Chapter 2 Variants of Normal and Common Benign Conditions
|
|
|
- Aileen Stevenson
- 5 years ago
- Views:
Transcription
1 Chapter 2 Variants of Normal and Common Benign Conditions Summary Fundamental to diagnosing oral pathologic conditions is the ability to recognize the spectrum of clinical findings that represents variation of normal within the population. The range of such variation is wide and findings can be very subtle or notably prominent. Some are purely developmental, while others have a clear inflammatory or traumatic etiology. This chapter describes the most commonly encountered variations of normal and benign conditions encountered in the oral cavity, with specific guidelines for diagnosis and management, when clinically indicated. Keywords Melanocytes Melanin Physiologic pigmentation Melanotic macule Melanoma Fordyce granule Sebaceous gland Gingival graft Free gingival graft Lingual tonsil Tonsil Fissured tongue Geographic tongue Benign migratory glossitis Stomatitis erythema migrans Erythema migrans Median rhomboid glossitis Fibroma Irritation fibroma Traumatic fibroma Inflammatory papillary hyperplasia Epulis fissuratum Torus Mandibular torus, Maxillary torus Exostosis Ankyloglossia Frenula 2.1 Introduction Fundamental to diagnosing oral pathologic conditions is the ability to recognize the spectrum of clinical findings that represents variation of normal within the population. The range of such variation is wide and findings can be very subtle or notably prominent. Some are purely developmental, while others have a clear inflammatory or traumatic etiology. These conditions, in large part, do not require therapy unless specifically noted in the text. 2.2 Physiologic Pigmentation Melanocytes are a normal component of the basal cell layer of the oral epithelium. They cause varying degrees of mucosal pigmentation, ranging from light brown to black, due to the production of melanin. Physiologic pigmentation is observed much more frequently in darker skinned individuals, however, even those with very fair complexions may demonstrate characteristic findings. Focal, freckle-like melanotic macules are very common (Fig. 2.1; see Chap. 6). The keratinized mucosa, in particular the gingiva, is most commonly affected (Fig. 2.2). Pigmentation is due to deposition of melanin into the connective tissue without an increase in the number or size of melanocytes, and lesions are therefore flat. This may become more pronounced in areas of chronic trauma or inflammation, such as along the occlusal bite line of the buccal mucosa (Fig. 2.3). In most cases, the diagnosis can be made clinically but occasionally a biopsy is warranted to rule out melanoma; particularly if any changes are noted in size, shape, or degree of pigmentation, or if a flat lesion becomes raised. Intraoral melanoma, however, is exceedingly rare, representing less than 1% of all melanomas. Other causes of pigmentation, including both intrinsic and extrinsic etiologies, are discussed in Chap. 6. Biopsy: No, with rare exception. Follow-up: Annual. J.M. Bruch and N.S. Treister, Clinical Oral Medicine and Pathology, DOI / _2, Humana Press, a Part of Science + Business Media, LLC
2 18 Clinical Oral Medicine and Pathology 2.3 Fordyce Granules Sebaceous glands, which are a normal feature of facial skin, can often be identified within the buccal mucosa due to the proximity of skin to the oral mucosa in this area. These are less commonly noted on the lip or the labial mucosa (Figs. 2.4 and 2.5). Fordyce granules appear white to yellow in color, are generally present in clusters, may be slightly raised, and are asymptomatic. Sebaceous glands in the oral mucosa are nonfunctional. Occasionally patients become aware of Fig. 2.1 Melanotic macule of the lower lip with dark brown pigmentation and sharply defined borders. The lips are slightly chapped. Fig. 2.2 Physiologic pigmentation in an African-American child. The interdental papillae are affected to a variable degree; the nonkeratinized mucosa is entirely unaffected. Fig. 2.4 Prominent Fordyce granules in the right buccal mucosa. Fig. 2.3 Postinflammatory pigmentation of the right buccal mucosa secondary to chronic cheek biting. Fig. 2.5 Dense concentration of Fordyce granules in the left buccal mucosa.
3 2.6 Fissured Tongue 19 their presence by detecting the raised surfaces with their tongue, or during self-examination with a mirror. Diagnostic tests: None; clinical appearance is usually classic and sufficient for diagnosis. Biopsy: No. 2.4 Gingival Grafts In cases of severe gingival recession, gingival grafting is performed as a periodontal surgical procedure to restore the attached soft tissue, reduce root-surface sensitivity, and prevent further tissue loss. The donor tissue, which is harvested from the patient s palate as an autograft, has a distinct appearance that is typically raised and more pale than the adjacent gingiva. Grafts are generally easily recognized, very sharply defined, and should not be mistaken for pathology (Fig. 2.6). If there is any doubt, the patient should be able to provide suitable history regarding whether such a procedure was performed. Biopsy: No. 2.5 Lingual Tonsil Lymphoid tissue is often found along the posterior lateral tongue, forming part of Waldeyer ring. The clinical presentation ranges from imperceptible to strikingly prominent. Lingual tonsils appear as exophytic mucosal colored masses that may exhibit folds and crypts as seen in the palatine tonsils. As with any lymphoid tissue, these can become enlarged and tender secondary to inflammation. It is generally under these circumstances that patients or physicians become aware of their presence. Unilateral or asymmetrically enlarged tissue should be considered for biopsy to rule out other pathology such as lymphoma or squamous cell carcinoma. Biopsy: No, unless unilateral or otherwise suspicious. 2.6 Fissured Tongue Fig. 2.6 Free gingival graft covering a prominent exostosis in an area of previous gingival recession. Note the thicker, more clearly defined keratinized mucosa compared to the adjacent nonkeratinized tissue. There is remarkable variation in the appearance of the tongue throughout the population. One common finding is the presence of fissures and grooves along the dorsal surface. These can range from shallowappearing cracks to deep, penetrating fissures (Fig. 2.7). These features may be associated with geographic tongue (see below) and may rarely predispose to recurrent candidiasis (see Chap. 7). Most patients are universally asymptomatic; it is not uncommon for a patient to examine his or her tongue and become aware of fissuring following the onset of otherwise unrelated symptoms, such as burning mouth syndrome (see Chap. 10).
4 20 Clinical Oral Medicine and Pathology Fig. 2.8 Benign migratory glossitis in a child. There is a very well-defined area of depapillation on the right side of the tongue dorsum, while the rest of the surface is unaffected. Fig. 2.7 Fissured tongue with extensive grooves and fissures over the entire dorsal surface. Biopsy: No. Fig. 2.9 Benign migratory glossitis of the ventral tongue and floor of mouth. As this region of the tongue does not normally contain papillae, only the white rimmed borders are noted. 2.7 Geographic Tongue Also referred to as benign migratory glossitis, geographic tongue is a common inflammatory condition of the tongue. Other oral mucosal sites can be affected less frequently, in which case the condition is called stomatitis erythema migrans or ectopic geographic tongue. Geographic tongue is usually evident in early childhood and rarely causes symptoms. The lesions demonstrate a wide variety of clinical patterns, ranging from irregularly shaped erythematous macules with surrounding elevated white borders to patchy areas of depapillation and smooth glossy mucosa (Figs ). These fea- Fig Extensive benign migratory glossitis affecting the entire tongue dorsum with prominent areas of depapillation surrounded by white rimmed borders.
