EM minor EM major SJS SJS-TEN TEN
|
|
|
- Arron Owens
- 5 years ago
- Views:
Transcription
1 North American study of pediatric SJS and TEN: Setting diagnostic criteria, systematic review and retrospective cohort analysis comparing outcomes of common treatments Michele Ramien, MDCM, FRCPC Dermatology, DABD Children s Hospital of Eastern Ontario/Alberta Children s Hospital On behalf of a PeDRA collaboration October 26, 2018
2 EM minor EM major SJS SJS-TEN TEN
3 This talk highlights our group s results and future directions Setting diagnostic criteria Systematic review and meta-analysis Retrospective cohort plan
4 Setting diagnostic criteria
5 Supported by: Redefining severe cutaneous reactions in children Amin Bahubeshi, Michele Ramien Children s Hospital of Eastern Ontario; Larry Eichenfeld Rady Children s Hospital; Irene Lara-Corrales, Elena Pope SickKids Hospital; Amy Jo Nopper Children s Mercy Kansas City; Moise Levy - Dell Children's Medical Center of Central Texas; Neil Shear Sunnybrook Health Sciences Centre BACKGROUND The RegiSCAR cohort study revolutionized the management of adult SJS-TEN but the results can t be directly applied to the pediatric population. Reliable and validated data informing the best intervention in the management of pediatric SJS/TEN are lacking. Case definitions are a critical first step to study the SJS/TEN spectrum in children. OBJECTIVE Create and validate pediatric-specific case definitions for the following: SJS, TEN, EM, and infection-related mucositis (including MIRM). METHODS 1. Literature review of key sources. 2. Expert panel assembled. 3. Modified nominal group technique for consensus: Literature review presented to expert panel, organized and informal discussion of diagnostic categories. Proposal of case definition elements and categories. 4. Literature review and case definition elements presented at the inflammatory session at PeDRA. Online survey on most relevant elements. 5. Expert panel reviewed survey results and proposed case definitions. RESULTS: PROPOSED REVISED CLASSIFICATION AND CRITERIA Current classification EM minor EM major SJS SJS-TEN TEN (M)IRM Revised classification Erythema multiforme 1. Patient must have fixed typical or atypical papular targets* 2. Patient must have at least 2 of the following: a) Acral distribution b) Recent history or lab evidence of HSV infection c) Systemically well d) Mucosal involvement Supporting features Recurrent episodes Symmetrical distribution Individual lesions last at least 5 days and resolve without sequelae Skin lesions fully developed within 72 hours What s new? Minor and major are grouped together Emphasis on HSV as a trigger Reactive infectious mucocutaneous or mucosal-predominant eruption (RIME) 1. Patient must have at least 2 of the following: a) Vesiculobullous skin lesions (<10%BSA) without typical papular targets b) Erosive mucositis, with at least 2 mucosal surfaces involved c) Non-contributory medication history** 2. Patient must have evidence of relevant infection as indicated by at least one of the following: a) Clinical symptoms (including cough, fever, malaise, arthralgias) b) Radiologic evidence of pneumonia c) Laboratory evidence of acute infection (ie. PCR, IgM, or similar) Supporting features Prodromal symptoms Histology excluding other immunobullous disease What s new? Encompasses MIRM, MPAM, mucositispredominant eruptions Considers infections other than mycoplasma Epidermal necrolysis 1. Patient must have rapidly progressing erythema and epidermal detachment with a relevant medication history* and histology that excludes alternative diagnoses 2. Patient must have at least 2 of the following: a) At least10% detached or detachable skin surface area b) Severe involvement of 2 or more mucosal surfaces c) Constitutional and site specific symptoms*** Supporting features Tender skin in the absence of other features of SSSS Generalized distribution and centrifugal Flat atypical targets What s new? Includes SJS, SJS-TEN, and TEN Relevant medication essential **Typical papular targets are described as well-defined round <3cm and having three concentric zones: a bright red outer ring, a paler pink and edematous center ring, and a dusky or purpuric-appearing center. An atypical papular target demonstrates only two zones and/or a poorly defined border. **This includes relevant medication and appropriate time interval. ***Constitutional symptoms include fever, malaise and arthralgias; site specific symptoms depend on areas of involvement and include lung (dyspnea, increased respiratory rate), genital (urethral stricture leading to voiding difficulty), ocular (eye pain, vision impairment), renal (proteinuria, microalbuminuria, hematuria), and gastrointestinal (melena, diarrhea) DISCUSSION Our proposed revised classification stratifies related severe cutaneous reactions by etiology, making it practical for management. The morphology of each category is distinguishable and decreases possible confusion between diagnoses. This classification provides a framework to consider mucositis-predominant disease within the spectrum. It also allows for inclusion of mucositis-predominant disease that is not caused by Mycoplasma. All drug-related reactions are considered one entity, facilitating management as these cases can evolve over time. CONCLUSIONS SJS/TEN spectrum diseases may be more effectively diagnosed to guide management with our proposed revised classification. These case definitions are critical for both practice and to study outcomes. REFERENCES Please see attached reference list.
