Total Retinal Volumetric Blood Flow Rate in Diabetic Patients With Poor Glycemic Control
|
|
|
- Isabella Kathlyn Elliott
- 5 years ago
- Views:
Transcription
1 Investigative Ophthalmology & Visual Science, Vol. 33, No. 2, February 1992 Copyright Association for Research in Vision and Ophthalmology Total Retinal Volumetric Blood Flow Rate in Diabetic Patients With Poor Glycemic Control Juan E. Grunwald, Charles E. Riva, Joan Baine, and Alexander J. Brucker Total retinal volumetric blood flow rate was measured in 12 normal subjects and 18 poorly controlled diabetic patients with background diabetic retinopathy. Maximum or center-line erythrocyte velocity (V max ) was assessed by bidirectional laser Doppler velocimetry in four to five major retinal veins of one eye of each subject. Venous diameter (D) was measured from monochromatic fundus photographs. Total venous cross-section and measured total retinal volumetric blood flow in the diabetic patients were significantly larger than normal (P = and P = 0.02, respectively). A positive linear correlation was found between V max and D in normal and diabetic eyes. Volumetric blood flow rate, Q, varied with D at a power of 2.87 in normal eyes and 2.67 in diabetic eyes. Total volumetric blood flow correlated with total venous cross-section. It was found that Q in the temporal retina was significantly larger than in the nasal retina in normal subjects {P = ) and diabetic patients (P = ). A significant difference in Q was observed between the superior and inferior retina in diabetic patients (P = 0.03) but not in normal subjects. The retinal vascular regulatory response to % oxygen breathing was reduced (P = 0.019) in diabetic patients and correlated with the level of background diabetic retinopathy. A close estimate of total volumetric blood flow may be obtained from blood flow measurement in one major retinal vein and the determination of total venous cross-section. This may be important for clinical studies in which measurements of all individual retinal veins may not be feasible. Invest Ophthalmol Vis Sci 33:36-363,1992 The retina is one of the major sites of the body affected by diabetic microvascular pathology. Abnormalities of the retinal circulation and its regulatory responses 1 " 12 are known to occur in the eyes of diabetic patients with retinopathy and are probably an important factor in the development of retinal diabetic pathology. Laser Doppler velocimetry studies of retinal hemodynamics in diabetes mellitus have been done previously. 6 " 11 In most of these studies, measurements of one single retinal vessel have been obtained in each eye. Because volumetric blood flow rate is a function of the size of the vessel measured and the area perfused, large variability in blood flow between patients has been reported. 8 " 11 In our study, to overcome this problem, we determined total retinal venous volumetric blood flow rate by adding the flows measured in four to five major retinal veins in each eye. From the Department of Ophthalmology, Scheie Eye Institute, School of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania. Supported by National Institutes of Health grants EY077, EY0322, and RR-0000 (Bethesda, Maryland) and the Vivian Simkins Lasko Retinal Vascular Research Fund. Submitted for publication: November, 1990; accepted September 17, Reprint requests: Dr. Juan E. Grunwald, Scheie Eye Institute, 1 North 39th Street, Philadelphia, PA Increased blood glucose levels and large fluctuations in these levels are associated with an increased incidence of diabetic retinopathy 13 ' 1 and are known to affect retinal hemodynamics in diabetic patients. 9 To characterize these retinal hemodynamic abnormalities further, we determined total retinal venous volumetric blood flow and the vascular regulatory response to hyperoxia in a group of poorly controlled patients with diabetes mellitus and compared the results with those obtained in normal control subjects. Materials and Methods Eighteen patients with insulin-dependent diabetes mellitus (age range, yr; mean ± standard deviation, 29 ± yr) were included in this study. The duration of diabetes ranged from 6-28 yr (mean, 17 ± 7 yr). All patients had background diabetic retinopathy, an otherwise normal eye examination, and glycosylated hemoglobin (GHb) values higher than three standard deviations above the mean for nondiabetic subjects. Average GHb measured by affinity chromatography was 12. ± 3.3% (upper limit of normal range, 8%). Blood glucose was determined from finger capillary blood samples using an Accu-Check blood glucose monitor (Boehringer Mannheim, Indianapolis, IN). The average blood glucose at the time of retinal volumetric blood flow determination was 192 ± mg/dl (Table 1). 36 Downloaded From: on 09/23/18
2 No. 2 TOTAL RETINAL DLOOD FLOW IN DIABETES / Grunwold er ol 37 Table 1. Subject characteristics Normal Diabetes Mean ± SD Range Mean ± SD Range Significance* Age (yr) Disease duration (yr) Glycosylated hemoglobin (%) Blood glucose (mg/dl) Mean brachial blood pressure (mmhg) Intraocular pressure (mmhg) 32 ±7 78 ± 17 8 ± 10 1± ±6 17±7 12. ± ± 8 ± 11 1± P = = not statistically significant. Nonpaired student t-test. Excluded from the study were patients who had: (1) previous treatment with three or more daily injections of insulin or an insulin pump; (2) three or more documented episodes of diabetic ketoacidosis requiring hospitalization; (3) history of systemic hypertension or substance abuse; () obesity, denned as body weight larger than 130% of ideal body weight; () presence of intraocular disease other than diabetic retinopathy; or (6) previous laser photocoagulation treatment. Results in diabetic patients were compared with those obtained from 12 normal volunteers (age range, 19- yr; mean, 32 ± 7) whose blood glucose level at the time of retinal volumetric flow measurements was an average of 78 ± 17 mg/dl (Table 1). All eyes studied had a best-refracted visual acuity of 6/7. or better, an intraocular pressure < 21 mm Hg, and a normal slit-lamp examination. A description and statistical comparison of the characteristics of normal subjects and diabetic patients is provided in Table 1. After a detailed explanation of the procedures, all subjects were asked to sign an appropriate consent form approved by the Internal Review Board of our institution. Only one eye, chosen at random, was investigated in each subject. After pupil dilation with tropicamide 1% and phenylephrine hydrochloride 10%, a Polaroid (Cambridge, MA) color fundus photograph of the posterior fundus was obtained to localize the sites of bidirectional laser Doppler velocimetry (BLDV) measurements. These measurements of the maximum, center-line erythrocyte velocity (V max ) were obtained in four to five major retinal veins. Velocity was measured on straight portions of veins at a distance of less than 2 disc diameters from the center of the optic nerve head. We avoided sites close to venous junctions or arteriovenous crossings and those where two vessels lay close to each other. The location of the measurement site was marked on the Polaroid photograph for later reference. We usedflowmeasurements from veins instead of arteries because the minimal flow pulsatility in these vessels permitted a more accurate determination of the average velocity. 81 During the BLDV measurements, an area of the posterior retina (30 in diameter) was illuminated at a wavelength of 70 nm with a retinal irradiance of about 0.30 mw/cm 2. The levels of laser light used during the experiments were within the maximum permissible levels for extended sources. 16 Fundus photographs were taken in monochromatic light at 70 nm using a Zeiss (Oberkochen, Germany) fundus camera and Plus-X pan film (Eastman Kodak, Rochester, NY). Intraocular pressure was measured by applanation tonometry, and brachial artery blood pressure was obtained by sphygmomanometry. Volumetric blood flow rate (Q) was calculated as described previously 89 as V mean TTD 2 /, where mean blood velocity (V mean ) was calculated as C V max. A value for C equal to 1/1.6 was used 17, and the relationship between V max and V mean was assumed to be the same in normal and diabetic subjects. This assumption has been discussed previously. 8 The venous diameter at the site of BLDV measurement, D (determined from projected photographic negatives), was an average obtained from six photographs. Total venous cross-section (S T ) was calculated by adding the crosssection of all visible veins observed around the disc. Measurements of V max and D were done on a major retinal vein during room air breathing and during -6 min of breathing % oxygen at atmospheric pressure. The retinal vascular regulatory response to hyperoxia (R), defined as the percentage decrease in Q between air and % oxygen breathing, was calculated using the formula: R = (Q air - Q ox )/Q air. All measurements of D were done by one examiner, and all V max determinations were done by another one. Both examiners were masked with regard to the results obtained by the other and the clinical status of the subject measured. In the diabetic subjects, seven standard field stereo color fundus photographs were obtained as in the Early Treatment of Diabetic Retinopathy Study (ETDRS) protocol. Retinopathy was assessed in a masked fashion at the Fundus Photographic Reading Center of the University of Wisconsin. An overall reti- Downloaded From: on 09/23/18
