The International Journal of Periodontics & Restorative Dentistry
|
|
|
- Myra Stevenson
- 6 years ago
- Views:
Transcription
1 The International Journal of Periodontics & Restorative Dentistry
2 313 Timing, Positioning, and Sequential Staging in Esthetic Implant Therapy: A Four-Dimensional Perspective Akiyoshi Funato, DDS* Maurice A. Salama, DMD** Tomohiro Ishikawa, DDS*** David A. Garber, DMD** Henry Salama, DMD**** Many articles address the predictability of immediate implant placement into extraction sockets; however, there are only a few reports that mention the indications and limitations of this technique. The aim of this article is to re-examine specific indications for immediate implant placement and to clarify the timing or fourth dimension relative to extraction and implant placement. The expanded concept of four-dimensional implant treatment planning involves the new axis of time, which must be considered along with the traditional spatial or threedimensional management of implant positioning. (Int J Periodontics Restorative Dent 2007;27: ) *Private Practice, Kanazawa, Ishikawa, Japan. **Clinical Assistant Professor, Department of Periodontics, University of Pennsylvania, Philadelphia, Pennsylvania; Medical College of Georgia; Private Practice, Atlanta, Georgia. ***Private Practice, Hamamatsu, Shizuoka, Japan. ****Clinical Assistant Professor, Department of Periodontics, University of Pennsylvania, Pennsylvania; Private Practice, Atlanta, Georgia. Correspondence to: Dr Maurice Salama, 600 Galleria Parkway, Suite 800, Atlanta, GA, 30339; fax: The key to successful implant therapy in the anterior esthetic region is a harmonious relationship between the implant-supported restoration and the remaining natural teeth. The creation of a natural-looking implant restoration depends not only on the appropriate placement of an osseointegrated implant and restoration, but also on the reconstruction of a natural gingival architecture around the implant that is in harmony with the lip line and face. To achieve this goal, an implant must be conceptually planned and placed as a vertical extension of an optimally visualized restoration, as described by Garber and Belser in their concept of restoration-driven implant treatment planning. 1,2 This approach involves three-dimensional (3D) treatment planning, followed by placement of the implant in a position that is optimal for both function and esthetics. The initial 3D evaluation of the potential site must include planning for augmentation or preservation of the existing osseous and gingival tissues around the compromised tooth. This should be an integral part of the process, because it is known that extraction is always followed by some bone resorption, with Volume 27, Number 4, 2007
3 314 concomitant soft tissue recession. 3 5 To achieve the optimal esthetic result, clinicians must go beyond using the most appropriate clinical techniques and armamentarium and must consider a fourth dimension: timing of the treatment sequence. This additional component in treatment planning incorporates the optimal sequential staging or timing of (1) tooth extraction, (2) preservation or enhancement of hard and soft tissue, (3) implant placement, (4) abutment connection, (5) tissue modeling with a provisional and/or a modified abutment, and (6) definitive restoration. This additional axis of time is added to the traditional 3D axes and described herein as the four-dimensional (4D) concept in implant therapy. Successful esthetic implant therapy, then, has several sequential objectives: 1. Restoration-driven 3D implant replacement, ie, placement of the implant in the optimal position to effectively support the restoration and surrounding soft and hard tissue 2. Any necessary reconstruction of an esthetic gingival soft tissue frame incorporating the harmony or curvature to the labial free gingival margin aspect of the restoration with the definitive vertical and buccolingual presence of adjacent interdental papillae 3. A provisional restoration to maintain or modify the degree of curvature of the labial free gingival margin and provide the necessary lateral support for the interproximal papillae 4. Placement of a definitive restoration that is in harmony with the adjacent natural teeth and surrounding soft tissue, with identical gingival color The actual timing of tooth extraction, implant placement, and abutment connection will ultimately influence the specific outcome by limiting the number of individual auxiliary procedures while enhancing predictability. Conceptually, then, it reduces the potential number of surgical/restorative interventions, shortening the treatment span and thereby enhancing esthetic predictability. Immediate implant placement has been well documented in the literature, and the data indicate similar predictability versus the staged approach Ongoing improvements in resorbable membranes have helped expand the potential indications for immediate implant placement with decreased complications during guided bone regeneration (GBR). Today, there is still a dichotomy of thought regarding the timing of extraction and implant placement, and it is the authors contention that no single method is a panacea; rather, there are specific clinical indications for each. The aim of this article is to re-examine specific indications for immediate implant placement and to clarify the timing or fourth dimension relative to extraction and implant placement. The expanded new concept of 4D implant treatment planning involves time, which must be included with the traditional spatial or 3D management of implant positioning. The timing of tooth extraction and implant placement is classified as follows: Class 1: Extraction, with immediate implant placement directly into the alveolar socket via (a) incisonless implant placement or (b) the raising of a mucoperiosteal flap and placement of the implant into the extraction socket concomitant with either (i) osseous augmentation or GBR or (ii) a connective tissue or allograft. Class 2: Early implant placement. The implant is placed after extraction, and soft tissues are allowed to heal for 6 to 8 weeks. GBR can be performed at the time of extraction and/or at the time of implant placement. Class 3: Delayed implant placement. The implant is placed a minimum of 4 to 6 months after extraction, with preservation of the alveolar ridge using grafting techniques and/or GBR, either at the time of extraction or concomitant with implant placement. Soft tissue reconstruction in these cases will invariably be required. Based on this classification, a tooth targeted for immediate implant placement should be diagnosed as nonsalvageable for the following reasons: (1) endodontic failure, (2) internal and/or root resorption, (3) subcrestal extensive caries, or (4) root fracture. Conceptually, the targeted tooth demonstrates no osseous compromise; clinically, the bone on the immediately adjacent teeth should be evaluated as to the relative height of the interproximal height of bone (IHB), 12,13 since it is this IHB on the adjacent tooth that effectively determines the absence or presence of a natural papilla. The International Journal of Periodontics & Restorative Dentistry