6 Our main reference for defining severe cutaneous reactions in children is not pediatric-specific and may lead to misdiagnosis Clinical Classification of Cases of Toxic Epidermal Necrolysis, Stevens-Johnson Syndrome, and Erythema Multiforme Sylvie Bastuji-Garin, MD; Berthold Rzany, MD; Robert S. Stern, MD; Neil H. Shear, MD, FRCPC; Luigi Naldi, MD; Jean-Claude Roujeau, MD Bastuji-Garin S et al. (1993). Clinical classification of cases of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme. Archives of Dermatology, 129(1),
7 Reliable diagnosis à Better outcome data à Better treatment/management for patients
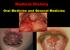
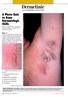
8 PART 4: INFLAMMATO annu. tinea dosis). necese diagforme thema ratum us will eristic ere are E may isease. a marthese enous Fig Cutaneous features of toxic epidermal necrolysis (TEN). EM is best regarded as a self limiting cytotoxic dermatitis resultcharacteristic dusky red color of the early macular eruption in TEN. Lesions ing from cell mediated hypersensitivity most commonly to lesions drugs with dermal with this color often progress to full-blown necrolytic or infection. It presents clinically with a spectrum of macular, papepidermal detachment. ular or urticarial lesions, as well as the classic acral iris or target lesions (Figure 47.1). Lesions may involve the palms or trunk, as well as the oral and genital mucosal membranes, which are associated with erosions. On the other hand, SJS, first described in 1922, comprises extensive EM of the trunk and mucous membranes (Figure 47.2), accompanied by fever, malaise, myalgia and arthralgia [6,7]. Lyell first reported TEN in 1956 [8], which was characterized by extensive, sheet like, skin erosions with widespread purpuric macules or flat, atypical, target lesions (Figure 47.3), accompanied by severe involvement of the conjunctival, corneal (Figure 47.4), irideal, buccal, labial and genital mucous membranes [9,10]. Our revised classification improves correlation with cause and management and includes mucositis-predominant disease n syndrome) atingly pt and of one svirus) d TEN 19 and may be Erythema multiforme <10% >30% 10-30% = Surface area of epidermal detachment SJS = Stevens-Johnson syndrome = Detached epidermis TEN = Toxic epidermal necrolysis Reactive infectious Epidermal necrolysis Fig Spectrum of disease based upon surface area of epidermal detachment. mucosal-predominant 466 Pediatric Dermatology Vol. 34 No. 4 July/August 2017 eruption (RIME) A EM minor Figure 47.1 Classic target lesion in erythema multiforme. A Figure 1. Severe cheilitis with multiple erosions and EM hemorrhagic major crusts on the upper and lower lips. Erosions SJS B SJS-TEN TEN were also noticeable on the and on the Fig. oral 20.12mucosa Stevens Johnson syndrome (SJS) versus SJS TEN overlap. A In anterior part of the tongue. addition to mucosal involvement and numerous dusky lesions with flaccid (M)IRM iffiths, Jonathan Barker, Tanya Bleiker, Robert Chalmers and Daniel Creamer. bullae, there are areas of coalescence and multiple sites of epidermal Ltd. B C detachment. Because the latter involved >10% body surface area, the patient including MIRM sine rash classified asmarkers having SJS TEN The remainder of the was biochemical were overlap. B Close-up of epidermal detachment, Fig Clinical features of toxic epidermal necrolysis (TEN). A Detachment whose appearance has been likened to wet cigarette paper. within normal parameters. Figure 2. Targetoid erosion on the glans penis that made of large sheets of necrolytic epidermis (>30% body surface area), leading foreskin retraction painful. With the physical findings and concern for to extensive areas of denuded skin. A few intact bullae are still present. dehydration andoforal discomfort, preliminary diagb Hemorrhagic crusts with mucosal involvement. C Epidermal detachment palmar skin. noses of primary herpes infection andpatients possible predicting which with SJS are likely to progress towards full- atypical pneumonia wereblown considered andcurrently the patient TEN are unavailable. in terms of classification, morphology, and pathogenin TEN, are several that(2 4). have been correlated with poor received supportive therapy with there rehydration andfactorsesis MIRM is more prevalent in boys. In outcome, including increasing and extent of epidermal detachment. pain medication. Intravenous acyclovir 5 mg/kg was agepatients in distinguishing between the two diseases. Differentiation is based with MIRM there is a predominance of In addition, the numbercare, of medications, elevation of serum urea, primarily on clinical characteristics, especially the of the alsoappearance administered. After the first day of inpatient mucosal involvement, with creativariable cutaneous and glucose levels, neutropenia, lymphopenia and thrombocytotarget lesions and their distribution. To retain the diagnosis erosions of EM, onnine he developed the glans penis (Fig. 2). No involvement. Prominent mucositis, particularly oral penia have been statistically to poor outcome. Late withdrawal typical target lesions must exist, whereas SJS should be considered if present. cutaneous lesions were Mucositis secondary linked involvement, is nearly universal in MIRM and is a
9 Poster 15 Current classification EM minor EM major SJS SJS-TEN TEN (M)IRM Revised classification Erythema multiforme 1. Patient must have fixed typical or atypical papular targets* 2. Patient must have at least 2 of the following: a) Acral distribution b) Recent history or lab evidence of HSV infection c) Systemically well d) Mucosal involvement Supporting features Recurrent episodes Symmetrical distribution Individual lesions last at least 5 days and resolve without sequelae Skin lesions fully developed within 72 hours Reactive infectious mucocutaneous or Epidermal necrolysis mucosal-predominant eruption (RIME) 1. Patient must have at least 2 of the following: a) Vesiculobullous skin lesions (<10%BSA) without typical papular targets b) Erosive mucositis, with at least 2 mucosal surfaces involved c) Non-contributory medication history** 2. Patient must have evidence of relevant infection as indicated by at least one of the following: a) Clinical symptoms (including cough, fever, malaise, arthralgias) b) Radiologic evidence of pneumonia c) Laboratory evidence of acute infection (ie. PCR, IgM, or similar) Supporting features Prodromal symptoms Histology excluding other immunobullous disease 1. Patient must have rapidly progressing erythema and epidermal detachment with a relevant medication history* and histology that excludes alternative diagnoses 2. Patient must have at least 2 of the following: a) At least10% detached or detachable skin surface area b) Severe involvement of 2 or more mucosal surfaces c) Constitutional and site specific symptoms*** Supporting features Tender skin in the absence of other features of SSSS Generalized distribution and centrifugal Flat atypical targets What s new? Minor and major are grouped together Emphasis on HSV as a trigger What s new? Encompasses MIRM, MPAM, mucositispredominant eruptions Considers infections other than mycoplasma What s new? Includes SJS, SJS-TEN, and TEN Relevant medication essential **Typical papular targets are described as well-defined round <3cm and having three concentric zones: a bright red outer ring, a paler pink and edematous center ring, and a dusky or purpuric-appearing center. An atypical papular target demonstrates only two zones and/or a poorly defined border. **This includes relevant medication and appropriate time interval. ***Constitutional symptoms include fever, malaise and arthralgias; site specific symptoms depend on areas of involvement and include lung (dyspnea, increased respiratory rate), genital (urethral stricture leading to voiding difficulty), ocular (eye pain, vision impairment), renal (proteinuria, microalbuminuria, hematuria), and gastrointestinal (melena, diarrhea)
10 Systematic review and meta-analysis
11 What is the best treatment for SJS, SJS-TEN,TEN in children? Del Pozzo-Magana et. al (2011) 31 studies 128 cases 4 groups: IVIG Corticosteroids Dressings +/- debridement Supportive care
12 A comprehensive search strategy (inception 2018) identified 257 studies with 1617 patients after screening PRISMA study flow diagram
13 Baseline characteristics were similar amongst diagnostic groups, other than that SJS-TEN was mainly diagnosed in males (84%) Overall 26% 43% 31% Average age / years
14 Antibiotics and anticonvulsants were the most common causes; analgesic/nsaid use was reported in 9% Many others (20%) Sulfonamides (6%) Antibiotics (34%) Analgesics (9%) Anticonvulsants (31%)
15 Data was extracted for the following primary and secondary outcomes: 1ry: SCORTEN Mortality Time to death Time to arrest of blister formation 2ry: Time to re-epithelialization Length of hospital stay Duration of followup
16 Regression models were fitted to estimate relationships between treatment and diagnosis for each of these outcomes 1ry: Mortality Time to arrest of blister formation 2ry: Time to re-epithelialization Length of hospital stay
17 Mortality rates were lower in pediatric patients than in adults and SJS-TEN had the lowest mortality rate Study reported mortality stratified by diagnosis SJS (n=837) SJS-TEN (n = 232) TEN (n=548) 2% 0.5% 11% Overall mortality = 4.9%
18 Mortality effect was assessed for supportive care, corticosteroids, IVIG, and combination IVIG + corticosteroids Treatment Number of patients Supportive care 732 Corticosteroids only 504 IVIG only 186 IVIG + corticosteroids 103 Other 92
19 Treatment with IVIG, corticosteroids, or both vs supportive care did not have a significant effect on mortality Post-model fit contrasts from multivariable regression on mortality Mortality Effect Treatment Group Estimate (95% CI) Odds Ratio (95% CI) P value* IVIG vs. Supportive care (-1.52 to 1.21) 0.86 (0.22 to 3.37) CS vs. Supportive care (-1.71 to 1.08) 0.73 (0.18 to 2.95) IVIG + CS vs. Supportive care (-3.80 to 0.98) 0.24 (0.02 to 2.67) *Level of significance was adjusted for multiple comparisons, a p<0.008 was used to detect statistical significance.
