Approximately one-third of newly diagnosed epilepsy
|
|
|
- Archibald Newton
- 5 years ago
- Views:
Transcription
1 clinical article J Neurosurg 122: , 2015 Intraoperative computed tomography for intracranial electrode implantation surgery in medically refractory epilepsy Darrin J. Lee, MD, PhD, 1 Marike Zwienenberg-Lee, MD, 1 Masud Seyal, MD, PhD, 2 and Kiarash Shahlaie, MD, PhD 1,2 Departments of 1 Neurological Surgery and 2 Neurology, UC Davis School of Medicine, Sacramento, California Object Accurate placement of intracranial depth and subdural electrodes is important in evaluating patients with medically refractory epilepsy for possible resection. Confirming electrode locations on postoperative CT scans does not allow for immediate replacement of malpositioned electrodes, and thus revision surgery is required in select cases. Intraoperative CT (ict) using the Medtronic O-arm device has been performed to detect electrode locations in deep brain stimulation surgery, but its application in epilepsy surgery has not been explored. In the present study, the authors describe their institutional experience in using the O-arm to facilitate accurate placement of intracranial electrodes for epilepsy monitoring. Methods In this retrospective study, the authors evaluated consecutive patients who had undergone subdural and/or depth electrode implantation for epilepsy monitoring between November 2010 and September The O-arm device is used to obtain ict images, which are then merged with the preoperative planning MRI studies and reviewed by the surgical team to confirm final positioning. Minor modifications in patient positioning and operative field preparation are necessary to safely incorporate the O-arm device into routine intracranial electrode implantation surgery. The device does not obstruct surgeon access for bur hole or craniotomy surgery. Depth and subdural electrode locations are easily identified on ict, which merge with MRI studies without difficulty, allowing the epilepsy surgical team to intraoperatively confirm lead locations. Results Depth and subdural electrodes were implanted in 10 consecutive patients by using routine surgical techniques together with preoperative stereotactic planning and intraoperative neuronavigation. No wound infections or other surgical complications occurred. In one patient, the hippocampal depth electrode was believed to be in a suboptimal position and was repositioned before final wound closure. Additionally, 4 strip electrodes were replaced due to suboptimal positioning. Postoperative CT scans did not differ from ict studies in the first 3 patients in the series and thus were not obtained in the final 7 patients. Overall, operative time was extended by approximately minutes for O-arm positioning, less than 1 minute for image acquisition, and approximately 10 minutes for image transfer, fusion, and intraoperative analysis (total time minutes). Conclusions The O-arm device can be easily incorporated into routine intracranial electrode implantation surgery in standard-sized operating rooms. The technique provides accurate 3D visualization of depth and subdural electrode contacts, and the intraoperative images can be easily merged with preoperative MRI studies to confirm lead positions before final wound closure. Intraoperative CT obviates the need for routine postoperative CT and has the potential to improve the accuracy of intracranial electroencephalography recordings and may reduce the necessity for revision surgery. Key Words epilepsy; intraoperative computed tomography; image-guided surgery; electroencephalography Approximately one-third of newly diagnosed epilepsy cases are refractory to medical management, and patients in these cases may be appropriate candidates for surgical intervention. 9,15 The patients often undergo intracranial electroencephalography (EEG) monitoring via implanted subdural and/or depth electrodes to identify a seizure onset zone. Subdural electrode strips and grids are sometimes implanted through bur holes or Abbreviations DBS = deep brain stimulation; EEG = electroencephalography; ict = intraoperative CT; imri = intraoperative MRI. Submitted May 3, Accepted September 23, include when citing Published online October 31, 2014; DOI: / JNS Disclosure The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. This study was supported by the UC Davis Bronte Epilepsy Research Program. 526 AANS, 2015
2 Intraoperative computed tomography in epilepsy surgery beyond the edges of a craniotomy; therefore, direct visualization of their final position may not be possible. Depth electrodes are often placed with a high degree of accuracy using stereotactic guidance but can occasionally be malpositioned as a result of errors in depth placement and/or lead deviation. Subdural grid and strip electrodes are more prone to suboptimal positioning since they are sometimes passed through a bur hole or beyond craniotomy edges. 10 Accurate placement of invasive EEG electrodes is important for correctly identifying a seizure onset zone that may be appropriate for resection. Preoperative MRI is typically used to evaluate for structural lesions and to plan electrode placement, and postoperative CT is often performed to confirm electrode placement. 2,6 This approach is problematic, however, since the repositioning of electrodes using this strategy requires an additional operation. Intraoperative fluoroscopy can be used to confirm electrode implantation relative to a stereotactic frame, but it is not effective in frameless operations. Moreover, fluoroscopy is limited in its ability to detect medial and/or lateral lead deviations, and radiographic studies do not easily fuse with preoperative neuronavigation plans developed from CT and MRI. 4,11 Intraoperative CTs (icts) can be obtained in standard operating rooms using the portable O-arm image acquisition system (Medtronic Inc.). This technique has been described in deep brain stimulation (DBS) surgery for confirming the accurate placement of electrodes into deep brain structures, 14 but its use in epilepsy surgery has not been investigated. In the present study, we report our institutional experience using the O-arm to facilitate accurate placement of intracranial electrodes for epilepsy monitoring. Methods The UC Davis Institutional Review Board approved this chart review. In this retrospective study, we evaluated consecutive patients who had undergone subdural and/or depth electrode implantation for epilepsy monitoring between November 2010 and September Preoperative Planning All patients undergo routine preoperative MRI as part of the evaluation for surgical intervention, and subsequent volumetric contrast-enhanced T1-weighted 3D MRI is performed for surgical planning. The StealthStation Cranial software package (Medtronic Inc.) is used, with the Brain Biopsy module selected for electrode planning. Surgical plans are developed for subdural electrode placement by creating a 3D rendering of the surface anatomy (Fig. 1). Depth electrode plans are developed using entry points and trajectories that meet the following criteria: 1) entering in the crest of the middle or inferior temporal gyrus, 2) avoiding transgression of a cortical sulcus, and 3) avoiding injury to visible vascular structures. O-Arm Positioning and Intraoperative Imaging After the induction of general anesthesia, the patient s head is secured in a Mayfield head clamp and attached to the operating table using a modified connector that will accommodate the gantry of the O-arm device. 