Position Paper CLINICAL PRACTICE GUIDELINE, PART 2
|
|
|
- Shon Dwayne Benson
- 6 years ago
- Views:
Transcription
1 CLINICAL PRACTICE GUIDELINE, PART 2 Principles of Appropriate Antibiotic Use for Acute Rhinosinusitis in Adults: Background John M. Hickner, MD, MSc; John G. Bartlett, MD; Richard E. Besser, MD; Ralph Gonzales, MD, MSPH; Jerome R. Hoffman, MA, MD; and Merle A. Sande, MD* The following principles of appropriate antibiotic use for adults with acute rhinosinusitis apply to the diagnosis and treatment of acute maxillary and ethmoid rhinosinusitis in adults who are not immunocompromised. 1. Most cases of acute rhinosinusitis diagnosed in ambulatory care are caused by uncomplicated viral upper respiratory tract infections. 2. Bacterial and viral rhinosinusitis are difficult to differentiate on clinical grounds. The clinical diagnosis of acute bacterial rhinosinusitis should be reserved for patients with rhinosinusitis symptoms lasting 7 days or more who have maxillary pain or tenderness in the face or teeth (especially when unilateral) and purulent nasal secretions. Patients with rhinosinusitis symptoms that last less than 7 days are unlikely to have bacterial infection, although rarely some patients with acute bacterial rhinosinusitis present with dramatic symptoms of severe unilateral maxillary pain, swelling, and fever. 3. Sinus radiography is not recommended for diagnosis in routine cases. 4. Acute rhinosinusitis resolves without antibiotic treatment in most cases. Symptomatic treatment and reassurance is the preferred initial management strategy for patients with mild symptoms. Antibiotic therapy should be reserved for patients with moderately severe symptoms who meet the criteria for the clinical diagnosis of acute bacterial rhinosinusitis and for those with severe rhinosinusitis symptoms especially those with unilateral facial pain regardless of duration of illness. For initial treatment, the most narrow-spectrum agent active against the likely pathogens, Streptococcus pneumoniae and Haemophilus influenzae, should be used. Ann Intern Med. 2001;134: For author affiliations and current addresses, see end of text The excessive use of antibiotics in ambulatory practice has contributed to the emergence and spread of antibiotic-resistant bacteria (1 4). Antibiotic treatment of common respiratory infections accounts for a large percentage of this excessive use. Rhinosinusitis is one of the 10 most common diagnoses in ambulatory practice and is the cause of an estimated 25 million U.S. physician office visits in 1995 (5). Fourteen percent of Americans claim to have had a previous diagnosis of sinusitis (6), but the term sinusitis typically has a different meaning for patients and for primary care physicians. When patients say I have sinus trouble, they usually describe acute or chronic symptoms, such as headache, facial pain, nasal congestion, or rhinorrhea, each of which may be due to a variety of causes. Primary care physicians tend to think of sinusitis as an acute bacterial infection, for which they prescribe an antibiotic in 85% to 98% of cases (7, 8). According to data from the National Ambulatory Medical Care Survey, sinusitis is the fifth most common diagnosis for which an antibiotic is prescribed (9). However, sinusitis is frequently caused by viral infection and will resolve in most patients without antibiotic treatment. These principles present an argument for a conservative approach to use of antibiotics in patients with sinusitis-like symptoms, consistent with efforts to reduce antibiotic use for respiratory infections in ambulatory patients. Background, rationale, and methods used for development of these principles have been published separately (10). 1.1 The term sinusitis refers to inflammation of the mucosa of the paranasal sinuses, regardless of cause. Because sinusitis is invariably accompanied by inflammation of the contiguous nasal mucosa, rhinosinusitis has become the preferred term. Most cases of rhinosinusitis *After the primary author (Dr. Hickner), authors are listed in alphabetical order. In addition to the Centers for Disease Control and Prevention, the principles outlined in this document have been endorsed by the American Academy of Family Physicians, the American College of Physicians American Society of Internal Medicine, and the Infectious Diseases Society of America. Annals of Internal Medicine encourages readers to copy and distribute this paper, providing such distribution is not for profit. Commercial distribution is not permitted without the express permission of the publisher American College of Physicians American Society of Internal Medicine
2 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part 2 involve more than one of the paranasal sinuses, most commonly the maxillary and ethmoid sinuses. Isolated infection of a frontal or sphenoid sinus is a rare and potentially dangerous condition, usually caused by bacteria, which presents very differently from the vast majority of cases of rhinosinusitis seen in primary care. Patients with this type of infection seem seriously ill and may show signs of cavernous sinus thrombosis or meningitis. Diagnosis and treatment of isolated frontal and sphenoid sinusitis are beyond the scope of this discussion. For purposes of diagnosis and treatment, rhinosinusitis is classified as acute (symptom duration 4 weeks), subacute (symptom duration 4 to 12 weeks), and chronic (symptom duration 12 weeks) (11). Patients may have recurrent acute attacks or acute exacerbations of chronic rhinosinusitis. Chronic and subacute bacterial sinus infections may require surgical consultation and management. Acute rhinosinusitis, however, makes up most cases in ambulatory care, and primary care clinicians treat most of these infections without consultation. These principles are limited to the diagnosis and treatment of acute maxillary and ethmoid rhinosinusitis in immunocompetent adults. 1.2 Acute bacterial rhinosinusitis is usually a secondary infection resulting from sinus ostia obstruction or impairment of mucus clearance mechanisms caused by an acute viral upper respiratory tract infection (12). Streptococcus pneumoniae and Haemophilus influenzae are the bacteria most commonly isolated from infected maxillary sinuses (13). Streptococcus pyogenes, Moraxella catarrhalis, and anaerobic bacteria each account for a small percentage of bacterial sinus infections. Current reviews providing more details of the pathogenesis of acute and chronic sinusitis have recently been published (11, 13). The gold standard for diagnosis of bacterial rhinosinusitis is sinus puncture with aspiration of purulent secretions that yield growth on culture of at least 10 5 organisms per milliliter of a likely respiratory pathogen (14). However, sinus puncture is an invasive procedure seldom performed in primary care and is usually indicated only in complicated cases, such as those resistant to treatment. Because no simple and accurate office-based tests for acute bacterial rhinosinusitis are available, clinicians rely on clinical findings to make the diagnosis. However, signs and symptoms of acute bacterial rhinosinusitis and of prolonged viral upper respiratory tract infections are extraordinarily similar, making the clinical diagnosis of acute bacterial rhinosinusitis difficult and resulting in frequent misclassification of viral cases. Antibiotics have potential value in treating acute rhinosinusitis only when true bacterial infection is present. Therefore, two issues must be addressed before use of antibiotics is considered for acute rhinosinusitis. First, can one reliably differentiate acute bacterial rhinosinusitis from acute viral rhinosinusitis and, if so, how? Second, are antibiotics effective in treatment of acute bacterial rhinosinusitis and, if so, how effective? PRINCIPLES Principle 1. Most cases of acute rhinosinusitis diagnosed in ambulatory care are caused by uncomplicated viral upper respiratory tract infections [A]. (Letters in square brackets are evidence ratings. See the background document in this issue [10] for explanation.) 