An hour behind schedule, the waiting room is
|
|
|
- Rose Caldwell
- 6 years ago
- Views:
Transcription
1 Key Technical Skills I Checked the Intraocular Pressure. Now What Do I Do? KEY TECHNICAL SKILLS By Janet Hunter, bs, comt An hour behind schedule, the waiting room is packed with anxious patients, and the physician is not in the best mood. Your current patient may have glaucoma. You ask yourself, Should I perform a visual field test? Do I need to refract? Should I dilate the pupil? Should I just go ask the doctor? The role of the ophthalmic technician has grown along with the many new technologies. You distinguish yourself not only by knowing how to perform the various diagnostic tests but also by knowing why and when to perform them. You, the technician, are the first clinical person with whom the patient has contact; hence, the patient s entire first impression of the office is based upon this experience. You serve as the gateway to effective and efficient doctorpatient relationships. An efficient technician provides clear and accurate information to support the physician s assessment, diagnosis, and treatment of the patient. To do this well, you must know more than the how to but also the why to. Vision Assessment Typically, the patient is unaware that he or she has glaucoma until after he or she experiences a serious loss of vision. This is the very reason that a careful assessment of visual acuity should take place at each visit. Never assume binocularity. Each eye must be tested separately. Make certain that the occluded eye is completely covered, and be sure to tell the patient he or she must not press on that eye. Patients do not realize this causes blurriness (Figure 1). Ensure that the patient wears his or her distance glasses for the Snellen chart and near spectacles for the Rosenbaum near vision assessment. The visual field test (perimetry) detects the loss of both peripheral and central vision and, in some cases, can indicate glaucomatous optic nerve damage. 1 To manage the glaucoma patient, the visual field test is typically performed every 3 to 6 months. An invaluable technician Figure 1. Pinhole disc testing is recommended if the patient presents with diminished visual acuity. It helps to differentiate whether the vision loss is refractive in nature, due to a disorder of the eye (eg, glaucoma, macular degeneration, retinal detachment, cataract), or owing to a brain lesion. 2 reviews a patient s chart to guarantee the timing of this practice. A quick field screening tool is the confrontation field test. This is a crude test performed simply by having the patient look straight ahead and count the examiner s fingers held within the periphery of the patient s field of view. In working with innumerable glaucoma specialists, I found it highly advantageous to ask each physician for his or her own test selection criteria. For example, you may find one physician prefers a 24-2 testing strategy for every patient, no matter what. Another may prefer 24-2 for all patients with a visual acuity of 20/200 or better but a 10-2 for patients with central islands or a visual acuity of 20/400 or worse. Kinetic visual fields may be helpful for observing patients with poor vision as well. Why not make your work go more smoothly by noting these preferences? 8 glaucoma today 2012 Ultimate Technician s Survival Guide
2 Refraction and Lensometry The Mayo Clinic has reported that both nearsighted and farsighted patients are at higher risk for glaucoma. For the farsighted, they report an increased risk of developing narrow-angle glaucoma and/or angle-closure glaucoma.³ The following glaucoma surgeries can also cause changes in refractive error, specifically, an induction of astigmatism: trabeculectomy canaloplasty deep sclerectomy 4 Check patients eye glasses at every visit, the exception s being the postoperative patient. Be advised that it is not unusual for glaucoma patients with poor vision to have several different pairs of glasses. They often bring one pair of spectacles for one visit and a different pair for a subsequent visit! This is another reason why you should perform lensometry at each visit. Figure 2. Direct response to flashlight test. Key Technical Skills Pupillary Evaluation A pupillary assessment can produce extremely significant clinical findings. Glaucoma, for instance, can cause pupillary abnormalities such as a relative afferent pupillary defect. The pupil s size, shape, and function can be indicators of related neurological (cranial nerve) function. Note that pupillary size, iris color, and refractive error can vary with age. Some causes of pupillary dilation include acute glaucoma attack (middilated and fixed pupil) retinal disease cranial nerve III palsy (consensual reflex absent) cyloplegia (2º to eyedrops) 5 Constricted pupils can be caused by the glaucoma medication pilocarpine. Swinging Flashlight Test Pupillary reaction to light is tested for each eye, one eye at a time. The direct and consensual pupillary reaction to light at near and distance are measured and noted along with the pupil s size and shape. Testing the afferent sensory stimulus pathway from eye to brain helps the physician determine whether the cause of the patient s reduced vision is ocular disease. An abnormal result indicates a relative afferent pupillary defect (Figure 2). Procedure To perform the procedure: Check the patient s left eye Shine the light onto the left eye and check for pupillary constriction of the left eye (direct) Shine the light onto the left eye and check for pupillary constriction of the right eye (consensual) Check the right eye Shine the light onto the right eye and check for pupillary constriction of the right eye (direct) Shine the light onto the right eye and check for pupillary constriction of the left eye (consensual) Figure 3. A left afferent pupillary defect. Relative Afferent Pupillary Defect Typically, both pupils should constrict when light is shone into either eye. An injury to the optic nerve, however, can decrease the amount of light ultimately transmitted to the brain, thus decreasing the pupil s normal reaction to the light. A typical result is dilation of the pupil rather than constriction. 6 For example, in Figure 3, the left pupil dilates with light. This can indicate a left optic nerve lesion, which will ultimately result in the attenuation of the light signal to the brain. Ocular Motility and Alignment Performing tests of ocular motility and alignment can be useful in the detection of potential ocular health problems (Figure 4). By observing how the eyes move when covered and uncovered, the physician can observe proper ocular alignment and how well the eyes move together. Problems with eye movement can be indicative of a large number of troubles neurologic, ocular, and/or systemic. Movement of the eyes is measured in all nine positions of gaze: primary up, down left, right four corners (up + right, up + left, down + right, down + left) Eye movements are tested individually (ductions) and together (versions). Cover and Uncover Test To perform the test, place the occluder over the right eye (Figure 5). Then, uncover and evaluate the eye for movement. Repeat for the left eye Ultimate Technician s Survival Guide glaucoma today 9
