Relationship between caffeine intake and autosomal dominant polycystic kidney disease progression: a retrospective analysis using the CRISP cohort
|
|
|
- Margaret Fowler
- 5 years ago
- Views:
Transcription
1 McKenzie et al. BMC Nephrology (2018) 19:378 RESEARCH ARTICLE Open Access Relationship between caffeine intake and autosomal dominant polycystic kidney disease progression: a retrospective analysis using the CRISP cohort Katelyn A. McKenzie 1*, Mirelle El Ters 2, Vicente E. Torres 2, Peter C. Harris 2, Arlene B. Chapman 3, Michal Mrug 4, Frederic F. Rahbari-Oskoui 5, Kyongtae Ty Bae 6, Douglas P. Landsittel 7, William M. Bennett 8, Alan S. L. Yu 9 and Jonathan D. Mahnken 1 Abstract Background: Caffeine has been proposed, based on in vitro cultured cell studies, to accelerate progression of autosomal dominant polycystic kidney disease (ADPKD) by increasing kidney size. Since ADPKD patients are advised to minimize caffeine intake, we investigated the effect of caffeine on disease progression in the Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease (CRISP), a prospective, observational cohort study. Methods: Our study included 239 patients (mean age = 32.3 ± 8.9 ys; 188 caffeine consumers) with a median follow-up time of 12.5 years. Caffeine intake reported at baseline was dichotomized (any vs. none). Linear mixed models, unadjusted and adjusted for age, race, sex, BMI, smoking, hypertension, genetics and time, were used to model height-adjusted total kidney volume (httkv) and iothalamate clearance (mgfr). Cox proportional hazards models and Kaplan-Meier plots examined the effect of caffeine on time to ESRD or death. Results: Caffeine-by-time was statistically significant when modeling ln(httkv) in unadjusted and adjusted models (p < 0.01) indicating that caffeine consumers had slightly faster kidney growth (by 0.6% per year), but httkv remained smaller from baseline throughout the study. Caffeine consumption was not associated with a difference in mgfr, or in the time to ESRD or death (p > 0.05). Moreover the results were similar when outcomes were modeled as a function of caffeine dose. Conclusion: We conclude that caffeine does not have a significant detrimental effect on disease progression in ADPKD. Keywords: Caffeine, CRISP, ESRD, Linear mixed models, Polycystic kidney disease Background Autosomal dominant polycystic kidney disease (ADPKD) is a systemic disease that primarily affects the kidneys. ADPKD occurs in both sexes, all races and the majority of cases are caused by a genetic mutation in one of two genes, PKD1 and PKD2 [1]. ADPKD is the most common inherited kidney disease. This disease causes irreversible kidney damage that begins in utero and * Correspondence: kmckenzie5@kumc.edu 1 Department of Biostatistics, University of Kansas Medical Center, Mail Stop 1026, 3901 Rainbow Blvd., Kansas City, KS 66160, USA Full list of author information is available at the end of the article eventually leads to end stage renal disease (ESRD), of which it is a major contributor [2]. While the incidence of ADPKD is estimated to be between 1:400 1:1000, there are no curative treatments [3] and one pharmacologic therapy, tolvaptan, that was recently approved in the United States [4]. Mechanistically, these genetic mutations lead to an abnormal response to high levels of 3 :5 -cyclic adenosine monophosphate (camp) when intracellular levels of calcium are low. This has two effects. First, an increase in camp will lead to activation of the ERK signaling pathway which ultimately causes an increase in cellular The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 McKenzie et al. BMC Nephrology (2018) 19:378 Page 2 of 10 proliferation. Second, an increase in camp will lead to activation of the cystic fibrosis transmembrane conductance regulator (CFTR), which causes an increase in chloride secretion and thus water into the cysts [5]. Additionally, while the exact role of vasopressin in ADPKD progression is not clear, it is known that vasopressin V2 receptor antagonists reduces the rate of kidney growth in ADPKD [6]. Due to the high proportion of patients who reach ESRD, it is important to understand the role of environmental factors, such as diet and other lifestyle exposures, in disease progression. Of interest is the role of caffeine. It is well known that caffeine increases camp levels by inhibiting phosphodiesterase, an enzyme that hydrolyzes camp. In 2002, Belibi et al. examined the effects of caffeine on ADPKD cyst epithelial cells in vitro [7]. They found that caffeine increased intracellular camp levels and potentiated the effect of desmopressin, a vasopressin analog, on chloride secretion and ERK activation. On the basis of this single, in vitro study, and on the predicted effects of increased camp to accelerate cell proliferation, fluid secretion, and hence kidney cyst growth, most physicians advise their patients who have ADPKD to limit caffeine intake [8]. This recommendation is open to question. In the Han:SPRD rat model of ADPKD, chronic caffeine intake to the age of 6 months did not accelerate kidney or cyst growth or the decline in GFR, although it did exacerbate hypertension [9]. There are limited studies on the effects of caffeine intake in patients with ADPKD. In 2012, Vendramini et al. studied the effects of caffeine on patients with ADPKD in a small cross-sectional study and found that renal volume, as measured by ultrasound, was not associated with caffeine intake [10]. In 2017, Girardat-Rotar et al. examined the association of coffee intake with ADPKD progression, as measured by height adjusted total kidney volume (httkv) and glomerular filtration rate (GFR) in a prospective longitudinal study of 151 patients followed for a median of 4 years, and concluded that coffee consumption was not a significant risk factor [11]. Although suggestive evidence is beginning to surface that caffeine may not contribute to disease progression, the goal of this analysis was to examine the effects of caffeine on ADPKD progression over a longer time period in a well-studied cohort of patients with ADPKD. Methods CRISP study design and participants Data were taken from the Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease (CRISP) study, which comprised of four clinical centers, University of Alabama, Emory University, University of Kansas and the Mayo Clinic. Patients were eligible to be enrolled in the CRISP study if they were diagnosed with ADPKD, had a creatinine clearance of at least 70 ml/min, serum creatinine level of either 1.6 mg/deciliter for men or 1.4 mg/deciliter for women, and were between 15 and 46 years of age at baseline. Patients were excluded from the study if they had any comorbidities that would affect kidney function besides hypertension. At each visit, TKV was determined from coronal T1- and T2-weighted MRI using a stereologic method, [12 14] and corrected for height (httkv, ml/m). GFR was measured by iothalamate clearance and indexed to body surface area (ml/min/1.73 m 2 ). Lifestyle exposures, including caffeine consumption and smoking status, were collected via written surveys in the form of closed questions (Additional file 1). Patients were screened for mutations in the PKD1 and PKD2 genes. Further details about the CRISP study have been previously published [13, 15]. Outcome measures Two outcomes were used to assess disease progression. The primary outcome was height-adjusted total kidney volume (httkv) [16]. Because kidney volume increases exponentially over time, httkv was natural log transformed. The second outcome was measured glomerular filtration rate (mgfr) calculated by iothalamate clearance [17]. We chose to have the primary outcome be httkv because httkv has been shown to be a good proxy for disease state [15] and the secondary outcome to be mgfr because mgfr is used to estimate kidney filtering capabilities and thus kidney function. Explanatory measure of interest Caffeine consumption at baseline was assessed as the number of cups of coffee/tea, and the number of glasses of other caffeinated beverages consumed per day, averaged over the prior month. For the primary analysis, the exposure variable of caffeine consumption was dichotomized (any vs. none). For further investigation of this relationship, we treated caffeine dose both as a continuous variable, and binned into daily quartiles of caffeine intake of 0 mg (n = 51), > 0-86 mg (n = 50), > mg (n = 47), > mg (n = 45) and > 301 mg (n =46). To obtain a quantitative estimate of caffeine dose, each source was converted into milligrams via the following conversions: 95 mg of caffeine = 1 cup of coffee/tea (8 oz.) and 43 mg of caffeine = 1 glass of other caffeinated beverage (12 oz.) [18, 19]. When converting caffeine consumption into milligrams, if the patient was missing either (but not both) number of cups of coffee or number of other caffeinated beverages per day, it was assumed they drank none (n =9). Patients missing both values at baseline (n =16) were imputed to have no caffeine intake.
