Supplementary Appendix
|
|
|
- Ethel Jefferson
- 6 years ago
- Views:
Transcription
1 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bagnall RD, Weintraub RG, Ingles J, et al. A prospective study of sudden cardiac death among children and young adults. N Engl J Med 2016;374: DOI: /NEJMoa
2 A Prospective, Population-Based Study of Sudden Cardiac Death in the Young SUPPLEMENTARY APPENDIX Richard D. Bagnall, Ph.D., Robert G. Weintraub, MBBS, Jodie Ingles, Grad.Dip.Gen.Couns., Ph.D., M.P.H., Johan Duflou, MBChB., M.Med., Laura Yeates, B.Sc., Grad.Dip.Gen.Couns., Lien Lam, Ph.D., Andrew Davis, MBBS, M.D., Tina Thompson, B.Nurs, Vanessa Connell, Dip. App. Sci., Jenny Wallace, R.N., Charles Naylor, M.A., MBBChir., Jackie Crawford, RN, Donald R. Love, Ph.D., Lavinia Hallam, B.Sc., MB BCh., Jodi White, MBBS, Christopher Lawrence, MBBS, Matthew Lynch, L.L.B., MBBS, Natalie Morgan, RN, Grad.Dip.Genetic.Couns., Paul James, Ph.D., M.D., Desirée du Sart, Ph.D., Rajesh Puranik M.B. Ph.D., Neil Langlois MBBChir M.A., M.D., Jitu Vohra, M.D., Ingrid Winship, MBChB., M.D., John Atherton, MBBS, Ph.D, Julie McGaughran, MBChB, M.D., Jonathan R. Skinner, MBChB., M.D., and Christopher Semsarian, MBBS, Ph.D., M.P.H. 1
3 TABLE OF CONTENTS Supplementary Methods Pages Postmortem criteria for diagnosis 3 Genetic analysis 6 Classification of variants 6 CNV and MLPA analysis 7 Statistical analysis 7 Supplementary Tables Supplementary Appendix Table S1 9 Supplementary Appendix Table S2 14 Supplementary Appendix Table S3 15 Supplementary Appendix Table S4 16 Supplementary Appendix Table S5 17 Supplementary Appendix Table S6 18 Supplementary Appendix Table S7 19 Supplementary Appendix Table S8 20 Supplementary Appendix Table S9 21 Supplementary Appendix Table S10 22 Supplementary Appendix Table S11 23 Supplementary Figures Figure Legends 24 Supplementary Appendix Figure S1 25 Supplementary Appendix Figure S2 26 Supplementary Appendix Figure S3 27 References 28 2
4 SUPPLEMENTARY METHODS 1. POSTMORTEM CRITERIA FOR DIAGNOSIS The following criteria were used for postmortem diagnosis of cardiovascular disease and further discussed by the adjudication committee before reaching a final cause of death. Specifically: Coronary artery disease/atherosclerotic cardiovascular disease/ischaemic heart disease: Autopsy diagnosis was based on the presence of typical atherosclerotic lesions involving epicardial coronary arteries, with stenosis of a major epicardial vessel in excess of 70% cross sectional area, and/or the presence of plaque haemorrhage or rupture in an atherosclerotic vessel, and/or the presence of occlusive or partially occlusive thrombus in the lumen of an atherosclerotic vessel. Areas of replacement fibrosis or acute myocardial infarction may also be present. Acute myocardial infarction: Autopsy diagnosis was based on the presence of localised geographic areas of any or all of the following in ventricular myocardium: coagulation necrosis, myocytolysis, contraction band necrosis, an acute inflammatory cell infiltrate consisting predominantly of neutrophils. Myocarditis: Autopsy diagnosis was based on the identification of myocarditis with/without fibrosis as defined in the Dallas Classification System for myocarditis. Hypertrophic cardiomyopathy: Autopsy diagnosis was based on the presence of left ventricular and/or interventricular septal hypertrophy, with or without the presence of outflow obstruction and mitral valve changes, and associated characteristic ventricular 3
5 myocardial histologic changes of myocyte hypertrophy with bizarre nuclei, myocyte disarray and/or myofibre disarray involving at least 5% of the histologically examined myocardium, often with associated abnormalities of the intima and media of small intramural arteries. Arrhythmogenic right ventricular cardiomyopathy: Autopsy diagnosis was based on the revised ARVC/D International task Force criteria, including pronounced generalised or segmental dilatation of the right ventricle, and histologically identified fibrofatty replacement of myocytes in the right ventricular free wall with or without associated chronic inflammation (Marcus FI, et al. Diagnosis of arrhythmogenic right ventricular cardiomyopathy/dysplasia: Proposed modification of the Task Force criteria. Circulation 2010;121: ). Dilated cardiomyopathy: Autopsy diagnosis was based on ventricular dilatation, with or without atrial dilatation in the absence of significant valvular, atherosclerotic, hypertensive and congenital heart disease. Histologic appearances are generally non-specific, but can include limited myocardial interstitial fibrosis and variation in myocyte morphology. Myocardial inflammation, if present must be limited in amount, and not sufficient for a diagnosis of myocarditis. Idiopathic cardiac hypertrophy: Macroscopically, a heart weight in excess of normal for age and height or weight, as detailed in commonly used heart weight tables (References: Scholz DG, et al. Age-related changes in normal human hearts during the first 10 decades of life. Part I (Growth): A quantitative anatomic study of 200 specimens from subjects from birth to 19 years old. Mayo Clinic Proceedings 1988;63(2): ); Kitzman DW, et al. Age-related changes in normal human hearts during the first 10 decades of life. Part II 4
6 (Maturity): A quantitative anatomic study of 765 specimens from subjects 20 to 99 years old. Mayo Clinic Proceedings 1988;63(2):137-46). Microscopically, normal ventricular myocardium or myocyte hypertrophy without myocyte disarray, inflammation or significant fibrosis. Anomalous coronary artery: Includes coronary arteries originating from the pulmonary trunk and those originating normally with a course passing between the aorta and pulmonary trunk, but does not include conditions such as tunnelling, high take-off of a coronary artery or other minor morphologic abnormalities. Thoracic aortic dissection: A tear in the thoracic aorta with or without aneurysm formation with resultant hemothorax or hemopericardium and/or ischemic lesions. Predisposing causes include natural inherited and acquired disease such as hypertension, Marfan syndrome, bicuspid aortic valve, familial thoracic aneurysm dissection syndrome and various arteritides, but excludes non-natural etiologies such as trauma and temporally associated cocaine use. Morphologically normal heart: A heart which on macroscopic and microscopic examination at autopsy does not appear significantly diseased. Specifically, there is no significant hypertensive, atherosclerotic or valvular disease, no structural congenital heart disease, no inflammatory, fibrotic or other infiltrate and no evidence of conditions such as hypertrophic or dilated cardiomyopathy. 5
7 2. GENETIC ANALYSIS Raw sequence reads were aligned to the human genome reference sequence (GRCh37/hg19/b37), using BWA-mem v0.7.8 with default parameters. 1 Sequence alignment files were compressed and sorted using SamTools v and duplicate reads were removed using Picard Tools v The Genome Analysis Tool Kit v was used for read realignment around short indels, base quality score recalibration, and genotyping of single nucleotide variants (SNVs) and indels, using HaplotypeCaller in gvcf mode. SNVs were filtered for QD <2.0, ReadPosRankSum <-8.5, Mapping Quality <35.0 and MQRankSum < Indels were filtered for FisherStrand >200.0, QD <1.8, ReadPosRankSum <-20.0 and InbreedingCoefficient <-0.8. Variants were annotated using SeattleSeq Annotation v8.07 tool ( and compared against the September 2014 release of the 1000 Genomes Project, phase 3, data ( and the Exome Variant Server, NHLBI GO Exome Sequencing Project (ESP) ( [Nov, 2013]. 3. CLASSIFICATION OF VARIANTS Pathogenic variants were variants previously reported as disease causing in a patient with a relevant clinical diagnosis and demonstrated to co-segregate with disease, or with functional evidence of pathogenicity. Likely pathogenic variants were variants at canonical splice dinucleotides, nonsense variants and insertion and deletions; and missense variants at conserved nucleotides (GERP score 2) that are predicted to be damaging by at least 2 out of 3 in silico pathogenicity prediction tools (SIFT, PolyPhen2 and Mutation Taster). Missense variants at conserved nucleotides and predicted to be damaging by fewer than 2 in silico tools were considered variants of uncertain significance (VUS). Missense variants 6
