multiple criterion-based scoring systems. Where multiple readings were required around individual and multiple implants, a mean score was calculated and recorded. Prosthesis supporting tissues for each arch were evaluated with a scoring system previously reported by. 1 Periimplant parameters were evaluated in the following locations: the Gingival Index as adapted from Loe and Silness 32 and the Plaque Index, as adapted from Silness and Loe, 33 were measured in 4 locations around each implant; measurements of the amount of keratinized mucosa were measured according to Apse et al 34 in 2 locations around each implant; the attachment level was measured in millimeters from the top of the implant to the level of implant-tissue attachment in 4 locations for each implant. The probing depth as adapted from Geertman et al 35 was measured in 4 locations in millimeters around each implant, and radiographic evaluation
6 July 2011 of each implant, as adapted from Geertman et al 35 was recorded from a paramic radiograph made for each treatment at the 12-month data collection appointment. Additionally, the radiographic bone-crest to inferior border-of-mandible measurement in millimeters was recorded for each implant, and the radiographic mandibular symphyseal bone height was recorded. Implant mobility was assessed by tapping the abutments alternatively back and forth with 2 instrument handles. Observable movement was identified as evidence of individual implant mobility using the criteria suggested by Smith and Zarb. 36 At each data collection appointment, subjects were asked to complete a 40-item denture complaint questionnaire. 37 Each item was rated on a 4-point scale: 0 = t at all; 1 = a little; 2 = quite a lot; 3 = extremely. The maximum score was 120 and the minimum score was 0, where lower scores corresponded to greater denture satisfaction. Additionally, an 8-item masticatory ability questionnaire was used that asked how well 8 different foods could be masticated. 38,39 The 8 items were answered according to a 3-point scale: 0 = good; 1 = moderate; 2 = bad. The maximum score was 16 and the minimum score 0, where lower scores corresponded to better masticatory ability. The score from each questionnaire and for each subject was determined and recorded. The clinical implant performance scale (CIP scale) as adapted from Geertman et al 35 was used to assess complications and failures. The CIP scale documents complications and categorizes them according to severity. Itemized complications were documented for each subject relative to type, date, and the treatment conditions in use at the time of the complicating outcome. Specific attention was given to ongoing changes in physical or mental health that could influence complications, failures, and adverse events. At the completion of all data collection, when subjects had experi- enced all IOD attachment systems, they were given an IOD treatment preference questionnaire, modified from. 2 It consisted of questions designed to determine subject preference among the 3 implant overdenture treatment modalities tested. Additional assessment of subject preference relative to treatment was established by allowing subjects to choose and receive their favorite treatment type at the end of the data gathering period. To minimize carryover influence, at the completion of a 12-month data collection period for each treatment type, selected tissue criteria scores were required to ensure standardized optimal healthy conditions before the next 12-month time period could begin. This provided an adequate amount of time to washout the effect of previous treatment influence before data collection for the next treatment in the sequence. As a result, it was necessary that the alveolar mucosa tissues were free of pathology with a maxillary and mandibular supporting tissue score of less than 3, a Gingival Index score of 1 or 2, and mobility around any independent, unattached implant. Any mobility excluded a subject from further study participation. If minimum scores were t met, at the discretion of the investigators, subjects could be temporarily returned to conventional denture treatment by replacing implant healing abutments and temporarily relining the mandibular denture base with resilient denture base lining material. The next 12-month investigative sequence was only initiated upon successful completion of this interim treatment period. This study used multiple variables as endpoint measurements. Because variation of endpoint outcomes could result in conflicting conclusions, equivalence in this investigation was defined as using prosthesis retention and stability (force gauge and criterion-based measurements) as primary indicators of equivalence. Also, to establish equivalence among treatment modalities, similar results from retention and stability measurements were required, with the largest difference being greater than 20% as documented in Imrey et al. 40 As a result, an adjustment for multiplicity was t required, and an alpha of.05 was used for all comparisons, except for an alpha of.1 for tests of carryover effect. Secondary measures were prosthesis supporting and periimplant tissue response, subject satisfaction and preference, and complications. All endpoints except for the criterion-based retention and stability scores and the IOD treatment preference questionnaire were analyzed to determine statistical equivalence using the Schuirmann s two one-sided tests (TOST) procedure from the 3-treatment, 6-sequence, 4-period, crossover model. The least square means presented in the figures and tables arose from a mixed effects model that included fixed effects for treatment types, sequence, period and carryover, and a random effect for subject. The Schuirmann s TOST was operationalized by calculating the 90% confidence interval about the paired difference between the least square means, and then if this 90% confidence interval fell within the interval ± 20% of the reference mean (for the group), the treatments were declared equivalent. Criterionbased retention and stability were tested for equivalence using the Wilcoxon rank sum TOST procedure. 43 Similar to the Schuirmann s TOST, the n-parametric Wilcoxon tested the equivalence of the medians by first calculating a 90% confidence interval about the median of the Walsh average difference, and then if this 90% confidence interval fell within the interval ± 20% of the reference median (for the group), the treatments were declared equivalent. For the Wilcoxon test, it was t possible to use the fourth period data, thus the testing used the 3-treatment, 6-sequence, 3-period, crossover model. Finally, the IOD treatment preference questionnaire responses were compared 17
7 18 Volume 106 Issue 1 among the 3 treatment modalities using a Chi-square test for superiority. RESULTS The potential influence of any carryover effect was monitored throughout the investigation using the clinical evaluation process previously described. No subjects were delayed from progressing to the next study period due to the influence of previous treatment on the health of the tissues or implants. No independent implant mobility was found for any implant during the investigative phase. Additionally, at the end of the investigation, potential carryover influence was tested for each study variable and statistically significant carryover effect was found. Figures 3 and 4 demonstrate the least mean square force gauge retention and stability values and standard errors. The force gauge retention was t equivalent for any of the 3 treatment types; however, the force gauge stability was equivalent across all 3 treatments. Figures 5 and 6 show the retention and stability criterion-based medians and interquartile range. Both the retention and stability criterionbased medians demonstrated equivalence among the 3 treatments. Table II shows the multiple criterion-based scoring systems used to assess the prosthesis-supporting oral mucosa and periimplant health. Maxillary and mandibular supporting tissue health was found to be equivalent among all treatment groups. Gingival and Plaque Index scores were t equivalent and showed more favorable tissue responses and less plaque associated with the attachment. The had the highest plaque scores and the least desirable Gingival Index scores of the 3 treatments. Other parameters were equivalent for all treatments. Masticatory ability and denture complaint data from subject questionnaires are shown in Figures 7 and 8, respectively. Even though there was demonstration of equivalence in either questionnaire, the and treatments provided the most favorable, and the treatment, the least Force Gauge Retention (N) Force gauge retention. Presented as least square means (± standard errors). Three treatment modalities were t statistically equivalent. Force Gauge Stability (N) Force gauge stability. Presented as least square means (± standard errors). Three treatment modalities were statistically equivalent. Criterion-based Retention Criterion-based Stability Criterion-based retention. Presented as medians (± interquartile range). Three treatment modalities were statistically equivalent Criterion-based stability. Presented as medians (± interquartile range). Three treatment modalities were statistically equivalent.
