Deep brain stimulation (DBS) is FDA approved for. Streamlining deep brain stimulation surgery by reversing the staging order
|
|
|
- Amice McCarthy
- 6 years ago
- Views:
Transcription
1 technical note J Neurosurg 122: , 2015 Streamlining deep brain stimulation surgery by reversing the staging order Craig G. van Horne, MD, PhD, 1,2 Scott W. Vaughan, DO, 1 Carla Massari, MS, 1 Michael Bennett, PA-C, MS, 1 Wissam S. Z. Asfahani, MD, 2 Jorge E. Quintero, PhD, 2 and Greg A. Gerhardt, PhD 2 1 Department of Neurosurgery, St. Elizabeth s Medical Center, Brighton, Massachusetts; and 2 Department of Neurosurgery, University of Kentucky, Lexington, Kentucky Deep brain stimulation (DBS) is approved for several clinical indications; however, the sequencing of DBS surgery and the timeline for implementing stimulation therapy are not standardized. In over 140 cases so far, the authors have reversed the sequencing for staged implantation of DBS systems that was conducive to minimizing patient anxiety and discomfort while providing the opportunity to shorten the time between implantation and programming for therapeutic management of symptoms. Stage I was performed with the patient under general anesthesia and consisted of implantation of the pulse generator and lead extensions and placement of the bur holes. Stage II was completed 1 7 days later, using only local anesthesia, and included stereotactic frame-based microelectrode recordings, semi-microstimulation and macrostimulation, and testing and placement of the stimulating electrodes. Stage I lasted approximately 90 minutes, whereas Stage II lasted approximately 230 minutes. All patients tolerated the procedures and received a complete implanted system. Deep brain stimulation therapy was typically initiated on the same day as lead implantation. When sequencing was reversed and bur holes were placed during the first stage while a patient was under general anesthesia, the patient was able to tolerate the second awake stage and was able to begin stimulation therapy within 48 hours of the second stage. Key Words deep brain stimulation; neuronavigation; anesthesia; functional neurosurgery Deep brain stimulation (DBS) is FDA approved for several clinical indications, including Parkinson s disease, essential tremor, and dystonia. Additional investigational applications, such as obsessive-compulsive disorder, dementia, depression, and obesity, are on the horizon for widespread clinical practice. 3,5,9 Appropriate DBS therapy involves proper patient evaluation and selection; surgical intervention; and device programming initiation, adjustment, and readjustment. Currently, there is no standard protocol for the timing, staging, or sequencing of these procedures. Although some neurosurgeons elect to perform all components of the surgery in 1 day, a recent survey indicates that 87% of North American and 34% of European DBS surgeries are performed in multiday stages. 1 Deep brain stimulation system implantations are performed in stages, in part to decrease the patient s time in surgery and, to some extent in the US, for reimbursement considerations. 8 Staged procedures can be performed in 2, 3, or as many as 4 separate surgeries. 1,2,6 8 Thus, in the most protracted scenario, patients undergo 2 surgeries while under general anesthesia, 2 stereotactic frame placements, and 2 awake surgeries. Meanwhile, the effi- Abbreviations CRW = Cosman-Roberts-Wells; DBS = deep brain stimulation. submitted April 2, accepted September 10, include when citing Published online March 6, 2015; DOI: / JNS Disclosure The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Dr. van Horne is a consultant for Medtronic. Support was provided in part by University of Kentucky start-up funds (C.vH.) and the National Center for Advancing Translational Sciences (Grant No. UL1TR000117). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH J Neurosurg Volume 122 May 2015 AANS, 2015
2 Reversed staging deep brain stimulation surgery cacy of the procedure and therapy may not be determined, sometimes for weeks after surgery, until the stimulator is activated and programming is initiated. The most common feature of the staging is the sequencing, in which the awake procedure for DBS lead placement is performed first, followed days to weeks later by pulse generator implantation under general anesthesia. Although many factors play a role in the specifics of the process, the precise sequencing and timing are ultimately determined by the attending neurosurgeon. Based on feedback from patients and clinicians, we critically reviewed the technical aspects of the complete procedure and designed several changes to the process. Our major goals focused on improving the patient experience and optimizing opportunities for ensuring successful DBS lead placement. The most substantial change was the reordering of the typical sequence of the two surgeries; that is, instead of performing the awake procedure and DBS lead placement followed by pulse generator placement under general anesthesia, we reversed the stages. Implementing this reversal required novel approaches to some of the surgical techniques. The specific details of the modifications and implications in a series of patients who underwent DBS surgery at our institutions are presented in this paper. Methods Patients Over 140 patients to date (Table 1), ranging in age from 21 to 81 years, have been treated via reversed staging DBS surgery for Parkinson s disease, dystonia, essential tremor, or tremor due to multiple sclerosis. Each patient was evaluated by a movement disorder neurology team and was deemed a good candidate for DBS therapy in accordance with standard criteria. 