Paediatric Neurology RCPCH. Level 3 Paediatrics Sub-Specialty Syllabus. Paediatric curriculum for excellence
|
|
|
- Anna Byrd
- 6 years ago
- Views:
Transcription
1 RCPCH Progress Paediatric curriculum for excellence Paediatric Neurology Level 3 Paediatrics Sub-Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College of Paediatrics and Child Health is a registered charity in England and Wales (105774) and in Scotland (SCO38299) RCPCH Royal College of Paediatrics and Child Health
2 This document outlines the syllabus to be used by doctors completing completing Level 3 Neurology training in the United Kingdom training in the United Kingdom (UK). It accompanies the RCPCH Progress curriculum and assessment strategy. Introduction This is Version 1.0. As the document is updated, version numbers will be changed, and content changes noted in the table below. Version number Date issued Summary of changes This syllabus supports the completion of the RCPCH Progress curriculum, and should be used in conjunction with the curriculum document. The purpose of the curriculum is to train doctors to acquire a detailed knowledge and understanding of health and illness in babies, children and young people. The curriculum provides a framework for training, articulating the standard required to work at Consultant level, and at key progression points during their training, as well as encouraging the pursuit of excellence in all aspects of clinical and wider practice. The curriculum comprises of Learning Outcomes which specify the standard that trainees must demonstrate as they progress through training and ultimately attain a Certificate of Completion of Training (CCT). The syllabi support the curriculum by providing further instructions and guidance as to how the Learning Outcomes can be achieved and demonstrated. Using the Syllabus Paediatric trainees are required to demonstrate achievement of generic and sub-specialty or General Paediatric Learning Outcomes throughout their training period. For all level 1 and level 2 trainees, there are 11 generic paediatric Learning Outcomes for each level. At level 3, there are a further 11 generic paediatric Learning Outcomes for all trainees, and several additional Learning Outcomes in either General Paediatrics or the GRID sub-specialty the trainee has been appointed into. This syllabus contains 5 interlinked elements, as outlined in figure 1 which illustrates how each element elaborates on the previous one. This information is correct and up to date at time of Publication. RCPCH
3 Elements of the Syllabus The Introductory Statement sets the scene for what makes a General Paediatrician. The Learning Outcomes are stated at the beginning of each section. These are the outcomes which the trainee must demonstrate they have met to be awarded their Certificate of Completion of Training (CCT) in Paediatrics. Progress towards achievement of the Learning Outcomes is reviewed annually at the Annual Review of Competence Progression (ARCP). Each Learning Outcome is mapped to the General Medical Council (GMC) Generic Professional Capabilities framework. Each trainee must achieve all the Generic Professional Capabilities to meet the minimum regulatory standards for satisfactory completion of training. Using the Syllabus with eportfolio Recording evidence in the eportfolio to demonstrate progression against the learning outcomes and key capabilities can be done from any assessment or event in the eportfolio. At the end of any event or assessment, there is an opportunity to add tags, documents and comments. Expanding this by clicking show more will enable you to link your assessment to the curriculum items, where you will find the learning outcomes for each domain, key capabilities and example illustrations. Trainees will therefore be able to track their progress in fulfilling the mandatory learning outcomes and key capabilities. The are mandatory capabilities which must be evidenced by the trainee, in their eportfolio, to meet the Learning Outcome. are therefore also mapped to the GMC Generic Professional Capabilities framework. The are examples of evidence and give the range of clinical contexts that the trainee may use to support their achievement of the. These are intended to provide a prompt to the trainee and trainer as to how the overall outcomes might be achieved. They are not intended to be exhaustive, and excellent trainees may produce a broader portfolio or include evidence that demonstrates deeper learning. It is not expected that trainees provide eportfolio evidence against every individual illustration (or a set quota); the aim of assessment is to provide evidence against every Key Capability. The Assessment Grid indicates suggested assessment methods, which may be used to demonstrate the. Trainees may use differing assessment methods to demonstrate each capability (as indicated in each Assessment Grid), but there must be evidence of the trainee having achieved all. Introductory Statement Learning Outcomes Assessment Grid Figure 1: The 5 elements of the syllabus 4 5
4 Paediatric Neurology Introductory Statement Sub-specialty Learning Outcomes Introductory Statement A Paediatric Neurologist is a doctor who has knowledge and understanding of disorders of the nervous system that affect infants, children and young people. They need to have expertise in conditions including; the epilepsies, movement disorders, cerebrovascular disease, neuromuscular disorders, neuro-genetic, inflammatory and demyelinating disorders, neonatal neurology, acquired brain injury and neurorehabilitation. There is an increasing range of neurological disorders that are amenable to more effective and innovative management and personalised medicine approaches. In addition, Paediatric Neurologists have generic expertise in neuroimaging, genetics (molecular) medicine and neurosurgical disorders. Some will sub-specialise and work largely or exclusively in this field. Paediatric Neurologists are usually based in a regional neuroscience centre providing tertiary and secondary level services working in out-patient and hospital settings. In the acute setting they manage a wide spectrum of disorders and provide shared care management of patients on Paediatric Intensive Care Units (PICU), Neonatal Intensive Care Units (NICU) and those undergoing neurosurgery. They provide specialist support advice to paediatric specialty colleagues. They advise on diagnosis and ongoing management of chronic and complex disease. Paediatric Neurologists work particularly closely with Neurodisability paediatricians, Neurosurgeons, Neurophysiologists, Neuropsychiatrists, Neuroradiologists and Neurogeneticists. Specialty Learning Outcomes 1. Recognises, assesses and manages the full range of paediatric neurological conditions, including acute neurological disorders with common and uncommon presentations, anticipating possible pitfalls and complications, while recognising and managing high-risk situations. 2. Coordinates urgent and complex clinical management, including the provision of non-acute clinic services and ward-based neurogenetic, neuroradiological or neurophysiological multidisciplinary meetings; completes appropriate onward referrals and discharges; and communicates clearly with colleagues. 3. Promotes the neurological and developmental health of a child with a neurological disorder. 4. Assumes the role of paediatric neurological team leader and takes responsibility for this area of service. 5. Practises safe child neurology, including when prescribing medication, and initiates and completes a quality improvement project applicable to child neurology. 6. Keeps up to date and engages in, supports and stimulates research in child neurology. GMC Generic Professional Capabilities GPC 1, 3, 4, 5 GPC 1, 3, 4, 5 GPC 1, 4, 5, 6, 7, 8, 9 GPC 1, 5, 6, 8 GPC 1, 5, 6, 9 GPC 9 6 7
5 Specialty Learning Outcome 1 Recognises, assesses and manages the full range of paediatric neurological conditions, including acute neurological disorders with common and uncommon presentations, anticipating possible pitfalls and complications, while recognising and managing high-risk situations. Assesses and manages children presenting with acute and sub-acute neurological emergencies from birth through to adulthood, including chronic developmental disorders and age-specific neurological syndromes, through the application of the understanding of neurogenetic, neuroradiological and neurophysiological techniques, in relation to: Epilepsies in the newborn, infancy, childhood and adolescence Neonatal neurology Cerebrovascular disorders Neuromuscular disorders Inflammatory and demyelinating disorders Neurodegenerative and neurometabolic disorders Movement disorders, including cerebral palsy Neuropsychiatric and neuropsychological disorders, and medically unexplained neurological syndromes Neurorehabilitation and acquired brain injury Headaches and disorders of raised intracranial pressure Neuro-oncology Carries out a wide range of routine, complex and challenging paediatric neurological assessments and investigations appropriately and consistently, based on the history and examination, the probability, costs and the risk benefit ratio. GPC 1, 3, 4, 5 GPC 1, 3, 5, 7 GPC 1, 3, 4, 5, 6, 7 1. Recognises acutely presenting neurological disorders e.g. encephalopathy, paralysis, seizures (including status epilepticus and status dystonicus), central nervous system (CNS) infection, traumatic brain injury, stroke and raised intracranial pressure. 2. Investigates and manages a wide range of childhood neurological disorders, including genetic and developmental malformations of the nervous system from neurometabolic, neurodegenerative, vascular, neuroinflammatory, toxic and traumatic causes. 