5 2.8 Median Rhomboid Glossitis 21 Fig Stomatitis erythema migrans showing subtle circular lesions with white borders of the right buccal mucosa and concurrent changes consistent with benign migratory glossitis. Fig Median rhomboid glossitis with a well-defined depapillated patch in the posterior midline of the tongue dorsum with normal surrounding tissue. tures can give the tongue a map-like appearance, thus the descriptive term geographic. In an affected individual, the presentation can change on a daily basis and therefore appear migratory. Although the clinical presentation can be striking, there are few if any other conditions that mimic geographic tongue (these include oral lichen planus, erythematous candidiasis, and leukoplakia), and with a good history and examination lesions rarely warrant biopsy. Albeit rare, patients may describe sensitivity of the tongue to otherwise normally tolerated food and beverages. This may or may not correlate with the extent of lesions noted clinically. Management with topical therapies may be effective in such cases. Importantly, other causes of tongue sensitivity must be considered, such as candidiasis or immune-mediated conditions, especially when there is recent or abrupt onset of symptoms. Diagnostic tests: None; diagnosis is based on clinical appearance. Biopsy: No, except very atypical presentations. Treatment: None in most cases. When symptomatic, rinses containing topical dexamethasone or diphenhydramine may be effective in reducing symptoms. Be sure to consider other causes of tongue discomfort, such as burning mouth syndrome (see Chap. 10). 2.8 Median Rhomboid Glossitis This is a poorly understood condition that affects the tongue dorsum. It is characterized by a chronic, atrophic, erythematous, depapillated patch in the posterior midline of the tongue dorsum typically measuring between 0.25 and 2.0 cm in diameter (Fig. 2.12). While there is great variation in clinical presentation among patients, the size and quality of the lesion do not tend to change significantly over time in a given individual. While many cases are never symptomatic, mild discomfort may develop specifically in the area of atrophic change. If so, symptoms tend to come and go and rarely persist for long. Because tissue biopsy often demonstrates superficial candidal colonization and an inflammatory infiltrate in the underlying connective tissue, there is some thought that median rhomboid glossitis is mediated by chronic candidal colonization. The tissue may be particularly susceptible to recurrent fungal infection due to the reduced thickness of the epithelium. Therefore, when a patient develops symptoms of tongue discomfort in the presence of median rhomboid glossitis, first-line treatment consists of topical or systemic antifungal therapy. If symptoms persist following an appropriate course of antifungal therapy, topical corticosteroid therapy should be instituted. If this is also ineffective and all other potential etiologies have been excluded, the discomfort should be managed as a neuropathic pain disorder (see Chap. 10).
6 22 Clinical Oral Medicine and Pathology Diagnostic tests: None routinely. A positive fungal culture or cytological smear may or may not represent a true infection (see Chap. 3). This may be clinically useful to determine baseline status prior to initiating antifungal therapy. Biopsy: No, except for atypical presentations. Treatment: None in most cases. When symptomatic, initial therapy should consist of a 1-week course of either clotrimazole troches or fluconazole. Be sure to consider other causes of tongue discomfort, such as geographic tongue or burning mouth syndrome. If there is no improvement following 1 week of antifungal therapy, treatment with high potency topical corticosteroid gels (fluocinonide 0.05% or clobetasol 0.05%), two to three times daily, should be initiated. If this is also ineffective, consider treating as a neuropathic condition (see Chap. 10). Follow-up: None if asymptomatic, otherwise patients should be re-evaluated after 1 week of antifungal therapy. and location, lesions may simply be an annoyance, or they may become quite uncomfortable due to repetitive trauma. Lesions may progressively enlarge with recurrent injury, thereby compounding the clinical situation. In such cases the surface mucosa often becomes ulcerated, characterized by a yellowish white pseudomembrane (Fig. 2.15). Treatment is surgical excision, after which lesions rarely recur. Histopathological examination demonstrates a dense collection of fibrous tissue with normal surface epithelium. Fibromas have no malignant potential; however, they should be excised and submitted for histopathological analysis if the clinical diagnosis is uncertain. 2.9 Fibroma Fibromas are probably the most commonly encountered oral soft tissue lesions. Frequently used terms include irritation fibroma and traumatic fibroma, indicating the underlying reactive etiology. These are initiated by trauma, typically a bite injury (that the patient may not recall) or secondary to friction from the sharp edge of a tooth or dental restoration. Fibromas present clinically as round or ovoid, firm, exophytic, smooth-surfaced masses that are the same color as, or slightly lighter than, the surrounding mucosa (Fig. 2.13). Lesions range in size from several millimeters to 1.0 cm in diameter (Fig. 2.14). Larger lesions are exceedingly rare and biopsy should be considered in such cases to rule out a neoplasm. As these are often caused by bite trauma, the most commonly involved areas are along the bite plane of the buccal mucosa and lateral tongue, although the lower labial mucosa and tongue dorsum can also be affected. There are no specific risk factors other than a history of minor trauma. Fibromas are generally asymptomatic and do not require treatment unless they are particularly bothersome to the patient. Depending on the size Fig Fibroma of the anterior tongue tip secondary to bite trauma. The lesion is well-defined and has a smooth, raised surface in comparison to the adjacent tissue; it is firm and nontender. Fig Large fibroma of the right buccal mucosa. The surface mucosa is thicker in appearance than the surrounding tissue.
7 2.10 Inflammatory Papillary Hyperplasia 23 Fig Fibroma of the left buccal mucosa with focal ulceration secondary to repetitive bite injury. Biopsy: Only if the appearance is suspicious. Treatment: None if asymptomatic; otherwise complete surgical excision. Fig Fibrous hyperplasia of the mandibular mucosa secondary to a poorly fitting denture. Note the folds of dense fibrous tissue in the anterior floor of mouth (epulis fissuratum) Inflammatory Papillary Hyperplasia This is a benign reactive condition that develops on denture-bearing mucosa. This includes the maxillary and mandibular alveolar mucosa, the hard palate, and the vestibular mucosa. It only affects denture wearers and not patients who wear other removable oral appliances. Inflammatory papillary hyperplasia can affect a very limited area of mucosa or be quite extensive, in some cases involving the entire hard palate. A focal lesion with a distinct wrinkled or folded appearance is often termed epulis fissuratum, and is most commonly encountered in the anterior buccal vestibule at the edge of a denture flange (Fig. 2.16). Lesions are characterized by pebbly, papillary changes that are variably associated with tissue hyperplasia, and verrucous-like changes that can be quite notable (Fig. 2.17). This condition is rarely symptomatic, however, patients are typically aware of its presence. Depending on the location and extent of tissue hyperplasia, lesions may be susceptible to secondary trauma or interfere with prosthesis fit and function (Fig. 2.18). Fig Inflammatory papillary hyperplasia in a patient with a full upper denture. A punch biopsy was obtained to rule out malignancy. As the lesion was asymptomatic and the denture was otherwise comfortable, no further treatment was necessary. Fig Ulcerated epulis fissuratum due to a poorly fitting removable partial denture.
