MANAGEMENT of BACTERIAL RHINOSINUSITIS
|
|
|
- Colleen Sanders
- 5 years ago
- Views:
Transcription
1 MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of Family Medicine, University of Illinois, College of Medicine, Rockford Behavioral Objectives After completing this continuing education article, the pharmacist should be able to: 1. Review the epidemiology and pathogenesis of rhinosinusitis, including a discussion of the bacteriologic etiology of rhinosinusitis. 2. Compare and contrast the clinical features of acute (bacterial versus viral) and chronic rhinosinusitis. 4. Formulate a therapeutic plan for a given case study of a patient with acute or chronic rhinosinusitis. 5. Describe the impact of resistance in the development of new drugs and dosage formulations. 3. Understand the importance of judicious use of antibiotics in the treatment of acute and chronic rhinosinusitis. Acute Bacterial Rhinosinusitis Acute bacterial rhinosinusitis (ABRS) occurs in approximately 0.5% to 2% of all cases of viral upper respiratory tract infections (URI). 1 It is estimated that 20 million people acquire ABRS each year in the United States. 2 Sinusitis is the 5th most common diagnosis for which an antibiotic is prescribed in the United States. 3 In fact, 9% and 21% of all antibiotic prescriptions in 2002 were written for pediatric and adult patients, respectively, with a diagnosis of sinusitis. 4 Antibiotic prescriptions for acute sinusitis accounted for approximately $400 million to $600 million in health care expenditures in The estimated total expenditures associated with sinusitis were $3.5 billion in Pathogenesis The 4 pairs of sinuses include the maxillary, ethmoid, frontal, and sphenoid sinuses. Most cases of sinusitis involve the maxillary and/or ethmoid sinuses. Far less common is an isolated infection of the frontal or sphenoid sinus. Sinusitis is more properly termed rhinosinusitis because it is an inflammatory process that involves the mucous membranes of the nose and paranasal sinuses. Rhinosinusitis is classified as acute (sudden onset of symptoms with duration of <4 weeks), subacute (duration 4 to 12 weeks), or chronic (duration >12 consecutive weeks). Viruses are responsible for the majority of acute rhinosinusitis. 6 The human rhinovirus accounts for almost 50% of all viral URIs. Other viruses that can cause acute rhinosinusitis include influenza A and B viruses, parainfluenza virus, respiratory syncytial virus, adenovirus, and enterovirus. Most cases of acute viral rhinosinusitis are selflimiting and resolve within 7 to 10 days. Viruses inhibit macrophage and lymphocyte function, increasing susceptibility to secondary bacterial infection. In addition, viruses cause inflammatory changes which can block the sinus ostia, impair mucous drainage, and cause poor aeration, which creates an environment conducive for developing a bacterial infection. 7 Therefore, ABRS is generally considered as a superinfection that can occur any time during a viral URI. Although infrequent, ABRS may complicate 0.5% to 2% of viral URIs. 1 The incidence of ABRS parallels the pattern of viral URIs and increases during early fall to early spring. Fungi, on rare occasions, can cause rhinosinusitis. Nasal allergy, trauma, swimming, local irritants, and nasal obstruction from polyps or foreign bodies may also precipitate ABRS. ABRS occurs when bacteria that colonize the nasopharynx invade the normally sterile paranasal sinuses. By early childhood, most children are colonized by at least 1 of 3 respiratory tract pathogens, including Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis Colonization may persist for up to 12 months and increases during the winter season when the incidence of viral November
2 Table 1 Distribution of Bacterial Pathogens Associated with Community-Acquired Acute Bacterial Rhinosinusitis in Adults and Children 13 Pathogen Adults (%) Children (%) Streptococcus pneumoniae Haemophilus influenzae Moraxella catarrhalis Anaerobic bacteria Streptococcus spp (specifically S pyogenes) Staphylococcus aureus 0-8 URI rises. 8 S pneumoniae and H influenzae are the most common bacteria isolated from adult patients with community-acquired ABRS (Table 1). 6,11-13 M catarrhalis, anaerobic bacteria, Staphylococcus aureus, and Streptococcus pyogenes can also cause ABRS. The distribution of bacterial pathogens in adults is similar in children, except M catarrhalis is more prevalent in children than adults. 11,12 Rhinosinusitis caused by anaerobic bacteria usually occurs after a dental root infection. 12 The clinical significance of atypical pathogens, including Chlamydia pneumoniae and Mycoplasma pneumoniae, in the pathogenesis of community-acquired ABRS remains unclear. Nosocomial ABRS may occur during hospitalization, especially in patients with nasal colonization by enteric gram-negative bacilli, patients being fed by nasogastric tubes, patients undergoing sedation, and those scoring 7 on the Glasgow coma score. 14 The common pathogens associated with nosocomial rhinosinusitis in adults and children include S aureus, Pseudomonas aeruginosa, Escherichia coli, Klebsiella pneumoniae, and other Enterobacteriaceae organisms. 15,16 Anaerobic bacteria, Candida species (especially Candida albicans), and fungi may also cause nosocomial ABRS. Polymicrobial infection may occur in the hospital setting. 15,16 Clinical Presentation and Diagnosis No single sign or symptom clinically distinguishes a viral rhinosinusitis ( common cold ) from ABRS, presenting a challenge to primary care physicians. Most patients with ABRS initially report symptoms of the common cold, including sneezing, rhinorrhea, nasal congestion, postnasal drip, sore throat, cough, fever, and myalgia. ABRS is a secondary infection that occurs after the onset of a viral URI, especially if symptoms persist after 7 to 10 days or symptoms worsen after 5 to 7 days of illness. 6,13 Double sickening, which occurs when a patient clinically worsens after initial improvement, is also suggestive of ABRS. In patients with rhinorrhea, nose blowing may create enough pressure to introduce bacteria from the middle meatus to the sinus cavity and thereby cause infection. 17 Inflammation of the nose and paranasal sinuses may persist for 2 months. Predictors for ABRS consist of maxillary dental pain, facial erythema/ swelling/pain (especially when unilateral), purulent (thick, colored, and opaque) nasal secretions, history of colored nasal discharge, poor response to decongestants, and fever. 6,13,18 It is important to note that purulent nasal secretions and a change in the color of nasal discharge are not specific indicators of bacterial infection. Purulent discharge can also occur in patients with viral rhinosinusitis. Localization of facial pain or tenderness may assist in determining the affected sinus (ie, cheek or upper teeth pain for maxillary infection, forehead pain for frontal, tenderness over the medial canthal region for ethmoid, or retro-orbital pain for sphenoid). Symptoms of ABRS may persist for 4 weeks. Community-acquired ABRS should be highly considered in patients with persistent symptoms of the common cold lasting more than 7 to 10 days or in patients with worsening symptoms after 5 to 7 days. Persistent or worsening symptoms are highly indicative of a secondary bacterial infection, especially in the presence of facial erythema/swelling/pain, fever, and poor response to decongestants. Some patients may present without initial symptoms of viral URI. In these patients, tooth pain or other signs of a dental infection, a history of allergy, swimming, and/or persistent nasal obstruction are usually present. Nosocomial ABRS should be considered in patients with nasal intubation or impaired sinus drainage. Complications of acute rhinosinusitis that involve the central nervous system, orbit of the eye, and periorbital tissues rarely occur. 