Dementia associated with the antiphospholipid syndrome: clinical and radiological characteristics of 30 patients
|
|
|
- Florence Heath
- 5 years ago
- Views:
Transcription
1 Rheumatology 2005;44:95 99 Advance Access publication 14 eptember 2004 Concise Report Dementia associated with the antiphospholipid syndrome: clinical and radiological characteristics of 30 patients J. A. Go mez-puerta, R. Cervera, L. M. Calvo, B. Gómez-Ansón 1, G. Espinosa, G. Claver,. Bucciarelli, A. Bové, M. Ramos-Casals, M. Ingelmo and J. Font doi: /rheumatology/keh408 Objective. To analyse the clinical and radiological characteristics of patients with dementia associated with the antiphospholipid syndrome (AP). Methods. Twenty-five patients were identified by a computer-assisted (MEDLINE, National Library of Medicine, Bethesda, MD) search of the literature to locate all cases of dementia associated with AP published in English, panish and French from 1983 to Additionally, we included five patients from our clinics. Results. There were 21 (70%) females and 9 (30%) males. The mean age of patients was 4915 yr (range yr). Fourteen (47%) of the patients suffered from primary AP, 9 (30%) had systemic lupus erythematosus and 7 (23%) had lupus-like syndrome. Ten (33%) patients had neddon s syndrome and 2 (7%) had cerebral lesions described as Binswanger s disease. Other AP-related manifestations included thrombocytopenia in 12 (40%) patients, cerebrovascular accidents in 11 (37%), heart valve lesions in 8 (27%), deep vein thrombosis in 7 (28%), migraine in 7 (23%), seizures in 4 (13%); five of the 21 (24%) female patients had nine spontaneous abortions. Lupus anticoagulant was present in 21/29 (72%) patients and anticardiolipin antibodies were present in 24/29 (83%) patients. Cortical infarcts were found in 19 (63%) patients, subcortical infarcts in 9 (30%), basal ganglia infarcts in 7 (23%) and signs of cerebral atrophy in 11 (37%). Anticoagulation was used in 14/25 (56%) patients, steroids in 12/25 (48%), aspirin in 6/25 (24%) and dypiridamole in 5/25 (20%). Conclusions. Dementia is an unusual manifestation of AP but one which has a high disability impact in a patient s daily life. In order to prevent these consequences, an echocardiographic and cerebral CT or MRI evaluation are recommended in all patients with AP. Furthermore, ruling out AP should be recommended in the clinical approach to dementia, especially in young patients. KEY WORD: Antiphospholipid syndrome, Dementia, Vascular dementia, Multi-infarct dementia, neddon s syndrome, Binswanger s disease. Dementia is being increasingly diagnosed in clinical practice and has a high disability impact in a patient s daily life. Alzheimer s disease is the main cause of dementia, followed by vascular multi-infarct dementia, Parkinson s disease, frontal lobe dementia and, less commonly, other metabolic and reversible causes of dementia [1]. The antiphospholipid syndrome (AP) is an autoimmune prothrombotic condition characterized by venous and/or arterial thrombosis and pregnancy morbidity in the presence of antiphospholipid antibodies (apl), i.e. lupus anticoagulant (LA) and anticardiolipin antibodies (acl) [2]. Involvement of cerebral large vessels is frequent in AP and patients usually present clinically with transient ischaemic attacks (TIA) and strokes. However, a wide spectrum of other neurological features has been described, including chorea, epilepsy, multiple sclerosis-like lesions, psychiatric features, migraine and also dementia, among others [2, 3]. A relationship between dementia and AP has been proposed by several authors [2 7]. Although most studies have focused on patients with dementia and cerebral vascular lesions, less severe cognitive impairment has also been associated with the presence of apl in the absence of imaging lesions in the brain [7]. Furthermore, the ischaemic stroke in neddon s syndrome may overlap with AP and some of these patients suffer from severe vascular dementia. The objective of this study was to analyse the clinical and radiological features of patients with dementia associated with AP, highlighting the importance of early diagnosis of this condition. Patients and methods Patients were identified by a computer-assisted (MEDLINE, National Library of Medicine, Bethesda, MD) search of the Department of Autoimmune Diseases, Institut Clı nic de Medicina i Dermatologia, per la Imatge, Hospital Clı nic, Barcelona, Catalonia, pain. 1 Department of Neuroradiology, Centre Clı nic de Diagnòstic ubmitted 8 July 2004; revised version accepted 10 August Correspondence to: R. Cervera, ervei de Malalties Autoimmunes, Hospital Clı nic, Villarroel, 170, Barcelona, Catalonia, pain. rcervera@clinic.ub.es 95 Rheumatology Vol. 44. No. 1 ß British ociety for Rheumatology 2004; all rights reserved