8 July Table II. Mean values (standard errors) from crossover analysis with results of equivalence testing Treatment * Equivalence Comparison Variable vs. vs. vs. Maxillary supporting tissue score 3.73 (0.08) 3.80 (0.09) 3.78 (0.09) Mandible supporting tissue score 3.73 (0.06) 3.73 (0.06) 3.71 (0.06) Gingival Index score (0.048) (0.048) (0.050) Plaque Index score (0.134) (0.136) (0.146) Probing depth (mm) (0.041) (0.041) (0.041) Keratinized tissue score (0.102) (0.103) (0.104) Attachment level (mm) (0.059) (0.059) (0.059) Radiographic implant bone height (mm) (1.18) (1.18) (1.18) Radiographic mid-symphyseal bone height (mm) (1.16) (1.16) (1.16) * Least square means (± standard errors) from crossover mixed effects model are presented except where ted otherwise. Equivalence assessed by Shuirman s TOST procedure using 3-treatment, 6-sequence, 4-period, crossover model except where ted ** Medians and interquartile range Equivalence assessed by n-parametric Wilcoxon-Mann-Whitney TOST procedure from 3-treatment, 6-sequence, 3-period, crossover model Denture Complaint Questionnaire Masticatory Ability Questionnaire Denture complaint questionnaire. Presented as least square means (± standard errors). 8 Masticatory ability questionnaire. Presented as least square means (± standard errors).
9 20 Volume 106 Issue 1 Table III. Frequency (%) of implant overdenture treatment preference (n=25) Question All Same No Opinion P Overall best satisfied 12 (48%) 8 (32%) 4 (16%) 1 (4%) 0.15 Selected treatment 13 (52%) 8 (32%) 4 (16%) 0.09 Easiest to get used to 11 (44%) 5 (20%) 3 (12%) 6 (24%) 0.12 Best denture retention 9 (36%) 8 (32%) 4 (16%) 4 (16%) 0.43 Best able to chew 11 (44%) 6 (24%) 3 (12%) 5 (20%) 0.14 Best able to speak 7 (28%) 5 (20%) 3 (12%) 10 (40%) 0.62 Greatest movement 4 (16%) 2 (8%) 12 (48%) 5 (20%) 2 (8%) 0.026* Easiest to keep clean 12 (48%) 1 (4%) 2 (8%) 8 (32%) 2 (8%) 0.01** Chi-square test of preference or equal preference * provides statistically significantly greater movement ** statistically significantly easier to keep clean favorable results. For the CIP data, there were complications ted for the vast majority of treatment visits across all 3 treatments. Of the 212 recorded subject visits, in which a subject received CIP ratings from 3 investigators, 93% (n=197) of the subject visits had all 3 ratings scored at 0 (success with complications) and were trouble free. Only 7% (n=15) of the visits included 1 or more of the ratings with a score of 1 (mir complications). None of the subject visits received CIP scores of 2, 3, or, 4. The 12-month CIP mean (SD) scores for the 3 treatment groups were 0.07 (0.28) for the, 0.09 (0.27) for the, and 0.10 (0.27) for the. From the small percentage of treatment visits that demonstrated mir complications, single treatment presented with greater complications. Radiographic bone height levels remained stable over time and equivalent among treatments. Subject treatment preference data are presented in Table III. Most often, subjects preferred treatment as the one to keep after experiencing all treatment options. Overall, subjects were best satisfied with the treatment, which had the highest frequency for all questions except for greatest movement. The showed the most favorable results, with the least favorable results found with the treatment; this was with the exception of the Easiest to keep clean question, where the treatment demonstrated the lowest frequency. DISCUSSION The standardization of methods was an important aspect of this investigation; therefore, all clips used for the bar-clip attachments were standardized to an arbitrary 10 N of retentive quality prior to use. This value was selected because it represented an appropriate retentive quality that subjects had preferred in a previous investigation. 1 The standardization assisted with comparisons among bar-clip attachments, but the 10 N provided an arbitrary retentive quality for the IOD that exceeded that of both the and IOD. This resulted in a greater retentive mean value for the IOD that was t equivalent to that of either the or IOD. Consequently, the study hypothesis was t supported, and the greater retentive mean could be considered an indicator of more favorable treatment. After completion of the study, however, the authors believe that this is directly associated with the arbitrary standardization of the bar clip retentive value and is t a valid conclusion. This is a significant limitation of the study. Currently, many IOD attachment systems allow for the adjustment of retentive quality. Patients may prefer a higher retentive quality, but because retention can be commonly adjusted within a range, the measured retentive quality at any given time may t provide an appropriate measure of treatment outcome. What is interesting about this study result is, that if indeed greater retention were a valid indicator of better treatment outcome, it would be expected that other data from the study would corroborate this finding. Instead, the IOD, with less retention than the IOD, showed equivalent or more favorable results according to other data collected in this study. These other combined data presented a clearer understanding of treatment outcome and provided compelling evidence that the treatment was a more favorable choice than the other treatment types. For instance, with both the masticatory ability and denture complaint questionnaires, the treatment showed more favorable