8 24 Clinical Oral Medicine and Pathology The etiology of inflammatory papillary hyperplasia is poorly understood. It is thought that chronic irritation due to a loose or poorly fitting denture, or inadequate denture hygiene (with candida colonizing the denture material), contributes to localized inflammatory-mediated reactive changes in the mucosa. As lesions may mimic other pathologic conditions, including proliferative verrucous leukoplakia and squamous cell carcinoma (see Chap. 9), biopsy may be necessary to rule out dysplasia or malignancy. Histopathological findings include benign papillary acanthosis (increased epithelial thickness) that is commonly associated with a chronic inflammatory infiltrate in the underlying connective tissue. The first step in treatment is careful evaluation of the prosthesis. The extension of the denture borders into the vestibule as well as overall stability should be examined closely by an appropriate specialist. Recommendation should be made to soak the prosthesis overnight in an over the counter denture disinfectant solution or prescription chlorhexidine gluconate 0.12%. Another simple and inexpensive option for nonmetal containing prostheses is use of a 1:10 dilution of sodium hypochlorite, or common household bleach. Even in the absence of obvious oral fungal infection, a 1 2- week course of fluconazole 100 mg once daily, in addition to daily denture hygiene, is reasonable empiric therapy. During this time, the prosthesis should be left out of the mouth as much as possible to avoid exacerbation of the lesion. Surgical excision is indicated for lesions that fail to respond to conservative therapy and are bothersome or interfere with function (Fig. 2.19). Biopsy: Yes, to rule out malignancy if the clinical appearance is suspicious. Treatment: Prosthesis should be evaluated for fit, stability, and hygiene and adjusted or otherwise managed appropriately. Hyperplastic tissue can be surgically excised or laser ablated if bothersome or otherwise symptomatic. Patients should be instructed to maintain good denture hygiene and return to their dentist for regular follow-up Tori and Exostoses These are benign, developmental bony growths that are commonly observed in the oral cavity. Tori are more common and are specific to the midline hard palate and anterolateral lingual mandible. Similar lesions involving the buccal aspect of the maxilla or mandible are called exostoses. These areas are covered by keratinized or nonkeratinized mucosa, depending on the anatomic location, and can be mistaken for mucosal growths. Changes are not typically evident until the second decade, and while highly variable, growth is generally very slow throughout life. Even when lesions become quite extensive, patients may be unaware of their presence due to the gradual incremental growth pattern over decades. Maxillary tori occur in the midline of the hard palate and range from barely discernable dome-shaped smooth swellings to large multilobulated masses (Figs ). Mandibular tori develop most commonly along Fig Areas of fibrous tissue shown in Fig were excised and submitted for histopathology in preparation for fabricating a new set of complete dentures. Fig Maxillary torus with smooth surface and well-defined borders in the midline of the hard palate.
9 2.12 Ankyloglossia and Prominent Frenula the lingual aspect of the mandible inferior to the premolars bilaterally. Mandibular tori also exhibit a wide range of presentations; however, lesions usually demonstrate two to three well-defined smooth lobules (Fig. 2.23). Exostoses appear clinically identical to mandibular tori on the buccal surface of the mandible or maxilla (Fig. 2.6). These can grow to be quite large yet rarely have any discernable effect on the external facial appearance. On intraoral periapical dental radiographs, the involved areas appear as dense radiopacities within the maxilla and mandible (Fig. 2.24). Tori and exostoses generally do not require any treatment. The covering mucosa may occasionally become irritated or ulcerated secondary to trauma, which is managed symptomatically. If denture fabrication is required, tori can be surgically removed to maximize retention of the prosthesis and minimize the risk of pressure-induced trauma. Fig Mandibular tori in the premolar region with multiple lobules. 25 Fig Radiographic appearance of a maxillary torus as a well-defined radiopacity. Fig Maxillary torus with a stalk-like attachment to the underlying palatal bone. Biopsy: No Ankyloglossia and Prominent Frenula Fig Multilobulated maxillary torus showing slight asymmetry. Abnormal prominence of frenula (tissue attachments of the anterior tongue and labial mucosa), can result in a variety of complications. In the case of the lingual frenulum, this can lead to problems with speech development or infant feeding, and is referred to ankyloglossia or tongue tie. Localized periodontal recession on the lingual aspect of the central incisors can also occur. A prominent labial mandibular frenulum can
10 26 Clinical Oral Medicine and Pathology Fig Thick maxillary frenulum in a 5-year-old before (a) and after (b) surgical repositioning. similarly affect the facial aspect of the same teeth. High insertion of the maxillary frenulum onto the gingiva may lead to formation of a gap, or diastema, between the central incisors (Fig. 2.25). These conditions are typically identified in young children by their dentist or pediatrician. If indicated, treatment is simple surgical repositioning or excision. Biopsy: No. Treatment: Referral to an oral surgeon that specializes in pediatrics for surgical evaluation. Sources Antoniades DZ, Belazi M, Papanayiotou P. Concurrence of torus palatines with palatal and buccal exostoses: case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998;85:552 7 Assimakopoulos D, Patrikakos C, Fotika C, et al. Benign migratory glossitis or geographic tongue: an enigmatic oral lesion. Am J Med 2002;15:751 5 Rogers RS, Bruce AJ. The tongue in clinical diagnosis. J Eur Acad Dermatol Venereol 2004;18:254 9 Canaan TJ, Meehan SC. Variations of structure and appearance of the oral mucosa. Dent Clin North Am 2005;49:1 14 Carter LC. Median rhomboid glossitis: review of a puzzling entity. Compendium 1990;11:446, Cicek Y, Ertas U. The normal and pathological pigmentation of oral mucous membrane: a review. J Contemp Dent Pract 2003;15:76 86 Infante-Cossio P, Martinez-de-Fuentes R, et al. Inflammatory papillary hyperplasia of the palate: treatment with carbon dioxide laser, followed by restoration with an implantsupported prosthesis. Br J Oral Maxillofac Surg 2006; 45: Jainkittivong A, Langlais R. Geographic tongue: clinical characteristics of 188 cases. J Contemp Dent Pract 2005;6: Segal LM, Stephenson R, Dawes M, et al. Prevalence, diagnosis, and treatment of ankyloglossia; methodologic review. Can Fam Physician 2007; 53:
11
Pharmacologyonline 2: (2008) Young Researchers Gavasova and Budev EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT. Dr G.Gavasova, Dr I.
 EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT Dr G.Gavasova, Dr I.Budev Medical University, Faculty of Dental Medicine Oral Surgery Department Head: Prof. Dr D. Atanasov, Ph.D, MD. Summary Continuous
EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT Dr G.Gavasova, Dr I.Budev Medical University, Faculty of Dental Medicine Oral Surgery Department Head: Prof. Dr D. Atanasov, Ph.D, MD. Summary Continuous
That. Name QUIZ. 60 SEPTEMBER 2017 // dentaltown.com
 QUIZ Name That General dentists are first in the line of practitioners that patients see for an oral lesion evaluation; therefore, a sound understanding of oral mucosal diseases and their clinical presentation
QUIZ Name That General dentists are first in the line of practitioners that patients see for an oral lesion evaluation; therefore, a sound understanding of oral mucosal diseases and their clinical presentation
Oral Health & HIV. Professor Sudeshni Naidoo Department of Community Dentistry University of the Western Cape
 Oral Health & HIV Professor Sudeshni Naidoo Department of Community Dentistry University of the Western Cape Importance & relevance of Oral HIV Lesions >70% of HIV+ve patients present with oral manifestations
Oral Health & HIV Professor Sudeshni Naidoo Department of Community Dentistry University of the Western Cape Importance & relevance of Oral HIV Lesions >70% of HIV+ve patients present with oral manifestations
Pre prosthetic surgery
 Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
Contents. 3 Diagnostic Tests and Studies Introduction Examination... 27
 Contents 1 Normal Anatomy... 1 1.1 Introduction... 1 1.2 Surface Landmarks... 1 1.3 Oral Mucosa... 3 1.4 Tongue... 5 1.5 Floor of Mouth... 6 1.6 Palate... 6 1.7 Dentition... 7 1.8 Temporomandibular Joint...