20 Surrogate markers of healing (secondary outcomes) were available for fewer patients Multivariable ordinary least squares regression to model treatment grouping with reported time to re-epithelialization, using supportive care as the reference treatment group Time to Arrest of Blistering Progression (days) Time to Re-Epithelialization (days) Length of Hospital Stay (days) Model coefficient P value* Model coefficient P value* Model coefficient P Treatment group (adjusted 95% CI) (adjusted 95% CI) (adjusted 95% CI) value* Surgical N/A N/A (-9.88 to -0.62) (7.21 to 17.83) <0.001 debridement only IVIG only (-9.13 to -0.20) ( to -7.63) < (-1.09 to 7.06) CS only (-4.35 to -0.29) ( to -3.25) (-8.78 to 2.73) Cyclosporine only (-8.90 to -0.58) ( to -3.88) < (1.78 to -1.78) TNF inhibitors (with any other) ( to -2.31) ( to -4.10) < (1.25 to 18.22) n = 102 n = 67 n = 238 *Level of significance was adjusted for multiple comparisons, a p<0.01 was used to detect statistical significance.
21 TNF-inhibitors decreased time to arrest of blistering progression vs supportive care (in a small sample of patients) Multivariable ordinary least squares regression to model treatment grouping with reported time to re-epithelialization, using supportive care as the reference treatment group Time to Arrest of Blistering Progression (days) Time to Re-Epithelialization (days) Length of Hospital Stay (days) Model coefficient P value* Model coefficient P value* Model coefficient P Treatment group (adjusted 95% CI) (adjusted 95% CI) (adjusted 95% CI) value* Surgical N/A N/A (-9.88 to -0.62) (7.21 to 17.83) <0.001 debridement only IVIG only (-9.13 to -0.20) ( to -7.63) < (-1.09 to 7.06) CS only (-4.35 to -0.29) ( to -3.25) (-8.78 to 2.73) Cyclosporine only (-8.90 to -0.58) ( to -3.88) < (1.78 to -1.78) TNF inhibitors (with any other) ( to -2.31) ( to -4.10) < (1.25 to 18.22) n = 102 n = 67 n = 238 n = 4 *Level of significance was adjusted for multiple comparisons, a p<0.01 was used to detect statistical significance.
22 All treatments except surgical debridement decreased time to reepithelialization vs supportive care Multivariable ordinary least squares regression to model treatment grouping with reported time to re-epithelialization, using supportive care as the reference treatment group Time to Arrest of Blistering Progression (days) Time to Re-Epithelialization (days) Length of Hospital Stay (days) Model coefficient P value* Model coefficient P value* Model coefficient P Treatment group (adjusted 95% CI) (adjusted 95% CI) (adjusted 95% CI) value* Surgical N/A N/A (-9.88 to -0.62) (7.21 to 17.83) <0.001 debridement only IVIG only (-9.13 to -0.20) ( to -7.63) < (-1.09 to 7.06) CS only (-4.35 to -0.29) ( to -3.25) (-8.78 to 2.73) Cyclosporine only (-8.90 to -0.58) ( to -3.88) < (1.78 to -1.78) TNF inhibitors (with any other) ( to -2.31) ( to -4.10) < (1.25 to 18.22) n = 36 n = 11 n = 8 n = 4 n = 102 n = 67 n = 238 *Level of significance was adjusted for multiple comparisons, a p<0.01 was used to detect statistical significance.
23 Surgical debridement significantly increased length of hospital stay vs supportive care; no other treatment had an impact Multivariable ordinary least squares regression to model treatment grouping with reported time to re-epithelialization, using supportive care as the reference treatment group Time to Arrest of Blistering Progression (days) Time to Re-Epithelialization (days) Length of Hospital Stay (days) Model coefficient P value* Model coefficient P value* Model coefficient P Treatment group (adjusted 95% CI) (adjusted 95% CI) (adjusted 95% CI) value* Surgical N/A N/A (-9.88 to -0.62) (7.21 to 17.83) <0.001 debridement only IVIG only (-9.13 to -0.20) ( to -7.63) < (-1.09 to 7.06) CS only (-4.35 to -0.29) ( to -3.25) (-8.78 to 2.73) Cyclosporine only (-8.90 to -0.58) ( to -3.88) < (1.78 to -1.78) TNF inhibitors (with any other) ( to -2.31) ( to -4.10) < (1.25 to 18.22) n = 102 n = 67 n = 238 n = 7 n = 2 *Level of significance was adjusted for multiple comparisons, a p<0.01 was used to detect statistical significance.