6,11 In the presence of these complications, immediate medical attention is necessary. Abnormal vision, altered mental status, and periorbital edema may signify the presence of complications. Patients presenting with these symptoms should be closely monitored. The gold standard for diagnosing ABRS is sinus puncture with subsequent aspirate culture. 6,12 Sinus puncture is rarely performed in the ambulatory setting for immunocompetent patients, however, because it is an invasive and painful procedure. As a result, the diagnosis of ABRS is almost always a clinical diagnosis. Although no single sign or symptom is highly sensitive or specific, the presumptive diagnosis of ABRS based on the overall constellation of clinical findings is generally sufficient for treatment. The use of imaging studies (radiography, computerized tomography [CT], or magnetic resonance imaging) is not necessary to confirm diagnosis because abnormal findings indicate presence of 4 November 2004
3 inflammation without providing the cause (ie, virus, bacteria, or allergy). Imaging studies should, however, be considered in patients with suspected acute complications (eg, orbital cellulitis) or in those individuals with persistent or recurrent infection who are unresponsive to therapy. 11 CT scanning is the imaging study of choice because it is more sensitive and specific than plain radiographs. Treatment Symptomatic relief is the primary goal in the treatment of viral rhinosinusitis. Initial therapy with decongestants, humidifiers, nonsteroidal antiinflammatory drugs (NSAIDs including ibuprofen and naproxen), acetaminophen, and/or possibly mucolytics may help suppress symptoms in patients with viral rhinosinusitis. In the presence of cough, a cough suppressant (dextromethorphan) may be added. Although commonly used, there is lack of evidence supporting the benefits of first-generation antihistamines (eg, chlorpheniramine, brompheniramine, and clemastine), mucolytic agents, and topical intranasal steroids for symptomatic treatment. 1,11 Saline nasal drops or spray, however, may be beneficial by serving as a mild vasoconstrictor, dissolving secretions, and preventing crust formation. 11 Treatment should continue for several days. If symptoms persist after 7 to 10 days or worsen after 5 to 7 days, initiation of antibiotic therapy to treat a potential secondary bacterial infection should be considered. Because the clinical features of viral rhinosinusitis and ABRS are similar, it is not surprising to observe excessive use of antibiotics. Overuse of antibiotics has contributed to emergence and increasing prevalence of resistance in the United States, particularly S pneumoniae to penicillin, trimethoprim/sulfamethoxazole (TMP/SMX), macrolides, doxycycline, and ofloxacin. 19 In addition, H influenzae and M catarrhalis produce -lactamases, which render resistance to all -lactam antibiotics except -lactamase inhibitor combinations and cephalosporins ABRS may spontaneously resolve without antibiotic treatment in both adults and children. 6,22 In fact, the results of 2 meta-analyses indicate that the benefit of using antibiotics in patients with ABRS is minimal and that 69% of patients receiving placebo improve by 14 days. 23,24 If initiated, antibiotic treatment of ABRS should target the common pathogens, particularly S pneumoniae, H influenzae, and M catarrhalis. Although ABRS is usually a self-limited infection, eradication of bacterial pathogens may lead to decreased duration of illness and prevent complications associated with ABRS. Bacterial resistance is an important concern when considering therapeutic options. The risk of acquiring infection caused by resistant pathogens increases with recent antibiotic use. 25 Treatment recommended by the Sinus and Allergy Health Partnership for adult patients with mild community-acquired ABRS and no recent antibiotic exposure are listed in Table The recommended first-line agents are amoxicillin (± clavulanate) and second- and third-generation cephalosporins (specifically, cefuroxime, cefpodoxime, and cefdinir). High-dose amoxicillin (± clavulanate) should be used in patients with suspected drugresistant pneumococci (eg, recent antibiotic use, immunodeficiency, and contact with children attending day care). When M catarrhalis is highly suspected, the use of amoxicillin alone is ineffective because most isolates produce -lactamases. Treatment options for M catarrhalis include amoxicillin with clavulanate and cephalosporins. Because failure rates can reach 25%, TMP/SMX, doxycycline, macrolides, and telithromycin should be reserved for patients with true allergy or intolerance to -lactam antibiotics. Patients generally respond to appropriate treatment within 48 to 72 hours. Recommendation for initial antibiotic treatment provided by the Centers for Disease Control and Prevention and the Infectious Diseases Society of America is similar to the Sinus and Allergy Health Partnership. Initial therapy should include narrow-spectrum agents including amoxicillin, doxycycline, and TMP/SMX. 6 Patients with mild disease who are unresponsive after 72 hours of antibiotic therapy, patients with mild ABRS and recent exposure to antibiotics (within the previous 4 to 6 months), and patients with moderate disease should be treated with respiratory fluoroquinolones (levofloxacin, gatifloxacin, and moxifloxacin), highdose amoxicillin/clavulanate (4 g/ 250 mg per day), or ceftriaxone. 13 Clinical response is predicted in 90% to 92% of patients receiving respiratory fluoroquinolones, ceftriaxone, or amoxicillin/clavulanate, and 83% to 88% with amoxicillin, cefpodoxime, cefixime, cefuroxime, and cefdinir. The recommended duration of therapy for all patients with ABRS is 10 to 14 days, although a 7-day course of amoxicillin (± clavulanate) has been evaluated. 13 Studies indicate that 5 days of ceftriaxone or telithromycin and 3 days of azithromycin are also effective. 13,26,27 Treatment options for ABRS in children (Table 2) are similar to adults, except doxycycline is contraindicated in children <8 years of age because of the risk for permanent teeth discoloration. 11,13 In addition, telithromycin has not been approved by the FDA for pediatric use. 26 Because of its safety, palatability, and low cost, the American Academy of Pediatrics recommends amoxicillin as first-line therapy in children with mild to moderate symptoms. High-dose amoxicillin should be used in patients with suspected drug-resistant pneumococci. High-dose amoxicillin with clavulanate is recommended for children with moderate to severe symptoms (fever 39 C with concurrent purulent nasal discharge for at least 3 to 4 consecutive days or persistent symptoms exceeding 10 days), recent antibiotic exposure, or in those who attend day November
