Intracranial hypotension caused by leakage of cerebrospinal fluid from the thecal sac after lumboperitoneal shunt placement
|
|
|
- Sibyl McCormick
- 6 years ago
- Views:
Transcription
1 J Neurosurg 107: , 2007 Intracranial hypotension caused by leakage of cerebrospinal fluid from the thecal sac after lumboperitoneal shunt placement Case report YAPING JOYCE LIAO, M.D., PH.D., 1 WILLIAM P. DILLON, M.D., 2 CYNTHIA T. CHIN, M.D., 2 MICHAEL W. MCDERMOTT, M.D., 3 AND JONATHAN C. HORTON, M.D., PH.D. 1,4 Departments of 1 Ophthalmology, 2 Radiology, 3 Neurosurgery, and 4 Neurology, University of California San Francisco, California The authors describe a newly recognized complication of lumboperitoneal (LP) shunt placement, namely, intracranial hypotension from leakage of cerebrospinal fluid (CSF) through a defect in the lumbar dura created by the shunt catheter. They report on a 47-year-old obese woman with idiopathic intracranial hypertension who underwent routine placement of an LP shunt. Following surgery, her headache became worse. Two radionuclide shunt studies showed no anterograde tracer flow, suggesting either obstruction or a leak. After shunt reservoir manometry indicated low pressure, spinal magnetic resonance (MR) imaging was performed. The MR images revealed a CSF leak from the lumbar thecal sac. A computed tomography (CT) myelogram, performed by injection into the shunt reservoir, confirmed the presence of a leak by showing extravasation of contrast agent into the epidural space. The patient was treated by application of a CT-guided blood patch at the leak site. Catheter-associated CSF leak is an unusual cause of intracranial hypotension that can occur following LP shunt placement. This case report outlines the clinical features of this condition, documents the neuroradiological findings, and demonstrates successful treatment with a blood patch. KEY WORDS blood patch idiopathic intracranial hypertension papilledema pseudotumor cerebri radionuclide shuntogram W HEN weight loss and carbonic anhydrase inhibitors fail in the treatment of patients with IIH, surgical intervention should not be delayed. 5 The operations performed most commonly are optic nerve sheath fenestration and LP shunt placement. 3 The latter procedure has the advantages of lowering ICP and relieving papilledema, whereas optic nerve sheath fenestration does not reduce ICP. 9 In principle, therefore, LP shunt placement accomplishes both of one s major therapeutic goals: preventing vision loss and curing headache. Unfortunately, some patients continue to report headache after LP shunt placement. 13 In these patients, the diagnostic challenge is to determine why headache persists. We treated a patient with IIH who had severe, intractable headache after uneventful placement of an LP shunt. The patient s headache was due to a newly recognized complication, namely, leakage of CSF from the lumbar thecal sac caused by the shunt catheter. Here we document the radiological appearance of CSF leak associated with an LP shunt catheter and describe the successful application of an epidural blood patch. Case Report History and Presentation. This 47-year-old woman developed headache, papilledema, and blurred vision. The results of an MR imaging study were normal. Elevated ICP was documented on numerous occasions by measurement of the lumbar subarachnoid opening pressure. Analysis of the CSF was normal. Idiopathic intracranial hypertension was diagnosed in the patient and her symptoms were controlled with acetazolamide and analgesics for several years. She was eventually referred to our institution for LP shunt placement because of advancing peripheral visual field loss and medically refractory headache. Examination. The patient weighed 90 kg and her height was 165 cm, for a body mass index of 33.1 (obese). Her visual acuity was 20/20 in each eye. Computerized Humphrey 1
2 Y. J. Liao et al. FIG. 1. Lateral radiograph of the lumbar spine showing the LP shunt, with the catheter entering the thecal sac at the L2 3 level and extending rostrally to the T11 12 level (arrowheads). The radiograph reveals no migration or disconnection of the LP shunt hardware. The arrow indicates the reservoir; the asterisk, the horizontal-vertical valves. FIG. 2. Graph showing the results of the radionuclide shunt study demonstrating impaired clearance of 99m Tc after injection of 0.34 mci of the isotope into the shunt reservoir (inset left), image obtained just after isotope injection). The percentage of 99m Tc remaining in the reservoir (solid circles) is graphed over time. For comparison, 99m Tc clearance from a normally functioning LP shunt is shown (dotted line). Minutes after tracer injection (inset right), partial retrograde flow is visible but there is no anterograde flow into the abdomen. visual fields showed peripheral constriction and enlarged blind spots in the visual fields of both eyes. Chronic papilledema and early optic atrophy were observed on fundus inspection. The results of the neurological examination were otherwise normal. First Operation and Postoperative Course. An LP shunt was placed without difficulty, employing a horizontal-vertical lumbar valve model # A with a horizontal valve closing pressure of 50 to 80 mm H 2 O and a vertical valve closing pressure of 230 to 320 mm H 2 O (Integra Neuro- Sciences). During laparoscopically guided insertion of the abdominal end of the catheter, multiple intraabdominal adhesions were noted, including one from the liver to the anterior abdominal wall. To avoid this adhesion, the catheter was placed closer than usual to the midline. Within a few days after surgery, the patient reported worsening headache, which required treatment with acetaminophen and hydrocodone. On the fifth day after surgery, an abdominal radiograph (Fig. 1) was obtained to assess the integrity of the shunt. The radiograph showed no evidence of shunt migration or disconnection. Two days later a radionuclide study was performed by injecting 99m Tc into the shunt reservoir. Dynamic imaging over the next 15 minutes showed no 99m Tc flow from the reservoir into the abdomen. Instead, there was reflux of tracer from the reservoir through the catheter toward the lumbar spine. The results of the study were interpreted as evidence of shunt obstruction between the reservoir and the abdomen, resulting from malfunction of the valve, blockage of the catheter tubing, or occlusion of the abdominal opening by one of the adhesions seen during shunt placement. Second Operation and Postoperative Course. Nine days after shunt placement the patient was taken back to the operating room. The flank incision was reopened to remove the reservoir and value. The free end of the lumbar catheter was placed in a dependent position, resulting in a slow trickle of CSF. From this observation it was