Overview of Diagnostic Criteria for Autoimmune Pancreatitis
|
|
|
- Sarah Powers
- 6 years ago
- Views:
Transcription
1 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Korea Ji Kon Ryu, M.D. Introduction 1n 1995, Yoshida et al. 1 summarized the clinical features of several patients with unusual chronic pancreatitis showing diffuse irregular narrowing of main pancreatic duct and proposed the concept of autoimmune pancreatitis (AIP). Thereafter, many cases of AIP have been reported in Western countries as well as Japan. In Korea, 1 st case of AIP was reported in and AIP is increasingly being reported. 3 The increments probably seems to be due to the growing awareness of the disease entity rather than a rise of the true incidence. According to the multicenter nationwide study in Korea, AIP was 2.0% among 814 patients with chronic pancreatitis. 4 For the past four decades, various morphologic descriptions have been proposed to characterize this disease: nonalcoholic duct-destructive chronic pancreatitis, lymphoplasmacytic sclerosing pancreatitis with cholangitis, chronic sclerosing pancreatitis, pseudotumorous pancreatitis, and duct-narrowing chronic pancreatitis. Recently, the term autoimmune pancreatitis has become widely accepted, although it is apparent that AIP is a heterogeneous disease. Although, Japan Pancreas Society proposed the diagnostic criteria for the first time in 2002, 5 the diagnosis of AIP is still challenging. Recently, several other diagnostic criteria were proposed as followings: revised proposal of JPS criteria 2006, 6 HISORt criteria by Mayo Clinic, 7 Kim s criteria, 8 Massachusetts General Hospital criteria. 9 So, the new diagnostic criteria which lead to less inter-observer variation and provide a strong base for the research with worldwide consensus are necessary. Historical Background of AIP In 1961, pancreatitis associated with hypergammaglobulinemia was first reported and autoimmunity was suggested as a pathogenetic mechanism. 10 Since then, there were several worldwide case reports about unusual chronic pancreatitis with extrapancreatic manifestations suggesting the possibility of AIP However, they did not have the concept of AIP and various terminology were used such as lymphoplasmacytic sclerosing pancreatitis with cholangitis, chronic sclerosing pancreatitis in Sjogren's syndrome, pseudotumor of the pancreas associated with retroperitoneal fibrosis with a dramatic response to corticosteroid therapy. After all, Yoshida et al. summarized the clinical features of several patients with unusual chronic pancreatitis showing diffuse irregular narrowing of main pancreatic duct and proposed the concept of AIP in 1995, for the first time. 1 In 1997, Ito T also reported three cases of AIP with effective steroid therapy, 14 and Irie H described CT and MR imaging characteristics in patients with AIP as diffuse pancreatic enlargement and capsule like rim in Since then, some European authors also reported 105
2 년도대한췌담도학회추계학술대회 the several cases with unusual chronic pancreatitis as a non-alcoholic duct destructive chronic pancreatitis and accepted the concept of AIP In 2000, Okazaki K studied the association of autoantibody and AIP in 17 patients and reported that more than one autoantibody such as antinuclear Ab, antilactoferrin Ab, anti-carbonic anhydrase II Ab was observed in all patients. 19 His study suggested that an autoimmune mechanism against carbonic anhydrase-ii or lactoferrin might be involved in AIP. In 2001, Japanese researchers have carefully studied the changes in immunoglobulin levels in AIP patients. They found a distinctive rise in serum IgG4 levels and an elevation of IgG4 containing immune complexes in the vast majority of patients with AIP. 20 Finally, based on the radiological, serological and pathological features of these patients, Japan Pancreas Society proposed the diagnostic criteria for the first time in In 2001, Whitcomb DC proposed new TIGAR-O classification system based on the etiologic risk factors associated with chronic pancreatitis and TIGAR-O system included AIP as a distinct entity of chronic pancreatitis. 21 There was a 1 st topic discussion session about controversies in clinical pancreatology (Autoimmune Pancreatitis: dose It Exist?) at the American Pancreatic Association meeting November 14, The Japanese, Italian and American doctors presented their experiences about AIP and discussed about the points of consensus and differences. Okazaki K presented the diagnostic criteria of AIP which was proposed by the Japan Pancreas society and Cavallini G talked about the Italian criteria. However, American doctors presented the clinicopathologic features of idiopathic tumefactive chronic pancreatitis. They concluded that the entity of AIP may be an important emerging clinical syndrome and patients presenting with painless obstructive jaundice with markers of autoimmunity, may deserve a short