2 96 J. A. Go mez-puerta et al. TABLE 1. General characteristics of 30 patients with dementia and AP Author Gender/ age Diagnosis Associated neddon a Other manifestation Dementia diagnosis apl CN imaging Treatment 1. Asherson et al. [12] F/52 Lupus-like LR, migraine, DVT imultaneously LA, aclþ CT: multiple hemispheric cortical infarcts,, D,, D 2. Asherson et al. [12] F/33 LE þ LR, migraine, DVT, AHA, TIA, chorea, VL 3. Asherson et al. [12] F/32 LE þ Migraine, LR, CVA DVT, thrombocytopenia 4. Asherson et al. [12] F/43 LE Migraine, A (2), sup. thrombophlebitis 7 yr later LA, aclþ CT: multiple cortical infarcts and thalamic lacunar infarct 7 yr later LA, aclþ CT: multiple cortical infarcts, D, AA 1.5 yr later acl IgG CT: multiple bilateral small lacunar and subcortical infarcts in the frontal cand occipitalwhite matter 5. Coull et al. [13] b M/59 PAP CVA, AHA, MI imultaneously aclþ CT: bilateral cortical cerebral infarcts 6. Coull et al. [13] M/43 PAP CVA, thrombocytopenia imultaneously aclþ CT: multiple cortical and subcortical infarctions 7. Coull et al. [13] M/69 PAP CVA 6 yr later aclþ CT: multiple small cortical infarctions AA, D 8. Coull et al. [13] F/28 PAP CVA 2.5 yr later aclþ CT: multiple cortical and subcortical AA, D infarctions 9. Montalba n et al. [14] M/47 Lupus-like Migraine, thrombocytopenia retinal vein occlusion, VL 10 yr later LA acl CT: multiple cortical infarcts 10. Montalba n et al. [14] F/37 LE-like A, seizure, CVA 5 yr later LA acl CT: one cerebral cortical infarction AA 11. Asherson et al. [15] M/42 Lupus-like þ LR, MI, skin ulcers, thrombocytopenia, VL, thrombotic glaucoma 3 yr later LA, aclþ CT: multiple bilateral occipital and parietotemporal infarcts 12. Asherson et al. [15] F/45 PAP Migraine 5 yr later aclþ CT: multiple cortical and small subcortical infarcts 13. Asherson et al. [15] F/42 Lupus-like þ PE (2), LR, CVA, A (3), VL imultaneously LA, acl CT: multiple small cortical infarcts, 14. Westerman et al. [16] b M/54 Lupus-like Thrombocytopenia imultaneously acl IgG MRI: multiple cortical and subcortical hyperintense areas 15. Charles et al. [17] F/16 PAP þ Thrombocytopenia, LR,VL imultaneously aclþ MRI: bilateral thalamic lesions of high signal intensity (infarctions) 16. Kurita et al. [18] M/39 PAP CVA imultaneuosly LAþ CT: multiple brain infarcts 17. Robin et al. [19] F/62 LE Optic neuritis 2 yr later LA, aclþ CT: atrophy and subcortical low-attenuation areas MRI: hyperintensities in periventricular white matter 18. Robin et al. [19] F/63 LE kin ulcers 2 yr later LAþ CT: atrophy and subcortical low-attenuation areas. MRI: hyperintensities in periventricular white matter 19. erra-mestres [20] M/68 PAP þ LR 5yr later aclþ MRI: diffuse white matter hyperintensitities 20. van-horn et al. [21] F/22 Lupus-like up. thrombophlebitis, chorea 1 yr later LA MRI: caudate and white matter hyperintensities., AA PECT: bilaterally decreased perfusion 21. Tomimoto et al. (22) F/60 PAP imultaneously LAþ MRI: diffuse patchy hyperintensities in basal ganglia and cerebral white matter 22. Rich et al. [23] F/34 PAP þ LR, thrombocytopenia, A, VL imultaneously LA, aclþ CT: atrophy. MRI: lacunar hyperintensities consistent with infarcts 23. Fukui et al. [24] F/50 LE Thrombocytopenia, retinal vein thrombosis, seizures 3 yr later LA, aclþ MRI: generalized and progressive, multiple hyperintensities. PECT: defects in bilateral temporoparietal regions 24. Hilker et al. [25] M/55 PAP DVT, thrombocytopenia 5 yr later LA, aclþ MRI: non-specific lacunar lesions in 25. Rodríguez Campello et al. [26] basal ganglia and hyperintensities in periventricular white matter, atrophy F/50 PAP þ Thrombocytopenia, LR imultaneously LA, aclþ CT: cortical and subcortical infarcts. MRI: cortical infarcts and white matter hyperintensities 26. PC 1 F/79 PAP Thrombocytopenia, CVA DVT, PE, A (2), migraine, seizures 1 yr later LA MRI: cortical, subcortical and basal ganglia infarcts, atrophy 27. PC 2 F/49 Lupus-like Thrombocytopenia, VL, seizures imultaneously LA, aclþ MRI: cortical and subcortical infarcts and periventricular white matter hyperintensities 28. PC 3 F/69 LE MI, DVT, CVA 2 yr later LA MRI: cortical infarct in right parietal lobe 29. PC 4 F/72 LE þ LR, thrombocytopenia, CVA, DVT, TIA 4 yr later LA, acl MRI: cortical infarct in occipital lobe 30. PC 5 F/52 PAP Thrombocytopenia, VL 4 yr later LA, aclþ CT: cortical infarcts,, AA, a Associated neddon s syndrome (the co-existence of hypertension, livedo reticularis and stroke). b Microthrombosis in cerebral biopsy. Abbreviations:, anticoagulation; AHA, autoimmune haemolytic anaemia; AA, aspirin; acl, anticardiolipin antibodies; apl, antiphospholipid antibodies; AP, antiphospholipid syndrome; CN, central nervous system; CT, computed tomography; CVA, cerebrovascular accident; D, dypiridamole; F, female; LA, lupus anticoagulant; LR, livedo reticularis; M, male; MI, myocardial infarction; MRI, magnetic resonance imaging;, none reported; PAP, primary antiphospholipid syndrome; PC, present case; PE, pulmonary embolism;, steroids; A, spontaneous abortions; LE, systemic lupus erythematosus; PECT, single-photon emission computed tomography; TIA, transient ischaemic attack; VL, valve lesions.
