Nutritional and prosthodontic care for geriatric patients
|
|
|
- Marlene Kennedy
- 6 years ago
- Views:
Transcription
1 Review Article DOI: / X Yogeshwari Krishnan 1,*, Lara Jain 2, Jyotsna Seth 3, Varun Kumar 4 1 UG Student, 2 PG Student, 3 Reader, 4 Professor, Dept. of Prosthodontics, Seema Dental College & Hospital, Rishikesh, Uttrakhand *Corresponding Author: yogeshwari11095@gmail.com Abstract Perfect health is a prize that has been the goal of mankind throughout all ages. It must be understood that there can be no separation between good bodily health and good dental health. Oral health is not separate from general health, but maintaining oral health is definitely difficult and different in old age. For older patients, clinicians should consider maintaining teeth and using functionally-orientated treatment strategies as an alternative to removable prostheses. When the remaining dentition has a poor prognosis, key teeth should be preserved as overdenture abutments and a gradual transition to edentulousness planned. Where complete dentures are provided, these can be retained using dental implants to overcome many of the problems associated with conventional replacement dentures. The elderly population of today is better informed and more demanding of oral healthcare providers than previous generations. Clinicians should be aware of all the prosthodontic treatment options available for older patients. Introduction Aging is a natural process. Old age should be regarded as a normal, inevitable biological phenomenon. Elders above 65 years (old age) have health problems as a result of aging process, which calls for special consideration. Proper nutrition is essential to the health and comfort of oral tissues and healthy tissues enhance the possibility of successful prosthodontic treatment in the elderly. (1) In patients with partial or complete tooth loss, prosthetic therapy may be important to maintain or restore masticatory function. However, many other factors also are essential for the nutritional status of older adults. Thus, many age-related medical problems and diseases have nutritional aspects and the patient s socioeconomic status and dietary habits have a profound influence on their dietary selection. The dental team must be aware of these potential detrimental effects of dental treatment and provide counteractive dietary guidance. (2) Problems vary with the patient and the dental condition, so suggestions must be tailored to meet the patient s specific needs. The purpose of this article is to describe management of a contemporary denture patient and to make recommendations for solving complete denture problems. Increased Life Expectancy The current denture population may be characterized as having a larger number of medical problems that require the care of 1 or more physicians. It has been reported that the typical complete denture patients of today have a greater mean age, live independently, are financially able to afford care, and are retaining more teeth. Additionally, missing teeth are being replaced by more fixed partial dentures, more removable partial dentures, and more implant-supported prostheses. These patients are frequently taking a large number of medications, often prescribed by different physicians, without collaboration. These factors may result in tissue responses to complete dentures being less satisfactory and reduce the healing capacity of the oral tissues. Subsequently, it may be more difficult to manage the edentulous patient with predictable success. Clinically, many of these patients are seen with severely resorbed residual ridges and prominent anatomic landmarks or bony abnormalities. The soft tissues are often redundant and unsupported. Maxillary arches frequently demonstrate enlarged tuberosities and reundant anterior tissues resultant to the use of maxillary complete denture opposing a mandibular removable partial denture with natural anterior teeth. Anterior teeth on existing prostheses are often in occlusal contact because of wear and loss of vertical dimension. Some patients expect the anterior teeth of the new dentures to contact in a manner similar to their natural teeth. In many situations, the restoration of natural anterior tooth contacts could result in compromised function and esthetics, making it necessary to educate the patient about the need to modify the tooth position and tooth contact to facilitate an acceptable functional prognosis. Expectation A thorough examination is invaluable for proper diagnosis, treatment planning, and identification of realistic goals or expectations. Many patients are aware that physical changes have occurred in their bodies, but some are unaware of the impact on their oral cavities. Burnett et al points out that attempts to improve denture hygiene (habits) of veteran denture wearers with either verbal or written instructions were equally ineffective in changing the habits when reviewed 6 months after the instructional material was delivered. International Journal of Oral Health Dentistry; July-September 2017;3(3):
2 Many common characteristics of an aged population, such as decreased neuromuscular coordination, reduced ability to sense where the mandible is in relation to the maxilla (oral awareness), and impaired ability to position the mandible or tongue in desired locations (oral dexterity), will complicate the complete denture treatment process. Oral factors that affect diet and nutritional status Xerostomia affects almost one in five older adults. Xerostomia is associated with difficulties in chewing and swallowing, all of which can adversely affect food selection and contribute to poor nutritional status. The use of drugs with hypo salivary side effects may have deleterious influence on denture bearing tissues. Nutrition and Age 1. To establish a balanced diet which is consistent with the physical, social, psychological and economic background of the patient. 2. To provide temporary dietary supportive treatment, directed towards specific goals such as carries control, postoperative healing, or soft tissue conditioning. 3. To interpret factors peculiar to the denture age group of patients, which may relate to or complicate nutritional therapy. Factors Affecting Nutrition Physiological factors: With a decline in lean body mass in the elderly, caloric needs decrease and risk of falling increases. Vitamin D deficiency in turn, is a major cause of metabolic bone disease in the elderly. Declines in gastric acidity often occur with age and can cause malabsorption of food-bound vitamin B12. Many nutrient deficiencies common in the elderly, including zinc and vitamin B6, seem to result in decreased or modified immune responses. Dehydration, caused by declines in kidney function and total body water metabolism, is a major concern in the older population. Overt deficiency of several vitamins is associated with neurological and/or behavioral impairment B1 (thiamin), B2, niacin, B6 [pyridoxine], B12, foliate, pantothenic acid, vitamin C and vitamine). Psychosocial factors: A host of life-situational factors increase nutritional risk in elders. Elders, particularly at risk, include those living alone, the physically handicapped with insufficient care, the isolated, those with chronic disease and/or restrictive diets, reduced economic status and the oldest old. Functional factors: Functional disabilities such as arthritis, stroke, vision, or hearing impairment, can affect nutritional. Pharmacological factors: Most elders take several prescription and over-the counter medications daily. Prescription drugs are the primary cause of anorexia, nausea, vomiting, gastrointestinal disturbances, xerostomia, taste loss and interference with nutrient absorption and utilization. These conditions can lead to nutrient deficiencies, weight loss and ultimate malnutrition. Age-related changes in taste and smell may alter food choice and decrease diet quality in some people. Factors contributing to this reported decreased function may include health