8 at non-conserved nucleotides were considered benign. All relevant variants with a read depth <15 were validated using standard Sanger DNA sequencing. 4. CNV ANALYSIS AND MULTIPLE LIGATION-DEPENDED PROBE AMPLIFICATION (MLPA) ANALYSIS Exome depth of coverage was calculated using GATK with the arguments -- minmeantargetrd 10, --maxmeantargetrd 500, --minmeansamplerd 25, and -- maxmeansamplerd 100. Exome targets with length <10 bp or >10 kb, or GC content >90% or <10%, or with >10% of bases masked by RepeatMasker were excluded. CNV calling was performed using XHMM with default parameters, and filtered with PLINK software to remove common CNVs and CNVs overlapping in more than 10% of all samples. CNVs with a quality score 60, and spanning 3 exome targets, with length 1 kb, and spanning or disrupting 125 autosomal cardiac disease genes were retained. MLPA was performed on 71 SUD cases as previously described using the SALSA MLPA LQTS P114 probe kit, which screens for large insertions and deletions in five LQTS genes (SCN5A, KCNH2, KCNQ1, KCNE1 and KCNE2). MLPA products were resolved on the ABI3730xl sequencer (Macrogen), sized using Peak Scanner TM v1.0 software (Applied Biosystems, CA, USA), and analysed using Coffalyser v2 software (MRC-Holland). Peak height ratios of <0.65 and >1.35 indicated a deletion and duplication, respectively. 5. STATISTICAL ANALYSIS The first step was to identify incidence rate of all SCD in the population then describe the cases where a known cause of death was ascertained. Characteristics of the disease groups were compared using Chi-square analysis and unpaired t-tests. SUD cases were 7
9 compared to those with a known cause of death to identify factors associated with this outcome, using univariate and multivariate logistic regression models. A final analysis to determine whether factors are associated with identification of a genetic diagnosis amongst SUD cases was also performed, however was based on small sub-groups of cases. Activity at time of death was converted in to a number of binary variables, including exercise (yes/no), which included death during or immediately post exercise. Sleep (yes/no) included any cases where they were presumed to be sleeping at time of death. Time of death was grouped in to a day/night binary variable, with night deaths being death between the hours 6pm and 6am. Due to the non-linear nature of age at death, 5-year age group categories were created for regression analysis, with year age group as the reference category. For regression analysis where gene result was the dependent variable, the outcome was defined as a pathogenic or likely pathogenic variant identified in cases where genetic testing was performed. Further analysis was performed where the outcome was defined as a pathogenic or likely pathogenic variant identified in arrhythmia genes, however due to the very small sample only minimal data is shown from this analysis. 8
10 SUPPLEMENTARY TABLES SUPPLEMENTARY APPENDIX TABLE S1. Target Gene List. Gene Symbol Gene Category OMIM Entry KCNH2 Molecular autopsy Long QT syndrome 2, (3); Short QT syndrome 1, (3) KCNQ1 Molecular autopsy Long QT syndrome 1, (3) RYR2 Molecular autopsy Ventricular tachycardia, catecholaminergic polymorphic, 1, (3) SCN5A Molecular autopsy Long QT syndrome-3, (3); Brugada syndrome 1, (3) AKAP9 Cardiac arrhythmia Long QT syndrome-11, (3) ANK2 Cardiac arrhythmia Long QT syndrome 4, (3); Cardiac arrhythmia, ankyrin-b-related, (3) CACNA1C Cardiac arrhythmia Brugada syndrome 3, (3); Timothy syndrome, (3) CACNB2 Cardiac arrhythmia Brugada syndrome 4, (3) CASQ2 Cardiac arrhythmia Ventricular tachycardia, catecholaminergic polymorphic, 2, (3) CAV3 Cardiac arrhythmia Long QT syndrome 9, (3) GPD1L Cardiac arrhythmia Brugada syndrome 2, (3) HCN4 Cardiac arrhythmia Brugada syndrome 8, (3); Sick sinus syndrome 2, (3) KCNE1 Cardiac arrhythmia Long QT syndrome 5, (3); Jervell and Lange-Nielsen syndrome 2, (3) KCNE2 Cardiac arrhythmia Long QT syndrome 6, (3); Atrial fibrillation, familial, 4, (3) KCNE3 Cardiac arrhythmia Brugada syndrome 6, (3) KCNJ2 Cardiac arrhythmia Andersen syndrome, (3); Atrial fibrillation, familial, 9, (3); Short QT syndrome 3, SCN1B Cardiac arrhythmia (3) Brugada syndrome 5, (3), Atrial fibrillation, familial, 13, (3); Cardiac conduction defect, nonspecific, (3) SCN3B Cardiac arrhythmia Brugada syndrome 7, (3); Atrial fibrillation, familial, 16, (3) SCN4B Cardiac arrhythmia Long QT syndrome-10, (3); Atrial fibrillation, familial, 17, (3) SNTA1 Cardiac arrhythmia Long QT syndrome 12, (3) DSC2 Major cardiomyopathy Arrhythmogenic right ventricular dysplasia 11, (3) DSG2 Major cardiomyopathy Arrhythmogenic right ventricular dysplasia 10, (3) DSP Major cardiomyopathy Arrhythmogenic right ventricular dysplasia 8, (3); Dilated cardiomyopathy with woolly hair and keratoderma, (3) 9
11 LDB3 Major cardiomyopathy Cardiomyopathy, dilated 1C, (3) LMNA Major cardiomyopathy Cardiomyopathy, dilated, 1A, (3) MYBPC3 Major cardiomyopathy Cardiomyopathy, familial hypertrophic, 4, (3) MYH7 Major cardiomyopathy Cardiomyopathy, familial hypertrophic, 1, (3) PKP2 Major cardiomyopathy Arrhythmogenic right ventricular dysplasia 9, (3) TNNI3 Major cardiomyopathy Cardiomyopathy, familial hypertrophic, 7, (3); Cardiomyopathy, dilated, 2A, (3) TNNT2 Major cardiomyopathy Cardiomyopathy, familial hypertrophic, 2, (3); Cardiomyopathy, dilated, 1D, (3) ACTC1 Minor cardiomyopathy Cardiomyopathy, familial hypertrophic, 11, (3); Cardiomyopathy, dilated, 1R, (3); Left ventricular noncompaction 4, (3) MYH6 Minor cardiomyopathy Cardiomyopathy, familial hypertrophic, 14, (3); Cardiomyopathy, dilated, 1EE, (3) MYL2 Minor cardiomyopathy Cardiomyopathy, familial hypertrophic, 10, (3) MYL3 Minor cardiomyopathy Cardiomyopathy, familial hypertrophic, 8, (3) TNNC1 Minor cardiomyopathy Cardiomyopathy, familial hypertrophic, 13, (3); Cardiomyopathy, dilated, 1Z, (3) TPM1 Minor cardiomyopathy Cardiomyopathy, familial hypertrophic, 3, (3); Cardiomyopathy, dilated, 1Y, (3) ABCC9 Rare cardiomyopathy Cardiomyopathy, dilated, 1O, (3) ACTN2 Rare cardiomyopathy Cardiomyopathy, dilated, 1AA, (3) CALR3 Rare cardiomyopathy Cardiomyopathy, familial hypertrophic, 19, (3) CSRP3 Rare cardiomyopathy Cardiomyopathy, familial hypertrophic, 12, (3); Cardiomyopathy, dilated, 1M, (3) DES Rare cardiomyopathy Cardiomyopathy, dilated, 1I, (3) FKTN Rare cardiomyopathy Cardiomyopathy, dilated, 1X, (3) GLA Rare cardiomyopathy Fabry disease, cardiac variant, (3) JPH2 Rare cardiomyopathy Cardiomyopathy, familial hypertrophic 17, (3) JUP Rare cardiomyopathy Arrhythmogenic right ventricular dysplasia 12, (3) LAMP2 Rare cardiomyopathy Danon disease, (3) MYLK2 Rare cardiomyopathy Cardiomyopathy, hypertrophic, midventricular, digenic, (3) MYOZ2 Rare cardiomyopathy Cardiomyopathy, familial hypertrophic, 16, (3) NEXN Rare cardiomyopathy Cardiomyopathy, dilated, 1CC, (3); Cardiomyopathy, familial hypertrophic, 20, (3) PLN Rare cardiomyopathy Cardiomyopathy, dilated, 1P, (3); Cardiomyopathy, familial hypertrophic, 18, (3) PRKAG2 Rare cardiomyopathy Cardiomyopathy, familial hypertrophic 6, (3); Wolff-Parkinson-White syndrome, (3) RBM20 Rare cardiomyopathy Cardiomyopathy, dilated, 1DD, (3) SGCD Rare cardiomyopathy Cardiomyopathy, dilated, 1L, (3) TAZ Rare cardiomyopathy Barth syndrome, (3) 10
12 TCAP Rare cardiomyopathy Cardiomyopathy, dilated, 1N, (3) TGFB3 Rare cardiomyopathy Arrhythmogenic right ventricular dysplasia 1, (3) TMEM43 Rare cardiomyopathy Arrhythmogenic right ventricular dysplasia 5, (3) TMPO Rare cardiomyopathy Cardiomyopathy, dilated, 1T, (3) VCL Rare cardiomyopathy Cardiomyopathy, familial hypertrophic, 15, (3) ALDH7A1 Epilepsy Epilepsy, pyridoxine-dependent, (3) ARHGEF9 Epilepsy Epileptic encephalopathy, early infantile, 8, (3) ARX Epilepsy Epileptic encephalopathy, early infantile, 1, (3) ASAH1 Epilepsy Spinal muscular atrophy with progressive myoclonic epilepsy, (3) CACNA1H Epilepsy {Epilepsy, childhood absence, susceptibility to, 6}, (3); {Epilepsy, idiopathic generalized, CACNB4 Epilepsy susceptibility to, 6}, (3) {Epilepsy, idiopathic generalized, susceptibility to, 9}, (3); {Epilepsy, juvenile myoclonic, susceptibility to, 6}, (3) CASR Epilepsy {Epilepsy idiopathic generalized, susceptibility to, 8}, (3) CARS2 Epilepsy Neurology Oct 31; PMID: CDKL5 Epilepsy Epileptic encephalopathy, early infantile, 2, (3) CHD2 Epilepsy Epileptic encephalopathy, childhood-onset, (3) CHRNA2 Epilepsy Epilepsy, nocturnal frontal lobe, type 4, (3) CHRNA4 Epilepsy Epilepsy, nocturnal frontal lobe, 1, (3) CHRNB2 Epilepsy Epilepsy, nocturnal frontal lobe, 3, (3) CLCN2 Epilepsy {Epilepsy, idiopathic generalized, susceptibility to, 11}, (3); {Epilepsy, juvenile absence, susceptibility to, 2}, (3);{Epilepsy, juvenile myoclonic, susceptibility to, 8}, (3) CLN8 Epilepsy Ceroid lipofuscinosis, neuronal, 8, Northern epilepsy variant, (3) CNTN2 Epilepsy?Epilepsy, familial adult myoclonic, 5, (3) CNTNAP2 Epilepsy Cortical dysplasia-focal epilepsy syndrome, (3) CPA6 Epilepsy Epilepsy, familial temporal lobe, 5, (3) CSTB Epilepsy Epilepsy, progressive myoclonic 1A (Unverricht and Lundborg), (3) DEPDC5 Epilepsy Epilepsy, familial focal, with variable foci, (3) DOCK7 Epilepsy Epileptic encephalopathy, early infantile, 23, (3) DNM1 Epilepsy Am J Hum Genet Oct 2;95(4):360-70; PMID: EFHC1 Epilepsy {Epilepsy, juvenile absence, susceptibility to, 1}, (3); {Myoclonic epilepsy, juvenile, susceptibility to, 1}, (3) EPM2A Epilepsy Epilepsy, progressive myoclonic 2A (Lafora), (3) 11