4 315 It has been determined that a distance of 4.5 mm from the desired contact point, or from the tip of a papilla to the peak of the interproximal height of bone on the teeth adjacent to the implant site, is the mean dimension for the predictable presence of a full papilla. 12 Immediate implant placement into these types of extraction sockets with four walls shows better esthetic predictability than the replacement of teeth with periodontal compromise. If the targeted tooth or any adjacent tooth shows an IHB with a distance in excess of 4.5 mm, then delayed placement is preferable, with preemptive orthodontic treatment of the tooth to be extracted or subsequent orthodontic treatment of the adjacent teeth to ensure esthetic predictability. In many cases, orthodontic eruption, as a preliminary step to extraction with immediate implant placement, even in a type 1 site, provides the clinician the esthetic and mechanical advantages of added osseous support to compensate for the bone loss inevitable with extraction. This is particularly necessary in Asian patients, who often have extremely thin labial plates of bone in the maxillary anterior region. In these thin scalloped biotypes, even though a thin labial alveolar bone is present following implant placement, 1 to 3 mm of gingival recession invariably occurs over time following the connection of the abutment because of remodeling of the hard and soft tissues around implants Orthodontic extrusion Salama and Salama 17 reported on the advantages of orthodontic eruption as a preliminary step to implant placement. These include the following: 1. It decreases or minimizes the gap between the implant body and the extraction socket by coronally relocating a narrower portion of the root for extraction and therefore resulting in a smallerdiameter socket. 2. It helps enhance primary stability in the alveolus by developing the alveolar bone beyond the root apex. 3. It augments the crestal alveolar bone and overlying gingival tissues, decreasing the negative impact of postoperative alveolar resorption and gingival recession. 4. By loosening the tooth, it helps facilitate extraction. 5. It increases the mitotic turnover of the cells in the region, enhancing the potential for more rapid healing. Orthodontic eruption should be used to generate at least 2 mm of additional vertical gingival tissue as compared to the adjacent teeth to provide for a harmonious gingival arrangement. After a 12-week period of retention, the alveolar osseous crest on the facial and interproximal aspects is confirmed by bone sounding. In addition, a computerized tomographic scan can be performed to evaluate whether there is sufficient bone available to facilitate extraction with immediate implant placement without resultant esthetic compromise. Potential or future extraction sites are now routinely augmented vertically by orthodontics from a class 2 to a class 1 site (based on the classification system described in next section) when needed. Classification of immediate implant placement sites The classification detailed below and in Table 1 is based on both the osseous and soft tissue levels of the potential site at the time of extraction. Class 1: The buccal bone is intact, with a thick gingival biotype. Incisionless implant placement without flap reflection is viable (Fig 1). Class 2: The buccal bone is intact with a thin, more scalloped gingival biotype. Incisionless implant placement is viable, but in combination with a connective tissue graft or a subsequent secondary connective tissue graft (staged) (Fig 2). Class 3: The buccal bone is lost, but the implant can still be placed immediately within the remaining alveolar housing of the extraction socket, with the necessary osseous support provided through regeneration using a membrane with GBR and incorporating a simultaneous connective tissue graft. Depending on the degree of compromise to the buccal plate, the case may alternatively be handled in a staged approach using a socket augmentation procedure and subsequent implant placement. In many instances, especially Volume 27, Number 4, 2007
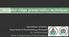
5 316 Table 1 Classification of immediate implant placement Viable Expected results Indication for implant placement of immediate immediate Class Buccal bone technique implant placement implant placement Class 1 Intact with thick Immediate without Optimal Yes gingival biotype flap reflection Class 2 Intact with thin Immediate with Good Yes gingival biotype CTG or staged CTG Class 3 Deficient but implant Simultaneous Acceptable Limited placement possible in immediate with GBR remaining alveolar housing and CTG or followed of extraction socket by staged CTG Class 4 Deficient and Delayed Unacceptable No implant may deviate from alveolar housing CTG = connective tissue graft. Fig 1a (left) This case is categorized as class 1. Following orthodontic extrusion, the maxillary left central incisor was extracted. The existing buccal bone was confirmed by bone sounding with a periodontal probe. A thick biotype was diagnosed. Fig 1b (right) An implant was placed incisionless without flap reflection, and a provisional restoration was placed immediately. Fig 1c (left) Facial view of the definitive implant analog and definitive abutment. An abutment access hole cannot be seen, confirming that the extended long axis of the implant would not be labial to the incisal edge of the restoration. Fig 1d (right) restoration. Facial view of the definitive The International Journal of Periodontics & Restorative Dentistry
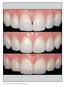
6 317 Fig 2a (left) This case is categorized as class 2. At the initial examination, an amalgam tattoo and root fracture were evident at the maxillary left central incisor. Fig 2b (right) The amalgam tattoo tissue was surgically excised, and a subepithelial connective tissue graft was placed. Fig 2c (left) Orthodontic eruption of the tooth intended for extraction was performed; following confirmation of the resulting bone level, both interproximally and labially, the tooth was extracted with the aid of a periotome. Fig 2d (right) Surgical guide in position prior to implant placement. The implant was placed, and an immediate provisional restoration, employed for both immediate esthetics and to provide optimal support for the soft tissues, was placed. Fig 2e (left) Facial view of the definitive restoration on the maxillary left central incisor. A diminished or concave labial contour and positive interproximal support maintain the form of the free gingival margin and the height of the papillae. Fig 2f (right) 1 year. Postoperative radiograph at Volume 27, Number 4, 2007
