Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
|
|
|
- Joel Rose
- 5 years ago
- Views:
Transcription
1 clinical article J Neurosurg Pediatr 17: , 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD, 1 and Daniel H. Fulkerson, MD 2 1 Department of Neurological Surgery, Indiana University School of Medicine; and 2 Department of Neurological Surgery, Division of Pediatric Neurosurgery, Goodman Campbell Brain and Spine, Indiana University School of Medicine, Indianapolis, Indiana Objective Children with skull fractures are often transferred to hospitals with pediatric neurosurgical capabilities. Historical data suggest that a small percentage of patients with an isolated skull fracture will clinically decline. However, recent papers have suggested that the risk of decline in certain patients is low. There are few data regarding the financial costs associated with transporting patients at low risk for requiring specialty care. In this study, the clinical outcomes and financial costs of transferring of a population of children with isolated skull fractures to a Level 1 pediatric trauma center over a 9-year period were analyzed. Methods A retrospective review of all children treated for head injury at Riley Hospital for Children (Indianapolis, Indiana) between 2005 and 2013 was performed. Patients with a skull fracture were identified based on ICD-9 codes. Patients with intracranial hematoma, brain parenchymal injury, or multisystem trauma were excluded. Children transferred to Riley Hospital from an outside facility were identified. The clinical and radiographic outcomes were recorded. A cost analysis was performed on patients who were transferred with an isolated, linear, nondisplaced skull fracture. Results Between 2005 and 2013, a total of 619 pediatric patients with isolated skull fractures were transferred. Of these, 438 (70.8%) patients had a linear, nondisplaced skull fracture. Of these 438 patients, 399 (91.1%) were transferred by ambulance and 39 (8.9%) by helicopter. Based on the current ambulance and helicopter fees, a total of $1,834,727 (an average of $ per patient) was spent on transfer fees alone. No patient required neurosurgical intervention. All patients recovered with symptomatic treatment; no patient suffered late decline or epilepsy. Conclusions This study found that nearly $2 million was spent solely on transfer fees for 438 pediatric patients with isolated linear skull fractures over a 9-year period. All patients in this study had good clinical outcomes, and none required neurosurgical intervention. Based on these findings, the authors suggest that, in the absence of abuse, most children with isolated, linear, nondisplaced skull fractures do not require transfer to a Level 1 pediatric trauma center. The authors suggest ideas for further study to refine the protocols for determining which patients require transport. KEY WORDS pediatric; linear; skull fracture; transfer; seizures; vomiting; cost; trauma Children diagnosed with skull fractures are often transferred to a hospital with pediatric neurosurgical capabilities, even if the child has no underlying brain injury. Prior studies have demonstrated a number of potential complications that may arise in patients with skull fractures, including seizures, intractable vomiting, decline in neurological status, and cerebral hemorrhage necessitating neurosurgical intervention. Currently, an estimated 85% of pediatric patients diagnosed with isolated skull fractures are admitted to a hospital. 2,8 The decision to admit a patient is based on the presumed risk of decline that requires specialty intervention. However, this risk is estimated based on data compiled before advanced imaging technology was widely available. More recent reviews show low rates of neurological decline and medical intervention in patients with isolated skull fractures with no associated clinical or radiographic risk factors. 8 Modern CT scanning is now readily available even in small emergency departments. Telemedicine is also becoming more common, allowing the transmission of radiographic images to specialists at a tertiary care center for consultation. ABBREVIATIONS NAT = nonaccidental trauma. submitted June 9, accepted September 23, include when citing Published online January 1, 2016; DOI: / PEDS AANS, 2016
2 Transfer of children with linear skull fractures The financial cost of health care is under increasing scrutiny in the United States. Expensive practices must be reevaluated. Practices that maximize outpatient care are encouraged because the cost of admitting a patient to the hospital is 3 to 4 times greater than the cost of treating and discharging the patient from the emergency department. 1,4 8 Transport costs are high and add to the financial burden. In this study, we analyze the transfer costs of patients with isolated skull fractures who were transported to a Level 1 pediatric trauma center between 2005 and We also evaluate the clinical and radiographic outcomes of these patients. Our goal is to provide data to help guide recommendations that are both clinically logical and fiscally responsible. Methods The study began after receiving approval from the Indiana University Institutional Review Board. We retrospectively evaluated the medical and radiographic records of all patients admitted between 2005 and 2013 for skull fractures to Riley Hospital for Children (Indianapolis, Indiana), a Level 1 pediatric trauma institution. Patients were identified by the ICD-9 skull fracture codes. We excluded patients with intracranial hematoma or intraparenchymal injury. We also excluded patients with known or highly suspected multisystem injuries. Patients who were transferred from an outside hospital to Riley Hospital for Children were identified. The transfer costs were calculated based on the local rates of the major providers of air and ambulance transport. All transport services included distance in their algorithms for cost; thus, the distances traveled were calculated for each transferred child. The decision to transfer a patient rests primarily with the outside hospital