14 Patient arms are padded and tucked such that arm boards can be removed, minimizing the table width that will be needed to accommodate the diameter of the O-arm gantry. If a standard operating table is used, the head and foot orientation is reversed to maximize the distance between the head of the bed and the base of the operating table. If a sliding table is used, it is slid to the head end of the bed to maximize this distance. The O-arm is then moved into position using techniques described elsewhere. 14 These techniques are modified for epilepsy surgery by sliding the O-arm below the patient s shoulders to provide maximal access to the head. The reference arc for the StealthStation navigation is positioned above the vertex of the head to provide direct line of sight to the infrared detection device without obstruction from the O-arm gantry. Specifically, the O-arm gantry is positioned around the torso at the level of the upper chest to allow access to create bur holes or larger craniotomies when necessary. The operative field is then prepared in a routine fashion, and a clear hip or shower curtain drape is used to cover the operative field as well as the anterior half of the O-arm machine (Fig. 2). This allows the O-arm to be moved between an operating/surgeon and an imaging/ anesthesia position without compromising the sterility of the operative field. Draping the operative field to include the O-arm gantry requires 3 people (primary surgeon, assistant surgeon or scrub technician, and non-scrubbed circulator) and is technically simple. By allowing sufficient redundancy in drape material between the patient s head and the O-arm ring, the machine is easily moved between the operating and imaging positions without compromising the sterility of the surgical field or colliding with the neuronavigation frame or other sterile equipment. Analysis of Intraoperative CT Scans After depth electrodes are placed, tunneled, and temporarily secured, the O-arm is moved to the imaging position to acquire an ict scan, which is obtained using previously described techniques that involve the entire convexity of the skull and skull base. 14 We immediately transfer O-arm images to the StealthStation surgical navigation system via a direct Ethernet/Cat5 connection, and the Automerge function is used to fuse the ict study with the preoperative 3D MRI study (Fig. 3). For successful fusion of ict and MRI, studies are obtained using the 3D and Medium settings of the O-arm, and care is taken to ensure that the entire convexity and skull base are included in the ict study. To determine if any modifications or replacements are necessary prior to final closure, we confirm the location of subdural grid and strip electrodes on a 3D rendering of the brain surface (Fig. 1). Depth electrode entry point, trajectory, and tip location are compared with those from the preoperative plan. Results Patient Population Ten patients underwent implantation of subdural and depth electrodes for invasive epilepsy monitoring at our Level 4 epilepsy center. The patient series included 6 wom- 527
3 D. J. Lee et al. Fig. 1. Three-dimensional surface-rendering images created on a Medtronic StealthStation to guide placement of subdural grid and strip electrodes. The preoperative MR image (A) was merged with the ict study in the operating room for immediate confirmation of subdural lead locations (B). Postoperatively, the merged image was processed to yield a 3D map of electrode locations that could be used for interpreting extraoperative EEG data (C). Blue dots represent strip electrodes, and white dots represent grid points. en and 4 men, with an average age of 33 years. All patients underwent placement of subdural electrodes (strips and/or grids), and 8 of the 10 patients had mesial temporal lobe depth electrodes placed as well (Table 1). Four patients underwent a second-stage resection for focal epilepsy. in this series and were identical to the ict scans with respect to electrode lead locations. One depth electrode was replaced because of suboptimal positioning of the electrode tip, which was posterior and lateral to the intended hippocampal target. Electrode Repositioning One hundred four subdural electrode arrays were placed in 10 patients using ict confirmation; the series included 45 temporal lobe strips, 48 frontal lobe strips, and 11 grid arrays. Four strips were replaced because of suboptimal positioning, including 1 anterior temporal and 3 inferior/ventral temporal strips. Thirty depth electrodes were placed in 8 of the 10 patients using ict to confirm final implantation. Postoperative CT scans were also obtained in the first 3 patients Complications There were no surgical site infections in this clinical series. Operative time was extended by approximately minutes for positioning the O-arm, less than 1 minute for image acquisition, and approximately 10 minutes for image transfer, fusion, and intraoperative analysis (total time minutes). In cases in which electrode repositioning was performed, the operative time was prolonged approximately 12 minutes to reposition electrodes and confirm final location with a repeat ict scan. Fig. 2. Example of operating room setup of the O-arm gantry and intraoperative navigation system. In the operating/surgeon position (A), operative access is maximized, and the navigation equipment is in a midline position that does not interfere with the surgical field (B). In the imaging/anesthesia position (C), the sterility of the operative field is maintained, and navigation and stereotactic equipment are not disturbed. 528