3. Recognises the neurological disorders that may present with a critical illness and require ICU management, and the neurological complications that may occur in patients admitted to ICU with non-neurological disorders. 4. Demonstrates understanding of normal neurological development patterns and their variants. 5. Demonstrates skills in the assessment of a child with a possible movement disorder. Recognises normal variants and differential diagnoses in infants, children and young people and formulates strategies for investigation and management. 6. Constructs clear management strategies for a child with a complex movement disorder, including relevant potential medical, surgical, physical and psychological therapies. 7. Demonstrates an understanding of the impact of associated learning and behavioural problems in a child with a neurological disorder. 8. Liaises effectively with hospital and community specialist teams who manage paediatric neurology. 9. Is conversant with the following essential specialty branches of children s neurosciences: Neurogenetics Neuroradiology Neurophysiology Headache and disorders of raised intracranial pressure Acute brain and spinal injury Epilepsies in the newborn, infancy, childhood and adolescence Neonatal neurology Cerebrovascular disorders Neuromuscular disorders Neurodegenerative and neurometabolic disorders Movement disorders, including cerebral palsy Neuropsychiatric and neuropsychological disorders, and medically unexplained syndromes Neurorehabilitation, including after acquired brain and spinal injury Neuro-oncology 8 9
6 10. Recognises the common false positive results of investigations in a healthy child that may present to a neurologist, e.g. imaging, biochemical investigations, electroencephalography (EEG), electroretinography (ERG), visual evoked potentials (VEP), brainstem auditory evoked potentials (BAEP), somatosensory evoked potential (SSEP), central motor conduction time (CMCT), electromyography (EMG), nerve conduction velocity (NCV), single-fibre electromyography (SFEMG), and other neurophysiological techniques. 11. Recognises disorders which require neurosurgical management and evaluates the suitability for surgical treatment, in collaboration with neurosurgical colleagues. 12. Demonstrates understanding of the peri-operative management of children undergoing neurosurgical procedures and the diagnosis and management of common complications. 13. Investigates and manages a child on the ICU following cardiac arrest or severe hypoxic ischaemic encephalopathy (e.g. near drowning) and is capable of conducting and interpreting brainstem death testing. 14. Recognises the clinical features, and has knowledge of the investigation and management of children with CNS tumours, including the late effects of treatment. 15. Supports the neurological management of a child with a posterior fossa tumour. Demonstrates knowledge of the risks of surgery, the management of complications including posterior fossa syndrome and neurorehabilitation goals. 16. Demonstrates knowledge of the international classification of headache disorders in children and applies it to support diagnosis and management in the outpatient setting. 17. Recognises the clinical features, and has knowledge of the investigation and management of neurological disorders typically presenting in adults but that may occur in children or young adults, e.g. multiple sclerosis (MS), parkinsonism, amyotrophic lateral sclerosis (ALS), and paraneoplastic disorders. 18. Recognises the symptoms and signs of inherited white matter disorders and is familiar with their magnetic resonance imaging (MRI) characteristics and classification. 19. Demonstrates understanding of the potential results of whole genome sequencing and discusses these with families, including the relevance of polymorphisms, variants of unknown significance, and likely pathogenic mutations 21. Demonstrates knowledge of potential management therapies in development for neurological disorders, for example: Immunomodulation for acute and chronic neuroinflammatory disorders Gene therapies, relevant therapeutic research studies and treatment programmes for neuromuscular disorders, such as spinal muscular atrophy and Duchenne muscular dystrophy Deep brain stimulation for movement disorders Acute stroke management in childhood 22. Recognises the complications of acute spinal cord injury and is familiar with their management, including autonomic dysfunction, neuropathic bladder and bowel disorders. 23. Recognises and manages neuropathic bladder and bowel disorders to prevent complications (e.g. chronic renal failure associated with a neuropathic bladder), by establishing a programme of clean intermittent catheterisation. 24. Describes the role of neurogenetics in patient stratification, precision medicine and counselling for management and treatment options (e.g. specific medication known to benefit specific neurogenetic conditions), opting to employ neurosurgical techniques for intractable epilepsy. 25. Differentiates between the epilepsies, movement disorders and parasomnias. 26. Confidently manages children with a wide range of childhood epilepsies and can discuss the risks and benefits of specific antiepileptic drug treatments. Recognises the role of non-pharmacological treatments such as the ketogenic diet and vagal nerve stimulation and the criteria for referral for epilepsy surgery. 27. Evaluates and manages children with sleep disorders, e.g. night terrors, sleep-disordered breathing, nocturnal epilepsies, narcolepsy and restless legs syndrome (RLS). 28. Evaluates a teenager with medically unexplained symptoms by discriminating functional and organic symptoms and signs. Discusses the likely diagnosis with the young person and their family and formulates a strategy for management involving the multidisciplinary team (MDT) 20. Coordinates the care of a young adult with Duchenne muscular dystrophy transitioning to adult services. Understands the risk of associated health problems and strategies for their management, including respiratory, cardiac and postural management. Formulates an individual care plan to support emotional, social and physical well-being
7 Specialty Learning Outcome 2 Coordinates urgent and complex clinical management, including the provision of non-acute clinic services and ward-based neurogenetic, neuroradiological or neurophysiological multidisciplinary meetings; completes appropriate onward referrals and discharges; and communicates clearly with colleagues. Considers the full range of treatment and management options available, including new and innovative therapies, relevant to paediatric neurology. Demonstrates skills in the management of all aspects of acute neurological disorders presenting to district general and regional centres. Recognises when management is required in a regional neuroscience unit, paediatric intensive care or a high dependency unit (HDU) setting, e.g. status epilepticus; status dystonicus, chorea and myoclonus; coma and acute disturbances of consciousness; traumatic brain injury; childhood stroke, metabolic and immune-mediated neuroinflammatory encephalopathy and infectious causes of encephalitis. Coordinates, supervises and performs urgent or complex clinical management, including the provision of non-acute clinic services and multidisciplinary meetings (e.g. ward-based multidisciplinary team [MDT], neurogenetics MDT, neuroradiology MDT, and neurophysiology MDT meetings). Completes appropriate onward referrals and discharges, and communicate clearly with colleagues. Describes and utilises genetic investigations in the diagnosis of neurological disorders, including knowledge of how to utilise and interpret the results of next generation sequencing (NGS), and utilises and interprets neuroradiological and neurophysiological investigations in the assessment and ongoing management of children with neurological and neurosurgical disorders. GPC 1, 3, 4, 5 GPC 3, 5 GPC 1, 3, 4, 5, 6, 7 GPC 1, 3, 5, 6, 7 GPC 1, 3, 5, 6, 7 1. Assesses indication(s) for urgent or elective neuroimaging with and without general anaesthesia and obtains informed consent for the procedure in discussion with clinical colleagues. 2. Determines indication for an EEG with and without sleep in the urgent or elective clinical setting, in discussion with clinical colleagues. 3. Evaluates indications for EEG video telemetry (VT) and the relative urgencies. 4. Considers the role of neurogenetic testing in the provision of personalised neurological management and counselling, in discussion with clinical colleagues. 5. Applies knowledge of anaesthetic, cardiac and respiratory risks for specific neurological disorders. 6. Interprets normal and abnormal intracranial pressure recordings and has knowledge of the factors that influence it. 7. Requests, interprets, acts on and communicates the significance of normal and abnormal neuroimaging within a multidisciplinary setting, including neurosurgical emergencies requiring emergency and out-of-hours neuroimaging interpretation. 8. Requests, interprets, acts on and communicates the results of neurophysiological investigations such as EEG, sleep EEG, video telemetry, electromyography, nerve conduction studies (NCS), electroretinography, visual evoked potentials, brainstem auditory evoked potentials, somatosensory evoked potential, central motor conduction time, transcranial magnetic stimulation (TMS), and transcranial direct current stimulation (tdcs). 9. Recognises the multisystem nature of many of the neurological disorders. 10. Demonstrates understanding of the pathophysiology, presentation, diagnosis, management, prognosis and outcome of neurological disorders including those outlined in other specialty programmes, e.g. neurological complications of cardiac, renal, haematological, endocrine, ENT, rheumatological, infectious, endocrine and dermatological diseases. Explains the role of neuroimaging in the clinical diagnostic and management plan. GPC 5 Describes the role of neurophysiological investigations in the clinical diagnostic and management plan. GPC