disorders, medications, oral hygiene, denture use and smoking. The presence of natural teeth and well-fitting dentures were associated with higher and more varied nutrition intakes and greater dietary quality, in the oldest old Iowans sampled. Effects of dentures on chewing ability as adult s age, they tend to use more strokes and chew longer, to prepare food for swallowing. Masticatory efficiency in complete denture wearers is approximately 80% lower than in people with intact natural dentition. Nutritional Care for Geriatric Patients Several of the larger studies noted that dentition status is associated with dietary intake however, most of the studies fail to show weather these associations are independent of common factors or total calorie intakes. Energy needs decline with age due to a decrease in basal metabolism and decreased physical activity. Cross-sectional surveys show that the average energy consumption of year old women is about 1300 kilocalories (Kcal) and 1800 Kcal for men of the same age. Caloric requirements decrease with advancing age. The mean RDA is 1600 Kcal for women and 2400 Kcal for men. As the patients become older, the amount of protein required increases. Protein depletion of body stores in the elderly, is seen primarily as a decrease of the skeletal muscle mass. Proteins is a must for denture wearers. The RDA for proteins, for persons aged 51 and over, is 0.8-g protein/kg body weight per day. (56 gms for males and 46 gms for females, or 9 and 10% respectively, of the recommended calorie intake. The best sources of proteins for the elderly diet are dairy products, poultry, meats and fish in the boiled and not dried form. Nuts, grains, legumes and vegetables contain protein, which if eaten in the proper combination, is of the same quality as animal sources of protein. The elderly consume a large proportion of their calories as carbohydrates, possibly at the expense of protein, because of their low cost, ability to be stored without refrigeration and ease of preparation. The recommended range of intake is 50 to 60 per cent of International Journal of Oral Health Dentistry; July-September 2017;3(3):
3 total calories. Food sources include grains and cereals, vegetables, fruits and dairy products. An important component of complex carbohydrates is fiber, which promotes bowel function. Fiber in the form of bran is frequently added to dry cereals and breads, but vegetable fiber is more effective and less expensive. Reduced selection of foods rich in fiber that are hard to chew, could provoke gastrointestinal disturbances in some edentulous elderly, with deficient masticatory performance. Elderly are particularly susceptible to negative water balance, usually caused by excessive water loss through damaged kidney. Inadequate intake of fluid by the elderly will lead to rapid dehydration and associated problems such as hypotension, elevated body temperature and dryness of the mucosa, decreased urine output and mental confusion. Under normal conditions, fluid intake should be at least 30 ml per kg body weight per day. The RDA for vitamin A is micrograms. Vitamin A in food occurs in two forms: retinal, or active Vitamin A in animal foods (liver, milk and milk products and beta-carotene or pro-vitamin A, found in deep green and yellow fruits and vegetables (apricots, carrots, spinach). Deficiency causes Bitot s spots (eyes), conjunctival and corneal xerosis (dryness), xerosis of skin, follicular hyperkeratosis, decreased salivary flow, dryness and keratosis of oral mucosa and decreased taste acuity. Long standing deficiency may cause hyperplasia of the gums, as well as generalized gingivitis The RDA has been set at 0.5 per 1000 calories, or at least 1 mg daily. Food sources include meats (especially pork and chicken), peas, whole grains, fortified grains, cereals and yeast. Deficiency causes beriberi. Vitamin B6 deficiency (pyridoxine) - ranges from 50 to 90% of the elderly affected. The RDA is mg. Deficiency causes nasolabial seborrhea, glossitis. Vitamin B12- RDA is 3.0 microgram. Food sources are kidney, heart, milk, eggs, liver and green leafy vegetables. Deficiency causes nasolabial seborrhea, fissuring and redness of eyelid corners and mouth magenta-colored tongue and genital dermatosis. The RDA is about 60 microgram. Food sources include citrus fruits, tomatoes, potatoes and leafy vegetables. Deficiency causes spongy, bleeding gums, petechiae, delayed healing tissues, painful joints. The elderly are frequently deficient in Vitamin D because of lack of sun exposure and an inability to synthesize Vitamin D in skin and convert it in the kidney. Vitamin D is found in fish liver oils. The RDA is 5 microgram. Deficiency causes bowlegs, beading of ribs. Vitamin E deficiency in the elderly does not seem to be a problem. Total plasma vitamin E levels increase with age. All minerals also plays very important role in maintenance of health. Good food sources of folic acid include leafy green vegetables, oranges, liver, legumes and yeast. Deficiency causes megaloblastic anemia, mouth ulcers, glossodynia, glossitis, stomatitis. The recommended daily allowance of calcium is 800 mg/day. Because calcium absorption decreased in the elderly (lack of hydrochloric acid in the stomach), the calcium must be acidulated before digestion. Food sources of calcium include milk and milk products, dried beans and peas, canned Salmon, leafy green vegetables and tofu. Elderly patients with complete dentures often experience a rapid and excessive ridge resorption, which may be related to negative balance of calcium, which contributes to development of osteoporosis. The RDA for iron is 10 mg. Good food sources include meat, fish, poultry, whole grains, fortified breads and cereals, leafy green vegetables, dried beans and peas. Deficiency causes burning tongue, dry mouth, anemia and angular cheilosis. Treatment planning for partially dentate patients with good prognosis As rates of edentulousness decline, clinicians are faced with treating increasing numbers of older partially dentate patients. If prosthodontic replacement of teeth is required, the majority receive removable partial dentures (RPDs) to meet functional and aesthetic demands. There is always a biological price associated with RPD provision, but the risk of disease can be reduced if patients maintain a good standard of oral hygiene and their previous dental history indicates a low risk of disease. Given the propensity for RPDs to complicate plaque control, it is vital that they are designed using hygienic principles. RPDs constructed with a cobalt-chromium framework can be used to minimize gingival coverage and ensure that International Journal of Oral Health Dentistry; July-September 2017;3(3):
4 components do not encroach on root surfaces. Frameworks for dentures should not be overly complicated, and the minimal number of components needed to provide adequate retention and support should be provided. Ideally, unless additions are planned, cobalt chromium frameworks should be favoured over acrylic baseplates. Acrylic RPDs often gain retention through extending over the soft tissues or engaging with the embrasure spaces of remaining teeth. They can be unhygienic and cause trauma to the soft tissues, thus their use should be limited where possible. Some researchers have suggested that older adults have different functional needs from young patients and therefore do not need a complete natural dentition. (4) The concept of minimally invasive dentistry (MID) has also been proposed as an effective and acceptable form of dental management for older adults. In addition to caries prevention strategies and conservative management of cavities, this strategy also includes the use of resin-bonded or cement-retained bridges to maintain shortened dental arches where anterior teeth are missing. The use of bridgework instead of RPDs. In this way has been shown to be an effective means of replacing missing teeth with a reduced maintenance burden. Especially in partially reduced