Current therapeutic protocols for chronic granulomatous fungal sinusitis*
|
|
|
- Domenic Richard Rich
- 5 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION Current therapeutic protocols for chronic granulomatous fungal sinusitis* V. Rupa, S. Maheswaran, J. Ebenezer, S.S. Mathews Rhinology 53: , 2015 DOI: /Rhino Department of ENT, Christian Medical College, Vellore, India *Received for publication: July 26, 2014 Accepted: December 13, 2014 Abstract Background: The treatment of chronic granulomatous fungal sinusitis (CGFS), a rare form of invasive fungal sinusitis, is controversial. Aim: To assess the response to postoperative antifungal therapy in patients with CGFS and suggest an effective treatment protocol. Methodology: Clinical records of patients with CGFS who had undergone excisive surgery followed by antifungal therapy were reviewed to assess current disease status. Results: Fourteen male and 4 female patients were diagnosed with CGFS, based on typical histopathological and fungal smear/ culture results. Aspergillus flavus was isolated from 88.9% cases. Stage 1 patients had resectable sinonasal disease, stage 2 had additional spread to orbit/palate and stage 3 had extensive disease. Follow up ranged from 6 months to 8 years. Residual disease was seen in all but one patient who received amphotericin B as first line therapy and in none of those who received itraconazole or voriconazole. Even those who received azoles as second line therapy were disease free at last follow-up. Conclusion: Surgery followed by itraconazole or voriconazole for Stage 1 and 2 disease and voriconazole for stage 3 disease is recommended for a good outcome. Amphotericin B is not recommended as first line therapy for CGFS. Keywords: Chronic granulomatous fungal sinusitis, amphotericin B, itraconazole, voriconazole Introduction Chronic granulomatous fungal sinusitis (CGFS) is a unique, chronic form of invasive fungal sinusitis seen in immunocompetent patients, typically from Sudan, India, Pakistan and Saudi Arabia. The disease, which runs an indolent course, chiefly involves the maxillary and ethmoid sinuses, nose, orbit and cheek (1,2). The distinctive presence of non-caseating granuloma containing fungal hyphae differentiates this disease from chronic invasive fungal sinusitis, a disease more commonly seen in Western populations. The diagnostic features of each of these 2 types of chronic fungal sinusitis (1) are listed in Table 1. Rarely, CGFS may coexist with other types of fungal sinusitis, particularly allergic fungal sinusitis (3). CGFS is most often caused by Aspergillus flavus and hence variably referred to as invasive rhinoorbital or rhinocerebral aspergillosis (1). The selection of an appropriate antifungal drug for treatment of invasive fungal sinusitis is largely based on clinical reports of patient s response to therapy rather than on antifungal susceptibility testing, which has limited reliability at present (4). For several years, the drug of choice for all invasive fungal infections was amphotericin B. The drug binds to ergosterol of the fungal cell 181
2 Rupa et al. Table 1. Diagnostic features of chronic granulomatous fungal sinusitis and chronic invasive fungal sinusitis. Geographical prevalence Clinical features Histological features Chronic granulomatous fungal sinusitis Chiefly Sudan, India, Pakistan and Saudi Arabia Mostly in immunocompetent patients May be diabetic Gradual onset Indolent course Unilateral proptosis, cheek or orbital swelling common Recurrences common Regional tissue invasion by fungal hyphae which are scanty Non caseating granulomas with foreign body or Langhan s type giant cells which may contain hyphae along with lymphocytes and plasma cells Occasional presence of central microgranulomata of eosinophils, fibrinoid necrosis, perivascular fibrosis and vasculitis Considerable fibrosis may be present Chronic invasive fungal sinusitis Chiefly described in Western populations Mostly in immunodeficient patients May be diabetic Gradual onset Progressive course Usually commences in deeper sinuses like posterior ethmoid and sphenoid Tissue necrosis with sparse chronic inflammatory infiltrate Numerous fungal hyphae see Invasion of mucosa, submucosa, blood vessels and bone by fungal hyphae Mycology A. flavus usually A. fumigatus usually membrane and makes it porous, leading to leakage of intracellular ions and cell death. The drug is associated with significant side-effects like nephrotoxicity, thrombophlebitis, fever and chills and cardiac arrhythmia. Lipid formulations of the drug such as lipid soluble amphotericin B and liposomal amphotericin B have less toxicity but are expensive. The azole derivatives, introduced in the late 1980s, act by selectively inhibiting fungal cytochrome P450 enzymes, which are involved in ergosterol synthesis, an early step in fungal cell membrane formation. Azoles can be classified into imidazoles or triazoles. The latter are characterized by three nitrogen atoms in the five membered azole ring and include itraconazole, fluconazole, voriconazole and posaconazole. Itraconazole has been shown to be effective in treating CGFS, often in combination with amphotericin B (5-8). While in some cases the drug was administered in a planned manner before or after a course of amphotericin B (5,8), in other cases, the drug was given when the patient became intolerant to amphotericin B (7) or showed persistent disease (6). Voriconazole is a triazole drug, which has shown great efficacy in patients with invasive aspergillosis (9,10). The drug is well absorbed orally and has few side-effects, making it a very attractive alternative to amphotericin B. Currently, it is recommended as a first line drug for treatment of invasive aspergillosis by the Infectious Disease Society of America (11). In the present study, we aimed to review the outcome following therapy with different kinds of antifungals in a series of patients with CGFS to develop an effective protocol for antifungal therapy for future use in such patients. Materials and methods We reviewed the clinical records of patients admitted with a diagnosis of CGFS in the ENT department of our hospital between January 2006 to May 2014 to note the clinical presentation, fungal culture results, histopathological features, radiological findings, surgical procedures, antifungal agents administered and outcome following treatment. We included only patients with biopsy proven evidence of CGFS who also had a positive smear and/or fungal culture. All patients were followed up at intervals of 1 to 3 months after commencing therapy. The clinical findings, rigid nasal endoscopy findings and radiological findings (whenever possible) were noted at each follow-up. The duration of follow-up for each patient was calculated from the date of initial presentation. Statistical analysis Descriptive statistics and frequency and percentages were reported for categorical variables. Fisher s exact test (2 tailed) was done to compare outcomes following first line therapy and to compare outcomes in relation to preoperative staging of the disease. Institutional Review Board approval Approval of the Institutional Review Board and Ethics committee, Christian Medical College, Vellore, was obtained for the performance of this study (IRB no. 8971). Results Demography The study included 14 males and 4 females whose ages ranged from 20 to 65 years (mean = 46.4 years). 182