10 July 2011 responses than the treatment. According to the preference data, nearly half of all subjects were most satisfied with the IOD and more than half preferred and selected the as the treatment they kept after completion of the investigation. In fact, for the preference questionnaire that was completed after subjects experienced all treatments and could make valid judgments, the IOD demonstrated the most favorable responses for most questions. Other factors such as subject treatment preference and satisfaction with prosthesis functional aspects, ease of subject accommodation to a treatment type, tissue health, hygiene and maintenance issues, and complications outweighed the superior retentive features of the 4-implant bar. When these factors were weighed together, prosthesis retention was only one aspect of the entire process. It is t surprising that subjects responded most favorably to the 2 independent-implant treatment, since it provides a satisfactory treatment outcome without the added treatment of 2 additional implants and interconnecting bar attachments. The 2 independent abutments require less space in the denture base, and data from this study demonstrate that they are easier to clean than those with a bar. Since the weak link in conventional mandibular denture treatment is inadequate prosthesis retention and stability, 10 subjects appear to prefer the ability to overcome these issues with only 2 implants that provide a near equivalent outcome to more costly and complex treatments using more implants or bar interconnection between implants. This finding is in agreement with the Feine et al 11 and Thomason et al 12 consensus reports that indicate that for the edentulous mandible, a 2-implant overdenture is the treatment of choice. There were few complications due to attachment-related or other problems. From the complications encountered, single treatment stood out as having more complications than any other. Other studies have found that attachment mechanism compli- cations can be problematic, but there is clear evidence that one treatment is more problematic than ather. 20, Of course the nature of this study involved frequent recall with new treatment on a yearly basis, and therefore, many complications were avoided. The benefits of the crossover design for this implant-related investigation were numerous. 28 The ability to accommodate a variety of treatment types by switching back and forth among implants and abutments worked well. Additionally, because all subjects were able to experience all treatments, fewer subjects required statistical testing, and the completed subject preference information gathered after the routine data collection provided a strong indicator of treatment outcome. Equivalence testing is new to dental research. In essence, if this investigation could prove equivalence among the treatment types, then the less expensive, simpler treatment would be the treatment of choice and the hypothesis would be proven. In a broader sense, results from this study for the IOD can probably be generalized to represent other similar 2-independent-implant treatment types, and this study might provide a greater understanding of the treatment outcomes for more contemporary 2-independent-implant attachment systems. Nonetheless, the O-ring attachment that was used is longer commercially available, a limitation of the study. In this regard, the findings from this study are in agreement with 2 consensus conferences 11,12 that both concluded that the 2-implant, independent IOD treatment was the best choice. CONCLUSIONS The results of this investigation showed that IOD retentive quality was less important than other clinical parameters in determining treatment outcome. Even though prosthesis retention for the IOD was less than the attachment, most other measured parameters showed equivalent or more favorable results for the system when compared with the or attachments. Subjects preferred the attachment to the other choices, and more than half the subjects selected the IOD as their prosthesis after the conclusion of the investigation. REFERENCES 1. Burns DR, Unger JW, Elswick RK Jr, Beck DA. Prospective clinical evaluation of mandibular implant overdentures. Part I: retention, stability and tissue response. J Prosthet Dent 1995;73: Burns DR, Unger JW, Elswick RK Jr, Giglio JA. Prospective clinical evaluation of mandibular implant overdentures. Part II: patient satisfaction and preference. J Prosthet Dent 1995;73: Melas F, Marcenes W, Wright PS. Oral health impact on daily performance in patients with implant-stabilized overdentures and patients with conventional complete dentures. Int J Oral Maxillofac Implants 2001;16: Thomason JM, Lund JP, Chehade A, Feine JS. Patient satisfaction with mandibular implant overdentures and conventional dentures 6 months after delivery. Int J Prosthodont 2003;16: Awad MA, Lund JP, Shapiro SH, Locker D, Klemetti E, Chehade A, et al. Oral health status and treatment satisfaction with mandibular implant overdentures and conventional dentures: a randomized clinical trial in a senior population. Int J Prosthodont 2003;16: Bakke M, Holm B, Gotfredsen K. Masticatory function and patient satisfaction with implant-supported mandibular overdentures: a prospective 5-year study. Int J Prosthodont 2002;15: Doundoulakis JH, Eckert SE, Lindquist CC, Jeffcoat MK. The implant-supported overdenture as an alternative to the complete mandibular denture. J Am Dent Assoc 2003;134: Heydecke G, Thomason JM, Awad MA, Lund JP, Feine JS. Do mandibular implant overdentures and conventional complete dentures meet the expectations of edentulous patients? Quintessence Int 2008;39: van der Bilt A, van Kampen FM, Cune MS. Masticatory function with mandibular implant-supported overdentures fitted with different attachment types. Eur J Oral Sci 2006;114: Redford M, Drury TF, Kingman A, Brown LJ. Denture use and the technical quality of dental prostheses among persons years of age: United States, J Dent Res 1996;75: Feine JS, Carlsson GE, Awad MA, Chehade A, Duncan WJ, Gizani S, et al. The McGill consensus statement on overdentures. Mandibular two-implant overdentures as first choice standard of care for edentulous patients. Montreal, Quebec, May 24-25, Int J Oral Maxillofac Implants 2002;17:
