Autoimmune pancreatitis (AIP), a clinical entity originally
|
|
|
- Aron Bishop
- 6 years ago
- Views:
Transcription
1 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and Jerome H. Siegel, MD, RPh All of the authors are affiliated with Mount Sinai Beth Israel in New York, New York. Dr Kim and Dr Voaklander are residents in the Department of Internal Medicine. Dr Mannan is a resident in the Department of Pathology. Dr Kasmin, Dr Brown, and Dr Siegel are attending physicians in the Department of Internal Medicine and codirectors of the Advanced Fellowship in Therapeutic Endoscopy. Dr Siegel is also a clinical professor of medicine at the Icahn School of Medicine at Mount Sinai in New York, New York. Abstract: Autoimmune pancreatitis (AIP), a clinical entity originally described in East Asia and more recently recognized in the United States and Europe, poses a diagnostic conundrum for clinicians in the West due to immunoglobulin G4 seronegativity. Although expert panels classify this disease into 2 types, it remains difficult to stratify the disease given that both types share most clinical, biochemical, and imaging characteristics. The classic presentation of AIP can mimic that of pancreatic carcinoma, which increases the urgency of evaluation, diagnosis, and treatment. In this article, we elucidate the differences between the 2 types of AIP, highlight the shortcomings of the current classification system, and propose a more inclusive view of the disorder. Address correspondence to: Dr Jerome H. Siegel 305 Second Avenue, Suite #3 New York, NY Tel: Fax: jhs215@aol.com Keywords Autoimmune pancreatitis, endoscopic retrograde cholangiopancreatography, endoscopic ultrasound, magnetic resonance cholangiopancreatography, fine-needle aspiration, seronegative, seropositive Autoimmune pancreatitis (AIP), a clinical entity originally described in East Asia 1-3 and more recently recognized in the United States and Europe, 4-6 poses a diagnostic conundrum for clinicians in the West due to the prevalence of immunoglobulin G4 (IgG4) seronegativity and extrapancreatic manifestations. Although expert panels classify this disease into 2 types, it remains difficult to stratify the disease given that both types share most clinical, biochemical, and imaging characteristics. Type 1 AIP is distinguished by the presence of IgG4 antibodies and is more common in patients of East Asian ethnicity. Type 2 is the seronegative form of AIP and is more common in patients of Western ethnicity. AIP is associated with disorders of other organs, including inflammatory bowel disease (IBD), sclerosing cholangitis, sclerosing sialadenitis, tubulointerstitial nephritis, and retroperitoneal fibrosis. The presentation of AIP can mimic that of a pancreatic neoplasm, increasing the urgency of evaluation and diagnosis. 3,7,8 In this article, we elucidate the differences between the 2 types of AIP. We also highlight the shortcomings of the current classification system and propose a more inclusive view of this disorder without subclassifying these entities, with the intention of alerting physicians to this confusing situation. Finally, we emphasize the importance of early evaluation to distinguish this relatively benign, corticosteroid-responsive disease from pancreatic carcinoma. 606 Gastroenterology & Hepatology Volume 11, Issue 9 September 2015
2 AUTOIMMUNE PANCREATITIS Table. Characteristics of the Types of Autoimmune Pancreatitis as Defined by the International Consensus Diagnostic Criteria Characteristics Type 1 Autoimmune Pancreatitis Type 2 Autoimmune Pancreatitis Epidemiology Asia > United States, Europe Europe > United States > Asia Age 60 years or older Younger (~40 years) Sex Men > women Men women Serology High serum IgG4, autoab+ Normal serum IgG4, autoab Histopathology Symptoms (overall) Marked lymphocyte and plasmacyte infiltration and fibrosis Infiltration of IgG4+ plasma cells Painless/obstructive jaundice Pancreatic exocrine insufficiency New-onset diabetes Abdominal pain Rare Common Radiologic findings Other organ involvement Pancreatic swelling ( sausage-shaped ) Salivary/submandibular/lacrimal glands Bile ducts (sclerosing cholangitis) Kidneys (renal mass, tubulointerstitial nephritis) Retroperitoneal fibrosis Association with IBD Rare Common Response to corticosteroids Responsive Relapse rate High Low AutoAb, autoantibody; IBD, inflammatory bowel disease; IgG4, immunoglobulin G4. Granulocytic epithelial lesion often with destruction and obliteration of the pancreatic duct Rare Classification AIP is a form of chronic pancreatitis that is clinically characterized by the presentation of cholestasis, obstructive jaundice, and/or a pancreatic mass; histologically characterized by fibrosis and a lymphoplasmacytic infiltrate; and therapeutically characterized by a dramatic response to corticosteroid treatment. In 2011, AIP was formally classified by the International Consensus Diagnostic Criteria into 2 categories: type 1 and type 2 (Table). 