24 To summarize our systematic review and meta-analysis findings: Low mortality rate Treatment did not significantly reduce mortality Some treatments may reduce healing time
25 Strengths Summarizes available data Large number of patients Weaknesses Missing data Included studies low quality evidence Food for thought: Would outcomes be different with our revised classification? How does timing of treatment affect response? What is the best primary outcome?
26 Retrospective cohort study
27 47.1 CHAPTER 47 Reactive Inflammatory Erythemas SECTION Malcolm Rustin1 and Rino Cerio2 4 1 Royal SPECTRUM OF DISEASE BASED UPON SURFACE AREA OF EPIDERMAL DETACHMENT URTICARIAS, ERYTHEMAS AND PURPURAS Free London NHS Foundation Trust, London, UK 2 The Royal London Hospital, Bart s Health NHS Trust, London; and Queen Mary s Medical and Dental School, University of London, London, UK SJS-TEN overlap SJS TEN The aim of this multicenter retrospective cohort study is identify best management for severe cutaneous reactions in children Erythema annulare centrifugum, 47.8 Erythema multiforme, 47.1 Erythema gyratum repens, Annular erythema of infancy, 47.6 Erythema marginatum, Introduction Multiple skin conditions can present with ring like or annular lesions for which a specific diagnosis can be made (e.g. tinea corporis, granuloma annulare, psoriasis or annular sarcoidosis). This chapter describes a group of conditions that do not necessarily lead to a specific underlying diagnosis and may pose diagnostic and therapeutic problems. It includes erythema multiforme (EM), annular erythema of infancy, necrolytic migratory erythema (NME), erythema annulare centrifugum, erythema gyratum repens and erythema marginatum. Subacute cutaneous lupus will be covered in Chapter 54. Each eruption may have characteristic features and although diagnosis of EM is often easy and there are a limited number of underlying causes, the diagnosis of NME may take time in view of the different manifestations of the disease. Physicians should be alert to the subtle eruption of erythema marginatum and the importance of diagnosing rheumatic fever. These cutaneous signs therefore present a challenge with heterogenous diseases presenting with varying morphologies. Eryth hema multtiform me Comprehensive Definition and terminology Data Collection Form Until recently, erythema multiforme (EM), Stevens Johnson syndrome (SJS), toxic epidermal necrolysis (TEN or Lyell syndrome) were considered to form a spectrum from mild to fulminatingly severe cases. There has been a re evaluation of this concept and a tendency to consider EM minor and EM major as part of one spectrum, often following infections (especially with herpesvirus) and sometimes due to drug reactions. On this basis SJS and TEN are separable from EM. The topic is discussed in Chapter 119 and is more closely linked to drug sensitivities. SJS and TEN may be regarded as severe variants of a single disease [1 5]. Necrolytic migratory erythema, Key references, EM is best regarded as a self limiting cytotoxic dermatitis resulting from cell mediated hypersensitivity most commonly to drugs or infection. It presents clinically with a spectrum of macular, papular or urticarial lesions, as well as the classic acral iris or target lesions (Figure 47.1). Lesions may involve the palms or trunk, as Fig Cutaneous features of toxic epidermal necrolysis (TEN). well as the dusky oral and genital membranes, which Characteristic red color of the mucosal early macular eruption in TEN. Lesionsare associwith colorerosions. often progress full-blown lesions with dermal in 1922, atedthis with Ontothe other necrolytic hand, SJS, first described epidermal detachment. comprises extensive EM of the trunk and mucous membranes (Figure 47.2), accompanied by fever, malaise, myalgia and arthralgia [6,7]. Lyell first reported TEN in 1956 [8], which was characterized by extensive, sheet like, skin erosions with widespread purpuric macules or flat, atypical, target lesions (Figure 47.3), accompanied by severe involvement of the conjunctival, corneal (Figure 47.4), irideal, buccal, labial and genital mucous membranes [9,10]. Erythema multiforme PART 4: INFLAMMATORY Introduction, 47.1 <10% >30% 10-30% = Surface area of epidermal detachment SJS = Stevens-Johnson syndrome = Detached epidermis TEN = Toxic epidermal necrolysis Reactive infectious Epidermal necrolysis Fig Spectrum of disease based upon surface area of epidermal mucosal-predominant detachment. 466 Pediatric Dermatology Vol. 34 No. 4 July/August 2017 eruption (RIME) A Figure 1. Severe cheilitis with multiple erosions and hemorrhagic crusts on the upper and lower lips. Erosions were also noticeable on the oral mucosa and on the anterior part of the tongue. A B The remainderfig. of the biochemical markers syndrome were Stevens Johnson (SJS) versus SJS TEN overlap. A In within normal addition parameters. to mucosal involvement and numerous lesions with flaccid Figure 2. dusky Targetoid erosion on the glans penis that made foreskin retraction With the physical findings and of concern for and bullae, there are areas coalescence multiple sitespainful. of epidermal B C dehydration and oral discomfort, preliminary diagdetachment. Because the latter involved >10% body surface area, the patient noses of primary herpes infection possible was classified as havingand SJS TEN overlap. B Close-up of epidermal detachment, Figure 47.1Clinical Classicfeatures target lesion in epidermal erythema multiforme. atypical pneumonia consideredhas andbeen the patient Fig of toxic necrolysis (TEN). A Detachment in terms of classification, whosewere appearance likened to wet cigarette paper. morphology, and pathogenreceived supportive therapy with rehydration and esis (2 4). MIRM is more prevalent in boys. In of large sheets of necrolytic epidermis (>30% body surface area), leading patients with MIRM there is a predominance of to extensive areas of denuded skin. A few intact bullae are still present. pain medication. Intravenous acyclovir 5 mg/kg was Rook s Textbook of Dermatology, Ninth Edition. Edited by Christopher Griffiths, Jonathan Barker, Tanya Bleiker, Robert Chalmers and Daniel Creamer. also administered. After the first day of inpatient care, mucosal involvement, with variable cutaneous B Hemorrhagic crusts with mucosal involvement. C Epidermal detachment of he developed erosions on thewhich glans penis (Fig. 2). No SJS involvement. Prominent oral 2016 John Wiley & Sons, Ltd. Published 2016 by John Wiley & Sons, Ltd. palmar skin. predicting patients with are likely to progressmucositis, towardsparticularly fullcutaneous lesions were present. Mucositis secondary involvement, is nearly universal in MIRM and is a Companion website: blown TEN are currently unavailable. to mycoplasma infection was suspected, and the major cause of morbidity and hospitalization (1). In TEN, there are several factors that havemirm been has correlated with poor (1). patient began therapy with azithromycin and methylhowever, an excellent prognosis outcome, including increasing extent of epidermal detachment. prednisolone. A polymerase chain reaction (PCR)age andthe in distinguishing between the two diseases. Differentiation is based pathophysiology