11 22 Volume 106 Issue 1 12.Thomason JM, Feine J, Exley C, Moynihan P, Müller F, Naert I, et al. Mandibular two implant-supported overdentures as the first choice standard of care for edentulous patients-the York Consensus Statement. Br Dent J 2009;207: Naert I, Quirynen M, Theuniers G, van Steenberghe D. Prosthetic aspects of osseointegrated fixtures supporting overdentures. A 4-year report. J Prosthet Dent 1991;65: Burns DR. Mandibular implant overdenture treatment: Consensus and controversy. J Prosthodont 2000;9: Zarb GA, Schmitt A. The longitudinal clinical effectiveness of osseointegrated dental implants: The Toronto study. Part II: The prosthetic results. J Prosthet Dent 1990;64: Visser A, Raghoebar GM, Meijer HJ, Batenburg RH, Vissink A. Mandibular overdentures supported by two or four endosseous implants. A 5-year prospective study. Clin Oral Implants Res 2005;16: Naert I, Alsaadi G, Quirynen M. Prosthetic aspects and patient satisfaction with twoimplant-retained mandibular overdentures: a 10-year randomized clinical study. Int J Prosthodont 2004;17: Naert I, Alsaadi G, van Steenberghe D, Quirynen M. A 10-year randomized clinical trial on the influence of splinted and unsplinted oral implants retaining mandibular overdentures: peri-implant outcome. Int J Oral Maxillofac Implants 2004;19: Wismeijer D, Van Waas MA, Vermeeren JI, Mulder J, Kalk W. Patient satisfaction with implant-supported mandibular overdentures. A comparison of three treatment strategies with ITI-dental implants. Int J Oral Maxillofac Surg 1997:26; Mau J, Behneke A, Behneke N, Fritzemeier CU, Gomez-Roman G, d Hoedt B, et al. Randomized multicenter comparison of 2 IMZ and 4 TPS screw implants supporting bar-retained overdentures in 425 edentulous mandibles. Int J Oral Maxillofac Implants 2003;18: Meijer HJ, Starmans FJ, Steen, WH, Bosman F. A three dimensional finite element study on two versus four implants in an edentulous mandible. Int J Prosthodont 1994;7: Timmerman R, Stoker GT, Wismeijer D, Oosterveld P, Vermeeren JI, van Waas MA. An eight-year follow-up to a randomized clinical trial of participant satisfaction with three types of mandibular implant-retained overdentures. J Dent Res 2004;83: Cune M, van Kampen F, van der Bilt A, Bosman F. Patient satisfaction and preference with magnet, bar-clip, and ball-socket retained mandibular implant overdentures: a cross-over clinical trial. Int J Prosthodont 2005;18: Walton JN, MacEntee MI, Glick N. One-year prosthetic outcomes with implant overdentures: a randomized clinical trial. Int J Oral Maxillofac Implants 2002;17: Watson CJ, Tinsley D, Sharma S. Implant complications and failures: the complete overdenture. Dent Update 2001;28:234-8, Gotfredsen K, Holm B. Implant-supported mandibular overdentures retained with ball or bar attachments: a randomized prospective 5-year study. Int J Prosthodont 2000;13: Stoker GT, Wismeijer D, van Waas MA. An eight-year follow-up to a randomized clinical trial of aftercare and cost-analysis with three types of mandibular implant-retained overdentures. J Dent Res 2007;86: Burns DR, Elswick RK Jr. Equivalence testing with dental clinical trials. J Dent Res 2001;80: Lekholm U, Zarb GA. Patient selection and preparation. in: Branemark P, Zarb GA, Albrektsson T (ed.). Tissue Integrated Prosthesis, 1st ed. Chicago: Quintessence Publishing Co; p Branemark P, Zarb GA, Albrektsson T (ed.). Tissue Integrated Prosthesis. 1st ed. Chicago: Quintessence Publishing Co; p Smith DE, Zarb GA. Criteria for success of osseointegrated endosseous implants. J Prosthet Dent 1989;62: Loe H, Silness J. Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand 1963;21: Silness P, Loe H. Periodontal disease in pregnanacy. Acta Odontol Scand 1964;22: Apse P, Zarb GA, Schmitt A, Lewis DW. The longitudinal effectiveness of osseointegrated dental implants. The Toronto study: peri-implant mucosal response. Int J Periodont Restorative Dent 1991;11: Geertman ME, Boerrigter EM, Van Waas MA, van Oort RP. Clinical aspects of a multicenter clinical trial of implant-retained mandibular overdentures in patients with severely resorbed mandibles. J Prosthet Dent 1996;75: Smith DE, Zarb GA. Criteria for success of osseointegrated endosseous implants. J Prosthet Dent 1989;62: Vervoorn, JM, Duinkerke AS, Luteijn F, van de Poel AC. Assessment of denture satisfaction. Community Dent Oral Epidemiol 1988;16: Boerrigter EM, Geertman ME, Van Oort RP, Bouma J, Raghoebar GM, van Waas MA, et al. Patient satisfaction with implantretained mandibular overdentures. A comparison with new complete dentures t retained by implants--a multicentre randomized clinical trial. Br J Oral Maxillofac Surg 1995;33: Geertman ME, van Waas MA, van t Hof MA, Kalk W. Denture satisfaction in a comparative study of implant-retained mandibular overdentures: a randomized clinical trial. Int J Oral Maxillofac Implants 1996;11: Imrey PB, Chilton NW, Pihlstrom BL, Proskin HM, Kingman A, Listgarten MA, et al. Proposed guidelines for American Dental Association acceptance of products for professional, n-surgical treatment of adult periodontitis. J Periodont Res 1994;29: Hauschke D, Volker S, Pigeot I. Bioequivalence Studies in Drug Development. New York, NY: John Wiley and Sons; p Chow SC, Liu J. Design and Analysis of Bioavailability and Bioequivalence Studies. New York, NY: Marcel Dekker; p Patterson S, Jones B. Bioequivalence and Statistics in Clinical Pharmacology. Boca Raton, FL: Chapman & Hall/CRC; p Corresponding Author: Dr David R. Burns Department of Prosthodontics Virginia Commonwealth University School of Dentistry P.O. Box Richmond, VA Fax: drburns@vcu.edu Copyright 2011 by the Editorial Council for.