Contents 1 Normal Anatomy... 1 1.1 Introduction... 1 1.2 Surface Landmarks... 1 1.3 Oral Mucosa... 3 1.4 Tongue... 5 1.5 Floor of Mouth... 6 1.6 Palate... 6 1.7 Dentition... 7 1.8 Temporomandibular Joint...
Differential Diagnosis of Oral Lesions. An Interactive Lecture Using Audience Response Polling. John L. Alonge, MS, DDS
 Differential Diagnosis of Oral Lesions An Interactive Lecture Using Audience Response Polling John L. Alonge, MS, DDS Goals 1. Review the diagnostic process needed to formulate a differential diagnosis
Differential Diagnosis of Oral Lesions An Interactive Lecture Using Audience Response Polling John L. Alonge, MS, DDS Goals 1. Review the diagnostic process needed to formulate a differential diagnosis
Lesions & Lifestyles
 Lesions & Lifestyles attended a 3 hour Continuing Education Seminar on Oral Pathology presented by Nancy Dewhirst, RDH,BS on (date) at (location):. Course material is directly related patient care. Notes:
Lesions & Lifestyles attended a 3 hour Continuing Education Seminar on Oral Pathology presented by Nancy Dewhirst, RDH,BS on (date) at (location):. Course material is directly related patient care. Notes:
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
Contents. 1 Normal Anatomy Introduction... 17
 Contents 1 Normal Anatomy... 1 Introduction... 1 Surface Landmarks... 1 Oral Mucosa... 1 Tongue... 4 Floor of Mouth... 6 Palate... 7 Dentition... 7 Temporomandibular Joint... 9 Innervation... 10 Jaws and
Contents 1 Normal Anatomy... 1 Introduction... 1 Surface Landmarks... 1 Oral Mucosa... 1 Tongue... 4 Floor of Mouth... 6 Palate... 7 Dentition... 7 Temporomandibular Joint... 9 Innervation... 10 Jaws and
4Ps LUMPS AND BUMPS B.L.&T. BUMPS, LUMPS, AND TATTOOS. Most Common BUMP in the oral cavity Fibroma INTERDENTAL PAPILLAE LESIONS
 B.L.&T. BUMPS, LUMPS, AND TATTOOS LUMPS AND BUMPS DIFFERENTIAL DIAGNOSIS FOR LUMPS AND BUMPS Traumatic Fibroma Papilloma Epulis Fissuratum Inflammatory Papillary Hyperplasia Lesions of Attached Gingiva
B.L.&T. BUMPS, LUMPS, AND TATTOOS LUMPS AND BUMPS DIFFERENTIAL DIAGNOSIS FOR LUMPS AND BUMPS Traumatic Fibroma Papilloma Epulis Fissuratum Inflammatory Papillary Hyperplasia Lesions of Attached Gingiva
Differential Diagnosis of Oral Masses. Gingival Lesions
 Differential Diagnosis of Oral Masses Gingival Lesions Gingival/Alveolar Ridge Masses Parulis Periodontal Abscess Tori and Exostoses Reactive Proliferations Peripheral Odontogenic Cysts Peripheral Odontogenic
Differential Diagnosis of Oral Masses Gingival Lesions Gingival/Alveolar Ridge Masses Parulis Periodontal Abscess Tori and Exostoses Reactive Proliferations Peripheral Odontogenic Cysts Peripheral Odontogenic
Premalignant lesions may expose to a promoting. factor & may be induced to undergo malignant. Carcinoma in situ displays the cytologic features of
 بسم رلاهللا Def. Premalignant lesions may expose to a promoting factor & may be induced to undergo malignant transformation. Carcinoma in situ displays the cytologic features of malignancy without invasion
بسم رلاهللا Def. Premalignant lesions may expose to a promoting factor & may be induced to undergo malignant transformation. Carcinoma in situ displays the cytologic features of malignancy without invasion
Differential Diagnosis of Oral Ulcerations
 Differential Diagnosis of Oral Ulcerations Dr. Nagamani Narayana Department of Oral Biology University of Nebraska Medical Center College of Dentistry Objectives Differential diagnosis of oral ulcerations
Differential Diagnosis of Oral Ulcerations Dr. Nagamani Narayana Department of Oral Biology University of Nebraska Medical Center College of Dentistry Objectives Differential diagnosis of oral ulcerations
The Oral Cavity. Image source:
 The Oral Cavity Anatomy Image source: http://anatomyforlayla.blogspot.co.za/2007/04/blog-post.html The major structures of the oral cavity are the lips, the teeth, the alveolar ridges (bony areas that
The Oral Cavity Anatomy Image source: http://anatomyforlayla.blogspot.co.za/2007/04/blog-post.html The major structures of the oral cavity are the lips, the teeth, the alveolar ridges (bony areas that
Pigmented lesions of the Oral cavity
 Oral medicine أ.م.د احسان عبد هللا كميل Pigmented lesions of the Oral cavity Pigmented oral lesions are a large group of disorders in which the dark or brown color is the essential clinical characteristic.
Oral medicine أ.م.د احسان عبد هللا كميل Pigmented lesions of the Oral cavity Pigmented oral lesions are a large group of disorders in which the dark or brown color is the essential clinical characteristic.
LESIONS OF THE ORAL CAVITY ORAL CAVITY. Oral Cavity Subsites 4/10/2013 LIPS TEETH GINGIVA ORAL MUCOUS MEMBRANES PALATE TONGUE ORAL LYMPHOID TISSUES
 LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
Lips and labial mucosa
 Lips and labial mucosa External portion of the lips: the vermilion border and the skin Vermilion border : the exposed red portion of the lip, covered by mucous membrane, no mucous glands Boundary: the
Lips and labial mucosa External portion of the lips: the vermilion border and the skin Vermilion border : the exposed red portion of the lip, covered by mucous membrane, no mucous glands Boundary: the
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Diagnostic sieve. Looking Beyond the Vermillion Border. Time bombs for medical GPs! Normal oral mucosa
 Sat 12 June 2010 Millennium WS 28 + 38 2.00-2.55; 3.05-4.00 PM Looking Beyond the Vermillion Border Laurence J. Walsh BDSc, PhD, DDSc, FFOP(RCPA), GCEd, FICD, FPFA, FADI, FIADFE The University of Queensland
Sat 12 June 2010 Millennium WS 28 + 38 2.00-2.55; 3.05-4.00 PM Looking Beyond the Vermillion Border Laurence J. Walsh BDSc, PhD, DDSc, FFOP(RCPA), GCEd, FICD, FPFA, FADI, FIADFE The University of Queensland
Diagnosis. overt Examination. Definitive Examination. History. atient interview. Personal History. Clinical Examination.
 Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Diagnosis overt Examination History Definitive Examination atient interview Personal History Mental Attitude Medical History Dental History Clinical Examination Extra Oral Oral Radiographic Evaluation
Figure (2-6): Labial frenum and labial notch.