3 Treatment of chronic granulomatous fungal sinusitis Symptoms The duration of symptoms varied from 1 month to 7 years with a mean of 22.9 months. The most common presenting symptoms were visual deterioration (44.4%), proptosis (38.9%), facial pain (38.9%), headache (33.3%) and nasal obstruction (33.3%). The disease was unilateral in all except 3 patients in whom the disease started as a unilateral lesion that progressed to become bilateral. Of 8 patients (44.4%) who had visual deterioration, 3 had total loss of vision in one eye. Signs Six (33.3%) patients had periorbital swelling and 5 (27.8%) had ipsilateral cheek swelling. On rigid nasal endoscopic examination, only 4 patients had an obvious nasal mass which was amenable to biopsy. Three (16.7%) patients had sinonasal polyposis. Prior surgery Nine (50%) patients had undergone at least 1 surgical procedure involving the sinuses prior to presentation. These included endoscopic sinus surgery in 7 patients, Caldwell Luc surgery in 2 patients, lateral rhinotomy and excision sinonasal mass in one and dental extraction followed by transalveolar biopsy and curettage in another. Comorbidities Six (33.3%) patients had diabetes mellitus and 4 (22.2%) were hypertensive. One patient had chronic renal failure. Fungal smear and culture results A. flavus was identified in 16 (88.9%) patients. Three patients (16.7%) had Mucor species, 1 with a combination with A. flavus and Mucor species, another with a combination of A. flavus and Rhizopus species and yet another with M. circinelloides alone. Fungal culture was negative in 1 patient. Radiological findings Based on the radiological extent, patients were categorized into 3 groups (Table 2). Stage 1 (n = 4) consisted of patients with completely resectable disease confined to the nose and paranasal sinuses. Stage 2 (n = 8) consisted of patients with completely resectable disease with extension to adjacent areas like the orbit and palate. Stage 3 (n = 6) consisted of patients with partially resectable disease or intracranial extension. Involvement of an individual sinus was best seen in contrast enhanced CT scan of the nose and paranasal sinuses, which showed soft tissue thickening with mild enhancement. Intracranial extension and dural involvement was best assessed by contrast enhanced MRI scanning of the paranasal sinuses and brain. Histopathology results All patients had features of CGFS. Typically, the tissue showed a Table 2. Staging of disease. Stage 1 Stage 2 Stage 3 chronic infiltrate of lymphocytes, plasma cells, histiocytes and Langhans type multinucleate giant cells with epithelioid granuloma with or without necrosis. Fungal hyphae were invariably seen invading tissue or bone. Angioinvasion was not seen in any specimen. Four of the patients in this series were diagnosed as having mixed fungal sinusitis with a combination of CGFS and allergic fungal sinusitis. These cases have been reported before (3). All these patients had predominant features of CGFS and areas with allergic fungal sinusitis. Surgical procedures Most patients (82.4%) underwent endoscopic excision of the sinonasal mass; in 2 patients this was combined with Caldwell Luc surgery and in another 2 with orbital exenteration. Both patients who had undergone orbital exenteration had total loss of vision in the affected eye. One patient underwent total maxillectomy and another underwent craniofacial resection of a frontal lobe mass. Operative findings most often included the finding of a pink or pale, firm, gritty mass with little vascularity infiltrating the underlying tissue. In patients with partial visual loss, orbital debridement was performed to the extent possible. Antifungal agents (Table 3) 1. Amphotericin B Areas involved Nose & paranasal sinuses alone Paranasal sinuses with immediate adjacent areas which are surgically resectable with minimal morbidity eg. orbit (extraconal), palate & oral cavity Intracranial extension (extradural/ intracerebral) or partially resectable with extension to pterygopalatine fossa, cavernous sinus, cheek and periorbital region Surgery Endoscopic resection; for maxilla partial / total maxillectomy Endoscopic / open resection; for maxilla partial / total maxillectomy Combined endoscopic and open approach with craniofacial resection for anterior skull base / frontal lobe disease Intravenous amphotericin B was commenced as first line of therapy after surgery in 6 patients (38.9%), 3 of whom had stage 2 disease and 3 of whom had stage 3 disease. Plain amphotericin B was administered to 4 patients and liposomal amphotericin B to another 2 patients. Three patients (50%) were intolerant to amphotericin B, one even with liposomal amphotericin B. These patients discontinued the drug without taking the full dose and 183
4 Rupa et al. Table 3. Response to first line therapy in relation to type of drug used and stage of disease (n = 18). Drugs given as first line therapy Amphotericin B alone (n = 5) Amphotericin B + Itraconazole (n = 1) Itraconazole alone (n = 8) Voriconazole alone (n = 4) Stage of disease Residual disease (n = 5) 3 2 No evidence of disease (n = 13) * *1 patient died after 4 months of therapy due to unrelated causes had residual disease. All except 1 of 6 patients who received amphotericin B as first line therapy had residual disease at the end of therapy. The sole patient without residual disease had received a combination of liposomal amphotericin B and itraconazole. Itraconazole Nine (50%) patients received itraconazole as first line therapy. Of these, 3 had stage 1 disease, 4 had stage 2 disease and 2 had stage 3 disease. All (except 1 patient) took the drug for a minimum of 6 months. One patient with stage 3 disease received the drug along with amphotericin B as first line therapy. Eight patients were disease-free at follow-up, which ranged from 6 months to 10 years. The sole patient with stage 3 disease who had taken the drug for 3 months had a poor general condition and died of unrelated causes. Three (16.6%) other patients with residual disease after failure / intolerance to amphotericin B were disease free after treatment with itraconazole for 1 year. Voriconazole Four patients (22%) were given oral voriconazole at a dose of 200mg twice daily as a first line of therapy. Of these 1 had stage 1 disease, another had stage 2 disease, and the other 2 had stage 3 disease. Two more patients who had residual disease following amphotericin B therapy received voriconazole as second line therapy for 1 year. Both were disease free at last follow-up. Follow-up (Table 3) Overall follow-up ranged from 6 months to 8 years with a mean of 2.6 years. Of a total of 18 patients, one patient who died from intercurrent illness was excluded from the analysis. All 12 patients who received one of the azoles alone as first line therapy showed no evidence of disease at follow-up, while all 5 patients who received amphotericin B alone as first line therapy had residual disease at follow-up and the difference between the groups was statistically significant (p = 0.001). Assessment of disease status was based on clinical and endoscopic resolution of disease in all patients. Post-treatment contrast enhanced CT scans were available in all those with residual disease (27.8%) and 4 (22.2%) of those with no evidence of disease. All 5 with residual disease and 7 patients with no disease also had biopsy of sinonasal lesions or mucosa confirming the presence / absence of residual disease. One patient died during the course of treatment due to unrelated causes. Four patients who are still on therapy have been disease free clinically and endoscopically over the last 6-9 months of treatment. When comparing the overall therapeutic response to first line therapy based on pre-treatment staging of disease, there was no significant difference between those patients who had completely resectable disease (stages 1 and 2) and those with partially resectable disease/ intracranial extension (stage 3) (p = 0.6) Discussion The therapy of CGFS has been controversial and there are no clearcut guidelines on staging and therapy. The disease occurs chiefly in Sudan and Asia and there are a limited number of reports concerning treatment and follow-up from this region. The various treatment options that are reported in the literature are considered below. I First line Single agent therapy Amphotericin B For several years, the gold standard of therapy for all types of invasive fungal sinusitis in both immunocompromised and immunocompetent patients has been amphotericin B. The optimal dose of intravenous amphotericin B is controversial. A dose of 3-5 gm is ideal but few patients are able to tolerate such high doses, because of its toxicity. There are frequent reports of stopping the drug within a few days of commencement of therapy (8,12). In the present series, 4 patients had to discontinue the drug because of toxicity. The efficacy of amphotericin B against aspergillus is variable (13,14). In our series only one of the 6 patients who received amphotericin B alone had no residual disease on follow-up. This patient had also received oral itraconazole concurrently. 184