underlying MIRM is thought for herpes virus infection tested negative. In addition, the number of medications, elevation of serum creati-and antito involve polyclonal B-cell urea, proliferation primarily on clinical characteristics, especially the appearancesample of the for Mycoplasma pneumonia bodylymphopenia production after pneumoniae infection, nine and glucose levels, showed neutropenia, and M. thrombocytotarget lesions and their distribution. To retain the diagnosisserologic of EM,testing positive immunoglobulin G (IgG) of 21.1 and mayoutcome. result in Late skin damage from immune penia have been titers statistically linkedwhich to poor withdrawal typical target lesions must exist, whereas SJS should be considered if low IgM (2.6), suggesting a previous infection. PCR 328 complex deposition and complement activation (5). of the causative drug is also associated with a less favorable outcome. target lesions are atypical (see Table 20.1). Unfortunately, criteria testing for on an oropharyngeal swab sample was negathis mechanism differs from the type IV delayed-type tive for M. pneumonia, but positive for Chlamydia hypersensitivity reaction involved in EM, SJS, and pneumoniae. Symptomatic resolution was achieved TEN (6). Molecular mimicry between mycoplasma P1 after 5 days of treatment and no further complicaadhesion molecules and a keratinocyte antigen has tions were observed. also been hypothesized, as well as a possible genetic susceptibility (7,8). In the current study we present a case of mucositis DISCUSSION without rash in the context of C. pneumoniae respiin a recent review by Canavan et al (1) based on 202 ratory infection. C. pneumoniae infection is often published cases, the term M. pneumonia induced rash asymptomatic (60% 80% of all infections) (9). Most and mucositis (MIRM) was proposed as a clinical infections involve the upper and lower respiratory term to include the different mucocutaneous eruptions tracts. In some cases, infection transforms into a associated with mycoplasma infection, distinguishing chronic, clinically oligosymptomatic or asympthis syndrome from drug-induced Stevens Johnson tomatic form that has been linked to coronary artery syndrome (SJS), toxic epidermolytic necrosis (TEN), disease, endocarditis, atherosclerosis, hypertension, and herpes-related erythema multiforme (EM), which vasculitis, multiple sclerosis, sarcoidosis, and asthma. are diseases that have historically defied concurrence Chronic forms of infection related to C. pneumoniae EM minor EM major SJS (M)IRM including MIRM sine rash SJS-TEN TEN
28 Reliable diagnosis/classification à Better outcome data à Better treatment/management for patients
29
30 PeDRA gives me a platform for collaborating with investigators on pediatric dermatology research. 40+ research studies, 215 members, 130 institutions
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Pediatric Dermatology
 Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving
 Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases
 10.5005/jp-journals-10011-1189 CASE REPORT JIAOMR Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases 1 M Venkateshwarlu, 2 B Radhika 1 Professor and Head, Department
10.5005/jp-journals-10011-1189 CASE REPORT JIAOMR Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases 1 M Venkateshwarlu, 2 B Radhika 1 Professor and Head, Department
Cutaneous Drug Reactions
 Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review
 Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Dilantin (phenytoin) ROBERT A. SCHWARTZ
 Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Bugs and Drugs: What s New in Hypersensitivity Reactions?
 Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
GOOD MORNING! AUGUST 5, 2014
 GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
Erythema Multiforme with Reference to Atypical Presentation in an HIV-Positive Patient Following Antiretroviral Therapy Discontinuation
 2009;17(1):9-15 CLINICAL ARTICLE Erythema Multiforme with Reference to Atypical Presentation in an HIV-Positive Patient Following Antiretroviral Therapy Discontinuation Liborija Lugović Mihić, Marija Buljan,
2009;17(1):9-15 CLINICAL ARTICLE Erythema Multiforme with Reference to Atypical Presentation in an HIV-Positive Patient Following Antiretroviral Therapy Discontinuation Liborija Lugović Mihić, Marija Buljan,
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Emergency Dermatology. Emergency Dermatology
 Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
Correspondence should be addressed to Wanjarus Roongpisuthipong; rr
 Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
DERMATOLOGIC EMERGENCIES. Mary Evers D.O., F.A.O.C.D. Georgetown, Texas
 DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis: a case report
 Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Objectives. Terminology. Recognize common pediatric dermatologic conditions. Review treatment plans Identify skin manifestations of systemic disease
 Pediatric Visual Dermatological Diagnosis Fernando Vega, M.D. Objectives Recognize common pediatric dermatologic conditions Expand differential diagnosis Review treatment plans Identify skin manifestations
Pediatric Visual Dermatological Diagnosis Fernando Vega, M.D. Objectives Recognize common pediatric dermatologic conditions Expand differential diagnosis Review treatment plans Identify skin manifestations
Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
 Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Herbal and homeopathic products, often considered natural and non-toxic, can also cause adverse drug reactions.
 Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Skin Manifestations of Drug Reactions
 Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Cutaneous Adverse Drug Reactions in Domestic Animals. Katherine Doerr, DVM, Dip. ACVD. Veterinary Dermatology Center
 Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive Patients
 Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
ACUTE ANNULAR URTICARIA IN A CHILD
 The West London Medical Journal 2013 Vol 5 No 2 pp 1-5 ACUTE ANNULAR URTICARIA IN A CHILD Aaron Yon Dayse Fernandes Michelle Pike Jodi Newcombe Colin Michie 1. ABSTRACT Urticarial skin rashes have a range
The West London Medical Journal 2013 Vol 5 No 2 pp 1-5 ACUTE ANNULAR URTICARIA IN A CHILD Aaron Yon Dayse Fernandes Michelle Pike Jodi Newcombe Colin Michie 1. ABSTRACT Urticarial skin rashes have a range
A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course
 Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash
 CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
HENOCH SCHÖNLEIN PURPURA (VASCULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests (SC)
 HENOCH HÖNLEIN PURPURA (VAULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests () 1. Choose the type of bleeding characteristic for the Henoch Schönlein purpura (vascular purpura, anaphylactoid
HENOCH HÖNLEIN PURPURA (VAULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests () 1. Choose the type of bleeding characteristic for the Henoch Schönlein purpura (vascular purpura, anaphylactoid
Skin Manifestations of Systemic Disease. Approach to Dermatalogic Diagnosis 9/6/2016. Go Ahead---Judge a Book by its Cover!
 Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital
 Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
VARICELLA. Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara
 VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW
 SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Questions. Answers. Share your photos and diagnoses with us!
 Illustrated quizzes on problems seen in everyday practice Case 1 A 56-year-old woman presented with a two-week history of pruritic urticarial plaques and tense bullae on both erythematous and normal skin.
Illustrated quizzes on problems seen in everyday practice Case 1 A 56-year-old woman presented with a two-week history of pruritic urticarial plaques and tense bullae on both erythematous and normal skin.
건강한성인에서의오진하기쉬운포도구균성열상피부증후군의치험례. Staphylococcal Scalded Skin Syndrome in a Healthy Adult: Easy to Misdiagnose
 Archives of Hand and Microsurgery Arch Hand Microsurg 2018;23(4):271-276. https://doi.org/10.12790/ahm.2018.23.4.271 pissn 2586-3290 eissn 2586-3533 Case Report 건강한성인에서의오진하기쉬운포도구균성열상피부증후군의치험례 김홍일ㆍ곽찬이ㆍ박언주
Archives of Hand and Microsurgery Arch Hand Microsurg 2018;23(4):271-276. https://doi.org/10.12790/ahm.2018.23.4.271 pissn 2586-3290 eissn 2586-3533 Case Report 건강한성인에서의오진하기쉬운포도구균성열상피부증후군의치험례 김홍일ㆍ곽찬이ㆍ박언주
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS
 STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
New product information wording Extracts from PRAC recommendations on signals
 12 October 2017 EMA/PRAC/610988/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 25-29 September 2017
12 October 2017 EMA/PRAC/610988/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 25-29 September 2017
Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center
 Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
In the past few years, beta-lactam-resistant gram-positive
 Early Diagnosis Is Key in Vancomycin-Induced Linear IgA Bullous Dermatosis and Stevens-Johnson Syndrome Douglas H. Jones, MS Michael Todd, MD Timothy J. Craig, DO Background: With the emergence of highly
Early Diagnosis Is Key in Vancomycin-Induced Linear IgA Bullous Dermatosis and Stevens-Johnson Syndrome Douglas H. Jones, MS Michael Todd, MD Timothy J. Craig, DO Background: With the emergence of highly
CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD
 CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD DERMATOLOGY Pathogenesis Immunologic: can involve Type I, II, III, IV hypersensitivity reactions.
CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD DERMATOLOGY Pathogenesis Immunologic: can involve Type I, II, III, IV hypersensitivity reactions.
Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review
 140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
Lab 3: Pathogenesis of Virus Infections & Pattern 450 MIC PRACTICAL PART SECTION (30397) MIC AMAL ALGHAMDI 1
 Lab 3: Pathogenesis of Virus Infections & Pattern 450 MIC PRACTICAL PART SECTION (30397) 2018 450 MIC AMAL ALGHAMDI 1 Learning Outcomes The pathogenesis of viral infection The viral disease pattern Specific
Lab 3: Pathogenesis of Virus Infections & Pattern 450 MIC PRACTICAL PART SECTION (30397) 2018 450 MIC AMAL ALGHAMDI 1 Learning Outcomes The pathogenesis of viral infection The viral disease pattern Specific
السكري للداء مرافقة فقاعات diabeticorum= Bullosis
 1 / 6 Bullosis diabeticorum Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus.
1 / 6 Bullosis diabeticorum Bullous disease of diabetes (bullosis diabeticorum) is a distinct, spontaneous, noninflammatory, blistering condition of acral skin unique to patients with diabetes mellitus.
Title: An unusual presentation of Erythema Multiforme in a paediatric patient. A. BaniHani *., H. Nazzal*., L. Webb*., KJ. Toumba. *, G. Fabbroni*.
 Title: An unusual presentation of Erythema Multiforme in a paediatric patient. A. BaniHani *., H. Nazzal*., L. Webb*., KJ. Toumba. *, G. Fabbroni*. Abstract: Background Erythema multiforme (EM) is an acute,
Title: An unusual presentation of Erythema Multiforme in a paediatric patient. A. BaniHani *., H. Nazzal*., L. Webb*., KJ. Toumba. *, G. Fabbroni*. Abstract: Background Erythema multiforme (EM) is an acute,
Syndrome de Lyell Approche diagnostique. seminaires iris. Veronique del Marmol Alexandre Chamoun Service de Dermatologie Hôpital Erasme.
