Perioperative care of children with inherited metabolic disorders
|
|
|
- Lorraine Arnold
- 5 years ago
- Views:
Transcription
1 Perioperative care of children with inherited metabolic disorders Grant Stuart FRCA Nargis Ahmad FRCA Matrix reference 2D02 Key points Although individually rare, collectively metabolic disorders are common, with a reported incidence of 1:800 to 1:5000 births. Advances in paediatric care have resulted in many children with metabolic disease surviving into adulthood. A wide phenotypic spectrum exists between individuals with the same metabolic disorder because levels of enzyme activity may vary altering the severity and timing of presentation. Elective surgery for these patients should always be undertaken in specialist centres with the involvement of multidisciplinary teams and with intensive care facilities available if required. Glucose replacement should be commenced at the start of the nil by mouth period to avoid the metabolic decompensation associated with starvation in many metabolic disorders. Grant Stuart FRCA Specialist Registrar in Anaesthesia Great Ormond Street Hospital Great Ormond Street London WC1N 3JH UK Nargis Ahmad FRCA Consultant Anaesthetist Great Ormond Street Hospital Great Ormond Street London WC1N 3JH UK Tel: þ Fax: þ ahmadn@gosh.nhs.uk (for correspondence) 62 The expression inborn error of metabolism was coined to describe disorders resulting from the failure of a step or steps within a metabolic pathway. The number and complexity of metabolic processes required to maintain homeostasis is vast and so it follows that the spectrum of human disorders ascribed to inherited defects in metabolism is considerable. 1 Although some of these conditions do not have much impact on the perioperative management plan, others such as the mucopolysaccharidoses (MPS) represent some of the most challenging patients who an anaesthetist is likely to encounter. This short article does not provide comprehensive details of all inherited metabolic disorders (IMDs) but aims to provide the reader with a concise description of some of these rare conditions and highlight some of the key principles of perioperative management. IMDs are a genetically heterogenous group and may present at any age. Inheritance is often autosomal but this is not invariable. Many conditions are extremely rare and reports of experience of anaesthesia in the literature are limited. An overview of some of the commoner IMDs is presented in Table 1. 2 Pathophysiology of IMDs Inherited metabolic diseases are caused by genetic deficiencies resulting in the absence or dysfunction of structural proteins or enzymes within a metabolic pathway. Symptoms and signs may be related to the accumulation of intermediate metabolites proximal to the blocked enzyme that may be toxic or inappropriately stored within cells resulting in their destruction, and/or to the deficiency of a metabolite downstream of the blocked enzyme. 1 Accumulation of substrate Examples include Hurler s disease where a deficient enzyme leads to glycosaminoglycan accumulation within cellular lysosomes. This multisystemic tissue deposition results in coarse facial features, airway abnormalities, organomegaly, cardiovascular impairment, joint and bony deformities, and visual, auditory, and intellectual deficits. In many urea cycle defects, the accumulation of ammonia results in an acute encephalopathy. In methylmalonic acidaemia (MMA), the accumulation of methylmalonic acid causes metabolic acidosis. 1 Accumulation of a normally minor metabolite A minor metabolite of galactose, when produced in excess, leads to cataract formation in patients with galactosaemia. 1 Deficiency of product There are several potential mechanisms, for example, the absence of an important product of metabolism such as arginine in some of the urea cycle defects may further exacerbate the accumulation of ammonia and encephalopathy. In glycogen storage diseases (GSD), glycogen breakdown is impaired and attempts to maintain glucose homeostasis can result in muscle degradation as amino acids are used as an alternative substrate. In defects of fatty acid metabolism, lack of availability of the products of fatty acid oxidation promotes over utilization of glucose leading to hypoglycaemia. 1 Secondary effects Many enzymatic processes indirectly influence one another and hence affect processes that may appear discrete biochemical pathways. In MMA, a secondary inhibitory influence of methylmalonic acid occurs on carbamylphosphate synthetase, an enzyme of the urea cycle, which can lead to hyperammonaemic encephalopathy. 2 doi: /bjaceaccp/mkq055 Advance Access publication 22 December, 2010 Continuing Education in Anaesthesia, Critical Care & Pain Volume 11 Number & The Author [2010]. Published by Oxford University Press on behalf of the British Journal of Anaesthesia. All rights reserved. For Permissions, please journals.permissions@oup.com
2 Table 1 Overview of inherited metabolic diseases Metabolic classification of inherited disorders Clinical examples, inheritance pattern, and incidence Clinical features Disorders of amino acid metabolism Disorders of branched-chain amino acid metabolism The urea cycle disorders The organic acidaemias Disorders of carbohydrate metabolism Lysosomal storage diseases Disorders of fatty acid oxidation Phenylketonuria (autosomal, 1: ) Homocystinuria (autosomal, 1: ) Maple syrup urine disease (autosomal, 1: ) Ornithine transcarbamylase deficiency (X-linked dominant, 1:80 000) 4 other urea cycle defects are autosomal Propionic acidaemia (autosomal, 1: ) Methylmalonic acidaemia (autosomal, 1:48 000) Galactosaemia (autosomal, 1:60 000) Mental retardation and seizures Marfanoid phenotype, neurodevelopmental delay, high risk of thromboembolism, and cardiovascular disease Hypotonia, hypoglycaemia, ketoacidosis, seizures, coma, sweet smell of urine Neonatal hyperammonaemic encephalopathy, seizures, coma. Ataxia and behavioural abnormalities in older children Similar in both: tachypnoea, lethargy, vomiting, dehydration, metabolic acidosis, hypoglycaemia, ketoacidosis, neutropaenia, hyperammonaemia, encephalopathy Jaundice, hepatomegaly, hypoglycaemia, seizures, Escherichia coli sepsis, cirrhosis, mental retardation Glycogen storage diseases See Table 2 Lipidoses (Tay-Sachs, Gaucher, Niemann Pick, Lysosomal accumulation of specific sphingolipid substrates, chronic presentation, Fabry, Krabbe disease) hepatomegaly, developmental delay Mucopolysaccharidoses See Table 3 Medium-chain acyl-coa dehydrogenase deficiency Acute encephalopathy, seizures, hypoglycaemia, elevated ammonia, cardiovascular (autosomal, 1:17 000) collapse Clinical presentations of IMDs IMDs can present at any age and multiple systems are usually involved. In the UK, all neonates are offered screening for phenylketonuria and medium-chain acyl-coa dehydrogenase deficiency. Acute decompensation in the neonatal period may be life threatening; encephalopathy (with or without metabolic acidosis) and hepatic syndromes associated with hypoglycaemia are common manifestations often in a child that was normal at birth. 