Chronic cluster headache: a review
|
|
|
- Joseph Higgins
- 5 years ago
- Views:
Transcription
1 J Headache Pain (2005) 6:3 9 DOI /s REVIEW Irene Favier Joost Haan Michel D. Ferrari Chronic cluster headache: a review Received: 18 October 2004 Accepted in revised form: 9 December 2004 Published online: 25 January 2005 I. Favier J. Haan M.D. Ferrari ( ) Department of Neurology, K5-Q Leiden University Medical Centre, PO Box 9600, 2300 RC Leiden, The Netherlands m.d.ferrari@lumc.nl Tel.: Fax: J. Haan Rijnland Hospital Leiderdorp, The Netherlands Abstract Cluster headache (CH) is a rare but severe headache disorder characterised by repeated unilateral head pain attacks accompanied by ipsilateral autonomic features. In episodic CH, there are periods of headache attacks with pain-free intervals of weeks, months or years in between. A minority of patients have the chronic form, without pain-free intervals between the headache attacks. Chronic CH can occur as primary or secondary chronic CH; the rarest form is episodic CH arising from chronic CH. In this article, we give a review of the chronic forms of CH and focus on demographics, clinical manifestations, social habits, predictive factors, head injury, genetics, neuroimaging and therapy. It is remarkable that little is known about risk factors that make CH chronic. Key words Chronic cluster headache Review Introduction Cluster headache (CH) is characterised by short-lasting, unilateral severe pain attacks, usually located in the orbitotemporal region, accompanied by ipsilateral autonomic phenomena and/or restlessness or agitation [1]. Untreated, the pain lasts 15 min to 3 h and can occur from once every other day to 8 times a day. It is an excruciating pain, driving some patients to thoughts of suicide. In episodic CH (ECH), the attacks occur in cluster periods lasting from one week to one year and are separated by remission periods of at least one month (Table 1). In chronic CH (CCH) the attacks occur almost every day for more than one year without remission or with remissions lasting less than one month. The chronic form can be unremitting from onset, primary chronic cluster headache (PCCH), or can evolve from the episodic form, secondary chronic cluster headache (SCCH). The rarest variety is the secondary episodic form (SECH), which begins as chronic and becomes episodic. In this review, we give an overview of demographics, clinical manifestations, social habits, predictive factors, head injury, genetics, neuroimaging and therapy of CCH. In the separate sections, we will first compare ECH with CCH, followed by a comparison of PCCH and SCCH. Demographics The exact prevalence of CH (and its subforms) is uncertain. In some epidemiological surveys, the prevalence of CH varies from 56 to 401 per [2]. The highest prevalence of 401 per was found in a study in which the diagnosis of CH was based on a review of
2 4 Table 1 Diagnostic criteria for CH [1] CH A. At least 5 attacks fulfilling criteria B D B. Severe or very severe unilateral orbital, supraorbital and/or temporal pain lasting min if untreated C. Headache is accompanied by at least one of the following: 1. Ipsilateral conjunctival injection and/or lacrimation 2. Ipsilateral nasal congestion and/or rhinorrhoea 3. Ipsilateral eyelid oedema 4. Ipsilateral forehead and facial sweating 5. Ipsilateral miosis and/or ptosis 6. A sense of restlessness or agitation D. Attacks have a frequency from one every other day to 8 per day E. Not attributed to another disease ECH A. Attacks fulfilling criteria A E for CH B. At least two cluster periods lasting days and separated by pain-free remission periods of 1 month CCH A. Attacks fulfilling criteria A E for CH B. Attacks recur >1 year without remission periods or with remission periods lasting <1 month charts from patients who had been seen and diagnosed by a wide variety of clinicians [3]. So, this high figure may be biased. The episodic form of CH is much more prevalent than the chronic form. The exact ratio between chronic and episodic CH, however, is unknown. Figures in the literature differ [4 6] (Table 2), probably because there is a difference in patient selection. Within the group of patients with CCH, the prevalence of the subgroups (PCCH, SCCH, SECH) is also not exactly known. In a follow-up study of 109 CCH patients during at least 5 years, 64% could be classified as PCCH and 36% as SCCH [7]. As to the course of CH, Pearce [8] conducted a followup study of 101 patients with ECH and 7 patients with CCH during 16 years. Four patients (3.96%) in the episodic group changed to a chronic pattern, whereas in the chronic group, 2 patients (28.6%) changed to an episodic pattern. Another study followed 189 patients with CH over a period longer than 10 years [9]. Almost 13% of ECH patients became secondarily chronic and 32.6% of CCH patients became secondarily episodic. In 1956, Horton [10] reported a male-to-female ratio of CH of 6.7:1 and this was used in clinical practice for years. Recently, the male-to-female ratio was found to be much lower, namely 2.5:1 [5]. This decrease in ratio might be explained by the fact that specific male behavioural traits are possible cluster triggers and that more women are taking over these traits. Also, more women are contributing to household incomes and therefore seek treatment sooner. Another explanation might be that in the past, many women Table 2 Episodic-to-chronic ratio Study Number Episodic-toof patients chronic ratio Manzoni (1997) [4] :1 Bahra et al. (2002) [5] 230 4:1 Van Vliet et al. (2003) [6] :1 with CH were first diagnosed with migraine, because of atypical features of the CH, such as longer duration of an attack. A male to female ratio of 3.6:1 was found for ECH and 4.2:1 for CCH [4]. Another study found a male to female ratio of 3.2:1 in PCCH and 2.4:1 in SCCH [11]. Mean age at onset appeared to be later in CCH than in ECH: 38 vs. 32 years [6]. Mean age at onset was later in PCCH compared to SCCH: approximately 37 vs. 29 years [11, 12]. In conclusion, the exact prevalence of CH and its subforms is uncertain, but it is clear that episodic CH is much more prevalent than chronic CH. There is a male preponderance in CH, especially in the chronic form. In chronic CH, the mean age at onset appeared to be about 6 years later than in episodic CH. The mean age at onset is especially late in primary chronic CH. Clinical manifestations The diagnostic criteria for CH do not differentiate between ECH and CCH in the clinical features of the attacks. The distinction is only made in the occurrence and duration of remission periods, but clinical studies also found some differences in the characteristics of ECH and CCH. First, patients with CCH appear to have a mild, continuous headache between the attacks more often than patients with ECH [6]. Second, a significant difference in the site of pain appears to exist [5]. In both forms the site of pain was predominantly retro-orbital and temporal, but in CCH, more patients reported pain also in the upper teeth, jaw, cheek, ear and shoulder. Besides, in CCH there was more often a side change of the pain. Third, differences in autonomic features were found between ECH and CCH. Lacrimation is the most often reported symptom in both conditions, but rhinorrhoea occurred significantly less in CCH. Osmophobia occurred more in CCH. Finally, the reported attack duration between ECH and CCH was shorter in the chronic group. There are also some differences in characteristics between PCCH and SCCH [11]. First, patients with PCCH more often reported right-sided pain than patients with