working with Riley Hospital s transportation center. The neurosurgeon at Riley is often notified or consulted. The mode of transfer (helicopter vs ambulance) is based on the evaluation of the clinical urgency by the outside emergency physician. Historically, Riley accepts all requested trauma transfers. Recorded Demographic Information Patient age at admission, hospital length of stay, detailed mechanism of injury, location of fracture, Glasgow Coma Scale score noted by the transferring hospital, Glasgow Coma Scale score upon arrival to Riley Hospital, and the mode of transfer (ambulance or helicopter) were recorded. Clinical symptoms were recorded, including intractable vomiting, seizures, and other injuries not identified on the initial evaluation. The types of medical treatments that were administered were identified, such as intracranial pressure monitoring, external ventricular drain placement, and other surgical interventions. Follow-up data from the neurosurgical service or the patient s pediatrician at a minimum of 1 year after injury were analyzed. Any subsequent imaging studies were noted. Results Mechanisms and Location of Injuries A total of 1426 patients were treated for traumatic brain injuries over the 9-year study period (Table 1). Of these 1426 patients, 724 (50.8%) patients had isolated skull fractures with no parenchymal injuries, hematomas, or other concurrent injuries. The mechanism of injury was most commonly falls or blunt trauma (74.3%), followed by nonaccidental trauma (NAT) (7.3%), bike or skateboard accidents (6.1%), motor vehicle accidents (5.5%), all-terrain vehicle or moped accidents (3.9%), and a pedestrian being struck by vehicle accidents (2.9%). The most common anatomical location of the fracture was the parietal bone (312 patients; 39.2%), followed by the occipital bone (27.9%), frontal bone (18.8%), and temporal bone (14.1%). A few patients sustained fractures that extended into several bones, and 2 patients had fractures extending into the skull base. Of the 724 patients with isolated skull fractures, 619 (85.5%) were transferred from an outside hospital by either helicopter or ambulance. There were 181 patients who were transferred with depressed skull fractures. The remaining 438 patients were transferred with linear, nondisplaced skull fractures. Patients Transferred With Linear, Nondisplaced Skull Fractures The demographic data, mechanisms of injury, and anatomical locations of the skull fractures are shown in Table 2. The average patient age in the linear fracture group was 3.4 ± 4.1 years, which was similar to that of the depressed fracture group (3.9 ± 4.1 years). There was a higher percentage of males than females (63.5% vs 36.5%). The mechanisms of injury and anatomical locations of the fractures were similarly distributed as the entire treated population. Calculation of Transfer Costs The transfer costs of the 438 patients with linear, non- TABLE 1. Mechanism of injury and location of all patients treated for isolated skull fractures during the study period Variable No. of Fractures (%) Total isolated skull fractures 724 Mechanism of injury Falls/blunt trauma 538 (74.3) Bike/skateboard 44 (6.1) Motor vehicle accident 40 (5.5) NAT 53 (7.3) Pedestrian 21 (2.9) All-terrain vehicle/moped 28 (3.9) Anatomical location Total fractures* 796 Temporal 112 (14.1) Frontal 150 (18.8) Parietal 312 (39.2) Occipital 222 (27.9) * The number of fractures exceeds the number of patients because certain patients had multiple fractures, and fractures affecting multiple bones were counted at each anatomical location. 603
3 I. K. White et al. TABLE 2. Demographic data, mode of transport, and cost analysis of 438 patients transferred with isolated, linear, nondisplaced skull fractures Variable Value* Mean age ± SD (yrs) 3.4 ± 4.1 Sex Male 278 (63.5) Female 160 (36.5) Mode of transfer Ambulance 399 (91.1) Air 39 (8.9) Mechanism of injury Falls/blunt trauma 335 (76.5) Bike/skateboard 30 (6.8) Motor vehicle accident 20 (4.6) NAT 31 (7.1) Pedestrian 9 (2.0) All-terrain vehicle/moped 13 (3.0) Anatomical location Total fractures 478 Temporal 67 (14.1) Frontal 80 (16.7) Parietal 185 (38.7) Occipital 146 (30.5) Transfer costs 2 yrs old 267 ($1,112,127) Ambulance 244 ($846,070) Air 23 ($266,087) NAT 31 ($107,492.50) Ambulance 31 ($107,492.50) Air 0 ($0.00) >2 yrs old 171 ($722,566.50) Ambulance 155 ($537,462.50) Air 16 ($185,104) NAT 0 ($0.00) Total 438 ($1,834,727.40) Ambulance 399 ($1,383,532.50) Air 39 ($451,194.90) * Values are reported as the number of fractures (%) unless otherwise indicated. Transfer costs are reported as the number of transfers (cost). displaced skull fractures are shown in Table 2. Most of the patients (399 patients; 91.1%) were transferred by ambulance, and 39 (8.9%) patients were transported by helicopter. The average distance for ambulance transfers was miles, and the distance for helicopter transfers was miles. Ambulance transfer fees were based on the distance traveled, with a $300 base fee and $25 per mile thereafter. Helicopter fees were based on time in the air and calculated individually by the carriers. The average ambulance transfer fee was $ Thus, the estimated cost for the ambulance transfers of 399 patients was $1,383,533. The average helicopter transfer cost was $11,569; thus, the estimated cost of the 39 helicopter transfers was $451,195. The total transfer costs for 438 pediatric patients with isolated linear skull fractures were estimated to be $1,834,727, with an average cost of $ per patient. Patients Younger Than 2 Years Of the 438 patients, 267 (61.0%) patients were children younger than 2 years. Most were transferred by ambulance (244 of 267 patients; 91.4%). Twenty-three (8.6%) were transported by helicopter. The total transfer costs of the children younger than 2 years of age were $1,112,157. Thirty-one (11.6%) of these patients were identified as victims of abuse or NAT. There was no diagnosis of NAT in any child older than 2 years. Clinical Outcomes Among the 438 patients transferred for linear, nondisplaced skull fractures, none experienced neurological