concluded that the portion of the LP shunt from the lumbar spine to the shunt reservoir was functioning properly. A new reservoir and valve were installed, and the portion of the shunt from the valve to the peritoneal cavity was replaced. The free end of the catheter in the abdomen was noted by laparoscopy to be positioned satisfactorily. The patient was discharged from the hospital 5 days later, with limited improvement in her headache. Further Examination. A week later the patient was readmitted to the hospital because of worsening headache, which could not be controlled by hydromorphone and topiramate. Another 99m Tc shuntogram was performed (Fig. 2). As before, the study showed no anterograde flow from the reservoir to the abdomen. At this point, the pressure in the reservoir was measured directly with a manometer. The pressure was 0 to 4 mm H 2 O with the patient supine, and fell to 9 to 12 mm H 2 O when she sat up at a 45 angle. These values were unexpectedly low, alerting us to the possibility of intracranial hypotension. An MR imaging study of the brain showed bilateral subdural fluid collections (Fig. 3), supporting the diagnosis of postoperative intracranial hypotension. There was no evidence of an acquired Chiari malformation type I, a complication associated with LP shunts. 12 A spinal MR imaging study was performed to search for 2
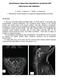
3 Intracranial hypotension after lumboperitoneal shunt placement FIG. 3. Coronal T2-weighted fluid-attenuated inversion recovery image showing bilateral subdural fluid collections over the convexities, consistent with intracranial hypotension following LP shunt placement. a leakage site. It demonstrated the expected course of the LP shunt catheter. The shunt pierced the dura mater dorsally, entered the subarachnoid space at the L2 3 level, and ascended parallel to the ventral aspect of the spinal cord. There was an epidural fluid collection located ventrally at the level of the LP shunt entry into the thecal sac (Fig. 4A and B). To pinpoint the locus of the apparent CSF leak, a CT myelogram was performed with injection of a contrast agent into the shunt reservoir. The injection led immediately to focal epidural extravasation of contrast material at the L2 3 level, with subsequent pooling of the contrast agent in the ventral epidural space (Fig. 4C and D). These imaging studies demonstrated the presence of a leak in the thecal sac at the level where the shunt was inserted, but the contrast material seemed to emanate from the ventral, rather than the dorsal, side of the thecal sac. It was unclear whether the leak arose from the actual catheter insertion site, located dorsally, or whether a separate hole was present in the ventral dura mater. Such a hole might have been caused by inadvertent puncture of the dura during the shunt insertion or by erosion of the catheter through the dura. In any event, the leakage of CSF and contrast agent seen on the spinal studies explained the patient s headache. It also explained the lack of 99m Tc clearance from the reservoir on both shunt studies. The leak reduced the pressure gradient for anterograde tracer flow from the reservoir to the abdomen. Additional Treatment and Posttreatment Course. To close the leak, a 15 cc blood patch was administered. The patient reported only transient improvement in her headache. Three days later the procedure was repeated with 28 cc of blood, again without permanent relief. These unsuccessful patches were applied at the bedside without the benefit of neuroradiological guidance. A third blood patch was applied, on FIG. 4. Neuroimages showing leakage of CSF from the lumbar thecal sac. A: A 5-mm-thick axial fast spin echo T2-weighted MR image through the lumbar spine revealing a CSF leak into the right ventral, extradural space (arrow) at the L2 3 level. B: The adjacent axial image (6 mm skip space) caudal to the image in A also shows collection of CSF in the epidural space (arrow). C: Sagittal CT myelographic image showing the catheter (arrowhead) entering the thecal sac at the L2 3 level and extending rostrally. An accumulation of contrast material, 12 cc of Omnipaque 240 (GE Healthcare) introduced via the reservoir, can be seen ventral to the thecal sac (arrow). D: Axial CT myelographic image showing the ventral, extradural CSF leak (between the arrow and the arrowhead). The LP shunt catheter appears as a circular bright object against the ventral dura mater. this occasion using CT to confirm that the needle was located in the L2 3 epidural space near the leak site (Fig. 5). The patch was delivered by injecting 5 cc of blood mixed with contrast agent. After the injection was made, CT images showed formation of a blood clot and compression of the thecal sac. The next day the patient reported nearly complete resolution of her headache. She was instructed to remain in bed for 2 days. Four days after application of the third blood patch she was discharged from the hospital in good condition. A year later the patient reported no recurrence of headache on a routine office visit. A neuroophthalmological examination showed no visual field loss or papilledema. Discussion Headache is a common symptom in patients with IIH who require LP shunt placement. Paradoxically, headache is also one of the most frequent symptoms experienced after surgery. 14 In a retrospective study involving 82 patients with IIH whose elevated ICP had been normalized by medication or surgery, 68% subsequently developed a new headache syndrome, consisting of episodic tension-type headache (30%), migraine without aura (20%), chronic tensiontype headache (10%), or analgesic overuse headache (8%). 7 In another retrospective study of 42 patients with surgically treated IIH, severe headache recurred in 48%, despite a properly functioning shunt. 13 These data suggest that patients with a history of IIH are predisposed to headache, even after successful placement of a LP shunt. 3