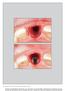
7 318 Fig 3a This case is categorized as class 3. Extraction with immediate implant placement was performed despite compromise to the buccal bone, but the implant was retained within the confines of the alveolar housing. Fig 3b Connective tissue grafting in combination with GBR was used, incorporating a resorbable membrane. The connective tissue graft was used to optimize the esthetic soft tissue profile. Fig 3c Facial view of the definitive restoration. While an adequate esthetic outcome was achieved, a small depression is evident in the buccal cervical region. in thin biotypes, this method provides a more predictable and safer outcome (Fig 3). Class 4: The buccal bone is severely compromised, and implant placement within the remaining palatal bone results in a significantly offaxis implant position. In these cases, following extraction, implant placement should be delayed. If performed immediately, the long axis of the implant inclines toward the buccal and will result in a significant esthetic compromise of the definitive restoration. In these situations, the delayed approach should be used with subsequent 3D bone and soft tissue augmentation of the deficient ridge followed by optimal implant positioning. In evaluating a potential site, care must be taken to ensure that the clinician s attempts to expedite implant placement within the available bone do not result in an implant that tends to extrude labially, thereby compromising the restorative esthetics. The long axis of the implant should be placed lingual to the incisor edge whenever possible to allow for both mechanical and surgical advantages in the definitive outcome. The lab will have more space to work with porcelain and to hide the prosthetic components, the restorative clinician will have more room to establish a proper emergence profile, and the surgeon will have less pressure placed onto the labial tissues. Implant positioning, the resulting long axis, and soft tissue considerations Vertical depth of implant head and direction of long axis The platform of the implant should be located 2 to 4 mm below the midfacial aspect of the free gingival margin, with the extended long axis directed slightly lingual to the incisal edge of the definitive restoration (Fig 4). When the long axis of the implant is inclined labially and projects beyond the incisal edge of the definitive restoration, the result is that the subgingival contours of the abutment or restoration will tend to deflect the gingival margin apically, resulting in an unharmonious esthetic profile. 18 To correct this problem, the profile extending from the implant head to the free gingival margin requires a straight or negative angulation. Immediate placement generally cannot be performd in the wrong position without esthetic compromise. Buccolingual position and labial region Tarnow et al 19 stated that a submerged implant, following abutment connection, will develop a vertical change in the osseous topography of 1.5 to 2 mm below the implant shoulder. In addition, circumferentially, or horizontally, this will create crater-shaped or horizontal/lateral bone resorption of 1.3 to 1.4 mm. 16 The International Journal of Periodontics & Restorative Dentistry
8 319 Fig 4 Examples of the positions of immediately placed implants following orthodontic extrusion. These positions are classified based on both the osseous and soft tissue levels at the potential site at the time of extraction. Ideally, the implant engages the palatal wall of the extraction socket, and the extended long axis is directed slightly lingual to the incisal edge of the definitive restoration. Immediate placement generally cannot be performed in the wrong position without esthetic compromise. Ideal position Acceptable positions Wrong position Grunder et al 20 stated that at least 2 mm of lateral alveolar bone must be present beyond the body of the implant to compensate for the effects of bone remodeling. In the case of extraction with immediate implant placement, an implant should be placed lingually, avoiding the coronal 5 mm of labial bone and allowing for a gap of less than 2 mm, measured laterally from the periphery of the implant to the labial aspect of the socket. Grunder et al indicated that to support the gingival profiles, at least 2 mm of bone are necessary at the head of the implant measured laterally to allow for sufficient bone to remain in the esthetic position despite the naturally occurring horizontal cratering. Therefore, in any extraction with immediate implant placement, despite the necessity of maximizing the gap at 2.2 mm, 21 it may be necessary to increase the size of this gap and actually refill it with a grafting material. 7,22 This will ensure that, following horizontal bone remodeling, 1.5 mm of bone will still remain lateral to the buccal aspect of the extraction socket following resorption to support the vertical height of the soft tissue. Implant designs that reportedly minimize crestal bone loss as a result of the abutment connection have recently been suggested Elimination of abutment-to-implant micromovement, development of a hermetic bacterial seal, or the use of platform switching (smaller abutment with wider implant platform) could make esthetic implant treatment particularly with adjacent implants more esthetically predictable. 24,25 However, the data on these potential solutions are still being evaluated. Maynard and Wilson 26 related the risk of potential gingival recession to the gingival biotype and underlying alveolar bone. They indicated that a biotype with thin gingival tissue and thin alveolar bone has the highest risk of gingival recession. 26 Kan et al 27 reported that the thick gingival biotype has a more coronal level of gingival margin, with greater predictability than thin gingival biotype. It is evident, then, that prior to implant placement, a thorough evaluation of the periodontal biotype is necessary; with the thin biotype, connective tissue grafting may be necessary to reduce soft and hard tissue compromise. Mesiodistal position relative to the interdental zone The head of an implant is positioned relative to the osseous on the direct labial; depending on the implant system used and particular philosophy, it is placed level or just coronal to it, or even slightly below the midcrestal bone. Of necessity and because of the flat head design of most implant systems, the interproximal aspect will extend well below the interproximal height of bone. This distance will vary with the periodontal biotype, ending up considerably deeper in the scalloped as opposed to the flat biotype. Salama et al 12 have developed a classification system for the predictable Volume 27, Number 4, 2007