1 Later decompensation associated with intercurrent illness or insidious presentation later in childhood may also occur. Commonly occurring clinical syndromes associated with IMDs are described below. Neurological syndromes Acute encephalopathy may occur with little warning in a previously normal child. Focal neurological deficits are uncommon and consciousness levels may deteriorate. 1 This may occur in urea cycle disorders, organic acidaemias, and fatty acid oxidation defects, or be secondary to hypoglycaemia. This is a medical emergency and may be the first presentation of an IMD. Chronic encephalopathy may manifest as global progressive developmental delay or psychomotor retardation. It is often associated with seizures that may be resistant to conventional treatment. 1 Examples include some MPS (Hunter and Sanfilippo). Other neurological symptoms include stroke-like episodes, which may occur in organic acidaemias, urea cycle disorders, and homocystinuria. Movement disorders such as ataxia in maple syrup urine disease (MSUD) or choreoathetosis in the Lesch Nyhan syndrome may occur. Myopathy can be a feature, for example, in GSD involving muscle glycogen (Pompe disease). Progressive myopathy in association with multisystem disease is often a feature of mitochondrial disorders. Neurobehavioural problems including hyperactivity, impulsiveness, and aggressive behaviour occur in many IMDs (Hunter, Sanfilippo, Lesch Nyhan syndrome). 1 Metabolic acidosis Lactic acidosis is the commonest cause of metabolic acidosis in children and is a feature of pyruvate dehydrogenase deficiency or mitochondrial electron transport chain defects. It may occur secondarily such as in glycogen storage disease type 1 where an enzyme defect prevents the conversion of glucose-6-phosphate to glucose. Glucose-6-phosphate is instead ultimately converted into lactate. 3 The accumulation of organic anions such as ketoacids (MSUD) and organic acids (organic acidaemias) will cause a metabolic acidosis often in association with hyperammonaemia or hypoglycaemia and acute encephalopathy. The measurement of the anion gap is essential in evaluating these patients. Urine and sweat have a peculiar smell in the organic acidaemias. 1 Hepatic syndromes Non-tender hepatomegaly is a feature of GSD and occurs in association with splenomegaly in lysosomal storage diseases. Hepatocellular dysfunction may be present (GSD, Gaucher disease). Jaundice may be conjugated, where hepatocellular dysfunction is present, or unconjugated secondary to disorders resulting in haemolysis, for example, glucose-6-phosphate dehydrogenase deficiency or pyruvate kinase deficiency. 1 Hypoglycaemia occurs where there are defects in mechanisms for gluconeogenesis, such as pyruvate carboxylase deficiency. Gluconeogenesis is the metabolic mechanism by which Continuing Education in Anaesthesia, Critical Care & Pain j Volume 11 Number
3 non-carbohydrates such as fatty acids are converted to glucose; pyruvate is a pivotal intermediate. Defects in fatty acid or ketone oxidation may also precipitate hypoglycaemia since these processes are mechanisms for decreasing peripheral glucose utilization and in their absence over utilization of glucose may occur. Examples include long-, medium-, and short-chain fatty acid acyl-coa dehydrogenase deficiencies. Cardiac syndromes Cardiac disease is usually manifest as a cardiomyopathy. This may be accompanied by arrhythmias and valvular insufficiency. Dilated cardiomyopathy is associated with inborn errors of fatty acid oxidation. The multisystemic nature of mitochondrial electron transport chain defects can include serious cardiac disease. Significant hypertrophic cardiomyopathy may be a feature of lysosomal storage diseases such as the MPS and Pompe disease. 1 Coronary artery disease may occur in younger patients with homocystinuria or familial hypercholesterolaemia. Dysmorphism and storage syndromes Dysmorphism, especially of facial features, is often found in patients with inherited metabolic disease and tends to become more pronounced with age. Children with inherited metabolic diseases often resemble patients with the same disorder and not their own family. 1 Storage disorders such as the MPS are associated with significant dysmorphism and are of particular interest to the anaesthetist. The accumulation of glycosaminoglycans leads to distortion of any tissue of which connective tissue is a significant component. The bone, cartilage, ligaments, skin, vasculature, dura mater, and heart valves may all be primarily affected with secondary disruption of other tissue occurring as a result of abnormalities of shape and growth. 2 Common themes in the perioperative management of IMDs Preoperative considerations A multidisciplinary approach is essential. All elective surgery for these patients should take place in a hospital with full access to the multidisciplinary team and intensive care facilities. Preoperative assessment should be undertaken in conjunction with the metabolic team and previous anaesthetic records should be consulted. Elective surgery should not proceed if there is significant evidence of coexisting infection since this increases the risk of metabolic decompensation. 3 Preoperative assessment should include evaluation of the child s cardiac and respiratory systems where these may be affected by the disease process. An ECG and a recent echocardiogram where relevant are important. The degree and distribution of any myopathy should be assessed. 