13 GABRA1 Epilepsy Epileptic encephalopathy, early infantile, 19, (3); {Epilepsy, childhood absence, susceptibility to, 4}, (3); {Epilepsy, juvenile myoclonic, susceptibility to, 5}, (3) GABRB3 Epilepsy {Epilepsy, childhood absence, susceptibility to, 5}, (3) GABRD Epilepsy {Epilepsy, generalized, with febrile seizures plus, type 5, susceptibility to}, (3); {Epilepsy, GABRG2 Epilepsy idiopathic generalized, 10}, (3); {Epilepsy, juvenile myoclonic, susceptibility to}, (3) Epilepsy, generalized, with febrile seizures plus, type 3, (3); {Epilepsy, childhood absence, susceptibility to, 2}, (3) GNAO1 Epilepsy Epileptic encephalopathy, early infantile, 17, (3) GOSR2 Epilepsy Epilepsy, progressive myoclonic 6, (3) GRIN2A Epilepsy Epilepsy, focal, with speech disorder and with or without mental retardation, (3) HCN1 Epilepsy Epileptic encephalopathy, early infantile, 24, (3) IER3IP1 Epilepsy Microcephaly, epilepsy, and diabetes syndrome, (3) KCNB1 Epilepsy Epileptic encephalopathy, early infantile, 26, (3) KCNA1 Epilepsy Epilepsia Nov;55(11): (PMID: ) KCNMA1 Epilepsy Generalized epilepsy and paroxysmal dyskinesia, (3) KCNQ2 Epilepsy Epileptic encephalopathy, early infantile, 7, (3) KCNT1 Epilepsy Epilepsy, nocturnal frontal lobe, 5, (3); Epileptic encephalopathy, early infantile, 14, (3) KCTD7 Epilepsy Epilepsy, progressive myoclonic 3, with or without intracellular inclusions, (3) LGI1 Epilepsy Epilepsy, familial temporal lobe, 1, (3) ME2 Epilepsy {Epilepsy, idiopathic generalized, susceptibility to}, (3) MEF2C Epilepsy Mental retardation, stereotypic movements, epilepsy, and/or cerebral malformations, (3) NECAP1 Epilepsy?Epileptic encephalopathy, early infantile, 21, (3) NHLRC1 Epilepsy Epilepsy, progressive myoclonic 2B (Lafora), (3) PAFAH1B1 Epilepsy Lissencephaly 1, (3) PCDH19 Epilepsy Epileptic encephalopathy, early infantile, 9, (3) PLCB1 Epilepsy Epileptic encephalopathy, early infantile, 12, (3) PNKP Epilepsy Nat Genet Mar;42(3):245-9 (PMID: ) PRICKLE1 Epilepsy Epilepsy, progressive myoclonic 1B, (3) PRICKLE2 Epilepsy Epilepsy, progressive myoclonic 5, (3) PRRT2 Epilepsy Neurology Nov 20;79(21): (PMID: ) SCARB2 Epilepsy Epilepsy, progressive myoclonic 4, with or without renal failure, (3) SCN1A Epilepsy Epilepsy, generalized, with febrile seizures plus, type 2, (3) 12
14 SCN1B Epilepsy/cardiac arrhythmia Epilepsy, generalized, with febrile seizures plus, type 1, (3) SCN2A Epilepsy Epileptic encephalopathy, early infantile, 11, (3) SCN8A Epilepsy Epileptic encephalopathy, early infantile, 13, (3) SCN9A Epilepsy Epilepsy, generalized, with febrile seizures plus, type 7, (3) SIAT9 Epilepsy Amish infantile epilepsy syndrome, (3) SLC13A5 Epilepsy Epileptic encephalopathy, early infantile, 25, (3) SLC25A22 Epilepsy Epileptic encephalopathy, early infantile, 3, (3) SLC2A1 Epilepsy {Epilepsy, idiopathic generalized, suscpetibility to, 12}, (3) SNIP1 Epilepsy Psychomotor retardation, epilepsy, and craniofacial dysmorphism, (3) SPTAN1 Epilepsy Epileptic encephalopathy, early infantile, 5, (3) SRPX2 Epilepsy?Rolandic epilepsy, mental retardation, and speech dyspraxia, (3) ST3GAL3 Epilepsy Epileptic encephalopathy, early infantile, 15, (3) STRADA Epilepsy Polyhydramnios, megalencephaly, and symptomatic epilepsy, (3) STXBP1 Epilepsy Epileptic encephalopathy, early infantile, 4, (3) SYN1 Epilepsy Epilepsy, X-linked, with variable learning disabilities and behavior disorders, (3) SYNGAP1 Epilepsy Nat Genet Jul;45(7):825-30; PMID: SZT2 Epilepsy Epileptic encephalopathy, early infantile, 18, (3) TBC1D24 Epilepsy Epileptic encephalopathy, early infantile, 16, (3); Myoclonic epilepsy, infantile, familial, (3) TNK2 Epilepsy Ann Neurol Sep;74(3): (PMID: ) 59 cardiac disease genes common to all sequencing panels were screened for rare variants in SUD cases. Genes were divided into Molecular Autopsy genes, Cardiac Arrhythmia genes, Major and Minor Cardiomyopathy genes and Rare Cardiomyopathy genes. Frequency of gene mutations in disease populations determined the Major (>5%), Minor (1 to 5%) and Rare (<1%) categories according to Wilde AA, Behr ER. Genetic testing for inherited cardiac disease. Nat Rev Cardiol Oct;10(10): On-line Mendelian Inheritance In Man (OMIM) entries for each gene are shown in right column. Epilepsy genes were defined by a review of recent literature and searching the OMIM database [Nov 01, 2014] for diseases containing the terms epilepsy or epileptic encephalopathy. 13
15 SUPPLEMENTARY APPENDIX TABLE S2. Cause of SCD vs Gender and Age Group Cause of SCD Number of Cases Male Female Age 1-5 Age 6-10 Age Age Age Age Age Average Age SUD (67%) 65 (33%) CAD (85%) 18 (15%) DCM (60%) 14 (40%) Myocarditits (56%) 14 (44%) ARVC (76%) 6 (24%) HCM (85%) 3 (15%) Aortic dissection (72%) 5 (27%) Other (73%) 12 (26%)
16 SUPPLEMENTARY APPENDIX TABLE S3: Activity at time of sudden death based on underlying disease Event Exercise Post exercise Light Activity Rest Sleep NA Total cases Aortic dissection 2 (11%) 0 2 (11%) 4 (22%) 1 (6%) 9 (50%) 18 ARVC 5 (20%) 3 (12%) 6 (24%) 5 (20%) 3 (12%) 3 (12%) 25 CAD 3 (3%) 4 (3%) 18 (15%) 32 (27%) 23 (20%) 38 (32%) 118 CPVT (100%) DCM 2 (6%) 0 4 (12%) 5 (14%) 11 (31%) 13 (37%) 35 HCM 4 (20%) 2 (10%) 3 (15%) 5 (25%) 5 (25%) 1 (5%) 20 LQTS (100%) Myocarditis 3 (10%) 0 1 (3%) 5 (16%) 9 (28%) 14 (43%) 32 Unexplained 18 (9%) 2 (1%) 28 (14%) 32 (17%) 80 (41%) 35 (18%) 195 Other 3 (7%) 3 (7%) 6 (14%) 7 (16%) 7 (16%) 18 (40%) 44 Total cases NA = (information) not available 15
17 SUPPLEMENTARY APPENDIX TABLE S4: Sudden death characteristics by 5-year age brackets 1-5 years 6-10 years years years years years years Exp SUD Total Exp SUD Total Exp SUD Total Exp SUD Total Exp SUD Total Exp SUD Total Exp SUD Total N (%) 12 (24) 37 (76) 49 (10) 2 (50) 2 (50) 4 (1) 13 (65) 7 (35) 20 (4) 26 (37) 45 (63) 71 (14) 38 (60) 25 (40) 63 (13) 70 (64) 40 (36) 110 (22) 131 (76) 42 (24) 173 (35) Male gender 5 (42) 26 (70) 31 (63) 0 (0) 1 (50) 1 (25) 9 (69) 5 (71) 14 (70) 18 (69) 38 (84) 56 (79) 32 (84) 15 (60) 47 (75) 54 (77) 24 (64) 78 (71) 102 (78) 24 (60) 126 (73) Exercise 0 (0) 0 (0) 0 (0) 1 (50) 0 (0) 1 (50) 4 (40) 1 (17) 5 (25) 5 (24) 8 (19) 13 (23) 6 (22) 5 (22) 11 (20) 6 (12) 4 (14) 10 (18) 12 (14) 4 (13) 16 (10) Sleep 5 (71) 30 (91) 35 (88) 0 (0) 0 (0) 0 (0) 3 (30) 2 (33) 5 (31) 9 (43) 19 (44) 28 (44) 7 (26) 10 (43) 17 (34) 13 (27) 9 (32) 22 (29) 22 (27) 10 (32) 32 (28) Night 5 (83) 19 (73) 24 (75) 0 (0) 1 (50) 1 (33) 3 (30) 2 (40) 5 (33) 17 (74) 24 (60) 41 (65) 10 (43) 14 (74) 24 (57) 25 (49) 17 (63) 42 (54) 43 (51) 24 (74) 67 (58) SUD = sudden unexplained death; Exp = explained sudden death 16
18 SUPPLEMENTARY APPENDIX TABLE S5: Unadjusted and Adjusted Odds Ratios for Factors Associated with SUD compared to Explained SCD Unadjusted OR (All cases n=490) Adjusted OR (n=349, R 2 =15%) n Unadjusted OR 95% CI p-value Adjusted OR 95% CI p-value Age, years < < ref - ref - Female gender Activity: Exercise Sleep Night death (6pm-6am) NB: Ref - reference age group for comparison, n - number of SCD cases 17
