Renal Pathology. SCBM342 Systemic Pathology 19 February Lecturer: Niwat Kangwanrangsan, Ph.D.
|
|
|
- Valerie Logan
- 5 years ago
- Views:
Transcription
1 SCBM342 Systemic Pathology 19 February 2018 Renal Pathology Lecturer: Niwat Kangwanrangsan, Ph.D. Department of Pathobiology Faculty of Science, Mahidol University
2 Outline I: Kidney diseases & associated syndromes A) Clinical manifestations of renal diseases B) Glomerular diseases C) Diseases affecting tubules and interstitium D) Diseases involving blood vessels E) Chronic kidney diseases F) Cystic Dieseases G) Urinary outflow obstruction H) Congenital and developmental anomalies I) Neoplasms 2
3 Outline II: Diseases of lower urinary tract (Ureter&Bladder) J) Ureter K) Urinary bladder 3
4 Urinary System Urinary Tract -Kidney 1) Glomeruli 2) Tubules 3) Interstitium 4) Blood vessels - Lower urinary tract 1) Ureter 2) Bladder 3) Urethra (diseases associated with reproductive tract) 4
5 5
6 6
7 Blood Flow in Kidney 7
8 8
9 9
10 10
11 11
12 12 1) Glomeruli 2) Tubules 3) Interstitium 4) Blood vessels
13 Lower Urinary Tract MALE FEMALE 1) Ureter 2) Bladder 13 3) Urethra associated with reproductive system
14 Technical terms Nephrosis non-inflammatory disease of kidney Nephritis inflammatory disease of kidney Nephrolith kidney stone Urethritis inflammation of urethra * final pathway for urine in both sexes & * common pathway for urine & semen in male Nocturia frequently getting up & urinating during the night Enuresis involuntary release of urine, most often in reference to bedwetting. 14
15 Oliguria / Anuria decrease / no urine flow Glomerulopathies non-inflammatory & inflammatory glomerular diseases Hereditary glomerulopathy(congenital disease) Neoplasm(tumor & cancer) Systemic diseases -tubulo-interstitial & vascular diseases 15
16 Azotemia Elevation of blood urea nitrogen (BUN) and creatinine level Usually reflects a decreased glomerular filtration rate (GFR) Decrease of GFR may come from intrinsic renal disease or extrarenal causes Prerenal azotemia encountered when there is hypoperfusion of kidney (uaually due to reduce extracellular fluid volume). Postrenalazotemia occurred when urine outflow is obstructed Azotemia gives rise to clinical manifestation and systemic biochemical abnormalities, it is termed uremia. 16
17 Uremia characterized by failureof renal excretory function and also by metabolic and endocrine functions that incident to renal damage may involved with -uremic gastroenteritis - peripheral neuropathy - uremic fibrinous pericarditis 17
18 A: Clinical manifestations and syndromes 1. Nephrotic syndrome 2. Nephritic syndrome 3. Asymptomatic hematuria 4. Rapid progressive glomerulonephritis (RPGN) 5. Acute kidney injury 6. Chronic kidney disease 7. End stage renal disease (ESRD) 8. Urinary tract infection (UTI) 9. Nephrolithiasis two most common syndromes associated with glomerular diseases 18
19 A1: Nephrotic Syndrome can be characterized by Proteinuria daily protein loss in urine >3.5 g in adult Hypoalbuminemia plasma albumin <3.0 g/dl Generalized edema, Anasarca fluid retention Hyperlipidemia / Lipiduria cholesterol >200 mg/dl/ oval fat body in urine 19
20 derangement in capillary walls of glomeruli increase in permeability of glomerular basement membrane (GBM) - Proteinuria - Hypoalbuminemia -leakage of fluid from blood into extravascular spaces -increase release of renin from juxtaglomerular cells, promote retention of water and salt by the kidney resulting in edema 20 this onset, there are little or no azotemia, hematuria, or hypertension
21 Primary glomerular lesions that related to nephrotic syndrome 1. Focal segmental glomerulosclerosis - more important in adults 2. Minimal-changes disease - more important in children 21
22 22
23 23
24 Minimal-change disease 24
25 25
26 26
27 27
28 A2: Nephritic Syndrome can be characterized by Hematuria red cells and red cell casts in urine Proteinuria with in sub-nephrotic range with or without edema Azotemia Hypertension 28
29 about nephritic syndrome usually has an acute onset usually caused by inflammatory lesions of glomeruli infiltration of leukocytes inflammatory reaction damages the capillary walls -blood pass to the urine = hematuria -reduction of GFR = oliguria, edema, azotemia 29
30 A3: Asymptomatic hematuria nonnephroticproteinuria combination of theses 2 clinical presentation - IgA nephropathy - Alport syndrome - other early presentations of glomerular diseases A4: Rapid progressive glomerulonephritis (RPGN) rapid loss of renal function (a few days or weeks) histologic finding is crescent (crescentic GN) can progress to renal failure within weeks or months 30
31 31
32 32
33 A5: Acute kidney injury acute increase in serum creatinine often associated with oliguria or anuria can be come from -glomerular injury - interstitial injury - vascular injury (thrombotic microangiopathy) - acute tubular epithelial cell injury A6: Chronic kidney disease progressive scarring of kidney various metabolic and electrolyte abnormalities e.g. hyperphosphatemia, dyslipidemia, metabolic acidosis often asymptomatic until uremia develop 33
34 A7: End-stage renal disease (ESRD) irreversible loss of renal function requirement of dialysis or transplantation typically due to progressive scarring of kidney A8: Urinary tract infection (UTI) bacteriuria and pyuria (bacteria and leukocytes in urine) symptomatic or asymptomatic affect to kidney (pyelonephritis) or bladder (cystitis) only A9: Nephrolithiasis formation of stone in collecting system, manifested by renal colic and hematuria (without RBC casts) 34
35 35
36 36
37 37
38 38
39 39
40 40
41 Kidney Dialysis 41
42 UTI 42
43 UTI 43
44 44
45 Glomerulus -an anastomosing network of capillaries invested by two layers of epithelium - Bowman capsule / Bowman space - fenestrated endothelial cells ( nm in diameter) - glomerular basement membrane (GBM) -podocytes - mesangial cells -permeability cut-off at molecular size and charge of albumin 45 (70,000 kda)
46 46
47 B: Glomerular diseases immune mechanism underlie most of primary glomerular diseases and many of secondary glomerular diseases Two possible mechanisms of antibody deposition in glomerulus 1) deposition of circulating immune complex 2) immune complexes form in situ + complement system + cell-mediated immune mechanism 47