5 Treatment of chronic granulomatous fungal sinusitis Itraconazole Itraconazole is an azole derivative, which selectively inhibits fungal cytochrome P450 enzymes and reduces the synthesis of ergosterol, a component of the fungal cell membrane. The drug is well absorbed orally after a meal but has poor CSF penetration. The exact dose and duration of itraconazole therapy is poorly defined. Gumaa et al. (15) described good response to oral itraconazole at a dose of 100mg twice daily for months in 22 patients. Higher doses of 200mg twice daily have also been recommended. Reports of good response to itraconazole, with or without amphotericin B, have been described by others too (8). Seven of the 8 patients in our series who had received itraconazole alone with long-term follow-up also showed a good response. Voriconazole The sole randomized, controlled trial of voriconazole (given at a dose of 6mg/Kg IV twice daily for 1 day followed by 4mg/ Kg twice daily) versus plain amphotericin B (given at a dose of 1-1.5mg/Kg/Day) in 277 immunocompromised patients with aspergillosis showed greater antifungal efficacy and improved survival at 12 weeks for voriconazole (9). Based on this study, the current guidelines of the Infectious Disease Society of America are that voriconazole should be given as first line therapy for invasive aspergillosis of the sinuses. There are fewer examples of therapy with voriconazole for CGFS in immunocompetent patients. Nakaya et al. (10) describe 3 patients with sinonasal CGFS who responded successfully to oral voriconazole. Our experience with 6 patients who received postoperative voriconazole, 3 as first line therapy and 3 as second line therapy following failure of response to amphotericin B has been encouraging. The 3 patients who received the drug as first line therapy had advanced disease with intracranial extension and yet responded favourably. The advantage of voriconazole over amphotericin B is that it is effective when given orally and the direct and indirect costs of administering the drug are substantially less as no hospitalisation is required. However, it is more expensive than itraconazole. The optimal duration of therapy of oral antifungals is controversial, with reports ranging from 6 to 18 months (5,10). The risk of recurrence necessitates prolonged treatment. In the present series, most patients with advanced disease received oral voriconazole for at least 9 months to 1 year with minimal side effects. Transient rise in liver enzymes not requiring stoppage of therapy, was seen in 2 patients. II. First line combination therapy: amphotericin B with itraconazole Figure 1. Suggested protocol for management of chronic granulomatous fungal sinusitis. Simultaneous therapy In a series of 21 patients with invasive aspergillosis, half of whom were given a combination of amphotericin B and itraconazole (16), the authors found that the response to combination therapy was much better (82%) than single drug therapy with amphotericin B alone (50%). No patient was given itraconazole alone in this series. Combination therapy was also found to be useful by other authors (5,7). In the present series, we had only one patient with stage 3 disease who received a combination of itraconazole and amphotericin B. This patient did not show recurrent disease at follow-up of 1 year and 3 months. The efficacy of this regimen could be attributed to the effect of itraconazole in this case, as all the other 5 patients who received amphotericin B alone had residual disease. Sequential therapy In a report of 11 patients with craniocerebral aspergillosis who were treated with sequential intravenous amphotericin B and itraconazole (8), 5 patients failed to receive the full dose of amphotericin B because they developed intolerance to the drug. These patients received a prolonged course of itraconazole (for 8 to 12 months or longer) and showed a good response, suggesting that itraconazole seemed to have effected the cure. Similar findings were noted by others (12). Salvage therapy Azoles have been used as salvage rather than as first line therapy in many reports (6,7). The advantage of azoles is that they can be given orally and have few side-effects. Hence, they are often used for long-term therapy to prevent recurrence. 185
6 Rupa et al. IV No medical therapy Isolated reports of cases of CGFS who have responded to excisive surgery without antifungal therapy exist in the literature (6,17). In one report, all 5 patients who did not receive postoperative antifungal therapy showed relapse of disease (14). None of our patients had resolution of disease with surgery alone and our view is that administration of systemic antifungal therapy is essential for invasive fungal disease. Our experience Our experience has been that patients with stage 1 and 2 disease do best with either postoperative itraconazole or voriconazole and those with stage 3 with postoperative voriconazole (Figure 1). Irrespective of the staging, all patients in the present series who were given amphotericin B alone showed evidence of residual or recurrent disease, making this drug unattractive as first/second line therapy for CGFS. Response to therapy is clearly more related to the type of antifungal drug used than the stage at presentation, if excisive surgery has been performed adequately. Author contributions VR: Study concept and design, acquisition of data, analysis of data, interpretation of data, drafting of the manuscript, critical revision of the manuscript. MS: acquisition of data, drafting of the manuscript, critical revision of the manuscript. JAE: acquisition of data, drafting of the manuscript, critical revision of the manuscript. SSM: acquisition of data, drafting of the manuscript, critical revision of the manuscript. Conflict of interest The authors declare that there is no conflict of interest. References 1. deshazo RD, O Brien M, Chapin K, Soto- Aguilar M, Gardner L, Swain R. A new classification and diagnostic criteria for invasive fungal sinusitis. Arch Otolaryngol Head Neck Surg. 1997; 123: Veress B, Malik OA, el-tayeb AA, el-daoud S, Mahgoub ES, el-hassan AM. Further observations on primary paranasal Aspergillus granuloma in the Sudan. A morphological study of 46 cases. Am J Trop Med Hyg. 1973; 2: Rupa V, Thomas M. Different types of fungal sinusitis occurring concurrently: implications for therapy. Eur Arch Otorhinolaryngol. 2013; 270: Ghannoum MA, Rex JH, Galgiani JN. Susceptibility testing of fungi: current status of correlation of in vitro data with clinical outcome. J Clin Microbiol. 1996; 34: Panda NK, Saravanan K, Chakrabarthi A. Combination antifungal therapy for invasive aspergillosis: can it replace high-risk surgery at the skull base? Am J Otolaryngol. 2008; 29: Busaba NY, Colden DG, Faquin WC, Salman SD. Chronic invasive fungal sinusitis: a report of two atypical cases. Ear Nose Throat J. 2002; 81: Streppel M, Bachmann G, Damm M, Arnold G, Stennert E.Successful treatment of an invasive aspergillosis of the skull base and paranasal sinuses with liposomal amphotericin B and itraconazole. Ann Otol Rhinol Laryngol. 1999; 108: Siddiqui AA, Shah AA, Bashir S. Craniocerebral aspergillosis of sinonasal originin immunocompetent patients: clinical spectrum and outcome in 25 cases. Neurosurgery. 2004; 55: Herbrecht R, Denning DW, Patterson TF, et al. Voriconazole versus amphotericin B for primary therapy of invasive aspergillosis. N Engl J Med. 2002; 347: Nakaya K, Oshima T, Kudo T, et al. New treatment for invasive fungal sinusitis: three cases of chronic invasive fungal sinusitis treated with surgery and voriconazole. Auris Nasus Larynx. 2010; 37: Walsh TJ, Anaissie EJ, Denning DW, et al. Treatment of aspergillosis: clinical practice guidelines of the Infectious Diseases Society of America. Clin Infect Dis. 2008; 46: Kim TH, Jang HU, Jung YY, Kim JS. Granulomatous invasive fungal rhinosinusitis extending into the pterygopalatine fossa and orbital floor: A case report. Med Mycol Case Rep. 2012; 1: Stringer SP, Ryan MW. Chronic invasive fungal rhinosinusitis. Otolaryngol Clin North Am. 2000; 33: Alrajhi AA, Enani M, Mahasin Z, Al-Omran. Chronic invasive aspergillosis of the paranasal sinuses in immunocompetent hosts from Saudi Arabia. Am J Trop Med Hyg. 2001; 65: Gumaa SA, Mahgoub ES, Hay RJ. Postoperative responses of paranasal Aspergillus granuloma to itraconazole. Trans R Soc Trop Med Hyg. 1992; 86: Popp AI, White MH, Quadri T, Walshe L, Armstrong D. Amphotericin B with and without itraconazole for invasive aspergillosis. A three year retrospective study. Int J Infect Dis. 1999; 3: Thakkar A, Sarkar C, Dhiwakar M, Bahadur S, Dahiya S. Allergic fungal sinusitis: expanding the clinicopathological spectrum Otolaryngol Head Neck Surg. 2004; 130: Dr. V. Rupa, M.S., D.L.O. Professor and Head Department of ENT Unit 3 Christian Medical College Hospital Vellore India Tel: Fax: rupavedantam@cmcvellore. ac.in 186
7 Copyright of Rhinology is the property of International Rhinologic Society and its content may not be copied or ed to multiple sites or posted to a listserv without the copyright holder's express written permission. However, users may print, download, or articles for individual use.