19 SUPPLEMENTARY APPENDIX TABLE S6: Rare Variants in Molecular Autopsy Genes Sample ID Gene cdna variation Amino acid change ESP MAF 1000G MAF ExAC count GERP++ score SIFT Polyphen2 Mutation Taster Pathogenicity Call NSW55A RYR2 NM_ :c.6506A>G Glu2169Gly D,D,D Likely Pathogenic VIC47A RYR2 NM_ :c.9673G>A Gly3225Ser D,P,D Likely Pathogenic VIC29A RYR2 NM_ :c.9680G>C Arg3227Pro D,P,D Likely Pathogenic NZ53A RYR2 NM_ :c.14266A>G Ile4756Val D,D,D Likely Pathogenic VIC56A SCN5A NM_ :c.659C>T Thr220Ile D,D,A Pathogenic NZ36A SCN5A NM_ :c.1637A>G Asp546Gly D,D,D Likely Pathogenic NSW123A SCN5A NM_ :c.1756_1761del Ala586_Leu587del Likely Pathogenic VIC44A SCN5A NM_ :c.5686C>T Arg1896Trp T,D,D Pathogenic NZ50A KCNH2 NM_ :c.784G>A Gly262Ser T,B,N VUS WA12A KCNH2 NM_ :c.889C>T Pro297Ser T,B,N VUS VIC83A KCNH2 NM_ :c.2246del Gly749Ala_fs* Likely Pathogenic WA5A KCNQ1 NM_ :c.1781G>C Arg594Pro D,D,D Pathogenic NB: ESP MAF - Minor allele frequency in ESP data; 1000G MAF - Minor allele frequency in 1000 Genomes Project data; ExAC count - Allele count in Exome Aggregate Consortium data; Rare MAF < 0.1%; T - Tolerated; B - Benign; D - Probably damaging; P - Possibly damaging; N - Neutral; A - Automatic pathogenic; VUS - Variant of uncertain significance. 18
20 SUPPLEMENTARY APPENDIX TABLE S7. Rare Variants in Cardiac Arrhythmia Genes. Sample ID Gene Symbol cdna variation Amino acid change ESP MAF 1000G MAF ExAC count GERP ++ score SIFT Polyphen2 Mutation Taster Pathogenicity Call VIC83A ANK2 NM_ :c.2474C>G Thr825Arg T,D,D Likely Pathogenic NSW14A ANK2 NM_ :c.8927C>G Ser2976Cys ,D,D Likely Pathogenic NSW12A ANK2 NM_ :c.9657T>G Ser3219Arg T,P,N VUS QLD42A ANK2 NM_ :c.11807A>G Tyr3936Cys D,D,N Likely Pathogenic NSW12A AKAP9 NM_ :c.2972C>T Ser991Leu T,B,N VUS NZ26A AKAP9 NM_ :C.3904del Thr1302Gln_fs* Likely Pathogenic NZ52A AKAP9 NM_ :c.5117A>G Asp1706Gly T,P,N VUS NSW105A AKAP9 NM_ :c.11189A>G Gln3730Arg D,D,D Likely Pathogenic WA7A SCN4B NM_ :c.40T>C Trp14Arg T,D,N VUS WA11A CACNA1C NM_ :c.521C>T Ala174Val D,P,D Likely Pathogenic NSW56A HCN4 NM_ :c.3206G>A Arg1069Gln T,B,N VUS NSW12A SCN1B NM_ :c.50C>G Ala17Gly T,D,N VUS ESP MAF - Minor allele frequency in ESP data; 1000G MAF - Minor allele frequency in 1000 Genomes Project data; ExAC count - Allele count in Exome Aggregate Consortium data; T - Tolerated; B - Benign; D - Probably damaging; P - Possibly damaging; N - Neutral; '.' - No prediction. VUS - Variant of uncertain significance 19
21 SUPPLEMENTARY APPENDIX TABLE S8: Rare Variants in Major and Minor Cardiomyopathy Genes Sample ID Gene cdna variation Amino acid change ESP MAF 1000G MAF ExAC count GERP++ score SIFT Polyphen2 Mutation Taster Pathogenicity Call NSW104A LMNA NM_ :c.1027C>T Arg343Trp D,D,D Likely Pathogenic NSW22A TNNT2 NM_ :c.452G>A Arg151Gln D,D,D Likely Pathogenic VIC72A MYL3 NM_ :c.220G>A Gly74Arg D,B,D Likely Pathogenic VIC11A DSP NM_ :c.2552T>A Leu851Gln T,P,D Likely Pathogenic QLD5A DSP NM_ :c.4352T>C Leu1451Pro D,P,D Likely Pathogenic NSW37A DSP NM_ :c.4565C>T Thr1522Met T,B,N VUS VIC60A DSP NM_ :c.4997G>A Arg1666Gln T,B,D VUS WA16A DSP NM_ :c.6046G>A Gly2016Arg T,D,D Likely Pathogenic VIC47A MYBPC3 NM_ :c.1003C>T Arg335Cys D,D,D Likely Pathogenic WA15A MYBPC3 NM_ :c.2980C>T Leu994Phe D,D,D Likely Pathogenic NSW100A PKP2 NM_ :c.253_256del Glu85Met_fs* Likely Pathogenic NZ14A PKP2 NM_ :c.968_972del Gln323Arg_fs* Likely Pathogenic WA6A MYH6 NM_ :c.440G>A Arg147Lys T,P,D Likely Pathogenic NSW55A MYH7 NM_ :c.1988G>A Arg663His T,P,D Pathogenic QLD50A MYH7 NM_ :c.2427C>A Asp809Glu T,B,D VUS NSW3A MYH7 NM_ :c.4321G>T Ala1441Ser T,B,D VUS VIC3A ACTC1 NM_ :c.961G>A Ala321Thr D,P,D Likely Pathogenic NSW20A TPM1 NM_ :c.161A>T Glu54Val D,D,D Likely Pathogenic QLD42A DSG2 NM_ :c.2563C>A Gln855Lys T,B,N VUS NB: ESP MAF - Minor allele frequency in ESP data; 1000G MAF - Minor allele frequency in 1000 Genomes Project data; ExAC count - Allele count in Exome Aggregate Consortium data; Rare MAF < 0.1%; T - Tolerated; B - Benign; D - Probably damaging; P - Possibly damaging; N Neutral; VUS - Variant of uncertain significance. 20
22 SUPPLEMENTARY APPENDIX TABLE S9. Rare Variants in Rare Cardiomyopathy Genes. Sample ID Gene Symbol cdna variation Amino acid change ESP MAF 1000G MAF ExAC count GERP ++ score SIFT Polyphen2 Mutation Taster Pathogenicity Call NSW56A NEXN NM_ :c.1499C>A Ala500Glu T,B,D VUS NZ14A ACTN2 NM_ :c.302A>G Asn101Ser D,D,D Likely pathogenic SA25A ACTN2 NM_ :c.2231C>T Thr744Met T,B,D VUS NZ38A DES NM_ :c.1310del Gly437Val_fs* Likely pathogenic NZ38A TMEM43 NM_ :c.355G>A Val119Met D,D,D Likely pathogenic SA22A PRKAG2 NM_ :c.452C>G Ser151Cys T,D,D Likely pathogenic QLD33A FKTN NM_ :c.743T>C Ile248Thr T,P,D Likely pathogenic WA11A FKTN NM_ :c.869A>T Lys290Ile T,B,N VUS NZ29A RBM20 NM_ :c.98C>A Pro33Gln D,B,N VUS NZ29A RBM20 NM_ :c.103C>G Pro35Ala D,B,N VUS VIC3A RBM20 NM_ :c.2588C>G Pro863Arg D,B,N VUS NZ49A RBM20 NM_ :c.3595G>A Glu1199Lys T,B,D VUS NSW28A CSRP3 NM_ :c.311_312del Thr104Lys_fs* Likely pathogenic VIC24A TCAP NM_ :c.175G>A Val59Met T,B,D VUS NSW22A JPH2 NM_ :c.1033G>C Val345Leu T,B,D VUS ESP MAF - Minor allele frequency in ESP data; 1000G MAF - Minor allele frequency in 1000 Genomes Project data; ExAC count - Allele count in Exome Aggregate Consortium data; T - Tolerated; B - Benign; D - Probably damaging; P - Possibly damaging; N - Neutral. VUS - Variant of uncertain significance 21
23 SUPPLEMENTARY APPENDIX TABLE S10. Likely Pathogenic Variants in Epilepsy Genes Implicated with Dominant Disorders. Sample ID Gene Symbol cdna variation Amino acid change ESP MAF 1000G MAF ExAC count GERP ++ score SIFT Polyphen2 Mutation Taster NZ29A CHD2 NM_ :c.907G>A Gly303Ser T,D,D VIC14A CHRNA4 NM_ :c.296G>A Arg99His D,B,D VIC24A SCN8A NM_ :c.4393C>T Arg1465Cys D,B,D QLD50A SPTAN1 NM_ :c.3604G>A Val1202Met T,P,D Pathogenicity call Likely pathogenic Likely pathogenic Likely pathogenic Likely pathogenic ESP MAF - Minor allele frequency in ESP data; 1000G MAF - Minor allele frequency in 1000 Genomes Project data; ExAC count - Allele count in Exome Aggregate Consortium data; T - Tolerated; B - Benign; D - Probably damaging; P - Possibly damaging; N - Neutral. VUS - Variant of uncertain significance 22
24 SUPPLEMENTARY APPENDIX TABLE S11: Likely pathogenic/pathogenic gene variants associated with SUD characteristics All Genes: Gene - Gene + p-value N (%) 86 (76) 27 (24) - Age, years (10) 6 (22) (1) 0 (0) (2) 1 (4) (29) 5 (19) (15) 3 (11) (23) 4 (15) (19) 8 (30) Male gender 64 (74) 19 (70) Activity Exercise 12 (16) 3 (13) Sleep 41 (53) 11 (48) Night death 52 (69) 18 (72) Arrhythmia Genes Only: Gene - Gene + p-value N (%) 97 (86) 16 (14) - Age, years (11) 4 (25) (1) 0 (0) (3) 0 (0) (30) 1 (6) (14) 2 (13) (22) 3 (19) (19) 6 (38) Male gender 72 (74) 11 (69) Activity Exercise 14 (16) 1 (7) Sleep 45 (52) 7 (50) Night death 60 (70) 10 (71)
25 SUPPLEMENTARY FIGURE LEGENDS SUPPLEMENTARY APPENDIX FIGURE S1: Variant classification scheme. Bioinformatic analysis pipeline used for variant classification. Abbreviations: MAF = minor allele frequency, VUS = variant of uncertain significance. SUPPLEMENTARY APPENDIX FIGURE S2: Clinical and demographic features comparing SUD with explained SCD cases by 5-year age groups. Sudden unexplained death (SUD) cases = grey bars; explained sudden death cases (SCD) = black bars; NC = no cases in the age group. SUPPLEMENTARY APPENDIX FIGURE S3: Clinical follow-up of SUD families. Abbreviations: SCD = sudden cardiac death, SUD = sudden unexplained death. 24
26 SUPPLEMENTARY FIGURES SUPPLEMENTARY APPENDIX FIGURE S1 25
27 SUPPLEMENTARY APPENDIX FIGURE S2 26
28 SUPPLEMENTARY APPENDIX FIGURE S3 27
29 REFERENCES 1. Li H, Durbin R. Fast and accurate short read alignment with Burrows-Wheeler transform. Bioinformatics 2009;25: Li H, Handsaker B, Wysoker A, et al. The Sequence Alignment/Map format and SAMtools. Bioinformatics 2009;25: McKenna A, Hanna M, Banks E, et al. The Genome Analysis Toolkit: a MapReduce framework for analyzing next-generation DNA sequencing data. Genome Res 2010;20:
The Genetics and Prevention of Sudden Cardiac Death
 The Genetics and Prevention of Sudden Cardiac Death Sudden cardiac death (SCD), a serious public health problem Every day, between 1,600 and 2,000 people die worldwide from genetically caused SCD. 1 SCD
The Genetics and Prevention of Sudden Cardiac Death Sudden cardiac death (SCD), a serious public health problem Every day, between 1,600 and 2,000 people die worldwide from genetically caused SCD. 1 SCD
A Prospective Study of Sudden Cardiac Death among Children and Young Adults
 The new england journal of medicine Original Article A Prospective Study of Sudden Cardiac Death among Children and Young Adults R.D. Bagnall, R.G. Weintraub, J. Ingles, J. Duflou, L. Yeates, L. Lam, A.M.
The new england journal of medicine Original Article A Prospective Study of Sudden Cardiac Death among Children and Young Adults R.D. Bagnall, R.G. Weintraub, J. Ingles, J. Duflou, L. Yeates, L. Lam, A.M.