4 Reversed staging for DBS has now been adapted at our institution as the standard of care. Materials Soletra, Kinetra, or Activa (Medtronic Inc.) pulse generators were unilaterally or bilaterally implanted in conjunction with lead extensions (model number 7482/7483, Medtronic Inc.) and stimulating electrode leads (model number 3387, Medtronic Inc.). Although for the first several patients we initially used the Navigus StimLoc hardware (Medtronic Inc.) to stabilize and secure the stimulating lead at the bur hole, we subsequently developed a low-profile method that utilizes the following: Hydroset (Stryker), a rapid-setting calcium phosphate cement; a 2-hole titanium adaptation plate TABLE 1. Diagnoses in patients who underwent DBS surgery, across 2 institutions Disease Institution 1 Institution 2 Parkinson s disease Essential tremor 8 33 Dystonia 2 6 Multiple sclerosis 1 0 Total (Synthes) along with 2 titanium cranial screws; and the lead end of the lead-extension connector boot (Medtronic Inc.) or, alternatively, a 1-cm segment of a large ventricular catheter ( , Codman). Brainlab intraoperative workstation and neuronavigation software (VectorVision2 and IPlanStereotaxy) were used for frameless stereotactic planning and targeting for bur hole placements as well as for frame-based targeting of the microelectrode recording trajectories. The Cosman- Roberts-Wells (CRW) stereotactic frame (Integra) was used for microelectrode and DBS lead targeting. Intraoperative microelectrode recordings were performed with the Alpha Omega system (Israel), Leadpoint (Medtronic Inc.), or Guideline 4000LP+ (FHC Inc.) workstations using microelectrodes (FHC Inc.). Description of Surgical Technique Stage I Our first-stage surgery is a preparatory procedure performed with the patient under general anesthesia. This stage consists of placing the pulse generator in a subclavicular pocket, tunneling and connecting lead extensions to the pulse generator, and creating unilateral or bilateral frontal bur holes. Several days or weeks before surgery, patients undergo outpatient noncontrast MRI. We use preoperative neuronavigational planning to determine the entry point for each lead, allowing appropriate placement for the skin incisions and the bur hole locations. Using neuronavigation software, we select targets for the DBS leads according to standard criteria. Corresponding trajectories are chosen and typically course close to the coronal suture, through a cortical gyrus to avoid the sulcal vasculature, and lateral to the lateral ventricle. The trajectory of the lead is surface matched using Z-touch and Softouch (Brainlab) and marked as the center at which the bur hole should be formed. An incision is then created in the postauricular area just above and behind the mastoid to facilitate tunneling. The extension leads (60 cm) are tunneled from the infraclavicular incision to the postauricular incision using the provided tunneler. The distal ends of the extension leads are then tunneled under the galea to the frontal incisions, capped, and tucked in the subgaleal space, where they will be accessible during the Stage II surgery (Fig. 1). All incisions are closed and sterile bandages are applied. A variation for the tunneling involves the use of a single 10-Fr (3.3 mm) Rob-Nel red rubber catheter, cut in 2 segments and trimmed to length, as a conduit system from the bur hole regions to the postauricular connector incision to pass the proximal end of the DBS leads under the scalp to the connector end of the lead extensions. We label the conduits at the site of the lead extension to permit accurate connection to the proximal DBS leads in Stage II. This technique allows the use of shorter extension leads and leaves extension lead connectors in the retroauricular area. Stage I is scheduled as an outpatient procedure. Although most patients go home the same day, some patients may be admitted for 24-hour observation and then discharged the following morning, depending on clinical indications. J Neurosurg Volume 122 May
3 C. G. van Horne et al. Fig. 1. Stage I surgery is performed with the patient under general anesthesia and involves the placement of bilateral frontal bur holes, subgaleal tunneling of the lead extensions to the coronal incision sites, and implantation of the pulse generator. Copyright University of Kentucky Analytics and Technologies. Published with permission. Figure is available in color online only. Stage II The second stage is performed within 3 7 days following the Stage I procedure. The second stage has been performed the following day in some patients for whom long distance travel was a significant factor. This stage focuses on the placement of DBS leads into the desired targets and is performed after applying a local anesthetic to allow microelectrode recording, test stimulation of DBS leads, and patient examination. On the morning of surgery in the preoperative area, a CRW frame is placed on the patient after a local anesthetic has been administered. A CT scan with the CRW localizer is obtained and fused with the MRI targeting data using the surgical planning software. The stereotactic coordinates of the targets are obtained and confirmed from the neuronavigation software, and the trajectory is adjusted, if necessary, to pass through the bur hole and a cortical gyrus while avoiding the sulcal vasculature and ventricle walls. Once in the operating room, patients receive intravenous Tylenol as an analgesic and, if needed, a Cardene drip for blood pressure control. No sedation is given. The previously created frontal incision is reopened after the injection of a local anesthetic, the dura mater is opened, and microelectrode recordings are obtained through the targeted trajectory. Microstimulation is performed, and the patient is tested for clinical benefit and stimulation side effects. When clinically satisfactory results have been obtained, a DBS lead is inserted into the appropriate area and tested for impedance performance as well as for clinical benefit and side effect profiling. After a satisfactory assessment, the lead is then secured and connected to the lead extension. As the proximal end of the extension leads are pretunneled to the frontal incision sites during Stage I, the extensions are easily found in the subgaleal space. To secure the lead, a small piece of Durepair (Medtronic, Inc.) is cut to the size of the bur hole and is placed around the lead on top of the dura. The bur hole is filled with Hydroset bone cement, which is then allowed to harden (approximately 3 minutes). The DBS lead is then secured to the underlying skull using a pre-bent 2-hole titanium plate and screws. A small piece of ventricular catheter or the lead end of the lead-extension connector boot is cut and opened lengthwise to serve as a protective sleeve around the lead at the site of contact with the titanium plate (Fig. 2). In our initial cases, we used red rubber conduits that were placed in the subgaleal space running from each bur hole to the connector incision. The conduits were then used to guide the distal end of the secured DBS leads from the bur holes to the connectors during Stage II, obviating the need for tunneling while the patient is awake. Conduits 1044 J Neurosurg Volume 122 May 2015