4 Intraoperative computed tomography in epilepsy surgery Fig. 3. Images obtained on a Medtronic StealthStation system during subdural and depth electrode placement for invasive epilepsy monitoring. Preoperative MRI was used to develop a plan to place the right hippocampal depth electrode, stereotactic guidance was used to implant the electrode along the planned trajectory, and an intraoperative CT scan was obtained and then merged with the preoperative MRI study to confirm trajectory and depth as well as the final anatomical location of the electrode. Discussion In this study, we demonstrated the feasibility of incorporating the O-arm machine into routine epilepsy surgery to facilitate the accurate placement of intracranial recording electrodes. Simple technical modifications allow the machine to be positioned such that it does not interfere with surgical access to the patient for bur hole or craniotomy procedures and can be easily moved between operating and imaging positions while maintaining the integrity of the sterile field. Intraoperative CT easily merges with preoperative planning studies to provide accurate 3D confirmation of subdural and depth electrode placement, allowing any necessary positioning adjustments to be made before leaving the operating room. This technique has the potential to improve the accuracy and quality of invasive EEG data and reduce the need for reoperation to replace electrodes. The ability to obtain 3D imaging data during neurosurgical procedures has many potential benefits and has been a topic of interest for the past few decades. Intraoperative MRI (imri) can provide excellent visualization of the brain anatomy, but it can only be performed in dedicated operative MRI suites or with smaller imri devices that have more limited imaging capabilities. Because of the ferromagnetic qualities of standard invasive electrodes and the intraoperative equipment needed to interrogate them during surgery, imri is not a feasible option for 3D imaging during invasive EEG electrode implantation. Intraoperative 3D imaging has been described in a variety of neurosurgical applications, including CT for brain tumor or skull base biopsy 3,8 and 3D fluoroscopy for different spine operations. 7,12,13,17 Over the past few years, interest in using intraoperative CT scanning to confirm placement of DBS electrodes has been increasing. The Medtronic TABLE 1. Electrode implantation patient series Right Electrodes Left Electrodes Patient Age (yrs), Sex Frontal Depths Grids Frontal Depths Grids 40, F , F , M , F , M , M , F , M , F , F Total
5 D. J. Lee et al. O-arm is a portable device that is available at most institutions given its use in spine surgery. The O-arm can be easily incorporated into standard frame-based 1,5,14 and frameless 16 DBS surgery with simple technical modifications. This imaging technique has been shown to provide accurate depictions of lead locations and has the potential to reduce the number of malpositioned DBS electrodes that might require subsequent revision surgery. 14 In the present study, we confirmed that these advantages of ict extend to epilepsy surgery. The techniques used to incorporate the O-arm device are simple to apply in standard-sized operating rooms and do not interfere with the ability to safely perform bilateral bur hole or craniotomy procedures to implant electrodes. Furthermore, direct line of sight can be maintained between the infrared detection device of neuronavigation systems and the aiming guides used for depth electrode implantation, so that current surgical procedures need not be modified. Computed tomography images can be obtained at any stage of the operation and can be used to confirm the location of depth and surface electrodes using preexisting software packages that rapidly merge ict with preoperative planning MRI studies. The technique has many potential advantages: 1) more useful intraoperative diagnostic EEG data given accurate placement of electrode contacts, 2) ability to reposition malpositioned electrodes before closing the surgical wound, 3) decreased hospital stay because of a reduced reoperation rate, and 4) no need for routine postoperative CT scanning to confirm electrode positions, reducing the need for patient transport after electrode implantation. The potential drawbacks to this technique warrant consideration. First, the O-arm provides excellent visualization of bone and implanted hardware (for example, electrode contacts), but it is inadequate for soft-tissue imaging. As a result, it cannot be used to reliably identify the presence of an intracranial hematoma, and the location of an electrode relative to deep brain structures can only be deduced by fusing O-arm images with preoperative MRI studies. If there is significant concern regarding intracerebral hematoma from the operation, a routine postoperative CT scan will still be necessary. In facilities with an operative CT suite (rather than a portable device), the intraoperative scan could provide adequate imaging of soft tissue and/or a hematoma as well as the electrode contacts. Second, the O-arm is large, and careful planning is required to maintain field sterility and provide adequate surgical access. We did not have any wound infections or other intraoperative complications associated with the presence of the O-arm machine during surgery, but it is important to note that our surgical team had significant experience using the O-arm during DBS surgery and other intracranial neurosurgical procedures before we incorporated the device into our surgical epilepsy practice. Moreover, repeat imaging with the O-arm introduces the possibility of increased patient exposure to ionizing radiation, particularly if electrodes are repositioned and an additional ict scan is obtained. Zhang et al. have characterized O-arm dosimetry 18 and have shown that when the O-arm is set at the 3D imaging mode it delivers 50% of the radiation dose of a 64-slice CT scanner. Thus, for patients who do not require repeat intraoperative or postoperative imaging, the O-arm has the potential to reduce total radiation exposure that would otherwise occur with routine postoperative CT scans. Finally, if an O-arm device is not already available at a particular institution, there is a significant capital cost associated with purchasing the device that could increase the costs of ict-assisted intracranial electrode implantation surgery. Conclusions The O-arm device can be easily incorporated into routine electrode implantation surgery with minimal effects on operative time. By merging ict images with preoperative MRI studies, the surgical team can visually confirm subdural and depth electrode positions before final wound closure. This approach improves the accuracy of intracranial electrode placement and may reduce the necessity for revision surgery. References 1. Caire F, Gantois C, Torny F, Ranoux D, Maubon A, Moreau JJ: Intraoperative use of the Medtronic O-arm for deep brain stimulation procedures. Stereotact Funct Neurosurg 88: , Chamoun RB, Nayar VV, Yoshor D: Neuronavigation applied to epilepsy monitoring with subdural electrodes. Neurosurg Focus 25(3):E21, Engle DJ, Lunsford LD: Brain tumor resection guided by intraoperative computed tomography. J Neurooncol 4: , Erõss L, Bagó AG, Entz L, Fabó D, Halász P, Balogh A, et al: Neuronavigation and fluoroscopy-assisted subdural strip electrode positioning: a simple method to increase intraoperative accuracy of strip localization in epilepsy surgery. Technical note. J Neurosurg 110: , Fiegele T, Feuchtner G, Sohm F, Bauer R, Anton JV, Gotwald T, et al: Accuracy of stereotactic electrode placement in deep brain stimulation by intraoperative computed tomography. Parkinsonism Relat