3 Blood workup should include full blood count, renal function, electrolytes, arterial blood gas analysis, and serum glucose. Consider preoperative correction of any significant degree of metabolic acidosis. Peritoneal or haemodialysis may be required to reduce the levels of metabolic acids. Maintain any special or restrictive diets perioperatively. Continue all supplemental cofactors, which optimize the abnormal metabolic pathway or help clear toxic metabolites, for example, carnitine to help eliminate organic acids, glycine in isovaleric acidaemia, and sodium benzoate and sodium phenylacetate in urea cycle defects. 3 The stress response to surgery and fasting increases the risk of metabolic decompensation. Avoid prolonged perioperative fasting and maintain hydration. A catabolic state will promote flux through the abnormal metabolic pathway in many IMDs. Schedule IMD patients first on the operating list and administer fluids containing 10% glucose once fasting commences. Calories in the form of i.v. fat emulsion can be included to minimize the glucose load. 3 Clear high carbohydrate energy drinks may be beneficial and can be consumed up to 2 h before surgery. Use sedative premedication with great caution especially in IMD patients with associated airway problems, for example, MPS. Whenever possible, emergency cases should be transferred to specialist centres. Close liaison between the patient s metabolic team, anaesthetists, surgeons, and intensive care is vital, particularly if the emergency occurs at a non-specialist hospital. Remember that the patient s family will also provide invaluable information regarding the IMD, its severity, and previous perioperative history. Intraoperative considerations There is a risk of significant hyperkalaemia associated with the use of succinylcholine in myopathic children. Use respiratory depressants and non-depolarizing neuromuscular blocking agents with care in the presence of myopathy. 3 Take care in positioning patients particularly where bone and joint disease including cervical spine instability may be present (e.g. MPS). Avoid lactate-containing fluids if lactic acidosis is a feature of the IMD. Limit intraoperative metabolic acidosis by ensuring adequate tissue perfusion. Bicarbonate administration may be necessary to compensate for intraoperative acidosis. 3 Hypothermia should be avoided as it may contribute to the development of metabolic acidosis. Arterial blood gases, serum electrolyte, blood glucose, and, if indicated, ammonia levels should be measured during prolonged surgery. For procedures involving oral or intestinal blood loss, place a nasogastric tube or throat pack to prevent the accumulation of blood in the stomach. Blood in the gastrointestinal tract 64 Continuing Education in Anaesthesia, Critical Care & Pain j Volume 11 Number
4 constitutes a large protein load and may trigger an acute decompensation in many metabolic disorders particularly those involving amino acid metabolism. 3 Avoid the prolonged use of nitrous oxide; it has been associated with megaloblastic anaemia in phenylketonuria. In MMA, it can inhibit methylmalonyl-coa mutase, and in homocystinuria, it has an inhibitory action on methionine synthase. 3 Postoperative considerations All patients should be observed closely after anaesthesia for signs of clinical deterioration. Monitoring in a highdependency environment is advisable where there is an increased risk of metabolic or clinical deterioration. 3 Regular monitoring of acid base status and plasma ammonia should be undertaken in order to detect decompensation early. Reinstitute the patient s specialized diet as soon as possible after anaesthesia. IMD patients should not usually be managed on a day-case basis. The following disorders are examined in more detail, either because of their ability to illustrate important management principles of IMDs or because of their particular relevance to the anaesthetist. The organic acidaemias: propionic and methylmalonic acidaemia The degradation of valine, isoleucine, odd-chain fatty acids, cholesterol, methionine, and threonine converges into three final steps, the propionate pathway. Propionyl-CoA is carboxylated to methylmalonic acid by the mitochondrial enzyme propionyl-coa carboxylase, using biotin as a cofactor. Methylmalonyl-CoA is then converted to succinyl-coa by the enzyme methylmalonyl- CoA mutase, with cobalamin as a cofactor. Succinyl-CoA is broken down into carbon dioxide and water by the citric acid cycle. 2 Propionic acidaemia is caused by a deficiency of propionyl-coa carboxylase and results in the accumulation of propionic acid. MMA is caused by a deficiency of methylmalonyl-coa mutase causing accumulation of methylmalonic acid. Clinical severity varies, but classically, presentation involves an acute decompensation. Features include tachypnoea, dehydration, vomiting, lethargy, hyperglycinaemia (caused by inhibition of glycine cleavage by high levels of organic acids), ketoacidosis, neutropenia, thrombocytopenia, hypoglycaemia, and metabolic acidosis. Decompensation is usually precipitated by a catabolic stress such as infection. Hyperammonaemia occurs and is thought to be the result of the organic acids causing inhibition of carbamylphosphate synthetase of the urea cycle. Treatment includes a protein-restricted diet. Carnitine will conjugate with organic acids to form a metabolite that is excreted by the kidneys, carnitine levels are often deficient, and hence, supplementation is important. In the event of an acute crisis, these children should be rehydrated, have infections aggressively identified and treated, and have measures to prevent catabolism instituted. Biotin and vitamin B12 should be given in propionic acidaemia and MMA, respectively. Acidosis and hyperammonaemia should be treated. 2 The acute treatment of hyperammonaemic coma involves both routine resuscitation and reduction of plasma ammonia. Protein intake should be restricted or stopped for h, and to avoid protein catabolism, an i.v. infusion of fluid and electrolytes with 8 10 mg kg 21 min 21 of glucose should be commenced. Sodium benzoate 250 mg kg 21 and sodium phenylacetate 250 mg kg 21 should be given i.v.; these agents react with glycine and glutamine, respectively, to form products that are more readily excreted by the kidneys than ammonia. For ammonia levels above 600 mmol litre 21, peritoneal or haemodialysis should be considered. 2 Liver transplantation is now a viable treatment option as it offers a potential cure with the donor liver providing the deficient enzymes. 4,5 Most of the general considerations for perioperative care of IMDs apply specifically to the organic acidaemias. 