8 Specialty Learning Outcome 3 Specialty Learning Outcome 4 Promotes the neurological and developmental health of a child with a neurological disorder. GPC 1, 4, 5, 6, 7, 8, 9 Assumes the role of paediatric neurological team leader and takes responsibility for this area of service. GPC 1, 5, 6, 8 Demonstrates understanding of the impact of having a disabled child in the family, including those with life-limiting disorders. Leads multidisciplinary discussions and coordinates multi-professional care for, and management of, children with neurological disorders. GPC 3, 4 Leads an MDT and applies communication skills in a range of environments and situations with children, young people and families in challenging circumstances, and communicates effectively with external agencies, including when authorising legal documents and child protection reports. GPC 3, 5, 7 Identifies and manages risks of safeguarding issues in children with complex neurological disorders, including those relating to child, family and wider society. GPC 3, 4, 7 Performs the full range of clinical investigations and procedures relevant to forming a diagnosis in paediatric neurology, including appropriately coordinating the skills of other health professionals when required. GPC 3 Anticipates the need for transition from paediatric services to adult services and plans accordingly. GPC 1, 4, 5 1. Applies interventions to prevent blindness through appropriate management and surveillance of hydrocephalus and other causes of raised intracranial pressure in collaboration with ophthalmic, neuroradiological and neurosurgical colleagues 2. Recognises the multisystem nature of many of the neurological disorders. 3. Ensures immunisations are up to date in children with long-standing neurological disorders, and in siblings of children with neurological disorders 1. Takes the lead in coordinating a regional case review and strategy planning meeting for a child following acute brain injury secondary to encephalitis. 2. Provides sub-specialist input into the MDT in the assessment, investigation and management of a child with a possible inflicted head and/or spinal injury. 3. Identifies factitious neurological diseases e.g. salt poisoning, medication overdose or non-compliance. 4. Coordinates an MDT meeting between paediatric intensive care, palliative care services, and family or carers regarding withdrawal of care. 5. Liaises effectively with the regional hospital and community specialist teams to ensure safety and timely assessment for children with a range of neurological disorders. 6. Liaises with other professionals to organise specialist investigations in another institution, e.g. positron emission tomography (PET) imaging for complex epilepsy. 7. Contributes to a national patient group meeting for a patient with a rare disease
9 Specialty Learning Outcome 5 Specialty Learning Outcome 6 Practises safe child neurology, including when prescribing medication, and initiates and completes a quality improvement project applicable to child neurology. GPC 1, 5, 6, 9 Keeps up to date and engages in, supports and stimulates research in child neurology. GPC 9 Takes responsibility for investigating, reporting and resolving risks to patients, including communication with patients and families or carers. Evaluates safety mechanisms across a range of healthcare settings, applying a reflective approach to self and team performance. Identifies quality improvement opportunities, supervises healthcare professionals in relation to improvement projects, and leads and facilitates reflective evaluation. GPC 5, 6 GPC 6 Demonstrates independent development and revision of guidelines and procedures to improve service delivery, centred around current clinical research and evidence-based healthcare. 1. Completes a higher degree qualification, e.g. MSc or PhD. 2. Publishes in a peer-reviewed journal. GPC 9 1. Effectively manages and coordinates patient flow, staffing, safety and quality in the context of a busy paediatric neurology department. 3. Participates in a clinical trial. 4. Participates in a British Paediatric Neurology Association (BPNA) National Clinical Research Network project to implement a guideline, undertake an audit, participate in a Delphi exercise, or estimate the incidence of a disease or condition. 2. Demonstrates participation in a serious case review. 3. Participates in regular mortality meetings, e.g. for a child who has experienced sudden unexpected death in epilepsy (SUDEP). 4. Initiates a quality improvement project for routine investigations, e.g. a survey of cost-effectiveness, or how the results influence management or cause inconvenience or harm
10 Assessment Grid Assessment / Supervised Learning Event suggestions This table suggests assessment tools which may be used to assess the for these Learning Outcomes. This is not an exhaustive list, and trainees are permitted to use other methods within the RCPCH Assessment Strategy to demonstrate achievement of the Learning Outcome, where they can demonstrate these are suitable. (epaed Mini-CEX) Paediatric Mini Clinical Evaluation Paediatric Case-based Discussion(ePaed CbD) Directly Observed Procedure / Assessment of Performance (DOP/ Acute Care Assessment Tool (ACAT) Discussion of Correspondence (DOC) Clinical Leadership Assessment Skills (LEADER) Handover Assessment Tool (HAT) Paediatric Multi Source Feedback (epaed MSF) Paediatric Carers for Children Feedback (Paed CCF) Other Paediatric Mini Clinical Evaluation (epaed Mini-CEX) Paediatric Case-based Discussion(ePaed CbD) Assessment / Supervised Learning Event suggestions AoP) Assessment of Performance (DOP/ Directly Observed Procedure / Discussion of Correspondence (DOC) Acute Care Assessment Tool (ACAT) Handover Assessment Tool (HAT) Clinical Leadership Assessment Skills (LEADER) Paediatric Multi Source Feedback (epaed MSF) Paediatric Carers for Children Feedback (Paed CCF) Other Explains and utilises genetic investigations in the diagnosis of neurological disorders, including knowledge of how to utilise and interpret the results of next generation sequencing (NGS), and utilises and interprets neuroradiological and neurophysiological investigations in the assessment and ongoing management of children with neurological and neurosurgical disorders. Describes the role of neuroimaging in the clinical diagnostic and management plan. Carries out a wide range of routine, complex and challenging paediatric neurological assessments and investigations appropriately and consistently, based on the history and examination, the probability, costs and the risk benefit ratio. Considers the full range of treatment and management options available, including new and innovative therapies, relevant to paediatric neurology. Describes the role of neurophysiological investigations in the clinical diagnostic and management plan. Demonstrates understanding of the impact of having a disabled child in the family, including those with life-limiting disorders. Leads multidisciplinary discussions and coordinates multiprofessional care for, and management of, children with neurological disorders. Identifies and manages risks of safeguarding Demonstrates skills in the management of all aspects of acute neurological disorders presenting to district general and regional centres. Recognises when management is required in a regional neuroscience unit, paediatric intensive care or a high dependency unit (HDU) setting, e.g. status epilepticus; status dystonicus, chorea and myoclonus; coma and acute disturbances of consciousness; traumatic brain injury; childhood stroke, metabolic and immune-mediated neuroinflammatory encephalopathy and infectious causes of encephalitis. Coordinates, supervises and performs urgent or complex clinical management, including the provision of non-acute clinic services and multidisciplinary meetings (e.g. ward-based multidisciplinary team [MDT], neurogenetics MDT, neuroradiology MDT, and neurophysiology MDT meetings). Completes appropriate onward referrals and discharges, and communicate clearly with colleagues. issues in children with complex neurological disorders, including those relating to child, family and wider society. Leads an MDT and applies communication skills in a range of environments and situations with children, young people and families in challenging circumstances, and communicates effectively with external agencies, including when authorising legal documents and child protection reports. Performs the full range of clinical investigations and procedures relevant to forming a diagnosis in paediatric neurology, including appropriately coordinating the skills of other health professionals when required. Anticipates the need for transition from paediatric services to adult services and plans accordingly
