Environmental exposure to lead and progressive diabetic nephropathy in patients with type II diabetes
|
|
|
- Emil Rose
- 5 years ago
- Views:
Transcription
1 & 2006 International Society of Nephrology original article Environmental exposure to lead and progressive diabetic nephropathy in patients with type II diabetes J-L Lin 1, D-T Lin-Tan 1, C-C Yu 1, Y-J Li 1, Y-Y Huang 2 and K-L Li 2 1 Division of Nephrology and Clinical Toxicology, Chang Gung Memorial Hospital, Lin-Kou Medical Center, Chang Gung University and School of Medicine, Taipei, Taiwan, ROC and 2 Division of Metabolism and Endocrinology, Chang Gung Memorial Hospital, Lin-Kou Medical Center, Chang Gung University and School of Medicine, Taipei, Taiwan, ROC Studies indicate that environmental exposure to lead is associated with reduced renal function. Whether lead affects progressive diabetic nephropathy is unclear. Eighty-seven patients with type II diabetes and diabetic nephropathy (serum creatinine of mg/dl) with normal body lead burden and no lead exposure history were observed over a 12-month period. Thirty subjects with high normal body lead burdens ( lg) were randomly assigned to a chelation and control group. For 3 months, the 15 chelation-group patients underwent lead-chelation therapy with calcium disodium ethylenediaminetetraacetic acid weekly until body lead burden fell o60 lg, and the 15 control group subjects received a weekly placebo. During the following 12 months, renal function was regularly assessed at 3-month intervals. The primary outcome was an elevation of serum creatinine to 1.5 times baseline value during the observation period. A secondary outcome was temporal changes in renal function following chelation therapy. Twenty-six patients achieved the primary outcome. Basal blood lead levels and body lead burden were the most important risk factors in predicting progressive diabetic nephropathy. Following chelation, the rates of decline in glomerular filtration rates in the chelation group and the control group, respectively, were ml and ml/min/year/1.73 m 2 of body surface area (P ¼ ) during follow-up, although both groups had similar rates of progression of renal function during the 12-month observation period. We concluded that low-level environmental lead exposure accelerates progressive diabetic nephropathy and lead-chelation therapy can decrease its rate of progression. Kidney International (2006) 69, doi: /sj.ki ; published online 26 April 2006 KEYWORDS: environmental lead exposure; lead-chelation therapy; blood lead levels; body lead burden; diabetic nephropathy Correspondence: J-L Lin, Division of Nephrology and Clinical Toxicology, Chang Gung memorial Hospital, 199, Tung-Hwa North Road, Taipei, Taiwan, ROC. jllin99@hotmail.com Received 5 October 2005; revised 9 January 2006; accepted 10 February 2006; published online 26 April 2006 The relationship between heavy long-term lead exposure and chronic interstitial nephropathy is well recognized. 1 3 Several epidemiological studies 4,5 have identified a positive correlation between blood lead levels and age-related decreases in renal function in the general population, indicating that environmental lead exposure decreases renal function in healthy persons. However, those studies did not address other factors potentially related to progressive renal function deterioration such as daily urinary protein excretion, daily protein intake, etc. Moreover, blood lead levels only represent recent lead exposure and do not indicate body lead burden. 6 8 The most reliable methods of measuring body lead burden are X-ray fluorescence studies of bone lead content and calcium disodium ethylenediaminetetraacetic acid (EDTA) mobilization tests. 9 A body lead burden 4600 mg (2.90 mmol), as determined by calcium disodium EDTA mobilization, is deemed lead poisoning. A previous study by the same authors utilized EDTA mobilization tests to assess body lead burden in non-diabetic chronic renal insufficiency patients without history of lead exposure; analytical results demonstrated that environmental lead exposure accelerates progressive renal insufficiency. The incidence of diabetes mellitus, particularly type II diabetes, is increasing worldwide. Current estimate claims that 410% of the United States population is 16 affected by diabetes mellitus and accounts for 440% of all cases with end-stage renal disease. Additionally, the number of patients starting renal replacement therapy in US has grown exponentially over the past 20 years. Cases of end-stage renal disease attributed to diabetes, especially type II diabetes, accounted for the majority of this increase. 17 A recent prospective epidemiological study, 18 which published after this study was begun, analyzed changes in renal function in relation to baseline lead levels, diabetes, and hypertension among 448 middle-aged men over a 6-year period. That study suggested that both blood lead levels and bone lead content are associated with progressive increase of serum creatinine in diabetic patients. As other epidemiological studies, failing to adjust for daily urine protein excretion and glycosylated hemoglobin confounds their findings. However, the association between environmental lead exposure and Kidney International (2006) 69,
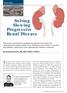
2 progressive renal insufficiency in patients with type II diabetes and diabetic nephropathy requires elucidation. This prospective study assessed whether chronic low-level environmental lead exposure increases the rate at which diabetic nephropathy progresses and whether lead-chelation therapy slows this progression in the type II diabetic patients. RESULTS Longitudinal observation period Eighty-seven patients completed the 12-month observation period (59 men and 28 women) (Figure 1). The following baseline data were obtained: patient mean age was years (range, years); body-mass index (weight in kilograms divided by the square of height in meters) was (range, ); serum creatinine level was mg/dl ( mmol/l; range, mg/dl ( mmol/l)); creatinine clearance rate was ml/min/1.73 m 2 of body surface area (range, ml/min/1.73 m 2 of body surface area); estimated glomerular filtration rate was ml/min/1.73 m 2 of body surface area (range, ml/min/1.73 m 2 of body surface area); daily protein excretion was g (range, g); daily protein intake was g/kg (range, g/kg); blood lead level was mg/dl ( mmol/l; range, mg/dl ( mmol/l)); and, body lead burden was mg ( mmol; range, mg, mmol)). Blood lead level correlated to body lead burden for all patients (r ¼ 0.306, P ¼ ). Fifty-seven patients (63.2%) had hyperlipidemia. Eighty-six patients (98.9%) had hypertension, that in 239 type II diabetes with serum Cr 1.5 and 3.9 mg/dl, without previous lead exposure 93 without laser therapy for diabetic retinopathy, 18 micro-hematuria, 14 daily urine protein excretion <0.5 g/day, 11 small-sized kidneys, three body lead burden >600 μg and 10 met exclusion criteria excluded 90 patients entered into the 12-month obervation period Two lost follow-up, and one died of acute myocardial infarction 87 completed the 12-month observation period Nine without diminished renal function at the end of observation period, 26 body lead burden < 80 μg, 16 serum creatinine > 3.9 mg/dl and six without written informed consents excluded 30 with BLB 80 μg and < 600 μg and serum Cr 1.5 and 3.9 mg/dl randomized 15 assigned to study group, received 3-month lead chelation 15 assigned to placebo group, received 3-month placebo therapy 15 completed the 12-month follow-up 15 completed the 12-month follow-up Figure 1 Flow chart showing the enrollment and status of patients Kidney International (2006) 69,
3 Table 1 Cox regression analysis of the overall risk of the primary outcome of progressive renal insufficiency, according to baseline prognostic factors Variable Hazard ratio (95% CI) a P-value Age (each increment of 1 year) 0.97 ( ) Female sex 1.56 ( ) Smoking 0.57 ( ) Use of insulin injection 0.96 ( ) Previous cardiovascular diseases 3.35 ( ) Baseline body-mass index (each 0.81 ( ) increment of 1) Mean arterial pressure (each increment 1.07 ( ) of 1 mm Hg) Baseline serum creatinine (each 1.36 ( ) increment of 1 mg/dl (88 mmol/l)) Body lead burden (each increment of 1.01 ( ) mg) HbA1c (%) (each increment of 1%) 0.92 ( ) Cholesterol (mg/dl) (each increment of 1.01 ( ) mg/dl) Baseline daily protein intake (each 5.29 ( ) increment of 1 g/kg) Baseline daily protein excretion (each increment of 1 g) 1.34 ( ) a CI denotes confidence interval. The body-mass index is the weight in kilograms divided by the square of the height in meters. The primary end point was defined as an increase in the serum creatinine level to 1.5 times the baseline value during the observation period. 