Preventing Sudden Death in Young Athletes. Outline. Scope of the Problem. Causes of SCD in Young Athletes. Sudden death in the young athlete
 Preventing Sudden Death in Young Athletes Ronn E. Tanel, MD Director, Pediatric Arrhythmia Service UCSF Children s Hospital Associate Professor of Pediatrics UCSF School of Medicine Outline Sudden death
Preventing Sudden Death in Young Athletes Ronn E. Tanel, MD Director, Pediatric Arrhythmia Service UCSF Children s Hospital Associate Professor of Pediatrics UCSF School of Medicine Outline Sudden death
Targeted Genes and Methodology Details for Epilepsy/Seizure Genetic Panels
 Targeted s and Methodology Details for Epilepsy/Seizure tic Panels Reference transcripts based on build GRCh37 (hg19) interrogated by Epilepsy/Seizure tic Panels Epilepsy Expanded Panel Epilepsy Expanded
Targeted s and Methodology Details for Epilepsy/Seizure tic Panels Reference transcripts based on build GRCh37 (hg19) interrogated by Epilepsy/Seizure tic Panels Epilepsy Expanded Panel Epilepsy Expanded
Molecular Diagnostic Laboratory 18 Sequencing St, Gene Town, ZY Tel: Fax:
 Molecular Diagnostic Laboratory 18 Sequencing St, Gene Town, ZY 01234 Tel: 555-920-3333 Fax: 555-920-3334 www.moldxlaboratory.com Patient Name: Jane Doe Specimen type: Blood, peripheral DOB: 04/05/1990
Molecular Diagnostic Laboratory 18 Sequencing St, Gene Town, ZY 01234 Tel: 555-920-3333 Fax: 555-920-3334 www.moldxlaboratory.com Patient Name: Jane Doe Specimen type: Blood, peripheral DOB: 04/05/1990
NGS in Diagnostics: a practical example in hereditary cardiomyopathies
 NGS in Diagnostics: a practical example in hereditary cardiomyopathies Patricia Norambuena University Hospital Motol, Prague. 2 nd Faculty of Medicine, Charles University VEP Course - November 6 th - 8th,
NGS in Diagnostics: a practical example in hereditary cardiomyopathies Patricia Norambuena University Hospital Motol, Prague. 2 nd Faculty of Medicine, Charles University VEP Course - November 6 th - 8th,
Molecular Diagnosis of Genetic Diseases: From 1 Gene to 1000s
 ROMA, 23 GIUGNO 2011 Molecular Diagnosis of Genetic Diseases: From 1 Gene to 1000s USSD Lab Genetica Medica Ospedali Riuniti Bergamo The problem What does the clinician/patient want to know?? Diagnosis,
ROMA, 23 GIUGNO 2011 Molecular Diagnosis of Genetic Diseases: From 1 Gene to 1000s USSD Lab Genetica Medica Ospedali Riuniti Bergamo The problem What does the clinician/patient want to know?? Diagnosis,
Genetic testing in Cardiomyopathies
 Genetic testing in Cardiomyopathies Silvia Giuliana Priori Cardiovascular Genetics, Langone Medical Center, New York University School of Medicine, New York, USA and Molecular Cardiology, IRCCS Fondazione
Genetic testing in Cardiomyopathies Silvia Giuliana Priori Cardiovascular Genetics, Langone Medical Center, New York University School of Medicine, New York, USA and Molecular Cardiology, IRCCS Fondazione
SUPPLEMENTAL MATERIAL ADDITIONAL TABLES
 SUPPLEMENTAL MATERIAL ADDITIONAL TABLES Table S1. List of distinct rare variants detected by high-throughput sequencing in our cohort. The number of patients with each variant and the reference for the
SUPPLEMENTAL MATERIAL ADDITIONAL TABLES Table S1. List of distinct rare variants detected by high-throughput sequencing in our cohort. The number of patients with each variant and the reference for the
Dr. Sarah Weckhuysen, MD, PhD. Neurogenetics Group, VIB-Department of Molecular Genetics University of Antwerp, Belgium
 Dr. Sarah Weckhuysen, MD, PhD Neurogenetics Group, VIB-Department of Molecular Genetics University of Antwerp, Belgium Common Prevalence 4-8/1000 Life time incidence 3% Key symptom = seizures Nature Reviews
Dr. Sarah Weckhuysen, MD, PhD Neurogenetics Group, VIB-Department of Molecular Genetics University of Antwerp, Belgium Common Prevalence 4-8/1000 Life time incidence 3% Key symptom = seizures Nature Reviews
Inherited Arrhythmia Syndromes
 Inherited Arrhythmia Syndromes When to perform Genetic testing? Arthur AM Wilde February 4, 2017 Which pts should undergo genetic testing? SCD victims with a likely diagnosis Pts diagnosed with an inherited
Inherited Arrhythmia Syndromes When to perform Genetic testing? Arthur AM Wilde February 4, 2017 Which pts should undergo genetic testing? SCD victims with a likely diagnosis Pts diagnosed with an inherited
J. Peter van Tintelen MD PhD Clinical Geneticist Amsterdam, the Netherlands
 Inherited arrhythmia syndromes I: What you always wanted to know, but were afraid to ask: The basics of inherited arrhythmia syndromes and gene:cs J. Peter van Tintelen MD PhD Clinical Geneticist Amsterdam,
Inherited arrhythmia syndromes I: What you always wanted to know, but were afraid to ask: The basics of inherited arrhythmia syndromes and gene:cs J. Peter van Tintelen MD PhD Clinical Geneticist Amsterdam,
Clinical Genetics in Cardiomyopathies
 Clinical Genetics in Cardiomyopathies Γεώργιος Κ Ευθυμιάδης Αναπληρωτής Καθηγητής Καρδιολογίας ΑΠΘ No conflict of interest Genetic terms Proband: The first individual diagnosed in a family Mutation: A
Clinical Genetics in Cardiomyopathies Γεώργιος Κ Ευθυμιάδης Αναπληρωτής Καθηγητής Καρδιολογίας ΑΠΘ No conflict of interest Genetic terms Proband: The first individual diagnosed in a family Mutation: A
Investigating the family after a sudden cardiac death. Dr Catherine Mercer Consultant Clinical Geneticist, Wessex
 Investigating the family after a sudden cardiac death Dr Catherine Mercer Consultant Clinical Geneticist, Wessex Sudden adult deaths subdivided Sudden Adult Death Sudden Cardiac Death Sudden Arrhythmic
Investigating the family after a sudden cardiac death Dr Catherine Mercer Consultant Clinical Geneticist, Wessex Sudden adult deaths subdivided Sudden Adult Death Sudden Cardiac Death Sudden Arrhythmic
Dr. Sarah Weckhuysen, MD, PhD. Neurogenetics Group, VIB-Department of Molecular Genetics University of Antwerp, Belgium
 Dr. Sarah Weckhuysen, MD, PhD Neurogenetics Group, VIB-Department of Molecular Genetics University of Antwerp, Belgium Sarah Weckhuysen No relevant financial relationships with any commercial interests.
Dr. Sarah Weckhuysen, MD, PhD Neurogenetics Group, VIB-Department of Molecular Genetics University of Antwerp, Belgium Sarah Weckhuysen No relevant financial relationships with any commercial interests.
A European Reference Network for rare and complex epilepsies. J Helen Cross Coordinator
 A European Reference Network for rare and complex epilepsies J Helen Cross Coordinator The epilepsies a group of rare diseases Early myoclonic encephalopathy PIGA, SETBP1, SIK1, SLC25A22 Dravet syndrome
A European Reference Network for rare and complex epilepsies J Helen Cross Coordinator The epilepsies a group of rare diseases Early myoclonic encephalopathy PIGA, SETBP1, SIK1, SLC25A22 Dravet syndrome
Homozygous PKP2 deletion associated with neonatal left ventricle noncompaction
 Clin Genet 2017: 91: 126 130 Printed in Singapore. All rights reserved Short Report 2016 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd CLINICAL GENETICS doi: 10.1111/cge.12780 Homozygous PKP2
Clin Genet 2017: 91: 126 130 Printed in Singapore. All rights reserved Short Report 2016 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd CLINICAL GENETICS doi: 10.1111/cge.12780 Homozygous PKP2
ERN EpiCARE. A European Reference Network for Rare and Complex Epilepsies. Petr Marusic Motol University Hospital, Prague
 ERN EpiCARE A European Reference Network for Rare and Complex Epilepsies Petr Marusic Motol University Hospital, Prague Disclosure I have no actual or potential conflict of interest in relation to this
ERN EpiCARE A European Reference Network for Rare and Complex Epilepsies Petr Marusic Motol University Hospital, Prague Disclosure I have no actual or potential conflict of interest in relation to this
Epileptogenesis: A Clinician s Perspective
 Epileptogenesis: A Clinician s Perspective Samuel F Berkovic Epilepsy Research Centre, University of Melbourne Austin Health Epileptogenesis The process of development and sustaining the propensity to
Epileptogenesis: A Clinician s Perspective Samuel F Berkovic Epilepsy Research Centre, University of Melbourne Austin Health Epileptogenesis The process of development and sustaining the propensity to
Name of Presenter: Marwan Refaat, MD
 NAAMA s 24 th International Medical Convention Medicine in the Next Decade: Challenges and Opportunities Beirut, Lebanon June 26 July 2, 2010 I have no actual or potential conflict of interest in relation
NAAMA s 24 th International Medical Convention Medicine in the Next Decade: Challenges and Opportunities Beirut, Lebanon June 26 July 2, 2010 I have no actual or potential conflict of interest in relation
Definition and classification of the cardiomyopathies. Georgios K Efthimiadis Ass Prof of Cardiology
 Definition and classification of the cardiomyopathies Georgios K Efthimiadis Ass Prof of Cardiology Historical Context WHO: 1980 classification "heart muscle diseases of unknown cause" WHO 1995 classification
Definition and classification of the cardiomyopathies Georgios K Efthimiadis Ass Prof of Cardiology Historical Context WHO: 1980 classification "heart muscle diseases of unknown cause" WHO 1995 classification
Whole Exome Sequencing (WES): Questions and Answers for Providers
 Whole Exome Sequencing (WES): Questions and Answers for Providers 1. What is Whole Exome Sequencing?... 2 2. What is the difference between Whole Exome Sequencing (WES) and Whole Exome Sequencing Plus
Whole Exome Sequencing (WES): Questions and Answers for Providers 1. What is Whole Exome Sequencing?... 2 2. What is the difference between Whole Exome Sequencing (WES) and Whole Exome Sequencing Plus
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Hereditary Cardiovascular Conditions. genetic testing for undiagnosed diseases
 Hereditary Cardiovascular Conditions genetic testing for undiagnosed diseases What is Hypertrophic Cardiomyopathy (HCM)? normal heart heart with hcm Extra or thick heart muscle Typically in the left ventricle
Hereditary Cardiovascular Conditions genetic testing for undiagnosed diseases What is Hypertrophic Cardiomyopathy (HCM)? normal heart heart with hcm Extra or thick heart muscle Typically in the left ventricle
Inherited Cardiomyopathies Molecular genetics and Clinical genetic testing
 Inherited Cardiomyopathies Molecular genetics and Clinical genetic testing Dr Shagun Aggarwal Associate Professor, Department of Medical Genetics Nizam s Institute of Medical Sciences Adjunct Scientist,
Inherited Cardiomyopathies Molecular genetics and Clinical genetic testing Dr Shagun Aggarwal Associate Professor, Department of Medical Genetics Nizam s Institute of Medical Sciences Adjunct Scientist,
Key determinants of pathogenicity
 Key determinants of pathogenicity Session 6: Determining pathogenicity and genotype-phenotype correlation J. Peter van Tintelen MD PhD Clinical geneticist Academic Medical Center Amsterdam, the Netherlands
Key determinants of pathogenicity Session 6: Determining pathogenicity and genotype-phenotype correlation J. Peter van Tintelen MD PhD Clinical geneticist Academic Medical Center Amsterdam, the Netherlands
Corporate Medical Policy
 Corporate Medical Policy Genetic Testing for Predisposition to Inherited Hypertrophic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_predisposition_to_inherited_hypertrophic_cardiomyopathy
Corporate Medical Policy Genetic Testing for Predisposition to Inherited Hypertrophic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_predisposition_to_inherited_hypertrophic_cardiomyopathy
Test Information Sheet
 Combined Cardiac Panel Test Information Sheet Panel Gene List: ABCC9, ACTC1, ACTN2, AKAP9, ALMS1, ALPK3, ANK2, ANKRD1, BAG3, BRAF, CACNA1C, CACNA2D1, CACNB2, CALM1, CALM2, CALM3, CASQ2, CAV3, CHRM2, CRYAB,
Combined Cardiac Panel Test Information Sheet Panel Gene List: ABCC9, ACTC1, ACTN2, AKAP9, ALMS1, ALPK3, ANK2, ANKRD1, BAG3, BRAF, CACNA1C, CACNA2D1, CACNB2, CALM1, CALM2, CALM3, CASQ2, CAV3, CHRM2, CRYAB,
Hypertrophic Cardiomyopathy
 Hypertrophic Cardiomyopathy From Genetics to ECHO Alexandra A Frogoudaki Second Cardiology Department ATTIKON University Hospital Athens University Athens, Greece EUROECHO 2010, Copenhagen, 11/12/2010
Hypertrophic Cardiomyopathy From Genetics to ECHO Alexandra A Frogoudaki Second Cardiology Department ATTIKON University Hospital Athens University Athens, Greece EUROECHO 2010, Copenhagen, 11/12/2010
Genetics of Sudden Cardiac Death. Geoffrey Pitt Ion Channel Research Unit Duke University. Disclosures: Grant funding from Medtronic.