11 Assessment / Supervised Learning Event suggestions Other Paediatric Carers for Children Feedback (Paed CCF) Paediatric Multi Source Feedback (epaed MSF) Handover Assessment Tool (HAT) Clinical Leadership Assessment Skills (LEADER) Discussion of Correspondence (DOC) Acute Care Assessment Tool (ACAT) Directly Observed Procedure / Assessment of Performance (DOP/ AoP) Paediatric Case-based Discussion(ePaed CbD) Paediatric Mini Clinical Evaluation (epaed Mini-CEX) Assesses and manages children presenting with acute and sub-acute neurological emergencies from birth through to adulthood, including chronic developmental disorders and developmentally age-specific neurological syndromes, through the application of the understanding of neurogenetic, neuroradiological and neurophysiological techniques, in relation to epilepsies in the newborn, infancy, childhood and adolescence, neonatal neurology, cerebrovascular disorders, neuromuscular disorders, Inflammatory and demyelinating disorders, neurodegenerative and neurometabolic disorders, movement disorders (including cerebral palsy), neuropsychiatric and neuropsychological disorders, and medically unexplained neurological syndromes, neurorehabilitation and acquired brain injury, headaches and disorders of raised intracranial pressure, neuro-oncology. Takes responsibility for investigating, reporting and resolving risks to patients, including communication with patients and families or carers. Evaluates safety mechanisms across a range of healthcare settings, applying a reflective approach to self and team performance. Identifies quality improvement opportunities, supervises healthcare professionals in relation to improvement projects, and leads and facilitates reflective evaluation. Demonstrates independent development and revision of guidelines and procedures to improve service delivery, centred around current clinical research and evidence-based healthcare
12 RCPCH Progress: Paediatric Neurology Level 3 Syllabus This information is correct and up to date at time of Publication. RCPCH 2017
General Paediatrics Syllabus
 RCPCH Progress Paediatric curriculum for excellence General Paediatrics Syllabus Level 3 Paediatrics Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
RCPCH Progress Paediatric curriculum for excellence General Paediatrics Syllabus Level 3 Paediatrics Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
Paediatric Respiratory Medicine
 RCPCH Progress Paediatric curriculum for excellence Paediatric Respiratory Medicine Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The
RCPCH Progress Paediatric curriculum for excellence Paediatric Respiratory Medicine Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The
A Framework of Competences for Special Interest Module in Paediatric Epilepsies
 A Framework of Competences for Special Interest Module in Paediatric Epilepsies 2 Section 1 CONTENTS Introduction 5 Section 2 Specific Competences in Paediatric Epilepsies 7 Knowledge and Understanding
A Framework of Competences for Special Interest Module in Paediatric Epilepsies 2 Section 1 CONTENTS Introduction 5 Section 2 Specific Competences in Paediatric Epilepsies 7 Knowledge and Understanding
Criteria for Registering as Paediatric Neurologist in Malaysia
 Criteria for Registering as Paediatric Neurologist in Malaysia A doctor can request to be registered as a paediatric neurologist if he/she fulfils ALL the following requirements: 1 A recognised basic medical
Criteria for Registering as Paediatric Neurologist in Malaysia A doctor can request to be registered as a paediatric neurologist if he/she fulfils ALL the following requirements: 1 A recognised basic medical
Paediatric Nephrology
 RCPCH Progress Paediatric curriculum for excellence Paediatric Nephrology Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
RCPCH Progress Paediatric curriculum for excellence Paediatric Nephrology Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
Criteria for Registering as a Developmental Paediatrician
 Criteria for Registering as a Developmental Paediatrician A doctor can apply to be registered as a Developmental Paediatrician if he/she fulfils ALL the following requirements: 1 A recognised basic medical
Criteria for Registering as a Developmental Paediatrician A doctor can apply to be registered as a Developmental Paediatrician if he/she fulfils ALL the following requirements: 1 A recognised basic medical
A Framework of Competences for the Level 3 Training Special Interest Module in Paediatric Neurodisability
 A Framework of Competences for the Level 3 Training Special Interest Module in Paediatric Neurodisability Feb 2010 Royal College of Paediatrics and Child Health www.rcpch.ac.uk CONTENTS Section 1 Introduction
A Framework of Competences for the Level 3 Training Special Interest Module in Paediatric Neurodisability Feb 2010 Royal College of Paediatrics and Child Health www.rcpch.ac.uk CONTENTS Section 1 Introduction
Paediatric Neurology Training Guide
 Version 1 2018 Background Guidance for grid trainees and trainers In 2018, the GMC approved a new syllabus for paediatric training: RCPCH progress Trainees with a CCT date after 15 September 2019 will
Version 1 2018 Background Guidance for grid trainees and trainers In 2018, the GMC approved a new syllabus for paediatric training: RCPCH progress Trainees with a CCT date after 15 September 2019 will
Research Perspectives in Clinical Neurophysiology
 Research Perspectives in Clinical Neurophysiology A position paper of the EC-IFCN (European Chapter of the International Federation of Clinical Neurophysiology) representing ~ 8000 Clinical Neurophysiologists
Research Perspectives in Clinical Neurophysiology A position paper of the EC-IFCN (European Chapter of the International Federation of Clinical Neurophysiology) representing ~ 8000 Clinical Neurophysiologists
Guidance on competencies for Paediatric Pain Medicine reviewed 2017
 Guidance on competencies for Paediatric Pain Medicine reviewed 2017 Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine Page 2 4 Appendix A: Curriculum 5 B: Competencies
Guidance on competencies for Paediatric Pain Medicine reviewed 2017 Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine Page 2 4 Appendix A: Curriculum 5 B: Competencies
Specific Standards of Accreditation for Residency Programs in Adult and Pediatric Neurology
 Specific Standards of Accreditation for Residency Programs in Adult and Pediatric Neurology INTRODUCTION 2011 A university wishing to have an accredited program in adult Neurology must also sponsor an
Specific Standards of Accreditation for Residency Programs in Adult and Pediatric Neurology INTRODUCTION 2011 A university wishing to have an accredited program in adult Neurology must also sponsor an
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Freedom of Information Act Request Physiotherapy Services for Neurological Conditions
 Freedom of Information Act Request Physiotherapy Services for Neurological Conditions 1. In total how many physiotherapists does C&V UHB employ? s services 33 qualified paediatric physiotherapy staff in
Freedom of Information Act Request Physiotherapy Services for Neurological Conditions 1. In total how many physiotherapists does C&V UHB employ? s services 33 qualified paediatric physiotherapy staff in
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level
 Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
5 Diagnosis. Timely diagnosis. Back to contents
 5 5 Diagnosis Back to contents Study Advisory Group questions: Are there delays in diagnosis? Is there variation in how the cerebral palsies are described? signs can fluctuate, to avoid over-diagnosis
5 5 Diagnosis Back to contents Study Advisory Group questions: Are there delays in diagnosis? Is there variation in how the cerebral palsies are described? signs can fluctuate, to avoid over-diagnosis
Guidelines for the appointment of. General Practitioners with Special Interests in the Delivery of Clinical Services. Epilepsy
 Guidelines for the appointment of General Practitioners with Special Interests in the Delivery of Clinical Services Epilepsy April 2003 Epilepsy This general practitioner with special interest (GPwSI)
Guidelines for the appointment of General Practitioners with Special Interests in the Delivery of Clinical Services Epilepsy April 2003 Epilepsy This general practitioner with special interest (GPwSI)
The Royal College of Anaesthetists THE STRUCTURE OF A STANDARD
 ROYAL COLLEGE OF ANAESTHETISTS ACCREDITATION The Royal College of Anaesthetists THE STRUCTURE OF A STANDARD Page 1 of 10 The ACSA standard has 5 DOMAINS: 1. The Care Pathway 2. Equipment, Facilities and
ROYAL COLLEGE OF ANAESTHETISTS ACCREDITATION The Royal College of Anaesthetists THE STRUCTURE OF A STANDARD Page 1 of 10 The ACSA standard has 5 DOMAINS: 1. The Care Pathway 2. Equipment, Facilities and
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
The Milestones are designed only for use in evaluation
 The Neurology Milestone Project The Milestones are designed only for use in evaluation of resident physicians in the context of their participation in Accreditation Council for Graduate Medical Education
The Neurology Milestone Project The Milestones are designed only for use in evaluation of resident physicians in the context of their participation in Accreditation Council for Graduate Medical Education
HEKSS CHILD & ADOLESCENT PSYCHIATRY PROGRAMME - HST Trainee Job Description. HST TRAINEE Community Eating Disorders Child and Adolescent
 HEKSS CHILD & ADOLESCENT PSYCHIATRY PROGRAMME - HST Trainee Job Description Job Title: HST TRAINEE Community Eating Disorders Child and National Post Number: Educational / Supervisor: Base: Hours of Work:
HEKSS CHILD & ADOLESCENT PSYCHIATRY PROGRAMME - HST Trainee Job Description Job Title: HST TRAINEE Community Eating Disorders Child and National Post Number: Educational / Supervisor: Base: Hours of Work:
Level 1 Course Khartoum, Sudan, Tuesday 27 January 2015
 GENERAL INFORMATION Paediatric Epilepsy Training (PET) courses were developed by the British Paediatric Neurology Association to improve the diagnosis and management of children with epilepsies for general
GENERAL INFORMATION Paediatric Epilepsy Training (PET) courses were developed by the British Paediatric Neurology Association to improve the diagnosis and management of children with epilepsies for general
Curriculum for Paediatric Training Neonatal Medicine Level 1, 2 and 3 Training
 Curriculum for Paediatric Training Neonatal Medicine Level 1, 2 and 3 Training Sept 2010 Revised and Approved by the GMC. For implementation from 1 st August 2016 QUICK START TO THE CURRICULUM... 4 INTRODUCTION...