Medical Mycology Case Reports
 Medical Mycology Case Reports 1 (2012) 107 111 Contents lists available at SciVerse ScienceDirect Medical Mycology Case Reports journal homepage: www.elsevier.com/locate/mmcr Granulomatous invasive fungal
Medical Mycology Case Reports 1 (2012) 107 111 Contents lists available at SciVerse ScienceDirect Medical Mycology Case Reports journal homepage: www.elsevier.com/locate/mmcr Granulomatous invasive fungal
Presentation of Invasive Fungal Rhinosinusitis in Sudanese Children: A Report of Four Cases
 Volume 13, Issue no. 2, DOI 10.18502/sjms.v13i2.2643 Production and Hosting by Knowledge E Case Report Presentation of Invasive Fungal Rhinosinusitis in Sudanese Children: A Report of Four Cases Faculty
Volume 13, Issue no. 2, DOI 10.18502/sjms.v13i2.2643 Production and Hosting by Knowledge E Case Report Presentation of Invasive Fungal Rhinosinusitis in Sudanese Children: A Report of Four Cases Faculty
Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients Marcus M. Monroe, MD; Max McLean, BA;
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients Marcus M. Monroe, MD; Max McLean, BA;
Case Report Chronic Invasive Nongranulomatous Fungal Rhinosinusitis in Immunocompetent Individuals
 Case Reports in Otolaryngology Volume 2016, Article ID 6854121, 7 pages http://dx.doi.org/10.1155/2016/6854121 Case Report Chronic Invasive Nongranulomatous Fungal Rhinosinusitis in Immunocompetent Individuals
Case Reports in Otolaryngology Volume 2016, Article ID 6854121, 7 pages http://dx.doi.org/10.1155/2016/6854121 Case Report Chronic Invasive Nongranulomatous Fungal Rhinosinusitis in Immunocompetent Individuals
Clinical Study of Fungal Granulomatous Diseases
 International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol2, Issue5, 2015, pp665-669 http://www.ijhsonline.com Review Article Clinical Study of Fungal Granulomatous Diseases Sunil Pai
International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol2, Issue5, 2015, pp665-669 http://www.ijhsonline.com Review Article Clinical Study of Fungal Granulomatous Diseases Sunil Pai
ORIGINAL ARTICLE. Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis
 ORIGINAL ARTICLE Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis John M. DelGaudio, MD; Ron E. Swain Jr, MD; Todd T. Kingdom, MD; Susan Muller, DMD; Patricia A. Hudgins, MD Objective:
ORIGINAL ARTICLE Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis John M. DelGaudio, MD; Ron E. Swain Jr, MD; Todd T. Kingdom, MD; Susan Muller, DMD; Patricia A. Hudgins, MD Objective:
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017
 Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Syndromes of invasive fungal sinusitis
 Medical Mycology 2009, 47 (Supplement 1), S309S314 Syndromes of invasive fungal sinusitis RICHARD D. DESHAZO University of Mississippi Medical Center, Department of Medicine, Jackson, Mississippi, USA
Medical Mycology 2009, 47 (Supplement 1), S309S314 Syndromes of invasive fungal sinusitis RICHARD D. DESHAZO University of Mississippi Medical Center, Department of Medicine, Jackson, Mississippi, USA
Controversies surrounding categorization of fungal sinusitis
 Controversies surrounding categorization of fungal sinusitis Arunaloke Chakrabarti Professor,Department of Medical Microbiology Center for Advanced Research in Medical Mycology Postgraduate Institute of
Controversies surrounding categorization of fungal sinusitis Arunaloke Chakrabarti Professor,Department of Medical Microbiology Center for Advanced Research in Medical Mycology Postgraduate Institute of
Fungal Sinusitis: A Ten-Year Experience at King Abdulaziz University Hospital
 JKAU: Med. Sci., Vol. 20 No. 3, pp: 29-41 (2013 A.D. / 1434 A.H.) DOI: 10.4197/Med. 20-3.3 Fungal Sinusitis: A Ten-Year Experience at King Abdulaziz University Hospital Khalid B. Al-Ghamdi, MD, Almoaidbellah
JKAU: Med. Sci., Vol. 20 No. 3, pp: 29-41 (2013 A.D. / 1434 A.H.) DOI: 10.4197/Med. 20-3.3 Fungal Sinusitis: A Ten-Year Experience at King Abdulaziz University Hospital Khalid B. Al-Ghamdi, MD, Almoaidbellah
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
Mucor Mycosis maxilla with palatal destruction An Interesting Case Report with Literature Review
 ISSN 2250-0359 Volume 3 Issue 3.5 2013 Mucor Mycosis maxilla with palatal destruction An Interesting Case Report with Literature Review 1 Balasubramanian Thiagarajan 2 Venkatesan Ulaganathan 1 Stanley
ISSN 2250-0359 Volume 3 Issue 3.5 2013 Mucor Mycosis maxilla with palatal destruction An Interesting Case Report with Literature Review 1 Balasubramanian Thiagarajan 2 Venkatesan Ulaganathan 1 Stanley
Original Article Intracranial Aspergillus Fungal Granuloma: Local Experience
 Egyptian Journal of Neurosurgery Volume 31 / No. 2 / April June 2016 67-72 Original Article Intracranial Aspergillus Fungal Granuloma: Local Experience Tariq Elemam Awad* and Khaled Elsayed Mohamed Department
Egyptian Journal of Neurosurgery Volume 31 / No. 2 / April June 2016 67-72 Original Article Intracranial Aspergillus Fungal Granuloma: Local Experience Tariq Elemam Awad* and Khaled Elsayed Mohamed Department
Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications: A Case-Control Study
 The Scientific World Journal Volume 2013, Article ID 453297, 5 pages http://dx.doi.org/10.1155/2013/453297 Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications:
The Scientific World Journal Volume 2013, Article ID 453297, 5 pages http://dx.doi.org/10.1155/2013/453297 Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications:
Is the Classical Classification of Aspergillosis of the Paranasal Sinuses to non invasive and invasive still valid or not?
 Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Is the Classical Classification of Aspergillosis of the Paranasal Sinuses to non invasive and invasive still valid or not? Abdul Aziz Ashoor (FA-HNO)*
Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Is the Classical Classification of Aspergillosis of the Paranasal Sinuses to non invasive and invasive still valid or not? Abdul Aziz Ashoor (FA-HNO)*
Clinical study of fungal sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Waghray J. Int J Otorhinolaryngol Head Neck Surg. 28 Sep;4():7-32 http://www.ijorl.com pissn 24-929 eissn 24-937 Original Research
International Journal of Otorhinolaryngology and Head and Neck Surgery Waghray J. Int J Otorhinolaryngol Head Neck Surg. 28 Sep;4():7-32 http://www.ijorl.com pissn 24-929 eissn 24-937 Original Research
Actinomycosis and aspergillosis in the nose of a diabetic: A case report
 Volume 2 Issue 3 2012 ISSN 2250-0359 Actinomycosis and aspergillosis in the nose of a diabetic: A case report 1 Meenu Khurana Cherian 1*, Rajarajeswari 2 1 Department of ENT, Gulf Medical College Hospital
Volume 2 Issue 3 2012 ISSN 2250-0359 Actinomycosis and aspergillosis in the nose of a diabetic: A case report 1 Meenu Khurana Cherian 1*, Rajarajeswari 2 1 Department of ENT, Gulf Medical College Hospital
OSTEITIS IN CRS. Rhinology Chair Meeting presented by Amal Binhazza a
 OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
Invasive Aspergillosis Associated Bacterial Infection in the Nasal Septum After Sphenoid Sinus Surgery
 Case Report Korean J Otorhinolaryngol-Head Neck Surg 2018;61(10):541-5 / pissn 2092-5859 / eissn 2092-6529 https://doi.org/10.3342/kjorl-hns.2017.17657 Invasive Aspergillosis Associated Bacterial Infection
Case Report Korean J Otorhinolaryngol-Head Neck Surg 2018;61(10):541-5 / pissn 2092-5859 / eissn 2092-6529 https://doi.org/10.3342/kjorl-hns.2017.17657 Invasive Aspergillosis Associated Bacterial Infection
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
Histopathology of Nasal Masses
 ORIGINAL ARTICLE Histopathology of Nasal Masses 1 Hemant Chopra, 2 Kapil Dua, 3 Neha Chopra, 4 Vikrant Mittal AIJCR Histopathology of Nasal Masses 1 Professor and Head, Dayanand Medical College, Ludhiana,
ORIGINAL ARTICLE Histopathology of Nasal Masses 1 Hemant Chopra, 2 Kapil Dua, 3 Neha Chopra, 4 Vikrant Mittal AIJCR Histopathology of Nasal Masses 1 Professor and Head, Dayanand Medical College, Ludhiana,
Mucin-Related Rhinosinusitis YOUSEF ALJATHLANY ORL-HNS RESIDENT
 Mucin-Related Rhinosinusitis YOUSEF ALJATHLANY ORL-HNS RESIDENT Free PPT Click to add title This PowerPoint Template has clean and neutral design that can be adapted to any content and meets various market
Mucin-Related Rhinosinusitis YOUSEF ALJATHLANY ORL-HNS RESIDENT Free PPT Click to add title This PowerPoint Template has clean and neutral design that can be adapted to any content and meets various market
A descriptive study of the patients with orbital complication of acute and chronic sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ORIGINAL ARTICLE. Group Chandler Maloney. First Inflammatory oedema Preseptal cellulitis. Second Orbital Cellulitis Subperiosteal abscess
 ORBITAL MANIFESTATIONS OF SINUS DISEASE T. Jyothirmayi 1, V. Meenakshi 2, M. Deepika 3 HOW TO CITE THIS ARTICLE: T. Jyothirmayi, V. Meenakshi, M. Deepika. Orbital Manifestations of Sinus Disease. Journal
ORBITAL MANIFESTATIONS OF SINUS DISEASE T. Jyothirmayi 1, V. Meenakshi 2, M. Deepika 3 HOW TO CITE THIS ARTICLE: T. Jyothirmayi, V. Meenakshi, M. Deepika. Orbital Manifestations of Sinus Disease. Journal
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
ASPERGILLOSIS IN THE NON-NEUTROPENIC HOST
 ASPERGILLOSIS IN THE NON-NEUTROPENIC HOST Dr J Garbino University Hospital Geneva ASPERGILLOSIS IN THE NON-NEUTROPENIC HOST INTRODUCTION SWISS ASPERGILLOSIS SURVEY IN THE NON-NEUTROPENIC HOST Introduction
ASPERGILLOSIS IN THE NON-NEUTROPENIC HOST Dr J Garbino University Hospital Geneva ASPERGILLOSIS IN THE NON-NEUTROPENIC HOST INTRODUCTION SWISS ASPERGILLOSIS SURVEY IN THE NON-NEUTROPENIC HOST Introduction
Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases
 Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
An Update in the Management of Candidiasis
 An Update in the Management of Candidiasis Daniel B. Chastain, Pharm.D., AAHIVP Infectious Diseases Pharmacy Specialist Phoebe Putney Memorial Hospital Adjunct Clinical Assistant Professor UGA College
An Update in the Management of Candidiasis Daniel B. Chastain, Pharm.D., AAHIVP Infectious Diseases Pharmacy Specialist Phoebe Putney Memorial Hospital Adjunct Clinical Assistant Professor UGA College
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Chronic Invasive Fungal Granuloma A Diagnostic Dilemma in an Immunocompetent Host
 Case Report Iranian Journal of Otorhinolaryngology, Vol.28(1), Serial No.84, Jan 2016 Chronic Invasive Fungal Granuloma A Diagnostic Dilemma in an Immunocompetent Host Shrinivas S. Chavan 1, K.S. Bhople
Case Report Iranian Journal of Otorhinolaryngology, Vol.28(1), Serial No.84, Jan 2016 Chronic Invasive Fungal Granuloma A Diagnostic Dilemma in an Immunocompetent Host Shrinivas S. Chavan 1, K.S. Bhople
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Allergic Fungal Rhinosinusitis
 Allergic Fungal Rhinosinusitis My Published Experience 1999-2018 Prof. Surayie H Al Dousary Professor of Rhinology Rhinology research Chair Director KSU Rhinology fellowship Program Director KSU Rhinology
Allergic Fungal Rhinosinusitis My Published Experience 1999-2018 Prof. Surayie H Al Dousary Professor of Rhinology Rhinology research Chair Director KSU Rhinology fellowship Program Director KSU Rhinology
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
Juvenile Angiofibroma
 Juvenile Angiofibroma Disclaimer The pictures used in this presentation have been obtained from a number of sources. Their use is purely for academic and teaching purposes. The contents of this presentation
Juvenile Angiofibroma Disclaimer The pictures used in this presentation have been obtained from a number of sources. Their use is purely for academic and teaching purposes. The contents of this presentation
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 81/ Oct 08, 2015 Page 14240
 INCREASED INCIDENCE OF FUNGAL SINUSITIS IN COASTAL REGION: A CASE SERIES I. Arumugam 1, Jalagandeesh B 2, Ganesh Bala 3, Ishani Borah 4, Sandeep Jith 5 HOW TO CITE THIS ARTICLE: I. Arumugam, Jalagandeesh
INCREASED INCIDENCE OF FUNGAL SINUSITIS IN COASTAL REGION: A CASE SERIES I. Arumugam 1, Jalagandeesh B 2, Ganesh Bala 3, Ishani Borah 4, Sandeep Jith 5 HOW TO CITE THIS ARTICLE: I. Arumugam, Jalagandeesh
Recovery of non-invasive Aspergillus sinusitis by endoscopic sinus surgery*
 Rhinology, 35, 84 88, 1997 Recovery of non-invasive Aspergillus sinusitis by endoscopic sinus surgery* Sheen-Yie Fang Department of Otolaryngology, Faculty of Medicine, National Cheng Kung University,
Rhinology, 35, 84 88, 1997 Recovery of non-invasive Aspergillus sinusitis by endoscopic sinus surgery* Sheen-Yie Fang Department of Otolaryngology, Faculty of Medicine, National Cheng Kung University,
FUNGAL RHINOSINUSITIS: A RETROSPECTIVE ANALYSIS OF CLINICOPATHOLOGIC FEATURES AND TREATMENT OUTCOMES AT RAMATHIBODI HOSPITAL
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH FUNGAL RHINOSINUSITIS: A RETROSPECTIVE ANALYSIS OF CLINICOPATHOLOGIC FEATURES AND TREATMENT OUTCOMES AT RAMATHIBODI HOSPITAL Pannathat Soontrapa 1, Noppadol Larbcharoensub
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH FUNGAL RHINOSINUSITIS: A RETROSPECTIVE ANALYSIS OF CLINICOPATHOLOGIC FEATURES AND TREATMENT OUTCOMES AT RAMATHIBODI HOSPITAL Pannathat Soontrapa 1, Noppadol Larbcharoensub
MANAGEMENT OF HOSPITAL-ACQUIRED FUNGAL INFECTIONS
 MANAGEMENT OF HOSPITAL-ACQUIRED FUNGAL INFECTIONS Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine Numbers of Cases of Sepsis in the United States, According