course of corticosteroid before surgical resection. They also expected the agreement of the pathology of AIP and simplification of terminology. Before the proposal of AIP, histopathologic features of chronic pancreatitis usually encountered in practice did not provide information about its etiology. However, in 2003, several American retrospective pathologic studies reported unusual characteristic chronic pancreatitis diagnosed after surgical resection which was clearly different from usual chronic pancreatitis and obstructive pancreatitis The titles were 1) Idiopathic tumefactive chronic pancreatitis: clinical profile, histology, and natural history after resection, 2) Lymphoplasmacytic sclerosing pancreatitis: inflammatory mimic of pancreatic carcinoma, 3) Pancreaticoduodenectomy (Whipple resections) in patients without malignancy: are they all chronic pancreatitis?, 4) Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration. Especially, Mayo Clinic collected retrospectively surgical pathology database underwent pancreatic resection for suspicion of pancreatic cancer owing to a mass and/or obstructive jaundice and on histology were diagnosed to have chronic pancreatitis. 22 They defined such patients as having tumefactive chronic pancreatitis in which three distinct histologic patterns were identified such as typical CP, lymphoplasmacytic sclerosing pancreatitis (LPSP), and idiopathic duct-centric CP (IDCP). Because LPSP had diffuse fibrosis with lymphoplasmacytic infiltration and obliterative phlebitis, they agreed that LPSP was pathologically similar to AIP. However, they only suggested the possibility of AIP and did not use the terminology of AIP. In 2003, European pathologists described the pathological, clinical, and immunological features of AIP based on the 54 patients that were accumulated in Germany, Belgium, and Italy. 26 However, they did
3 Ji Kon Ryu:Overview of Diagnostic Criteria for Autoimmune Pancreatitis 107 not propose the diagnostic criteria of AIP. In 2003, close relationship between autoimmune pancreatitis and multifocal fibrosclerosis was reported by Japanese. 27 They suggested that AIP may not be a simple pancreatitis but one lesion of systemic disease of multifocal fibrosclerosis including sclerosing cholangitis, retroperotoneal fibrosis and Riedel's thyroiditis, fibrotic pseudotumour of the orbit and fibrosis of the salivary glands. In 2006, the concept of IgG4 related autoimmune disease was first proposed by Kamisawa T et al, who showed a number of IgG4 antibody stained plasma cells in number of organs in human body. 28 Kamisawa T insisted that the elevation of serum IgG4 levels and infiltration of abundant IgG4 positive plasma cells into various organs were rather specific to AIP patients. Recently, in 2007, Bjornsson E reviewed the literature about steroid response unusual cholangitis on new emerging clinical entity and suggested that this condition of steroid responsive biliary strictures be named IgG4 associated cholangitis which seemed to have a better prognosis than primary sclerosing cholangitis and were often, but not always, associated with AIP. 29 Many Kinds of Diagnostic Criteria for AIP Because AIP can mimic pancreatic cancer both clinically and radiographically, and because it is responsive to steroid therapy, the goal is to make a diagnosis preoperatively to avoid unnecessary surgery. The overall impact of a missed diagnosis of AIP is not trivial. In one large series, 11 (2.5%) of 442 Whipple resections were for AIP; all were thought to be malignant preoperatively. 24 For the first time, the Japanese published diagnostic criteria in 2002 based on their clinical experience (Fig. 1) The criteria contained three components: pancreatic imaging, laboratory data, and histopathologic findings. At the American Pancreatic Association meeting November 14, 2002, Italian doctor, Giorgio Cavallini presented their own criteria which consisted of histology and cytology, the association with other autoimmune disease, response to steroid therapy. 5 In 2005, Spain group published their own diagnostic criteria using scoring system. The criteria included clinical manifestation, morphologic parameters, laboratory parameters (serum IgG and ANA) and definite diagnosis was made only with histopathology. 30 A total joint score of 0 or 1 was considered probably not AIP, 2 as possible AIP, and 3 as probable AIP. In 2006, four diagnostic criteria were published in Korea, Japan and U.S.A. In Korea, Kim MH proposed Kim's criteria based on his experience of 28 patients with AIP at single center. 8 Kim s criteria included pancreatic imaging, laboratory findings, histopathologic findings and response to steroid. He had designed a system where patients are stratified by evidence strength for AIP into definite, probable and possible. He emphasized Fig. 1. Diagnostic criteria of 2002 autoimmune pancreatitis by Japan Pancreas Society.