48 Antibody-mediated glomerular injury 48
49 49
50 Patterns of immune complex deposition by immunofluorescence microscopy A) Granular, characteristic of circulation immune complex deposition B) Linear, characteristic of in situ immune complex deposition 50
51 51
52 52
53 Minimal-change disease 53
54 Focal and segmental glomerulosclerosis PAS staining 54
55 Membranous nephropathy PAS staining 55
56 Membranoproliferativeglomerulonephritis 56
57 Poststreptococcalglomerulonephritis 57
58 IgA nephropathy 58
59 Crescentic glomerulonephritis silver stain 59
60 Non-immune mechanism of glomerular injury Podocyte injury -can be induced by toxin (or Ab to podocyte Ag) - morphological changes - effacement of foot process - vacuolization -detachment of cell from GBM -associated with proteinuria Nephron loss - scarring of glomerulus (glomerulosclerosis) - glomeruli hypertrophy to maintain the renal function -maladaptive changes increase in single-nephron GFR, blood flow, and transcapillary pressure (capillary hypertension) 60
61 C: Diseases Affecting Tubule and Interstitium most of tubular injuries also involve the interstitium the diseases can be characterized by 1) inflammatory involvement tubulointerstitialnephritis 2) ischemic or toxic injury acute tubular necrosis acute kidney injury 61
62 62
63 TubulointerstitialNephritis (TIN) glomeruli may be affected only in late stage usually caused by non-bacterial in origin e.g. drugs, hypokalemia, irradiation, viral infection, and immune reaction pyelonephritis can be described in cases of TIN caused by bacterial infection - acute pyelonephritis - chronic pyelonephritis pyelo = pelvis 63
64 Pathways of renal infection 1) ascending infection from combination of - bladder infection - vesicoureteral reflux 2) hematogenous infection 64
65 Acute pyelonephritis the most important manifestation of UTI principal pathogens are enteric gram-negative bacteria, the most common is E. coli, the other important pathogens are Proteus, Klebsiella, Enterobacter, and Pseudomonas uncommon pathogens are Staphylococciand Streptococci ascending infection is frequent route commonly affects females (the close proximity of urethra and rectum) vesicoureteral reflux (VUR) aloe bacteria to ascend the ureter into pelvis 65
66 Clinical features for uncomplicated acute pyelonephritis pain, chills, fever, nausea, malaise, dysuria, frequency and urgency turbid urine (pyuria) usually is unilateral and do not develop renal failure may become recurrent or chronic 66
67 Acute pyelonephritis - abscesses (focal pale) - congestion (dark vessels) 67
68 68
69 Chronic pyelonephritis common in patients with history of UTI marked by uneven scarring and deformity of pelvicalyceal system uneven interstitial fibrosis, infiltration of lymphocytes, plasma cells, and occasionally neutrophils, dilation or contraction of tubules with thyroidization, atrophy of epithelial lining important cause of chronic kidney disease there are 2 forms -chronic obstructive pyelonephritis - chronic reflux-associated pyelonephritis 69
70 Chronic obstructive pyelonephritis obstruction predisposes the kidney to infection inflammation and scarring unilateral or bilateral Chronic reflux-associated pyelonephritis most common cause of chronic pyelonephritis resulted from superimposition of UTI on congenital vesicoureteral reflux and intrarenal reflux may develop secondary glomerulosclerosis 70
71 Typical coarse scars (found in vesicoureteral reflux ) 71
72 72
73 Drug-induce tubulointerstitialnephritis also called acute drug-induced TIN drugs in associated with disease including penicillins, riflampin, diuretics, proton pump inhibitors, non-steroidal anti-inflammatory agents, immune checkpoint inhibitors drugs act as haptenthat can bind to cytoplasmic or extracellular components of tubular cells clinical feature related with immune mechanism (increase in serum IgE with eosinophilia suggested Type I Hypersensitivity) in others cases might be Type IV hypersensitivity reaction 73
74 prominent eosinophilic and mononuclear cells infiltration 74
75 Acute tubular necrosis/injury (ATN/ATI) but necrosis is rarely observed in the kidney biopsy, so later use ATI most common cause of kidney injury damage of tubular cells with an acute decline in kidney function decrease GFR, elevation of serum creatinine, oliguria (urine output <400 ml/day) shedding of tubular casts and tubular cells into urine 2 forms of ATI which differ in underlying cause 1) Ischemic ATI -a period of inadequate blood flow (hypotension/ shock) 2) Nephrotoxic ATI -a variety of poisons e.g. heavy metals (mercury), organic solvents (CCl 4 ), gentamycin and other antibiotics 75
76 ATI 76
77 ATI - tubular epithelial cell injury - blebbing into the lumen - detachment of tubular cells - proteinaceous casts - interstitial edema 77
78 78
79 79
80 Postulate sequence in ischemic or toxic tubular injury 80
81 D: Diseases Involving Blood Vessels Nearly all diseases of the kidney affect the renal blood vessels secondarily. Systemic vascular diseases, such as various forms of vasculitis, also involve renal blood vessels, and often produce clinically important effects on renal function. kidney is intimately involved in the pathogenesis of both essential and secondary hypertension. This part covers the renal lesions associated with hypertension. 81
82 Nephrosclerosis refers to sclerosis of small renal arteries and arterioles that is strongly associated with hypertension morphological changes of the small arterioles are called hyaline arteriolosclerosis cause ischemia, which leads to various combinations of interstitial fibrosis, tubular atrophy, and focal global glomerulosclerosis frequency and severity of the lesions are increased at any age when hypertension or diabetes are present 82
83 Two processes participate in the arterial lesions of nephrosclerosis: 1. Medial and intimal thickening, as a response to hemodynamic changes, aging, genetic defects, or some combination of these 2. Hyalinization of arteriolar walls, caused by extravasation of plasma proteins through injured endothelium and by increased deposition of basement membrane matrix 83