 Genetics of Sudden Cardiac Death Geoffrey Pitt Ion Channel Research Unit Duke University Disclosures: Grant funding from Medtronic Duke U N I V E R S I T Y Sudden Cardiac Death High incidence 50-100 per
Genetics of Sudden Cardiac Death Geoffrey Pitt Ion Channel Research Unit Duke University Disclosures: Grant funding from Medtronic Duke U N I V E R S I T Y Sudden Cardiac Death High incidence 50-100 per
COMPLETE A FORM FOR EACH SAMPLE SUBMITTED ETHNIC BACKGROUND REPORTING INFORMATION
 DATE SAMPLE DRAWN: SAMPLE TYPE: BLOOD OTHER (SPECIFY): COMPLETE A FORM FOR EACH SAMPLE SUBMITTED PATIENT FIRST NAME: LAST NAME: DOB: SEX: M F UNKNOWN ADDRESS: HOME PHONE: ( ) WORK: ( ) EUROPEAN CAUCASIAN
DATE SAMPLE DRAWN: SAMPLE TYPE: BLOOD OTHER (SPECIFY): COMPLETE A FORM FOR EACH SAMPLE SUBMITTED PATIENT FIRST NAME: LAST NAME: DOB: SEX: M F UNKNOWN ADDRESS: HOME PHONE: ( ) WORK: ( ) EUROPEAN CAUCASIAN
The Genetics and Genomics of Familial Heart Disease. The Genetics and Genomics of Familial Heart Disease
 The Genetics and Genomics of Familial Heart Disease Bringing Precision Medicine to Life! Ray Hershberger, MD Professor Department of Internal Medicine Director, Division of Human Genetics Joint Appointment,
The Genetics and Genomics of Familial Heart Disease Bringing Precision Medicine to Life! Ray Hershberger, MD Professor Department of Internal Medicine Director, Division of Human Genetics Joint Appointment,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_epilepsy 1/28/14 10/2017 10/2018 10/2017 Description of Procedure or Service Description
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_epilepsy 1/28/14 10/2017 10/2018 10/2017 Description of Procedure or Service Description
Sudden cardiac death: focus on the genetics of channelopathies and cardiomyopathies
 Magi et al. Journal of Biomedical Science (2017) 24:56 DOI 10.1186/s12929-017-0364-6 REVIEW Sudden cardiac death: focus on the genetics of channelopathies and cardiomyopathies Simona Magi 1*, Vincenzo
Magi et al. Journal of Biomedical Science (2017) 24:56 DOI 10.1186/s12929-017-0364-6 REVIEW Sudden cardiac death: focus on the genetics of channelopathies and cardiomyopathies Simona Magi 1*, Vincenzo
Strength and weakness of genetic testing in clinical routine.
 Strength and weakness of genetic testing in clinical routine. Silvia G Priori MD PhD Molecular Cardiology, IRCCS Fondazione Maugeri Pavia, Italy AND Leon Charney Division of Cardiology, Cardiovascular
Strength and weakness of genetic testing in clinical routine. Silvia G Priori MD PhD Molecular Cardiology, IRCCS Fondazione Maugeri Pavia, Italy AND Leon Charney Division of Cardiology, Cardiovascular
Family stories: to illustrate inheritance and the impact on families. Dr Claire Turner Consultant clinical geneticist
 Family stories: to illustrate inheritance and the impact on families Dr Claire Turner Consultant clinical geneticist Overview With respect to inherited cardiac conditions Simple modes of inheritance (Mendelian)
Family stories: to illustrate inheritance and the impact on families Dr Claire Turner Consultant clinical geneticist Overview With respect to inherited cardiac conditions Simple modes of inheritance (Mendelian)
What genetic abnormalities should we search for after a sudden death?
 What genetic abnormalities should we search for after a sudden death? Dr Estelle GANDJBAKHCH Hôpital Pitié salpêtrière Rythmologie Centre de référence pour les maladies cardiaques héréditaires Disclosure
What genetic abnormalities should we search for after a sudden death? Dr Estelle GANDJBAKHCH Hôpital Pitié salpêtrière Rythmologie Centre de référence pour les maladies cardiaques héréditaires Disclosure
THE ROLE OF MOLECULAR AUTOPSY IN 2014: FROM THE ANATOMICAL THEATRE TO THE DOUBLE HELIX. Gaetano Thiene, MD
 THE ROLE OF MOLECULAR AUTOPSY IN 2014: FROM THE ANATOMICAL THEATRE TO THE DOUBLE HELIX Gaetano Thiene, MD Torino, October 23, 2014 The Role of the Autopsy in SD To establish or consider: whether the death
THE ROLE OF MOLECULAR AUTOPSY IN 2014: FROM THE ANATOMICAL THEATRE TO THE DOUBLE HELIX Gaetano Thiene, MD Torino, October 23, 2014 The Role of the Autopsy in SD To establish or consider: whether the death
No mutations were identified.
 Hereditary Heart Health Test DOB: May 25, 1977 ID: 123456 Sex: Female Requisition #: 123456 ORDERING PHYSICIAN Dr. Jenny Jones Sample Medical Group 123 Main St. Sample, CA SPECIMEN Type: Saliva Barcode:
Hereditary Heart Health Test DOB: May 25, 1977 ID: 123456 Sex: Female Requisition #: 123456 ORDERING PHYSICIAN Dr. Jenny Jones Sample Medical Group 123 Main St. Sample, CA SPECIMEN Type: Saliva Barcode:
Epilepsy. Genetic Test Submission Guide. 2. Samples. 1. Forms. 3. Ship RESULTS. impactgenetics.com
 Epilepsy Genetic Test Submission Guide 1. Forms 2. Samples Form 1d: If applicable Form 1b: Requisition Form Form 1a: Informed Consent 3. Ship RESULTS Impact Genetics, Dynacare 4-1100 Bennett Rd. Bowmanville,
Epilepsy Genetic Test Submission Guide 1. Forms 2. Samples Form 1d: If applicable Form 1b: Requisition Form Form 1a: Informed Consent 3. Ship RESULTS Impact Genetics, Dynacare 4-1100 Bennett Rd. Bowmanville,
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Supplementary Figure 1: Classification scheme for non-synonymous and nonsense germline MC1R variants. The common variants with previously established
 Supplementary Figure 1: Classification scheme for nonsynonymous and nonsense germline MC1R variants. The common variants with previously established classifications 1 3 are shown. The effect of novel missense
Supplementary Figure 1: Classification scheme for nonsynonymous and nonsense germline MC1R variants. The common variants with previously established classifications 1 3 are shown. The effect of novel missense
Epilepsie & ernstige mentale retardatie: (nieuwe) genen en genotype-fenotype correlatie
 Epilepsie & ernstige mentale retardatie: (nieuwe) genen en genotype-fenotype correlatie dr. Hannah Stamberger prof. dr. Peter De Jonghe Neurogenetics group, DMG, VIB http://www.molgen.vib-ua.be Disclosures
Epilepsie & ernstige mentale retardatie: (nieuwe) genen en genotype-fenotype correlatie dr. Hannah Stamberger prof. dr. Peter De Jonghe Neurogenetics group, DMG, VIB http://www.molgen.vib-ua.be Disclosures
Genetic Cardiomyopathies
 2017 HFCT Annual Scientific Meeting The Heart Failure Crosstalk Genetic Cardiomyopathies Teerapat Yingchoncharoen M.D. Ramathibodi Hospital Cardiomyopathy Group of diseases of the myocardium associated
2017 HFCT Annual Scientific Meeting The Heart Failure Crosstalk Genetic Cardiomyopathies Teerapat Yingchoncharoen M.D. Ramathibodi Hospital Cardiomyopathy Group of diseases of the myocardium associated
Review. The Genetics of Cardiac Disease Associated with Sudden Cardiac Death
 ASIP 2012 JMD CME Program Review The Journal of Molecular Diagnostics, Vol. 14, No. 5, September 2012 Copyright 2012 American Society for Investigative Pathology and the Association for Molecular Pathology.
ASIP 2012 JMD CME Program Review The Journal of Molecular Diagnostics, Vol. 14, No. 5, September 2012 Copyright 2012 American Society for Investigative Pathology and the Association for Molecular Pathology.