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
REVIEWS. 10 Stomatologija, Baltic Dental and Maxillofacial Journal, 2008, Vol. 10, No. 1 SUMMARY
 Maxillary complete denture outcome with two-implant supported mandibular overdentures. A systematic review Vygandas Rutkunas, Hiroshi Mizutani, Vytaute Peciuliene, Ruta Bendinskaite, Tomas Linkevicius
Maxillary complete denture outcome with two-implant supported mandibular overdentures. A systematic review Vygandas Rutkunas, Hiroshi Mizutani, Vytaute Peciuliene, Ruta Bendinskaite, Tomas Linkevicius
Simplified Method for fabrication of O- Ring Implant Supported Overdenture- Case Report
 CASE REPORT Simplified Method for fabrication of O- Ring Implant Supported Overdenture- Case Report Dr. Vikas Punia 1, Dr. Mohit Handa 2, Dr.Nikhil Verma 3, Dr.Virender Singh 4, Dr. Vivek Lath 5. M.D.S.,
CASE REPORT Simplified Method for fabrication of O- Ring Implant Supported Overdenture- Case Report Dr. Vikas Punia 1, Dr. Mohit Handa 2, Dr.Nikhil Verma 3, Dr.Virender Singh 4, Dr. Vivek Lath 5. M.D.S.,
The treatment of the completely edentulous mandible
 A prosthetic solution to restoring the edentulous mandible with limited interarch space using an implant-tissue-supported overdenture: A clinical report Marianna Pasciuta, DDS, MS, a Yoav Grossmann, DMD,
A prosthetic solution to restoring the edentulous mandible with limited interarch space using an implant-tissue-supported overdenture: A clinical report Marianna Pasciuta, DDS, MS, a Yoav Grossmann, DMD,
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Patient Satisfaction and Dissatisfaction with Mandibular Two-Implant Overdentures Using Different Attachment Systems: 5-Year Outcomescid_
 Patient Satisfaction and Dissatisfaction with Mandibular Two-Implant Overdentures Using Different Attachment Systems: 5-Year Outcomescid_306 696..707 Mohammed I. Al-Zubeidi, BDS, MDS;* Nabeel H.M. Alsabeeha,
Patient Satisfaction and Dissatisfaction with Mandibular Two-Implant Overdentures Using Different Attachment Systems: 5-Year Outcomescid_306 696..707 Mohammed I. Al-Zubeidi, BDS, MDS;* Nabeel H.M. Alsabeeha,
Prosthetic RehabilitationofaPatientwithAlzheimersDiseaseusingaCombinedBallBarandClipRetainedImplantSupportedOverdentureA Case Report
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers
 Original Article The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers Emre Mumcu, Hakan Bilhan and Onur Geckili Department
Original Article The effect of attachment type and implant number on satisfaction and quality of life of mandibular implant-retained overdenture wearers Emre Mumcu, Hakan Bilhan and Onur Geckili Department
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction
 Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction Corina-Marinela Cristache 1, Ionela-Ruxandra Sfeatcu 2, Mihai Burlibaºa 3, Gheorghe Cristache
Implant supported mandibular overdenture - a literature review of costs, maintenance and patient satisfaction Corina-Marinela Cristache 1, Ionela-Ruxandra Sfeatcu 2, Mihai Burlibaºa 3, Gheorghe Cristache
Radiographic Stent for Simplified Placement of Implants in the Mandible
 10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Evaluation of subjective satisfaction of dental implant patients
 ORIGINAL ARTICLE http://dx.doi.org/0.525/jkaoms.204.40.3.30 pissn 2234-7550 eissn 2234-5930 Evaluation of subjective satisfaction of dental implant patients Young-Kyun Kim, Hyun-Suk Kim, Yang-Jin Yi 2,
ORIGINAL ARTICLE http://dx.doi.org/0.525/jkaoms.204.40.3.30 pissn 2234-7550 eissn 2234-5930 Evaluation of subjective satisfaction of dental implant patients Young-Kyun Kim, Hyun-Suk Kim, Yang-Jin Yi 2,
EFFECT OF IMPLANTS ON MAXIMUM BITE FORCE
 CLINICAL EFFECT OF IMPLANTS ON MAXIMUM BITE FORCE IN EDENTULOUS PATIENTS Mansour Rismanchian, DMD, MS; Farshad Bajoghli, DMD, MS; Zahra Mostajeran, DDS; Akbar Fazel, DMD, MS; P. sadr Eshkevari, DDS One
CLINICAL EFFECT OF IMPLANTS ON MAXIMUM BITE FORCE IN EDENTULOUS PATIENTS Mansour Rismanchian, DMD, MS; Farshad Bajoghli, DMD, MS; Zahra Mostajeran, DDS; Akbar Fazel, DMD, MS; P. sadr Eshkevari, DDS One
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Number of implants for mandibular implant overdentures: a systematic review
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.204 Number of implants for mandibular implant overdentures: a systematic review Jeong-Yol Lee 1, DDS, MSc, PhD, Ha-Young Kim 1, DDS, Sang-Wan Shin
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.204 Number of implants for mandibular implant overdentures: a systematic review Jeong-Yol Lee 1, DDS, MSc, PhD, Ha-Young Kim 1, DDS, Sang-Wan Shin
Evaluation of supported overdenture by implant and magnet
 * * 26 Evaluation of supported overdenture by implant and magnet Arab H.R * Assistant Professor, Dep. Of Periodontics, School of Dentistry, Mashhad University of Medical Sciences, Mashhad, Iran. Tamizi
* * 26 Evaluation of supported overdenture by implant and magnet Arab H.R * Assistant Professor, Dep. Of Periodontics, School of Dentistry, Mashhad University of Medical Sciences, Mashhad, Iran. Tamizi
Rehabilitation of an Edentulous Patient with Implant Supported Overdenture
 10.5005/jp-journals-10031-1036 CASE REPORT Rehabilitation of an Edentulous Patient with Implant Supported Overdenture Swapnali Mhatre, Sabita M Ram, Janani Mahadevan, Malika Karthik ABSTRACT The conventional
10.5005/jp-journals-10031-1036 CASE REPORT Rehabilitation of an Edentulous Patient with Implant Supported Overdenture Swapnali Mhatre, Sabita M Ram, Janani Mahadevan, Malika Karthik ABSTRACT The conventional
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Comparison of Patient s Satisfaction with Implant supported Mandibular Overdentures and Complete Dentures
 Original Article 156 Comparison of Patient s Satisfaction with Implant supported Mandibular Overdentures and Complete Dentures Yu Hwa Pan 1, Tai Min Lin 1, Chao Hua Liang 2 Background: The purpose of this
