Treatment of acute rhinosinusitis diagnosed by clinical criteria or ultrasound in primary care A placebo-controlled randomised trial
|
|
|
- Nicholas Hudson
- 6 years ago
- Views:
Transcription
1 ORIGINAL PAPER Treatment of acute rhinosinusitis diagnosed by clinical criteria or ultrasound in primary care A placebo-controlled randomised trial Helena Varonen 1, Ilkka Kunnamo 2, Seppo Savolainen 3, Marjukka Mäkelä 4, Matti Revonta 5, Jarkko Ruotsalainen 6 and Henrik Malmberg 1 1 Department of Otorhinolaryngology, University of Helsinki, Finland, 2 Karstula Health Centre, Karstula, Finland, 3 Department of Otolaryngology, Central Military Hospital, Helsinki, Finland, 4 Stakes, Finnish Office for Health Technology Assessment, Helsinki, Finland, 5 Department of Otolaryngology, Central Hospital, Hämeenlinna, 6 Juuka Pharmacy, Juuka, Finland. Scand J Prim Health Care 2003;21: ISSN Results A total of 146 patients completed the 2-week follow-up. Patients receiving antibiotics achieved a slightly higher rate of Objecti es To compare antibiotics and placebo in patients with clinical success than patients receiving placebo (80% vs 66%; p= clinically diagnosed acute maxillary sinusitis (AMS). To study 0.068). whether sinus ultrasound examination would help to detect those Conclusions Antibiotics hasten symptom relief in AMS. Yet many patients who benefit from antibiotic therapy. patients recover in 2 weeks without antimicrobial treatment. Only Design A double-blind, randomised, placebo-controlled multicentre half of patients with a clinical diagnosis of AMS have sinusitis in trial. ultrasound examination. Setting Nine primary care sites in Finland. Subjects 150 adult patients (mean age 39.7 years) with a clinical Key words: maxillary sinusitis, randomised controlled trial, sinusitis, diagnosis of sinusitis. ultrasound. Inter ention Antibiotics (amoxicillin 750 mg 2, doxycycline 100 mg 2 or penicillin V 1500 mg 2) or placebo twice daily for 7 days; Helena Varonen, Kuninkaantie 4, FIN Kirkkonummi, Fin- all patients were examined with sinus ultrasound after randomisation. land. helena. aronen@duodecim.fi Main outcome measure Clinical success (patients report of recovery) in telephone interview at 2 weeks. Acute maxillary sinusitis (AMS) is a common infectious disease and by no means a settled question. In a Finnish survey, 12% of patients consulting for infectious diseases were diagnosed as having sinusitis (1). Rhinoviruses are common in the sinus epithelium of AMS patients (2,3), and may cause AMS in up to 50% of cases (4). Symptoms and signs are unspecific (5 7), and if AMS is diagnosed solely by clinical criteria, antibiotics are prescribed unnecessarily to many patients with viral infections (8). In a previous primary care study, antibiotic treatment did not improve the clinical course of AMS (9). Despite limited research evidence on the effectiveness of antibiotics for AMS, this disease nevertheless is most often treated with antibiotics (10,11). Fluid retention is usually regarded as indicating bacterial infection in sinusitis (12). In studies of AMS therapy, the diagnosis is most often based on radiography or aspiration (13). However, these diagnostic methods are impractical in the primary care setting and not recommended in recent guidelines (8,14). Ultrasound examination has been suggested as a means to detect fluid in sinuses and to improve AMS diagnosis (15,16). In this diagnostic therapeutic trial we compared the effect of antibiotics to that of placebo in clinically diagnosed AMS in adults, and studied whether sinus ultrasound examination would help to detect patients who would benefit from antibiotic therapy. PATIENTS AND METHODS Setting and patients The study took place in nine health centres in Finland from November 1998 to October 1999 Although antibiotics are widely used for maxillary sinusitis, research evidence on their effectiveness is still limited. Antibiotics hasten symptom relief in acute maxillary sinusitis. However, many patients recover in two weeks without antimicrobial treatment. Only about 50% of patients with a clinical diagnosis of acute maxillary sinusitis have sinusitis confirmed by ultrasound. DOI /
2 122 H. Varonen et al. (Karstula, Saarijärvi, Halikko, Salo, Katriina, Simo, Kuivaniemi, Heinävesi and Tikkurila). Ear, nose and throat (ENT) specialists (SS and MR) gave a small group tutorial of 1.5 h on sinus ultrasound to 60 physicians in participating health centres. Our inclusion criteria covered adult patients (over 18 years of age) with a clinical diagnosis of AMS. Reasons for exclusion were AMS symptoms lasting over 30 days, antibiotics during the previous month, allergy to study medications, pregnancy or breastfeeding, exacerbation of a diagnosed chronic maxillary sinusitis, previous paranasal sinus surgery, and clinical suspicion of dental or frontal sinusitis or pansinusitis or suspicion of a severe complication, and previous sinus surgery. Data collection Nurse receptionists at health centres screened patients with upper respiratory tract infections to find study patients. Nurses gave written information of the study to possible rhinosinusitis patients and asked them to fill in the patient information form while waiting for the physician s consultation. Data were collected on 12 symptoms related to AMS (nasal obstruction, nasal discharge, headache, postnasal drip, cough, sinus pain, unilateral facial pain, maxillary toothache, hyposmia, anosmia, malaise and fever), and three clinical signs (purulent secretion in the nasal cavity, discharge in the pharynx and tenderness in sinus tapping). Patients assessed the symptoms on a 3-step scale (1=no, 2=little, 3=much). A symptom score of the 12 symptoms was counted by giving 2 points for much answers and 1 point for little answers. The points for the three most important symptoms (maxillary pain, postnasal drip and cough) were doubled. The maximum symptom score was thus 30. We also asked the patients whether they had had symptoms for more than 5 days before the visit and whether they had experienced 2 phases in the disease (double sickening). The physicians discussed the study with the patients, recorded history and clinical findings, and delivered the study medication if the patient had AMS on clinical