Disord 14: , Hogan RE, Lowe VJ, Bucholz RD: Triple-technique (MR imaging, single-photon emission CT, and CT) coregistration for image-guided surgical evaluation of patients with intractable epilepsy. AJNR Am J Neuroradiol 20: , Ito Y, Sugimoto Y, Tomioka M, Hasegawa Y, Nakago K, Yagata Y: Clinical accuracy of 3D fluoroscopy-assisted cervical pedicle screw insertion. Clinical article. J Neurosurg Spine 9: , Kitai R, Sato K, Ido K, Sakuma T, Handa Y, Kubota T: Single burr hole surgery for the spheno-orbital fibrous dysplasia using intraoperative computed tomography. Minim Invasive Neurosurg 48:44 46, Kwan P, Sander JW: The natural history of epilepsy: an epidemiological view. J Neurol Neurosurg Psychiatry 75: , LaViolette PS, Rand SD, Ellingson BM, Raghavan M, Lew SM, Schmainda KM, et al: 3D visualization of subdural electrode shift as measured at craniotomy reopening. Epilepsy Res 94: , Miller KJ, Makeig S, Hebb AO, Rao RPN, dennijs M, Ojemann JG: Cortical electrode localization from X-rays and simple mapping for electrocorticographic research: the Location on Cortex (LOC) package for MATLAB. J Neurosci Methods 162: ,
6 Intraoperative computed tomography in epilepsy surgery 12. Nottmeier EW, Seemer W, Young PM: Placement of thoracolumbar pedicle screws using three-dimensional image guidance: experience in a large patient cohort. Clinical article. J Neurosurg Spine 10:33 39, Rajasekaran S, Vidyadhara S, Shetty AP: Intra-operative Iso- C3D navigation for pedicle screw instrumentation of hangman s fracture: a case report. J Orthop Surg (Hong Kong) 15:73 77, Shahlaie K, Larson PS, Starr PA: Intraoperative computed tomography for deep brain stimulation surgery: technique and accuracy assessment. Neurosurgery 68 (1 Suppl Operative): , Sillanpää M, Schmidt D: Natural history of treated childhood-onset epilepsy: prospective, long-term population-based study. Brain 129: , Smith AP, Bakay RA: Frameless deep brain stimulation using intraoperative O-arm technology. Clinical article. J Neurosurg 115: , Villavicencio AT, Burneikiene S, Bulsara KR, Thramann JJ: Intraoperative three-dimensional fluoroscopy-based computerized tomography guidance for percutaneous kyphoplasty. Neurosurg Focus 18(3):E3, Zhang J, Weir V, Fajardo L, Lin J, Hsiung H, Ritenour ER: Dosimetric characterization of a cone-beam O-arm imaging system. J XRay Sci Technol 17: , 2009 Author Contributions Conception and design: Shahlaie, Zwienenberg-Lee. Acquisition of data: Shahlaie, Lee, Seyal. Analysis and interpretation of data: Shahlaie, Lee, Zwienenberg-Lee. Drafting the article: Lee. Critically revising the article: all authors. Reviewed submitted version of manuscript: all authors. Approved the final version of the manuscript on behalf of all authors: Shahlaie. Study supervision: Shahlaie. Correspondence Kiarash Shahlaie, Department of Neurological Surgery, University of California, Davis School of Medicine, 4860 Y St., Ste. 3740, Sacramento, CA krshahlaie@ucdavis. edu. 531
The American Approach to Depth Electrode Insertion December 4, 2012
 The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
Introduction of FIREFLY Technology
 Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT. Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018
 EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
Intraoperative case studies. Portable full body 32-slice CT scanner
 Intraoperative case studies Portable full body 32-slice CT scanner Point-of-care CT imaging Your multi-departmental imaging solution Orthopedic surgery Arthroplasty Musculoskeletal disorders Hip replacement
Intraoperative case studies Portable full body 32-slice CT scanner Point-of-care CT imaging Your multi-departmental imaging solution Orthopedic surgery Arthroplasty Musculoskeletal disorders Hip replacement
Multimodal Imaging in Extratemporal Epilepsy Surgery
 Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study
 Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Go Yoshida, Tokumi Kanemura, Yoshimoto Ishikawa. Department of Orthopedic Surgery, Spine Center, Konan Kosei Hospital, Konan, Japan
 194 Asian / Spine Journal Vol. 6, No. 3, pp 194~198, 2012 ASJ: Vol. 6, No. 3, 2012 http://dx.doi.org/10.4184/asj.2012.6.3.194 Percutaneous Pedicle Screw Fixation of a Hangman s Fracture Using Intraoperative,
194 Asian / Spine Journal Vol. 6, No. 3, pp 194~198, 2012 ASJ: Vol. 6, No. 3, 2012 http://dx.doi.org/10.4184/asj.2012.6.3.194 Percutaneous Pedicle Screw Fixation of a Hangman s Fracture Using Intraoperative,
Error analysis in neuronavigation
 Fakultät für Informatik - Humanoids and Intelligence Systems Lab Institut für Anthropomatik Mittwochs von 12:15-13:45 Error analysis in neuronavigation Uwe Spetzger Neurochirurgische Klinik, Klinikum Karlsruhe
Fakultät für Informatik - Humanoids and Intelligence Systems Lab Institut für Anthropomatik Mittwochs von 12:15-13:45 Error analysis in neuronavigation Uwe Spetzger Neurochirurgische Klinik, Klinikum Karlsruhe
SUPPLEMENTAL DIGITAL CONTENT
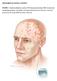 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Neuronavigation applied to epilepsy monitoring with subdural electrodes
 Neurosurg Focus 25 (3):E21, 2008 Neuronavigation applied to epilepsy monitoring with subdural electrodes Technical note ROUKOZ B. CHAMOUN, M.D., VIKRAM V. NAYAR, M.D., AND DANIEL YOSHOR, M.D. Department
Neurosurg Focus 25 (3):E21, 2008 Neuronavigation applied to epilepsy monitoring with subdural electrodes Technical note ROUKOZ B. CHAMOUN, M.D., VIKRAM V. NAYAR, M.D., AND DANIEL YOSHOR, M.D. Department
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective
 Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan
 Keeping up with technology Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan Abdullah al-akayleh Department of Neuosurgery, King Hussean Medical Center, Jordan. ABSTRACT
Keeping up with technology Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan Abdullah al-akayleh Department of Neuosurgery, King Hussean Medical Center, Jordan. ABSTRACT
Disclosures. Sacroiliac Joint (SIJ) Pain. Modified Triplanar Fluoroscopic Approach in Percutaneous Fixation of Sacroiliac Joint 5/12/2017
 Modified Triplanar Fluoroscopic Approach in Percutaneous Fixation of Sacroiliac Joint J.E. Barrett, M.D. Atlanta Medical Center Atlanta Trauma Symposium 22 April 2017 Disclosures None Sacroiliac Joint
Modified Triplanar Fluoroscopic Approach in Percutaneous Fixation of Sacroiliac Joint J.E. Barrett, M.D. Atlanta Medical Center Atlanta Trauma Symposium 22 April 2017 Disclosures None Sacroiliac Joint
Surgery for Medically Refractory Focal Epilepsy
 Surgery for Medically Refractory Focal Epilepsy Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence
Surgery for Medically Refractory Focal Epilepsy Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence
W. CHRISTOPHER FOX, M.D., 1 SCOTT WAWRZYNIAK, 2 AND WILLIAM F. CHANDLER, M.D. 1. be very useful during transsphenoidal pituitary surgery as well.