3 McKenzie et al. BMC Nephrology (2018) 19:378 Page 3 of 10 Additional covariates Additional baseline variables that were included as covariates in the multivariable adjusted models were age, race, sex, BMI, smoking, hypertension, and genetic profile. The patient s race was categorized as either White or Other due to the small sample sizes of subsets of the other races. Based on the current understanding of the prognostic significance of ADPKD mutations, we classified the mutation data into three subgroups of gene types: truncating PKD1, non-truncating PKD1, and PKD2 + no mutation detected (NMD) [20, 21]. Statistical analysis Descriptive analyses for continuous variables were expressed as means (± standard deviations) and for categorical variables were expressed as frequencies and relative frequencies. If a continuous variable did not appear to be normally distributed by its quantile-quantile (QQ) plot and histogram, the median and inter-quartile range (IQR) was reported as well. Two-sampled t-tests and Pearson s chi square test for continuous and categorical variables, respectively, were used to assess differences in measures between caffeine and non-caffeine consumers among our sample. QQ plots and histogram residuals were used to check for assumption of normality of the two-sampled t-tests. If the assumptions for the t-tests were violated, the Wilcoxon rank sum test was used. Expected cell counts were used to assess assumptions for Pearson s chi square test. When computing the median follow-up time, the last available time was used. Four patients had 4 follow-up visits during CRISP I without times or dates, so we imputed their follow-up time to be 3 years as these all corresponded to the year three visit. The main statistical method utilized in this analysis was a linear mixed effect model (LME) with random intercepts. LMEs were utilized because the CRISP study has more than one measurement of all outcome measures for each patient collected over 14 years. Thus we used random effects that allowed each patient to have their own intercept parameter (i.e., the random effect). All other covariates were fixed effects. Single factor association models for each variable were first computed with adjustment only for time. Then, multivariable models, adjusting for age, sex, race, BMI, smoking, hypertension, gene type and time, were computed for each outcome variable (referred to as Model 1 for ln(httkv) and Model 1 for mgfr). Lastly, models were adjusted for caffeine, time and their interaction for each outcome variable (referred to as Model 2 for ln(httkv) and Model 2 for mgfr). The coefficient (β) for the effect of the interaction between caffeine and time on the outcome of ln(httkv) represents the effect of caffeine consumption on the slope of ln(httkv) over time. The effect size, as measured by the constant, annual difference in percentage growth of httkv (without log-transformation) in caffeine-consumers compared to non-caffeine consumers, was calculated by taking (e β )*100% [22]. Additional file 2: Table S1 summarizes the models used in this study. Model assumptions were checked using QQ plots and plots of residuals, with appropriate adjustments for model violations such as log transformations using the natural log function. Multivariable models using daily caffeine dose as continuous and multicategory variables were centered and used in sensitivity analyses, as were models which excluded subjects missing both caffeine exposure variables (cups of coffee/tea and glasses of other caffeinated beverages per day). In some cases identified as missing visits, subjects contributed some of their study measures, just not all. Linear contrasts of Model 2 for ln(httkv) were performed to quantify the effect of caffeine over time. Kaplan Meier plots with right-censored data were used to examine the effect of caffeine on time until ESRD or death, along with corresponding log-rank tests to compare survival between caffeine groups (any vs. none). Cox proportional hazard regression analysis was performed to examine the effects of age, sex, race, BMI, smoking, hypertension, gene type and caffeine. Statistical significance was accepted if p < R (Vienna, Austria) was used for data processing and analysis. Results Patient characteristics In 2001, 241 patients were enrolled in the CRISP study and were evaluated until Of these 241 patients, we excluded 2 because of missing genetic information, thus giving us a sample size of 239 patients. Additionally, 16 patients were missing data for both caffeine sources (coffee/tea and other caffeinated beverages) at baseline. We computed models based on the inclusion of these patients, with their caffeine intake assumed to be 0 mg, then performed additional sensitivity analyses in which these patients were excluded. The median follow-up time was 12.5 years (IQR: 8.7,13.0). The minimum number of patient visits was 4 and the maximum number of visits was 8 (25th, 50th and 75th percentiles were 6, 8 and 8, respectively). At baseline, the average (± standard deviation [sd]) and median (IQR) age of our sample was 32.3 (±8.7) and 33.8 (25.1, 39.7) years, respectfully. Sixty percent of our patients were female and 87% were white. 61% of our patients had hypertension at baseline and 17% of our patients reported smoking. The majority of our patients had a truncating mutation in the PKD1 gene (53%) while 25% of the patients had a non-truncating mutation in PKD1 and 22% had either a mutation in PKD2 or no mutations detected (NMD) in either PKD1 or PKD2.
4 McKenzie et al. BMC Nephrology (2018) 19:378 Page 4 of 10 The mgfr was relatively preserved, as the average (± sd) and median (IQR) values were 97.7 (±24.8) and 94.7 (78.8, 114.8) ml/min/1.73m 2, respectively. At baseline, the average (± sd) and median (IQR) of httkv in our sample was (±373.9) and (350.2, 773.9) ml/m, respectfully. At baseline, 79% of the patients reported consuming caffeine. The minimum amount of caffeine consumed was 0 mg/day and the maximum was 1425 mg/day (25th, 50th and 75th percentiles = 29.3, 129, and 233 mg/day, which would be equivalent to 0.31, 1.36 and 2.45 eight-ounce cups of coffee per day, respectively). Table 1 shows the baseline characteristics of caffeine consumers compared to non-caffeine consumers. While there were no statistically significant differences between baseline characteristics, 19% of caffeine consumers reported smoking at baseline compared to 8% of non-caffeine consumers (p-value = 0.088). Caffeine consumers had a slightly lower median (IQR) baseline httkv compared to non-caffeine consumers [479.9 (342.4, 726.9) ml/m compared to (382.6, 872.7) ml/m; p-value = 0.22] and slightly higher mgfr [96.4 (78.7, 114.7) ml/min/1.73m 2 compared to 88.7 (79.1, 114.8) ml/min/1.73m 2 ; p-value = 0.36) but neither of these were statistically significant. At the time of this analysis, 42 patients had reached end-stage renal disease (ESRD) and 3 patients died, while 194 had not reached ESRD or were censored. Association of caffeine intake with kidney volume and GFR over time Linear mixed models were first fit for each covariate separately to determine each single factor association over time (eg. baseline age and time as fixed effects in the first model, baseline hypertension and time as fixed effects in the second model, etc., see Additional file 2: Table S2). When using ln(httkv) as the outcome variable, age, BMI, hypertension, race and gene type were statistically significant, as has been reported previously [23, 24]. The caffeine-by-time interaction term also showed a small, but statistically significant (p-value = 0.007), positive association with ln(httkv), whereas the main effect of caffeine in this model was not statistically significant (p-value = 0.205). In models with mgfr over time as the outcome, age, BMI and hypertension were the only statistically significant measures in our single factor analyses. Next we fit multivariable models for ln(httkv) and mgfr adjusted for age, sex, race, BMI, smoking, hypertension, gene type and time (Model 1). As with the single factor associations over time, age and hypertension were found to be statistically significant in Model 1 for both ln(httkv) and mgfr (Additional file 2: Table S3). Gene type was also statistically significant for Model 1 for both outcomes (Additional file 2: Table S3). BMI was not statistically significant in Model 1. Table 1 Demographics and estimates of kidney function in the CRISP population at baseline Characteristic Total N = 239 Caffeine Consumer N = 188 (79) Non-Caffeine Consumer N = 51 (21) Age*, years Mean (± sd) 32.3 ± ± ± Median (IQR) 33.8 (25.1, 39.7) 33.6 (25.0, 39.7) 34.2 (16.0, 39.4) Race (White), n (%) 207 (87) 167 (89) 40 (78) Sex (Male), n (%) 96 (40) 78 (41) 18 (35) BMI*, kg/m 2 Mean (± sd) ± ± ± Median (IQR) (21.98, 28.64) (22.04, 29.03) (22.06, 27.64) Smoking, n (%) 40 (17) 36 (19) 4 (8) Hypertension, n (%) 146 (61) 113 (60) 33 (65) P-value for difference between caffeine and non-caffeine consumers Genotype, n (%) PKD1 + truncation 127 (53) 100 (53) 27 (53) PKD1 + no truncation 60 (25) 49 (26) 11 (22) PKD2 + NMD 52 (22) 39 (21) 13 (25) httkv*, ml/m Mean (± sd) ± ± ± Median (IQR) (350.2, 773.9) (342.4, 726.9) (382.6, 872.7) Iothalamate Clearance* ϕ, Mean (± sd) 97.7 ± ± ± ml/min/1.73m 2 Median (IQR) (78.78, ) (78.74, ) (79.05, ) Values are given for the total population and based on caffeine intake. *P-value based on Wilcoxon rank sum test due to violation of t-test assumptions. ϕ N = 234 (5 values missing at baseline but contributed subsequent measures for mixed model results). NMD refers to no mutation detected in the genetic analysis
5 McKenzie et al. BMC Nephrology (2018) 19:378 Page 5 of 10 Finally, we added caffeine consumption (any vs. none) to the multivariable models (Model 2) for both outcomes. These results are presented in Table 2. For both outcomes, the variables that were significant in Model 1 remained significant after the inclusion of caffeine consumption. The effect of caffeine on ln(httkv) varied over time as indicated by tests of interactions between caffeine and time (p-value = 0.007) but not for mgfr (p-value = 0.811). The expected difference in ln(httkv) between caffeine consumers and non-caffeine consumers at baseline was (95% CI: , 0.003; p-value = 0.061). This corresponds to a 13.6% (95% CI: 0.3, 25.5%) lower baseline httkv associated with caffeine consumption. The expected difference in the rate of change of ln(httkv) over time between caffeine consumers and non-caffeine consumers was (95% CI: 0.002, 0.011; p = 0.007). This corresponds to a 0.6% (95% CI: 0.2, 1.1%) greater rate of kidney growth each year associated with caffeine, so the annual rate of kidney growth for caffeine consumers was 5.3% compared to 4.6% for non-caffeine consumers. The difference in baseline mgfr associated with caffeine consumption was 1.40 ml/min/1.73m 2 (95% CI: -5.91, 8.71; p = 0.713) and the difference in the rate of change of mgfr was ml/ min/1.73m 2 (95% CI: , 0.631; p = 0.811). Caffeine intake and the risk of ESRD or death Among caffeine consumers, 15.4% reached ESRD and 1.1% died during the study, while in non-caffeine consumers, 25.5% reached ESRD and 1.2% died. The Kaplan-Meier curves for survival free of ESRD or death (Fig. 1) were not statistically significantly different (log rank test p = 0.10). In a multivariable proportional hazards model adjusted for the effects of age, sex, race, BMI, smoking, hypertension and gene type on time until ESRD or death (Additional file 2: Table S11), we found that age, smoking, hypertension and genetic status were statistically significant. When caffeine consumption (any vs. none) was added to this model, age, smoking, hypertension and gene type remained statistically significant (Table 3). There were no substantive changes in hazard for any of these variables. However, caffeine consumption was not found to be a statistically significant risk factor for the time to ESRD or death (Hazard Ratio (HR) = 0.556; 95% CI: 0.279, 1.110; p = 0.096). Sensitivity analyses We performed sensitivity analyses using different measures of amount of caffeine consumed examined as continuous and multicategory variables. We also generated these results excluding patients who were missing baseline data on both sources of caffeine (cups of coffee/tea and glasses of other caffeinated beverages). Both unadjusted and adjusted models were estimated. See Additional file 2: Tables S1-S10. When modeling ln(httkv) as the outcome, caffeine:time interactions were statistically significant in most models but with estimates near zero. When modeling mgfr as the outcome, caffeine was not statistically significant. Therefore, the sensitivity analyses were not qualitatively different than Table 2 Results from multivariable Model 2 (adjusted for caffeine) for ln(httkv) and for mgfr Fixed Effects Ln(htTKV) mgfr Estimate 95% CI P-value Estimate 95% CI P-value Age , < , < Sex (Male) , , Race (White) , , BMI , , Smoke (Yes) , , Hypertension (Yes) , < , < Gene type < 0.001* 0.018* PKD1 + truncation Reference Reference PKD1 + no truncation , , PKD2 + NMD , , Caffeine (Any) , , Caffeine:Time (Any) , , Time , < , < Random Effect Variance Standard Deviation Variance Standard Deviation Patient Residual *P-value based on F-test with 3 groups. NMD refers to no mutation detected in the genetic analysis
6 McKenzie et al. BMC Nephrology (2018) 19:378 Page 6 of 10 Fig. 1 Kaplan Meier plot of probability free from ESRD or death according to caffeine intake our primary results and showed that caffeine does not have a strong and consistent effect on disease progression. Discussion In this analysis using data from the CRISP study, we found a statistically significant association between the interaction of time with caffeine (any vs. none) and ln(httkv). Table 3 Cox Regression model with caffeine (any vs. none) Risk Factor Estimate P-value Hazard Ratio (HR) (95% CI for HR) Age < (1.034, 1.133) Sex (Male) (0.638, 2.224) Race (White) (0.117, 1.085) BMI (0.986, 1.114) Smoke (Yes) (1.204, 6.683) Hypertension (Yes) (1.711, ) Gene type a PKD1 + no truncation (0.745, 2.841) PKD2 + NMD (0.057, 0.672) Caffeine (Any) (0.279, 1.110) a Reference group: PKD1 + truncation. NMD refers to no mutation detected in the genetic analysis This interaction term was positive, indicating that the rate of ln(httkv) growth is higher with caffeine intake. However, the effect size of the interaction was quantitatively very small: 0.6% per year difference in the httkv among caffeine consumers. Compared to the 4.6% average annual rate of increase in kidney size in non-caffeine consumers, the increased rate of 5.3% due to caffeine was small and unlikely to be clinically important. While the rate of kidney growth in caffeine consumers was higher, the expected httkv at baseline and throughout the follow-up period showed a trend to be lower than for patients who did not consume caffeine (Fig. 2). Similar to the expected httkv being lower throughout the follow-up period, the expected mgfr at baseline and throughout the follow-up period was higher for patients who consumed caffeine, although these results were not statistically significant (Fig. 3). The lack of association between caffeine and mgfr has been reported previously, including a metaanalysis that examined coffee consumption and chronic kidney disease in nearly 15,000 individuals [25]. These relationships were generally consistent throughout our sensitivity analyses. Taken together, these findings indicate that caffeine consumption is unlikely to have a clinically significant effect on ADPKD progression.