grounds. The minimum criterion for clinical diagnosis of AMS was the presence of at least three symptoms and one clinical sign. After the treatment decision was made, the ultrasound examination was performed by using a technique described in detail earlier (12,15). The ultrasound device used was Sinuscan 102 (Oriola, Espoo, Finland) with a frequency of 3 MHz and a transducer with an 8-mm diameter. The criterion for AMS was a back wall echo on the screen of the device at a distance of 3.5 cm or more, indicating fluid in the maxillary sinus. None of the other findings were considered sinusitis. To avoid bias, the result was not disclosed to the patient because the ultrasound-negative cases also received treatment. To control the severity of AMS at the Karstula health centre, also nasal samples for bacteriological culture were taken and sinus radiography (occipitomental, Waters view) was examined between 15 min and 1 h after the ultrasound examination. Criteria for AMS were total opacification or an air fluid level or mucosal thickening of 6 mm or more. Bacterial culture was performed according to common bacteriological methods. Randomisation and treatments The patients were randomised to 1 of 4 treatment options, all for 7 days: amoxicillin 750 mg 2, penicillin V 1500 IU 2, doxycyclin 100 mg 2 or placebo 1 2. The placebo group was doubled: two patients out of five received placebo. The treatments were previously randomised in blocks of 20 consecutive patients at the Military Pharmacy in Helsinki and distributed in identical sealed bottles. The study medications were coded with six-number individual codes and physicians, patients and the main researcher (HV) remained blind to the treatments until the recruitment was ended. During the trial, the senior researcher (SS) kept the code and was the primary contact in the case of adverse effects or severe complications. All study centres also had the code in a closed envelope to be opened only if SS could not be reached. Symptomatic treatments with xylometazoline, paracetamol or anti-inflammatory agents were possible if the physician considered them necessary, and their use was recorded. Follow-up The patients received diaries for recording their symptoms daily over 2 weeks. The same list of 12 symptoms with a 3-step scale as in the initial patient form was used. Possible self-medication and side effects were recorded daily in the diary as well as the patients overall estimate of whether they thought they continued to have sinusitis. Two weeks (14 16 days) after the initial consultation, the researcher (HV) interviewed the patients by telephone, asking about subjective symptoms, their severity, possible side effects and the patient s estimate of recovery or recurrence. The interviewer did not know the patient s history, treatment or the result of the ultrasound examination. After 1 year the researcher (HV) checked the patient records to register recurrent or chronic sinusitis in the study patients. Recurrent sinusitis was defined as another episode of sinusitis diagnosed by a primary care physician. Chronic sinusitis was defined as sinusitis with symptoms lasting for more than 3 months.
3 Outcome measures Our main outcome measure was frequency of recovery at the 2-week follow-up (according to the telephone interview). Other outcome measures included subjective symptom scores on days 3 and 10 in patient diaries, frequency of side effects, duration of sinusitis, use of additional medication and the frequency of chronic or recurrent sinusitis and number of physician consultations during the 1-year followup. Study size and statistical analysis Previous studies have shown that approximately 75 80% of patients with AMS treated with placebo recover in 2 weeks (9,17). To find a 15% treatment difference from 75% to 90% at the significance level of =0.05 and =0.20 (power=0.80), a sample size of 98 patients in each treatment arm was needed. We analysed the data by intention-to-treat in main outcomes. Differences in proportions in study groups were tested with the chi-squared or Fisher exact test. Duration of sinusitis was analysed only in patients who recovered fully during the 2-week follow-up. We investigated differences in symptom scores between the group using descriptive statistics, unpaired t-tests and the Mann-Whitney U-test. All reported p-values are two-sided. We analysed all data with StatView software (SAS Institute Inc.). Ethical aspects The ethics committee of the National Research and Development Centre for Welfare and Health and the local ethics committees at study centres accepted the study protocol. The patients received written information on the study and its possible harmful effects. Because the study was placebo-controlled, study centres were provided with a second medication, doxycycline for the amoxicillin group and amoxicillin for the others. The second medication was given if the patient reconsulted with worsened symptoms and the physician considered antibiotics necessary. Patients and physicians stayed blind also to the second medication, knowing only that it contained an active agent. Physicians ensured that the patients had sufficient information and understood the process of the study. The patients gave their written informed consent. Treatment of acute rhinosinusitis 123 RESULTS Patients The trial profile is presented in Fig. 1. Thirty-five primary care physicians in nine health centres participated in patient recruitment. Of 187 patients with suspected AMS considered for study, 150 were eligible and randomised; 105 females (70%) and 45 males (30%). Reasons for exclusion are presented in Fig. 1. Patients were aged between 18 and 75 years (mean 39.7 years). The baseline characteristics of the study patients are presented in Table I. Ultrasound examination was performed on 148 patients, and 74 (50%) tested positive for AMS. At Karstula health centre, 32 patients had sinus radiographies taken, and 13 (41%) had a radiologically diagnosed AMS. Nasal bacterial cultures were obtained from 28 patients in Karstula, and in the culture of 8 cases (29%) grew pathogens for acute maxillary sinusitis. Main outcome The main outcome, recovery at the 2-week follow-up, was slightly better in patients receiving active