4 Table 2 Recommended Therapy for Community-Acquired Acute Bacterial Rhinosinusitis in Adults and Children 11,13 Daily Dose a Initial Antibiotic Adult Children b Mild disease without recent antibiotic exposure Amoxicillin g/day twice to three times daily mg/kg/day twice daily Amoxicillin/clavulanate c g/250 mg/day twice daily Cefpodoxime proxetil 200 mg twice daily 10 mg/kg/day once daily Cefuroxime axetil 250 mg twice daily 30 mg/kg/day twice daily Cefdinir 600 mg once or 300 mg twice daily 14 mg/kg/day once to twice daily TMP(160 mg)/smx(800 mg) d One tablet twice daily e Doxycycline d 100 mg twice daily NR Clarithromycin d,f 500 mg twice daily 15 mg/kg/day twice daily Azithromycin c 500 mg once daily 10 mg/kg/day once daily Telithromycin d 800 mg daily NR Moderate disease or mild disease with recent antibiotic exposure (previous 4-6 weeks) Respiratory fluoroquinolones d,g NR High-dose amox/clavulanate 4 g/250 mg/day twice daily mg/kg/day amox, 6.4 mg/kg/day clav twice daily Ceftriaxone (IV or IM) 1 g once daily 50 mg/kg/day once daily Clindamycin (± rifampin) d,h mg four times daily mg/kg/day three times daily i TMP/SMX = trimethoprim/sulfamethoxazole; NR = Not recommended; IV = Intravenously; IM = Intramuscularly. a Recommended duration of therapy for most antibiotics is days except for ceftriaxone (5 days), azithromycin (3 days), and telithromycin (5-10 days). b Refer to text for complete description of recommended treatment in children. c Amoxicillin/clavulanate extended-release 1 g/62.5 mg twice daily. d Serve as alternatives for patients with severe allergy or intolerant to -lactam. e TMP/SMX is not an appropriate choice for patients failing amoxicillin. f Clarithromycin extended-release 500 mg once daily. g Levofloxacin 500 mg once daily, gatifloxacin 400 mg once daily, moxifloxacin 400 mg once daily. h Clindamycin is inactive against Haemophilus influenzae and Moraxella catarrhalis. Since resistance may develop, rifampin should not be used as monotherapy. i Other combination therapies for children include clindamycin plus cefixime, TMP/SMX plus rifampin, or high-dose amoxicillin plus cefixime or clindamycin. care. 11 When using high-dose amoxicillin with clavulanate, the recommended dose of clavulanate is 6.4 mg/kg/day to limit the incidence of diarrhea. Other therapeutic options include cefpodoxime, cefuroxime, cefdinir, and ceftriaxone. Except for a history of immediate Type I hypersensitivity reaction to -lactams, children with other types of reactions to one specific -lactam antibiotic may tolerate another -lactam. Therapy should continue for 10 to 14 days, or 7 days after the beginning of clinical improvement. The bacterial pathogens associated with nosocomial rhinosinusitis differ from those in community-acquired rhinosinusitis. Empiric antimicrobial therapy for nosocomial rhinosinusitis should provide adequate coverage for S aureus and gram-negative bacteria. If sinus aspirate culture and sensitivity information are available, treatment should be tailored toward the specific pathogen. Polymicrobial infection may occur in patients with nosocomial bacterial rhinosinusitis. Chronic Rhinosinusitis Chronic rhinosinusitis (CRS) is a commonly diagnosed illness that affected almost 30 million people in the United States in The socioeconomic impact of CRS is significant. CRS results in an estimated 18 million to 22 million physician office visits annually and $200 million in expenditures on medications. 29,30 Furthermore, this chronic disease may lead to functional and emotional impairments that affect quality of life. 31 Pathogenesis The pathogenesis of CRS is an ongoing area of research. The cause of CRS is believed to be multifactorial. Potential causes or predisposing factors include microorganisms (bacteria, fungi), inflammatory agents (eg, allergens, pollutants, smoke), asthma, cystic fibrosis, immunodeficiency, nasal polyposis, and autoimmune diseases (eg, systemic lupus erythematosus, 6 November 2004
5 Wegener s granulomatosis). 30 These factors may appear concurrently to cause persistent inflammation of the nose and paranasal sinuses. The microbiology and role of bacteria in the pathogenesis of CRS are not as well established as for ABRS. The presence of bacteria may provide a direct insult to the nose and paranasal sinuses to cause CRS. Alternatively, the bacteria can indirectly cause CRS by aggravating a noninfectious inflammatory process. The predominant bacteria associated with CRS are coagulase-negative staphylococci (24% to 36%), S aureus (22% to 25%), Streptococcus species (20% to 27%), and anaerobes (6% to 10%) The clinical significance of coagulase-negative Staphylococcus is uncertain. Some studies report a high incidence (19% to 48%) of anaerobic bacteria isolated in patients with CRS. 35,36 The most common anaerobes are Prevotella species, anaerobic streptococci, and Fusobacterium species. Polymicrobial infections occur more often in CRS than ABRS. 37 The clinical significance of fungi remains controversial. Some studies demonstrate a role of fungi in the pathogenesis of CRS. 30 Disease occurs either by formation of fungal balls or inflammatory response to the presence of the fungus. A clinically distinct form of CRS is allergic fungal rhinosinusitis. Patients with allergic fungal rhinosinusitis present with nasal polyposis, allergy, production of eosinophilic mucin, and unilateral predominance. 38 Clinical Presentation and Diagnosis The clinical features of CRS are comparable to acute sinusitis, making diagnosis of CRS very difficult. The main distinction between chronic and acute disease is duration of symptoms. Patients with CRS present with persistent inflammation of the mucosa of the nose and paranasal sinuses lasting >12 weeks. 30 The most common and problematic symptoms experienced by patients with chronic infection include nasal obstruction or congestion, headache, and fatigue. 39 The presence of nasal polyps, crusts, and turbinate edema or hypertrophy are also common findings in patients with CRS. In contrast to ABRS, purulent nasal discharge is highly suggestive of a bacterial etiology in patients with CRS. A diagnosis of CRS should be confirmed by physical evidence of mucosal inflammation. 30 Patients with CRS who are unresponsive to treatment are candidates for sinus cultures and/or imaging studies. A standard sinus CT scan is the preferred method to locate, confirm, and determine severity of disease. 40,41 It should be used to evaluate patients before undergoing sinus surgery. Treatment Because the pathogenesis may involve multiple factors, which currently remain largely unknown, the optimal treatment of CRS is uncertain. In fact, there are currently no antimicrobials approved by the FDA for treatment of CRS. Antibiotics that have been studied in patients with bacterial CRS or acute exacerbation of CRS are amoxicillin/clavulanate and cefuroxime. 