9 Fig 5a (left) Classification of interproximal bone height (IHB). 1 = Optimal result; IHB 2 mm from the cementoenamel junction (CEJ) and 4 to 5 mm from contact point. 2 = Unfavorable result; IHB 4 mm from CEJ and 5 to 7 mm from contact point. 3 = Severe result; IHB > 5 mm from CEJ and > 7 mm from contact point. Fig 5b (right) Apical extent of the contact point (A), IHB on the natural tooth (B), and IHB on the implant (C). 4.5 mm B A C C C A 3.5 mm Table 2 Salama et al 12 classification of predicted height of interdental papillae Restorative Proximity Vertical soft tissue Class environment limitations limitations 1 Tooth-tooth 1.0 mm 5.0 mm 2 Tooth-pontic N/A 6.5 mm 3 Pontic-pontic N/A 6.0 mm 4 Tooth-implant 1.5 mm 4.5 mm 5 Implant-pontic N/A 5.5 mm 6 Implant-implant 3.0 mm 3.5 mm height of the interdental papillae, as determined by the restorative elements on either side of the implant site (Table 2, Fig 5). The six classifications are differentiated by whether a papilla has a tooth, a pontic, or an implant on either side of it. Their data indicated that the vertical height from the tip of the interdental papilla between two implants was in excess of 2 mm less than that between an implant and a pontic; this resulted in a much shorter papilla and a longer restorative contact point. 12 This classification system and its associated treatment planning algorithm allow the clinician to prognostically plan for esthetic soft tissue contours by selecting the most appropriate fixed restorative option based upon the available vertical bone support. The numeric values just described may well be a result of the difference in the attachment modality of soft tissue in the natural tooth or pontic as opposed to the implant, in combination with the result of the remodeling of the peri-implant bone following abutment connection. The Salama et al 12 classification also described the horizontal dimension necessary between the restorative elements to facilitate the predictable presence of a papilla for instance, the implant-to-implant dimension should, at a minimum, be 3 mm, whereas the necessary dimension between an implant and a tooth can be considerably less, at only 1.5 mm. 20,28 It is their contention that, with the present design of implants, the use of a pontic between implants improves the relative height of the papillae and the overall esthetic gingival outcome Evolving changes in implant design, such as the single-body design or a two-piece implant system with a biologically invisible connection, may decrease the potential for crestal bone remodeling and resultant soft tissue changes. In addition, it appears from the work of Abrahamson et al 29 that every incident of abutment connection and disconnection enhances the process of bone remodeling. The 4D concept in complex cases In multiple-implant cases associated with bone defects (Fig 6), the use of strategically timed serial extractions is exceedingly important to support a fixed provisional restoration during ridge reconstruction and implant site development. Key abutments are selected at optimal positions to sup- The International Journal of Periodontics & Restorative Dentistry
10 321 Fig 6a Case 4. Preoperative facial view. The maxillary anterior teeth show collapse of the supporting bone. Fig 6b The left central and lateral incisors exhibit bone resorption beyond the apex. Fig 6c Three-dimensional image using computer simulation software exhibits the horizontal and vertical bone defects in the anterior region. Fig 6e Lateral view of the right side after definitive cementation. In the canine area, implant placement allowed for the preservation of the tissue around the implant. This natural-looking outcome was achieved by using the 4D concept. Fig 6f The definitive result. A moderately natural appearance was obtained and acceptable interdental papillae maintained. Fig 6d Implants were placed in the positions of the right first molar, right first premolar, right central incisor, and left canine with sinus augmentation and GBR. The right central incisor site was an immediate placement site categorized as a class 3. At the right canine site, which was categorized as class 1, extraction and immediate implant placement were postponed until the previously placed implants were integrated and placed into function in the provisional prosthesis. The implant was placed toward the palate to secure a full 2 mm of distance from the labial bone. It was determined that if the existing contour was maintained, the IHB presented a high potential to preserve the papilla between the implants. Fig 6g Postoperative periapical radiographs. The bone crest between the maxillary right canine and first premolar was maintained at a higher level than the horizontal platform of the implant. The appropriate interproximal height of bone was retained in the implant region. Volume 27, Number 4, 2007
11 322 port a splinted full-arch provisional restoration while the ineffectual teeth are extracted and hard and soft tissues are reconstructed; implants are then placed. Following osseointegration, these implants are in turn used to support a new provisional restoration or incorporated into the existing provisional. The decision needs to be made on a tooth-by-tooth basis as to whether the remaining teeth that previously supported the provisional should be extracted and made into a pontic site with socket preservation techniques or sectioned below the crest of the ridge and below a connective tissue graft to preserve or redevelop the soft tissue esthetics. During implant placement, these key natural abutment teeth are used as guides to the vertical potential for augmented tissues as well as to the level of vertical placement of the implant. The preexisting IHB on these remaining teeth is the limiting factor in the soft tissue potential for an esthetic restoration. Obviously these key abutments need to be relatively stable to support the restoration. These provisional abutment teeth demonstrate the key role of the fourth dimension of time in 4D implant therapy, as the relative timing of the extractions is obviously a key component in predictable implant treatment planning. Conclusion A correct understanding of the indications and classification for immediate implant placement will dramatically aid the clinician in determining an appropriate treatment plan and time frame for individual tooth extractions and implant placement in single implant cases as well as complex multiple implant cases. This expansion of the 3D spatial placement of implants into a 4D concept uses timing as a key variable in the development of esthetic implant restorations. Acknowledgments The authors would like to thank Dr Myron Nevins and Dr Yoshiro