Aging Well. Vol. 2 No. 2 P. 16, January/February Cognitive Camouflage How Alzheimer s Can Mask Mental Illness
|
|
|
- Clara Francis
- 6 years ago
- Views:
Transcription
1 Aging Well Vol. 2 No. 2 P. 16, January/February 2009 Cognitive Camouflage How Alzheimer s Can Mask Mental Illness By Michael B. Friedman, LMSW; Gary J. Kennedy, MD; and Kimberly A. Williams, LMSW It s not unusual for mental illness, particularly depression, to occur in the early stages of Alzheimer s disease. But accurate diagnosis and treatment can improve cognitive function. When he was in his early 70s, Frank, a successful and active lawyer, began to notice a significant deterioration in his memory and ability to think clearly. It wasn t just that he forgot names that had been occurring for years. He couldn t recall legal precedents that had been at the center of his work for nearly 50 years. He forgot appointments. He got lost on his way to a meeting at a place he had been to many times before. He wasn t surprised when his doctor said he might have Alzheimer s disease (AD), but the diagnosis put him into a funk. He felt his life was now hopeless because he would become increasingly disabled and dependent. Death would be a blessing, he thought. He was consumed by such thoughts, unable to concentrate on his work, and distracted when he was with his wife, children, grandchildren, or friends. He slept less and less. Fortunately, his physician recognized that Frank was depressed and persuaded him to go into therapy. He found a therapist who understood how to treat an individual with a combination of AD and depression. He involved Frank s wife in the process and offered suggestions on ways to be helpful to her husband. With the combination of cognitive-behavioral therapy and psychoeducation, Frank s depression lifted a bit. He was able to retire gracefully with his reputation intact. He rediscovered an old interest in music, and he was able to respond to care and affection from his family long after his capacity to speak had passed. For him, as for most older adults with AD, love was the last memory to die. AD took its inevitable toll, but overcoming his depression gave Frank some additional time to live as he wanted and helped him prepare emotionally for the gradual decline into a life that he had previously dreaded. It wasn t easy for Frank or his wife or their daughter, who also helped out. It never is. But their emotional bond carried them through the difficult times. Frank and his family were fortunate to have a physician who could distinguish between the effects of AD and the effects of depression. Frequently, that s not the case. It was also fortuitous to locate a therapist who had expertise in the mental disorders of older adults. Most do not. As the population of older adults explodes over the next 25 years, more elders will have similar problems, but very few will receive the skilled treatment they need. An Alzheimer s disease (AD) diagnosis is usually greeted as a death sentence and with good reason. The disease grows progressively worse and currently cannot be reversed or even stopped, although it can be slowed in some cases. In 2006, it was the sixth leading cause of death, according to the Centers for Disease Control and Prevention (CDC).
2 But awareness of the ultimate outcome of AD often blinds people to the fact that, before reaching the end stage, elders with AD can engage in activities they find meaningful and maintain caring and pleasurable relationships. In addition, an AD diagnosis frequently results in the failure to recognize that cognitive problems may have other often treatable causes. Among these are other mental illnesses especially depression that are quite common among older adults in the early and midstages of AD. With accurate diagnosis and appropriate treatment, cognitive functioning often improves. The course of AD cannot be reversed, but life can be better at least for a time. Frightening Facts AD is the most common, but not the only form, of dementia and occurs in 6% to 7% of the U.S. population aged 55 and older. The prevalence increases with age to more than 40% by the age of 85. As the population of older adults doubles over the next quarter century, so will the number of older adults with dementia. AD is a progressive disorder. Although it can t be reversed or arrested, medications are available to slow its progress. It disrupts memory, thought, perception of reality, and behavior to such a degree that eventually it impairs the ability to work, engage in normal adult relationships, participate in ordinary social and leisure activities, carry out basic tasks such as shopping or paying bills, and ultimately manage basic activities of daily living, such as eating, toileting, and dressing. The early signs forgetting a recent event, neglecting to pay a bill, not recalling a friend s name are often indistinguishable from typical senior moments. To the older adults experiencing them, their families and friends, and their healthcare providers, they may seem like minor problems and a normal part of aging. As time passes, however, the cognitive dysfunction worsens, and the disease becomes more obvious and problematic, both for the individuals and those who care about and, increasingly, for them. The caregiver burden can become tremendous, with mental, physical, and financial consequences. Families and friends who care for older adults with AD are at increased risk for depression, anxiety disorders, and physical illness. Many family caregivers manage to persevere despite the stress, but many burn out and, understandably, place family members in institutions to relieve themselves of the burden. Mental Illness With AD The inherent difficulty of living with AD is exacerbated when it co-occurs with other mental disorders such as depression, anxiety disorders, and psychotic conditions. Serious symptoms of depression occur in up to 50% of older adults with AD, and major depression occurs in roughly 25% of cases, according to the CDC. Depression is often thought to be an older adult s reaction due to awareness of progressive decline, and this is probably the case. However, some research suggests that there may be a biological connection between AD and depression. Anxiety disorders, including generalized nervousness, fear of leaving home, agitation about changes of routine, and suspiciousness sometimes to paranoia proportions are also common, occurring in up to 30% of older adults with AD. Anxiety seems easily understandable in older adults who are aware of their diminishing abilities. But it is possible that, like depression, it may be physically, as well as psychologically, linked to AD.
