THE USE OF NEUROIMAGING IN THE MANAGEMENT OF CHRONIC HEADACHE IN CHILDREN IN CLINICAL PRACTICE VERSUS CLINICAL PRACTICE GUIDELINES
|
|
|
- Heather Williamson
- 5 years ago
- Views:
Transcription
1 Acta Clin Croat 2014; 53: Professional Paper THE USE OF NEUROIMAGING IN THE MANAGEMENT OF CHRONIC HEADACHE IN CHILDREN IN CLINICAL PRACTICE VERSUS CLINICAL PRACTICE GUIDELINES Igor Prpić 1, Tea Ahel 2, Krešimir Rotim 3, Domagoj Gajski 4, Petar Vukelić 1 and Antun Sasso 1 1 Clinical Department of Pediatrics, Rijeka University Hospital Center, School of Medicine, University of Rijeka; 2 Emergency Medicine Institute of Primorje-Gorski Kotar County, Rijeka; 3 Clinical Department of Neurosurgery, Sestre milosrdnice University Hospital Center; 4 Department of Anatomy and Physiology, University of Applied Health Sciences, Zagreb, Croatia SUMMARY In daily practice, neuroimaging studies are frequently performed for the management of childhood headache. The aim of this study was to determine whether there is significant discrepancy between clinical practice and clinical practice guidelines on the indications for neuroimaging studies. Medical records of children with chronic headache, aged 2 to 18 years and treated at Rijeka University Hospital Center, Kantrida Department of Pediatrics, were retrospectively reviewed. Indications for brain magnetic resonance imaging and computed tomography (MRI/CT) scanning were reviewed and compared with clinical practice guidelines. Brain imaging was performed in 164 (76.3%) of 215 children, MRI in 93 (56.7%) and CT in 71 (43.3%) children. Indications for brain MRI/CT were as follows: anxiety and/or insistence by the child s family (71.3%), presence of associated features suggesting neurologic dysfunction (13.4%), age under 5 years (12.8%) and abnormal neurologic examination (2.4%). The majority of children (71.4%) had normal neuroimaging findings. In the rest of imaging studies (28.1%), MRI/CT revealed different intracerebral/extracerebral findings not influencing changes in headache management. Only one (0.60%) patient required change in headache management after MRI/CT. Study results proved that, despite available evidence-based clinical guidelines, brain imaging in children with chronic headaches is overused, mostly in order to decrease anxiety of the family/patient. Key words: Children; Headache; Neuroimaging; Practice guidelines Introduction Headache is the most common neurological disorder and a frequent complaint in children and adolescents. Epidemiological studies reveal different data on the incidence of childhood headaches depending on diagnostic criteria, studied population and study duration 1-3. However, most clinicians agree that the Correspondence to: Prof. Igor Prpić, MD, PhD, Clinical Department of Pediatrics, Rijeka University Hospital Center, Istarska 43, HR Rijeka, Croatia igor.prpic@medri.uniri.hr Received April 9, 2014, accepted October 7, 2014 prevalence of childhood headaches increases with age. According to some studies, it ranges from 37% to 51% in 7-year-olds, gradually increasing to 57% to 82% by the age of 15 years 4-6. By the age of 16 years, more than 90% of all adolescents have already experienced at least one episode of intense headache 7. Consequently, the management of children with headache makes a major component of daily pediatric practice. Diagnosis of headache disorders in children rests mostly on clinical criteria as defined by the International Headache Society (IHS) 8. Most children have primary headache disorders such as migraine or tension-type headaches 1,9,10. Secondary headache disor- Acta Clin Croat, Vol. 53, No. 4,
2 ders, although much less common, can be due to various etiologies, which can range from relatively benign to life-threatening 10. Therefore, the accurate diagnosis of headache is crucial for successful management and treatment and represents a real challenge for everyday pediatric practice. For that reason, several clinical practice guidelines have been developed for the management of childhood headache According to these, thorough medical history followed by methodical physical and neurological examination is considered sufficient to exclude the possible secondary causes of headache. Even so, neuroimaging studies, such as magnetic resonance imaging (MRI) and computed tomography (CT), are still frequently performed in children with headache Hence, the purpose of our study was to determine whether there is significant discrepancy between clinical practice and clinical practice guidelines in the management of chronic headache in children, primarily considering indications for neuroimaging studies. Subjects and Methods Medical records of children admitted due to headache to the Rijeka University Hospital Center, Kantrida Clinical Department of Pediatrics, during the period were retrospectively reviewed. All children were referred by a primary care pediatrician to a pediatric neurology outpatient clinic for additional evaluation. The study focused on children aged from 2 to 18 years with chronic headache defined as headaches present for at least 3 months and persisting for more than or equal to 15 days per month 8. Children whose headache was associated with recent traumatic brain injury or who had previous diagnosis of hydrocephalus, significant neurodevelopmental disorder or neurocutaneous syndrome were excluded. Children diagnosed with any other type of headache were excluded from the study too. Medical records were reviewed regarding clinical indications for MRI/CT studies and imaging results. Indications used for MRI/CT scanning were defined and compared to those recommended by the current clinical practice guidelines for the management of chronic headache in children 11. Clinical indications for performing neuroimaging studies, according to established guidelines, were clustered in two groups: 1) abnormal neurological examination (focal deficit, clear signs of increased intracranial pressure, alteration of consciousness); and 2) associated features that suggest neurological dysfunction (morning vomiting, nausea, dizziness, worst headache ). Moreover, we added anxiety and/or insistence of children s families and age under 5 years in neurologically intact children as separate indications for neuroimaging studies. Neuroimaging results were presented as normal, incidental or abnormal. Abnormal neuroimaging findings were defined as pathologic neuroanatomic findings that resulted in significant change in the child s clinical management. Incidental findings were any remarks, observations revealed by neuroradiologist of unexpected, incidental detection that was believed to be unrelated to the child presenting headache symptoms and did not require any