Ono for their encouragement and support. References 1. Garber DA, Belser UC. Restoration driven implant placement with restoration-generated site development. Compend Contin Educ Dent 1995;16: Garber DA. The esthetic dental implant: Letting restoration be the guide. J Am Dent Assoc 1995;126: Carlsson GE, Thilander H, Hedgegard B. Histologic changes in the upper alveolar process after extractions with or without insertion of an immediate full denture. Acta Odontol Scand 1967;25: Schropp L, Wenzel A, Kostopoulos L, Karning T. Bone healing and soft tissue contour changes following single-tooth extraction: A clinical and radiographic 12- month prospective study. Int J Periodontics Restorative Dent 2003;23: Nevins M, Camero M, Friedland B, et al. A study of the fate of the buccal wall of extraction sockets of teeth with prominent roots. Int J Periodontics Restorative Dent 2006;26: Lazzara RJ. Immediate implant placement into extraction sites: Surgical and restorative advantages. Int J Periodontics Restorative Dent 1989;9: Wilson TG, Schenk R, Buser D, Cochran D. Implants placed in immediate extraction sites: A report of histologic and histometric analyses of human biopsies. Int J Oral Maxillofac Implants 1998;13: Paolantonio M, Dolci M, Scarano A, et al. Immediate implantation in fresh extraction sockets. A controlled clinical and histological study in man. J Periodontol 2001;72: Chen ST, Wilson TG Jr, Hammerle CH. Immediate or early placement of implants following tooth extraction: Review of biologic basis, clinical procedures, and outcomes. Int J Oral Maxillofac Implants 2004;19(suppl): Chen ST, Darby IB, Adams GG, Reynolds EC. A prospective clinical study of bone augmentation techniques at immediate implants. Clin Oral Implants Res 2005; 16: Covani U, Barone A, Cornelini R, Crespi R. Soft tissue healing around implants placed immediately after tooth extraction without incision: A clinical report. Int J Oral Maxillofac Implants 2004 Jul Aug;19: Salama H, Salama MA, Garber D, Adar P. The interproximal height of bone: A guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Pract Periodontics Aesthet Dent 1998;10: Grunder U. Stability of the mucosal topography around single-tooth implants and adjacent teeth: 1-year results. Int J Periodontics Restorative Dent 2000; 20: The International Journal of Periodontics & Restorative Dentistry
12 Cochran DL, Hermann JS, Schenk RK, Higginbottom FL, Buser D. Biologic width around titanium implants. A histometric analysis of the implanto-gingival junction around unloaded and loaded nonsubmerged implants in the canine mandible. J Periodontol 1997;68: Berglundh T, Lindhe J. Dimension of the peri-implant mucosa. Biological width revisited. Clin Periodontol 1996;23: Small PN, Tarnow DP. Gingival recession around implants: A 1-year longitudinal prospective study. Int J Oral Maxillofac Implants 2000;15: Salama H, Salama M. The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: A systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent 1993;13: Saadoun AP, Le Gall M. Selection and ideal three-dimensional implant position in the anterior aesthetic zone. Int Mag Oral Implantol 2003;4(4): Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol 2000;71: Grunder U, Gracis S, Capelli M. Influence of 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent 2005;25: Botticelli D, Berglundh T, Lindhe J. Resolution of bone defects of varying dimension and configuration in the marginal portion of the peri-implant bone. An experimental study in the dog. J Clin Periodontol 2004; 31: Saadoun AP, LeGall M, Toutai B. Current trends in implantology: Part II Treatment planning, aesthetic consideration, and tissue regeneration. Pract Proced Aesthet Dent 2004;16: Wohrle PS. Nobel Perfect esthetic scalloped implant: Rationale for a new design. Clin Implant Dent Relat Res 2003;5(suppl 1): Lazzara RJ, Porter SS. Platform switching: A new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent 2006;26: Baumgarten H, Cacchetto R, Testori T, Meltzer A, Porter S. A new implant design for crestal bone preservation: Initial observations and case report. Pract Proced Aesthet Dent 2005;17: Maynard JG Jr, Wilson RD. Physiologic dimensions of the periodontium significant to the restorative dentist. J Periodontol 1979;50: Kan JYK, Rungcharassaeng K, Umezu K, Kois J. Dimensions of peri-implant mucosa: An evaluation of maxillary anterior single implants in humans. J Periodontol 2003; 74: Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontal 2000;71: Abrahamson I, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol 1997;24: Volume 27, Number 4, 2007
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The following resources related to this article are available online at jada.ada.org ( this information is current as of July 11, 2011):
 Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
Implants or Pontics: Decision Making for Anterior Tooth Replacement Frank Spear J Am Dent Assoc 2009;140;1160-1166 The following resources related to this article are available online at jada.ada.org (
The 2B-3D rule for implant planning, placement and restoration
 IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Patients esthetic demands and
 Predictable Periimplant Gingival Esthetics: Use of the Natural Tooth as a Provisional following Implant Placement ROBERT C. MARGEAS, DDS* ABSTRACT Maintaining the interdental papilla and bone height following
Predictable Periimplant Gingival Esthetics: Use of the Natural Tooth as a Provisional following Implant Placement ROBERT C. MARGEAS, DDS* ABSTRACT Maintaining the interdental papilla and bone height following
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The refinement of adhesive technology and contemporary
 CONTINUING EDUCATION 3 4 THE INTERPROXIMAL HEIGHT OF BONE: A GUIDEPOST TO PREDICTABLE AESTHETIC STRATEGIES AND SOFT TISSUE CONTOURS IN ANTERIOR TOOTH REPLACEMENT Henry Salama, DMD* Maurice A. Salama, DMD
CONTINUING EDUCATION 3 4 THE INTERPROXIMAL HEIGHT OF BONE: A GUIDEPOST TO PREDICTABLE AESTHETIC STRATEGIES AND SOFT TISSUE CONTOURS IN ANTERIOR TOOTH REPLACEMENT Henry Salama, DMD* Maurice A. Salama, DMD
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Dental Implant Placement in the Maxillary Anterior Region: Guidelines for Aesthetic Success Michael Tischler, DDS
 Page 1 of 10 Issue Date: March 2005, Posted On: 5/2/2005 Dental Implant Placement in the Maxillary Anterior Region: Guidelines for Aesthetic Success Michael Tischler, DDS Figure 1. A 43-year-old female
Page 1 of 10 Issue Date: March 2005, Posted On: 5/2/2005 Dental Implant Placement in the Maxillary Anterior Region: Guidelines for Aesthetic Success Michael Tischler, DDS Figure 1. A 43-year-old female
The patient gave a history of hypertension and gastritis for which was taking Lacidipine 4mg, Omeprazole 20mg and Simvastatin 40mg.