3 AD can also co-occur with psychotic conditions. Older adults with schizophrenia, for example, are as likely to develop AD as those without severe mental illness. And individuals with schizophrenia in old age are at higher risk for depression, creating the possibility of all three co-occurring mental disorders. Symptoms of these disorders include the following: profound sadness; hopelessness; disinterest in people and activities that have previously been a source of pleasure; irritability; anxiety about change, strangers, going out, etc.; suspiciousness or even paranoid ideas; sleep disturbances; agitation; restlessness; aggression; pacing or immobility; delusions; hallucinations; and various behaviors that are dangerous or distressing to others, including hoarding, verbal or physical abusiveness, and refusal to cooperate. Such symptoms often have negative consequences for elders with AD and those who care for them. These include the following: the subjective distress of the person experiencing such symptoms; inability to participate in satisfying activities and relationships; increased disability and mortality; heightened caregiver burden; heightened risk of depression, anxiety disorders, and physical illness in caregivers; and earlier placement in institutions despite the preference of both the older adults with AD and their families for them to remain in community settings. While suicide does not appear to be more prevalent for older adults with AD than other elders, its risk should not be ignored. Fortunately, treatment of these disorders often results in improved functioning and quality of life for both the older adults with the disorders and their family caregivers. Differential Diagnosis Signs of depression include not only sadness and loss of interest in life, but can also include
4 cognitive impairments such as memory loss, difficulty concentrating, slow information processing, inability to think clearly, and distorted views of reality. Because these depression symptoms are so similar to dementia symptoms, the two disorders are frequently confused, especially when an AD diagnosis has already been made. Therefore, a good differential diagnosis is critical but not easy. Symptoms of AD that are not common in depression include forgetting recently learned information, trouble performing once-familiar tasks, problems with remembering words, and impaired judgment, such as not perceiving the need to dress warmly in severe winter weather. Screening tools can be helpful in distinguishing depression from AD. The Mini-Mental State Examination and the clock test are useful for revealing dementia. Depression scales include Patient Health Questionnaires 2 and 9 and the Geriatric Depression Scale, all of which can be easily administered unless dementia is fairly advanced, in which case interviewing family members and caregivers is essential, though not totally reliable. Effective Interventions Because there has been little research on the treatment of depression or anxiety in older adults with AD, there are no formally established, evidence-based practices. However, widespread consensus among experts in geriatric mental health is that there are effective interventions for depression and anxiety, sleep disturbances, and behavior problems. Depression and anxiety can be treated effectively in older adults with and without AD. However, in older adults with AD, it needs to be approached differently from those without. In particular, it is important to begin with nonpharmacological interventions directed both at the patient and the caregiver to avoid the risks associated with antidepressant and antipsychotic medication use in older adults with AD. Such risks include falls the major cause of disability in old age severe weight loss and malnutrition, and increased confusion. Except in cases of very severe depression, antidepressants should be prescribed only after sufficient time has elapsed for the nonpharmacological interventions to succeed. And for frail older adults, electroconvulsive therapy should be used only as a last resort. Nonpharmacological interventions can be as simple as providing pleasant activities, a normal routine, and exercise. Behavioral interventions and environmental modifications can help reduce anxiety, agitation, and hopelessness. In addition, formal cognitive behavioral therapy can be effective. And providing psychoeducation for caregivers can help them better deal with the elder with AD, which may have a positive impact on the individual s mood and general frame of mind. Sleep disturbances are quite common among older adults with AD, especially those with cooccurring depression. Treatment for depression often results in improved sleeping. But there are also specific psychosocial interventions such as sleep restriction, sleep compression, multicomponent cognitive-behavioral therapy, and stimulus control that are quite effective. Promising interventions include muscle relaxation and sleep hygiene education. Very cautious use of sedative/hypnotics should be considered only when behavioral treatments are not effective. Behavior Problems In addressing problem behaviors, it is important for informal and formal caregivers and for healthcare and mental health providers to understand that problematic behavior is not
5 inherent in the patient, but rather is a problem in the interaction between the older adult with AD and the caregiver. Caregivers who develop insight into the experience of the elder for whom they re caring, who cultivate tolerance and patience, and who retain a sense of the humanity and dignity of the elder are likely to fare better than those who do not have these qualities. Although not all experts agree, it may be particularly important for caregivers to be aware that not all mental functions decline as cognitive functions diminish. It may be that some people become more emotionally open and caring and that some develop more interest in creative activities such as music, art, and poetry. Affectionate, often nonverbal interactions may occur, and engagement in the arts may become more satisfying. In addition, individually tailored behavioral management techniques such as antecedentbehavior-consequence interventions, where caregivers recognize the behavior, identify antecedents, and modify their reaction, the physical environment, and/or the older adult s routine, can be very effective at reducing problem behaviors when practiced with consistency. Environmental modifications such as changing the visual environment, using mirrors, posting signs, and unlocking doors for a period of time on closed wards can also be effective. There is also emerging evidence of the effectiveness of aromatherapy and bright light therapy for reducing agitation. When behaviors are more severe or fail to respond to such nonpharmacological approaches, atypical antipsychotics may be considered. However, due to risks of enervation, clouded thinking and perception, falls, and premature mortality, they should be prescribed with great caution and monitored carefully. Addressing the Needs of Family Caregivers Family members are the most common caregivers for older adults with disabilities, including AD. They provide about 80% of all care at great cost to themselves and great savings to society. The financial value of the care they provided was about $375 billion in 2007 the equivalent of nearly 20% of all healthcare costs in the United States, according to the CDC. The stress borne by caregivers makes them highly vulnerable to depression, anxiety disorders, and physical illness. Many become overburdened, and some burn out. While not all need support, many can benefit from interventions such as psychoeducation, counseling, support groups, and respite. Mary Mittelman, DPH, a research professor at New York University s School of Medicine, has conducted research indicating that a combination of individual and family therapy, support groups, and ad hoc counseling for spousal caregivers reduces depression, anxiety, and physical illness in caregivers of older adults with AD and can delay nursing home placement by up to 18 months. Caregivers mental health also may benefit from behavioral management therapy for the elder with AD, as well as from learned coping strategies. Care and Treatment Settings Most older adults with AD receive treatment on an outpatient basis either in treatment settings or their homes. Some, however, live in residential care settings such as assisted living facilities, life care communities, and nursing homes.
6 For many, paid caregivers who come to the home, such as personal care attendants, home health aides, and case managers, make remaining at home possible. Unfortunately, many of these workers, despite their caring and skill in attending to physical needs, are not skilled in managing behaviors that can be troublesome or in identifying and responding to other mental disorders. Some elders with AD receive care and have opportunities for activity and social interaction in day programs, including senior centers, social adult day care, and adult medical day care. These programs also function as a kind of respite service for family caregivers who work during the day. Unfortunately, it s not common in such programs to have staff with expertise in mental conditions such as depression, which, as previously noted, can make life far worse for older adults with AD. Over the past several decades, there has been an increase in numbers of older adults moving to assisted living facilities, many of which have special programs or units for people with advanced dementia. Unfortunately, there is rarely much expertise in co-occurring mental disorders at such facilities. Finally, of course, a significant number of older adults with AD go to nursing homes. While some of these facilities provide good care for people with co-occurring mental and behavioral disorders, many do not. There are grave concerns about inadequate attention to mental conditions and the overuse of antipsychotic medications, which can induce stupor and hasten death. Future Directions Although much has been learned about AD over the past few decades and treatment and other interventions have become more effective, the sad facts include the following: We do not know how to reverse, stop, or even substantially slow AD s progressive decline. AD takes a terrible toll, not only on the older adults who develop the disease, but also on their families and friends. There are also enormous costs to society, not only for care and treatment, but also in lost productivity of both elders with AD and their families. Unfortunately, health, mental health, and aging services policies in the United States are not adequately responsive to these facts. Fundamental policy changes are needed, including enhanced research to develop and document effective interventions and enhanced translation of research findings into practice. Also critical are enhancing the quality of care in outpatient, home, community, and residential settings, as well as increasing training and education to build a health, mental health, and aging services workforce competent to meet the needs of older adults with co-occurring mental illnesses and their families. Additional focus needs to be directed toward enhanced family support, expansion of affordable services, expansion of affordable residential alternatives to institutions, and enhanced integration of mental health and long-term care services. Ultimately, bringing about the kinds of policy changes necessary to meet the needs of older adults with AD will depend on building political will. Unfortunately, we have a long way to go in that direction.
7 Michael B. Friedman, LMSW, is chair of the Geriatric Mental Health Alliance of New York. Gary J. Kennedy, MD, is director of the division of geriatric psychiatry at Montefiore Medical Center in New York City. Kimberly A. Williams, LMSW, is director of the Geriatric Mental Health Alliance of New York.