9,10 Type 1 AIP is characterized by the histologic description of lymphoplasmacytic sclerosing pancreatitis. It is associated with IgG4-positive serology and other organ involvement (sclerosing cholangitis, sclerosing sialadenitis, tubulointerstitial nephritis, and retroperitoneal fibrosis). This type of AIP is more common in older men and people of East Asian ethnicity, and it has a high relapse rate. Type 2 AIP is characterized by the histopathologic pattern of chronic pancreatitis called idiopathic duct centric pancreatitis or by the presence of granulocyte epithelial lesions. It is associated with IBD but has no known serologic biomarker. This type is more common in younger people of Western (European and American) ethnicity, does not show a sex predilection, and rarely recurs. Clinical Presentation Classically, AIP presents with obstructive jaundice and/or a pancreatic mass. 9 There may be an insidious prodrome of feeling unwell, with complaints of a gnawing midline discomfort sometimes associated with ingestion of food, medications, or alcohol. Mild weight loss is not uncommon. A minority of patients present with a more acute, painful pancreatitis. An international, multicenter survey of 731 AIP patients found obstructive jaundice to be a more frequent presentation in type 1 vs type 2 AIP (75% vs 47%; P<.001), whereas abdominal pain (41% vs 68%; P<.001) and acute pancreatitis (5% vs 34%; P<.001) were more frequent in type 2 AIP. 10 Patients with type 1 AIP have a high relapse rate, and patients with type 2 AIP rarely experience relapse. 11 Imaging The characteristic findings seen on computed tomography (CT), magnetic resonance imaging (MRI), pancreatography, and endoscopic ultrasound (EUS) are common for both types of AIP CT/MRI in AIP shows an enlarged pancreas with featureless borders often described as sausage-shaped (Figure 1). Imaging scans frequently demonstrate pancreatic swelling and occasionally show a Gastroenterology & Hepatology Volume 11, Issue 9 September
3 KIM ET AL Figure 1. A sausage-shaped pancreas. Figure 2. A mass in the head of the pancreas, which can produce biliary obstruction and cholestasis. sion tomography studies, uptake of fluorodeoxyglucose in organs known to be affected by IgG4-related disease other than the pancreas suggests AIP.19 The classic EUS finding in AIP is hyperechoic parenchyma of a pancreatic mass with clear margins. However, with EUS, a definitive diagnosis must be established histologically via multiple fine-needle aspirations or a core biopsy of the lesion Other Organ Involvement Figure 3. A photomicrograph of a pancreatic biopsy showing pancreatic acini and ducts surrounded by dense inflammation comprised of clusters of plasma cells, lymphocytes, and an occasional eosinophil (hematoxylin and eosin stain, 400 magnification). mass, both of which affect biliary obstruction and cholestasis (Figure 2).16 In such cases, the bile duct morphology can be attenuated (stricturing) or dilated, obfuscating the clinical picture because these findings are also present in sclerosing cholangitis and cholangiocarcinoma, which are entities associated with IBD.17 Pancreatographic features include segmental or diffuse irregular narrowing of the main duct.18 CT/MRI can be used to differentiate neoplasms from AIP, which demonstrates clear anatomic surgical planes. Vascular structures are unaffected in most AIP patients, with the exception of venous thrombosis and the development of collateral vessels secondary to the inflammatory process. However, inflammatory changes may extend to peripancreatic lymph nodes, in which case a biopsy is required to rule out neoplasia. In positron emis- Both types of AIP can be associated with extrapancreatic disease. Type 1 commonly has other organ involvement related to IgG4 infiltration. Although previously regarded as isolated single-organ diseases without any known underlying systemic condition, IgG4-related diseases were recently recognized as a unified entity.19,23,24 These diseases can manifest as sclerosing cholangitis, sclerosing sialadenitis, tubulo interstitial nephritis, and/or retroperitoneal fibrosis.6,25 Other affected areas include the lung, prostate, aorta, pericardium, pituitary gland, and lymph