significant change in the child s headache management. Incidental findings were divided into intracerebral or extracerebral. For data interpretation we used frequencies (real numbers and percentage). Results Patient characteristics Two-hundred and fifteen patients were admitted to the hospital due to chronic headache. The subjects age ranged from 2 to 18 years, mean age 11 years, median 12; there were 100 (46.5%) male children, mean age 9.7 years and 115 (53.5%) female children, mean age 11.8 years. The majority of patients, 168/215 (78.1%), had general physical and neurological examination, as well as past medical history unremarkable. There were 4/215 (1.9%) children with abnormal neurological examination; 22/215 (10.2%) children with the presence of associated features suggesting neurological dysfunction, and 21/215 (9.8%) children aged under 5 years (Table 1). In four patients with altered neurological status, the following abnormalities were described: diplopia, motor and gait dysfunction, alteration of consciousness, speech impediment, horizontal nystagmus, asymmetry of deep tendon reflexes, and unilateral hand tremor. Associated features suggesting neurological dysfunction included nonspecific vision disturbances such as blurred vision, impaired visual acuity, un- 450 Acta Clin Croat, Vol. 53, No. 4, 2014
3 Table 1. Indications for neuroimaging procedures and neuroimaging findings in children with chronic daily headache Family insistence Neuroimaging indications Abnormal neurologic examination Possible neurologic dysfunction Age <5 years Neuroimaging results n % n % n % n % N % Normal findings Incidental findings Abnormal findings Total Total specific optic fundus examination in 13/215 (6.0%) children, nausea and/or vomiting and/or dizziness in 7/215 (3.3%) children, and unilateral facial numbness in 2/215 (0.9%) children. Neuroimaging results Brain imaging was performed in 164/215 (76.3%) children. MRI was performed in 93 (56.7%) and CT in 71 (43.3%) children. Indications for neuroimaging studies as well as neuroimaging results are presented in Table 1. In the great majority of children, 117/164 (71.3%), neuroimaging studies were performed upon insistence and/or due to concern of their families because of the associated features suggesting neurological dysfunction (13.4%), age under 5 years (12.8%) and abnormal neurological examination (2.4%). Most of the children (117/164; 71.3%) had normal neuroimaging findings. In 46/164 (28.1%) children, MRI/CT results were incidental, i.e. different intracerebral/extracerebral findings revealed asymmetry of the ventricular system, enlargement of cisterna magna and retrocerebellar cistern, foci of gliosis, pineal and/or subarachnoid cyst, calcification of falx cerebri, cortical atrophy, white matter hyperintensities, sinusitis, adenoid enlargement and fluid retention in mastoid cells, which did not influence changes in headache management. Only one child (1/164=0.6%) in which MRI revealed brain tumor required change in headache management after brain imaging. This child demonstrated abnormal neurological examination on the day of presentation (balance disturbances, motor asymmetry and asymmetry of deep tendon reflexes). Discussion Routine clinical practice of neuropediatricians clearly shows that neuroimaging studies have a limited value in children with chronic headache. These observations have been comprehensively investigated and discussed during the past decades Consequently, recommendations for the use of neuroimaging have been established in clinical practice guidelines on the basis of the principles of evidence-based medicine 11. According to these, obtaining a neuroimaging study on a routine basis is not indicated in children with recurrent headaches and normal neurological examination. The practice guidelines do not differentiate children with recurrent headache younger than 5 years as a specific group of patients, nor are the recommendations altered by the child s age. Headache in young children may not always meet the usual diagnostic criteria and a higher percentage of children aged 2 to 5 years have a life-threatening cause of headache when compared with older children 12. Moreover, dangerous headache caused by brain tumors may be more common in this population and requires prompt specific management. Therefore, diagnostic approach to this group of children is of great importance and requires specific reflections, thus neuroimaging should also be justifiably considered in these patients. Our Department routine in children with headache is to obtain detailed history, perform complete systemic physical examination including arterial blood pressure measurement, detailed neurological examination, complete ophthalmologic examination, Acta Clin Croat, Vol. 53, No. 4,
4 ear-nose-throat specialist examination as well as psychological evaluation. Electroencephalogram was also usually performed. Our routine is to perform neuroimaging studies after a clinical follow up of maximum one month in children younger than 5 years with normal neurological examination and no associated features indicative of neurological dysfunction. Using this approach in this series of children we treated 21 (12.8%) children with headache younger than 5 years with normal neurological examination and no associated features suggesting neurological dysfunction. All children had normal MRI/CT findings (19 children had normal and two incidental findings), i.e. we did not detect any pathology that would require significant change in headache management. Therefore, our results suggest that the routine use of MRI/CT is not warranted in preschool children with normal neurological examination, with no associated features indicative of neurological dysfunction and with clearly defined headache type. Even these results confirm conclusions of similar studies that only prospective study in this specific age group of children would give a definite answer regarding neuroimaging use in young children with headache. We performed MRI/CT in 76.3% of children, meaning that in daily clinical practice neuroimaging studies are not only performed to exclude intracranial pathology. CT scan was mostly performed because parents insisted on it, even though they knew that it was not healthy for their children. Our data are consistent with other reports where the rates of neuroimaging studies in children with chronic headache ranged from 35% to 81% 16,18. In the present study, true indications for obtaining neuroimaging studies, such as the presence of neurological abnormalities and atypical headache pattern suggesting neurological dysfunction, were established in four (2.4%) and 22 (13.4%) children, respectively (26 children; 15.8%). In the