treatment, antibiotics (70/88, 80%), than in the placebo group (39/59 patients, 66%, chi-squared=3.33, d.f. =1, p=0.068). There were no differences between antibiotics (clinical success rates 18/23, 78% for amoxicillin, 26/33, 79% for doxycycline and 26/32, 81% for penicillin V). Other outcomes Patients receiving antibiotics recovered faster than those receiving placebo. On day 3, the difference in symptom scores was 2.1 (p=0.048, Table II). By day 10, the difference had disappeared. Mean disease duration of AMS was 6.4 days in the placebo group and 6.0 days in the antibiotics group (Table II). Patients receiving placebo used additional medication, especially analgesics, more often than those receiving antibiotics (Table II). Patients in the placebo group started other antibiotics more often (10/58, 17%) than patients in the active treatment group (6/88, 7%, p=0.09 Table II). Subgroups of ultrasound positi e and negati e patients Ultrasound positive and negative patients had similar symptom scores at the beginning of study (15.3, SD 4.3 and 15.4, SD 4.3, respectively). At the 2-week follow-up, patients with sinusitis on ultrasound examination had recovered better (symptom score 2.8, SD 3.2) than those without findings (symptom score 4.1, SD 3.8, p=0.03). In the placebo group, patients who had sinusitis on ultrasound started other antibiotics and withdrew from the study more often than those with no sinusitis on ultrasound (7/32, 22% versus 3/25, 12%, p=0.33). Side effects We analysed side effects in the 130 patients who completed the 2-week follow-up in the initial treat-
4 124 H. Varonen et al. Fig. 1. Flow chart of the study population. Table I. Baseline characteristics of study patients (n=148). Antibiotic Placebo (n=88) (n=60) Patient characteristics Mean age (SD) in years 40.6 (14.1) 38.1 (12.3) Male/female 24 (27%)/ 20 (33%)/ 64 (73%) 40(67%) History Previous sinusitis 74 (84%) 49 (82%) Allergic rhinitis 24 (28%) 10 (17%) Vasomotor rhinitis 6 (7%) 5 (8%) Asthma 8 (9%) 2 (3%) Symptoms and signs Mean initial symptom score (SD) 15.3 (4.6) 15.3 (4.1) Symptoms for more than 5 days 63 (72%) 45 (75%) Double sickening 45 (51%) 35 (58%) ment arm. In the telephone interview at 2 weeks, 13 out of 48 (27%) patients in the placebo group and 32 out of the 82 (39%) receiving antibiotics reported side effects (Table III). Stomach pain, diarrhoea and fatigue were the most common side effects (Table III). Two patients receiving penicillin V withdrew: one got nausea and the other stomach pain and skin rash. One patient receiving amoxicillin stopped treatment because of diarrhoea, and one in the placebo group discontinued treatment because of stomach pain and headache. Follow-up One-year follow-up data were available for 144 patients (60 in the placebo arm and 84 in the antibiotics group). Two patients in the placebo group developed chronic sinusitis in follow-up, and both
5 Treatment of acute rhinosinusitis 125 Table II. Other outcome measures. Outcome measure Antibiotics Placebo Difference (95% CI) p-value Mean symptom score (SD) on day (4.7) 11.5 (5.2) Mean symptom score (SD) on day (4.9) 5.4 (4.7) Mean duration of sinusitis (days) Percentage of patients using additional medication 37/88 (42%) 32/58 (55%) 13% ( 3% to 29%) Analgesics 26% 43% 17% (1% to 32%) Vasoconstrictors and antihistamines 10% 12% 2% ( 8% to 14%) Antibiotics 7% 17% 10% ( 1% to 21%) Mean number (SD) of physician consultations during 3.9 (3.5) 5.1 (6.1) year follow-up Percentage of patients having recurrent sinusitis during 26% 24% 2% ( 16% to 13%) year follow-up Percentage of patients consulting because of respiratory 32% 26% 6% ( 21% to 9%) tract infections during 1-year follow-up 1 Mann-Whitney U-test. 2 T-test. 3 Chi-squared test. lem is that our study lacks power and the ultrasound subgroups are too small for definite conclusions to be drawn. For the same reason, we cannot draw conclusions about the different antibiotics in the study. This randomised study in primary care has several strengths: we combined diagnosis and treatment, the study was conducted in a real-life situation and the length of follow-up was adequate. The slow rate of patient recruitment was a disappointment to us, and we tried to find out what the barriers had been. The barrier first mentioned was work pressure. Sinusitis is mostly treated during busy on-call hours, when filling study forms may be too much of a burden for the physician. Another problem was the placebo arm. Giving placebo to patients who normally would be treated with antibiotics was such a radical change of practice that the physicians might have needed better support from the researchers. Also, financial support was lacking: we did not remunerate the participating physicians for their work. Overall, most patients with clinically diagnosed AMS recovered well without antibiotics. Also patients with AMS diagnosed by radiography and with pathogens in nasal culture improved sometimes well when treated with placebo. Our study confirms previous findings (13,18): up to two-thirds of patients with sinusitis recover well in 2 weeks with or without antibiotics. However, from the patients point of view, clinical success at the 2-week follow-up point may not be the primary outcome. Patients with suspected AMS seek faster relief for their symptoms. A recent study showed that adding fluticasone to xylometazoline and antimicrobial therapy improves clinical success in acute rhinosinusitis (19). We designed this study after the findings of van Buchem et al. (9) were published: a primary carehad AMS in ultrasound examination. There were no differences in the number of cases with recurrent sinusitis in the study groups, but the patients who received antibiotics consulted slightly more often because of respiratory tract infections during the follow-up year (32% vs 26%, p=0.42). DISCUSSION In our study, antibiotics were slightly more effective than placebo for patients with sinusitis diagnosed by clinical criteria. Recovery was similar at 2 weeks, however, patients who received antibiotics recovered faster, having lower symptom scores on day 3. Half of the study patients had AMS on ultrasound examination, and two of them developed chronic sinusitis, both in the placebo group. No complications were seen in the ultrasound-negative patients. It seems that the ultrasound-positive patients in our study had a more severe pattern of disease and, if given placebo, they withdrew from the study and started antibiotics during the 2-week follow-up more often than the ultrasound-negative patients. A prob- Table III. Side effects in patients who completed the 2-week follow-up in the initial treatment arm. Side effect Antibiotics Placebo p-value (n=82) (n=48) ( 2 -test) Diarrhoea 6 (7%) 3 (6%) 0.81 Stomach pain 18 (22%) 6 (12%) 0.18 Headache 3 (6%) 3 (4%) 0.50 Rash 2 (2%) Vaginal discharge 3 (4%) Fatigue 5 (6%) 3 (6%) 0.73 All 32 (39%) 13 (27%) 0.17