dentitions with (almost) sound remaining teeth, resin-bonded bridges offer a good treatment alternative to RPDs. They are relatively easy to place, are relatively inexpensive and well accepted by the patient. The biological price is low compared to conventional bridges and RPDs. Glass fibre-reinforced composite bridgework can also be used to restore patients with a shortened dental arch. Fibre-reinforced composite, resin-bonded bridges can be made both directly in the mouth by the clinician or indirectly in a dental laboratory. However, for use in the management of partially reduced dentitions in the elderly, this is compensated for by the relative ease with which they can be repaired and extended, if necessary. These functionally-oriented treatment strategies aim to reduce the burden of maintenance for older adults. It is essential that the remaining natural dentition has a good long-term prognosis, and that the patient is sufficiently motivated (and physically able) to be able to maintain a good standard of oral hygiene and thus reduce the risk of further tooth loss. Treatment planning for partially edentulous with poor prognosis (2) In certain clinical situations, it is very likely that the patient will eventually lose all of his/her natural teeth. These situations can include the following considerations: Questionable patient motivation, advanced periodontal disease, poorly controlled caries, advanced tooth wear, financial considerations. Immediate Denture: The goal of Immediate Denture therapy is to maintain satisfactory appearance and function during the post-extraction phase of treatment. When providing immediate replacement dentures. The patient must also be advised that immediate dentures are intended to be temporary, and will probably have to be replaced after 6 12 months. Removable partial dentures can be used to replace mainly posterior teeth in the first instance. An existing partial denture can be immediately added to or an acrylic prosthesis fabricated. After a suitable transitional period, six months is usually sufficient, the clinician may convert the transitional partial denture to a complete immediate replacement denture. Occasionally, it is possible to rebase the immediate replacement dentures but, in most cases, new replacement complete dentures would be required after 6 12 months. Maintaining key teeth OVERDENTURES: Providing an older person with his/her first complete replacement denture can be a difficult experience for both clinician and patient. One possible alternative to complete tooth loss is the retention of a number of strategically important teeth and the utilization of overdentures. Overdentures have proven to be very successful, especially in the mandible where bone resorption can severely compromise denture stability and retention. Advantages of overdentures As the oral health of older adults improves, it seems likely that older adults will be less likely to accept that tooth loss is an inevitable part of the ageing process. Consequently, retaining some portion of their natural dentition will be of great benefit. They can be useful if partial denture construction is proving difficult, for example in cases with unsuitable abutment teeth or where saddles have conflicting paths of insertion. Overdentures can prove successful in hypodontia cases as well as cleft palate or surgical defect cases. With non-carious tooth surface loss, an increasing problem amongst older patients, overdentures can be used as diagnostic or definitive prostheses to restore teeth. Planning for overdentures requires the careful assessment of potential abutment teeth. The prognosis for the retained teeth should be good, and they should be considered restorable. (4) Saving some of the remaining natural teeth can convey huge psychological benefits to the patient. As International Journal of Oral Health Dentistry; July-September 2017;3(3):
5 well as making the denture feel more secure, patients are comforted by the fact that they still retain some of their own natural teeth. Through the retained roots, sensory feedback and proprioception are maintained, helping to provide an awareness of jaw-space relationships and improving chewing efficiency. Greatly enhance support for the denture. By utilizing teeth to retain the prosthesis, alveolar bone is preserved, thus reducing loss of vertical dimension and lip support. Patients for whom overdentures may be indicated are often not ideal dental patients. They will have lost teeth due to a combination of disease susceptibility and neglect. Vigilance is therefore essential and a programme of intensive maintenance will be required. Unfortunately, caries and periodontal disease are common problems associated with overdenture abutments. In addition, if an adequate thickness of acrylic is not provided over the abutment teeth, the prosthesis can be susceptible to fracture. In cases where retention is severely compromised, the clinician can consider the use of precision attachments to enhance denture retention. A precision attachment is an interlocking device, one component of which is fixed to an abutment, while the other is incorporated into a denture or bridge. Precision attachments can be particularly useful when providing elderly patients with a complete denture for the first time. They can also be utilized successfully in patients with poor muscular control, including those suffering from Parkinson s disease or a post-cerebrovascular accident. Treatment planning in completely edentulous patients Despite falling rates of edentulousness, many elderly patients still require prosthodontic replacement of all their natural teeth. Successful provision of complete dentures, even for patients with experience of wearing previous prostheses, can be challenging as many have resorbed alveolar ridges and postural jaw relationships. However, many patients can be successfully managed using conventional complete replacement dentures when fundamental prosthodontics principles are applied. Care should be taken to ensure that dentures are well extended, especially in the mandible, to take advantage of retention from the retromolar pads, and that balanced articulation has been achieved. Patients who present wearing existing complete dentures which have proved successful can be candidates for copy dentures, or at least incorporation of the successful features into new conventional dentures. Preprosthetic Care (5) Long-term denture use, especially of a poorly maintained or ill-fitting denture, can lead to tissue trauma and chronic soreness. These conditions must be corrected before new denture fabrication by use of tissue rest, tissue conditioning, or preprosthetic surgery. Adequate tissue rest by way of denture removal for a period of days is a common method of correction. The use of tissue conditioners is the next procedure that can help return the tissues to a healthy condition. Tissue conditioning therapy is often requisite to surgical procedures and can provide suitable modification of an existing complete denture for use during the treatment phase. Preprosthetic surgery may be viewed as a questionable treatment recommendation by an experienced denture wearer unaware of the deleterious tissue response that has developed. One of the more frequent treatment recommendations is the surgical management of large tuberosities. Failure to recognize and manage enlarged tuberosities may impede the clinician s ability to develop proper vertical dimension and occlusal plane orientation. Both of these considerations impact the forces applied to the denture bases during function and parafunction. Denture base movement and lack of stability is a common cause of soreness and lack of retention. Another preprosthetic procedure frequently overlooked is soft tissue removal from the superior and lingual surfaces of the retromolar pad. This procedure provides a firm retromolar pad with a shallower slope in the molar area. When unrecognized, this region may be distorted during impression making, potentially resulting in tissue impingement and patient soreness. The removal of redundant tissues covering a sharp or highly resorbed residual ridge, or augmentation of redundant tissue with artificial materials has fallen into disfavor because of frequent complications. With the predictability of osseo-integration there has been a growing shift towards the routine use of implants to stabilize complete removable prostheses. International Journal of Oral Health Dentistry; July-September 2017;3(3):