remaining patients (71.3%), excluding those younger than 5 years, brain MRI/CT was obtained due to the parents concern about a serious underlying brain disease, mostly brain tumor. The incidence of brain tumors is low, 3-5 per 100,000. Moreover, only 1 of 10 children present with headache as the only symptom. In our series of 82 children with primary brain tumors, the most prominent symptoms were vomiting or vomiting with headache, and all children had abnormal neurological examination 20,21. Morris et al. in their meta-analysis regarding incidental findings on brain MRI have shown that 0.7% of people (135 of ) were found to have incidental neoplastic brain findings 22. In our study, only one of 164 children imaged for headache was found to have brain tumor, yielding 0.6%, a rate that is even lower than the rate in healthy people. Moreover, none of the children with normal neurological examination had neuroimaging studies that required change in headache management. The child with the brain tumor presented to the Department with evident and recognizable neurological signs of posterior intracranial pathology. It is very rare that a child has brain tumor that is unpredictable by thorough clinical assessment and ophthalmologic examination. It is important to mention that delay in the diagnosis of brain tumor in children does not decrease the probability of survival 23. Our results showed that 28.1% of children had some sort of intracerebral or extracerebral findings on neuroimaging studies. Most of these findings were incidental and required neither significant nor any change in headache management at all. Intracerebral findings were generally physiological variations of brain anatomical structures. When using modern sequences, incidental findings of intracerebral alterations were relatively high 24,25. Depending on the criteria for incidental findings and studied populations, their incidence ranged from 20% do 50% 26,27. However, in a very low percentage of children (0.3% to 3.8%), the incidental findings described were relevant to headache The most common extracerebral findings in our series were sinusitis, adenoid enlargement and fluid retention in mastoid cells. Sinus disease has been previously reported in 1% to 13% of patients imaged for headache Whether these findings had a significant clinical implication on headache remains to be found out. Our practice is to refer patient to otolaryngologist when neuroimaging studies show any alteration in sinuses, mastoid cells or nose. By experience, in extremely rare cases, these children received antibiotic or other specific therapy. By our practice, incidental neuroimaging findings in children with chronic headache, whether intra- or extracerebral, usually increase the parental/family 452 Acta Clin Croat, Vol. 53, No. 4, 2014
5 fear and anxiety rather than providing them with reconciliation. Furthermore, all extensive blood tests, cerebrospinal fluid tests, repeated neuroimaging studies in children without clinical and history specific diseases but with incidental MRI/CT findings revealed no specific pathology Each neuropediatrician can find valid and reasonable reasons to disrespect practice guidelines after weighing estimated benefits against the potential risks, harms and costs in individual child s surroundings. In practice, pediatricians usually take into account their personal experience and expertise with evidence-based guidelines in decision-making on behalf of their particular patients. In this study, neuroimaging was performed in 71.3% of children without any indications proposed by the valid clinical guidelines. If we add the children younger than 5 years, that will make 138/164 or 84% of children who were exposed to unnecessary diagnostic procedures. This defensive medicine was also noted in other studies Yilmaz et al. report on a series of 449 children with headache where neuroimaging studies were performed in 72.2% of children and the indication for MRI were parental anxiety about brain tumors in 81.8% of patients 16. Plausible reasons for overuse of pediatric neuroimaging procedures may be pediatrician s judgment/ behavior such as time constraints in primary care practice, pediatrician s anxiety (fear of liability), unreliable history/examination, indoctrination of imaging technology use, misunderstanding of appropriateness of the guidelines, false belief in the need of documentation, delayed availability of neurology consultation, and financial/reimbursement incentives 14. On the other hand, even parental expectations or demands must be taken into account, i.e. parental anxiety as fear from brain tumor, exaggeration of pain severity, parental reassurance (i.e. anxiolytic use of technology), mistrust in physician reassurance, direct-to-consumer marketing of imaging centers, or medicalization of the childhood stress phenomena 14. This study was performed at a single institution, regional children s hospital that serves a large urban, suburban and rural area. Two pediatric neurologists worked at the Department during the study period. The Department is the main center for pediatric neurology, and there were no pediatric neurologists in practice in the area. The great majority of children presented with headache, therefore were seen by a neuropediatrician, and these results represent the institution experience. A limitation of this study is retrospective design and lack of prospective clinical follow up data after neuroimaging study was performed. Possibly, in that manner, we may be able to prove that in some cases neuroimaging studies serve not only as a diagnostic method, but also as a therapeutic procedure. Even so, this study proved that, despite available evidence-based clinical guidelines, brain imaging in children with chronic headaches is overused, mostly in order to decrease the family/patient concerns. It is of utmost importance that the parents who insist on neuroimaging procedure be aware of the possibility of a high chance of discovering incidental findings, which does not and will not negatively influence their child s health. Physicians should devote more time to explaining the nature of the headache to patients and families, thus reducing their anxiety. References 1. Brna PM, Dooley JM. Headaches in the pediatric population. Semin Pediatr Neurol 2006;13: Pogliani L, Spiri D, Penagini F, et al. Headache in children and adolescents aged 6-18 years in northern Italy: prevalence and risk factors. Eur J Paediatr Neurol 2011;15: Sillanpaa M. Prevalence of headache in prepuberty. Headache 1983;23: Liner MS, Stewart WF, Celentano DD, Ziegler D, Sprecher M. An epidemiologic study of headache among adolescents and young adults. JAMA 1989;261: Stewart WF, Linet MS, Celentano DD, Van Natta M, Siegler D. Age- and sex-specific incidence rates of migraine with and without visual aura. Am J Epidemiol 1991;34: Karli N, Akis N, Zarifoglu M, et al. Headache prevalence in adolescents aged 12 to 17: a student based epidemiological study in Bursa. Headache 2006;46: Guidetti V, Galli F. Recent development in pediatric headache. Curr Opin Neurol 2001;14: Headache Classification Subcommittee of the International Headache Society. The international classification of headache disorders, 2 nd edn. Cephalgia 2004;24(Suppl): Olesen J. The international classification of headache disorders, 2 nd edition: application to practice. Funct Neurol 2005;20:61-8. Acta Clin Croat, Vol. 53, No. 4,
