Simple Techniques of Skin Grafting Horses. Jim Schumacher
|
|
|
- Diana Dixon
- 5 years ago
- Views:
Transcription
1 Simple Techniques of Skin Grafting Horses Jim Schumacher The most common indication for skin grafting horses is to promote healing of a wound so large that it cannot heal by second intention (Fig. 1.), but nearly any open wound can be grafted. The more rapid healing achieved with a skin graft may make grafting more economical than a lengthy period of bandaging, and it may allow the horse to return to athletic performance sooner. Skin grafting should not be regarded as an option of last resort but instead should be considered when treating a horse for any open wound that cannot be closed primarily, especially if the wound is in area where healing by second intention is likely to be prolonged or result in unsightly scarring. The two basic types of skin grafting are pedicle grafting and free grafting. A pedicle graft is created adjacent to the wound and remains connected to the donor site by a vascular pedicle, ensuring its viability. It imparts a good cosmetic appearance because the graft is composed of all components of skin. Pedicle grafts are rarely used to cover wounds of horses because mobilizing skin of horses to advance a pedicle graft to cover the adjacent wound is difficult. Fig. 1. This degloving injury to the carpus of a horse is too extensive to heal by contraction and epithelization. It can be healed only with a skin graft. A free skin graft is a segment of skin that has no vascular connections because it has been detached completely from its donor site and relocated to a wound at a remote site. An autograft, or isograft, is a graft transferred from one site to another on the same individual and is the most practical type of graft applied to wounds of horses because the graft provokes no immune response. An allograft, or homograft, is a graft transferred between two members of the same species, and a xenograft, or heterograft, is a graft transferred from a member of one species to a member of another species. An allograft or xenograft is sometimes applied to a wound as a biological dressing. Free skin grafts can be also classified as full-thickness or split-thickness. Full- or split-thickness skin grafts can be applied to the surface of wounds as sheets (i.e., sheet grafts) or implanted within the wound (i.e., island or seed grafts). Each technique of skin grafting has its advantages and disadvantages, and so, the technique selected depends on the circumstances, such as the size and location of the wound, the necessity for a good cosmetic appearance, available instrumentation, experience of the surgeon, and the financial resources of the owner. A free graft can be accepted by nearly any type of tissue, except bone devoid of periosteum, tendon devoid of paratenon, and cartilage devoid of perichondrium, but to accept a free graft, the wound should be vascular and free of infection and necrotic tissue. 1-3 The graft attaches to the wound by fibrin within minutes after being applied and is nourished initially by imbibing plasma by capillary action into the lumen of the graft s vessels, a process referred to as plasmatic imbibition. 3-5 Blood vessels and fibroblasts from the wound invade the fibrin within 48 to 72 hours. After several days, new capillaries from the wound cross the fibrin matrix to anastomose with capillaries in the graft, a process called inosculation. 3,4 New capillaries from the wound invade other vessels within the graft and cut new vascular channels into its dermis, a process referred to as neovascularization. The graft is revascularized by day 5 and is attached firmly to wound by day 10. Infection is, by far, the most common cause of failure of skin grafts to be accepted, 6 but other causes are excessive inflammation of the wound, accumulation of fluid beneath the graft, and motion. 1,2,5 The
2 wound becomes infected when the tissue concentration of bacteria surpasses 10 5 organisms per gram of tissue, but the concentration necessary to infect a wound can be much less than 10 5 per gram of tissue for some bacteria, particularly ß-hemolytic streptococci and pseudomonads. 3,5 Wounds of the distal portion of limbs of horses that heal by second intention are inherently inflamed, and therefore, grafts applied to wounds of horses may be more prone to failure than are grafts applied to wounds of other species. 7,8 Blood, serum, or exudate accumulated beneath a graft prevents fibrin from attaching the graft to the wound and obstructs influx of capillaries from the wound into the graft. 9 Shearing forces between the graft and the wound, caused by movement of the bandage, disrupt the fibrin attachment and impair re-vascularization. A fresh wound accepts a graft more readily than does a granulating wound, and a wound filled with immature granulation tissue accepts a graft more readily than does a wound filled with mature granulation tissue. Survival of a skin graft is better correlated to the concentration of bacteria in the wound than to any other factor. 10 The bacterial status of a wound is usually assessed qualitatively, however, rather than quantitatively. A wound should be assumed to be infected if it shows signs of inflammation, but even a wound showing no signs of inflammation may still be infected. 10 Infection is most often caused by streptococcal or pseudomonas spp. Streptococcae are nearly always susceptible to a ß-lactam antibiotic, 11 and pseudomonads are usually sensitive to aminoglycoside antibiotics. 2 A ß-lactam antibiotic may become ineffective in resolving a streptococcal infection if other bacteria in the wound secrete ß-lactamase, an enzyme that inactivates ß-lactam antibiotics. 12 The efficacy of the ß-lactam antibiotic against streptococci is preserved if the ß-lactam antibiotic applied to the wound is effective against ß-lactamase producing bacteria also present in the wound. The efficacy of the ß-lactam antibiotic can also be preserved by concomitant administration of clavulanic acid, a potent inhibitor of ß-lactamase. Clavulanic acid is combined most commonly with amoxicillin or ticarcillin. Infection of a granulating wound is best resolved by administering the appropriate antibiotic topically, rather than systemically, because an antibiotic administered systemically often fails to reach a therapeutic concentration in the granulation tissue. 3,13 Most bacteria and inflammatory cells can be removed from an infected, granulating wound by excising the granulation tissue to the level of or slightly below the margin of the surrounding skin. Island Grafting The simplest method of grafting is island grafting, which is a technique in which a small disc or strip of full-thickness or partial thickness skin is implanted into a granulating wound for the purpose of increasing the area of epidermis from which epithelialization can proceed. Types of island grafts applied to wounds of horses are punch grafts, pinch grafts, and tunnel grafts. Punch grafts are full-thickness plugs of skin harvested and implanted into granulation tissue using skin biopsy punches. Punch grafts are harvested with a punch directly from an inconspicuous site on the horse, such as the portion of the neck that lies beneath the mane. After preparing the donor site, grafts are harvested about 1 cm apart using a 6- to 8-mm diameter skin biopsy punch. The small wounds created by the punch can be closed with a suture or staple but are usually left unsutured to heal by second intention. Subcutaneous fascia is excised from each graft to expose dermal vasculature to permit plasmatic imbibition and inosculation. 14 One technique used to remove subcutaneous fascia from the graft is to penetrate the skin with the skin biopsy punch, and then, using thumb forceps, lift the edge of the graft to expose subcutaneous tissue, which is excised from the dermis. Removing subcutaneous tissue from each plug is tedious (Fig. 2), and therefore, some clinicians prefer to harvest punch grafts from a section of skin excised from the cranial pectoral region. 15 The donor site is closed