4 년도대한췌담도학회추계학술대회 that a diagnostic trial of steroid can be initiated even though serologic markers or pathologic findings do not fulfill the Japanese criteria, providing that pancreatic image are typical to AIP. In Japan, clinical diagnostic criteria of AIP were published as a revised proposal by the research Fig. 2. Clinical diagnostic criteria of autoimmune pancreatitis (2006 Revised Proposal) by Japan Pancreas Society. Fig. 3. Diagnostic criteria of autoimmune pancreatitis (HISORt criteria) by Mayo Clinic.
5 Ji Kon Ryu:Overview of Diagnostic Criteria for Autoimmune Pancreatitis 109 committee of intractable disease of the pancreas supported by the Japan Pancreas Society (Fig. 2). 6 They focused on how to distinguish it from pancreatic or biliary cancer. The criteria contained three components as same as previous Japan criteria and some minor modification were done. The Japanese criteria are based on the minimum consensus features of AIP in order to avoid the misdiagnosis of malignancy as far as possible, but not to pick up suspicious cases of AIP. The HISORt criteria were proposed by the Mayo Clinic based on the 29 patients who met histologic criteria for AIP at single center (Fig. 3). 7 The criteria included 5 categories: histology, imaging, serology, other organ involvement and response to steroid therapy. According to HISORt criteria, AIP can be diagnosed by three groups of diagnostic criteria: group A with typical histology and IgG4 immunostaining, group B with typical imaging and serology, group C with unexplained pancreatic disease with serology and response to steroid. The authors pointed out that the Japanese criteria for AIP focus heavily on characteristic pancreatic imaging and therefore lack sensitivity to diagnose the wide spectrum of manifestations of AIP. They insisted that HISORt criteria reflected the current understanding of AIP as a systemic steroid-responsive disorder characterized by tissue infiltration with IgG4-positive cells and clearly identify a wider. Another new diagnostic criteria were proposed by Brugge WR at Massachusetts General Hospital (MGH) (Fig. 4). 9 They defined AIP as a type of chronic pancreatitis characterized by an autoimmune inflammatory process in which prominent lymphocyte infiltration with associated fibrosis of the pancreas causes organ dysfunction. The MGH criteria were modified from those of the Japan Pancreas Society and minor modifications were done to elevate diagnostic sensitivity. They also suggested the diagnostic and treatment algorithm for AIP according to their diagnostic criteria. Recently, Japanese authors examined the imaging findings of 37 AIP cases and also examined misdiagnosed cases of AIP to determine their reasons for Fig. 4. Diagnostic criteria of autoimmune pancreatitis by MGH.