 A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
A.S. was referred by her general dental practitioner for assessment for possible implant placement to restore the space where her bridge replacing her maxillary central incisors had recently failed. Fig
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Immediate implant placement in a single staged
 Bone and Crescent Shaped Free Gingival Grafting for Anterior Immediate Implant Placement: Technique and Case Report Han et al Thomas Han, DDS, MS 1 2 Abstract Immediate implant placement in a single staged
Bone and Crescent Shaped Free Gingival Grafting for Anterior Immediate Implant Placement: Technique and Case Report Han et al Thomas Han, DDS, MS 1 2 Abstract Immediate implant placement in a single staged
Planning for esthetics Part II: adjacent implant restorations
 C L I N I C A L Planning for esthetics Part II: adjacent implant restorations William C Martin, 1 Emma Lewis, 2 Dean Morton 3 1 DMD, MS, Associate Professor & Clinical Director, Center for Implant Dentistry,
C L I N I C A L Planning for esthetics Part II: adjacent implant restorations William C Martin, 1 Emma Lewis, 2 Dean Morton 3 1 DMD, MS, Associate Professor & Clinical Director, Center for Implant Dentistry,
Several extraction socket classifications have been
 Case Report Type 3 ReceSSion DefeCTS Clinical Management of Type 3 Recession Defects With Immediate Implant and Provisional Restoration Therapy: A Case Report Dennis P. Tarnow, DDS; and Stephen J. Chu,
Case Report Type 3 ReceSSion DefeCTS Clinical Management of Type 3 Recession Defects With Immediate Implant and Provisional Restoration Therapy: A Case Report Dennis P. Tarnow, DDS; and Stephen J. Chu,
Dental Implant Treatment Planning and Restorative Considerations
 Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Dental Implant Treatment Planning and Restorative Considerations Aldo Leopardi, BDS, DDS, MS Practice Limited to Implant, Fixed and Removable Prosthodontics Greenwood Village, Colorado www.knowledgefactoryco.com
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry
 Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Controlling Tissue Contours with a Prosthetically Driven Approach to Implant Dentistry Go online for in-depth content by Timothy F. Kosinski, DDS, MAGD With continual improvements in the design and production
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Advanced Esthetic Management of Dental Implants: Surgical and Restorative Considerations to Improve Outcomes
 CLINICAL ARTICLE Advanced Esthetic Management of Dental Implants: Surgical and Restorative Considerations to Improve Outcomes BARRY P. LEVIN, DMD*, SERGIO RUBINSTEIN, DDS, LOUIS F. ROSE, DDS, MD ** ABSTRACT
CLINICAL ARTICLE Advanced Esthetic Management of Dental Implants: Surgical and Restorative Considerations to Improve Outcomes BARRY P. LEVIN, DMD*, SERGIO RUBINSTEIN, DDS, LOUIS F. ROSE, DDS, MD ** ABSTRACT
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Then and Now. Implant Therapy:
 Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Immediate Restorations on Implants in the Esthetic Area
 CLINICAL SCIENCE IJOICR Immediate Restorations on Implants in the Esthetic Area Immediate Restorations on Implants in the Esthetic Area 1 Pedro Peña Martinez, 2 Ramón Palomero Langner, 3 Ramón Palomero
CLINICAL SCIENCE IJOICR Immediate Restorations on Implants in the Esthetic Area Immediate Restorations on Implants in the Esthetic Area 1 Pedro Peña Martinez, 2 Ramón Palomero Langner, 3 Ramón Palomero
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 2011 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.. 215 Dental Cone Beam Computed Tomography
The International Journal of Periodontics & Restorative Dentistry 2011 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.. 215 Dental Cone Beam Computed Tomography
Extraction Defect: Assessment, Classification and Management
 International Extraction Journal Defect: of Clinical Assessment, Implant Dentistry, Classification January-April and Management 2009;1(1):1-11 Extraction Defect: Assessment, Classification and Management
International Extraction Journal Defect: of Clinical Assessment, Implant Dentistry, Classification January-April and Management 2009;1(1):1-11 Extraction Defect: Assessment, Classification and Management
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Available online at International Journal of Current Research Vol. 7, Issue, 12, pp , December, 2015
 z Available online at http://www.journalcra.com International Journal of Current Research Vol. 7, Issue, 12, pp.24212-24216, December, 2015 INTERNATIONAL JOURNAL OF CURRENT RESEARCH ISSN: 0975-833X REVIEW
z Available online at http://www.journalcra.com International Journal of Current Research Vol. 7, Issue, 12, pp.24212-24216, December, 2015 INTERNATIONAL JOURNAL OF CURRENT RESEARCH ISSN: 0975-833X REVIEW
Smile Line Rehabilitation with Dental Implants. Agenda. Agenda. Smile line revitalization with implants Priest Prosthodontics, LLC 1
 Smile Line Rehabilitation with Dental Implants Board Certified Prosthodontist Hilton Head Island, SC Agenda Implant placement and esthetic potential Single immediate implant placement Soft tissue preservation
Smile Line Rehabilitation with Dental Implants Board Certified Prosthodontist Hilton Head Island, SC Agenda Implant placement and esthetic potential Single immediate implant placement Soft tissue preservation
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
IMPACT OF IMMEDIATE AND NON-IMMEDIATE PROVISIONALIZATION ON THE SOFT TISSUE ESTHETICS OF FINAL RESTORATIONS ON IMMEDIATELY PLACED IMPLANTS
 ORIGINAL ARTICLE IMPACT OF IMMEDIATE AND NON-IMMEDIATE PROVISIONALIZATION ON THE SOFT TISSUE ESTHETICS OF FINAL RESTORATIONS ON IMMEDIATELY PLACED IMPLANTS Chong-Hyun Han 1, DDS, PhD, Jeong-Won Paik 2,
ORIGINAL ARTICLE IMPACT OF IMMEDIATE AND NON-IMMEDIATE PROVISIONALIZATION ON THE SOFT TISSUE ESTHETICS OF FINAL RESTORATIONS ON IMMEDIATELY PLACED IMPLANTS Chong-Hyun Han 1, DDS, PhD, Jeong-Won Paik 2,
In the esthetic zone, osseointegration