4 Y. J. Liao et al. FIG. 5. The CT-guided application of an epidural blood patch at the L2 3 level. The LP shunt catheter (arrowheads) can be seen lying ventrally in the subarachnoid space. A: Axial CT image showing the needle entering dorsolaterally. B: Axial CT image showing the injection of blood mixed with contrast medium (asterisk) into the epidural space. C: Axial CT image obtained after application of the blood patch shows that the thecal sac is compressed, with a concave dorsal border. Faced with the dilemma of a patient with postoperative headache, the neurosurgeon s main responsibility is to make sure that the LP shunt is functioning properly. Once infection has been excluded, the principal concerns are obstruction or excessive shunting. Any of these shunt complications can produce postoperative headache. In every case series, obstruction remains the most common cause of shunt failure. 2,4,6,11,15 The problem of excessive shunting has become less prevalent, owing to the routine use of valves with two pressure settings (for erect and recumbent postures). However, it can still occur, even when these devices are used. 8 A radionuclide shuntogram is useful to differentiate between obstruction and excessive shunting, but results must be interpreted cautiously because testing protocols, normal values, and rates of false positive or negative results vary widely among clinical centers. 16 It should also be emphasized that published data pertain almost exclusively to ventriculoperitoneal shunts, rather than LP shunts. In principle, overdrainage should be easy to recognize because of rapid clearance of the tracer from the shunt reservoir and early spillage into the abdominal cavity. However, tracer clearance can occur rapidly in a patient with a normally functioning shunt, especially if a large tracer volume is administered or the patient is crying or upright during the procedure. For this reason, a radionuclide study cannot always differentiate reliably between a shunt that is overdraining and one that is working properly. In our patient, the lack of anterograde flow of 99m Tc from the shunt reservoir to the abdomen in the first shuntogram was interpreted as evidence for shunt obstruction. Had distal obstruction been present, direct measurement of the pressure in the reservoir would have yielded an elevated reading. Unfortunately, we did not perform a pressure measurement because the results of the shuntogram convinced us that the shunt was obstructed. To our surprise, after replacement of the distal shunt apparatus, a follow-up shuntogram still showed no anterograde flow. At this point, the pressure in the reservoir was measured. The low-pressure reading altered our interpretation of the findings of the shunt study. A low pressure in the shunt reservoir without anterograde tracer flow is compatible with either shunt breakage or proximal obstruction between the lumbar region and the shunt reservoir. With proximal obstruction, little retrograde flow of tracer should occur from the shunt reservoir because the catheter is blocked. However, some degree of retrograde flow may be detected due to 99m Tc reflux into the catheter, especially if a large volume of tracer is injected under sufficient pressure. In our patient, proximal obstruction was deemed unlikely because CSF had been observed to trickle from the open end of the catheter when it was disconnected from the reservoir during the shunt revision procedure. A single prior case has been reported of a patient with severe postural headache following LP shunt placement, due to a probable CSF leak from the thecal sac. 1 Neuroimaging was not performed in that case, but the patient was treated empirically with a blood patch, resulting in immediate relief. We now report a second case, this time proving the existence of a CSF leak by neuroimaging. The complication of fluid leakage from the thecal sac probably occurs more often than realized after LP shunt placement, but it has probably been confused with a low-pressure syndrome resulting from excessive shunting. Wider recognition that a low-pressure syndrome can also occur from chronic leakage of CSF in the lumbar region may help avoid unnecessary shunt removal or revision. A simple blood patch can suffice to treat this complication. As we have shown, CT can facilitate the application of the blood patch to ensure that it is delivered to the actual leak site. After routine lumbar puncture, CSF continues to drain into the paraspinous area for several days before the dural puncture eventually seals. 10 In our patient, a 14-gauge Tuohy needle was used to pierce the dura and a 1.6-mm (outside diameter) catheter was threaded into the subarachnoid space. For the defect to close, a watertight seal must develop between the dura and the shunt catheter. Given this requirement, it is rather surprising that a permanent leak does not occur more commonly after LP shunt placement. The fact that the paraspinous area can absorb enough CSF to restore ICP to normal in patients with IIH raises the possibil- 4
5 Intracranial hypotension after lumboperitoneal shunt placement ity that in the future one might invent a controlled drainage device for implantation in the lumbar dura mater that does not require the shunting of fluid to the peritoneal cavity. Conclusions Leakage of CSF from the thecal sac into the epidural space can occur as a complication of LP shunt placement. This problem produces a low ICP syndrome that may be confused with the results of excessive shunting, or even obstruction. To accurately diagnose the condition, it is useful to combine a radionuclide shuntogram with direct measurement of CSF pressure. Both MR imaging and CT studies can also show the leak site in the thecal sac that is associated with the lumbar shunt catheter. References 1. Allmond LR, Stratmann G, Kunwar SM, Burkhardt DH: Epidural blood patch for headache after lumboperitoneal shunt placement. Anesth Analg 101: , Aoki N: Benign intracranial hypertension. Childs Nerv Syst 1: 243, Binder DK, Horton JC, Lawton MT, McDermott MW: Idiopathic intracranial hypertension. Neurosurgery 54: , Chumas PD, Kulkarni AV, Drake JM, Hoffman HJ, Humphreys RP, Rutka JT: Lumboperitoneal shunting: a retrospective study in the pediatric population. Neurosurgery 32: , Corbett JJ: The 1982 Silversides lecture. Problems in the diagnosis and treatment of pseudotumor cerebri. Can J Neurol Sci 10: , Eggenberger ER, Miller NR, Vitale S: Lumboperitoneal shunt for the treatment of pseudotumor cerebri. Neurology 46: , Friedman DI, Rausch EA: Headache diagnoses in patients with treated idiopathic intracranial hypertension. Neurology 58: , Garton HJ: Cerebrospinal fluid diversion procedures. J Neuroophthalmol 24: , Horton JC, Seiff SR, Pitts LH, Weinstein PR, Rosenblum ML, Hoyt WF: Decompression of the optic nerve sheath for visionthreatening papilledema caused by dural sinus occlusion. Neurosurgery 31: , Iqbal J, Davis LE, Orrison WW Jr: An MRI study of lumbar puncture headaches. Headache 35: , Johnston I, Besser M, Morgan MK: Cerebrospinal fluid diversion in the treatment of benign intracranial hypertension. J Neurosurg 69: , Karabatsou K, Quigley G, Buxton N, Foy P, Mallucci C: Lumboperitoneal shunts: are the complications acceptable? Acta Neurochir (Wien) 146: , McGirt MJ, Woodworth G, Thomas G, Miller N, Williams M, Rigamonti D: Cerebrospinal fluid shunt placement for pseudotumor cerebri-associated intractable headache: predictors of treatment response and an analysis of long-term outcomes. J Neurosurg 101: , Ramadan NM: Headache caused by raised intracranial pressure and intracranial hypotension. Curr Opin Neurol 9: , Rosenberg ML, Corbett JJ, Smith C, Goodwin J, Sergott R, Savino P, et al: Cerebrospinal fluid diversion procedures in pseudotumor cerebri. Neurology 43: , Vassilyadi M, Tataryn ZL, Matzinger MA, Briggs V, Ventureyra EC: Radioisotope shuntograms at the Children s Hospital of Eastern Ontario. Childs Nerv Syst 22:43 49, 2006 Manuscript submitted July 28, Accepted November 7, This work was supported in part by Grant No. K08 NS from the National Institute of Neurological Diseases and Stroke and a Career Award in Biomedical Sciences from the Burroughs Wellcome Foundation to Dr. Liao and by an unrestricted grant from Research to Prevent Blindness to Dr. Horton. Address reprint requests to: Jonathan C. Horton, M.D., Ph.D., Beckman Vision Center, 10 Koret Way, University of California San Francisco, San Francisco, California hortonj@ vision.ucsf.edu. 5