Curriculum for Paediatric Training Neonatal Medicine Level 1, 2 and 3 Training Sept 2010 Revised and Approved by the GMC. For implementation from 1 st August 2016 QUICK START TO THE CURRICULUM... 4 INTRODUCTION...
SAFE PAEDIATRIC NEUROSURGERY A Report from the SOCIETY OF BRITISH NEUROLOGICAL SURGEONS
 SAFE PAEDIATRIC NEUROSURGERY 2001 A Report from the SOCIETY OF BRITISH NEUROLOGICAL SURGEONS SAFE PAEDIATRIC NEUROSURGERY 2001 INTRODUCTION In 1997 the SBNS agreed to the setting up of a task force to
SAFE PAEDIATRIC NEUROSURGERY 2001 A Report from the SOCIETY OF BRITISH NEUROLOGICAL SURGEONS SAFE PAEDIATRIC NEUROSURGERY 2001 INTRODUCTION In 1997 the SBNS agreed to the setting up of a task force to
A. Service Specification
 A. Service Specification Service Specification No: 1767 Service Adult Highly Specialist Pain Management Services Commissioner Lead For local completion Lead For local completion 1. Scope 1.1 Prescribed
A. Service Specification Service Specification No: 1767 Service Adult Highly Specialist Pain Management Services Commissioner Lead For local completion Lead For local completion 1. Scope 1.1 Prescribed
Curriculum for Paediatric Training Paediatric Clinical Pharmacology Level 1, 2 and 3 Training
 Curriculum for Paediatric Training Paediatric Clinical Pharmacology Level 1, 2 and 3 Training Sept 2010 Revised and Approved by the GMC 1 st July 2013 until July 2015 2 QUICK START TO THE CURRICULUM...
Curriculum for Paediatric Training Paediatric Clinical Pharmacology Level 1, 2 and 3 Training Sept 2010 Revised and Approved by the GMC 1 st July 2013 until July 2015 2 QUICK START TO THE CURRICULUM...
NEUROPSYCHOLOGY TRACK COORDINATOR: Dr. Ellen Vriezen
 NEUROPSYCHOLOGY TRACK COORDINATOR: Dr. Ellen Vriezen The Neuropsychology Track offers two Resident Positions: NMS Code Number: 181516 1 position with an Adult emphasis, which provide training for residents
NEUROPSYCHOLOGY TRACK COORDINATOR: Dr. Ellen Vriezen The Neuropsychology Track offers two Resident Positions: NMS Code Number: 181516 1 position with an Adult emphasis, which provide training for residents
European Paediatric Neurology Training Programme
 European Paediatric Neurology Training Programme FIRST REVISION 5 JANUARY 2009/ O. F. Brouwer and L. Palm Approved by The European Paediatric Neurology Society and by the European Committee of National
European Paediatric Neurology Training Programme FIRST REVISION 5 JANUARY 2009/ O. F. Brouwer and L. Palm Approved by The European Paediatric Neurology Society and by the European Committee of National
Report of the Welsh Neuroscience External Expert Review Group. All Wales Recommendations
 Report of the Welsh Neuroscience External Expert Review Group All Wales Recommendations Main Recommendations 1. The workforce delivering all aspects of care to people with acute and long term neurological
Report of the Welsh Neuroscience External Expert Review Group All Wales Recommendations Main Recommendations 1. The workforce delivering all aspects of care to people with acute and long term neurological
European Paediatric Neurology Training Programme
 UNION EUROPÉENNE DES MÉDECINS SPÉCIALISTES EUROPEAN UNION OF MEDICAL SPECIALISTS 20, Av.de la Couronne tel: +32-2-649.5164 B-1050 BRUSSELS fax: +32-2-640.3730 www.uems.net e-mail: uems@skynet.be D 0313
UNION EUROPÉENNE DES MÉDECINS SPÉCIALISTES EUROPEAN UNION OF MEDICAL SPECIALISTS 20, Av.de la Couronne tel: +32-2-649.5164 B-1050 BRUSSELS fax: +32-2-640.3730 www.uems.net e-mail: uems@skynet.be D 0313
Epilepsy12 Round 3 Organisational Audit dataset
 Organisational Audit (Service Descriptor) Questionnaire Yearly published reports will be based on completion and submission by a defined time after the yearly census day Fields can be updated at any time
Organisational Audit (Service Descriptor) Questionnaire Yearly published reports will be based on completion and submission by a defined time after the yearly census day Fields can be updated at any time
Neurology. Access Center 24/7 access for referring physicians (866) 353-KIDS (5437)
 Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Care Coordination / Care Programme Approach Learning Disability PGN Management of Epilepsy in Learning Disability (LD) Planned and Urgent Care V03
 Care Coordination / Care Programme Approach Learning Disability PGN Management of Epilepsy in Learning Disability (LD) Planned and Urgent Care V03 V03 issued Issue 1 Dec 14 Issue 2 Dec 17 Planned review
Care Coordination / Care Programme Approach Learning Disability PGN Management of Epilepsy in Learning Disability (LD) Planned and Urgent Care V03 V03 issued Issue 1 Dec 14 Issue 2 Dec 17 Planned review
2010 Paediatric Cardiology ARCP Decision Aid August 2014
 2010 Paediatric Cardiology ARCP Decision Aid August 2014 The following tables set out the requirements for satisfactory ARCP outcome at the end of each training year. This document replaces previous versions
2010 Paediatric Cardiology ARCP Decision Aid August 2014 The following tables set out the requirements for satisfactory ARCP outcome at the end of each training year. This document replaces previous versions
Basic Standards for Residency Training in General Neurology
 Basic Standards for Residency Training in General Neurology American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Revised 2/2003 Revised 7/2004 Revised 6/2006
Basic Standards for Residency Training in General Neurology American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Revised 2/2003 Revised 7/2004 Revised 6/2006
Bristol, February 2015
 GENERAL INFORMATION This course has been developed to improve practice within childhood epilepsies and is delivered by means of didactic teaching sessions and small workshops. PET2 concentrates on general
GENERAL INFORMATION This course has been developed to improve practice within childhood epilepsies and is delivered by means of didactic teaching sessions and small workshops. PET2 concentrates on general
Adult Neurology Residency Training Program McGill University Objectives of Training and Training Requirements. For Outpatient Neurology Clinics
 Neurology Residency Program Department of Neurology & Neurosurgery Postal address: Montreal Neurological Institute 3801 University Street Montreal, PQ, Canada H3A 2B4 Tel.: (514) 398-1904 Fax: (514) 398-4621
Neurology Residency Program Department of Neurology & Neurosurgery Postal address: Montreal Neurological Institute 3801 University Street Montreal, PQ, Canada H3A 2B4 Tel.: (514) 398-1904 Fax: (514) 398-4621
Physical health of children and adolescents
 Physical health of children and adolescents FR/CAP/02 What specialist child and adolescent psychiatrists need to know and do Faculty of Child and Adolescent Psychiatry, Royal College of Psychiatrists FACULTY
Physical health of children and adolescents FR/CAP/02 What specialist child and adolescent psychiatrists need to know and do Faculty of Child and Adolescent Psychiatry, Royal College of Psychiatrists FACULTY
Training in palliative and end-of-life care: Guidance for trainees (and their trainers) in non-palliative medicine training posts
 Training in palliative and end-of-life care: Guidance for trainees (and their trainers) in non-palliative medicine training posts August 204 Produced by Dr Fiona Hicks onsultant in Palliative Medicine
Training in palliative and end-of-life care: Guidance for trainees (and their trainers) in non-palliative medicine training posts August 204 Produced by Dr Fiona Hicks onsultant in Palliative Medicine
SPECIALTY TRAINING CURRICULUM FOR CLINICAL NEUROPHYSIOLOGY AUGUST 2010 (WITH AMENDMENTS AUGUST 2012)
 SPECIALTY TRAINING CURRICULUM FOR CLINICAL NEUROPHYSIOLOGY AUGUST 2010 (WITH AMENDMENTS AUGUST 2012) Joint Royal Colleges of Physicians Training Board 5 St Andrews Place Regent s Park London NW1 4LB Telephone:
SPECIALTY TRAINING CURRICULUM FOR CLINICAL NEUROPHYSIOLOGY AUGUST 2010 (WITH AMENDMENTS AUGUST 2012) Joint Royal Colleges of Physicians Training Board 5 St Andrews Place Regent s Park London NW1 4LB Telephone:
02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical POOLE HOSPITAL NHS FOUNDATION TRUST
 Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Service Specification No. Service Commissioner Leads 02/GMS/0030 ADULT EPILEPSY SERVICE CCP for General Medical and Surgical Provider Lead POOLE HOSPITAL NHS FOUNDATION TRUST Period 1 April 2013 to 31
Neurology Goals: Knowledge:
 Neurology Goals: A solid understanding of normal neurological development, anatomy and neurophysiology is imperative to the treatment of neurological pathology. The goal is to sensitize the family medicine
Neurology Goals: A solid understanding of normal neurological development, anatomy and neurophysiology is imperative to the treatment of neurological pathology. The goal is to sensitize the family medicine
Proposed Neurosciences National Structure. Accountability Framework Neurological Alliance (Feedback Loop) National Advisory Group (Neurosciences)
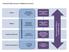 Accountability Framework Neurological Alliance (Feedback Loop) Proposed s National Structure National NHS England National Medical Director National Advisory Group (s) Regional NHS England Sub-Regional
Accountability Framework Neurological Alliance (Feedback Loop) Proposed s National Structure National NHS England National Medical Director National Advisory Group (s) Regional NHS England Sub-Regional
IOM at University of. Training for physicians. art of IOM. neurologic. injury during surgery. surgery on by IOM. that rate is.