3 38 INVESTIGATIVE OPHTHALMOLOGY & VISUAL SCIENCE / February 1992 Vol. 33 nopathy level according to the ETDRS grading protocol was assigned to the study eye of each patient. Mean brachial artery blood pressure (BP m ) was calculated as BP d + V3(BP S - BP d ), where BP S and BP d are the brachial artery systolic and diastolic pressures. Paired and unpaired two-tailed student t-tests, correlation analysis based on r 2 values obtained from regression fits of the data, and rank correlation analysis were used in the evaluation of the results. All data in which student t-tests were applied were validated for normality using the Wilk-Shapiro test. A Wilcoxon rank-sum test was used in those cases in which the data were not distributed normally. We used P < 0.0 for statistical significance. Results Table 1 shows the studied subjects' characteristics. There were no significant differences in age, BP m, or intraocular pressure between diabetic patients and normal subjects. Blood glucose determined at the time of BLDV was significantly higher than normal in diabetic patients (P = 0.001, by unpaired student t- test). Figures 1 and 2 illustrate the dependence of V max and Q on the D of each of the four to five individual veins measured in normal subjects and diabetic patients. The D ranged from ixm in normal subjects and from nm in diabetic patients. When all points shown in Figure 1 were considered as independent data points, which they were not, a positive correlation was found between V max and D in normal subjects (correlation coefficient, r = 0.7) and in dia Normals 1 Diabetics Vessel Diameter (/xm) Fig. 1. Relationship between maximum erythrocyte velocity (V max ) and venous diameter (D), based on measurements obtained from four to five largest retinal veins in eyes of normal subjects (squares) and diabetic patients (circles). Correlation coefficients, r, for the linear fit are 0.7, (linear regression equation V max = X D) for normals, and 0.37 (linear regression equation V max = X D) for diabetic patients when all points are considered as independent observations. 'Normals Diabetics Vessel Diameter (/Am) Fig. 2. Relationship between volumetric blood flow (Q) and venous diameter (D), based on measurements obtained from four to five largest retinal veins in eyes of normal subjects (squares) and diabetic patients (circles). Correlation coefficients for the power curve fit are r = 0.96 for normals, and r = 0.83 for diabetic patients when all points are considered simultaneously as independent observations. Q varies as 6.1 X 10" 6 D 287 in normals and as 1. X 10" D 267 in diabetic patients. betic patients (r = 0.37), showing that erythrocyte velocity increases with increasing D. When the relationship between V max and D was investigated in each subject separately, a positive correlation with an average r = 0.88 ± 0.12 (range, ) was seen in normal subjects and an average r = 0.71 ± 0.27 (range, ) in diabetic patients. The average correlation coefficient was not significantly lower than normal in diabetic patients (P > 0.0, by Wilcoxon rank-sum test). The correlation coefficient between Q and D based on a power curve fit was r = 0.96 for normal subjects and r = 0.83 for diabetic patients when all vessels were analyzed as independent data points (Fig. 2). When the relationship between Q and D was investigated in each subject separately, a positive correlation with an average r of 0.98 ± 0.01 (range, ) was observed in normal subjects and an average r of 0.93 ±0.06 (range, ) in diabetic patients. The average r between D and Q was significantly smaller than normal in diabetic patients (P < 0.01, by Wilcoxoh rank-sum test). Q varied as ~ 6 D 287 in normal subjects and as 1. 10" D 267 in diabetic patients. Values of total measured Q (Q M ), obtained by adding the Q of the four to five vessels in which BLDV determinations were done in each eye, are summarized in Table 2 for normal subjects and in Table 3 for diabetic patients. Average Q M in diabetic patients was approximately % larger than normal (P = 0.02, by two-tailed, unpaired student t-test; Tables 2,3). Average S T of all visible veins in diabetic patients was also Downloaded From: on 09/23/18
4 No. 2 TOTAL RETINAL DLOOD FLOW IN DIADETE / Grunwald er al 39 Table 2. Total venous cross-section (S T ), total measured volumetric blood flow (Q M ), and corrected total volumetric blood flow (Q T ) in normal subjects Subject Mean SD # Veins Q measured %S T S T (cm 2 X W~ ) QM (iil/min) Qr (id/min) %S T : Sum of cross-section of all veins from which volumetric blood flow measurements were obtained expressed as a percentage of the cross-section of all visible veins (S T ). Q T : Corrected value of Q M based on an estimation of flow rates for vessels in which volumetric flow rate was not measured. Q T = Q M /%Sr X. significantly larger than normal, by approximately 30% {P = 0.001; Tables 2, 3). The BLDV measurements of V max, and therefore also of Q, were not obtained in all visible veins in all eyes studied. The percent S T values shown in Tables 2 and 3 represent the sum of the cross-section of all veins from which volumetric blood flow measurements were obtained expressed as a percentage of the cross-section of all visible veins present in each studied eye. To include those vessels in which Q was not determined, a total volumetric blood flow rate (Q T ) was calculated based on an estimation offlowrates for the vessels in which volumetricflowrate was not measured using the formula: Q T = Q M /%S T X (Tables 2, 3). Average Q T was also significantly larger than normal in diabetic patients (P = 0.009; Tables 2, 3). Nine patients with the mildest form of retinopathy (level ) already had an average Q T of.6 ± 6.6 /Lil/min and S T of ± 1.1 cm 2-10" ; these were significantly larger than normal (P < 0.0 and P < 0.01, respectively). Significant positive correlations were observed between S T and Q T in normal subjects (r = 0.88, P = , with a linear-regression equation of Q T = S T ) and in diabetic patients (r = 0.9, P = 0.0, with a linear-regression equation of Q T = S T ). Average D, V max, and Q for the largest retinal vein in normal subjects and diabetic patients are shown in Table. No significant differences from normal in D, Vmax> or Q were observed when the measurements obtained in the largest vein in diabetic patients and normal subjects were compared. We measured R in one of the major temporal veins; it was significantly reduced in diabetic patients (P Table 3. Total venous cross-section (S T ), total measured volumetric blood flow (Q M ), and corrected total volumetric blood flow (Q T ) in diabetic patients Subject Retinopathy level #Veins Q measured %S T S T (cm 2 X 10~ ) QM (til/mm) Qr (nl/min) Mean SD Significance* P = P = P = %Sr: Sum of cross-section of all veins from which volumetric blood flow measurements were obtained expressed as a percentage of the cross-section of all visible veins (ST). Q T : Corrected value of Q M based on an estimation of flow rates for vessels in which Q was not measured. Q T = Q M /%S T X. * Significantly different from normal by nonpaired student t-test. Downloaded From: on 09/23/18
5 360 INVESTIGATIVE OPHTHALMOLOGY 6 VISUAL SCIENCE / February 1992 Vol. 33 Table. Average venous diameter (D), maximum erythrocyte velocity (V max ), and retinal volumetric blood flow (Q) in the largest retinal vein of diabetic patients and normal subjects D( M m) V max (cm/sec) Q Oil/min) Normal (n = 12) 166 ± 13f 1.77 ± ± 2.6 = not statistically significant. * Nonpaired student t-test. tsd. Diabetes (n = 18) Significance* 179 ± 1.72 ± ±3.9 N.S. N.S. N.S. = 0.019, by unpaired student's t-test). Whereas Q decreased by ± 9% during hyperoxia in normal subjects, it decreased by only 6 ± 11% in diabetic patients. Patients with more advanced retinopathy showed smaller regulatory responses (Fig. 3), as demonstrated by the significant correlation present between R and retinopathy level (Spearman's rank correlation coefficient = 0.2, P < 0.0). Although average R for patients with mild retinopathy (level ) was smaller than normal (9 ± 11%), the difference was not statistically significant. No significant correlation was found between Q T and retinopathy level (Spearman's rank correlation coefficient = 0.01, In 16 diabetic patients, measurements of Q and R in one of the major temporal veins were repeated a few weeks later. The average percentage change in Q between the two measurements was 2.8 ± 12%. The difference in R between the two measurements (R 2 (%) - R,(%)) was 1.9 ± 7.7%. The distribution of Q in different areas of the retina is shown in Table. On average, Q was significantly larger in the temporal retina than in the nasal retina Table. Average of the sum of the venous volumetric flow rate, Q Oul/min), in the temporal, nasal, superior, and inferior regions of the retina Temporal retina Nasal retina Significancef Superior hemiretina Inferior hemiretina Significance! Normal Diabetes (n = 12) (n = 18) Significance* 2.0 ± ±6.2 P = ± ± ± ±7.0 P = ± ±6.3 P = 0.03 P = 0.00 = not statistically significant. * Nonpaired t-test comparing flow in normal subjects and diabetic patients. f Paired t-test comparing flow in the temporal and nasal or the superior and inferior retina. by 9% in normal eyes (P = ) and by 83% in the diabetic eyes (P = ). In addition, Q in the superior retina was significantly larger than that observed in the inferior retina in diabetic eyes (P = 0.03). In normal subjects, however, this difference was not statistically significant (P = 0.8). When normal subjects and diabetic patients were grouped together, Q was also significantly larger in the superior retina than in the inferior retina (P = 0.02). We attempted to estimate total volumetric blood flow rate from blood flow measurements obtained in only one major retinal vein and from the total venous cross-section using the following two procedures: (1) Q was measured in the largest vein and scaled by a factor consisting of the total venous cross-section/ largest vein cross-section (the result was defined as Qnaisest) or (2) Q was measured in the second largest vein and scaled by a factor consisting of the total venous cross-section/second largest vein cross-section (QTsecond largest)- Both Q Tlargesl and Q Ts econd largest Were On average about 1% larger than Q T both in normal and diabetic eyes (Table 6). In addition, a highly significant correlation was found between Q T and Qriargest (r J Retinopathy Level 0 Fig. 3. Relationship between the retinal vascular regulatory response to % oxygen breathing (R) and retinopathy level of the study eye. Spearman's Rank Correlation, r s = 0.2, P < 0.0. Average R in normal subjects was % ± 9%. Table 6. Average corrected total volumetric blood flow (Q T ) and estimated total volumetric blood flow rates from the largest (QriargestX an d the second largest (Q Tsecond largest) retinal vein Normal eyes Diabetic eyes Qr (nl/min) 38.1 ±6.2* 7.0 ± 9.7 \ctlargest (fil/min) 3.1 ±9..6 ± 13.0 \J-Tsecond largest (nl/min) 3. ± 8.9. ± 13.6 QTUIJCSV Estimated total volumetric blood flow from Q measured in the largest vein scaled by a factor Total Venous Cross-Section/Largest Vein Cross-Section. QTsecond iarsrai : Estimated total volumetric blood flow from Q measured in the second largest vein scaled by a factor Total Venous Cross-Section/Second Largest Vein Cross-Section. *SD. Downloaded From: on 09/23/18