A New Mechanism of Cerebrospinal Fluid Leakage after Lumboperitoneal Shunt: A Theory of Shunt Side Hole Case Report
 Case Report Neurol Med Chir (Tokyo) xx, xxx xxx, 20xx doi: 10.2176/nmc.cr2013-0067 Online November 20, 2013 A New Mechanism of Cerebrospinal Fluid Leakage after Lumboperitoneal Shunt: A Theory of Shunt
Case Report Neurol Med Chir (Tokyo) xx, xxx xxx, 20xx doi: 10.2176/nmc.cr2013-0067 Online November 20, 2013 A New Mechanism of Cerebrospinal Fluid Leakage after Lumboperitoneal Shunt: A Theory of Shunt
Khalil Zahra, M.D Neuro-interventional radiology
 Khalil Zahra, M.D Neuro-interventional radiology 1 Disclosure None 2 Outline Etiology and pathogensis Imaging techniques and Features Literature review Treatment modalities Endovascular techniques Long
Khalil Zahra, M.D Neuro-interventional radiology 1 Disclosure None 2 Outline Etiology and pathogensis Imaging techniques and Features Literature review Treatment modalities Endovascular techniques Long
NANOS Patient Brochure
 NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
Occult Cerebrospinal Fluid Fistula between Ventricle and Extra-Ventricular Position of the Ventriculoperitoneal Shunt Tip
 197 Occult Cerebrospinal Fluid Fistula between Ventricle and Extra-Ventricular Position of the Ventriculoperitoneal Shunt Tip Ching-Yi Lee 1, Chieh-Tsai Wu 1, Kuang-Lin Lin 2, Hsun-Hui Hsu 3 Abstract-
197 Occult Cerebrospinal Fluid Fistula between Ventricle and Extra-Ventricular Position of the Ventriculoperitoneal Shunt Tip Ching-Yi Lee 1, Chieh-Tsai Wu 1, Kuang-Lin Lin 2, Hsun-Hui Hsu 3 Abstract-
Amin B. Kassam, MD. 1. Idiopathic Intracranial Hypertension 2. Ventriculoperitoneal Shunt 3. Lumboperitoneal Shunt 4. Lumbar Drain
 CSF SHUNTING PROCEDURES IN IDIOPATHIC INTRACRANIAL HYPERTENSION (IIH) Amin B. Kassam, MD The Ottawa Hospital Ottawa, Canada Learning Objectives 1. To become familiar with the different CSF shunting options
CSF SHUNTING PROCEDURES IN IDIOPATHIC INTRACRANIAL HYPERTENSION (IIH) Amin B. Kassam, MD The Ottawa Hospital Ottawa, Canada Learning Objectives 1. To become familiar with the different CSF shunting options
 Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
MOHAMED LOTFY, M.D.*; MOATAZ A. EL-AWADY, M.D.**; ASHRAF E. ZAGHLOUL, M.D.** and TAREK NEHAD, M.D.***
 Med. J. Cairo Univ., Vol. 84, No. 2, December: 301-306, 2016 www.medicaljournalofcairouniversity.net Effect of Therapeutic Lumbar Puncture on the Visual Outcome and the Further Need for Surgery in Patients
Med. J. Cairo Univ., Vol. 84, No. 2, December: 301-306, 2016 www.medicaljournalofcairouniversity.net Effect of Therapeutic Lumbar Puncture on the Visual Outcome and the Further Need for Surgery in Patients
Intracranial hypertension and headache. Daniel Tibussek, MD
 Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
What is IIH? Idiopathic Intracranial Hypertension (IIH)
 What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
Surgical treatments in severe IIH
 Surgical treatments in severe IIH You will have been told by your Doctor that you need to have a surgical procedure for Idiopathic Intracranial Hypertension. This may be because all the other treatments
Surgical treatments in severe IIH You will have been told by your Doctor that you need to have a surgical procedure for Idiopathic Intracranial Hypertension. This may be because all the other treatments
THE SWOLLEN DISC. Valerie Biousse, MD Emory University School of Medicine Atlanta, GA
 THE SWOLLEN DISC Valerie Biousse, MD Emory University School of Medicine Atlanta, GA Updated from: Neuro-Ophthalmology Illustrated. Biousse V, Newman NJ. Thieme, New-York,NY. 2 nd Ed, 2016. Edema of the
THE SWOLLEN DISC Valerie Biousse, MD Emory University School of Medicine Atlanta, GA Updated from: Neuro-Ophthalmology Illustrated. Biousse V, Newman NJ. Thieme, New-York,NY. 2 nd Ed, 2016. Edema of the
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings. Jonathan A. Micieli, MD Valérie Biousse, MD
 Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
National Hospital for Neurology and Neurosurgery
 National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
BMB Disclosures. Papilledema can be a. Neurological Emergency, Causing Preventable Blindness
 Reasonable Doubt: Can High Intracranial Pressure Occur Without Papilledema? 15 February 2013 Jonathan C. Horton hortonj@vision.ucsf.edu http://www.ucsf.edu/hortonlab BMB Disclosures Financial Disclosures
Reasonable Doubt: Can High Intracranial Pressure Occur Without Papilledema? 15 February 2013 Jonathan C. Horton hortonj@vision.ucsf.edu http://www.ucsf.edu/hortonlab BMB Disclosures Financial Disclosures
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Spontaneous Intracranial Hypotension Diagnosis and Treatment
 Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
 ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
ORIGINAL ARTICLE Year : 2015 Volume : 63 Issue : 5 Page : 707 711 Neuromodulation as a last resort option in the treatment of chronic daily headaches in patients with idiopathic intracranial hypertension
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Incidental durotomy during spine surgery occurs in. Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks
 J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
Management of Pseudo Tumor Cerebri by Frequent Tapping VS lumboperitoneal Shunt
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (5), Page 4556-4560 Management of Pseudo Tumor Cerebri by Frequent Tapping VS lumboperitoneal Shunt Ali K. Ali, Maamoun M. Abo Shousha, Mohammed
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (5), Page 4556-4560 Management of Pseudo Tumor Cerebri by Frequent Tapping VS lumboperitoneal Shunt Ali K. Ali, Maamoun M. Abo Shousha, Mohammed
Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections in Patients with Hydrocephalus
 The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
(Hi-dro-SEF-ah-lus) Hydrocephalus is a build-up of Cerebrospinal Fluid, or CSF within the spaces inside the brain, called ventricles.