Session outline. Introduction to dementia Assessment of dementia Management of dementia Follow-up Review
 Dementia 1 Session outline Introduction to dementia Assessment of dementia Management of dementia Follow-up Review 2 Activity 1: Person s story Present a person s story of what it feels like to live with
Dementia 1 Session outline Introduction to dementia Assessment of dementia Management of dementia Follow-up Review 2 Activity 1: Person s story Present a person s story of what it feels like to live with
ADDRESSING THE MENTAL HEALTH NEEDS OF OLDER ADULTS IN AGE-FRIENDLY COMMUNITIES A Guide for Planners
 Geriatric Mental Health Alliance Of New York ADDRESSING THE MENTAL HEALTH NEEDS OF OLDER ADULTS IN AGE-FRIENDLY COMMUNITIES A Guide for Planners By Kimberly A. Williams Michael B. Friedman January 2010
Geriatric Mental Health Alliance Of New York ADDRESSING THE MENTAL HEALTH NEEDS OF OLDER ADULTS IN AGE-FRIENDLY COMMUNITIES A Guide for Planners By Kimberly A. Williams Michael B. Friedman January 2010
HELPING A PERSON WITH SCHIZOPHRENIA
 HELPING A PERSON WITH SCHIZOPHRENIA OVERCOMING CHALLENGES WHILE TAKING CARE OF YOURSELF The love and support of family plays an important role in schizophrenia treatment and recovery. If someone close
HELPING A PERSON WITH SCHIZOPHRENIA OVERCOMING CHALLENGES WHILE TAKING CARE OF YOURSELF The love and support of family plays an important role in schizophrenia treatment and recovery. If someone close
In-Service Education. workbook 3. by Hartman Publishing, Inc. second edition
 In-Service Education workbook 3 second edition by Hartman Publishing, Inc. Alzheimer s Disease Dignity Diabetes Restraints and Restraint Alternatives Abuse and Neglect Death and Dying Managing Stress Perf
In-Service Education workbook 3 second edition by Hartman Publishing, Inc. Alzheimer s Disease Dignity Diabetes Restraints and Restraint Alternatives Abuse and Neglect Death and Dying Managing Stress Perf
GERIATRIC SERVICES CAPACITY ASSESSMENT DOMAIN 5 - CAREGIVING
 GERIATRIC SERVICES CAPACITY ASSESSMENT DOMAIN 5 - CAREGIVING Table of Contents Introduction... 2 Purpose... 2 Serving Senior Medicare-Medicaid Enrollees... 2 How to Use This Tool... 2 5 Caregiving... 3
GERIATRIC SERVICES CAPACITY ASSESSMENT DOMAIN 5 - CAREGIVING Table of Contents Introduction... 2 Purpose... 2 Serving Senior Medicare-Medicaid Enrollees... 2 How to Use This Tool... 2 5 Caregiving... 3
Recognition and Management of Behavioral Disturbances in Dementia
 Recognition and Management of Behavioral Disturbances in Dementia Danielle Hansen, DO, MS (Med Ed), MHSA INTRODUCTION 80% 90% of patients with dementia develop at least one behavioral disturbances or psychotic
Recognition and Management of Behavioral Disturbances in Dementia Danielle Hansen, DO, MS (Med Ed), MHSA INTRODUCTION 80% 90% of patients with dementia develop at least one behavioral disturbances or psychotic
Introduction to Dementia: Complications
 Introduction to Dementia: Complications Created in March 2005 Duration: about 15 minutes Axel Juan, MD The Geriatrics Institute axel.juan@med.va.gov 305-575-3388 Credits Principal medical contributor:
Introduction to Dementia: Complications Created in March 2005 Duration: about 15 minutes Axel Juan, MD The Geriatrics Institute axel.juan@med.va.gov 305-575-3388 Credits Principal medical contributor:
Depression: More than just the blues
 Depression: More than just the blues August 2011 Knowing When to Get Help Is it depression? How do you know if you re depressed? That s a good question! Depression can be a byproduct of stress and anxiety.
Depression: More than just the blues August 2011 Knowing When to Get Help Is it depression? How do you know if you re depressed? That s a good question! Depression can be a byproduct of stress and anxiety.
10 steps to planning for Alzheimer s disease & other dementias A guide for family caregivers
 10 steps to planning for Alzheimer s disease & other dementias A guide for family caregivers Caring for a person with memory loss or dementia can be challenging. The following ten steps can help caregivers
10 steps to planning for Alzheimer s disease & other dementias A guide for family caregivers Caring for a person with memory loss or dementia can be challenging. The following ten steps can help caregivers
Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego
 Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
This information explains the advice about supporting people with dementia and their carers that is set out in NICE SCIE clinical guideline 42.
 Supporting people with dementia and their carers Information for the public Published: 1 November 2006 nice.org.uk About this information NICEclinicalguidelinesadvisetheNHSoncaringforpeoplewithspe cificconditionsordiseasesandthetreatmentstheyshouldreceive.
Supporting people with dementia and their carers Information for the public Published: 1 November 2006 nice.org.uk About this information NICEclinicalguidelinesadvisetheNHSoncaringforpeoplewithspe cificconditionsordiseasesandthetreatmentstheyshouldreceive.
Research & Policy Brief
 USM Muskie School of Public Service Maine DHHS Office of Elder Services Research & Policy Brief Caring for People with Alzheimer s Disease or Dementia in Maine A Matter of Public Health Alzheimer s disease
USM Muskie School of Public Service Maine DHHS Office of Elder Services Research & Policy Brief Caring for People with Alzheimer s Disease or Dementia in Maine A Matter of Public Health Alzheimer s disease
10/17/2017. Causes of Dementia Alzheimer's Disease Vascular Dementia Diffuse Lewy Body Disease Alcoholic Dementia Fronto-Temporal Dementia Others
 1 Dementia Dementia comes from the Latin word demens, meaning out of mind. It is the permanent loss of multiple intellectual functions. It is progressive deterioration of mental powers accompanied by changes
1 Dementia Dementia comes from the Latin word demens, meaning out of mind. It is the permanent loss of multiple intellectual functions. It is progressive deterioration of mental powers accompanied by changes
If you have dementia, you may have some or all of the following symptoms.