2.0 Causes of acute sinus inflammation include infection, allergy, and local irritants. Cases due to allergy and irritants can usually be distinguished from infection on the basis of a careful history. Symptoms due to allergy and environmental irritants are usually more chronic or recurrent, are infrequently associated with purulent nasal discharge, frequently include itching and sneezing, and are often associated with specific exposures. Adult patients are often accurate in self-diagnosis of allergic rhinitis (15). Infectious causes of acute rhinosinusitis include respiratory viruses, fungi, and bacteria. Fungal infections are rare in immunocompetent hosts. Viruses cause most cases of acute sinus inflammation. Maxillary sinus radiographs of young adults with typical viral upper respiratory tract infections showed mucosal abnormalities in 39% of cases on the seventh day of illness (16), and computed tomographic scans were abnormal in 87% of similar cases (17). These studies show that some degree of sinus mucosa inflammation is very common in viral upper respiratory tract infections. On the basis of epidemiologic estimates, only 0.2% to 2% of viral upper respiratory tract infections in adults are complicated by bacterial rhinosinusitis (18, 19), and approximately 15% of people with symptoms of acute respiratory infection seek medical care (20). Presuming a 2% bacterial rhinosinusitis infection rate, if all patients with bacterial rhinosinusitis were among those seeking care, no more than approximately 13% (0.02/0.15) of 20 March 2001 Annals of Internal Medicine Volume 134 Number 6 499
3 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part 2 Table. Studies on the Clinical Diagnosis of Acute Rhinosinusitis Study (Reference) Year Diagnostic Standard Sample Size, n Predictors of Bacterial Rhinosinusitis Hansen et al. (22) 1995 Sinus puncture (presence of purulent or mucopurulent material) Berg and Carenfelt (23) 1988 Sinus puncture (presence of purulent or mucopurulent material) Lindbaek et al. (24) 1996 Computed tomography (air-fluid level or complete opacity) Williams et al. (25) 1992 Abnormal results on sinus radiography (mucosal thickening 6 mm, air-fluid level, or complete opacity) Axelsson and Runze (28) 1976 Abnormal results on sinus radiography (mucosal thickening 6mmor complete opacity) 174 Purulent or mucopurulent nasal discharge, unilateral maxillary pain, maxillary toothache, unilateral maxillary tenderness 155 Purulent rhinorrhea, unilateral facial pain, pus in the nasal cavity 127 Purulent rhinorrhea, purulent secretions, double sickening * 247 Maxillary toothache, poor response to decongestants or antihistamines, history of colored nasal discharge, mucopurulent nasal discharge on examination 164 Purulent rhinorrhea, previous upper respiratory tract infection, cough, hyposmia, malaise van Duijn et al. (26) 1992 Abnormal results on ultrasonography 212 Previous common cold, purulent rhinorrhea, facial pain on bending forward, unilateral maxillary pain, maxillary tooth pain van Buchem et al. (27) 1995 Sinus radiography, sonography, or sinus puncture 113 No consistent predictors * Worsening of symptoms after initial improvement. patients who presented with symptoms of acute respiratory infection would have bacterial rhinosinusitis. Yet the ratio of cases in which primary care physicians diagnose upper respiratory tract infection and acute rhinosinusitis in adults is approximately 1:1 (7, 8), suggesting that clinicians frequently misclassify viral upper respiratory tract infections as acute bacterial rhinosinusitis. Principle 2. Bacterial and viral rhinosinusitis are difficult to differentiate on clinical grounds [B]. The clinical diagnosis of acute bacterial rhinosinusitis should be reserved for patients with rhinosinusitis symptoms lasting 7 days or more who have maxillary pain or tenderness in the face or teeth (especially when unilateral) and purulent nasal secretions. Patients who have rhinosinusitis symptoms for less than 7 days are unlikely to have bacterial infection. 3.0 Overdiagnosis of acute bacterial rhinosinusitis is not surprising, considering the lack of specific clinical features that distinguish it from nonbacterial upper respiratory tract infections. Relying on overall clinical impression, primary care physicians classifying patients as highly likely to have bacterial rhinosinusitis are correct in approximately 40% to 50% of cases (18 22). Often, patients and physicians believe that an upper respiratory tract infection has gone on for too long and that antibiotic treatment is therefore needed. Gwaltney and colleagues (21) studied the natural history of rhinovirus illness in young adults. Length of illness ranged from 1 to 33 days, and only one fourth of the patients had symptoms lasting longer than 14 days. Most were well or nearly well in 7 to 10 days. However, in clinical trials of diagnosis and treatment of rhinosinusitis, duration of illness alone does not reliably distinguish prolonged viral infection from bacterial rhinosinusitis (Williams J, Hansen JG, Lindbaek M. Personal communication). For example, Lindbaek found that, among patients with sinusitis-like symptoms referred from primary care physicians, 80% of those with computed tomography criteria for bacterial sinusitis (air-fluid level or total opacification) had had symptoms for longer than 7 days, while 70% of those without computed tomography criteria for bacterial rhinosinusitis also had symptoms for more than 7 days. Nonetheless, bacterial rhinosinusitis was seen in only 20% of patients whose symptoms lasted less than 7 days (Lindbaek M. Personal communication). Therefore, duration of symptoms of 7 days or greater is a moderately sensitive but nonspecific predictor of bacterial rhinosinusitis. 3.1 Aside from duration of illness, are any symptoms and signs helpful in distinguishing between bacterial and viral rhinosinusitis? Since 1976, seven investigators have published reports attempting to identify signs and symptoms specific to acute bacterial rhinosinusitis (22 28). All seven studies are limited by use of imperfect diagnostic standards. None used the best criterion for diagnosing bacterial rhinosinusitis, which is aspiration of purulent secretions on sinus puncture that grow at least 10 5 organisms per milliliter of a likely respiratory March 2001 Annals of Internal Medicine Volume 134 Number 6