 Hydrocephalus in adults What is hydrocephalus? (Hi-dro-SEF-ah-lus) Hydrocephalus is a build-up of Cerebrospinal Fluid, or CSF within the spaces inside the brain, called ventricles. There are 4 ventricles
Hydrocephalus in adults What is hydrocephalus? (Hi-dro-SEF-ah-lus) Hydrocephalus is a build-up of Cerebrospinal Fluid, or CSF within the spaces inside the brain, called ventricles. There are 4 ventricles
Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage
 DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
SURGICAL OUTCOME OF BENIGN INTRACRANIAL HYPERTENSION IN TERMS OF IMPROVEMENT IN VISION
 O R I G I N A L A R T I C L E SURGICAL OUTCOME OF BENIGN INTRACRANIAL HYPERTENSION IN TERMS OF IMPROVEMENT IN VISION Naeem ul haq 1, Naseer hassan 1, Muhammad ishaq 1,Muhammad usman 2 1Neurosurgery unit,
O R I G I N A L A R T I C L E SURGICAL OUTCOME OF BENIGN INTRACRANIAL HYPERTENSION IN TERMS OF IMPROVEMENT IN VISION Naeem ul haq 1, Naseer hassan 1, Muhammad ishaq 1,Muhammad usman 2 1Neurosurgery unit,
IDIOPATHIC INTRACRANIAL HYPERTENSION
 IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
Ventriculoperitoneal Shunt with Communicating Peritoneal & Subcutaneous Pseudocysts Formation
 International Journal of Health Sciences, Qassim University, Vol. 8, No. 1 (January-March 2014) Case Report Ventriculoperitoneal Shunt with Communicating Peritoneal & Subcutaneous Pseudocysts Formation
International Journal of Health Sciences, Qassim University, Vol. 8, No. 1 (January-March 2014) Case Report Ventriculoperitoneal Shunt with Communicating Peritoneal & Subcutaneous Pseudocysts Formation
Sabah Al-Rashed, Haider Kareem, Neeraj Kalra, Linda D Antona, Mouness Obeidat 1, Bhavesh Patel 1, Ahmed Toma 1
 RESEARCH ARTICLE Lumboperitoneal shunt insertion without fluoroscopy guidance: Accuracy of placement in a series of 107 procedures [version 2; referees: 3 approved] 1 2 2 1 Sabah Al-Rashed, Haider Kareem,
RESEARCH ARTICLE Lumboperitoneal shunt insertion without fluoroscopy guidance: Accuracy of placement in a series of 107 procedures [version 2; referees: 3 approved] 1 2 2 1 Sabah Al-Rashed, Haider Kareem,
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA)
 Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
UNDERSTANDING HYDROCEPHALUS
 UNDERSTANDING HYDROCEPHALUS Offering solutions for patients. 1 UNDERSTANDING HYDROCEPHALUS Dear Reader: Your doctor has either recommended the CODMAN HAKIM Precision Fixed Pressure Valve, the CODMAN HAKIM
UNDERSTANDING HYDROCEPHALUS Offering solutions for patients. 1 UNDERSTANDING HYDROCEPHALUS Dear Reader: Your doctor has either recommended the CODMAN HAKIM Precision Fixed Pressure Valve, the CODMAN HAKIM
The headache profile of idiopathic intracranial hypertension
 The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Sudden Headache and visual disturbances in a young woman
 Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Shunt malfunction and Slight edema surrounding the ventricles: Ten case series
 ISSN: 47-5 Volume Number 8 (August-04) pp. 4-45 www.ijcrar.com Shunt malfunction and Slight edema surrounding the ventricles: Ten case series Firooz Salehpoor, Arastoo Pezeshki, Amirhossein Haghir *, Aidin
ISSN: 47-5 Volume Number 8 (August-04) pp. 4-45 www.ijcrar.com Shunt malfunction and Slight edema surrounding the ventricles: Ten case series Firooz Salehpoor, Arastoo Pezeshki, Amirhossein Haghir *, Aidin
Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch
 J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series
 CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
While some patients with SIH recover without intervention
 ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
Coexistence of migraine and idiopathic intracranial hypertension without papilledema
 / GX'~C1~.. Coexistence of migraine and idiopathic intracranial hypertension without papilledema Ninan T. Mathew, MD; K. Ravishankar, MD; and Luis C. Sanin, MD!
/ GX'~C1~.. Coexistence of migraine and idiopathic intracranial hypertension without papilledema Ninan T. Mathew, MD; K. Ravishankar, MD; and Luis C. Sanin, MD!