4 Reversed staging deep brain stimulation surgery Fig. 2. In the Stage II surgery, while the patient is awake, the DBS distal leads are positioned at the desired target and secured to create a lower profile. The proximal portions of the leads are connected to the lead extensions implanted in Stage I. In turn, the use of conscious sedation is avoided. Copyright University of Kentucky Analytics and Technologies. Published with permission. Figure is available in color online only. were removed prior to connecting the proximal end of the DBS lead to the lead extensions. At the conclusion of Stage II, the patient is removed from the CRW frame, transported to the postanesthesia care unit for recovery, and admitted overnight for observation. Postoperative CT scanning is performed to verify targeting and assess the possibility of pneumocephalus or hemorrhage. Results For the initial 31 patients, we noted that the Stage I surgery lasted approximately 90 minutes from incision to closing, whereas Stage II lasted approximately 230 minutes. The timing of subsequent surgeries agreed with these measurements. Nearly all patients were discharged within 48 hours of implantation. In our series, none of the attempted electrode placements had to be aborted because of technical difficulties or patient intolerability, and complete systems were implanted in all patients. We found no infections of the red rubber catheters or scarring around the proximal connector that interfered with placement of the DBS electrode. One patient developed a liver abscess, discovered on preoperative evaluation before his second-stage surgery. Thus, his second stage was postponed, and he was treated for the infection. As the infection was remote from the hardware, his system remained in place, and bilateral stimulating electrodes were successfully implanted several months later. Nearly all patients underwent initial programming of their stimulator systems during the postoperative hospital stay. Initial configurations were chosen based on intraoperative results and clinical tolerance. Medications were adjusted according to clinical need. We have not observed any significant adverse events related to early stimulation. Discussion The conventional approach to DBS surgery involves microelectrode recordings and placement of the DBS leads using conscious sedation and local anesthesia during the first stage, followed by a second stage in which the pulse generator and lead extensions are implanted while the patient is under general anesthesia. Traditionally, staging has depended on surgeon preference, the surgical center, and the number of devices implanted. Rather than making a claim that our reversed-stages procedural modification is superior to the conventional staging approach, we have outlined details on the new approach to provide an additional option for surgical DBS teams to consider. J Neurosurg Volume 122 May
5 C. G. van Horne et al. One potential criticism of the technique is that the pulse generator and lead extensions are implanted before the stimulating leads are placed, and a problem could arise that would prevent final placement of the leads, rendering the implanted system nonfunctional. We have found that this risk is very low given that we have used this staging sequence in over 140 cases without having to abandon placement of the stimulating electrodes. Additionally, advances in target visualization, target computation, and electrophysiological analysis have significantly improved the success rate of intraoperative target localization and stimulation electrode placement. Therefore, we do not believe that there is a substantial downside to implanting the pulse generator and lead extensions first. Conversely, we have encountered several patients from other centers at our clinic who have decided to not undergo the second stimulating electrode implantation, citing the anxiety and discomfort created by the experience of the bur hole drilling. In the protocol described here, patients undergo the targeting MRI without a frame before the preoperative visit. Acquiring images in advance of the preoperative visit allows ample time for review to confirm image quality and to determine that there are no extenuating anatomical or pathological circumstances. In addition, having the MRI studies at that point allows adequate surgical planning for target location and trajectory placement. Furthermore, on the day of the Stage I surgery, only a CT scan is required after frame placement, which facilitates operating room workflow and creates less stress for the patient. Patients also undergo bur hole placement under general anesthesia during Stage I, which has several advantages. First, patients do not have to experience drilling during the awake portion of the procedure. During conventionally staged procedures, a short-acting anesthetic or conscious sedation is used and then reversed after the bur hole is placed. Nevertheless, several patients treated at our clinic who have undergone the conventional techniques clearly recall the experience and described it as unpleasant and anxiety provoking. In addition, some patients, especially those with Parkinson s disease who are off their medications, may have difficulty tolerating the experience and the effects of sedation. Thus, with our protocol, patients can undergo microelectrode recordings without any sedation and are more likely to be fully awake and interactive during the clinical testing portion of the procedure. The lack of sedative medications also decreases the possibility for interference with the electrophysiological recordings throughout the targeted areas. We have also observed that our patients are more likely to make it through a bilateral procedure with less fatigue and more mental clarity. With respect to operating room workflow, the timing we observed for each of our stages approximately 90 minutes for Stage I and 230 minutes for Stage II is in accordance with the reported times for these bilateral procedures under conventional conditions. 