4 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part 2 pathogen on culture. The findings of these trials, listed by diagnostic standard, are summarized in the Table. No single sign or symptom had strong diagnostic value in any study, although certain combinations of signs and symptoms seem to be helpful The study by Hansen and coworkers (22) is the best of the seven. The authors studied 172 patients with suspected bacterial rhinosinusitis referred from general practitioners in Denmark and used maxillary sinus aspiration of purulent or mucopurulent fluid as the diagnostic criterion. Of these patients, 53% had pus or mucopurulent fluid on sinus aspiration, and of this 53%, three fourths had positive bacterial cultures. Unilateral maxillary pain, maxillary toothache, unilateral tenderness of the maxillary sinus, and mucopurulent nasal discharge were statistically more likely in patients with positive sinus aspirates. However, the magnitude of association was small (odds ratio, 1.9 to 2.5), and these findings were common in patients with and without bacterial infection. The results of the study did not change when analyzed by culture results. In patients presenting to an emergency department with sinusitis-like symptoms of less than 3 months duration, Berg and Carenfelt (23) noted that the following four findings were associated with an increased likelihood of bacterial infection (defined as purulent secretions on sinus aspiration): a history of purulent nasal discharge with unilateral predominance, a history of facial pain with unilateral predominance, a history of bilateral purulent nasal discharge, and pus in the nasal cavity on physical examination. When at least two of these findings were present, 67% to 85% of patients had bacterial rhinosinusitis. If one or none were present, fewer than 10% had bacterial infection. The relevance of Berg and Carenfelt s findings to patients with acute rhinosinusitis in primary care is limited by inclusion of patients whose symptoms had lasted for more than 30 days The five other investigators (24 28) used noninvasive sinus imaging for the diagnosis of acute bacterial rhinosinusitis, including plain radiography, computed tomography scanning, and ultrasonography. Lindbaek and associates (24) used air-fluid level or complete sinus opacification on computed tomography sinus radiography as the diagnostic standard. In patients with high clinical probability of bacterial rhinosinusitis, these techniques have an approximately 90% positive predictive value for purulent or mucopurulent secretions on sinus aspiration. Lindbaek found that worsening of symptoms of upper respiratory tract infection after initial improvement, purulent rhinorrhea, and purulent secretions in the nasal cavities were the best independent clinical predictors of acute rhinosinusitis Using plain radiography as the diagnostic standard, Williams and colleagues (25) identified five independent predictors of acute bacterial rhinosinusitis in a study of men with suspected rhinosinusitis in a Veterans Administration outpatient clinic. The five predictors were history of colored nasal discharge, purulent nasal secretions on examination, poor response to decongestants, maxillary toothache, and abnormal transillumination. Previous upper respiratory tract infection, purulent rhinorrhea, facial pain on bending forward, unilateral maxillary pain, and tooth pain were significantly associated with positive ultrasonography in a Dutch study of 400 primary care patients with 441 episodes of suspected rhinosinusitis (26). Studies that rely on plain sinus radiography or ultrasonography as the diagnostic standard must be interpreted cautiously because these techniques overestimate the presence of bacterial infection by as much as 50%, offering a large opportunity for misclassification bias (29, 30). 3.2 Considering the results of all seven studies, purulent nasal discharge, maxillary tooth or facial pain (especially when unilateral), unilateral maxillary sinus tenderness, and worsening of symptoms after initial improvement seem to be helpful for predicting a higher likelihood of bacterial infection in patients with rhinosinusitis-like symptoms. Although generalized facial pain or tenderness, postnasal drainage, headache, and cough are commonly thought to have diagnostic value, no convincing evidence shows that they are helpful in distinguishing acute bacterial rhinosinusitis from prolonged viral rhinosinusitis. A previous diagnosis of rhinosinusitis is also not a predictor of bacterial rhinosinusitis. Principle 3. Sinus radiography is not recommended for diagnosis in routine cases [B]. 4.0 Several investigators have studied the accuracy of sinus radiography in predicting the presence of purulent sinus fluid by using complete opacification, air-fluid level, or various degrees of mucosa thickening as the diagnostic criteria (31 34). Complete opacification and air-fluid level are the most specific findings, with specificities of 85% (range, 76% to 91%) and 80% (range, 20 March 2001 Annals of Internal Medicine Volume 134 Number 6 501
5 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part 2 71% to 87%), respectively (30). The finding of mucosal thickening has a low specificity, probably no better than that of skilled clinical judgment, which is 40% to 50%. The absence of all three findings has an estimated sensitivity of approximately 90% and is helpful in ruling out bacterial rhinosinusitis (35). Given these test characteristics and the known high prevalence of abnormal radiography findings in patients with viral rhinosinusitis, sinus radiography has limited value in routine diagnosis of acute bacterial rhinosinusitis. Principle 4. Acute rhinosinusitis resolves without antibiotic treatment in most cases [A]. Symptomatic treatment and reassurance is the preferred initial management strategy for patients with mild symptoms. Antibiotic therapy should be reserved for patients with moderately severe symptoms who meet the criteria for the clinical diagnosis of acute bacterial rhinosinusitis (symptoms that last 7 days and include maxillary pain in the face or teeth and purulent nasal secretions) and for those with severe rhinosinusitis symptoms, regardless of duration of illness. For initial treatment, the most narrow-spectrum agent that is active against the likely pathogens, S. pneumoniae and H. influenzae, should be used. 5.0 Randomized, double-blind, placebo-controlled trials of antibiotic treatment for acute bacterial rhinosinusitis using pretreatment and post-treatment culture of sinus aspirates have not been performed. However, nonrandomized treatment trials have shown appropriate antibiotics to be highly effective in eradicating or substantially reducing bacterial growth in the sinuses (13). Antibiotic treatment is effective from a bacteriologic standpoint. Is it effective from a clinical standpoint? 5.1 Five randomized, double-blind clinical trials with good methods have compared antibiotics with placebo for treatment of acute rhinosinusitis in adults (35 39). Two meta-analyses, one performed under the auspices of the Cochrane Collaboration (40) and the other performed under contract from the Agency for Healthcare Research and Quality (41), have recently been published. Both studies concluded that, although antibiotics are statistically more effective than placebo in reducing or eliminating symptoms at 10 and 14 days, the effect size (degree of benefit) is relatively small and most placebo-treated patients improve without antibiotic therapy. The specific findings of each of these five trials are well summarized by Williams and coworkers (40). Four used plain radiography for diagnosis of sinusitis (36 39), and one (35) used computed tomography. When considered in aggregate, 47% of the antibiotic-treated patients and 32% of controls were considered cured at 10 to 14 days of follow-up, while 81% of antibiotictreated patients and 66% of controls were responders (with clinical findings of either cure or improvement) (39). This is an absolute benefit of 15%, with a number needed to treat for benefit of approximately seven. 