84 patients (96.6%) was treated with angiotensin-converting enzyme inhibitors or angiotensin II receptor antagonists. Fifteen patients (17.2%) smoked. All patients had retinopathy that was treated with laser therapy. Among all study patients, 25 (28.7%) had a history of cardiovascular diseases, including myocardial infarction, stroke and diabetic foot. At the end of the 12-month observation period the following data were obtained: serum creatinine level was mg/dl ( mmol/l; range, mg/dl ( mmol/l)); creatinine clearance rate was ml/min/1.73 m 2 of body surface area (range, ml/min/1.73 m 2 of body surface area); and, estimated glomerular filtration rate was ml/min/1.73 m 2 of body surface area (range, /min/1.73 m 2 of body surface area). Twenty-six patients (29.9%) achieved the primary end point during the observation period; none, however, required hemodialysis. Only two of these 26 subjects had body lead burdens of o80 mg. Cox regression analysis demonstrated that after adjusting for other factors history of cardiovascular disease, baseline mean arterial pressure, baseline daily urinary protein excretion, and body lead burden were significant risk factors for progression of renal insufficiency associated with diabetic nephropathy in type II diabetic patients (Table 1). Body lead burdens and blood lead levels are the most powerful predictors of progressive decline in renal function. Longitudinal multivariate analysis with a generalized estimating equation of data for all patients revealed that body lead burden and high blood lead levels were the only significant predictors of a progressive reduction in the glomerular Table 2 Longitudinal analysis of body lead burden and other predictors of progressive change in the glomerular filtration rate, using generalized estimating equations, during the 12-month longitudinal study period Variable Estimate (interactive effect) a P-value Age (each increment of 1 year) Sex (female versus male) Smoking (no versus yes) Use of insulin injection (no versus yes) Previous cardiovascular diseases (no versus yes) Baseline body-mass index (each increment of 1 kg/m 2 ) Mean arterial pressure (each increment of 1 mm Hg) Baseline serum creatinine (each increment of 1 mg/dl (88 mmol/l)) Body lead burden (each increment of 1 mg) o HbA1c (%) (each increment of 1%) Cholesterol (mg/dl) (each increment of 1 mg/dl) Baseline daily protein intake (each increment of 1 g/kg) Baseline daily protein excretion (each increment of 1 g) HbA1c: glycosylated hemoglobin. a The interactive effect of variables was calculated by a generalized estimating equation. Negative values for the interactive effect indicate a decline in the glomerular filtration rate, and positive values indicate an increase. filtration rate. Each increase of 100 mg (0.48 mmol) in body lead burden caused a reduction in the glomerular filtration rate of 7.2 ml/min/1.73 m 2 of body surface area (Po0.0001) (Table 2). Moreover, after adjustment for other relating factors, each increase of 1 mg/dl (0.043 mmol/l) in blood lead levels resulted in a reduction in the glomerular filtration rate of 0.56 ml/min/1.73 m 2 of body surface area during the observation period (P ¼ ). Intervention period Chelation therapy. In total, 30 patients with a highnormal body lead burdens were enrolled in the intervention trial. Patients were randomly assigned to two groups, each with 15. The chelation group underwent chelation therapy for 3 months and the control group received a placebo. Both groups had similar baseline characteristics with the exception of borderline significant differences for renal function indices (Table 3). Following 3 months of lead-chelation therapy, body lead burden in the chelation group reduced to mg ( mmol; range, mg ( mmol)), and blood lead levels decreased to mg/dl ( mmol/l; range, mg/dl ( mmol/l)). The therapeutic dosage of calcium disodium EDTA averaged g (range, 4 14 g). After chelation therapy, the change in the glomerular filtration rate in the chelation group was ml/min/1.73 m 2 of body surface area, compared with ml/min/1.73 m 2 of body surface area in the control group (P ¼ by the Mann Whitney U-test). Kidney International (2006) 69,
4 Table 3 Baseline characteristics of patients with high normal body lead burden in the control and study groups at the beginning of the clinical trial a Variable The control group The study group P-value (N=15) (N=15) Age (year) Mean7s.d Range Sex (no. of patients) Male/female 13/2 11/ b Body-mass index (kg/m 2 ) Mean7s.d Range HBA1c (%) Mean7s.d Range Use of insulin at entry (no. of patients) (%) 4 (26.7) 6 (40.0) w Serum creatinine (mg/dl) b Mean7s.d Range Creatinine clearance rate (ml/min/1.73 m 2 ) Mean7s.d Range Glomerular filtration rate c (ml/min/1.73 m 2 ) Mean7s.d Range Blood lead (mg/dl) d Mean7s.d Range Body lead burden (mg) d Mean7s.d Range Daily protein excretion (g) Mean7s.d Range Daily protein intake (g/kg) Mean7s.d Range Hyperlipidemia (no. of patients) (%) e 11 (73.3) 10 (66.7) w Use of statin drugs (no. of patients) (%) 10 (66.7) 9 (60.0) w Hypertension (no. of patients) (%) f 15 (100) 14 (93.3) w Use of angiotensin-converting enzyme inhibitors or angiotensin-receptor 15 (100) 14 (93.3) w antagonists (no. of patients) (%) Use of nondihydropyridine calcium channel blockers (no. of patients) (%) 3 (20) 5 (33.3) w Use of dihydropyridine calcium channel blockers (no. of patients) (%) 6 (40) 7 (46.7) w Smoking (no. of patients) (%) 3 (20) 6 (40) w Previous myocardial infarction (no. of patients) (%) 3 (20) 1 (6.7) w Previous stroke (no. of patients) (%) 3 (20%) 3 (20) w HbA1c: glycosylated hemoglobin; MDRD: Modification of Diet in Renal Disease. a A high-normal body lead burden was defined as a lead value of at least 80 mg (0.39 mmol) but o600 mg (2.9mmol). b To convert values for serum creatinine to micromoles per liter, multiply by c Glomerular filtration rate was calculated by the MDRD formula. d To convert values for lead to micromoles per liter, multiply by e Hyperlipidemia was defined as a serum cholesterol level above 240 mg per deciliter (6.2 mmol per liter) after diet control. f Hypertension was defined by the presence of at least two blood pressure measurements above 140/90 mm Hg in a patient who was receiving antihypertensive drugs. w P-values were calculated by Fisher s w 2 test, except in the comparisons of age, body-mass index, serum creatinine, creatinine clearance, glomerular filtration rate, blood lead level, and body lead burden, which were calculated by Student s t-test Kidney International (2006) 69,
5 Follow-up period No significant differences were noted between the two groups throughout the study period for body-mass index, mean arterial pressure, glycosylated hemoglobin, serum cholesterol level, daily urinary protein excretion, or daily protein intake. Progression of renal insufficiency ( ml/min/year) following initial chelation therapy in the chelation group was slower than that ( ml/min/year, P ¼ ) of the control group for at minimum 12 months (Table 4). Conversely, the rate of decline in the glomerular filtration rate for both groups (control group: ml/min/year versus chelation group: ml/min/year, P ¼ ) was similar during the observation period (Figure 2). Neither chelation nor control group patients were lost during the final 12 months of the follow-up period. DISCUSSION Analytical results demonstrated that basal body lead burdens and blood lead levels, even when at low levels, were major risk factors in diabetic nephropathy progression in type II Table 4 The means of renal function during the 27-month of study period Renal function (ml/min/1.73 m 2 ) The control group (N=15) The study group (N=15) P (95% CI) Basal observation period (months 0 12) Month 0 Ccr ( ) GFR ( ) Month 3 Ccr ( ) GFR ( ) Month 6 Ccr ( ) GFR ( ) Month 9 Ccr ( ) GFR ( ) Month 12 Ccr ( ) GFR ( ) Rate of decrease of renal function (ml/min/year) during the observation period Ccr ( ) # GFR ( ) # Initial lead chelation period (months 12 15) Increased renal function (ml/min) after initial 3-month lead-chelation therapy Ccr ( ) # GFR ( ) # Post-lead chelation period (months 15 27) Month 15 Ccr ( ) GFR ( ) Month 18 Ccr ( ) GFR ( ) Month 21 Ccr ( ) GFR ( ) Month 24 Ccr ( ) GFR ( ) Month 27 Ccr ( ) GFR ( ) Rate of decrease of renal function (ml/min/year) after the chelation Ccr ( ) # GFR ( ) # Decrements of renal function (ml/min) at the end of clinical trial Ccr ( ) # GFR ( ) # Ccr: creatinine clearance rate; GFR: glomerular filtration rate. Data were measured by the Student s t-test except # data by Mann Whitney method. Po0.05 means significant differences. Kidney International (2006) 69,