6 No. 2 TOTAL RETINAL BLOOD FLOW IN DIABETES / Grunwold er ol 361 = 0.89, P = , with a linear-regression equation of Q T = Q Tlargest ) or Q Ts econd u^est (X = 0.87, P = , with a linear-regression equation of Q T = Q Tsecond lareest ). Discussion We attempted to measure total retinal venous blood flow in patients with poorly controlled diabetes mellitus and background diabetic retinopathy. Our results suggest that, in these patients, total retinal volumetric blood flow rate is significantly larger than normal by approximately 23% (Table 6). Measurements obtained in the largest retinal vein in each eye showed an average Q that was only 12% higher than normal, and this difference was not statistically significant (Table ). This was similar to the results in our previous study, 8 in which average Q obtained in a single retinal vessel of patients with background retinopathy was approximately 8% above normal (also not statistically significant). The results of our current study also show largerthan-normal veins in diabetic patients (Table 3), a finding that agreed with previous reports demonstrating vasodilatation in diabetic patients. 818 Both Q T and S T were already significantly larger than normal in the nine patients with the mildest form of retinopathy (level ). However, V max was not significantly different from normal in poorly controlled diabetic patients with background retinopathy (Table ). These results differed from those in our previous study 8 in which a decrease in average V max of 18% was observed in eyes with background diabetic retinopathy. There were important differences between the two studies that might explain the discrepancy in V max results. In our current investigation, most of the patients had mild retinopathic changes (Fig. 3); in our previous study, 8 approximately one half of the subjects had severe background retinopathy. Because V ma x seems to decrease with disease progression, 8 a more prevalent presence of severe background retinopathy could be related to the lower than normal V max value found in our previous study. In our current study, we selected only type I diabetic patients with poor glycemic control. Most of the patients had GHb levels that were three standard deviations or more higher than the mean for nondiabetic subjects. In our previous study, GHb levels were not measured, and no attempt was made to select patients specifically with poor control. It is possible that patients with poor glycemic control could have a higher V max than those with better control. This hypothesis was supported by our previous article, 9 showing that in very poorly controlled diabetic patients during marked hyperglycemia, V max is significantly above normal and that normalization of blood glucose with insulin administration results in significant decreases in Q and V max. We stress, however, that the actual blood glucose levels at the time offlowmeasurements in our current study were, on average, close to those observed in our previous one. 8 Further studies are needed to clarify the importance of the influences on the retinal circulation of chronically elevated blood glucose levels versus acutely elevated blood glucose levels. As shown by our results, total retinal volumetric blood flow was significantly larger than normal in patients with poorly controlled diabetes mellitus and background retinopathy. This increase was caused mainly by vasodilatation, which probably constitutes a regulatory response of the retinal vasculature attempting to normalize a reduced supply of nutrients or an increased concentration of metabolic waste products in the retinal tissue. The average r between Q and D in diabetic patients was significantly smaller than that observed in normal subjects. Moreover, among diabetic patients, there was also a greater heterogeneity in r values, as demonstrated by a larger standard deviation. The reason for this effect was not clear, but the changes in retinal architecture and/or blood rheology, known to occur in patients with diabetic retinopathy, might alter the normal relationship between Q and D, leading to a weaker or perhaps different association between these parameters. We found no correlation, however, between the r values and retinopathy level or disease duration, and therefore, we could not conclude that more advanced diabetic pathology is associated with a weaker correlation between Q and D. In our previous study, in which measurements were obtained in a single major retinal vein of each eye, a large variability in Q was found in diabetic (12.3 =h. iul/min) and normal (11.3 ± 3. ^1/min) eyes. 8 This variability mainly was related to the differences in D of the veins measured and the retinal areas perfused by these vessels. Because of this variability, the sensitivity of the technique to detect differences in Q between groups of patients was approximately 23%, ie, only changes larger than 23% could be demonstrated in that study. In our current study, we estimated Q T by adding the flows measured in the four to five largest retinal veins and estimating theflowsin the few vessels in which Q could not be measured. The variability in Q T between subjects was smaller than that observed for the largest retinal veins (Table ) and than seen in our previous study. 8 This intersubject variability in Q T may be explained by the variability in S T because both quantities correlate significantly in diabetic patients (P Downloaded From: on 09/23/18
7 362 INVESTIGATIVE OPHTHALMOLOGY & VISUAL SCIENCE / February 1992 Vol. 33 = 0.0) and normal subjects (P = ). Although total retinal flow was significantly larger than normal in the diabetic eyes, the difference in flow in the larger retinal vein was not statistically significant. From determinations of Q obtained a few weeks apart in each of 16 diabetic subjects, we calculated that our technique had a sensitivity of approximately 10%. Thus, we could detect an average change in Q of 10% or larger {P < 0.01, by two-tailed paired student t-test). Two determinations of R done a few weeks apart in 16 diabetic patients showed an average difference in R (R 2 (%) - R,(%)) of 1.9 ± 7.7%. From these values, we determined that our technique had a sensitivity to detect average changes in R of approximately 6% (P < 0.01, by two-tailed paired student t-test), when applied as described in a group of 16 diabetic patients. These values are important for the design of experimental protocols to study the effects of disease or treatments on retinal hemodynamics. We found R was significantly reduced in diabetic patients, as reported previously. 6 In addition, the significant decrease in R with progression of background diabetic retinopathy (Fig. 3) further strengthened our previous hypothesis that the decreased vascular regulatory response to hyperoxia may be related to the degree of retinal hypoxia. 6-9 " 11 Measurements of Q T are laborious and time consuming because determinations of V max must be made separately in each individual major retinal vein. In large-scale clinical studies, it may not be possible to do all these measurements. We attempted to estimate Q T from the measurement of Q obtained in the largest or second largest retinal vein and S-r (Table 6). This estimation was close to the actual value (higher by 1%, on average), and furthermore, there was a strong correlation between these quantities, suggesting that this method may provide a rough estimation of total retinal flow when actual total flow cannot be measured. Average total retinal volumetric bloodflowsin normal subjects were close to the average of 3 ± 6.3 /zl/min reported previously 1 in seven normal eyes. Retinal volumetric bloodflowrates in individual major retinal veins were also similar to those reported previously by our laboratory. 8 These values of total volumetricflow,however, are about 0% smaller than those reported by others 19 using laser Doppler velocimetry. The exact source of this discrepancy has not been identified and probably stems from differences in the way the technique was used. The significantly larger Q observed in the temporal retina than in the nasal retina of normal subjects agreed with previous results. 