5.2 However, the two most recent placebo-controlled trials of acute rhinosinusitis in primary care failed to find a significant clinical effect of antibiotic treatment. Stalman and colleagues (38) studied the effectiveness of doxycycline compared with placebo in general practice patients with symptoms of bacterial rhinosinusitis. The inclusion criteria were based on guidelines of the Dutch College of General Practitioners: three main symptoms (reports of symptoms after a common cold or influenza, purulent nasal discharge, and pain in the maxillary sinuses on bending forward) or two main symptoms and one other symptom (predominately unilateral maxillary pain, toothache, or pain when chewing). There was no significant difference in time to resolution of facial pain and return to normal activities. Using radiography as the diagnostic standard, van Buchem and associates (40) found no statistically significant advantage of a 7-day course of amoxicillin over placebo at follow-up on day 14. Symptoms were substantially improved or resolved in 83% of patients receiving amoxicillin and 77% of patients receiving placebo. The one modern placebo-controlled trial in a primary care population that showed a positive treatment effect for amoxicillin or penicillin used computed tomographic scanning for diagnosis and study eligibility (35). Only patients with an air-fluid level or complete opacification of a sinus were eligible for inclusion. At day 10 of treatment, 56% of patients who received placebo, 82% of those who received penicillin, and 89% of those who received amoxicillin were substantially better. 5.3 The reason these clinical trials as a whole show antibiotic treatment of sinusitis to be less efficacious than one might predict from the bacteriologic studies can be explained by the Pollyanna phenomenon (42). That is, because the clinical and radiologic diagnosis of acute bacterial rhinosinusitis is inaccurate, the measured treatment effect of antibiotics for the entire treatment group is diluted by the cases that do not truly have March 2001 Annals of Internal Medicine Volume 134 Number 6
6 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part 2 bacterial infection. Thus, the treatment trial that used a more specific diagnostic standard (positive results on computed tomography scan) showed a significant benefit for antibiotics. In contrast, the trials using the lessspecific diagnostic standards clinical diagnosis (38) and radiographic diagnosis (39) did not. High rates of recovery and resolution in the placebo groups could also be caused by symptomatic treatments (local nasal decongestants or analgesics) that have a large impact on illness resolution. When the 40% to 50% prevalence of bacterial rhinosinusitis in patients whose diagnosis is established by signs and symptoms and the modest effectiveness of antibiotic treatment were considered, a cost-effectiveness model sponsored by the Agency for Healthcare Research and Quality favored antibiotic treatment for patients with moderate to severe symptoms and symptomatic treatment for those with mild symptoms (Balk EM, Zucher DR, Engels EA, Wong JB, Williams JW, Lau J. Strategies for diagnosing and treating acute bacterial sinusitis: a cost-effectiveness analysis. Submitted for publication). 5.4 Three recent meta-analyses have concluded that newer and broad-spectrum antibiotics are not significantly more effective than narrow-spectrum agents (40, 41, 43). However, because of the rapid increase in antibiotic resistance of S. pneumoniae and H. influenzae, physicians must consider current recommendations for treating infection with these organisms when making treatment decisions. 5.5 Serious complications of acute bacterial rhinosinusitis, such as meningitis, brain abscess, and periorbital cellulitis, are rare, and good data on the frequency of these events in treated compared with untreated patients are not available (41). An estimated 1 of hospital discharges in the United States is for brain abscess, and the proportion of these admissions due to acute sinusitis is unknown (41). No serious complications have been reported in sinusitis treatment trials among patients who received placebo. Nonetheless, some patients with acute bacterial rhinosinusitis may rarely present with dramatic symptoms of severe unilateral maxillary pain, swelling, and fever. These patients must be treated promptly with an appropriate antibiotic and may require surgical referral for sinus drainage. Patients with a clinical diagnosis of acute bacterial sinusitis who do not respond to antibiotic treatment should be referred for further evaluation. Additional diagnostic procedures to guide therapy at this juncture may include computed tomography to assess anatomic abnormalities or sinus aspiration for culture. 6.0 The results of eight randomized trials of various symptomatic treatments of rhinosinusitis symptoms in adults have been inconclusive (44 51). Topically or orally administered -adrenergic agents, proteolytic enzymes, mucolytic agents, antihistamines, and corticosteroids have been used. Theoretically, agents that encourage drainage of sinus secretions may be of value. Well-designed placebo-controlled trials of these ancillary treatments are needed to determine their effectiveness in treating acute rhinosinusitis. These treatments can be offered to patients with mild symptoms as an alternative to an antibiotic. Pain control is always important because more than 50% of patients with acute bacterial rhinosinusitis report facial pain (24 28). Topical and oral decongestants may ameliorate some of the nasal symptoms and promote mucus clearance. All patients should receive a careful explanation of the rationale for management; they should also be educated about signs and symptoms of worsening that should prompt them to contact a physician. CONCLUSIONS 7.0 The greatest barrier to efficient antibiotic treatment of acute bacterial rhinosinusitis is lack of a simple and accurate diagnostic test. Until a better test is widely available in office practice, the office diagnosis of acute bacterial rhinosinusitis will continue to depend largely on clinical judgment and will remain imprecise. Duration of illness is a useful clinical criterion because acute bacterial sinusitis is not common in patients whose symptoms last less than 7 days. Patients who do not have persistent maxillary facial or tooth pain or tenderness accompanied by purulent nasal drainage are unlikely to have bacterial rhinosinusitis, regardless of duration of illness. We do not recommend routine sinus radiography or limited sinus computed tomography series given the high prevalence of abnormal radiographic findings in patients with viral rhinosinusitis. Recent recommendations from the Sinus and Allergy Foundation also recommend radiography for patients who do not respond within 72 hours after antibiotics are given (52). 7.1 Because most patients with a clinical diagnosis 20 March 2001 Annals of Internal Medicine Volume 134 Number 6 503