6 년도대한췌담도학회추계학술대회 misdiagnosis. 31 Only 7 patients had typical AIP findings and six patients were misdiagnosed with pancreatic cancer and 2 with bile-duct cancer. Seven cases were surgically treated. They pointed out that Japanese criteria are too narrow and do not capture the broad spectrum of presentation. They suggest that AIP presents a variety of imaging findings and the most important diagnostic factor is clinician awareness of the concept of AIP and the diverse nature of imaging findings. Can a tissue biopsy be the gold standard for the diagnosis of AIP? Theoretically, the answer is yes, because there are histopathologic features of AIP that are distinct from other forms of chronic pancreatitis. The histology of AIP, termed lymphoplasmacytic sclerosing pancreatitis, is characterized by a lymphoplasmacytic infiltrate around small-sized ducts, swirling fibrosis centered around ducts and veins (storiform fibrosis), and obliterative phlebitis wherein the infiltrate surrounds pancreatic venules while sparing arterioles. AIP is a heterogeneous disease, however, and the diagnostic features can be missed on a single core biopsy. Interestingly, in the study by Chari ST et al, 7 7 (44%) of 16 core biopsies showed the characteristic features of AIP, including periductal lymphoplasmacytic inflammation with fibrosis and obliterative phlebitis. In a separate report by the same institution, the diagnosis of AIP can not be made in patients undergoing EUS with fine-needle aspiration (nine patients) because of the lack of tissue Korean Criteria for Autoimmune Pancreatitis Definite Diagnosis: Criterion I with anyone of Criterion II to IV Criterion I. Imaging (Both required) 1. Imaging (CT or MRI) of pancreatic parenchyma; Diffusely/segmentally/focally enlarged gland, occasionally with mass and/or hypoattenuation rim 2. Imaging (ERCP or MRCP) of pancreaticobiliary ducts; Diffuse/segmental/focal pancreatic ductal narrowing, often with the stenosis of bile duct Criterion II. Serology (One required) 1. Elevated level of serum IgG or IgG4 2. Detected autoantibodies Criterion III. Histopathology of pancreatic / extrapancreatic lesions (One required) 1. Lymphoplasmacytic infiltration & fibrosis, often with obliterative phlebitis 2. Presence of abundant (>10 cells/hpf) IgG4-positive plasma cells Criterion IV. Response to steroids 1. Resolution/marked improvement of pancreatic/ extrapancreatic lesion with steroid therapy Probable Diagnosis: Criterion V or VI Criterion V. Unexplained pancreatic disease but only with characteristic pancreatic histology Criterion VI. (Both required) 1. Other organ involvement and/or serologic abnormalities* 2. Various atypical pancreatic imaging suggesting chronic pancreatitis with negative workup for known etiologies * The confirmation of other organ involvement detected on imaging findings (One required). i) The histology of other organ shows changes of full spectrum of lymphoplasmacytic sclerosing pancreatitis (LPSP). ii) The histology of other organ shows abundant IgG4-positive cell infiltration on immunostaining. iii) The elevated serum IgG/IgG4 level in combination with marked improvement/resolution of the organ lesion after steroid therapy. Fig. 5. Korean Diagnostic Criteria of Autoimmune Pancreatitis by Korean Society of Pancreatobiliary Diseases.
7 Ji Kon Ryu:Overview of Diagnostic Criteria for Autoimmune Pancreatitis 111 architecture. 32 EUS guided pancreatic aspiration is preferred to percutaneous core biopsy because the low risk of complication and cancer seeding risk if the pancreatic mass is malignant. In most clinical situation, it is not common to use the histological criteria to diagnose AIP unless surgical biopsy. In Korea, new Korean diagnostic criteria are established by the Korean Society of Pancreatobiliary Diseases and based on the Kim s criteria including response to steroid therapy to improved the diagnostic sensitivity and specificity (Fig. 5). Korean criteria considered the variety of imaging findings of AIP and low yield of histologic acquisition. The Korean criteria will be published sooner or later. Conclusions AIP is a benign, IgG4-related, fibroinflammatory form of chronic pancreatitis that can mimic pancreatic ductal adenocarcinoma both clinically and radiologically. Clinically, AIP most commonly presents as obstructive jaundice