119 A similar difference also was found in our study in diabetic patients (Table ). These differences can be explained by the larger area of the temporal retina. In addition, increased retinal thickness and perhaps an increased metabolic rate in the macular region also may explain this finding. By comparison with the inferior retina, the superior retina showed a significantly larger Q when normal subjects and diabetic patients were grouped together. The inferior visual field is larger than the superior visualfield. In addition, the fovea is located slightly below the center of the optic nerve head. 21 These two facts suggest that there may be a physiologic explanation for the differences in flow observed between the superior and inferior retina. Our results suggest that Q varies with D at a power of 2.87 in normal eyes and 2.67 in eyes of diabetic patients (Figs. 1, 2). The difference between these two values was not statistically significant, and therefore, we cannot conclude at this time that diabetes mellitus affects this factor. A vascular tissue in which Q varies with D at a power of 3 is the ideal system in terms of the amount of energy needed to push blood through the vessels. 22 Any change from 3 represents a departure from the ideal situation. Key words: retinal volumetric bloodflow,laser Doppler velocimetry, diabetic retinopathy, vascular regulation, erythrocyte velocity, hyperoxia Acknowledgments The authors thank Sharon Grunwald and Jim Gowan for statistical consultation and analysis of the data and Dolly A. Scott for preparation of this manuscript. References 1. Hickam JB and Sieker HO: Retinal vascular reactivity in patients with diabetes mellitus and with atherosclerosis. Circulation 22:23, Kohner EM, Hamilton AM, Saunders SJ, Sutcliffe BA, and Bulpitt CJ: The retinal blood flow in diabetes. Diabetologia 11:27, Blair NP, Feke GT, Morales-Stoppello J, Riva CE, Goger DG, Collas G, and McMeel JW: Prolongation of retinal mean circulation time in diabetes. Arch Ophthalmol :76, Sinclair SH, Grunwald JE, Riva CE, Braunstein SN, Nichols CW, and Schwartz SS: Retinal vascular autoregulation in diabetes mellitus. Ophthalmology 89:78, Yoshida A, Feke GT, Morales-Stoppello J, Collas GD, Goger DG, and McMeel JW: Retinal blood flow alterations during progression of diabetic retinopathy. Arch Ophthalmol 101:22, Grunwald JE, Riva CE, Brucker AJ, Sinclair SH, and Petrig BL: Altered retinal vascular response to % oxygen breathing in diabetes mellitus. Ophthalmology 91:17, Feke GT, Tagawa G, Yoshida A, Goger DG, Weiter J, Buzney SM, and McMeel JW: Retinal circulatory changes related to retinopathy progression in insulin-dependent diabetes mellitus. Ophthalmology 92:117, Grunwald JE, Riva CE, Sinclair SH, Brucker AJ, and Petrig BL: Laser Doppler velocimetry study of retinal circulation in diabetes mellitus. Arch Ophthalmol 10:991, Downloaded From: on 09/23/18
8 No. 2 TOTAL RETINAL DLOOD FLOW IN DIABETES / Grunwold er ol Grunwald JE, Riva CE, Martin DB, Quint AR, and Epstein PA: Effect of insulin-induced decrease in blood glucose on the human diabetic retinal circulation. Ophthalmology 9:161, Grunwald JE, Brucker AJ, Petrig BL, and Riva CE: Retinal blood flow regulation and the clinical response to panretinal photocoagulation in proliferative diabetic retinopathy. Ophthalmology 96:118, Grunwald JE, Brucker AJ, Schwartz SS, Braunstein SN, Baker L, Petrig BL, and Riva CE: Diabetic glycemic control and retinal blood flow. Diabetes 39:602, Riva CE, Petrig BL, and Grunwald JE: Retinal blood flow. In Laser Doppler Flowmetry, Shepherd AP and Oberg PA, editors. Boston, KJuwer Academic, 1990, pp Chase HP, Jackson WE, Hoops SL, Cockerham RS, Archer PG, and O'Brien D: Glucose control and the renal and retinal complications of insulin-dependent diabetes. JAMA 261:11, Klein BE, Moss SE, and Klein R: Longitudinal increase of glycemic control and diabetic retinopathy. Diabetes Care 10:273, Riva CE, Grunwald JE, Sinclair SH, and Petrig BL: Blood velocity and volumetricflowrate in human retinal vessels. Invest Ophthalmol Vis Sci 26:112, Sliney DH and Freasier BL: Evaluation of optical radiation hazards. Applied Optics 12:1, Damon DN and Duling BR: A comparison between mean blood velocities and center-line red cell velocities as measured with a mechanical image streaking velocimeter. Microvasc Res 17:330, Skovborg F, Nielsen A, Lauritzen E, and Hartkopp D: Diameter of retinal vessels in diabetic and normal subjects. Diabetes, 18:292, Feke GT, Tagawa H, Deupree DM, Goger DG, Sebag J, and Weiter J: Bloodflowin the normal human retina. Invest Ophthalmol Vis Sci 30:8, Anderson DR: Perimetry With and Without Automation. St. Louis, CV Mosby, 1987, pp Bishop PO: Binocular vision. In Adler's Physiology of the Eye, Moses RA, editor. St. Louis, CV Mosby, 197, p Mayrovitz HN and Roy J: Microvascular bloodflow:evidence indicating a cubic dependence on arteriolar diameter. Am J Physiol2:H1013, Downloaded From: on 09/23/18
Retinal Hemodynamics in Proliferative Diabetic Retinopathy A Laser Doppler Velocimetry Study
 Retinal Hemodynamics in Proliferative Diabetic Retinopathy A Laser Doppler Velocimetry Study Juan E. Grunwald, Alexander J. Brucker, Sharon E. Grunwald, and Charles E. Riva Purpose. This study investigated
Retinal Hemodynamics in Proliferative Diabetic Retinopathy A Laser Doppler Velocimetry Study Juan E. Grunwald, Alexander J. Brucker, Sharon E. Grunwald, and Charles E. Riva Purpose. This study investigated
Effects of Oxygen and Carbon Dioxide on Human Retinal Circulation
 Effects of ygen and on Dioxide on Human Retinal Circulation Stephen]. Pakola and Juan E. Grunwald Purpose. ogen, a gas mixture of 95% O 2 and 5% CO 2, is given to patients with retinal artery obstruction
Effects of ygen and on Dioxide on Human Retinal Circulation Stephen]. Pakola and Juan E. Grunwald Purpose. ogen, a gas mixture of 95% O 2 and 5% CO 2, is given to patients with retinal artery obstruction
Effect of Timolol Maleate on the Retinal Circulation of Human Eyes with Ocular Hypertension
 Investigative Ophthalmology & Visual Science, Vol. 31, No. 3, March 1990 Copyright Association for Research in Vision and Ophthalmology Effect of Maleate on the Retinal Circulation of Human Eyes with Ocular
Investigative Ophthalmology & Visual Science, Vol. 31, No. 3, March 1990 Copyright Association for Research in Vision and Ophthalmology Effect of Maleate on the Retinal Circulation of Human Eyes with Ocular
Retinal circulation during a spontaneous rise of intraocular pressure
 British Journal of Ophthalmology, 1988, 72, 75-758 Retinal circulation during a spontaneous rise of intraocular pressure JUAN E GRUNWALD, CHARLES E RIVA AND DAVID M KOZART From the Scheie Eye Institute,
British Journal of Ophthalmology, 1988, 72, 75-758 Retinal circulation during a spontaneous rise of intraocular pressure JUAN E GRUNWALD, CHARLES E RIVA AND DAVID M KOZART From the Scheie Eye Institute,
Laser Doppler Velocimefry Study of the Effect of Pure Oxygen Breathing on Retinal Blood Flow
 Laser Doppler Velocimefry Study of the Effect of Pure Oxygen Breathing on Retinal Blood Flow C. E. Riva, J. E. Grunwald,* and S. H. Sinclair The noninvasive Laser Doppler Velocimetry (LDV) technique was
Laser Doppler Velocimefry Study of the Effect of Pure Oxygen Breathing on Retinal Blood Flow C. E. Riva, J. E. Grunwald,* and S. H. Sinclair The noninvasive Laser Doppler Velocimetry (LDV) technique was
Strict control of glycaemia: effects on blood flow
 British Journal of Ophthalmology 1995; 79: 735-741 Department of Ophthalmology, Scheie Eye Institute, Philadelphia, USA J E Grunwald C E Riva B L Petrig A J Brucker J DuPont S Grunwald Department of Medicine,
British Journal of Ophthalmology 1995; 79: 735-741 Department of Ophthalmology, Scheie Eye Institute, Philadelphia, USA J E Grunwald C E Riva B L Petrig A J Brucker J DuPont S Grunwald Department of Medicine,
Retinal vessel dilatation and elongation precedes diabetic macular oedema
 274 Department of Ophthalmology, University of Iceland, Landakotsspítali, Reykjavík, Iceland K Kristinsson M S Gottfredsdóttir E Stefánsson Correspondence to: Einar Stefánsson, MD, PhD, University of Iceland,
274 Department of Ophthalmology, University of Iceland, Landakotsspítali, Reykjavík, Iceland K Kristinsson M S Gottfredsdóttir E Stefánsson Correspondence to: Einar Stefánsson, MD, PhD, University of Iceland,
Blood Velocity ond Volumetric Flow Rote in Humon Retinal Vessels
 Blood Velocity ond Volumetric Flow Rote in Humon Retinal Vessels Charles E. Riva, Juan E. Grunwald, Stephen H. Sinclair, and Benno L. Perrig The distributions of blood velocity and volumetric flow rate
Blood Velocity ond Volumetric Flow Rote in Humon Retinal Vessels Charles E. Riva, Juan E. Grunwald, Stephen H. Sinclair, and Benno L. Perrig The distributions of blood velocity and volumetric flow rate
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Retinal blood flow in type 1 diabetes patients with no or mild diabetic retinopathy during euglycemic clamp
 Diabetes Care Publish Ahead of Print, published online June 28, 2010 Retinal blood flow in type 1 diabetes patients with no or mild diabetic retinopathy during euglycemic clamp Berthold Pemp MD 1, Elżbieta
Diabetes Care Publish Ahead of Print, published online June 28, 2010 Retinal blood flow in type 1 diabetes patients with no or mild diabetic retinopathy during euglycemic clamp Berthold Pemp MD 1, Elżbieta
Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
Abnormalities of the retinal veins are. loops and reduplications in diabetic retinopathy. Prevalence, distribution, and pattern of development
 Venous loops and reduplications in diabetic retinopathy Prevalence, distribution, and pattern of development Toke Bek Department of Ophthalmology, Århus University Hospital, DK-8000 Århus C, Denmark ABSTRACT.