7 McKenzie et al. BMC Nephrology (2018) 19:378 Page 7 of 10 Fig. 2 Spaghetti plot of ln(httkv) (on left) and httkv (on right) over time for each individual patient (randomly jittered to preclude presentation of any individual s actual data). The final adjusted model is overlayed (Model 2), showing the differences in slope and intercept for patients who reported consuming caffeine and patients who did not report consuming caffeine at baseline The reason why caffeine intake did not accelerate disease progression is unclear. One possible reason might be that the amount of caffeine that reaches the kidney instead of being metabolized in the liver may simply be too small [26]. Only 3% of caffeine is excreted intact [27]. Theoretically it is possible for caffeine to affect renal epithelial camp, but only in the patients with very high caffeine intake and high excretion rates of unmetabolized caffeine. In our analysis, patients in the highest category of caffeine intake did not have increased rates of kidney growth or GFR decline. In the majority of caffeine consumers, tissue exposure to caffeine may be too low to significantly increase camp in collecting duct cells and thus increase cyst and kidney Fig. 3 Spaghetti plot of mgfr over time for each individual patient (randomly jittered to preclude presentation of any individual s actual data). The final adjusted model is overlayed (Model 2), showing the differences in slope and intercept for patients who reported consuming caffeine and patients who did not report consuming caffeine at baseline
8 McKenzie et al. BMC Nephrology (2018) 19:378 Page 8 of 10 volume. Additionally, this study examined caffeine intake at baseline only. Since patients with ADPKD are advised to limit caffeine intake, the patients in this study may have consumed less caffeine on average than what was reported at baseline. This could further decrease the amount of caffeine reaching the kidneys intact. Another possible reason is because of the presumed natriuretic effects of caffeine [28]. Caffeine has been reported to be a potential acute inhibitor of sodium and hence water reabsorption in the proximal convoluted tubule [29]. If this were to be compensated by increased water intake, serum sodium concentration and osmolarity would tend to decrease thus suppressing vasopressin secretion. Vasopressin is believed to accelerate ADPKD progression by acting on V2 vasopressin receptors in cyst epithelial cells to increase camp. Tolvaptan, the only approved therapy for ADPKD, is a V2 receptor antagonist and has been shown to slow the increase in kidney volume [30]. As such, caffeine might have a beneficial effect on cellular camp levels through suppressing vasopressin levels that might counteract some or all of its effects on phosphodiesterases. However, no studies have shown the effects of caffeine intake on serum sodium concentration, urine osmolarity, urine volume and body fluid parameters in patients with chronic kidney disease. It is also important to note that studies completed on healthy adults have shown no effect of caffeine on these values [31, 32]. Finally, the effect of caffeine may have been masked by the presence of hypertension. Hypertension was a significant risk factor for disease progression in all of our models, and it is well known that acute consumption of caffeine increases blood pressure [33]. The relationship between chronic consumption of caffeine and hypertension is less clear. In some studies, chronic consumption of caffeine did not increase the frequency or severity of hypertension while in others, including one specifically studying ADPKD rats, it was associated with worsening of hypertension [9, 21, 34, 35]. Additionally, it is believed that caffeine exerts a variable response on hypertension due to genetic differences [36]. Thus it is possible that caffeine may exacerbate the deleterious effects of hypertension on ADPKD progression. There are several limitations of this study. We assessed caffeine intake at baseline. Although caffeine intake is thought to be habitual and is not expected to change over time, some patients in our sample reported varying caffeine intake over time. This could be for many reasons. In 2015, KDIGO Guidelines included a formal recommendation for patients with ADPKD to avoid caffeine intake [8]. While this formal recommendation most likely did not impact this study because this data was collected before 2015, these guidelines reflect the general tendency to recommend that patients with ADPKD restrict caffeine intake. While these factors may have contributed to the results of this study, by analyzing only the baseline caffeine values, we emulated the clinical situation in which information might be limited to a single snapshot of the patient s environmental and lifestyle exposures. Another limitation is that CRISP was an observational prospective cohort study and the lifestyle data was self-reported. Additionally, caffeine content from food and the variability of caffeine content in beverages was not recorded in the CRISP questionnaire. As our primary analysis examined caffeine consumption as any vs. none, it may be limited by not including caffeine sources beyond coffee, tea and soft drinks. Finally, because the patients in CRISP were enrolled when they had relatively preserved GFR, the average rate of GFR decline is slow and few patients have reached ESRD so far, thus limiting the power to detect the effect of caffeine consumption on these outcomes. Our study has several important strengths. CRISP is the largest and longest cohort study of ADPKD with a follow-up time of 14 years. This gave us the opportunity to explore the longitudinal relationship between caffeine and ADPKD progression, as measured by both httkv and mgfr, over an extended timeframe. Another strength of this study was the availability of information on the intake of caffeinated beverages other than coffee and tea. This is important because beverages such as sodas constitute a significant source of dietary caffeine, particularly in the U.S. population. Finally, all the patients in this study were genotyped for PKD1 and PKD2 mutations, allowing us to adjust for the confounding effect of the PKD genes and allelic effects on both outcomes. The most important strength of this study is that it used data from the CRISP cohort. The only other longitudinal study of caffeine and ADPKD progression was the study completed by Girardat-Rotar et al. in the Swiss ADPKD cohort [11]. While this study agreed with the conclusions of the Swiss ADPKD study, there are several key distinctions. First, this study had a sample size of 239 compared to the Swiss ADPKD sample size of 151. Second, the Swiss ADPKD study had a median follow-up time of 4.4 years while this study had a median follow-up time of 12.5 years. Third, the Swiss ADPKD study examined only coffee consumption as a caffeine source while this study included caffeinated beverages beyond coffee. Lastly, the Swiss study did not adjust for genotype while this study was able to utilize genetic information. Conclusions In summary, we did not find compelling evidence that caffeine had a clinically significant detrimental effect on
9 McKenzie et al. BMC Nephrology (2018) 19:378 Page 9 of 10 disease progression in patients with ADPKD. These conclusions are consistent with recent publications including the Girardat-Rotar et al. study [11] and a metaanalysis [25] all concluding that caffeine was not associated with chronic kidney disease. Current recommendations to avoid caffeine exposure in ADPKD are not supported by this and other clinical evidence. Additional files Additional file 1: Survey questions asked of patients concerning their environmental exposures, specifically regarding caffeine consumption. (PDF 231 kb) Additional file 2: Description of all models and results from sensitivity analyses. (DOCX 102 kb) Abbreviations ADPKD: Autosomal dominant polycystic kidney disease; camp: 3 :5 -cyclic adenosine monophosphate; CFTR: Cystic fibrosis transmembrane conductance regulator; CRISP: Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease; ESRD: End stage renal disease; httkv: Height adjusted total kidney volume; mgfr: Iothalamate clearance; NMD: No mutation detected Acknowledgements We are grateful to Dr. Michael Flessner of the NIDDK for providing guidance to the CRISP consortium. The investigators are indebted to the study coordinators in CRISP. The results presented in this paper have not been published previously in whole or part, except in abstract format. The data analysis for this research was completed at the University of Kansas Medical Center. Funding The CRISP study is supported by cooperative agreements from the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) of the National Institutes of Health (DK056943, DK056956, DK056957, DK056961). This study was also supported in part by the NIDDK through P30 grants to the Kansas PKD Research and Translation Core Center (DK106912) and the Mayo Translational