decline or required neurosurgical intervention (Table 3). Only 9 (2.1%) patients had experienced episodes of intractable vomiting that required intravenous fluid support. Eighteen of these 438 (4.1%) patients required treatment from another medical service for injuries that were not identified on the initial outside evaluation. Peri-injury seizures were documented in 9 of the total 619 patients (1.4%) transferred with either a linear or depressed skull fracture. Six of these were patients with only linear fractures (1% of total; 1.4% of linear fracture patients). All patients with seizures were younger than 2 years, except one 12-year-old child who suffered a skull fracture from a fall that was caused by a seizure. All seizures were witnessed before or during the child s initial presentation at the initial transferring hospital. There was no definite association between seizures and either the anatomical location of the fracture or the mechanism of injury. All patients who experienced seizures were started on seizure treatment at the initial hospital, and there were no episodes of status epilepticus or late seizures. Clinical and Radiological Follow-Up Data The clinical and radiological outcomes were evaluated TABLE 3. Clinical outcomes of 438 transferred patients with isolated, linear, nondisplaced skull fractures Variable No. (%) Neurological decline 0 Neurosurgical intervention 0 (0) Intracranial pressure monitoring 0 (0) External ventricular drain placement 0 (0) Craniotomy 0 (0) Bur hole 0 (0) Elective neurosurgical intervention 0 (0) Intractable vomiting 9 (2.1) Seizure 6 (1.4) Treatment for nonneurosurgical injuries not identified on 18 (4.1) the initial examination 604
4 Transfer of children with linear skull fractures for all 619 patients transferred for skull fractures. Of these, 42 (6.8%) patients received additional CT scanning while in the hospital; none of these patients had any new clinically relevant findings. Outpatient follow-up CT scanning was performed on 560 (90.4%) patients. There were no clinically relevant additional findings noted on follow-up imaging. Clinical follow-up data were available at 1 year for 90% of the patients. These patients were followed by either their pediatrician or the neurosurgical service. No new long-term clinical symptoms or late seizures were identified. Discussion It is a common practice to transfer children with isolated skull fractures to a pediatric trauma center because of the potential for decline that may require specialized intervention. Studies have demonstrated a number of potential complications that must be considered in patients with skull fractures, including seizures, intractable vomiting, decline in neurological status, and cerebral hemorrhage necessitating neurosurgical intervention. 2,3,6 9 However, these potential complications are based on prior studies in the literature, many of which preceded the current widespread availability of CT scanning. Over the 9-year study period, 619 patients were transferred to Riley Hospital for Children (a Level 1 pediatric trauma center) with isolated skull fractures. No patients required subsequent neurosurgical intervention. Nine patients had peri-injury seizures, including 1 patient whose seizure preceded the fall that caused the fracture. No patients developed epilepsy. Of the total patient population, 438 transferred patients had linear, nondisplaced skull fractures. Nine of these 438 (2.1%) patients had prolonged vomiting that required intravenous fluid hydration and medications. Eighteen (4.1%) patients were treated for injuries that were not identified at the primary evaluation prior to transfer. NAT was the mechanism of injury in 31 (7.1%) patients. This rate is consistent with the findings of Laskey et al. 4 All of the patients with NAT were younger than 2 years. The transfer costs for these 31 patients was $107,493. Excluding the patients with NAT, the total transfer costs of the patients with linear, nondisplaced skull fractures was estimated to be $1,727, A second or follow-up CT scan was obtained for 560 of the 619 transferred patients (90.4%). Previously at our institution, CT scanning was performed routinely during the outpatient follow-up appointment. No new clinically relevant findings were discovered. Follow-up clinical data were available at 1 year for 90% of patients. No patients had new long-term neurological findings or epilepsy. Financial Considerations The financial concerns in the current medical environment in the United States are forcing clinicians to reevaluate accepted practices. Our data suggest a low rate of complications that require specialty care in pediatric patients who have sustained isolated linear, nondisplaced skull fractures. In our series, nearly $2 million was spent just on the transfer of these children over a 9-year period. Moreover, the cost of admitting these patients is 3 to 4 times higher than the cost of observing and discharging a patient to home. This represents a discrepancy of $1,500 to $2,000 per patient at our institution and is consistent with the literature. 2,5,6 Transferred patients are universally admitted for observation at our institution. Thus, the cost of admission could also be added to every patient transferred. In total, we calculated that more than $3.5 million was spent purely on the transfer and admission of patients with a very low risk of need for neurosurgical intervention. This estimated cost is before the addition of any treatment costs (intravenous fluid administration, laboratory work, imaging, etc.). Limitations The study is limited by its retrospective nature. We also did not have access to the original records of the transferring facility. Thus, our data are based solely on the records of the receiving hospital (Riley Hospital). Therefore, mitigating circumstances leading to the decision to transfer may have been missed. The costs were estimated, although we made every effort to make this as accurate and representative as possible. Conclusions Our data suggest an extremely low risk of clinical decline that requires neurosurgical intervention