84 84
85 hyaline arteriosclerosis 85
86 Malignant hypertension defined as blood pressure usually greater than 200/120 mm Hg may present with severe acute kidney injury and renal failure renal changes are confined to the vasculature and may include thrombotic microangiopathy resulting from long-standing hypertension causes increased permeability of the vessels to fibrinogen and other plasma proteins, endothelial injury, and platelet deposition, leads to the appearance of fibrinoidnecrosis of arterioles and small arteries and intravascular thrombosis mitogenicfactors from platelets (e.g., platelet-derived growth factor) and plasma cause intimal hyperplasia of vessels, resulting in hyperplastic arteriosclerosis 86
87 87
88 fibrinoid necrosis of afferent arteriole hyperplastic arteriosclerosis onion-skin lesion 88
89 E: Chronic Kidney Diseases a broad term that describes the final common pathway of progressive nephron loss resulting from any type of kidney disease remaining intact nephrons are ultimately maladaptive and cause further scarring eventually results in an end-stage kidney with sclerosedglomeruli, tubules, interstitium and vessels unless the disorder is treated with dialysis or transplantation, death from uremia, electrolyte disturbances, or other complications of endstage renal disease results 89
90 Pathogenesis destroys more and more nephrons makes adaptive mechanisms are initated that try to maintain renal function glomerular hyperfiltrationtends to compensate for decreased glomerular filtration rate resulting from the loss of nephrons increased plasma creatinine, decreased tubular reabsorption (for sodium, phosphate, and calcium), or increased tubular secretion (for potassium and hydrogen ions) helps to maintain homeostasis until the late stages of chronic kidney disease, however, renal function often deteriorates progressively even when the original insult is controlled Uncontrolled hypertension, regardless of the etiology, results in more rapid renal functional decline 90
91 Clinical Features chronic kidney disease may develop insidiously and be discovered late in its course, because it is often asymptomatic. frequently, renal disease is first detected by the discovery of proteinuria, hypertension, or azotemia on routine medical examination. in patients with glomerular disease resulting in nephrotic syndrome, as the glomeruli undergo sclerotic changes and result in nephron loss, the avenue for protein loss is progressively lessened, and the nephrotic syndrome thus becomes less severe with advanced disease some degree of proteinuria, however, is present in almost all cases hypertension is very common. microscopic hematuria is usually present, grossly bloody urine is infrequent at this late stage 91
92 chronic glomerulonephritis, Masson s trichrome stain 92
93 93
94 94
95 F: Cystic Diseases of the Kidney comprising of 1) hereditary, 2) developmental, and 3) acquired disorders often present diagnostic problems for clinicians, radiologists, and pathologists and can occasionally be confused with malignant tumors 95
96 Simple cysts generally innocuous lesions that occur as multiple or single cystic spaces of variable size commonly, they are 1 to 5 cm in diameter; translucent; lined by a gray, glistening, smooth membrane; and filled with clear fluid microscopic examination, these membranes are seen to be composed of a single layer of cuboidal or flattened cuboidal epithelium cysts usually are confined to the cortex. common postmortem finding that has no clinical significance the main importance of cysts lies in their differentiation from kidney tumors, when they are discovered either incidentally or during evaluation of hemorrhage and pain radiographic studies show that in contrast with renal tumors, renal cysts have smooth contours, are almost always avascular, and produce fluid rather than solid tissue signals on ultrasonography 96
97 Autosomal Dominant (Adult) Polycystic Kidney Disease characterized by multiple expanding cysts affecting both kidneys that ultimately destroy the intervening parenchyma approximately found 1 in individuals and accounts for 10% of cases of chronic kidney disease genetically heterogeneous. It can be caused by inheritance of one of at least two autosomal dominant genes of very high penetrance. 97
98 Pathogenesis in 85% to 90% of families, PKD1,on the short arm of chromosome 16, is the defective gene, this gene encodes a large (460-kDa) and complex cell membrane associated protein called polycystin-1 Polycystin-1 localizes to the primary cilium of tubular cells, giving rise to the concept of renal cystic diseases as a type of ciliopathy Cilia serve as mechanosensorsof fluid flow. Current evidence suggests that polycystin mutations produce defects in mechanosensing in turn, alters downstream signaling events involving calcium influx, leading to dysregulation of cell polarity, proliferation, and cell cell and cell matrix adhesion increase in intracellular calcium is thought to stimulate proliferation and secretion from the tubular epithelial cells, which together lead to the formation of cysts cyst formation and interstitial fibrosis are characteristic of progressive polycystic kidney disease tumor suppressor genes, a second somatic hit is required for cyst development 98
99 Clinical Features does not produce symptoms until the fourth decade of life, by which time the kidneys are quite large. most common presenting complaint is flank pain or a heavy, dragging sensation. Acute distention of a cyst, either by intracystichemorrhage or by obstruction, may cause excruciating pain. Sometimes attention is first drawn to the lesion on palpation of an abdominal mass. intermittent gross hematuria commonly occurs most important complications are hypertension and urinary infection hypertension of variable severity develops in about 75% of individuals although the disease is ultimately fatal, the outlook is generally more favorable than with most chronic kidney diseases. The condition progresses very slowly. End-stage renal disease occurs at about 50 years of age, but there is wide variation in the course 99