 About Dementia Dementia may be caused by a number of illnesses that affect the brain. Dementia typically leads to memory loss, inability to do everyday things, difficulty in communication, confusion, frustration,
About Dementia Dementia may be caused by a number of illnesses that affect the brain. Dementia typically leads to memory loss, inability to do everyday things, difficulty in communication, confusion, frustration,
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION
 ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
Delirium Information for patients and relatives. Delirium is common Delirium is treatable Relatives can stay to help us
 Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Dementia and Fall Geriatric Interprofessional Training. Wael Hamade, MD, FAAFP
 Dementia and Fall Geriatric Interprofessional Training Wael Hamade, MD, FAAFP Prevalence of Dementia Age range 65-74 5% % affected 75-84 15-25% 85 and older 36-50% 5.4 Million American have AD Dementia
Dementia and Fall Geriatric Interprofessional Training Wael Hamade, MD, FAAFP Prevalence of Dementia Age range 65-74 5% % affected 75-84 15-25% 85 and older 36-50% 5.4 Million American have AD Dementia
Post-Traumatic Stress Disorder
 Post-Traumatic Stress Disorder Teena Jain 2017 Post-Traumatic Stress Disorder What is post-traumatic stress disorder, or PTSD? PTSD is a disorder that some people develop after experiencing a shocking,
Post-Traumatic Stress Disorder Teena Jain 2017 Post-Traumatic Stress Disorder What is post-traumatic stress disorder, or PTSD? PTSD is a disorder that some people develop after experiencing a shocking,
Management of Behavioral Symptoms in Dementia. Brenda Jordan, MS, ARNP, BC- PCM Dartmouth-Hitchcock Kendal
 Management of Behavioral Symptoms in Dementia Brenda Jordan, MS, ARNP, BC- PCM Dartmouth-Hitchcock Kendal Behavioral Symptoms Common & troubling At least one will occur in 61-92% of those with any dementia
Management of Behavioral Symptoms in Dementia Brenda Jordan, MS, ARNP, BC- PCM Dartmouth-Hitchcock Kendal Behavioral Symptoms Common & troubling At least one will occur in 61-92% of those with any dementia
Communication with Cognitively Impaired Clients For CNAs
 Communication with Cognitively Impaired Clients For CNAs This course has been awarded one (1.0) contact hour. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction
Communication with Cognitively Impaired Clients For CNAs This course has been awarded one (1.0) contact hour. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction
Contemporary Psychiatric-Mental Health Nursing. Descriptive Terms. Healthy Elders. Chapter 28
 Contemporary Psychiatric-Mental Health Nursing Chapter 28 Elders Descriptive Terms Young-old (65 to 74) Middle-old (75 to 84) Old-old (85+) Frail old (65+ with chronic limitations) 5% of the over-65 population
Contemporary Psychiatric-Mental Health Nursing Chapter 28 Elders Descriptive Terms Young-old (65 to 74) Middle-old (75 to 84) Old-old (85+) Frail old (65+ with chronic limitations) 5% of the over-65 population
Know the 10 Signs: Early Detection Matters
 Know the 10 Signs: Early Detection Matters 1 Importance of Early Detection If we could have had a correct diagnosis even two years earlier, it would have given us more time to plan, to do the things that
Know the 10 Signs: Early Detection Matters 1 Importance of Early Detection If we could have had a correct diagnosis even two years earlier, it would have given us more time to plan, to do the things that
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017.
 DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
Living in the Community with a Diagnosis of Dementia
 Living in the Community with a Diagnosis of Dementia Tara A. Cortes PhD,RN,FAAN Executive Director and Professor The Hartford Institute for Geriatric Nursing, NYU College of Nursing 2014 Primary Care Symposium
Living in the Community with a Diagnosis of Dementia Tara A. Cortes PhD,RN,FAAN Executive Director and Professor The Hartford Institute for Geriatric Nursing, NYU College of Nursing 2014 Primary Care Symposium
Risks of Antipsychotics use In Dementia
 AHCA/NCAL Quality Initiative for Assisted Living Webinar Series: Safely Reducing the Off-Label Use of Antipsychotics Risks of Antipsychotics use In Dementia Sanjay P. Singh, MD Chairman & Professor, Department
AHCA/NCAL Quality Initiative for Assisted Living Webinar Series: Safely Reducing the Off-Label Use of Antipsychotics Risks of Antipsychotics use In Dementia Sanjay P. Singh, MD Chairman & Professor, Department
Early Warning Signs of Psychotic Disorders and the Importance of Early Intervention
 Early Warning Signs of Psychotic Disorders and the Importance of Early Intervention Margaret Migliorati, MA, LPCC The University of New Mexico mmigliorati@salud.unm.edu Mental Health As a Public Health
Early Warning Signs of Psychotic Disorders and the Importance of Early Intervention Margaret Migliorati, MA, LPCC The University of New Mexico mmigliorati@salud.unm.edu Mental Health As a Public Health
Session outline. Introduction to depression Assessment of depression Management of depression Follow-up Review
 Depression 1 Session outline Introduction to depression Assessment of depression Management of depression Follow-up Review 2 Activity 1: Person s story followed by group discussion Present the first person
Depression 1 Session outline Introduction to depression Assessment of depression Management of depression Follow-up Review 2 Activity 1: Person s story followed by group discussion Present the first person
Dementia Facts and Resources Dementia Warning Signs Getting a Diagnosis Dementia Communication Tips Dementia Risk Reduction.
 Dementia Facts and Resources Dementia Warning Signs Getting a Diagnosis Dementia Communication Tips Dementia Risk Reduction Intermission Dementia Stages and Behaviors Caregiving and Self-Care Overview
Dementia Facts and Resources Dementia Warning Signs Getting a Diagnosis Dementia Communication Tips Dementia Risk Reduction Intermission Dementia Stages and Behaviors Caregiving and Self-Care Overview
ASAM Criteria, Third Edition Matrix for Matching Adult Severity and Level of Function with Type and Intensity of Service
 1: Acute Intoxication and/or Withdrawal Potential Risk Rating: 0 1: Acute Intoxication and/or Withdrawal Potential Risk Rating: 1 1: Acute Intoxication and/or Withdrawal Potential Risk Rating: 2 The patient
1: Acute Intoxication and/or Withdrawal Potential Risk Rating: 0 1: Acute Intoxication and/or Withdrawal Potential Risk Rating: 1 1: Acute Intoxication and/or Withdrawal Potential Risk Rating: 2 The patient
Getting Help for Patients with Dementia and their Caregivers. Erica Salamida Associate Director of Programs and Services Alzheimer s Association-NENY
 Getting Help for Patients with Dementia and their Caregivers Erica Salamida Associate Director of Programs and Services Alzheimer s Association-NENY In this session you will learn about: Symptoms of dementia,
Getting Help for Patients with Dementia and their Caregivers Erica Salamida Associate Director of Programs and Services Alzheimer s Association-NENY In this session you will learn about: Symptoms of dementia,
Know the 10 Signs: Early Detection Matters
 Importance of Early Detection Know the 10 Signs: Early Detection Matters If we could have had a correct diagnosis even two years earlier, it would have given us more time to plan, to do the things that
Importance of Early Detection Know the 10 Signs: Early Detection Matters If we could have had a correct diagnosis even two years earlier, it would have given us more time to plan, to do the things that
SECTION 1. Children and Adolescents with Depressive Disorder: Summary of Findings. from the Literature and Clinical Consultation in Ontario
 SECTION 1 Children and Adolescents with Depressive Disorder: Summary of Findings from the Literature and Clinical Consultation in Ontario Children's Mental Health Ontario Children and Adolescents with
SECTION 1 Children and Adolescents with Depressive Disorder: Summary of Findings from the Literature and Clinical Consultation in Ontario Children's Mental Health Ontario Children and Adolescents with
Every 67seconds, someone will develop Alzheimer's.
 We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
homeinstead.com Each Home Instead Senior Care franchise office is independently owned and operated Home Instead, Inc.