Lumbar drains. Information for patients Neurosurgery
 Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
BMI Medical. Ventricular Catheter T
 Shunting System Ventricular Catheter 01101 01101T Barium-impregnated silicone catheter provides resistance to kinking and compression. Stainless steel stylet allows catheter to be directed during catheter
Shunting System Ventricular Catheter 01101 01101T Barium-impregnated silicone catheter provides resistance to kinking and compression. Stainless steel stylet allows catheter to be directed during catheter
LV-EBP: Record-setting large volume epidural blood patch
 LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
A Case of Stent Placement for Intracranial Hypertension Associated with Venous Sinus Stenosis
 DOI: 10.5797/jnet.cr.2016-0080 A Case of Stent Placement for Intracranial Hypertension Associated with Venous Sinus Stenosis Rei Yamaguchi, Koji Sato, Hiroya Fujimaki, and Ken Asakura Objective: We encountered
DOI: 10.5797/jnet.cr.2016-0080 A Case of Stent Placement for Intracranial Hypertension Associated with Venous Sinus Stenosis Rei Yamaguchi, Koji Sato, Hiroya Fujimaki, and Ken Asakura Objective: We encountered
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Managing life with neurological symptoms
 Managing life with neurological symptoms Petra M Klinge Professor of Neurosurgery Director, Division of Pediatric Neurosurgery Director, CSF center of the brain and Spine Rhode Island Hospital and Hasbro
Managing life with neurological symptoms Petra M Klinge Professor of Neurosurgery Director, Division of Pediatric Neurosurgery Director, CSF center of the brain and Spine Rhode Island Hospital and Hasbro
Body position and eerebrospinal fluid pressure. Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point
 Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Hydrocephalus 1/16/2015. Hydrocephalus. Functions of Cerebrospinal fluid (CSF) Flow of CSF
 Hydrocephalus Hydrocephalus Ruth Arms, MSN, CNS-BC, SCRN Hydrocephalus is the buildup of fluid in the cavities (ventricles) deep within the brain. The excess fluid increases the size of the ventricles
Hydrocephalus Hydrocephalus Ruth Arms, MSN, CNS-BC, SCRN Hydrocephalus is the buildup of fluid in the cavities (ventricles) deep within the brain. The excess fluid increases the size of the ventricles
Clinical Study Endoscopic Third Ventriculostomy in Previously Shunted Children
 Minimally Invasive Surgery Volume 2013, Article ID 584567, 4 pages http://dx.doi.org/10.1155/2013/584567 Clinical Study Endoscopic Third Ventriculostomy in Previously Shunted Children Eva Brichtova, 1
Minimally Invasive Surgery Volume 2013, Article ID 584567, 4 pages http://dx.doi.org/10.1155/2013/584567 Clinical Study Endoscopic Third Ventriculostomy in Previously Shunted Children Eva Brichtova, 1
Radiological evaluation of ventriculoperitoneal shunt systems
 Radiological evaluation of ventriculoperitoneal shunt systems Poster No.: C-702 Congress: ECR 2009 Type: Educational Exhibit Topic: Neuro Authors: T. Rodt, C. von Falck, C. Tschan, M. Diensthuber, J. Zajaczek,
Radiological evaluation of ventriculoperitoneal shunt systems Poster No.: C-702 Congress: ECR 2009 Type: Educational Exhibit Topic: Neuro Authors: T. Rodt, C. von Falck, C. Tschan, M. Diensthuber, J. Zajaczek,
Dural venous sinus angioplasty and stenting for the treatment of idiopathic intracranial hypertension
 1 Department of Interventional Neuroradiology, Oregon Health and Science University, Portland, Oregon, USA 2 School of Medicine, Oregon Health and Science University, Portland, Oregon, USA 3 Department
1 Department of Interventional Neuroradiology, Oregon Health and Science University, Portland, Oregon, USA 2 School of Medicine, Oregon Health and Science University, Portland, Oregon, USA 3 Department
HIROSHI NAKAGUCHI, M.D., PH.D., TAKEO TANISHIMA, M.D., PH.D., Clinical Material and Methods
 J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
ASJ. Spinal Intradural Hematoma and Permanent Paraparesis after a Lumboperitoneal Shunt Operation: An Unusual Complication. Asian Spine Journal
 Asian Spine Journal 516 Recep Basaran Case Report et al. http://dx.doi.org/10.4184/asj.2014.8.4.516 Spinal Intradural Hematoma and Permanent Paraparesis after a Lumboperitoneal Shunt Operation: An Unusual
Asian Spine Journal 516 Recep Basaran Case Report et al. http://dx.doi.org/10.4184/asj.2014.8.4.516 Spinal Intradural Hematoma and Permanent Paraparesis after a Lumboperitoneal Shunt Operation: An Unusual
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Efficacy of Lumboperitoneal Shunting in Patients with Normal Pressure Hydrocephalus
 DOI: 10.5137/1019-5149.JTN.18702-16.1 Received: 17.08.2016 / Accepted: 17.09.2016 Published Online: 14.11.2016 Turk Neurosurg 28(1):62-66, 2018 Original Investigation Efficacy of Lumboperitoneal Shunting
DOI: 10.5137/1019-5149.JTN.18702-16.1 Received: 17.08.2016 / Accepted: 17.09.2016 Published Online: 14.11.2016 Turk Neurosurg 28(1):62-66, 2018 Original Investigation Efficacy of Lumboperitoneal Shunting
Use of scanning laser ophthalmoscopy to monitor papilloedema in idiopathic intracranial hypertension
 Br J Ophthalmol 998;8:35 3 Ophthalmology, Royal Victoria Hospital, Belfast D A Mulholland S J A Rankin Neurology, Royal Victoria Hospital, Belfast J J Craig Correspondence to: Mr David A Mulholland, Ophthalmology,
Br J Ophthalmol 998;8:35 3 Ophthalmology, Royal Victoria Hospital, Belfast D A Mulholland S J A Rankin Neurology, Royal Victoria Hospital, Belfast J J Craig Correspondence to: Mr David A Mulholland, Ophthalmology,
Mechanisms of Headache in Intracranial Hypotension
 Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
I diopathic intracranial hypertension (IIH) is an uncommon
 1662 PAPER Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting J N P Higgins, C Cousins, B K Owler, N Sarkies, J D Pickard... See end of article for authors affiliations...