6 Glomerular filtration rate (ml/min/1.73 m 2 ) Chelation Control Month Figure 2 Estimated mean (72 s.e.) glomerular filtration rate according to time in the chelation group (N ¼ 15) and control group (N ¼ 15) during the study period. The patients in the chelation group received chelation therapy from month 12 to 15. # P ¼ and *P ¼ by Student s t-tests. # * diabetic patients. The correlation between environmental lead exposure and progressive diabetic nephropathy was dose dependent, even after potentially related covariates were comprehensively adjusted. These findings are similar to those obtained in previous epidemiological work, 18 which found that a longitudinal decline of renal function among middleaged individuals was dependent on both basal bone and blood lead levels; this effect was most pronounced in diabetic patients. However, this study is able to draw a more supportable conclusion than before as factors related to progressive renal function were adjusted during analyses and diabetic patients with possible primary renal diseases were strictly excluded. Mean blood lead level of this study patients was 6.5 mg/dl, a level similar to those obtained in a nationwide survey of blood lead levels in Taiwan (7.7 mg/dl) 19 and is situated between that of general population in Europe (11.4 mg/dl) 4 and America (2.8 mg/dl). 5 Mean body lead burden was mg, far less than the upper normal limit (blood lead level was o20 mg/dl (0.97 mmol/l) in Taiwan and body lead burden was o600 mg (2.90 mmol)). 10 This study suggested that a single course of chelation therapy can significantly retard progression of diabetic nephropathy for at least 1 year, even when other treatable factors are controlled. These analytical findings indicate that chronic low-level environmental lead exposure can accelerate the progression of diabetic nephropathy in patients with type II diabetes. Notably, no safe limits for lead indices were identified in this work. The influence of body lead burden on progressive renal insufficiency was more pronounced in diabetic nephropathy patients than in non-diabetic chronic renal disease patients; that is, each increase of 100 mg (0.48 mmol) in body lead burden reduced the glomerular filtration rate by 7.2 ml/ min/year/1.73 m 2 of body surface area, 24 times a previously published reduction in the glomerular filtration rate in nondiabetic patients. 15 This analytical finding is similar to that of recent study for a general population, 18 which demonstrated that an increase in the basal bone lead content from midpoints of the lowest to highest quartiles was associated with an age-related increase in the rate of increase in serum creatinine per year (a 17.6-fold greater increase in diabetics than in nondiabetics). Furthermore, each increase of 1 mg/dl (0.043 mmol/l) in the blood lead levels reduced the glomerular filtration rate by 0.56 ml/min/year/1.73 m 2 of body surface area. This work indicated that blood lead level is also a predictor of progressive diabetic nephropathy, which can be easily monitored in clinical practice. Large population studies 20,21 also identified a strong correlation between measured blood lead levels and body lead burdens, when environmental lead exposure remained constant. Since environmental lead exposure is commonly neglected and is potentially preventable, removal of lead sources and avoiding potential environmental lead exposure, particularly for patients with diabetic nephropathy, are crucial public health issues. Whether increased body lead burden is the cause or a consequence of chronic renal insufficiency is under debate. 22 However, most studies have determined that high body lead burden is a causal factor for, rather than a consequence of, reduced renal function. 20,23 26 A previous study 23 demonstrated that no differences existed in blood lead levels or bone lead contents in 188 persons with normal renal function or mild to severe renal dysfunction. Other studies also demonstrated that impaired renal function does not cause an increase in body lead burden or blood lead levels and that chronic renal failure does not effect lead accumulation. 20,24 26 The rate of diabetic nephropathy progression in the chelation group following chelation therapy was markedly slower than that in the control group and only approximately 40% of the initial progression rate during the observation period. Although renal function in the control group was superior to that in the chelation group at the beginning of the clinical trial, at study end, renal function in the control group was significantly worse than that in the chelation group. These analytical findings indicate that lead-chelation therapy slows diabetic nephropathy progression in patients with type II diabetes and high-normal body lead burdens, even when they have received all currently available treatments to retard progressive renal insufficiency. A small dose of calcium disodium EDTA at lengthy intervals has been extensively applied for chronic renal disease patients and nontoxic effects were observed. 15,20 Lead-chelation therapy reportedly improved renal function in an animal study of long-term low-level lead exposure, 27 an investigation of lead nephropathy in lead workers, 2 and a study of non-diabetic patients with chronic renal disease; 11 the mechanism accounting for the improvement in renal function by lead-chelation therapy, however, remains unclear. Environmental low-level exposure to lead can increase oxidation stress causing functional nitric oxide deficiency 28 and activation of the renin angiotensin aldosterone system in animals and humans. 29 Lead chelation reduces levels of reactive oxygen species associated with nitric oxide inactivation, enhancing the availability of nitric oxide to the vascular smooth muscle or inhibiting rennin and angiotensin II activity, thereby potentially improving renal 2054 Kidney International (2006) 69,
7 function following body lead removal. However, substantial research is required to clarify the lead-chelation mechanism. EDTA chelation removes other metals, such as zinc, copper, etc. However, patients with history of exposure to lead or other heavy metals were excluded from this study. Additionally, rare studies noted that exposure to low-level EDTA chelatable ions other than lead affect renal function. Conversely, considerable evidence in animal and human studies 4,5,10 15,27 indicated that low-level lead exposure results in kidney injury. Hence, suggesting that removing body lead slowed progressive diabetic nephropathy is reasonable. The use of creatinine clearance to assess altered renal function may limit this study s results. However, an investigation into the glomerular filtration rate by Levey et al. 30 demonstrated a strong correlation between estimated glomerular filtration rate and isotopic glomerular filtration rate (r 2 ¼ 0.91). Another limitation is this study s relatively short duration. However, rapidly progressing renal insufficiency about 10 ml/min/year due to the strictly selective criterion of diabetic nephropathy and relative low basal glomerular filtration rate made performing a long-term study impossible. In conclusion, this prospective study suggested that chronic low-level environmental lead exposure accelerates deterioration of renal insufficiency in type II diabetic patients with diabetic nephropathy. Moreover, lead-chelation therapy slows rapid progression of diabetic nephropathy in patients with high-normal body lead burdens, when other treatable factors are controlled. As diabetes is the leading cause of end-stage renal disease in many countries, these findings are important. MATERIALS AND METHODS Subjects The Medical Ethics Committee of Chang Gung Memorial Hospital (CGMH), Taipei, Taiwan, approved study protocol. Each patient provided informed written consent. Patients aged years with type II diabetes mellitus and nephropathy who received follow-up at CGMH for 41 year were enrolled if they met all of the following criteria: a serum creatinine concentration between 1.5 mg/dl (132.6 mmol/l) and 3.9 mg/dl (344.8 mmol/l); daily urinary protein excretion of 40.5 g/day; no micro-hematuria present in urinalysis tests; normal-sized kidneys by echograms; history of retinopathy with laser therapy by an ophthalmologist; and, diabetes for 45 years and no history of exposure to lead or other heavy metals (body lead burden of o600 mg (2.90 mmol)), as measured by EDTA mobilization testing and 72-h urine collection. Diagnosis of diabetic nephropathy was also based on renal histological examination findings when a renal biopsy was performed. Exclusion criteria were as follows: type I diabetes; renal insufficiency with a potentially reversible cause such as malignant hypertension, urinary tract infection, hypercalcemia, or drug-induced nephrotoxic effects; presence of other systemic diseases such as connective-tissue diseases; use of drugs that may affect the course of renal disease, such as nonsteroidal anti-inflammatory agents, steroids, immunosuppressive drugs or aristolochic acid-containing herbal drugs; previous substantial exposure to lead (lead poisoning or occupational exposure); drug allergies; and, absence of informed consent. Blood pressure of each patient was maintained at o140/90 mm Hg with diuretics and angiotensin-converting enzyme inhibitors or angiotensin II receptor antagonists, with or without calcium-blocking agents and/or vasodilators. Patients with systolic blood pressure o100 mm Hg were not administered angiotensin-converting enzyme inhibitors or angiotensin II receptor antagonists. Calcium carbonate was prescribed to maintain phosphate levels. No patients received vitamin D3 supplements or erythropoietin treatment. Each patient underwent a dietary consultation. A diabetic diet (35 kcal/kg of body weight/day) with normal-protein intake ( g of high biological value protein/kg of body weight/day) was recommended for each patient. A nutritionist reviewed the dietary intake of each patient every 3 6 months. A 24-h urea excretion was assessed every 3 months for nitrogen balance and dietary compliance. 