3 in one or two layers. Subcutaneous fascia is excised from the section of skin to expose the dermal vasculature, and plugs are harvested from the excised section of skin by using the biopsy punch. The recipient holes in the wound are created about 5 or 6 mm apart and should be created before the grafts are harvested to ensure that haemorrhage has ceased before the grafts are implanted. Creation of the holes should begin distally and proceed proximally. The recipient holes are created with a slightly smaller punch than that used to harvest the grafts to allow for contraction of the graft. A cotton-tipped applicator inserted into the holes prevents a blood clot from forming within the hole and facilitates locating the holes for inserting the grafts (Fig. 3). The grafts are inserted into recipient holes, using a hemostat or tissue forceps, with the graft s epidermis oriented toward the surface of the wound. Fig. 3. A cotton-tipped applicator inserted into the recipient hole for a punch graft prevents clots from forming and facilitates locating the hole. Pinch grafts are small discs of skin, harvested by tenting skin to create a cone of skin and then excising this cone to create a small disc, which is implanted into granulation tissue. Pinch grafts can be harvested directly from an inconspicuous site, such as the horse s perineum, neck, ventrolateral aspect of the abdomen, or pectoral region. Hair is clipped from the donor site, the site is cleaned, and desensitised by injecting local anaesthetic solution subcutaneously. Skin is most easily tented by using a 20-gauge, hypodermic needle with a bent point (Fig. 4). The cone of skin is excised with a #11 scalpel blade to create a 3-mm diameter disc. Discs 3 mm or less in diameter are split-thickness, whereas the center of larger grafts tends to be full-thickness. 16 The graft is placed on the wound, with its epidermal side up, and a pocket into which the disc is implanted is created in the granulation tissue immediately distal to the graft by using a #15 scalpel blade inserted into the granulation tissue at an acute angle to create a shallow pocket. The disc, which adheres to the wound, is pushed into the pocket using the scalpel blade used to make the pocket. By using this technique, the surgeon can create and implant the pockets without averting his or her eyes from the wound. No consideration need be given to the direction of hair growth as the graft inserted because orienting the hair in its proper direction has little Fig. 2. Fascia can be removed from each punch graft, but an assistant is required. Fig. 4. To harvest a pinch graft, a cone of skin at the donor site is elevated with a hypodermic needle, the point of which is bent, and excised with a scalpel blade. effect on the cosmetic outcome and is tedious. Implantation should begin distally and proceed proximally so that the haemorrhage from the sites of implantation does not obscure that portion of the wound that has yet to be implanted. The thin layer of granulation tissue overlying each pinch graft sloughs, usually between the first and second week. 16 The superficial, pigmented portion of pinch and punch grafts frequently sloughs at about this time exposing pale dermis, which may be difficult to distinguish from surrounding granulation tissue, giving the impression that all of the graft has sloughed. A red ring of advancing epithelium is seen surrounding each pinch or punch graft by three weeks, and these rings of epithelium increasingly expand until they converge to cover the entire wound (Fig. 5). Half or more of pinch and punch grafts
4 can be expected to survive. The time required for the wound to epithelialize is inversely proportional to the amount pinch or punch grafts applied. Tunnel grafts are thin strips of full-thickness or split-thickness skin implanted into tunnels created in granulation tissue Tunnel grafts can be harvested, using a variety of techniques, from many sites and can be implanted with the horse sedated or anaesthetized. They can be harvested from the ventral aspect of the flank with the horse anaesthetized or from the neck or cranial pectoral region with the horse sedated. One technique of harvesting strips of skin is, after preparing the donor site, to create linear wheals, 2- to 3-cm wide and slightly longer than the width of the wound to be grafted by subcutaneously injecting isotonic saline solution (if the grafts are harvested with the horse anaesthetized) or local anaesthetic solution (if the grafts are harvested with the horse sedated) A straight intestinal forceps is applied to the base of the wheal so that skin protrudes from the jaws of the forceps, and the protruding skin is excised with a scalpel blade. The width and thickness of the graft is Fig. 5. Epithelium advances across the wound from the grafts within the wound and from the periphery of the wound. determined by the amount of skin protruding above the jaws. If a full-thickness strip of skin is harvested, the donor site should be closed with sutures or staples. If a split-thickness strip is harvested, the partialthickness wound created is left unsutured. Subcutaneous fascia must be excised from full-thickness tunnel grafts to expose the dermis. A method of harvesting full-thickness strips of skin is to excise a 2- to 3-cm wide, full-thickness, elliptical section of skin from the ventrolateral aspect of the flank or cranial pectoral region, and, after sharply excising subcutaneous tissue from the graft, to divide this skin into 2- to 3-mm wide strips. The wound is closed in one or two layers. Split-thickness strips of skin can be cut from a split-thickness section of skin harvested from the ventrolateral aspect of the thorax or the ventral aspect of the abdomen (see split-thickness skin grafting below). To implant a tunnel graft, the shaft of a long, thin, alligator forceps is inserted through the granulation tissue at the edge of the wound, perpendicular to the long axis of the limb, at a depth of 2 to 3 mm until the end of the forceps emerges at the other side of the wound tissue. One end of the graft is grasped with the forceps, and the forceps and graft are pulled back through tunnel created by the forceps, taking care that the graft s epidermis is oriented toward the surface of the wound. The protruding ends of the graft are fixed to the skin surrounding the wound with a suture, staple, or cyanoacrylate glue. The graft is implanted in two steps if the wound is too convex to be spanned by the alligator forceps In this situation, the end of the forceps is inserted at the margin of the wound and exited in the centre of the wound. The graft is grasped by the jaws of the forceps and pull through the tunnel. The end of the forceps is inserted into the margin of the opposite side of the wound and exited at or close to the site of entry of the graft in the center of the wound. The end of the graft is grasped by the jaws of the forceps and pulled back through the second tunnel. Grafts are implanted about 2 cm apart. If the graft was implanted shallowly (i.e., at < 2 mm), the granulation tissue overlying the graft is likely to slough within a week exposing the re-vascularized graft. If the graft was implanted deeply (i.e., at 4 to 5 mm), granulation tissue overlying the grafts must be excised six to 10 days later, with the horse sedated or anaesthetized Island grafting requires no expensive equipment and little expertise and can usually be performed with the horse sedated. Island grafts are often accepted by wounds that have little chance of accepting a sheet graft, such as inflamed wounds or wounds in areas of high motion. Rejection of one graft has no effect on acceptance of other grafts. Island grafting is usually reserved for small wounds and for circumstances where epithelial scarring is unimportant to the owner. Island grafting is tedious, and the