nodes. This involvement can present at any time before or after the diagnosis of AIP.26 Both types of AIP are associated with IBD, although much less commonly in type 1.7,8,27-29 This association is predominantly with ulcerative colitis; however, there are reports of AIP associated with Crohn s disease. The incidence is much greater in type 2 AIP (seronegative patients in the West) compared with type 1 AIP (seropositive Asian patients). Histopathology Given the clinical and radiologic similarities between AIP and pancreatic carcinoma, a tissue sample is essential for establishing a definitive diagnosis. This requires EUS, CT guidance, or surgical intervention. The find- 608 Gastroenterology & Hepatology Volume 11, Issue 9 September 2015
4 AUTOIMMUNE PANCREATITIS ing of lymphoplasmacytic infiltration is diagnostic for AIP (Figure 3), and tissue samples often stain positive for IgG4, confirming the diagnosis. 30,31 The Japanese Pancreas Society introduced the first diagnostic criteria, which were expanded by the Mayo Clinic and named the HISORt criteria (histology, imaging, serology, other organ involvement, and response to corticosteroid therapy). 32 These criteria allow for the noninvasive diagnosis of type 1 AIP; however, obtaining tissue for histologic confirmation remains essential to diagnose type 2 AIP and rule out carcinoma. 31,33,34 Treatment Corticosteroids are generally considered to be very effective in the treatment of AIP. A clinical and radiologic response to corticosteroids is usually seen in 2 to 4 weeks, which, per the HISORt criteria, corroborates the diagnosis of AIP in patients without a biopsy. 35 Patients usually receive prednisone at 40 to 50 mg daily (weight adjusted, mg/kg daily) for 4 weeks; this dose is slowly reduced by 5 mg per week for up to 11 or 12 weeks. 36,37 Relapse is common in type 1 AIP and most often affects the proximal biliary tree and/or pancreas. Another course of corticosteroid treatment should be initiated, and longterm corticosteroid maintenance therapy for up to 3 years may benefit patients with continuous relapses. If patients do not tolerate corticosteroids or if the risks and complications associated with long-term therapy are unacceptable, corticosteroid-sparing immunomodulators such as azathioprine or rituximab (Rituxan, Genentech/Biogen Idec) have been utilized with long-term success. 38,39 Neoplasms Associated With Autoimmune Pancreatitis Patients with IgG4-related disease are suspected to have an increased risk of malignancies. 36,40,41 A report from Japan revealed that, over a 3-year period of observation, 11 of 106 patients with IgG4-related disease were diagnosed with cancer, including colon cancer, lung cancer, and lymphoma. 41 This is 3.5 times more frequent than in the general population. Another report from Japan similarly demonstrated that 15% of their cohort of 108 patients developed cancer within the first year of diagnosis. 26 An issue of whether to distinguish AIP from cancer on initial presentation remains a dilemma. This dilemma is especially imposing in patients who present with seronegative studies, as most patients do in the West. When other imaging studies and core biopsies are completed, and the results are negative, most experts recommend a short course of corticosteroids. The follow-up imaging studies and the patient s response should verify the diagnosis. Figure 4. Resolution of a pancreatic mass on a repeat computed tomography scan. If the results are equivocal and the lesion is resectable, surgery is recommended. However, in our institution, where we have experienced pancreatic surgeons, surgery is performed very infrequently. Analysis The original diagnosis of AIP was one of exclusion until the 1960s when hypergammaglobulinemia was determined to be a more objective marker for diagnosis. 42 Decades later, investigators noted 2 distinct patterns of the disease. 5,6 It was not until the early 2000s that a more definitive set of guidelines and classifications were established. The guidelines defined 2 types of AIP, classifying them by their serologic and histologic characteristics, and discussing other distinguishing features of each type (Table). Our intention is to alter the strict classifications accepted today and demystify these associations. The 2 types of AIP are interrelated, but we feel that classification into 2 simple but tightly defined groups is misguided. AIP was originally described in East Asia using criteria for what is now defined as type 1 AIP. IBD is much less common in East Asians compared with whites; thus, a concurrent diagnosis of AIP and IBD in East