Venous loops and reduplications in diabetic retinopathy Prevalence, distribution, and pattern of development Toke Bek Department of Ophthalmology, Århus University Hospital, DK-8000 Århus C, Denmark ABSTRACT.
Reduced response of retinal vessel diameters to flicker stimulation in patients with diabetes
 887 SCIENTIFIC REPORT Reduced response of retinal vessel diameters to flicker stimulation in patients with diabetes G Garhöfer, C Zawinka, H Resch, P Kothy, L Schmetterer, G T Dorner... Background/aim:
887 SCIENTIFIC REPORT Reduced response of retinal vessel diameters to flicker stimulation in patients with diabetes G Garhöfer, C Zawinka, H Resch, P Kothy, L Schmetterer, G T Dorner... Background/aim:
Retinal Blood Flow Changes in Patients With Insulin- Dependent Diabetes Mellitus and No Diabetic Retinopathy
 Retinal Blood Flow Changes in Patients With Insulin- Dependent Diabetes Mellitus and No Diabetic Retinopathy A Video Fluorescein Angiography Study Sven-Erik Bursell,* Allen C. Clermont* Brendan T. Kinsley,f
Retinal Blood Flow Changes in Patients With Insulin- Dependent Diabetes Mellitus and No Diabetic Retinopathy A Video Fluorescein Angiography Study Sven-Erik Bursell,* Allen C. Clermont* Brendan T. Kinsley,f
CLINICAL SCIENCES. The Effect of Ocular Warming on Ocular Circulation in Healthy Humans 1-3 RECENTLY
 The Effect of Ocular Warming on Ocular Circulation in Healthy Humans Taiji Nagaoka, MD, PhD; Akitoshi Yoshida, MD, PhD CLINICAL SCIENCES Objective: To examine the effect of ocular warming on retinal blood
The Effect of Ocular Warming on Ocular Circulation in Healthy Humans Taiji Nagaoka, MD, PhD; Akitoshi Yoshida, MD, PhD CLINICAL SCIENCES Objective: To examine the effect of ocular warming on retinal blood
Diabetes Care 24: , 2001
 Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
Diffuse luminance flicker increases blood flow in major retinal arteries and veins
 Vision Research 44 (2004) 833 838 www.elsevier.com/locate/visres Diffuse luminance flicker increases blood flow in major retinal arteries and veins G. Garh ofer a,b, C. Zawinka a, H. Resch a, K.H. Huemer
Vision Research 44 (2004) 833 838 www.elsevier.com/locate/visres Diffuse luminance flicker increases blood flow in major retinal arteries and veins G. Garh ofer a,b, C. Zawinka a, H. Resch a, K.H. Huemer
Retinal vessel calibre and micro- and macrovascular complications in type 1 diabetes
 Diabetologia (2009) 52:2213 2217 DOI 10.1007/s00125-009-1459-8 SHORT COMMUNICATION Retinal vessel calibre and micro- and macrovascular complications in type 1 diabetes J. Grauslund & L. Hodgson & R. Kawasaki
Diabetologia (2009) 52:2213 2217 DOI 10.1007/s00125-009-1459-8 SHORT COMMUNICATION Retinal vessel calibre and micro- and macrovascular complications in type 1 diabetes J. Grauslund & L. Hodgson & R. Kawasaki
N umerous techniques have shown vascular abnormalities
 1487 EXTENDED REPORT Association between lower optic nerve laser Doppler blood volume measurements and glaucomatous visual field progression J M Zink, J E Grunwald, J Piltz-Seymour, A Staii, J Dupont...
1487 EXTENDED REPORT Association between lower optic nerve laser Doppler blood volume measurements and glaucomatous visual field progression J M Zink, J E Grunwald, J Piltz-Seymour, A Staii, J Dupont...
Intravenous Nicardipine in Cats Increases Optic Nerve Head But Not Retinal Blood Flow
 Investigative Ophthalmology & Visual Science, Vol. 33, No. 10, September 1992 Copyright Association for Research in Vision and Ophthalmology Intravenous Nicardipine in Cats Increases Optic Nerve Head But
Investigative Ophthalmology & Visual Science, Vol. 33, No. 10, September 1992 Copyright Association for Research in Vision and Ophthalmology Intravenous Nicardipine in Cats Increases Optic Nerve Head But
New vessel formation in retinal branch vein occlusion
 Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
The retinal renin-angiotensin system: implications for therapy in diabetic retinopathy
 (2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
(2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion
 Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
The Effect of Caffeine on the Human Macular Circulation
 Investigative Ophthalmology & Visual Science, Vol. 32, o. 12, ovember 1991 opyright Association for Research in Vision and Ophthalmology The Effect of affeine on the Human Macular irculation Karan Lotfi
Investigative Ophthalmology & Visual Science, Vol. 32, o. 12, ovember 1991 opyright Association for Research in Vision and Ophthalmology The Effect of affeine on the Human Macular irculation Karan Lotfi
Real-Time Blood Velocity Measurements in Human Retinal Vein Using the Laser Speckle Phenomenon
 Real-Time Blood Velocity Measurements in Human Retinal Vein Using the Laser Speckle Phenomenon Miyuki Nagahara,* Yasuhiro Tamaki, Makoto Araie* and Hitoshi Fujii *Department of Ophthalmology, University
Real-Time Blood Velocity Measurements in Human Retinal Vein Using the Laser Speckle Phenomenon Miyuki Nagahara,* Yasuhiro Tamaki, Makoto Araie* and Hitoshi Fujii *Department of Ophthalmology, University
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Reproducibility of Scanning Laser Doppler Flowmetry in the Rat Retina and Optic Nervehead
 Reproducibility of Scanning Laser Doppler Flowmetry in the Rat Retina and Optic Nervehead Akitaka Tsujikawa,* Junichi Kiryu,* Atsushi Nonaka,* Kenji Yamashiro,* Yuichiro Ogura and Yoshihito Honda* *Department
Reproducibility of Scanning Laser Doppler Flowmetry in the Rat Retina and Optic Nervehead Akitaka Tsujikawa,* Junichi Kiryu,* Atsushi Nonaka,* Kenji Yamashiro,* Yuichiro Ogura and Yoshihito Honda* *Department
Optic Disc Cupping: Four Year Follow-up from the WESDR
 Investigative Ophthalmology & Visual Science, Vol. 30, o., February 989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Four Year Follow-up from the WER Barbara E. K.
Investigative Ophthalmology & Visual Science, Vol. 30, o., February 989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Four Year Follow-up from the WER Barbara E. K.