7 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part 2 of acute rhinosinusitis improve without antibiotic treatment, symptomatic treatment or reassurance is the preferred initial management strategy, except for patients with moderate to severe symptoms. In most cases, only patients with the specific findings of maxillary pain or tenderness in the face or teeth and persistent purulent nasal discharge who are not improving after 7 days and those with severe rhinosinusitis symptoms, regardless of duration, should be treated with antibiotics. When an antibiotic is prescribed, it should be the most narrowspectrum agent that is active against the likely pathogens, S. pneumoniae and H. influenzae. Prescribing physicians should consider factors that predispose patients to antibiotic-resistant bacteria, such as contact with children in daycare centers or recent antibiotic use. Amoxicillin is commonly recommended, and previous reviews have failed to demonstrate that any antibiotic is superior to amoxicillin in clinical response. According to many authorities, amoxicillin continues to be the favored drug, although higher-than-customary doses may be required in some cases (52). From Michigan State University, East Lansing, Michigan; Johns Hopkins University, Baltimore, Maryland; Centers for Disease Control and Prevention, Atlanta, Georgia; University of Colorado Health Sciences Center, Denver, Colorado; University of California, Los Angeles, Los Angeles, California; and University of Utah, Salt Lake City, Utah. Acknowledgments: External review has included feedback from the Centers for Disease Control and Prevention; the Clinical Efficacy Assessment Subcommittee; and representatives of the American Academy of Family Physicians, the American College of Emergency Physicians, and the Infectious Diseases Society of America. Role of the Funding Source: The Centers for Disease Control and Prevention provided partial support for the development of the principles and required final approval of all manuscripts submitted for publication. Requests for Single Reprints: Richard E. Besser, MD, Respiratory Diseases Branch (C-23), Centers for Disease Control and Prevention, 1600 Clifton Road NE, Atlanta, GA 30333; , rbesser@cdc.gov. Current Author Addresses: Dr. Hickner: B111 Clinical Center, Michigan State University Department of Family Practice, East Lansing, MI Dr. Bartlett: Johns Hopkins University School of Medicine, 1830 East Monument Street, Suite 463A, Baltimore, MD Dr. Besser: Respiratory Diseases Branch (C-23), Centers for Disease Control and Prevention, 1600 Clifton Road NE, Atlanta, GA Dr. Gonzales: Campus Box B-180, 4200 East Ninth Avenue, Denver, CO Dr. Hoffman: University of California, Los Angeles, 924 Westwood Boulevard, Los Angeles, CA Dr. Sande: University of Utah, 50 North Medical Drive, Salt Lake City, UT References 1. Dowell SF, Schwartz B. Resistant pneumococci: protecting patients through judicious use of antibiotics. Am Fam Physician. 1997;55: , [PMID: ] 2. Kunin CM. Resistance to antimicrobial drugs a worldwide calamity. Ann Intern Med. 1993;118: [PMID: ] 4. Cohen ML. Epidemiology of drug resistance: implications for a post-antimicrobial era. Science. 1992;257: [PMID: ] 5. Ambulatory care visits to physician s offices, hospital outpatient departments, and emergency departments: United States, National Center for Health Statistics. Series 13, No Hyattsville, MD: U.S. Dept. of Health and Human Services; Willett LR, Carson JL, Williams JW Jr. Current diagnosis and management of sinusitis. J Gen Intern Med. 1994;9: [PMID: ] 7. Gonzales R, Steiner JF, Lum A, Barrett PH Jr. Decreasing antibiotic use in ambulatory practice: impact of a multidimensional intervention on the treatment of uncomplicated acute bronchitis in adults. JAMA. 1999;281: [PMID: ] 8. Dosh SA, Hickner JM, Mainous AG 3rd, Ebell MH. Predictors of antibiotic prescribing for nonspecific upper respiratory infections, acute bronchitis, and acute sinusitis. An UPRNet study. Upper Peninsula Research Network. J Fam Pract. 2000;49: [PMID: ] 9. McCaig LF, Hughes JM. Trends in antimicrobial drug prescribing among office-based physicians in the United States. JAMA. 1995;273: [PMID: ] 10. Gonzales R, Bartlett JG, Besser RE, Cooper RJ, Hickner JM, Hoffman JR, et al. Principles of appropriate antibiotic use for treatment of acute respiratory tract infections in adults: background, specific aims, and methods. Ann Intern Med. 2001;134: Infectious rhinosinusitis in adults: classification, etiology and management. International Rhinosinusitis Advisory Board. Ear Nose Throat J. 1997;76:1-22. [PMID: ] 12. Stammberger H. Endoscopic endonasal surgery concepts in treatment of recurring rhinosinusitis. Part I. Anatomic and pathophysiologic considerations. Otolaryngol Head Neck Surg. 1986;94: [PMID: ] 13. Gwaltney JM Jr. Acute community-acquired sinusitis. Clin Infect Dis. 1996; 23: [PMID: ] 14. Hamory BH, Sande MA, Sydnor A Jr, Seale DL, Gwaltney JM Jr. Etiology and antimicrobial therapy of acute maxillary sinusitis. J Infect Dis. 1979;139: [PMID: ] 15. Williams RB 3d, Gwaltney JM Jr. Allergic rhinitis or virus cold? Nasal smear eosinophilia in differential diagnosis. Ann Allergy. 1972;30: [PMID: ] 16. Puhakka T, Makela MJ, Alanen A, Kallio T, Korsoff L, Arstila P, et al. Sinusitis in the common cold. J Allergy Clin Immunol. 1998;102: [PMID: ] 17. Gwaltney JM Jr, Phillips CD, Miller RD, Riker DK. Computed tomographic study of the common cold. N Engl J Med. 1994;330: [PMID: ] March 2001 Annals of Internal Medicine Volume 134 Number 6
8 Appropriate Antibiotic Use for Acute Rhinosinusitis, Part Berg O, Carenfelt C, Rystedt G, Anggard A. Occurrence of asymptomatic sinusitis in common cold and other acute ENT-infections. Rhinology. 1986;24: [PMID: ] 19. Dingle JH, Badger GF, Jordan WS Jr. Illness in the Home: A Study of 25,000 Illnesses in a Group of Cleveland Families. Cleveland, OH: Western Reserve Univ Pr; 1964: McIsaac WJ, Levine N, Goel V. Visits by adults to family physicians for the common cold. J Fam Pract. 1998;47: [PMID: ] 21. Gwaltney JM Jr, Hendley JO, Simon G, Jordan WS Jr. Rhinovirus infections in an industrial population. II. Characteristics of illness and antibody response. JAMA. 1967;202: [PMID: ] 22. Hansen JG, Schmidt H, Rosborg J, Lund E. Predicting acute maxillary sinusitis in a general practice population. BMJ. 1995;311: [PMID: ] 23. Berg O, Carenfelt C. Analysis of symptoms and clinical signs in the maxillary sinus empyema. Acta Otolaryngol. 1988;105: [PMID: ] 24. Lindbaek M, Hjortdahl P, Johnsen UL. Use of symptoms, signs, and blood tests to diagnose acute sinus infections in primary care: comparison with computed tomography. Fam Med. 1996;28: [PMID: ] 25. Williams JW Jr, Simel DL, Roberts L, Samsa GP. Clinical evaluation for sinusitis. Making the diagnosis by history and physical examination. Ann Intern Med. 1992;117: [PMID: ] 26. van Duijn NP, Brouwer HJ, Lamberts H. Use of symptoms and signs to diagnose maxillary sinusitis in general practice: comparison with ultrasonography. BMJ. 1992;305: [PMID: ] 27. van Buchem L, Peeters M, Beaumont J, Knottnerus JA. Acute maxillary sinusitis in general practice: the relation between clinical picture and objective findings. European Journal of General Practice. 1995;1: Axelsson A, Runze U. Symptoms and signs of acute maxillary sinusitis. ORL J Otorhinolaryngol Relat Spec. 1976;38: [PMID: ] 29. Evans FO Jr, Sydnor JB, Moore WE, Moore GR, Manwaring JL, Brill AH, et al. Sinusitis of the maxillary antrum. N Engl J Med. 1975;293: [PMID: ] 30. Engels EA, Terrin N, Barza M, Lau J. Meta-analysis of diagnostic tests for acute sinusitis. J Clin Epidemiol. 