3 Key Technical Skills Figure 4. Extraocular muscles and eye movement. Figure 5. Cover and uncover test. Figure 6. Alternate cover test. This test evaluates the patient for the presence of a phoria, a muscular imbalance or an ocular misalignment that only occurs some of the time. The goal is to disrupt fusion of the eyes and to observe the direction in which the covered eye moves. Figure 7. Hirshberg test. Alternate Cover Test This test evaluates the patient for the presence of tropia, a misalignment that is always present. The test is performed after the cover test. Cover the right eye, and then switch to cover the left eye. Now, repeat by moving the cover from the left eye to the right (Figure 6). Hirshberg Test The Hirshberg test gives a rough estimate of any ocular deviation (Figure 7). A light is shone onto the patient s eyes while he or she fixates on a distant target. The location of the light reflex relative to the pupil should be noted. The light reflex may be on the nasal edge of the pupil (eso), the temporal edge (exo), or central (ortho). Krimsky Test The Krimsky test also assesses the binocular alignment of the patient s eyes (Figure 8). The test is performed in the same way as the Hirshberg test but situates prisms of different strength in front of the eye in such a way as to center the light reflex inside the pupil. 7 Figure 8. Krimsky test. Intraocular Pressure Measurement Applanation Tonometry During a glaucoma evaluation, one of the most important measurements a technician makes is applanation tonometry. The Goldmann applanation tonometer is the gold standard for intraocular pressure (IOP) measurements and provides acceptable accuracy for most patients. The Goldmann tonometer measures a 3.06-mm-diameter area on the cornea. Correct endpoint mire alignment is seen 10 glaucoma today 2012 Ultimate Technician s Survival Guide
4 Key Technical Skills Figure 9. Examples of IOP measurement mire alignment. Key Technical Skills Figure 11. Measuring corneal pachymetry. when the two inner margins of the semicircles just touch (Figure 9). Mire Patterns Few things frustrate the physician more than inaccurate IOP measurements taken by the technical staff. Equipment lacking calibration can lead to an inaccurate reading. To ensure quality control and minimize factors in incorrect measurements, do the following: Check the tonometer s calibration at least once a month (a must). Inspect the tonometer prism for scratches or signs of degradation (Figure 10). Become familiar with the slit lamp. Different models function differently. You should be comfortable with the movement of the slit lamp prior to performing applanation tonometry. Improve your applanation technique and work on corneal centering. Question differences of more than 3 mm Hg between a patient s two eyes. This is a red flag. Possible causes include poor technique, glaucoma, and uveitis, among others. Ensure that the patient s eye is in the primary position. Note the presence of any venous pulsations observed during applanation. Do not put any pressure on the globe when checking the IOP. Pressure on the globe will raise the patient s IOP. Lids and eyelashes should not touch the tonometer s head. Instruct patients to breathe normally and not to hold their breath, which can alter IOP. Ask men wearing neckties or with tight collars to loosen them prior to tonometry, because constriction Figure 10. Goldmann applanation tonometer prism. can alter IOP. Instruct patients who have difficulty getting their chin into the chin rest cup to move to the edge of the chair so that they are not leaning so far forward. Account for corneal astigmatism. Regular astigmatism of greater than 3.00 D may result in an underestimation of IOP in eyes that have with-the-rule astigmatism and an overestimation of IOP in eyes with against-the-rule astigmatism. Rotate the tonometer prism so that the red line of the prism lines up with the axis of the flattest meridian (in minus cylinder). Corneal irregularities/scarring may cause errors due to difficulty in endpoint determination. 8 Corneal Pachymetry Corneal pachymetry is the measurement of corneal thickness (Figure 11). It has been used to evaluate people with corneal disease and aids in the assessment of individuals at risk for glaucoma. 9 Studies have shown that corneal thickness can alter the accuracy of IOP measurements. 10 For patients with thick corneas, the actual IOP may be overestimated. For those with thin corneas, the actual IOP may be underestimated. Since the procedure is noninvasive and painless, you can perform it with ease using a topical Figure 12. Flashlight test Ultimate Technician s Survival Guide glaucoma today 13
5 Key Technical Skills A B Flashlight Test In the flashlight test, a light is shone from the temporal side onto the cornea along an angle parallel to the iris. A shadow on the nasal limbus will identify an eye with a shallow anterior chamber (Figure 12). Van Herrick Test The Van Herrick test uses a slit beam to compare the depth of the peripheral anterior chamber to the thickness of the cornea. When the depth of the peripheral anterior chamber is less than one-quarter of the corneal thickness, it is considered shallow. If the anterior chamber depth is as deep as the cornea is thick, then the angle is presumed to be wide open. If only a slit of aqueous is visible, then the angle is estimated to be dangerously narrow (Figure 13). C Figure 13. Wide-open anterior chamber angle (A). Open anterior chamber angle (B). Dangerously narrow anterior chamber angle (C). local anesthetic. With this measurement, you can develop a better appreciation of the relationship between elevated IOP measurements and corneal thickness. 11,12 Slit-Lamp Examination The slit lamp provides a three-dimensional view of the structures in the eye. It is used to examine the front (anterior) portion of the eye. This allows the physician to make a careful observation of the orbits, lids, conjunctiva, cornea, anterior chamber, and iris. The angle of aqueous drainage at the peripheral edge of the iris should also be measured. Two methods of determining the draining angle are flashlight test Van Herrick test How Is the Test Performed? The slit-lamp settings are as follows: 60º angle narrow beam right beam magnification of 16 The slit beam is very bright and thin, and it is offset 60º temporally to the slit-lamp oculars. The temporal sclera is illuminated, and the slit lamp beam is brought slowly toward the cornea until the anterior chamber is first identified. Here, the thickness of the cornea is compared to the depth of the peripheral anterior chamber. If the anterior chamber is as deep as the cornea is thick, then the angle is presumed to be wide open. If there is only a slit of aqueous, then the angle is estimated to be dangerously narrow. None of the aforementioned tests is a definitive determination of suspected occludable angles and, therefore, should not be used as a replacement for gonioscopy. They are, however, means of confirming what the gonioscopic examination reveals. 