1 Unilateral procedures took considerably less time. All patients, either with unilateral or with bilateral implantations, received implants in 2 stages; that is, none of the patients selected for bilateral implantation underwent 2 separate unilateral procedures. Our current protocol allows patients to have DBS systems implanted and completely functional within 3 5 days. This is the shortest timespan possible without performing the surgeries in a single inpatient setting. Although patients can tolerate a shorter gap between surgeries, as when they are performed in one hospital admission, US hospitals lose a significant amount of money because of reimbursement restrictions set forth by coding regulations. Conversely, in most states, there is a financial advantage to staging the stimulator implantation surgeries separately by more than 30 days. Under these conditions, the second stimulator implant is considered a stand-alone procedure rather than a staged procedure or an add-on procedure. In summary, we believe that the approach outlined here has several potential advantages that could benefit the patients as well as the surgical teams and is worth considering as an alternative to the traditional staging paradigm. We have found that it is particularly beneficial in situations in which patients need to be fully awake and interactive to ensure accurate targeting and the avoidance of stimulation side effects. Conclusions We present a DBS surgical protocol in which the typical staging sequence is reversed: the pulse generator and lead extensions are implanted during the first stage, and the microelectrode recordings and stimulating lead placements are performed during the second stage. We take advantage of this sequence by creating the bur holes during the first stage while the patient is under general anesthesia. One of the main benefits of this particular surgical staging sequence is the minimization of patient discomfort and anxiety by eliminating any awareness of the bur hole experience. Additionally, we feel we have the ability to devote more time to microelectrode recordings and DBS lead placement given that the bur holes have already been placed, and the patients are free of any effects from sedatives. Finally, patients have the opportunity to begin stimulation therapy in a more streamlined fashion after having their complete system implanted within 3 5 days. Acknowledgment We thank Tom Dolan at the UK Academic Technology Group for the illustrations. References 1. Abosch A, Timmermann L, Bartley S, Rietkerk HG, Whiting D, Connolly PJ, et al: An international survey of deep brain stimulation procedural steps. Stereotact Funct Neurosurg 91:1 11, Bejjani BP, Dormont D, Pidoux B, Yelnik J, Damier P, Arnulf I, et al: Bilateral subthalamic stimulation for Parkinson s disease by using three-dimensional stereotactic magnetic resonance imaging and electrophysiological guidance. J Neurosurg 92: , Halpern CH, Torres N, Hurtig HI, Wolf JA, Stephen J, Oh MY, et al: Expanding applications of deep brain stimulation: a potential therapeutic role in obesity and addiction management. Acta Neurochir (Wien) 153: , Lang AE, Widner H: Deep brain stimulation for Parkinson s 1046 J Neurosurg Volume 122 May 2015
6 Reversed staging deep brain stimulation surgery disease: patient selection and evaluation. Mov Disord 17 Suppl 3:S94 S101, Lozano AM, Lipsman N: Probing and regulating dysfunctional circuits using deep brain stimulation. Neuron 77: , Rezai AR, Kopell BH, Gross RE, Vitek JL, Sharan AD, Limousin P, et al: Deep brain stimulation for Parkinson s disease: surgical issues. Mov Disord 21 (Suppl 14):S197 S218, Shrivastava RK, Germano IM: Deep brain stimulation for the treatment of Parkinson s disease. Contemp Neurosurg 23:1 9, Sierens DK, Kutz S, Pilitsis JG, Bakay RAE: Stereotactic surgery with microelectrode recordings, in Bakay RAE (ed): Movement Disorder Surgery: The Essentials. New York: Thieme, 2009, pp Yeremeyeva E, Taghva A, Rezai AR: Seeking new solutions: stimulation of diseased circuits in depression and other neurobehavioral disorders. Clin Neurosurg 59:44 49, 2012 Author Contributions Conception and design: van Horne. Drafting the article: van Horne, Vaughan, Massari, Bennett. Critically revising the article: van Horne, Asfahani, Quintero, Gerhardt. Reviewed submitted version of manuscript: all authors. Approved the final version of the manuscript on behalf of all authors: van Horne. Administrative/technical/ material support: Massari. Study supervision: van Horne. Correspondence Craig G. van Horne, Department of Neurosurgery, University of Kentucky, 800 Rose St., Lexington, KY craigvanhorne@uky.edu. J Neurosurg Volume 122 May
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
The Surgical Management of Essential Tremor
 The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
SUPPLEMENTAL DIGITAL CONTENT
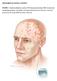 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
S ince the pioneering work of Benabid et and Pollak
 409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
Pallidal Deep Brain Stimulation
 Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Over the last few years, laser interstitial thermotherapy. focus Neurosurg Focus 41 (4):E3, 2016
 neurosurgical focus Neurosurg Focus 41 (4):E3, 2016 The use of custom 3D printed stereotactic frames for laser interstitial thermal ablation: technical note Nicholas J. Brandmeir, MD, James McInerney,
neurosurgical focus Neurosurg Focus 41 (4):E3, 2016 The use of custom 3D printed stereotactic frames for laser interstitial thermal ablation: technical note Nicholas J. Brandmeir, MD, James McInerney,
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Palladotomy and Pallidal Deep Brain Stimulation
 Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri)
 1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Surgical Options. A History of Surgical Treatment. Patient selection. Essential Tremor (ET)
 Essential tremor (ET) is the most common movement disorder, impacting the lives of an estimated 10 million Americans and millions more worldwide. At this time, there is no cure for ET and only about 50%
Essential tremor (ET) is the most common movement disorder, impacting the lives of an estimated 10 million Americans and millions more worldwide. At this time, there is no cure for ET and only about 50%
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group
 Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
YOur Values Your PReferences. Should You Have Deep Brain Stimulation?