2000;53: [PMID: ] 31. McNeill RA. Comparison of findings on transillumination, x-ray and lavage of the maxillary sinus. Journal of Laryngology and Otology. 1963;77: Revonta M. Ultrasound in the diagnosis of maxillary and frontal sinusitis. Acta Otolaryngol Suppl. 1980;370:1-55. [PMID: ] 33. Laine K, Maatta T, Varonen H, Makela M. Diagnosing acute maxillary sinusitis in primary care: a comparison of ultrasound, clinical examination and radiography. Rhinology. 1998;36:2-6. [PMID: ] 34. Savolainen S, Pietola M, Kiukaanniemi H, Lappalainen E, Salminen M, Mikkonen P. An ultrasound device in the diagnosis of acute maxillary sinusitis. Acta Otolaryngol Suppl. 1997;529: [PMID: ] 35. Lindbaek M, Hjortdahl P, Johnsen UL. Randomised, double blind, placebo controlled trial of penicillin V and amoxycillin in treatment of acute sinus infections in adults. BMJ. 1996;313: [PMID: ] 36. Axelsson A, Chidekel N, Grebelius N, Jensen C. Treatment of acute maxillary sinusitis. A comparison of four different methods. Acta Otolaryngol. 1970; 70:71-6. [PMID: ] 37. Gananca M, Trabulsi LR. The therapeutic effects of cyclacillin in acute sinusitis: in vitro and in vivo correlations in a placebo-controlled study. Curr Med Res Opin. 1973;1: [PMID: ] 38. Stalman W, van Essen GA, van der Graaf Y, de Melker RA. The end of antibiotic treatment in adults with acute sinusitis-like complaints in general practice? A placebo-controlled double-blind randomized doxycycline trial. Br J Gen Pract. 1997;47: [PMID: ] 39. van Buchem FL, Knottnerus JA, Schrijnemaekers VJ, Peeters MF. Primarycare-based randomised placebo-controlled trial of antibiotic treatment in acute maxillary sinusitis. Lancet. 1997;349: [PMID: ] 40. Williams JW Jr, Aguilar C, Makela M, Cornell J, Hollman D, Chiquette E, et al. Antibiotic therapy for acute sinusitis: a systematic literature review. In: Douglas R, Bridges-Webb C, Glasziou P, Lozano J, Steinhoff M, Wang E, eds. Acute Respiratory Infections Module of The Cochrane Database of Systematic Reviews. The Cochrane Library. Oxford: Updated Software; Zucher DR, Balk E, Engels E, Barza M, Lau J. Agency for Health Care Policy and Research Publication No. 99-E016: Evidence Report/Technology Assessment Number 9. Diagnosis and Treatment of Acute Bacterial Rhinosinusitis. Available at: Marchant CD, Carlin SA, Johnson CE, Shurin PA. Measuring the comparative efficacy of antibacterial agents for acute otitis media: the Pollyanna phenomenon. J Pediatr. 1992;120:72-7. [PMID: ] 43. de Bock GH, Dekker FW, Stolk J, Springer MP, Kievit J, van Houwelingen JC. Antimicrobial treatment in acute maxillary sinusitis: a meta-analysis. J Clin Epidemiol. 1997;50: [PMID: ] 44. Taub SJ. The use of bromelains in sinusitis: a double-blind clinical evaluation. Eye Ear Nose Throat Mon. 1967;46: [PMID: ] 45. Ryan RE. A double-blind clinical evaluation of bromelains in the treatment of acute sinusitis. Headache. 1967;7:13-7. [PMID: ] 46. Seltzer AP. Adjunctive use of bromelains in sinusitis: a controlled study. Eye Ear Nose Throat Mon. 1967;46: [PMID: ] 47. Lewison E. Comparison of the effectiveness of topical and oral nasal decongestants. Eye Ear Nose Throat Mon. 1970;49:16-8. [PMID: ] 48. Wiklund L, Stierna P, Berglund R, Westrin KM, Tonnesson M. The efficacy of oxymetazoline administered with a nasal bellows container and combined with oral phenoxymethyl-penicillin in the treatment of acute maxillary sinusitis. Acta Otolaryngol Suppl. 1994;515: [PMID: ] 49. Harris PG. A comparison of bisolvomycin and oxytetracycline in the treatment of acute infective sinusitis. Practitioner. 1971;207: [PMID: ] 50. Meltzer EO, Orgel HA, Backhaus JW, Busse WW, Druce HM, Metzger WJ, et al. Intranasal flunisolide spray as an adjunct to oral antibiotic therapy for sinusitis. J Allergy Clin Immunol. 1993;92: [PMID: ] 51. Braun JJ, Alabert JP, Michel FB, Quiniou M, Rat C, Cougnard J, et al. Adjunct effect of loratadine in the treatment of acute sinusitis in patients with allergic rhinitis. Allergy. 1997;52: [PMID: ] 52. Antimicrobial treatment guidelines for acute bacterial rhinosinusitis. Sinus and Allergy Health Partnership. Otolaryngol Head Neck Surg. 2000;123(1 Pt 2): [PMID: ] 20 March 2001 Annals of Internal Medicine Volume 134 Number 6 505
The clinical diagnosis of acute purulent sinusitis in general practice a review
 The clinical diagnosis of acute purulent sinusitis in general practice a review Morten Lindbæk and Per Hjortdahl SUMMARY Acute sinusitis is a common illness in primary care. Studies have demonstrated the
The clinical diagnosis of acute purulent sinusitis in general practice a review Morten Lindbæk and Per Hjortdahl SUMMARY Acute sinusitis is a common illness in primary care. Studies have demonstrated the
Acute rhinosinusitis is defined as. Acute Bacterial Rhinosinusitis in Adults: Part I. Evaluation
 This is a corrected version of the article that appeared in print. Acute Bacterial Rhinosinusitis in Adults: Part I. Evaluation DEWEY C. SCHEID, M.D., M.P.H., and ROBERT. M. HAMM, PH.D. University of Oklahoma
This is a corrected version of the article that appeared in print. Acute Bacterial Rhinosinusitis in Adults: Part I. Evaluation DEWEY C. SCHEID, M.D., M.P.H., and ROBERT. M. HAMM, PH.D. University of Oklahoma
How Family Physicians Distinguish Acute Sinusitis From Upper Respiratory Tract Infection: A Retrospective Analysis
 How Family Physicians Distinguish Acute Sinusitis From Upper Respiratory Tract Infection: A Retrospective Analysis David R. Little, MD, MS, Barbara 1. Mann, PhD, and Christopher j. Godbout, MD Background:
How Family Physicians Distinguish Acute Sinusitis From Upper Respiratory Tract Infection: A Retrospective Analysis David R. Little, MD, MS, Barbara 1. Mann, PhD, and Christopher j. Godbout, MD Background:
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Diagnosing acute maxillary sinusitis in primary care: A comparison of ultrasound, clinical examination and radiography*
 Rhinology, 36, 2 6, 1998 Diagnosing acute maxillary sinusitis in primary care: A comparison of ultrasound, clinical examination and radiography* Karri Laine 1, Tuomo Määttä 2, Helena Varonen 3, Marjukka
Rhinology, 36, 2 6, 1998 Diagnosing acute maxillary sinusitis in primary care: A comparison of ultrasound, clinical examination and radiography* Karri Laine 1, Tuomo Määttä 2, Helena Varonen 3, Marjukka
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Treatment of acute rhinosinusitis diagnosed by clinical criteria or ultrasound in primary care A placebo-controlled randomised trial
 ORIGINAL PAPER Treatment of acute rhinosinusitis diagnosed by clinical criteria or ultrasound in primary care A placebo-controlled randomised trial Helena Varonen 1, Ilkka Kunnamo 2, Seppo Savolainen 3,
ORIGINAL PAPER Treatment of acute rhinosinusitis diagnosed by clinical criteria or ultrasound in primary care A placebo-controlled randomised trial Helena Varonen 1, Ilkka Kunnamo 2, Seppo Savolainen 3,
UPPER RESPIRATORY TRACT INFECTIONS. IAP UG Teaching slides
 UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
Acute Bacterial Sinusitis
 The new england journal of medicine clinical practice Acute Bacterial Sinusitis Jay F. Piccirillo, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
The new england journal of medicine clinical practice Acute Bacterial Sinusitis Jay F. Piccirillo, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
Upper Respiratory Tract Infections / 42
 Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
ORIGINAL ARTICLE. Validity of Ultrasonography in Diagnosis of Acute Maxillary Sinusitis