MANAGEMENT OF HOSPITAL-ACQUIRED FUNGAL INFECTIONS Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine Numbers of Cases of Sepsis in the United States, According
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
Prophylaxis versus Diagnostics-driven approaches to treatment of Invasive fungal diseases. Y.L. Kwong Department of Medicine University of Hong Kong
 Prophylaxis versus Diagnostics-driven approaches to treatment of Invasive fungal diseases Y.L. Kwong Department of Medicine University of Hong Kong Pathogenic yeast Candida Cryptococcus Trichosporon Pathogenic
Prophylaxis versus Diagnostics-driven approaches to treatment of Invasive fungal diseases Y.L. Kwong Department of Medicine University of Hong Kong Pathogenic yeast Candida Cryptococcus Trichosporon Pathogenic
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
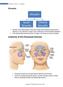 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
, Aspergillus A. terreus. 4 Candida albicans. 2 Otomycosis. , Histoplasmosis Paracoccidiomycosis
 Jpn. J. Med. Mycol. Vol. 44, 277 283, 2003 ISSN 0916 4804 1 2 2 1 2, Aspergillus A. terreus, A. flavus, A. niger, Candida,. A. terreus,, CT, fungus ball, drainage,, Key words: otolaryngologic mycosis,
Jpn. J. Med. Mycol. Vol. 44, 277 283, 2003 ISSN 0916 4804 1 2 2 1 2, Aspergillus A. terreus, A. flavus, A. niger, Candida,. A. terreus,, CT, fungus ball, drainage,, Key words: otolaryngologic mycosis,
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus
 Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Destructive Giant Maxillary Sinus Mucocele: A Case Report
 Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Head & Neck Clinical Sub Group. Network Agreed Imaging Guidelines for UAT and Thyroid Cancer. Measure Nos: 11-1C-105i & 11-1C-106i
 Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
A Prospective Clinical Study on Types and Diagnostic Criteria of Fungal Rhinosinusitis used in Tertiary Teaching Hospital of Telangana
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/247 A Prospective Clinical Study on Types and Diagnostic Criteria of Fungal Rhinosinusitis used in Tertiary Teaching
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/247 A Prospective Clinical Study on Types and Diagnostic Criteria of Fungal Rhinosinusitis used in Tertiary Teaching
ESCMID Online Lecture Library. by author. Salvage Therapy of Invasive Aspergillosis Refractory to Primary Treatment with Voriconazole
 Salvage Therapy of Invasive Aspergillosis Refractory to Primary Treatment with Voriconazole J.A. Maertens, hematologist, MD, PhD University Hospital Gasthuisberg Leuven, Belgium Current guidelines: first-line
Salvage Therapy of Invasive Aspergillosis Refractory to Primary Treatment with Voriconazole J.A. Maertens, hematologist, MD, PhD University Hospital Gasthuisberg Leuven, Belgium Current guidelines: first-line
ENT Infections. Case 1. Diagnosis. Marlene L. Durand, M.D. Mass. General Hospital Mass. Eye & Ear Infirmary
 ENT Infections Marlene L. Durand, M.D. Mass. General Hospital Mass. Eye & Ear Infirmary Case 1 18 yr-old patient presents with L eyelid swelling, redness, and pain. He was well until 10 days ago, when
ENT Infections Marlene L. Durand, M.D. Mass. General Hospital Mass. Eye & Ear Infirmary Case 1 18 yr-old patient presents with L eyelid swelling, redness, and pain. He was well until 10 days ago, when
Oliver A. Cornely. Department I for Internal Medicine Haematology / Oncology / Infectious Diseases / Intensive Care 2. Centre for Clinical Research
 Management of Confirmed Aspergillosis Oliver A. Cornely 1 Department I for Internal Medicine Haematology / Oncology / Infectious Diseases / Intensive Care 2 Centre for Clinical Research University of Cologne
Management of Confirmed Aspergillosis Oliver A. Cornely 1 Department I for Internal Medicine Haematology / Oncology / Infectious Diseases / Intensive Care 2 Centre for Clinical Research University of Cologne
Introduction. Ophthalmic manifestations can result from a myriad of Non Sinogenic and Sinogenic Disease :
 Ophthalmic Manifestations of Paranasal Sinus Disease; A Clinical Grading System Surayie Al Dousary, MD Associate Professor Director Rhinology Research Chair & Fatma Al Anazy, MD Associate Professor Rhinology
Ophthalmic Manifestations of Paranasal Sinus Disease; A Clinical Grading System Surayie Al Dousary, MD Associate Professor Director Rhinology Research Chair & Fatma Al Anazy, MD Associate Professor Rhinology
ISSN: Volume 4 Issue CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS
 ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
Clinical analysis of 29 cases of nasal mucosal malignant melanoma
 1166 Clinical analysis of 29 cases of nasal mucosal malignant melanoma HUANXIN YU and GANG LIU Department of Otorhinolaryngology Head and Neck Surgery, Tianjin Huanhu Hospital, Tianjin 300060, P.R. China
1166 Clinical analysis of 29 cases of nasal mucosal malignant melanoma HUANXIN YU and GANG LIU Department of Otorhinolaryngology Head and Neck Surgery, Tianjin Huanhu Hospital, Tianjin 300060, P.R. China
Successful Treatment of Two Cases of Invasive Aspergillus Sinusitis With Voriconazole
 TZU CHI MED J June 2010 Vol 22 No 2 available at http://www.tzuchimedjnl.com/ Tzu Chi Medical Journal Case Report Successful Treatment of Two Cases of Invasive Aspergillus Sinusitis With Voriconazole Chen-Hao
TZU CHI MED J June 2010 Vol 22 No 2 available at http://www.tzuchimedjnl.com/ Tzu Chi Medical Journal Case Report Successful Treatment of Two Cases of Invasive Aspergillus Sinusitis With Voriconazole Chen-Hao
Condition First line Alternative Comments Candidemia Nonneutropenic adults
 Recommendations for the treatment of candidiasis. Clinical Practice Guidelines for the Management of Candidiasis: 2009 Update by the Infectious Diseases Society of America. Condition First line Alternative
Recommendations for the treatment of candidiasis. Clinical Practice Guidelines for the Management of Candidiasis: 2009 Update by the Infectious Diseases Society of America. Condition First line Alternative
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
Outline. Sinonasal Endoscopic Surgery 6/1/2011
 Kathleen Kthl T. Montone, M.D. Department of Pathology and Laboratory Medicine University of Pennsylvania Outline Evaluation of sinonasal ethmoidectomy specimens. Overview of Sinonasal fungal diseases
Kathleen Kthl T. Montone, M.D. Department of Pathology and Laboratory Medicine University of Pennsylvania Outline Evaluation of sinonasal ethmoidectomy specimens. Overview of Sinonasal fungal diseases
Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p
 Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Common Fungi. Catherine Diamond MD MPH
 Common Fungi Catherine Diamond MD MPH Birth Month and Day & Last Four Digits of Your Cell Phone # BEFORE: http://tinyurl.com/kvfy3ts AFTER: http://tinyurl.com/lc4dzwr Clinically Common Fungi Yeast Mold
Common Fungi Catherine Diamond MD MPH Birth Month and Day & Last Four Digits of Your Cell Phone # BEFORE: http://tinyurl.com/kvfy3ts AFTER: http://tinyurl.com/lc4dzwr Clinically Common Fungi Yeast Mold
Successful treatment of larynxtracheobronchial-pulmonary
 Case Report Successful treatment of larynxtracheobronchial-pulmonary aspergillosis in an immunocompetent host W.X. Qu, X.W. Feng and L. Zhao The First Respiratory Department of Shengjing Hospital, China
Case Report Successful treatment of larynxtracheobronchial-pulmonary aspergillosis in an immunocompetent host W.X. Qu, X.W. Feng and L. Zhao The First Respiratory Department of Shengjing Hospital, China
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Rhinosinusitis: A Prospective Study
 االله الرحمن الرحيم بسم Pathological l & Radiological i l Evidences in the Pathogenesis es s of Chronic Rhinosinusitis: A Prospective Study Prof. Dr. H. ABDEL FATAH, MD A. Prof. Dr. K. NOWEAM, MD Dr. Z.