PKD Center (DK090728), by the National Center for Research Resources General Clinical Research Centers at each institution (RR000039, Emory University; RR00585, Mayo College of Medicine; RR23940, Kansas University Medical Center; RR000032, University of Alabama at Birmingham), and the National Center for Advancing Translational Sciences Clinical and Translational Science Awards at each institution (RR and TR000454, Emory; RR and TR000135, Mayo College of Medicine; RR and TR000001, Kansas University Medical Center; RR025777, TR and TR001417, University of Alabama at Birmingham; RR and TR000005, University of Pittsburgh School of Medicine). A program officer from the funding body (NIDDK) participated in the overall design of the CRISP study. The NIDDK had no role in the collection, analysis and interpretation of data and in writing the manuscript. Availability of data and materials The complete deidentified dataset ( Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease ) supporting the conclusions of this article is available upon written request to the NIDDK Data repository ( )andsigningofadatause Agreement. Authors contributions VET, PCH, ABC, MM, FFRO, KTB, DPL, WMB, ASLY contributed to the conception and overall design of the study and acquisition of the data. KAM, MET, ASLY, and JDM contributed to the implementation, design and interpretation of the analysis. KAM, ASLY and JDM drafted the initial manuscript. All authors were involved in critically revising the manuscript for important intellectual content and approved the submitted manuscript. Ethics approval and consent to participate Each participant in the CRISP study signed an informed consent to participate in the study. The study was approved by the Institutional Review Board (IRB) at the University of Kansas Medical Center (STUDY ). Consent for publication No individual level data was presented in this manuscript. Competing interests VET, PCH and MM have received research funding from Otsuka Pharmaceuticals. FFR is a consultant for Keryx and Kadmon and has received research funding from Otsuka and Genzyme. ABC is a consultant for Otsuka, Pfizer and Sanofi, and has received research funding from Boston Scientific, Kadmon and Otsuka. MM is also a consultant for Otsuka and Sanofi. All other authors declare no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Biostatistics, University of Kansas Medical Center, Mail Stop 1026, 3901 Rainbow Blvd., Kansas City, KS 66160, USA. 2 Division of Nephrology and Hypertension, Mayo Clinic, Rochester, MN, USA. 3 Section of Nephrology, University of Chicago School of Medicine, Chicago, IL, USA. 4 Division of Nephrology, University of Alabama and the Department of Veterans Affairs Medical Center, Birmingham, AL, USA. 5 Department of Internal Medicine, Emory University School of Medicine, Atlanta, GA, USA. 6 Department of Radiology, University of Pittsburgh School of Medicine, Pittsburgh, PA, USA. 7 Department of Biomedical Informatics, University of Pittsburgh School of Medicine, Pittsburgh, PA, USA. 8 Legacy Good Samaritan Hospital, Portland, OR, USA. 9 Division of Nephrology and Hypertension and the Jared Grantham Kidney Institute, University of Kansas Medical Center, Kansas City, KS, USA. Received: 19 March 2018 Accepted: 10 December 2018 References 1. Grantham JJ. Clinical practice. Autosomal dominant polycystic kidney disease. N Engl J Med. 2008;359(14): Brunelli SM, et al. End-stage renal disease in autosomal dominant polycystic kidney disease: a comparison of dialysis-related utilization and costs with other chronic kidney diseases. Clinicoecon Outcomes Res. 2015;7: Torres VE, Harris PC. Autosomal dominant polycystic kidney disease: the last 3 years. Kidney Int. 2009;76(2): US Food and Drug Administration. Drug Approval Package: Jynarque (tolvaptan). 2018; Available from: drugsatfda_docs/nda/2018/204441orig1s000toc.cfm. Accessed Oct Belibi FA, et al. Cyclic AMP promotes growth and secretion in human polycystic kidney epithelial cells. Kidney Int. 2004;66(3): Rinschen MM, Schermer B, Benzing T. Vasopressin-2 receptor signaling and autosomal dominant polycystic kidney disease: from bench to bedside and back again. J Am Soc Nephrol. 2014;25(6): Belibi FA, et al. The effect of caffeine on renal epithelial cells from patients with autosomal dominant polycystic kidney disease. J Am Soc Nephrol. 2002;13(11): Chapman AB, et al. Autosomal-dominant polycystic kidney disease (ADPKD): executive summary from a kidney disease: improving global outcomes (KDIGO) controversies conference. Kidney Int. 2015;88(1): Tanner GA, Tanner JA. Chronic caffeine consumption exacerbates hypertension in rats with polycystic kidney disease. Am J Kidney Dis. 2001;38(5): Vendramini LC, et al. Caffeine intake by patients with autosomal dominant polycystic kidney disease. Braz J Med Biol Res. 2012;45(9): Girardat-Rotar L, et al. Long-term effect of coffee consumption on autosomal dominant polycystic kidneys disease progression: results from the Suisse ADPKD, a prospective longitudinal cohort study. J Nephrol. 2018; 31(1): Bae KT, Commean PK, Lee J. Volumetric measurement of renal cysts and parenchyma using MRI: phantoms and patients with polycystic kidney disease. J Comput Assist Tomogr. 2000;24(4):614 9.
10 McKenzie et al. BMC Nephrology (2018) 19:378 Page 10 of Chapman AB, et al. Renal structure in early autosomal-dominant polycystic kidney disease (ADPKD): the consortium for radiologic imaging studies of polycystic kidney disease (CRISP) cohort. Kidney Int. 2003;64(3): Bae KT, et al. MRI-based kidney volume measurements in ADPKD: reliability and effect of gadolinium enhancement. Clin J Am Soc Nephrol. 2009;4(4): Grantham JJ, et al. Volume progression in polycystic kidney disease. N Engl J Med. 2006;354(20): Chapman AB, et al. Kidney volume and functional outcomes in autosomal dominant polycystic kidney disease. Clin J Am Soc Nephrol. 2012;7(3): Stevens LA, Levey AS. Measured GFR as a confirmatory test for estimated GFR. J Am Soc Nephrol. 2009;20(11): US Department of Agriculture, A.R.S., nutrient data laboratory. USDA National Nutrient Database for standard reference, release 28 (slightly revised). Version Current: May Beverages, coffee, brewed, prepared with tap water. Internet: Accessed June Caffeine in food Available from: from: health-canada/services/food-nutrition/food-safety/food-additives/caffeinefoods/foods.html. Accessed June Cornec-Le Gall E, et al. The PROPKD score: a new algorithm to predict renal survival in autosomal dominant polycystic kidney disease. J Am Soc Nephrol. 2016;27(3): Heyer CM, et al. Predicted mutation strength of nontruncating PKD1 mutations aids genotype-phenotype correlations in autosomal dominant polycystic kidney disease. J Am Soc Nephrol. 2016;27(9): Draper NR, Smith H. Applied regression analysis. New York: Wiley; Ozkok A, et al. Clinical characteristics and predictors of progression of chronic kidney disease in autosomal dominant polycystic kidney disease: a single center experience. Clin Exp Nephrol. 2013;17(3): Schrier RW, et al. Predictors of autosomal dominant polycystic kidney disease progression. J Am Soc Nephrol. 2014;25(11): Wijarnpreecha K, et al. Association of coffee consumption and chronic kidney disease: a meta-analysis. Int J Clin Pract. 2017;71(1) /ijcp Petrovic D, et al. Relation of 24-hour urinary caffeine and caffeine metabolite excretions with self-reported consumption of coffee and other caffeinated beverages in the general population. Nutr Metab (Lond). 2016;13: Birkett DJ, Miners JO. Caffeine renal clearance and urine caffeine concentrations during steady state dosing. Implications for monitoring caffeine intake during sports events. Br J Clin Pharmacol. 1991;31(4): Osswald H, Schnermann J. Methylxanthines and the kidney. Handb Exp Pharmacol. 2011;200: Shirley DG, Walter SJ, Noormohamed FH. Natriuretic effect of caffeine: assessment of segmental sodium reabsorption in humans. Clin Sci (Lond). 2002;103(5): Higashihara E, et al. Tolvaptan in autosomal dominant polycystic kidney disease: three years' experience. Clin J Am Soc Nephrol. 2011;6(10): Killer SC, Blannin AK, Jeukendrup AE. No evidence of dehydration with moderate daily coffee intake: a counterbalanced cross-over study in a free-living population. PLoS One. 2014;9(1):e Zhang Y, et al. Caffeine and diuresis during rest and exercise: a meta-analysis. J Sci Med Sport. 2015;18(5): Robertson D, et al. Effects of caffeine on plasma renin activity, catecholamines and blood pressure. N Engl J Med. 1978;298(4): Mesas AE, et al. The effect of coffee on blood pressure and cardiovascular disease in hypertensive individuals: a systematic review and meta-analysis. Am J Clin Nutr. 2011;94(4): Cano-Marquina A, Tarin JJ, Cano A. The impact of coffee on health. Maturitas. 2013;75(1): Renda G, et al. Genetic determinants of blood pressure responses to caffeine drinking. Am J Clin Nutr. 2012;95(1):241 8.
HHS Public Access Author manuscript Am J Kidney Dis. Author manuscript; available in PMC 2017 July 05.