6 126 H. Varonen et al. based study found no benefit in antibiotic therapy for AMS diagnosed by radiography. At that point, we considered that another placebo-controlled study comparing the first-line antibiotics would be ethical and justified. Concentrating on one active treatment instead of three might have been a better strategy. A Cochrane review (13) and another meta-analysis (18) on the therapy of AMS have later shown that there is a small treatment effect and that different antibiotics have similar efficacy. More research is needed to compare feasible strategies of AMS diagnosis in primary care to bridge the gap between current practice and the evidence. Ultrasound seems accurate and practical and has no adverse effects. Its use warrants further studies in primary care. CONCLUSIONS Antibiotics hasten symptom relief in AMS. However, many patients recover in 2 weeks without antimicrobial treatment. Only half of patients with a clinical diagnosis of AMS have sinusitis in ultrasound examination. ACKNOWLEDGEMENTS We thank all the patients and physicians who participated in this study as well as the nurses at the study centres for their assistance. Stakes, the National Research and Development Centre for Welfare and Health covered the administrative and travel costs of this study. Leiras-Schering and SmithKline Beecham provided the study medication. REFERENCES 1. Rautakorpi UM, Klaukka T, Honkanen P, Makela M, Nikkarinen T, Palva E, et al. Antibiotic use by indication: a basis for active antibiotic policy in the community. Scand J Infect Dis 2001;33: Pitkaranta A, Starck M, Savolainen S, Poyry T, Suomalainen I, Hyypia T, et al. Rhinovirus RNA in the maxillary sinus epithelium of adult patients with acute sinusitis. Clin Infect Dis 2001;33: Gwaltney Jr JM, Scheld WM, Sande MA, Sydnor A. The microbial etiology and antimicrobial therapy of adults with acute community-acquired sinusitis: a fifteen-year experience at the University of Virginia and review of other selected studies. J Allergy Clin Immunol 1992;90: Pitkaranta A, Arruda E, Malmberg H, Hayden FG. Detection of rhinovirus in sinus brushings of patients with acute community-acquired sinusitis by reverse transcription PCR. J Clin Microbiol 1997;35: Hansen JG, Schmidt H, Rosborg J, Lund E. Predicting acute maxillary sinusitis in general practice population. BMJ 1995;311: Williams Jr JW, Simel DL, Roberts L, Samsa GP. Clinical evaluation for sinusitis. Making the diagnosis by history and physical examination. Ann Intern Med 1992;117: Varonen H, Makela M, Savolainen S, Laara E, Hilden J. Comparison of ultrasound, radiography, and clinical examination in the diagnosis of acute maxillary sinusitis: a systematic review. J Clin Epidemiol 2000;53: Hickner JM, Bartlett JG, Besser RE, Gonzales R, Hoffman JR, Sande MA. Principles of appropriate antibiotic use for acute rhinosinusitis in adults: background. Ann Emerg Med 2001;37: Van Buchem FL, Knottnerus JA, Schrijnemaekers VJ, Peeters MF. Primary-care-based randomised placebo-controlled trial of antibiotic treatment in acute maxillary sinusitis. Lancet 1997;349: Piccirillo JF, Mager DE, Frisse ME, Brophy RH, Goggin A. Impact of first-line vs second-line antibiotics for the treatment of acute uncomplicated sinusitis. JAMA 2001;286: Poole MD. A focus on acute sinusitis in adults: changes in disease management. Am J Med 1999;106: Savolainen S, Pietola M, Kiukaanniemi H, Lappalainen E, Salminen M, Mikkonen P. An ultrasound device in the diagnosis of acute maxillary sinusitis. Acta Otolaryngol Suppl 1997;529: Williams Jr JW, Aguilar C, Makela M, Cornell J, Holleman DR, Chiquette E, et al. Antibiotics for acute maxillary sinusitis. Cochrane Database Syst Rev 2000;2:CD Brooks I, Gooch WM, Jenkins SG, Pichichero ME, Reiner SA, Sher L, et al. Medical management of acute bacterial sinusitis. Recommendations of a clinical advisory committee on pediatric and adult sinusitis. Ann Otol Rhinol Laryngol Suppl 2000;182: Revonta M. Ultrasound in the diagnosis of maxillary and frontal sinusitis. Acta Otolaryngol Suppl 1980;370: Puhakka T, Heikkinen T, Makela MJ, Alanen A, Kallio T, Korsoff L, et al. Validity of ultrasonography in diagnosis of acute maxillary sinusitis. Arch Otolaryngol Head Neck Surg 2000;126: Stalman W, van Essen GA, van der Graaf Y, de Melker RA. Maxillary sinusitis in adults: an evaluation of placebocontrolled double-blind trials. Fam Pract 1997;14: de Ferranti SD, Ioannidis JP, Lau J, Anninger WV, Barza M. Are amoxycillin and folate inhibitors as effective as other antibiotics for acute sinusitis? A meta-analysis. BMJ 1998;317: Dolor RJ, Witsell DL, Hellkamp AS, Williams Jr JW, Califf RM, Simel DL. Comparison of cefuroxime with or without intranasal fluticasone for the treatment of rhinosinusitis. The CAFFS Trial: a randomized controlled trial. JAMA 2001;286:
The clinical diagnosis of acute purulent sinusitis in general practice a review
 The clinical diagnosis of acute purulent sinusitis in general practice a review Morten Lindbæk and Per Hjortdahl SUMMARY Acute sinusitis is a common illness in primary care. Studies have demonstrated the
The clinical diagnosis of acute purulent sinusitis in general practice a review Morten Lindbæk and Per Hjortdahl SUMMARY Acute sinusitis is a common illness in primary care. Studies have demonstrated the
Diagnosing acute maxillary sinusitis in primary care: A comparison of ultrasound, clinical examination and radiography*
 Rhinology, 36, 2 6, 1998 Diagnosing acute maxillary sinusitis in primary care: A comparison of ultrasound, clinical examination and radiography* Karri Laine 1, Tuomo Määttä 2, Helena Varonen 3, Marjukka