االله الرحمن الرحيم بسم Pathological l & Radiological i l Evidences in the Pathogenesis es s of Chronic Rhinosinusitis: A Prospective Study Prof. Dr. H. ABDEL FATAH, MD A. Prof. Dr. K. NOWEAM, MD Dr. Z.
International Journal of Research and Review E-ISSN: ; P-ISSN:
 International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Incidence of Fungal Rhinosinusitis in Bihar and Its Management Shelendra
International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Incidence of Fungal Rhinosinusitis in Bihar and Its Management Shelendra
Apophysomyces elegans Caused Rhino-Orbito Mucormycosis: An Emerging Infection in Immunocompetent Individuals
 JMID/ 2017; 7 (4):207-212 Journal of Microbiology and Infectious Diseases doi: 10.5799/jmid.369276 CASE REPORT Apophysomyces elegans Caused Rhino-Orbito Mucormycosis: An Emerging Infection in Immunocompetent
JMID/ 2017; 7 (4):207-212 Journal of Microbiology and Infectious Diseases doi: 10.5799/jmid.369276 CASE REPORT Apophysomyces elegans Caused Rhino-Orbito Mucormycosis: An Emerging Infection in Immunocompetent
HAEMATOLOGY ANTIFUNGAL POLICY
 HAEMATOLOGY ANTIFUNGAL POLICY PROPHYLAXIS Primary Prophylaxis Patient Group Patients receiving intensive remissioninduction chemotherapy for Acute Leukaemia (excluding patients receiving vinca alkaloids)
HAEMATOLOGY ANTIFUNGAL POLICY PROPHYLAXIS Primary Prophylaxis Patient Group Patients receiving intensive remissioninduction chemotherapy for Acute Leukaemia (excluding patients receiving vinca alkaloids)
Medical Management of Fungal Sinusitis
 ISSN: 2250-0359 Volume 3 Supplement 2 2013 Medical Management of Fungal Sinusitis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Medical therapy constitutes an useful
ISSN: 2250-0359 Volume 3 Supplement 2 2013 Medical Management of Fungal Sinusitis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Medical therapy constitutes an useful
A Rare case of Tubercular Gingivitis Case Report
 Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
Cigna Drug and Biologic Coverage Policy
 Cigna Drug and Biologic Coverage Policy Subject Voriconazole Effective Date... 3/15/2018 Next Review Date... 3/15/2019 Coverage Policy Number... 4004 Table of Contents Coverage Policy... 1 General Background...
Cigna Drug and Biologic Coverage Policy Subject Voriconazole Effective Date... 3/15/2018 Next Review Date... 3/15/2019 Coverage Policy Number... 4004 Table of Contents Coverage Policy... 1 General Background...
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Aspergillus species. The clinical spectrum of pulmonary aspergillosis
 Pentalfa 3 maart 2016 The clinical spectrum of pulmonary aspergillosis Pascal Van Bleyenbergh, Pneumologie UZ Leuven Aspergillus species First described in 1729 * >250 species * ubiquitous Inhalation of
Pentalfa 3 maart 2016 The clinical spectrum of pulmonary aspergillosis Pascal Van Bleyenbergh, Pneumologie UZ Leuven Aspergillus species First described in 1729 * >250 species * ubiquitous Inhalation of
Isolated sphenoid inflammatory diseases
 International Journal of Otorhinolaryngology and Head and Neck Surgery http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original Research Article DOI: http://dx.doi.org/10.18203/issn.2454-5929.ijohns20183688
International Journal of Otorhinolaryngology and Head and Neck Surgery http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original Research Article DOI: http://dx.doi.org/10.18203/issn.2454-5929.ijohns20183688
Allergic Fungal Rhinosinusitis in Patients with Nasal Polyposis
 Iraqi JMS Published by Al-Nahrain College of Medicine P-ISSN 1681-6579 E-ISSN 2224-4719 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-alnahrain.edu.iq http://www.iraqijms.net Allergic Fungal
Iraqi JMS Published by Al-Nahrain College of Medicine P-ISSN 1681-6579 E-ISSN 2224-4719 Email: iraqijms@colmed-alnahrain.edu.iq http://www.colmed-alnahrain.edu.iq http://www.iraqijms.net Allergic Fungal
Antifungal Agents - Cresemba (isavuconazonium), Vfend. Prior Authorization Program Summary
 Antifungal Agents - Cresemba (isavuconazonium), Noxafil (posaconazole), Vfend (voriconazole) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2,14 Drug FDA Indication(s) Dosing Cresemba
Antifungal Agents - Cresemba (isavuconazonium), Noxafil (posaconazole), Vfend (voriconazole) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2,14 Drug FDA Indication(s) Dosing Cresemba
Acute invasive fungal rhinosinusitis: our experience with 18 cases
 DOI 10.1007/s00405-016-4109-z RHINOLOGY Acute invasive fungal rhinosinusitis: our experience with 18 cases Mehdi Bakhshaee 1 Amin Bojdi 2 Abolghasem Allahyari 3 Mohammad Reza Majidi 4 Sherwin Tavakol 5
DOI 10.1007/s00405-016-4109-z RHINOLOGY Acute invasive fungal rhinosinusitis: our experience with 18 cases Mehdi Bakhshaee 1 Amin Bojdi 2 Abolghasem Allahyari 3 Mohammad Reza Majidi 4 Sherwin Tavakol 5
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE
 INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE RHINOCEREBRAL MUCORMYCOSIS DUE TO RHIZOPUS IN A RECENTLY DIAGNOSED DIABETIC FEMALE: A CASE REPORT KULKARNI KV 1, PATHAK NP 2 1. Assistant
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE RHINOCEREBRAL MUCORMYCOSIS DUE TO RHIZOPUS IN A RECENTLY DIAGNOSED DIABETIC FEMALE: A CASE REPORT KULKARNI KV 1, PATHAK NP 2 1. Assistant
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases.
 Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
An estimated 1.5 million fungal species inhabit Earth, with the
 NARAC Review The role of fungi in diseases of the nose and sinuses Zachary M. Soler M.D., M.Sc., and Rodney J. Schlosser, M.D. ABSTRACT Background: Human exposure to fungal elements is inevitable, with
NARAC Review The role of fungi in diseases of the nose and sinuses Zachary M. Soler M.D., M.Sc., and Rodney J. Schlosser, M.D. ABSTRACT Background: Human exposure to fungal elements is inevitable, with
STUDY OF CORRELATION BETWEEN NASAL ENDOSCOPY AND RHINOGENIC HEADACHE Santhosha Kumar B 1, Manjunath Rao S. V 2
 STUDY OF CORRELATION BETWEEN NASAL ENDOSCOPY AND RHINOGENIC HEADACHE Santhosha Kumar B 1, Manjunath Rao S. V 2 HOW TO CITE THIS ARTICLE: Santhosha Kumar B, Manjunath Rao S. V. Study of Correlation between
STUDY OF CORRELATION BETWEEN NASAL ENDOSCOPY AND RHINOGENIC HEADACHE Santhosha Kumar B 1, Manjunath Rao S. V 2 HOW TO CITE THIS ARTICLE: Santhosha Kumar B, Manjunath Rao S. V. Study of Correlation between
14.25 UBC SINUS & SKULL BASE COURSE 2018 STANDARD COURSE : AUG (FRI-SAT) SKULL BASE COURSE : AUG 12 (SUN) ubccpd.ca CESEI CENTRE VANCOUVER, BC
 14.25 MOC SECTION 1 UBC SINUS & SKULL BASE COURSE 2018 STANDARD COURSE : AUG 10 11 (FRI-SAT) SKULL BASE COURSE : AUG 12 (SUN) CESEI CENTRE VANCOUVER, BC WHO SHOULD ATTEND Surgeons Advanced Trainees Fellows
14.25 MOC SECTION 1 UBC SINUS & SKULL BASE COURSE 2018 STANDARD COURSE : AUG 10 11 (FRI-SAT) SKULL BASE COURSE : AUG 12 (SUN) CESEI CENTRE VANCOUVER, BC WHO SHOULD ATTEND Surgeons Advanced Trainees Fellows
Four cases of Pleomorphic Adenoma of the nasal cavity: An unusual entity
 J. Acad. Indus. Res. Vol. 1(4) September 2012 203 RESEARCH ARTICLE ISSN: 2278-5213 Four cases of Pleomorphic Adenoma of the nasal cavity: An unusual entity Kiran Naik Dept. of ENT, Adichunchanagiri Inst.
J. Acad. Indus. Res. Vol. 1(4) September 2012 203 RESEARCH ARTICLE ISSN: 2278-5213 Four cases of Pleomorphic Adenoma of the nasal cavity: An unusual entity Kiran Naik Dept. of ENT, Adichunchanagiri Inst.
Retrospective Analysis of Patients with Allergy Sinusitis
 Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
POST-DOCTORAL FELLOWSHIP PROGRAMME IN RHINOLOGY
 POST-DOCTORAL FELLOWSHIP PROGRAMME IN RHINOLOGY DURATION OF THE COURSE : 2 YEARS Aim of the Course To provide a broad experience in surgical and evaluative Rhinology. Background: Rhinology is an area of
POST-DOCTORAL FELLOWSHIP PROGRAMME IN RHINOLOGY DURATION OF THE COURSE : 2 YEARS Aim of the Course To provide a broad experience in surgical and evaluative Rhinology. Background: Rhinology is an area of
BJORL Retrospective analysis of 26 cases of inverted nasal papillomas
 Braz J Otorhinolaryngol. 2012;78(1):26-30. ORIGINAL ARTICLE BJORL Retrospective analysis of 26 cases of inverted nasal papillomas Ana Maria Almeida de Sousa 1, Alcioni Boldrini Vicenti 2, José Speck Filho
Braz J Otorhinolaryngol. 2012;78(1):26-30. ORIGINAL ARTICLE BJORL Retrospective analysis of 26 cases of inverted nasal papillomas Ana Maria Almeida de Sousa 1, Alcioni Boldrini Vicenti 2, José Speck Filho
A CONTRIBUTION TO THE ETIOPATHOGENESIS, DIAGNOSIS AND MANAGEMENT OF SINONASAL INVERTED PAPILLOMAS
 UNIVERSITY OF MEDICINE AND PHARMACY OF TÂRGU MUREȘ ROMANIA A CONTRIBUTION TO THE ETIOPATHOGENESIS, DIAGNOSIS AND MANAGEMENT OF SINONASAL INVERTED PAPILLOMAS PhD THESIS ABSTRACT PhD Student Viorel Emanoil
UNIVERSITY OF MEDICINE AND PHARMACY OF TÂRGU MUREȘ ROMANIA A CONTRIBUTION TO THE ETIOPATHOGENESIS, DIAGNOSIS AND MANAGEMENT OF SINONASAL INVERTED PAPILLOMAS PhD THESIS ABSTRACT PhD Student Viorel Emanoil
ECMM Excellence Centers Quality Audit
 ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
The Incidence of Concha Bullosa and Its Association with Chronic Rhinosinusitis Deviated Nasal Septum and Osteomeatal Complex Obstruction
 1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 The Incidence of Concha Bullosa and Its Association with Chronic Rhinosinusitis Deviated Nasal Septum and Osteomeatal Complex Obstruction Fatma
1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 The Incidence of Concha Bullosa and Its Association with Chronic Rhinosinusitis Deviated Nasal Septum and Osteomeatal Complex Obstruction Fatma
Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction
 1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
Nasal Polyposis. DEPARTMENT OF ENT K.S.Hegde Medical Academy Deralakatte, Mangalore
 Nasal Polyposis DEPARTMENT OF ENT K.S.Hegde Medical Academy Deralakatte, Mangalore Def: INTRODUCTION Chronic inflammatory disease of the mucous membrane in the nose & PNS, presenting as pedunculated smooth
Nasal Polyposis DEPARTMENT OF ENT K.S.Hegde Medical Academy Deralakatte, Mangalore Def: INTRODUCTION Chronic inflammatory disease of the mucous membrane in the nose & PNS, presenting as pedunculated smooth
Chronic pulmonary aspergillosis diagnosis and management in resource-limited setting
 Chronic pulmonary aspergillosis diagnosis and management in resource-limited setting Professor Retno Wahyuningsih Professor of Medical Mycology Department of Parasitology, Faculty of Medicine Universitas
Chronic pulmonary aspergillosis diagnosis and management in resource-limited setting Professor Retno Wahyuningsih Professor of Medical Mycology Department of Parasitology, Faculty of Medicine Universitas
Allergic fungal rhinosinusitis a new staging system*
 ORIGINAL CONTRIBUTION Rhinology 49: 318-323, 2011 Allergic fungal rhinosinusitis a new staging system* Carl M. Philpott 1,2, Allan Clark 2, Amin R. Javer 1 1 St Paul s Sinus Centre, Vancouver, British
ORIGINAL CONTRIBUTION Rhinology 49: 318-323, 2011 Allergic fungal rhinosinusitis a new staging system* Carl M. Philpott 1,2, Allan Clark 2, Amin R. Javer 1 1 St Paul s Sinus Centre, Vancouver, British
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
The ROLE OF ALPHINTERN IN TREATMENT OF NASAL POLYPOSIS
 The ROLE OF ALPHINTERN IN TREATMENT OF NASAL POLYPOSIS Prospective study was performed on patients diagnosed as chronic nasalpolyposis who referred to ENT clinic, Benghazi medical center, Benghazi- Libya
The ROLE OF ALPHINTERN IN TREATMENT OF NASAL POLYPOSIS Prospective study was performed on patients diagnosed as chronic nasalpolyposis who referred to ENT clinic, Benghazi medical center, Benghazi- Libya