5 grafts can be applied only to granulating wounds. Complications of tunnel grafting include inadvertent dislodging of a graft while attempting to expose it and failure to locate buried grafts. Full-Thickness Sheet Grafting A full-thickness graft is most easily harvested from the cranial pectoral region - one of the few places on a horse where the skin is relatively mobile. The graft is usually harvested with the horse sedated, after desensitising the donor site with local anaesthetic solution. The donor site is sutured in one or two layers. Subcutaneous tissue is sharply excised to expose the dermal vasculature to permit plasmatic imbibition and inosculation, Hair follicles in the dermis are visible when the subcutaneous tissue has been adequately removed. The graft is attached to the recipient site with staples, sutures, or cyanoacrylate glue. When attaching the graft with staples or sutures, the recipient site must be desensitised with local or regional anaesthesia. Attaching the graft to the recipient site with slight tension opens the small dermal vessels for plasmatic imbibition and inosculation. 20 Full-thickness grafting is usually reserved for fresh, uncontaminated wounds because full-thickness grafts are not as readily accepted as split-thickness grafts because full-thickness grafts require more nourishment and because they have fewer exposed blood vessels for inosculation and revascularization. 9,21 Full-thickness sheet grafting can be performed with the horse sedated without using expensive instruments. Wounds healed with a full-thickness skin graft resist trauma better and are more cosmetic than are wounds healed with any other type of grafts. Full-thickness grafts can be used to cover only small wounds because the horse s lack of redundant skin limits the availability of donor skin. The largest graft that can be harvested from the chest, while allowing the donor site to be easily closed with sutures, is an ellipse usually not wider than 8 cm. The owner should be cautioned that the sutured donor site might dehisce but reassured that an open wound on the chest heals rapidly and cosmetically, almost entirely by contraction. Split-Thickness Sheet Grafting A split-thickness sheet graft is composed of epidermis and a portion of dermis. A split-thickness graft is harvested by splitting the dermis with a power-driven dermatome, a drum dermatome, or a free-hand knife. Power-driven dermatomes and drum dermatomes allow harvesting of grafts of precise width and thickness, and they can be operated with little experience, but they are expensive, require skilled maintenance and may fail to operate properly when proper functioning is critical. Drum dermatomes are seldom, if ever, used to harvest sheet grafts from horses. Although they are not as expensive as powerdriven dermatomes, their major disadvantage for harvesting grafts from horses is that the length of the graft is limited by the circumference of the drum. Split-thickness grafts large enough to cover extensive wounds of horses can be harvested economically with any one of a assortment of free-hand dermatomes designed for harvesting skin of human beings. A free-hand knife is far less expensive than is a power-driven dermatome or a drum dermatome, requires no skilled maintenance, does not malfunction, is easily cleaned and sterilized, and can be transported easily. Wider grafts can be harvested with the free-hand knife than with most power-driven dermatomes, and a great advantage of a freehand knife over a power-driven dermatome is that using a free-hand knife, a split-thickness sheet graft can be harvested from the ventral aspect of the abdomen, which is a difficult feat using most power-driven dermatomes. Fig. 6. A hand-held skin grafting knife should have an adjustable roller and a disposable blade.
6 The most easily used hand-held knives have an adjustable roller in front of a disposable blade. An example is the Watson skin grafting knife (Watson Skin Grafting Knife; Padgett Instruments, Inc., 1520 Grand, Kansas City, MO) (Fig. 6.). Only a moderate amount of practice is required to become proficient in in the use of this knife because the adjustable roller controls the depth of cut. The position of the adjustable roller in relation to the blade is controlled by a calibrated knob at one end of the roller and a lock at the other end. The correlation between each calibration on the knob and the thickness of the graft is learned by experience. The depth of cut depends on the distance of the roller from the blade, the pressure applied to the knife during the harvest, and the angle of incidence at which the knife is held. 11 By applying greater pressure to the knife or by increasing the knife s angle of incidence, the thickness of the graft can be increased without changing the position of the roller. A split-thickness sheet graft can be harvested safely only with the horse anaesthetized. The donor site of a split-thickness graft heals leaving a large epithelial scar, and, therefore, a split-thickness graft should be harvested from an inconspicuous site. The ventral aspect of the abdomen is the least conspicuous site from which to harvest a split-thickness graft on a horse, but harvesting from this site using a power-driven dermatome is difficult to impossible. A surface firmer than the ventral aspect of the abdomen, such as the ventrolateral aspect of the thorax, is usually required to harvest a splitthickness graft using a power dermatome. A free-hand knife is generally required to harvest splitthickness skin from the ventral aspect of the abdomen. To harvest skin from the ventral aspect of the abdomen using a freehand knife, the horse is positioned in lateral recumbency with the ventral portion of the abdomen protruding over the edge of the table so that the movement of the knife is not restricted by the table. The donor site is prepared for aseptic surgery, but draping is unnecessary. Harvesting usually begins at the umbilicus and proceeds cranially, and so, if the surgeon is right-handed, the horse is best positioned in right lateral recumbency. The knife and donor site should be lubricated with isotonic saline solution to reduce friction between the skin and the knife. The knife is pressed into the abdomen with moderate pressure at an acute angle of 5 to 10 degrees. The dermis is cut by moving the blade up and down and forward while an assistant applies slight tension to the cut end of the graft (Fig. 7). After harvesting several centimeters of graft, the surgeon should stop to examine the graft and donor site to determine if the graft is being harvested at the desired thickness. A deep cut through the Fig. 7. To harvest a graft from the ventral aspect of the abdomen, the horse s abdomen should protrude beyond the edge of the table to allow unrestricted up-and-down movement of the free-hand knife. dermis transects large but few vessels and creates an opaque graft, whereas a shallow cut creates a semi-transparent graft and transects many small vessels. To change the depth of cut, the adjustable roller can be repositioned, pressure applied to the knife can be changed, or the knife s angle of incidence can changed. A thin, split-thickness skin graft is harvested with much more difficulty than is a thick graft. The graft is separated from the donor site by tilting the knife upward. The graft is fixed to the margins of the wound with sutures, staples, or cyanoacrylate glue while the horse is anaesthetized, but if the graft is applied after the horse recovers from anaesthesia, the margin of the wound must be desensitised by using local or regional anaesthesia when attaching the graft with sutures or staples. The graft can be attached to the margin of the wound with cyanoacrylate glue without using local or regional anaesthesia. The overlapped and glued margin of the graft eventually desiccates and sloughs. Applying the graft after the horse recovers from anaesthesia removes the risk of damage to the graft that might occur during recovery and decrease the time of anaesthesia.