42 The use of clarithromycin, clindamycin, or a respiratory fluoroquinolone can be considered in patients with allergy to penicillin. 43 The recommended duration of therapy is 3 to 6 weeks; however a 14-day course has been shown to produce a 90% clinical response. 42 Other treatment modalities that show benefit in providing symptomatic relief are nasal lavage and topical steroids. Nasal irrigation with a warm saline solution (isotonic or hypertonic) twice daily has been shown to reduce nasal congestion. 44,45 In patients with allergic disease, steroidal intranasal sprays (fluticasone) may help reduce mucosal inflammation and swelling. 46 Nebulized antibiotics, decongestants, mucolytic agents, and antihistamines may serve as adjunctive therapies; the evidence for their value in treatment of CRS, however, is either inconclusive or deficient. Sinus surgery may be considered in patients who fail aggressive pharmacologic therapy. Challenges of Bacterial Resistance Over the past few decades, antibiotic resistance has increased dramatically. To address resistance, the most recent guidelines for treatment of acute rhinosinusitis focus on judicious use of antibiotics. 6,11,13,47 Improper diagnosis of ABRS leading to overuse of antibiotics may have contributed to the increasing trend of resistance among respiratory bacterial pathogens. Multidrug-resistant pneumococci, defined as strains resistant to at least 3 classes of antibiotics, were recovered in 26% of all isolates. 19 The most common bacterial pathogens associated with ABRS are S pneumoniae, H influenzae, and M catarrhalis. Alteration of the penicillin-binding proteins, a resistance mechanism acquired by pneumococci, renders the organism resistant to penicillins, cephalosporins, and other -lactam antibiotics. In the United States, the prevalence of penicillin-nonsusceptible (include resistant and intermediately susceptible) strains of S pneumoniae reached a peak of 36% in In addition, penicillin-nonsusceptible strains of S pneumoniae are associated with cross-resistance to other classes of antibiotics; thus these isolates are termed drug-resistant S pneumoniae (DRSP). Resistance of DRSP to other antibiotics includes TMP/SMX (37%), macrolides (29%), doxycycline (21%), clindamycin (10%), and ofloxacin (7%). 19 Most isolates of S pneumoniae remain susceptible to respiratory fluoroquinolones (including gatifloxacin, gemifloxacin, levofloxacin, and moxifloxacin). However, concern for development of resistance is arising from extensive use of fluoroquinolones in the treatment of community-acquired respiratory tract infections, however. 49 Cross-resistance between erythromycin and clindamycin occurred in approximately 32% of S pneumoniae isolates in the United States. 19 Resistance to both erythromycin and clindamycin is mediated by the ermb ribosomal methylation mechanism (MLSB-phenotype), which inhibits November
6 binding of the antibiotic to the target site. 50,51 Most erythromycin-resistant S pneumoniae strains (68%) remain susceptible to clindamycin, however. 52 In these isolates, resistance occurs by the mefa efflux pump (M-phenotype), which decreases antibiotic accumulation in the bacteria. 50,53 H influenzae (30%) and M catarrhalis (92%) confer resistance to penicillins by producing -lactamases. 19 -lactamase-inhibitor combinations (eg, amoxicillin with clavulanate) and cephalosporins (specifically, ceftriaxone, cefixime, and cefdinir) retain excellent activity against these pathogens. Both H influenzae and M catarrhalis are highly susceptible to the fluoroquinolones. Resistance of H influenzae to TMP/SMX (22%) has been observed. 19 Recently Available Agents Newer antibiotics and dosage formulations provide treatment options for infections caused by resistant respiratory pathogens. High-dose amoxicillin with clavulanate is now available in formulations intended to enhance compliance and effectiveness against DRSP (1000 mg amoxicillin and 62.5 mg clavulanate per extended-release tablet; 14:1 ratio of amoxicillin to clavulanate in powder for oral suspension). Amoxicillin (± clavulanate), which exerts its bactericidal activity by inhibiting cell-wall synthesis, remains a first-line agent in the treatment of ABRS. In addition, the clavulanate component provides activity against -lactamase producers, H influenzae and M catarrhalis. Pharmacokinetic and pharmacodynamic studies demonstrate that highdose amoxicillin (± clavulanate), defined as 4 g/day in adults and 80 mg/kg/day to 90 mg/kg/day in children, provides enhanced activity against DRSP. 54,55 The most common adverse effects are gastrointestinalrelated, including nausea and diarrhea. The incidence of adverse effects associated with high-dose amoxicillin is comparable to standard-dose amoxicillin. 55,56 Compared with twice-daily dosing, however, 3-times-daily dosing of high-dose amoxicillin was associated with significantly higher incidence of diarrhea. 54 Fluoroquinolones bind to DNA gyrase and topoisomerase IV to inhibit bacterial DNA synthesis. The respiratory fluoroquinolones provide excellent coverage against respiratory pathogens, including atypical bacteria. The role of atypical bacteria in rhinosinusitis is uncertain, however. Levofloxacin, gatifloxacin, and moxifloxacin, which have been available for a number of years, provide excellent activity against S pneumoniae, H influenzae, M catarrhalis, and S aureus 57 and are FDAapproved for treatment of ABRS. A newer agent, gemifloxacin, also provides excellent activity against respiratory pathogens, but this agent has yet to gain FDA approval for use in ABRS. Ciprofloxacin, while active against H influenzae and M catarrhalis, has limited activity against pneumococci. The primary concern with the use of fluoroquinolones is the recent emergence of pneumococci with reduced susceptibility to fluoroquinolones. 47,49,58 The more recent macrolides, including clarithromycin and azithromycin, also possess excellent activity against S pneumoniae, H influenzae, M catarrhalis, and atypical respiratory pathogens. By binding to the 50S ribosomal subunit, macrolides inhibit protein synthesis to exert their bacteriostatic activity. FDA recently approved the extended-release formulation of clarithromycin for once-daily dosing to enhance compliance. Fluoroquinolones and macrolides are therapeutic options in patients with true hypersensitivity to penicillin. They have been associated with emerging resistance, however, particularly among penicillin-nonsusceptible pneumococcal isolates in the United States. 19,47,59 A new class of antibiotics called the ketolides was developed to address macrolide-resistant bacteria. 60 In the presence of the ermb gene (and in the case of telithromycin, ermb and mefa genes), ketolides remain active against macrolide-resistant pathogens. 61 Although similar to the macrolides, ketolides bind more tightly to the 50S ribosomal subunit to enhance activity against respiratory pathogens. 62 Telithromycin, the first ketolide, recently received FDA approval for the treatment of acute bacterial rhinosinusitis. The spectrum of activity of telithromycin in acute bacterial sinusitis includes S pneumoniae, H influenzae, M catarrhalis, and S aureus. 63 Telithromycin 800 mg once daily for 5 days provided a clinical cure rate of 75% to 91%. 