 The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
Case Report A Giant Cell Fibroma and Focal Fibrous Hyperplasia in a Young Child: A Case Report
 Hindawi Publishing Corporation Case Reports in Dentistry Volume 2012, Article ID 370242, 5 pages doi:10.1155/2012/370242 Case Report A Giant Cell Fibroma and Focal Fibrous Hyperplasia in a Young Child:
Hindawi Publishing Corporation Case Reports in Dentistry Volume 2012, Article ID 370242, 5 pages doi:10.1155/2012/370242 Case Report A Giant Cell Fibroma and Focal Fibrous Hyperplasia in a Young Child:
Index. Dent Clin N Am 49 (2005) Note: Page numbers of article titles are in boldface type.
 Dent Clin N Am 49 (2005) 273 278 Index Note: Page numbers of article titles are in boldface type. A Acanthosis nigricans, familial, 251 Amalgam tattoo, 197 198 Amphotericin B, 62 Ankyloglossia, 11 Anti-inflammatory
Dent Clin N Am 49 (2005) 273 278 Index Note: Page numbers of article titles are in boldface type. A Acanthosis nigricans, familial, 251 Amalgam tattoo, 197 198 Amphotericin B, 62 Ankyloglossia, 11 Anti-inflammatory
04/09/2018. Squamous Cell Neoplasia and Precursor Lesions. Agenda. Squamous Dysplasia. Squamo-proliferative lesions. Architectural features
 Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
DEVELOPING ANALOGUE/SUBTITUTE FOR THE MANDIBULAR DENTURE BEARING AREA. Dr Muhammad Rizwan Memon FCPS Assistant Professor
 DEVELOPING ANALOGUE/SUBTITUTE FOR THE MANDIBULAR DENTURE BEARING AREA Dr Muhammad Rizwan Memon FCPS Assistant Professor Crest of Residual Ridge Buccal Shelf Shape of supporting structure Mylohyoid Ridge
DEVELOPING ANALOGUE/SUBTITUTE FOR THE MANDIBULAR DENTURE BEARING AREA Dr Muhammad Rizwan Memon FCPS Assistant Professor Crest of Residual Ridge Buccal Shelf Shape of supporting structure Mylohyoid Ridge
WOMEN'S INTERAGENCY HIV STUDY ORAL PROTOCOL FORM OP 4: ORAL MUCOSAL TISSUE EXAM
 WOMEN'S INTERAGENCY HIV STUDY ORAL PROTOCOL FORM OP 4: ORAL MUCOSAL TISSUE EXAM COMPLETING THE FORM GENERAL INFORMATION Affix the Participant ID label in the space indicated. Record the visit number. Be
WOMEN'S INTERAGENCY HIV STUDY ORAL PROTOCOL FORM OP 4: ORAL MUCOSAL TISSUE EXAM COMPLETING THE FORM GENERAL INFORMATION Affix the Participant ID label in the space indicated. Record the visit number. Be
Dental Morphology and Vocabulary
 Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
MAXILLARY INJECTION TECHNIQUE. Chinthamani Laser Dental Clinic
 MAXILLARY INJECTION TECHNIQUE Chinthamani Laser Dental Clinic Introduction A number of injection techniques are available to aid in providing clinically adequate anesthesia of the teeth and soft and hard
MAXILLARY INJECTION TECHNIQUE Chinthamani Laser Dental Clinic Introduction A number of injection techniques are available to aid in providing clinically adequate anesthesia of the teeth and soft and hard
Head and Neck Case 1 PATIENT HISTORY
 Head and Neck Case 1 PATIENT HISTORY Patient History May 7, 2007 Otolaryngology Head & Neck Subjective: Patient was recently seen by a dentist, who noted a roughness in his lower alveolus, and wanted to
Head and Neck Case 1 PATIENT HISTORY Patient History May 7, 2007 Otolaryngology Head & Neck Subjective: Patient was recently seen by a dentist, who noted a roughness in his lower alveolus, and wanted to
NEOPLASMS OF THE SURFACE EPITHELIUM (KERATINOCYTES)
 NEOPLASMS OF THE SURFACE EPITHELIUM (KERATINOCYTES) Papillary Lesions Precancerous Lesions Keratinocyte Proliferations Carcinomas Melanotic Lesions Melanomas Normal Mucosa Keratin layer Spinous layer Basal
NEOPLASMS OF THE SURFACE EPITHELIUM (KERATINOCYTES) Papillary Lesions Precancerous Lesions Keratinocyte Proliferations Carcinomas Melanotic Lesions Melanomas Normal Mucosa Keratin layer Spinous layer Basal
Vascular. Extravasated blood. Melanocytic. Tattoo. Epidermolysis bullosa. Lichen planus. Pemphigoid Pemphigus Lupus. Candidosis. Surface Epithelial
 Oral Soft Tissue Pathology Epithelial Thickening (white) Combination Erythema migrans Epithelial atrophy (red) Surface Lesions Clinical Impression Enlargements Surface Debris Pigmented Vesicular Ulcerated
Oral Soft Tissue Pathology Epithelial Thickening (white) Combination Erythema migrans Epithelial atrophy (red) Surface Lesions Clinical Impression Enlargements Surface Debris Pigmented Vesicular Ulcerated
Subdivided into Vestibule & Oral cavity proper
 Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
Oral Cancer Dr Christine Goodall Consultant Oral Surgeon University of Glasgow Dental School
 Oral Cancer Dr Christine Goodall Consultant Oral Surgeon University of Glasgow Dental School christine.goodall@glasgow.ac.uk Locations Lip, mouth, oropharynx Tongue, floor of mouth, buccal mucosa, palate,
Oral Cancer Dr Christine Goodall Consultant Oral Surgeon University of Glasgow Dental School christine.goodall@glasgow.ac.uk Locations Lip, mouth, oropharynx Tongue, floor of mouth, buccal mucosa, palate,
A Rare case of Tubercular Gingivitis Case Report
 Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
CASE REPORT PLAQUE TYPE ORAL VERRUCOUS HYPERPLASIA AND IRRITATIONAL FIBROMA: A REPORT OF CONJOINT OCCURRENCE
 CASE REPORT PLAQUE TYPE ORAL VERRUCOUS HYPERPLASIA AND IRRITATIONAL FIBROMA: A REPORT OF CONJOINT OCCURRENCE Alphy Alphonsa Sebastian, Hasan Subhi 1. Phd student, Department of Oral Medicine and Oral Pathology,
CASE REPORT PLAQUE TYPE ORAL VERRUCOUS HYPERPLASIA AND IRRITATIONAL FIBROMA: A REPORT OF CONJOINT OCCURRENCE Alphy Alphonsa Sebastian, Hasan Subhi 1. Phd student, Department of Oral Medicine and Oral Pathology,
Evaluation of Gradual Trend of Patients Satisfaction with Complete Dentures in the Department of Prosthodontics: A Cross-sectional Study
 ISSN: 2203-1413 Vol.04 No.02 Evaluation of Gradual Trend of Patients Satisfaction with Complete Dentures in the Department of Prosthodontics: A Cross-sectional Study Ramin Negahdari 1, Seyyed Mahdi Vahid
ISSN: 2203-1413 Vol.04 No.02 Evaluation of Gradual Trend of Patients Satisfaction with Complete Dentures in the Department of Prosthodontics: A Cross-sectional Study Ramin Negahdari 1, Seyyed Mahdi Vahid
TANYA A. WRIGHT, DDS OBJECTIVES
 TANYA A. WRIGHT, DDS OBJECTIVES One will be able to recognize pathological entities One will be able to establish a reasonable differential diagnosis One will be able to identify various types of lesions
TANYA A. WRIGHT, DDS OBJECTIVES One will be able to recognize pathological entities One will be able to establish a reasonable differential diagnosis One will be able to identify various types of lesions
-Ibrahim Al-Naser. -Dr Al- Muhtaseb. 1 P a g e
 -1 -Ibrahim Al-Naser - -Dr Al- Muhtaseb 1 P a g e The Digestive System The doctor started the lecture by talking about the class rules. The GI system is an organ system, it is divided into: The Alimentary
-1 -Ibrahim Al-Naser - -Dr Al- Muhtaseb 1 P a g e The Digestive System The doctor started the lecture by talking about the class rules. The GI system is an organ system, it is divided into: The Alimentary
Kings College London Dental Institute. Guy s & St Thomas NHS Foundation Trust Oral Medicine Unit. Disease Activity Scoring sheets
 Kings College London Dental Institute Guy s & St Thomas NHS Foundation Trust ral Medicine Unit Disease Activity Scoring sheets Clinical scoring systems for oral mucosal Diseases The routine clinical management
Kings College London Dental Institute Guy s & St Thomas NHS Foundation Trust ral Medicine Unit Disease Activity Scoring sheets Clinical scoring systems for oral mucosal Diseases The routine clinical management
CLASSIFICATIONS. Established in 1994 as a subcommittee of the. Prosthodontic Care Committee
 CLASSIFICATIONS Established in 1994 as a subcommittee of the Prosthodontic Care Committee Committee Members Thomas J. McGarry, DDS, Chair Arthur Nimmo, DDS James F. Skiba, DDS Christopher R. Smith, DDS
CLASSIFICATIONS Established in 1994 as a subcommittee of the Prosthodontic Care Committee Committee Members Thomas J. McGarry, DDS, Chair Arthur Nimmo, DDS James F. Skiba, DDS Christopher R. Smith, DDS
Let s start from the basics for a little review. The Mouth Is Like a Black Hole. But he s friendly at home. Always Wear Gloves!