6 This is driven by the fact that implants can overcome many of the functional, psychological and physiological consequences of edentulousness. Implants help to preserve alveolar bone and bite force is increased when compared with conventional complete dentures. This may enable the patient to chew food with a higher nutritional value, which is important for general health. However, providing implant supported prosthodontics involves more complex and lengthy treatment procedures than conventional care. Prior to implant placement, careful planning is required to assess the width and height of the alveolar ridge present. Bone augmentation may be required prior to implant surgery if insufficient bone levels are present to support the implants. Patients suffering from any condition that precludes a minor oral surgical procedure, eg poorly controlled diabetes mellitus, blood dyscrasia, immunologically compromised, would be unsuitable for implant placement. Amongst elderly patients, particular attention should also be paid to any history of head and neck radiotherapy and use of bisphosphonate medications. Whilst not universally considered an absolute contra-indication, patients who smoke should be advised that the failure of implants and postoperative complications are much higher in smokers than non-smokers. In addition, as with other prosthodontic treatment options, implant-retained dentures require careful maintenance from both the patient and clinician. Implant-retained prostheses have been a major advance in the treatment of patients with denture wearing difficulties, and offer the possibility of overcoming many of the problems associated with conventional replacement dentures. Evidence suggests that implantretained mandibular overdentures should be considered as first choice treatment for edentulous patients. However, for many elderly patients who could benefit most from implant-retained prosthodontics, they remain financially prohibitive. References 1. Barone JV. Nutrition-Phase one of the edentulous patient. J Prosthet Dent 1978;40: Ramsey WO. The role of nutrition in conditioning edentulous patients. J Prosthet Dent 1970;23: Mich D. Nutrition for the aging patient. J Pros Dent 1960; 10: Fisher WT. Prosthetics and geriatric nutrition. J Pros Dent 1955; 5: Silverman SI. Geriatrics and tissue changes problems of aging denture patients. J Pros Dent 1958; 8: Schweiger JW. Prosthetic considerations for the aging. J Pros Dent 1959; 9: Conclusion Many Prosthesis failures are the result of nutritional deficiencies. Good health and nutrition of older patients are necessary for the successful wearing of dentures or any prosthesis. A better informed, more demanding elderly population is less likely to accept traditional treatment philosophies based around extractions and replacement of teeth with complete dentures. Functionally-orientated and minimally invasive treatment strategies can enable older patients to maintain natural teeth and avoid the need for a removable prosthesis. For those patients who will lose natural teeth, key teeth should be preserved to support overdentures or a careful transition to edentulousness should be planned. International Journal of Oral Health Dentistry; July-September 2017;3(3):
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Review Article. Keywords Denture; Diet Counselling; Malnutrition; Nutrition
 Review Article Role of Nutrition Assessment and Dietary Counselling in Geriatric Denture Population- An Overview Manu Rathee, 1 Shefali Singla, 2 Mohaneesh Bhoria, 3 Renu Kundu, 4 1- Senior Professor and
Review Article Role of Nutrition Assessment and Dietary Counselling in Geriatric Denture Population- An Overview Manu Rathee, 1 Shefali Singla, 2 Mohaneesh Bhoria, 3 Renu Kundu, 4 1- Senior Professor and
ACRYLIC REMOVABLE PARTIAL DENTURE(RPD)
 ACRYLIC REMOVABLE PARTIAL DENTURE(RPD) is a dental prosthesis which artificially supplies teeth and associated structure in a partially edentulous arch, made from acrylic resin and can be inserted and
ACRYLIC REMOVABLE PARTIAL DENTURE(RPD) is a dental prosthesis which artificially supplies teeth and associated structure in a partially edentulous arch, made from acrylic resin and can be inserted and
Lect. 14 Prosthodontics Dr. Osama
 Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
Lect. 14 Prosthodontics Dr. Osama Principles of Removable Partial Denture Design Difference in Prosthesis Support and Influence on Design: For a tooth-supported prosthesis, the movement potential is less
Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete Denture and Mandibular Teeth supported Overdenture
 Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Patient's Guide to Dental Implants. an investment for a lifelong smile
 Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Principles of. By: Dr. Ahmad Rabah
 Principles of By: Dr. Ahmad Rabah 1. Utilize what's present: Whenever possible, select a design that fits the teeth and soft tissues, rather than choosing one that requires tissue alteration. When minimal
Principles of By: Dr. Ahmad Rabah 1. Utilize what's present: Whenever possible, select a design that fits the teeth and soft tissues, rather than choosing one that requires tissue alteration. When minimal
Diagnosis. overt Examination. Definitive Examination. History. atient interview. Personal History. Clinical Examination.
 Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Mandibular ridge changes after adaptation. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss
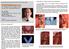 (Journal of Dental Outlook, Vol.110, Vol.6:1021~1027, Japan 2007. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss Dr. Jiro Abe Abe Dental Clinic
(Journal of Dental Outlook, Vol.110, Vol.6:1021~1027, Japan 2007. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss Dr. Jiro Abe Abe Dental Clinic
Vitamin A. Vitamin D
 Vitamin A Fat Soluble Vitamin Maintains hair and skin cells. Helps prevent night blindness. Orange and dark green vegetables, dairy products, and fish oils Works with calcium to build and maintain healthy
Vitamin A Fat Soluble Vitamin Maintains hair and skin cells. Helps prevent night blindness. Orange and dark green vegetables, dairy products, and fish oils Works with calcium to build and maintain healthy
Pre prosthetic surgery
 Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
VITAMIN BASICS VITAMIN WHAT IT DOES TOO LITTLE TOO MUCH SOURCES. Night blindness Total blindness Reduced resistance to infection Can lead to death
 VITAMIN BASICS VITAMIN WHAT IT DOES TOO LITTLE TOO MUCH SOURCES Fat-Soluble Vitamin A Maintains vision Maintains epithelial tissues (skin) Develops immune cells Bone growth Night blindness Total blindness
VITAMIN BASICS VITAMIN WHAT IT DOES TOO LITTLE TOO MUCH SOURCES Fat-Soluble Vitamin A Maintains vision Maintains epithelial tissues (skin) Develops immune cells Bone growth Night blindness Total blindness
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Removable partial dentures
 Removable partial dentures Feb, 4, 2015 McCracken's Removable Partial Prosthodontics, Twelfth Edition Carr, Alan B 1 Prosthesis that replaces the missing teeth and associated supporting structures in a
Removable partial dentures Feb, 4, 2015 McCracken's Removable Partial Prosthodontics, Twelfth Edition Carr, Alan B 1 Prosthesis that replaces the missing teeth and associated supporting structures in a
Nutrients. The food you eat is a source of nutrients. Nutrients are defined as the substances found in food that keep your body functioning.