 HHS Public Access Author manuscript Published in final edited form as: Am J Kidney Dis. 2017 March ; 69(3): 482 484. doi:10.1053/j.ajkd.2016.10.021. Performance of the Chronic Kidney Disease Epidemiology
HHS Public Access Author manuscript Published in final edited form as: Am J Kidney Dis. 2017 March ; 69(3): 482 484. doi:10.1053/j.ajkd.2016.10.021. Performance of the Chronic Kidney Disease Epidemiology
Shuma Hirashio 1,2, Shigehiro Doi 1 and Takao Masaki 1*
 Hirashio et al. Renal Replacement Therapy (2018) 4:24 https://doi.org/10.1186/s41100-018-0164-9 CASE REPORT Open Access Magnetic resonance imaging is effective for evaluating the therapeutic effect of
Hirashio et al. Renal Replacement Therapy (2018) 4:24 https://doi.org/10.1186/s41100-018-0164-9 CASE REPORT Open Access Magnetic resonance imaging is effective for evaluating the therapeutic effect of
Autosomal Dominant Polycystic Kidney Disease. Dr. Sameena Iqbal Nephrologist CIUSSS West Island
 Autosomal Dominant Polycystic Kidney Disease Dr. Sameena Iqbal Nephrologist CIUSSS West Island Disclosure Honorarium for Consulting on the Reprise trial from Otsuka Mayo clinic preceptorship for PKD with
Autosomal Dominant Polycystic Kidney Disease Dr. Sameena Iqbal Nephrologist CIUSSS West Island Disclosure Honorarium for Consulting on the Reprise trial from Otsuka Mayo clinic preceptorship for PKD with
clinical investigation see commentary on page 14
 clinical investigation http://www.kidney-international.org 21 International Society of Nephrology see commentary on page 14 A comparison of ultrasound and magnetic resonance imaging shows that kidney length
clinical investigation http://www.kidney-international.org 21 International Society of Nephrology see commentary on page 14 A comparison of ultrasound and magnetic resonance imaging shows that kidney length
Nephrology Grand Rounds. Vasishta Tatapudi, MD January 24 th, 2013
 Nephrology Grand Rounds Vasishta Tatapudi, MD January 24 th, 2013 Case Summary Chief complaint: A twenty-six year old African American female veteran presented to ER with left flank pain for two days.
Nephrology Grand Rounds Vasishta Tatapudi, MD January 24 th, 2013 Case Summary Chief complaint: A twenty-six year old African American female veteran presented to ER with left flank pain for two days.
Volume Progression in Polycystic Kidney Disease
 The new england journal of medicine original article Volume Progression in Polycystic Kidney Disease Jared J. Grantham, M.D., Vicente E. Torres, M.D., Arlene B. Chapman, M.D., Lisa M. Guay-Woodford, M.D.,
The new england journal of medicine original article Volume Progression in Polycystic Kidney Disease Jared J. Grantham, M.D., Vicente E. Torres, M.D., Arlene B. Chapman, M.D., Lisa M. Guay-Woodford, M.D.,
Total Kidney Volume (TKV) in Autosomal Dominant Polycystic Kidney Disease as model for biomarker qualification
 Total Kidney Volume (TKV) in Autosomal Dominant Polycystic Kidney Disease as model for biomarker qualification Roslyn Simms NIHR Clinical Lecturer in Nephrology NIHR Clinical Trials Fellow Monday 23 rd
Total Kidney Volume (TKV) in Autosomal Dominant Polycystic Kidney Disease as model for biomarker qualification Roslyn Simms NIHR Clinical Lecturer in Nephrology NIHR Clinical Trials Fellow Monday 23 rd
Age- and height-adjusted total kidney volume growth rate in autosomal dominant polycystic kidney diseases
 https://doi.org/10.1007/s10157-018-1617-8 ORIGINAL ARTICLE Age- and height-adjusted total kidney volume growth rate in autosomal dominant polycystic kidney diseases Eiji Higashihara 1 Kouji Yamamoto 5
https://doi.org/10.1007/s10157-018-1617-8 ORIGINAL ARTICLE Age- and height-adjusted total kidney volume growth rate in autosomal dominant polycystic kidney diseases Eiji Higashihara 1 Kouji Yamamoto 5
Summary. 20 May 2014 EMA/CHMP/SAWP/298348/2014 Procedure No.: EMEA/H/SAB/037/1/Q/2013/SME Product Development Scientific Support Department
 20 May 2014 EMA/CHMP/SAWP/298348/2014 Procedure No.: EMEA/H/SAB/037/1/Q/2013/SME Product Development Scientific Support Department evaluating patients with Autosomal Dominant Polycystic Kidney Disease
20 May 2014 EMA/CHMP/SAWP/298348/2014 Procedure No.: EMEA/H/SAB/037/1/Q/2013/SME Product Development Scientific Support Department evaluating patients with Autosomal Dominant Polycystic Kidney Disease
SUISSE ADPKD Cohort Treatment and Outcomes with Tolvaptan, first in class Vasopressin V2 Antagonist. Hirslanden, 22 March 2018 Stefan Russmann
 SUISSE ADPKD Cohort Treatment and Outcomes with Tolvaptan, first in class Vasopressin V2 Antagonist Hirslanden, 22 March 2018 Stefan Russmann 4 th of July 2004 Database development with outcomes and safety
SUISSE ADPKD Cohort Treatment and Outcomes with Tolvaptan, first in class Vasopressin V2 Antagonist Hirslanden, 22 March 2018 Stefan Russmann 4 th of July 2004 Database development with outcomes and safety
ADPKD, what have the last 10 years taught us? Arlene B. Chapman MD Professor of Medicine Director, Section of Nephrology University of Chicago
 2016 ADPKD, what have the last 10 years taught us? Arlene B. Chapman MD Professor of Medicine Director, Section of Nephrology University of Chicago 2016 Can we TRUMP the cysts? Disclosures Consultant for
2016 ADPKD, what have the last 10 years taught us? Arlene B. Chapman MD Professor of Medicine Director, Section of Nephrology University of Chicago 2016 Can we TRUMP the cysts? Disclosures Consultant for
Cost-effectiveness of tolvaptan (Jinarc ) for the treatment of autosomal dominant polycystic kidney disease (ADPKD)
 Cost-effectiveness of tolvaptan (Jinarc ) for the treatment of autosomal dominant polycystic kidney disease (ADPKD) The NCPE has issued a recommendation regarding the cost-effectiveness of tolvaptan (Jinarc
Cost-effectiveness of tolvaptan (Jinarc ) for the treatment of autosomal dominant polycystic kidney disease (ADPKD) The NCPE has issued a recommendation regarding the cost-effectiveness of tolvaptan (Jinarc
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Weintraub WS, Grau-Sepulveda MV, Weiss JM, et al. Comparative
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Weintraub WS, Grau-Sepulveda MV, Weiss JM, et al. Comparative
Predictors of the progression of renal disease in the Modification of Diet in Renal Disease Study
 Kidney International, Vol. 51 (/997), pp. 198 19/9 Predictors of the progression of renal disease in the Modification of Diet in Renal Disease Study MODIFICATION OF DIET IN RENAL DISEASE STUDY GROUP, prepared
Kidney International, Vol. 51 (/997), pp. 198 19/9 Predictors of the progression of renal disease in the Modification of Diet in Renal Disease Study MODIFICATION OF DIET IN RENAL DISEASE STUDY GROUP, prepared
HHS Public Access Author manuscript Kidney Int. Author manuscript; available in PMC 2018 February 01.
 Dietary salt restriction is beneficial to the management of Autosomal Dominant Polycystic Kidney Disease Vicente E. Torres, MD PhD, Kaleab Z. Abebe, PhD, Robert W. Schrier, MD, Ronald D. Perrone, MD, Arlene
Dietary salt restriction is beneficial to the management of Autosomal Dominant Polycystic Kidney Disease Vicente E. Torres, MD PhD, Kaleab Z. Abebe, PhD, Robert W. Schrier, MD, Ronald D. Perrone, MD, Arlene
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
Supplementary Online Content
 Supplementary Online Content Tangri N, Stevens LA, Griffith J, et al. A predictive model for progression of chronic kidney disease to kidney failure. JAMA. 2011;305(15):1553-1559. eequation. Applying the
Supplementary Online Content Tangri N, Stevens LA, Griffith J, et al. A predictive model for progression of chronic kidney disease to kidney failure. JAMA. 2011;305(15):1553-1559. eequation. Applying the
Segmentation of Individual Renal Cysts from MR Images in Patients with Autosomal Dominant Polycystic Kidney Disease
 Article Segmentation of Individual Renal Cysts from MR Images in Patients with Autosomal Dominant Polycystic Kidney Disease Kyungsoo Bae,* Bumwoo Park,* Hongliang Sun,* Jinhong Wang,* Cheng Tao,* Arlene
Article Segmentation of Individual Renal Cysts from MR Images in Patients with Autosomal Dominant Polycystic Kidney Disease Kyungsoo Bae,* Bumwoo Park,* Hongliang Sun,* Jinhong Wang,* Cheng Tao,* Arlene
Lecture Outline. Biost 517 Applied Biostatistics I. Purpose of Descriptive Statistics. Purpose of Descriptive Statistics
 Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 3: Overview of Descriptive Statistics October 3, 2005 Lecture Outline Purpose
Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 3: Overview of Descriptive Statistics October 3, 2005 Lecture Outline Purpose
Supplementary Online Content
 Supplementary Online Content Tsai WC, Wu HY, Peng YS, et al. Association of intensive blood pressure control and kidney disease progression in nondiabetic patients with chronic kidney disease: a systematic
Supplementary Online Content Tsai WC, Wu HY, Peng YS, et al. Association of intensive blood pressure control and kidney disease progression in nondiabetic patients with chronic kidney disease: a systematic
Lecture Outline Biost 517 Applied Biostatistics I
 Lecture Outline Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 2: Statistical Classification of Scientific Questions Types of
Lecture Outline Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 2: Statistical Classification of Scientific Questions Types of
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
MANAGEMENT CALL TO DISCUSS LONGER-TERM IMPROVEMENTS IN KIDNEY FUNCTION WITH BARDOXOLONE
 MANAGEMENT CALL TO DISCUSS LONGER-TERM IMPROVEMENTS IN KIDNEY FUNCTION WITH BARDOXOLONE Introduction Substantial body of prior CKD clinical data characterizes Bard s unique profile Bard has demonstrated
MANAGEMENT CALL TO DISCUSS LONGER-TERM IMPROVEMENTS IN KIDNEY FUNCTION WITH BARDOXOLONE Introduction Substantial body of prior CKD clinical data characterizes Bard s unique profile Bard has demonstrated
Patient Survey of current water Intake practices in autosomal dominant Polycystic kidney disease: the SIPs survey
 Clinical Kidney Journal, 2017, 1 5 doi: 10.1093/ckj/sfw153 Original Article ORIGINAL ARTICLE Patient Survey of current water Intake practices in autosomal dominant Polycystic kidney disease: the SIPs survey