in patients with linear, nondisplaced skull fractures. There was a low rate of prolonged vomiting that was treated with standard therapy. No patients suffered late seizures. A small percentage of patients (4.1%) required treatment for nonneurosurgical injuries that were not identified on the initial examination. There were no new, neurosurgically relevant findings on follow-up head CT scan. The cost of transfer alone was estimated to be $1,834,727 over the 9-year study period for children with linear, nondisplaced skull fractures without other injuries. Moreover, the actual time from evaluation at the outside facility to arrival via transfer to the tertiary care center was often well over 6 to 8 hours, which is the suggested observation time for these patients. Thus, many patients likely could have been safely discharged from the original facility rather than transferred to a Level 1 pediatric trauma center. 2,8,9 The possibility of abuse must be considered in children with head injury. In our series, 31 of the 438 (7.1%) patients with linear, nondisplaced skull fractures were victims of NAT. All of these patients were younger than 2 years. Unfortunately, we do not have data on how many of these patients were suspected of abuse at the initial evaluation versus those whose abuse was discovered later. It is currently our policy to have a social evaluation for all children younger than 2 years with a skull fracture. We believe that any child with even a slight suspicion of NAT should be transferred to a center with dedicated child abuse services available, especially if they are younger than 2 years. A follow-up CT scan was obtained for 90.4% of patients, either in the hospital or in an outpatient follow-up setting. No new, clinically relevant findings were discovered. There is a growing concern about the long-term effect of ionizing radiation on children. We have subsequent- 605
5 I. K. White et al. ly reevaluated the practice of routine follow-up CT. We now recommend follow-up imaging in these patients only when clinically indicated (e.g., neurological decline and concern for spinal fluid leakage). We therefore suggest that most children with isolated skull fractures do not need transfer to a Level 1 center. Most patients require observation and symptomatic support that is well within the capabilities of most emergency departments. However, for various reasons, community physicians may not feel comfortable observing headinjured children, even if the risk of decline is low. The growing availability of telemedicine may help identify patients who truly need transfer to a tertiary care facility. Pediatric neurosurgeons are now often able to remotely view locally acquired CT images. Thus, a specialist may be able to consult with a local emergency department to identify radiographic risk factors such as fractures near a major vascular structure, fracture depression, pneumocephalus, or intracranial blood. The neurosurgeon may be able to counsel the treating physician in signs of abuse. It is important to note that we excluded patients with many of the characteristic radiological findings of abuse, such as a subdural hematoma or concurrent injuries (rib or longbone fractures). A consulting neurosurgeon may be able to detect subtle but worrisome radiographic signs of NAT and recommend transportation to an appropriate facility. We encourage neurosurgeons to develop national and local protocols for transfer. We encourage efforts to increase the ease and availability of telemedicine and remote specialty consulting. With educational efforts and collaboration with local facilities, we believe many children may avoid a costly, often unnecessary transfer. References 1. Erlichman DB, Blumfield E, Rajpathak S, Weiss A: Association between linear skull fractures and intracranial hemorrhage in children with minor head trauma. Pediatr Radiol 40: , Greenes DS, Schutzman SA: Infants with isolated skull fracture: what are their clinical characteristics, and do they require hospitalization? Ann Emerg Med 30: , Gruskin KD, Schutzman SA: Head trauma in children younger than 2 years: are there predictors for complications? Arch Pediatr Adolesc Med 153:15 20, Laskey AL, Stump TE, Hicks RA, Smith JL: Yield of skeletal surveys in children 18 months of age presenting with isolated skull fractures. J Pediatr 162:86 89, Mannix R, Monuteaux MC, Schutzman SA, Meehan WP III, Nigrovic LE, Neuman MI: Isolated skull fractures: trends in management in US pediatric emergency departments. Ann Emerg Med 62: , Metzger RR, Smith J, Wells M, Eldridge L, Holsti M, Scaife ER, et al: Impact of newly adopted guidelines for management of children with isolated skull fracture. J Pediatr Surg 49: , Reid SR, Liu M, Ortega HW: Nondepressed linear skull fractures in children younger than 2 years: is computed tomography always necessary? Clin Pediatr (Phila) 51: , Rollins MD, Barnhart DC, Greenberg RA, Scaife ER, Holsti M, Meyers RL, et al: Neurologically intact children with an isolated skull fracture may be safely discharged after brief observation. J Pediatr Surg 46: , Russo CA, Owens PL, Stocks C: Common injuries that result in hospitalization, 2004: Statistical Brief #19. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. Rockville, MD: Agency for Health Care Policy and Research, 2006 Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author Contributions Conception and design: all authors. Acquisition of data: all authors. Analysis and interpretation of data: all authors. Drafting the article: all authors. Critically revising the article: all authors. Reviewed submitted version of manuscript: all authors. Approved the final version of the manuscript on behalf of all authors: Fulkerson. Study supervision: Fulkerson. Correspondence Daniel H. Fulkerson, Goodman Campbell Brain and Spine, Riley Hospital for Children, 702 Barnhill Dr. #1134, Indianapolis, IN dfulkers@iupui.edu. 606
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Head trauma is an important cause of morbidity and. Linear nondisplaced skull fractures in children: who should be observed or admitted?
