Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
|
|
|
- Elmer Sanders
- 5 years ago
- Views:
Transcription
1 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn eissn 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis in Korea Jong Kyun Lee Division of Gastroenterology, Department of Internal Medicine, Sungkyunkwan University School of Medicine, Samsung Medical Center, Seoul, Korea Autoimmune pancreatitis should be differentiated from pancreatobiliary cancers because they often have similar clinical features and images. Accurate and practical diagnostic algorithm for AIP is important to avoid unnecessary surgery and delayed treatment. International Consensus Diagnostic Criteria for AIP suggested that diagnostic algorithms and the practical patterns considerably vary worldwide. Patients with clinically suspected AIP can be categorized into patients with typical features of AIP and patients with indeterminate features based on CT findings. Serology and other organ involvement can be used as collateral evidence of AIP. If a patient presents with diffuse pancreatic enlargement but is lack of collateral evidence, pancreatogram could be useful. If a patient has obstructive jaundice, biliary drainage and endobiliary biopsy are recommended. Duodenal papillary biopsy for IgG4 immunostain can be used during ERCP. In case of atypical imaging findings, EUS-guided FNA/biopsy is recommended to exclude pancreatic cancer and to obtain the suggestive findings of AIP. If type 2 is clinically suspected, EUS-guided core biopsy is required for the definite diagnosis. Short-term steroid trial can be performed to confirm the diagnosis of AIP when pancreatobiliary cancer workup shows negative results. However, clinical practice in diagnosing AIP varies depending on the local expertise, facilities, cost, prevalence of AIP and its subtypes. Korean J Pancreatobiliary 2014;19(1):7-12 Keywords: Autoimmune pancreatitis, International Consensus Diagnostic Criteria, Algorithm, IgG4 Received Revised Accepted Corresponding author : Jong Kyun Lee Division of Gastroenterology, Department of Internal Medicine, Sungkyunkwan University School of Medicine, Samsung Medical Center, 81 Irwon-ro, Gangnam-gu, Seoul , Korea Tel Fax ; jongk.lee@samsung.com This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( creativecommons.org / licenses/by-nc/3.0/ ) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright 2014 by The Korean Journal of Pancreas and Biliary Tract INTRODUCTION Autoimmune pancreatitis (AIP) is a rare systemic fibroinflammatory disease which can affect not only the pancreas but also a variety of organs such as the bile duct, salivary glands, kidney, prostate, lung, retroperitoneum and lymph nodes. This inflammatory process dramatically responds to steroid therapy. AIP should be differentiated from pancreatic and bile duct cancer because they often have similar clinical features and imaging findings such as pancreatic enlargement, mass formation and obstructive jaundice. Therefore, accurate and practical diagnostic algo- 7
2 Volume_19 Number_1 January 2014 rithm for AIP is important to avoid unnecessary surgery for AIP and delayed operation for pancreatobiliary malignancies. In 2011, International Consensus Diagnostic Criteria (ICDC) for AIP was introduced. 1 The concepts of typical type, indeterminate/atypical type and 5 cardinal features (radiologic images, serology, other organ involvement, histology and response to steroid) are generally agreed. Although ICDC suggested a diagnostic algorithm for AIP, clinical practice still considerably varies worldwide. 