Original Article 156 Comparison of Patient s Satisfaction with Implant supported Mandibular Overdentures and Complete Dentures Yu Hwa Pan 1, Tai Min Lin 1, Chao Hua Liang 2 Background: The purpose of this
At present, there are several
 CLINICAL USE OF NEW MAGNETIC ATTACHMENTS FOR IMPLANT-SUPPORTED OVERDENTURES Takehiro Fujimoto, DDS, PhD Atsushi Niimi, DDS, DMSc Itsuki Murakami, DDS, MS, PhD Minoru Ueda, DDS, PhD KEY WORDS Brånemark
CLINICAL USE OF NEW MAGNETIC ATTACHMENTS FOR IMPLANT-SUPPORTED OVERDENTURES Takehiro Fujimoto, DDS, PhD Atsushi Niimi, DDS, DMSc Itsuki Murakami, DDS, MS, PhD Minoru Ueda, DDS, PhD KEY WORDS Brånemark
A SURVEY TO ASSESS PATIENT SATISFACTION AFTER RECEIVING COMPLETE DENTURE PROSTHESES IN A.B. SHETTY MEMORIAL INSTITUTE OF DENTAL SCIENCES
 Short Communication A SURVEY TO ASSESS PATIENT SATISFACTION AFTER RECEIVING COMPLETE DENTURE PROSTHESES IN A.B. SHETTY MEMORIAL INSTITUTE OF DENTAL SCIENCES 2 Vinaya S. Bhat, Krishna Prasad D. & Prakyath
Short Communication A SURVEY TO ASSESS PATIENT SATISFACTION AFTER RECEIVING COMPLETE DENTURE PROSTHESES IN A.B. SHETTY MEMORIAL INSTITUTE OF DENTAL SCIENCES 2 Vinaya S. Bhat, Krishna Prasad D. & Prakyath
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
J. Mark Thomason Guido Heydecke Jocelyne S. Feine Janice S. Ellis. 168 c 2007 The Authors. Journal compilation c 2007 Blackwell Munksgaard
 J. Mark Thomason Guido Heydecke Jocelyne S. Feine Janice S. Ellis How do patients perceive the benefit of reconstructive dentistry with regard to oral health-related quality of life and patient satisfaction?
J. Mark Thomason Guido Heydecke Jocelyne S. Feine Janice S. Ellis How do patients perceive the benefit of reconstructive dentistry with regard to oral health-related quality of life and patient satisfaction?
Implants are a part of IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY CLINICAL
 CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Oral health impact profile and prosthetic condition in edentulous patients rehabilitated with implant-supported overdentures and fixed prostheses
 535 Journal of Oral Science, Vol. 51, No. 4, 535-543, 2009 Original Oral health impact profile and prosthetic condition in edentulous patients rehabilitated with implant-supported overdentures and fixed
535 Journal of Oral Science, Vol. 51, No. 4, 535-543, 2009 Original Oral health impact profile and prosthetic condition in edentulous patients rehabilitated with implant-supported overdentures and fixed
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Mandibular implant-supported hybrid prostheses
 Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
CASE REPORT. Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report.
 1828 CASE REPORT Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report Meisha Gul, Muhammad Rizwan Nazeer, Robia Ghafoor Abstract Removable complete
1828 CASE REPORT Prosthetic rehabilitation of edentulous mandible with two-implant retained fixed hybrid prosthesis: A case report Meisha Gul, Muhammad Rizwan Nazeer, Robia Ghafoor Abstract Removable complete
Clinical evaluation of mandibular implant overdentures via Locator implant attachment and Locator bar attachment
 http://jap.or.kr J Adv Prosthodont 2016;8:313-20 http://dx.doi.org/10.4047/jap.2016.8.4.313 Clinical evaluation of mandibular implant overdentures via Locator implant attachment and Locator bar attachment
http://jap.or.kr J Adv Prosthodont 2016;8:313-20 http://dx.doi.org/10.4047/jap.2016.8.4.313 Clinical evaluation of mandibular implant overdentures via Locator implant attachment and Locator bar attachment
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Figure 5: Facebow transfer Figure 6: Surgical guide
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. IX (May. 2016), PP 86-90 www.iosrjournals.org A Novel Technique to Restore An Edentulous
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. IX (May. 2016), PP 86-90 www.iosrjournals.org A Novel Technique to Restore An Edentulous
Attachment systems for mandibular implant overdentures: a systematic review
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.197 Attachment systems for mandibular implant overdentures: a systematic review Ha-Young Kim 1, DDS, Jeong-Yol Lee 1, DDS, MSc, PhD, Sang-Wan Shin
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.197 Attachment systems for mandibular implant overdentures: a systematic review Ha-Young Kim 1, DDS, Jeong-Yol Lee 1, DDS, MSc, PhD, Sang-Wan Shin
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Saudi Journal of Oral and Dental Research. DOI: /sjodr. ISSN (Print) Dubai, United Arab Emirates Website:
 DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24625
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24625
Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: A clinical report
 Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: A clinical report Avinash S., BDS, MS a University of Connecticut Health Center, Farmington, Conn.
Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: A clinical report Avinash S., BDS, MS a University of Connecticut Health Center, Farmington, Conn.
Design and Manufacturing of Titanium Attachment for Single Implant Retained Mandibular Overdenture: A Review
 Original article: Design and Manufacturing of Titanium Attachment for Single Implant Retained Mandibular Overdenture: A Review *RupaliRaut 1, Dr. S. B. Jaju 2, Dr. N. H. Rathi 3 1Student, M. Tech CAD/CAM,
Original article: Design and Manufacturing of Titanium Attachment for Single Implant Retained Mandibular Overdenture: A Review *RupaliRaut 1, Dr. S. B. Jaju 2, Dr. N. H. Rathi 3 1Student, M. Tech CAD/CAM,
University of Groningen
 University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
University of Groningen Mandibular Overdentures Supported by 6-mm Dental Implants Gulje, Felix; Raghoebar, Gerry; Ter Meulen, Jan-Willem P.; Vissink, Arjan; Meijer, Hendrikus; GuljÃ, Felix Published in:
Does mandibular edentulous bone height affect prosthetic treatment success?