3 5 SCCH, a finding that is not easily explained. Second, in PCCH and SCCH, attack duration was most often between 15 and 120 min, but there was a statistically significant larger proportion of patients with SCCH who reported attacks lasting min. Finally, patients with SCCH were more likely to have their headache associated with lacrimation, nasal congestion, rhinorrhoea and ptosis while patients with PCCH more frequently reported facial sweating and eyelid oedema. In conclusion, there are some clinical differences between episodic and chronic CH and also between the two chronic forms. Social habits Some studies have looked at lifestyle habits in episodic vs. chronic CH. Up to 90% of CH patients are smokers or former smokers [12] and there seem to be some differences between the episodic and chronic forms (Tables 3 and 4). In an Italian study, more male CCH patients smoked compared to ECH patients and the chronic patients also smoked more cigarettes a day [12]. Comparing the two chronic forms, there were more and also more heavy smokers in the SCCH group [11]. Table 3 Social habits in ECH vs. CCH [12] Social habit ECH, % CCH, % Smoking habit No. of patients >20 cig/day Alcohol intake No. of patients >100 g/day Coffee intake No. of patients >6 cups/day Table 4 Social habits in PCCH vs. SCCH [11] Social habit PCCH, % SCCH, % Smoking habit No. of patients >20 cig/day Alcohol intake No. of patients g/day Coffee intake No. of patients cups/day There were a few more alcohol drinkers in CCH compared to ECH, but the chronic patients were evidently heavier drinkers [12]. PCCH patients were more frequently heavy drinkers compared to SCCH patients [11]. A minor difference was found in the number of ECH and CCH patients consuming coffee, but the chronic patients drank more cups of coffee a day [12]. The percentage of regular coffee drinkers was the same in both chronic conditions, however PCCH patients drank more cups of coffee a day [11]. In conclusion, lifestyle habits such as smoking and the consumption of alcohol or coffee are common habits in CH, especially in chronic CH. Comparing the two chronic conditions, smoking is a more common habit in SCCH patients while consuming alcohol or coffee is more common among PCCH patients. Secondary chronic cluster headache: predictive factors Three factors were discovered that seemed to predict a shift from ECH to CCH [9]. Firstly, the shift was associated with the duration of the disease. In 20.5% of episodic patients with a course of CH longer than 20 years, there was a shift towards the chronic form, versus a shift in 9.4% of patients with a shorter course than 20 years. Secondly, a late age at onset appeared to predict a pattern change. Mean age at onset was 27.1 years in ECH, while the mean age at onset was 34.9 years in SCCH. Thirdly, male sex was slightly related to a shift to a chronic condition: in SCCH, the percentage of females was 9.1% and the percentage of males was 13.6%. The characteristics of cluster and remission periods were also found to be predictive factors in the shift from ECH to SCCH (Table 5). More SCCH patients reported cluster periods lasting more than 8 weeks before the CH became chronic, compared to ECH patients who stayed episodic [13]. Also, a larger proportion of SCCH patients reported remission periods lasting less than 6 months. More SCCH patients reported more than one cluster period a year and more frequently reported sporadic attacks. Table 5 Characteristics of cluster and remission periods in ECH and SCCH [13] ECH, % SCCH, % Cluster periods >8 weeks Remission periods <6 months More than 1 cluster/year Sporadic attacks 5 25
4 6 In conclusion, factors that were found to predict a shift from episodic to chronic CH are: a longer course, a late age at onset, male sex, longer cluster periods, shorter remission periods, more cluster periods per year and more frequent sporadic attacks. Secondary episodic cluster headache: predictive factors Four factors were found that favoured the evolution of CCH into SECH [9]. The first one was the use of prophylactic treatment (usually lithium). Of the chronic patients who became secondary episodic, about 56% used prophylactic medication. The second factor was an earlier headache onset. CH onset was 26 years for SECH and almost 35 years for PCCH. Thirdly, duration of the disease longer than 20 years was positively related to the evolution from CCH to ECH. Only in 46.6% of patients with CCH and a course longer than 20 years did the chronic form persist. Fourthly, male sex appeared to relate positively to a shift from CCH to ECH: all of the patients in the SECH group were men. In conclusion, factors that were found to predict a shift from chronic to episodic CH are: the use of prophylactic treatment, an earlier age at onset, a longer course and male sex. Head injury Head injury and CH have been frequently associated. In a case-control study [14], significantly more CH patients had a previous head trauma compared to the control group (30.8% vs. 15.8%), and in another study, almost 37% of CH individuals reported head injury vs. almost 17% of age- and gender-matched migrainous controls [12]. Patients with CCH reported a head injury more often, whether with or without loss of consciousness, compared to patients with ECH (Table 6). Also, head injury occurred more often on the same side as the headache in chronic patients. Head injury preceded the onset of CH more often in chronic patients [11] than episodic patients [13]. Individuals with PCCH reported head injury in their history less frequently compared to SCCH [11], but in a Table 6 Head injury in CH [11 13] Head injury ECH, % CCH, % PCCH, % SCCH, % No. of patients Pre-CH higher percentage of PCCH patients, the head injury preceded onset of CH. A significant difference was found in the average number of years elapsing between head injury and onset of CH when the analysis was restricted to headinjured males with loss of consciousness. The average latency period was 21.8 years for PCCH men and 5.5 years for SCCH men. Four of 28 SCCH patients had a second head injury and in all these 4 patients, the second head injury preceded the evolution from episodic to chronic [13]. The mean latency period between the second head injury and the evolution into SCCH was 11.0 years. In conclusion, many CH patients report a head injury in their medical history. The frequency of head injury is higher in chronic than episodic patients and also higher in SCCH patients compared to PCCH patients. In most chronic patients, the head injury preceded the onset of CH. Genetics It has been suggested that there is a genetic influence in CH. CH has been described in monozygotic twins and also in families in consecutive generations. In a French study [15], a positive family history was found in 10.75% of CH patients. Familial CH was found in 9.52% of ECH patients and in 20% of CCH patients; the difference was not statistically significant. Different forms of CH can occur within the same family. Spierings et al. [16] described a family with the occurrence of CH in three generations: an 8-yearold boy with PCCH, his 42-year-old father with SCCH and his 73-year-old paternal grandfather with ECH. In conclusion, no difference in genetic factors seems to exist between the episodic and chronic form. Different forms of CH can occur in the same family. Neuroimaging PET studies in CH patients revealed that the ipsilateral inferior posterior hypothalamus is activated during a CH attack [17]. No difference was made between CCH and ECH, because the ECH patients were used as controls while they were not in a cluster period. With voxel-based morphometry, a significant structural difference in grey matter density bilateral in the inferior posterior hypothalamus was found between CH patients and healthy volunteers [18]. No comparison was made between CCH and ECH patients. In conclusion, the difference between ECH and CCH in hypothalamic function and grey matter density has not been studied yet.