6 10. Uberall MA, Denecke H, Kroner-Hedwig B. Therapy of headaches in childhood and adolescence. Schmerz 2000;14: Lewis DW, Ashwal S, Dahl G, et al. Practice parameter: evaluation of children and adolescents with recurrent headaches: report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 2002;59: Cummings E, Wittick L, Cantor R. Evaluation and management of headache in the pediatric patient. Emerg Med 2009;41: Hershey AD. Current approaches to the diagnosis and management of paediatric migraine. Lancet Neurol 2010;9: Graf WD, Kayyali HR, Alexander JJ, Simon SD, Morriss MC. Neuroimaging-use trends in nonacute pediatric headache before and after clinical practice parameters. Pediatrics 2008;122: Alexiou GA, Argyropoulou MI. Neuroimaging in childhood headache: a systematic review. Pediatr Radiol 2013;43: Yilmas U, Celegen M, Sevim Yilmaz T, Gurcinar M, Unalp A. Childhood headaches and brain magnetic resonance imaging findings. Eur J Paediatr Neurol 2014;18: Lewis DW, Dorbad D. The utility of neuroimaging in the evaluation of children with migraine or chronic daily headache who have normal neurological examinations. Headache 2000;40: Rho YI, Chung HJ, Suh ES, et al. The role of neuroimaging in children and adolescents with recurrent headaches, a multicenter study. Headache 2011;51: Alehan FK. Value of neuroimaging in the evaluation of neurologically normal children with recurrent headache. J Child Neurol 2002;17: Prpić I, Paučić-Kirinčić E, Smokvina M, et al. Kliničko-epidemiološke značajke primarnih tumora mozga u djece liječene u Klinici za pedijatriju Kantrida u razdoblju od do godine. Paediatr Croat 2000;44(Suppl 3): Mučić-Pucić B, Cvitanović-Šojat Lj, Hajnžić T, Mataija M. Neurologic symptoms as first signs of brain tumor in children. Acta Clin Croat 2001;40: Morris Z, Whiteley WN, Longstreth WT, et al. Incidental findings on brain magnetic resonance imaging: systematic review and meta-analysis. BMJ 2009;339(1). b3016: Kukal K, Dobrovoljac M, Boltshauser E, Ammann RA, Grotzer MA. Does diagnostic delay result in decreased survival in paediatric brain tumours? Eur J Pediatr 2009;168: Japan Children s Study Group. Incidental findings of brain magnetic resonance imaging study in a pediatric cohort in Japan and recommendation for a model management protocol. J Epidemiol 2010;20(Suppl 2): Schwedt TJ, Guo Y, Rothner AD. Benign imaging abnormalities in children and adolescents with headache. Headache 2006;46: Gupta SN, Belay B. Intracranial findings on brain MR images in a pediatric neurology practice: a retrospective study. J Neurol Sci 2008;264: Bayram E, Topcu Y, Karaoglu P, et al. Incidental white matter lesions in children presenting with headache. Headache 2013;53: Fisch N, Konen O, Halevy A, Cohen R, Shuper A. Incidental multifocal white matter lesions in pediatric magnetic resonance imaging. Pediatr Neurol 2012;47:7-12. Sažetak neuroslikovne pretrage u djece s kroničnom glavoboljom u kliničkoj praksi I. Prpić, T. Ahel, K. Rotim, D. Gajski, P. Vukelić i A. Sasso Cilj rada bio je utvrditi postoji li značajan nesrazmjer između kliničke prakse i kliničkih smjernica u svezi indikacija za provođenje neuroslikovnih pretraga u djece s kroničnom glavoboljom. Analizirana je medicinska dokumentacija djece s kroničnom glavoboljom u dobi od 2 do 18 godina liječene u Kliničkom bolničkom centru Rijeka, Klinika za pedijatriju Kantrida. Indikacije za provođenje magnetske rezonancije i kompjutorizirane tomografije (MR/CT) mozga uspoređene su s indikacijama preporučenim u smjernicama. MR je učinjen u 93 (56,7%) djece, a CT u 71 (43,3%) djeteta, ukupno u 164 (76,3%) od 215 djece. Indikacije za MR/CT mozga bile su: tjeskoba i/ili inzistiranje obitelji (71.3%), prisutnost pridruženih simptoma koji su ukazivali na neurološki poremećaj (13.4%), djeca mlađa od 5 godina (12,8%) i promijenjen neurološki status (2,4%). U većine djece (71,4%) nalaz MR/CT bio je uredan. U ostalim MR/CT nalazima opisane su intra-/ekstracerebralne promjene koje nisu utjecale na promjene u terapijskom pristupu (28,1%). U samo jednog djeteta (0,60%) promijenjen je terapijski pristup nakon provedene neuroslikovne pretrage. Ovo ispitivanje dokazuje da se, unatoč dostupnim kliničkim smjernicama, neuroslikovne pretrage mozga u djece s kroničnim glavoboljama prekomjerno provode, uglavnom s ciljem umanjivanja tjeskobe roditelja i/ili zbog njihovog inzistiranja da se iste učine. Ključne riječi: Djeca; Glavobolja; Neuroslikovne pretrage; Praktične smjernice 454 Acta Clin Croat, Vol. 53, No. 4, 2014
Neuroimaging in Migraine Critically Appraised Topic (CAT)
 Neuroimaging in Migraine Critically Appraised Topic (CAT) PICOT Question: Does a head CT scan compared to no head CT scan change the management of a child with migraine? Clinical bottom line based on literature
Neuroimaging in Migraine Critically Appraised Topic (CAT) PICOT Question: Does a head CT scan compared to no head CT scan change the management of a child with migraine? Clinical bottom line based on literature
Headache in an Italian pediatric emergency department
 J Headache Pain (2008) 9:83 87 DOI 10.1007/s10194-008-0014-1 ORIGINAL Headache in an Italian pediatric emergency department Paola Scagni Æ Rosaura Pagliero Received: 2 October 2007 / Revised: 3 January
J Headache Pain (2008) 9:83 87 DOI 10.1007/s10194-008-0014-1 ORIGINAL Headache in an Italian pediatric emergency department Paola Scagni Æ Rosaura Pagliero Received: 2 October 2007 / Revised: 3 January
Paediatric headaches. Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services. Brevity, levity, repetition
 Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
Headache. Karen Thaxter
 Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #419: Overuse Of Neuroimaging For Patients With Primary Headache And A Normal Neurological Examination National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL
Quality ID #419: Overuse Of Neuroimaging For Patients With Primary Headache And A Normal Neurological Examination National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL
Vague Neurological Conditions
 Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Clinical Policy: EEG in the Evaluation of Headache Reference Number: CP.MP.155
 Clinical Policy: EEG in the Evaluation of Headache Reference Number: CP.MP.155 Effective Date: 12/17 Last Review Date: 12/17 Coding Implications Revision Log See Important Reminder at the end of this policy
Clinical Policy: EEG in the Evaluation of Headache Reference Number: CP.MP.155 Effective Date: 12/17 Last Review Date: 12/17 Coding Implications Revision Log See Important Reminder at the end of this policy
Review Evaluation of Residuals of Traumatic Brain Injury (R-TBI) Disability Benefits Questionnaire * Internal VA or DoD Use Only*
 Review Evaluation of Residuals of Traumatic Brain Injury (R-TBI) Disability Benefits Questionnaire * Internal VA or DoD Use Only* Name of patient/veteran: SSN: Your patient is applying to the U. S. Department
Review Evaluation of Residuals of Traumatic Brain Injury (R-TBI) Disability Benefits Questionnaire * Internal VA or DoD Use Only* Name of patient/veteran: SSN: Your patient is applying to the U. S. Department
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Pediatric Imaging Spine MRI and Spine CT Test Request Tip Sheet
 Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of ongoing back pain, six weeks of conservative
Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of ongoing back pain, six weeks of conservative
Pediatric Imaging Spine MRI and Spine CT Test Request Tip Sheet
 Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of
Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of
EVALUATION OF CHRONIC HEADACHE BY COMPUTED TOMOGRAPHY: A RETROSPECTIVE STUDY
 EVALUATION OF CHRONIC HEADACHE BY COMPUTED TOMOGRAPHY: A RETROSPECTIVE STUDY Abstract: Anish Subedee Objective: To find out the proportion of intracranial abnormalities in patients with chronic headache
EVALUATION OF CHRONIC HEADACHE BY COMPUTED TOMOGRAPHY: A RETROSPECTIVE STUDY Abstract: Anish Subedee Objective: To find out the proportion of intracranial abnormalities in patients with chronic headache
Admission criteria to the Danish Brain Cancer Program are moderately associated with magnetic resonance imaging findings
 Dan Med J 60/3 March 2013 danish medical JOURNAL 1 Admission criteria to the Danish Brain Cancer Program are moderately associated with magnetic resonance imaging findings Thomas Winther Hill, Mie Kiszka
Dan Med J 60/3 March 2013 danish medical JOURNAL 1 Admission criteria to the Danish Brain Cancer Program are moderately associated with magnetic resonance imaging findings Thomas Winther Hill, Mie Kiszka
Referral Criteria for Medical CT Radiation Exposures. Neuro Referrals
 Referral Criteria for Medical CT Radiation Exposures Neuro Referrals CHH & HRI The Ionising Radiation (Medical Exposure) Regulations 2017 Document Control Reference No: 3.2 First published: 2016 Version:
Referral Criteria for Medical CT Radiation Exposures Neuro Referrals CHH & HRI The Ionising Radiation (Medical Exposure) Regulations 2017 Document Control Reference No: 3.2 First published: 2016 Version:
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level
 Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL
 University of Florida, Pediatric Integrated Care System UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL Policy: Program(s): Approval Criteria for Neuroimaging of Headaches Title XIX and Title XXI Effective
University of Florida, Pediatric Integrated Care System UTILIZATION MANAGEMENT POLICY AND PROCEDURE MANUAL Policy: Program(s): Approval Criteria for Neuroimaging of Headaches Title XIX and Title XXI Effective
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Cinnarizine versus Topiramate in Prophylaxis of Migraines among Children and Adolescents: A Randomized, Double-Blind Clinical Trial
 original ARTICLE Cinnarizine versus Topiramate in Prophylaxis of Migraines among Children and Adolescents: A Randomized, Double-Blind Clinical Trial How to Cite This Article: Ashrafi MR, Najafi Z, Shafiei
original ARTICLE Cinnarizine versus Topiramate in Prophylaxis of Migraines among Children and Adolescents: A Randomized, Double-Blind Clinical Trial How to Cite This Article: Ashrafi MR, Najafi Z, Shafiei
Outpatient Headache Care Guideline
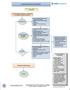 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Specific features of migraine syndrome in children
 J Headache Pain (2006) 7:206 210 DOI 10.1007/s10194-006-0312-4 RAPID COMMUNICATION Marija Knezevic-Pogancev Specific features of migraine syndrome in children Received: 16 April 2006 Accepted in revised
J Headache Pain (2006) 7:206 210 DOI 10.1007/s10194-006-0312-4 RAPID COMMUNICATION Marija Knezevic-Pogancev Specific features of migraine syndrome in children Received: 16 April 2006 Accepted in revised
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
DBQ Initial Evaluation of Residuals of Traumatic Brain Injury (I-TBI) Disability
 DBQ Initial Evaluation of Residuals of Traumatic Brain Injury (I-TBI) Disability Name of patient/veteran: SSN: SECTION I 1. Diagnosis Does the Veteran now have or has he/she ever had a traumatic brain
DBQ Initial Evaluation of Residuals of Traumatic Brain Injury (I-TBI) Disability Name of patient/veteran: SSN: SECTION I 1. Diagnosis Does the Veteran now have or has he/she ever had a traumatic brain
Headache Syndrome. Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL
 Headache Syndrome Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL What is a headache? A headache or cephalgia is defined as pain anywhere in the region of head or neck Where does
Headache Syndrome Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL What is a headache? A headache or cephalgia is defined as pain anywhere in the region of head or neck Where does
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Clinical profile of patients with chronic headache in a tertiary care hospital
 International Journal of Advances in Medicine Senthil C et al. Int J Adv Med. 2016 Aug;3(3):721-726 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20162524
International Journal of Advances in Medicine Senthil C et al. Int J Adv Med. 2016 Aug;3(3):721-726 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20162524
11. HEADACHE 1. Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH
 11. HEADACHE 1 Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language
11. HEADACHE 1 Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language
Dizziness: Neurological Aspect
 Dizziness: Neurological Aspect..! E-mail: somtia@kku.ac.th http://epilepsy.kku.ac.th Features between peripheral and central vertigo 1. Peripheral Central 2.! " # $ " Imbalance Mild-moderate Severe 3.!