Clinical Kidney Journal, 2017, 1 5 doi: 10.1093/ckj/sfw153 Original Article ORIGINAL ARTICLE Patient Survey of current water Intake practices in autosomal dominant Polycystic kidney disease: the SIPs survey
Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol
 Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Autosomal dominant polycystic kidney disease (AD-
 A Pilot Clinical Study to Evaluate Changes in Urine Osmolality and Urine camp in Response to Acute and Chronic Water Loading in Autosomal Dominant Polycystic Kidney Disease Irina Barash,* Manish P. Ponda,*
A Pilot Clinical Study to Evaluate Changes in Urine Osmolality and Urine camp in Response to Acute and Chronic Water Loading in Autosomal Dominant Polycystic Kidney Disease Irina Barash,* Manish P. Ponda,*
Laura Girardat-Rotar 1, Julia Braun 1, Milo A. Puhan 1, Alison G. Abraham 1,2 and Andreas L. Serra 1,3*
 Girardat-Rotar et al. BMC Nephrology (2017) 18:241 DOI 10.1186/s12882-017-0654-y RESEARCH ARTICLE Open Access Temporal and geographical external validation study and extension of the Mayo Clinic prediction
Girardat-Rotar et al. BMC Nephrology (2017) 18:241 DOI 10.1186/s12882-017-0654-y RESEARCH ARTICLE Open Access Temporal and geographical external validation study and extension of the Mayo Clinic prediction
Long-term outcomes in nondiabetic chronic kidney disease
 original article http://www.kidney-international.org & 28 International Society of Nephrology Long-term outcomes in nondiabetic chronic kidney disease V Menon 1, X Wang 2, MJ Sarnak 1, LH Hunsicker 3,
original article http://www.kidney-international.org & 28 International Society of Nephrology Long-term outcomes in nondiabetic chronic kidney disease V Menon 1, X Wang 2, MJ Sarnak 1, LH Hunsicker 3,
Dominant Polycystic Kidney Disease (ADPKD) with a Focus on Imaging
 158 Klinische Kurzstandards Recommendations for Diagnostic and Prognostic Evaluation of Autosomal The Swiss Society of Radiology (SGR- SSR) and the Swiss Society of Nephrology Working Group of Inherited
158 Klinische Kurzstandards Recommendations for Diagnostic and Prognostic Evaluation of Autosomal The Swiss Society of Radiology (SGR- SSR) and the Swiss Society of Nephrology Working Group of Inherited
To treat patients with early chronic kidney disease
 Comparison of Methods for Determining Renal Function Decline in Early Autosomal Dominant Polycystic Kidney Disease: The Consortium of Radiologic Imaging Studies of Polycystic Kidney Disease Cohort Andrew
Comparison of Methods for Determining Renal Function Decline in Early Autosomal Dominant Polycystic Kidney Disease: The Consortium of Radiologic Imaging Studies of Polycystic Kidney Disease Cohort Andrew
3 generations of ADPKD. 1 long-awaited treatment.
 3 generations of ADPKD. 1 long-awaited treatment. HOPE is finally here now that treatment is available for people with autosomal dominant polycystic kidney disease (ADPKD). JYNARQUE is proven to slow kidney
3 generations of ADPKD. 1 long-awaited treatment. HOPE is finally here now that treatment is available for people with autosomal dominant polycystic kidney disease (ADPKD). JYNARQUE is proven to slow kidney
Delaying Progression of Renal Complications of Autosomal Dominant Polycystic Kidney Disease by Tolvaptan Inhibition of Arginine Vasopressin
 Delaying Progression of Renal Complications of Autosomal Dominant Polycystic Kidney Disease by Tolvaptan Inhibition of Arginine Vasopressin Briefing Document for 5 August 2013 Advisory Committee Meeting
Delaying Progression of Renal Complications of Autosomal Dominant Polycystic Kidney Disease by Tolvaptan Inhibition of Arginine Vasopressin Briefing Document for 5 August 2013 Advisory Committee Meeting
Magnetic Resonance Imaging of Kidney and Cyst Volume in Children with ADPKD
 Article Magnetic Resonance Imaging of Kidney and Cyst Volume in Children with ADPKD Melissa A. Cadnapaphornchai,* Amirali Masoumi, John D. Strain, Kim McFann, and Robert W. Schrier Summary Background and
Article Magnetic Resonance Imaging of Kidney and Cyst Volume in Children with ADPKD Melissa A. Cadnapaphornchai,* Amirali Masoumi, John D. Strain, Kim McFann, and Robert W. Schrier Summary Background and
Chapter 1: CKD in the General Population
 Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
The Seventh Report of the Joint National Commission
 The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
Lecture Outline. Biost 590: Statistical Consulting. Stages of Scientific Studies. Scientific Method
 Biost 590: Statistical Consulting Statistical Classification of Scientific Studies; Approach to Consulting Lecture Outline Statistical Classification of Scientific Studies Statistical Tasks Approach to
Biost 590: Statistical Consulting Statistical Classification of Scientific Studies; Approach to Consulting Lecture Outline Statistical Classification of Scientific Studies Statistical Tasks Approach to
Individual Study Table Referring to Part of Dossier: Volume: Page:
 Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Autosomal dominant polycystic kidney disease (ADPKD)
 CJASN epress. Published on November 29, 2010 as doi: 10.2215/CJN.03780410 Magnetic Resonance Imaging of Kidney and Cyst Volume in Children with ADPKD Melissa A. Cadnapaphornchai,* Amirali Masoumi, John
CJASN epress. Published on November 29, 2010 as doi: 10.2215/CJN.03780410 Magnetic Resonance Imaging of Kidney and Cyst Volume in Children with ADPKD Melissa A. Cadnapaphornchai,* Amirali Masoumi, John
Tolvaptan and Kidney Pain in Patients With Autosomal Dominant Polycystic Kidney Disease: Secondary Analysis From a Randomized Controlled Trial
 Tolvaptan and Kidney Pain in Patients With Autosomal Dominant Polycystic Kidney Disease: Secondary Analysis From a Randomized Controlled Trial Niek F. Casteleijn, University of Groningen Jaime D. Blais,
Tolvaptan and Kidney Pain in Patients With Autosomal Dominant Polycystic Kidney Disease: Secondary Analysis From a Randomized Controlled Trial Niek F. Casteleijn, University of Groningen Jaime D. Blais,
KDIGO Controversies Conference on Autosomal Dominant Polycystic Kidney Disease (ADPKD)
 KDIGO Controversies Conference on Autosomal Dominant Polycystic Kidney Disease (ADPKD) January 16 19, 2014 Edinburgh, United Kingdom Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Autosomal Dominant Polycystic Kidney Disease (ADPKD) January 16 19, 2014 Edinburgh, United Kingdom Kidney Disease: Improving Global Outcomes (KDIGO) is an international
ABSTRACT. n engl j med 371;24 nejm.org december 11,
 The new england journal of medicine established in 1812 december 11, 2014 vol. 371 no. 24 Blood Pressure in Early Autosomal Dominant Polycystic Kidney Disease Robert W. Schrier, M.D., Kaleab Z. Abebe,
The new england journal of medicine established in 1812 december 11, 2014 vol. 371 no. 24 Blood Pressure in Early Autosomal Dominant Polycystic Kidney Disease Robert W. Schrier, M.D., Kaleab Z. Abebe,
University of Groningen. Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste
 University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Academic Insights for Biomarker Priorities and Candidate Pilot Project(s)
 Academic Panel Session Academic Insights for Biomarker Priorities and Candidate Pilot Project(s) Moderators: Dr. Chirag Parikh (Yale) Dr. Kumar Sharma (UCSD) Panelists: Dr. Ronald Perrone (Tufts Medical
Academic Panel Session Academic Insights for Biomarker Priorities and Candidate Pilot Project(s) Moderators: Dr. Chirag Parikh (Yale) Dr. Kumar Sharma (UCSD) Panelists: Dr. Ronald Perrone (Tufts Medical
PRIMARY PHASE 2 ANALYSES FROM CARDINAL: A PHASE 2/3 STUDY OF BARDOXOLONE METHYL IN PATIENTS WITH ALPORT SYNDROME
 PRIMARY PHASE 2 ANALYSES FROM CARDINAL: A PHASE 2/3 STUDY OF BARDOXOLONE METHYL IN PATIENTS WITH ALPORT SYNDROME 217 American Society of Nephrology Meeting Geoffrey A. Block 1, Pablo E. Pergola 2, Lesley
PRIMARY PHASE 2 ANALYSES FROM CARDINAL: A PHASE 2/3 STUDY OF BARDOXOLONE METHYL IN PATIENTS WITH ALPORT SYNDROME 217 American Society of Nephrology Meeting Geoffrey A. Block 1, Pablo E. Pergola 2, Lesley
Tolvaptan: Slowing Progression of Autosomal Dominant Polycystic Kidney Disease (ADPKD)
 Tolvaptan: Slowing Progression of Autosomal Dominant Polycystic Kidney Disease (ADPKD) Cardiovascular and Renal Drugs Advisory Committee August 5, 2013 Introduction Robert McQuade, PhD Executive Vice President
Tolvaptan: Slowing Progression of Autosomal Dominant Polycystic Kidney Disease (ADPKD) Cardiovascular and Renal Drugs Advisory Committee August 5, 2013 Introduction Robert McQuade, PhD Executive Vice President
Clinical Experience with Tolvaptan. Prof. Dr. med. O. Devuyst
 Clinical Experience with Tolvaptan Prof. Dr. med. O. Devuyst 1 Outline 1. ADPKD generalities and tolvaptan in ADPKD 2. Who to treat with tolvaptan? How to start? 3. Clinical experience with tolvaptan in
Clinical Experience with Tolvaptan Prof. Dr. med. O. Devuyst 1 Outline 1. ADPKD generalities and tolvaptan in ADPKD 2. Who to treat with tolvaptan? How to start? 3. Clinical experience with tolvaptan in
Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new (MDRD) prediction equation
 Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
ALLHAT RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR)
 1 RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR) 6 / 5 / 1006-1 2 Introduction Hypertension is the second most common cause of end-stage
1 RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR) 6 / 5 / 1006-1 2 Introduction Hypertension is the second most common cause of end-stage
Biost 590: Statistical Consulting
 Biost 590: Statistical Consulting Statistical Classification of Scientific Questions October 3, 2008 Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics, University of Washington 2000, Scott S. Emerson,
Biost 590: Statistical Consulting Statistical Classification of Scientific Questions October 3, 2008 Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics, University of Washington 2000, Scott S. Emerson,
Is tolvaptan a promising ally in the treatment strategy of autosomal dominant polycystic kidney disease?