26,64,65 The most common adverse effects reported were gastrointestinalrelated, including nausea and diarrhea. Conclusion To optimize treatment of acute and chronic rhinosinusitis, the clinician must understand the pathogenesis and distinct clinical features of these infections. Viruses are responsible for most cases of acute rhinosinusitis. The cause of chronic rhinosinusitis is multifactorial, and the role of bacteria in its pathogenesis is not well established. The use of antibiotics in viral acute rhinosinusitis is inappropriate and contributes to the increasing prevalence of bacterial resistance. Antibiotic resistance is a limitation in the management of ABRS, thereby necessitating appropriate use of antibiotics. To encourage judicious use of antibiotics, the clinician must determine when bacterial infection is highly probable and subsequently consider guidelines when selecting the optimal therapy. P T For a list of references, send a stamped, self-addressed envelope to: References Department, Attn. A. Stahl, Pharmacy Times, 241 Forsgate Drive, Jamesburg, NJ 08831; or send an request to: astahl@mwc.com. 8 November 2004
Prefe f rred d t e t rm: : rhi h no n s o inu n s u iti t s
 HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Update on Rhinosinusitis 2013 AAP Guidelines Review
 Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
4/7/13 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC
 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
Acute Bacterial Sinusitis: The latest treatment recommendations. Objectives Having completed the learning activities, the participant will be able to:
 Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Choosing an appropriate antimicrobial agent. 3) the spectrum of potential pathogens
 Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Upper Respiratory Tract Infections / 42
 Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
Upper Respiratory Tract Infections 1 Upper Respiratory Tract Infections Acute tonsillitispharyngitis Acute otitis media Acute sinusitis Common cold Acute laryngitis Otitis externa Mastoiditis Acute apiglottis
Sinusitis & its complication. MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University
 Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
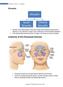 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
Sinusitis in Adults UP TO DATE
 Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
UPPER RESPIRATORY TRACT INFECTIONS. IAP UG Teaching slides
 UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
27/11/2012. Parainfuenza 1, 2 3 Rhinovirus Coronavirus Adenovirus Respiratory syncytial virus (RSV) Chlamydophila pneumoniae Mycoplasma pneumonite
 8 «Evidence-based Medicine-» 27/11/2012,,,, : :,,,,,,,, (30%-50%) () (5%-10%) (40%-50%) 20% Infuenza A B Parainfuenza 1, 2 3 Rhinovirus Coronavirus Adenovirus Respiratory syncytial virus (RSV) Chlamydophila
8 «Evidence-based Medicine-» 27/11/2012,,,, : :,,,,,,,, (30%-50%) () (5%-10%) (40%-50%) 20% Infuenza A B Parainfuenza 1, 2 3 Rhinovirus Coronavirus Adenovirus Respiratory syncytial virus (RSV) Chlamydophila
Respiratory Infections
 Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Infections of the head, neck, and lower respiratory tract
 Infections of the head, neck, and lower respiratory tract Infections of the upper respiratory tract Common 25% bacteria antibiotics 75% viruses Diagnosis on clinical grounds Nonspecific infections of the
Infections of the head, neck, and lower respiratory tract Infections of the upper respiratory tract Common 25% bacteria antibiotics 75% viruses Diagnosis on clinical grounds Nonspecific infections of the
Sinusitis. 12 weeks. Subacute sinusitis: An inflammation lasting 4 to 8 weeks. weeks or longer Re urre t si usitis: Se eral atta ks ithi a year
 Sinusitis 12 weeks. Sinusitis, also known as a sinus infection or rhinosinusitis, is inflammation of the sinuses resulting in symptoms. Common signs and symptoms include thick nasal mucous, a plugged nose,
Sinusitis 12 weeks. Sinusitis, also known as a sinus infection or rhinosinusitis, is inflammation of the sinuses resulting in symptoms. Common signs and symptoms include thick nasal mucous, a plugged nose,
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief.
 Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD)
 Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
+ Conflict of interest. + Sinus and Nasal Anatomy. + What is your diagnosis? 1) Allergic Rhinitis. 2) Non-Allergic rhinitis. 3) Chronic Rhinosinusitis
 Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
PIDS AND RESPIRATORY DISORDERS
 PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
ب ه نام خد ا فارماکوویژیالنس و عوارض ناخواسته داروها آذر ماه 1396
 ب ه نام خد ا فارماکوویژیالنس و عوارض ناخواسته داروها آذر ماه 1396 Upper Respiratory Tract Infections Z. Sahraei Pharm. D., Ph.D. Infectious Disease Clinical Pharmacist Rhinosinusitis Definition Acute rhinosinusitis
ب ه نام خد ا فارماکوویژیالنس و عوارض ناخواسته داروها آذر ماه 1396 Upper Respiratory Tract Infections Z. Sahraei Pharm. D., Ph.D. Infectious Disease Clinical Pharmacist Rhinosinusitis Definition Acute rhinosinusitis
Jimmy's Got Cooties! Common Childhood Infections and How Best to Treat Them
 Jimmy's Got Cooties! Common Childhood Infections and How Best to Treat Them Objectives:! Recognize and manage several infections commonly seen in Pediatric practice! Discuss best practices and current
Jimmy's Got Cooties! Common Childhood Infections and How Best to Treat Them Objectives:! Recognize and manage several infections commonly seen in Pediatric practice! Discuss best practices and current
Management of URTI s in Children
 Management of URTI s in Children Robin J Green PhD Antibiotics - Dilemmas for General Practitioners Antibiotic overuse = Resistance Delay in antibiotic use = Mortality Patient expectation Employer expectation
Management of URTI s in Children Robin J Green PhD Antibiotics - Dilemmas for General Practitioners Antibiotic overuse = Resistance Delay in antibiotic use = Mortality Patient expectation Employer expectation
Diagnosis and Treatment of Respiratory Illness in Children and Adults Guideline
 Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
CLINICAL PRACTICE GUIDELINE
 This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
Clinical Practice Guideline for the Diagnosis and Management of Acute Bacterial Sinusitis in Children Aged 1 to 18 Years
 Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE Clinical Practice Guideline for the Diagnosis and Management
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE Clinical Practice Guideline for the Diagnosis and Management
PNEUMONIA IN CHILDREN. IAP UG Teaching slides
 PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
Upper Respiratory Tract Infections Masoud Mardani. M. D. MPH, FIDSA
 Upper Respiratory Tract Infections Masoud Mardani. M. D. MPH, FIDSA Professor Of Infectious Diseases Shahid Beheshti Medical University URTI s Sinusitis Acute Otitis Media Pharyngitis Question One: What
Upper Respiratory Tract Infections Masoud Mardani. M. D. MPH, FIDSA Professor Of Infectious Diseases Shahid Beheshti Medical University URTI s Sinusitis Acute Otitis Media Pharyngitis Question One: What