Rhinology, 36, 2 6, 1998 Diagnosing acute maxillary sinusitis in primary care: A comparison of ultrasound, clinical examination and radiography* Karri Laine 1, Tuomo Määttä 2, Helena Varonen 3, Marjukka
ORIGINAL ARTICLE. Validity of Ultrasonography in Diagnosis of Acute Maxillary Sinusitis
 ORIGINAL ARTICLE Validity of Ultrasonography in Diagnosis of Acute Maxillary Sinusitis Tuomo Puhakka, MD; Terho Heikkinen, MD; Mika J. Mäkelä, MD; Anu Alanen, MD; Timo Kallio, MD; Leo Korsoff, MD; Jouko
ORIGINAL ARTICLE Validity of Ultrasonography in Diagnosis of Acute Maxillary Sinusitis Tuomo Puhakka, MD; Terho Heikkinen, MD; Mika J. Mäkelä, MD; Anu Alanen, MD; Timo Kallio, MD; Leo Korsoff, MD; Jouko
Position Paper CLINICAL PRACTICE GUIDELINE, PART 2
 CLINICAL PRACTICE GUIDELINE, PART 2 Principles of Appropriate Antibiotic Use for Acute Rhinosinusitis in Adults: Background John M. Hickner, MD, MSc; John G. Bartlett, MD; Richard E. Besser, MD; Ralph
CLINICAL PRACTICE GUIDELINE, PART 2 Principles of Appropriate Antibiotic Use for Acute Rhinosinusitis in Adults: Background John M. Hickner, MD, MSc; John G. Bartlett, MD; Richard E. Besser, MD; Ralph
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
How Family Physicians Distinguish Acute Sinusitis From Upper Respiratory Tract Infection: A Retrospective Analysis
 How Family Physicians Distinguish Acute Sinusitis From Upper Respiratory Tract Infection: A Retrospective Analysis David R. Little, MD, MS, Barbara 1. Mann, PhD, and Christopher j. Godbout, MD Background:
How Family Physicians Distinguish Acute Sinusitis From Upper Respiratory Tract Infection: A Retrospective Analysis David R. Little, MD, MS, Barbara 1. Mann, PhD, and Christopher j. Godbout, MD Background:
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Implementing guidelines on acute maxillary sinusitis in general practice a randomized controlled trial
 Ó The Author 2007. Published by Oxford University Press. All rights reserved. For permissions, please e-mail: journals.permissions@oxfordjournals.org. doi:10.1093/fampra/cml074 Family Practice Advance
Ó The Author 2007. Published by Oxford University Press. All rights reserved. For permissions, please e-mail: journals.permissions@oxfordjournals.org. doi:10.1093/fampra/cml074 Family Practice Advance
Acute rhinosinusitis is defined as. Acute Bacterial Rhinosinusitis in Adults: Part I. Evaluation
 This is a corrected version of the article that appeared in print. Acute Bacterial Rhinosinusitis in Adults: Part I. Evaluation DEWEY C. SCHEID, M.D., M.P.H., and ROBERT. M. HAMM, PH.D. University of Oklahoma
This is a corrected version of the article that appeared in print. Acute Bacterial Rhinosinusitis in Adults: Part I. Evaluation DEWEY C. SCHEID, M.D., M.P.H., and ROBERT. M. HAMM, PH.D. University of Oklahoma
Acute Bacterial Sinusitis
 The new england journal of medicine clinical practice Acute Bacterial Sinusitis Jay F. Piccirillo, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
The new england journal of medicine clinical practice Acute Bacterial Sinusitis Jay F. Piccirillo, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
Treatment & Management of Acute Sinusitis in the Primary Care Setting
 University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Original Article Maxillary Sinusitis Pak Armed Forces Med J 2018; 68 (3): Yasar Shakeel, Muhammad Asad Khan*, Rashid Mehmood**
 Open Access Original Article Maxillary Sinusitis Pak Armed Forces Med J 2018; 68 (3): 594-600 DIAGNOSTIC ACCURACY OF ULTRASONOGRAPHY IN DIAGNOSING MAXILLARY SINUSITIS Yasar Shakeel, Muhammad Asad Khan*,
Open Access Original Article Maxillary Sinusitis Pak Armed Forces Med J 2018; 68 (3): 594-600 DIAGNOSTIC ACCURACY OF ULTRASONOGRAPHY IN DIAGNOSING MAXILLARY SINUSITIS Yasar Shakeel, Muhammad Asad Khan*,
Early release, published at on August 7, Subject to revision.
 CMAJ Early release, published at www.cmaj.ca on August 7, 2012. Subject to revision. Research Systemic corticosteroid monotherapy for clinically diagnosed acute rhinosinusitis: a randomized controlled
CMAJ Early release, published at www.cmaj.ca on August 7, 2012. Subject to revision. Research Systemic corticosteroid monotherapy for clinically diagnosed acute rhinosinusitis: a randomized controlled
Sinusitis in the common cold
 Sinusitis in the common cold Tuomo Puhakka, MD, a Mika J. Mäkelä, MD, a,b Anu Alanen, MD, c Timo Kallio, MD, c Leo Korsoff, MD, c Pertti Arstila, MD, e Maija Leinonen, PhD, f Markku Pulkkinen, RN, g Jouko
Sinusitis in the common cold Tuomo Puhakka, MD, a Mika J. Mäkelä, MD, a,b Anu Alanen, MD, c Timo Kallio, MD, c Leo Korsoff, MD, c Pertti Arstila, MD, e Maija Leinonen, PhD, f Markku Pulkkinen, RN, g Jouko
Upper Respiratory Tract Infections / 42
 Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Retrospective Analysis of Patients with Allergy Sinusitis
 Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
SINUSITIS/RHINOSINUSITIS
 1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
Evaluation of Ultrasound Efficiency in the Diagnosis of Acute Maxillary Sinusitis in Comparison with CT Scan Findings in Children Aged 5 to 15 Years
 Journal of Research in Medical and Dental Sciences 2018, Volume 6, Issue 3, Page No: 363-367 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Evaluation
Journal of Research in Medical and Dental Sciences 2018, Volume 6, Issue 3, Page No: 363-367 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Evaluation
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Sinusitis/Rhinosinusitis SINUSITIS/RHINOSINUSITIS
 1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
Sinusitis in Thai Asthmatic Children
 ORIGINAL ARTICLES Sinusitis in Thai Asthmatic Children Nualanong Visitsuntorn 1 Kampanad Balankura 1 Sriprapai Keorochana 2 Suprida Habanananda Pakit Vlchyanond 1 and Montri Tuchlnda 1 Sinusitis has been
ORIGINAL ARTICLES Sinusitis in Thai Asthmatic Children Nualanong Visitsuntorn 1 Kampanad Balankura 1 Sriprapai Keorochana 2 Suprida Habanananda Pakit Vlchyanond 1 and Montri Tuchlnda 1 Sinusitis has been
JMSCR Vol 05 Issue 10 Page October 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-45 DOI: https://dx.doi.org/1.18535/jmscr/v5i1.116 Nasal Polyps- Causes and Associated Symptoms-