 YOur Values Your PReferences Your Choice Should You Have Deep Brain Stimulation? Understanding Deep Brain Stimulation Your Brain and Central Nervous System Nerve cells (neurons) communicate with your body
YOur Values Your PReferences Your Choice Should You Have Deep Brain Stimulation? Understanding Deep Brain Stimulation Your Brain and Central Nervous System Nerve cells (neurons) communicate with your body
UNPRECEDENTED BENEFITS TRANSFORMATIVE RESULTS. In clinical studies, patients reported an immediate, significant reduction of tremor.
 UNPRECEDENTED BENEFITS TREMOR IMPROVEMENT In clinical studies, patients reported an immediate, significant reduction of tremor. * NON-INVASIVE Focused ultrasound is capable of penetrating the skull without
UNPRECEDENTED BENEFITS TREMOR IMPROVEMENT In clinical studies, patients reported an immediate, significant reduction of tremor. * NON-INVASIVE Focused ultrasound is capable of penetrating the skull without
DEEP TMS TREATMENT CONSENT FORM
 DEEP TMS TREATMENT CONSENT FORM My doctor has recommended that I receive treatment with Brainsway Deep TMS. The nature of this treatment, including the benefits and risks that I may experience, has been
DEEP TMS TREATMENT CONSENT FORM My doctor has recommended that I receive treatment with Brainsway Deep TMS. The nature of this treatment, including the benefits and risks that I may experience, has been
1. POLICY: Magnetic Resonance Image Guided High Intensity Focused Ultrasound (MRgFUS) for Essential Tremor
 Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
2014 AAPM 56 th Annual Meeting
 2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
2014 AAPM 56 th Annual Meeting SAM Diagnostic Radiology MR Safety - Deep Brain Stimulator and Other Neurostimulators Yunhong Shu, Ph.D. Mayo Clinic, Rochester, MN Outline Background of Neurostimulator
Imagine your tremor free life! Non-Invasive Treatment for Essential Tremor
 Imagine your tremor free life! Non-Invasive Treatment for Essential Tremor The non-invasive treatment for Essential Tremor (ET) is performed using Neuravive. WHAT IS ESSENTIAL TREMOR? Essential Tremor
Imagine your tremor free life! Non-Invasive Treatment for Essential Tremor The non-invasive treatment for Essential Tremor (ET) is performed using Neuravive. WHAT IS ESSENTIAL TREMOR? Essential Tremor
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
HealthTalks. Deep Brain Stimulation for Parkinson s Disease Patients
 HealthTalks Parkinson s Disease and Wellness Ali Rezai, MD Neurological Institute Director, Center for Neurological Restoration Cleveland Clinic Appointments: 216.444.4720 Deep Brain Stimulation for Parkinson
HealthTalks Parkinson s Disease and Wellness Ali Rezai, MD Neurological Institute Director, Center for Neurological Restoration Cleveland Clinic Appointments: 216.444.4720 Deep Brain Stimulation for Parkinson
Dual floor burr hole technique in deep brain stimulation: A retrospective study on 209 patients
 SNI: Stereotactic OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Antonio F. DeSalles, M.D., University of California at Los Angeles, Los Angeles, CA, USA Technical
SNI: Stereotactic OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Antonio F. DeSalles, M.D., University of California at Los Angeles, Los Angeles, CA, USA Technical
Deep Brain Stimulation (DBS)
 Patient & Family Guide 2016 Deep Brain Stimulation (DBS) www.nshealth.ca Deep Brain Stimulation (DBS) Deep brain stimulation (DBS) is used to help control stiffness or uncontrollable movements. Your neurosurgeon
Patient & Family Guide 2016 Deep Brain Stimulation (DBS) www.nshealth.ca Deep Brain Stimulation (DBS) Deep brain stimulation (DBS) is used to help control stiffness or uncontrollable movements. Your neurosurgeon
A Patient s Guide to SRS
 A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
Approximately one-third of newly diagnosed epilepsy
 clinical article J Neurosurg 122:526 531, 2015 Intraoperative computed tomography for intracranial electrode implantation surgery in medically refractory epilepsy Darrin J. Lee, MD, PhD, 1 Marike Zwienenberg-Lee,
clinical article J Neurosurg 122:526 531, 2015 Intraoperative computed tomography for intracranial electrode implantation surgery in medically refractory epilepsy Darrin J. Lee, MD, PhD, 1 Marike Zwienenberg-Lee,
Deep Brain Stimulation (DBS) For patients with tremor
 Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Introduction of FIREFLY Technology
 Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT. Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018
 EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
Deep brain stimulation
 About insertion of a deep brain stimulator The deep brain stimulator sends electrical impulses to the brain interrupting the abnormal signals that are causing the symptoms. The impulses are adjusted by
About insertion of a deep brain stimulator The deep brain stimulator sends electrical impulses to the brain interrupting the abnormal signals that are causing the symptoms. The impulses are adjusted by
Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic surgery
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