31 Subjects who did not return for regular clinical assessments were contacted by telephone or home visits during the study period. Measurements of blood lead levels and body lead burden Blood lead levels and body lead burden were measured as described previously. 15,16,32 Body lead burden was measured utilizing EDTA mobilization tests modified by Behringer et al. 30 Urinary excretions (72 h) after the intravenous infusion of 1 g of calcium disodium EDTA (edetate calcium disodium (Calcium Disodium Versenate), Abbott Laboratories, North Chicago, IL, USA) were used to measure body lead burden. Blood lead and urine lead levels were determined by electro-thermal atomic-absorption spectrometry (model 5100 PC, Perkin-Elmer, Boston, MA, USA) with Zeeman background correction and an L vov platform. Both internal and external quality-control procedures applied throughout this study, achieved consistently satisfactory results. A certified commercially prepared product (Seronorm Trace Elements, Sero AS, Billingstads, Norway) was utilized to monitor intra-batch accuracy and ensure inter-batch standardization. The coefficient of variation for lead measurement was p5.3%. External quality control was maintained via participation in two major programs: the governmental National Quality-Control Program, and an international program administrated by the College of American Pathologists. 15 Study protocol Baseline data collection period (months 6 to 0). Baseline blood lead levels, hemoglobin levels, and body lead burdens were assessed for 6 months prior to the study for the 90 patients enrolled. Serum creatinine, blood urea nitrogen, potassium, glycosylated hemoglobin, fasting blood sugar and cholesterol, urinary protein, creatinine, and urea excretion were measured at 3-month intervals during the pre-study 6-month period and throughout 27-month study period using an auto-analyzer system (Hitachi, Tokyo, Japan) to ensure that entry criteria were met. All study patients received standard treatment of diabetes, including dietary, blood pressure, sugar, hyperlipdemia, and body weight control. Longitudinal observation period (months 1 12). All biochemical data were measured at 3-month intervals starting at months Each urinary excretion value was the average from two consecutive 24-h urine collection samples. Renal function was assessed utilizing creatinine clearance and estimated glomerular filtration rate 21 (both in ml/min/1.73 m 2 of body surface area). The formula of estimated glomerular filtration rate 33 is 198 (serum creatinine) (age) (0.882 if patient is a women) (1.178 if patient is a black) (blood urea nitrogen) (urine urea nitrogen) In total, 87 patients completed initial study period. Intervention period (months 12 15). The 12-month observational investigation was followed by a 3-month single-blind randomized placebo-controlled study. Based on previous works, 12,15,32 Kidney International (2006) 69,
8 a high-normal body lead burden was defined as at minimum 80 mg (0.39 mmol) and o600 mg (2.90 mmol) of lead. Thirty patients with high-normal body lead burdens and serum creatinine levels o4.0 mg/dl (353.6 mmol/l) were randomly assigned to a control or chelation group. During the first 3 months, chelation group patients received 2-h weekly intravenous infusions of one vial (1 g) of calcium disodium EDTA mixed with 200 ml of normal saline until body lead burden was o60 mg (0.29 mmol). Control patients received weekly 2-h infusions of one vial (20 ml) of 50% glucose mixed with 200 ml of normal saline over a period of 5 weeks. 15 Follow-up period (months 15 27). Laboratory measurements were conducted at 3-month intervals for an additional 12 months after initial placebo or chelation therapy to document possible changes in renal function. Outcome measures The primary end point was an elevation in serum creatinine measured twice, each 1 month apart to 1.5 times that at baseline or need for hemodialysis during the 12-month observation period. A secondary end point was temporal changes in renal function following chelation therapy. Statistical analysis The sample size was calculated with PASS software (power analysis and sample-size package, NCSS statistical software). For a two-tailed test with a 0.05 significance level, a sample size of 30 patients (15 per group) was deemed adequate to permit detection of differences between treatment groups for rate of change to the glomerular filtration rate of 0.31 ml/min per 3-month interval, 11 with a power of Randomization was utilized with the random-digit method and was based on computer-generated numbers. The Cox proportional-hazards model was applied to determine the significance of variables for predicting the primary end point during the observation period. This model consisted of all variables identified in literature as related to renal insufficiency progression. 7,8,17 Generalized estimating equations were employed in longitudinal multivariate analyses using SAS statistical software (Version 6.12) to further assess a variable s association with renal insufficiency progression during the observation period. Differences in rates of progression for renal failure between the two groups were analyzed via a w 2 test combined with Fisher s test, and Student s t-test. The Mann Whitney U-test was employed for data not normally distributed. A simple linear regression analysis was used to identify the relationship between blood lead level and body lead burden. All P-values were two tailed, and all results are presented as means7s.d. A value of Po0.05 was statistically significant. ACKNOWLEDGMENTS We thank the National Science Council of the Republic of China, Taiwan for financially supporting this research under Contract No. NSC_ B-182A-079. REFERENCES 1. Wedeen RP, Maesaka JK, Weiner B et al. Occupational lead nephropathy. Am J Med 1975; 59: Wedeen RP, Mallick DK, Batuman V. Detection and treatment of occupational lead nephropathy. Arch Intern Med 1979; 139: Nuyts GD, Daelemans RA, Jorens PG et al. Does lead play a role in the development of chronic renal disease? Nephrol Dial Transplant 1991; 6: Staessen JA, Lauwerys RR, Buchet J-P et al. Impairment of renal function with increasing blood lead concentrations in the general population. N Engl J Med 1992; 327: Kim R, Rotnitsky A, Sparrow D et al. A longitudinal study of lowlevel lead exposure and impairment of renal function: the Normative Aging Study. JAMA 1996; 275: Brenner BM, Meyer TW, Hostetter TH. Dietary protein intake and the progressive nature of kidney disease: the role of hemodynamically mediated glomerular injury in the pathogenesis of progressive glomerular sclerosis in aging, renal ablation, and intrinsic renal disease. N Engl J Med 1982; 307: Obrador GT, Arora P, Kausz AT, Pereira BJ. Pre-end-stage renal disease care in the United States: a state of disrepair. J Am Soc Nephrol 1998; 9(Suppl): S44 S Hunsicker LG, Adler S, Caggiula A et al. Predictors of the progression of renal disease in the Modification of Diet in Renal Disease Study. Kidney Int 1997; 51: Pollock CA, Ibels LS. Lead nephropathy a preventable cause of renal failure. Int J Artif Organs 1988; 11: Lin JL, Yeh KH, Tseng HC et al. Urinary N-acetyl-glucosaminidase excretion and environmental lead exposure. Am J Nephrol 1993; 13: Lin JL, Ho HH, Yu CC. Chelation therapy for patients with elevated body lead burden and progressive renal insufficiency: a randomized, controlled trial. Ann Intern Med 1999; 130: Lin JL, Tan DT, Hsu KH, Yu CC. Environmental lead exposure and progressive renal insufficiency. Arch Intern Med 2001; 161: Yu CC, Lin JL, Lin-Tan DT. Evironmental exposure to lead and progression of chronic renal disease: a four-year prospective longitudinal study. J Am Soc Nephrol 2004; 15: Lin JL, Tan DT, Ho HH, Yu CC. Environmental lead exposure and urate excretion in the general population. Am J Med 2002; 113: Lin JL, Lin-Tan DT, Hsu KH, Yu CC. Environmental lead exposure and progression of chronic renal diseases in patients without diabetes. N Engl J Med 2003; 348: Ford ES. Vitamin supplement use and diabetes mellitus incidence among adults in the United States. Am J Epidemiol 2001; 153: Jones CA, Krolewski AS, Rogus J et al. Epidemic of end-stage renal disease in people with diabetes in the United States population: do we know the cause? Kidney Int 2005; 67: Tsaih SW, Korrick S, Schwartz J et al. Lead, diabetes, hypertension, and renal function: the normative aging study. Environ Health Perspect 2004; 112: Liou SH, Wu TN, Chiang HC et al. Three-year survey of blood lead levels in 8828 Taiwanese adults. Int Arch Occup Environ Health 1996; 68: Batuman V. Lead nephropathy, gout, and hypertension. Am J Med Sci 1993; 305: Loghman-Adham M. Renal effects of environmental and occupational lead exposure. Environ Health Perspect 1997; 105: Marsden PA. Increased body