 Nutrients The food you eat is a source of nutrients. Nutrients are defined as the substances found in food that keep your body functioning. Your body needs nutrients to Provide energy. Build and repair
Nutrients The food you eat is a source of nutrients. Nutrients are defined as the substances found in food that keep your body functioning. Your body needs nutrients to Provide energy. Build and repair
30/01/2012. Aim. Learning Objectives. Learning Objectives. We know that. Learning Objectives. Diagnosing. Treatment planning.
 Aim Advanced Partial Dentures A contradiction or a true advance? Looking to the Partial denture option Learning Objectives Diagnosing Treatment planning Learning Objectives Expectations have greatly overtaken
Aim Advanced Partial Dentures A contradiction or a true advance? Looking to the Partial denture option Learning Objectives Diagnosing Treatment planning Learning Objectives Expectations have greatly overtaken
TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT
 TJPRC: International Journal of Prosthetic Dentistry & Research (TJPRC:IJPDR) Vol. 1, Issue 1, Jun 2017, 5-10 TJPRC Pvt. Ltd. TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT ANSUIA GUPTA 1,
TJPRC: International Journal of Prosthetic Dentistry & Research (TJPRC:IJPDR) Vol. 1, Issue 1, Jun 2017, 5-10 TJPRC Pvt. Ltd. TOOTH SUPPORTED MANDIBULAR OVERDENTURE: A FORGOTTEN CONCEPT ANSUIA GUPTA 1,
Removable Partial Dentures
 Removable Partial Dentures Replacement of missing teeth Fixed partial denture Removable partial denture Complete removable Transitional denture Partial removable Implant retained prosthodontics No prosthetic
Removable Partial Dentures Replacement of missing teeth Fixed partial denture Removable partial denture Complete removable Transitional denture Partial removable Implant retained prosthodontics No prosthetic
F. To provide energy, to spare body protein, to prevent ketosis. G. Food sources include breads, vegetables, fruit, and milk.
 Nutrition: Nutrients for the Body Nutrients are chemical substances supplied by food that the body needs for growth, maintenance, and repair. The six nutrients are: 1. Carbohydrates. 2. Proteins. 3. Fats.
Nutrition: Nutrients for the Body Nutrients are chemical substances supplied by food that the body needs for growth, maintenance, and repair. The six nutrients are: 1. Carbohydrates. 2. Proteins. 3. Fats.
Intro to Vitamins, Minerals & Water
 Intro to Vitamins, Minerals & Water 1. What is the main function of vitamins and minerals? To regulate body functions 2. What foods are a lot of the vitamins and minerals we need found in? Fruits and Vegetables
Intro to Vitamins, Minerals & Water 1. What is the main function of vitamins and minerals? To regulate body functions 2. What foods are a lot of the vitamins and minerals we need found in? Fruits and Vegetables
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY
 RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
Prosthodontic Rehabilitation with Overdenture Using Modified Impression Technique: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
Dental Management of the Older Patient
 Dental Management of the Older Patient Aim: This article will discuss the management of the older patient in dental practice; ageing of the population and increasingly prolonged retention of teeth has
Dental Management of the Older Patient Aim: This article will discuss the management of the older patient in dental practice; ageing of the population and increasingly prolonged retention of teeth has
STANDARDS & GUIDELINES
 STANDARDS & GUIDELINES 3.1.1. Complete Dentures 2 APPENDIX A FOR 3.1.1 Complete Dentures.. 3 Patient History and Treatment Plan Impressions Centric and Protrusive Denture Try In Insertion 3.1.2. Partial
STANDARDS & GUIDELINES 3.1.1. Complete Dentures 2 APPENDIX A FOR 3.1.1 Complete Dentures.. 3 Patient History and Treatment Plan Impressions Centric and Protrusive Denture Try In Insertion 3.1.2. Partial
REMOVABLE PROSTHODONTICS
 REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.
 This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
FIXED PROSTHODONTICS
 FIXED PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG017.02 Effective Date: May 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS... 1 COVERAGE
FIXED PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG017.02 Effective Date: May 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS... 1 COVERAGE
There are three referral categories used in the dental referral system:
 Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
Restorative Dentistry Referral Criteria Restorative Dentistry referral criteria are outlined to provide General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists, Primary Care Specialists,
OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC
 Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
M.D.S. DEGREE EXAMINATION. (Revised Regulations) Branch VI PROSTHODONTICS. (For Candidates admitted from onwards)
 September 2008 [KT 389] Sub. Code: 2422. (Revised Regulations) Branch VI PROSTHODONTICS (For Candidates admitted from 2004-2005 onwards) Paper II REMOVABLE PROSTHODONTICS AND Time : Three hours Q.P. Code
September 2008 [KT 389] Sub. Code: 2422. (Revised Regulations) Branch VI PROSTHODONTICS (For Candidates admitted from 2004-2005 onwards) Paper II REMOVABLE PROSTHODONTICS AND Time : Three hours Q.P. Code
Name Unit # Period Score 159 points possible Dietary Guidelines, Food Pyramid and Nutrients Test
 Name Unit # Period Score 159 points possible Dietary Guidelines, Food Pyramid and Nutrients Test 1. List the ten dietary guidelines recommended for Americans. (10) a. b. c. d. e. f. g. h. i. j. Multiple
Name Unit # Period Score 159 points possible Dietary Guidelines, Food Pyramid and Nutrients Test 1. List the ten dietary guidelines recommended for Americans. (10) a. b. c. d. e. f. g. h. i. j. Multiple
Nutrition for Health. Nutrients. Before You Read
 CHAPTER 10 LESSON 2 Nutrition for Health Nutrients BIG Idea Each nutrient in your diet plays a unique and essential role in keeping you healthy. Before You Read Sometimes figuring out what to eat can be
CHAPTER 10 LESSON 2 Nutrition for Health Nutrients BIG Idea Each nutrient in your diet plays a unique and essential role in keeping you healthy. Before You Read Sometimes figuring out what to eat can be
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Complete denture impressions
 Lec.5 Complete denture impressions د. غسان الطائي Dental Impression: a negative imprint of an oral structure used to produce a positive replica of the structure to be used as a permanent record or in the
Lec.5 Complete denture impressions د. غسان الطائي Dental Impression: a negative imprint of an oral structure used to produce a positive replica of the structure to be used as a permanent record or in the
Everything You Need to Know about Vitamins and Minerals
 Everything You Need to Know about Vitamins and Minerals A Beta-Carotene Thiamine (B 1 ) Riboflavin (B 2 ) Vitamin A is needed for new cell growth. Helps fight infection. Essential for healthy skin, good
Everything You Need to Know about Vitamins and Minerals A Beta-Carotene Thiamine (B 1 ) Riboflavin (B 2 ) Vitamin A is needed for new cell growth. Helps fight infection. Essential for healthy skin, good
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Chapter Why do we eat & Nutrition and Nutrients
 Chapter 15.1 Why do we eat & Nutrition and Nutrients Why do we eat? Physical Needs: Nutrients chemicals found in food, the body needs to function properly. Nutrition study of foods and the way your body
Chapter 15.1 Why do we eat & Nutrition and Nutrients Why do we eat? Physical Needs: Nutrients chemicals found in food, the body needs to function properly. Nutrition study of foods and the way your body
A perfect fit for ultimate comfort. Soft and Extra Soft
 A perfect fit for ultimate comfort GC RELINE Soft and Extra Soft GC RELINE Soft & GC RELINE Extra Soft Ready-to-use, temporary soft silicone based reline materials. Vinyl polysiloxane materials in cartridges
A perfect fit for ultimate comfort GC RELINE Soft and Extra Soft GC RELINE Soft & GC RELINE Extra Soft Ready-to-use, temporary soft silicone based reline materials. Vinyl polysiloxane materials in cartridges
ISPUB.COM. Habitual Centric: A Case Report. Manisha, N Kathuria, A Gupta, N Gupta INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
Immediate Complete Denture: A Case Report
 Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
A GUIDE TO THE BENEFIT OF DENTAL IMPLANTS A permanent alternative to dentures! Restore your teeth and win back your life!