5 7 Therapy More patients with ECH than with CCH had success with oxygen: 78.8% vs. 68.4% [19]. The greatest difference was found when comparing ECH patients under 50 years of age (92.9%) with CCH patients over 49 years of age (57.1%). CH can also be treated with a hyperbaric form of oxygen. In a placebo-controlled study, the treatment of CCH patients with hyperbaric oxygen in 15 sessions every other day for 4 weeks was more effective than placebo [20]. The number of attacks and the analgesic consumption declined in the group treated with hyperbaric oxygen, while there was no change in the placebo group. However, it is difficult to treat patients with this therapy, because it requires hyperbaric chambers. Patients with CCH responded well to the use of subcutaneous sumatriptan, but to a lesser extent than ECH patients: 72.9% of ECH patients were pain free within 15 min compared to 60% of CCH patients [21]. Also, CCH patients responded more slowly than patients with ECH. In an open-label study [22], intranasal sumatriptan was more effective in ECH than in CCH, but only 4 patients with CCH and 6 with ECH participated. Within 30 min, 42% of headache attacks improved in ECH patients compared to only 16% of headache attacks in CCH patients. In a placebo-controlled study [23], no difference in efficacy of sumatriptan nasal spray was found between episodic and chronic patients. Unfortunately, no percentages were given. Dihydroergotamine was more effective for ECH than for CCH [24]: there was complete resolution in 73% of ECH patients and in 46% of CCH patients. Dihydroergotamine appeared to induce transformation from CCH to ECH: of the 17 patients with CCH who achieved complete success with dihydroergotamine, 3 experienced a transformation to ECH. In a double-blind crossover study, significantly more patients with ECH reported efficacy of oral zolmitriptan than placebo (46.8% vs. 28.9%) [25]. In CCH however, there was no significant difference. In an open study with 48 patients [26], it was found that ECH patients more often improved than CCH patients on verapamil prophylaxis (73% vs. 60%), but this difference was not significant. Headache relief was obtained after an average of 1.7 weeks in the episodic group and after an average of 5 weeks in the chronic group. The required average daily dose of verapamil was 354 mg in ECH and 572 mg in CCH. In an open study [27], 19 male CH patients (8 with CCH and 11 with ECH) were treated with lithium. In all chronic patients, there was at least a 75% improvement within 2 weeks after starting the treatment. In the episodic patients, there was an average improvement of only 15% with no improvement in 3 patients. Lithium was compared with verapamil in a double-blind crossover trial in CCH patients [28]. It appeared that both medications were efficacious in preventing CCH, without significant differences. Methysergide appeared effective in approximately 65% of ECH patients and in only 20% of CCH patients [29]. In an open-label study with 77 episodic and 15 chronic patients, there was a marked relief with prednisone therapy in 76.6% of patients with ECH and in 40% of patients with CCH [29]. In an open-label study, topiramate rapidly induced cluster remission in 64.3% of CCH patients and in 50% of ECH patients [30]. All chronic patients and 75% of episodic patients had poor or no response to other preventive treatments. Serum melatonin levels are reduced in CH patients during a cluster period [31, 32]. In a double blind, placebo-controlled trial in 18 ECH and 2 PCCH patients, melatonin appeared only effective in the prophylaxis of ECH [33]. In another study, in 6 CCH patients and 3 ECH patients who did not react to conventional therapy, there was no effect of melatonin [34]. The lack of response in CCH may reflect a fundamental difference between the chronic and episodic condition. In a placebo-controlled trial, capsaicin was superior to placebo in reducing headache severity when delivered twice a day in the ipsilateral nostril for seven days [35]. Episodic patients appeared to benefit more than chronic patients. In CCH cases resistant to medical management, surgery could be a feasible option. Of 17 patients with intractable CCH who underwent a partial or complete section of the trigeminal nerve, 15 (88%) had complete or near-complete relief of their CH in the immediate postoperative period [36]. Complete section produced better results than partial section, but this difference was not significant. Two patients had recurrence of the CH after initial complete relief. In another study, 28 CCH patients underwent in total 39 microvascular decompression procedures of the trigeminal nerve, alone or in combination with section and/or microvascular decompression of the nervus intermedius [37]. In 22 of 30 (73.3%) first time procedures, there was a 50% relief or better. At follow-up, this success rate dropped to 46.6%. Repeating the procedure was ineffective. Stimulation of the ipsilateral posterior hypothalamus with stereotactic implants in five patients with medically refractory CCH was successful [38]. All patients achieved complete pain relief. The relief of pain occurred in two patients after a couple of hours, in three patients in 1 4 weeks. Three patients remained pain free with prophylactic medication, the other two patients stayed pain free without medication. There were no adverse side effects of the stimulation and there were no acute complications from
6 8 the electrode implant procedure. Of course, these results are from a limited number of patients. In a long-term follow-up study of a patient with bilateral hypothalamic stimulation, the stimulation appeared very successful, but there were some adverse events, consisting of transient vertigo and bradycardia [39]. Besides, the hypothalamus is important for internal metabolic homeostasis and circadian rhythms, so an extremely cautious patient selection for hypothalamic stimulation is mandatory. Recently, proposals for patient selection are published [40]. In conclusion, symptomatic treatment with oxygen and subcutaneous sumatriptan is more effective in ECH than in CCH. Prophylactic medications are also more effective in ECH than in CCH with the exception of topiramate and especially lithium. Dihydroergotamine is more effective in ECH, but appears to induce transformation from CCH to ECH. Surgery could be a feasible option for CCH patients resistant to medical management. Stimulation of the posterior hypothalamus seemed to be very effective in medically refractory CCH, but the results are from a very limited number of patients. Conclusions CH is a severe headache disorder. Especially its chronic forms are very disabling and difficult to treat. In approximately 4 13% of cases, the episodic condition can develop to a chronic form of CH. It is remarkable that little is known about factors that influence the evolution of ECH to CCH. Such knowledge can, however, be of great value, as it may lead to treatment or preventive measures to avoid this evolution. In our present review of (mainly retrospective) studies, three factors seemed to predict the shift from ECH to CCH: a longer course of CH, a late age at onset and male sex. The influence of male sex may have been overestimated, as there were not many women examined in these studies. The role of a long duration of CH is also not very strong, because the longer the duration of a disease, the more time there is for a pattern change. The characteristics of cluster and remission periods also seemed to predict a shift from ECH to CCH. When comparing ECH with CCH, there did not appear to be many clinical differences. The main difference we found was the effect of prophylactic medication, which is larger in ECH than in CCH, with the exception of topiramate and lithium. Selection bias is a likely cause for these findings. It is striking that dihydroergotamine, although more effective in ECH, appears to induce transformation from CCH to ECH. The comparison of PCCH with SCCH revealed a male preponderance in PCCH, but not many clinical differences. Not much is known about the pathophysiology of CH. Even less is known about the chronic forms of CH. Patients with CCH more often report a head injury and some studies point to differences in social habits between ECH and CCH. These social habits are more often displayed by chronic patients. But are these habits secondary phenomena to the suffering of chronic CH, or do they play a role in the onset? Also, are there more factors that could favour the development of chronic CH, besides a head injury and lifestyle habits? For instance, does the frequent use of triptans play a role? Further research, for example by means of prospective and longitudinal studies, might lead to more insight in the pathophysiology of CCH. References 1. (2004) The international classification of headache disorders, 2nd edn. Headache Classification Subcommittee of the International Headache Society. Cephalalgia 24[Suppl 1]: Russell MB (2004) Epidemiology and genetics of cluster headache. Lancet Neurol 3(5): Dodick DW, Rozen TD, Goadsby PJ, Silberstein SD (2000) Cluster headache. Cephalalgia 20(9): Manzoni GC (1997) Male preponderance of is progressively decreasing over the years. Headache 37(9): Bahra A, May A, Goadsby PJ (2002) Cluster headache. A prospective clinical study with diagnostic implications. Neurology 58(3): Van Vliet JA, Eekers PJE, Haan J, Ferrari MD (2003) Features involved in the diagnostic delay of cluster headache. J Neurol Neurosurg Psychiatry 74(8): Kunkel RS, Frame JR (1994) Chronic cluster headache. Long-term followup. In: Olesen J (ed.) Headache classification and epidemiology. Raven Press, New York, pp Pearce JMS (1993) Natural history of cluster headache. Headache 33(5): Manzoni GC, Micieli G, Granella F, Tassorelli C, Zanferrari C, Cavallini A (1991) Cluster headache course over ten years in 189 patients. Cephalalgia 11(4): Horton BT (1956) Histaminic cephalalgia: differential diagnosis and treatment. Proc Staff Meet Mayo Clin 31: Torelli P, Cologno D, Cademartiri C, Manzoni GC (2000) Primary and secondary chronic cluster headache: two separate entities? Cephalalgia 20(9):