lead burden cause or consequence of chronic renal insufficiency? N Engl J Med 2003; 348: Van de Vyver FL, D Haese PC, Visser WJ et al. Bone lead in dialysis patients. Kidney Int 1988; 33: Batuman V, Maesaka JK, Haddad B et al. The role of lead in gout nephropathy. N Engl J Med 1981; 304: Batuman V, Landy E, Maesaka JK, Wedeen RP. Contribution of lead to hypertension with renal impairment. N Engl J Med 1983; 309: Emmerson BT. Lead stores in patients with renal insufficiency. Nephron 1991; 58: Khalil-Manesh F, Gonick HC, Cohen A et al. A Experimental model of lead nephropathy. II. Effect of removal from lead exposure and chelation treatment with dimercaptosuccinic acid (DMSA). Environ Res 1992; 58: Ding Y, Vaziri ND, Gonick HC. Lead-induced hypertension. II. Response to sequential infusions of L-arginine, superoxide dismutase, and nitroprusside. Environ Res 1998; 76: Boscolo P, Carmignani M. Neurohumoral blood pressure regulation in lead exposure. Environ Health Perspect 1988; 78: Behringer D, Craswell P, Mohl C et al. Urinary lead excretion in uremic patients. Nephron 1986; 42: Isaksson B. Urinary nitrogen output as a validity test in dietary surveys. Am J Clin Nutr 1980; 33: Lin JL, Yu CC, Lin-Tan DT, Ho HH. Lead chelation therapy and urate excretion in patients with chronic renal diseases and gout. Kidney Int 2001; 60: Levey AS, Bosch JP, Lewis JB et al. A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Ann Intern Med 1999; 130: Kidney International (2006) 69,
Ja-Liang Lin, M.D., Dan-Tzu Lin-Tan, R.N., Kuang-Hung Hsu, Ph.D., and Chun-Chen Yu, M.D. abstract
 The new england journal of medicine established in 1812 january 23, 2003 vol. 348 no. 4 Environmental Lead Exposure and Progression of Chronic Renal Diseases in Patients without Diabetes Ja-Liang Lin,
The new england journal of medicine established in 1812 january 23, 2003 vol. 348 no. 4 Environmental Lead Exposure and Progression of Chronic Renal Diseases in Patients without Diabetes Ja-Liang Lin,
Low-level Environmental Exposure to Lead and Progressive Chronic Kidney Diseases
 The American Journal of Medicine (2006) 119, 707.e1-707.e9 CLINICAL RESEARCH STUDY Low-level Environmental Exposure to Lead and Progressive Chronic Kidney Diseases Ja-Liang Lin, MD, Dan-Tzu Lin-Tan, RN,
The American Journal of Medicine (2006) 119, 707.e1-707.e9 CLINICAL RESEARCH STUDY Low-level Environmental Exposure to Lead and Progressive Chronic Kidney Diseases Ja-Liang Lin, MD, Dan-Tzu Lin-Tan, RN,
Long-term outcome of repeated lead chelation therapy in progressive non-diabetic chronic kidney diseases
 Nephrol Dial Transplant (2007) 22: 2924 2931 doi:10.1093/ndt/gfm342 Advance Access publication 7 June 2007 Original Article Long-term outcome of repeated lead chelation therapy in progressive non-diabetic
Nephrol Dial Transplant (2007) 22: 2924 2931 doi:10.1093/ndt/gfm342 Advance Access publication 7 June 2007 Original Article Long-term outcome of repeated lead chelation therapy in progressive non-diabetic
ORIGINAL INVESTIGATION. Environmental Lead Exposure and Progressive Renal Insufficiency
 ORIGINAL INVESTIGATION Environmental Lead Exposure and Progressive Renal Insufficiency Ja-Liang Lin, MD; Dan-Tzu Tan, RN; Kuan-Huang Hsu, PhD; Chun-Chen Yu, MD Background: Several recent studies show that
ORIGINAL INVESTIGATION Environmental Lead Exposure and Progressive Renal Insufficiency Ja-Liang Lin, MD; Dan-Tzu Tan, RN; Kuan-Huang Hsu, PhD; Chun-Chen Yu, MD Background: Several recent studies show that
The CARI Guidelines Caring for Australasians with Renal Impairment. Protein Restriction to prevent the progression of diabetic nephropathy GUIDELINES
 Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Prevention And Treatment of Diabetic Nephropathy. MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan
 Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
ALLHAT RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR)
 1 RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR) 6 / 5 / 1006-1 2 Introduction Hypertension is the second most common cause of end-stage
1 RENAL DISEASE OUTCOMES IN HYPERTENSIVE PATIENTS STRATIFIED INTO 4 GROUPS BY BASELINE GLOMERULAR FILTRATION RATE (GFR) 6 / 5 / 1006-1 2 Introduction Hypertension is the second most common cause of end-stage
(renoprotective (end-stage renal disease, ESRD) therapies) (JAMA)
 [1], 1., 2. 3. (renoprotective (end-stage renal disease, ESRD) therapies) (JAMA) (multiple risk (renal replacement therapy, RRT) factors intervention treatment MRFIT) [2] ( 1) % (ESRD) ( ) ( 1) 2001 (120
[1], 1., 2. 3. (renoprotective (end-stage renal disease, ESRD) therapies) (JAMA) (multiple risk (renal replacement therapy, RRT) factors intervention treatment MRFIT) [2] ( 1) % (ESRD) ( ) ( 1) 2001 (120
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Reducing proteinuria
 Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
The CARI Guidelines Caring for Australians with Renal Impairment. Specific effects of calcium channel blockers in diabetic nephropathy GUIDELINES
 Specific effects of calcium channel blockers in diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. Non-dihydropyridine calcium channel
Specific effects of calcium channel blockers in diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. Non-dihydropyridine calcium channel
Objectives. Pre-dialysis CKD: The Problem. Pre-dialysis CKD: The Problem. Objectives
 The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
Lead chelation therapy and urate excretion in patients with chronic renal diseases and gout
 Kidney International, Vol. 60 (2001), pp. 266 271 Lead chelation therapy and urate excretion in patients with chronic renal diseases and gout JA-LIANG LIN, CHUN-CHEN YU, DAN-TZU LIN-TAN, and HUEI-HONG
Kidney International, Vol. 60 (2001), pp. 266 271 Lead chelation therapy and urate excretion in patients with chronic renal diseases and gout JA-LIANG LIN, CHUN-CHEN YU, DAN-TZU LIN-TAN, and HUEI-HONG
Renal Protection Staying on Target
 Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
The Seventh Report of the Joint National Commission
 The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
Management of early chronic kidney disease
 Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new (MDRD) prediction equation
 Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Association of Blood Lead Levels With Mortality in Patients on Maintenance Hemodialysis
 CLINICAL RESEARCH STUDY Association of Blood Lead Levels With Mortality in Patients on Maintenance Hemodialysis Ja-Liang Lin, MD, a Dan-Tzu Lin-Tan, RN, a Ching-Wei Hsu, MD, a Tzung-Hai Yen, MD, a Kuan-Hsing
CLINICAL RESEARCH STUDY Association of Blood Lead Levels With Mortality in Patients on Maintenance Hemodialysis Ja-Liang Lin, MD, a Dan-Tzu Lin-Tan, RN, a Ching-Wei Hsu, MD, a Tzung-Hai Yen, MD, a Kuan-Hsing
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
The CARI Guidelines Caring for Australasians with Renal Impairment. ACE Inhibitor and Angiotensin II Antagonist Combination Treatment GUIDELINES
 ACE Inhibitor and Angiotensin II Antagonist Combination Treatment Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES No recommendations possible based on Level
ACE Inhibitor and Angiotensin II Antagonist Combination Treatment Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES No recommendations possible based on Level
Contrast Induced Nephropathy
 Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
University of Groningen. Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste
 University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
DIABETES AND CHRONIC KIDNEY DISEASE
 DIABETES AND CHRONIC KIDNEY DISEASE Stages 1 4 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
DIABETES AND CHRONIC KIDNEY DISEASE Stages 1 4 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
Solving Slowing Progressive Renal Disease
 Focus on CME at Memorial University of Newfoundland Solving Slowing Progressive Risk factors and treatment strategies for patients with kidney and cardiovascular disease overlap. Thus, evaluating renal
Focus on CME at Memorial University of Newfoundland Solving Slowing Progressive Risk factors and treatment strategies for patients with kidney and cardiovascular disease overlap. Thus, evaluating renal
The CARI Guidelines Caring for Australasians with Renal Impairment. Specific management of IgA nephropathy: role of steroid therapy GUIDELINES
 Specific management of IgA nephropathy: role of steroid therapy Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES Steroid therapy may protect against progressive
Specific management of IgA nephropathy: role of steroid therapy Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES Steroid therapy may protect against progressive
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
The CARI Guidelines Caring for Australasians with Renal Impairment. Blood Pressure Control role of specific antihypertensives
 Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Prof. Armando Torres Nephrology Section Hospital Universitario de Canarias University of La Laguna Tenerife, Canary Islands, Spain.