4 6 Disorders of carbohydrate metabolism: glycogen storage diseases Glucose is the primary substrate for aerobic metabolism generating adenosine triphosphate via glycolysis and oxidative phosphorylation. Blood glucose levels are maintained by dietary intake, gluconeogenesis, and most importantly the breakdown of glycogen via glycogenolysis. The breakdown of hepatic glycogen ensures a rapid release of glucose into the bloodstream to maintain a euglycaemic state, whereas the breakdown of muscle glycogen provides the main source of stored energy within muscles, particularly important during exercise. 2 Inherited defects in glycogen metabolism prevent the mobilization of glucose from glycogen and typically cause the accumulation of glycogen within tissues such as the liver or muscles, hence the collective term GSD. These disorders have an overall frequency of 1 in live births and their classification is summarized in Table 2. 2 The management of the GSD involves maintaining an adequate blood glucose level and provision of alternate energy sources. In infants, this usually involves regular daytime snacking and nocturnal intragastric glucose feeds, or uncooked cornstarch in older children. Pompe disease may be treated with recombinant human a-glucosidase enzyme replacement therapy. 7 Specific anaesthetic considerations Fasting should be minimized. To prevent hypoglycaemia, blood glucose should be monitored and perioperative glucose- Continuing Education in Anaesthesia, Critical Care & Pain j Volume 11 Number
5 Table 2 The glycogen storage diseases Disease and eponym Inheritance and incidence Organs affected Clinical features Type I (von Gierke disease) Autosomal, 1: Liver (and renal) Hypoglycaemia, lactic acidosis, ketosis, hepatomegaly, truncal obesity, short stature, hypertriglyceridaemia, hyperuricaemia and gout, platelet dysfunction, renal dysfunction. Good prognosis with supportive treatment Hypotonia and skeletal muscle weakness, hypertrophic cardiomyopathy. Death from cardio respiratory failure by 2 yr in severe infantile form Hypoglycaemia, ketonuria, hepatomegaly, muscle fatigue. Good prognosis Type II (Pompe disease) Autosomal, 1: Cardiac, muscle, liver Type III (Cori disease) Autosomal, Liver, muscles 1: Type IV (Andersen disease) Autosomal, Liver Failure to thrive, hypotonia, hepatosplenomegaly. Hepatic cirrhosis leading to death by 5 yr 1: Type V (McArdle disease) Autosomal, Muscle Exercise intolerance, muscle cramps, fatigability. Good prognosis 1: Type VI (Hers disease) 1: Liver Hepatomegaly, mild hypoglycaemia, hyperlipidaemia, ketosis. Good prognosis Type VII (Tarui disease) Autosomal, Muscle Similar to GSD type V 1: Type VIII/IX (phosphorylase Autosomal and X-linked Liver Similar to GSD type III, but no myopathy kinase deficiency) containing fluids should be administered. In Tarui disease where the enzymatic defect is part of the glycolytic pathway rather than the glycogenolytic path, glucose cannot be utilized by muscles. 3 Check renal function and platelets in patients with von Gierke disease. 3 Check coagulation and liver function in patients with Andersen disease who may have hepatic cirrhosis. 3 Preoperative cardiac assessment, including ECG and echocardiography, is important where cardiomyopathy may be a feature (Cori, Andersen, and Tarui diseases). This is of particular importance in Pompe disease where hypertrophic cardiomyopathy may cause significant left ventricular outflow tract obstruction. Reduced coronary perfusion pressure causing subendocardial ischaemia and cardiac arrest under general anaesthesia has been reported. Myocardial depressants should be used with care. 8 Limitation of respiratory reserve, postoperative atelectasis, and respiratory tract infections may be a consequence of myopathy which is particularly a feature of Pompe disease. 8 Truncal obesity may be present in von Gierke and Cori diseases. Macroglossia is a feature of Pompe disease and can cause airway difficulties. Tourniquets can cause muscle damage and should be avoided in McArdle disease. 3 Lysosomal storage diseases: mucopolysaccharidoses Lysosomes contain enzymes that are responsible for breaking down specific macromolecules. Enzyme defects in lysosomal storage disorders lead to abnormal sequestration of partially degraded glycosaminoglycans, an essential component of connective tissue. This results in a progressive, multisystemic disease with organomegaly, visual, auditory, and intellectual deficits, airway abnormalities, cardiovascular impairment, joint and bony deformities, and characteristic coarse facial features 9 (Table 3). Until recently, the management of these disorders has been palliative with the focus on the control of cardiac and respiratory complications, hydrocephalus, hearing loss, and spinal column abnormalities. Treatment options now include haematopoetic stem cell transplantation and enzyme replacement therapy. 10 Stem cell transplantation halts the progression of these diseases, reduces hepatosplenomegaly, joint stiffness, obstructive sleep apnoea, facial dysmorphism, heart disease, hydrocephalus, and hearing loss. Skeletal and ocular abnormalities are not corrected and neurological outcomes remain poor. 11 Enzyme replacement therapy has been approved for use in MPS I, II, and VI after clinical trials demonstrating improvements in these conditions. 10,11 Recombinant human a-l-iduronidase for MPS I, idursulfase for MPS II, and arylsulfatase B for MPS VI are available for treatment. 10 Specific anaesthetic considerations An experienced anaesthetic team should always manage these children. Anaesthesia should not be undertaken lightly and the risks of anaesthesia must be carefully considered and explained to the parents and the child (if appropriate) along with the benefits of the scheduled procedure. 12 The airway is often severely compromised and anaesthesia in patients with MPS may be extremely challenging. Evidence of obstructive sleep apnoea should be sought; preoperative sleep studies may required for full evaluation and risk stratification. 13 Previous anaesthetic records should be evaluated, but the progression of any airway and clinical findings is to be expected and the view at direct laryngoscopy may be significantly less favourable with increasing age. 13 Lateral cervical films may be useful; cervical spine instability most often occurs in MPS I (Hurler) and IV (Morquio) and these patients may benefit from assessment with flexion extension images taken under specialist supervision. Cervical 66 Continuing Education in Anaesthesia, Critical Care & Pain j Volume 11 Number