7 Split-thickness sheet grafts can be harvested in sheets large enough to cover wounds too large to be covered by a full-thickness graft, and they are accepted more readily than are full-thickness grafts because split-thickness grafts require less nourishment and have more exposed vessels in the dermis for inosculation and revascularization. The appearance and durability of a wound healed with a splitthickness skin graft are poorer than that of a wound healed with a full-thickness skin graft. Harvesting a split-thickness graft is far less convenient and far more expensive than harvesting a full-thickness graft or island grafts because the horse must be anaesthetized. Unlike island grafts, which are independent of one another, failure of a portion of a sheet graft may result in loss of the entire graft. Epithelial scarring at the donor site of a split-thickness sheet graft can be extensive. Meshing Sheet Grafts A split- or full-thickness sheet graft can be applied to a wound as a solid or meshed sheet, but most are meshed before they applied to a horse. The primary reason to mesh, or fenestrate, a sheet graft is to expand the graft to allow it to cover a wound larger than the graft itself. Meshing a sheet graft also prevents exudate or blood from becoming interposed between the graft and the wound and enables a topically applied antimicrobial agent to uniformly contact a large portion wound. Fibrin fills the fenestrations increasing the graft s stability on the wound, and because it can expand, a meshed graft is better able to tolerate motion. 22 A graft can be meshed with a scalpel blade or with a meshgraft dermatome, such as the relatively inexpensive, Padgett mechanical skin mesher (Mesh Skin Graft Expander, No. Z- PD-170; Padgett Instruments, Kansas City, MO), which Fig. 8. A mechanical skin mesher. The graft is pushed into staggered, parallel rows of blades by using a Teflon-covered rolling pin. consists of staggered parallel rows of blades, housed in an aluminum block (Fig. 8.). The graft is placed on the block, dermal side down, and pressed into the cutting blades with a Teflon-covered rolling pin. The cutting blades fenestrate the graft in a staggered pattern allowing the graft to be expanded to three times its original area. To manually mesh a sheet graft, the graft is fixed to a sterile piece of cardboard or plastic, and, using a scalpel, staggered, parallel rows of incisions are created in the graft. The longer and more numerous the incisions, the greater is the expansion. Meshing a graft manually is tedious and time-consuming, especially if the graft must be greatly expanded, or if the graft is large. Full-thickness sheet grafts of horses are difficult to mesh on commercial mesh graft dermatomes and so must usually be meshed manually. Expanding a meshed graft exposes portions of the wound within the fenestrations, and each exposed portion of the wound must heal by contraction and epithelialization. The exposed portions of the wound epithelialize rapidly because of the extensive amount of borders from which epithelial cells can migrate. The healed wound is eventually covered with a uniform pattern of diamond-shaped, epithelial scars within the fenestrations. Aftercare The grafted wound is covered with a sterile, non-adherent dressing, to which an appropriate antimicrobial agent has been applied. The dressing is secured to the wound with conforming rolled gauze, and a bandage is applied over the dressing. If the wound is located in a region hard to immobilize, shearing forces can be minimized by securing the dressing to the wound with elastic, adhesive tape instead of rolled gauze, or a cast can be applied to completely immobilize the grafted portion of the limb. A splint applied to the outside of a bandage may suffice if casting the limb is impractical. The bandage is usually not changed for 4 to 5 days after grafting to avoid disrupting the
8 graft, unless nosocomial infection with virulent bacteria, such as Streptococcus and Pseudomonas spp. is a problem, in which case, the bandage should be changed daily. An antimicrobial agent effective against both ß-hemolytic Streptococcus and Pseudomonas spp., such as ticarcillin with clavulanic acid (Timentin; GlaxcoSmithKline, Research Triangle Park, NC) should be applied topically to the wound at each bandage change. 23 Storing Split-thickness Sheet Grafts Skin grafts submerged in isotonic saline solution or lactated Ringer s solution can be stored in a refrigerator for at least week. 9,24 Using a culture medium, such as McCoy s 5A medium, to which a small volume of serum has been added, extends the life of the stored graft to 3 weeks or longer. 25 McCoy s 5A medium is a balanced electrolyte solution containing amino acids, vitamins, dextrose, and a ph indicator, phenol red. The horse s own serum or a commercially available, antibody-free, equine serum should be used to avoid antigenic reaction of the serum to the graft. 26 The concentration of serum in the McCoy s 5A medium should be between 10 and Stored skin can be used to cover defects created by partial or complete loss of the primary graft. A graft harvested when a horse is anaesthetised for treatment for a wound can be stored until the condition of the wound has improved sufficiently to permit grafting. A stored graft is more readily accepted than a fresh graft because grafts stored for 24 hours or more undergo anaerobic metabolism, which causes release of metabolites that encourage rapid vascularization of the graft. 28 Using Grafts as Biological Bandages A wound can be dressed temporarily with a cutaneous allograft or xenograft to stimulate angiogenesis, speed epithelialization, prevent infection, and retard the formation of exuberant granulation tissue A cutaneous allograft or xenograft vascularizes before it is rejected, which enhances its ability to defend the wound against infection, but even a graft that is rejected before it can vascularize helps protect the wound from bacterial infection by trapping bacteria in the fibrin attaching the graft to the underlying wound. Wounds treated with an allograft or xenograft require far fewer bandage changes than do wounds covered with a non-biological dressing. References 1. Flowers RS: Unexpected postoperative problems in skin grafting. Surg Clin North Am 1970;50: Rudolph R, Fisher JC, Ninnemann JL: Skin Grafting. Little, Brown and Company, Boston, Argenta LC, Dingman RO: Skin Grafting. p In Epstein E (ed): Skin Surgery. 6th Ed. Saunders, Philadelphia, Mir Y ML: Biology of the skin graft. Plast Reconstr Surg 8: 1951; Teh B: Why do skin grafts fail? Plast Reconstr Surg 1979;63: Booth L: Equine wound reconstruction using free skin grafting. Calif Vet 1991;45: Wilmink JM, Nederbragt H, van Weeren PR, et al: Differences in wound contraction between horses and ponies: the in vitro contraction capacity of fibroblasts. Equine Vet J 2001;33: Wilmink JM, van Weeren PR, Stolk PW, et al: Differences in second-intention wound healing between horses and ponies: histological aspects. Equine Vet J 1999;31: Vistnes LM: Grafting of skin. Surg Clin North Am 1977;57: Robson M, Krizek TJ: Predicting skin graft survival. J Trauma 1973;13: Cason J: Skin Grafting and Diagnosis of Depth of Burn. P In Cason J, (ed): Treatment of Burns. Chapman and Hall, London, Boon RJ, Beale AS: Response of Streptococcus pyogenes to therapy with amoxicillin or amoxicillinclavulanic acid in a mouse model of mixed infection caused by Staphylococcus aureus and Streptococcus pyogenes. Antimicrob Agents Chemother 1987;31: Robson MC, Edstom LE, Krizek, TJ: The efficacy of systemic antibiotics in the treatment of granulating wounds. J Surg Res 1974;16: Lindsay WA: Step-by-step instructions for equine skin grafting techniques. Vet Med 1988;83:598.