Pearls of the ESC/ERS Guidelines 2015 Channelopathies
 Pearls of the ESC/ERS Guidelines 2015 Channelopathies Carina Blomstrom Lundqvist Dept Cardiology, Uppsala, Sweden Content 2015 ESC Guidelines for the Management of Patients with Ventricular Arrhythmias
Pearls of the ESC/ERS Guidelines 2015 Channelopathies Carina Blomstrom Lundqvist Dept Cardiology, Uppsala, Sweden Content 2015 ESC Guidelines for the Management of Patients with Ventricular Arrhythmias
Implications of the new diagnostic criteria for ARVC
 EUROECHO 2010 Echocardiographic assessment of cardiomyopathies Implications of the new diagnostic criteria for ARVC Barbara Bauce, MD, PhD Department of Cardiac, Thoracic and Vascular Sciences University
EUROECHO 2010 Echocardiographic assessment of cardiomyopathies Implications of the new diagnostic criteria for ARVC Barbara Bauce, MD, PhD Department of Cardiac, Thoracic and Vascular Sciences University
Cardiac Conditions in Sport & Exercise. Cardiac Conditions in Sport. USA - Sudden Cardiac Death (SCD) Dr Anita Green. Sudden Cardiac Death
 Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Test Information Sheet
 Genetic Testing for Epilepsy: Childhood Epilepsy Panel Sequence Analysis and Exon-Level Deletion/Duplication Testing of 58 Genes Panel Gene List: SL, CACNA1A, CDKL5, CHD2, CHRNA2, CHRNA4, CHRNA7*, CHRNB2,
Genetic Testing for Epilepsy: Childhood Epilepsy Panel Sequence Analysis and Exon-Level Deletion/Duplication Testing of 58 Genes Panel Gene List: SL, CACNA1A, CDKL5, CHD2, CHRNA2, CHRNA4, CHRNA7*, CHRNB2,
HA Convention 2010 Dr Liz YP Yuen Department of Chemical Pathology Prince of Wales Hospital
 HA Convention 2010 Dr Liz YP Yuen Department of Chemical Pathology Prince of Wales Hospital 1 2 Sudden death an unexpected natural death within a short time period, generally 1 hour or less from the onset
HA Convention 2010 Dr Liz YP Yuen Department of Chemical Pathology Prince of Wales Hospital 1 2 Sudden death an unexpected natural death within a short time period, generally 1 hour or less from the onset
Epi4K. Epi4K Consortium. Epi4K: gene discovery in 4,000 genomes, Epilepsia, 2012 Aug;53(8):
 Epi4K Epi4K Consortium. Epi4K: gene discovery in 4,000 genomes, Epilepsia, 2012 Aug;53(8):1457-67. Genetics of Epileptic Encephalopathies Infantile Spasms (IS) 1 in 3000 live births and onset between 4-12
Epi4K Epi4K Consortium. Epi4K: gene discovery in 4,000 genomes, Epilepsia, 2012 Aug;53(8):1457-67. Genetics of Epileptic Encephalopathies Infantile Spasms (IS) 1 in 3000 live births and onset between 4-12
Genetics of cardiomyopathy and channelopathy
 Genetics of cardiomyopathy and channelopathy Heart Failure Research Center, Department of Experimental Cardiology, AMC, Amsterdam, The Netherlands Correspondence: C. R. Bezzina, Heart Failure Research
Genetics of cardiomyopathy and channelopathy Heart Failure Research Center, Department of Experimental Cardiology, AMC, Amsterdam, The Netherlands Correspondence: C. R. Bezzina, Heart Failure Research
Cardiology Genetics Report Long QT Syndrome (LQTS) Panel
 Patient Name: Test(s) Requested: The ordered test and the genes analyzed are Genes Evaluated (Disease): Result: Only mutations detected appear here KCNQ1 (LQT1 and Jervell and LangeNielsen syndrome), KCNH2
Patient Name: Test(s) Requested: The ordered test and the genes analyzed are Genes Evaluated (Disease): Result: Only mutations detected appear here KCNQ1 (LQT1 and Jervell and LangeNielsen syndrome), KCNH2
Family Education and Support
 Family Education and Support Key Topics First Aid Seizure Safety Sports Physical Activity Driving Familial Psychosocial Needs in Treating Pediatric Epilepsy Poll Question 1 Which of the following is not
Family Education and Support Key Topics First Aid Seizure Safety Sports Physical Activity Driving Familial Psychosocial Needs in Treating Pediatric Epilepsy Poll Question 1 Which of the following is not
Code CPT Descriptor Test Purpose and Method Crosswalk Recommendation SEPT9 (Septin9) (e.g., colorectal cancer) methylation analysis
 ASSOCIATION FOR MOLECULAR PATHOLOGY Education. Innovation & Improved Patient Care. Advocacy. 9650 Rockville Pike. Bethesda, Maryland 20814 Tel: 301-634-7939 Fax: 301-634-7995 amp@amp.org www.amp.org August
ASSOCIATION FOR MOLECULAR PATHOLOGY Education. Innovation & Improved Patient Care. Advocacy. 9650 Rockville Pike. Bethesda, Maryland 20814 Tel: 301-634-7939 Fax: 301-634-7995 amp@amp.org www.amp.org August
SEMINAIRES IRIS. Sudden cardiac death in the adult. Gian Battista Chierchia. Heart Rhythm Management Center, UZ Brussel. 20% 25% Cancers !
 Sudden cardiac death in the adult Gian Battista Chierchia. Heart Rhythm Management Center, UZ Brussel.! " # $ % Cancers National Vital Statistics Report, Vol 49 (11), Oct. 12, 2001. 20% 25% State-specific
Sudden cardiac death in the adult Gian Battista Chierchia. Heart Rhythm Management Center, UZ Brussel.! " # $ % Cancers National Vital Statistics Report, Vol 49 (11), Oct. 12, 2001. 20% 25% State-specific
The Screening Debate. Robert M. Campbell, MD Children s Healthcare of Atlanta Emory University School of Medicine
 The Screening Debate Robert M. Campbell, MD Children s Healthcare of Atlanta Emory University School of Medicine No Disclosures Screening screen ing ˈskrēniNG/ noun noun: screening; plural noun: screenings
The Screening Debate Robert M. Campbell, MD Children s Healthcare of Atlanta Emory University School of Medicine No Disclosures Screening screen ing ˈskrēniNG/ noun noun: screening; plural noun: screenings
Clinical phenotypes associated with Desmosome gene mutations
 Clinical phenotypes associated with Desmosome gene mutations Serio A, Serafini E, Pilotto A, Pasotti M, Gambarin F, Grasso M, Disabella E, Diegoli M, Tagliani M, Arbustini E Centre for Inherited Cardiovascular
Clinical phenotypes associated with Desmosome gene mutations Serio A, Serafini E, Pilotto A, Pasotti M, Gambarin F, Grasso M, Disabella E, Diegoli M, Tagliani M, Arbustini E Centre for Inherited Cardiovascular
Paediatric Cardiomyopathy
 Paediatric Cardiomyopathy Contact details: Bristol Genetics Laboratory Pathology Sciences Southmead Hospital Bristol, BS10 5NB Enquiries: 0117 414 6174 FAX: 0117 414 6464 Head of department: Eileen Roberts
Paediatric Cardiomyopathy Contact details: Bristol Genetics Laboratory Pathology Sciences Southmead Hospital Bristol, BS10 5NB Enquiries: 0117 414 6174 FAX: 0117 414 6464 Head of department: Eileen Roberts
The landscape of genetic variation in dilated cardiomyopathy as surveyed by clinical DNA sequencing
 American College of Medical Genetics and Genomics Original Research Article The landscape of genetic variation in dilated cardiomyopathy as surveyed by clinical DNA sequencing Trevor J. Pugh, PhD 1,2,3,
American College of Medical Genetics and Genomics Original Research Article The landscape of genetic variation in dilated cardiomyopathy as surveyed by clinical DNA sequencing Trevor J. Pugh, PhD 1,2,3,
CardioPathy panel. versie V4 (167 genen) Centrum voor Medische Genetica Gent
 CardioPathy panel versie V4 (167 genen) Centrum voor Medische Genetica Gent Gene OMIM gene ID ABCC9 601439 Associated phenotype, OMIM phenotype ID, phenotype mapping key and inheritance pattern Atrial
CardioPathy panel versie V4 (167 genen) Centrum voor Medische Genetica Gent Gene OMIM gene ID ABCC9 601439 Associated phenotype, OMIM phenotype ID, phenotype mapping key and inheritance pattern Atrial
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI).
 1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
Cardiac MRI: Clinical Application to Disease
 Cardiac MRI: Clinical Application to Disease Jessi Smith, MD Cardiothoracic imaging, Indiana University Slides courtesy of Stacy Rissing, MD Outline Imaging planes Disease findings Pulse sequences used
Cardiac MRI: Clinical Application to Disease Jessi Smith, MD Cardiothoracic imaging, Indiana University Slides courtesy of Stacy Rissing, MD Outline Imaging planes Disease findings Pulse sequences used
Pondering Epilepsy Classification (actually a few thoughts on the impact of genetic analyses of the epilepsies) Genetics of Epilepsies
 Pondering Epilepsy Classification (actually a few thoughts on the impact of genetic analyses of the epilepsies) Dan Lowenstein UCSF Department of Neurology and the UCSF Epilepsy Center To Cover: 1. Update
Pondering Epilepsy Classification (actually a few thoughts on the impact of genetic analyses of the epilepsies) Dan Lowenstein UCSF Department of Neurology and the UCSF Epilepsy Center To Cover: 1. Update
Identifying Mutations Responsible for Rare Disorders Using New Technologies
 Identifying Mutations Responsible for Rare Disorders Using New Technologies Jacek Majewski, Department of Human Genetics, McGill University, Montreal, QC Canada Mendelian Diseases Clear mode of inheritance
Identifying Mutations Responsible for Rare Disorders Using New Technologies Jacek Majewski, Department of Human Genetics, McGill University, Montreal, QC Canada Mendelian Diseases Clear mode of inheritance
Arrhythmias (II) Ventricular Arrhythmias. Disclosures
 Arrhythmias (II) Ventricular Arrhythmias Amy Leigh Miller, MD, PhD Cardiovascular Electrophysiology, Brigham & Women s Hospital Disclosures None Rhythms and Mortality Implantable loop recorder post-mi
Arrhythmias (II) Ventricular Arrhythmias Amy Leigh Miller, MD, PhD Cardiovascular Electrophysiology, Brigham & Women s Hospital Disclosures None Rhythms and Mortality Implantable loop recorder post-mi
Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations
 Sports Cardiology Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations Domenico Corrado, MD, PhD Inherited Arrhytmogenic Cardiomyopathy Unit Department of Cardiac, Thoracic and
Sports Cardiology Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations Domenico Corrado, MD, PhD Inherited Arrhytmogenic Cardiomyopathy Unit Department of Cardiac, Thoracic and
Medical Policy. MP Genetic Testing for Epilepsy
 Medical Policy MP 2.04.109 BCBSA Ref. Policy: 2.04.109 Last Review: 02/26/2018 Effective Date: 02/26/2018 Section: Medicine Related Policies 2.04.81 Genetic Testing for Rett Syndrome 2.04.83 Genetic Testing
Medical Policy MP 2.04.109 BCBSA Ref. Policy: 2.04.109 Last Review: 02/26/2018 Effective Date: 02/26/2018 Section: Medicine Related Policies 2.04.81 Genetic Testing for Rett Syndrome 2.04.83 Genetic Testing
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): October 1, 2014 Most Recent Review Date (Revised): May 20, 2014 Effective Date: October 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): October 1, 2014 Most Recent Review Date (Revised): May 20, 2014 Effective Date: October 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Adenosine in idiopathic AV block, 445 446 Adolescent(s) syncope in, 397 409. See also Syncope, in children and adolescents AECG monitoring.
Index Note: Page numbers of article titles are in boldface type. A Adenosine in idiopathic AV block, 445 446 Adolescent(s) syncope in, 397 409. See also Syncope, in children and adolescents AECG monitoring.