Retinal blood flow reduction after panretinal photocoagulation in Type 2 diabetes mellitus: Doppler optical coherence tomography flowmeter pilot study
 RESEARCH ARTICLE Retinal blood flow reduction after panretinal photocoagulation in Type 2 diabetes mellitus: Doppler optical coherence tomography flowmeter pilot study Youngseok Song ID 1 *, Tomofumi Tani
RESEARCH ARTICLE Retinal blood flow reduction after panretinal photocoagulation in Type 2 diabetes mellitus: Doppler optical coherence tomography flowmeter pilot study Youngseok Song ID 1 *, Tomofumi Tani
Retinal tissue has an intrinsic ability to maintain a relatively
 Special Issue Retinal Blood Flow Response to Hyperoxia Measured With En Face Doppler Optical Coherence Tomography Alex D. Pechauer, Ou Tan, Liang Liu, Yali Jia, Vivian Hou, William Hills, and David Huang
Special Issue Retinal Blood Flow Response to Hyperoxia Measured With En Face Doppler Optical Coherence Tomography Alex D. Pechauer, Ou Tan, Liang Liu, Yali Jia, Vivian Hou, William Hills, and David Huang
Visual fields in diabetic retinopathy
 Brit. J. Ophthal. (I97I) 55, I83 Visual fields in diabetic retinopathy K. I. WISZNIA, T. W. LIEBERMAN, AND I. H. LEOPOLD From the Department of Ophthalmology, Mount Sinai School of Medicine, City University
Brit. J. Ophthal. (I97I) 55, I83 Visual fields in diabetic retinopathy K. I. WISZNIA, T. W. LIEBERMAN, AND I. H. LEOPOLD From the Department of Ophthalmology, Mount Sinai School of Medicine, City University
Retinal Blood Flow Changes During Pregnancy in Women With Diabetes
 Retinal Blood Flow Changes During Pregnancy in Women With Diabetes H. C. Chen,* R. S. B. Newsom,* V. Patel,* J. Cassar,\ H. Mather,\ and E. M. Kohner* Purpose. To study retinal blood flow (RBF) during
Retinal Blood Flow Changes During Pregnancy in Women With Diabetes H. C. Chen,* R. S. B. Newsom,* V. Patel,* J. Cassar,\ H. Mather,\ and E. M. Kohner* Purpose. To study retinal blood flow (RBF) during
Study of 189 Cases of Diabetic Retinopathy at CMC Larkana
 Original Article Study of 189 Cases of Diabetic Retinopathy at CMC Larkana Shahid Jamal Siddiqui, Sayed Imtiaz Ali Shah, Abdul Qadir Shaikh, Mohammed Yousuf Depar, Safder Ali Abbassi Pak J Ophthalmol 2007,
Original Article Study of 189 Cases of Diabetic Retinopathy at CMC Larkana Shahid Jamal Siddiqui, Sayed Imtiaz Ali Shah, Abdul Qadir Shaikh, Mohammed Yousuf Depar, Safder Ali Abbassi Pak J Ophthalmol 2007,
Factors Associated with Visual Outcome after Photocoagulation for Diabetic Retinopathy
 Investigative Ophthalmology & Visual Science, Vol. 30, No. 1, January 1989 Copyright Association for Research in Vision and Ophthalmology Factors Associated with Visual Outcome after Photocoagulation for
Investigative Ophthalmology & Visual Science, Vol. 30, No. 1, January 1989 Copyright Association for Research in Vision and Ophthalmology Factors Associated with Visual Outcome after Photocoagulation for
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Use of Scanning Laser Ophthalmoscope Microperimetry in Clinically Significant Macular Edema in Type 2 Diabetes Mellitus
 Use of Scanning Laser Ophthalmoscope Microperimetry in Clinically Significant Macular Edema in Type 2 Diabetes Mellitus Fumihiko Mori, Satoshi Ishiko, Norihiko Kitaya, Taiichi Hikichi, Eiichi Sato, Akira
Use of Scanning Laser Ophthalmoscope Microperimetry in Clinically Significant Macular Edema in Type 2 Diabetes Mellitus Fumihiko Mori, Satoshi Ishiko, Norihiko Kitaya, Taiichi Hikichi, Eiichi Sato, Akira
BLOOD VESSEL DIAMETER MEASUREMENT ON RETINAL IMAGE
 Journal of Computer Science 10 (5): 879-883, 2014 ISSN: 1549-3636 2014 doi:10.3844/jcssp.2014.879.883 Published Online 10 (5) 2014 (http://www.thescipub.com/jcs.toc) BLOOD VESSEL DIAMETER MEASUREMENT ON
Journal of Computer Science 10 (5): 879-883, 2014 ISSN: 1549-3636 2014 doi:10.3844/jcssp.2014.879.883 Published Online 10 (5) 2014 (http://www.thescipub.com/jcs.toc) BLOOD VESSEL DIAMETER MEASUREMENT ON
Hyperglycemia affects flicker-induced vasodilation in the retina of healthy subjects
 Vision Research 43 (2003) 1495 1500 www.elsevier.com/locate/visres Hyperglycemia affects flicker-induced vasodilation in the retina of healthy subjects Guido T. Dorner a,b, Gerhard Garh ofer a, Karl H.
Vision Research 43 (2003) 1495 1500 www.elsevier.com/locate/visres Hyperglycemia affects flicker-induced vasodilation in the retina of healthy subjects Guido T. Dorner a,b, Gerhard Garh ofer a, Karl H.
Diabetic Maculopathy in Nonproliferative Diabetic Retinopathy in Tertiary Eye Care Hospital in India: A Prospective Nonrandomized Clinical Study
 Original Article Print ISSN: 3-639 Online ISSN: 3-595X DOI: 0.35/ijss/0/ Diabetic Maculopathy in Nonproliferative Diabetic Retinopathy in Tertiary Eye Care Hospital in India: A Prospective Nonrandomized
Original Article Print ISSN: 3-639 Online ISSN: 3-595X DOI: 0.35/ijss/0/ Diabetic Maculopathy in Nonproliferative Diabetic Retinopathy in Tertiary Eye Care Hospital in India: A Prospective Nonrandomized
Optic Disc Cupping: Prevalence Findings from the WESDR
 Investigative Ophthalmology & Visual Science, Vol., o. 2, February 1989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Prevalence Findings from the WER Barbara E. K.
Investigative Ophthalmology & Visual Science, Vol., o. 2, February 1989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Prevalence Findings from the WER Barbara E. K.
Foveolar Choroidal Circulation and Choroidal Neovascularization in Age-Related Macular Degeneration
 Foveolar Choroidal Circulation and Choroidal Neovascularization in Age-Related Macular Degeneration Tatyana I. Metelitsina, Juan E. Grunwald, Joan C. DuPont, Gui-Shuang Ying, Alexander J. Brucker, and
Foveolar Choroidal Circulation and Choroidal Neovascularization in Age-Related Macular Degeneration Tatyana I. Metelitsina, Juan E. Grunwald, Joan C. DuPont, Gui-Shuang Ying, Alexander J. Brucker, and
DR as a Biomarker for Systemic Vascular Complications
 DR as a Biomarker for Systemic Vascular Complications Lihteh Wu MD Asociados de Mácula, Vítreo y Retina de Costa Rica San José, Costa Rica LW65@cornell.edu Disclosures Dr Wu has received lecture fees from
DR as a Biomarker for Systemic Vascular Complications Lihteh Wu MD Asociados de Mácula, Vítreo y Retina de Costa Rica San José, Costa Rica LW65@cornell.edu Disclosures Dr Wu has received lecture fees from
Predictors of postoperative bleeding after vitrectomy for vitreous hemorrhage in patients with diabetic retinopathy
 ORIGINAL ARTICLE Predictors of postoperative bleeding after vitrectomy for vitreous hemorrhage in patients with diabetic retinopathy Saori Motoda 1, Nobuhiko Shiraki 2, Takuma Ishihara 3, Hirokazu Sakaguchi
ORIGINAL ARTICLE Predictors of postoperative bleeding after vitrectomy for vitreous hemorrhage in patients with diabetic retinopathy Saori Motoda 1, Nobuhiko Shiraki 2, Takuma Ishihara 3, Hirokazu Sakaguchi
Retinal Hemodynamic Effects of Carbon Dioxide, Hyperoxia, and Mild Hypoxia
 Investigative Ophthalmology & Visual Science, Vol. 33, No. 6, May 1992 Copyright Association for Research in Vision and Ophthalmology Retinal Hemodynamic Effects of Carbon Dioxide, Hyperoxia, and Mild
Investigative Ophthalmology & Visual Science, Vol. 33, No. 6, May 1992 Copyright Association for Research in Vision and Ophthalmology Retinal Hemodynamic Effects of Carbon Dioxide, Hyperoxia, and Mild
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Fluctuations on the Humphrey and Octopus Perimeters
 May 987 Vol. 28/ Investigative Ophthalmology & Visual Science A Journal of Dosic and Clinical Research Articles Fluctuations on the and Perimeters Randall S. Drenton and William A. Argus Fluctuation of
May 987 Vol. 28/ Investigative Ophthalmology & Visual Science A Journal of Dosic and Clinical Research Articles Fluctuations on the and Perimeters Randall S. Drenton and William A. Argus Fluctuation of
THE PREVALENCE OF CAUSES FOR DIABETIC RETINOPATHY USING MATHEMATICAL MODELS
 International Journal of Advanced Research in Engineering and Technology (IJARET) Volume 9, Issue 6, November-December 2018, pp. 167 171, Article ID: IJARET_09_06_017 Available online at http://www.iaeme.com/ijaret/issues.asp?jtype=ijaret&vtype=9&itype=6
International Journal of Advanced Research in Engineering and Technology (IJARET) Volume 9, Issue 6, November-December 2018, pp. 167 171, Article ID: IJARET_09_06_017 Available online at http://www.iaeme.com/ijaret/issues.asp?jtype=ijaret&vtype=9&itype=6
Diabetologia 9 by Springer-Verlag 1978
 Diabetologia 15, 105-111 (1978) Diabetologia 9 by Springer-Verlag 1978 Diabetic Retinopathy and Pregnancy J. Cassar, Eva M. Kohner, A. M. Hamilton, H. Gordon 1, and G. F. Joplin The Endocrine Unit and
Diabetologia 15, 105-111 (1978) Diabetologia 9 by Springer-Verlag 1978 Diabetic Retinopathy and Pregnancy J. Cassar, Eva M. Kohner, A. M. Hamilton, H. Gordon 1, and G. F. Joplin The Endocrine Unit and
Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus
 Original article: Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus 1Dr Apoorva*, 2 Dr Sabhia Jan 1Senior Resident, 2
Original article: Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus 1Dr Apoorva*, 2 Dr Sabhia Jan 1Senior Resident, 2
MATERIALS AND METHODS
 Automated Detection of Diabetic Retinopathy in a Fundus Photographic Screening Population Nicolai Larsen, 1,2 Jannik Godt, 3 Michael Grunkin, 3 Henrik Lund-Andersen, 1,2 and Michael Larsen 1 PURPOSE. To
Automated Detection of Diabetic Retinopathy in a Fundus Photographic Screening Population Nicolai Larsen, 1,2 Jannik Godt, 3 Michael Grunkin, 3 Henrik Lund-Andersen, 1,2 and Michael Larsen 1 PURPOSE. To
Diffuse luminance flicker increases retinal vessel diameter in humans
 Current Eye Research Diffuse luminance flicker increases retinal vessel diameter in humans F. Formaz 1, C. E. Riva 1,2 and M. Geiser 1,3 1 Institut de Recherche en Ophtalmologie, Sion, 2 Medical School
Current Eye Research Diffuse luminance flicker increases retinal vessel diameter in humans F. Formaz 1, C. E. Riva 1,2 and M. Geiser 1,3 1 Institut de Recherche en Ophtalmologie, Sion, 2 Medical School
Association of Retinal Vessel Caliber to Optic Disc and Cup Diameters. Kristine E. Lee, Barbara Eden Kobrin Klein, Ronald Klein, and Stacy M.