 The Mouth Is Like a Black Hole Seek and ye shall find: Recognition of Oral Lesions in the Exam Room Lisa Fink, DVM, DAVDC Dentistry & Oral Surgery Service October 4, 2015 But he s friendly at home Part
The Mouth Is Like a Black Hole Seek and ye shall find: Recognition of Oral Lesions in the Exam Room Lisa Fink, DVM, DAVDC Dentistry & Oral Surgery Service October 4, 2015 But he s friendly at home Part
Diagnostic difficulties with lesions of the oral mucosa
 BDIAP London, November 2010 School of Clinical Dentistry University of Sheffield Diagnostic difficulties with lesions of the oral mucosa Paul M Speight Dept Oral & Maxillofacial Pathology University of
BDIAP London, November 2010 School of Clinical Dentistry University of Sheffield Diagnostic difficulties with lesions of the oral mucosa Paul M Speight Dept Oral & Maxillofacial Pathology University of
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Component parts of Chrome Cobalt Removable Partial Denture
 Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Role of the Dental Hygienist in Oral Pathology. Role of the Dental Hygienist in Oral Pathology. Cancers of the Oral Cavity.
 Gum Gardeners Study Club April 25, 2016 Early Detection of Oral Cancer Cindy Kleinegger, DDS, MS NW Oral Pathology Tigard, OR nworalpathology.com Role of the Dental Hygienist in Oral Pathology Work closely
Gum Gardeners Study Club April 25, 2016 Early Detection of Oral Cancer Cindy Kleinegger, DDS, MS NW Oral Pathology Tigard, OR nworalpathology.com Role of the Dental Hygienist in Oral Pathology Work closely
الطلاوة = Leukoplakia LEUKOPLAKIA
 LEUKOPLAKIA Leukoplakia is a clinical term that refers to a predominantly white lesion of the oral mucosa that cannot be rubbed off or characterized by any other definable lesion or known disease. 130
LEUKOPLAKIA Leukoplakia is a clinical term that refers to a predominantly white lesion of the oral mucosa that cannot be rubbed off or characterized by any other definable lesion or known disease. 130
RISK FACTORS OF BURNING MOUTH SYNDROME: UN UPDATE
 RISK FACTORS OF BURNING MOUTH SYNDROME: UN UPDATE Cristina Popa, Carmen Stelea, Eugenia Popescu Department of Oral and Maxilo-facial Surgery Abstract: Burning mouth syndrome has never been associated with
RISK FACTORS OF BURNING MOUTH SYNDROME: UN UPDATE Cristina Popa, Carmen Stelea, Eugenia Popescu Department of Oral and Maxilo-facial Surgery Abstract: Burning mouth syndrome has never been associated with
LEUKOPLAKIA Definition Epidemiology Clinical presentation
 LEUKOPLAKIA Definition Leukoplakia is the most common premalignant or "potentially malignant" lesion of the oral mucosa. Leukoplakia is a predominantly white lesion of the oral mucosa than cannot be clinicopathologically
LEUKOPLAKIA Definition Leukoplakia is the most common premalignant or "potentially malignant" lesion of the oral mucosa. Leukoplakia is a predominantly white lesion of the oral mucosa than cannot be clinicopathologically
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
Oral cavity cancer accounts for approximately 3% of all malignancies and is a significant worldwide health problem.
 Oral cavity cancer accounts for approximately 3% of all malignancies and is a significant worldwide health problem. Majority are SCC ( 5-year survival rate only about 50-60% ) Many SCC arrive from premalignant
Oral cavity cancer accounts for approximately 3% of all malignancies and is a significant worldwide health problem. Majority are SCC ( 5-year survival rate only about 50-60% ) Many SCC arrive from premalignant
Oral Tumors in Dogs Gingival Enlargement
 Oral Tumors in Dogs Is that lump you re seeing in your dog s mouth normal? Or is it something to be concerned about? The easiest way to know for sure is to have it evaluated by a veterinarian. When you
Oral Tumors in Dogs Is that lump you re seeing in your dog s mouth normal? Or is it something to be concerned about? The easiest way to know for sure is to have it evaluated by a veterinarian. When you
أ.م. هدى عباس عبد اهلل CROWN AND BRIDGE جامعة تكريت كلية. Lec. (2) طب االسنان
 Lec. (2) CROWN AND BRIDGE أ.م. هدى عباس عبد اهلل Patient selection and examination A thorough diagnosis must first be made of the patient's dental condition, considering both hard and soft tissues. this
Lec. (2) CROWN AND BRIDGE أ.م. هدى عباس عبد اهلل Patient selection and examination A thorough diagnosis must first be made of the patient's dental condition, considering both hard and soft tissues. this
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper. Oral vestibule : is slit like space between.