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-45 DOI: https://dx.doi.org/1.18535/jmscr/v5i1.116 Nasal Polyps- Causes and Associated Symptoms-
Respiratory System Virology
 Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Acute rhinosinusitis is a common disease in family practice.1 Most. Predicting Prognosis and Effect of Antibiotic Treatment in Rhinosinusitis
 Predicting Prognosis and Effect of Antibiotic Treatment in Rhinosinusitis An De Sutter, MD, PhD 1 Marieke Lemiengre, MD 2 Georges Van Maele, PhD 3 Mieke van Driel, MD, MS 1 Marc De Meyere, MD, PhD 1 Thierry
Predicting Prognosis and Effect of Antibiotic Treatment in Rhinosinusitis An De Sutter, MD, PhD 1 Marieke Lemiengre, MD 2 Georges Van Maele, PhD 3 Mieke van Driel, MD, MS 1 Marc De Meyere, MD, PhD 1 Thierry
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
AMERICAN ACADEMY OF PEDIATRICS
 AMERICAN ACADEMY OF PEDIATRICS Technical Report: Evidence for the Diagnosis and Treatment of Acute Uncomplicated Sinusitis in Children: A Systematic Overview John P. A. Ioannidis, MD*, and Joseph Lau,
AMERICAN ACADEMY OF PEDIATRICS Technical Report: Evidence for the Diagnosis and Treatment of Acute Uncomplicated Sinusitis in Children: A Systematic Overview John P. A. Ioannidis, MD*, and Joseph Lau,
Diagnosis of maxillary sinusitis in Finnish primary care. Use of imaging techniques
 of maxillary sinusitis in Finnish primary care. Use of imaging techniques Marjukka Mikela' and Kirsiliina Leinonen2 ' National research and development centre for welfare and health, Helsinki, * Helsinki
of maxillary sinusitis in Finnish primary care. Use of imaging techniques Marjukka Mikela' and Kirsiliina Leinonen2 ' National research and development centre for welfare and health, Helsinki, * Helsinki
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Evaluation of Children with Chronic Rhinosinusitis after Adenotonsillectomy
 Iranian Journal of Otorhinolaryngology No.2, Vol.24, Serial No.67, Spring-2012 Original Article Abstract Evaluation of Children with Chronic Rhinosinusitis after Adenotonsillectomy 1* Fatholah Behnoud
Iranian Journal of Otorhinolaryngology No.2, Vol.24, Serial No.67, Spring-2012 Original Article Abstract Evaluation of Children with Chronic Rhinosinusitis after Adenotonsillectomy 1* Fatholah Behnoud
Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief.
 Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Treatment Options for Chronic Sinusitis
 Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
Acute sinusitis is almost always a FAMILY PRACTICE
 JFP_0906_Williamson OR.Final 8/21/06 9:22 AM Page 789 Acute sinusitis: Which factors do FPs believe are most diagnostic and best predict antibiotic efficacy? A questionnaire-and-case-vignette study reveals
JFP_0906_Williamson OR.Final 8/21/06 9:22 AM Page 789 Acute sinusitis: Which factors do FPs believe are most diagnostic and best predict antibiotic efficacy? A questionnaire-and-case-vignette study reveals
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
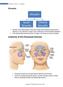 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
RoleofAllergyinNasalPolyposis. Role of Allergy in Nasal Polyposis
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 1 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 1 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
Prefe f rred d t e t rm: : rhi h no n s o inu n s u iti t s
 HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
THE PHARMA INNOVATION - JOURNAL Acute exacerbation of chronic obstructive pulmonary disease, caused by viruses: the need of combined antiinfective
 Received: 19-11-2013 Accepted: 28-12-2013 ISSN: 2277-7695 CODEN Code: PIHNBQ ZDB-Number: 2663038-2 IC Journal No: 7725 Vol. 2 No. 11. 2014 Online Available at www.thepharmajournal.com THE PHARMA INNOVATION
Received: 19-11-2013 Accepted: 28-12-2013 ISSN: 2277-7695 CODEN Code: PIHNBQ ZDB-Number: 2663038-2 IC Journal No: 7725 Vol. 2 No. 11. 2014 Online Available at www.thepharmajournal.com THE PHARMA INNOVATION
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Reducing Antibiotic Use in Common Infections in Family Practice
 Reducing Antibiotic Use in Common Infections in Family Practice W. Rosser Emeritus Professor Department of Family Medicine Queen s University Discussion with Honorary Teachers, University of Hong Kong
Reducing Antibiotic Use in Common Infections in Family Practice W. Rosser Emeritus Professor Department of Family Medicine Queen s University Discussion with Honorary Teachers, University of Hong Kong
UPPER RESPIRATORY TRACT INFECTIONS. IAP UG Teaching slides
 UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
Received 25 November 2002/Returned for modification 14 February 2003/Accepted 11 April 2003
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
Disclaimers. Topical Therapy. The Problem. Topical Therapy for Chronic Rhinosinusitis No Disclosures
 Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Background. Background. AAP (2013) Guidelines. Background 4/19/2016
 Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Research Article Predictive Factors for Medical Consultation for Sore Throat in Adults with Recurrent Pharyngotonsillitis
 International Otolaryngology Volume 2016, Article ID 6095689, 5 pages http://dx.doi.org/10.1155/2016/6095689 Research Article Predictive Factors for Medical Consultation for Sore Throat in Adults with
International Otolaryngology Volume 2016, Article ID 6095689, 5 pages http://dx.doi.org/10.1155/2016/6095689 Research Article Predictive Factors for Medical Consultation for Sore Throat in Adults with
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
4/7/13 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC
 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
NOVEMBER 2016 DRUG ANTIBIOTICS ACUTE RHINOSINUSITIS IN ADULTS
 NOVEMBER 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
NOVEMBER 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
Diagnosis and Treatment of Respiratory Illness in Children and Adults Guideline
 Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Sinusitis in Adults UP TO DATE
 Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Dates to which data relate The effectiveness data were gathered from 1 July 1996 to 20 June No price year was reported.