100 Autosomal dominant adult polycystic kidney 100
101 101
102 102
103 Autosomal Recessive (Childhood) Polycystic Kidney Disease this is a rare autosomal recessive disorder that is genetically distinct from adult polycystic kidney disease. occurs in approximately 1 in 20,000 live births perinatal, neonatal, infantile, and juvenile subcategories have been defined, depending on age at presentation and the presence of associated hepatic lesions all types result from mutations in the PKHD1gene, coding for a putative membrane receptor protein called fibrocystin. Fibrocystinis found in cilia in tubular epithelial cells, but its function remains unknown serious manifestations usually are present at birth, and young infants may die quickly from hepatic or renal failure. Patients who survive infancy develop liver cirrhosis (congenital hepatic fibrosis) 103
104 Medullary Diseases with Cysts There are two major types of cystic disease affecting the medulla: 1) medullary sponge kidney, a relatively common and usually innocuous condition, occasionally associated with nephrolithiasis, which will not be discussed further, and 2) nephronophthisis-medullary cystic disease complex, which is almost always associated with renal dysfunction. Nephronophthisisusually begins in childhood. Four variants are recognized on the basis of the timing of onset: infantile, juvenile (most common), and adolescent nephronophthisis, and medullary cystic disease developing later in adult life. 15% to 20% of children with juvenile nephronophthisishave extrarenal manifestations, often appear as retinal abnormalities, including retinitis pigmentosa, and even early-onset blindness At least nine gene loci (NHP1 to NHP9) have been identified for the autosomal recessive forms of the nephronophthisiscomplex. 104
105 105
106 G: Urinary Outflow Obstruction G1: Renal stones (Urolithiasis) G2: Hydronephrosis 106
107 G1: Renal Stones (Urolithiasis) among the parts of urinary system, most of stones arise in the kidney symptomatic diseases are common in men, unilateral 3 major types: 1) calcium oxalate /or mixed with calcium phosphate, 2) magnesium ammonium phosphate, 3) uric acid or cysteine 2.5% of stone weight is mucoprotein most important cause is supersaturation of urine, other causes can be changes in urine ph, or bacterial infections progressive accretion of salts leads to branching structure (staghorn) stones may present without symptoms or significant renal damage smaller stone may pass into urine, that can make intense pain known as renal colic characterized by paroxysm of flank pain radiation toward the groin, gross hematuria can cause trauma resulting ulceration and bleeding Gout and leukemia lead to high uric acid levels can be the cause of 107 uric acid stones
108 108
109 109
110 G2: Hydronephrosis dilation of real pelvis and calyces atrophy of parenchyma from obstruction of outflow of urine obstruction can occur at any parts of the urinary system most common causes are 1) congenital 2) acquired - foreign bodies - proliferative lesions - inflammatory lesions - neurogenic - normal pregnancy bilateral hydronephrosisoccurs only when obstruction is below the level of ureter, complete bilateral hydronephrosis can make anuria incomplete bilateral obstruction cause polyuria rather than oliguria before irreversible stage, removal of obstruction usually permits full return of function within a few weeks 110
111 dilation of pelvis and calyces thin of renal cortex 111
112 H: Congenital and Developmental Anomalies represent the most common cause of end-stage renal disease in individuals younger than 21 years of age and account for 40% to 50% of pediatric renal failure worldwide abnormalities can affect the kidney (dysplasia, agenesis, hypoplasia), collecting system (duplicated collecting system, hydronephrosis, megaureter), bladder (ureteroceleand vesicoureteral reflux), or urethra (posterior urethral valves) may present as an isolated feature or as part of a syndrome in association with extrarenalmanifestations. Most result from sporadic developmental defects of unknown cause. Others are caused by germline mutations in genes that impact the development of the kidney and especially the ureteric bud. 112
113 Multicystic dysplasia the most common form of renal cystic disease in childhood a developmental rather than a preneoplasticlesion. Because renal dysplasia is often associated with obstruction in the lower urinary tract, increased hydrostatic pressure in the developing kidney is thought to play a role in its development. kidneys are usually grossly distorted; the cysts range from microscopic to several centimeters in diameter. The histologic hallmarks are ducts and tubules lined by epithelial cells and surrounded by cuffs of cellular mesenchyme. 113
114 Renal agenesis Bilateral agenesis is incompatible with life and usually is encountered in stillborn infants often associated with other congenital disorders (e.g., limb defects, hypoplasticlungs). Unilateral agenesis is uncommon and compatible with normal life if no other abnormalities exist. Hypoplasia may occur bilaterally, resulting in renal failure in early childhood, but is more commonly encountered as a unilateral defect the hypoplastickidney shows no scars and has a reduced number of renal lobes and pyramids, usually six or fewer. 114
115 I: Neoplasms of Kidney there are many types of benign and malignant neoplasms occur in urinary tract the most common malignant neoplasm of the kidney is renal cell carcinoma, followed in frequency by nephroblastoma (Wilms tumor) and by primary neoplasms of the calyces and pelvis other types of renal cancer are rare neoplasms of the lower urinary tract are about twice as common as renal cell carcinomas I1: Oncocytoma I2: Renal cell carcinoma I3: Wilm Tumor 115
116 I1: Oncocytoma benign neoplasm arise from intercalated cells of collecting ducts associated with loss of Chr.1 and Y characterized by plethora of mitochondria, providing the basis of their tan color and finely granular eosinophilic cytoplasm 116 tubolocystic pattern