1662 PAPER Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting J N P Higgins, C Cousins, B K Owler, N Sarkies, J D Pickard... See end of article for authors affiliations...
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Idiopathic Intracranial Hypertension (Pseudotumor Cerebri) David I. Kaufman, D.O. Michigan State University Department of Neurology and Ophthalmology
 Idiopathic Intracranial Hypertension (Pseudotumor Cerebri) David I. Kaufman, D.O. Michigan State University Department of Neurology and Ophthalmology 26 year old 5 3, 300 pound female with papilledema,
Idiopathic Intracranial Hypertension (Pseudotumor Cerebri) David I. Kaufman, D.O. Michigan State University Department of Neurology and Ophthalmology 26 year old 5 3, 300 pound female with papilledema,
Adult hydrocephalus and shunts. Information for patients
 Adult hydrocephalus and shunts Information for patients Contents What is hydrocephalus? 3 Causes 4 Symptoms 4 What is hydrocephalus? Hydrocephalus is a condition in which cerebrospinal fluid (CSF) builds
Adult hydrocephalus and shunts Information for patients Contents What is hydrocephalus? 3 Causes 4 Symptoms 4 What is hydrocephalus? Hydrocephalus is a condition in which cerebrospinal fluid (CSF) builds
NEUROSURGEON VS. HOSPITALIST Pediatric Hospital Medicine meeting Nashville, TN July 21, 2017*±
 NEUROSURGEON VS. HOSPITALIST Pediatric Hospital Medicine meeting Nashville, TN July 21, 2017*± *no pediatricians were harmed in the making of this presentation ±nonetheless, please do not try this at home
NEUROSURGEON VS. HOSPITALIST Pediatric Hospital Medicine meeting Nashville, TN July 21, 2017*± *no pediatricians were harmed in the making of this presentation ±nonetheless, please do not try this at home
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
In patients with idiopathic intracranial hypertension
 Neurosurg Focus 37 (5):E4, 2014 AANS, 2014 A comparison of lumboperitoneal and ventriculoperitoneal shunting for idiopathic intracranial hypertension: an analysis of economic impact and complications using
Neurosurg Focus 37 (5):E4, 2014 AANS, 2014 A comparison of lumboperitoneal and ventriculoperitoneal shunting for idiopathic intracranial hypertension: an analysis of economic impact and complications using
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Literature Review: Neurosurgery
 NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
NEURO QUIZ 45 EHLERS DANLOS SYNDROME
 NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
Evaluation of CSF Shunt Function: Value of Functional Examination with Contrast Material
 143 Evaluation of CSF Shunt Function: Value of Functional Examination with Contrast Material Edward C. Benzel 1 Mansour Mirfakhraee 2 Theresa A. Hadden 1 Functional positive-contrast shuntography includes
143 Evaluation of CSF Shunt Function: Value of Functional Examination with Contrast Material Edward C. Benzel 1 Mansour Mirfakhraee 2 Theresa A. Hadden 1 Functional positive-contrast shuntography includes
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Case Report Pneumocephalus Associated with Cerebrospinal Fluid Fistula as a Complication of Spinal Surgery: A Case Report
 Case Reports in Medicine Volume 2010, Article ID 328103, 4 pages doi:10.1155/2010/328103 Case Report Pneumocephalus Associated with Cerebrospinal Fluid Fistula as a Complication of Spinal Surgery: A Case
Case Reports in Medicine Volume 2010, Article ID 328103, 4 pages doi:10.1155/2010/328103 Case Report Pneumocephalus Associated with Cerebrospinal Fluid Fistula as a Complication of Spinal Surgery: A Case
The Behavior of Pantopaque on MR: In Vivo and In Vitro
 997 The Behavior of Pantopaque on MR: In Vivo and In Vitro Analyses Ira F. Braun 1 John A. Maiko Patricia C. Davis James C. Hoffman, Jr. Louis H. Jacobs MR imaging is considered by many to be the procedure
997 The Behavior of Pantopaque on MR: In Vivo and In Vitro Analyses Ira F. Braun 1 John A. Maiko Patricia C. Davis James C. Hoffman, Jr. Louis H. Jacobs MR imaging is considered by many to be the procedure
Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat with minimal invasive surgery
 Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Infusion studies in clinical practice. Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London
 Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Differential Diagnosis of Orthostatic Headache
 Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Anesthetic Management of Laparoscopic Surgery for a Patient with
 Anesthetic Management of Laparoscopic Surgery for a Patient with a Ventriculoperitoneal shunt Abstract With the advances in the management of hydrocephalus, patients with ventriculoperitoneal shunt are
Anesthetic Management of Laparoscopic Surgery for a Patient with a Ventriculoperitoneal shunt Abstract With the advances in the management of hydrocephalus, patients with ventriculoperitoneal shunt are
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Intracranial Hypotension Concurrent Presented with Pseudo-Subarachnoid Hemorrhage and Transverse Sinus Thrombosis: A Case Report
 NNQ Intracranial Hypotension Concurrent Presented with Pseudo-Subarachnoid Hemorrhage and Transverse Sinus Thrombosis: A Case Report Chieh-Yang Cheng 1, Che-Chuan Wang 1, Tai-Yuan Chen 2, Jinn-Rung Kuo
NNQ Intracranial Hypotension Concurrent Presented with Pseudo-Subarachnoid Hemorrhage and Transverse Sinus Thrombosis: A Case Report Chieh-Yang Cheng 1, Che-Chuan Wang 1, Tai-Yuan Chen 2, Jinn-Rung Kuo
In some patients with pituitary macroadenoma, visual acuity
 ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
Chapter IV: Percutaneous Puncture of Spinal Cord Cysts
 Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
MR imaging the post operative spine - What to expect!