6 Table 3 The mucopolysaccharidoses Mucopolysaccharidosis (and eponyms) MPS I (Hurler, Scheie and the Hurler Scheie intermediate spectrum) MPS II (Hunter) MPS III (Sanfillippo types A to D) MPS IV (Morquio types A and B) MPS VI (Maroteaux Lamy) MPS VII (Sly) Incidence and genetics 1: , autosomal 1: , X-linked 1:24 000, autosomal 1: , autosomal 1: , autosomal Rare autosomal Clinical features Severe (Hurler) phenotype includes macrocephaly, coarse facies, and macroglossia. Hydrocephalus and mental retardation. High incidence of respiratory tract infections, obstructive sleep apnoea. Cardiomyopathy, coronary intimal and valvular thickening, mitral regurgitation. Dysostosis multiplex, stiff joints, thoracolumbar kyphosis, short neck, short stature. Corneal clouding, middle ear disease, and hearing loss. Hepatosplenomegaly. Usually death before 10 yr Mild (Scheie) has less coarse facies and normal intelligence. Aortic valvular disease, stiff joints, and corneal clouding. Survival into adulthood Wide spectrum of severity. Phenotype of macrocephaly, coarse facies similar to Hurler. Mental retardation and hydrocephalus, slower neurological deterioration than Hurler. Obstructive sleep apnoea. Coronary intimal thickening and ischaemic cardiomyopathy. Dysostosis multiplex, diffuse joint limitation, short neck, short stature. No corneal clouding. Hepatosplenomegaly. Death before 15 yr Mild somatic features, coarse hair, and hirsutism. Severe behavioural disturbance and profound mental deterioration, hyperactivity, aggression, dementia, and seizures. Sleep disorders. Short stature, lumbar vertebral dysplasia. Death in second decade Neurological abnormalities secondary to cervical myelopathy. Normal intelligence. Aortic regurgitation. Unique and distinct skeletal abnormalities, short trunk dwarfism, stature,120 cm, odontoid hypoplasia with C1 C2 and C2 C3 subluxation possible, severe kyphoscoliosis, ligamentous laxity. Fine corneal opacities, wide spaced teeth Macrocephaly, coarse facies, macroglossia. Normal intelligence. Airway difficulties. Mitral and aortic valvular thickening and regurgitation. Dysostosis multiplex, mild joint stiffness, kyphoscoliosis, odontoid hypoplasia, cervical myelopathy, short stature. Corneal clouding and organomegaly Wide clinical spectrum, macrocephaly, coarse facies. Mental retardation. Dysostosis multiplex, joint flexion contractures, short stature, thoracolumbar gibbus, hip dysplasia, odontoid hypoplasia. Corneal clouding, organomegaly. Severe neonatal form of hydrops foetalis canal stenosis may lead to compression in patients with MPS IV and should cervical myelopathy be suspected then it is best evaluated with magnetic resonance imaging. 13 Behavioural problems may be considerable; however, sedative premedication should be used with great caution. An antisialogogue is useful to aid airway management during induction. Preoperative assessment should include thorough clinical evaluation of the child s cardiac and respiratory systems. 12,13 A recent echocardiogram should be reviewed to evaluate cardiomyopathy, valvular heart disease, or both. Respiratory tract infections should have fully resolved before elective surgery. Always anticipate a difficult airway in patients with MPS and ensure the full range of difficult airway adjuncts is available. The overall incidence of airway difficulties is 25%, with failure to intubate in 8% of MPS cases (rising to 54% and 23%, respectively, in Hurler s syndrome). 13 This is due to a combination of factors including airway tissue deposition of glycosaminoglycans, a short, often unstable neck, poor joint mobility including the cervical spine and temporomandibular joints, macroglossia, and micrognathia. All of these factors get worse with age. Facemasks may not fit appropriately due to the abnormal facies, and these children often readily obstruct on induction. This may not be relieved by oropharyngeal airways, which can push the enlarged epiglottis downwards causing laryngeal obstruction. Nasopharyngeal airways are difficult to pass due to nasal tissue deposits. Some authors have advised forward traction of the tongue. 12 Any neck manipulation should be avoided, and where there is atlanto-axial subluxation, as in Morquio syndrome, manual inline immobilization should be used. 13 The laryngeal mask airway (LMA) has been found to be particularly useful and the use of the LMA as a conduit for intubation is well described. 13,14 The tracheal tube size required will be smaller than that expected for age. The McCoy blade can be useful where an enlarged epiglottis is obstructing the view. Fibreoptic intubation may be necessary where cervical spine instability exists or the view at laryngoscopy is poor. The equipment and staff for emergency tracheostomy should be available. Post-obstructive pulmonary oedema has been described in patients with advanced disease. Pre-existing supraglottic obstruction may be compounded by an exacerbation of preexisting glottic obstruction after tracheal extubation and this may lead to negative pressure pulmonary oedema. This can occur some hours after the obstructive event. Extubation should occur once fully awake and dexamethasone may be helpful. 12,14 Postoperative care should take place in a monitored environment (high dependency or intensive care) and humidified oxygen and early physiotherapy are advised. 12 Continuing Education in Anaesthesia, Critical Care & Pain j Volume 11 Number