9 15. Boyd CL, Hanselka DV: A skin punch technique for equine skin grafting. J Am Vet Med Assoc 1971;158: Mackay-Smith MP, Marks D: A skin grafting technique for horses. J Am Vet Med Assoc 1968;152: Bjorck GTK: Tunnel skin grafting in the equine species. Proc Am Assoc Equine Pract 1971;17: Lees ML, Fretz PB, Bailey JV, et al: Principles of grafting. Comp Cont Educ Pract Vet 1989;11: Wilson DG: Applications of skin grafting in large animals. Probl Vet Med 1990;2: Davis JS, Trout HF: Origin and development of the blood supply of whole thickness skin grafts: An experimental study. Ann Surg 1925;82: Valencia IC, Falabella AF, Eaglestein WH: Skin grafting. Dermatol Clin 2000;18: Booth LC: Split-thickness autogenous skin transplantation in the horse. J Am Vet Med 1982;180: Moore R: Antimicrobial Therapy in Horses. p In Colahan P, Merritt AM, Moore JN, et al (eds): Equine Medicine and Surgery. 5th Ed. Mosby, St Louis, Rothstein AS: Skin grafting techniques. J Am Podiatry Assoc 1983;73: Schumacher J, Chambers M, Hanselka DV, et al: Preservation of skin by refrigeration for autogenous grafting in the horse. Vet Surg 1987;16: Gresham RB, Perry VP, Thompson VK: Practical methods of short-term storage of homografts. Arch Surg 1963;87: Allgoewer M, Blocker TGJ: Viability of skin in relation to various methods of storage. Texas Rep Bio Med J 1952;10: Smahel J: Preparation-phenomenon in a free skin graft. Br J Plast Surg 1971;24: Burleson MD, Eiseman B: Mechanism of antibacterial effect of biological dressing. Ann Surg 1973;177: Ambler J: Porcine xenografts to facilitate integumental wound healing. Vet Rec 1980;106: Diehl M, Ersek RA: Porcine xenografts for treatment of skin defects in horses. J Am Vet Med Assoc 1980;177: Diehl M, Jeanmonod CA, Muller M, et al: Porcine skin as temporary covering of extensive skin defects in the horse. Schweiz Arch Tierheilk 1979;121:23.
Pinch and punch skin grafting: something not to be scared of
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Pinch and punch skin grafting: something not to be scared of Author : Sarah Boys Smith Categories : Equine, Vets Date : October
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Pinch and punch skin grafting: something not to be scared of Author : Sarah Boys Smith Categories : Equine, Vets Date : October
SKIN GRAFTING FOR THE GENERAL EQUINE PRACTITIONER
 SKIN GRAFTING FOR THE GENERAL EQUINE PRACTITIONER Yes you can do it in the field! Sarah J. Waxman, DVM, MS, Diplomate ACVS- LA Clinician in Equine Community Practice Purdue University LEARNING OBJECTIVES
SKIN GRAFTING FOR THE GENERAL EQUINE PRACTITIONER Yes you can do it in the field! Sarah J. Waxman, DVM, MS, Diplomate ACVS- LA Clinician in Equine Community Practice Purdue University LEARNING OBJECTIVES
Principles of plastic and reconstructive surgery
 Plastic surgery - in general Principles of plastic and reconstructive surgery Dr. T. Németh, DVM, Ph.D, Diplomate ECVS Assoc. Professor and Head Definition: Surgical correction of morphological and/or
Plastic surgery - in general Principles of plastic and reconstructive surgery Dr. T. Németh, DVM, Ph.D, Diplomate ECVS Assoc. Professor and Head Definition: Surgical correction of morphological and/or
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
Benign vs. Cancer. Oculofacial Biopsy. Evolution of skin cancer. Richard E. Castillo, OD, DO
 Oculofacial Biopsy Richard E. Castillo, OD, DO Benign vs. Cancer Evolution of skin cancer Metaplasia Dysplasia Carcinoma-in-situ Invasive carcinoma Intravasation Overview Preoperative Planning Choosing
Oculofacial Biopsy Richard E. Castillo, OD, DO Benign vs. Cancer Evolution of skin cancer Metaplasia Dysplasia Carcinoma-in-situ Invasive carcinoma Intravasation Overview Preoperative Planning Choosing
7/1/2014 FUNDAMENTALS OF SKIN GRAFTING No conflicts of interest in this talk.
 FUNDAMENTALS OF SKIN GRAFTING- 2014 Superficial Anatomy and Cutaneous Surgery Course July 2014 David E. Kent, MD Clinical Instructor Division of Dermatology Georgia Health Sciences University Dermatologic
FUNDAMENTALS OF SKIN GRAFTING- 2014 Superficial Anatomy and Cutaneous Surgery Course July 2014 David E. Kent, MD Clinical Instructor Division of Dermatology Georgia Health Sciences University Dermatologic
Placing PEG and Jejunostomy Tubes in Dogs and Cats
 Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration.
 Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
From the Orthopaedic Department, St. George's Hospital Medical School, London S.W.I.
 TRANSPLANTATION OF THE NAIL: A CASE REPORT By NICHOLAS P. PAPAVASSlI.IOU, M.D. 1 From the Orthopaedic Department, St. George's Hospital Medical School, London S.W.I. THE loss of a finger nail may be of
TRANSPLANTATION OF THE NAIL: A CASE REPORT By NICHOLAS P. PAPAVASSlI.IOU, M.D. 1 From the Orthopaedic Department, St. George's Hospital Medical School, London S.W.I. THE loss of a finger nail may be of
How-To Booklet: Pediatric Spay-Neuter. Surgical Techniques Pictorial
 How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
How-To Booklet: Pediatric Spay-Neuter Surgical Techniques Pictorial Brenda Griffin, DVM, MS, DACVIM 1. Approach to Scrotal Neuter for Puppies 2. Cord Tie 3. Figure 8 Knot 4. Ovarian Pedicle Tie 5. Modified
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
ompanionport Speciality Medical Devices For The Veterinary Community Surgical Suggestions
 Speciality Medical Devices For The Veterinary Community suture holes Place the CompanionPort in the subcutaneous port pocket off to one side so that the septum of the port will not lie directly beneath
Speciality Medical Devices For The Veterinary Community suture holes Place the CompanionPort in the subcutaneous port pocket off to one side so that the septum of the port will not lie directly beneath
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE
 CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Chapter 14 8/23/2016. Surgical Wound Care. Wound Classifications. Wound Healing. Classified According to. Phases
 Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
Chapter 14 Surgical Wound Care All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Wound Classifications Classified According to Cause Incision
We are IntechOpen, the first native scientific publisher of Open Access books. International authors and editors. Our authors are among the TOP 1%
 We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
The Reverse Galeal Hinge Flap: Another Valuable Technique in the Repair of Scalp
 TITLE PAGE TITLE: The Reverse Galeal Hinge Flap: Another Valuable Technique in the Repair of Scalp Defects Extending to the Calvarium AUTHORS: Lam, Thomas, BA; Indiana University School of Medicine Miletta,