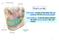 Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Maryland AGD AE and Socket Grafting. Advanced Implant Mentoring Rob D Orazio, DDS. Day 1 Morning 1
 Page1 Page2 advancedimplantmentoring.com Page3 7:30am 8:00am Continental Breakfast & Registration 8:00am 9:30am Lecture- Effects of Tooth Loss on Bone -Site Preservation and Augmentation 9:30am 9:45am
Page1 Page2 advancedimplantmentoring.com Page3 7:30am 8:00am Continental Breakfast & Registration 8:00am 9:30am Lecture- Effects of Tooth Loss on Bone -Site Preservation and Augmentation 9:30am 9:45am
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
MEDICAL POLICY SUBJECT: DENTAL AND ORAL CARE UNDER MEDICAL PLANS
 MEDICAL POLICY SUBJECT: DENTAL AND ORAL CARE UNDER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: DENTAL AND ORAL CARE UNDER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Arrangement of the artificial teeth:
 Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Treatment planning of nonskeletal problems. in preadolescent children
 In the name of GOD Treatment planning of nonskeletal problems in preadolescent children Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 7 William R. Proffit,
In the name of GOD Treatment planning of nonskeletal problems in preadolescent children Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 7 William R. Proffit,
Proliferative Verrucous Leukoplakia of the Gingiva, Report of two Cases with Malignant Transformation
 Journal of Clinical and Anatomic Pathology Case Report Open Access Proliferative Verrucous Leukoplakia of the Gingiva, Report of two Cases with Malignant Transformation Nadereh Ghanee DMD, Selene Saraf
Journal of Clinical and Anatomic Pathology Case Report Open Access Proliferative Verrucous Leukoplakia of the Gingiva, Report of two Cases with Malignant Transformation Nadereh Ghanee DMD, Selene Saraf
Image: Blend Images/Punchstock Image: Blend Images/Punchstock Image: Ablestock/Punchstock. Copyright STFM
 Image: Blend Images/Punchstock Image: Blend Images/Punchstock Image: Ablestock/Punchstock Copyright STFM 2005-2014 Third Edition June 2010 www.smilesforlifeoralhealth.org Last Modified: April, 2014 2 Course
Image: Blend Images/Punchstock Image: Blend Images/Punchstock Image: Ablestock/Punchstock Copyright STFM 2005-2014 Third Edition June 2010 www.smilesforlifeoralhealth.org Last Modified: April, 2014 2 Course
6610 NE 181st Street, Suite #1, Kenmore, WA
 660 NE 8st Street, Suite #, Kenmore, WA 9808 www.northshoredentalacademy.com.08.900 READ CHAPTER The Professional Dental Assistant (p.-9) No Key Terms Recall Questions:,,,, and 6 CLASS SYLLABUS DAY READ
660 NE 8st Street, Suite #, Kenmore, WA 9808 www.northshoredentalacademy.com.08.900 READ CHAPTER The Professional Dental Assistant (p.-9) No Key Terms Recall Questions:,,,, and 6 CLASS SYLLABUS DAY READ
A clinical study on tongue lesions among Iraqi dental outpatients
 A clinical study on lesions among Iraqi dental outpatients Sura Ali Fuoad College of Dentistry, Gulf Medical University, Ajman, UAE ABSTRACT Objective: The aim of this study was to assess the frequency
A clinical study on lesions among Iraqi dental outpatients Sura Ali Fuoad College of Dentistry, Gulf Medical University, Ajman, UAE ABSTRACT Objective: The aim of this study was to assess the frequency
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Anatomy of Oral Cavity DR. MAAN AL-ABBASI
 Anatomy of Oral Cavity DR. MAAN AL-ABBASI By the end of this lecture you should be able to: 1. Differentiate different parts of the oral cavity 2. Describe the blood and nerve supply of mucosa and muscles
Anatomy of Oral Cavity DR. MAAN AL-ABBASI By the end of this lecture you should be able to: 1. Differentiate different parts of the oral cavity 2. Describe the blood and nerve supply of mucosa and muscles
Medical History. Oral Medicine and General Medicine
 Medical History Oral Medicine and General Medicine Gingivitis herpetica acuta NECROTIZÁLÓ SIALOMETAPLASIA SOOR Medical History The life expectancy has recently increased and increasing By dental prevention
Medical History Oral Medicine and General Medicine Gingivitis herpetica acuta NECROTIZÁLÓ SIALOMETAPLASIA SOOR Medical History The life expectancy has recently increased and increasing By dental prevention
LOCAL ANESTHESIA IN PEDIATRIC DENTISTRY
 Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of local anesthesia in pediatric dentistry must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of local anesthesia in pediatric dentistry must be made in conjunction
Basic Anatomy and Physiology of the Lips and Oral Cavity. Dr. Faghih
 Basic Anatomy and Physiology of the Lips and Oral Cavity Dr. Faghih It is divided into seven specific subsites : 1. Lips 2. dentoalveolar ridges 3. oral tongue 4. retromolar trigone 5. floor of mouth 6.
Basic Anatomy and Physiology of the Lips and Oral Cavity Dr. Faghih It is divided into seven specific subsites : 1. Lips 2. dentoalveolar ridges 3. oral tongue 4. retromolar trigone 5. floor of mouth 6.
Allergic contact stomatitis is a rare disorder,
 Allergic Contact Stomatitis: A Case Report and Review of Literature P Lokesh, T Rooban, Joshua Elizabeth, K Umadevi, K Ranganathan Abstract Allergic contact stomatitis is a well-recognized entity, which
Allergic Contact Stomatitis: A Case Report and Review of Literature P Lokesh, T Rooban, Joshua Elizabeth, K Umadevi, K Ranganathan Abstract Allergic contact stomatitis is a well-recognized entity, which
Dentures. Types of Dentures
 Dentures Here The Implant Dentist we have a master technician on site who works alongside Dr Pather to ensure perfect aesthetics, fit and comfort. As we age, our teeth gradually deteriorate. Ageing teeth
Dentures Here The Implant Dentist we have a master technician on site who works alongside Dr Pather to ensure perfect aesthetics, fit and comfort. As we age, our teeth gradually deteriorate. Ageing teeth
TASKS. 2. Apply a disclosing agent to make the plaque visible.
 TASKS EQUIPMENT AND MATERIALS Personal protective equipment Assortment of nylon, soft-bristled toothbrushes Assortment of dental Floss, waxed and nonwaxed Disclosing solution Face mirror 3. Demonstrate
TASKS EQUIPMENT AND MATERIALS Personal protective equipment Assortment of nylon, soft-bristled toothbrushes Assortment of dental Floss, waxed and nonwaxed Disclosing solution Face mirror 3. Demonstrate
DIAGNOSIS & TREATMENT PLANNING For RPD
 DIAGNOSIS & TREATMENT PLANNING For RPD Introduction Goals of Treatment a) Eliminate disease b) Preserve what remains c) Restore esthetics & function d) Make up of patient psychology Functions of a RPD
DIAGNOSIS & TREATMENT PLANNING For RPD Introduction Goals of Treatment a) Eliminate disease b) Preserve what remains c) Restore esthetics & function d) Make up of patient psychology Functions of a RPD
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Appendix 4. Case Summary Template. Social history. Patient (Name and Date of birth): Presenting complaints. History Medical history
 Appendix 4 Case Summary Template Patient (Name and Date of birth): Presenting complaints Chief complaint Subsidiary complaints History of complaints Patient s expectations History Medical history Medical
Appendix 4 Case Summary Template Patient (Name and Date of birth): Presenting complaints Chief complaint Subsidiary complaints History of complaints Patient s expectations History Medical history Medical
Vertical relation: It is the amount of separation between the maxilla and
 Vertical relations Vertical relation: It is the amount of separation between the maxilla and the mandible in a frontal plane. Vertical dimension: It is the distance between two selected points, one on
Vertical relations Vertical relation: It is the amount of separation between the maxilla and the mandible in a frontal plane. Vertical dimension: It is the distance between two selected points, one on
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
EAR, NOSE, THROAT DISORDERS
 EAR, NOSE, THROAT DISORDERS A Case of Recurrent Pyogenic Granuloma of Gingiva ABSTRACT A case of pyogenic granuloma of gingiva is presented. Aetiology factors, clinical presentations and different treatment
EAR, NOSE, THROAT DISORDERS A Case of Recurrent Pyogenic Granuloma of Gingiva ABSTRACT A case of pyogenic granuloma of gingiva is presented. Aetiology factors, clinical presentations and different treatment
Case Report Soft Tissue Reconstruction with Free Gingival Graft Technique following Excision of a Fibroma
 Case Reports in Dentistry Volume 2015, Article ID 248363, 4 pages http://dx.doi.org/10.1155/2015/248363 Case Report Soft Tissue Reconstruction with Free Gingival Graft Technique following Excision of a
Case Reports in Dentistry Volume 2015, Article ID 248363, 4 pages http://dx.doi.org/10.1155/2015/248363 Case Report Soft Tissue Reconstruction with Free Gingival Graft Technique following Excision of a
World Articles of Ear, Nose and Throat Page 1
 World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
From the Cradle to the Grave: Oral pathology through the life span
 From the Cradle to the Grave: Oral pathology through the life span Conditions Exhibited in Infants and Children: Dental Lamina Cysts Etiology: Developmental Clinical appearance: Cystic nodules on alveolar
From the Cradle to the Grave: Oral pathology through the life span Conditions Exhibited in Infants and Children: Dental Lamina Cysts Etiology: Developmental Clinical appearance: Cystic nodules on alveolar
Dr Omar Kujan Clinical examination Chapter 2. Al-Farabi Colleges for Dentistry and Nursing. Oral Diagnosis 1. Clinical examination.