117 I2: Renal cell carcinoma derived from renal tubular epithelium locate predominantly in the cortex represent 80-85% or primary malignant neoplasms of kidney men are affect twice as commonly as women risk groups: smokers, hypertensive or obese patients, people with cadmium exposure closely relate with acquired polycystic disease as a complication of kidney dialysis classified by morphology and growth pattern 1) clear cell carcinoma (most common) 2) papillary renal cell carcinoma 3) chromophobe renal carcinoma 117
118 clear cell pattern 118
119 I3: Wilms tumor (nephroblastoma) common renal cancer in children at the age <10 year-old the cancer mass contains cells and tissues derived from mesoderm typically large, solitary, well-circumscribed mass relate with congenital malformation 1) WAGR syndrome 2) Denys-Drashsyndrome 3) Beck-with-Wiedemann syndrome 119
120 120
121 J: Ureter Ureteropelvic junction obstruction congenital disorder, usually found in infancy or childhood result in hydronephrosis Retroperitoneal fibrosis uncommon cause of ureteral obstruction inflammatory process causing hydronephrosis Malignant tumor pathologically similar to those are found in renal pelvis, calyces, or bladder most are urothelial carcinoma 121
122 K: Urinary bladder K1: Nonneoplasticconditions K2: Neoplasms 122
123 K1: Nonneoplasticconditions Bacterial cystitis common in women coliform bacteria Hemorrhagic cystitis occur in patients receiving cytotoxic antitumor drugs sometimes complicates adenovirus infection Interstitial cystitis causes chronic pelvic pain syndrome suprapubic pain when bladder filling and relieved by bladder empty hematuria and dysuria can be occurred later develop to contracted bladder 123
124 Malakoplakia uncommon inflammatory disease defect of phagocytic or degradative function of macrophages undigested bacteria accumulation within phagosomes macrophages contain laminated mineralized concretions known as Michaelis-Gutmann bodies Polypoid cystitis caused by inflammation condition resulting from irritation of bladder mucosa submucosal edema 124
125 K2: Neoplasms majority of bladder cancer is urothelial carcinoma the latter is squamous cell carcinoma, which related with urinary schistosomiasis (e.g. in Egypt) precursor of invasive urothelial carcinoma: 1) noninvasive papillary tumor (most common) 2) carcinoma in situ 125
126 Morphologic patterns of urothelial neoplasia 126
127 Papillary urothelial tumor, resembling coral within bladder 127
128 Noninvasive low-grade papillary urothelial carcinoma 128
129 Carcinoma in situ, hyperchromatic nuclei and a mitotic figure (arrow) 129
130 130
131 131
132 References 1. Robbins Basic Pathology (2018) 10 th Edition, Vinay Kumar, AbulK. Abbas, Jon C. Aster. Elsevier. 2. Rubins Pathology: Clinicopathologic Foundations of Medicine (2012) 6 th Edition, Raphael Rubin, David Strayer, Emanuel Rubin. Lippincott Williams & Wilkins 132
Functions of the kidney:
 Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
CYSTIC DISEASES of THE KIDNEY. Dr. Nisreen Abu Shahin
 CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Advanced Concept of Nursing- II UNIT-VI Advance Nursing Management of Genitourinary (GU) Diseases.
 In The Name of God (A PROJECT OF NEW LIFE COLLEGE OF NURSING KARACHI) Advanced Concept of Nursing- II UNIT-VI Advance Nursing Management of Genitourinary (GU) Diseases. Shahzad Bashir RN, BScN, DCHN,MScN
In The Name of God (A PROJECT OF NEW LIFE COLLEGE OF NURSING KARACHI) Advanced Concept of Nursing- II UNIT-VI Advance Nursing Management of Genitourinary (GU) Diseases. Shahzad Bashir RN, BScN, DCHN,MScN
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Chapter 20 Diseases of the kidney:
 Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Dr. Najla a Aldaoud. Omar Ayman Khasawneh
 Pathology 1 Congenital & Cystic diseases of the kidney Dr. Najla a Aldaoud Omar Ayman Khasawneh 1 P a g e Slides are included بسم هللا الرحمن الرحيم Today is our first pathology lectures, Dr Najla' will
Pathology 1 Congenital & Cystic diseases of the kidney Dr. Najla a Aldaoud Omar Ayman Khasawneh 1 P a g e Slides are included بسم هللا الرحمن الرحيم Today is our first pathology lectures, Dr Najla' will
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
DISEASES AFFECTING TUBULES AND INTERSTITIUM
 DISEASES AFFECTING TUBULES AND INTERSTITIUM Acute tubular injury (ATI) Pyelonephritis Drug-induced tubulointerstitial nephritis (TIN) Myeloma cast NP Renal stones Urinary outflow obstruction: hydronephrosis
DISEASES AFFECTING TUBULES AND INTERSTITIUM Acute tubular injury (ATI) Pyelonephritis Drug-induced tubulointerstitial nephritis (TIN) Myeloma cast NP Renal stones Urinary outflow obstruction: hydronephrosis
Renal pathophysiology.
 Renal pathophysiology basa.konecna@gmail.com Outline Intro basic structure & physiology Nephrotic syndrome Nephritic syndrome Acute renal failure Chronic kidney disease Gross structure and location Kidney
Renal pathophysiology basa.konecna@gmail.com Outline Intro basic structure & physiology Nephrotic syndrome Nephritic syndrome Acute renal failure Chronic kidney disease Gross structure and location Kidney
Some renal vascular disorders
 Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Renal Disease. Please refer to the assignment page Three online modules TBLs
 Renal Disease Please refer to the assignment page Three online modules TBLs 1 Renal Embryology 2 Lab Tests UA CBC Enzymes Creatinine Creatinine clearance Ammonia Abs C Bx 3 BUN Creatinine Creatinine Clearance
Renal Disease Please refer to the assignment page Three online modules TBLs 1 Renal Embryology 2 Lab Tests UA CBC Enzymes Creatinine Creatinine clearance Ammonia Abs C Bx 3 BUN Creatinine Creatinine Clearance
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System. Analyze the Anatomy and Physiology of the urinary system
 Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
network of thin-walled capillaries closely surrounded by a pear-shaped epithelial membrane called the Bowman s capsule
 Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Ordering Physician. Collected REVISED REPORT. Performed. IgG IF, Renal MCR. Lambda IF, Renal MCR. C1q IF, Renal. MCR Albumin IF, Renal MCR
 RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
Renal. Pathology. Kris%ne Kra*s, M.D.