Dizziness: Neurological Aspect..! E-mail: somtia@kku.ac.th http://epilepsy.kku.ac.th Features between peripheral and central vertigo 1. Peripheral Central 2.! " # $ " Imbalance Mild-moderate Severe 3.!
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
Intracranial hypertension and headache. Daniel Tibussek, MD
 Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
The tentorial nerve is a branch from V1. Do you think, diagnostic neuroimaging
 Radiology in headache: your patient wants a scando you want it too? The tentorial nerve is a branch from V1 Arne May, Dept. of Systems Neuroscience, University of Hamburg (UKE) (Feindel et al., Neurology
Radiology in headache: your patient wants a scando you want it too? The tentorial nerve is a branch from V1 Arne May, Dept. of Systems Neuroscience, University of Hamburg (UKE) (Feindel et al., Neurology
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA)
 Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely
Spine MRI and Spine CT With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely
Health Learning Partnership 13 th September Neuroimaging. Headache Dementia Incidentalomas DR MARCUS BRADLEY CONSULTANT NEURORADIOLOGIST
 Health Learning Partnership 13 th September 2017 Neuroimaging DR MARCUS BRADLEY CONSULTANT NEURORADIOLOGIST Headache Dementia Incidentalomas Dr Marcus Bradley Consultant Neuroradiologist Interventional
Health Learning Partnership 13 th September 2017 Neuroimaging DR MARCUS BRADLEY CONSULTANT NEURORADIOLOGIST Headache Dementia Incidentalomas Dr Marcus Bradley Consultant Neuroradiologist Interventional
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
The headache profile of idiopathic intracranial hypertension
 The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Migraine Diagnosis and Treatment: Results From the American Migraine Study II
 Migraine Diagnosis and Treatment: Results From the American Migraine Study II Richard B. Lipton, MD; Seymour Diamond, MD; Michael Reed, PhD; Merle L. Diamond, MD; Walter F. Stewart, MPH, PhD Objective.
Migraine Diagnosis and Treatment: Results From the American Migraine Study II Richard B. Lipton, MD; Seymour Diamond, MD; Michael Reed, PhD; Merle L. Diamond, MD; Walter F. Stewart, MPH, PhD Objective.
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017
 Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
MIGRAINE CLASSIFICATION
 MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
Migraine Types and Triggering Factors in Children
 original ARTICLE Migraine Types and Triggering Factors in Children How to Cite this Article: Nejad Biglari H, Karimzadeh P, Mohammadi Kord-kheyli M, Hashemi SM. Migraine Types and Triggering Factors in
original ARTICLE Migraine Types and Triggering Factors in Children How to Cite this Article: Nejad Biglari H, Karimzadeh P, Mohammadi Kord-kheyli M, Hashemi SM. Migraine Types and Triggering Factors in
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Occult Cerebrospinal Fluid Fistula between Ventricle and Extra-Ventricular Position of the Ventriculoperitoneal Shunt Tip
 197 Occult Cerebrospinal Fluid Fistula between Ventricle and Extra-Ventricular Position of the Ventriculoperitoneal Shunt Tip Ching-Yi Lee 1, Chieh-Tsai Wu 1, Kuang-Lin Lin 2, Hsun-Hui Hsu 3 Abstract-
197 Occult Cerebrospinal Fluid Fistula between Ventricle and Extra-Ventricular Position of the Ventriculoperitoneal Shunt Tip Ching-Yi Lee 1, Chieh-Tsai Wu 1, Kuang-Lin Lin 2, Hsun-Hui Hsu 3 Abstract-
Transcranial ultrasound diagnosis of intracranial lesions in children with headaches Wang H S, Kuo M F, Huang S C, Chou M L, Hung P C, Lin K L
 Transcranial ultrasound diagnosis of intracranial lesions in children with headaches Wang H S, Kuo M F, Huang S C, Chou M L, Hung P C, Lin K L Record Status This is a critical abstract of an economic evaluation
Transcranial ultrasound diagnosis of intracranial lesions in children with headaches Wang H S, Kuo M F, Huang S C, Chou M L, Hung P C, Lin K L Record Status This is a critical abstract of an economic evaluation
Secondary Headaches: A Strategic Approach. Emerg Med 40(4):18, 2008
 Secondary Headaches: A Strategic Approach Emerg Med 40(4):18, 2008 Headaches are common complaints in the emergency department, but the causes of secondary headaches are often misdiagnosed. The authors
Secondary Headaches: A Strategic Approach Emerg Med 40(4):18, 2008 Headaches are common complaints in the emergency department, but the causes of secondary headaches are often misdiagnosed. The authors
Background. Background. Headache Examination. Headache History. Primary vs. Secondary Headaches. Headaches In Children: Why Worry?