 A GUIDE TO THE BENEFIT OF DENTAL IMPLANTS A permanent alternative to dentures! Restore your teeth and win back your life! We recommend using this guide to learn about the benefits of Dental Implants, the
A GUIDE TO THE BENEFIT OF DENTAL IMPLANTS A permanent alternative to dentures! Restore your teeth and win back your life! We recommend using this guide to learn about the benefits of Dental Implants, the
Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT
 Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT About Implants 01. What if a tooth is lost and the toothless area is left alone? 02. Do you want to restore the confidence in your appearance? 03.
Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT About Implants 01. What if a tooth is lost and the toothless area is left alone? 02. Do you want to restore the confidence in your appearance? 03.
Vitamins and Minerals
 Eating Right Vitamins and Minerals Many claims about vitamins and minerals may be misleading and confusing. The following lists tell what vitamins and minerals do, where they are found and the current
Eating Right Vitamins and Minerals Many claims about vitamins and minerals may be misleading and confusing. The following lists tell what vitamins and minerals do, where they are found and the current
Arrangement of the artificial teeth:
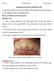 Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Oral rehabilitation of patient with access-post retained overdenture denture.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 10 Ver. 3 (October. 2018), PP 08-13 www.iosrjournals.org Oral rehabilitation of patient with
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 10 Ver. 3 (October. 2018), PP 08-13 www.iosrjournals.org Oral rehabilitation of patient with
أ.م. هدى عباس عبد اهلل CROWN AND BRIDGE جامعة تكريت كلية. Lec. (2) طب االسنان
 Lec. (2) CROWN AND BRIDGE أ.م. هدى عباس عبد اهلل Patient selection and examination A thorough diagnosis must first be made of the patient's dental condition, considering both hard and soft tissues. this
Lec. (2) CROWN AND BRIDGE أ.م. هدى عباس عبد اهلل Patient selection and examination A thorough diagnosis must first be made of the patient's dental condition, considering both hard and soft tissues. this
Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers
 Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Saudi Journal of Oral and Dental Research. DOI: /sjodr. ISSN (Print) Dubai, United Arab Emirates Website:
 DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
Denture Sufferers Guide Provided By The Dental Spa at Garden City. Cary Ganz DDS 300 Garden City Plaza Garden City NY 11530
 Denture Sufferers Guide Provided By The Dental Spa at Garden City Cary Ganz DDS 300 Garden City Plaza Garden City NY 11530 Tel. 516 741-1230 Fax 516 741-2257 http://www.cosmeticdentistrylongisland.net
Denture Sufferers Guide Provided By The Dental Spa at Garden City Cary Ganz DDS 300 Garden City Plaza Garden City NY 11530 Tel. 516 741-1230 Fax 516 741-2257 http://www.cosmeticdentistrylongisland.net
NUTRITION CONCEPTS MACRONUTRIENTS FAT SOLUBLE VITAMINS
 NUTRITION CONCEPTS MACRONUTRIENTS Carbohydrates Found in breads, cereals, fruits, vegetables, sugar and potatoes. good source of energy fiber in fruits and vegetables aid in eliminating wastes from the
NUTRITION CONCEPTS MACRONUTRIENTS Carbohydrates Found in breads, cereals, fruits, vegetables, sugar and potatoes. good source of energy fiber in fruits and vegetables aid in eliminating wastes from the
Parkinson s Disease. Diagnostic Symptoms
 Parkinson s Disease What is Parkinson s disease? Parkinson s disease (PD) is a progressive disease that affects an individual s movement and motor skills. It is progressive in that symptoms of the disease
Parkinson s Disease What is Parkinson s disease? Parkinson s disease (PD) is a progressive disease that affects an individual s movement and motor skills. It is progressive in that symptoms of the disease
Construction of Removable Partial Denture
 Construction of Removable Partial Denture Peter Hermann Department of Prosthodontics Semmelweis University Treatment options for edentulous spaces Fixed prosthodontics (crowns/bridges) Removable prosthodontics
Construction of Removable Partial Denture Peter Hermann Department of Prosthodontics Semmelweis University Treatment options for edentulous spaces Fixed prosthodontics (crowns/bridges) Removable prosthodontics
Full mouth occlusal rehabilitation; by Pankey Mann Schuyler philosophy
 Case Report DOI: 10.18231/2455-8486.2017.0006 Jinsa P. Devassy 1, Ankitha Sivadas 2, Shabas Muhammed 3 1 Consultant Prosthodontist, Ernakulam, Kerala, 2 Assistant Professor, 3 PG Student, Dept. of Prosthodontics,
Case Report DOI: 10.18231/2455-8486.2017.0006 Jinsa P. Devassy 1, Ankitha Sivadas 2, Shabas Muhammed 3 1 Consultant Prosthodontist, Ernakulam, Kerala, 2 Assistant Professor, 3 PG Student, Dept. of Prosthodontics,
CLASSIFICATION OF RPDs AND PARTIALLY EDENTULOUS ARCHES
 د.حكمت جميل Lec: 2 Prosthodontic CLASSIFICATION OF RPDs AND PARTIALLY EDENTULOUS ARCHES The classification of RPDs and partially edentulous arches simplifies communication and discussions. Requirements
د.حكمت جميل Lec: 2 Prosthodontic CLASSIFICATION OF RPDs AND PARTIALLY EDENTULOUS ARCHES The classification of RPDs and partially edentulous arches simplifies communication and discussions. Requirements
Telescopic Overdenture: A Case Report
 INTERNATIONAL JOURNAL of BIOMEDICAL SCIENCE CASE REPORT Telescopic Overdenture: A Case Report C. S. Shruthi 1, R. Poojya 2, Swati Ram 3, Anupama 4 1 Professor, Department of Prosthodontics, M R Ambedkar
INTERNATIONAL JOURNAL of BIOMEDICAL SCIENCE CASE REPORT Telescopic Overdenture: A Case Report C. S. Shruthi 1, R. Poojya 2, Swati Ram 3, Anupama 4 1 Professor, Department of Prosthodontics, M R Ambedkar
Safety and esthetics with
 Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
More than a beautiful smile. A new quality of life with dental implants.