 Syndrome de Lyell Approche diagnostique Veronique del Marmol Alexandre Chamoun Service de Dermatologie Hôpital Erasme Serge Jennes Hôpital Militaire Rash benign Pustulose exanthematique Aigue et généralisée
Syndrome de Lyell Approche diagnostique Veronique del Marmol Alexandre Chamoun Service de Dermatologie Hôpital Erasme Serge Jennes Hôpital Militaire Rash benign Pustulose exanthematique Aigue et généralisée
Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements
 249 Special Issue: Inflammation in Ophthalmology Review Article Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements 1, 2, ) Mayumi Ueta 1) Department
249 Special Issue: Inflammation in Ophthalmology Review Article Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements 1, 2, ) Mayumi Ueta 1) Department
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Medical History. Oral Medicine and General Medicine
 Medical History Oral Medicine and General Medicine Gingivitis herpetica acuta NECROTIZÁLÓ SIALOMETAPLASIA SOOR Medical History The life expectancy has recently increased and increasing By dental prevention
Medical History Oral Medicine and General Medicine Gingivitis herpetica acuta NECROTIZÁLÓ SIALOMETAPLASIA SOOR Medical History The life expectancy has recently increased and increasing By dental prevention
Department of Dermatology, Nippon Medical School, 1-1-5, Sendagi, Bunkyo-ku, Tokyo , Japan 2
 Dermatology Research and Practice Volume 2010, Article ID 931340, 5 pages doi:10.1155/2010/931340 Case Report Paraneoplastic Pemphigus Presenting as Mild Cutaneous Features of Pemphigus Foliaceus and Lichenoid
Dermatology Research and Practice Volume 2010, Article ID 931340, 5 pages doi:10.1155/2010/931340 Case Report Paraneoplastic Pemphigus Presenting as Mild Cutaneous Features of Pemphigus Foliaceus and Lichenoid
Endocarditis. By : Mehrnoush. dianatkhah
 Endocarditis By : Mehrnoush. dianatkhah Case 5.31, 31 years old woman CC : Fever, dyspnea, 3 days postpartum PMH : Mitral prolapse Fever 38.5 WBC : 8900 ESR : 84 CRP : 10.4 Cr : 0.6 NT Pro BNP: 5469 Physical
Endocarditis By : Mehrnoush. dianatkhah Case 5.31, 31 years old woman CC : Fever, dyspnea, 3 days postpartum PMH : Mitral prolapse Fever 38.5 WBC : 8900 ESR : 84 CRP : 10.4 Cr : 0.6 NT Pro BNP: 5469 Physical
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Visual Diagnosis. Q-PEM: Jan Dr. Rafah F. Sayyed PEC - Al Sadd, Doha
 Visual Diagnosis Q-PEM: Jan 2017 Dr. Rafah F. Sayyed PEC - Al Sadd, Doha DISCLOSURE I do not have any relevant financial relationship with commercial interest to disclose. Introduction Speed and Accuracy
Visual Diagnosis Q-PEM: Jan 2017 Dr. Rafah F. Sayyed PEC - Al Sadd, Doha DISCLOSURE I do not have any relevant financial relationship with commercial interest to disclose. Introduction Speed and Accuracy
allergy Asia Pacific Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from
 pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
الاكزيماتيد= Eczematid
 1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
SJS/TEN spectrum. Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) 10/7/2016
 Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME
 EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
Alphaherpesvirinae. Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV)
 Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
EXANTHEMATOUS ILLNESS. IAP UG Teaching slides
 EXANTHEMATOUS ILLNESS 1 DEFINITIONS Exanthema eruption of the skin Exanthema eruption of mucosae Macule flat nonpalpable lesion Papule small palpable lesion Nodule large palpable lesion Vesicle small fluid
EXANTHEMATOUS ILLNESS 1 DEFINITIONS Exanthema eruption of the skin Exanthema eruption of mucosae Macule flat nonpalpable lesion Papule small palpable lesion Nodule large palpable lesion Vesicle small fluid
Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center
 Dermatologic Emergencies Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center Clinical Features of SJS/TEN Initial symptoms Fever, stinging
Dermatologic Emergencies Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center Clinical Features of SJS/TEN Initial symptoms Fever, stinging
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Case Report Title: A Case
: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Case Report Title: A Case
Severe cutaneous reactions caused by barbiturates in seven Iranian children
 Pharmacology and therapeutics Severe cutaneous reactions caused by barbiturates in seven Iranian children Setareh Mamishi, MD, Fatemeh Fattahi, MD, Zahra Pourpak, MD, PhD, Farzaneh Mirza Aghaee, MD, Zeinab
Pharmacology and therapeutics Severe cutaneous reactions caused by barbiturates in seven Iranian children Setareh Mamishi, MD, Fatemeh Fattahi, MD, Zahra Pourpak, MD, PhD, Farzaneh Mirza Aghaee, MD, Zeinab
A. Viral infections whose main symptom is blistering
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Viral Infections A virus is a particle of DNA or RNA enclosed by structural proteins. Viruses infect cells and proliferate to
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Viral Infections A virus is a particle of DNA or RNA enclosed by structural proteins. Viruses infect cells and proliferate to
Case Presentation. By Eman El Sharkawy Ass. Professor of cardiology Alexandria University
 Case Presentation By Eman El Sharkawy Ass. Professor of cardiology Alexandria University 6m old baby girl Past history : - At the age of 2m attack of fever, diarrhea, mouth ulcers, difficult breast feeding
Case Presentation By Eman El Sharkawy Ass. Professor of cardiology Alexandria University 6m old baby girl Past history : - At the age of 2m attack of fever, diarrhea, mouth ulcers, difficult breast feeding
Bacteria: Scarlet fever, Staph infection (sepsis, 4S,toxic shock syndrome), Meningococcemia, typhoid Mycoplasma Rickettsial infection
 Exanthematous Fever objectives FEVER WITH RASH 1 Determine the feature of skin rashes 2 Enumerate the most common causes of skin rashes in children (measles, chicken pox, rubella,erythema infectiosum,
Exanthematous Fever objectives FEVER WITH RASH 1 Determine the feature of skin rashes 2 Enumerate the most common causes of skin rashes in children (measles, chicken pox, rubella,erythema infectiosum,
LESIONS OF THE ORAL CAVITY ORAL CAVITY. Oral Cavity Subsites 4/10/2013 LIPS TEETH GINGIVA ORAL MUCOUS MEMBRANES PALATE TONGUE ORAL LYMPHOID TISSUES
 LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
LESIONS OF THE ORAL CAVITY David I. Kutler, MD, FACS Associate Professor Division of Head and Neck Surgery Department of Otolaryngology HNS Weill Cornell Medical Center ORAL CAVITY LIPS TEETH GINGIVA ORAL
Guideline on the clinical management of Henoch Schonlein Purpura (HSP)
 Guideline on the clinical management of Henoch Schonlein Purpura (HSP) Purpose To ensure a standardised approach in the management of children with HSP in southern Derbyshire. Scope The scope of this guideline
Guideline on the clinical management of Henoch Schonlein Purpura (HSP) Purpose To ensure a standardised approach in the management of children with HSP in southern Derbyshire. Scope The scope of this guideline
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease:
 Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
Classification: 1. Infective: 2. Traumatic: 3. Idiopathic: Recurrent Aphthous Stomatitis (RAS) 4. Associated with systemic disease: Hematological GIT Behcet s HIV 5. Associated with dermatological diseases:
Learning Objectives. History 8/1/2016. An Approach to Pediatric Rashes
 An Approach to Pediatric Rashes Neethi Patel, D.O. Learning Objectives 1.To identify common features of rashes seen in the pediatric population as well as pathognomonic features of certain pathologies
An Approach to Pediatric Rashes Neethi Patel, D.O. Learning Objectives 1.To identify common features of rashes seen in the pediatric population as well as pathognomonic features of certain pathologies
Journal of Global Trends in Pharmaceutical Sciences
 An Elsevier Indexed Journal ISSN-2230-7346 Journal of Global Trends in Pharmaceutical Sciences A CASE STUDY ON HERBAL THERAPY INDUCED ERYTHEMA MULTIFORME S. Showkath Ali * 1, S. Priyanka 2, Bandla Aswani
An Elsevier Indexed Journal ISSN-2230-7346 Journal of Global Trends in Pharmaceutical Sciences A CASE STUDY ON HERBAL THERAPY INDUCED ERYTHEMA MULTIFORME S. Showkath Ali * 1, S. Priyanka 2, Bandla Aswani
Fluconazole erythema multiforme
 Fluconazole erythema multiforme Search 1. Eur J Dermatol. 2012 Sep-Oct;22(5):693-4. doi: 10.1684/ejd.2012.1806. Fluconazoleinduced fixed drug eruption imitating herpes labialis with erythema multiforme.