Medical Review Criteria Implantable Neurostimulators
 Medical Review Criteria Implantable Neurostimulators Subject: Implantable Neurostimulators Effective Date: April 14, 2017 Authorization: Prior authorization is required for covered implantable stimulators
Medical Review Criteria Implantable Neurostimulators Subject: Implantable Neurostimulators Effective Date: April 14, 2017 Authorization: Prior authorization is required for covered implantable stimulators
WayPoint Implant and Surgical Kits
 WayPoint Implant and Surgical Kits Directions For Use L011-68 (Rev C0, 2017-03-20) Contains directions for the following products: 66-WP-BKS, 66-WP-IKS, 66-WP-SKS www.fh-co.com FHC, Inc. 1201 Main Street
WayPoint Implant and Surgical Kits Directions For Use L011-68 (Rev C0, 2017-03-20) Contains directions for the following products: 66-WP-BKS, 66-WP-IKS, 66-WP-SKS www.fh-co.com FHC, Inc. 1201 Main Street
Radiofrequency Ablation (RFA) / Microwave Ablation (MWA) of Lung Tumors
 Scan for mobile link. Radiofrequency Ablation (RFA) / Microwave Ablation (MWA) of Lung Tumors Radiofrequency ablation (RFA) and microwave ablation (MWA) are treatments that use image guidance to place
Scan for mobile link. Radiofrequency Ablation (RFA) / Microwave Ablation (MWA) of Lung Tumors Radiofrequency ablation (RFA) and microwave ablation (MWA) are treatments that use image guidance to place
Positively Impacting Patient Outcomes With imri Suite
 In Practice Positively Impacting Patient Outcomes With imri Suite In Practice Something pretty amazing is happening in the middle of America s Dairyland. Neurosurgery tumor resection and deep brain stimulation
In Practice Positively Impacting Patient Outcomes With imri Suite In Practice Something pretty amazing is happening in the middle of America s Dairyland. Neurosurgery tumor resection and deep brain stimulation
Citation for published version (APA): Contarino, M. F. (2013). Improving surgical treatment for movement disorders
 UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
National Institute for Health and Clinical Excellence 319 Deep brain stimulation for tremor and dystonia (excluding Parkinson s disease) nts table IPAC date: 16 June 2006 Consultee name nts The Dystonia
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy (all ages) NHS England Reference: P
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy (all ages) NHS England Reference: 1736P NHS England INFORMATION READER BOX Directorate Medical Operations and Information
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy (all ages) NHS England Reference: 1736P NHS England INFORMATION READER BOX Directorate Medical Operations and Information
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
PATIENT SPECIFIC PLATES FOR MANDIBLE Custom made plates for trauma and reconstruction
 PATIENT SPECIFIC PLATES FOR MANDIBLE Custom made plates for trauma and reconstruction Derived from patient CT data Customizable design features Strength with low profile This publication is not intended
PATIENT SPECIFIC PLATES FOR MANDIBLE Custom made plates for trauma and reconstruction Derived from patient CT data Customizable design features Strength with low profile This publication is not intended
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. What is Parkinson s Disease?
 Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Parkinson s Disease Webcast January 31, 2008 Jill Ostrem, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学
 Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Bilateral deep brain stimulation (DBS) has become
 technical note J Neurosurg 125:85 89, 2016 Simultaneous bilateral stereotactic procedure for deep brain stimulation implants: a significant step for reducing operation time Erich Talamoni Fonoff, MD, PhD,
technical note J Neurosurg 125:85 89, 2016 Simultaneous bilateral stereotactic procedure for deep brain stimulation implants: a significant step for reducing operation time Erich Talamoni Fonoff, MD, PhD,
Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes
 Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
The American Approach to Depth Electrode Insertion December 4, 2012
 The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
As clinical experience with deep-brain stimulation (DBS) of
 ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
Deep Brain Stimulation for Movement Disorders
 1 2 Deep Brain Stimulation for Movement Disorders Overview Deep brain stimulation (DBS) is a surgery to implant a device that sends electrical signals to brain areas responsible for body movement. Electrodes
1 2 Deep Brain Stimulation for Movement Disorders Overview Deep brain stimulation (DBS) is a surgery to implant a device that sends electrical signals to brain areas responsible for body movement. Electrodes
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Value Units
 Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
NCB Proximal Humerus Plating System
 NCB Proximal Humerus Plating System Surgical Technique The right locking option for tough fractures Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