Asia was considered an outlier and not part of the AIP manifestation. As AIP was recognized more in the West and type 2 AIP was described, the association with IBD gained more attention. Interestingly, both AIP and IBD are associated with other organ involvement, many types of which they share in common. This commonality causes us to question whether AIP is a separate entity or part of the complex of extracolonic manifestations of IBD. Figures 1 through 3 are from a patient who has the potential to manifest characteristics from both types 1 and 2 AIP (an elderly white man with a history of Crohn s disease, nonsarcoid hilar adenopathy, and recurrent AIP). Gastroenterology & Hepatology Volume 11, Issue 9 September
5 KIM ET AL Initial and repeat biopsies confirmed the presence of IgG4-negative type 1 AIP. The patient s response to corticosteroid treatment was confirmed with repeat CT imaging (Figure 4). However, several months later, the patient seroconverted positive for IgG4 with markedly elevated serum levels. Cases such as this one suggest that AIP (both types 1 and 2) is not an isolated disease, but rather part of a syndrome with a unifying autoimmune component. The conclusive diagnosis of seronegative AIP has been challenging until recently. Historically, AIP was a diagnosis of exclusion. After other causes of pancreatitis were evaluated more easily (gallstones, alcohol, viruses, or medications), these seronegative patients were left with the ambiguous diagnosis of idiopathic pancreatitis. With this vague diagnosis and suspicion for AIP, clinicians were sometimes reluctant to commit patients to a course of corticosteroid treatment, especially when the possibility of a neoplasm had not been completely eliminated. The precision of AIP diagnosis has greatly improved in recent years, secondary to the concomitant evolution of diagnostic technologies. CT can distinguish auto immune from other types of pancreatitis, and the use of EUS with fine-needle aspirations and core biopsies has further defined the diagnosis. These techniques are significantly less invasive modes of obtaining definitive histology, thus ruling out carcinoma and confirming a diagnosis of AIP that is otherwise difficult to make, especially in IgG4- negative patients in the West. Of concern to many clinicians is when the pancreatic histopathology is inconclusive or when tissue biopsy is not possible. In this not-uncommon scenario, one is tempted to refer patients for immediate surgical consultation for a definitive operation for cancer or palliative bypass decompression. However, it is recommended that a short trial of corticosteroid treatment be given first. Such a trial can elucidate the difference between AIP and carcinoma because AIP has a dramatic and lasting response to this therapy. Pancreatic carcinoma may show temporary clinical improvement with corticosteroid treatment; however, rapid recurrence of symptoms and/or radiologic findings is highly suggestive of neoplasm and warrants aggressive surgical intervention. A correct and timely recognition of AIP prevents unnecessary surgery and reduces patient anxiety, whereas a misdiagnosis of AIP can be very problematic, especially if patients are misdiagnosed with pancreatic cancer. We suspect that the number of AIP patients who mistakenly have undergone surgical resection for suspected carcinoma has altered the epidemiologic data on pancreatic cancer survivorship. We emphasize, however, that early pancreatic cancer detection is paramount to patient survival. We conclude that early, accurate differentiation between AIP and pancreatic carcinoma can reduce patient morbidity. Conclusion AIP is ubiquitous, presents in several ways, and is associated with other intercurrent medical problems, including IBD and other autoimmune disorders. The classic presentation of AIP can mimic that of pancreatic carcinoma. This presents a conundrum for clinicians in the West because a majority of white patients are IgG4-seronegative, making the definitive diagnosis of AIP nearly impossible without tissue biopsy. In this scenario, rather than immediate invasive surgical intervention, we recommend obtaining tissue for diagnosis via EUS- or CT-guided biopsy and beginning treatment with corticosteroids. The clinical response to corticosteroids is rapid and dramatic in both types of AIP, reassuring the clinician that the decision to start this medication was appropriate. Serial follow-up imaging studies will ultimately justify this decision. The authors have no relevant conflicts of interest to disclose. References 1. Yoshida K, Toki F, Takeuchi T, Watanabe S, Shiratori K, Hayashi N. Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig Dis Sci. 1995;40(7): Nishimori I, Tamakoshi A, Otsuki M; Research Committee on Intractable Diseases of the Pancreas, Ministry of Health, Labour, and Welfare of Japan. Prevalence of autoimmune pancreatitis in Japan from a nationwide survey in J Gastroenterol. 2007;42(suppl 18): Kamisawa T, Egawa N, Nakajima H. Autoimmune pancreatitis is a systemic autoimmune disease. Am J Gastroenterol. 2003;98(12): Kasmin FE, Cooperman A, Cohen SA, Wayne M, Brown WH, Siegel JH. Seronegative autoimmune pancreatitis a commonly missed diagnosis in U.S. patients? Gastroenterology. 2008;134(4):A Sutton R. Autoimmune pancreatitis also a Western disease. Gut. 2005;54(5): Raina A, Yadav D, Krasinskas AM, et al. Evaluation and management of autoimmune pancreatitis: experience at a large US center. Am J Gastroenterol. 2009;104(9): Ravi K, Chari ST, Vege SS, Sandborn WJ, Smyrk TC, Loftus EV Jr. Inflammatory bowel disease in the setting of autoimmune pancreatitis. Inflamm Bowel Dis. 2009;15(9): Pitchumoni CS, Chari S. Ulcerative colitis and autoimmune pancreatitis. J Clin Gastroenterol. 2013;47(6): Shimosegawa T, Chari ST, Frulloni L, et al; International Association of Pancreatology. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas. 2011;40(3): Kamisawa T, Chari ST, Giday SA, et al. Clinical profile of autoimmune pancreatitis and its histological subtypes: an international multicenter survey. Pancreas. 2011;40(6): Sah RP, Chari ST, Pannala R, et al. Differences in clinical profile and relapse rate of type 1 versus type 2 autoimmune pancreatitis. Gastroenterology. 2010;139(1): Proctor RD, Rofe CJ, Bryant TJ, Hacking CN, Stedman B. Autoimmune pancreatitis: an illustrated guide to diagnosis. Clin Radiol. 2013;68(4): Park SH, Kim MH, Kim SY, et al. Magnetic resonance cholangiopancreatography for the diagnostic evaluation of autoimmune pancreatitis. Pancreas. 2010;39(8): Hoki N, Mizuno N, Sawaki A, et al. Diagnosis of autoimmune pancreatitis using endoscopic ultrasonography. J Gastroenterol. 2009;44(2): Sugumar A, Levy MJ, Kamisawa T, et al. Endoscopic retrograde pancreatography criteria to diagnose autoimmune pancreatitis: an international multicentre study. Gut. 2011;60(5): Gastroenterology & Hepatology Volume 11, Issue 9 September 2015
6 AUTOIMMUNE PANCREATITIS 16. Kamisawa T, Tu Y, Egawa N, Nakajima H, Tsuruta K, Okamoto A. Involvement of pancreatic and bile ducts in autoimmune pancreatitis. World J Gastroenterol. 2006;12(4): Nakazawa T, Ohara H, Sano H, et al. Cholangiography can discriminate sclerosing cholangitis with autoimmune pancreatitis from primary sclerosing cholangitis. Gastrointest Endosc. 2004;60(6): Horiuchi A, Kawa S, Hamano H, Hayama M, Ota H, Kiyosawa K. ERCP features in 27 patients with autoimmune pancreatitis. Gastrointest Endosc. 2002;55(4): Kamisawa T, Zen Y, Pillai S, Stone JH. IgG4-related disease. Lancet. 2015;385(9976): Moon SH, Kim MH. The role of endoscopy in the diagnosis of autoimmune pancreatitis. Gastrointest Endosc. 2012;76(3): Levy MJ. Endoscopic ultrasound-guided trucut biopsy of the pancreas: prospects and problems. Pancreatology. 2007;7(2-3): Mizuno N, Bhatia V, Hosoda W, et al. Histological diagnosis of autoimmune pancreatitis using EUS-guided trucut biopsy: a comparison study with EUS-FNA. J Gastroenterol. 2009;44(7): Stone JH, Brito-Zerón P, Bosch X, Ramos-Casals M. Diagnostic approach to the complexity of IgG4-related disease. Mayo Clin Proc. 2015;90(7): Islam AD, Selmi C, Datta-Mitra A, et al. The changing faces of IgG4-related disease: clinical manifestations and pathogenesis [published online June 23, 2015]. Autoimmun Rev. doi: /j.autrev Ghazale A, Chari ST, Smyrk TC, et al. Value of serum IgG4 in the diagnosis of autoimmune pancreatitis and in distinguishing it from pancreatic cancer. Am J Gastroenterol. 2007;102(8): Shiokawa M, Kodama Y, Yoshimura K, et al. Risk of cancer in patients with autoimmune pancreatitis. Am J Gastroenterol. 2013;108(4): Danese S, Semeraro S, Papa A, et al. Extraintestinal manifestations in inflammatory bowel disease. World J Gastroenterol. 2005;11(46): Kawa S, Okazaki K, Notohara K, et al. Autoimmune pancreatitis complicated with inflammatory bowel disease and comparative study of type 1 and type 2 autoimmune pancreatitis. J Gastroenterol. 2015;50(7): Park SH, Kim D, Ye BD, et al. The characteristics of ulcerative colitis associated with autoimmune pancreatitis. J Clin Gastroenterol. 2013;47(6): Notohara K, Burgart LJ, Yadav D, Chari S, Smyrk TC. Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am J Surg Pathol. 