 J Neurosurg 108:746 750, 2008 Intraoperative acquisition of three-dimensional imaging for frameless stereotactic guidance during transsphenoidal pituitary surgery using the Arcadis Orbic System W. CHRISTOPHER
J Neurosurg 108:746 750, 2008 Intraoperative acquisition of three-dimensional imaging for frameless stereotactic guidance during transsphenoidal pituitary surgery using the Arcadis Orbic System W. CHRISTOPHER
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Since its introduction in spine surgery, pedicle screw
 SPINE Volume 37, Number 25, pp E1580 E1587 2012, Lippincott Williams & Wilkins SURGERY A Prospective Multicenter Registry on the Accuracy of Pedicle Screw Placement in the Thoracic, Lumbar, and Sacral
SPINE Volume 37, Number 25, pp E1580 E1587 2012, Lippincott Williams & Wilkins SURGERY A Prospective Multicenter Registry on the Accuracy of Pedicle Screw Placement in the Thoracic, Lumbar, and Sacral
ChosingPhase 2 Electrodes
 ChosingPhase 2 Electrodes ACNS Course ECoG/Invasive EEG Houston, February 4 th, 2015 Stephan Schuele, MD, MPH Comprehensive Epilepsy Center Northwestern Memorial Hospital Northwestern University, Feinberg
ChosingPhase 2 Electrodes ACNS Course ECoG/Invasive EEG Houston, February 4 th, 2015 Stephan Schuele, MD, MPH Comprehensive Epilepsy Center Northwestern Memorial Hospital Northwestern University, Feinberg
Faculty/Presenter Disclosure. Intracranial EEG Recording. Objectives. General Themes. Why invasive recordings? 6/27/2018
 CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure Intracranial EEG Recording Faculty: Dr Richard S McLachlan Relationships with financial sponsors: None currently
CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure Intracranial EEG Recording Faculty: Dr Richard S McLachlan Relationships with financial sponsors: None currently
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Difficult-to-Localize Intractable Focal Epilepsy: An In-Depth Look
 Current Literature In Clinical Science Difficult-to-Localize Intractable Focal Epilepsy: An In-Depth Look Stereoelectroencephalography in the Difficult to Localize Refractory Focal Epilepsy: Early Experience
Current Literature In Clinical Science Difficult-to-Localize Intractable Focal Epilepsy: An In-Depth Look Stereoelectroencephalography in the Difficult to Localize Refractory Focal Epilepsy: Early Experience
BAK/C Cervical Anterior Interbody Fusion System
 Surgical Technique BAK/C Cervical Anterior Interbody Fusion System The Comfortable Choice for Cervical Fusion BAK/C Cervical Surgical Technique 1 The BAK/C Cervical Fusion System is an alternative to conventional
Surgical Technique BAK/C Cervical Anterior Interbody Fusion System The Comfortable Choice for Cervical Fusion BAK/C Cervical Surgical Technique 1 The BAK/C Cervical Fusion System is an alternative to conventional
Single-Thread Screw Available in 25-45mm lengths (5mm Increments) Dual-Thread Screw Available in 30-45mm lengths (5mm Increments)
 Single-Thread Screw Available in 25-45mm lengths (5mm Increments) Dual-Thread Screw Available in 30-45mm lengths (5mm Increments) 4.5mm diameter screws All screws cannulated 12mm percutaneous incision
Single-Thread Screw Available in 25-45mm lengths (5mm Increments) Dual-Thread Screw Available in 30-45mm lengths (5mm Increments) 4.5mm diameter screws All screws cannulated 12mm percutaneous incision
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Signature Personalized Patient Care
 Surgical Technique Acetabular Guide System Contents One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Surgical Technique Acetabular Guide System Contents One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Asnis. Micro Cannulated screw system. Xpress operative technique
 Asnis Micro Cannulated screw system Xpress operative technique Asnis Micro Cannulated screw system Table of contents Indications, precautions & contraindications 3 Operative technique 4 This publication
Asnis Micro Cannulated screw system Xpress operative technique Asnis Micro Cannulated screw system Table of contents Indications, precautions & contraindications 3 Operative technique 4 This publication
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
A Patient s Guide to SRS
 A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE
 OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE Authors: Daipayan Guha 1, Raphael J akubovic 2, Shaurya Gupta 1, Albert
OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE Authors: Daipayan Guha 1, Raphael J akubovic 2, Shaurya Gupta 1, Albert
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Technique Guide. C1/C2 Access System. Percutaneous transarticular screw fixation.
 Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Primary low-grade brain tumors in
 O R I G I N A L A R T I C L E S Copyright 2009, Barrow Neurological Institute Functional Cortical Mapping Using Subdural Grid Electrodes in Patients with Low-Grade Gliomas Presenting with Seizure Andrew
O R I G I N A L A R T I C L E S Copyright 2009, Barrow Neurological Institute Functional Cortical Mapping Using Subdural Grid Electrodes in Patients with Low-Grade Gliomas Presenting with Seizure Andrew
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
The Changing Surgical Landscape in Kids
 The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Introduction. Case. Case Report. Jin-gyu Choi 1, Si-hoon Lee 2, Young-Min Shon 2,3, Byung-chul Son 1,3
 96 Journal of Epilepsy Research Vol. 5, No. 2, 2015 Long-Term Migration of a Deep Brain Stimulation (DBS) Lead in the Third Ventricle Caused by Cerebral Atrophy in a Patient with Anterior Thalamic Nucleus
96 Journal of Epilepsy Research Vol. 5, No. 2, 2015 Long-Term Migration of a Deep Brain Stimulation (DBS) Lead in the Third Ventricle Caused by Cerebral Atrophy in a Patient with Anterior Thalamic Nucleus
WINSTA-C. Clavicle Plating System
 Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
IMAGE-GUIDED SPINE SURGERY
 SPINE NAVIGATION IMAGE-GUIDED SPINE SURGERY CONFIDENCE AND ACCURACY Brainlab Spinal Navigation combines state-of-the-art touch screen based image control with best-in-class registration methods for image-guided
SPINE NAVIGATION IMAGE-GUIDED SPINE SURGERY CONFIDENCE AND ACCURACY Brainlab Spinal Navigation combines state-of-the-art touch screen based image control with best-in-class registration methods for image-guided
100 Interpace Parkway Parsippany, NJ
 100 Interpace Parkway Parsippany, NJ 07054 www.biometspine.com 800-526-2579 All trademarks are the property of Biomet, Inc. or one of its subsidiaries, unless otherwise indicated. Rx Only. 2009 EBI, LLC.
100 Interpace Parkway Parsippany, NJ 07054 www.biometspine.com 800-526-2579 All trademarks are the property of Biomet, Inc. or one of its subsidiaries, unless otherwise indicated. Rx Only. 2009 EBI, LLC.
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
FEE RULES RADIATION ONCOLOGY FEE SCHEDULE CONTENTS
 Tel: +27-21-9494060 Fax: +27-21-9494112 E-mail: leon.gouws@cancercare.co.za FEE RULES RADIATION ONCOLOGY FEE SCHEDULE CONTENTS 1. EXTERNAL BEAM RADIATION... 2 2. PLANNING OF TREATMENT... 2 3. DELIVERY
Tel: +27-21-9494060 Fax: +27-21-9494112 E-mail: leon.gouws@cancercare.co.za FEE RULES RADIATION ONCOLOGY FEE SCHEDULE CONTENTS 1. EXTERNAL BEAM RADIATION... 2 2. PLANNING OF TREATMENT... 2 3. DELIVERY
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting?
 High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM
 For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
OPERATIVE TECHNIQUE. CONSTRUX Mini PTC. Mini PTC Spacer System
 OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Original Date: April 2016 Page 1 of 7 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
Cervical Solutions. Optio-C Anterior Cervical Plate. with Allograft/Autograft. Surgical Technique Guide
 Cervical Solutions Optio-C Anterior Cervical Plate with Allograft/Autograft Surgical Technique Guide 2 Optio-C Anterior Cervical Plate with Allograft/Autograft Surgical Technique Guide The Optio-C System
Cervical Solutions Optio-C Anterior Cervical Plate with Allograft/Autograft Surgical Technique Guide 2 Optio-C Anterior Cervical Plate with Allograft/Autograft Surgical Technique Guide The Optio-C System
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
Evaluation of intraoperative MRI-assisted stereotactic brain tissue biopsy: a singlecenter experience in China
 Lu et al. Chinese Neurosurgical Journal (2019) 5:4 https://doi.org/10.1186/s41016-019-0152-0 CHINESE MEDICAL ASSOCIATION RESEARCH Evaluation of intraoperative MRI-assisted stereotactic brain tissue biopsy:
Lu et al. Chinese Neurosurgical Journal (2019) 5:4 https://doi.org/10.1186/s41016-019-0152-0 CHINESE MEDICAL ASSOCIATION RESEARCH Evaluation of intraoperative MRI-assisted stereotactic brain tissue biopsy:
Epilepsy & Functional Neurosurgery
 Epilepsy & Functional Neurosurgery An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Epilepsy Neurosurgery What is a seizure? continuous
Epilepsy & Functional Neurosurgery An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Epilepsy Neurosurgery What is a seizure? continuous
Fibula Rod System. Lateral Malleolus Fracture Indications:
 Fibula Rod System Fibula Rod System Since 1988, Acumed has been designing solutions for the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy has been to know
Fibula Rod System Fibula Rod System Since 1988, Acumed has been designing solutions for the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy has been to know
WayPoint Implant and Surgical Kits
 WayPoint Implant and Surgical Kits Directions For Use L011-68 (Rev C0, 2017-03-20) Contains directions for the following products: 66-WP-BKS, 66-WP-IKS, 66-WP-SKS www.fh-co.com FHC, Inc. 1201 Main Street