 Topics covered: Overview of science and art of IOM IOM at University of Michigan Hospital and Health Systems What is the purpose of Intraoperative monitoring? Training for physicians Overview of science
Topics covered: Overview of science and art of IOM IOM at University of Michigan Hospital and Health Systems What is the purpose of Intraoperative monitoring? Training for physicians Overview of science
The UW Medicine Neurosciences Institute
 The UW Medicine Neurosciences Institute is a multi-disciplinary team that diagnoses and treats disorders of the nervous system. Our physicians conduct world class research, and combine the latest technology
The UW Medicine Neurosciences Institute is a multi-disciplinary team that diagnoses and treats disorders of the nervous system. Our physicians conduct world class research, and combine the latest technology
AMERICAN CLINICAL NEUROPHYSIOLOGY SOCIETY Continuing Medical Education Committee Professional Practice Gap Analysis Revised January 2016
 AMERICAN CLINICAL NEUROPHYSIOLOGY SOCIETY Continuing Medical Education Committee Professional Practice Gap Analysis Revised January 2016 Sources of Data AAN Member reports 2004, 2009, 2010 AAN Core Curricula
AMERICAN CLINICAL NEUROPHYSIOLOGY SOCIETY Continuing Medical Education Committee Professional Practice Gap Analysis Revised January 2016 Sources of Data AAN Member reports 2004, 2009, 2010 AAN Core Curricula
Meeting the Future Challenge of Stroke
 Meeting the Future Challenge of Stroke Stroke Medicine Consultant Workforce Requirements 2011 201 Dr Christopher Price BASP Training and Education Committee Stroke Medicine Specialist Advisory Committee
Meeting the Future Challenge of Stroke Stroke Medicine Consultant Workforce Requirements 2011 201 Dr Christopher Price BASP Training and Education Committee Stroke Medicine Specialist Advisory Committee
NEUROLOGY CORE CURRICULUM
 NEUROLOGY CORE CURRICULUM The goal of our residency program is to train Neurology physicians who excel in each of the six competency areas and maintain a life-long commitment to continue to grow and develop
NEUROLOGY CORE CURRICULUM The goal of our residency program is to train Neurology physicians who excel in each of the six competency areas and maintain a life-long commitment to continue to grow and develop
ENTRY-LEVEL COMPETENCIES: PAEDIATRIC DENTISTRY
 DBA1605 06 ENTRY-LEVEL COMPETENCIES: PAEDIATRIC DENTISTRY This document describes the entry-level competency standard for paediatric dentistry expected of applicants for registration with the Dental Board
DBA1605 06 ENTRY-LEVEL COMPETENCIES: PAEDIATRIC DENTISTRY This document describes the entry-level competency standard for paediatric dentistry expected of applicants for registration with the Dental Board
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
British Association of Stroke Physicians Strategy 2017 to 2020
 British Association of Stroke Physicians Strategy 2017 to 2020 1 P age Contents Introduction 3 1. Developing and influencing local and national policy for stroke 5 2. Providing expert advice on all aspects
British Association of Stroke Physicians Strategy 2017 to 2020 1 P age Contents Introduction 3 1. Developing and influencing local and national policy for stroke 5 2. Providing expert advice on all aspects
SPECIALTY OF NEUROLOGY Delineation of Clinical Privileges
 SPECIALTY OF NEUROLOGY Delineation of Clinical Privileges Criteria for granting privileges: Current board certification in Neurology by the American Board of Psychiatry and Neurology or the American Osteopathic
SPECIALTY OF NEUROLOGY Delineation of Clinical Privileges Criteria for granting privileges: Current board certification in Neurology by the American Board of Psychiatry and Neurology or the American Osteopathic
Location: HARBOR STUDENT EXPERIENCES INPATIENT: 70% OUTPATIENT: 30% CONSULTATION: PRIMARY CARE: 100% 0% TYPICAL WEEKLY SCHEDULE
 NE250.01 Advanced al Clerkship CLINICAL NEUROLOGY Location: HARBOR Revised: 11/20/07 COURSE CHAIR: Hugh B. McIntyre, M.D., Ph.D. (310) 222-3897 E-MAIL: hbmcintyre@pol.net Drs. T. Anderson, T. Edwards-Lee,
NE250.01 Advanced al Clerkship CLINICAL NEUROLOGY Location: HARBOR Revised: 11/20/07 COURSE CHAIR: Hugh B. McIntyre, M.D., Ph.D. (310) 222-3897 E-MAIL: hbmcintyre@pol.net Drs. T. Anderson, T. Edwards-Lee,
United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline
 United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline REV 3/24/09 The UCNS Geriatric Neurology examination was established to determine the level of competence
United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline REV 3/24/09 The UCNS Geriatric Neurology examination was established to determine the level of competence
Vanessa G. BA (Hons), MSc. Post Grad Diploma Neuropsychology
 Vanessa G BA (Hons), MSc. Post Grad Diploma Neuropsychology HCPC Registration No. PYL26754 DBS Registration No. 001481251441 PROFESSIONAL QUALIFICATIONS & EXPERTISE Professional Qualification(s) Consultant
Vanessa G BA (Hons), MSc. Post Grad Diploma Neuropsychology HCPC Registration No. PYL26754 DBS Registration No. 001481251441 PROFESSIONAL QUALIFICATIONS & EXPERTISE Professional Qualification(s) Consultant
Hofstra Northwell School of Medicine Department of Neurology Epilepsy Fellowship Program. Skills and Competencies Rotation Goals and Objectives
 Hofstra Northwell School of Medicine Department of Neurology Epilepsy Fellowship Program Skills and Competencies Rotation Goals and Objectives The purpose of the Epilepsy fellowship program is to provide
Hofstra Northwell School of Medicine Department of Neurology Epilepsy Fellowship Program Skills and Competencies Rotation Goals and Objectives The purpose of the Epilepsy fellowship program is to provide
Guidance on competencies for Spinal Cord Stimulation Reviewed
 Guidance on competencies for Spinal Cord Stimulation Reviewed 2016 Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine Page 2 4 Appendix A: Curriculum 5 B: Competencies
Guidance on competencies for Spinal Cord Stimulation Reviewed 2016 Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine Page 2 4 Appendix A: Curriculum 5 B: Competencies
Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form
 Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form Type of Fellowship Epilepsy Fellowship. Name of Fellowship Supervisor Dr. Bernard Rosenblatt Fellowship
Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form Type of Fellowship Epilepsy Fellowship. Name of Fellowship Supervisor Dr. Bernard Rosenblatt Fellowship
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 Chronic fatigue syndrome myalgic encephalomyelitis elitis overview bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated
Chronic fatigue syndrome myalgic encephalomyelitis elitis overview bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated
Adult Neurology Residency Training Program McGill University Rotation Specific Objectives. EEG/Epilepsy Rotation
 Neurology Residency Program Department of Neurology & Neurosurgery Postal address: Montreal Neurological Institute 3801 University Street Montreal, PQ, Canada H3A 2B4 Tel.: (514) 398-1904 Fax: (514) 398-4621
Neurology Residency Program Department of Neurology & Neurosurgery Postal address: Montreal Neurological Institute 3801 University Street Montreal, PQ, Canada H3A 2B4 Tel.: (514) 398-1904 Fax: (514) 398-4621