 More than a beautiful smile. A new quality of life with dental implants. Why tooth loss matters Think of tooth loss and the first thing that comes to mind may be an unattractive appearance. It s true that
More than a beautiful smile. A new quality of life with dental implants. Why tooth loss matters Think of tooth loss and the first thing that comes to mind may be an unattractive appearance. It s true that
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Basic Review of Digestion
 Basic Review of Digestion In the mouth, food is broken down, mixed with saliva, and formed into a bolus. Wave like muscle movements, called peristalsis, push the food throughout the rest of the digestive
Basic Review of Digestion In the mouth, food is broken down, mixed with saliva, and formed into a bolus. Wave like muscle movements, called peristalsis, push the food throughout the rest of the digestive
Physiological Role: B-vitamins are coenzymes of many enzymes systems of body metabolism. Thiamine {B 1 }
 Food Constituents [continued] Micronutrients B-Vitamins The B group of vitamin {water soluble} includes: Thiamine: vitamin B 1, ant beriberi vitamin. Riboflavin: vitamin B 2. Niacin: nicotinic acid, PP
Food Constituents [continued] Micronutrients B-Vitamins The B group of vitamin {water soluble} includes: Thiamine: vitamin B 1, ant beriberi vitamin. Riboflavin: vitamin B 2. Niacin: nicotinic acid, PP
Nutrients are: water carbohydrates lipids proteins. minerals vitamins fiber
 Nutrients are: water carbohydrates lipids proteins minerals vitamins fiber WATER Essential nutrient 55-65% body weight Body loses water through evaporation, excretion, and respiration The only nutrient
Nutrients are: water carbohydrates lipids proteins minerals vitamins fiber WATER Essential nutrient 55-65% body weight Body loses water through evaporation, excretion, and respiration The only nutrient
Prosthetic RehabilitationofaPatientwithAlzheimersDiseaseusingaCombinedBallBarandClipRetainedImplantSupportedOverdentureA Case Report
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
VIRGINIA COOPERATIVE EXTENSION SERVICE
 VIRGINIA COOPERATIVE EXTENSION SERVICE VIRGINDl 'IECH VIRGINDl S'Dtt.E Blacksburg, Virginia 24061 Publication 348-337 August 1984 Lesson 3 Diet, Exercise, and Behavior Modification (Weight Control by Mail)
VIRGINIA COOPERATIVE EXTENSION SERVICE VIRGINDl 'IECH VIRGINDl S'Dtt.E Blacksburg, Virginia 24061 Publication 348-337 August 1984 Lesson 3 Diet, Exercise, and Behavior Modification (Weight Control by Mail)
Multivitamins are a mixture of vitamins and minerals which are essential for the body to work and stay healthy.
 MULTIVITAMINS Multivitamins are a mixture of vitamins and minerals which are essential for the body to work and stay healthy. Vitamins are vital substances that are required for normal growth and functioning
MULTIVITAMINS Multivitamins are a mixture of vitamins and minerals which are essential for the body to work and stay healthy. Vitamins are vital substances that are required for normal growth and functioning
The CMC approved a motion to accept all editorial action requests that remain on the consent calendar 21 Yea / 0 Nay / 0 Abstain
 PAGE 1 OF 14 Editorial Actions One or more member organizations requested that the following editorial action submissions be removed from the consent calendar and addressed individually: #s 4, 7, 8, 9,
PAGE 1 OF 14 Editorial Actions One or more member organizations requested that the following editorial action submissions be removed from the consent calendar and addressed individually: #s 4, 7, 8, 9,
Vitamins Minerals Chapter 12
 DH 250 Water soluble B1 Thiamin B2 Riboflavin B3 Niacin Vitamins Minerals Chapter 12 Role RDA Source Deficiency Toxicity Clinical Use intermediary coenzymes 1.2mg 1.1mg 1.2mg 1.1mg 16mg 14mg dairy B6 Pyridoxine
DH 250 Water soluble B1 Thiamin B2 Riboflavin B3 Niacin Vitamins Minerals Chapter 12 Role RDA Source Deficiency Toxicity Clinical Use intermediary coenzymes 1.2mg 1.1mg 1.2mg 1.1mg 16mg 14mg dairy B6 Pyridoxine
NUTRITION IN CHILDHOOD
 NUTRITION IN CHILDHOOD Nutrient requirement Children growing & developing need more nutritious food May be at risk for malnutrition if : - poor appetite for a long period - eat a limited number of food
NUTRITION IN CHILDHOOD Nutrient requirement Children growing & developing need more nutritious food May be at risk for malnutrition if : - poor appetite for a long period - eat a limited number of food
A PERIO-PROSTHETIC. with the BIO-GLASS. DR. Mirko Paoli (DDS) DT. Roberto Fabris ABUTMENT SYSTEM
 A PERIO-PROSTHETIC with the TREATMENT use of ABUTMENT SYSTEM BIO-GLASS DR. Mirko Paoli (DDS) DT. Roberto Fabris 110 SUMMER 2015 The implant therapy in dentistry has allowed the modification of prosthetic
A PERIO-PROSTHETIC with the TREATMENT use of ABUTMENT SYSTEM BIO-GLASS DR. Mirko Paoli (DDS) DT. Roberto Fabris 110 SUMMER 2015 The implant therapy in dentistry has allowed the modification of prosthetic
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
KEY INDICATORS OF NUTRITION RISK
 NUTRITION TOOLS KEY INDICATORS OF Consumes fewer than 2 servings of fruit or fruit juice per day. Consumes fewer than 3 servings of vegetables per day. Food Choices Fruits and vegetables provide dietary
NUTRITION TOOLS KEY INDICATORS OF Consumes fewer than 2 servings of fruit or fruit juice per day. Consumes fewer than 3 servings of vegetables per day. Food Choices Fruits and vegetables provide dietary
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Locator retained mandibular complete prosthesis (isy Implant System)
 Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
Cast Partial Denture Improving Emergence and Masticatory Function - A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VI (Sep. 2015), PP 51-56 www.iosrjournals.org Cast Partial Denture Improving Emergence
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. VI (Sep. 2015), PP 51-56 www.iosrjournals.org Cast Partial Denture Improving Emergence
Selection and arrangement of teeth in rpd
 Selection and arrangement of teeth in rpd upon completion of the articulator mounting and a thorough assessment of the occlusal requirements, the practitioner should be able to perform the proper arrangement
Selection and arrangement of teeth in rpd upon completion of the articulator mounting and a thorough assessment of the occlusal requirements, the practitioner should be able to perform the proper arrangement
Restoration of the worn dentition
 Clin Dent Rev (2017) 1:4 https://doi.org/10.1007/s41894-017-0003-3 TREATMENT Restoration of the worn dentition Paul King 1 Received: 16 March 2017 / Accepted: 31 May 2017 / Published online: 30 June 2017
Clin Dent Rev (2017) 1:4 https://doi.org/10.1007/s41894-017-0003-3 TREATMENT Restoration of the worn dentition Paul King 1 Received: 16 March 2017 / Accepted: 31 May 2017 / Published online: 30 June 2017
2002 Learning Zone Express
 1 Nutrients The food you eat is a source of nutrients. Nutrients are defined as the substances found in food that keep your body functioning. Your body needs nutrients to 2 Fuel your energy. Help you grow.