associated with a biliary stricture and tends to respond to steroid therapy. Radiologically, AIP can appear as a focal lesion or mass, or can diffusely involve the pancreas with associated focal or diffuse narrowing of the pancreatic duct. Histopathologically, the hallmark features of AIP are a periductal lymphoplasmacytic infiltrate; obliterative phlebitis; and abundant IgG4-positive plasma cells. These features are used as diagnostic criteria in AIP. Making a diagnosis of AIP can be challenging but is important to prevent unnecessary surgery. Diagnostic criteria have been proposed that incorporate histologic, radiologic, serologic, and clinical information, including the presence of other associated diseases and response to steroid therapy. Because the distinction between AIP and pancreatic cancer is difficult to make in many cases, every attempt needs to be made to exclude the possibility of malignancy, even if it results in a pancreatic resection for benign disease in some patients. As more data are gathered on AIP across the world, the diagnostic criteria will be shifted. REFERENCES 1. Yoshida K, Toki F, Takeuchi T, Watanabe S, Shiratori K, Hayashi N: Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig Dis Sci 1995; 40: Kim JY, Chang HS, Kim MH, et al: A case of autoimmune chronic pancreatitis improved with oral steroid therapy. Korean J Gastroenterol 2002; 39: Kim KP, Kim MH, Lee YJ, et al: Clinical characteristics of 17 cases of autoimmune chronic pancreatitis. Korean J Gastroenterol 2004; 43: Ryu JK, Lee JK, Kim YT, et al: Clinical features of chronic pancreatitis in Korea: a multicenter nationwide study. Digestion 2005; 72: Pearson RK, Longnecker DS, Chari ST, Smyrk TC, Okazaki K, Frulloni L, Cavallini G. Controversies in clinical pancreatology: autoimmune pancreatitis: does it exist? Pancreas 2003; 27: Okazaki K, Kawa S, Kamisawa T, et al: Clinical diagnostic criteria of autoimmune pancreatitis: revised proposal. J Gastroenterol 2006; 41: Chari ST, Smyrk TC, Levy MJ, et al: Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol 2006; 4: Kim KP, Kim MH, Kim JC, Lee SS, Seo DW, Lee SK: Diagnostic criteria of autoimmune chronic pancreatitis revisited. World J Gastroenterol 2006; 12: Finkelberg DL, Sahani D, Deshpande V, Brugge WR: Autoimmune pancreatitis. N Engl J Med 2006; 355: Sarles H, Sarles JC, Muratoren R, Guien C: Chronic inflammatory sclerosis of the pancreas--an autonomous pancreatic disease? Am J Dig Dis 1961; 6: Kawaguchi K, Koike M, Tsuruta K, Okamoto A, Tabata I, Fujita N: Lymphoplasmacytic sclerosing pancreatitis with cholangitis: a variant of primary sclerosing cholangitis extensively involving pancreas. Hum Pathol 1991; 22:
8 년도대한췌담도학회추계학술대회 12. Sood S, Fossard DP, Shorrock K: Chronic sclerosing pancreatitis in Sjogren's syndrome: a case report. Pancreas 1995; 10: Chutaputti A, Burrell MI, Boyer JL: Pseudotumor of the pancreas associated with retroperitoneal fibrosis: a dramatic response to corticosteroid therapy. Am J Gastroenterol 1995; 90: Ito T, Nakano I, Koyanagi S, Miyahara T, Migita Y, Ogoshi K, Sakai H, Matsunaga S, Yasuda O, Sumii T, Nawata H: Autoimmune pancreatitis as a new clinical entity. Three cases of autoimmune pancreatitis with effective steroid therapy. Dig Dis Sci 1997; 42: Irie H, Honda H, Baba S, Kuroiwa T, Yoshimitsu K, Tajima T, Jimi M, Sumii T, Masuda K: Autoimmune pancreatitis: CT and MR characteristics. AJR Am J Roentgenol 1998; 170: Ectors N, Maillet B, Aerts R, et al: Non-alcoholic duct destructive chronic pancreatitis. Gut 1997; 41: Van Hoe L, Gryspeerdt S, Ectors N: Non-alcoholic duct-destructive chronic pancreatitis: imaging findings. Am J Roentgenol 1998; 170: Eerens I, Vanbeckevoort D, Vansteenbergen W, et al: Autoimmune pancreatitis associated with primary sclerosing cholangitis: MR imaging findings. Eur Radiol 2001; 11: Okazaki K, Uchida K, Ohana M, Nakase H, Uose S, Inai M, Matsushima Y, Katamura K, Ohmori K, Chiba T: Autoimmune-related pancreatitis is associated with autoantibodies and a Th1/Th2-type cellular immune response. Gastroenterology 2000; 118: Hamano H, Kawa S, Horiuchi A, et al: High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 2001; 344: Etemad B, WhitcombDC: Chronic pancreatitis: diagnosis, classification and new genetic developments. Gastroenterology 2001; 120: Yadav D, Notahara K, Smyrk