13 n 1. Recommended standard procedures for the clinical measurement and specification of visual acuity. Report of Working Group 39. Committee on Vision. Assembly of Behavioral and Social Sciences, National Research Council, National Academy of Sciences, Washington, D.C. Adv Ophthalmol. 1980;41: Ginsburg AP, et al. Functional assessment of glaucoma using visual fields, contrast sensitivity and night driving simulation. Presented at: ASCRS/ASOA Symposium on Cataract, IOL and Refractive Surgery; April 1-5, 1995; San Diego, CA. 3. Mayo Clinic Staff. Glaucoma. Accessed May 2, Grødum K, Heijl A, Bengtsson B. Refractive error and glaucoma. Acta Ophthalmol Scand. 2001;79(6): Meeker M, Du R, Bacchetti P, et al. Pupil examination: validity and clinical utility of an automated pupillometer. J Neurosci Nurs. 2005;37(1): Brenner FD. Pupil assessment in optic nerve disorders. Eye. 2004;18: n11/full/ a.html. Accessed May 22, James CB, Benjamin L. Ophthalmology: Investigation and Examination Techniques. Oxford, UK: Butterworth-Heinemann; Amjad A, Amir Y, Jamal DA, Fiaz. Pitfalls in intraocular pressure measurement by Goldmann-type applanation tonometers. Pak J Ophthalmol. 2009;25(4). 9. Argues WA. Ocular hypertension and central corneal thickness. Ophthalmology. 1995;102(12): Brant J, Beisser J, Gordon M. Central corneal thickness in Ocular Hypertension Treatment Study (OHTS). Ophthalmology. 2001;108(10): Ehlers N, Bramsen T, Sperling S. Applanation tonometry and central corneal thickness in low tension glaucoma. Acta Ophthalmol (Copenh). 1975;52: Smith MF, Doyle JW. Clinical examination of glaucoma. clinical-examination-of-glaucoma. Accessed May 22, Friedman NJ, Kaiser PK. Essentials of Ophthalmology. 1st ed. Philadelphia, PA: W. B. Saunders: 2007; glaucoma today 2012 Ultimate Technician s Survival Guide
6 PATIENT WORKUP by Janet hunter, bs, comt Patient WorkUp History and Chief Complaint byline History taking is one of the most important skills taught to ophthalmic technical personnel. Most troubles can be uncovered by taking a comprehensive history of the patient, which will greatly assist the physician Body in determining the patient s needs and risk factors. The history of a patient with glaucoma should specifically include the following: Any ocular redness, discomfort, or pain? In which eye? For how long? Any blurred vision? In which eye? For how long? Do you see any halos around lights? In which eye? For how long? Are you experiencing glare? In which eye? For how long? Which glaucoma eye drops are you taking? How frequently? In which eye? Are you taking the drops as prescribed? Did you use the glaucoma drops today? When was the last time you used your drops? At what time? In which eye? Any burning or stinging when you instill the glaucoma drops? Are you performing punctal occlusion? For how long per eye? Are you having difficulty with dark/light adaptation? Are you having difficulty following fast-moving objects with your eyes? Past Ocular History A complete history of past surgery, trauma, and previous ocular disease is imperative. Key areas for direct questioning include glaucoma, macular degeneration, retinal tears or detachment amblyopia diabetes strabismus contact lenses and spectacles past ocular trauma When taking the history of patients who were diagnosed in the past with glaucoma, ask the following: How long ago were you diagnosed with glaucoma? Do you use eye drops? Which one(s)? How frequently? In which eye? Any history of surgery? Laser treatment? What type? In which eye? On what date? Any history of refractive surgery? In which eye? On what date? Do you have a family history of glaucoma? Who? Have you taken any steroid medications? If yes, which type? Have you ever suffered ocular trauma? If yes, what type? Past Medical History Carefully study the patient s records for a past diagnosis of glaucoma. Certain glaucoma medications are contraindicated should the patient suffer from other medical problems such as hypertension, asthma, chronic obstructive pulmonary disease, etc. It cannot be overstated that these are an absolute red flag for a potential glaucoma patient. If these facts are left out of the chart, they may compromise the physician s choice of glaucoma therapy and, in some cases, may become life threatening to the patient. Pertinent questions to ask the glaucoma patient include the following: Do you have a history of high blood pressure? Low blood pressure? Do you have a history of elevated cholesterol? Do you have a history of migraines? Do you suffer from cold hands or feet (Raynaud disease)? Do you snore (sleep apnea)? Do you have a history of any autoimmune disease? Social History A patient s lifestyle can also be a significant determining factor of how the physician ultimately decides to treat the glaucoma. A number of studies have shown an association between alcohol consumption and the risk of glaucoma. 1 Emotional upsets and stress can increase external blood pressure and thus affect intraocular pressure. For this reason, the technician s documentation of the patient s lifestyle and use of alcohol and tobacco is imperative. Allergies Many physicians speculate whether allergies affect glaucoma. People who suffer from food or environmental allergies or from a compromised immune function can appear to be at higher risk of developing glaucoma. It is imperative that the technician chart any allergies in addition to the patient s current medications. The documentation of any 2012 Ultimate Technician s Survival Guide glaucoma today 15