Sleep Medicine Maintenance of Certification Examination Blueprint
 Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Proposed Highly Specialised Technology Evaluation
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Highly Specialised Technology Evaluation Drisapersen for treating Duchenne muscular Draft scope (pre-referral) Draft remit/evaluation objective
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Highly Specialised Technology Evaluation Drisapersen for treating Duchenne muscular Draft scope (pre-referral) Draft remit/evaluation objective
Specialist List in Special Care Dentistry
 Specialist List in Special Care Dentistry Definition of Special Care Dentistry Special Care Dentistry (SCD) is concerned with providing enabling the delivery of oral care for people with an impairment
Specialist List in Special Care Dentistry Definition of Special Care Dentistry Special Care Dentistry (SCD) is concerned with providing enabling the delivery of oral care for people with an impairment
PREVIOUS EMPLOYMENT. Associate OT : CJ Occupational Therapy * Assessment and treatment for adults with neurological conditions
 CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
The Clinical Neurophysiology Milestone Project
 The Clinical Neurophysiology Milestone Project A Joint Initiative of The Accreditation Council for Graduate Medical Education and The American Board of Psychiatry and Neurology July 2015 The Clinical Neurophysiology
The Clinical Neurophysiology Milestone Project A Joint Initiative of The Accreditation Council for Graduate Medical Education and The American Board of Psychiatry and Neurology July 2015 The Clinical Neurophysiology
Purple Day, Saskatchewan Celebration March 24, 2016
 Saskatchewan Comprehensive Epilepsy Program Newsletter Spring 2016, Issue 4 Approximately 50 million people worldwide have epilepsy (300,000 people in Canada), making it one of the most common neurological
Saskatchewan Comprehensive Epilepsy Program Newsletter Spring 2016, Issue 4 Approximately 50 million people worldwide have epilepsy (300,000 people in Canada), making it one of the most common neurological
CERTIFICATE IN SPECIAL CARE DENTAL NURSING
 NATIONAL EXAMINING BOARD FOR DENTAL NURSES CERTIFICATE IN SPECIAL CARE DENTAL NURSING PROSPECTUS 108-110 LONDON STREET FLEETWOOD LANCASHIRE FY7 6EU NEBDN is a limited company registered in England & Wales
NATIONAL EXAMINING BOARD FOR DENTAL NURSES CERTIFICATE IN SPECIAL CARE DENTAL NURSING PROSPECTUS 108-110 LONDON STREET FLEETWOOD LANCASHIRE FY7 6EU NEBDN is a limited company registered in England & Wales
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Self- Assessment. Self- assessment checklist
 Self- Assessment Peer Review Self- assessment checklist (Based on RCA guidelines for the provision of anaesthetic services 2004, RCA/AA Guide for Departments of Anaesthesia 2002, NSF for children Standard
Self- Assessment Peer Review Self- assessment checklist (Based on RCA guidelines for the provision of anaesthetic services 2004, RCA/AA Guide for Departments of Anaesthesia 2002, NSF for children Standard
Volume of practice and workplace-based assessment requirements for each of the ANZCA Clinical Fundamentals
 Appendix Four Volume of practice and workplace-based assessment requirements for each of the ANZCA Clinical Fundamentals This appendix contains tables setting out both the volume of practice and workplace-based
Appendix Four Volume of practice and workplace-based assessment requirements for each of the ANZCA Clinical Fundamentals This appendix contains tables setting out both the volume of practice and workplace-based
Medical Training Initiative Post Paediatric Oncology Fellow Retrieval. Job Description Lead Clinician Dr Emma Ross
 Leicester Royal Infirmary, University Hospitals of Leicester NHS Trust Medical Training Initiative Post Paediatric Oncology Fellow Retrieval. Job Description Lead Clinician Dr Emma Ross 2018 Hospital:
Leicester Royal Infirmary, University Hospitals of Leicester NHS Trust Medical Training Initiative Post Paediatric Oncology Fellow Retrieval. Job Description Lead Clinician Dr Emma Ross 2018 Hospital:
Specialists in Old Age Psychiatry
 A Competency Based Curriculum for Specialist Training in Psychiatry Specialists in Old Age Psychiatry Royal College of Psychiatrists February 2010 (update approved 2014, revised March 2015, revised March
A Competency Based Curriculum for Specialist Training in Psychiatry Specialists in Old Age Psychiatry Royal College of Psychiatrists February 2010 (update approved 2014, revised March 2015, revised March
Physiotherapy Department
 POSITION DESCRIPTION Grade 3 Physiotherapist Physiotherapy Department Date revised: April 2013 POSITION: AWARD/AGREEMENT: Senior Clinician Physiotherapist Neurological and Spinal Cord Injury Rehabilitation
POSITION DESCRIPTION Grade 3 Physiotherapist Physiotherapy Department Date revised: April 2013 POSITION: AWARD/AGREEMENT: Senior Clinician Physiotherapist Neurological and Spinal Cord Injury Rehabilitation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice 1 Guideline title SCOPE Autism: the management and support of children and young people on the autism spectrum 1.1 Short
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice 1 Guideline title SCOPE Autism: the management and support of children and young people on the autism spectrum 1.1 Short
SUBSPECIALIST TRAINING PROGRAMME
 EUROPEAN BOARD AND COLLEGE OF OBSTETRICIANS AND GYNAECOLOGISTS (EBCOG) AND EUROPEAN SOCIETY OF GYNAECOLOGICAL ONCOLOGY (ESGO) SUBSPECIALIST TRAINING PROGRAMME IN GYNAECOLOGICAL ONCOLOGY This Programme
EUROPEAN BOARD AND COLLEGE OF OBSTETRICIANS AND GYNAECOLOGISTS (EBCOG) AND EUROPEAN SOCIETY OF GYNAECOLOGICAL ONCOLOGY (ESGO) SUBSPECIALIST TRAINING PROGRAMME IN GYNAECOLOGICAL ONCOLOGY This Programme
Specialised Services Policy: CP23 Vagal Nerve Stimulation
 Specialised Services Policy: CP23 Vagal Nerve Stimulation Document Author: Specialist Services Planning Manager for Neurosciences and Complex Conditions Executive Lead: Director of Planning and Performance
Specialised Services Policy: CP23 Vagal Nerve Stimulation Document Author: Specialist Services Planning Manager for Neurosciences and Complex Conditions Executive Lead: Director of Planning and Performance
Specialists in Old Age Psychiatry
 A Competency Based Curriculum for Specialist Training in Psychiatry Specialists in Old Age Psychiatry Royal College of Psychiatrists February 2010 (update approved 2014, revised March 2015, revised March
A Competency Based Curriculum for Specialist Training in Psychiatry Specialists in Old Age Psychiatry Royal College of Psychiatrists February 2010 (update approved 2014, revised March 2015, revised March
COMPETENCES REQUIRED FOR APPLICANTS TO ATTAIN HPC REGISTRATION AS CLINICAL SCIENTISTS
 This document comprises a discipline-specific version of the general competence document and provides additional guidance as to how to complete the general document, Appendix 1 of the Guidelines, that
This document comprises a discipline-specific version of the general competence document and provides additional guidance as to how to complete the general document, Appendix 1 of the Guidelines, that