7 Regional analgesia is useful; alternatively, a mutimodal approach to analgesia should occur. Great care should be taken when using opioid analgesia in MPS patients. Conclusion Inherited metabolic diseases, while individually rare conditions, contribute significantly to paediatric morbidity and mortality. Anaesthetists may encounter patients with inherited metabolic diseases presenting for both emergency and elective surgery. The management of these patients is often challenging due to the multisystemic manifestations of many IMDs. Catastrophic metabolic decompensation may occur in the perioperative period and a multidisciplinary approach is essential to ensure safe management of these patients. Conflict of interest None declared. References 1. Clarke JTR. Inherited Metabolic Diseases, 3rd Edn. New York: Cambridge University Press, Rezvani I, Hen YT. Metabolic diseases: defects in metabolism of amino acids and carbohydrates. In: Behrman RE, Kliegman R, Jenson HB, eds. Nelson Textbook of Pediatrics, 18th Edn. Philadelphia: W.B. Saunders Company, 2000; Baum VC, O Flaherty JE. Anesthesia for Genetic, Metabolic and Dysmorphic Syndromes of Childhood, 2nd Edn. Philadelphia: Lippincott Williams and Wilkins, Kim TW, Hall SR. Liver transplantation for propionic acidaemia in a 14-month-old male. Paediatr Anaesth 2003; 13: Ho D, Harrison V, Street N. Anaesthesia for liver transplantation in a patient with methylmalonic acidaemia. Paediatr Anaesth 2000; 10: Harker HE, Emhardt JD, Hainline BE. Propionic acidaemia in a four-month-old male: a case study and anesthetic implications. Anesth Analg 2000; 91: Koeberl DD, Kishnani PS, Chen YT. Glycogen storage disease types I and II: treatment updates. J Inherit Metab Dis 2007; 30: Ing RJ, Cook DR, Bengur RA et al. Anaesthetic management of infants with glycogen storage disease type II: a physiological approach. Pediatr Anaesth 2004; 14: Wraith JE. The mucopolysaccharidoses: a clinical review and guide to management. Arch Dis Child 1995; 72: Martin R, Beck M, Eng C, Giugliani R, Harmatz P. Recognition and diagnosis of mucopolysaccharidosis II (Hunter syndrome). Pediatrics 2008; 121: Giugliani R, Harmatz, Wraith JE. Management guidelines for mucopolysaccharidosis VI. Pediatrics 2007; 120: Diaz JH, Belani KG. Perioperative management of children with mucopolysaccharidoses. Anesth Analg 1993; 77: Walker RWM, Darowski M, Morris P, Wraith JE. Anaesthesia and mucopolysaccharidoses. Anaesthesia 1994; 49: Walker RWM, Colovic V, Robinson DN, Dearlove OR. Postobstructive pulmonary oedema during anaesthesia in children with mucopolysaccharidoses. Paediatr Anaesth 2003; 13: Please see multiple choice questions Continuing Education in Anaesthesia, Critical Care & Pain j Volume 11 Number
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Anaesthesia recommendations for patients suffering from Methylmalonic acidemia (or aciduria)
 orphananesthesia Anaesthesia recommendations for patients suffering from Methylmalonic acidemia (or aciduria) Disease name: Methylmalonic acidemia ICD 10: E71.1 Synonyms: Methylmalonic aciduria, MMA, isolated
orphananesthesia Anaesthesia recommendations for patients suffering from Methylmalonic acidemia (or aciduria) Disease name: Methylmalonic acidemia ICD 10: E71.1 Synonyms: Methylmalonic aciduria, MMA, isolated
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is mandated and administered by the Illinois Department of
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is mandated and administered by the Illinois Department of
HEREDITARY METABOLIC DISEASES
 HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
Anesthesia recommendations for patients suffering from Mucolipidosis II and III
 orphananesthesia Anesthesia recommendations for patients suffering from Mucolipidosis II and III Disease name: Mucolipidosis Type 2 and 3 ICD 10: E77.0 Synonyms: Mucolipidosis type 2 - I-cell disease N-acetyl-glucosamine
orphananesthesia Anesthesia recommendations for patients suffering from Mucolipidosis II and III Disease name: Mucolipidosis Type 2 and 3 ICD 10: E77.0 Synonyms: Mucolipidosis type 2 - I-cell disease N-acetyl-glucosamine
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
What s New in Newborn Screening?
 What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
What s New in Newborn Screening? Funded by: Illinois Department of Public Health Information on Newborn Screening Newborn screening in Illinois is administered by the Illinois Department of Public Health.
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Inborn Errors of Metabolism (IEM)
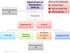 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
Methylmalonic aciduria
 Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Current Management and Future Developments in Metabolic Disease
 Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
Glycogen Storage Disease
 Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Hurler s Syndrome: Anaesthetic Challenges and Management
 Hurler s Syndrome: Anaesthetic Challenges and Management Dr.Arun Kr. Gupta, Dr. Vinod Kharde, Dr. Varun Gawer, Dr.R.V.Sidhaye, Dr.D.S.Divekar. Department. Of Anaesthesiology, Rural Medical College, Loni
Hurler s Syndrome: Anaesthetic Challenges and Management Dr.Arun Kr. Gupta, Dr. Vinod Kharde, Dr. Varun Gawer, Dr.R.V.Sidhaye, Dr.D.S.Divekar. Department. Of Anaesthesiology, Rural Medical College, Loni
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona
 BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
By: Dr Hadi Mozafari 1
 By: Dr Hadi Mozafari 1 Gluconeogenesis is the process of converting noncarbohydrate precursors to glucose or glycogen. The major substrates are the glucogenic amino acids, and lactate, glycerol, and propionate.
By: Dr Hadi Mozafari 1 Gluconeogenesis is the process of converting noncarbohydrate precursors to glucose or glycogen. The major substrates are the glucogenic amino acids, and lactate, glycerol, and propionate.
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
For healthcare professionals Methylmalonic Acidurias
 www.e-imd.org For healthcare professionals Methylmalonic Acidurias Methylmalonic acidurias (MMAurias) comprise a group of inborn errors of metabolism characterized by an isolated accumulation of methylmalonic
www.e-imd.org For healthcare professionals Methylmalonic Acidurias Methylmalonic acidurias (MMAurias) comprise a group of inborn errors of metabolism characterized by an isolated accumulation of methylmalonic
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Metabolic Disorders Screened Overseas but not Screened in Australia Condition Features Inherited Diagnosis Treatment Newborn Screen
 Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
CHY2026: General Biochemistry UNIT 7& 8: CARBOHYDRATE METABOLISM
 CHY2026: General Biochemistry UNIT 7& 8: CARBOHYDRATE METABOLISM Metabolism Bioenergetics is the transfer and utilization of energy in biological systems The direction and extent to which a chemical reaction
CHY2026: General Biochemistry UNIT 7& 8: CARBOHYDRATE METABOLISM Metabolism Bioenergetics is the transfer and utilization of energy in biological systems The direction and extent to which a chemical reaction