 Does RAS blockade improve outcomes after kidney transplantation? Armando Torres, La Laguna, Spain Chairs: Hans De Fijter, Leiden, The Netherlands Armando Torres, La Laguna, Spain Prof. Armando Torres Nephrology
Does RAS blockade improve outcomes after kidney transplantation? Armando Torres, La Laguna, Spain Chairs: Hans De Fijter, Leiden, The Netherlands Armando Torres, La Laguna, Spain Prof. Armando Torres Nephrology
Analysis of Factors Causing Hyperkalemia
 ORIGINAL ARTICLE Analysis of Factors Causing Hyperkalemia Kenmei Takaichi 1, Fumi Takemoto 1, Yoshifumi Ubara 1 and Yasumichi Mori 2 Abstract Objective Patients with impaired renal function or diabetes
ORIGINAL ARTICLE Analysis of Factors Causing Hyperkalemia Kenmei Takaichi 1, Fumi Takemoto 1, Yoshifumi Ubara 1 and Yasumichi Mori 2 Abstract Objective Patients with impaired renal function or diabetes
Kidney Disease. Chronic kidney disease (CKD) requiring dialysis. The F.P. s Role in the Management of Chronic. Stages
 Focus on CME at McMaster University The F.P. s Role in the Management of Chronic Kidney Disease By David N. Churchill, MD, FRCPC, FACP Presented at McMaster University CME Half-Day in Nephrology for Family
Focus on CME at McMaster University The F.P. s Role in the Management of Chronic Kidney Disease By David N. Churchill, MD, FRCPC, FACP Presented at McMaster University CME Half-Day in Nephrology for Family
The CARI Guidelines Caring for Australasians with Renal Impairment. Specific management of IgA nephropathy: role of fish oil
 Specific management of IgA nephropathy: role of fish oil Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES Early and prolonged treatment with fish oil may retard
Specific management of IgA nephropathy: role of fish oil Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES Early and prolonged treatment with fish oil may retard
Dr. Mehmet Kanbay Department of Medicine Division of Nephrology Istanbul Medeniyet University School of Medicine Istanbul, Turkey.
 The uric acid dilemma: causal risk factor for hypertension and CKD or mere bystander? Mehmet Kanbay, Istanbul, Turkey Chairs: Anton H. van den Meiracker, Rotterdam, The Netherlands Claudia R.C. Van Roeyen,
The uric acid dilemma: causal risk factor for hypertension and CKD or mere bystander? Mehmet Kanbay, Istanbul, Turkey Chairs: Anton H. van den Meiracker, Rotterdam, The Netherlands Claudia R.C. Van Roeyen,
An acute fall in estimated glomerular filtration rate during treatment with losartan predicts a slower decrease in long-term renal function
 original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
BASELINE CHARACTERISTICS OF THE STUDY POPULATION
 Study Summary DAILY ORAL SODIUM BICARBONATE PRESERVES GLOMERULAR FILTRATION RATE BY SLOWING ITS DECLINE IN EARLY HYPERTENSIVE NEPHROPATHY This was a 5-year, single-center, prospective, randomized, placebo-controlled,
Study Summary DAILY ORAL SODIUM BICARBONATE PRESERVES GLOMERULAR FILTRATION RATE BY SLOWING ITS DECLINE IN EARLY HYPERTENSIVE NEPHROPATHY This was a 5-year, single-center, prospective, randomized, placebo-controlled,
Elevation of Serum Creatinine: When to Screen, When to Refer. Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC
 Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
2 Furthermore, quantitative coronary angiography
 ORIGINAL PAPER Estimated Glomerular Filtration Rate Reversal by Blood Pressure Lowering in Chronic Kidney Disease: Japan Multicenter Investigation for Cardiovascular DiseaseB CKD Study Yoshiki Yui, MD;
ORIGINAL PAPER Estimated Glomerular Filtration Rate Reversal by Blood Pressure Lowering in Chronic Kidney Disease: Japan Multicenter Investigation for Cardiovascular DiseaseB CKD Study Yoshiki Yui, MD;
Special Challenges and Co-Morbidities
 Special Challenges and Co-Morbidities Renal Disease/ Hypertension/ Diabetes in African-Americans M. Keith Rawlings, MD Medical Director Peabody Health Center AIDS Arms, Inc Dallas, TX Chair, Internal Medicine
Special Challenges and Co-Morbidities Renal Disease/ Hypertension/ Diabetes in African-Americans M. Keith Rawlings, MD Medical Director Peabody Health Center AIDS Arms, Inc Dallas, TX Chair, Internal Medicine
Uric acid and CKD. Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George
 Uric acid and CKD Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George Hospital @Badves Case Mr J, 52 Male, referred in June 2015 DM type 2 (4 years), HTN, diabetic retinopathy, diabetic
Uric acid and CKD Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George Hospital @Badves Case Mr J, 52 Male, referred in June 2015 DM type 2 (4 years), HTN, diabetic retinopathy, diabetic
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Diabetes in Renal Patients. Contents. Understanding Diabetic Nephropathy
 Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Chronic kidney disease (CKD) has received
 Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
THE PROGNOSIS OF PATIENTS WITH CHRONIC KIDNEY DISEASE AND DIABETES MELLITUS
 214 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 21(3):23-212 doi: 1.2478/rjdnmd-214-25 THE PROGNOSIS OF PATIENTS WITH CHRONIC KIDNEY DISEASE AND DIABETES
214 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 21(3):23-212 doi: 1.2478/rjdnmd-214-25 THE PROGNOSIS OF PATIENTS WITH CHRONIC KIDNEY DISEASE AND DIABETES
Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects
 ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
Individual Study Table Referring to Part of Dossier: Volume: Page:
 Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Preoperative Serum Bicarbonate Levels Predict Acute Kidney Iinjry after Cardiac Surgery
 International Journal of ChemTech Research CODEN (USA): IJCRGG, ISSN: 0974-4290, ISSN(Online):2455-9555 Vol.11 No.06, pp 203-208, 2018 Preoperative Serum Bicarbonate Levels Predict Acute Kidney Iinjry
International Journal of ChemTech Research CODEN (USA): IJCRGG, ISSN: 0974-4290, ISSN(Online):2455-9555 Vol.11 No.06, pp 203-208, 2018 Preoperative Serum Bicarbonate Levels Predict Acute Kidney Iinjry
Chronic Kidney Disease
 Chronic Kidney Disease Chronic Kidney Disease (CKD) Educational Objectives Outline Demographics Propose Strategies to slow progression and improve outcomes Plan for treatment of CKD Chronic Kidney Disease
Chronic Kidney Disease Chronic Kidney Disease (CKD) Educational Objectives Outline Demographics Propose Strategies to slow progression and improve outcomes Plan for treatment of CKD Chronic Kidney Disease
S150 KEEP Analytical Methods. American Journal of Kidney Diseases, Vol 55, No 3, Suppl 2, 2010:pp S150-S153
 S150 KEEP 2009 Analytical Methods American Journal of Kidney Diseases, Vol 55, No 3, Suppl 2, 2010:pp S150-S153 S151 The Kidney Early Evaluation program (KEEP) is a free, communitybased health screening
S150 KEEP 2009 Analytical Methods American Journal of Kidney Diseases, Vol 55, No 3, Suppl 2, 2010:pp S150-S153 S151 The Kidney Early Evaluation program (KEEP) is a free, communitybased health screening
CRAIOVA UNIVERSITY OF MEDICINE AND PHARMACY FACULTY OF MEDICINE ABSTRACT DOCTORAL THESIS
 CRAIOVA UNIVERSITY OF MEDICINE AND PHARMACY FACULTY OF MEDICINE ABSTRACT DOCTORAL THESIS RISK FACTORS IN THE EMERGENCE OF POSTOPERATIVE RENAL FAILURE, IMPACT OF TREATMENT WITH ACE INHIBITORS Scientific
CRAIOVA UNIVERSITY OF MEDICINE AND PHARMACY FACULTY OF MEDICINE ABSTRACT DOCTORAL THESIS RISK FACTORS IN THE EMERGENCE OF POSTOPERATIVE RENAL FAILURE, IMPACT OF TREATMENT WITH ACE INHIBITORS Scientific
ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour
 ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour Dr Indranil Dasgupta Rationale No national practical