ANTIBIOTICS ACUTE RHINOSINUSITIS IN CHILDREN
 MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
Respiratory System Virology
 Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Objectives. Pneumonia. Pneumonia. Epidemiology. Prevalence 1/7/2012. Community-Acquired Pneumonia in infants and children
 Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
An Open Multicenter Study of the Use of Gatifloxacin for the Treatment of Non- Complicated Acute Bacterial Rhinosinusitis in Adults
 162 BJID 2005; 9 (April) An Open Multicenter Study of the Use of Gatifloxacin for the Treatment of Non- Complicated Acute Bacterial Rhinosinusitis in Adults Weckx L.L.M. 1, Campos C.A.H. 2, Sakano E. 3,
162 BJID 2005; 9 (April) An Open Multicenter Study of the Use of Gatifloxacin for the Treatment of Non- Complicated Acute Bacterial Rhinosinusitis in Adults Weckx L.L.M. 1, Campos C.A.H. 2, Sakano E. 3,
Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center
 Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center Kathy Peters is a 63 y.o. patient that presents to your urgent care office today with a history
Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center Kathy Peters is a 63 y.o. patient that presents to your urgent care office today with a history
Shirin Abadi, B.Sc.(Pharm.), ACPR, Pharm.D. Clinical Pharmacy Specialist & Pharmacy Education Coordinator, BC Cancer Agency Clinical Associate
 Shirin Abadi, B.Sc.(Pharm.), ACPR, Pharm.D. Clinical Pharmacy Specialist & Pharmacy Education Coordinator, BC Cancer Agency Clinical Associate Professor of Pharmacy & Associate Member of Medicine, UBC
Shirin Abadi, B.Sc.(Pharm.), ACPR, Pharm.D. Clinical Pharmacy Specialist & Pharmacy Education Coordinator, BC Cancer Agency Clinical Associate Professor of Pharmacy & Associate Member of Medicine, UBC
Community Acquired Pneumonia - Pediatric Clinical Practice Guideline MedStar Health Antibiotic Stewardship
 Community Acquired Pneumonia - Pediatric Clinical Practice Guideline MedStar Health Antibiotic Stewardship These guidelines are provided to assist physicians and other clinicians in making decisions regarding
Community Acquired Pneumonia - Pediatric Clinical Practice Guideline MedStar Health Antibiotic Stewardship These guidelines are provided to assist physicians and other clinicians in making decisions regarding
INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES
 Upper Respiratory Tract Infections Return to Syllabus INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES General Goal: To know the major mechanisms of defense in the URT, the major mechanisms invaders use
Upper Respiratory Tract Infections Return to Syllabus INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES General Goal: To know the major mechanisms of defense in the URT, the major mechanisms invaders use
Molina Healthcare of Washington, Inc. Guideline for the Judicious use of Antibiotics
 Molina Healthcare of Washington, Inc. Guideline for the Judicious use of Antibiotics The Washington State Clinical Practice Guidelines for the Judicious Use of Antibiotics in URI (Sinusitis, Otitis Media,
Molina Healthcare of Washington, Inc. Guideline for the Judicious use of Antibiotics The Washington State Clinical Practice Guidelines for the Judicious Use of Antibiotics in URI (Sinusitis, Otitis Media,
AXITAB-CV TAB. COMPOSITION :
 AXITAB-CV TAB. COMPOSITION : Each film coated tablet contains: Cefuroxime Axetil I.P. Eq. to Anhydrous 500mg. Potassium Clavulanate Diluted I.P. Eq. to Clavulanic Acid 125mg DESCRIPTION : Cefuroxime Axetil
AXITAB-CV TAB. COMPOSITION : Each film coated tablet contains: Cefuroxime Axetil I.P. Eq. to Anhydrous 500mg. Potassium Clavulanate Diluted I.P. Eq. to Clavulanic Acid 125mg DESCRIPTION : Cefuroxime Axetil
Study of Nasal Mucosal Flora in Acute and Chronic Sinusitis
 Study of Nasal Mucosal Flora in Acute and Chronic Sinusitis Rupeshkumar TS 1, Rajesh K 2, Prabhusaran N 3*, Jesudoss A 4 Original Research Article 1MBBS Student, 2Associate Professor, 4 Professor & Head,
Study of Nasal Mucosal Flora in Acute and Chronic Sinusitis Rupeshkumar TS 1, Rajesh K 2, Prabhusaran N 3*, Jesudoss A 4 Original Research Article 1MBBS Student, 2Associate Professor, 4 Professor & Head,
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Antibiotics, Expectorants, and Cough Suppressants. Center For Cardiac Fitness Pulmonary Rehab The Miriam Hospital
 Antibiotics, Expectorants, and Cough Suppressants Center For Cardiac Fitness Pulmonary Rehab The Miriam Hospital Objectives Review the mechanism of action (MOA), dosing, benefits, and various options for:
Antibiotics, Expectorants, and Cough Suppressants Center For Cardiac Fitness Pulmonary Rehab The Miriam Hospital Objectives Review the mechanism of action (MOA), dosing, benefits, and various options for:
Middleton Chapter 43 (pages ) Rhinosinusitis and Nasal Polyps Prepared by: Malika Gupta, MD
 FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
Sinusitis. What are the sinuses? Who develops sinusitis?
 Sinusitis Health experts estimate that 37 million Americans are affected by sinusitis every year. Americans spend nearly $6 billion each year on health care costs related to sinusitis. Sinusitis is an
Sinusitis Health experts estimate that 37 million Americans are affected by sinusitis every year. Americans spend nearly $6 billion each year on health care costs related to sinusitis. Sinusitis is an
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
Patricia M. Wegner, BS Pharm, PharmD, FASHP PEER REVIEWERS: Nathaniel James Rhodes, PharmD, BCPS Linda O. Martinez, CPhT
 Pharmacy Tech Topics VOLUME 18 NO. 2 APRIL 2013 Cough, Sneeze, Sniffle: Management of Respiratory Tract Infections AUTHOR: Sarah M. Wieczorkiewicz, PharmD, BCPS EDITOR: Patricia M. Wegner, BS Pharm, PharmD,
Pharmacy Tech Topics VOLUME 18 NO. 2 APRIL 2013 Cough, Sneeze, Sniffle: Management of Respiratory Tract Infections AUTHOR: Sarah M. Wieczorkiewicz, PharmD, BCPS EDITOR: Patricia M. Wegner, BS Pharm, PharmD,
Nursing care for children with respiratory dysfunction
 Nursing care for children with respiratory dysfunction 1 Lung Development Specific Immunity to Respiratory Infection Secretory IgA in mucosal immunity IgG in systemic immunity Risk Factors Associated with
Nursing care for children with respiratory dysfunction 1 Lung Development Specific Immunity to Respiratory Infection Secretory IgA in mucosal immunity IgG in systemic immunity Risk Factors Associated with
Pediatric Respiratory Infections
 Pediatric Respiratory Infections Brenda Kelly PharmD BCPS Residency Program Director Virginia Mason Memorial, Yakima, Washington brendakelly@yvmh.org Disclosure The presenter has no actual or potential
Pediatric Respiratory Infections Brenda Kelly PharmD BCPS Residency Program Director Virginia Mason Memorial, Yakima, Washington brendakelly@yvmh.org Disclosure The presenter has no actual or potential
POLICY FOR TREATMENT OF UPPER RESPIRATORY TRACT INFECTIONS
 POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: July 2013 Approved by: The Drugs & Therapeutics Committee Date: April 2016 Implementation
POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: July 2013 Approved by: The Drugs & Therapeutics Committee Date: April 2016 Implementation
MEDICAL MANAGEMENT OF ACUTE BACTERIAL SINUSITIS
 MEDICAL MANAGEMENT OF ACUTE BACTERIAL SINUSITIS RECOMMENDATIONS OF A CLINICAL ADVISORY COMMITTEE ON PEDIATRIC AND ADULT SINUSITIS ADVISORY COMMITTEE MEMBERS Itzhak Brook, MD, MSc Professor, Department
MEDICAL MANAGEMENT OF ACUTE BACTERIAL SINUSITIS RECOMMENDATIONS OF A CLINICAL ADVISORY COMMITTEE ON PEDIATRIC AND ADULT SINUSITIS ADVISORY COMMITTEE MEMBERS Itzhak Brook, MD, MSc Professor, Department
Received 25 November 2002/Returned for modification 14 February 2003/Accepted 11 April 2003
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
SINUSITIS/RHINOSINUSITIS
 1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
Current Trend in URTI
 Current Trend in URTI Dr Chow Chun Kuen Specialist in Otorhinolaryngology Upper respiratory tract infection Nonspecific Most common cause of physician visits & sick leaves Acute infection of noes, sinuses,
Current Trend in URTI Dr Chow Chun Kuen Specialist in Otorhinolaryngology Upper respiratory tract infection Nonspecific Most common cause of physician visits & sick leaves Acute infection of noes, sinuses,
Facilitator s Guide. Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama. Active Learning Module
 Facilitator s Guide Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama Active Learning Module Core Concepts In order to master this topic area, students must
Facilitator s Guide Prescription Writing/Patient Safety Author: Benjamin Estrada, MD, University of South Alabama Active Learning Module Core Concepts In order to master this topic area, students must
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Sinusitis/Rhinosinusitis SINUSITIS/RHINOSINUSITIS
 1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
Disclaimers. Topical Therapy. The Problem. Topical Therapy for Chronic Rhinosinusitis No Disclosures
 Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Discrepancies in the recovery of bacteria from multiple sinuses in acute and chronic sinusitis
 Journal of Medical Microbiology (2004), 53, 879 885 DOI 10.1099/jmm.0.45655-0 Short Communication Correspondence Itzhak Brook ib6@georgetown.edu Received 1 March 2004 Accepted 18 May 2004 Discrepancies
Journal of Medical Microbiology (2004), 53, 879 885 DOI 10.1099/jmm.0.45655-0 Short Communication Correspondence Itzhak Brook ib6@georgetown.edu Received 1 March 2004 Accepted 18 May 2004 Discrepancies
Concepts in Rhinosinusitis. Nick Jones University of Nottingham
 Concepts in Rhinosinusitis Nick Jones University of Nottingham Definition of rhinosinusitis Very broad and is based on clinical symptoms, CT and endoscopy NOT on pathology Definition of rhinosinusitis
Concepts in Rhinosinusitis Nick Jones University of Nottingham Definition of rhinosinusitis Very broad and is based on clinical symptoms, CT and endoscopy NOT on pathology Definition of rhinosinusitis
Will sulfamethoxazole treat sinus infection
 Will sulfamethoxazole treat sinus infection Find information about which conditions Sulfamethoxazole- Trimethoprim by a Fungus; Bacterial Infection of Heart Valve; Sinus Irritation and Congestion. Bactrim
Will sulfamethoxazole treat sinus infection Find information about which conditions Sulfamethoxazole- Trimethoprim by a Fungus; Bacterial Infection of Heart Valve; Sinus Irritation and Congestion. Bactrim
(cilia) that help sweep away fluids and/or particles International Journal of Pharmaceutical Sciences and Research 2055
 IJPSR (2014), Vol. 5, Issue 5 (Research Article) Received on 29 November, 2013; received in revised form, 21 February, 2014; accepted, 16 April, 2014; published 01 May, 2014 EVALUATION OF EFFICACY AND
IJPSR (2014), Vol. 5, Issue 5 (Research Article) Received on 29 November, 2013; received in revised form, 21 February, 2014; accepted, 16 April, 2014; published 01 May, 2014 EVALUATION OF EFFICACY AND
General Surgery >>>>>[[ sheet # 4]]
![General Surgery >>>>>[[ sheet # 4]] General Surgery >>>>>[[ sheet # 4]]](/thumbs/82/86768776.jpg) General Surgery 11-3-2014 >>>>>[[ sheet # 4]] *Note *: this sheet includes the slides and extra notes >> and what the dr were mentioned are in the bold font Acute Rhinosinusitis Sinusitis commonly used
General Surgery 11-3-2014 >>>>>[[ sheet # 4]] *Note *: this sheet includes the slides and extra notes >> and what the dr were mentioned are in the bold font Acute Rhinosinusitis Sinusitis commonly used
Upper Respiratory tract Infec1on. Gassem Gohal FAAP FRCPC
 Upper Respiratory tract Infec1on Gassem Gohal FAAP FRCPC Anatomy Contents Sinusitis Common Cold Otitis media pharyngitis Epiglottitis Croup Trachitis Sinuses Sinus development Born with ME ( Maxillary,
Upper Respiratory tract Infec1on Gassem Gohal FAAP FRCPC Anatomy Contents Sinusitis Common Cold Otitis media pharyngitis Epiglottitis Croup Trachitis Sinuses Sinus development Born with ME ( Maxillary,
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
Macrolides & Ketolides. Objectives. Protein Synthesis
 Macrolides & Ketolides Elizabeth D. Hermsen, Pharm.D. Infectious Diseases Research Fellow University of Minnesota College of Pharmacy bjectives Participant should be able to explain macrolide/ketolide
Macrolides & Ketolides Elizabeth D. Hermsen, Pharm.D. Infectious Diseases Research Fellow University of Minnesota College of Pharmacy bjectives Participant should be able to explain macrolide/ketolide
Anti-Microbial Drugs
 Name: Date: Monday March 7 th 2011 Class: I "Pharmacology Anti-Microbial Drugs Lecture 5 د. حيدر الشكرجي Macrolides: Anti-Microbial Drugs Erythromycin was the 1 st of macrolides to find clinical application,
Name: Date: Monday March 7 th 2011 Class: I "Pharmacology Anti-Microbial Drugs Lecture 5 د. حيدر الشكرجي Macrolides: Anti-Microbial Drugs Erythromycin was the 1 st of macrolides to find clinical application,
POLICY FOR TREATMENT OF UPPER RESPIRATORY TRACT INFECTIONS
 POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: June 2018 Approved by: Date: July 2018 The Drugs & Therapeutics Committee Implementation
POLICY F TREATMENT OF UPPER RESPIRATY TRACT INFECTIONS Written by: Dr M Milupi, Consultant Microbiologist Date: June 2018 Approved by: Date: July 2018 The Drugs & Therapeutics Committee Implementation
Population-based approaches: Regulatory issues and Population simulations
 Population-based approaches: Regulatory issues and Population simulations Michael R. Jacobs, MD, PhD Case Western Reserve University University Hospitals of Cleveland Cleveland, OH Topics Regulatory issues
Population-based approaches: Regulatory issues and Population simulations Michael R. Jacobs, MD, PhD Case Western Reserve University University Hospitals of Cleveland Cleveland, OH Topics Regulatory issues
Community Acquired Pneumonia Pediatric Ages 3 month to 18 years Clinical Practice Guideline MedStar Health Antibiotic Stewardship
 Community Acquired Pneumonia Pediatric Ages 3 month to 18 years Clinical Practice Guideline MedStar Health Antibiotic Stewardship These guidelines are provided to assist physicians and other clinicians
Community Acquired Pneumonia Pediatric Ages 3 month to 18 years Clinical Practice Guideline MedStar Health Antibiotic Stewardship These guidelines are provided to assist physicians and other clinicians