2003;27(8): Kawaguchi K, Koike M, Tsuruta K, Okamoto A, Tabata I, Fujita N. Lymphoplasmacytic sclerosing pancreatitis with cholangitis: a variant of primary sclerosing cholangitis extensively involving pancreas. Hum Pathol. 1991;22(4): Chari ST, Smyrk TC, Levy MJ, et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol. 2006;4(8): Sah RP, Chari ST. Autoimmune pancreatitis: an update on classification, diagnosis, natural history and management. Curr Gastroenterol Rep. 2012;14(2): Chari ST, Takahashi N, Levy MJ, et al. A diagnostic strategy to distinguish autoimmune pancreatitis from pancreatic cancer. Clin Gastroenterol Hepatol. 2009;7(10): Moon SH, Kim MH, Park DH, et al. Is a 2-week steroid trial after initial negative investigation for malignancy useful in differentiating autoimmune pancreatitis from pancreatic cancer? A prospective outcome study. Gut. 2008;57(12): Kamisawa T, Shimosegawa T, Okazaki K, et al. Standard steroid treatment for autoimmune pancreatitis. Gut. 2009;58(11): Pannala R, Chari ST. Corticosteroid treatment for autoimmune pancreatitis. Gut. 2009;58(11): Sandanayake NS, Church NI, Chapman MH, et al. Presentation and management of post-treatment relapse in autoimmune pancreatitis/immunoglobulin G4-associated cholangitis. Clin Gastroenterol Hepatol. 2009;7(10): Topazian M, Witzig TE, Smyrk TC, et al. Rituximab therapy for refractory biliary strictures in immunoglobulin G4-associated cholangitis. Clin Gastroenterol Hepatol. 2008;6(3): Hart PA, Kamisawa T, Brugge WR, et al. Long-term outcomes of autoimmune pancreatitis: a multicentre, international analysis. Gut. 2013;62(12): Yamamoto M, Takahashi H, Tabeya T, et al. Risk of malignancies in IgG4- related disease. Mod Rheumatol. 2012;22(3): Sarles H, Sarles JC, Muratore R, Guien C. Chronic inflammatory sclerosis of the pancreas an autonomous pancreatic disease? Am J Dig Dis. 1961;6: Gastroenterology & Hepatology Volume 11, Issue 9 September
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
FOR PUBLIC CONSULTATION ONLY. Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD)
 Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
University of Texas-MD Anderson Cancer Center, Houston, Texas, USA. University of Medicine and Pharmacy Craiova, Romania
 Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones
 MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
Dilemmas in autoimmune pancreatitis. Surgical resection or not?
 DOI: 10.4149/BLL_2016_090 Bratisl Med J 2016; 117 (8) CLINICAL STUDY Dilemmas in autoimmune pancreatitis. Surgical resection or not? Hoffmanova I 1, Gurlich R 2, Janik V 3, Szabo A 4, Vernerova Z 4 Second
DOI: 10.4149/BLL_2016_090 Bratisl Med J 2016; 117 (8) CLINICAL STUDY Dilemmas in autoimmune pancreatitis. Surgical resection or not? Hoffmanova I 1, Gurlich R 2, Janik V 3, Szabo A 4, Vernerova Z 4 Second
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term Follow-Up Study of 73 Japanese Patients
 International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Incidence of Malignancies in Patients with IgG4-related Disease
 ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
Cerebral involvement in IgG4-related disease
 ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
Immunoglobulin G4 (IgG4)-related disease, a systemic,
 IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases
 MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Clinical Study Evaluation and Clinical Validity of a New Questionnaire for Mikulicz s Disease
 International Rheumatology Volume 2, Article ID 283459, pages doi:1.1155/2/283459 Clinical Study Evaluation and Clinical Validity of a New Questionnaire for Mikulicz s Disease Motohisa Yamamoto, 1 Hiroki
International Rheumatology Volume 2, Article ID 283459, pages doi:1.1155/2/283459 Clinical Study Evaluation and Clinical Validity of a New Questionnaire for Mikulicz s Disease Motohisa Yamamoto, 1 Hiroki
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers
 Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Overview of PSC Making the Diagnosis
 Overview of PSC Making the Diagnosis Tamar Taddei, MD Assistant Professor of Medicine Yale University School of Medicine Overview Definition Epidemiology Diagnosis Modes of presentation Associated diseases
Overview of PSC Making the Diagnosis Tamar Taddei, MD Assistant Professor of Medicine Yale University School of Medicine Overview Definition Epidemiology Diagnosis Modes of presentation Associated diseases
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Evaluation and Management of Refractory Biliary Stricture. J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc.
 Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
A case of retroperitoneal fibrosis responding to steroid therapy
 Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
IgG4-Related Disease: Dataset of 235 Consecutive Patients
 IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hideaki Miura, Yasutaka Miyachi. Department of Internal Medicine, Social Insurance Central General Hospital. Tokyo, Japan
 CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Autoimmune pancreatitis (AIP) is a chronic fibroinflammatory
 Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
ENDOSCOPY IN COMPETITION DIAGNOSTICS. Dr. med. Dirk Hartmann Klinikum Ludwigshafen
 Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune pancreatitis
 J Gastroenterol (2014) 49:961 970 DOI 10.1007/s00535-014-0945-z SPECIAL ARTICLE Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune
J Gastroenterol (2014) 49:961 970 DOI 10.1007/s00535-014-0945-z SPECIAL ARTICLE Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN
 Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Immunoglobulin G4-related sclerosing cholangitis
 REVIEW Korean J Intern Med 2018;33:841-850 https://doi.org/10.3904/kjim.2018.018 Immunoglobulin G4-related sclerosing cholangitis George Goodchild, Stephen P. Pereira, and George Webster Department of
REVIEW Korean J Intern Med 2018;33:841-850 https://doi.org/10.3904/kjim.2018.018 Immunoglobulin G4-related sclerosing cholangitis George Goodchild, Stephen P. Pereira, and George Webster Department of
Autoimmune pancreatitis can transform into chronic features similar to advanced
 Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up
 CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids. Cholestasis
 Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
LIVER SPECIALTY CONFERENCE USCAP Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA
 LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
Autoimmune Pancreatitis Novel Insights on Diagnosis, Treatment and Outcome. Jorie Buijs
 Autoimmune Pancreatitis Novel Insights on Diagnosis, Treatment and Outcome Jorie Buijs COLOFON Jorie Buijs, The Netherlands, 2015 ISBN: 978-94-6182-621-3 All rights reserved. No parts of this thesis may
Autoimmune Pancreatitis Novel Insights on Diagnosis, Treatment and Outcome Jorie Buijs COLOFON Jorie Buijs, The Netherlands, 2015 ISBN: 978-94-6182-621-3 All rights reserved. No parts of this thesis may
Pediatric Primary Sclerosing Cholangitis and Potential Therapies
 Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal
 CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
Frank Burton Memorial Update on Pancreato-biliary Cancers
 Frank Burton Memorial Update on Pancreato-biliary Cancers Diagnosis and management of pancreatic cancer: common dilemmas Moderators: Banke Agarwal, MD Paul Buse, MD Evaluation of patients with obstructive
Frank Burton Memorial Update on Pancreato-biliary Cancers Diagnosis and management of pancreatic cancer: common dilemmas Moderators: Banke Agarwal, MD Paul Buse, MD Evaluation of patients with obstructive
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid
 The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
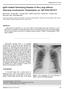 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Title: Painless jaundice as an initial presentation of lung adenocarcinoma
 Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Chronic Cholestatic Liver Diseases
 Chronic Cholestatic Liver Diseases - EASL Clinical Practice Guidelines - Rome, 8 October 2010 Ulrich Beuers Department of Gastroenterology and Hepatology Tytgat Institute of Liver and Intestinal Research
Chronic Cholestatic Liver Diseases - EASL Clinical Practice Guidelines - Rome, 8 October 2010 Ulrich Beuers Department of Gastroenterology and Hepatology Tytgat Institute of Liver and Intestinal Research