7 9 12. Manzoni GC (1999) Cluster headache and lifestyle: remarks on a population of 374 male patients. Cephalalgia 19(2): Torelli P, Cologno D, Cademartiri C, Manzoni GC (2000) Possible predictive factors in the evolution of episodic to chronic cluster headache. Headache 40(10): Italian Cooperative Study Group on the Epidemiology of Cluster Headache (1995) Case-control study on the epidemiology of cluster headache I: Etiological factors and associated conditions. Neuroepidemiology 14(3): El Amrani M, Ducros A, Boulan P, Aidi S, Crassard I, Visy JM, Tournier- Lasserve E, Bousser MG (2002) Familial cluster headache: a series of 186 index patients. Headache 42(10): Spierings ELH, Vincent AJPE (1992) Familial cluster headache: occurrence in three generations. Neurology 42(7): May A, Bahra A, Büchel C, Frackowiak RSJ, Goadsby PJ (2000) PET and MRA findings in cluster headache and MRA in experimental pain. Neurology 55(9): May A, Ashburner J, Büchel C, McGonigle DJ, Friston KJ, Frackowiak RSJ, Goadsby PJ (1999) Correlation between structural and functional changes in brain in an idiopathic headache syndrome. Nat Med 5(7): Kudrow L (1981) Response of cluster headache attacks to oxygen inhalation. Headache 21(1): Di Sabato F, Rocco M, Martelletti P, Giacovazzo M (1997) Hyperbaric oxygen in chronic cluster headaches: influence on serotonergic pathways. Undersea Hyperb Med 24(2): Göbel H, Lindner V, Heinze A, Ribbat M, Deuschl G (1998) Acute therapy for cluster headache with sumatriptan: Findings of a one-year long-term study. Neurology 51(3): Schuh-Hofer S, Reuter U, Kinze S, Einhäupl KM, Arnold G (2002) Treatment of acute cluster headache with 20 mg sumatriptan nasal spray an open pilot study. J Neurol 249(1): Van Vliet JA, Bahra A, Martin V, Ramadan N, Aurora SK, Mathew NT, Ferrari MD, Goadsby PJ (2003) Intranasal sumatriptan in cluster headache. Randomized placebo-controlled double-blind study. Neurology 60(4): Magnoux E, Zlotnik G (2004) Outpatient intravenous dihydroergotamine for refractory cluster headache. Headache 44(3): Bahra A, Gawel MJ, Hardebo JE, Millson D, Breen SA, Goadsby PJ (2000) Oral zolmitriptan is effective in the acute treatment of cluster headache. Neurology 54(9): Gabai IJ, Spierings ELH (1989) Prophylactic treatment of cluster headache with verapamil. Headache 29(3): Ekbom K (1981) Lithium for cluster headache: review of the literature and preliminary results of long-term treatment. Headache 21(4): Bussone G, Leone M, Peccarisi C, Micieli G, Granella F, Magri M, Manzoni GC, Nappi G (1990) Double blind comparison of lithium and verapamil in cluster headache prophylaxis. Headache 30(7): Kudrow L (1980) The management of cluster headache. In: Kudrow L (ed.) Cluster headache. Oxford University Press, New York, pp Láinez MJA, Pascual J, Pascual AM, Santonja JM, Ponz A, Salvador A (2003) Topiramate in the prophylactic treatment of cluster headache. Headache 43(7): Leone M, Bussone G (1993) A review of hormonal findings in cluster headache. Evidence for hypothalamic involvement. Cephalalgia 13(5): Leone M, Lucini V, D Amico D, Moschiano F, Maltempo C, Fraschini F, Bussone G (1995) Twenty-four-hour melatonin and cortisol plasma levels in relation to timing of cluster headache. Cephalalgia 15(3): Leone M, D Amico D, Moschiano F, Fraschini F, Bussone G (1996) Melatonin versus placebo in the prophylaxis of cluster headache: a doubleblind pilot study with parallel groups. Cephalalgia 16(7): Pringsheim T, Magnoux E, Dobson CF, Hamel E, Aubé M (2002) Melatonin as adjunctive therapy in the prophylaxis of cluster headache: A pilot study. Headache 42(8): Marks DR, Rapoport A, Padla D, Weeks R, Rosum R, Sheftell F, Arrowsmith F (1993) A double-blind placebo-controlled trial of intranasal capsaicin for cluster headache. Cephalalgia 13(2): Jarrar RG, Black DF, Dodick DW, Davis DH (2003) Outcome of trigeminal nerve section in the treatment of chronic cluster headache. Neurology 60(8): Lovely TJ, Kotsiakis X, Jannetta PJ (1998) The surgical management of chronic cluster headache. Headache 38(8): Franzini A, Ferroli P, Leone M, Broggi G (2003) Stimulation of the posterior hypothalamus for treatment of chronic intractable cluster headaches: first reported series. Neurosurgery 52(5): Leone M, Franzini A, Broggi G, May A, Bussone G (2004) Long-term follow-up of bilateral hypothalamic stimulation for intractable cluster headache. Brain 127: Leone M, May A, Franzini A, Broggi G, Dodick D, Rapoport A, Goadsby PJ, Schoenen J, Bonavita V, Bussone G (2004) Deep brain stimulation for intractable chronic cluster headache: proposals for patient selection. Cephalalgia 24(11):
CLUS 42 PRACTICAL NEUROLOGY. Pract Neurol: first published as /j x on 1 October Downloaded from
 42 PRACTICAL NEUROLOGY Pract Neurol: first published as 10.1046/j.1474-7766.2001.00505.x on 1 October 2001. Downloaded from http://pn.bmj.com/ CLUS on 31 August 2018 by guest. Protected by copyright. OCT
42 PRACTICAL NEUROLOGY Pract Neurol: first published as 10.1046/j.1474-7766.2001.00505.x on 1 October 2001. Downloaded from http://pn.bmj.com/ CLUS on 31 August 2018 by guest. Protected by copyright. OCT
Cluster headache (CH): epidemiology, classification and clinical picture
 Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Trigeminal Autonomic Cephalalgias. Disclosures. Objectives 6/20/2018. Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018
 Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE
 Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
23 How Cluster Headache and Other Trigeminal Autonomic Cephalalgias Present
 23 How Cluster Headache and Other Trigeminal Autonomic Cephalalgias Present Henrik Winther Schytz 1. Cristina Tassorelli 2. Messoud Ashina 1 1 Glostrup Hospital, University of Copenhagen, Glostrup, Copenhagen,
23 How Cluster Headache and Other Trigeminal Autonomic Cephalalgias Present Henrik Winther Schytz 1. Cristina Tassorelli 2. Messoud Ashina 1 1 Glostrup Hospital, University of Copenhagen, Glostrup, Copenhagen,
Cluster headache in women: clinical characteristics and comparison with cluster headache in men
 J Neurol Neurosurg Psychiatry 2001;70:613 617 613 Department of Neurology, JeVerson Headache Center, Thomas University Hospital, 111 South 11th Street, Gibbon Building, Suite 8130, Philadelphia, Pennsylvania
J Neurol Neurosurg Psychiatry 2001;70:613 617 613 Department of Neurology, JeVerson Headache Center, Thomas University Hospital, 111 South 11th Street, Gibbon Building, Suite 8130, Philadelphia, Pennsylvania
Miller S, Matharu MS. Managing patients with cluster headache in primary care
 Miller S, Matharu MS. Managing patients with cluster headache in primary care Miller S, Matharu MS. Managing patients with cluster headache in primary care. Practitioner 2013;257 (1764):15-20 Dr Sarah
Miller S, Matharu MS. Managing patients with cluster headache in primary care Miller S, Matharu MS. Managing patients with cluster headache in primary care. Practitioner 2013;257 (1764):15-20 Dr Sarah
Does repeated subcutaneous administration of sumatriptan produce an unfavorable evolution in cluster headache?
 J Headache Pain (2004) 5:110 114 DOI 10.1007/s10194-004-0078-5 ORIGINAL Virginie Dousset Virginie Chrysostome Bruno Ruiz S. Irachabal Magalie Lafittau Françoise Radat Bruno Brochet Patrick Henry Does repeated
J Headache Pain (2004) 5:110 114 DOI 10.1007/s10194-004-0078-5 ORIGINAL Virginie Dousset Virginie Chrysostome Bruno Ruiz S. Irachabal Magalie Lafittau Françoise Radat Bruno Brochet Patrick Henry Does repeated
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis
 Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Cluster headache and paroxysmal hemicrania: differential diagnosis
 Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 2004254244248Original ArticleCH and PH: differential diagnosisj Zidverc-Trajkovic et al. Cluster headache and paroxysmal hemicrania:
Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 2004254244248Original ArticleCH and PH: differential diagnosisj Zidverc-Trajkovic et al. Cluster headache and paroxysmal hemicrania:
VIEWS & REVIEWS Acute and preventive pharmacologic treatment of cluster headache
 VIEWS & REVIEWS Acute and preventive pharmacologic treatment of cluster headache George J. Francis, BSc Werner J. Becker, MD Tamara M. Pringsheim, MD Address correspondence and reprint requests to Dr.
VIEWS & REVIEWS Acute and preventive pharmacologic treatment of cluster headache George J. Francis, BSc Werner J. Becker, MD Tamara M. Pringsheim, MD Address correspondence and reprint requests to Dr.