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Anaesthesia recommendations for patients suffering from. Maple syrup urine disease
 orphananesthesia Anaesthesia recommendations for patients suffering from Disease name: Maple syrup urine disease ICD 10: E71.0 Maple syrup urine disease Synonyms: MSUD, branched-chain ketoaciduria, branched-chain-alpha-ketoacid
orphananesthesia Anaesthesia recommendations for patients suffering from Disease name: Maple syrup urine disease ICD 10: E71.0 Maple syrup urine disease Synonyms: MSUD, branched-chain ketoaciduria, branched-chain-alpha-ketoacid
Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION
 Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
Metabolism. Chapter 5. Catabolism Drives Anabolism 8/29/11. Complete Catabolism of Glucose
 8/29/11 Metabolism Chapter 5 All of the reactions in the body that require energy transfer. Can be divided into: Cell Respiration and Metabolism Anabolism: requires the input of energy to synthesize large
8/29/11 Metabolism Chapter 5 All of the reactions in the body that require energy transfer. Can be divided into: Cell Respiration and Metabolism Anabolism: requires the input of energy to synthesize large
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Hurler Syndrome (Severe Type) -A Rare Case Report
 Annals of Dental Research (2012) Vol 2 (1): 26-30 Mind Reader Publications: All Rights Reserved Annals of Dental Research www.adres.yolasite.com Case Report Hurler Syndrome (Severe Type) -A Rare Case Report
Annals of Dental Research (2012) Vol 2 (1): 26-30 Mind Reader Publications: All Rights Reserved Annals of Dental Research www.adres.yolasite.com Case Report Hurler Syndrome (Severe Type) -A Rare Case Report
Biol 219 Lec 7 Fall 2016
 Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Amino acid Catabolism
 Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Lysosomal Storage Disorders. Karen Fieggen UCT Human Genetics Groote Schuur Hospital
 Lysosomal Storage Disorders Karen Fieggen UCT Human Genetics Groote Schuur Hospital Disclosures: Employed full time in public sector Flights and accommodation to this conference kindly paid for by Sanofi
Lysosomal Storage Disorders Karen Fieggen UCT Human Genetics Groote Schuur Hospital Disclosures: Employed full time in public sector Flights and accommodation to this conference kindly paid for by Sanofi
Clinical Approach to Diagnosis of Lysosomal Storage Diseases
 Clinical Approach to Diagnosis of Lysosomal Storage Diseases M. Rohrbach, MD, PhD FMH Pädiatrie und FMH Medizinische Genetik Abteilung Stoffwechsel Universitätskinderklinik Zürich Lysosomal storage disorders
Clinical Approach to Diagnosis of Lysosomal Storage Diseases M. Rohrbach, MD, PhD FMH Pädiatrie und FMH Medizinische Genetik Abteilung Stoffwechsel Universitätskinderklinik Zürich Lysosomal storage disorders
Lipid Metabolism. Remember fats?? Triacylglycerols - major form of energy storage in animals
 Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
DNA Day Illinois 2013 Webinar: Newborn Screening and Family Health History. Tuesday, April 16, 2013
 DNA Day Illinois 2013 Webinar: Newborn Screening and Family Health History Tuesday, April 16, 2013 Objectives Recognize the importance & impact of newborn screening Describe the process of newborn screening
DNA Day Illinois 2013 Webinar: Newborn Screening and Family Health History Tuesday, April 16, 2013 Objectives Recognize the importance & impact of newborn screening Describe the process of newborn screening
Disclosures. Learning Objectives. Inheritance patterns. Lysosomal function. Mucopolysaccharidoses (MPS): Keys to Early Recognition and Intervention
 39 th National Conference on Pediatric Health Care March 19-22, 2018 CHICAGO Disclosures Mucopolysaccharidoses (MPS): Keys to Early Recognition and Intervention Lindsay Torrice, MSN, CPNP PC Clinical Instructor
39 th National Conference on Pediatric Health Care March 19-22, 2018 CHICAGO Disclosures Mucopolysaccharidoses (MPS): Keys to Early Recognition and Intervention Lindsay Torrice, MSN, CPNP PC Clinical Instructor
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Understanding metabolic disease
 Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
Anaesthesia recommendations for patients suffering from Sanfilippo disease
 orphananesthesia Anaesthesia recommendations for patients suffering from Sanfilippo disease Disease name: Mucopolysaccharidosis type III ICD 10: E76.2 Synonyms: MPS III, Sanfilippo syndrome, Mucopolisaccaridosi
orphananesthesia Anaesthesia recommendations for patients suffering from Sanfilippo disease Disease name: Mucopolysaccharidosis type III ICD 10: E76.2 Synonyms: MPS III, Sanfilippo syndrome, Mucopolisaccaridosi
Nutritional Interventions in Primary Mitochondrial Disorders
 Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Date of commencement: February Principal Investigator Dr. Jayesh J. Sheth CASE RECORD FORM
 ICMR-FRIGE-MULTICENTRIC LSDs Project Foundation for Research in Genetics & Endocrinology [FRIGE], FRIGE House, Jodhpur Gam road, Satellite, Ahmedabad-380015 Tel no: 079-26921414, Fax no: 079-26921415 E-mail:
ICMR-FRIGE-MULTICENTRIC LSDs Project Foundation for Research in Genetics & Endocrinology [FRIGE], FRIGE House, Jodhpur Gam road, Satellite, Ahmedabad-380015 Tel no: 079-26921414, Fax no: 079-26921415 E-mail:
Genomics & Modern Health Care Caring for the Special Children & Adults of Isolated Populations. Propionic Acidemia
 Genomics & Modern Health Care Caring for the Special Children & Adults of Isolated Populations Propionic Acidemia D. Holmes Morton MD Pediatrician, Clinic for Special Children Strasburg, Pennsylvania 17579
Genomics & Modern Health Care Caring for the Special Children & Adults of Isolated Populations Propionic Acidemia D. Holmes Morton MD Pediatrician, Clinic for Special Children Strasburg, Pennsylvania 17579
Clinical Management of Organic Acidemias and OAA Natural History Registry. Kim Chapman MD PhD Children s National Rare Disease Institute
 Clinical Management of Organic Acidemias and OAA Natural History Registry Kim Chapman MD PhD Children s National Rare Disease Institute Disclosure Nothing to disclose concerning this lecture Organic acid?
Clinical Management of Organic Acidemias and OAA Natural History Registry Kim Chapman MD PhD Children s National Rare Disease Institute Disclosure Nothing to disclose concerning this lecture Organic acid?