 PERSPECTIVE Port J Nephrol Hypert 2017; 31(4): 243-248 Advance Access publication 4 January 2018 Is tolvaptan a promising ally in the treatment strategy of autosomal dominant polycystic kidney disease?
PERSPECTIVE Port J Nephrol Hypert 2017; 31(4): 243-248 Advance Access publication 4 January 2018 Is tolvaptan a promising ally in the treatment strategy of autosomal dominant polycystic kidney disease?
The CARI Guidelines Caring for Australasians with Renal Impairment. Protein Restriction to prevent the progression of diabetic nephropathy GUIDELINES
 Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Hasan Fattah 3/19/2013
 Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
Hasan Fattah 3/19/2013 AASK trial Rational: HTN is a leading cause of (ESRD) in the US, with no known treatment to prevent progressive declines leading to ESRD. Objective: To compare the effects of 2 levels
Research Introduction
 Research Introduction 9.17.13 Altered metabolism in polycystic kidney disease Telomerase activity in polycystic kidney disease cells Autosomal dominant polycystic kidney disease ADPKD is the most common
Research Introduction 9.17.13 Altered metabolism in polycystic kidney disease Telomerase activity in polycystic kidney disease cells Autosomal dominant polycystic kidney disease ADPKD is the most common
microrna Therapeutics Harnessing the power of micrornas to target multiple pathways of disease
 microrna Therapeutics Harnessing the power of micrornas to target multiple pathways of disease January 2018 Safe Harbor Statement Statements contained in this presentation regarding matters that are not
microrna Therapeutics Harnessing the power of micrornas to target multiple pathways of disease January 2018 Safe Harbor Statement Statements contained in this presentation regarding matters that are not
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Biostatistics II
 Biostatistics II 514-5509 Course Description: Modern multivariable statistical analysis based on the concept of generalized linear models. Includes linear, logistic, and Poisson regression, survival analysis,
Biostatistics II 514-5509 Course Description: Modern multivariable statistical analysis based on the concept of generalized linear models. Includes linear, logistic, and Poisson regression, survival analysis,
Title:Impaired renal function and associated risk factors in newly diagnosed HIV-infected Adults in Gulu Hospital, Northern Uganda
 Author's response to reviews Title:Impaired renal function and associated risk factors in newly diagnosed HIV-infected Adults in Gulu Hospital, Northern Uganda Authors: Pancras Odongo (odongopancras@gmail.com)
Author's response to reviews Title:Impaired renal function and associated risk factors in newly diagnosed HIV-infected Adults in Gulu Hospital, Northern Uganda Authors: Pancras Odongo (odongopancras@gmail.com)
Tolvaptan bei ADPKD: Kritische Beurteilung der Studien
 Tolvaptan bei ADPKD: Kritische Beurteilung der Studien Johannes Mann & Stewart Lambie * KfH Nierenzentrum München Schwabing, Klinik für Nieren- & Hochdruckkrankheiten, Friedrich Alexander Univ. Erlangen-Nürnberg
Tolvaptan bei ADPKD: Kritische Beurteilung der Studien Johannes Mann & Stewart Lambie * KfH Nierenzentrum München Schwabing, Klinik für Nieren- & Hochdruckkrankheiten, Friedrich Alexander Univ. Erlangen-Nürnberg
Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts Future Cardiovascular Events
 Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Grayscale ultrasound characteristics of autosomal dominant polycystic kidney disease severity an adult and pediatric cohort study
 Original paper Cite as: Strzelczyk M, Podgórski M, Afshari S, Tkaczyk M, Pawlak-Bratkowska M, Grzelak P: Grayscale ultrasound characteristics of autosomal dominant polycystic kidney disease severity an
Original paper Cite as: Strzelczyk M, Podgórski M, Afshari S, Tkaczyk M, Pawlak-Bratkowska M, Grzelak P: Grayscale ultrasound characteristics of autosomal dominant polycystic kidney disease severity an
BEST PRACTICES FOR IMPLEMENTATION AND ANALYSIS OF PAIN SCALE PATIENT REPORTED OUTCOMES IN CLINICAL TRIALS
 BEST PRACTICES FOR IMPLEMENTATION AND ANALYSIS OF PAIN SCALE PATIENT REPORTED OUTCOMES IN CLINICAL TRIALS Nan Shao, Ph.D. Director, Biostatistics Premier Research Group, Limited and Mark Jaros, Ph.D. Senior
BEST PRACTICES FOR IMPLEMENTATION AND ANALYSIS OF PAIN SCALE PATIENT REPORTED OUTCOMES IN CLINICAL TRIALS Nan Shao, Ph.D. Director, Biostatistics Premier Research Group, Limited and Mark Jaros, Ph.D. Senior
Autosomal-dominant polycystic kidney disease (AD-
 Magnetic Resonance Imaging Evaluation of Hepatic Cysts in Early Autosomal-Dominant Polycystic Kidney Disease: The Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease Cohort Kyongtae
Magnetic Resonance Imaging Evaluation of Hepatic Cysts in Early Autosomal-Dominant Polycystic Kidney Disease: The Consortium for Radiologic Imaging Studies of Polycystic Kidney Disease Cohort Kyongtae
DISCLOSURES OUTLINE OUTLINE 9/29/2014 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE
 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
Survival Prediction Models for Estimating the Benefit of Post-Operative Radiation Therapy for Gallbladder Cancer and Lung Cancer
 Survival Prediction Models for Estimating the Benefit of Post-Operative Radiation Therapy for Gallbladder Cancer and Lung Cancer Jayashree Kalpathy-Cramer PhD 1, William Hersh, MD 1, Jong Song Kim, PhD
Survival Prediction Models for Estimating the Benefit of Post-Operative Radiation Therapy for Gallbladder Cancer and Lung Cancer Jayashree Kalpathy-Cramer PhD 1, William Hersh, MD 1, Jong Song Kim, PhD
Lucia Cea Soriano 1, Saga Johansson 2, Bergur Stefansson 2 and Luis A García Rodríguez 1*
 Cea Soriano et al. Cardiovascular Diabetology (2015) 14:38 DOI 10.1186/s12933-015-0204-5 CARDIO VASCULAR DIABETOLOGY ORIGINAL INVESTIGATION Open Access Cardiovascular events and all-cause mortality in
Cea Soriano et al. Cardiovascular Diabetology (2015) 14:38 DOI 10.1186/s12933-015-0204-5 CARDIO VASCULAR DIABETOLOGY ORIGINAL INVESTIGATION Open Access Cardiovascular events and all-cause mortality in
Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York
 Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York 4th International Conference on Nephrology & Therapeutics September 14, 2015 Baltimore,
Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York 4th International Conference on Nephrology & Therapeutics September 14, 2015 Baltimore,
Learning Objectives 9/9/2013. Hypothesis Testing. Conflicts of Interest. Descriptive statistics: Numerical methods Measures of Central Tendency
 Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Last-Chance Ambulatory Care Webinar Thursday, September 5, 2013 Learning Objectives For
Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Last-Chance Ambulatory Care Webinar Thursday, September 5, 2013 Learning Objectives For
Discontinuation and restarting in patients on statin treatment: prospective open cohort study using a primary care database
 open access Discontinuation and restarting in patients on statin treatment: prospective open cohort study using a primary care database Yana Vinogradova, 1 Carol Coupland, 1 Peter Brindle, 2,3 Julia Hippisley-Cox
open access Discontinuation and restarting in patients on statin treatment: prospective open cohort study using a primary care database Yana Vinogradova, 1 Carol Coupland, 1 Peter Brindle, 2,3 Julia Hippisley-Cox
9/4/2013. Decision Errors. Hypothesis Testing. Conflicts of Interest. Descriptive statistics: Numerical methods Measures of Central Tendency
 Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Pharmacotherapy Webinar Review Course Tuesday, September 3, 2013 Descriptive statistics:
Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Pharmacotherapy Webinar Review Course Tuesday, September 3, 2013 Descriptive statistics:
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
Senior Vice President, Medical Affairs and Health Outcomes, 150 South Saunders Road, Lake Forest, IL 60045, Horizon Pharma USA, Inc, USA
 Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
AKI: definitions, detection & pitfalls. Jon Murray
 AKI: definitions, detection & pitfalls Jon Murray Previous conventional definition Acute renal failure (ARF) An abrupt and sustained decline in renal excretory function due to a reduction in glomerular
AKI: definitions, detection & pitfalls Jon Murray Previous conventional definition Acute renal failure (ARF) An abrupt and sustained decline in renal excretory function due to a reduction in glomerular
Technology appraisal guidance Published: 28 October 2015 nice.org.uk/guidance/ta358
 Tolvaptan for treating autosomal dominant polycystic kidney disease Technology appraisal guidance Published: 28 October 2015 nice.org.uk/guidance/ta358 NICE 2017. All rights reserved. Subject to Notice
Tolvaptan for treating autosomal dominant polycystic kidney disease Technology appraisal guidance Published: 28 October 2015 nice.org.uk/guidance/ta358 NICE 2017. All rights reserved. Subject to Notice
HHS Public Access Author manuscript Kidney Int. Author manuscript; available in PMC 2015 March 01.