 CASE REPORT A Method for Obtaining Peri-Implant Soft-Tissue Contours by Using Screw- Retained Provisional Restorations as Impression Copings: A Clinical Report Bi-Yuan Tsai, DDS, MS* In the esthetic zone,
CASE REPORT A Method for Obtaining Peri-Implant Soft-Tissue Contours by Using Screw- Retained Provisional Restorations as Impression Copings: A Clinical Report Bi-Yuan Tsai, DDS, MS* In the esthetic zone,
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique
 e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
Successful osseointegration of implants has been
 Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 559 Emergence Profile Design Based on Implant Position in the Esthetic Zone Marius Steigmann, DDS 1,2 Alberto Monje, DDS 3 Hsun-Liang Chan,
The International Journal of Periodontics & Restorative Dentistry 559 Emergence Profile Design Based on Implant Position in the Esthetic Zone Marius Steigmann, DDS 1,2 Alberto Monje, DDS 3 Hsun-Liang Chan,
Dental Implants and Esthetics
 Continuing Education Brought to you by Dental Implants and Esthetics Course Author(s): Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD CE Credits: 1 hour Intended Audience: Dentists, Dental Hygienists,
Continuing Education Brought to you by Dental Implants and Esthetics Course Author(s): Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD CE Credits: 1 hour Intended Audience: Dentists, Dental Hygienists,
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Factors influencing ridge alterations following immediate implant placement into extraction sockets
 Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Significance of crown shape in the replacement of a central incisor with a single implantsupported
 PROSTHODONTICS Significance of crown shape in the replacement of a central incisor with a single implantsupported crown Luca Gobbato, DDS 1 /Gianluca Paniz, DDS 2 /Fabio Mazzocco, DDS 3 / Andrea Chierico,
PROSTHODONTICS Significance of crown shape in the replacement of a central incisor with a single implantsupported crown Luca Gobbato, DDS 1 /Gianluca Paniz, DDS 2 /Fabio Mazzocco, DDS 3 / Andrea Chierico,
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants
 r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association
 All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 335 Considerations of Implant Abutment and Crown Contour: Critical Contour and Subcritical Contour Huan Su, DDS* Oscar González-Martín,
The International Journal of Periodontics & Restorative Dentistry 335 Considerations of Implant Abutment and Crown Contour: Critical Contour and Subcritical Contour Huan Su, DDS* Oscar González-Martín,
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Immediate Implant Placement: A Review
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. IV (May. 2017), PP 90-95 www.iosrjournals.org Immediate Implant Placement: A Review
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. IV (May. 2017), PP 90-95 www.iosrjournals.org Immediate Implant Placement: A Review
Esthetic Implant Dentistry: Diagnosis and Treatment Planning
 SECTION 4 Implant Surgery 26 Esthetic Implant Dentistry: Diagnosis and Treatment Planning SAJ JIVRAJ, MAMALY RESHAD Introduction Achieving esthetics with implant restorations is significantly more challenging
SECTION 4 Implant Surgery 26 Esthetic Implant Dentistry: Diagnosis and Treatment Planning SAJ JIVRAJ, MAMALY RESHAD Introduction Achieving esthetics with implant restorations is significantly more challenging
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Use of the natural tooth as a provisional after immediate implant placement
 Use of the natural tooth as a provisional after immediate implant placement By Robert Margeas, DDS Research on the preservation of the tissue architecture, reduction of surgical sequences and greater aesthetic
Use of the natural tooth as a provisional after immediate implant placement By Robert Margeas, DDS Research on the preservation of the tissue architecture, reduction of surgical sequences and greater aesthetic
The Socket Shield Technique A case Report
 The Socket Shield Technique A case Report Haseeb H. Al-Dary Private Practice, Amman Jordan dary_haseeb@yahoo.com ABSTRACT In the aim of achieving an optimal esthetic result, implant dentistry has become
The Socket Shield Technique A case Report Haseeb H. Al-Dary Private Practice, Amman Jordan dary_haseeb@yahoo.com ABSTRACT In the aim of achieving an optimal esthetic result, implant dentistry has become
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Ten tips that everyone should know before performing a treatment involving implants in the aesthetic zone.
 Ten tips that everyone should know before performing a treatment involving implants in the aesthetic zone. Introduction Francisco Teixeira Barbosa. Private practice. Barcelona. Spain. Nowadays, implantology
Ten tips that everyone should know before performing a treatment involving implants in the aesthetic zone. Introduction Francisco Teixeira Barbosa. Private practice. Barcelona. Spain. Nowadays, implantology
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Case Report Alveolar Ridge Augmentation using Subepithelial Connective Tissue Grafts: A Case report
 Alveolar Ridge Augmentation using Subepithelial Connective Tissue Grafts: A Case report Po-Yu Lai, DDS, MS School of Dentistry, National Yang-Ming University Shing-Wai Yip, DDS, MS, DScD Prosthodontics
Alveolar Ridge Augmentation using Subepithelial Connective Tissue Grafts: A Case report Po-Yu Lai, DDS, MS School of Dentistry, National Yang-Ming University Shing-Wai Yip, DDS, MS, DScD Prosthodontics
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Inclusive Tooth Replacement System
 Optimizing Anterior Esthetics with the Inclusive Tooth Replacement System by Timothy F. Kosinski, DDS, MAGD Implant treatment has changed so much over the years. In the past it was acceptable to place
Optimizing Anterior Esthetics with the Inclusive Tooth Replacement System by Timothy F. Kosinski, DDS, MAGD Implant treatment has changed so much over the years. In the past it was acceptable to place