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: occipital_nerve_stimulation 8/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Occipital nerve
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: occipital_nerve_stimulation 8/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Occipital nerve
The Clinical Profile of Sumatriptan: Cluster Headache Key Words
 Paper Eur Neurol 1994;34(suppl 2):35-39 P.J. Peter J. Goadsby Department of Neurology, The Prince Henry Hospital, Little Bay, Sydney, NSW, Australia The Clinical Profile of Sumatriptan: Cluster Headache
Paper Eur Neurol 1994;34(suppl 2):35-39 P.J. Peter J. Goadsby Department of Neurology, The Prince Henry Hospital, Little Bay, Sydney, NSW, Australia The Clinical Profile of Sumatriptan: Cluster Headache
Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache
 Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Prevention and treatment of cluster headache
 Anna S Cohen PhD, MRCP, Peter J Goadsby MD, PhD, FRACP, FRCP Prevention and treatment of cluster headache Cluster headache is an excruciatingly painful primary headache syndrome with rapid onset attacks
Anna S Cohen PhD, MRCP, Peter J Goadsby MD, PhD, FRACP, FRCP Prevention and treatment of cluster headache Cluster headache is an excruciatingly painful primary headache syndrome with rapid onset attacks
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias
 Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Disease Description and Statistics Current State: Medicare Denial of Coverage Expert Opinion Clinical Studies Gap in Medical Care Cost to US
 Oxygen Therapy Disease Description and Statistics Current State: Medicare Denial of Coverage Expert Opinion Clinical Studies Gap in Medical Care Cost to US Taxpayers Recommendations Cluster headaches are
Oxygen Therapy Disease Description and Statistics Current State: Medicare Denial of Coverage Expert Opinion Clinical Studies Gap in Medical Care Cost to US Taxpayers Recommendations Cluster headaches are
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Atypical presentations of cluster headache
 Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Original Policy Date
 MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
MP 7.01.105 Occipital Nerve Stimulation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
Oxygen treatment for cluster headache attacks at different flow rates: a doubleblind, randomized, crossover study
 Dirkx et al. The Journal of Headache and Pain (2018) 19:94 https://doi.org/10.1186/s10194-018-0917-4 The Journal of Headache and Pain RESEARCH ARTICLE Open Access Oxygen treatment for cluster headache
Dirkx et al. The Journal of Headache and Pain (2018) 19:94 https://doi.org/10.1186/s10194-018-0917-4 The Journal of Headache and Pain RESEARCH ARTICLE Open Access Oxygen treatment for cluster headache
Cluster Headache: Diagnosis and Treatment
 Cluster Headache: Diagnosis and Treatment Rashmi Halker, M.D., 1 Bert Vargas, M.D., 1 and David W. Dodick, M.D. 1 ABSTRACT Cluster headache is a rare yet exquisitely painful primary headache disorder occurring
Cluster Headache: Diagnosis and Treatment Rashmi Halker, M.D., 1 Bert Vargas, M.D., 1 and David W. Dodick, M.D. 1 ABSTRACT Cluster headache is a rare yet exquisitely painful primary headache disorder occurring
Cluster headache in Greece: an observational clinical and demographic study of 302 patients
 Vikelis and Rapoport The Journal of Headache and Pain (2016) 17:88 DOI 10.1186/s10194-016-0683-0 The Journal of Headache and Pain RESEARCH ARTICLE Open Access Cluster headache in Greece: an observational
Vikelis and Rapoport The Journal of Headache and Pain (2016) 17:88 DOI 10.1186/s10194-016-0683-0 The Journal of Headache and Pain RESEARCH ARTICLE Open Access Cluster headache in Greece: an observational
The trigeminal autonomic cephalgias (TACs) are a group of primary headache disorders characterised
 c CLUSTER Correspondence to: Professor Peter J Goadsby, Institute of Neurology, Queen Square, London WC1N 3BG, UK; peterg@ion.ucl.ac.uk TRIGEMINAL AUTONOMIC CEPHALGIAS Manjit S Matharu, Peter J Goadsby
c CLUSTER Correspondence to: Professor Peter J Goadsby, Institute of Neurology, Queen Square, London WC1N 3BG, UK; peterg@ion.ucl.ac.uk TRIGEMINAL AUTONOMIC CEPHALGIAS Manjit S Matharu, Peter J Goadsby
It s like, oh, I m going to have a headache and bam! I have a headache.
 American Headache Society P R O F I L E S CASE VIGNETTE It s like, oh, I m going to have a headache and bam! I have a headache. Volume I Number 4 Howard, a 57-year-old museum curator, was referred upon
American Headache Society P R O F I L E S CASE VIGNETTE It s like, oh, I m going to have a headache and bam! I have a headache. Volume I Number 4 Howard, a 57-year-old museum curator, was referred upon
Cluster headache associated with acute maxillary sinusitis.
 Cluster headache associated with acute maxillary sinusitis. Edvardsson, Bengt Published in: SpringerPlus DOI: 10.1186/2193-1801-2-509 2013 Link to publication Citation for published version (APA): Edvardsson,
Cluster headache associated with acute maxillary sinusitis. Edvardsson, Bengt Published in: SpringerPlus DOI: 10.1186/2193-1801-2-509 2013 Link to publication Citation for published version (APA): Edvardsson,
CLUSTER HEADACHE IS A STEREOtypical
 ORIGINAL CONTRIBUTION High-Flow Oxygen for Treatment of Cluster Headache A Randomized Trial Anna S. Cohen, PhD, MRCP Brian Burns, MD, MRCP Peter J. Goadsby, MD, PhD, DSc, FRACP, FRCP CLUSTER HEADACHE IS
ORIGINAL CONTRIBUTION High-Flow Oxygen for Treatment of Cluster Headache A Randomized Trial Anna S. Cohen, PhD, MRCP Brian Burns, MD, MRCP Peter J. Goadsby, MD, PhD, DSc, FRACP, FRCP CLUSTER HEADACHE IS
Policy #: 411 Latest Review Date: January 2014
 Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
Name of Policy: Occipital Nerve Stimulation Policy #: 411 Latest Review Date: January 2014 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross
A new questionnaire for assessment of adverse events associated with triptans: methods of assessment influence the results. Preliminary results
 J Headache Pain (2004) 5:S112 S116 DOI 10.1007/s10194-004-0123-4 Michele Feleppa Fred D. Sheftell Luciana Ciannella Amedeo D Alessio Giancarlo Apice Nino N. Capobianco Donato M.T. Saracino Walter Di Iorio
J Headache Pain (2004) 5:S112 S116 DOI 10.1007/s10194-004-0123-4 Michele Feleppa Fred D. Sheftell Luciana Ciannella Amedeo D Alessio Giancarlo Apice Nino N. Capobianco Donato M.T. Saracino Walter Di Iorio
Clinical Commissioning Policy Statement: Sphenopalatine Ganglion Stimulation for Refractory Chronic Cluster Headache (Adults)
 Clinical Commissioning Policy Statement: Sphenopalatine Ganglion Stimulation for Refractory Chronic Cluster Headache (Adults) NHS England Reference: 170083P 1 Contents 1. Plain Language Summary... 3 2.
Clinical Commissioning Policy Statement: Sphenopalatine Ganglion Stimulation for Refractory Chronic Cluster Headache (Adults) NHS England Reference: 170083P 1 Contents 1. Plain Language Summary... 3 2.