Protein Synthesis Inhibitors. Ass Prof. Dr. Naza M. Ali 15 Nov 2018 Lec 8
 Protein Synthesis Inhibitors Ass Prof. Dr. Naza M. Ali 15 Nov 2018 Lec 8 These drugs selectively inhibit bacterial protein synthesis. The selectivity is due to the differences between bacterial and human
Protein Synthesis Inhibitors Ass Prof. Dr. Naza M. Ali 15 Nov 2018 Lec 8 These drugs selectively inhibit bacterial protein synthesis. The selectivity is due to the differences between bacterial and human
NOVEMBER 2016 DRUG ANTIBIOTICS ACUTE RHINOSINUSITIS IN ADULTS
 NOVEMBER 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
NOVEMBER 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
AMERICAN ACADEMY OF PEDIATRICS. Clinical Practice Guideline: Management of Sinusitis
 AMERICAN ACADEMY OF PEDIATRICS Subcommittee on Management of Sinusitis and Committee on Quality Improvement Clinical Practice Guideline: Management of Sinusitis ABSTRACT. This clinical practice guideline
AMERICAN ACADEMY OF PEDIATRICS Subcommittee on Management of Sinusitis and Committee on Quality Improvement Clinical Practice Guideline: Management of Sinusitis ABSTRACT. This clinical practice guideline
IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults
 Clinical Infectious Diseases Advance Access published March 20, 2012 IDSA GUIDELINES IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults Anthony W. Chow, 1 Michael
Clinical Infectious Diseases Advance Access published March 20, 2012 IDSA GUIDELINES IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults Anthony W. Chow, 1 Michael
KAISER PERMANENTE OHIO COMMUNITY ACQUIRED PNEUMONIA
 KAISER PERMANENTE OHIO COMMUNITY ACQUIRED PNEUMONIA Methodology: Expert opinion Issue Date: 8-97 Champion: Pulmonary Medicine Most Recent Update: 6-08, 7-10, 7-12 Key Stakeholders: Pulmonary Medicine,
KAISER PERMANENTE OHIO COMMUNITY ACQUIRED PNEUMONIA Methodology: Expert opinion Issue Date: 8-97 Champion: Pulmonary Medicine Most Recent Update: 6-08, 7-10, 7-12 Key Stakeholders: Pulmonary Medicine,
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Preventing sinusitis Health24. Page 3
 DOWNLOAD OR READ : TREAT AND PREVENT SINUSITIS WHAT YOUR DOCTOR ISNT TELLING YOU SINUS INFECTION SINUSITIS SYMPTOMS SINUSITIS TREATMENT SINUS CURE CHRONIC SINUSITIS SYMPTOMS TRANSCEND MEDIOCRITY BOOK 35
DOWNLOAD OR READ : TREAT AND PREVENT SINUSITIS WHAT YOUR DOCTOR ISNT TELLING YOU SINUS INFECTION SINUSITIS SYMPTOMS SINUSITIS TREATMENT SINUS CURE CHRONIC SINUSITIS SYMPTOMS TRANSCEND MEDIOCRITY BOOK 35
Swedish guidelines for the treatment of rhinosinusitis, pharyngotonsillitis and acute media otitis in children.
 Swedish guidelines for the treatment of rhinosinusitis, pharyngotonsillitis and acute media otitis in children. The guidelines are produced by STRAMA in collaboration with the Swedish Medical Products
Swedish guidelines for the treatment of rhinosinusitis, pharyngotonsillitis and acute media otitis in children. The guidelines are produced by STRAMA in collaboration with the Swedish Medical Products
STUDY SELECTION AND DATA EXTRACTION:
 Pediatrics Treatment and Prevention of Otitis Media John Erramouspe and Catherine A Heyneman OBJECTIVE: To review and summarize recent advances in the treatment and prevention of otitis media (OM). DATA
Pediatrics Treatment and Prevention of Otitis Media John Erramouspe and Catherine A Heyneman OBJECTIVE: To review and summarize recent advances in the treatment and prevention of otitis media (OM). DATA
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o
 A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
Allergy, Asthma & Clinical Immunology 2011, 7:2
 Allergy, Asthma & Clinical Immunology This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Canadian
Allergy, Asthma & Clinical Immunology This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Canadian
COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN
 ١ ٢ COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN Dr mostafavi SN Pediatric Infectious Disease Department Isfahan University of Medical Sciences Case 1 ٣ An 18 month old infant brought with high
١ ٢ COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN Dr mostafavi SN Pediatric Infectious Disease Department Isfahan University of Medical Sciences Case 1 ٣ An 18 month old infant brought with high
What are the causes of nasal congestion?
 Stuffy Noses Nasal congestion, stuffiness, or obstruction to nasal breathing is one of the oldest and most common human complaints. For some, it may only be a nuisance; for others, nasal congestion can
Stuffy Noses Nasal congestion, stuffiness, or obstruction to nasal breathing is one of the oldest and most common human complaints. For some, it may only be a nuisance; for others, nasal congestion can
continuing education for pharmacists
 continuing education for pharmacists Common Cold, Sinusitis, Influenza: The Diseases, Prevention, Treatment Volume XXX, No. 11 Mona T. Thompson, R.Ph., PharmD Dr. Mona T. Thompson has no relevant financial
continuing education for pharmacists Common Cold, Sinusitis, Influenza: The Diseases, Prevention, Treatment Volume XXX, No. 11 Mona T. Thompson, R.Ph., PharmD Dr. Mona T. Thompson has no relevant financial
I have no disclosures
 Disclosures Streptococcal Pharyngitis: Update and Current Guidelines Richard A. Jacobs, MD, PhD Emeritus Professor of Medicine Division of Infectious Diseases I have no disclosures CID 2012:55;e 86-102
Disclosures Streptococcal Pharyngitis: Update and Current Guidelines Richard A. Jacobs, MD, PhD Emeritus Professor of Medicine Division of Infectious Diseases I have no disclosures CID 2012:55;e 86-102
Management of community-acquired lower respiratory tract infections: gemifloxacin, a new economic paradigm
 Management of community-acquired lower respiratory tract infections: gemifloxacin, a new economic paradigm DRUG PROFILE Gary Patou, Glenn Tillotson & Joseph Blondeau Author for correspondence University
Management of community-acquired lower respiratory tract infections: gemifloxacin, a new economic paradigm DRUG PROFILE Gary Patou, Glenn Tillotson & Joseph Blondeau Author for correspondence University
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
Upper...and Lower Respiratory Tract Infections
 Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
The Importance of Appropriate Treatment of Chronic Bronchitis
 ...CLINICIAN INTERVIEW... The Importance of Appropriate Treatment of Chronic Bronchitis An interview with Antonio Anzueto, MD, Associate Professor of Medicine, University of Texas Health Science Center,
...CLINICIAN INTERVIEW... The Importance of Appropriate Treatment of Chronic Bronchitis An interview with Antonio Anzueto, MD, Associate Professor of Medicine, University of Texas Health Science Center,
FULL PRESCRIBING INFORMATION: CONTENTS*
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use OTIPRIO safely and effectively. See full prescribing information for OTIPRIO. OTIPRIO (ciprofloxacin
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use OTIPRIO safely and effectively. See full prescribing information for OTIPRIO. OTIPRIO (ciprofloxacin