 Renal Pathology Kris%ne Kra*s, M.D. Renal Pathology Outline Introductory stuff Glomerular diseases Tubular and inters%%al diseases Diseases involving blood vessels Cys%c diseases Tumors Renal Pathology
Renal Pathology Kris%ne Kra*s, M.D. Renal Pathology Outline Introductory stuff Glomerular diseases Tubular and inters%%al diseases Diseases involving blood vessels Cys%c diseases Tumors Renal Pathology
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
The Urinary System Pathology. Dr. Methaq Mueen د.ميثاق معين
 The Urinary System Pathology Dr. Methaq Mueen د.ميثاق معين objectives To Know normal anatomy physiology and histology of renal system To discuss Kidney pathology: congenital, cystic disease, Glmerular
The Urinary System Pathology Dr. Methaq Mueen د.ميثاق معين objectives To Know normal anatomy physiology and histology of renal system To discuss Kidney pathology: congenital, cystic disease, Glmerular
Tubulointerstitial Renal Disease. Anna Vinnikova, MD Division of Nephrology
 Tubulointerstitial Renal Disease Anna Vinnikova, MD Division of Nephrology Part I: Cystic Renal Disease www.pathguy.com Simple cysts Simple cysts May be multiple Usually 1 5cm, may be bigger Translucent,
Tubulointerstitial Renal Disease Anna Vinnikova, MD Division of Nephrology Part I: Cystic Renal Disease www.pathguy.com Simple cysts Simple cysts May be multiple Usually 1 5cm, may be bigger Translucent,
Renal Cystic Disease. Dr H Bierman
 Renal Cystic Disease Dr H Bierman Objectives Be able to diagnose renal cystic disease Genetic / non-genetic Be able to describe patterns of various renal cystic disease on routine imaging studies Be able
Renal Cystic Disease Dr H Bierman Objectives Be able to diagnose renal cystic disease Genetic / non-genetic Be able to describe patterns of various renal cystic disease on routine imaging studies Be able
Pathology of Hypertension
 2016-03-07 Pathology of Hypertension Honghe Zhang honghezhang@zju.edu.cn Tel:88208199 Department of Pathology ❶ Genetic predisposition ❷ Dietary factors ❸ Environmental factors ❹ Others Definition and
2016-03-07 Pathology of Hypertension Honghe Zhang honghezhang@zju.edu.cn Tel:88208199 Department of Pathology ❶ Genetic predisposition ❷ Dietary factors ❸ Environmental factors ❹ Others Definition and
Urinary tract pathology Renal syndromes Acute nephritic syndrome syndrome includes oliguria hematuria proteinuria edema hypertension typically occurs
 Urinary tract Structure [Figs. 13-1, 13-2] Kidneys (left and right) cortex (glomeruli and tubules) medulla (tubules, loops of Henle, and collecting ducts) calices and pelvis forming the collecting system
Urinary tract Structure [Figs. 13-1, 13-2] Kidneys (left and right) cortex (glomeruli and tubules) medulla (tubules, loops of Henle, and collecting ducts) calices and pelvis forming the collecting system
Glomerular pathology-2 Nephritic syndrome. Dr. Nisreen Abu Shahin
 Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Urinary system disorders Chapter 29
 Urinary system disorders Chapter 29 1 The Nephron Anatomy 2 Physiology 1.25 L per minute blood flow 25% of Cardiac Output Kidney compensates if one is lost - 2 weeks 3 Urine Formation 1. Filtration 2.
Urinary system disorders Chapter 29 1 The Nephron Anatomy 2 Physiology 1.25 L per minute blood flow 25% of Cardiac Output Kidney compensates if one is lost - 2 weeks 3 Urine Formation 1. Filtration 2.
AN APPROACH TO HEMATURIA. Dr Saima Ali
 AN APPROACH TO HEMATURIA Dr Saima Ali Definition Microscopic hematuria hematuria is defined as the presence of 5 or more RBCs per high-power field in 3 of 3 consecutive centrifuged specimens obtained at
AN APPROACH TO HEMATURIA Dr Saima Ali Definition Microscopic hematuria hematuria is defined as the presence of 5 or more RBCs per high-power field in 3 of 3 consecutive centrifuged specimens obtained at
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features.
 Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need
Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need
CLASSIFICATION OF RENAL DISEASE
 COMMONWEALTH OF AUSTRALIA Copyright Regulations 1969 WARNING This material has been reproduced and communicated to you by or on behalf of Adelaide University pursuant to Part VB of the Copyright Act 1968
COMMONWEALTH OF AUSTRALIA Copyright Regulations 1969 WARNING This material has been reproduced and communicated to you by or on behalf of Adelaide University pursuant to Part VB of the Copyright Act 1968
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
URINARY SYSTEM I. Kidneys II. Nephron Unit and Urine Formation
 URINARY SYSTEM I. Kidneys A. Location and Structure 1. Retroperitoneal 2. Between T12 and L3 3. Rt. kidney slightly lower 4. Two bean shaped organs 5. Adrenal gland 6. Internal construction a. Renal cortex
URINARY SYSTEM I. Kidneys A. Location and Structure 1. Retroperitoneal 2. Between T12 and L3 3. Rt. kidney slightly lower 4. Two bean shaped organs 5. Adrenal gland 6. Internal construction a. Renal cortex
Renal tumors of adults
 Renal tumors of adults Urinary Tract Tumors 2%-3% of all cancers in adults. The most common malignant tumor of the kidney is renal cell carcinoma. Tumors of the lower urinary tract are twice as common
Renal tumors of adults Urinary Tract Tumors 2%-3% of all cancers in adults. The most common malignant tumor of the kidney is renal cell carcinoma. Tumors of the lower urinary tract are twice as common
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
1. Disorders of glomerular filtration
 RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Tumors of kidney and urinary bladder
 Tumors of kidney and urinary bladder Overview of kidney tumors Benign and malignant Of the benign: papillary adenoma -cortical -small (0.5cm) -in 40% of population -clinically insignificant The most common
Tumors of kidney and urinary bladder Overview of kidney tumors Benign and malignant Of the benign: papillary adenoma -cortical -small (0.5cm) -in 40% of population -clinically insignificant The most common
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Lecture 7. The Urinary System
 Lecture 7 The Urinary System Copyright 2006 Thomson Delmar Learning The Urinary System The urinary system removes wastes from the body The urinary system also maintains homeostasis or a constant internal
Lecture 7 The Urinary System Copyright 2006 Thomson Delmar Learning The Urinary System The urinary system removes wastes from the body The urinary system also maintains homeostasis or a constant internal
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Basic Urinary Tract Anatomy and Histology
 Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
GLOMERULAR TUBULAR/INTERSTITIAL BLOOD VESSELS
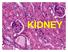 KIDNEY RENAL PATHOLOGY NORMAL CONGENITAL CYSTS GLOMERULAR TUBULAR/INTERSTITIAL BLOOD VESSELS OBSTRUCTION TUMORS 1. Renal Vein 2. Renal Artery 3. Renal Calyx 4. Medullary Pyramid 5. Renal Cortex 6. Segmental
KIDNEY RENAL PATHOLOGY NORMAL CONGENITAL CYSTS GLOMERULAR TUBULAR/INTERSTITIAL BLOOD VESSELS OBSTRUCTION TUMORS 1. Renal Vein 2. Renal Artery 3. Renal Calyx 4. Medullary Pyramid 5. Renal Cortex 6. Segmental
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Urinary tract infections, renal malformations and scarring
 Urinary tract infections, renal malformations and scarring Yaacov Frishberg, MD Division of Pediatric Nephrology Shaare Zedek Medical Center Jerusalem, ISRAEL UTI - definitions UTI = growth of bacteria
Urinary tract infections, renal malformations and scarring Yaacov Frishberg, MD Division of Pediatric Nephrology Shaare Zedek Medical Center Jerusalem, ISRAEL UTI - definitions UTI = growth of bacteria
Urinary System. Dr. Thorson
 Urinary System Dr. Thorson Lesson Objectives Upon completion of this lesson, students should be able to Define and spell the terms to learn for this chapter. Describe the purpose and function of the urinary
Urinary System Dr. Thorson Lesson Objectives Upon completion of this lesson, students should be able to Define and spell the terms to learn for this chapter. Describe the purpose and function of the urinary
Dr P Sigwadi 30 May 2012
 Dr P Sigwadi 30 May 2012 Introduction Haematuria Positive blood on urine dipstick 5 red blood cells/ microliter of urine Prevalence Gross haematuria ( macroscopic) 0.13 % Microscopic- 1.5% Haematuria +
Dr P Sigwadi 30 May 2012 Introduction Haematuria Positive blood on urine dipstick 5 red blood cells/ microliter of urine Prevalence Gross haematuria ( macroscopic) 0.13 % Microscopic- 1.5% Haematuria +
Crescentic Glomerulonephritis (RPGN)
 Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Day 1 Bell Work We will be discussing one of FIVE excretory organs in the human body. We have already studied four of them. The kidneys are considered
 URINARY SYSTEM 1 Day 1 Bell Work We will be discussing one of FIVE excretory organs in the human body. We have already studied four of them. The kidneys are considered the main organ in the excretory system.
URINARY SYSTEM 1 Day 1 Bell Work We will be discussing one of FIVE excretory organs in the human body. We have already studied four of them. The kidneys are considered the main organ in the excretory system.
HTN, retenopathy, edema, encephalopathy
 ARF Uremic syndrom Uremic syndrome (uremia) is a serious complication of CRF & ARF. It occurs when urea and other waste products build up in the body because the kidneys are unable to eliminate them. These
ARF Uremic syndrom Uremic syndrome (uremia) is a serious complication of CRF & ARF. It occurs when urea and other waste products build up in the body because the kidneys are unable to eliminate them. These
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
(Calcium and Phosphorus are a part of the CKD objectives)
 Course Objectives Electrolytes and Water: 1. Differentiate the effects of changes in sodium content from changes in water content 2. Describe how the body compensates for volume loss and volume overload
Course Objectives Electrolytes and Water: 1. Differentiate the effects of changes in sodium content from changes in water content 2. Describe how the body compensates for volume loss and volume overload
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
PATHOLOGY OF THE URINARY SYSTEM Dr. Ameer Dhahir Part one
 PATHOLOGY OF THE URINARY SYSTEM Dr. Ameer Dhahir Part one Objectives: Defining certain clinical terms related to urinary disorders. Describing the pathogenesis of glomerular diseases Defining certain clinical
PATHOLOGY OF THE URINARY SYSTEM Dr. Ameer Dhahir Part one Objectives: Defining certain clinical terms related to urinary disorders. Describing the pathogenesis of glomerular diseases Defining certain clinical