2-4 In particular, there is a discrepancy in the use of endoscopy for the diagnosis of AIP between Eastern and Western countries. Korean and Japanese doctors still use endoscopic retrograde cholangiopancreatography (ERCP) for the differentiation of AIP from pancreatic cancer (PC). However, Western doctors prefer magnetic resonance cholangiopancreatography (MRCP) to ERCP and frequently perform endoscopic ultrasonography (EUS)- guided core biopsy not only to diagnose AIP but also to differentiate two types of AIP. The difference in practice also depends on the fact whether pancreatologists themselves are endoscopists or not, facilities, cost of endoscopy, and prevalence of type 2 AIP. DIAGNOSTIC METHODS AND ALGORITHM Because symptoms and laboratory findings are nonspecific and similar between AIP and pancreatobiliary malignancies, cross-sectional images are first used for the differential diagnosis. Dynamic computed tomography (CT) provides many information including enhancement patterns, peripancreatic low density rim, ductal dilatation, surrounding lymph nodes and organs. CT features can be classified into typical of AIP, indeterminate features and typical of PC. There are many studies on the typical CT imaging features of AIP and PC. 3,5 Therefore, most diagnostic algorithms start from CT-based stratification. Highly suggestive findings for AIP are diffuse enlargement with delayed homogenous enhancement, capsule-like rim and lack of significant dilatation of upstream pancreatic duct. Highly suggestive findings for PC are non-enhanced mass with prominent dilatation of upstream pancreatic duct and the parenchymal atrophy. Magnetic resonance imaging (MRI) is also helpful to differentiate AIP from PC. However, imaging alone is not perfect to distinguish AIP from PC. In the following step for the diagnosis of AIP, ICDC recommended to check serology and the presence of other organ involvement (OOI). In serology, total serum immunoglobulin G (IgG), IgG4 and autoantibodies have been used for the diagnosis of AIP. If total serum IgG is included in diagnostic criteria, the sensitivity increases but specificity can be sacrificed. ICDC included only IgG4 as a serologic marker of AIP to exclude the false positivity in pancreatic cancer and other diseases. Serum IgG4 ( 135 mg/ dl) is the most sensitive (52-80%) and specific (93-99%) serologic marker for the diagnosis of AIP. 6-8 Serum IgG4 may be mildly elevated in 5-10% of pancreatic cancer. Serum IgG level ( 1,800 mg/dl) is less sensitive (43-70%) and less specific (88-93%). ICDC divided the serologic criterion into level 1 and level 2; level 1 if serum IgG4 level is higher than two times the upper limit of normal and level 2 if it is lower than two times the upper limit of normal. When the cut-off value of serum IgG4 is raised to two times the upper limit of normal, the specificity improves to % but the sensitivity decreases to 34-50%. Level 1 of serum IgG4 is not necessarily sufficient to exclude pancreatic cancer. A variety of extrapancreatic lesions have been noted in patients with AIP including bile duct, lachrymal and salivary glands, retroperitoneum, thyroid, kidney and prostate. The presence of extrapancreatic involvement could be used for the collateral evidence of AIP. ICDC stratified the level of OOI. Sclerosing cholangitis, retroperitoneal fibrosis or 8 The Korean Journal of Pancreas and Biliary Tract
3 JK Lee, et al. Diagnostic Algorithm for Autoimmune Pancreatitis in Korea strong histologic evidence of other organs are included in level 1 criterion. Salivary/lacrimal glands and renal involvement are included in level 2. However, it is unclear why Mikulicz s disease and renal involvement are classified as level 2 OOI. Mediastinal or hilar lymphadenopathies and intrapancreatic bile duct strictures are not specific to AIP. 9 ICDC also recommended ampullary biopsy as collateral evidence if there is insufficient evidence of OOI and serology. Ampullary biopsy with IgG4 immunostain (more than 10 IgG4-positive cells per high power field) has a sensitivity of 52% to 89% and specificity of 89% to 100% It is a simple and safe adjunctive method to get collateral evidences of AIP. However, ampullary biopsy can be