 clinical article J Neurosurg Pediatr 16:703 708, 2015 Linear nondisplaced skull fractures in children: who should be observed or admitted? Eliel N. Arrey, BS, Marcia L. Kerr, RN, Stephen Fletcher, DO,
clinical article J Neurosurg Pediatr 16:703 708, 2015 Linear nondisplaced skull fractures in children: who should be observed or admitted? Eliel N. Arrey, BS, Marcia L. Kerr, RN, Stephen Fletcher, DO,
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES
 PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Mild traumatic brain injury (mtbi) has been increasingly. Follow-up issues in children with mild traumatic brain injuries
 clinical article J Neurosurg Pediatr 18:224 230, 2016 Follow-up issues in children with mild traumatic brain injuries Katarzyna Kania, MPH, 1 Kashif Ajaz Shaikh, MD, 1,2 Ian Kainoa White, MD, 1,2 and Laurie
clinical article J Neurosurg Pediatr 18:224 230, 2016 Follow-up issues in children with mild traumatic brain injuries Katarzyna Kania, MPH, 1 Kashif Ajaz Shaikh, MD, 1,2 Ian Kainoa White, MD, 1,2 and Laurie
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA
 GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA Approximately 800 patients with head injuries die or are hospitalized in the state of Alaska each year 1. In addition, thousands
GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA Approximately 800 patients with head injuries die or are hospitalized in the state of Alaska each year 1. In addition, thousands
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision
 Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
PEDIATRIC MILD TRAUMATIC HEAD INJURY
 PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Author Manuscript. Received Date : 27-Oct Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Correlation of D-Dimer level with outcome in traumatic brain injury
 2014; 17 (1) Original Article Correlation of D-Dimer level with outcome in traumatic brain injury Pradip Prasad Subedi 1, Sushil Krishna Shilpakar 2 Email: Abstract Introduction immense. The major determinant
2014; 17 (1) Original Article Correlation of D-Dimer level with outcome in traumatic brain injury Pradip Prasad Subedi 1, Sushil Krishna Shilpakar 2 Email: Abstract Introduction immense. The major determinant
The New England Journal of Medicine A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES
 A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
Resource Utilization in Helicopter Transport of Head-Injured Children
 Resource Utilization in Helicopter Transport of Head-Injured Children Clay M. Elswick MD, Deidre Wyrick MD, Lori Gurien MD, Mallik Rettiganti PhD, Marie Saylors MS, Ambre Pownall APRN, Diaa Bahgat MD,
Resource Utilization in Helicopter Transport of Head-Injured Children Clay M. Elswick MD, Deidre Wyrick MD, Lori Gurien MD, Mallik Rettiganti PhD, Marie Saylors MS, Ambre Pownall APRN, Diaa Bahgat MD,
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
O ne million patients are treated annually in United
 859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
Research Article Analysis of Repeated CT Scan Need in Blunt Head Trauma
 Hindawi Publishing Corporation Emergency Medicine International Volume 2013, Article ID 916253, 5 pages http://dx.doi.org/10.1155/2013/916253 Research Article Analysis of Repeated CT Scan Need in Blunt
Hindawi Publishing Corporation Emergency Medicine International Volume 2013, Article ID 916253, 5 pages http://dx.doi.org/10.1155/2013/916253 Research Article Analysis of Repeated CT Scan Need in Blunt
A bout million patients present to UK hospitals
 420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study of Paediatric Head Injuries and Its Outcome Raje Vinayak, Raje Vaishali, Pednekar Akshay,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study of Paediatric Head Injuries and Its Outcome Raje Vinayak, Raje Vaishali, Pednekar Akshay,
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Summary of Pediatric Trauma Patients
 Santa Rosa Memorial Hospital Trauma Services Summary of Pediatric Trauma Patients Reporting Dates Jan 1, 2004 May 31, 2006 The mission of the Santa Rosa Memorial Hospital Trauma Services is to provide
Santa Rosa Memorial Hospital Trauma Services Summary of Pediatric Trauma Patients Reporting Dates Jan 1, 2004 May 31, 2006 The mission of the Santa Rosa Memorial Hospital Trauma Services is to provide
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
A National Review of Inpatient Admissions for Pediatric Concussion
 A National Review of Inpatient Admissions for Pediatric Concussion Tara Rhine, MD MS 1 Lynn Babcock, MD MS 1 Mekibib Altaye, PhD 2 1 Division of Emergency Medicine, Cincinnati Children s Hospital Medical
A National Review of Inpatient Admissions for Pediatric Concussion Tara Rhine, MD MS 1 Lynn Babcock, MD MS 1 Mekibib Altaye, PhD 2 1 Division of Emergency Medicine, Cincinnati Children s Hospital Medical
Decreasing No-Show Rates to Pediatric Neurosurgery Outpatient Clinic - Back to Basics
 Decreasing No-Show Rates to Pediatric Neurosurgery Outpatient Clinic - Back to Basics Alan P. Yaacoub, Linda Beatson, Velda Green, Daniel Fulkerson, Jodi Smith, Laurie Ackerman, Andrew Jea, Jeffrey S.