Pain and behaviour in cluster headache. A prospective study and review of the literature
 Pain and behaviour in cluster headache. A prospective study and review of the literature Paola Torelli Gian Camillo Manzoni Headache Centre, Institute of Neurology, University of Parma, Italy Reprint requests
Pain and behaviour in cluster headache. A prospective study and review of the literature Paola Torelli Gian Camillo Manzoni Headache Centre, Institute of Neurology, University of Parma, Italy Reprint requests
Outpatient Headache Care Guideline
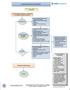 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Trigeminal Autonomic. Trigeminal Autonomic Cephalalgias (TACs) María-Carmen Wilson,MD
 Trigeminal Autonomic Cephalalgias (TACs) María-Carmen Wilson,MD Director, Headache and Facial Pain Program Ochsner, North Shore Region Trigeminal Autonomic Cephalgias gwith autonomic features gcluster
Trigeminal Autonomic Cephalalgias (TACs) María-Carmen Wilson,MD Director, Headache and Facial Pain Program Ochsner, North Shore Region Trigeminal Autonomic Cephalgias gwith autonomic features gcluster
Symptoms. What/Where, When, How Long
 Cluster Headaches Symptoms What/Where, When, How Long *Symptoms include: *Unilateral pain in head (one sided) *Typically centred over one eye, temple or forehead but can spread to a larger area. *Difficulty
Cluster Headaches Symptoms What/Where, When, How Long *Symptoms include: *Unilateral pain in head (one sided) *Typically centred over one eye, temple or forehead but can spread to a larger area. *Difficulty
Received: 21 September 2009 / Accepted: 27 October 2009 / Published online: 21 November 2009 Springer-Verlag F. Dubois Pain Department,
 J Headache Pain (2010) 11:23 31 DOI 10.1007/s10194-009-0169-4 ORIGINAL Safety and efficacy of deep brain stimulation in refractory cluster headache: a randomized placebo-controlled double-blind trial followed
J Headache Pain (2010) 11:23 31 DOI 10.1007/s10194-009-0169-4 ORIGINAL Safety and efficacy of deep brain stimulation in refractory cluster headache: a randomized placebo-controlled double-blind trial followed
Occipital Nerve Stimulation
 Occipital Nerve Stimulation Policy Number: 7.01.125 Last Review: 5/2018 Origination: 5/2006 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Occipital Nerve Stimulation Policy Number: 7.01.125 Last Review: 5/2018 Origination: 5/2006 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
FINANCIAL DISCLOSURE. No relevant financial relationships
 Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Post-Operative Cluster Headache Following Carotid Endarterectomy
 Review Received: October 31, 2016 Accepted: January 11, 2017 Published online: February 3, 2017 Post-Operative Cluster Headache Following Carotid Endarterectomy Thijs H.T. Dirkx Peter J. Koehler Department
Review Received: October 31, 2016 Accepted: January 11, 2017 Published online: February 3, 2017 Post-Operative Cluster Headache Following Carotid Endarterectomy Thijs H.T. Dirkx Peter J. Koehler Department
Occipital Nerve Stimulation Corporate Medical Policy
 Occipital Nerve Stimulation Corporate Medical Policy File name: Occipital Nerve Stimulation File code: UM.SPSVC.14 Origination: 2011 Last Review: 11/2017 Next Review: 11/2018 Effective Date: 05/01/2018
Occipital Nerve Stimulation Corporate Medical Policy File name: Occipital Nerve Stimulation File code: UM.SPSVC.14 Origination: 2011 Last Review: 11/2017 Next Review: 11/2018 Effective Date: 05/01/2018
Headache: Using Neuromodulation as Therapy
 Headache: Using Neuromodulation as Therapy Rashmi Halker, MD, FAHS Assistant Professor of Neurology Department of Neurology Mayo Clinic Phoenix Arizona Disclosures Nothing to disclose 2013 MFMER slide-2
Headache: Using Neuromodulation as Therapy Rashmi Halker, MD, FAHS Assistant Professor of Neurology Department of Neurology Mayo Clinic Phoenix Arizona Disclosures Nothing to disclose 2013 MFMER slide-2
By Nathan Hall Associate Editor
 By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine Cluster
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Transcutaneous stimulation of the cervical branch of the vagus nerve for cluster headache and migraine Cluster
One of the most debilitating headache LONG-TERM RESULTS OF RADIOSURGERY CLINICAL STUDIES FOR REFRACTORY CLUSTER HEADACHE
 CLINICAL STUDIES LONG-TERM RESULTS OF RADIOSURGERY FOR REFRACTORY CLUSTER HEADACHE Shearwood McClelland III, M.D. Department of Neurosurgery, University of Minnesota Medical School, Minneapolis, Minnesota
CLINICAL STUDIES LONG-TERM RESULTS OF RADIOSURGERY FOR REFRACTORY CLUSTER HEADACHE Shearwood McClelland III, M.D. Department of Neurosurgery, University of Minnesota Medical School, Minneapolis, Minnesota
Clinical Characteristics of Chronic Daily Headache Patients Visit to University Hospital
 Clinical Characteristics of Chronic Daily Headache Patients Visit to University Hospital Jin-Kuk Do, M.D., Hee-Jong Oh, M.D., Dong-Kuck Lee, M.D. Department of Neurology, Taegu Hyosung Catholic University
Clinical Characteristics of Chronic Daily Headache Patients Visit to University Hospital Jin-Kuk Do, M.D., Hee-Jong Oh, M.D., Dong-Kuck Lee, M.D. Department of Neurology, Taegu Hyosung Catholic University
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
Trigeminal autonomic cephalalgias
 IV Trigeminal autonomic cephalalgias CQ IV-1 How are trigeminal autonomic cephalalgias classified and typed? Recommendation The International Classification of Headache Disorders 3rd Edition (beta version;
IV Trigeminal autonomic cephalalgias CQ IV-1 How are trigeminal autonomic cephalalgias classified and typed? Recommendation The International Classification of Headache Disorders 3rd Edition (beta version;
The main features of the TACs:
 Pathophysiology of trigeminal autonomic cephalalgias Jasna Zidverc Trajković Headache center The main features of the TACs: 1. Trigeminal distribution of the pain 2. Ipsilateral cranial autonomic features
Pathophysiology of trigeminal autonomic cephalalgias Jasna Zidverc Trajković Headache center The main features of the TACs: 1. Trigeminal distribution of the pain 2. Ipsilateral cranial autonomic features
doi: /brain/awl202 Brain (2006), 129,
 doi:10.1093/brain/awl202 Brain (2006), 129, 2746 2760 Short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) or cranial autonomic features (SUNA) a prospective
doi:10.1093/brain/awl202 Brain (2006), 129, 2746 2760 Short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) or cranial autonomic features (SUNA) a prospective
CLUSTER HEADACHES: THE WORST PAIN POSSIBLE? QUESTIONS:
 CLUSTER HEADACHES: THE WORST PAIN POSSIBLE? QUESTIONS: 1. Have any of you heard of cluster headaches? 2. Do you know someone who suffers from cluster headaches? 1 WHAT ARE CLUSTER HEADACHES? A neurological
CLUSTER HEADACHES: THE WORST PAIN POSSIBLE? QUESTIONS: 1. Have any of you heard of cluster headaches? 2. Do you know someone who suffers from cluster headaches? 1 WHAT ARE CLUSTER HEADACHES? A neurological
Management of headache
 Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
Management of headache TJ Steiner Imperial College London Based on European principles of management of common headache disorders TJ Steiner, K Paemeleire, R Jensen, D Valade, L Savi, MJA Lainez, H-C Diener,
Medication overuse headache: a critical review of end points in recent follow-up studies
 J Headache Pain (2010) 11:373 377 DOI 10.1007/s10194-010-0221-4 REVIEW ARTICLE Medication overuse headache: a critical review of end points in recent follow-up studies Knut Hagen Rigmor Jensen Magne Geir
J Headache Pain (2010) 11:373 377 DOI 10.1007/s10194-010-0221-4 REVIEW ARTICLE Medication overuse headache: a critical review of end points in recent follow-up studies Knut Hagen Rigmor Jensen Magne Geir
The trigeminal autonomic cephalalgias (TACs) are a group of. Cluster Headache and Other Trigeminal Autonomic Cephalalgias By Mark Burish, MD, PhD
 Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Cluster headache (CH) is a type of primary headache
 Real-World Health Plan Claims Analysis of Differences in Healthcare Utilization and Total Cost in Patients Suffering From and Those Without Headache- Related Conditions Michael Polson, MS, PharmD; Todd
Real-World Health Plan Claims Analysis of Differences in Healthcare Utilization and Total Cost in Patients Suffering From and Those Without Headache- Related Conditions Michael Polson, MS, PharmD; Todd
Clinical case. Clinical case 3/15/2018 OVERVIEW. Refractory headaches and update on novel treatment. Refractory headache.
 OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OH, MY ACHING HEAD! I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE MANAGING HEADACHE IN THE OUTPATIENT SETTING SECONDARY HEADACHES
 1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
Prednisone vs. placebo in withdrawal therapy following medication overuse headache
 doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
doi:10.1111/j.1468-2982.2007.01488.x Prednisone vs. placebo in withdrawal therapy following medication overuse headache L Pageler 1,2, Z Katsarava 2, HC Diener 2 & V Limmroth 1,2 1 Department of Neurology,
...SELECTED ABSTRACTS...