performed at the same time during ERCP. Pancreatogram is important to differentiate AIP from pancreatic cancer Four ERP features are highly specific to AIP; long (>1/3 of the length of main pancreatic duct) narrow stricture, a lack of upstream dilatation from the stricture (<5 mm), multiple strictures, side branches arising from the stricture site. 16 Highly suggestive findings for PC are cut-off of pancreatic duct or prominent dilatation of upstream pancreatic duct. ERCP also provides endobiliary biopsy and biliary drainage in patients with obstructive jaundice. ERCP is helpful to diagnose AIP with atypical CT findings but has little added benefits in patients with typical CT findings. Western endoscopists generally avoid ERCP to diagnose AIP due to the fear of post-ercp pancreatitis. However, post- ERCP pancreatitis is rare and mild in patients with AIP because AIP is a kind of chronic pancreatitis in which post-ercp pancreatitis develops less frequently due to fibrosis and decreased enzymatic activity.that Magnetic resonance cholangiopancreatography (MRCP) is a noninvasive alternative method to evaluate pancreatic ducts. It can be used to support the diagnosis of AIP. However, it could not reveal the narrowed portion of the main pancreatic duct and sometimes inadequate to differentiate massforming AIP from PC. MRCP cannot entirely replace ERCP. 17 Accuracy of MRCP in depicting the main pancreatic duct morphology of AIP is moderate (65-69%). 18,19 Multiple narrowing or skipped pancreatic duct and absence of upstream ductal dilatation suggest AIP. Therefore, MRCP may be useful in patients with diffuse pancreatic enlargement without other collateral evidence and jaundice. MRCP is also useful to evaluate treatment response in AIP. Positron emission tomography shows increased uptake of fluorodeoxyglucose in both AIP and PC. The pattern of fluorodeoxyglucose uptake in PC is nodular, homogenous and solitary whereas the uptake in AIP is longitudinal, heterogenous and multiple in the pancreas and extrapancreatic sites including salivary glands, bile duct, retropreitoneum and kidney However, routine use of positron emission tomography is not recommended because of the high cost and high dose of radiation exposure. In some case of AIP, the diagnosis can be only made by resected tissue or biopsy specimen. According to ICDC, AIP is classified into 2 subtypes: type 1 is related with IgG4 (lymphoplasmacytic sclerosing pancreatitis, LPSP) and type 2 is related with granulocytic epithelial lesion (idiopathic duct centric pancreatitis, IDCP). 23 These two types were identified by pathologic studies of resected pancreases misdiagnosed with pancreatic cancer. While IDCP patients account for at least one-third of all AIP patients in Europe and the USA, they are still rare in Korea and Japan. Because patients with type 2 AIP are unlikely to have OOI and do not have serologic markers, type 2 can be definitely diagnosed only by histologic examination. Normal s-igg4 level and absence of OOI do not necessarily mean type 2 AIP. Indeed, type 1 AIP with normal serum IgG4 and absence of OOI is more probable than type 2 AIP in Korea. Histologic diagnosis could be achieved by endoscopic ultrasound (EUS)-guided core biopsy but it is technically difficult, especially in pancreatic head lesion. 24 In addition, sampling error may occur as the pancreas is not uniformly involved. 9
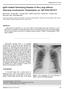