 journal of dentistry 38 (2010) 899 907 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Does mandibular edentulous bone height affect prosthetic treatment
journal of dentistry 38 (2010) 899 907 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Does mandibular edentulous bone height affect prosthetic treatment
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
Mandibular Implant-Retained Overdentures with two Different Implant Designs. Ibrahim R. Eltorky
 Mandibular Implant-Retained Overdentures with two Different Implant Designs Ibrahim R. Eltorky Associate professor of Prosthodontics, Faculty of Dentistry, Tanta University, Egypt. ibrahim_eltorky@yahoo.com
Mandibular Implant-Retained Overdentures with two Different Implant Designs Ibrahim R. Eltorky Associate professor of Prosthodontics, Faculty of Dentistry, Tanta University, Egypt. ibrahim_eltorky@yahoo.com
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
The Immediately Loaded Single Implant Retained Mandibular Overdenture: A 36-Month Prospective Study
 The Immediately Loaded Single Implant Retained Mandibular Overdenture: A 36-Month Prospective Study Glen Liddelow, BDSc, MScD, DClinDent, FRACDS a /Patrick Henry, BDSc, MSD, DDSchc, FRACDS b Purpose: The
The Immediately Loaded Single Implant Retained Mandibular Overdenture: A 36-Month Prospective Study Glen Liddelow, BDSc, MScD, DClinDent, FRACDS a /Patrick Henry, BDSc, MSD, DDSchc, FRACDS b Purpose: The
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function
 Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
 C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
Cost-effectiveness of Mandibular Two-implant Overdentures and Conventional Dentures in the Edentulous Elderly
 RESEARCH REPORTS Clinical G. Heydecke 1, J.R. Penrod 1,2, Y. Takanashi 1, J.P. Lund 1,4, J.S. Feine 1,5 *, and J.M. Thomason 1,3 1 Faculty of Dentistry, McGill University, 3640 University Street, M73,
RESEARCH REPORTS Clinical G. Heydecke 1, J.R. Penrod 1,2, Y. Takanashi 1, J.P. Lund 1,4, J.S. Feine 1,5 *, and J.M. Thomason 1,3 1 Faculty of Dentistry, McGill University, 3640 University Street, M73,
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
There is overwhelming evidence that implant-retained
 CLINICAL Two-Year Success Rate of Implant-Retained Mandibular Overdentures by Novice General Dentistry Residents Hans Malmstrom, DDS 1 * Jin Xiao, DDS, MS, PhD 1 Georgios Romanos, DDS, PhD 1,2 Yan-Fang
CLINICAL Two-Year Success Rate of Implant-Retained Mandibular Overdentures by Novice General Dentistry Residents Hans Malmstrom, DDS 1 * Jin Xiao, DDS, MS, PhD 1 Georgios Romanos, DDS, PhD 1,2 Yan-Fang
Prosthodontic Rehabilitation with Overdenture Using Modified Impression Technique: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate Loading Protocol: An In-Vivo Study
 J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized Balanced Occlusion
 Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Med. J. Cairo Univ., Vol. 83, No. 2, June: 93-97, 2015 www.medicaljournalofcairouniversity.net Clinical and Radiographic Evaluation of Implant Ball Retained Mandibular Complete Overdentures with Lingualized
Clinical Efficacy of Single One Piece Implant Retained Mandibular Overdentures Kyaw Naing 1, Myat Nyan 2, Ko Ko 2, Than Swe 1
 Original Article Clinical Efficacy of Single One Piece Implant Retained Mandibular Overdentures Kyaw Naing 1, Myat Nyan 2, Ko Ko 2, Than Swe 1 1 Department of Prosthodontics, University of Dental Medicine,
Original Article Clinical Efficacy of Single One Piece Implant Retained Mandibular Overdentures Kyaw Naing 1, Myat Nyan 2, Ko Ko 2, Than Swe 1 1 Department of Prosthodontics, University of Dental Medicine,
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
The use of two interforaminal implants to retain/
 Immediate Loading of Unsplinted Implants in the Anterior Mandible for Overdentures: 3-Year Results Phillip Roe, DDS, MS 1 /Joseph Y. K. Kan, DDS, MS 2 / Kitichai Rungcharassaeng, DDS, MS 3 /Jaime L. Lozada,
Immediate Loading of Unsplinted Implants in the Anterior Mandible for Overdentures: 3-Year Results Phillip Roe, DDS, MS 1 /Joseph Y. K. Kan, DDS, MS 2 / Kitichai Rungcharassaeng, DDS, MS 3 /Jaime L. Lozada,
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Evaluation of Gradual Trend of Patients Satisfaction with Complete Dentures in the Department of Prosthodontics: A Cross-sectional Study
 ISSN: 2203-1413 Vol.04 No.02 Evaluation of Gradual Trend of Patients Satisfaction with Complete Dentures in the Department of Prosthodontics: A Cross-sectional Study Ramin Negahdari 1, Seyyed Mahdi Vahid
ISSN: 2203-1413 Vol.04 No.02 Evaluation of Gradual Trend of Patients Satisfaction with Complete Dentures in the Department of Prosthodontics: A Cross-sectional Study Ramin Negahdari 1, Seyyed Mahdi Vahid
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
ACRYLIC REMOVABLE PARTIAL DENTURE(RPD)
 ACRYLIC REMOVABLE PARTIAL DENTURE(RPD) is a dental prosthesis which artificially supplies teeth and associated structure in a partially edentulous arch, made from acrylic resin and can be inserted and
ACRYLIC REMOVABLE PARTIAL DENTURE(RPD) is a dental prosthesis which artificially supplies teeth and associated structure in a partially edentulous arch, made from acrylic resin and can be inserted and
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Preserving the Integrity of Facial Structures with Implant-Retained Overdentures
 Preserving the Integrity of Facial Structures with Implant-Retained Overdentures Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD The Centers for Disease Control and Prevention (CDC) has
Preserving the Integrity of Facial Structures with Implant-Retained Overdentures Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD The Centers for Disease Control and Prevention (CDC) has
OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES
 GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES Since the McGill Consensus in 2002, the dental industry has recognized that implant-supported
GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES Since the McGill Consensus in 2002, the dental industry has recognized that implant-supported
OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES
 GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES Since the McGill Consensus in 2002, the dental industry has recognized that implant-supported
GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. OPENING MINDS AND EXPANDING PRACTICE REVENUE OPPORTUNITIES Since the McGill Consensus in 2002, the dental industry has recognized that implant-supported
Opening minds and expanding practice revenue opportunities
 GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. Opening minds and expanding practice revenue opportunities Since the McGill Consensus in 2002, the dental industry has recognized that implant-supported
GIVE YOUR PATIENTS THE FREEDOM TO EAT, SPEAK AND LAUGH AGAIN. Opening minds and expanding practice revenue opportunities Since the McGill Consensus in 2002, the dental industry has recognized that implant-supported
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Social changes, evolution in dentistry, and changes
 695-702 Naert 9/21/04 2:37 PM Page 695 A 10-year Randomized Clinical Trial on the Influence of Splinted and Unsplinted Oral Implants Retaining Mandibular Overdentures: Peri-implant Outcome Ignace Naert,
695-702 Naert 9/21/04 2:37 PM Page 695 A 10-year Randomized Clinical Trial on the Influence of Splinted and Unsplinted Oral Implants Retaining Mandibular Overdentures: Peri-implant Outcome Ignace Naert,
The indication for implant treatment as the first
 RESEARCH Patients Expectation Before and Satisfaction After Full- Arch Fixed Implant-Prosthesis Rehabilitation Miriã Corália da Cunha, DDS 1 Jarbas Francisco Fernandes dos Santos, DDS, MSD, PhD 1,2 Mateus
RESEARCH Patients Expectation Before and Satisfaction After Full- Arch Fixed Implant-Prosthesis Rehabilitation Miriã Corália da Cunha, DDS 1 Jarbas Francisco Fernandes dos Santos, DDS, MSD, PhD 1,2 Mateus
TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT
 TJPRC: International Journal of Prosthetic Dentistry & Research (TJPRC:IJPDR) Vol. 1, Issue 1, Jun 2017, 5-10 TJPRC Pvt. Ltd. TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT ANSUIA GUPTA 1,
TJPRC: International Journal of Prosthetic Dentistry & Research (TJPRC:IJPDR) Vol. 1, Issue 1, Jun 2017, 5-10 TJPRC Pvt. Ltd. TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT ANSUIA GUPTA 1,
Orthodontic-prosthetic implant anchorage in a partially edentulous patient
 Journal of Dental Sciences (2011) 6, 176e180 available at www.sciencedirect.com journal homepage: www.e-jds.com Clinical Report Orthodontic-prosthetic implant anchorage in a partially edentulous patient
Journal of Dental Sciences (2011) 6, 176e180 available at www.sciencedirect.com journal homepage: www.e-jds.com Clinical Report Orthodontic-prosthetic implant anchorage in a partially edentulous patient
Department of Prosthodontics, Faculty of Oral and Dental Medicine, Cairo University, Cairo, Egypt 2
 Impact of single implant versus two-implant mandibular retained overdentures on retention and success rate in totally edentulous patients. A Randomized Controlled Clinical Trial A. A. AlSourori 1, 2, M.
Impact of single implant versus two-implant mandibular retained overdentures on retention and success rate in totally edentulous patients. A Randomized Controlled Clinical Trial A. A. AlSourori 1, 2, M.
Low-Cost Implant Overdenture Option for Patients Treated in a Predoctoral Dental School Curriculum
 Milieu in Dental School and Practice Low-Cost Implant Overdenture Option for Patients Treated in a Predoctoral Dental School Curriculum Michael S. McCracken, D.D.S., Ph.D.; Ruth Aponte-Wesson, D.D.S.,
Milieu in Dental School and Practice Low-Cost Implant Overdenture Option for Patients Treated in a Predoctoral Dental School Curriculum Michael S. McCracken, D.D.S., Ph.D.; Ruth Aponte-Wesson, D.D.S.,
Uppers are from Mars, Lowers from Venus Clarifying Overdentures
 Uppers are from Mars, Lowers from Venus Clarifying Overdentures M. Nader Sharifi, D.D.S., M.S. Thomas P. Hinman Dental Meeting Atlanta, GA March 23, 2017 About Your Speaker: M. Nader Sharifi, D.D.S., M.S.
Uppers are from Mars, Lowers from Venus Clarifying Overdentures M. Nader Sharifi, D.D.S., M.S. Thomas P. Hinman Dental Meeting Atlanta, GA March 23, 2017 About Your Speaker: M. Nader Sharifi, D.D.S., M.S.
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Immediate Complete Denture: A Case Report
 Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Fixed full-arch implant-supported acrylic resin prostheses
 Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Evaluation of Patient Satisfaction in Implant-supported Dentures retained with Ball and Bar Attachment /jp-journals
 Evaluation of Patient Satisfaction in Implant-supported Dentures retained with Ball and Bar Attachment 10.5005/jp-journals-10029-1144 through Verbal Rating System ORIGINAL ARTICLE Evaluation of Patient
Evaluation of Patient Satisfaction in Implant-supported Dentures retained with Ball and Bar Attachment 10.5005/jp-journals-10029-1144 through Verbal Rating System ORIGINAL ARTICLE Evaluation of Patient
Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete Denture and Mandibular Teeth supported Overdenture
 Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Determination of the Rate of Need for Relining Complete Dentures in Patients Referring to a Department of Prosthodontics
 ISS: 2203-1413 Vol.04 o.02 Determination of the Rate of eed for Relining Complete Dentures in Patients Referring to a Department of Prosthodontics Ramin egahdari 1, Seyyed Mahdi Vahid Pakdel 2, Sepideh
ISS: 2203-1413 Vol.04 o.02 Determination of the Rate of eed for Relining Complete Dentures in Patients Referring to a Department of Prosthodontics Ramin egahdari 1, Seyyed Mahdi Vahid Pakdel 2, Sepideh
RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
 Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
ISPUB.COM. Habitual Centric: A Case Report. Manisha, N Kathuria, A Gupta, N Gupta INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