 The following abstracts, from medical journals containing literature on migraine management, were selected for their relevance to this Special Report supplement. Two Sumatriptan Studies Two double-blind
The following abstracts, from medical journals containing literature on migraine management, were selected for their relevance to this Special Report supplement. Two Sumatriptan Studies Two double-blind
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
The temporal evolution of a facial pain syndrome associated with neurovascular contact: a case report
 Khan et al. The Journal of Headache and Pain (2015) 16:12 DOI 10.1186/s10194-015-0497-5 CASE REPORT Open Access The temporal evolution of a facial pain syndrome associated with neurovascular contact: a
Khan et al. The Journal of Headache and Pain (2015) 16:12 DOI 10.1186/s10194-015-0497-5 CASE REPORT Open Access The temporal evolution of a facial pain syndrome associated with neurovascular contact: a
Inpatient Treatment of Status Migraine With Dihydroergotamine in Children and Adolescents
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Subject: CGRP Inhibitors
 ARCHIVED (NOT ACTIVE RETIRED) Archived: 08/01/18 09-J2000-98 Original Effective Date: 06/15/18 Reviewed: 05/09/18 Revised: 08/01/18 Next Review: ARCHIVED (NOT ACTIVE RETIRED) Subject: CGRP Inhibitors THIS
ARCHIVED (NOT ACTIVE RETIRED) Archived: 08/01/18 09-J2000-98 Original Effective Date: 06/15/18 Reviewed: 05/09/18 Revised: 08/01/18 Next Review: ARCHIVED (NOT ACTIVE RETIRED) Subject: CGRP Inhibitors THIS
Application of ICHD 2nd edition criteria for primary headaches with the aid of a computerised, structured medical record for the specialist
 J Headache Pain (2005) 6:205 210 DOI 10.1007/s10194-005-0186-x ICHD-II: EVALUATION AND PROPOSALS Paola Sarchielli Mauro Pedini Andrea Alberti Cristiana Rossi Antonio Baldi Ilenia Corbelli Paolo Calabresi
J Headache Pain (2005) 6:205 210 DOI 10.1007/s10194-005-0186-x ICHD-II: EVALUATION AND PROPOSALS Paola Sarchielli Mauro Pedini Andrea Alberti Cristiana Rossi Antonio Baldi Ilenia Corbelli Paolo Calabresi
Anti-Migraine Agents
 DRUG POLICY BENEFIT APPLICATION Anti-Migraine Agents Benefit determinations are based on the applicable contract language in effect at the time the services were rendered. Exclusions, limitations or exceptions
DRUG POLICY BENEFIT APPLICATION Anti-Migraine Agents Benefit determinations are based on the applicable contract language in effect at the time the services were rendered. Exclusions, limitations or exceptions
Hemicrania continua-like headache associated with carotid dissection may respond to indomethacin
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology January 2007 Hemicrania continua-like headache associated with carotid dissection may
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology January 2007 Hemicrania continua-like headache associated with carotid dissection may
A New Minimally Invasive Technique for Cauterizing the Maxillary Artery and Its Application in the Treatment of Cluster Headache
 A New Minimally Invasive Technique for Cauterizing the Maxillary Artery and Its Application in the Treatment of Cluster Headache Elliot Shevel, BDS, DipMFOS, MBBCh* Purpose: To describe a new, relatively
A New Minimally Invasive Technique for Cauterizing the Maxillary Artery and Its Application in the Treatment of Cluster Headache Elliot Shevel, BDS, DipMFOS, MBBCh* Purpose: To describe a new, relatively
Treatment of Intractable Hemicrania Continua by Occipital Nerve Stimulation
 Treatment of Intractable Hemicrania Continua by Occipital Nerve Stimulation 1 Sarah Miller MBBS, MRCP 2 Laurence Watkins FRCS, PhD and 1 Manjit Matharu FRCP, PhD 1 Headache Group, Institute of Neurology
Treatment of Intractable Hemicrania Continua by Occipital Nerve Stimulation 1 Sarah Miller MBBS, MRCP 2 Laurence Watkins FRCS, PhD and 1 Manjit Matharu FRCP, PhD 1 Headache Group, Institute of Neurology
Cluster and Other Nonmigraine Primary Headaches With Aurahead_1875. Randolph W. Evans, MD; Abouch V. Krymchantowski, MD, MSc, PhD, FAHS
 604..608 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01875.x Published by Wiley Periodicals, Inc. Expert Opinion Cluster and Other Nonmigraine Primary Headaches
604..608 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.01875.x Published by Wiley Periodicals, Inc. Expert Opinion Cluster and Other Nonmigraine Primary Headaches
Value of postmarketing surveillance studies in achieving a complete picture of antimigraine agents: using almotriptan as an example
 J Headache Pain (2006) 7:27 33 DOI 10.1007/s10194-006-0266-6 ORIGINAL Julio Pascual Hans-Christoph Diener Hélène Massiou Value of postmarketing surveillance studies in achieving a complete picture of antimigraine
J Headache Pain (2006) 7:27 33 DOI 10.1007/s10194-006-0266-6 ORIGINAL Julio Pascual Hans-Christoph Diener Hélène Massiou Value of postmarketing surveillance studies in achieving a complete picture of antimigraine
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
David W. Dodick M.D. Professor Director of Headache Medicine Department of Neurology Mayo Clinic Phoenix Arizona USA
 Headache Masters School 2013 in Asia Sunday March 24, 2013 Procedural Medicine Workshop Onabotulinumtoxin A: Evidence, Injection Technique, and Mechanism of Action David W. Dodick M.D. Professor Director
Headache Masters School 2013 in Asia Sunday March 24, 2013 Procedural Medicine Workshop Onabotulinumtoxin A: Evidence, Injection Technique, and Mechanism of Action David W. Dodick M.D. Professor Director
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Chronic migraine classification: current knowledge and future perspectives
 J Headache Pain (2011) 12:585 592 DOI 10.1007/s10194-011-0393-6 REVIEW ARTICLE Chronic migraine classification: current knowledge and future perspectives Gian Camillo Manzoni Vincenzo Bonavita Gennaro
J Headache Pain (2011) 12:585 592 DOI 10.1007/s10194-011-0393-6 REVIEW ARTICLE Chronic migraine classification: current knowledge and future perspectives Gian Camillo Manzoni Vincenzo Bonavita Gennaro
MEDICAL POLICY I. POLICY II. PRODUCT VARIATIONS TOP III. DESCRIPTION/BACKGROUND POLICY TITLE SPHENOPALATINE GANGLION BLOCK POLICY NUMBER MP-4.