 Each Home Instead Senior Care franchise office is independently owned and operated. 2010 Home Instead, Inc. homeinstead.com Many of us may joke about having old timers disease, but when cognitive impairment
Each Home Instead Senior Care franchise office is independently owned and operated. 2010 Home Instead, Inc. homeinstead.com Many of us may joke about having old timers disease, but when cognitive impairment
Dealing with Depression Feature Article July 2008
 Dealing with Depression Feature Article July 2008 Marjorie and Ann were housemates for about three years. Everyone thought that they did not like each other very much. Direct support staff said that they
Dealing with Depression Feature Article July 2008 Marjorie and Ann were housemates for about three years. Everyone thought that they did not like each other very much. Direct support staff said that they
Senior Moments or Something More? Copyright James L. West Alzheimer s Center, 2013 All Rights Reserved
 Senior Moments or Something More? Copyright James L. West Alzheimer s Center, 2013 All Rights Reserved Defining Dementia Dementia is a group of symptoms affecting intellectual and social abilities severely
Senior Moments or Something More? Copyright James L. West Alzheimer s Center, 2013 All Rights Reserved Defining Dementia Dementia is a group of symptoms affecting intellectual and social abilities severely
Managing Behavioral Issues
 2:45 3:45pm Caring for the Older Patient Handling Behavioral Issues Presenter Disclosure Information The following relationships exist related to this presentation: Samir Sabbag, MD, has no financial relationships
2:45 3:45pm Caring for the Older Patient Handling Behavioral Issues Presenter Disclosure Information The following relationships exist related to this presentation: Samir Sabbag, MD, has no financial relationships
Depression Fact Sheet
 Depression Fact Sheet Please feel free to alter and use this fact sheet to spread awareness of depression, its causes and symptoms, and what can be done. What is Depression? Depression is an illness that
Depression Fact Sheet Please feel free to alter and use this fact sheet to spread awareness of depression, its causes and symptoms, and what can be done. What is Depression? Depression is an illness that
Cluster 1 Common Mental Health Problems (mild)
 Cluster 1 Common Mental Health Problems (mild) You have recently sought help for the first time. You have experienced depression and/or anxiety. This may cause distraction or minor disruption to you as
Cluster 1 Common Mental Health Problems (mild) You have recently sought help for the first time. You have experienced depression and/or anxiety. This may cause distraction or minor disruption to you as
Aging may affect memory by changing the way the brain stores information and by making it harder to recall stored information.
 Return to Web version Dementia Overview How does the brain store information? Information is stored in different parts of your memory. Information stored in recent memory may include what you ate for breakfast
Return to Web version Dementia Overview How does the brain store information? Information is stored in different parts of your memory. Information stored in recent memory may include what you ate for breakfast
9/11/2012. Clare I. Hays, MD, CMD
 Clare I. Hays, MD, CMD Review regulatory background for current CMS emphasis on antipsychotics Understand the risks and (limited) benefits of antipsychotic medications Review non-pharmacologic management
Clare I. Hays, MD, CMD Review regulatory background for current CMS emphasis on antipsychotics Understand the risks and (limited) benefits of antipsychotic medications Review non-pharmacologic management
10 symptoms of caregiver stress
 10 symptoms of caregiver stress If you experience any of these signs of stress on a regular basis, make time to talk to your doctor. 1. Denial about the disease and its effect on the person who s been
10 symptoms of caregiver stress If you experience any of these signs of stress on a regular basis, make time to talk to your doctor. 1. Denial about the disease and its effect on the person who s been
Schizophrenia: an inside view. Nepean High School, November 2016 Introduction to Psychology class.
 Schizophrenia: an inside view Nepean High School, November 2016 Introduction to Psychology class. Schizophrenia: basic definition Schizophrenia is a chronic and severe mental disorder that affects how
Schizophrenia: an inside view Nepean High School, November 2016 Introduction to Psychology class. Schizophrenia: basic definition Schizophrenia is a chronic and severe mental disorder that affects how
Recognizing Signs and Symptoms of Alzheimer's Disease in Earlier Stages Can Lead to Diagnosis
 A joint publication of the Illinois Health Care Association and CE Solutions November 2015 Recognizing Signs and Symptoms of Alzheimer's Disease in Earlier Stages Can Lead to Diagnosis Early diagnosis
A joint publication of the Illinois Health Care Association and CE Solutions November 2015 Recognizing Signs and Symptoms of Alzheimer's Disease in Earlier Stages Can Lead to Diagnosis Early diagnosis
UNDERSTANDING CAPACITY & DECISION-MAKING VIDEO TRANSCRIPT
 I m Paul Bourque, President and CEO of the Investment Funds Institute of Canada. IFIC is preparing materials to assist advisors and firms in managing effective and productive relationships with their aging
I m Paul Bourque, President and CEO of the Investment Funds Institute of Canada. IFIC is preparing materials to assist advisors and firms in managing effective and productive relationships with their aging
Dementia Carer s factsheet
 Dementia Carer s factsheet Who is this factsheet for? This factsheet is for people caring for someone who may be experiencing memory problems or who has a diagnosis of dementia. Contents Page What is dementia?...
Dementia Carer s factsheet Who is this factsheet for? This factsheet is for people caring for someone who may be experiencing memory problems or who has a diagnosis of dementia. Contents Page What is dementia?...
Disruptive Behavior in Long Term Care. Victor Molinari, PhD Byrd Institute Excellence in Geriatric Health Care Conference
 Disruptive Behavior in Long Term Care Victor Molinari, PhD Byrd Institute Excellence in Geriatric Health Care Conference Goals Learn the appropriate & inappropriate use of psychoactive medications in NHs
Disruptive Behavior in Long Term Care Victor Molinari, PhD Byrd Institute Excellence in Geriatric Health Care Conference Goals Learn the appropriate & inappropriate use of psychoactive medications in NHs
Decline in Mental Capacity
 Decline in Mental Capacity Elder Law: Issues, Answers and Opportunities ALI-ABA, February 23-24, 2006 Robert B. Fleming 1 FLEMING & CURTI, P.L.C. 330 N. Granada Ave. Tucson, Arizona 85701 www.elder-law.com
Decline in Mental Capacity Elder Law: Issues, Answers and Opportunities ALI-ABA, February 23-24, 2006 Robert B. Fleming 1 FLEMING & CURTI, P.L.C. 330 N. Granada Ave. Tucson, Arizona 85701 www.elder-law.com
Delirium, Depression and Dementia
 Delirium, Depression and Dementia Martha Watson, MS, APRN, GCNS Some material included in this presentation is adapted from: NICHE (2009). Geriatric Resource Nurse Core Curriculum [Power Point presentation].
Delirium, Depression and Dementia Martha Watson, MS, APRN, GCNS Some material included in this presentation is adapted from: NICHE (2009). Geriatric Resource Nurse Core Curriculum [Power Point presentation].