7 Patient WorkUp adverse reaction to medications is urgent. Severe allergic reactions to medication can include itching redness hives difficulty breathing death Ocular Medications Many patients simply do not remember the names of their glaucoma medications. This is quite understandable when some of them are well beyond the layman s pronunciation capabilities. For this reason, technicians should familiarize themselves with the cap color associated with each different type of medication (Table). Systemic Medications Many nonocular medications can significantly increase intraocular pressure and even cause glaucoma. A few examples of these medications are Corticosteroids, which can lead to ocular hypertension and open-angle glaucoma Anticholinergics and tricyclic antidepressants, which can cause angle closure Anticonvulsants, which can cause nasal peripheral visual field loss Antihistamines Topiramate (Topomax; Janssen Pharmaceuticals, Inc.) Birth control medications 2,3 Examinations In addition to the patient s history, the following physical examinations should also be completed. New Glaucoma Patient Workup - Ocular examinations Visual acuity, which includes checking glasses and refraction Confrontation visual fields (may defer if automated perimetry performed) Motility and alignment Pupils Tonometry, using tonopen on corneal transplant patients Table. Ocular Medications CAP COLOR CLASS EXAMPLES MECHANISM Yellow and blue b-blocker Generic: timolol maleate solution Branded: Betimol (Santen, Inc.), Istalol (Ista Pharmaceuticals, Inc.) Decreases volume of aqueous humor produced Green Miotic Generic: pilocarpine Stimulates iris sphincter to contract and pupillary constriction, which increase aqueous outflow Purple a-adrenergic agonist Generic: brimonidine Branded: Alphagan P (Allergan, Inc.) Decreases fluid production Orange Carbonic anhydrase inhibitor Branded: Trusopt (Merck & Co., Inc.) Decreases fluid production Clear or teal Prostaglandin analogue Generic: latanoprost Branded: Lumigan (Allergan, Inc.), Travatan (Alcon Laboratories, Inc.), Xalatan (Pfizer, Inc.), Zioptan (Merck & Co., Inc.) Increases aqueous humor drainage Red Mydriatic or cycloplegic Generic: atropine, cyclopentolate Dilates the pupil Pink Anti-inflammatory drug or steroid Branded: Durezol (Alcon Laboratories, Inc.), Lotemax (Bausch + Lomb), Pred Forte (Allergan, Inc.) Controls inflammation. Note: steroids should not be used for long periods of time; these drugs can cause the intraocular pressure to rise and induce glaucoma glaucoma today 2012 Ultimate Technician s Survival Guide
8 Corneal pachymetry (three measurements for each eye) - Gonioscopy Before pupillary dilation - Glaucoma flow sheet Patient identification information Diagnosis Date and time of tonometry Tonometry measurements (right, left) Medications, including dosing, allergies, ineffectiveness Corneal pachymetry average - Prescriptions Medication Glasses Returning Glaucoma Patient Workup - Review of last clinical notes and instructions - Photograph file placed with chart - IOP recorded on flow sheet - Last dilated examination and last visual field recorded General Patient Workup - Detailed history - Ocular examinations Visual acuity, which includes checking glasses and refraction Confrontation visual fields Motility and alignment Pupils Tonometry - Corneal pachymetry, glaucoma flow sheets, and stereodisc photography deferred - Review of last clinical notes and instructions - Last dilated examination recorded - Prescriptions for medication and glasses n 1. Pasquale LR, Kang JH. Lifestyle, nutrition, and glaucoma. J Glaucoma. 2009;18(6): Katz J, Sommer A. Risk factors for primary open angle glaucoma. Am J Prev Med. 1988; 4: Life Extension. Health concerns: glaucoma. Accessed May 22, Brian D, Kershner RM. Ophthalmic Medications and Pharmacology. 1st ed. Thorofare, NJ: Slack Inc.; Patient WorkUp 2012 Ultimate Technician s Survival Guide glaucoma today 17
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Written by Administrator Wednesday, 13 January :27 - Last Updated Thursday, 21 January :34
 angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
1/31/2018. Course Objectives. Diagnostic Testing. Optic Nerve Damage ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY TECHNICIAN: -SDP
 ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
THE CHRONIC GLAUCOMAS
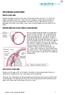 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Glaucoma What You Should Know
 Glaucoma What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research that leads
Glaucoma What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research that leads
Visit Type (Check one)
 Page 1 of 14 OHFV21.01 MULE: Page 1 Visit Type (Check one) Visit prior to 078 month visit enter visit window 0 Semi-Annual: Annual: 078 mo. 090 mo. 102 mo. 114 mo. 126 mo. 138 mo. 150 mo. 162 mo. 084 mo.
Page 1 of 14 OHFV21.01 MULE: Page 1 Visit Type (Check one) Visit prior to 078 month visit enter visit window 0 Semi-Annual: Annual: 078 mo. 090 mo. 102 mo. 114 mo. 126 mo. 138 mo. 150 mo. 162 mo. 084 mo.
Glaucoma. Cornea. Iris
 Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Vision Health: Conditions, Disorders & Treatments GLAUCOMA
 Vision Health: Conditions, Disorders & Treatments GLAUCOMA Glaucoma is a disease of the optic nerve, which transmits the images you see from the eye to the brain. The optic nerve is made up of many nerve
Vision Health: Conditions, Disorders & Treatments GLAUCOMA Glaucoma is a disease of the optic nerve, which transmits the images you see from the eye to the brain. The optic nerve is made up of many nerve
Treatments for Open-Angle Glaucoma. A Review of the Research for Adults
 Treatments for Open-Angle Glaucoma A Review of the Research for Adults Is This Information Right for Me? Yes, this information is for you if: Your eye doctor has said that you have open-angle glaucoma,
Treatments for Open-Angle Glaucoma A Review of the Research for Adults Is This Information Right for Me? Yes, this information is for you if: Your eye doctor has said that you have open-angle glaucoma,
GLAUCOMA. An Overview
 GLAUCOMA An Overview Compiled by Campbell M Gold (2004) CMG Archives http://campbellmgold.com --()-- IMPORTANT The health information contained herein is not meant as a substitute for advice from your
GLAUCOMA An Overview Compiled by Campbell M Gold (2004) CMG Archives http://campbellmgold.com --()-- IMPORTANT The health information contained herein is not meant as a substitute for advice from your
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma. What is glaucoma? Eye Words to Know. What causes glaucoma?
 2014 2015 Glaucoma What is glaucoma? Glaucoma is a disease that damages your eye s optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure
2014 2015 Glaucoma What is glaucoma? Glaucoma is a disease that damages your eye s optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
It all begins with CASE HISTORY
 1 It all begins with CASE HISTORY This is one of the most important procedures in any eye examination. You become the detective Ask open ended questions Let the patient tell you their story Chief Complaint
1 It all begins with CASE HISTORY This is one of the most important procedures in any eye examination. You become the detective Ask open ended questions Let the patient tell you their story Chief Complaint
WORLD GLAUCOMA WEEK What is Glaucoma? Can I develop glaucoma if I have increased eye pressure?