 Background Headaches In Children: Why Worry? Marcy Yonker MD FAHS Associate Professor of Pediatrics University of Arizona Director, Pediatric Headache Program Phoenix Children s Hospital Headaches are
Background Headaches In Children: Why Worry? Marcy Yonker MD FAHS Associate Professor of Pediatrics University of Arizona Director, Pediatric Headache Program Phoenix Children s Hospital Headaches are
Suspected neurological conditions: clinical questions
 Suspected neurological clinical questions For questions on signs and symptoms, the committee wanted to consider any studies that determine whether a certain sign or symptom accompanying a main presenting
Suspected neurological clinical questions For questions on signs and symptoms, the committee wanted to consider any studies that determine whether a certain sign or symptom accompanying a main presenting
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
It s Always a Stroke; Except For When It s Not..
 It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
Concussions. Recognition, Management, and Care
 Concussions Recognition, Management, and Care Sports Concussion: Complex, pathophysiological process affecting the brain, induced by traumatic bio-mechanical forces. 1 1.6-3.8 million concussions occur
Concussions Recognition, Management, and Care Sports Concussion: Complex, pathophysiological process affecting the brain, induced by traumatic bio-mechanical forces. 1 1.6-3.8 million concussions occur
Electroencephalogram (EEG) for First Nonfebrile Seizure - Critically Appraised Topic (CAT)
 Electroencephalogram (EEG) for First Nonfebrile Seizure - Critically Appraised Topic (CAT) PICOT Question: For the child who presents to the ED after a first nonfebrile seizure should an EEG be obtained
Electroencephalogram (EEG) for First Nonfebrile Seizure - Critically Appraised Topic (CAT) PICOT Question: For the child who presents to the ED after a first nonfebrile seizure should an EEG be obtained
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of multimodality supervised
Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of multimodality supervised
Vertigo. Tunde Magyar MD, PhD
 Vertigo Tunde Magyar MD, PhD What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea
Vertigo Tunde Magyar MD, PhD What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea
Management of TIA. Dr Ali Ali Consultant Stroke and Geriatrics Royal Hallamshire Hospital
 Management of TIA Dr Ali Ali Consultant Stroke and Geriatrics Royal Hallamshire Hospital Objectives Definition TIA and stroke TIA: Diagnosis & mimics Risk assessment Referral and emergency management Secondary
Management of TIA Dr Ali Ali Consultant Stroke and Geriatrics Royal Hallamshire Hospital Objectives Definition TIA and stroke TIA: Diagnosis & mimics Risk assessment Referral and emergency management Secondary
Neurosurgery Sample Case
 120 Beulah Road, NE, Suite 200 Vienna, Virginia 22180 Toll Free: 800-336-0332 Fax: 703-255-6134 www.malpracticeexperts.com Neurosurgery Sample Case The patient had an intra-cerebral artery aneurysm operated
120 Beulah Road, NE, Suite 200 Vienna, Virginia 22180 Toll Free: 800-336-0332 Fax: 703-255-6134 www.malpracticeexperts.com Neurosurgery Sample Case The patient had an intra-cerebral artery aneurysm operated
Recurrent Headaches in Children -- An Analysis of 47 Cases
 ---------------------------------------------- Recurrent Headaches in Children -- An Analysis of Cases I H M I Hussain, MRCP Neurology Unit Paediatric Institute, Kuala Lumpur Hospital, )aian Pahang, 50586
---------------------------------------------- Recurrent Headaches in Children -- An Analysis of Cases I H M I Hussain, MRCP Neurology Unit Paediatric Institute, Kuala Lumpur Hospital, )aian Pahang, 50586
What could be reffered to as dizziness by the patient?
 What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea Loss of memory Loss of confidence
What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea Loss of memory Loss of confidence
Pearls in Child Neurology. Edgard Andrade, MD, FAAP Assistant Professor University of Florida
 Pearls in Child Neurology Edgard Andrade, MD, FAAP Assistant Professor University of Florida Outline 1. Autism 2. Bell s Palsy 3. First unprovoked seizure in children 4. Migraine headache Objectives 1.
Pearls in Child Neurology Edgard Andrade, MD, FAAP Assistant Professor University of Florida Outline 1. Autism 2. Bell s Palsy 3. First unprovoked seizure in children 4. Migraine headache Objectives 1.
PFO closure group total no. PFO closure group no. of males
 Suppl Table. Characteristics of the five trials included in this meta-analysis. Trial name Device used for Definition of medical Primary Endpoint group total no. group no. of males group age (yrs) group
Suppl Table. Characteristics of the five trials included in this meta-analysis. Trial name Device used for Definition of medical Primary Endpoint group total no. group no. of males group age (yrs) group
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
The determination of eligible population for this measure requires administrative claims data.
 Overuse of Imaging Measure 6: Ratio of Magnetic Resonance Imaging Scans to Computed Tomography Scans for the Evaluation of Children with Atraumatic Headache Description This measure assesses the ratio
Overuse of Imaging Measure 6: Ratio of Magnetic Resonance Imaging Scans to Computed Tomography Scans for the Evaluation of Children with Atraumatic Headache Description This measure assesses the ratio
What Do You Think of My Posterior?