4 Volume_19 Number_1 January 2014 Therefore, it is challenging to make a definite diagnosis of AIP and perform typing with small biopsy specimen. For this reason, correlation with other clinical and radiologic features is necessary. 25,26 Also, some features of type 1 could be seen in type 2 AIP and GEL could be seen in 27% of type 1 AIP. Instead, EUS-guided fine needle aspiration may show suggestive findings of AIP such as lymphoplasmacytic infiltration and many IgG4-positive plasma cells or inconclusive results. Because some features of LPSP and IDCP can be also seen in pancreatic cancer, we have to be careful. Nevertheless, EUS-FNA has an important role for the exclusion of PC in atypical cases because it provides a sensitivity of 80-90% and specificity of % for the diagnosis of PC. 12 Recently, fine needle aspiration biopsy is available and easier to be performed than trucut core biopsy at pancreatic head lesion. 27 We also need to keep in mind that PC is about 100 times more prevalence than AIP. Therefore, EUS-guided FNA/biopsy is recommended in all patients with focal mass-forming pancreatitis to exclude malignancy. In patients with appropriate collateral evidence of AIP, steroid trial can be used to assist in making the diagnosis when it is used appropriately. Steroid trial should not be abused and must be performed only when workup results for pancreatobiliary malignancies are negative. Objective improvement of the pancreatic parenchymal and ductal images should be evident within 2 to 4 weeks. Improvement of symptoms, laboratory findings, tumor markers Fig. 1. Algorithm for the diagnosis of autoimmune pancreatitis (AIP) in Korea. OOI; other organ involvement, LPSP; lymphoplasmacytic sclerosing pancreatitis, IDCP; idiopathic duct-centric pancreatitis, MPD; main pancreatic duct. 10 The Korean Journal of Pancreas and Biliary Tract
5 JK Lee, et al. Diagnostic Algorithm for Autoimmune Pancreatitis in Korea and serum IgG4 level should not be used to assess response to steroids. CONCLUSIONS Diagnostic algorithm for AIP can be different according to countries, institutions and physicians. Figure 1 is my suggestion of practical algorithm for Korean population. Patients with clinically suspected AIP can be first categorized into patients with typical features of AIP, patients with indeterminate CT features and patients with typical features of PC based on the CT findings. Then, serology and other organ involvement can be used as collateral evidence of AIP. If a patient has diffusely enlarged pancreas but lacks of collateral evidence, pancreatogram by ERCP or MRCP can be performed. If a patient has obstructive jaundice, biliary drainage and endobiliary biopsy are recommended. Duodenal papillary biopsy for IgG4 immunostain can be used at the same time during ERCP. If a patient shows atypical imaging, EUS-guided FNA/biopsy is recommended to exclude pancreatic cancer and could obtain the suggestive findings of AIP. If type 2 AIP is clinically suspected, EUS-guided core biopsy is required for the definite diagnosis. Short-term steroid trial can be performed to confirm the diagnosis of AIP when workup results for pancreatobiliary cancer are negative. 국문색인 : 자가면역췌장염, 진단전략, 면역글로불린 G4 Conflicts of Interest The author has no conflicts to disclose. REFERENCES 1. Shimosegawa T, Chari ST, Frulloni L, et al. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas. 2011;40: Agrawal S, Daruwala C, Khurana J. Distinguishing autoimmune pancreatitis from pancreaticobiliary cancers: current strategy. Ann Surg. 2012;255: Kamisawa T, Imai M, Yui Chen P, et al. Strategy for differentiating autoimmune pancreatitis from pancreatic cancer. Pancreas 2008;37:e62- e67 4. Frulloni L, Amodio A, Katsotourchi AM.A practical approach to the diagnosis of anutoimmune pancreatitis. World J Gastroenterol 2011;28: Chang WI, Kim BJ, Lee JK, et al. The clinical and radiological characteristics of focal mass-forming autoimmune pancreatitis: comparison with chronic pancreatitis and pancreatic cancer. Pancreas 2009;38: Sah RP, Chari ST. Serologic issues in IgG4-related systemic disease and autoimmune pancreatitis. Curr Opin Rheumatol 2011;23: Song TJ, Kim MH, Moon SH, et al. The combined measurement of total serum IgG and IgG4 may increase diagnostic sensitivity for autoimmune pancreatitis without sacrificing specificity, compared with IgG4 alone. Am J Gastroenterol. 