Decreasing No-Show Rates to Pediatric Neurosurgery Outpatient Clinic - Back to Basics Alan P. Yaacoub, Linda Beatson, Velda Green, Daniel Fulkerson, Jodi Smith, Laurie Ackerman, Andrew Jea, Jeffrey S.
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
CORE STANDARDS STANDARDS USED IN TARN REPORTS
 CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
Chapter 2 Triage. Introduction. The Trauma Team
 Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Stair falls: caregiver s missed step as a source of childhood fractures
 J Child Orthop (2014) 8:77 81 DOI 10.1007/s11832-014-0551-x ORIGINAL CLINICAL ARTICLE Stair falls: caregiver s missed step as a source of childhood fractures Andrew T. Pennock George D. Gantsoudes Jennifer
J Child Orthop (2014) 8:77 81 DOI 10.1007/s11832-014-0551-x ORIGINAL CLINICAL ARTICLE Stair falls: caregiver s missed step as a source of childhood fractures Andrew T. Pennock George D. Gantsoudes Jennifer
Instructional Course #34. Review of Neuropharmacology in Pediatric Brain Injury. John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD
 Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
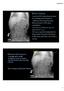 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
Clarifying Murky Waters: Head Injuries in Children
 Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Skull fracture is a common feature of traumatic
 CLINICAL ARTICLE J Neurosurg Pediatr 20:598 603, 2017 Posttraumatic complications in pediatric skull fracture: dural sinus thrombosis, arterial dissection, and cerebrospinal fluid leakage Adedamola Adepoju,
CLINICAL ARTICLE J Neurosurg Pediatr 20:598 603, 2017 Posttraumatic complications in pediatric skull fracture: dural sinus thrombosis, arterial dissection, and cerebrospinal fluid leakage Adedamola Adepoju,
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Is The Routine CT Head Scan Justified for Psychiatric Patients? A Prospective Study
 RESEARCH PAPERS Is The Routine CT Head Scan Justified for Psychiatric Patients? A Prospective Study Jambur Ananth, M.D., Reda Gamal, M.D., Milton Miller, M.D., Marcy Wohl, R.N., Steven Vandewater, Ph.D.
RESEARCH PAPERS Is The Routine CT Head Scan Justified for Psychiatric Patients? A Prospective Study Jambur Ananth, M.D., Reda Gamal, M.D., Milton Miller, M.D., Marcy Wohl, R.N., Steven Vandewater, Ph.D.
Correlation of Computed Tomography findings with Glassgow Coma Scale in patients with acute traumatic brain injury
 Journal of College of Medical Sciences-Nepal, 2014, Vol-10, No-2 ABSTRACT OBJECTIVE To correlate Computed Tomography (CT) findings with Glasgow Coma Scale (GCS) in patients with acute traumatic brain injury
Journal of College of Medical Sciences-Nepal, 2014, Vol-10, No-2 ABSTRACT OBJECTIVE To correlate Computed Tomography (CT) findings with Glasgow Coma Scale (GCS) in patients with acute traumatic brain injury
Phenytoin versus Levetiracetam for Prevention of Early Posttraumatic Seizures: A Prospective Comparative Study
 136 Original Article Phenytoin versus Levetiracetam for Prevention of Early Posttraumatic Seizures: A Prospective Comparative Study Kairav S. Shah 1 Jayun Shah 1 Ponraj K. Sundaram 1 1 Department of Neurosurgery,
136 Original Article Phenytoin versus Levetiracetam for Prevention of Early Posttraumatic Seizures: A Prospective Comparative Study Kairav S. Shah 1 Jayun Shah 1 Ponraj K. Sundaram 1 1 Department of Neurosurgery,
NICE Guidelines for C-Spine Imaging: Real Life Impact
 NICE Guidelines for C-Spine Imaging: Real Life Impact Poster No.: C-1367 Congress: ECR 2017 Type: Scientific Exhibit Authors: D. Weinberg, I. Djoukhadar, G. Potter; Salford/UK Keywords: Trauma, Audit and
NICE Guidelines for C-Spine Imaging: Real Life Impact Poster No.: C-1367 Congress: ECR 2017 Type: Scientific Exhibit Authors: D. Weinberg, I. Djoukhadar, G. Potter; Salford/UK Keywords: Trauma, Audit and
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
INDEX&NEUROTRAUMA&(INCLUDING&SPINAL&CORD&INJURIES)&!!