 Impact of first-line vs second-line antibiotics for the treatment of acute uncomplicated sinusitis Piccirillo J F, Mager D E, Frisse M E, Bophy R H, Goggin A Record Status This is a critical abstract of
Impact of first-line vs second-line antibiotics for the treatment of acute uncomplicated sinusitis Piccirillo J F, Mager D E, Frisse M E, Bophy R H, Goggin A Record Status This is a critical abstract of
The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults
 The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults *Kolo ES Department of Otorhinolaryngology, Bayero University Kano/Aminu Kano Teaching Hospital, Kano, Nigeria
The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults *Kolo ES Department of Otorhinolaryngology, Bayero University Kano/Aminu Kano Teaching Hospital, Kano, Nigeria
Malik Sallam. Ola AL-juneidi. Ammar Ramadan. 0 P a g e
 1 Malik Sallam Ola AL-juneidi Ammar Ramadan 0 P a g e Today's lecture will be about viral upper respiratory tract infections. Those include: common cold, sinusitis, otitis, etc. Infections in the upper
1 Malik Sallam Ola AL-juneidi Ammar Ramadan 0 P a g e Today's lecture will be about viral upper respiratory tract infections. Those include: common cold, sinusitis, otitis, etc. Infections in the upper
Supplementary Online Content
 Supplementary Online Content de la Poza Abad M, Mas Dalmau G, Moreno Bakedano M, et al; Delayed Antibiotic Prescription (DAP) Group. Prescription strategies in acute uncomplicated respiratory infections:
Supplementary Online Content de la Poza Abad M, Mas Dalmau G, Moreno Bakedano M, et al; Delayed Antibiotic Prescription (DAP) Group. Prescription strategies in acute uncomplicated respiratory infections:
Chest radiography in patients suspected of pneumonia in primary care: diagnostic yield, and consequences for patient management
 Chest radiography in patients suspected of pneumonia in primary care: diagnostic yield, and consequences for patient management 4 Speets AM, Hoes AW, Van der Graaf Y, Kalmijn S, Sachs APE, Mali WPThM.
Chest radiography in patients suspected of pneumonia in primary care: diagnostic yield, and consequences for patient management 4 Speets AM, Hoes AW, Van der Graaf Y, Kalmijn S, Sachs APE, Mali WPThM.
Does osteopathic treatments improve the symptoms of headache and/or head-pressure in patients with Chronic Rhinosinusitis (CRS)?
 Does osteopathic treatments improve the symptoms of headache and/or head-pressure in patients with Chronic Rhinosinusitis (CRS)? A randomized controlled trial Roos S 1, Steinbauer U 1, Amann P 1, Schwerla
Does osteopathic treatments improve the symptoms of headache and/or head-pressure in patients with Chronic Rhinosinusitis (CRS)? A randomized controlled trial Roos S 1, Steinbauer U 1, Amann P 1, Schwerla
A Winter Free of Cold Understanding the Common Cold and Flu. Camille Aizarani, MD Family Medicine Specialist
 A Winter Free of Cold Understanding the Common Cold and Flu Camille Aizarani, MD Family Medicine Specialist Outline Introduction Is it a cold or flu? The Common Cold Symptoms of Common Cold Tansmission
A Winter Free of Cold Understanding the Common Cold and Flu Camille Aizarani, MD Family Medicine Specialist Outline Introduction Is it a cold or flu? The Common Cold Symptoms of Common Cold Tansmission
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
An Evidence-Based Treatment of Upper Respiratory Tract Infections
 An Evidence-Based Treatment of Upper Respiratory Tract Infections Ralph Gonzales, MD, MSPH Professor of Medicine; Epidemiology & Biostatistics University of California, San Francisco May 25, 2008 Outline
An Evidence-Based Treatment of Upper Respiratory Tract Infections Ralph Gonzales, MD, MSPH Professor of Medicine; Epidemiology & Biostatistics University of California, San Francisco May 25, 2008 Outline
Module 3. Sinusitis and Congestion
 Module Sinusitis and Congestion What are sinuses? Sinuses are air-filled spaces or cavities within the skull that are lined with mucous membranes a. What is sinusitis? Sinusitis is the inflammation of
Module Sinusitis and Congestion What are sinuses? Sinuses are air-filled spaces or cavities within the skull that are lined with mucous membranes a. What is sinusitis? Sinusitis is the inflammation of
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
+ Conflict of interest. + Sinus and Nasal Anatomy. + What is your diagnosis? 1) Allergic Rhinitis. 2) Non-Allergic rhinitis. 3) Chronic Rhinosinusitis
 Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
An Open Multicenter Study of the Use of Gatifloxacin for the Treatment of Non- Complicated Acute Bacterial Rhinosinusitis in Adults
 162 BJID 2005; 9 (April) An Open Multicenter Study of the Use of Gatifloxacin for the Treatment of Non- Complicated Acute Bacterial Rhinosinusitis in Adults Weckx L.L.M. 1, Campos C.A.H. 2, Sakano E. 3,
162 BJID 2005; 9 (April) An Open Multicenter Study of the Use of Gatifloxacin for the Treatment of Non- Complicated Acute Bacterial Rhinosinusitis in Adults Weckx L.L.M. 1, Campos C.A.H. 2, Sakano E. 3,
Pediatric Imaging Spine MRI and Spine CT Test Request Tip Sheet
 Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of ongoing back pain, six weeks of conservative
Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of ongoing back pain, six weeks of conservative
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre
 Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
Chronic Rhinosinusitis-Treatment
 Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
PFIZER INC. Study Initiation Date and Completion Dates: Information not available (Date of Statistical Report: 16 May 2004)
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
SINUSITIS IS ASSOCIATED WITH
 ORIGINAL CONTRIBUTION Impact of First-Line vs Second-Line Antibiotics for the Treatment of Acute Uncomplicated Sinusitis Jay F. Piccirillo, MD Douglas E. Mager, BS Mark E. Frisse, MD, MS, MBA Robert H.