TITLE PAGE TITLE: The Reverse Galeal Hinge Flap: Another Valuable Technique in the Repair of Scalp Defects Extending to the Calvarium AUTHORS: Lam, Thomas, BA; Indiana University School of Medicine Miletta,
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Nipple-areolar complex (nac) composite grafts in the Management of macromastia: Review of complications
 Nigerian Journal of Surgical Research Vol 8 No 1 2,2006: 86-89 Short Report Nipple-areolar complex (nac) composite grafts in the Management of macromastia: Review of complications P gbenorku Plastic &
Nigerian Journal of Surgical Research Vol 8 No 1 2,2006: 86-89 Short Report Nipple-areolar complex (nac) composite grafts in the Management of macromastia: Review of complications P gbenorku Plastic &
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Fournier's gangrene: skin grafting and negative pressure dressing
 BJU International 2001 88 (1), 124 CASE REPORTS Fournier's gangrene: skin grafting and negative pressure dressing F. Schonauer, S. Grimaldi*, J.A. Pereira, G. Molea and G. Barone* Plastic Surgery Unit,
BJU International 2001 88 (1), 124 CASE REPORTS Fournier's gangrene: skin grafting and negative pressure dressing F. Schonauer, S. Grimaldi*, J.A. Pereira, G. Molea and G. Barone* Plastic Surgery Unit,
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP. By MICHAL KRAUSS. Plastic Surgery Hospital, Polanica-Zdroj, Poland
 RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
RECONSTRUCTION OF SUBTOTAL DEFECTS OF THE NOSE BY ABDOMINAL TUBE FLAP By MICHAL KRAUSS Plastic Surgery Hospital, Polanica-Zdroj, Poland RECONSTRUCTION of the nose is one of the composite procedures in
SURGICAL PROCEDURE DESCRIPTIONS
 SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
SURGICAL PROCEDURE DESCRIPTIONS GONADECTOMY: CASTRATION USING SCROTAL METHOD 1. The animal is anesthetized and placed in dorsal recumbency with the tail toward the surgeon. 2. The abdominal and scrotal
The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are
 The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are inserted in a multiplanar and multi-directional fashion
The NBX Non-Bridging External Fixator A Non-Bridging External Fixator/Locking Plate capturing a series of.062mm K-wires and 3mm half-pins that are inserted in a multiplanar and multi-directional fashion
Surgical Management of wounds, flaps, grafts, and scars
 Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
MODULE 2 THE LABORATORY RAT
 University Animal Care Committee LABORATORY ANIMAL BIOMETHODOLOGY WORKSHOP MODULE 2 THE LABORATORY RAT SUBSTANCE ADMINISTRATION AND BLOOD COLLECTION Substance Administration: Subcutaneous injection Intramuscular
University Animal Care Committee LABORATORY ANIMAL BIOMETHODOLOGY WORKSHOP MODULE 2 THE LABORATORY RAT SUBSTANCE ADMINISTRATION AND BLOOD COLLECTION Substance Administration: Subcutaneous injection Intramuscular
THE USE OF DEEPITHELIALIZATION
 THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
Human lamellar tendon graft in corneal surgery
 Human lamellar tendon graft in corneal surgery Armando Signorelli, Jr, MD, Carlos Roberto Signorelli, MD, Ernest Rifgatovich Muldashev, MD Refractive and Corneal surgery - 1993 - V.9(2) - P. 135-139 ABSTRACT
Human lamellar tendon graft in corneal surgery Armando Signorelli, Jr, MD, Carlos Roberto Signorelli, MD, Ernest Rifgatovich Muldashev, MD Refractive and Corneal surgery - 1993 - V.9(2) - P. 135-139 ABSTRACT
Fundamentals and Principles of Tissue Transfer
 4 Fundamentals and Principles of Tissue Transfer G.H. Jordan, K. Rourke 4.1 Tissue Composition and Physical Characteristics 20 4.1.1 Tissue Composition 20 4.1.2 Vascularity 21 4.1.3 Tissue Characteristics
4 Fundamentals and Principles of Tissue Transfer G.H. Jordan, K. Rourke 4.1 Tissue Composition and Physical Characteristics 20 4.1.1 Tissue Composition 20 4.1.2 Vascularity 21 4.1.3 Tissue Characteristics
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
Chapter 6: Integumentary System
 Shier, Butler, and Lewis: Hole s Human Anatomy and Physiology, 12 th ed. Chapter 6: Skin and the Integumentary System Chapter 6: Integumentary System I. Introduction 1. The skin is composed of of tissues.
Shier, Butler, and Lewis: Hole s Human Anatomy and Physiology, 12 th ed. Chapter 6: Skin and the Integumentary System Chapter 6: Integumentary System I. Introduction 1. The skin is composed of of tissues.
Case Study. TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis.
 Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
INTRA-CORNEAL LAMELLAR KERATOPLASTY*
 Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
THE WOUND SOLUTION. (Freeze dried Acellular Dermal Matrix) (Cryopreserved Acellular Dermal Matrix)
 (Freeze dried Acellular Dermal Matrix) (Cryopreserved Acellular Dermal Matrix) What is / CGCryoDerm?? /CGCryoDerm are processed by the CGBio co. and is available through Daewoong Bio. /CGCryoDerm are an
(Freeze dried Acellular Dermal Matrix) (Cryopreserved Acellular Dermal Matrix) What is / CGCryoDerm?? /CGCryoDerm are processed by the CGBio co. and is available through Daewoong Bio. /CGCryoDerm are an
Dynamics of FUE. Parsa Mohebi, MD, FISHRS I Encino, California, USA I Jeanette Straga, DO I Encino, California, USA
 Dynamics of FUE Parsa Mohebi, MD, FISHRS I Encino, California, USA I info@parsamohebi.com; Jeanette Straga, DO I Encino, California, USA ABSTRACT There are a number of basic principles that every hair
Dynamics of FUE Parsa Mohebi, MD, FISHRS I Encino, California, USA I info@parsamohebi.com; Jeanette Straga, DO I Encino, California, USA ABSTRACT There are a number of basic principles that every hair
GASTROCNEMIUS TENDON REPAIR VETLIG USING THE STIF CAT 30 SOFT TISSUE INTERNAL FIXATION VETLIG
 VETLIG SOFT TISSUE INTERNAL FIXATION GASTROCNEMIUS TENDON REPAIR USING THE STIF CAT 30 VETLIG A R T I F I C I A L L I G A M E N T S F O R V E T E R I N A R Y U S E VETLIG MANAGEMENT OF CHRONIC GASTROCNEMIUS
VETLIG SOFT TISSUE INTERNAL FIXATION GASTROCNEMIUS TENDON REPAIR USING THE STIF CAT 30 VETLIG A R T I F I C I A L L I G A M E N T S F O R V E T E R I N A R Y U S E VETLIG MANAGEMENT OF CHRONIC GASTROCNEMIUS
All surgery carries some uncertainty and risk
 Dr Mi chel s on@mi chel s onmd. com All surgery carries some uncertainty and risk While scar revision is normally safe, there is always the possibility of complications. These may include infection, bleeding,
Dr Mi chel s on@mi chel s onmd. com All surgery carries some uncertainty and risk While scar revision is normally safe, there is always the possibility of complications. These may include infection, bleeding,
WOUND CARE UPDATE. -Commonly Used Skin Substitute Products For Wound. -Total Contact Casting. Jack W. Hutter DPM, FACFAS, C. ped.
 WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
Synevovet Symposium, Bucharest October 25 th, Difficult wound closure. what works best for me. Tumour resections
 Difficult wound closure what works best for me Guenter Schwarz Dr. med. vet., Dipl. ECVS, FTA f. Kleintiere Tierklinik Hollabrunn A-2020 Hollabrunn www.tierklinik-hollabrunn.at g.schwarz@tierklinik-hollabrunn.at
Difficult wound closure what works best for me Guenter Schwarz Dr. med. vet., Dipl. ECVS, FTA f. Kleintiere Tierklinik Hollabrunn A-2020 Hollabrunn www.tierklinik-hollabrunn.at g.schwarz@tierklinik-hollabrunn.at
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Carpal Tunnel Release
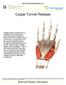 Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Anatomy Ch 6: Integumentary System
 Anatomy Ch 6: Integumentary System Introduction: A. Organs are body structures composed of two or more different tissues. B. The skin and its accessory organs make up the integumentary system. Types of
Anatomy Ch 6: Integumentary System Introduction: A. Organs are body structures composed of two or more different tissues. B. The skin and its accessory organs make up the integumentary system. Types of
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
Chapter 6: Skin and the Integumentary System
 Shier, Butler, and Lewis: Hole s Human Anatomy and Physiology, 10 th ed. Chapter 6: Skin and the Integumentary System Chapter 6: Skin and the Integumentary System I. Skin and Its Tissues A. Introduction
Shier, Butler, and Lewis: Hole s Human Anatomy and Physiology, 10 th ed. Chapter 6: Skin and the Integumentary System Chapter 6: Skin and the Integumentary System I. Skin and Its Tissues A. Introduction
Hole s Essentials of Human Anatomy & Physiology
 Hole s Essentials of Human Anatomy & Physiology David Shier Jackie Butler Ricki Lewis Created by Dr. Melissa Eisenhauer Head Athletic Trainer/Assistant Professor Trevecca Nazarene University Chapter 6
Hole s Essentials of Human Anatomy & Physiology David Shier Jackie Butler Ricki Lewis Created by Dr. Melissa Eisenhauer Head Athletic Trainer/Assistant Professor Trevecca Nazarene University Chapter 6
Burn & Soft Tissue Service Orientation Slides
 Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
SAMPLE. HLTEN406A Undertake basic wound care. Learner resource. HLT07 Health Training Package. Version 2
 HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Expanded Transposition Flap Technique for Total and Subtotal Resurfacing of the Face and Neck
 Expanded Transposition Flap Technique for Total and Subtotal Resurfacing of the Face and Neck Robert J. Spence, MD, FACS Johns Hopkins School of Medicine, Baltimore, MD Correspondence: rspence@jhmi.edu
Expanded Transposition Flap Technique for Total and Subtotal Resurfacing of the Face and Neck Robert J. Spence, MD, FACS Johns Hopkins School of Medicine, Baltimore, MD Correspondence: rspence@jhmi.edu
Strength and Predictability. Zimmer Collagen Repair Patch
 Strength and Predictability Zimmer Collagen Repair Patch Durable Reinforcement The Zimmer Collagen Repair Patch is a biological implant consisting of an acellular scaffold of collagen and elastin, derived
Strength and Predictability Zimmer Collagen Repair Patch Durable Reinforcement The Zimmer Collagen Repair Patch is a biological implant consisting of an acellular scaffold of collagen and elastin, derived
Surgical Technique. Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix. conexatm. Surgical Technique Described by Tom Chang, DPM
 Surgical Technique Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix Surgical Technique Described by Tom Chang, DPM conexatm r e c o n s t r u c t i v e t i s s u e m a t r i x Achilles
Surgical Technique Achilles Tendon Repair Using Conexa Reconstructive Tissue Matrix Surgical Technique Described by Tom Chang, DPM conexatm r e c o n s t r u c t i v e t i s s u e m a t r i x Achilles
TRANSPOSITIONAL ADIPOFASCIAL FLAPS FOR COMPLICATED ACUTE FINGER INJURIES
 K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress RECONSTRUCTIVE SURGERY I: LOCAL FLAPS Bryden J. Stanley, BVMS, MACVSc, MVetSc, Diplomate ACVS College of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress RECONSTRUCTIVE SURGERY I: LOCAL FLAPS Bryden J. Stanley, BVMS, MACVSc, MVetSc, Diplomate ACVS College of Veterinary
DISTANT FLAPS KEY FIGURES:
 Chapter 14 DISTANT FLAPS KEY FIGURES: Chest flap Cross arm flap Cross leg flap Design of groin flap Examples of groin flap Examples of free flaps A distant flap involves moving tissue (skin, fascia, muscle,
Chapter 14 DISTANT FLAPS KEY FIGURES: Chest flap Cross arm flap Cross leg flap Design of groin flap Examples of groin flap Examples of free flaps A distant flap involves moving tissue (skin, fascia, muscle,
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
INFORMED-CONSENT-SKIN GRAFT SURGERY
 INFORMED-CONSENT-SKIN GRAFT SURGERY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
INFORMED-CONSENT-SKIN GRAFT SURGERY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY
 NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
Wound Management for Nurses/Technicians What do we need to know?
 Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft
 Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Integumentary System
 Chapter 5 Integumentary System 5-1 Skin: composed of dermis and epidermis Dermis. Gives structural strength. C.T. with many fibers, fibroblasts, macrophages. Some adipocytes and blood vessels. Contains
Chapter 5 Integumentary System 5-1 Skin: composed of dermis and epidermis Dermis. Gives structural strength. C.T. with many fibers, fibroblasts, macrophages. Some adipocytes and blood vessels. Contains
frontalis muscle while the patient makes an attempt to open the eye. With the first and third classes I am not now concerned, except
 OPERATION FOR THE RELIEF OF CONGENITAL PTOSIs 741 AN OPERATION FOR THE RELIEF OF CONGENITAL PTOSIS* BY R. AFFLECK GREEVES LONDON CASES of congenital ptosis may be conveniently divided, clinically, into
OPERATION FOR THE RELIEF OF CONGENITAL PTOSIs 741 AN OPERATION FOR THE RELIEF OF CONGENITAL PTOSIS* BY R. AFFLECK GREEVES LONDON CASES of congenital ptosis may be conveniently divided, clinically, into
micromend Skin Closure Device Pre-clinical Studies of Closure of Surgical Wounds in Live Pigs
 micromend Skin Closure Device Pre-clinical Studies of Closure of Surgical Wounds in Live Pigs RONALD BERENSON, M.D. and PAUL LEUNG, M.S. EXECUTIVE SUMMARY KitoTech Medical has developed a revolutionary
micromend Skin Closure Device Pre-clinical Studies of Closure of Surgical Wounds in Live Pigs RONALD BERENSON, M.D. and PAUL LEUNG, M.S. EXECUTIVE SUMMARY KitoTech Medical has developed a revolutionary
Articular Cartilage Resurfacing Single Osteochondral Allograft Plug Surgical Technique
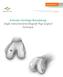 Articular Cartilage Resurfacing Single Osteochondral Allograft Plug Surgical Technique PATIENT CONDYLE PREPARATION Step 1: Perform a parapatellar arthrotomy, and retract the patella to expose the condyle.