TC, et al: Idiopathic tumefactive chronic pancreatitis: clinical profile, histology, and natural history after resection. Clin Gastroenterol Hepatol 2003; 1: Weber SM, Cubukcu-Dimopulo O, Palesty JA, et al: Lymphoplasmacytic sclerosing pancreatitis: inflammatory mimic of pancreatic carcinoma. J Gastrointest Surg 2003; 7: Abraham SC, Wilentz RE, Yeo CJ, et al: Pancreaticoduodenectomy (Whipple resections) in patients without malignancy: are they all 'chronic pancreatitis'? Am J Surg Pathol 2003; 27: Notohara K, Burgart L J, Yadav D, et al: Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am J Surg Pathol 2003; 27: Kloppel G, Luttges J, Lohr M, et al: Autoimmune pancreatitis: pathological, clinical, and immunological features. Pancreas 2003; 27: Kamisawa T, Funata N, Hayashi Y, et al: Close relationship between autoimmune pancreatitis and multifocal fibrosclerosis. Gut 2003; 52: Kamisawa T and Okamoto A: Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J Gastroenterol 2006; 41: Bjornsson E, Chari ST, Smyrk TC, Lindor K: Immunoglobulin G4 associated cholangitis: description of an emerging clinical entity based on review of the literature. Hepatology 2007; 45: Aparisi L, Farre A, Gomez-Cambronero, et al: Antibodies to carbonic anhydrase and IgG4 levels in idiopathic chronic pancreatitis: relevance for diagnosis of autoimmune pancreatitis. Gut 2005; 54: Nakazawa T, Ohara H, Sano H, Ando T, Imai H, Takada H, Hayashi K, Kitajima Y, Joh T: Difficulty in diagnosing autoimmune pancreatitis by imaging findings. Gastrointest Endosc 2007; 65: Levy MJ, Wiersema MJ, Chari ST: Chronic pancreatitis: focal pancreatitis or cancer? Is there a role for FNA/biopsy? Autoimmune pancreatitis. Endoscopy 2006; 38(Suppl 1): S30-35.
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Autoimmune Pancreatitis: Pathological Findings
 AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Pathological Findings Günter Klöppel 1, Jutta Lüttges 1, Bence Sipos 1, Paola Capelli 2, Giuseppe Zamboni 2
AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Pathological Findings Günter Klöppel 1, Jutta Lüttges 1, Bence Sipos 1, Paola Capelli 2, Giuseppe Zamboni 2
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid
 The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Autoimmune pancreatitis (AIP) is a chronic fibroinflammatory
 Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
Review Article Autoimmune Pancreatitis More Than Just a Pancreatic Disease? A Contemporary Review of Its Pathology Vikram Deshpande, MD; Mari Mino-Kenudson, MD; William Brugge, MD; Gregory Y. Lauwers,
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis: Case Series and Review of the Literature.
 Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones
 MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
EUS-FNA Contribution in the Identification of Autoimmune Pancreatitis: A Case Report
 CASE REPORT EUS-FNA Contribution in the Identification of Autoimmune Pancreatitis: A Case Report Charitini Salla 1, Paschalis Chatzipantelis 2, Panagiotis Konstantinou 1, Ioannis Karoumpalis 3, Akrivi
CASE REPORT EUS-FNA Contribution in the Identification of Autoimmune Pancreatitis: A Case Report Charitini Salla 1, Paschalis Chatzipantelis 2, Panagiotis Konstantinou 1, Ioannis Karoumpalis 3, Akrivi
Autoimmune pancreatitis / IgG4-associated cholangitis and primary sclerosing cholangitis Overlapping or separate diseases? q
 Journal of Hepatology 51 (2009) 398 402 Review Autoimmune pancreatitis / IgG4-associated cholangitis and primary sclerosing cholangitis Overlapping or separate diseases? q George J.M. Webster 1,2, *, Stephen
Journal of Hepatology 51 (2009) 398 402 Review Autoimmune pancreatitis / IgG4-associated cholangitis and primary sclerosing cholangitis Overlapping or separate diseases? q George J.M. Webster 1,2, *, Stephen
During the last decade, patients with steroid
 REVIEWS Immunoglobulin G4 Associated Cholangitis: Description of an Emerging Clinical Entity Based on Review of the Literature Einar Björnsson, 1 Suresh T. Chari, 2 Thomas C. Smyrk, 2 and Keith Lindor
REVIEWS Immunoglobulin G4 Associated Cholangitis: Description of an Emerging Clinical Entity Based on Review of the Literature Einar Björnsson, 1 Suresh T. Chari, 2 Thomas C. Smyrk, 2 and Keith Lindor
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features.
 'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term Follow-Up Study of 73 Japanese Patients
 International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
Autoimmune pancreatitis can transform into chronic features similar to advanced
 Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
University of Texas-MD Anderson Cancer Center, Houston, Texas, USA. University of Medicine and Pharmacy Craiova, Romania
 Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Case Report A Diagnostic Challenge: Pancreatic Cancer or Autoimmune Pancreatitis? IRINA MIHAELA CAZACU 1,2, ADRIANA ALEXANDRA LUZURIAGA CHAVEZ 1, ADRIAN SAFTOIU 2, TONYA G. WHITLOW 1, PRIYA BHOSALE 3,
Kazuichi Okazaki 1 and Hisanori Umehara Introduction. 2. The Concept of IgG4-Related Disease
 Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 357071, 9 pages doi:10.1155/2012/357071 Review Article Are Classification Criteria for IgG4-RD Now Possible?
Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 357071, 9 pages doi:10.1155/2012/357071 Review Article Are Classification Criteria for IgG4-RD Now Possible?
Immunoglobulin G4 (IgG4)-related disease, a systemic,
 IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Autoimmune pancreatitis characterized by predominant CD8+ T lymphocyte infiltration
 Online Submissions: http://www.wjgnet.com/17-9327office wjg@wjgnet.com doi:1.3748/wjg.v17.i41.4635 World J Gastroenterol 11 November 7; 17(41): 4635-4639 ISSN 17-9327 (print) ISSN 2219-28 (online) 11 Baishideng.
Online Submissions: http://www.wjgnet.com/17-9327office wjg@wjgnet.com doi:1.3748/wjg.v17.i41.4635 World J Gastroenterol 11 November 7; 17(41): 4635-4639 ISSN 17-9327 (print) ISSN 2219-28 (online) 11 Baishideng.
IgG4 cholangitis Case Report: Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam.
 IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Autoimmune Pancreatitis: Instrumental Diagnosis
 AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Instrumental Diagnosis Giovanni Morana 1, Margherita Tapparelli 2, Niccolò Faccioli 2, Mirko D Onofrio 2, Roberto
AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Instrumental Diagnosis Giovanni Morana 1, Margherita Tapparelli 2, Niccolò Faccioli 2, Mirko D Onofrio 2, Roberto
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Hideaki Miura, Yasutaka Miyachi. Department of Internal Medicine, Social Insurance Central General Hospital. Tokyo, Japan
 CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CHRONIC PANCREATITIS OR DUCTAL ADENOCARCINOMA? N. Volkan Adsay, \ MD
 CHRONIC PANCREATITIS OR DUCTAL ADENOCARCINOMA? N. Volkan Adsay, \ MD Case for discussion 67 y/o male Back pain and weight loss CT: 4.5 cm ill-defined, solid lesion in the head FNA/Core bx: Inconclusive
CHRONIC PANCREATITIS OR DUCTAL ADENOCARCINOMA? N. Volkan Adsay, \ MD Case for discussion 67 y/o male Back pain and weight loss CT: 4.5 cm ill-defined, solid lesion in the head FNA/Core bx: Inconclusive
Review Article From Pathogenesis, Clinical Manifestation, and Diagnosis to Treatment: An Overview on Autoimmune Pancreatitis
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3246459, 11 pages https://doi.org/10.1155/2017/3246459 Review Article From Pathogenesis, Clinical Manifestation, and Diagnosis to
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3246459, 11 pages https://doi.org/10.1155/2017/3246459 Review Article From Pathogenesis, Clinical Manifestation, and Diagnosis to
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Cerebral involvement in IgG4-related disease
 ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer
 What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer 9 Th Annual Symposium on Gastrointestinal Cancers, St. Louis University School of Medicine Carlos
What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer 9 Th Annual Symposium on Gastrointestinal Cancers, St. Louis University School of Medicine Carlos
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids. Cholestasis
 Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Autoimmune Liver Diseases
 2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
NEW-ONSET JAUNDICE IN A PATIENT WITH HISTORY OF RETROPERITONEAL FIBROSIS, A CASE REPORT
 Acta Medica Mediterranea, 2015, 31: 1099 NEW-ONSET JAUNDICE IN A PATIENT WITH HISTORY OF RETROPERITONEAL FIBROSIS, A CASE REPORT PIETRO VALERIO FOTI 1, GIANCARLO ATTINÀ 1, GIUSEPPINA CAPPELLO 1, STEFANO