 ORIGINAL ARTICLE Validity of Ultrasonography in Diagnosis of Acute Maxillary Sinusitis Tuomo Puhakka, MD; Terho Heikkinen, MD; Mika J. Mäkelä, MD; Anu Alanen, MD; Timo Kallio, MD; Leo Korsoff, MD; Jouko
ORIGINAL ARTICLE Validity of Ultrasonography in Diagnosis of Acute Maxillary Sinusitis Tuomo Puhakka, MD; Terho Heikkinen, MD; Mika J. Mäkelä, MD; Anu Alanen, MD; Timo Kallio, MD; Leo Korsoff, MD; Jouko
Choosing an appropriate antimicrobial agent. 3) the spectrum of potential pathogens
 Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
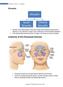 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
4/7/13 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC
 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Prefe f rred d t e t rm: : rhi h no n s o inu n s u iti t s
 HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
CAREFUL ANTIBIOTIC USE
 Make promoting appropriate antibiotic use part of your routine clinical practice When parents ask for antibiotics to treat viral infections: PRACTICE TIPS Create an office environment to promote the reduction
Make promoting appropriate antibiotic use part of your routine clinical practice When parents ask for antibiotics to treat viral infections: PRACTICE TIPS Create an office environment to promote the reduction
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Sinusitis/Rhinosinusitis SINUSITIS/RHINOSINUSITIS
 1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
Retrospective Analysis of Patients with Allergy Sinusitis
 Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Sinusitis in the common cold
 Sinusitis in the common cold Tuomo Puhakka, MD, a Mika J. Mäkelä, MD, a,b Anu Alanen, MD, c Timo Kallio, MD, c Leo Korsoff, MD, c Pertti Arstila, MD, e Maija Leinonen, PhD, f Markku Pulkkinen, RN, g Jouko
Sinusitis in the common cold Tuomo Puhakka, MD, a Mika J. Mäkelä, MD, a,b Anu Alanen, MD, c Timo Kallio, MD, c Leo Korsoff, MD, c Pertti Arstila, MD, e Maija Leinonen, PhD, f Markku Pulkkinen, RN, g Jouko
SINUSITIS/RHINOSINUSITIS
 1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
AMERICAN ACADEMY OF PEDIATRICS. Clinical Practice Guideline: Management of Sinusitis
 AMERICAN ACADEMY OF PEDIATRICS Subcommittee on Management of Sinusitis and Committee on Quality Improvement Clinical Practice Guideline: Management of Sinusitis ABSTRACT. This clinical practice guideline
AMERICAN ACADEMY OF PEDIATRICS Subcommittee on Management of Sinusitis and Committee on Quality Improvement Clinical Practice Guideline: Management of Sinusitis ABSTRACT. This clinical practice guideline
Diagnosis and Treatment of Respiratory Illness in Children and Adults Guideline
 Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Reducing Antibiotic Use in Common Infections in Family Practice
 Reducing Antibiotic Use in Common Infections in Family Practice W. Rosser Emeritus Professor Department of Family Medicine Queen s University Discussion with Honorary Teachers, University of Hong Kong
Reducing Antibiotic Use in Common Infections in Family Practice W. Rosser Emeritus Professor Department of Family Medicine Queen s University Discussion with Honorary Teachers, University of Hong Kong
Respiratory System Virology
 Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief.
 Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Middleton Chapter 43 (pages ) Rhinosinusitis and Nasal Polyps Prepared by: Malika Gupta, MD
 FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
Calling Acute Bronchitis a Chest Cold May Improve Patient Satisfaction with Appropriate Antibiotic Use
 Calling Acute Bronchitis a Chest Cold May Improve Patient Satisfaction with Appropriate Antibiotic Use T. Grant Phillips, MD, and John Hickner, MD, MS Background: Overuse of antibiotics for acute respiratory
Calling Acute Bronchitis a Chest Cold May Improve Patient Satisfaction with Appropriate Antibiotic Use T. Grant Phillips, MD, and John Hickner, MD, MS Background: Overuse of antibiotics for acute respiratory
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Preventing sinusitis Health24. Page 3
 DOWNLOAD OR READ : TREAT AND PREVENT SINUSITIS WHAT YOUR DOCTOR ISNT TELLING YOU SINUS INFECTION SINUSITIS SYMPTOMS SINUSITIS TREATMENT SINUS CURE CHRONIC SINUSITIS SYMPTOMS TRANSCEND MEDIOCRITY BOOK 35
DOWNLOAD OR READ : TREAT AND PREVENT SINUSITIS WHAT YOUR DOCTOR ISNT TELLING YOU SINUS INFECTION SINUSITIS SYMPTOMS SINUSITIS TREATMENT SINUS CURE CHRONIC SINUSITIS SYMPTOMS TRANSCEND MEDIOCRITY BOOK 35
Definition. Otitis Media with effusion (OME)
 Otitis Media. 1 Dr,wegdan saeed ALFHAL 2 Definition Acute Otitis Media (AOM) acute onset of symptoms, evidence of a middle ear effusion, and signs or symptoms of middle ear inflammation. Otitis Media with
Otitis Media. 1 Dr,wegdan saeed ALFHAL 2 Definition Acute Otitis Media (AOM) acute onset of symptoms, evidence of a middle ear effusion, and signs or symptoms of middle ear inflammation. Otitis Media with
Acute sinusitis is almost always a FAMILY PRACTICE
 JFP_0906_Williamson OR.Final 8/21/06 9:22 AM Page 789 Acute sinusitis: Which factors do FPs believe are most diagnostic and best predict antibiotic efficacy? A questionnaire-and-case-vignette study reveals
JFP_0906_Williamson OR.Final 8/21/06 9:22 AM Page 789 Acute sinusitis: Which factors do FPs believe are most diagnostic and best predict antibiotic efficacy? A questionnaire-and-case-vignette study reveals
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD)
 Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Background. Background. AAP (2013) Guidelines. Background 4/19/2016
 Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Sinusitis. 12 weeks. Subacute sinusitis: An inflammation lasting 4 to 8 weeks. weeks or longer Re urre t si usitis: Se eral atta ks ithi a year
 Sinusitis 12 weeks. Sinusitis, also known as a sinus infection or rhinosinusitis, is inflammation of the sinuses resulting in symptoms. Common signs and symptoms include thick nasal mucous, a plugged nose,
Sinusitis 12 weeks. Sinusitis, also known as a sinus infection or rhinosinusitis, is inflammation of the sinuses resulting in symptoms. Common signs and symptoms include thick nasal mucous, a plugged nose,
Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre
 Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
Acute rhinosinusitis is a common disease in family practice.1 Most. Predicting Prognosis and Effect of Antibiotic Treatment in Rhinosinusitis
 Predicting Prognosis and Effect of Antibiotic Treatment in Rhinosinusitis An De Sutter, MD, PhD 1 Marieke Lemiengre, MD 2 Georges Van Maele, PhD 3 Mieke van Driel, MD, MS 1 Marc De Meyere, MD, PhD 1 Thierry
Predicting Prognosis and Effect of Antibiotic Treatment in Rhinosinusitis An De Sutter, MD, PhD 1 Marieke Lemiengre, MD 2 Georges Van Maele, PhD 3 Mieke van Driel, MD, MS 1 Marc De Meyere, MD, PhD 1 Thierry
Treatment Options for Chronic Sinusitis
 Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Sinusitis in Adults UP TO DATE
 Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Treatment & Management of Acute Sinusitis in the Primary Care Setting
 University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
PIDS AND RESPIRATORY DISORDERS
 PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
+ Conflict of interest. + Sinus and Nasal Anatomy. + What is your diagnosis? 1) Allergic Rhinitis. 2) Non-Allergic rhinitis. 3) Chronic Rhinosinusitis
 Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy.