 Original Issue Date (Created): 2/1/2018 Most Recent Review Date (Revised): 7/5/2018 Effective Date: 9/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Original Issue Date (Created): 2/1/2018 Most Recent Review Date (Revised): 7/5/2018 Effective Date: 9/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_
 doi:10.1111/j.1468-2982.2009.01842.x Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_1842 1149..1155 RB Grande 1,2, K Aaseth 1,3, C Lundqvist
doi:10.1111/j.1468-2982.2009.01842.x Prevalence of new daily persistent headache in the general population. The Akershus study of chronic headachecha_1842 1149..1155 RB Grande 1,2, K Aaseth 1,3, C Lundqvist
ADVANCES IN MIGRAINE MANAGEMENT
 ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
Headache and Facial Pain. Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology
 Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Implantation of a sphenopalatine ganglion stimulation device for chronic cluster headache
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a sphenopalatine ganglion stimulation device for chronic cluster headache Cluster headaches
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a sphenopalatine ganglion stimulation device for chronic cluster headache Cluster headaches
medications. This was an openlabel study consisting of patients with migraines who historically failed to respond to oral triptan
 J Headache Pain (2007) 8:13 18 DOI 10.1007/s10194-007-0354-7 ORIGINAL Seymour Diamond Fred G. Freitag Alexander Feoktistov George Nissan Sumatriptan 6 mg subcutaneous as an effective migraine treatment
J Headache Pain (2007) 8:13 18 DOI 10.1007/s10194-007-0354-7 ORIGINAL Seymour Diamond Fred G. Freitag Alexander Feoktistov George Nissan Sumatriptan 6 mg subcutaneous as an effective migraine treatment
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions
 Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Pause for thought. Dr Jane Anderson Consultant Neurologist
 Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Posterior Cerebral Hypoperfusion in Migraine without Aura Marie Denuelle, MD Neurology Service, Rangueil Hospital Toulouse, France
 Posterior Cerebral Hypoperfusion in Migraine without Aura Marie Denuelle, MD Neurology Service, Rangueil Hospital Toulouse, France Most of the cerebral blood flow (CBF) studies in migraine have introduced
Posterior Cerebral Hypoperfusion in Migraine without Aura Marie Denuelle, MD Neurology Service, Rangueil Hospital Toulouse, France Most of the cerebral blood flow (CBF) studies in migraine have introduced
10/17/2017 CHRONIC MIGRAINES BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES PATIENT CASE EPIDEMIOLOGY EPIDEMIOLOGY
 BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with the PREEMPT paradigm
 Pedraza et al. SpringerPlus (2015) 4:176 DOI 10.1186/s40064-015-0957-z a SpringerOpen Journal RESEARCH Open Access OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with
Pedraza et al. SpringerPlus (2015) 4:176 DOI 10.1186/s40064-015-0957-z a SpringerOpen Journal RESEARCH Open Access OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with
Medical Policy. Description/Scope. Position Statement. Rationale
 Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
Subject: Document#: Current Effective Date: 06/28/2017 Status: Reviewed Last Review Date: 05/04/2017 Description/Scope This document addresses occipital nerve stimulation (ONS), which involves delivering
6/2/2017. Objectives. Statement of Problem: Migraine Headaches Are Common. Chronic Headache In Pediatrics, Botox and Beyond
 Chronic Headache In Pediatrics, Botox and Beyond Ken Mack MD PhD Mayo Clinic 2015 MFMER slide-1 Objectives Understand pediatric chronic headache presentations Review evidence for the treatment of chronic
Chronic Headache In Pediatrics, Botox and Beyond Ken Mack MD PhD Mayo Clinic 2015 MFMER slide-1 Objectives Understand pediatric chronic headache presentations Review evidence for the treatment of chronic
MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache
 MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache Measure Description Percentage of patients age 12 years and older with a diagnosis of migraine who were prescribed a guideline recommended
MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache Measure Description Percentage of patients age 12 years and older with a diagnosis of migraine who were prescribed a guideline recommended
TRIGEMINAL AUTONOMIC CEPHALALGIAS
 TRIGEMINAL AUTONOMIC CEPHALALGIAS A. Trigeminal autonomic cephalalgias Christopher J. Boes, MD Mayo Clinic Rochester, MN Trigeminal autonomic cephalalgias (TACs) defined Headaches characterized by pain
TRIGEMINAL AUTONOMIC CEPHALALGIAS A. Trigeminal autonomic cephalalgias Christopher J. Boes, MD Mayo Clinic Rochester, MN Trigeminal autonomic cephalalgias (TACs) defined Headaches characterized by pain
Zolmitriptan nasal spray provides fast relief of migraine symptoms and is preferred by patients: a Swedish study of preference in clinical practice
 J Headache Pain (2004) 5:237 242 DOI 10.1007/s10194-004-0132-3 ORIGINAL Carl G.H. Dahlöf Mattias Linde Erika Kerekes Zolmitriptan nasal spray provides fast relief of migraine symptoms and is preferred
J Headache Pain (2004) 5:237 242 DOI 10.1007/s10194-004-0132-3 ORIGINAL Carl G.H. Dahlöf Mattias Linde Erika Kerekes Zolmitriptan nasal spray provides fast relief of migraine symptoms and is preferred
its short- and long-term therapeutic efficacy
 Lithium carbonate in cluster headache: assessment of its short- and long-term therapeutic efficacy Gian Camillo Manzoni, Giorgio Bono, Marina Lanfranchi, Giuseppe Micieli, Mario Giovanni Terzano and Giuseppe
Lithium carbonate in cluster headache: assessment of its short- and long-term therapeutic efficacy Gian Camillo Manzoni, Giorgio Bono, Marina Lanfranchi, Giuseppe Micieli, Mario Giovanni Terzano and Giuseppe
American Headache Society Guideline
 ISSN 0017-8748 Headache doi: 10.1111/head.12866 VC 2016 American Headache Society Published by Wiley Periodicals, Inc. American Headache Society Guideline Treatment of Cluster Headache: The American Headache
ISSN 0017-8748 Headache doi: 10.1111/head.12866 VC 2016 American Headache Society Published by Wiley Periodicals, Inc. American Headache Society Guideline Treatment of Cluster Headache: The American Headache
The Role of Allergies and Sinus Disorders in Headache & Facial Pain
 The Role of Allergies and Sinus Disorders in Headache & Facial Pain Vincent T. Martin, MD Professor of Medicine Co-director of the Headache & Facial Pain Center University of Cincinnati College of Medicine
The Role of Allergies and Sinus Disorders in Headache & Facial Pain Vincent T. Martin, MD Professor of Medicine Co-director of the Headache & Facial Pain Center University of Cincinnati College of Medicine
Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse
 DOI 10.1186/s40064-015-1386-8 RESEARCH Open Access Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse Fayyaz Ahmed *, Hassan
DOI 10.1186/s40064-015-1386-8 RESEARCH Open Access Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse Fayyaz Ahmed *, Hassan
MIGRAINE ASSOCIATION OF IRELAND
 MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
What is new in the migraine world! Modar Khalil Consultant neurologist Hull Royal Infirmary
 What is new in the migraine world! Modar Khalil Consultant neurologist Hull Royal Infirmary Overview Understanding the burden Commonly used terms Acute therapy What we currently have What we are going
What is new in the migraine world! Modar Khalil Consultant neurologist Hull Royal Infirmary Overview Understanding the burden Commonly used terms Acute therapy What we currently have What we are going
A one-year prospective costing study of botulinum toxin type A treatment of chronic tension headache
 J Headache Pain (2004) 5:192 196 DOI 10.1007/s10194-004-0100-3 ORIGINAL Fabio Palazzo Francesco S. Mennini Laura Fioravanti Laura Piasini Gabriella Coloprisco Paolo Martelletti A one-year prospective costing
J Headache Pain (2004) 5:192 196 DOI 10.1007/s10194-004-0100-3 ORIGINAL Fabio Palazzo Francesco S. Mennini Laura Fioravanti Laura Piasini Gabriella Coloprisco Paolo Martelletti A one-year prospective costing
Cluster headaches (CHs) (migrainous
 TECHNIQUE APPLICATIONS STIMULATION OF THE POSTERIOR HYPOTHALAMUS FOR TREATMENT OF CHRONIC INTRACTABLE CLUSTER HEADACHES: FIRST REPORTED SERIES Angelo Franzini, M.D. Department of Neurosurgery, Besta, Milan,
TECHNIQUE APPLICATIONS STIMULATION OF THE POSTERIOR HYPOTHALAMUS FOR TREATMENT OF CHRONIC INTRACTABLE CLUSTER HEADACHES: FIRST REPORTED SERIES Angelo Franzini, M.D. Department of Neurosurgery, Besta, Milan,
Zolmitriptan is effective and well tolerated in Japanese patients with migraine: a dose response study
 is effective and well tolerated in Japanese patients with migraine: a dose response study F Sakai 1, M Iwata 2, K Tashiro 3, Y Itoyama 4, S Tsuji 5, Y Fukuuchi 6, G Sobue 7, K Nakashima 8 & M Morimatsu
is effective and well tolerated in Japanese patients with migraine: a dose response study F Sakai 1, M Iwata 2, K Tashiro 3, Y Itoyama 4, S Tsuji 5, Y Fukuuchi 6, G Sobue 7, K Nakashima 8 & M Morimatsu