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Metabolism of pentoses, glycogen, fructose and galactose. Jana Novotna
 Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Chapter 7- Metabolism: Transformations and Interactions Thomson - Wadsworth
 Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Volume of practice and workplace-based assessment requirements for each of the ANZCA Clinical Fundamentals
 Appendix Four Volume of practice and workplace-based assessment requirements for each of the ANZCA Clinical Fundamentals This appendix contains tables setting out both the volume of practice and workplace-based
Appendix Four Volume of practice and workplace-based assessment requirements for each of the ANZCA Clinical Fundamentals This appendix contains tables setting out both the volume of practice and workplace-based
Summary. Syndromic versus Etiologic. Definitions. Why does it matter? ASD=autism
 Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
A Rare disease: MPS III San Filippo disease
 A Rare disease: MPS III San Filippo disease Annick Raas-Rothschild, MD Pediatrician-Medical Geneticist Director of the Rare Diseases institute Institute of Genetics Sheba Tel Hashomer Medical Center Annick.rothschild@sheba.health.gov.il
A Rare disease: MPS III San Filippo disease Annick Raas-Rothschild, MD Pediatrician-Medical Geneticist Director of the Rare Diseases institute Institute of Genetics Sheba Tel Hashomer Medical Center Annick.rothschild@sheba.health.gov.il
Muscle Metabolism. Dr. Nabil Bashir
 Muscle Metabolism Dr. Nabil Bashir Learning objectives Understand how skeletal muscles derive energy at rest, moderate exercise, and strong exercise. Recognize the difference between aerobic and anaerobic
Muscle Metabolism Dr. Nabil Bashir Learning objectives Understand how skeletal muscles derive energy at rest, moderate exercise, and strong exercise. Recognize the difference between aerobic and anaerobic
MetBioNet Best Practice Guidelines. Investigation of an inherited metabolic cause of cardiomyopathy
 Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Metabolic integration and Regulation
 Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Very-long-chain acyl-coa dehydrogenase deficiency
 Very-long-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Very-long-chain acyl-coa dehydrogenase
Very-long-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Very-long-chain acyl-coa dehydrogenase
anabolic pathways- Catabolic Amphibolic
 METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
Glycogen function. Cellular glucose store. Local emergency store Local short term use
 Glycogen function Cellular glucose store Liver Brain Muscle Body sump Local emergency store Local short term use Glycogen storage diseases Accumulation abnormal amount/type glycogen Hypoglycaemia, lactic
Glycogen function Cellular glucose store Liver Brain Muscle Body sump Local emergency store Local short term use Glycogen storage diseases Accumulation abnormal amount/type glycogen Hypoglycaemia, lactic
Catabolism of Carbon skeletons of Amino acids. Amino acid metabolism
 Catabolism of Carbon skeletons of Amino acids Amino acid metabolism Carbon skeleton Carbon Skeleton a carbon skeleton is the internal structure of organic molecules. Carbon Arrangements The arrangement
Catabolism of Carbon skeletons of Amino acids Amino acid metabolism Carbon skeleton Carbon Skeleton a carbon skeleton is the internal structure of organic molecules. Carbon Arrangements The arrangement
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
LESSON 2.4 WORKBOOK. Part two: Glucose homeostasis in the blood Un-Storing energy
 DEFINITIONS OF TERMS Fasting A state of abstinence from all food or drinks that provide calories. For a complete list of defined terms, see the Glossary. LESSON 2.4 WORKBOOK Part two: Glucose homeostasis
DEFINITIONS OF TERMS Fasting A state of abstinence from all food or drinks that provide calories. For a complete list of defined terms, see the Glossary. LESSON 2.4 WORKBOOK Part two: Glucose homeostasis
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM
 5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
Fatty Acids Synthesis L3
 Fatty Acids Synthesis L3 The pathway for fatty acid synthesis occurs in the cytoplasm, whereas, oxidation occurs in the mitochondria. The other major difference is the use of nucleotide co-factors. Oxidation
Fatty Acids Synthesis L3 The pathway for fatty acid synthesis occurs in the cytoplasm, whereas, oxidation occurs in the mitochondria. The other major difference is the use of nucleotide co-factors. Oxidation
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
OVERVIEW M ET AB OL IS M OF FR EE FA TT Y AC ID S
 LIPOLYSIS LIPOLYSIS OVERVIEW CATABOLISM OF FREE FATTY ACIDS Nonesterified fatty acids Source:- (a) breakdown of TAG in adipose tissue (b) action of Lipoprotein lipase on plasma TAG Combined with Albumin
LIPOLYSIS LIPOLYSIS OVERVIEW CATABOLISM OF FREE FATTY ACIDS Nonesterified fatty acids Source:- (a) breakdown of TAG in adipose tissue (b) action of Lipoprotein lipase on plasma TAG Combined with Albumin
Secondary Energy Deficiencies in Organic Acidemias. Kimberly A Chapman MD PhD Children s National July 26, 2014
 Secondary Energy Deficiencies in Organic Acidemias Kimberly A Chapman MD PhD Children s National July 26, 2014 2 Goals of this talk Describe the secondary energy deficiencies seen in organic acidemias
Secondary Energy Deficiencies in Organic Acidemias Kimberly A Chapman MD PhD Children s National July 26, 2014 2 Goals of this talk Describe the secondary energy deficiencies seen in organic acidemias
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
Unusual Mucopolysaccharidoses cases. Tim Hutchin and Louise Allen Newborn Screening and Biochemical Genetics, Birmingham Children s Hospital
 Unusual Mucopolysaccharidoses cases Tim Hutchin and Louise Allen Newborn Screening and Biochemical Genetics, Birmingham Children s Hospital A Brief MPS History Lesson.. In 1917 Hunter (type II) reported
Unusual Mucopolysaccharidoses cases Tim Hutchin and Louise Allen Newborn Screening and Biochemical Genetics, Birmingham Children s Hospital A Brief MPS History Lesson.. In 1917 Hunter (type II) reported
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
Glycogen Storage Disease Type III, VI and IX - basics -
 Glycogen Storage Disease Type III, VI and IX - basics - Wyboston Lakes 10.10.2015 Urike Steuerwald Tórshavn / Hannover usteuerwald@web.de GSD III, VI and IX - Questions What goes wrong in glycogen storage
Glycogen Storage Disease Type III, VI and IX - basics - Wyboston Lakes 10.10.2015 Urike Steuerwald Tórshavn / Hannover usteuerwald@web.de GSD III, VI and IX - Questions What goes wrong in glycogen storage