Articular Cartilage Resurfacing Single Osteochondral Allograft Plug Surgical Technique PATIENT CONDYLE PREPARATION Step 1: Perform a parapatellar arthrotomy, and retract the patella to expose the condyle.
PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA
 PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA Pages with reference to book, From 72 To 76 Mohammad Arshad Cheema ( Department of Surgery,
PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA Pages with reference to book, From 72 To 76 Mohammad Arshad Cheema ( Department of Surgery,
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
LESSON ASSIGNMENT. Urinary System Diseases/Disorders. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
LESSON ASSIGNMENT LESSON 4 Urinary System Diseases/Disorders LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 4-1. Identify the purposes
Ophthalmology Wet Lab Notes - Kimberly Hsu, DVM, MSc, DACVO
 Ophthalmology Wet Lab Notes - Kimberly Hsu, DVM, MSc, DACVO If you have questions, please do not hesitate to call Dr. Hsu at Eye Care for Animals, St. Charles at 630-444-0393 or email at stcharlesinfo@eyecareforanimals.com
Ophthalmology Wet Lab Notes - Kimberly Hsu, DVM, MSc, DACVO If you have questions, please do not hesitate to call Dr. Hsu at Eye Care for Animals, St. Charles at 630-444-0393 or email at stcharlesinfo@eyecareforanimals.com
Objectives. Major Changes to Section M. MDS 3.0 Section M Pressure Ulcers. Risk assessment Introduction of NPUAP guidelines
 MDS 3.0 Section M Pressure Ulcers Moderator: Barbara Baylis Sr. VP of Clinical and Residential Services, Kindred Healthcare Presenter: Glenda Mack, Sr. Director of Clinical Operations, Peoplefirst Rehabilitation
MDS 3.0 Section M Pressure Ulcers Moderator: Barbara Baylis Sr. VP of Clinical and Residential Services, Kindred Healthcare Presenter: Glenda Mack, Sr. Director of Clinical Operations, Peoplefirst Rehabilitation
17 Follicular Unit Extraction
 In: Haber RS, Stough DB, editors: Hair Transplantation, Chapter 17. Elsevier Saunders, 2006: 133-137. 2006, Elsevier Inc 17 Follicular Unit Extraction William R. Rassman, James A. Harris, Robert M. Bernstein
In: Haber RS, Stough DB, editors: Hair Transplantation, Chapter 17. Elsevier Saunders, 2006: 133-137. 2006, Elsevier Inc 17 Follicular Unit Extraction William R. Rassman, James A. Harris, Robert M. Bernstein
THE HUMERUS 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW
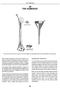 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A.
 UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
Surgery/Integumentary System ( )
 10030 The provider inserts a catheter through the skin using imaging to view the fluid. He then drains the fluid from the soft tissue in cases such as abscess, hematoma, seroma, lymphocele, or cyst. Imaging
10030 The provider inserts a catheter through the skin using imaging to view the fluid. He then drains the fluid from the soft tissue in cases such as abscess, hematoma, seroma, lymphocele, or cyst. Imaging
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
Extracapsular Repair Monofilament Nylon Suture
 Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
ACL Reconstruction for BTB Grafts
 Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
THAL EQUINE LLC Regional Equine Hospital Horse Owner Education & Resources Santa Fe, New Mexico
 THAL EQUINE LLC Regional Equine Hospital Horse Owner Education & Resources Santa Fe, New Mexico 505-438-6590 www.thalequine.com Equine Wounds: What Horse Owners Should Know Wounds are one of the most common
THAL EQUINE LLC Regional Equine Hospital Horse Owner Education & Resources Santa Fe, New Mexico 505-438-6590 www.thalequine.com Equine Wounds: What Horse Owners Should Know Wounds are one of the most common
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
TABLE OF CONTENTS. 2 (8144 Rev 2)
 1 (8144 Rev 2) TABLE OF CONTENTS Introduction Conventus CAGE TM - Proximal Humerus...3 Indications and Contraindications...4 Surgical Summary...5 Patient Positioning & Approach...6 Surgical Technique Plate
1 (8144 Rev 2) TABLE OF CONTENTS Introduction Conventus CAGE TM - Proximal Humerus...3 Indications and Contraindications...4 Surgical Summary...5 Patient Positioning & Approach...6 Surgical Technique Plate
South West Regional Wound Care Toolkit F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE)
 F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE) F.5 SURGICAL WOUND (CLOSED AND OPEN) 5.1 Background to Etiology Closed surgical wounds are well-approximated with a palpable healing ridge
F. PRINCIPLES OF TREATMENT BASED ON ETIOLOGY (TREAT THE CAUSE) F.5 SURGICAL WOUND (CLOSED AND OPEN) 5.1 Background to Etiology Closed surgical wounds are well-approximated with a palpable healing ridge
FOR THE SERVICE MEMBER: Rx3 REHABILITATION PROGRAM
 CREATED BY THE HUMAN PERFORMANCE RESOURCE CENTER / HPRC-ONLINE.ORG / FROM THE CONSORTIUM FOR HEALTH AND MILITARY PERFORMANCE HUMAN PERFORMANCE RESOURCE CENTER Injury/Condition: Injury/Condition: What is
CREATED BY THE HUMAN PERFORMANCE RESOURCE CENTER / HPRC-ONLINE.ORG / FROM THE CONSORTIUM FOR HEALTH AND MILITARY PERFORMANCE HUMAN PERFORMANCE RESOURCE CENTER Injury/Condition: Injury/Condition: What is
Chapter 23 Caring for Clients with Burns
 Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
MULTIFIX S Knotless Implants
 Technique Guide MULTIFIX S Knotless Implants The MULTIFIX S system offers 5.5mm and 6.5mm knotless, all-peek, poundin implants. The system provides multiple fixation options, a streamlined technique, and
Technique Guide MULTIFIX S Knotless Implants The MULTIFIX S system offers 5.5mm and 6.5mm knotless, all-peek, poundin implants. The system provides multiple fixation options, a streamlined technique, and
Chapter 11 Worksheet Code It
 Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
ATI Skills Modules Checklist for Central Venous Access Devices
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden
 A NEW METHOD OF SHAPING DEFORMED EARS By A. RAGNELL, M.D. Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden NUMEROUS methods of shaping
A NEW METHOD OF SHAPING DEFORMED EARS By A. RAGNELL, M.D. Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden NUMEROUS methods of shaping