Nicholas Caplanis DMD MS 6/13/2012
 Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 69 Analysis of the Shapes of Maxillary Central Incisors in a Caucasian Population Luca Gobbato, DDS*/Teppei Tsukiyama, DDS*/Paul A. Levi,
The International Journal of Periodontics & Restorative Dentistry 69 Analysis of the Shapes of Maxillary Central Incisors in a Caucasian Population Luca Gobbato, DDS*/Teppei Tsukiyama, DDS*/Paul A. Levi,
Bone Grafting and Immediate Implant Placement in the Anterior
 Bone Grafting and Immediate Implant Placement in the Anterior by Timothy F. Kosinski, DDS, MAGD Whether a consequence of periodontal disease, caries or trauma to the root, losing an anterior tooth is psychologically
Bone Grafting and Immediate Implant Placement in the Anterior by Timothy F. Kosinski, DDS, MAGD Whether a consequence of periodontal disease, caries or trauma to the root, losing an anterior tooth is psychologically
Initially, implant dentistry was focused on
 CASE LETTER Correction of Esthetic Complications of a Malpositioned Implant: A Case Letter Sergio Alexandre Gehrke, PhD INTRODUCTION Initially, implant dentistry was focused on successful osseointegration
CASE LETTER Correction of Esthetic Complications of a Malpositioned Implant: A Case Letter Sergio Alexandre Gehrke, PhD INTRODUCTION Initially, implant dentistry was focused on successful osseointegration
The success of implant-supported dental prostheses is
 CASE LETTER Pouch Roll Technique for Implant Soft-Tissue Augmentation of Small Defects: Two Case Reports With 5-Year Follow-Up Jorge Saade, DDS, MD 1, PhD 1 Bruno Salles Sotto-Maior, DDS, MD, PhD 2 * Carlos
CASE LETTER Pouch Roll Technique for Implant Soft-Tissue Augmentation of Small Defects: Two Case Reports With 5-Year Follow-Up Jorge Saade, DDS, MD 1, PhD 1 Bruno Salles Sotto-Maior, DDS, MD, PhD 2 * Carlos
ABSTRACT INTRODUCTION /jp-journals
 Prathapan Parayaruthottam, Vincy Antony Case Report 10.5005/jp-journals-10012-1137 Replacement of Missing Maxillary Central Incisor with an Osseointegrated Implant-supported Prosthesis from an Orthodontic
Prathapan Parayaruthottam, Vincy Antony Case Report 10.5005/jp-journals-10012-1137 Replacement of Missing Maxillary Central Incisor with an Osseointegrated Implant-supported Prosthesis from an Orthodontic
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
APOSTILA(DE(ARTIGOS( ( WEBINAR( INSTALAÇÃO*DE*IMPLANTES*NA*REGIÃO*POSTERIOR*DE* MAXILA*COM*POUCA*DISPONIBILIDADE*ÓSSEA* * * * * * * * * * * * * * * *
 APOSTILA(DE(ARTIGOS( ( WEBINAR( INSTALAÇÃO*DE*IMPLANTES*NA*REGIÃO*POSTERIOR*DE* MAXILA*COM*POUCA*DISPONIBILIDADE*ÓSSEA* * * * * * * * * * * * * * * * * * DR.(EDUARDO(DIAS( 2015( CONTINUING EDUCATION 34
APOSTILA(DE(ARTIGOS( ( WEBINAR( INSTALAÇÃO*DE*IMPLANTES*NA*REGIÃO*POSTERIOR*DE* MAXILA*COM*POUCA*DISPONIBILIDADE*ÓSSEA* * * * * * * * * * * * * * * * * * DR.(EDUARDO(DIAS( 2015( CONTINUING EDUCATION 34
Course Objectives. HDA 2018 Dental Implant Complications. What are some common failures / problems we all encounter?
 HDA 2018 Dental Implant Complications 1 Course Objectives - Understand protocols for diagnosing and treatment planning to minimize complications - Recognize and manage intraoperative complications during
HDA 2018 Dental Implant Complications 1 Course Objectives - Understand protocols for diagnosing and treatment planning to minimize complications - Recognize and manage intraoperative complications during
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 401 Guidelines for Selecting the Implant Diameter During Immediate Implant Placement of a Fresh Extraction Socket: A Case Series Ariádene
The International Journal of Periodontics & Restorative Dentistry 401 Guidelines for Selecting the Implant Diameter During Immediate Implant Placement of a Fresh Extraction Socket: A Case Series Ariádene
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Prosthodonticstown. Immediate Implant Placement in Fresh Extraction Sites. clinical. Table I
 Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
Prosthodonticstown clinical Immediate Implant Placement in Fresh Extraction Sites Charles A. Babbush, DDS, MScD Table I Benefits Of Immediate Implantation Improved prosthesis fabrication and/or design
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 47 Provisional Restorations Used in Immediate Implant Placement Provide a Platform to Promote Peri-implant Soft Tissue Healing: A Pilot
The International Journal of Periodontics & Restorative Dentistry 47 Provisional Restorations Used in Immediate Implant Placement Provide a Platform to Promote Peri-implant Soft Tissue Healing: A Pilot
ThinkIR: The University of Louisville's Institutional Repository
 University of Louisville ThinkIR: The University of Louisville's Institutional Repository Electronic Theses and Dissertations 12-2006 Implant esthetics using a Nobel Replace Standard implant vs. Nobel
University of Louisville ThinkIR: The University of Louisville's Institutional Repository Electronic Theses and Dissertations 12-2006 Implant esthetics using a Nobel Replace Standard implant vs. Nobel
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Natural preservation of the emergence profile
 case report Natural preservation of the emergence profile Authors: Dr Umut Baysal & Dr Arzu Tuna, Germany Supplying single-tooth gaps with implants in the aesthetic zone is subject to strict evaluation.
case report Natural preservation of the emergence profile Authors: Dr Umut Baysal & Dr Arzu Tuna, Germany Supplying single-tooth gaps with implants in the aesthetic zone is subject to strict evaluation.
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Abstract. A Case Of External Resorption
 SHGDDS 1 BY Steven H. Goldstein, DDS Abstract External resorption is a condition that leads to the irreversible loss of enamel, dentin, cementum, and in some cases bone. Its cause is not fully understood,
SHGDDS 1 BY Steven H. Goldstein, DDS Abstract External resorption is a condition that leads to the irreversible loss of enamel, dentin, cementum, and in some cases bone. Its cause is not fully understood,