 MR imaging the post operative spine - What to expect! Poster No.: C-2334 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Jain, M. Paravasthu, M. Bhojak, K. Das ; Warrington/UK, 1 1 1 2 1 2 Liverpool/UK
MR imaging the post operative spine - What to expect! Poster No.: C-2334 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Jain, M. Paravasthu, M. Bhojak, K. Das ; Warrington/UK, 1 1 1 2 1 2 Liverpool/UK
Spontaneous Intracranial Hypotension Syndrome in a Patient With Marfan Syndrome and Autosomal Dominant Polycystic Kidney Disease
 632 April 2008 secondary causes of intracranial hypertension can be lifethreatening. Review of the imaging studies by an experienced neuro-radiologist is of paramount importance. Low threshold for repeat
632 April 2008 secondary causes of intracranial hypertension can be lifethreatening. Review of the imaging studies by an experienced neuro-radiologist is of paramount importance. Low threshold for repeat
Lumbar cistern is site of lumbar puncture for removal of CSF sample LC contains cauda equina. Anatomical Review
 Lumbar Puncture Lumbar cistern is site of lumbar puncture for removal of CSF sample LC contains cauda equina Anatomical Review Anatomical review Overview An LP (lumbar puncture) is an invasive diagnostic
Lumbar Puncture Lumbar cistern is site of lumbar puncture for removal of CSF sample LC contains cauda equina Anatomical Review Anatomical review Overview An LP (lumbar puncture) is an invasive diagnostic
Intradural Spinal Vein Enlargement in Craniospinal Hypotension
 AJNR Am J Neuroradiol 26:34 38, January 2005 Case Report Intradural Spinal Vein Enlargement in Craniospinal Hypotension M. Todd Burtis, John L. Ulmer, Glenn A. Miller, Alexandru C. Barboli, Scott A. Koss,
AJNR Am J Neuroradiol 26:34 38, January 2005 Case Report Intradural Spinal Vein Enlargement in Craniospinal Hypotension M. Todd Burtis, John L. Ulmer, Glenn A. Miller, Alexandru C. Barboli, Scott A. Koss,
Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities
 DOI 10.1007/s10072-013-1364-2 BRIEF COMMUNICATION Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities Angelo Franzini G. Messina L. Chiapparini G.
DOI 10.1007/s10072-013-1364-2 BRIEF COMMUNICATION Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities Angelo Franzini G. Messina L. Chiapparini G.
Total improvement after surgery for obstructive sleep apnea syndrome in a patient with concurrent malignant idiopathic intracranial hypertension
 CASE REPORT Total improvement after surgery for obstructive sleep apnea syndrome in a patient with concurrent malignant idiopathic intracranial hypertension Halil Onder, MD, 1 Onur Ergun, MD, 2 Mehmet
CASE REPORT Total improvement after surgery for obstructive sleep apnea syndrome in a patient with concurrent malignant idiopathic intracranial hypertension Halil Onder, MD, 1 Onur Ergun, MD, 2 Mehmet
Intracranial Hypotension: The Duke Experience
 Intracranial Hypotension: The Duke Experience SATURDAY, MARCH 23, 2019 7:30 A.M. TO 12:15 P.M. RENAISSANCE RALEIGH NORTH HILLS HOTEL Course Director: Linda Gray Leithe, MD Space is limited, and registration
Intracranial Hypotension: The Duke Experience SATURDAY, MARCH 23, 2019 7:30 A.M. TO 12:15 P.M. RENAISSANCE RALEIGH NORTH HILLS HOTEL Course Director: Linda Gray Leithe, MD Space is limited, and registration
Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
Glossary. Working to relieve the pressure!
 A Acetazolamide - see Diamox Amitriptyline - a drug which is used in low dosage in IIH to treat some of the symptoms of the condition. Analgesic - a drug used to relieve pain, often referred to as painkillers.
A Acetazolamide - see Diamox Amitriptyline - a drug which is used in low dosage in IIH to treat some of the symptoms of the condition. Analgesic - a drug used to relieve pain, often referred to as painkillers.
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Two Cases of Secondary Intracranial Hypotension
 online ML Comm CASE REPORT J Korean Neurotraumatol Soc 2011;7:103-107 ISSN 1738-8708 Two Cases of Secondary Intracranial Hypotension Yong-Sang Kim, MD, Byung Moon Cho, MD, Sung-Min Cho, MD, Se-Hyuck Park,
online ML Comm CASE REPORT J Korean Neurotraumatol Soc 2011;7:103-107 ISSN 1738-8708 Two Cases of Secondary Intracranial Hypotension Yong-Sang Kim, MD, Byung Moon Cho, MD, Sung-Min Cho, MD, Se-Hyuck Park,
Management of Symptomatic Sacral Perineural Cysts
 Management of Symptomatic Sacral Perineural Cysts Jianqiang Xu 1, Yongdong Sun 1, Xin Huang 1, Wenzhong Luan 2 * 1 Department of Neurosurgery, General Hospital of Fengfeng Group, Handan, China, 2 Department
Management of Symptomatic Sacral Perineural Cysts Jianqiang Xu 1, Yongdong Sun 1, Xin Huang 1, Wenzhong Luan 2 * 1 Department of Neurosurgery, General Hospital of Fengfeng Group, Handan, China, 2 Department
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Case Report Ventriculoperitoneal Shunt Peritoneal Catheter Knot Formation
 Case Reports in Neurological Medicine Volume 2013, Article ID 628493, 4 pages http://dx.doi.org/10.1155/2013/628493 Case Report Ventriculoperitoneal Shunt Peritoneal Catheter Knot Formation Anwar Ul-Haq,
Case Reports in Neurological Medicine Volume 2013, Article ID 628493, 4 pages http://dx.doi.org/10.1155/2013/628493 Case Report Ventriculoperitoneal Shunt Peritoneal Catheter Knot Formation Anwar Ul-Haq,
Eldor Epidural Kit (CSEN 68) Epidural catheter technique
 Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