WayPoint Implant and Surgical Kits Directions For Use L011-68 (Rev C0, 2017-03-20) Contains directions for the following products: 66-WP-BKS, 66-WP-IKS, 66-WP-SKS www.fh-co.com FHC, Inc. 1201 Main Street
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES. Mr. Johnson. Seizures at 29 Years of Age. Dileep Nair, MD Juan Bulacio, MD
 Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Reduction of Radiation Exposure in Percutaneous Pedicle Screw Placement by Using a New Extension Instrument
 Reduction of Radiation Exposure in Percutaneous Pedicle Screw Placement by Using a New Extension Instrument Franquiz M. Juan, Myers J.Behnam, Thomas A. Michael, Greenhalgh J. Travis, Shoup J. Andrew Study
Reduction of Radiation Exposure in Percutaneous Pedicle Screw Placement by Using a New Extension Instrument Franquiz M. Juan, Myers J.Behnam, Thomas A. Michael, Greenhalgh J. Travis, Shoup J. Andrew Study
Intracranial Studies Of Human Epilepsy In A Surgical Setting
 Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Surgical Technique 4.5/8.5MM BEAMING SYSTEM. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The 4.5/8.5 screw system is intended for fixation arthrodesis of
1105 two (2) vertebrae... 1, add on per additional vertebra
 SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
SPINE STAGE OPERATIONS Staged operations shall be paid at 100% for the first stage and 85% for the second stage. Where the second stage pays a higher fee 100% shall be paid and the first stage shall be
Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity
 Eur Spine J (2013) 22:2130 2135 DOI 10.1007/s00586-013-2942-y OPEN OPERATING THEATRE (OOT) Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity Ibrahim Obeid Fethi Laouissat
Eur Spine J (2013) 22:2130 2135 DOI 10.1007/s00586-013-2942-y OPEN OPERATING THEATRE (OOT) Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity Ibrahim Obeid Fethi Laouissat
Navigated placement of iliac bolts: description of a new technique
 The Spine Journal 11 (2011) 331 335 Technical Report Navigated placement of iliac bolts: description of a new technique Ben J. Garrido, MD*, Ken E. Wood, MD Lake Norman Orthopedic Spine Center, 170 Medical
The Spine Journal 11 (2011) 331 335 Technical Report Navigated placement of iliac bolts: description of a new technique Ben J. Garrido, MD*, Ken E. Wood, MD Lake Norman Orthopedic Spine Center, 170 Medical
Stereotactic Minimally Invasive Brain Repair brings hope for patients with seizure disorders
 Stereotactic Minimally Invasive Brain Repair brings hope for patients with seizure disorders It is well known that, currently, the incidence rate of epilepsy is approximately 20-50/100,000 worldwide. This
Stereotactic Minimally Invasive Brain Repair brings hope for patients with seizure disorders It is well known that, currently, the incidence rate of epilepsy is approximately 20-50/100,000 worldwide. This
1. POLICY: Magnetic Resonance Image Guided High Intensity Focused Ultrasound (MRgFUS) for Essential Tremor
 Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012
 Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012 Case Hans O. Lűders Epilepsy Center Medical Center, University Hospitals, Cleveland
Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012 Case Hans O. Lűders Epilepsy Center Medical Center, University Hospitals, Cleveland
COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION
 C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
ASJ. Feasibility Study of Free-Hand Technique for Pedicle Screw Insertion at C7 without Fluoroscopy-Guidance. Asian Spine Journal
 Asian Spine Journal 38 Gun Woo Clinical Lee et al. Study Asian Spine J 2016;10(1):38-45 http://dx.doi.org/10.4184/asj.2016.10.1.38 Asian Spine J 2016;10(1):38-45 Feasibility Study of Free-Hand Technique
Asian Spine Journal 38 Gun Woo Clinical Lee et al. Study Asian Spine J 2016;10(1):38-45 http://dx.doi.org/10.4184/asj.2016.10.1.38 Asian Spine J 2016;10(1):38-45 Feasibility Study of Free-Hand Technique
Intracranial EEG for seizure focus localization: evolving techniques, outcomes, complications, and utility of combining surface and depth electrodes
 CLINICAL ARTICLE Intracranial EEG for seizure focus localization: evolving techniques, outcomes, complications, and utility of combining surface and depth electrodes Yasunori Nagahama, MD, 1 Alan J. Schmitt,
CLINICAL ARTICLE Intracranial EEG for seizure focus localization: evolving techniques, outcomes, complications, and utility of combining surface and depth electrodes Yasunori Nagahama, MD, 1 Alan J. Schmitt,
TABLE OF CONTENTS. 2 (8144 Rev 2)
 1 (8144 Rev 2) TABLE OF CONTENTS Introduction Conventus CAGE TM - Proximal Humerus...3 Indications and Contraindications...4 Surgical Summary...5 Patient Positioning & Approach...6 Surgical Technique Plate
1 (8144 Rev 2) TABLE OF CONTENTS Introduction Conventus CAGE TM - Proximal Humerus...3 Indications and Contraindications...4 Surgical Summary...5 Patient Positioning & Approach...6 Surgical Technique Plate
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
Quality Assurance of Ultrasound Imaging in Radiation Therapy. Zuofeng Li, D.Sc. Murty S. Goddu, Ph.D. Washington University St.