NCB Proximal Humerus Plating System Surgical Technique The right locking option for tough fractures Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients
 J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
Deep Brain Stimulation For Parkinson s Disease
 Deep Brain Stimulation For Parkinson s Disease What s new in brain circuit training Associate Professor Robert Wilcox Flinders University & University of South Australia Neurology Department, Flinders
Deep Brain Stimulation For Parkinson s Disease What s new in brain circuit training Associate Professor Robert Wilcox Flinders University & University of South Australia Neurology Department, Flinders
Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease
 CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
Customized Cranial and Craniofacial Implants. Instructions For Use. 7000revD_Instructions_For_Use. Page 1 of 8
 Customized Cranial and Craniofacial Implants Instructions For Use Page 1 of 8 Table of Contents INDICATIONS... 3 DESCRIPTION OF DEVICE... 3 CONDITIONS OF USE... 3 CONTRAINDICATIONS... 3 KELYNIAM GLOBAL
Customized Cranial and Craniofacial Implants Instructions For Use Page 1 of 8 Table of Contents INDICATIONS... 3 DESCRIPTION OF DEVICE... 3 CONDITIONS OF USE... 3 CONTRAINDICATIONS... 3 KELYNIAM GLOBAL
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Deep Brain Stimulation for Movement Disorders
 Deep Brain Stimulation for Movement Disorders Overview Deep brain stimulation (DBS) is a surgery to implant a device that sends electrical signals to brain areas responsible for body movement. Electrodes
Deep Brain Stimulation for Movement Disorders Overview Deep brain stimulation (DBS) is a surgery to implant a device that sends electrical signals to brain areas responsible for body movement. Electrodes
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Neurosurgery. MR GUIDED FOCUSED ULTRASOUND (MRgFUS) Non-invasive thalamotomy for movement disorders & pain
 Neurosurgery MR GUIDED FOCUSED ULTRASOUND (MRgFUS) Non-invasive thalamotomy for movement disorders & pain INSIGHTEC NEURO - NEXT GENERATION NEUROSURGERY INSIGHTEC the global leader in Magnetic Resonance
Neurosurgery MR GUIDED FOCUSED ULTRASOUND (MRgFUS) Non-invasive thalamotomy for movement disorders & pain INSIGHTEC NEURO - NEXT GENERATION NEUROSURGERY INSIGHTEC the global leader in Magnetic Resonance
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
The Calcaneal Plate. The Synthes non-locking solution for the Calcaneus.
 The Calcaneal Plate. The Synthes non-locking solution for the Calcaneus. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
The Calcaneal Plate. The Synthes non-locking solution for the Calcaneus. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Vascular Procedures 1
 GE Healthcare Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Vascular Procedures 1 January, 2013 www.gehealthcare.com/reimbursement This overview addresses coding, coverage,
GE Healthcare Reimbursement Information for Diagnostic Ultrasound and Ultrasound-guided Vascular Procedures 1 January, 2013 www.gehealthcare.com/reimbursement This overview addresses coding, coverage,
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Diagnostic Laparoscopy patient information from your surgeon & SAGES
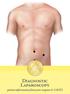 Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
All Indiana Health Coverage Programs Hospitals, Ambulatory Surgical Centers, Physicians, and Durable Medical Equipment Providers
 P R O V I D E R B U L L E T I N B T 2 0 0 0 3 2 S E P T E M B E R 8, 2 0 0 0 To: Subject: All Indiana Health Coverage Programs Hospitals, Ambulatory Surgical Centers, Physicians, and Durable Medical Equipment
P R O V I D E R B U L L E T I N B T 2 0 0 0 3 2 S E P T E M B E R 8, 2 0 0 0 To: Subject: All Indiana Health Coverage Programs Hospitals, Ambulatory Surgical Centers, Physicians, and Durable Medical Equipment
Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections in Patients with Hydrocephalus
 The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
Neurostimulation. Spinal cord stimulators use electrodes placed in the space surrounding the spinal cord (epidural space).
 Neurostimulation.305145613.pdf 1 8/11/12 11:32 PM Neurostimulation Neurostimulation, also called electrostimulation, uses low-level electrical impulses to interfere with pain signals or block them from
Neurostimulation.305145613.pdf 1 8/11/12 11:32 PM Neurostimulation Neurostimulation, also called electrostimulation, uses low-level electrical impulses to interfere with pain signals or block them from
deep brain Dive into stimulation This technique provides new hope for patients with movement disorders.
 BRAIN SPECIAL Dive into deep brain stimulation This technique provides new hope for patients with movement disorders. By Kathryn Murphy, DNSc, NP Historically, electrical stimulation has been used to modulate
BRAIN SPECIAL Dive into deep brain stimulation This technique provides new hope for patients with movement disorders. By Kathryn Murphy, DNSc, NP Historically, electrical stimulation has been used to modulate
Case Study. Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor.
 Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature11239 Introduction The first Supplementary Figure shows additional regions of fmri activation evoked by the task. The second, sixth, and eighth shows an alternative way of analyzing reaction
doi:10.1038/nature11239 Introduction The first Supplementary Figure shows additional regions of fmri activation evoked by the task. The second, sixth, and eighth shows an alternative way of analyzing reaction
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
EasyStep. Operative technique
 Operative technique EasyStep - Step staple This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments. It offers guidance that you should heed,
Operative technique EasyStep - Step staple This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments. It offers guidance that you should heed,
Catherine Carson, V.P. Quality and Performance Improvement. Universal Protocol Policy Template
 Memo TO: FROM: Hospital Quality Committee Catherine Carson, V.P. Quality and Performance Improvement Date: October 22, 2008 SUBJECT: Universal Protocol Policy Template 2009 At the Committee s request,
Memo TO: FROM: Hospital Quality Committee Catherine Carson, V.P. Quality and Performance Improvement Date: October 22, 2008 SUBJECT: Universal Protocol Policy Template 2009 At the Committee s request,
Total Number Programs Evaluated: 382 January 1, 2000 through October 31, 2017
 Page 1 Oral and Maxillofacial Surgery -Residency INFORMATIONAL REPORT ON FREQUENCY OF CITINGS OF ACCREDITATION STANDARDS FOR ADVANCED SPECIALTY EDUCATION PROGRAMS IN ORAL AND MAXILLOFACIAL SURGERY Frequency
Page 1 Oral and Maxillofacial Surgery -Residency INFORMATIONAL REPORT ON FREQUENCY OF CITINGS OF ACCREDITATION STANDARDS FOR ADVANCED SPECIALTY EDUCATION PROGRAMS IN ORAL AND MAXILLOFACIAL SURGERY Frequency
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
History of Deep Brain Stimulation in la Pitié-Salpêtrière hospital
 History of Deep Brain Stimulation in la Pitié-Salpêtrière hospital Since the beginning of Deep Brain Stimulation (DBS) in the 80 s, DBS changed very much following evolution of technologies, but also following
History of Deep Brain Stimulation in la Pitié-Salpêtrière hospital Since the beginning of Deep Brain Stimulation (DBS) in the 80 s, DBS changed very much following evolution of technologies, but also following
Rob McAlpine Legacy Initiative. Cutting Edge NeuroTechnologies for Improved Neurological Health: High Intensity Focused Ultrasound (HIFU) Proposal
 Rob McAlpine Legacy Initiative Cutting Edge NeuroTechnologies for Improved Neurological Health: High Intensity Focused Ultrasound (HIFU) Proposal Rob McAlpine Legacy Initiative Rob McAlpine is an outstanding
Rob McAlpine Legacy Initiative Cutting Edge NeuroTechnologies for Improved Neurological Health: High Intensity Focused Ultrasound (HIFU) Proposal Rob McAlpine Legacy Initiative Rob McAlpine is an outstanding
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Deep Brain Stimulation Surgery Staging and Surgical Instructions
 Deep Brain Stimulation Surgery Staging and Surgical Instructions Stage 1: Outpatient imaging and fiducial insertion (to allow the fabrication of the StarFix platform) MRI Date: Anchor implantation and
Deep Brain Stimulation Surgery Staging and Surgical Instructions Stage 1: Outpatient imaging and fiducial insertion (to allow the fabrication of the StarFix platform) MRI Date: Anchor implantation and
LCP Metaphyseal Plates. For extra-articular fractures.
 LCP Metaphyseal Plates. For extra-articular fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
LCP Metaphyseal Plates. For extra-articular fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Intravascular Ultrasound
 Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Radiological evaluation of ventriculoperitoneal shunt systems
 Radiological evaluation of ventriculoperitoneal shunt systems Poster No.: C-702 Congress: ECR 2009 Type: Educational Exhibit Topic: Neuro Authors: T. Rodt, C. von Falck, C. Tschan, M. Diensthuber, J. Zajaczek,
Radiological evaluation of ventriculoperitoneal shunt systems Poster No.: C-702 Congress: ECR 2009 Type: Educational Exhibit Topic: Neuro Authors: T. Rodt, C. von Falck, C. Tschan, M. Diensthuber, J. Zajaczek,
DBS THERAPY FOR ESSENTIAL TREMOR, PARKINSON S DISEASE, DYSTONIA AND OBSESSIVE- COMPULSIVE DISORDER COMMONLY BILLED CODES EFFECTIVE JANUARY 2017
 FOR ESSENTIAL TREMOR, PARKINSON S DISEASE, DYSTONIA AND OBSESSIVE- COMPULSIVE DISORDER EFFECTIVE JANUARY 2017 Medtronic provides this information for your convenience only. It does not constitute legal
FOR ESSENTIAL TREMOR, PARKINSON S DISEASE, DYSTONIA AND OBSESSIVE- COMPULSIVE DISORDER EFFECTIVE JANUARY 2017 Medtronic provides this information for your convenience only. It does not constitute legal
Catheter-directed Thrombolysis
 Scan for mobile link. Catheter-directed Thrombolysis Catheter-directed thrombolysis treats vascular blockages and improves blood flow by dissolving abnormal blood clots. A blood clot, or thrombus, can
Scan for mobile link. Catheter-directed Thrombolysis Catheter-directed thrombolysis treats vascular blockages and improves blood flow by dissolving abnormal blood clots. A blood clot, or thrombus, can
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
Coding Companion for Podiatry. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Podiatry comprehensive illustrated guide to coding and reimbursement 2016 Contents Contents Foot and Toes 28043-28045 [28039, 28041] 28043 28039 28045 28041 Excision, tumor, soft tissue
Coding Companion for Podiatry comprehensive illustrated guide to coding and reimbursement 2016 Contents Contents Foot and Toes 28043-28045 [28039, 28041] 28043 28039 28045 28041 Excision, tumor, soft tissue