Alzheimer Disease and Related Dementias
 Alzheimer Disease and Related Dementias Defining Generic Key Terms and Concepts Mild cognitive impairment: (MCI) is a state of progressive memory loss after the age of 50 that is beyond what would be expected
Alzheimer Disease and Related Dementias Defining Generic Key Terms and Concepts Mild cognitive impairment: (MCI) is a state of progressive memory loss after the age of 50 that is beyond what would be expected
University Counselling Service
 Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
Depression: what you should know
 Depression: what you should know If you think you, or someone you know, might be suffering from depression, read on. What is depression? Depression is an illness characterized by persistent sadness and
Depression: what you should know If you think you, or someone you know, might be suffering from depression, read on. What is depression? Depression is an illness characterized by persistent sadness and
Schizophrenia is a serious mental health condition that affects
 Schizophrenia Schizophrenia is a serious mental health condition that affects a person s thoughts, feelings and behaviours. Whilst it is serious, schizophrenia is both treatable and manageable, and we
Schizophrenia Schizophrenia is a serious mental health condition that affects a person s thoughts, feelings and behaviours. Whilst it is serious, schizophrenia is both treatable and manageable, and we
Handout 3: Mood Disorders
 Handout 3: Mood Disorders Mood disorders are called affective (emotional) disorders. There are two categories of mood disorders: Depressive Disorders Bipolar Affective Disorders Depressive Disorders Minor
Handout 3: Mood Disorders Mood disorders are called affective (emotional) disorders. There are two categories of mood disorders: Depressive Disorders Bipolar Affective Disorders Depressive Disorders Minor
SCHIZOPHRENIA IS COGNITION IMPAIRED IN SCHIZOPHRENIA?
 CHAPTER 10: DISTURBED COGNITION IN SCHIZOPHRENIA Traditionally, functioning of the mind is described under four headings: perception, emotion, cognition, and conation. Perception refers to awareness of
CHAPTER 10: DISTURBED COGNITION IN SCHIZOPHRENIA Traditionally, functioning of the mind is described under four headings: perception, emotion, cognition, and conation. Perception refers to awareness of
WEBINAR SERIES: AGING IN INDIVIDUALS WITH INTELLECTUAL AND DEVELOPMENTAL DISABILITIES
 WEBINAR SERIES: AGING IN INDIVIDUALS WITH INTELLECTUAL AND DEVELOPMENTAL DISABILITIES 1 CMS Medicare-Medicaid Coordination Office (MMCO) Established by Section 2602 of the Affordable Care Act Purpose:
WEBINAR SERIES: AGING IN INDIVIDUALS WITH INTELLECTUAL AND DEVELOPMENTAL DISABILITIES 1 CMS Medicare-Medicaid Coordination Office (MMCO) Established by Section 2602 of the Affordable Care Act Purpose:
Cognitive and Behavioral Changes in ALS: A Guide for People with ALS and their Families
 Cognitive and Behavioral Changes in ALS: A Guide for People with ALS and their Families Overview If you had asked doctors about ALS 15 years ago, the majority of providers would have told you that ALS
Cognitive and Behavioral Changes in ALS: A Guide for People with ALS and their Families Overview If you had asked doctors about ALS 15 years ago, the majority of providers would have told you that ALS
Know the 10 Signs: Early Detection Matters
 Know the 10 Signs: Early Detection Matters 1 Importance of Early Detection If we could have had a correct diagnosis even two years earlier, it would have given us more time to plan, to do the things that
Know the 10 Signs: Early Detection Matters 1 Importance of Early Detection If we could have had a correct diagnosis even two years earlier, it would have given us more time to plan, to do the things that
Addressing Difficult Behaviors in Dementia
 Addressing Difficult Behaviors in Dementia GEORGE SCHOEPHOERSTER, MD GERIATRICIAN GENEVIVE/CENTRACARE CLINIC Objectives By the end of the session, you will be able to: 1) Explain the role of pain management
Addressing Difficult Behaviors in Dementia GEORGE SCHOEPHOERSTER, MD GERIATRICIAN GENEVIVE/CENTRACARE CLINIC Objectives By the end of the session, you will be able to: 1) Explain the role of pain management
Excerpted From "Staying Sober" By: Terence T. Gorski
 Excerpted From "Staying Sober" By: Terence T. Gorski With additions by: Lee Jamison When most people think about alcoholism or drug addiction they think only of the alcohol/drug-based symptoms and forget
Excerpted From "Staying Sober" By: Terence T. Gorski With additions by: Lee Jamison When most people think about alcoholism or drug addiction they think only of the alcohol/drug-based symptoms and forget
We Will Discuss. Dementia and Alzheimer s Disease Basics. Dementia. Developmental Disabilities and Dementia: A Behavior Management Guide
 10/18/2013 1 Dayna Thompson M.S., LMHC Alzheimer s Educator Developmental Disabilities and Dementia: A Behavior Management Guide Alzheimer s Resource Service IU Health Bloomington-Community Health 812-353-9299
10/18/2013 1 Dayna Thompson M.S., LMHC Alzheimer s Educator Developmental Disabilities and Dementia: A Behavior Management Guide Alzheimer s Resource Service IU Health Bloomington-Community Health 812-353-9299
Typical or Troubled? Teen Mental Health
 Typical or Troubled? Teen Mental Health Adolescence is a difficult time for many teens, but how does one know the difference between typical teen issues and behavior that might signal a more serious problem?
Typical or Troubled? Teen Mental Health Adolescence is a difficult time for many teens, but how does one know the difference between typical teen issues and behavior that might signal a more serious problem?
Aging and Mental Health Current Challenges in Long Term Care
 Aging and Mental Health Current Challenges in Long Term Care Stephanie Saur & Christina Pacheco Acute Care Behavioural Consultants Alzheimer Society Peel What is Mental Health? Mental health includes our
Aging and Mental Health Current Challenges in Long Term Care Stephanie Saur & Christina Pacheco Acute Care Behavioural Consultants Alzheimer Society Peel What is Mental Health? Mental health includes our
Dementia in Independent Senior Housing: Concerns, Barriers and Solutions
 Dementia in Independent Senior Housing: Concerns, Barriers and Solutions LeadingAge NY April 13, 2016 Kelly Papa, MSN, RN Masonicare Corporate Director of Learning The Big Question How can we create systems
Dementia in Independent Senior Housing: Concerns, Barriers and Solutions LeadingAge NY April 13, 2016 Kelly Papa, MSN, RN Masonicare Corporate Director of Learning The Big Question How can we create systems
Psychosis, Mood, and Personality: A Clinical Perspective
 Psychosis, Mood, and Personality: A Clinical Perspective John R. Chamberlain, M.D. Assistant Director, Psychiatry and the Law Program Assistant Clinical Professor University of California San Francisco
Psychosis, Mood, and Personality: A Clinical Perspective John R. Chamberlain, M.D. Assistant Director, Psychiatry and the Law Program Assistant Clinical Professor University of California San Francisco
National Audit of Dementia
 National Audit of Dementia (Care in General Hospitals) Date: December 2010 Preliminary of the Core Audit Commissioned by: Healthcare Quality Improvement Partnership (HQIP) Conducted by: Royal College of
National Audit of Dementia (Care in General Hospitals) Date: December 2010 Preliminary of the Core Audit Commissioned by: Healthcare Quality Improvement Partnership (HQIP) Conducted by: Royal College of
SUBOXONE TREATMENT PROGRAM
 SUBOXONE TREATMENT PROGRAM What is Suboxone? Suboxone is a medication used for the treatment of addiction to prescription pain medication, heroin addiction, methadone or other opioid dependence. The primary
SUBOXONE TREATMENT PROGRAM What is Suboxone? Suboxone is a medication used for the treatment of addiction to prescription pain medication, heroin addiction, methadone or other opioid dependence. The primary
Schizophrenia. Introduction. Overview and Facts
 Introduction is a chronic, severe and disabling brain disease that typically shows its first clear symptoms in late adolescence or early adulthood. It is one of several types of Psychotic Disorders. It
Introduction is a chronic, severe and disabling brain disease that typically shows its first clear symptoms in late adolescence or early adulthood. It is one of several types of Psychotic Disorders. It
Mental Health Issues in Nursing Homes. I m glad you asked.