1 Nutrients The food you eat is a source of nutrients. Nutrients are defined as the substances found in food that keep your body functioning. Your body needs nutrients to 2 Fuel your energy. Help you grow.
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Surveying. 3rd year / College of Dentistry/University of Baghdad ( ) Page 1
 د. فائزة Lec.3 Prosthodontics Surveying The ideal requirements for successful removable partial denture are: 1. Be easily inserted and removed by the patient. 2. Resist dislodging forces. 3. It should
د. فائزة Lec.3 Prosthodontics Surveying The ideal requirements for successful removable partial denture are: 1. Be easily inserted and removed by the patient. 2. Resist dislodging forces. 3. It should
Chapter 12. Prosthodontics
 Chapter 12 Prosthodontics Golbarg Kolahi 1 Prosthesis [prahs-thee-sis] A replacement for a missing body part Golbarg Kolahi 2 Prosthesis In the dental field, it is a fixed or removable appliance replacing
Chapter 12 Prosthodontics Golbarg Kolahi 1 Prosthesis [prahs-thee-sis] A replacement for a missing body part Golbarg Kolahi 2 Prosthesis In the dental field, it is a fixed or removable appliance replacing
INDIAN DENTAL JOURNAL
 ATTACHMENT RETAINED CAST PARTIAL DENTURE USING RHEIN 83 OT-CAP Dr. Charu Gupta 1 Dr. Harshul Sharma 2 Dr. Merrily Nongsiej 3 Dr. AbhinavShekhar 4 1 Senior Resident, Department of Prosthodontics, King George
ATTACHMENT RETAINED CAST PARTIAL DENTURE USING RHEIN 83 OT-CAP Dr. Charu Gupta 1 Dr. Harshul Sharma 2 Dr. Merrily Nongsiej 3 Dr. AbhinavShekhar 4 1 Senior Resident, Department of Prosthodontics, King George
Jaw relation registration in RPD
 Jaw relation registration in RPD Why to Record the Jaw Relations? To establish and maintain a harmonious relationship with all oral structures and to provide a masticatory apparatus that is efficient and
Jaw relation registration in RPD Why to Record the Jaw Relations? To establish and maintain a harmonious relationship with all oral structures and to provide a masticatory apparatus that is efficient and
Denture Troubleshooting Guide
 Denture Troubleshooting Guide Technical bulletin from National Dentex Comfort Sore spot in vestibule upper or lower denture Sore spot in upper post dam. (posterior limit of upper) Single sore spots on
Denture Troubleshooting Guide Technical bulletin from National Dentex Comfort Sore spot in vestibule upper or lower denture Sore spot in upper post dam. (posterior limit of upper) Single sore spots on
JIGSAW READING CARBOHYDRATES
 Date: CARBOHYDRATES Carbohydrates provide an important source of energy for our bodies. There are two types of carbohydrates: Sugars are found in foods which taste sweet like candies, jams and desserts.
Date: CARBOHYDRATES Carbohydrates provide an important source of energy for our bodies. There are two types of carbohydrates: Sugars are found in foods which taste sweet like candies, jams and desserts.
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Immediate fixed teeth a treatment concept for edentulous patients
 52 Maxillary rehabilitation using the All-on-4 concept Immediate fixed teeth a treatment concept for edentulous patients DR DUSAN VASILJEVIC AND VLADAN VASILJEVIC, FRIEDEBURG, GERMANY The number of edentulous
52 Maxillary rehabilitation using the All-on-4 concept Immediate fixed teeth a treatment concept for edentulous patients DR DUSAN VASILJEVIC AND VLADAN VASILJEVIC, FRIEDEBURG, GERMANY The number of edentulous
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
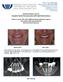 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
An Introduction to Dental Implants
 An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
Vertical relation: It is the amount of separation between the maxilla and
 Vertical relations Vertical relation: It is the amount of separation between the maxilla and the mandible in a frontal plane. Vertical dimension: It is the distance between two selected points, one on
Vertical relations Vertical relation: It is the amount of separation between the maxilla and the mandible in a frontal plane. Vertical dimension: It is the distance between two selected points, one on
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Fixed Partial Dentures /FPDs/, Implant Supported. in implant prosthodontics
 Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Eat Well, Live Well Nutritional Guidelines for those 50+ April 10, 2014 Laura Vandervet, Registered Dietitian
 Eat Well, Live Well Nutritional Guidelines for those 50+ April 10, 2014 Laura Vandervet, Registered Dietitian Outline Benefits of healthy eating Meeting your nutritional requirements Using Canada s Food
Eat Well, Live Well Nutritional Guidelines for those 50+ April 10, 2014 Laura Vandervet, Registered Dietitian Outline Benefits of healthy eating Meeting your nutritional requirements Using Canada s Food