 This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/92131/
This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/92131/
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
Received 25 November 2002/Returned for modification 14 February 2003/Accepted 11 April 2003
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
MANAGEMENT of BACTERIAL RHINOSINUSITIS
 MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of
MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017
 Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Chronic Rhinosinusitis-Treatment
 Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Appropriate Antibiotic Prescribing. Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy
 Appropriate Antibiotic Prescribing Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy Objectives Discuss CDCs Core Elements of abx stewardship.
Appropriate Antibiotic Prescribing Frank Romanelli, Pharm.D., MPH, AAHIVP Professor & Associate Dean Paul F. Parker Endowed Professor of Pharmacy Objectives Discuss CDCs Core Elements of abx stewardship.
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Consumer summary. Endoscopic modified Lothrop procedure for the. treatment of chronic frontal sinusitis
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Sinusitis & its complication. MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University
 Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Update on Rhinosinusitis 2013 AAP Guidelines Review
 Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
AMERICAN ACADEMY OF PEDIATRICS
 AMERICAN ACADEMY OF PEDIATRICS Technical Report: Evidence for the Diagnosis and Treatment of Acute Uncomplicated Sinusitis in Children: A Systematic Overview John P. A. Ioannidis, MD*, and Joseph Lau,
AMERICAN ACADEMY OF PEDIATRICS Technical Report: Evidence for the Diagnosis and Treatment of Acute Uncomplicated Sinusitis in Children: A Systematic Overview John P. A. Ioannidis, MD*, and Joseph Lau,
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
JMSCR Vol 05 Issue 10 Page October 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-45 DOI: https://dx.doi.org/1.18535/jmscr/v5i1.116 Nasal Polyps- Causes and Associated Symptoms-
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-45 DOI: https://dx.doi.org/1.18535/jmscr/v5i1.116 Nasal Polyps- Causes and Associated Symptoms-
Influenza. What Is Influenza?
 Flu is usually a mild, but uncomfortable disease. You can treat it yourself by staying home and drinking plenty of fluids. What Is?, often just called the flu, is the most common disease in the world,
Flu is usually a mild, but uncomfortable disease. You can treat it yourself by staying home and drinking plenty of fluids. What Is?, often just called the flu, is the most common disease in the world,
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o
 A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488
 National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Evaluation of Ultrasound Efficiency in the Diagnosis of Acute Maxillary Sinusitis in Comparison with CT Scan Findings in Children Aged 5 to 15 Years
 Journal of Research in Medical and Dental Sciences 2018, Volume 6, Issue 3, Page No: 363-367 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Evaluation
Journal of Research in Medical and Dental Sciences 2018, Volume 6, Issue 3, Page No: 363-367 Copyright CC BY-NC-ND 4.0 Available Online at: www.jrmds.in eissn No. 2347-2367: pissn No. 2347-2545 Evaluation
Section Editor Mark D Aronson, MD
 1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Measure #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Disclaimers. Topical Therapy. The Problem. Topical Therapy for Chronic Rhinosinusitis No Disclosures
 Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Follow this and additional works at:
 Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 5-1-2004 Chris Del Mar Bond University, chris_del_mar@bond.edu.au Paul Glasziou
Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 5-1-2004 Chris Del Mar Bond University, chris_del_mar@bond.edu.au Paul Glasziou
Diagnosis of maxillary sinusitis in Finnish primary care. Use of imaging techniques
 of maxillary sinusitis in Finnish primary care. Use of imaging techniques Marjukka Mikela' and Kirsiliina Leinonen2 ' National research and development centre for welfare and health, Helsinki, * Helsinki
of maxillary sinusitis in Finnish primary care. Use of imaging techniques Marjukka Mikela' and Kirsiliina Leinonen2 ' National research and development centre for welfare and health, Helsinki, * Helsinki
Optimizing the Management of Upper Respiratory Tract Infections.
 Optimizing the Management of Upper Respiratory Tract Infections. Tania Sih Introduction Until recently, physicians placed very high value the patient s history, and and their clinical assessment. In addition
Optimizing the Management of Upper Respiratory Tract Infections. Tania Sih Introduction Until recently, physicians placed very high value the patient s history, and and their clinical assessment. In addition
Commen Nose Diseases
 Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
CLINICAL PRACTICE GUIDELINE
 This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
Malik Sallam. Ola AL-juneidi. Ammar Ramadan. 0 P a g e
 1 Malik Sallam Ola AL-juneidi Ammar Ramadan 0 P a g e Today's lecture will be about viral upper respiratory tract infections. Those include: common cold, sinusitis, otitis, etc. Infections in the upper
1 Malik Sallam Ola AL-juneidi Ammar Ramadan 0 P a g e Today's lecture will be about viral upper respiratory tract infections. Those include: common cold, sinusitis, otitis, etc. Infections in the upper
Subspecialty Rotation: Otolaryngology
 Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
SINUSITIS IS ASSOCIATED WITH
 ORIGINAL CONTRIBUTION Impact of First-Line vs Second-Line Antibiotics for the Treatment of Acute Uncomplicated Sinusitis Jay F. Piccirillo, MD Douglas E. Mager, BS Mark E. Frisse, MD, MS, MBA Robert H.
ORIGINAL CONTRIBUTION Impact of First-Line vs Second-Line Antibiotics for the Treatment of Acute Uncomplicated Sinusitis Jay F. Piccirillo, MD Douglas E. Mager, BS Mark E. Frisse, MD, MS, MBA Robert H.
Streptococcal Pharyngitis
 Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Respiratory Infections
 Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
ISSN X (Print) Research Article. *Corresponding author Dr.V. Krishna Chaitanya
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
ANTIBIOTICS ACUTE RHINOSINUSITIS IN CHILDREN
 MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
Corporate Medical Policy Septoplasty
 Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Whatever the reason, whatever the season,
 Whatever the reason, whatever the season, S4 AVAMYS Nasal Spray (Suspension). REGISTRATION NUMBER: 41/21.5.1/0968. Each 50 µl spray contains 27,5 µg of fluticasone furoate. Preservative: Benzalkonium chloride
Whatever the reason, whatever the season, S4 AVAMYS Nasal Spray (Suspension). REGISTRATION NUMBER: 41/21.5.1/0968. Each 50 µl spray contains 27,5 µg of fluticasone furoate. Preservative: Benzalkonium chloride
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
Clinical Practice Guideline: Tonsillectomy in Children, Baugh et al Otolaryngology Head and Neck Surgery, 2011 J and: 144 (1 supplement) S1 30.
 Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