 Quality Assurance of Ultrasound Imaging in Radiation Therapy Zuofeng Li, D.Sc. Murty S. Goddu, Ph.D. Washington University St. Louis, Missouri Typical Applications of Ultrasound Imaging in Radiation Therapy
Quality Assurance of Ultrasound Imaging in Radiation Therapy Zuofeng Li, D.Sc. Murty S. Goddu, Ph.D. Washington University St. Louis, Missouri Typical Applications of Ultrasound Imaging in Radiation Therapy
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
Technique Guide. LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
EPILEPSY. New Ideas about an Old Disease. Gregory D. Cascino, MD
 EPILEPSY New Ideas about an Old Disease Gregory D. Cascino, MD Disclosure Research-Educational Grants Neuro Pace, Inc. American Epilepsy Society American Academy of Neurology Neurology (Associate Editor)
EPILEPSY New Ideas about an Old Disease Gregory D. Cascino, MD Disclosure Research-Educational Grants Neuro Pace, Inc. American Epilepsy Society American Academy of Neurology Neurology (Associate Editor)
Computational Medical Imaging Analysis Chapter 7: Biomedical Applications
 Computational Medical Imaging Analysis Chapter 7: Biomedical Applications Jun Zhang Laboratory for Computational Medical Imaging & Data Analysis Department of Computer Science University of Kentucky Lexington,
Computational Medical Imaging Analysis Chapter 7: Biomedical Applications Jun Zhang Laboratory for Computational Medical Imaging & Data Analysis Department of Computer Science University of Kentucky Lexington,
Subject: Magnetoencephalography/Magnetic Source Imaging
 01-95805-16 Original Effective Date: 09/01/01 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Magnetoencephalography/Magnetic Source Imaging THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
01-95805-16 Original Effective Date: 09/01/01 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Magnetoencephalography/Magnetic Source Imaging THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
FIELD SAFETY NOTICE / PRODUCT NOTIFICATION
 FIELD SAFETY NOTICE / PRODUCT NOTIFICATION Subject: Brainlab Cranial Navigation System: Effect of setup on overall navigation accuracy Product Reference: Brainlab Cranial Navigation System (all versions)
FIELD SAFETY NOTICE / PRODUCT NOTIFICATION Subject: Brainlab Cranial Navigation System: Effect of setup on overall navigation accuracy Product Reference: Brainlab Cranial Navigation System (all versions)
Zimmer Periarticular Proximal Humeral Locking Plate
 Zimmer Periarticular Proximal Humeral Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Humeral Locking Plate 1 Surgical Technique Table of Contents Introduction
Zimmer Periarticular Proximal Humeral Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Humeral Locking Plate 1 Surgical Technique Table of Contents Introduction
PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique 2957 Bow Broch_REV_B.indd 1 2/10/11 12:47 PM Surgical Technique Bowed Femur Plate The technique description herein is made available to the
PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique 2957 Bow Broch_REV_B.indd 1 2/10/11 12:47 PM Surgical Technique Bowed Femur Plate The technique description herein is made available to the
Department of Neurological Surgery
 Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Medtronic International Ltd
 This report will reflect on the Business Department of Student working for in terms of purpose, values and responsibilities to the company and the community in large. As well as, future standing of its
This report will reflect on the Business Department of Student working for in terms of purpose, values and responsibilities to the company and the community in large. As well as, future standing of its
Imaging Strategies for Endovascular Cardiovascular Procedures and Percutaneous Aortic Valves. Roy K Greenberg, MD
 Imaging Strategies for Endovascular Cardiovascular Procedures and Percutaneous Aortic Valves Roy K Greenberg, MD Disclosure Research support Cook Inc, Boston Scientific, W.L.Gore, Cordis, Vascutek, Terarecon
Imaging Strategies for Endovascular Cardiovascular Procedures and Percutaneous Aortic Valves Roy K Greenberg, MD Disclosure Research support Cook Inc, Boston Scientific, W.L.Gore, Cordis, Vascutek, Terarecon
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Pedicle screw instrumentation is used in the
 SPINE Volume 43, Number 17, pp E983 E989 ß 2018 Wolters Kluwer Health, Inc. All rights reserved. BIOMECHANICS Pullout Strength of Pedicle Screws Following Redirection After Lateral or Medial Wall Breach
SPINE Volume 43, Number 17, pp E983 E989 ß 2018 Wolters Kluwer Health, Inc. All rights reserved. BIOMECHANICS Pullout Strength of Pedicle Screws Following Redirection After Lateral or Medial Wall Breach
OPERATIVE TECHNIQUE GALAXY FIXATION SHOULDER
 OPERATIVE TECHNIQUE GALAXY FIXATION SHOULDER cop2 OPERATIVE TECHNIQUE INTRODUCTION 1 FEATURES OF SHOULDER COMPONENTS 2 EQUIPMENT REQUIRED 5 PREOPERATIVE PLANNING 6 SURGICAL PROCEDURE 8 POST OPERATIVE MANAGEMENT
OPERATIVE TECHNIQUE GALAXY FIXATION SHOULDER cop2 OPERATIVE TECHNIQUE INTRODUCTION 1 FEATURES OF SHOULDER COMPONENTS 2 EQUIPMENT REQUIRED 5 PREOPERATIVE PLANNING 6 SURGICAL PROCEDURE 8 POST OPERATIVE MANAGEMENT
Surgical Technique. Olecranon Locking Plate
 Surgical Technique Olecranon Locking Plate PERI-LOC Locked Plating System Olecranon Locking Plate Surgical Techniquealog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Olecranon Locking Plate PERI-LOC Locked Plating System Olecranon Locking Plate Surgical Techniquealog Infor Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
PROXIMAL TIBIAL PLATE
 SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
Hinged Laminoplasty System surgical technique
 BlackbirdTM Hls Hinged Laminoplasty System surgical technique Blackbird TM Hls The ChoiceSpine Blackbird Hinged Laminoplasty System (HLS) design eliminates fitting plates through trial and error bending.
BlackbirdTM Hls Hinged Laminoplasty System surgical technique Blackbird TM Hls The ChoiceSpine Blackbird Hinged Laminoplasty System (HLS) design eliminates fitting plates through trial and error bending.
Epilepsy surgery. Loránd Eross. National Institute of Clinical Neurosciences. Semmelweis University, 2018.
 Epilepsy surgery Loránd Eross National Institute of Clinical Neurosciences Semmelweis University, 2018. Epilepsy surgery Medicaltreatment Seizure free:70% Surgical treatment Seizure fee:15% Neuromodulation
Epilepsy surgery Loránd Eross National Institute of Clinical Neurosciences Semmelweis University, 2018. Epilepsy surgery Medicaltreatment Seizure free:70% Surgical treatment Seizure fee:15% Neuromodulation
Certification Review. Module 28. Medical Coding. Radiology
 Module 28 is the study of x-rays, using radiant energy and other imaging techniques, such as resonance imaging or ultrasound, to diagnose illnesses and diseases. Vocabulary Barium enema (BE): lower gastrointestinal
Module 28 is the study of x-rays, using radiant energy and other imaging techniques, such as resonance imaging or ultrasound, to diagnose illnesses and diseases. Vocabulary Barium enema (BE): lower gastrointestinal
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