 WORLD GLAUCOMA WEEK What is Glaucoma? Glaucoma is a group of diseases that damage the optic nerve and can result in gradual vision loss and blindness. However, with early detection and treatment, you can
WORLD GLAUCOMA WEEK What is Glaucoma? Glaucoma is a group of diseases that damage the optic nerve and can result in gradual vision loss and blindness. However, with early detection and treatment, you can
glaucoma a closer look
 0AMERICAN ACADEMY OF OPHTHALMOLOGY The Eye M.D. Association 2012-2013 glaucoma a closer look WHAT IS GLAUCOMA? < Glaucoma is a disease of the optic nerve the part of the eye that carries the images we
0AMERICAN ACADEMY OF OPHTHALMOLOGY The Eye M.D. Association 2012-2013 glaucoma a closer look WHAT IS GLAUCOMA? < Glaucoma is a disease of the optic nerve the part of the eye that carries the images we
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Training Checking Vision Tonometry
 Training 101-2 Checking Vision Tonometry Checking Vision The classic example of an eye chart is the Snellen eye chart, in general they show 11 rows of capital letters. The top row contains one letter (usually
Training 101-2 Checking Vision Tonometry Checking Vision The classic example of an eye chart is the Snellen eye chart, in general they show 11 rows of capital letters. The top row contains one letter (usually
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
OCULAR PHARMACOLOGY GLAUCOMA. increased intraocular pressure. normally mm Hg. when to Tx no fixed level.
 OCULAR PHARMACOLOGY GLAUCOMA increased intraocular pressure normally 12 20 mm Hg. when to Tx no fixed level. literature sets ~21 mm Hg as upper limit of normal. some safe at 30 mm Hg some may have damage
OCULAR PHARMACOLOGY GLAUCOMA increased intraocular pressure normally 12 20 mm Hg. when to Tx no fixed level. literature sets ~21 mm Hg as upper limit of normal. some safe at 30 mm Hg some may have damage
Glaucoma. How is Glaucoma Diagnosed? Glaucoma Testing
 Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
@HUHEYE in Haiti 2018
 @HUHEYE in Haiti 2018 Eye Evaluation and Common Eye Diseases Leslie S. Jones, MD Associate Professor and Interim Chair Residency Program Director Glaucoma Services Director Department of Ophthalmology
@HUHEYE in Haiti 2018 Eye Evaluation and Common Eye Diseases Leslie S. Jones, MD Associate Professor and Interim Chair Residency Program Director Glaucoma Services Director Department of Ophthalmology
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Save time at your check-in and register online before your appointment! It s as easy as 1-2-3
 Save time at your check-in and register online before your appointment! It s as easy as 1-2-3 1. Go online to www.blackhillseyes.com 2. Click this logo on our home page for the link to register: 3. Set-up
Save time at your check-in and register online before your appointment! It s as easy as 1-2-3 1. Go online to www.blackhillseyes.com 2. Click this logo on our home page for the link to register: 3. Set-up
Closed Angle Glaucoma Or Narrow Angle Glaucoma. What s is a closed angle type of glaucoma,
 Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
OCT : retinal layers. Extraocular muscles. History. Central vs Peripheral vision. History: Temporal course. Optical Coherence Tomography (OCT)
 Optical Coherence Tomography (OCT) OCT : retinal layers 7 Central vs Peripheral vision Extraocular muscles RPE E Peripheral Vision: Rods (95 million) 30% Ganglion cells Central Vision: Cones (5 million)
Optical Coherence Tomography (OCT) OCT : retinal layers 7 Central vs Peripheral vision Extraocular muscles RPE E Peripheral Vision: Rods (95 million) 30% Ganglion cells Central Vision: Cones (5 million)
Resources from the American Academy of Ophthalmology...1 Meet the Eye Care Team...1 Eye Myths... 3
 CONTENTS Preface...ix Acknowledgments... x About the Executive Editors... x Introduction to Ophthalmology... 1 Resources from the American Academy of Ophthalmology...1 Meet the Eye Care Team...1 Eye Myths...
CONTENTS Preface...ix Acknowledgments... x About the Executive Editors... x Introduction to Ophthalmology... 1 Resources from the American Academy of Ophthalmology...1 Meet the Eye Care Team...1 Eye Myths...
The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options
 The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options What is a cataract? A cataract is a clouding of the lens of the eye. This blocks
The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options What is a cataract? A cataract is a clouding of the lens of the eye. This blocks
The cataract laser technology of tomorrow is here for you today.
 The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting options Thanks to recent advancements, this is a great time to have cataract surgery Laser precision
The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting options Thanks to recent advancements, this is a great time to have cataract surgery Laser precision
GLAUCOMA (2006) PHILIPPINE GLAUCOMA SOCIETY
 GLAUCOMA (2006) PHILIPPINE GLAUCOMA SOCIETY CPM 9 TH EDITION Philippine Glaucoma Society (PGS) Correspondence to: Eye Referral Center, T. M. Kalaw Street, Ermita, Manila Telephone: 524-7119/525-9360 Mobile:
GLAUCOMA (2006) PHILIPPINE GLAUCOMA SOCIETY CPM 9 TH EDITION Philippine Glaucoma Society (PGS) Correspondence to: Eye Referral Center, T. M. Kalaw Street, Ermita, Manila Telephone: 524-7119/525-9360 Mobile:
Divakar Gupta Glaucoma Fellow, Duke Eye Center 5/14/16
 Divakar Gupta Glaucoma Fellow, Duke Eye Center 5/14/16 Pathophysiology of glaucoma Consider risk factors of glaucoma Understand the side effects of glaucoma medications Diagnostic testing Leading cause
Divakar Gupta Glaucoma Fellow, Duke Eye Center 5/14/16 Pathophysiology of glaucoma Consider risk factors of glaucoma Understand the side effects of glaucoma medications Diagnostic testing Leading cause
VN 122 MODULE F EYE AND VISION DISORDERS OCULAR HISTORY 1. PATIENT PERCEPTION OF PROBLEM 2. DECREASED VISION? 3. BLURRED, DOUBLE, DISTORTED?