Urinary System Multiple Choice Practice Test. c. Kidneys have three protective layers d. The adrenal gland is located deep within the kidney
 Urinary System Multiple Choice Practice Test 1. Which of the following is a function of the urinary system? a. Regulates water b. Regulates balance of acids, bases, and electrolytes c. Filters waste from
Urinary System Multiple Choice Practice Test 1. Which of the following is a function of the urinary system? a. Regulates water b. Regulates balance of acids, bases, and electrolytes c. Filters waste from
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Nephritic vs. Nephrotic Syndrome
 Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Chapter 6: Genitourinary and Gastrointestinal Systems 93
 Chapter 6: Genitourinary and Gastrointestinal Systems 93 Chapter 6 Genitourinary and Gastrointestinal Systems Embryology Three sets of excretory organs or kidneys develop in human embryos: Pronephros:
Chapter 6: Genitourinary and Gastrointestinal Systems 93 Chapter 6 Genitourinary and Gastrointestinal Systems Embryology Three sets of excretory organs or kidneys develop in human embryos: Pronephros:
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Pathophysiology. Renal basic structure / function. Page 1. JP Advis DVM, Ph.D. Bartlett Hall, Animal Sciences, Cook, ,
 Pathophysiology JP Advis DVM, Ph.D. Bartlett Hall, Animal Sciences, Cook, 932-9240, advis@aesop.rutgers.edu 17 Course website: rci.rutgers.edu/~advis Lectures, tests, grades, office hours, textbook, Material
Pathophysiology JP Advis DVM, Ph.D. Bartlett Hall, Animal Sciences, Cook, 932-9240, advis@aesop.rutgers.edu 17 Course website: rci.rutgers.edu/~advis Lectures, tests, grades, office hours, textbook, Material
Renal and Urinary Tract Disorders
 Renal and Urinary Tract Disorders Objectives: Congenital Kidney Disorders, Obstructive Kidney Disorders and Kidney cancer. Glomerular and Tubulointerstitial Disorders Acute Kidney Injury and Chronic Kidney
Renal and Urinary Tract Disorders Objectives: Congenital Kidney Disorders, Obstructive Kidney Disorders and Kidney cancer. Glomerular and Tubulointerstitial Disorders Acute Kidney Injury and Chronic Kidney
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
II.Tubulointerstitial diseases
 II.Tubulointerstitial diseases two major groups of processes (1) ischemic or toxic tubular injury, leading to acute kidney injury (AKI) and acute renal failure, and (2) inflammatory reactions of the tubules
II.Tubulointerstitial diseases two major groups of processes (1) ischemic or toxic tubular injury, leading to acute kidney injury (AKI) and acute renal failure, and (2) inflammatory reactions of the tubules
Chapter 14 The Urinary System. Anatomy
 Chapter 14 The Urinary System Anatomy 14.1 Overview Role in removal of wastes to maintain homeostasis Acts as filtering system of the blood Produces urine Removes wastes, maintains ph, electrolyte composition,
Chapter 14 The Urinary System Anatomy 14.1 Overview Role in removal of wastes to maintain homeostasis Acts as filtering system of the blood Produces urine Removes wastes, maintains ph, electrolyte composition,
UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys.
 UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys. 1-3% of Below 1 yr. male: female ratio is 4:1 especially among uncircumcised males,
UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys. 1-3% of Below 1 yr. male: female ratio is 4:1 especially among uncircumcised males,
Genetics in Nephrology. Saeid Morovvati Associate Professor of BMSU Director of Biogene Laboratory
 Genetics in Nephrology Saeid Morovvati Associate Professor of BMSU Director of Biogene Laboratory Genetics in: A. Congenital Anomalies of the Kidney and Urinary Tract B. Cystic Diseases of the Kidney C.
Genetics in Nephrology Saeid Morovvati Associate Professor of BMSU Director of Biogene Laboratory Genetics in: A. Congenital Anomalies of the Kidney and Urinary Tract B. Cystic Diseases of the Kidney C.
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a.
 I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Diseases of the Kidney. Janos Vasko
 Diseases of the Kidney Janos Vasko Congenital anomalies Glomerular diseases Tubulointerstitial diseases Infections Vascular diseases Stones Tumours POLYCYSTIC KIDNEY DISEASE INFANTILE TYPE ADULT TYPE Autosomal
Diseases of the Kidney Janos Vasko Congenital anomalies Glomerular diseases Tubulointerstitial diseases Infections Vascular diseases Stones Tumours POLYCYSTIC KIDNEY DISEASE INFANTILE TYPE ADULT TYPE Autosomal
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
ESRD Dialysis Prevalence - One Year Statistics
 Age Group IL Other Total 00-04 12 1 13 05-09 5 2 7 10-14 15 1 16 15-19 55 2 57 20-24 170 10 180 25-29 269 14 283 30-34 381 9 390 35-39 583 14 597 40-44 871 20 891 45-49 1,119 20 1,139 50-54 1,505 35 1,540
Age Group IL Other Total 00-04 12 1 13 05-09 5 2 7 10-14 15 1 16 15-19 55 2 57 20-24 170 10 180 25-29 269 14 283 30-34 381 9 390 35-39 583 14 597 40-44 871 20 891 45-49 1,119 20 1,139 50-54 1,505 35 1,540
27-Apr-15 1 UAF ANOMALIES OF DEVELOPMENT RENAL SYSTEM - 1 DR. MUHAMMAD TARIQ JAVED UAF UAF
 RENAL SYSTEM - 1 DR. MUHAMMAD TARIQ JAVED Professor, Department of Pathology, Faculty of Veterinary Science, University of Agriculture, Faisalabad, Pakistan. Email: mtjaved@uaf.edu.pk RENAL AGENESIS Renal
RENAL SYSTEM - 1 DR. MUHAMMAD TARIQ JAVED Professor, Department of Pathology, Faculty of Veterinary Science, University of Agriculture, Faisalabad, Pakistan. Email: mtjaved@uaf.edu.pk RENAL AGENESIS Renal
Functions of the Urinary System
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
Interpretation of Renal Transplant Biopsy. Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA
 Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Renal Pathology 1: Glomerulus. With many thanks to Elizabeth Angus PhD for EM photographs
 Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis
 GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Chapter 11 Lecture Outline
 Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
H I S T O L O G Y O F T H E U R I N A R Y S Y S T E M
 SCPA 602- Anatomical Basis For Pathological Study H I S T O L O G Y O F T H E U R I N A R Y S Y S T E M S O M P H O N G N A R K P I N I T, M. D. D E P A R T M E N T O F P A T H O B I O L O G Y F A C U
SCPA 602- Anatomical Basis For Pathological Study H I S T O L O G Y O F T H E U R I N A R Y S Y S T E M S O M P H O N G N A R K P I N I T, M. D. D E P A R T M E N T O F P A T H O B I O L O G Y F A C U
The Excretory System
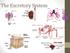 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