2010 National Audit of Dementia (Care in General Hospitals)
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Description of the specialty and clinical needs of patients
 Neurology i Description of the specialty and clinical needs of patients Neurology is the branch of medicine dealing with disorders of the nervous system, including the brain, spinal cord, peripheral nerves
Neurology i Description of the specialty and clinical needs of patients Neurology is the branch of medicine dealing with disorders of the nervous system, including the brain, spinal cord, peripheral nerves
Neurological Alliance of Ireland. Submission to the National Dementia Strategy August 2012
 Neurological Alliance of Ireland Submission to the National Dementia Strategy August 2012 1.1 Background The Neurological Alliance of Ireland is the national umbrella for over thirty not for profit organisations
Neurological Alliance of Ireland Submission to the National Dementia Strategy August 2012 1.1 Background The Neurological Alliance of Ireland is the national umbrella for over thirty not for profit organisations
Location: HARBOR STUDENT EXPERIENCES INPATIENT: OUTPATIENT: 70% 30% CONSULTATION: PRIMARY CARE: 100% 0% TYPICAL WEEKLY SCHEDULE
 NE250.01 Advanced Clinical Clerkship CLINICAL NEUROLOGY Location: HARBOR COURSE CHAIR: Natalie Diaz, MD (310) 222-3897 E-MAIL: nadiaz@dhs.lacounty.gov Drs. T. Anderson, M. Goldberg, D. Naylor, N. Diaz,
NE250.01 Advanced Clinical Clerkship CLINICAL NEUROLOGY Location: HARBOR COURSE CHAIR: Natalie Diaz, MD (310) 222-3897 E-MAIL: nadiaz@dhs.lacounty.gov Drs. T. Anderson, M. Goldberg, D. Naylor, N. Diaz,
A Framework of Competences for the Special Interest Module in Paediatric Allergy
 A Framework of Competences for the Special Interest Module in Paediatric Allergy Version 2 To be used from March 2016 Royal College of Paediatrics and Child Health www.rcpch.ac.uk 1 This guide is for trainees
A Framework of Competences for the Special Interest Module in Paediatric Allergy Version 2 To be used from March 2016 Royal College of Paediatrics and Child Health www.rcpch.ac.uk 1 This guide is for trainees
Young onset dementia service Doncaster
 Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Specialty Training Committee in Respiratory and Sleep Medicine. Application for Accreditation of Advanced Training Sites in Adult Sleep Medicine
 Specialty Training Committee in Respiratory and Sleep Medicine Application for Accreditation of Advanced Training Sites in Adult Sleep Medicine Information on Completion of Survey 1. A separate survey
Specialty Training Committee in Respiratory and Sleep Medicine Application for Accreditation of Advanced Training Sites in Adult Sleep Medicine Information on Completion of Survey 1. A separate survey
AMERICAN BOARD OF CLINICAL NEUROPHYSIOLOGY
 AMERICAN BOARD OF CLINICAL NEUROPHYSIOLOGY Part I Content Outline I. Physiology and Instrumentation 30% A. Physiology 1. Anatomy of neural generation 2. Mechanisms of EEG and evoked potential generation
AMERICAN BOARD OF CLINICAL NEUROPHYSIOLOGY Part I Content Outline I. Physiology and Instrumentation 30% A. Physiology 1. Anatomy of neural generation 2. Mechanisms of EEG and evoked potential generation
Specialists in General Psychiatry
 A Competency Based Curriculum for Specialist Training in Psychiatry Specialists in General Psychiatry Royal College of Psychiatrists February 2010 (update approved 2 October 2014) Royal College of Psychiatrists
A Competency Based Curriculum for Specialist Training in Psychiatry Specialists in General Psychiatry Royal College of Psychiatrists February 2010 (update approved 2 October 2014) Royal College of Psychiatrists
Run Through Pilot in Otolaryngology
 Run Through Pilot in Otolaryngology October 2017 What does run through training mean? Run through training is a programme whereby trainees appointed to ST1 posts in the specialty will continue through
Run Through Pilot in Otolaryngology October 2017 What does run through training mean? Run through training is a programme whereby trainees appointed to ST1 posts in the specialty will continue through
GERIATRIC MEDICINE Stroke
 Post CSCST TRAINING IN GERIATRIC MEDICINE Stroke Royal College of Physicians of Ireland, 1 This curriculum of training in Stroke was developed in 2017 and undergoes an annual review by Prof David Williams,
Post CSCST TRAINING IN GERIATRIC MEDICINE Stroke Royal College of Physicians of Ireland, 1 This curriculum of training in Stroke was developed in 2017 and undergoes an annual review by Prof David Williams,
LLANDUDNO HOSPITAL PROJECT CYCLE ONE REPORT FOR REHABILITATION PROJECT TEAM: ASSESSMENT OF POTENTIAL SOLUTIONS FOR DEVELOPING SERVICES MARCH 2010
 LLANDUDNO HOSPITAL PROJECT CYCLE ONE REPORT FOR REHABILITATION PROJECT TEAM: ASSESSMENT OF POTENTIAL SOLUTIONS FOR DEVELOPING SERVICES MARCH 2010 SITUATION The Rehabilitation Project Team has been established
LLANDUDNO HOSPITAL PROJECT CYCLE ONE REPORT FOR REHABILITATION PROJECT TEAM: ASSESSMENT OF POTENTIAL SOLUTIONS FOR DEVELOPING SERVICES MARCH 2010 SITUATION The Rehabilitation Project Team has been established
Plymouth University. Pathway Specification
 Plymouth University Faculty of Health and Human Sciences School of Health Professions Pathway Postgraduate Certificate Postgraduate diploma Master of Science In Advanced Professional Practice in Neurological
Plymouth University Faculty of Health and Human Sciences School of Health Professions Pathway Postgraduate Certificate Postgraduate diploma Master of Science In Advanced Professional Practice in Neurological
UK Standards of Care
 UK Standards of Care Service Provision of Physiotherapy For Children with Haemophilia & other Inherited Bleeding Disorders Page 1 of 10 Background Standards were originally written by the Haemophilia Chartered
UK Standards of Care Service Provision of Physiotherapy For Children with Haemophilia & other Inherited Bleeding Disorders Page 1 of 10 Background Standards were originally written by the Haemophilia Chartered
THE NEUROSCIENCE INSTITUTE OF NEW YORK HOSPITAL QUEENS
 THE NEUROSCIENCE INSTITUTE OF NEW YORK HOSPITAL QUEENS PROVIDING A HIGHER LEVEL OF COMPREHENSIVE CARE OF THE BRAIN AND NERVOUS SYSTEM. RIGHT HERE. IN QUEENS. The Neuroscience Institute is The Center for
THE NEUROSCIENCE INSTITUTE OF NEW YORK HOSPITAL QUEENS PROVIDING A HIGHER LEVEL OF COMPREHENSIVE CARE OF THE BRAIN AND NERVOUS SYSTEM. RIGHT HERE. IN QUEENS. The Neuroscience Institute is The Center for
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
POSITION DESCRIPTION Grade 4 Physiotherapist Physiotherapy Department
 POSITION DESCRIPTION Grade 4 Physiotherapist Physiotherapy Department Date revised: June 2015 POSITION: AWARD/AGREEMENT: Grade 4 Physiotherapists Health Professionals (Public Sector Victoria) CLASSIFICATION
POSITION DESCRIPTION Grade 4 Physiotherapist Physiotherapy Department Date revised: June 2015 POSITION: AWARD/AGREEMENT: Grade 4 Physiotherapists Health Professionals (Public Sector Victoria) CLASSIFICATION
Muscular Dystrophy UK s Adult North Star Network. Care recommendations for adults with Duchenne a consultation
 Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
2010 National Audit of Dementia (Care in General Hospitals) Guy's and St Thomas' NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