 Urinary sodium excretion and kidney failure in non-diabetic chronic kidney disease Li Fan, MD 1, Hocine Tighiouart 2, Andrew S. Levey, MD 1, Gerald J. Beck, PhD 3, and Mark J. Sarnak, MD, MS 1 1 Division
Urinary sodium excretion and kidney failure in non-diabetic chronic kidney disease Li Fan, MD 1, Hocine Tighiouart 2, Andrew S. Levey, MD 1, Gerald J. Beck, PhD 3, and Mark J. Sarnak, MD, MS 1 1 Division
BASELINE CHARACTERISTICS OF THE STUDY POPULATION
 COMPARISON OF TREATING METABOLIC ACIDOSIS IN CKD STAGE 4 HYPERTENSIVE KIDNEY DISEASE WITH FRUITS & VEGETABLES OR SODIUM BICARBONATE This was a 1-year, single-center, prospective, randomized, interventional
COMPARISON OF TREATING METABOLIC ACIDOSIS IN CKD STAGE 4 HYPERTENSIVE KIDNEY DISEASE WITH FRUITS & VEGETABLES OR SODIUM BICARBONATE This was a 1-year, single-center, prospective, randomized, interventional
AGING KIDNEY IN HIV DISEASE
 AGING KIDNEY IN HIV DISEASE Michael G. Shlipak, MD, MPH Professor of Medicine, Epidemiology and Biostatistics, UCSF Chief, General Internal Medicine, San Francisco VA Medical Center Kidney, Aging and HIV
AGING KIDNEY IN HIV DISEASE Michael G. Shlipak, MD, MPH Professor of Medicine, Epidemiology and Biostatistics, UCSF Chief, General Internal Medicine, San Francisco VA Medical Center Kidney, Aging and HIV
tolvaptan 15mg, 30mg, 45mg, 60mg and 90mg tablets (Jinarc ) Otsuka Pharmaceuticals (UK) Ltd SMC No. (1114/15)
 tolvaptan 15mg, 30mg, 45mg, 60mg and 90mg tablets (Jinarc ) Otsuka Pharmaceuticals (UK) Ltd SMC No. (1114/15) 04 December 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the
tolvaptan 15mg, 30mg, 45mg, 60mg and 90mg tablets (Jinarc ) Otsuka Pharmaceuticals (UK) Ltd SMC No. (1114/15) 04 December 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the
A Study on Type 2 Diabetes Mellitus Patients Using Regression Model and Survival Analysis Techniques
 Available online at www.ijpab.com Shaik et al Int. J. Pure App. Biosci. 6 (1): 514-522 (2018) ISSN: 2320 7051 DOI: http://dx.doi.org/10.18782/2320-7051.5999 ISSN: 2320 7051 Int. J. Pure App. Biosci. 6
Available online at www.ijpab.com Shaik et al Int. J. Pure App. Biosci. 6 (1): 514-522 (2018) ISSN: 2320 7051 DOI: http://dx.doi.org/10.18782/2320-7051.5999 ISSN: 2320 7051 Int. J. Pure App. Biosci. 6
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Tolvaptan: a Possible Treatment for Autosomal Dominant Polycystic Kidney Disease
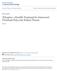 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Fall 9-20-2013 Tolvaptan: a Possible Treatment for Autosomal Dominant Polycystic Kidney
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Fall 9-20-2013 Tolvaptan: a Possible Treatment for Autosomal Dominant Polycystic Kidney
Closeout of the HALT Polycystic Kidney Disease Treatment Network Trials
 Closeout of the HALT Polycystic Kidney Disease Treatment Network Trials Society for Clinical Trials Philadelphia, PA Monday, May 19, 2014 Charity G. Moore, PhD Susan Spillane, RN, CCRP Marie Hogan, MD,
Closeout of the HALT Polycystic Kidney Disease Treatment Network Trials Society for Clinical Trials Philadelphia, PA Monday, May 19, 2014 Charity G. Moore, PhD Susan Spillane, RN, CCRP Marie Hogan, MD,
Acknowledgements. National Kidney Foundation of Connecticut Mark Perazella. Co-PI Slowing the progression of chronic kidney disease to ESRD
 A Practical Approach to Chronic Kidney Disease Management for the Primary Care Practioner: A web-site sponsored by the National Kidney Foundation of Connecticut Robert Reilly, M.D. Acknowledgements National
A Practical Approach to Chronic Kidney Disease Management for the Primary Care Practioner: A web-site sponsored by the National Kidney Foundation of Connecticut Robert Reilly, M.D. Acknowledgements National
Chronic kidney disease (CKD) has received
 Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Reducing proteinuria
 Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
A systematic review of the predictors of disease progression in patients with autosomal dominant polycystic kidney disease
 Woon et al. BMC Nephrology DOI 10.1186/s12882-015-0114-5 RESEARCH ARTICLE Open Access A systematic review of the predictors of disease progression in patients with autosomal dominant polycystic kidney
Woon et al. BMC Nephrology DOI 10.1186/s12882-015-0114-5 RESEARCH ARTICLE Open Access A systematic review of the predictors of disease progression in patients with autosomal dominant polycystic kidney
Catherine A. Welch 1*, Séverine Sabia 1,2, Eric Brunner 1, Mika Kivimäki 1 and Martin J. Shipley 1
 Welch et al. BMC Medical Research Methodology (2018) 18:89 https://doi.org/10.1186/s12874-018-0548-0 RESEARCH ARTICLE Open Access Does pattern mixture modelling reduce bias due to informative attrition
Welch et al. BMC Medical Research Methodology (2018) 18:89 https://doi.org/10.1186/s12874-018-0548-0 RESEARCH ARTICLE Open Access Does pattern mixture modelling reduce bias due to informative attrition
Appendix D - NICE s response to consultee and commentator comments on the draft scope and provisional matrix
 Comment 1: the draft remit Appendix D - NICE s response to consultee and commentator comments on the draft scope and provisional matrix Single Technology Appraisal (STA) Tolvaptan for treating autosomal
Comment 1: the draft remit Appendix D - NICE s response to consultee and commentator comments on the draft scope and provisional matrix Single Technology Appraisal (STA) Tolvaptan for treating autosomal
Renal tubular secretion in chronic kidney disease: description, determinants, and outcomes. Astrid M Suchy-Dicey
 Renal tubular secretion in chronic kidney disease: description, determinants, and outcomes Astrid M Suchy-Dicey A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor
Renal tubular secretion in chronic kidney disease: description, determinants, and outcomes Astrid M Suchy-Dicey A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor
Clinical Study Acute Kidney Injury in ADPKD Patients with Pneumonia
 SAGE-Hindawi Access to Research International Nephrology Volume 2, Article ID 6794, 6 pages doi:.46/2/6794 Clinical Study Acute Kidney Injury in ADPKD Patients with Pneumonia Carlos Franco Palacios,, 2
SAGE-Hindawi Access to Research International Nephrology Volume 2, Article ID 6794, 6 pages doi:.46/2/6794 Clinical Study Acute Kidney Injury in ADPKD Patients with Pneumonia Carlos Franco Palacios,, 2
Disclosures. Outline. Outline 5/23/17 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
The CARI Guidelines Caring for Australasians with Renal Impairment. Blood Pressure Control role of specific antihypertensives
 Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
STATISTICS INFORMED DECISIONS USING DATA
 STATISTICS INFORMED DECISIONS USING DATA Fifth Edition Chapter 4 Describing the Relation between Two Variables 4.1 Scatter Diagrams and Correlation Learning Objectives 1. Draw and interpret scatter diagrams
STATISTICS INFORMED DECISIONS USING DATA Fifth Edition Chapter 4 Describing the Relation between Two Variables 4.1 Scatter Diagrams and Correlation Learning Objectives 1. Draw and interpret scatter diagrams
Chapter 2: Identification and Care of Patients With Chronic Kidney Disease
 Chapter 2: Identification and Care of Patients With Chronic Kidney Disease Introduction The examination of care in patients with chronic kidney disease (CKD) is a significant challenge, as most large datasets
Chapter 2: Identification and Care of Patients With Chronic Kidney Disease Introduction The examination of care in patients with chronic kidney disease (CKD) is a significant challenge, as most large datasets
Objectives. Pre-dialysis CKD: The Problem. Pre-dialysis CKD: The Problem. Objectives
 The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
Evidence-based practice in nephrology : Meta-analysis
 Evidence-based practice in nephrology : Meta-analysis Paweena Susantitaphong, MD,Ph.D 1-3 1 Associate Professor, Division of Nephrology, Department of Medicine, King Chulalongkorn Memorial Hospital, Chulalongkorn
Evidence-based practice in nephrology : Meta-analysis Paweena Susantitaphong, MD,Ph.D 1-3 1 Associate Professor, Division of Nephrology, Department of Medicine, King Chulalongkorn Memorial Hospital, Chulalongkorn
Disclosures. Outline. Outline 7/27/2017 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Dialysis Initiation and Optimal Vascular Access: Outcomes and Mortality
 Dialysis Initiation and Optimal Vascular Access: Outcomes and Mortality Shannon H. Norris, BSN, RN June 6, 2018 Dialysis Initiation and Optimal Vascular Access: Outcomes and Mortality DISCUSSION: End Stage
Dialysis Initiation and Optimal Vascular Access: Outcomes and Mortality Shannon H. Norris, BSN, RN June 6, 2018 Dialysis Initiation and Optimal Vascular Access: Outcomes and Mortality DISCUSSION: End Stage

 www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to
www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to