2010;105: Yoon H, Kim MH, Won SH, et al. A Comparative Study on Serum Immunoglobulin and Tumor Marker Levels in the Patients with Autoimmune Pancreatitis and Pancreatobiliary Malignancies. Korean J Gastroenterol 2013;61: Naitoh I, Nakazawa T, Hayashi K, et al. Clinical differences between mass-forming autoimmune pancreatitis and pancreatic cancer. Scan J Gastroenterol 2012;47: Kamisawa T, Tu Y, Nakajima H, Egawa N, Tsuruta K, Okamoto A. Usefulness of biopsying the major papilla to diagnose autoimmune pancreatitis: A prospective study using IgG4-immunostaining. World J Gastroenterl 2006;12: Moon SH, Kim MH, Park do H, et al. IgG4 immunostaining of duodenal papillary biopsy specimens may be useful for supporting a diagnosis of autoimmune pancreatitis. Gastrointest Endosc 2010;71: Moon SH, Kim MH. The role of endoscopy in the diagnosis of autoimmune pancreatitis. Gastrointest Endosc 2012;76: Horiuchi A, Kawa S, Hamano H, et al. ERCP features in 27 patients with autoimmune pancreatitis. Gastrointest Endosc 2002;55: Nishino T, Oyama H, Toki F, Shiratori K. Differentiation between autoimmune pancreatitis and pancreatic carcinoma based on endoscopic retrograde cholangiopancreatography findings. J Gastroenterol 2010;45: Kim JH, Kim MH, Byun JH, et al. Diagnostic Strategy for Differentiating Autoimmune Pancreatitis From Pancreatic Cancer: Is an Endoscopic Retrograde Pancreatography Essential? Pancreas Jan 5. [Epub ahead of print]. 16. Sugumar A, Levy MJ, Kamisawa T, wt al. Endoscopic Retrograde Pancreatography criteria to diagnose autoimmune pancreatitis: an 11
6 Volume_19 Number_1 January 2014 international multicenter study. Gut 2011;60: Kamisawa T, Tu Y, Egawa N, et al. Can MRCP replace ERCP for the diagnosis of autoimmune pancreatitis? Abdom Imaging 2009;34: Takuma K, Kamisawa T, Tabata T, Inaba Y, Egawa N, Igarashi Y. Utility of pancreatography for diagnosing autoimmune pancreatitis. World J Gastroenterol 2011;17: Park SH, Kim MH, Kim SY, et al. Magnetic resonance cholangiopancreatography for the diagnostic evaluation of autoimmune pancreatitis. Pancreas 2012;39: Sato M, Okumura T, Shioyama Y, Imura J. Extrapancreatic F-18 FDG accumulation in autoimmune pancreatitis. Ann Nucl Med 2008;22: Ozaki Y, Oguchi K, Hamano H, et al. Differentiation of autoimmune pancreatitis from suspected pancreatic cancer by fluorine-18 fluorodeoxyglucose positron emission tomography. J Gastroenterol 2008;43: Lee TY, Kim MH, Park do H, et al. Utility of 18F-FDG PET/CT for differentiation of autoimmune pancreatitis with atypical pancreatic imaging findings from pancreatic cancer. AJR Am J Roentgenol 2009;193: Zhang L, Chari S, Smyrk TC, et al. Autoimmune pancreatitis (AIP) type 1 and type 2: an international consensus study on histopathologic diagnostic criteria. Pancreas 2011;40: Levy MJ, Wiersema MJ, Chari ST. Chronic pancreatitis: Focal pancreatitis or cancer? Is there a role for FNA/biopsy? Autoimmune pancreatitis. Endoscopy 2006;38:S30-S Mizuno N, Bhatia V, Hosoda W, et al. Histological diagnosis of autoimmune pancreatitis using EUS-guided trucut biopsy: a comparison study with EUS-FNA. J Gastroenterol 2009;44: Hirano K, Fukushima N, Tada M, Diagnostic utility of biopsy specimens for autoimmune pancreatitis. J Gastroenterol 2009;44: Larghi A, Iglesias-Garcia J, Poley JW, et al. Feasibility and yield of a novel 22-gauge histology EUS needle in patients with pancreatic masses: a multicenter prospective cohort study. Surg Endosc 2013;27: The Korean Journal of Pancreas and Biliary Tract
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
autoimmune pancreatitis from pancreatic cancer
 Zhang et al. BMC Cancer (2017) 17:695 DOI 10.1186/s12885-017-3665-y RESEARCH ARTICLE Open Access 18 F- FDG PET/CT helps differentiate autoimmune pancreatitis from pancreatic cancer Jian Zhang 1,2, Guorong