 VN 122 MODULE F EYE AND VISION DISORDERS OCULAR HISTORY 1. PATIENT PERCEPTION OF PROBLEM 2. DECREASED VISION? 3. BLURRED, DOUBLE, DISTORTED? 4. PAIN? QUALITY OF PAIN? 5. ITCHING, DRY? 6. BOTH EYES? 7.
VN 122 MODULE F EYE AND VISION DISORDERS OCULAR HISTORY 1. PATIENT PERCEPTION OF PROBLEM 2. DECREASED VISION? 3. BLURRED, DOUBLE, DISTORTED? 4. PAIN? QUALITY OF PAIN? 5. ITCHING, DRY? 6. BOTH EYES? 7.
11/30/2009. Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil
 Normal Ocular Anatomy Glaucoma Dr Sunil Deokule, MD Asst. Prof and Glaucoma Specialist University of Kentucky Definition Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil Optic
Normal Ocular Anatomy Glaucoma Dr Sunil Deokule, MD Asst. Prof and Glaucoma Specialist University of Kentucky Definition Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil Optic
Assisting in Ophthalmology. Copyright 2011, 2007, 2003, 1999 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
8/30/2018. Eye Disorders. Patrick Sarte. Anatomy of the Eye Uveitis Scleritis vs. Episcleritis Glaucoma Retinal Findings Eyelids
 Eye Disorders Patrick Sarte Anatomy of the Eye Uveitis Scleritis vs. Episcleritis Glaucoma Retinal Findings Eyelids 1 Anatomy of the Eye Anatomy of the Eye 2 Anatomy of the Eye 3 4 A 26 year old woman
Eye Disorders Patrick Sarte Anatomy of the Eye Uveitis Scleritis vs. Episcleritis Glaucoma Retinal Findings Eyelids 1 Anatomy of the Eye Anatomy of the Eye 2 Anatomy of the Eye 3 4 A 26 year old woman
VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz)
 PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
GENERAL INFORMATION GLAUCOMA GLAUCOMA
 GENERAL INFORMATION GLAUCOMA GLAUCOMA WHAT IS GLAUCOMA? Glaucoma is commonly known as the sneak thief of sight because it can cause irreversible vision loss without any obvious symptoms. The term glaucoma
GENERAL INFORMATION GLAUCOMA GLAUCOMA WHAT IS GLAUCOMA? Glaucoma is commonly known as the sneak thief of sight because it can cause irreversible vision loss without any obvious symptoms. The term glaucoma
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care
 The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
STANDARDIZED CLINICAL PROTOCOLS. OPD and Refraction Protocols. Aravind Eye Care System 1, Anna Nagar, Madurai , Tamilnadu, India
 STANDARDIZED CLINICAL PROTOCOLS OPD and Refraction Protocols Aravind Eye Care System 1, Anna Nagar, Madurai - 625 020, Tamilnadu, India STANDARDIZED PROTOCOLS FOR OUTPATIENT EXAMINATION Guidelines for
STANDARDIZED CLINICAL PROTOCOLS OPD and Refraction Protocols Aravind Eye Care System 1, Anna Nagar, Madurai - 625 020, Tamilnadu, India STANDARDIZED PROTOCOLS FOR OUTPATIENT EXAMINATION Guidelines for
FROM CATARACTS TO CLARITY
 Cathy Cataracts FROM CATARACTS TO CLARITY If you re 55 or older, you may have cataracts and not even know it. What You Need to Know Seeing Beyond the Symptoms Cataracts are one of the leading causes of
Cathy Cataracts FROM CATARACTS TO CLARITY If you re 55 or older, you may have cataracts and not even know it. What You Need to Know Seeing Beyond the Symptoms Cataracts are one of the leading causes of
ALTERNATIVES TO PHAKIC IMPLANT SURGERY
 Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
PATIENT CASE HISTORY. General Health Medications Allergies
 OCULAR PHARMACOLOGY What I Need to Know Before I Medicate A Patient Lynn Lawrence, CPOT, ABOC, COA ROLE of the ASSISTANT AND TECHNICIAN Accurate documentation/recording Patient Education can assist in
OCULAR PHARMACOLOGY What I Need to Know Before I Medicate A Patient Lynn Lawrence, CPOT, ABOC, COA ROLE of the ASSISTANT AND TECHNICIAN Accurate documentation/recording Patient Education can assist in
Long Term Care Formulary RS 14. RESTRICTED STATUS Topical Medical Treatment of Glaucoma 1 of 5
 RESTRICTED STATUS Topical Medical Treatment of Glaucoma 1 of 5 PREAMBLE Significance: Glaucoma occurs in 1-2% of white people aged over 40 years, rising to 5% at 70 years and exponentially with advancing
RESTRICTED STATUS Topical Medical Treatment of Glaucoma 1 of 5 PREAMBLE Significance: Glaucoma occurs in 1-2% of white people aged over 40 years, rising to 5% at 70 years and exponentially with advancing
East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults
 East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults Introduction Glaucoma is a group of eye diseases causing optic nerve damage. In most cases
East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults Introduction Glaucoma is a group of eye diseases causing optic nerve damage. In most cases
8 USE IN SPECIFIC POPULATIONS Patients with Open-Angle Glaucoma or Ocular Hypertension
 3 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use Isopto Carpine safely and effectively. See full prescribing information for Isopto Carpine. Isopto
3 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use Isopto Carpine safely and effectively. See full prescribing information for Isopto Carpine. Isopto
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA
 PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
PATIENT GUIDE TO LUMIGAN 0.01%
 Treatment Tracker enclosed PATIENT GUIDE TO LUMIGAN 0.01% LUMIGAN (bimatoprost ophthalmic solution) 0.01% is used for the treatment of high eye pressure, also called intraocular pressure (IOP), in people
Treatment Tracker enclosed PATIENT GUIDE TO LUMIGAN 0.01% LUMIGAN (bimatoprost ophthalmic solution) 0.01% is used for the treatment of high eye pressure, also called intraocular pressure (IOP), in people
Acute Eyes for ED. Enis Kocak. The Alfred Ophthalmology
 Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
By Darlene Jones, Nurse. May 2017
 By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
By Darlene Jones, Nurse May 2017 Disclosure of potential conflict of interest Darlene Jones, Nurse I have no conflict of interest Course objectives Become familiar with the different pathologies in ophthalmology
Pre-Operative Health Questionnaire. 3. Are you currently taking any of the following medications for. glaucoma: TRAVATAN LUMIGAN XALATAN
 Pre-Operative Health Questionnaire 1. Are you Diabetic? YES / NO 2. Are you currently on dialysis? YES / NO 3. Are you currently taking any of the following medications for glaucoma: TRAVATAN LUMIGAN XALATAN
Pre-Operative Health Questionnaire 1. Are you Diabetic? YES / NO 2. Are you currently on dialysis? YES / NO 3. Are you currently taking any of the following medications for glaucoma: TRAVATAN LUMIGAN XALATAN
Disclosure Ocular Anatomy and Motility
 Disclosure Ocular Anatomy and Motility Jenean Carlton BA, ABOC, NCLC President, Carlton & Associates, LLC Carlton and Associates, LLC provides communications and educational materials for the optical industry
Disclosure Ocular Anatomy and Motility Jenean Carlton BA, ABOC, NCLC President, Carlton & Associates, LLC Carlton and Associates, LLC provides communications and educational materials for the optical industry
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
ASSESSING THE EYES. Structures. Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris.
 ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
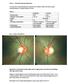 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Glaucoma. Glaucoma. Glaucoma. Trevor Arnold, MS, DVM, DACVO
 Glaucoma Trevor Arnold, MS, DVM, DACVO Glaucoma Physiology of Aqueous Humor Produced in the ciliary body Flows out the iridocorneal angle and ciliary cleft High intraocular pressures are caused by a decreased
Glaucoma Trevor Arnold, MS, DVM, DACVO Glaucoma Physiology of Aqueous Humor Produced in the ciliary body Flows out the iridocorneal angle and ciliary cleft High intraocular pressures are caused by a decreased
Ophthalmology. Caring For Your Eyes. Jurong Medical Centre
 Ophthalmology Caring For Your Eyes Jurong Medical Centre Your eyes and you At Jurong Medical Centre, we have a dedicated team of ophthalmologists that specialise in treating a wide range of acute and chronic
Ophthalmology Caring For Your Eyes Jurong Medical Centre Your eyes and you At Jurong Medical Centre, we have a dedicated team of ophthalmologists that specialise in treating a wide range of acute and chronic
Cataract Surgery Co-Management
 Cataract Surgery Co-Management Phacoemulsification, Clear-Lens Extraction, and LensX INCLUSION CRITERIA: Significant visual complaints (decreased VA, increased glare, decreased Activities of Daily Living
Cataract Surgery Co-Management Phacoemulsification, Clear-Lens Extraction, and LensX INCLUSION CRITERIA: Significant visual complaints (decreased VA, increased glare, decreased Activities of Daily Living
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Around The Globe in 60 Minutes
 Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Reason for Unscheduled Visit
 Page 1 of 7 OHUN16.01 MULE: UNREASONS Reason for Unscheduled Visit * On any given page, any section started should be completed. Check all that apply: 1. Confirmation of IOP... Complete Snellen, IOP, Ocular
Page 1 of 7 OHUN16.01 MULE: UNREASONS Reason for Unscheduled Visit * On any given page, any section started should be completed. Check all that apply: 1. Confirmation of IOP... Complete Snellen, IOP, Ocular
Managing the Patient with POAG
 Managing the Patient with POAG Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Ocular Hypertension (OHT) Most
Managing the Patient with POAG Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Ocular Hypertension (OHT) Most
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
UC SF. g h. Eye Trauma. Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California
 UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
A LITTLE ANATOMY. three layers of eye: 1. outer: corneosclera. 2. middle - uvea. anterior - iris,ciliary body. posterior - choroid
 GLAUCOMA A LITTLE ANATOMY three layers of eye: 1. outer: corneosclera 2. middle - uvea anterior - iris,ciliary body posterior - choroid connection at the pars plana between post and ant uvea 3. retina
GLAUCOMA A LITTLE ANATOMY three layers of eye: 1. outer: corneosclera 2. middle - uvea anterior - iris,ciliary body posterior - choroid connection at the pars plana between post and ant uvea 3. retina
Your First Appointment:
 Your First Appointment: The Important Questions to Ask When Choosing a Cataract Surgeon www.kremereyecenter.com / 866-270-2773 Cataract 1 Surgery Kremer Eye Center Table of Contents Introduction... 3 Finding
Your First Appointment: The Important Questions to Ask When Choosing a Cataract Surgeon www.kremereyecenter.com / 866-270-2773 Cataract 1 Surgery Kremer Eye Center Table of Contents Introduction... 3 Finding
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
02/03/2014. Average Length: 23mm (Infant ~16mm) Approximately the size of a quarter Volume: ~5mL
 Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
VI.2.2 Summary of treatment benefits
 EU-Risk Management Plan for Bimatoprost V01 aetiology), both OAG and ACG can be secondary conditions. Secondary glaucoma refers to any case in which another disorder (e.g. injury, inflammation, vascular
EU-Risk Management Plan for Bimatoprost V01 aetiology), both OAG and ACG can be secondary conditions. Secondary glaucoma refers to any case in which another disorder (e.g. injury, inflammation, vascular
Advanced Eyecare of Orange County/ Kim T. Doan, M.D.
 Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Technicians & Nurses Program
 ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans I have none Sunday, May 8, 2016, 10:30-11:30am Amy Jost, BS, COMT, CCRC Cincinnati Eye Institute Identify the tech
ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans I have none Sunday, May 8, 2016, 10:30-11:30am Amy Jost, BS, COMT, CCRC Cincinnati Eye Institute Identify the tech
Cataract Surgery: Patient Information
 Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
KEY MESSAGES. Details of the evidence supporting these recommendations can be found in the above CPG, available on the following websites:
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS KEY MESSAGES 1. Glaucoma is a chronic eye disease that damages the optic nerve, & can result in serious vision loss and irreversible blindness. 2. Glaucoma diagnosis
QUICK REFERENCE FOR HEALTHCARE PROVIDERS KEY MESSAGES 1. Glaucoma is a chronic eye disease that damages the optic nerve, & can result in serious vision loss and irreversible blindness. 2. Glaucoma diagnosis
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Corporate Medical Policy
 Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
THE 35 GOLDEN EYE RULES
 THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
Cataract. A cataract is a clouding of the lens in your eye. It
 Cataract A cataract is a clouding of the lens in your eye. It affects your vision. Cataracts are very common in older people. By age 80, more than half of all Americans either have a cataract or have had
Cataract A cataract is a clouding of the lens in your eye. It affects your vision. Cataracts are very common in older people. By age 80, more than half of all Americans either have a cataract or have had
YOUR VYZULTA TREATMENT GUIDE. Please see Important Safety Information on pages 1, 9, 10, 17 and 18. Please see accompanying Prescribing Information.
 YOUR VYZULTA TREATMENT GUIDE Please see Important Safety Information on pages 1, 9, 10, 17 and 18. Please see accompanying Prescribing Information. INDICATION VYZULTA TM (latanoprostene bunod ophthalmic
YOUR VYZULTA TREATMENT GUIDE Please see Important Safety Information on pages 1, 9, 10, 17 and 18. Please see accompanying Prescribing Information. INDICATION VYZULTA TM (latanoprostene bunod ophthalmic
INFORMED CONSENT FOR CORNEAL COLLAGEN CROSS-LINKING WITH RIBOFLAVIN (C3-R) FOR PATIENTS WITH KERATOCONUS OR CORNEAL ECTASIA
 INFORMED CONSENT FOR CORNEAL COLLAGEN CROSS-LINKING WITH RIBOFLAVIN (C3-R) FOR PATIENTS WITH KERATOCONUS OR CORNEAL ECTASIA INTRODUCTION: This information is to help you make an informed decision about
INFORMED CONSENT FOR CORNEAL COLLAGEN CROSS-LINKING WITH RIBOFLAVIN (C3-R) FOR PATIENTS WITH KERATOCONUS OR CORNEAL ECTASIA INTRODUCTION: This information is to help you make an informed decision about
More possibilities after.
 Many possibilities during cataract surgery. More possibilities after. Knowing your options can help you focus on the breathtaking experiences still to come. AcrySof IQ IOL Family Advancing CATARACT SURGERY
Many possibilities during cataract surgery. More possibilities after. Knowing your options can help you focus on the breathtaking experiences still to come. AcrySof IQ IOL Family Advancing CATARACT SURGERY
Cairo University Faculty of Medicine. Course Specifications Course title: Ophthalmology (Code): OPH-409. Department of Ophthalmology
 Cairo University Faculty of Medicine Department of Ophthalmology Course Specifications Course title: Ophthalmology (Code): OPH-409 Department of Ophthalmology Fourth academic year of M.B.B.Ch. program
Cairo University Faculty of Medicine Department of Ophthalmology Course Specifications Course title: Ophthalmology (Code): OPH-409 Department of Ophthalmology Fourth academic year of M.B.B.Ch. program
Chronicity. Narrow Minded. Course Outline. Acute angle closure. Subacute angle closure. Classification of Angle Closure 5/19/2014
 Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
5/12/2014. Lynn E. Lawrence, CPOT, ABOC, COA
 Lynn E. Lawrence, CPOT, ABOC, COA Glaucoma is an optic neuropathy characterized by a loss of ganglion cells and their axons, in the RNFL. The loss of retinal ganglion cells in glaucoma is irreversible
Lynn E. Lawrence, CPOT, ABOC, COA Glaucoma is an optic neuropathy characterized by a loss of ganglion cells and their axons, in the RNFL. The loss of retinal ganglion cells in glaucoma is irreversible
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Glaucoma: diagnosis and management (large print version)
 Glaucoma: diagnosis and management (large print version) 1 November 2017 Recommendations People have the right to be involved in discussions and make informed decisions about their care, as described in
Glaucoma: diagnosis and management (large print version) 1 November 2017 Recommendations People have the right to be involved in discussions and make informed decisions about their care, as described in
Texas Definition of Eye Exam. Definitions of Eye Examinations BILLING AND CODING: WHY IS THIS STUFF SO HARD? Optometry School Definition
 BILLING AND CODING: WHY IS THIS STUFF SO HARD? Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Definitions of Eye Examinations Optometry School definition
BILLING AND CODING: WHY IS THIS STUFF SO HARD? Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Definitions of Eye Examinations Optometry School definition
SAMPLE WHAT LASIK CAN DO
 DECIDING ON LASIK Imagine being able to work, drive, and play sports without having to depend on glasses or contact lenses. LASIK (laser in-situ keratomileusis) may make this a reality for you. This laser
DECIDING ON LASIK Imagine being able to work, drive, and play sports without having to depend on glasses or contact lenses. LASIK (laser in-situ keratomileusis) may make this a reality for you. This laser
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. OPTOMETRIC MEDICINE CLINICAL GUIDELINES: TABLE OF CONTENTS
 NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. OPTOMETRIC MEDICINE CLINICAL GUIDELINES: 2012-2013 TABLE OF CONTENTS CONDITION PAGE(S) Complete Eye and Vision Examination 2 Vision Screening Procedure
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. OPTOMETRIC MEDICINE CLINICAL GUIDELINES: 2012-2013 TABLE OF CONTENTS CONDITION PAGE(S) Complete Eye and Vision Examination 2 Vision Screening Procedure