Informed Consent Columbia Whole Genome or Whole Exome Sequencing
 Informed Consent Columbia Whole Genome or Whole Exome Sequencing Please read the following form carefully and discuss with your ordering physician before signing consent. This consent is intended for the
Informed Consent Columbia Whole Genome or Whole Exome Sequencing Please read the following form carefully and discuss with your ordering physician before signing consent. This consent is intended for the
Genetic Testing for Heredity Cardiac Disease
 Clinical Appropriateness Guidelines Genetic Testing for Heredity Cardiac Disease EFFECTIVE DECEMBER 1, 2017 Appropriate.Safe.Affordable 2017 AIM Specialty Health 2064-1217 Table of Contents Scope... 3
Clinical Appropriateness Guidelines Genetic Testing for Heredity Cardiac Disease EFFECTIVE DECEMBER 1, 2017 Appropriate.Safe.Affordable 2017 AIM Specialty Health 2064-1217 Table of Contents Scope... 3
Genetic Testing for Cardiac Ion Channelopathies
 Genetic Testing for Cardiac Ion Channelopathies Policy Number: 2.04.43 Last Review: 11/2018 Origination: 6/2007 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Genetic Testing for Cardiac Ion Channelopathies Policy Number: 2.04.43 Last Review: 11/2018 Origination: 6/2007 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Pre-Participation Athletic Cardiac Screening
 Pre-Participation Athletic Cardiac Screening Kimberly A Krabill, MD Pediatric and Fetal Cardiologist Northwest Congenital Heart Care, Division of MedNax Cardiology Update for Primary Care Symposium July
Pre-Participation Athletic Cardiac Screening Kimberly A Krabill, MD Pediatric and Fetal Cardiologist Northwest Congenital Heart Care, Division of MedNax Cardiology Update for Primary Care Symposium July
Pharmacogenomics of Drug-Induced Conditions
 Pharmacogenomics of Drug-Induced Conditions Dan M. Roden, M.D. Professor of Medicine and Pharmacology Director, Oates Institute for Experimental Therapeutics Assistant Vice-Chancellor for Personalized
Pharmacogenomics of Drug-Induced Conditions Dan M. Roden, M.D. Professor of Medicine and Pharmacology Director, Oates Institute for Experimental Therapeutics Assistant Vice-Chancellor for Personalized
Cardiac MRI: Clinical Application to Disease
 Cardiac MRI: Clinical Application to Disease Stacy Rissing, MD! Cardiothoracic imaging, Indiana University! Outline Imaging planes Disease findings Pulse sequences used for each indication Pathophysiology
Cardiac MRI: Clinical Application to Disease Stacy Rissing, MD! Cardiothoracic imaging, Indiana University! Outline Imaging planes Disease findings Pulse sequences used for each indication Pathophysiology
The Role of Defibrillator Therapy in Genetic Arrhythmia Syndromes
 The Role of Defibrillator Therapy in Genetic Arrhythmia Syndromes RHEA C. PIMENTEL, MD, FACC, FHRS UNIVERSITY OF KANSAS HOSPITAL MID AMERICA CARDIOLOGY AUGUST 19, 2012 Monogenic Arrhythmia Syndromes Mendelian
The Role of Defibrillator Therapy in Genetic Arrhythmia Syndromes RHEA C. PIMENTEL, MD, FACC, FHRS UNIVERSITY OF KANSAS HOSPITAL MID AMERICA CARDIOLOGY AUGUST 19, 2012 Monogenic Arrhythmia Syndromes Mendelian
Plotse hartdood & genetica
 Onder spanning inspannen Utrecht, 17 April 2018 Plotse hartdood & genetica N. Hofman, PhD Academic Medical Centre Amsterdam, the Netherlands European Reference Network Network of centres in Europe sharing
Onder spanning inspannen Utrecht, 17 April 2018 Plotse hartdood & genetica N. Hofman, PhD Academic Medical Centre Amsterdam, the Netherlands European Reference Network Network of centres in Europe sharing
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Basics of Structure/Function of Sodium and Potassium Channels Barry London, MD PhD
 Basics of Structure/Function of Sodium and Potassium Channels Barry London, MD PhD University of Pittsburgh Medical Center Pittsburgh, PA International Symposium of Inherited Arrhythmia Disorders and Hypertrophic
Basics of Structure/Function of Sodium and Potassium Channels Barry London, MD PhD University of Pittsburgh Medical Center Pittsburgh, PA International Symposium of Inherited Arrhythmia Disorders and Hypertrophic
Sudden cardiac death (SCD) accounts for 20% of mortality. Sudden Cardiac Death Compendium. Genetics of Sudden Cardiac Death
 Sudden Cardiac Death Compendium Circulation Research Compendium on Sudden Cardiac Death The Spectrum of Epidemiology Underlying Sudden Cardiac Death Sudden Cardiac Death Risk Stratification Genetics of
Sudden Cardiac Death Compendium Circulation Research Compendium on Sudden Cardiac Death The Spectrum of Epidemiology Underlying Sudden Cardiac Death Sudden Cardiac Death Risk Stratification Genetics of
Genetics of Atrial Fibrillation: does it help in treatment decisions?
 Genetics of Atrial Fibrillation: does it help in treatment decisions? Atrial fibrillation Pathophysiology of atrial fibrillation (AF) Genetic loci identified for AF Role in therapy outcome ardiologie Molecular
Genetics of Atrial Fibrillation: does it help in treatment decisions? Atrial fibrillation Pathophysiology of atrial fibrillation (AF) Genetic loci identified for AF Role in therapy outcome ardiologie Molecular
Sudden cardiac death (SCD) is a leading cause of mortality
 Sudden Unexplained Nocturnal Death Syndrome: The Hundred Years Enigma Jingjing Zheng, MD; Da Zheng, MD; Terry Su, MD; Jianding Cheng, MD, PhD Sudden cardiac death (SCD) is a leading cause of mortality
Sudden Unexplained Nocturnal Death Syndrome: The Hundred Years Enigma Jingjing Zheng, MD; Da Zheng, MD; Terry Su, MD; Jianding Cheng, MD, PhD Sudden cardiac death (SCD) is a leading cause of mortality
Risk Factors for Sudden cardiac Death
 Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
Index. cardiacep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A AEDs. See Automated external defibrillators (AEDs) AF. See Atrial fibrillation (AF) Age as factor in SD in marathon runners, 45 Antiarrhythmic
Note: Page numbers of article titles are in boldface type. A AEDs. See Automated external defibrillators (AEDs) AF. See Atrial fibrillation (AF) Age as factor in SD in marathon runners, 45 Antiarrhythmic
Familial DilatedCardiomyopathy Georgios K Efthimiadis, MD
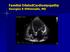 Familial DilatedCardiomyopathy Georgios K Efthimiadis, MD Dilated Cardiomyopathy Dilated LV/RV, reduced EF, in the absence of CAD valvulopathy pericardial disease Prevalence:40/100.000 persons Natural
Familial DilatedCardiomyopathy Georgios K Efthimiadis, MD Dilated Cardiomyopathy Dilated LV/RV, reduced EF, in the absence of CAD valvulopathy pericardial disease Prevalence:40/100.000 persons Natural
Rhythm and Blues Drugs and QT Prolongation
 Rhythm and Blues Drugs and QT Prolongation Dr Martin Quinn St Vincents University Hospital Irish Medication Safety Network conference Farmleigh 18 Oct 2013 Drugs and QT Prolongation Anti-psychotic, antidepressant,
Rhythm and Blues Drugs and QT Prolongation Dr Martin Quinn St Vincents University Hospital Irish Medication Safety Network conference Farmleigh 18 Oct 2013 Drugs and QT Prolongation Anti-psychotic, antidepressant,
UKGTN Testing Criteria
 Test name: Epilepsy 53 Gene Panel UKGTN Testing Criteria Approved name and symbol of disorder/condition(s): Epilepsy Panel Test See Appendix 1 Approved name and symbol of gene(s): See Appendix 2 OMIM number(s):
Test name: Epilepsy 53 Gene Panel UKGTN Testing Criteria Approved name and symbol of disorder/condition(s): Epilepsy Panel Test See Appendix 1 Approved name and symbol of gene(s): See Appendix 2 OMIM number(s):
Integration of Next-Generation Sequencing into Epilepsy Clinical Care. Michelle Demos University of British Columbia BC Children s Hospital
 Integration of Next-Generation Sequencing into Epilepsy Clinical Care Michelle Demos University of British Columbia BC Children s Hospital No Disclosures Learning Objectives To review: the impact of using
Integration of Next-Generation Sequencing into Epilepsy Clinical Care Michelle Demos University of British Columbia BC Children s Hospital No Disclosures Learning Objectives To review: the impact of using
MI Acute occlusion of the proximal left anterior descending (LAD) artery is the cause of 40% to 50% of all MIs. *
 MI *33% -50% die before hospital lethal arrhythmia Sudden Cardiac Death. * Arrhythmias are caused by electrical abnormalities of the ischemic myocardium and conduction system. *Acute occlusion of the proximal
MI *33% -50% die before hospital lethal arrhythmia Sudden Cardiac Death. * Arrhythmias are caused by electrical abnormalities of the ischemic myocardium and conduction system. *Acute occlusion of the proximal
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Genetic Testing for Dilated Cardiomyopathy. Description
 Subject: Genetic Testing for Dilated Cardiomyopathy Page: 1 of 12 Last Review Status/Date: March 2015 Genetic Testing for Dilated Cardiomyopathy Description Dilated cardiomyopathy (DCM) is characterized
Subject: Genetic Testing for Dilated Cardiomyopathy Page: 1 of 12 Last Review Status/Date: March 2015 Genetic Testing for Dilated Cardiomyopathy Description Dilated cardiomyopathy (DCM) is characterized
Managing Hypertrophic Cardiomyopathy with Imaging. Gisela C. Mueller University of Michigan Department of Radiology
 Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
EVALUATION OF THE ATHLETE. Karen Stout, MD Professor, Medicine and Pediatrics University of Washington
 EVALUATION OF THE 12 ATHLETE Karen Stout, MD Professor, Medicine and Pediatrics University of Washington NO DISCLOSURES OUTLINE Why evaluate athletes? What s the problem? What evaluation should be done?
EVALUATION OF THE 12 ATHLETE Karen Stout, MD Professor, Medicine and Pediatrics University of Washington NO DISCLOSURES OUTLINE Why evaluate athletes? What s the problem? What evaluation should be done?
Cardiac MRI: Cardiomyopathy
 Cardiac MRI: Cardiomyopathy Laura E. Heyneman, MD I do not have any relevant financial relationships with any commercial interests Cardiac MRI: Cardiomyopathy Laura E. Heyneman, MD Duke University Medical
Cardiac MRI: Cardiomyopathy Laura E. Heyneman, MD I do not have any relevant financial relationships with any commercial interests Cardiac MRI: Cardiomyopathy Laura E. Heyneman, MD Duke University Medical
Aerobic Exercise Screening Stratification Tool
 Aerobic Screening Stratification Tool Disclaimer: The Aerobics Screening Stratification Tool is a working document currently used within the Stroke Rehabilitation Service of St. Joseph s Care Group- Thunder
Aerobic Screening Stratification Tool Disclaimer: The Aerobics Screening Stratification Tool is a working document currently used within the Stroke Rehabilitation Service of St. Joseph s Care Group- Thunder
What is New in CPVT? Diagnosis Genetics Arrhythmia Mechanism Treatment. Andreas Pflaumer
 What is New in CPVT? Diagnosis Genetics Arrhythmia Mechanism Treatment Andreas Pflaumer Diagnosis of CPVT Induction of different types of VES or VT by exercise or catecholamines AND exclusion of of other
What is New in CPVT? Diagnosis Genetics Arrhythmia Mechanism Treatment Andreas Pflaumer Diagnosis of CPVT Induction of different types of VES or VT by exercise or catecholamines AND exclusion of of other