 Al-Farabi Colleges for Dentistry and Nursing Oral Diagnosis 1 Clinical examination Dr Omar Kujan DDS DipOPath MSc PhD 1 Clinical Examination The dentist is responsible for understanding and recognizing
Al-Farabi Colleges for Dentistry and Nursing Oral Diagnosis 1 Clinical examination Dr Omar Kujan DDS DipOPath MSc PhD 1 Clinical Examination The dentist is responsible for understanding and recognizing
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
ORAL MELANOMA Definition Epidemiology Clinical Presentation
 ORAL MELANOMA Definition Melanoma is a highly malignant neoplasia, arising from melanocytes, the cells that produce the brownish pigment melanin. Melanin is the determinant in skin colour and protects
ORAL MELANOMA Definition Melanoma is a highly malignant neoplasia, arising from melanocytes, the cells that produce the brownish pigment melanin. Melanin is the determinant in skin colour and protects
Differential Diagnosis of Oral Masses. Palatal Lesions
 Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
Diseases of the breast (1 of 2)
 Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
ORTHODONTIC INITIAL ASSESSMENT FORM (OIAF) w/ INSTRUCTIONS
 Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
Use the accompanying Tip Sheet and How to Score the Orthodontic Initial Assessment Form for guidance in completion of the assessment form. You will need this score sheet and a disposable ruler (or a Boley
ARAB AMERICAN UNIVERSITY. Lab. Manual. Prosthetic Dentistry1; Removable Prosthodontics. 3 rd year
 ARAB AMERICAN UNIVERSITY Lab. Manual Prosthetic Dentistry1; Removable Prosthodontics 3 rd year Department of Fixed and removable prosthetic Dentistry Faculty of Dentistry 2012/2013 Course Instructor Dr.
ARAB AMERICAN UNIVERSITY Lab. Manual Prosthetic Dentistry1; Removable Prosthodontics 3 rd year Department of Fixed and removable prosthetic Dentistry Faculty of Dentistry 2012/2013 Course Instructor Dr.
Development of occlusion
 Development of occlusion The development of dentition is an important part of craniofacial growth as the formation, eruption, exfoliation and exchange of teeth take place during this period. Term occlusion
Development of occlusion The development of dentition is an important part of craniofacial growth as the formation, eruption, exfoliation and exchange of teeth take place during this period. Term occlusion
Squamous Cell Neoplasia and Precursor Lesions
 Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
Squamous Cell Neoplasia and Precursor Lesions Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical
INTRA/EXTRA ORAL EXAMINATION
 INTRA/EXTRA ORAL EXAMINATION www.dentalelle.com Dentalelle Tutoring Intraoral/Extraoral Examination 1. If you notice a typical finding after reviewing the head and neck on a new patient, what does this
INTRA/EXTRA ORAL EXAMINATION www.dentalelle.com Dentalelle Tutoring Intraoral/Extraoral Examination 1. If you notice a typical finding after reviewing the head and neck on a new patient, what does this
ORAL MELANOTIC NEVI: A CASE REPORT AND REVIEW OF LITERATURE
 ORAL MELANOTIC NEVI: A CASE REPORT AND REVIEW OF LITERATURE Abstract: *V.T Beena **Isha Chauhan *** R. Heera ***R. Rajeev Oral melanotic nevi are uncommon oral lesions causing focal. Melanotic nevi are
ORAL MELANOTIC NEVI: A CASE REPORT AND REVIEW OF LITERATURE Abstract: *V.T Beena **Isha Chauhan *** R. Heera ***R. Rajeev Oral melanotic nevi are uncommon oral lesions causing focal. Melanotic nevi are
WHITE LESIONS OF THE ORAL CAVITY - diagnostic appraisal & management strategies
 WHITE LESIONS OF THE ORAL CAVITY - diagnostic appraisal & management strategies * Joshy V.R ** Hari.S * Reader, Dept of Oral Pathology, Yenepoya Dental College, Yenepoya University, Mangalore 575 018.
WHITE LESIONS OF THE ORAL CAVITY - diagnostic appraisal & management strategies * Joshy V.R ** Hari.S * Reader, Dept of Oral Pathology, Yenepoya Dental College, Yenepoya University, Mangalore 575 018.
DEVELOPING ANALOGUE SUBTITUTE FOR THE MAXILLARY DENTURE BEARING AREA. Dr Muhammad Rizwan Memon FCPS Assistant Professor
 DEVELOPING ANALOGUE SUBTITUTE FOR THE MAXILLARY DENTURE BEARING AREA Dr Muhammad Rizwan Memon FCPS Assistant Professor Mucous membrane Residual Ridge Incisive papilla Rugae area Mid palatine raphe Hard
DEVELOPING ANALOGUE SUBTITUTE FOR THE MAXILLARY DENTURE BEARING AREA Dr Muhammad Rizwan Memon FCPS Assistant Professor Mucous membrane Residual Ridge Incisive papilla Rugae area Mid palatine raphe Hard
External Neoplasms in Goats: A Clinicopathological Study on Five Types. Abu-Seida, A.M and Kawkab, A. Ahmed
 External Neoplasms in Goats: A Clinicopathological Study on Five Types By Abu-Seida, A.M and Kawkab, A. Ahmed Introduction Introduction Neoplasia is occasionally diagnosed in goats. A survey of 800000
External Neoplasms in Goats: A Clinicopathological Study on Five Types By Abu-Seida, A.M and Kawkab, A. Ahmed Introduction Introduction Neoplasia is occasionally diagnosed in goats. A survey of 800000
PH-04A: Clinical Photography Production Checklist With A Small Camera
 PH-04A: Clinical Photography Production Checklist With A Small Camera Operator Name Total 0-49, Passing 39 Your Score Patient Name Date of Series Instructions: Evaluate your Series of photographs first.
PH-04A: Clinical Photography Production Checklist With A Small Camera Operator Name Total 0-49, Passing 39 Your Score Patient Name Date of Series Instructions: Evaluate your Series of photographs first.