Acta Medica Mediterranea, 2015, 31: 1099 NEW-ONSET JAUNDICE IN A PATIENT WITH HISTORY OF RETROPERITONEAL FIBROSIS, A CASE REPORT PIETRO VALERIO FOTI 1, GIANCARLO ATTINÀ 1, GIUSEPPINA CAPPELLO 1, STEFANO
A Case of IgG4-Related Disease Presenting as Massive Pleural Effusion and Thrombophlebitis
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.76.4.179 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;76:179-183 A Case of IgG4-Related Disease Presenting as Massive Pleural Effusion
CASE REPORT http://dx.doi.org/10.4046/trd.2014.76.4.179 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;76:179-183 A Case of IgG4-Related Disease Presenting as Massive Pleural Effusion
Ornela Dervishaj, Harish Lavu, Charles J Yeo, Agnieszka K Witkiewicz ABSTRACT INTRODUCTION ********* *********
 CASE REPORT 1 OPEN ACCESS The quandary autoimmune pancreatitis and pancreatic ductal adenocarcinoma: A case report and review IgG4 immunostaining in a cohort patients receiving neoadjuvant chemotherapy
CASE REPORT 1 OPEN ACCESS The quandary autoimmune pancreatitis and pancreatic ductal adenocarcinoma: A case report and review IgG4 immunostaining in a cohort patients receiving neoadjuvant chemotherapy
IgG4 ᛶ ᝈ䛸 ᶫᮏ ᕫච ᛶ ⅖ ḷᒣ Ꮫ య Ꮫ ぬ㐨
 IgG4 Autoimmune pancreatitis Histopathological features: Diffuse lymphoplasmacytic infiltration Stromal fibrosis Acinar atrophy Obliterative phlebitis 1. Hamano et al reported that serum IgG4 levels were
IgG4 Autoimmune pancreatitis Histopathological features: Diffuse lymphoplasmacytic infiltration Stromal fibrosis Acinar atrophy Obliterative phlebitis 1. Hamano et al reported that serum IgG4 levels were
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
1. Introduction. needle aspiration (EUS/FNA), and serology testing is performed before the decision for surgery is made.
 Diagnostic and erapeutic Endoscopy, Article ID 701535, 6 pages http://dx.doi.org/10.1155/2014/701535 Research Article Increased Incidence of Benign Pancreatic Pathology following Pancreaticoduodenectomy
Diagnostic and erapeutic Endoscopy, Article ID 701535, 6 pages http://dx.doi.org/10.1155/2014/701535 Research Article Increased Incidence of Benign Pancreatic Pathology following Pancreaticoduodenectomy
Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune pancreatitis
 J Gastroenterol (2014) 49:961 970 DOI 10.1007/s00535-014-0945-z SPECIAL ARTICLE Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune
J Gastroenterol (2014) 49:961 970 DOI 10.1007/s00535-014-0945-z SPECIAL ARTICLE Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune
CME/SAM. Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin
 Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin Julia S. Lehman, MD, 1,2 Thomas C. Smyrk, MD, 1 and Mark R. Pittelkow,
Increased Immunoglobulin (Ig) G4 Positive Plasma Cell Density and IgG4/IgG Ratio Are Not Specific for IgG4- Related Disease in the Skin Julia S. Lehman, MD, 1,2 Thomas C. Smyrk, MD, 1 and Mark R. Pittelkow,
Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor
 International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases
 MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
IgG4-Related Disease: Dataset of 235 Consecutive Patients
 IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
A utoimmunity is considered an aetiological factor
 73 PANCREAS Antibodies to carbonic anhydrase and IgG4 levels in idiopathic chronic pancreatitis: relevance for diagnosis of autoimmune pancreatitis L Aparisi, A Farre, L Gomez-Cambronero, J Martinez, G
73 PANCREAS Antibodies to carbonic anhydrase and IgG4 levels in idiopathic chronic pancreatitis: relevance for diagnosis of autoimmune pancreatitis L Aparisi, A Farre, L Gomez-Cambronero, J Martinez, G
Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor
 ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
Diagnosis of IgG4-related sclerosing cholangitis
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i43.7661 World J Gastroenterol 2013 November 21; 19(43): 7661-7670 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i43.7661 World J Gastroenterol 2013 November 21; 19(43): 7661-7670 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
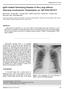 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Case Report IgG4-Related Nasal Pseudotumor
 Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