ABCD and Renal Association Clinical Guidelines for Diabetic Nephropathy-CKD. Management of Dyslipidaemia and Hypertension in Adults Dr Peter Winocour Dr Indranil Dasgupta Rationale No national practical
The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival
 ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.1.55 The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival Seoung Gu Kim 1 and Nam Ho Kim 2 Department of Internal Medicine,
ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.1.55 The Effect of Residual Renal Function at the Initiation of Dialysis on Patient Survival Seoung Gu Kim 1 and Nam Ho Kim 2 Department of Internal Medicine,
Long-term outcomes in nondiabetic chronic kidney disease
 original article http://www.kidney-international.org & 28 International Society of Nephrology Long-term outcomes in nondiabetic chronic kidney disease V Menon 1, X Wang 2, MJ Sarnak 1, LH Hunsicker 3,
original article http://www.kidney-international.org & 28 International Society of Nephrology Long-term outcomes in nondiabetic chronic kidney disease V Menon 1, X Wang 2, MJ Sarnak 1, LH Hunsicker 3,
Masatoshi Kawashima 1, Koji Wada 2, Hiroshi Ohta 2, Rika Moriya 3 and Yoshiharu Aizawa 1. Journal of Occupational Health
 176 J Occup Health, Vol. 54, 2012 J Occup Health 2012; 54: 176 180 Journal of Occupational Health Evaluation of Validity of the Urine Dipstick Test for Identification of Reduced Glomerular Filtration Rate
176 J Occup Health, Vol. 54, 2012 J Occup Health 2012; 54: 176 180 Journal of Occupational Health Evaluation of Validity of the Urine Dipstick Test for Identification of Reduced Glomerular Filtration Rate
RENAAL, IRMA-2 and IDNT. Three featured trials linking a disease spectrum IDNT RENAAL. Death IRMA 2
 Treatment of Diabetic Nephropathy and Proteinuria Background End stage renal disease is a major cause of death and disability among diabetics BP reduction is important to slow the progression of diabetic
Treatment of Diabetic Nephropathy and Proteinuria Background End stage renal disease is a major cause of death and disability among diabetics BP reduction is important to slow the progression of diabetic
Morbidity & Mortality from Chronic Kidney Disease
 Morbidity & Mortality from Chronic Kidney Disease Dr. Lam Man-Fai ( 林萬斐醫生 ) Honorary Clinical Assistant Professor MBBS, MRCP, FHKCP, FHKAM, PDipID (HK), FRCP (Edin, Glasg) Hong Kong Renal Registry Report
Morbidity & Mortality from Chronic Kidney Disease Dr. Lam Man-Fai ( 林萬斐醫生 ) Honorary Clinical Assistant Professor MBBS, MRCP, FHKCP, FHKAM, PDipID (HK), FRCP (Edin, Glasg) Hong Kong Renal Registry Report
Supplementary Online Content
 Supplementary Online Content Afkarian M, Zelnick L, Hall YN, et al. Clinical manifestations of kidney disease among US adults with diabetes, 1988-2014. JAMA. doi:10.1001/jama.2016.10924 emethods efigure
Supplementary Online Content Afkarian M, Zelnick L, Hall YN, et al. Clinical manifestations of kidney disease among US adults with diabetes, 1988-2014. JAMA. doi:10.1001/jama.2016.10924 emethods efigure
The CARI Guidelines Caring for Australasians with Renal Impairment
 Specific management of IgA nephropathy: role of triple therapy and cytotoxic therapy Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES a. Triple therapy with cyclophosphamide,
Specific management of IgA nephropathy: role of triple therapy and cytotoxic therapy Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES a. Triple therapy with cyclophosphamide,
Efficacy and Safety of Benazepril for Advanced Chronic Renal Insufficiency
 The new england journal of medicine original article Efficacy and Safety of Benazepril for Advanced Chronic Renal Insufficiency Fan Fan Hou, M.D., Ph.D., Xun Zhang, M.D., Guo Hua Zhang, M.D., Ph.D., Di
The new england journal of medicine original article Efficacy and Safety of Benazepril for Advanced Chronic Renal Insufficiency Fan Fan Hou, M.D., Ph.D., Xun Zhang, M.D., Guo Hua Zhang, M.D., Ph.D., Di
CLINICIAN INTERVIEW A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY. Interview with Ralph Rabkin, MD
 A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY Interview with Ralph Rabkin, MD Dr Rabkin is Professor of Medicine, Emeritus, Active, at Stanford University School of Medicine, Stanford,
A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY Interview with Ralph Rabkin, MD Dr Rabkin is Professor of Medicine, Emeritus, Active, at Stanford University School of Medicine, Stanford,
AGING KIDNEY IN HIV DISEASE
 AGING KIDNEY IN HIV DISEASE Michael G. Shlipak, MD, MPH Professor of Medicine, Epidemiology and Biostatistics, UCSF Chief, General Internal Medicine, San Francisco VA Medical Center Kidney, Aging and HIV
AGING KIDNEY IN HIV DISEASE Michael G. Shlipak, MD, MPH Professor of Medicine, Epidemiology and Biostatistics, UCSF Chief, General Internal Medicine, San Francisco VA Medical Center Kidney, Aging and HIV
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005
 VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
Hypertension and diabetic nephropathy
 Hypertension and diabetic nephropathy Elisabeth R. Mathiesen Professor, Chief Physician, Dr sci Dep. Of Endocrinology Rigshospitalet, University of Copenhagen Denmark Hypertension Brain Eye Heart Kidney
Hypertension and diabetic nephropathy Elisabeth R. Mathiesen Professor, Chief Physician, Dr sci Dep. Of Endocrinology Rigshospitalet, University of Copenhagen Denmark Hypertension Brain Eye Heart Kidney
Diabetic Nephropathy
 Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
The estimation of kidney function with different formulas in overall population
 137 G E R I A T R I A 213; 7: 137-141 Akademia Medycyny ARTYKUŁ ORYGINALNY/ORIGINAL PAPER Otrzymano/Submitted: 28.8.213 Zaakceptowano/Accepted: 2.9.213 The estimation of kidney function with different
137 G E R I A T R I A 213; 7: 137-141 Akademia Medycyny ARTYKUŁ ORYGINALNY/ORIGINAL PAPER Otrzymano/Submitted: 28.8.213 Zaakceptowano/Accepted: 2.9.213 The estimation of kidney function with different
ACEIs / ARBs NDHP dihydropyridine ( DHP ) ACEIs ARBs ACEIs ARBs NDHP. ( GFR ) 60 ml/min/1.73m ( chronic kidney disease, CKD )
 005 16 175-180 1 1 ( chronic kidney disease, CKD ) 003 ( end-stage renal disease, ESRD ) Angiotensin-converting enzyme inhibitors ( ) angiotensin receptor blockers ( ) nondihydropyridine ( NDHP ) / NDHP
005 16 175-180 1 1 ( chronic kidney disease, CKD ) 003 ( end-stage renal disease, ESRD ) Angiotensin-converting enzyme inhibitors ( ) angiotensin receptor blockers ( ) nondihydropyridine ( NDHP ) / NDHP
The CARI Guidelines Caring for Australasians with Renal Impairment. Membranous nephropathy role of steroids GUIDELINES
 Membranous nephropathy role of steroids Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES There is currently no data to support the use of short-term courses of
Membranous nephropathy role of steroids Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES There is currently no data to support the use of short-term courses of
Predicting and changing the future for people with CKD
 Predicting and changing the future for people with CKD I. David Weiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University
Predicting and changing the future for people with CKD I. David Weiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University
Microvascular Disease in Type 1 Diabetes
 Microvascular Disease in Type 1 Diabetes Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine The Course
Microvascular Disease in Type 1 Diabetes Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine The Course
The CARI Guidelines Caring for Australians with Renal Impairment. Cardiovascular Risk Factors
 Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Clinical Study Factors Associated with the Decline of Kidney Function Differ among egfr Strata in Subjects with Type 2 Diabetes Mellitus
 International Endocrinology Volume 2012, Article ID 687867, 6 pages doi:10.1155/2012/687867 Clinical Study Factors Associated with the Decline of Kidney Function Differ among egfr Strata in Subjects with
International Endocrinology Volume 2012, Article ID 687867, 6 pages doi:10.1155/2012/687867 Clinical Study Factors Associated with the Decline of Kidney Function Differ among egfr Strata in Subjects with
BASELINE CHARACTERISTICS OF THE STUDY POPULATION
 COMPARISON OF TREATING METABOLIC ACIDOSIS IN CKD STAGE 4 HYPERTENSIVE KIDNEY DISEASE WITH FRUITS & VEGETABLES OR SODIUM BICARBONATE This was a 1-year, single-center, prospective, randomized, interventional
COMPARISON OF TREATING METABOLIC ACIDOSIS IN CKD STAGE 4 HYPERTENSIVE KIDNEY DISEASE WITH FRUITS & VEGETABLES OR SODIUM BICARBONATE This was a 1-year, single-center, prospective, randomized, interventional
Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care
 Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What
Nice CKD Clinical Guidelines 2014 The challenges and benefits they may bring toprimary care Paula D Souza Senior CKD Nurse Specialist Royal Devon and Exeter Healthcare Trust Introduction Background What
Serum Creatinine and Blood Urea Nitrogen Levels in Patients with Coronary Artery Disease
 Serum Creatinine and Blood Urea Nitrogen Levels in Patients with Coronary Artery Disease MAK Akanda 1, KN Choudhury 2, MZ Ali 1, MK Kabir 3, LN Begum 4, LA Sayami 1 1 National Institute of Cardiovascular
Serum Creatinine and Blood Urea Nitrogen Levels in Patients with Coronary Artery Disease MAK Akanda 1, KN Choudhury 2, MZ Ali 1, MK Kabir 3, LN Begum 4, LA Sayami 1 1 National Institute of Cardiovascular
Management of Hypertensive Chronic Kidney Disease: Role of Calcium Channel Blockers. Robert D. Toto, MD
 R e v i e w P a p e r Management of Hypertensive Chronic Kidney Disease: Role of Calcium Channel Blockers Robert D. Toto, MD Both the prevalence and incidence of end-stage renal disease have been increasing
R e v i e w P a p e r Management of Hypertensive Chronic Kidney Disease: Role of Calcium Channel Blockers Robert D. Toto, MD Both the prevalence and incidence of end-stage renal disease have been increasing
Outline. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 7/23/2013. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
Prevalence of anemia and cardiovascular diseases in chronic kidney disease patients: a single tertiary care centre study
 International Journal of Advances in Medicine Sathyan S et al. Int J Adv Med. 2017 Feb;4(1):247-251 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20170120
International Journal of Advances in Medicine Sathyan S et al. Int J Adv Med. 2017 Feb;4(1):247-251 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20170120
Analytical Methods: the Kidney Early Evaluation Program (KEEP) The Kidney Early Evaluation program (KEEP) is a free, community based health
 Analytical Methods: the Kidney Early Evaluation Program (KEEP) 2000 2006 Database Design and Study Participants The Kidney Early Evaluation program (KEEP) is a free, community based health screening program
Analytical Methods: the Kidney Early Evaluation Program (KEEP) 2000 2006 Database Design and Study Participants The Kidney Early Evaluation program (KEEP) is a free, community based health screening program
Chronic Kidney Disease - An Overview
 REVIEW ARTICLE KERALA MEDICAL JOURNAL Chronic Kidney Disease - An Overview Rajesh R Nair Department of Nephrology, Amrita Institute of Medical Sciences, Kochi, Kerala* ABSTRACT Published on 28 th December
REVIEW ARTICLE KERALA MEDICAL JOURNAL Chronic Kidney Disease - An Overview Rajesh R Nair Department of Nephrology, Amrita Institute of Medical Sciences, Kochi, Kerala* ABSTRACT Published on 28 th December
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
The hypertensive kidney and its Management
 The hypertensive kidney and its Management Dr H0 Chung Ping Hypertension Management Seminar 20061124 Hypertensive kidney Kidney damage asymptomatic till late stage Viscous cycle to augment renal damage
The hypertensive kidney and its Management Dr H0 Chung Ping Hypertension Management Seminar 20061124 Hypertensive kidney Kidney damage asymptomatic till late stage Viscous cycle to augment renal damage
HYPERTENSION IN CKD. LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL
 HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
HYPERTENSION IN CKD LEENA ONGAJYOOTH, M.D., Dr.med RENAL UNIT SIRIRAJ HOSPITAL Stages in Progression of Chronic Kidney Disease and Therapeutic Strategies Complications Normal Increased risk Damage GFR
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
COMPOSITION. A film coated tablet contains. Active ingredient: irbesartan 75 mg, 150 mg or 300 mg. Rotazar (Film coated tablets) Irbesartan
 Rotazar (Film coated tablets) Irbesartan Rotazar 75 mg, 150 mg, 300 mg COMPOSITION A film coated tablet contains Active ingredient: irbesartan 75 mg, 150 mg or 300 mg. Rotazar 75 mg, 150 mg, 300 mg PHARMACOLOGICAL
Rotazar (Film coated tablets) Irbesartan Rotazar 75 mg, 150 mg, 300 mg COMPOSITION A film coated tablet contains Active ingredient: irbesartan 75 mg, 150 mg or 300 mg. Rotazar 75 mg, 150 mg, 300 mg PHARMACOLOGICAL
Outline. Outline 10/14/2014 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW. Question 1: Which of these patients has CKD?
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
DIABETES AND YOUR KIDNEYS
 DIABETES AND YOUR KIDNEYS OR AS WE CALL IT DIABETIC NEPHROPATHY The latest guidelines to keep you safe, healthy, fit, and out of danger from needing dialysis A UCLA HEALTH EDUCATIONAL SEMINAR Ramy M. Hanna
DIABETES AND YOUR KIDNEYS OR AS WE CALL IT DIABETIC NEPHROPATHY The latest guidelines to keep you safe, healthy, fit, and out of danger from needing dialysis A UCLA HEALTH EDUCATIONAL SEMINAR Ramy M. Hanna
Diabetes and kidney disease.
 Diabetes and kidney disease. What are the implications? Can it be prevented? Nice 18 june 2010 Lars G Weiss. M.D. Ph.D. Department of Neprology Central Hospital Karlstad Sweden Diabetic nephropathy vs
Diabetes and kidney disease. What are the implications? Can it be prevented? Nice 18 june 2010 Lars G Weiss. M.D. Ph.D. Department of Neprology Central Hospital Karlstad Sweden Diabetic nephropathy vs
Lab Values Explained. working at full strength. Other possible causes of an elevated BUN include dehydration and heart failure.
 Patient Education Lab Values Explained Common Tests to Help Diagnose Kidney Disease Lab work, urine samples and other tests may be given as you undergo diagnosis and treatment for renal failure. The test
Patient Education Lab Values Explained Common Tests to Help Diagnose Kidney Disease Lab work, urine samples and other tests may be given as you undergo diagnosis and treatment for renal failure. The test
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
HIV AND CHRONIC KIDNEY DISEASE. Understanding GFR
 HIV AND CHRONIC KIDNEY DISEASE Understanding GFR in PEOPLE WITH HIV contents Introduction... 4 Chronic Kidney Disease... 5 What are kidneys and what do they do?... 5 What is glomerular filtration rate
HIV AND CHRONIC KIDNEY DISEASE Understanding GFR in PEOPLE WITH HIV contents Introduction... 4 Chronic Kidney Disease... 5 What are kidneys and what do they do?... 5 What is glomerular filtration rate

 www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to
www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to