 Mental Health Issues in Nursing Homes I m glad you asked. I m glad you asked Susan Wehry, M.D. Associate Professor of Psychiatry, College of Medicine, University of Vermont Consultant, State of Vermont
Mental Health Issues in Nursing Homes I m glad you asked. I m glad you asked Susan Wehry, M.D. Associate Professor of Psychiatry, College of Medicine, University of Vermont Consultant, State of Vermont
Behavioral Interventions
 Behavioral Interventions Linda K. Shumaker, R.N.-BC, MA Pennsylvania Behavioral Health and Aging Coalition Behavioral Management is the key in taking care of anyone with a Dementia! Mental Health Issues
Behavioral Interventions Linda K. Shumaker, R.N.-BC, MA Pennsylvania Behavioral Health and Aging Coalition Behavioral Management is the key in taking care of anyone with a Dementia! Mental Health Issues
Delirium in Palliative care. Presentation to Volunteers 2016 David Falk
 Delirium in Palliative care Presentation to Volunteers 2016 David Falk Delirium What is delirium? Case Study - Delirium 60+ year old PQ presents to hospice very somnolent. She was admitted with her adult
Delirium in Palliative care Presentation to Volunteers 2016 David Falk Delirium What is delirium? Case Study - Delirium 60+ year old PQ presents to hospice very somnolent. She was admitted with her adult
Dementia. Presented By Jennifer L. Nanson
 Dementia Presented By Jennifer L. Nanson Dementia QuickTime and a decompressor are needed to see this picture. Dementia: Current Definition DSM-IV-TR Does not imply a prognosis Refers to a framework of
Dementia Presented By Jennifer L. Nanson Dementia QuickTime and a decompressor are needed to see this picture. Dementia: Current Definition DSM-IV-TR Does not imply a prognosis Refers to a framework of
Evaluations. Alzheimer s Disease A Public Health Response. Viewer Call-In. July 19, Guest Speakers. Thanks to our Sponsors:
 Alzheimer s Disease A Public Health Response July 19, 2007 1 2 Guest Speakers Thanks to our Sponsors: Earl A. Zimmerman, M.D. Bender Endowed Chair of Neurology and Director of the Alzheimer s Center at
Alzheimer s Disease A Public Health Response July 19, 2007 1 2 Guest Speakers Thanks to our Sponsors: Earl A. Zimmerman, M.D. Bender Endowed Chair of Neurology and Director of the Alzheimer s Center at
GERIATRIC WORKFORCE ENHANCEMENT PROGRAM (GWEP) FACULTY DEVELOPMENT MASTERWORKS SERIES
 UNIVERSITY OF SOUTH FLORIDA GERIATRIC WORKFORCE ENHANCEMENT PROGRAM (GWEP) FACULTY DEVELOPMENT MASTERWORKS SERIES Kathryn Hyer, PhD, MPP Principal Investigator h Providers of Continuing Education For additional
UNIVERSITY OF SOUTH FLORIDA GERIATRIC WORKFORCE ENHANCEMENT PROGRAM (GWEP) FACULTY DEVELOPMENT MASTERWORKS SERIES Kathryn Hyer, PhD, MPP Principal Investigator h Providers of Continuing Education For additional
Antipsychotic Medication in Dementia; The good, the bad and the ugly! Anthony Bainbridge Deputy Director of Nursing Sheffield Health and Social Care
 Antipsychotic Medication in Dementia; The good, the bad and the ugly! Anthony Bainbridge Deputy Director of Nursing Sheffield Health and Social Care Different types of antipsychotic medication Antipsychotic
Antipsychotic Medication in Dementia; The good, the bad and the ugly! Anthony Bainbridge Deputy Director of Nursing Sheffield Health and Social Care Different types of antipsychotic medication Antipsychotic
Chapter 15: Late Life and Psychological Disorders
 \ Chapter 15: Late Life and Psychological Disorders 1. Ageism refers to a. the physical deterioration that accompanies old age. b. the intellectual deterioration that frequently occurs as a person ages.
\ Chapter 15: Late Life and Psychological Disorders 1. Ageism refers to a. the physical deterioration that accompanies old age. b. the intellectual deterioration that frequently occurs as a person ages.
Overview. Case #1 4/20/2012. Neuropsychological assessment of older adults: what, when and why?
 Neuropsychological assessment of older adults: what, when and why? Benjamin Mast, Ph.D. Associate Professor & Vice Chair, Psychological & Brain Sciences Associate Clinical Professor, Family & Geriatric
Neuropsychological assessment of older adults: what, when and why? Benjamin Mast, Ph.D. Associate Professor & Vice Chair, Psychological & Brain Sciences Associate Clinical Professor, Family & Geriatric
Men and Depression. If so, you may have depression. National Institute of Mental Health
 Men and Depression Are you tired and irritable all the time? Have you lost interest in your work, family, or hobbies? Are you having trouble sleeping and feeling angry or aggressive, sad, or worthless?
Men and Depression Are you tired and irritable all the time? Have you lost interest in your work, family, or hobbies? Are you having trouble sleeping and feeling angry or aggressive, sad, or worthless?
Frequently Asked Questions About Dementia
 Frequently Asked Questions About Dementia Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please consult
Frequently Asked Questions About Dementia Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please consult
Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia
 Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia I. Key Points a. Schizophrenia is a chronic illness affecting all aspects of person s life i. Treatment Planning Goals 1.
Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia I. Key Points a. Schizophrenia is a chronic illness affecting all aspects of person s life i. Treatment Planning Goals 1.
DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include:
 DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include: 1. Memory loss The individual may repeat questions or statements,
DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include: 1. Memory loss The individual may repeat questions or statements,
Meeting The Dementia Challenge In Home Care
 Meeting The Dementia Challenge In Home Care 6 { th Annual New England Home Care & Hospice Conference: May 16, 2016 Amy E. MaHhews, Engaging Alzheimer s, LLC Dementia is not a normal process of aging Ñ
Meeting The Dementia Challenge In Home Care 6 { th Annual New England Home Care & Hospice Conference: May 16, 2016 Amy E. MaHhews, Engaging Alzheimer s, LLC Dementia is not a normal process of aging Ñ
Understanding Depression
 Understanding Depression What causes Depression? Family History Having family members who have depression may increase a person s risk Deficiencies of certain chemicals in the brain may lead to depression
Understanding Depression What causes Depression? Family History Having family members who have depression may increase a person s risk Deficiencies of certain chemicals in the brain may lead to depression
Mood Disorders. Moderate depression that will go away without therapy. Restlessness, inability to concentrate, and rapid speech. Dysthymic Disorder
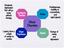 Moderate depression that will go away without therapy Dysthymic Disorder Mania Restlessness, inability to concentrate, and rapid speech Mood Disorders Lasting from a couple of weeks to months Major Depression
Moderate depression that will go away without therapy Dysthymic Disorder Mania Restlessness, inability to concentrate, and rapid speech Mood Disorders Lasting from a couple of weeks to months Major Depression
Depression in Older Adults. Key Issues
 Depression in Older Adults Key Issues Depression and Older Adults: Key Issues is an overview of important information that you should know about depression in older adults. Depression is one of the most
Depression in Older Adults Key Issues Depression and Older Adults: Key Issues is an overview of important information that you should know about depression in older adults. Depression is one of the most
Department of Geriatric Medicine
 Department of Geriatric Medicine Pre-Visit Questionnaire for Dementia Evaluation Name: MR#: Imprint Area This questionnaire is to be filled out by someone who knows you well. Name of Person completing
Department of Geriatric Medicine Pre-Visit Questionnaire for Dementia Evaluation Name: MR#: Imprint Area This questionnaire is to be filled out by someone who knows you well. Name of Person completing
dementia work training
 dementia friendly @ work training Participant s Guide In our communities, nearly 60 percent of people with Alzheimer s disease, a form of dementia, live in their own homes and need support from families
dementia friendly @ work training Participant s Guide In our communities, nearly 60 percent of people with Alzheimer s disease, a form of dementia, live in their own homes and need support from families
FTD/PPA Caregiver Education Conference March 11, 2011
 FTD/PPA Caregiver Education Conference March 11, 2011 Question and Answer Session Answered by Joseph Cooper, MD, Darby Morhardt, MSW, LCSW, Mary O Hara, AM, LCSW, Jaimie Robinson, MSW, LCSW, Emily Rogalski,
FTD/PPA Caregiver Education Conference March 11, 2011 Question and Answer Session Answered by Joseph Cooper, MD, Darby Morhardt, MSW, LCSW, Mary O Hara, AM, LCSW, Jaimie Robinson, MSW, LCSW, Emily Rogalski,
Your aging brain. Contact your local chapter to learn more. Find a chapter near you at or visit alz.org/findus.
 Your aging brain. Being told that additional tests are needed because your inability to remember things or problems with talking or thinking can trigger fear, denial and other worries. You are not alone.
Your aging brain. Being told that additional tests are needed because your inability to remember things or problems with talking or thinking can trigger fear, denial and other worries. You are not alone.
Geriatric Alterations Associated with Neurological Conditions
 Geriatric Alterations Associated with Neurological Conditions I have no conflicts of interest. Julie Bronson The Older Adult According to the World Health Organization Africa 50-55 or 50-65 United Nations
Geriatric Alterations Associated with Neurological Conditions I have no conflicts of interest. Julie Bronson The Older Adult According to the World Health Organization Africa 50-55 or 50-65 United Nations
The place for treatments of associated neuropsychiatric and other symptoms
 The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
Dementia. Information for service users and carers. RDaSH leading the way with care
 Dementia Information for service users and carers RDaSH leading the way with care What is Dementia is a term that is used to describe the symptoms that occur when the brain is affected by specific diseases
Dementia Information for service users and carers RDaSH leading the way with care What is Dementia is a term that is used to describe the symptoms that occur when the brain is affected by specific diseases
PREVENTING CAREGIVER BURNOUT
 PREVENTING CAREGIVER BURNOUT Tips and Support for Caregivers De Anna Looper, RN CHPN Carrefour Associates Management Company for Crossroads Hospice December 2009 PREVENTING CAREGIVER BURNOUT Caring for
PREVENTING CAREGIVER BURNOUT Tips and Support for Caregivers De Anna Looper, RN CHPN Carrefour Associates Management Company for Crossroads Hospice December 2009 PREVENTING CAREGIVER BURNOUT Caring for
Why does someone develop bipolar disorder?
 Bipolar Disorder Do you go through intense moods? Do you feel very happy and energized some days, and very sad and depressed on other days? Do these moods last for a week or more? Do your mood changes
Bipolar Disorder Do you go through intense moods? Do you feel very happy and energized some days, and very sad and depressed on other days? Do these moods last for a week or more? Do your mood changes
Section 3. Objectives. Vocabulary clinical depression cutting suicide cluster suicides
 Section 3 I Objectives ~ Explain why it is important to identify and treat clinical depression. ~ Explain why individuals might deliberately injure themselves. ~ Describe one major risk factor for suicide.
Section 3 I Objectives ~ Explain why it is important to identify and treat clinical depression. ~ Explain why individuals might deliberately injure themselves. ~ Describe one major risk factor for suicide.
Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia (BPSD) Summary document for Primary Care
 Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia (BPSD) Summary document for Primary Care Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia
Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia (BPSD) Summary document for Primary Care Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia
The Revised Treatment Manual for the Brief Behavioral Activation Treatment for Depression (BATD-R) Pre - Session
 The Revised Treatment Manual for the Brief Behavioral Activation Treatment for Depression (BATD-R) Pre-Session Key Elements: 1. Discussion of Depression Pre - Session 2. Introduction to Treatment Rationale
The Revised Treatment Manual for the Brief Behavioral Activation Treatment for Depression (BATD-R) Pre-Session Key Elements: 1. Discussion of Depression Pre - Session 2. Introduction to Treatment Rationale
Alzheimer s disease affects patients and their caregivers. experience employment complications,
 Alzheimer s Disease and Dementia A growing challenge The majority of the elderly population with Alzheimer s disease and related dementia are in fair to poor physical health, and experience limitations
Alzheimer s Disease and Dementia A growing challenge The majority of the elderly population with Alzheimer s disease and related dementia are in fair to poor physical health, and experience limitations
Dementia Training Session for Carers. By Dr Rahul Tomar Consultant Psychiatrist
 Dementia Training Session for Carers By Dr Rahul Tomar Consultant Psychiatrist Dementia in the UK: Facts & Figures National Dementia strategy launched in 2009 800,000 people living with dementia (2012)
Dementia Training Session for Carers By Dr Rahul Tomar Consultant Psychiatrist Dementia in the UK: Facts & Figures National Dementia strategy launched in 2009 800,000 people living with dementia (2012)
Substance and Alcohol Related Disorders. Substance use Disorder Alcoholism Gambling Disorder
 Substance and Alcohol Related Disorders Substance use Disorder Alcoholism Gambling Disorder What is a Substance Use Disorder? According to the DSM-5, a substance use disorder describes a problematic pattern
Substance and Alcohol Related Disorders Substance use Disorder Alcoholism Gambling Disorder What is a Substance Use Disorder? According to the DSM-5, a substance use disorder describes a problematic pattern