ORIGINAL CONTRIBUTION Impact of First-Line vs Second-Line Antibiotics for the Treatment of Acute Uncomplicated Sinusitis Jay F. Piccirillo, MD Douglas E. Mager, BS Mark E. Frisse, MD, MS, MBA Robert H.
Clinical Practice Guideline: Tonsillectomy in Children, Baugh et al Otolaryngology Head and Neck Surgery, 2011 J and: 144 (1 supplement) S1 30.
 Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Appropriate Antibiotic Prescribing. Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy
 Appropriate Antibiotic Prescribing Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy Objectives Discuss CDCs Core Elements of abx stewardship.
Appropriate Antibiotic Prescribing Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy Objectives Discuss CDCs Core Elements of abx stewardship.
CAREFUL ANTIBIOTIC USE
 Make promoting appropriate antibiotic use part of your routine clinical practice When parents ask for antibiotics to treat viral infections: PRACTICE TIPS Create an office environment to promote the reduction
Make promoting appropriate antibiotic use part of your routine clinical practice When parents ask for antibiotics to treat viral infections: PRACTICE TIPS Create an office environment to promote the reduction
Follow this and additional works at:
 Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 5-1-2004 Chris Del Mar Bond University, chris_del_mar@bond.edu.au Paul Glasziou
Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 5-1-2004 Chris Del Mar Bond University, chris_del_mar@bond.edu.au Paul Glasziou
Streptococcal Pharyngitis
 Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Update on Rhinosinusitis 2013 AAP Guidelines Review
 Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Table S1. Data on IgG substitution for participants that were included in the per protocol analysis (n=62/arm).
 Bergman et al, Vitamin D 3 supplementation in patients with frequent respiratory tract infections - a randomised, double blind intervention study Supplementary tables Table S1. Data on IgG substitution
Bergman et al, Vitamin D 3 supplementation in patients with frequent respiratory tract infections - a randomised, double blind intervention study Supplementary tables Table S1. Data on IgG substitution
Commen Nose Diseases
 Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
A study of causes of nasal obstruction in Garhwal region of Uttarakhand
 Original Research Article Amit Arya 1, R S Bisht 2,*, Venkatashivareddy B 3, Richa Mina 4 1,4 Senior Resident, 2 Professor, Dept. of ENT, 3 Assistant Professor, Dept. of Community Medicine, VCSGGMS & RI
Original Research Article Amit Arya 1, R S Bisht 2,*, Venkatashivareddy B 3, Richa Mina 4 1,4 Senior Resident, 2 Professor, Dept. of ENT, 3 Assistant Professor, Dept. of Community Medicine, VCSGGMS & RI
Subspecialty Rotation: Otolaryngology
 Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
ORIGINAL ARTICLE. The Impact of Sinus Computed Tomography on Treatment Decisions for Chronic Sinusitis. widespread condition, affecting
 ORIGINAL ARTICLE The Impact of Sinus Computed Tomography on Treatment Decisions for Chronic Sinusitis Yoshimi Anzai, MD; Ernest A. Weymuller, Jr, MD; Bevan Yueh, MD, MPH; Nicole Maronian, MD; Jeffrey G.
ORIGINAL ARTICLE The Impact of Sinus Computed Tomography on Treatment Decisions for Chronic Sinusitis Yoshimi Anzai, MD; Ernest A. Weymuller, Jr, MD; Bevan Yueh, MD, MPH; Nicole Maronian, MD; Jeffrey G.
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Pediatric Imaging Spine MRI and Spine CT Test Request Tip Sheet
 Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of
Pediatric Imaging Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of
Assessment Of Different Strengths Of Levofloxacin In The Treatment Of Acute Bacterial Sinusitis
 Science Journal of Medicine & Clinical Trial ISSN: 2276-7487 http://www.sjpub.org/sjmct.html Author(s) 2013. CC Attribution 3.0 License. Research Article Published By Science Journal Publication Volume
Science Journal of Medicine & Clinical Trial ISSN: 2276-7487 http://www.sjpub.org/sjmct.html Author(s) 2013. CC Attribution 3.0 License. Research Article Published By Science Journal Publication Volume
Research articles last 5 years- ENT
 Research articles last 5 years- ENT Throats and tonsils Tonsillectomy versus antibiotics in children for recurrent tonsillitis Randomised controlled trial (BMJ May 2007) Tonsillectomy is more beneficial
Research articles last 5 years- ENT Throats and tonsils Tonsillectomy versus antibiotics in children for recurrent tonsillitis Randomised controlled trial (BMJ May 2007) Tonsillectomy is more beneficial
Section Editor Mark D Aronson, MD
 1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD)
 Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Functional Endoscopic Sinus Surgery (FESS)
 Functional Endoscopic Sinus Surgery (FESS) Last Review Date: December 12, 2017 Number: MG.MM.SU.56C2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Functional Endoscopic Sinus Surgery (FESS) Last Review Date: December 12, 2017 Number: MG.MM.SU.56C2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Original Article. Relieving Symptoms of Chronic Sinusitis in Children By Adenoidectomy
 Original Article Relieving Symptoms of Chronic Sinusitis in Children By Adenoidectomy * C.A.B.M.S/ENT Summary: Background: To determine the efficacy of adenoidectomy in relieving symptoms of chronic sinusitis
Original Article Relieving Symptoms of Chronic Sinusitis in Children By Adenoidectomy * C.A.B.M.S/ENT Summary: Background: To determine the efficacy of adenoidectomy in relieving symptoms of chronic sinusitis
Respiratory Infections
 Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M.
 UvA-DARE (Digital Academic Repository) Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M. Link to publication Citation for published version (APA): Videler, W.
UvA-DARE (Digital Academic Repository) Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M. Link to publication Citation for published version (APA): Videler, W.