 1 INDEX&NEUROTRAUMA&(INCLUDING&SPINAL&CORD&INJURIES)& Prehospital,care,in,patients,with,severe,traumatic,brain,injury:,does,the,level,of,prehospital, care,influence,mortality?,...,3 Contralateral,extraaxial,hematomas,after,urgent,neurosurgery,of,a,mass,lesion,in,patients,
1 INDEX&NEUROTRAUMA&(INCLUDING&SPINAL&CORD&INJURIES)& Prehospital,care,in,patients,with,severe,traumatic,brain,injury:,does,the,level,of,prehospital, care,influence,mortality?,...,3 Contralateral,extraaxial,hematomas,after,urgent,neurosurgery,of,a,mass,lesion,in,patients,
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level
 Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Preliminary Results Using a Reduced Radiation Cervical Spine Clearance Algorithm In Pediatric Trauma Patients: A Simplified Approach
 Preliminary Results Using a Reduced Radiation Cervical Spine Clearance Algorithm In Pediatric Trauma Patients: A Simplified Approach M A T T H E W M O R O N T M D D I R E C T O R O F T R A U M A S E R
Preliminary Results Using a Reduced Radiation Cervical Spine Clearance Algorithm In Pediatric Trauma Patients: A Simplified Approach M A T T H E W M O R O N T M D D I R E C T O R O F T R A U M A S E R
USE OF CT SCAN IN A CHILD WITH MTBI
 TO SCAN OR NOT TO SCAN USE OF CT SCAN IN A CHILD WITH MTBI LISA AYOUB-RODRIGUEZ MD PEDIATRIC HOSPITALIST MIKE LEE MD PEDIATRIC RESIDENT BERT JOHANSSON MD PEDIATRIC HOSPITALIST DISCLOSURES I M NOT A SURGEON
TO SCAN OR NOT TO SCAN USE OF CT SCAN IN A CHILD WITH MTBI LISA AYOUB-RODRIGUEZ MD PEDIATRIC HOSPITALIST MIKE LEE MD PEDIATRIC RESIDENT BERT JOHANSSON MD PEDIATRIC HOSPITALIST DISCLOSURES I M NOT A SURGEON
17. Imaging and interventional radiology
 17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
Results of delayed follow-up imaging in traumatic brain injury
 clinical article J Neurosurg 124:703 709, 2016 Results of delayed follow-up imaging in traumatic brain injury Adam Ross Befeler, MD, MS, 1 William Gordon, MD, 1 Nickalus Khan, MD, 1 Julius Fernandez, MD,
clinical article J Neurosurg 124:703 709, 2016 Results of delayed follow-up imaging in traumatic brain injury Adam Ross Befeler, MD, MS, 1 William Gordon, MD, 1 Nickalus Khan, MD, 1 Julius Fernandez, MD,
Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults
 Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Neck CTA: When? How? The Innsbruck Experience Marius C. Wick, M.D. Department of Radiology Karolinska University Hospital Solna Stockholm, Sweden
 Neck CTA: When? How? The Innsbruck Experience Marius C. Wick, M.D. Department of Radiology Karolinska University Hospital Solna Stockholm, Sweden No financial or non-financial competing interests to declare
Neck CTA: When? How? The Innsbruck Experience Marius C. Wick, M.D. Department of Radiology Karolinska University Hospital Solna Stockholm, Sweden No financial or non-financial competing interests to declare
ACO #44 Use of Imaging Studies for Low Back Pain
 Measure Information Form (MIF) DATA SOURCE Medicare Claims Medicare beneficiary enrollment data MEASURE SET ID ACO #44 VERSION NUMBER AND EFFECTIVE DATE Version 1, effective 01/01/18 CMS APPROVAL DATE
Measure Information Form (MIF) DATA SOURCE Medicare Claims Medicare beneficiary enrollment data MEASURE SET ID ACO #44 VERSION NUMBER AND EFFECTIVE DATE Version 1, effective 01/01/18 CMS APPROVAL DATE
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Validity of Caregivers Reports on Head Trauma Due to Falls in Young Children Aged Less than 2 Years
 Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Cervical Spine Injury: A Clinical Decision Rule to Identify High-Risk Patients for Helical CT Screening
 Julian A. Hanson 1 C. Craig Blackmore 1,2 Frederick A. Mann 1 Anthony J. Wilson 1 Received July 2, 1999; accepted after revision August 31, 1999. 1 Department of Radiology, Harborview Medical Center, University
Julian A. Hanson 1 C. Craig Blackmore 1,2 Frederick A. Mann 1 Anthony J. Wilson 1 Received July 2, 1999; accepted after revision August 31, 1999. 1 Department of Radiology, Harborview Medical Center, University
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
ARTICLE IN PRESS. doi: /j.jemermed TRAUMA PATIENTS CAN SAFELY BE EXTUBATED IN THE EMERGENCY DEPARTMENT
 doi:10.1016/j.jemermed.2009.05.033 The Journal of Emergency Medicine, Vol. xx, No. x, pp. xxx, 2009 Copyright 2009 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/09 $ see front matter
doi:10.1016/j.jemermed.2009.05.033 The Journal of Emergency Medicine, Vol. xx, No. x, pp. xxx, 2009 Copyright 2009 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/09 $ see front matter
Rehabilitation/Geriatrics ADMISSION CRITERIA. Coordinated Entry System
 Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
County of Santa Clara Emergency Medical Services System
 County of Santa Clara Emergency Medical Services System EMS System Policy Change Coversheet EMS SYSTEM POLICY CHANGE COVERSHEET Policy Number and Name: 605: Prehospital Trauma Triage Date: May 27, 2014
County of Santa Clara Emergency Medical Services System EMS System Policy Change Coversheet EMS SYSTEM POLICY CHANGE COVERSHEET Policy Number and Name: 605: Prehospital Trauma Triage Date: May 27, 2014
ORIGINAL ARTICLE. Temporal Lobe Injury in Temporal Bone Fractures. imaging (MRI) to evaluate lesions of the temporal
 ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