 Association of Retinal Vessel Caliber to Optic Disc and Cup Diameters Kristine E. Lee, Barbara Eden Kobrin Klein, Ronald Klein, and Stacy M. Meuer PURPOSE. To investigate whether optic disc size is related
Association of Retinal Vessel Caliber to Optic Disc and Cup Diameters Kristine E. Lee, Barbara Eden Kobrin Klein, Ronald Klein, and Stacy M. Meuer PURPOSE. To investigate whether optic disc size is related
Arterial Branching in Man and Monkey
 Published Online: 1 March, 1982 Supp Info: http://doi.org/10.1085/jgp.79.3.353 Downloaded from jgp.rupress.org on December 13, 2018 Arterial Branching in Man and Monkey M. ZAMIR and J. A. MEDEIROS From
Published Online: 1 March, 1982 Supp Info: http://doi.org/10.1085/jgp.79.3.353 Downloaded from jgp.rupress.org on December 13, 2018 Arterial Branching in Man and Monkey M. ZAMIR and J. A. MEDEIROS From
chorioretinal atrophy
 British Journal of Ophthalmology, 1987, 71, 757-761 Retinal microangiopathy in pigmented paravenous chorioretinal atrophy SURESH R LIMAYE AND MUNEERA A MAHMOOD From the Ophthalmology Service, DC General
British Journal of Ophthalmology, 1987, 71, 757-761 Retinal microangiopathy in pigmented paravenous chorioretinal atrophy SURESH R LIMAYE AND MUNEERA A MAHMOOD From the Ophthalmology Service, DC General
Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy
 European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
The Effect of Glycemic Exposure on the Risk of Microvascular Complications in the Diabetes Control and Complications Trial -- Revisited
 Diabetes Publish Ahead of Print, published online January 25, 2008 The Effect of Glycemic Exposure on the Risk of Microvascular Complications in the Diabetes Control and Complications Trial -- Revisited
Diabetes Publish Ahead of Print, published online January 25, 2008 The Effect of Glycemic Exposure on the Risk of Microvascular Complications in the Diabetes Control and Complications Trial -- Revisited
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic Retinopathy Screening Programme
 (2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
(2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
Influence of diffuse luminance flicker on choroidal and optic nerve head blood flow
 Current Eye Research 0271-3683/02/2402-109$16.00 2002, Vol. 24, No. 2, pp. 109 113 Swets & Zeitlinger Influence of diffuse luminance flicker on choroidal and optic nerve head blood flow G. Garhöfer 1,
Current Eye Research 0271-3683/02/2402-109$16.00 2002, Vol. 24, No. 2, pp. 109 113 Swets & Zeitlinger Influence of diffuse luminance flicker on choroidal and optic nerve head blood flow G. Garhöfer 1,
Proliferative diabetic retinopathy
 Brit. J. Ophthal. (1970) 54, 535 Proliferative diabetic retinopathy Regression of optic disc neovascularization after retinal photocoagulation ENID TAYLOR Ophthalmic Department, St. Bartholomew's Hospital,
Brit. J. Ophthal. (1970) 54, 535 Proliferative diabetic retinopathy Regression of optic disc neovascularization after retinal photocoagulation ENID TAYLOR Ophthalmic Department, St. Bartholomew's Hospital,
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Chapter 9. Body Fluid Compartments. Body Fluid Compartments. Blood Volume. Blood Volume. Viscosity. Circulatory Adaptations to Exercise Part 4
 Body Fluid Compartments Chapter 9 Circulatory Adaptations to Exercise Part 4 Total body fluids (40 L) Intracellular fluid (ICF) 25 L Fluid of each cell (75 trillion) Constituents inside cell vary Extracellular
Body Fluid Compartments Chapter 9 Circulatory Adaptations to Exercise Part 4 Total body fluids (40 L) Intracellular fluid (ICF) 25 L Fluid of each cell (75 trillion) Constituents inside cell vary Extracellular
Retinal blood flow in diabetic retinopathy
 cholinergic activity may also contribute to the observed reactions. Until clinical operational criteria for diagnosing senile dementia of Lewy body type are validated it is not possible to predict accurately
cholinergic activity may also contribute to the observed reactions. Until clinical operational criteria for diagnosing senile dementia of Lewy body type are validated it is not possible to predict accurately
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
Amin Aboali Hassan. Department Of Ophthalmology, Sohag University Hospital, Faculty of Medicine, Sohag University, Egypt
 Three -Year Incidence and Risk Factors for Retinal Vein Occlusion in Sohag University Hospital Amin Aboali Hassan Department Of Ophthalmology, Sohag University Hospital, Faculty of Medicine, Sohag University,
Three -Year Incidence and Risk Factors for Retinal Vein Occlusion in Sohag University Hospital Amin Aboali Hassan Department Of Ophthalmology, Sohag University Hospital, Faculty of Medicine, Sohag University,
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Influence of Flickering Light on the Retinal Vessels in Diabetic Patients
 Pathophysiology/Complications O R I G I N A L A R T I C L E Influence of Flickering Light on the Retinal Vessels in Diabetic Patients ALEKSANDRA MANDECKA, MD 1 JENS DAWCZYNSKI, MD 2 MARCUS BLUM, MD 3 NICOLLE
Pathophysiology/Complications O R I G I N A L A R T I C L E Influence of Flickering Light on the Retinal Vessels in Diabetic Patients ALEKSANDRA MANDECKA, MD 1 JENS DAWCZYNSKI, MD 2 MARCUS BLUM, MD 3 NICOLLE
Retinopathy in a diabetic population
 Kathmandu University Medical Journal (2007), Vol. 5, No. 2, Issue 18, 204-209 Retinopathy in a diabetic population Shrestha S 1, Malla OK 2, Karki DB 3, Byanju RN 4 2 Fellow of NAMS, 3 Professor, NAMS,
Kathmandu University Medical Journal (2007), Vol. 5, No. 2, Issue 18, 204-209 Retinopathy in a diabetic population Shrestha S 1, Malla OK 2, Karki DB 3, Byanju RN 4 2 Fellow of NAMS, 3 Professor, NAMS,
Fundus Fluorescein Angiography in Diabetic Retinopathy: Correlation of Angiographic Findings to the Clinical Maculopathy Abstract: Purpose:
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XII (Feb. 2016), PP 80-88 www.iosrjournals.org Fundus Fluorescein Angiography in Diabetic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XII (Feb. 2016), PP 80-88 www.iosrjournals.org Fundus Fluorescein Angiography in Diabetic
CLINICAL SCIENCES. Repeatability and Reproducibility of Fast Macular Thickness Mapping With Stratus Optical Coherence Tomography
 CLINICAL SCIENCES Repeatability and Reproducibility of Fast Macular Thickness Mapping With Stratus Optical Coherence Tomography Antonio Polito, MD; Michele Del Borrello, MD; Miriam Isola, MHS; Nicola Zemella,
CLINICAL SCIENCES Repeatability and Reproducibility of Fast Macular Thickness Mapping With Stratus Optical Coherence Tomography Antonio Polito, MD; Michele Del Borrello, MD; Miriam Isola, MHS; Nicola Zemella,
Microaneurysms in the development of diabetic retinopathy (UKPDS 42)
 Diabetologia (1999) 42: 1107±1112 Ó Springer-Verlag 1999 Microaneurysms in the development of diabetic retinopathy (UKPDS 42) E.M. Kohner 1, I. M. Stratton 2, S. J. Aldington 3, R. C. Turner 2, D. R. Matthews
Diabetologia (1999) 42: 1107±1112 Ó Springer-Verlag 1999 Microaneurysms in the development of diabetic retinopathy (UKPDS 42) E.M. Kohner 1, I. M. Stratton 2, S. J. Aldington 3, R. C. Turner 2, D. R. Matthews
Indocyanine green angiography of the anterior segment in patients undergoing strabismus surgery
 214 Br J Ophthalmol 2001;85:214 218 SCIENTIFIC CORRESPONDENCE Department of Ophthalmology, University of California, Los Angeles, CA, USA T K J Chan A L Rosenbaum R Rao S D Schwartz P Santiago D Thayer
214 Br J Ophthalmol 2001;85:214 218 SCIENTIFIC CORRESPONDENCE Department of Ophthalmology, University of California, Los Angeles, CA, USA T K J Chan A L Rosenbaum R Rao S D Schwartz P Santiago D Thayer
Ultrahigh Speed Imaging of the Rat Retina Using Ultrahigh Resolution Spectral/Fourier Domain OCT
 Ultrahigh Speed Imaging of the Rat Retina Using Ultrahigh Resolution Spectral/Fourier Domain OCT The MIT Faculty has made this article openly available. Please share how this access benefits you. Your
Ultrahigh Speed Imaging of the Rat Retina Using Ultrahigh Resolution Spectral/Fourier Domain OCT The MIT Faculty has made this article openly available. Please share how this access benefits you. Your
Diabetic retinopathy (DR) was first PROCEEDINGS DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT
 DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT Diabetic retinopathy (DR) is characterized by the development of retinal microaneurysms, hemorrhages, deposits of leaked lipoproteins (hard exudates),
DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT Diabetic retinopathy (DR) is characterized by the development of retinal microaneurysms, hemorrhages, deposits of leaked lipoproteins (hard exudates),
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Association of retinal vessel calibre with diabetic retinopathy in an urban Australian Indigenous population *
 Original Article Clinical Science Association of retinal vessel calibre with diabetic retinopathy in an urban Australian Indigenous population * Mohamed Dirani PhD, 1 Annie K McAuley BSc, 1 Louise Maple-Brown
Original Article Clinical Science Association of retinal vessel calibre with diabetic retinopathy in an urban Australian Indigenous population * Mohamed Dirani PhD, 1 Annie K McAuley BSc, 1 Louise Maple-Brown
NIH Public Access Author Manuscript Br J Ophthalmol. Author manuscript; available in PMC 2010 May 1.
 NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2009 May ; 93(5): 634 637. doi:10.1136/bjo.2008.150276. Measurement of total blood flow in the normal human retina
NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2009 May ; 93(5): 634 637. doi:10.1136/bjo.2008.150276. Measurement of total blood flow in the normal human retina
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma. Module 3a GDx
 STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
STRUCTURE & FUNCTION An Integrated Approach for the Detection and Follow-up of Glaucoma Module 3a GDx Educational Slide Deck Carl Zeiss Meditec, Inc. November 2005 1 Structure & Function Modules Module
Diabetic Learning Event: Diabetic Eye Screening and Retinopathy- Samantha Mann & Mark Frost
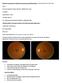 Diabetic Learning Event: Diabetic Eye Screening and Retinopathy- Samantha Mann & Mark Frost Case 1 : 63 yr-old Caucasian woman with type-2 Diabetes for 8 years Ex-smoker Hypertension- 5 years FH: father
Diabetic Learning Event: Diabetic Eye Screening and Retinopathy- Samantha Mann & Mark Frost Case 1 : 63 yr-old Caucasian woman with type-2 Diabetes for 8 years Ex-smoker Hypertension- 5 years FH: father
Retinal vascular calibre and response to light exposure and serial imaging
 Retinal vascular calibre and response to light exposure and serial imaging Therese von Hanno, 1,2 Anne Katrin Sjølie 1,3, and Ellisiv B. Mathiesen 1,4 1 Brain and Circulation Research Group, Department
Retinal vascular calibre and response to light exposure and serial imaging Therese von Hanno, 1,2 Anne Katrin Sjølie 1,3, and Ellisiv B. Mathiesen 1,4 1 Brain and Circulation Research Group, Department
Changes in retinal vascular caliber may carry important
 Measurement of Retinal Vascular Caliber: Issues and Alternatives to Using the Arteriole to Venule Ratio Gerald Liew, 1 A. Richey Sharrett, 2 Richard Kronmal, 3 Ronald Klein, 4 Tien Yin Wong, 5,6,7 Paul
Measurement of Retinal Vascular Caliber: Issues and Alternatives to Using the Arteriole to Venule Ratio Gerald Liew, 1 A. Richey Sharrett, 2 Richard Kronmal, 3 Ronald Klein, 4 Tien Yin Wong, 5,6,7 Paul
UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT*
 Brit. J. Ophthal. (1962) 46, 737. UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT* BY Nuffield Laboratory of Ophthalmology, Oxford, and Cape Town, Union of South Africa THis paper illustrates
Brit. J. Ophthal. (1962) 46, 737. UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT* BY Nuffield Laboratory of Ophthalmology, Oxford, and Cape Town, Union of South Africa THis paper illustrates
CHAPTER 8 EVALUATION OF FUNDUS IMAGE ANALYSIS SYSTEM
 CHAPTER 8 EVALUATION OF FUNDUS IMAGE ANALYSIS SYSTEM Diabetic retinopathy is very common retinal disease associated with diabetes. Efforts to prevent diabetic retinopathy though have yielded some results;
CHAPTER 8 EVALUATION OF FUNDUS IMAGE ANALYSIS SYSTEM Diabetic retinopathy is very common retinal disease associated with diabetes. Efforts to prevent diabetic retinopathy though have yielded some results;
Retinal blood flow. 1.Retinal circulation. 1. Retinal circulation Ø Supplies the inner retinal layers Ø Non fenestrated capillaries
 www.ophtalmique.ch Glucose Retinal blood flow Pournaras Jean-Antoine C Vitreoretinal Surgery Unit Constantly regulated hemodynamics assuming delivery of and metabolic substrates, as well as intact blood-retinal
www.ophtalmique.ch Glucose Retinal blood flow Pournaras Jean-Antoine C Vitreoretinal Surgery Unit Constantly regulated hemodynamics assuming delivery of and metabolic substrates, as well as intact blood-retinal
MAGNITUDE OF DIABETIC EYE DISEASE IN INDIA
 Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after Pattern Scanning Laser Photocoagulation in Patients with Diabetic Retinopathy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(3):220-225 http://dx.doi.org/10.3341/kjo.2014.28.3.220 Original Article Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(3):220-225 http://dx.doi.org/10.3341/kjo.2014.28.3.220 Original Article Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after
EVect of isosorbide mononitrate on the human optic nerve and choroidal circulations
 162 Department of Ophthalmology, Scheie Eye Institute, School of Medicine, University of Pennsylvania, Philadelphia, USA J E Grunwald A Iannaccone* J DuPont *Currently ayliated with the Department of Ophthalmology,
162 Department of Ophthalmology, Scheie Eye Institute, School of Medicine, University of Pennsylvania, Philadelphia, USA J E Grunwald A Iannaccone* J DuPont *Currently ayliated with the Department of Ophthalmology,
Incidence of ophthalmoscopic fundus changes in hypertensive patients
 Original Article Incidence of ophthalmoscopic fundus changes in hypertensive Karki KJD 1 1 Associate Professor, Department of Ophthalmology, Kathmandu Medical College. Abstract A prospective, hospital
Original Article Incidence of ophthalmoscopic fundus changes in hypertensive Karki KJD 1 1 Associate Professor, Department of Ophthalmology, Kathmandu Medical College. Abstract A prospective, hospital
The Natural History of Diabetic Retinopathy and How Primary Care Makes A Difference
 The Natural History of Diabetic Retinopathy and How Primary Care Makes A Difference We will discuss - How exactly does blood sugar control affect retinopathy? - What are other factors that we measure in
The Natural History of Diabetic Retinopathy and How Primary Care Makes A Difference We will discuss - How exactly does blood sugar control affect retinopathy? - What are other factors that we measure in
EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion
 EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina
EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina
7Progression and regression:
 7Progression and regression: Distinct developmental patterns of diabetic retinopathy in patients with type 2 diabetes treated in the Diabetes Care System West-Friesland, the Netherlands Hata Zavrelova,
7Progression and regression: Distinct developmental patterns of diabetic retinopathy in patients with type 2 diabetes treated in the Diabetes Care System West-Friesland, the Netherlands Hata Zavrelova,
Haemorrhagic glaucoma
 Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Variation associated with measurement of retinal vessel diameters at different points in the pulse cycle
 57 SCIENTIFIC REPORT Variation associated with measurement of retinal vessel diameters at different points in the pulse cycle M D Knudtson, B E K Klein, R Klein, T Y Wong, L D Hubbard, K E Lee, S M Meuer,
57 SCIENTIFIC REPORT Variation associated with measurement of retinal vessel diameters at different points in the pulse cycle M D Knudtson, B E K Klein, R Klein, T Y Wong, L D Hubbard, K E Lee, S M Meuer,