Fluconazole erythema multiforme Search 1. Eur J Dermatol. 2012 Sep-Oct;22(5):693-4. doi: 10.1684/ejd.2012.1806. Fluconazoleinduced fixed drug eruption imitating herpes labialis with erythema multiforme.
Case No. 5; Slide No. B13/8956/2
 Interface diseases Case No. 5; Slide No. B13/8956/2 Histological findings Severe hydropic vacuolation of epidermal and follicular basal cells/ interface dermatitis Multifocally apoptotic keratinocytes
Interface diseases Case No. 5; Slide No. B13/8956/2 Histological findings Severe hydropic vacuolation of epidermal and follicular basal cells/ interface dermatitis Multifocally apoptotic keratinocytes
International Journal of Basic & Clinical Pharmacology. Profile of cutaneous adverse drug reactions of carbamazepine
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175211 Original Research Article Profile of cutaneous
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175211 Original Research Article Profile of cutaneous
Dermclinic
 Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
SEVERE CUTANEUS ADVERSE DRUGS EFFECTS MANIFESTED AS TOXIC EPIDERMAL NECROLYSIS (TEN) DUE TO ORAL ANTITUBERCULOSIS DRUGS AND REVIEW OF THE LITERATURE
 SEVERE CUTANEUS ADVERSE DRUGS EFFECTS MANIFESTED AS TOXIC EPIDERMAL NECROLYSIS (TEN) DUE TO ORAL ANTITUBERCULOSIS DRUGS AND REVIEW OF THE LITERATURE * HM Nataprawira, ** M Soepriadi * Respirology Division,
SEVERE CUTANEUS ADVERSE DRUGS EFFECTS MANIFESTED AS TOXIC EPIDERMAL NECROLYSIS (TEN) DUE TO ORAL ANTITUBERCULOSIS DRUGS AND REVIEW OF THE LITERATURE * HM Nataprawira, ** M Soepriadi * Respirology Division,
Rashes Not To Be Missed In Children
 May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
What's New in Oncodermatopathology: Immunotherapy Reactions
 What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
Bacterial Infections in Pediatric Dermatology. Patrick McMahon, MD Children s Hospital of Philadelphia
 Bacterial Infections in Pediatric Dermatology Patrick McMahon, MD Children s Hospital of Philadelphia Fill In The Blank When you see on the skin, you think of a bacterial skin infection SEND SWABS VIRAL
Bacterial Infections in Pediatric Dermatology Patrick McMahon, MD Children s Hospital of Philadelphia Fill In The Blank When you see on the skin, you think of a bacterial skin infection SEND SWABS VIRAL
Crescentic Glomerulonephritis (RPGN)
 Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
An Approach to Common and not so Common Rashes in the Office FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 An Approach to Common and not so Common Rashes in the Office FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc 1 Common Rashes Tinea Corporis: Annular- this is not the only criteria Advancing erythematous
An Approach to Common and not so Common Rashes in the Office FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc 1 Common Rashes Tinea Corporis: Annular- this is not the only criteria Advancing erythematous
The Old, The New and the Reemerging-HIV Dermatology. Toby Maurer, MD
 The Old, The New and the Reemerging-HIV Dermatology Toby Maurer, MD 1 Psoriasis Widespread psoriasis, especially if it was once stable, predicts falling CD4 count?resistance to ART??Non-adherence? Tx:
The Old, The New and the Reemerging-HIV Dermatology Toby Maurer, MD 1 Psoriasis Widespread psoriasis, especially if it was once stable, predicts falling CD4 count?resistance to ART??Non-adherence? Tx:
MEASLES (campak, rubeola, gabak, kerumut) Infectious and Tropical Pediatric Division Department of Child Health, Medical Faculty, University of Sumate
 MEASLES (campak, rubeola, gabak, kerumut) Infectious and Tropical Pediatric Division Department of Child Health, Medical Faculty, University of Sumatera Utara 1 Maculapapular eruption : 1. Measles 2. Atypical
MEASLES (campak, rubeola, gabak, kerumut) Infectious and Tropical Pediatric Division Department of Child Health, Medical Faculty, University of Sumatera Utara 1 Maculapapular eruption : 1. Measles 2. Atypical
Discussion. Infection & ER combine meeting. Fever and rash. Fever and rash. Fever and skin rash Measles
 Discussion Infection & ER combine meeting Fever and skin rash Measles Reporter R2 李尚 Supervisor VS 陳威宇洪世文 Date 99/03/20 Fever and rash Age of the patient Season of the year Travel history, Geographic location
Discussion Infection & ER combine meeting Fever and skin rash Measles Reporter R2 李尚 Supervisor VS 陳威宇洪世文 Date 99/03/20 Fever and rash Age of the patient Season of the year Travel history, Geographic location
Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin
 Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
Dermatology Pearls for Inpatient Medicine. Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University
 Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review
 Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Infectious Disease. Chloe Duke
 Infectious Disease Chloe Duke Learning Objectives Essential - Causes, recognition and Treatment of: Meningitis Sepsis Purpura Important Cervical Adenopathy Tonsillitis and Pharyngitis Otitis Media Pneumonia
Infectious Disease Chloe Duke Learning Objectives Essential - Causes, recognition and Treatment of: Meningitis Sepsis Purpura Important Cervical Adenopathy Tonsillitis and Pharyngitis Otitis Media Pneumonia
Dermergency! An Approach to Identification and Management of Life-Threatening Rashes
 Dermergency! An Approach to Identification and Management of Life-Threatening Rashes Gabby Anderson, PharmD PGY2 Emergency Medicine Pharmacy Resident anderson.gabrielle@mayo.edu Pharmacy Grand Rounds January
Dermergency! An Approach to Identification and Management of Life-Threatening Rashes Gabby Anderson, PharmD PGY2 Emergency Medicine Pharmacy Resident anderson.gabrielle@mayo.edu Pharmacy Grand Rounds January