emeasure Title Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 18 Years and Older
 emeasure Title Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 18 Years and Older emeasure Identifier (Measure Authoring Tool) NQF Number Measurement
emeasure Title Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 18 Years and Older emeasure Identifier (Measure Authoring Tool) NQF Number Measurement
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Correspondence should be addressed to Sorayouth Chumnanvej;
 Neurology Research International Volume 2016, Article ID 2737028, 7 pages http://dx.doi.org/10.1155/2016/2737028 Research Article Assessment and Predicting Factors of Repeated Brain Computed Tomography
Neurology Research International Volume 2016, Article ID 2737028, 7 pages http://dx.doi.org/10.1155/2016/2737028 Research Article Assessment and Predicting Factors of Repeated Brain Computed Tomography
Lowering epilepsy-related treatment costs in the era of patient choice and value-based care
 Lowering epilepsy-related treatment costs in the era of patient choice and value-based care In-home EEG offers cost-effective, reliable alternative to traditional diagnostic services 01 Introduction One
Lowering epilepsy-related treatment costs in the era of patient choice and value-based care In-home EEG offers cost-effective, reliable alternative to traditional diagnostic services 01 Introduction One
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
North Carolina Stroke Systems of Care Survey. Presented on behalf of the Integrating & Accessing Care Work Group of the Stroke Advisory Council
 North Carolina Stroke Systems of Care Survey Presented on behalf of the Integrating & Accessing Care Work Group of the Stroke Advisory Council Survey Overview The survey was developed with input from the
North Carolina Stroke Systems of Care Survey Presented on behalf of the Integrating & Accessing Care Work Group of the Stroke Advisory Council Survey Overview The survey was developed with input from the
Seizure Disorders. Guidelines for assessment of fitness to work as Cabin Crew
 Seizure Disorders Guidelines for assessment of fitness to work as Cabin Crew General Considerations As with all medical guidelines, it is important that each individual case is assessed on its own merits.
Seizure Disorders Guidelines for assessment of fitness to work as Cabin Crew General Considerations As with all medical guidelines, it is important that each individual case is assessed on its own merits.
MR imaging as predictor of delayed posttraumatic cerebral hemorrhage
 J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
6/23/2017. What do you see? skull fracture
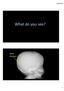 What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Circumcision bleeding complications: Neonatal intensive care infants compared to. those in the normal newborn nursery
 Circumcision bleeding complications: Neonatal intensive care infants compared to those in the normal newborn nursery Abigail R. Litwiller MD 1, David M. Haas MD, MS 2 1 Department of OB/GYN, University
Circumcision bleeding complications: Neonatal intensive care infants compared to those in the normal newborn nursery Abigail R. Litwiller MD 1, David M. Haas MD, MS 2 1 Department of OB/GYN, University
Each year more than children are seen in hospital
 CMAJ Research CATCH: a clinical decision rule for the use of computed tomography in children with minor head injury Martin H. Osmond MD CM, Terry P. Klassen MD, George A. Wells PhD, Rhonda Correll RN,
CMAJ Research CATCH: a clinical decision rule for the use of computed tomography in children with minor head injury Martin H. Osmond MD CM, Terry P. Klassen MD, George A. Wells PhD, Rhonda Correll RN,
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May Leslie M. Quinn M.D.
 CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
Audit Report. National Audit of Paediatric Radiology Services in Hospitals
 Audit Report National Audit of Paediatric Radiology Services in Hospitals www.rcr.ac.uk 2 Contents Introduction 3 Standards 4 Material and methods 5 Results 6 Discussion 8 References 10 www.rcr.ac.uk 3
Audit Report National Audit of Paediatric Radiology Services in Hospitals www.rcr.ac.uk 2 Contents Introduction 3 Standards 4 Material and methods 5 Results 6 Discussion 8 References 10 www.rcr.ac.uk 3
STATE OPERATIONS MANUAL
 STATE OPERATIONS MANUAL Appendix W Survey Protocol, Regulations and Interpretive Guidelines for Critical Access Hospitals (CAHs) And Swing-Beds in CAHs Revisions 84, 06-07-21013 C-0151 Physician Ownership
STATE OPERATIONS MANUAL Appendix W Survey Protocol, Regulations and Interpretive Guidelines for Critical Access Hospitals (CAHs) And Swing-Beds in CAHs Revisions 84, 06-07-21013 C-0151 Physician Ownership
Head trauma is a common chief complaint among children visiting
 Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY
 SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY PURPOSE: To identify those patients who are at greatest risk for severe injury and determine the most appropriate facility to transport persons with different
SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY PURPOSE: To identify those patients who are at greatest risk for severe injury and determine the most appropriate facility to transport persons with different