 What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
David Dredge, MD MGH Child Neurology CME Course September 9, 2017
 David Dredge, MD MGH Child Neurology CME Course September 9, 2017 } 25-40,000 children experience their first nonfebrile seizure each year } AAN/CNS guidelines developed in early 2000s and subsequently
David Dredge, MD MGH Child Neurology CME Course September 9, 2017 } 25-40,000 children experience their first nonfebrile seizure each year } AAN/CNS guidelines developed in early 2000s and subsequently
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Epilepsy (and first seizure) on the acute take. Phil Smith Consultant Neurologist University Hospital of Wales, Cardiff
 Epilepsy (and first seizure) on the acute take Phil Smith Consultant Neurologist University Hospital of Wales, Cardiff Epilepsy (and first seizure) on the acute take First suspected seizure Acute symptomatic
Epilepsy (and first seizure) on the acute take Phil Smith Consultant Neurologist University Hospital of Wales, Cardiff Epilepsy (and first seizure) on the acute take First suspected seizure Acute symptomatic
VA/DoD Clinical Practice Guideline for the Management of Concussion/mTBI
 VA/DoD Clinical Practice Guideline for the Management of Concussion/mTBI Chief, Evidence-Based Practice US Army Medical Command Clinical Program Specialist Office of Performance and Quality Improvement
VA/DoD Clinical Practice Guideline for the Management of Concussion/mTBI Chief, Evidence-Based Practice US Army Medical Command Clinical Program Specialist Office of Performance and Quality Improvement
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Childhood Craniopharyngioma Treatment (PDQ )
 1 di 12 27/06/2016 09.45 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 12 27/06/2016 09.45 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Comprehensive History, Consult, and Evaluation Form
 1 Comprehensive History, Consult, and Evaluation Form 1.Patient Information: Today s Date: Mr. Ms. Miss Mrs. Dr. Name Age: Date of Birth: Male Female Address: City/State/Zip: Home Phone: Work Phone: Cell
1 Comprehensive History, Consult, and Evaluation Form 1.Patient Information: Today s Date: Mr. Ms. Miss Mrs. Dr. Name Age: Date of Birth: Male Female Address: City/State/Zip: Home Phone: Work Phone: Cell
Adult with headache. Problem-specific video guides to diagnosing patients and helping them with management and prevention
 Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
American Osteopathic College of Occupational and Preventive Medicine 2012 Mid-Year Educational Conference St Petersburg, Florida
 Neurological Neurological Liz Clark, D.O., MPH & TM FAOCOPM MY-2012 49 CFR 391.41(b)(7) "A person is physically qualified to drive a commercial motor vehicle if that person Has no established medical history
Neurological Neurological Liz Clark, D.O., MPH & TM FAOCOPM MY-2012 49 CFR 391.41(b)(7) "A person is physically qualified to drive a commercial motor vehicle if that person Has no established medical history
Classification of Pediatric HIV CNS Disease: Comparison of CNS and Systemic Disease Markers of Children Treated in the HAART Era
 Classification of Pediatric HIV CNS Disease: Comparison of CNS and Systemic Disease Markers of Children Treated in the HAART Era Pam Wolters, Staci Martin, Maryanne Tamula, Steven Zeichner, Lucy Civitello,
Classification of Pediatric HIV CNS Disease: Comparison of CNS and Systemic Disease Markers of Children Treated in the HAART Era Pam Wolters, Staci Martin, Maryanne Tamula, Steven Zeichner, Lucy Civitello,
Young Patient Suffers Cardiac Arrest and Brain Damage After Delayed Referral to Specialist
 Young Patient Suffers Cardiac Arrest and Brain Damage After Delayed Referral to Specialist Theodore Passineau, JD, HRM, RPLU, CPHRM, FASHRM Introduction Diagnostic errors including delay in diagnosis,
Young Patient Suffers Cardiac Arrest and Brain Damage After Delayed Referral to Specialist Theodore Passineau, JD, HRM, RPLU, CPHRM, FASHRM Introduction Diagnostic errors including delay in diagnosis,
Understanding Stroke
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Understanding Stroke About This Kit Stroke is the fourth leading cause of death in Canada after heart disease and
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Understanding Stroke About This Kit Stroke is the fourth leading cause of death in Canada after heart disease and
Laboratory Testing for First Nonfebrile Seizure - Critically Appraised Topic (CAT)
 Laboratory Testing for First Nonfebrile Seizure - Critically Appraised Topic (CAT) PICOT Question: For the child who presents to the emergency department (ED) after a first nonfebrile should laboratory
Laboratory Testing for First Nonfebrile Seizure - Critically Appraised Topic (CAT) PICOT Question: For the child who presents to the emergency department (ED) after a first nonfebrile should laboratory
The Big 3 of Vertigo
 They feel it, you see it, few know it: Common vertigo conditions seen, but rarely diagnosed Peter Johns MD, FRCPC University of Ottawa pjohns@toh.ca Twitter @peterjohns84 The Big 3 of Vertigo BPPV Vestibular
They feel it, you see it, few know it: Common vertigo conditions seen, but rarely diagnosed Peter Johns MD, FRCPC University of Ottawa pjohns@toh.ca Twitter @peterjohns84 The Big 3 of Vertigo BPPV Vestibular
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013
 F-15 Pilot with ACOUSTIC NEUROMA Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013 Disclosure Information 84 th Annual AsMA Scientific Meeting Nazim ATA I have no financial relationships
F-15 Pilot with ACOUSTIC NEUROMA Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013 Disclosure Information 84 th Annual AsMA Scientific Meeting Nazim ATA I have no financial relationships
Neurology. Access Center 24/7 access for referring physicians (866) 353-KIDS (5437)
 Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Gascon GG 1, Coskun CJ 2, Brown WD 1
 Gascon et al. Gascon GG 1, Coskun CJ 2, Brown WD 1 Department of Clinical Neuroscience & Pediatrics, Brown University 1, Neurology, Rhode Island Hospital 2, USA Aim: To review the clinical presentation
Gascon et al. Gascon GG 1, Coskun CJ 2, Brown WD 1 Department of Clinical Neuroscience & Pediatrics, Brown University 1, Neurology, Rhode Island Hospital 2, USA Aim: To review the clinical presentation
HEADACHE 1 Pablo Lapuerta, M.D., and Steven Asch, M.D., M.P.H.
 - 253-13. HEADACHE 1 Pablo Lapuerta, M.D., and Steven Asch, M.D., M.P.H. We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language articles
- 253-13. HEADACHE 1 Pablo Lapuerta, M.D., and Steven Asch, M.D., M.P.H. We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language articles
What is IIH? Idiopathic Intracranial Hypertension (IIH)
 What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Headaches in the Pediatric Emergency Dept
 Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