Zhang et al. BMC Cancer (2017) 17:695 DOI 10.1186/s12885-017-3665-y RESEARCH ARTICLE Open Access 18 F- FDG PET/CT helps differentiate autoimmune pancreatitis from pancreatic cancer Jian Zhang 1,2, Guorong
Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:316 322 Use of Samples From Endoscopic Ultrasound Guided 19-Gauge Fine- Needle Aspiration in Diagnosis of Autoimmune Pancreatitis TAKUJI IWASHITA,* ICHIRO
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term Follow-Up Study of 73 Japanese Patients
 International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up
 CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones
 MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Title: Painless jaundice as an initial presentation of lung adenocarcinoma
 Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
ENDOSCOPY IN COMPETITION DIAGNOSTICS. Dr. med. Dirk Hartmann Klinikum Ludwigshafen
 Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Falk Symposium 166 GI Endoscopy Standards and Innovations Mainz, 18. 19. September 2008 ENDOSCOPY IN COMPETITION DIAGNOSTICS Dr. med. Dirk Hartmann Klinikum Ludwigshafen ENDOSCOPY IN COMPETITION Competing
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
Review Article Imaging of Focal Autoimmune Pancreatitis and Differentiating It from Pancreatic Cancer
 Hindawi Publishing Corporation ISRN Radiology Volume 2013, Article ID 569489, 8 pages http://dx.doi.org/10.5402/2013/569489 Review Article Imaging of Focal Autoimmune Pancreatitis and Differentiating It
Hindawi Publishing Corporation ISRN Radiology Volume 2013, Article ID 569489, 8 pages http://dx.doi.org/10.5402/2013/569489 Review Article Imaging of Focal Autoimmune Pancreatitis and Differentiating It
Incidence of Malignancies in Patients with IgG4-related Disease
 ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE
 ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori
 Gut and Liver, Vol. 6, No. 2, April 2012, pp. 270-274 CASE REPORT Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori Soo-Kyung Park, Hwoon-Yong Jung, Do Hoon Kim,
Gut and Liver, Vol. 6, No. 2, April 2012, pp. 270-274 CASE REPORT Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori Soo-Kyung Park, Hwoon-Yong Jung, Do Hoon Kim,
Contrast-Enhanced Endoscopic Ultrasound for Differentially Diagnosing Autoimmune Pancreatitis and Pancreatic Cancer
 Gut and Liver, Vol. 12, No. 5, September 2018, pp. 591-596 ORiginal Article Contrast-Enhanced Endoscopic Ultrasound for Differentially Diagnosing Autoimmune Pancreatitis and Pancreatic Cancer Min Keun
Gut and Liver, Vol. 12, No. 5, September 2018, pp. 591-596 ORiginal Article Contrast-Enhanced Endoscopic Ultrasound for Differentially Diagnosing Autoimmune Pancreatitis and Pancreatic Cancer Min Keun
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Evidence based imaging of the pancreas
 Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
CURRICULUM VITAE
 CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Title. CitationHepato-Gastroenterology, 61(135): Issue Date Doc URL. Type. File Information. IgG4-Related Sclerosing Cholangitis
 Title Difference from Bile Duct Cancer and Relationship be IgG4-Related Sclerosing Cholangitis Kuwatani, Masaki; Kawakami, Hiroshi; Zen, Yoh; Kawak Author(s) Sakamoto, Naoya CitationHepato-Gastroenterology,
Title Difference from Bile Duct Cancer and Relationship be IgG4-Related Sclerosing Cholangitis Kuwatani, Masaki; Kawakami, Hiroshi; Zen, Yoh; Kawak Author(s) Sakamoto, Naoya CitationHepato-Gastroenterology,
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid
 The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
Diagnosis of autoimmune pancreatitis
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i44.16559 World J Gastroenterol 2014 vember 28; 20(44): 16559-16569 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i44.16559 World J Gastroenterol 2014 vember 28; 20(44): 16559-16569 ISSN 1007-9327
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features.
 'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
'I GO FOR' (IG4) Autoimmune pancreatitis (AIP) and extrapancreatic imaging features. Poster No.: C-2649 Congress: ECR 2013 Type: Educational Exhibit Authors: R. P. Patel, T. M. Chandler, S. Barrett, J.
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Autoimmune pancreatitis can transform into chronic features similar to advanced
 Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Evaluation and Management of Refractory Biliary Stricture. J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc.
 Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases
 MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Magnetic resonance cholangiopancreatography (MRCP) is an imaging. technique that is able to non-invasively assess bile and pancreatic ducts,
 SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
Frank Burton Memorial Update on Pancreato-biliary Cancers
 Frank Burton Memorial Update on Pancreato-biliary Cancers Diagnosis and management of pancreatic cancer: common dilemmas Moderators: Banke Agarwal, MD Paul Buse, MD Evaluation of patients with obstructive
Frank Burton Memorial Update on Pancreato-biliary Cancers Diagnosis and management of pancreatic cancer: common dilemmas Moderators: Banke Agarwal, MD Paul Buse, MD Evaluation of patients with obstructive
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer
 What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer 9 Th Annual Symposium on Gastrointestinal Cancers, St. Louis University School of Medicine Carlos
What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer 9 Th Annual Symposium on Gastrointestinal Cancers, St. Louis University School of Medicine Carlos
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
CASE REPORT. Introduction
 doi: 10.2169/internalmedicine.9818-17 Intern Med Advance Publication http://internmed.jp CASE REPORT Autoimmune Hemolytic Anemia Obscured by the Obstructive Jaundice Associated with IgG4-related Sclerosing
doi: 10.2169/internalmedicine.9818-17 Intern Med Advance Publication http://internmed.jp CASE REPORT Autoimmune Hemolytic Anemia Obscured by the Obstructive Jaundice Associated with IgG4-related Sclerosing
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
A Case of Pancreatic Carcinoma with Bilateral Hilar
 Shinshu Med J, 66⑵:151~155, 2018 A Case of Pancreatic Carcinoma with Bilateral Hilar 18 F-FDG and 67 Ga Hyperaccumulation Satoshi Kawakami 1 )*, Yasunari Fujinaga 1), Shin Yanagisawa 1) Masumi Kadoya 1),
Shinshu Med J, 66⑵:151~155, 2018 A Case of Pancreatic Carcinoma with Bilateral Hilar 18 F-FDG and 67 Ga Hyperaccumulation Satoshi Kawakami 1 )*, Yasunari Fujinaga 1), Shin Yanagisawa 1) Masumi Kadoya 1),
Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected Pancreatic Cancer
 Gastroenterology Research and Practice Volume 2010, Article ID 268290, 4 pages doi:10.1155/2010/268290 Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected
Gastroenterology Research and Practice Volume 2010, Article ID 268290, 4 pages doi:10.1155/2010/268290 Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Imaging Guided Biopsy. Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer
 Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Pancreatic Cancer Masquerading as Pancreatitis
 Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
Pancreatic Cancer Masquerading as Pancreatitis Poster No.: C-2553 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Cahalane, Y. M. Purcell, L. Lavelle, E. R. Ryan, S. Skehan ; 1 1 2 2 2 2 2 Dublin,
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Acute Pancreatitis. Case: NG. Idiopathic Pancreatitis is Common. Investigation and Management of Idiopathic Acute Recurrent Pancreatitis (IARP)
 BRIGHAM AND WOMENS HOSPITAL Investigation and Management of (IARP) Acute Pancreatitis j Darwin L. Conwell MD, MS Associate Professor of Medicine Harvard Medical School Boston, MA Case: NG 54 year old female
BRIGHAM AND WOMENS HOSPITAL Investigation and Management of (IARP) Acute Pancreatitis j Darwin L. Conwell MD, MS Associate Professor of Medicine Harvard Medical School Boston, MA Case: NG 54 year old female