3 Dementia and antiphospholipid syndrome 97 literature to locate all cases of AP published in English, panish and French from 1983 (when AP was first defined) to December 2003 (keywords used were: anticardiolipin antibodies, lupus inhibitor, cardiolipin, coagulation inhibitor, lupus anticoagulant, antiphospholipid syndrome, antiphospholipid antibodies, multiinfarct dementia, vascular dementia, neddon s syndrome, Alzheimer s disease and Binswanger s disease). Cases having neddon s syndrome with dementia but without apl were not included. Only cases with well-documented clinical summaries and relevant information were included in this review. Data from these cases were summarized using a standardized data form, including gender, age, diagnosis of the underlying condition, the major thrombotic clinical manifestations, immunological features, time of the evolution since the diagnosis of AP until the development of dementia, imaging features and treatment. Five new cases with dementia and AP from our clinics were added to the review. Those patients diagnosed as having dementia who were included in large AP series, but in whom no well-documented clinical data were recorded, were not considered for analysis in the present study. Patients were defined as having dementia according to the Diagnostic and tatistical Manual of Mental Disorders (DM-IV) [8]. They were classified as having systemic lupus erythematosus (LE) if they met four or more criteria of the American College of Rheumatology [9, 10], as lupus-like syndrome if they met only two or three criteria and as primary AP if they met criteria of the International Consensus tatement on Preliminary Classification Criteria for definite AP, and did not meet any of the above described criteria for LE or lupus-like syndrome [11]. Ethical approval and informed patient consent were not required because the study was an analysis of patients that were located by means of a computer-assisted (MEDLINE, National Library of Medicine, Bethesda, MD) search of the literature. Results A total of 25 patients with dementia associated with AP were found in the literature search [12 26]. We did not include those cases where clinical, immunological and imaging characteristics were not described in detail. Five additional patients from our clinics were also reviewed. General characteristics General clinical features of these 30 patients are shown in Table 1. There were 21 (70%) females and 9 (30%) males. The mean age of patients was yr (range yr). Fourteen (47%) of the patients suffered from primary AP, 9 (30%) had LE and 7 (23%) patients had lupus-like syndrome. Ten (33%) patients had neddon s syndrome and 2 (7%) had cerebral lesions described as Binswanger s disease. Clinical presentation Dementia was the presenting manifestation of the AP in 11 (37%) patients. A clinically evident past history of CVA was detected in 11 (37%) patients. Other neurological features included migraine in 7 (23%) patients, seizures in 4 (13%), TIA in 2 (7%), chorea in 2 (7%), and retinal thrombosis in 2 (7%) patients. Thrombotic glaucoma and optic neuritis were present in 1 (3%) case each. kin involvement in the form of livedo reticularis (as a manifestation of neddon s syndrome) was reported in 10 (33%) patients, and skin ulcers in 3 (10%). Other AP-related manifestations were as follows: 8 (27%) patients had heart valve lesions, 7 (23%) deepvein thrombosis (DVT), 2 (7%) pulmonary embolism, 3 (10%) myocardial infarction and 2 (7%) superficial thrombophlebitis. Previous spontaneous abortions (n ¼ 9) were reported in 5 of the 21 (24%) female patients. Laboratory profile Twelve (40%) patients had thrombocytopenia and 2 (7%) had autoimmune haemolytic anaemia. LA was present in 21/29 (72%) patients, whilst acl was present in 24/29 (83%) patients. Neuroimaging features Most patients exhibited several types of lesions on cerebral computed tomography (CT) scan or magnetic resonance imaging (MRI). Cortical infarcts were detected in 19 (63%) patients, subcortical infarcts in 9 (30%), basal ganglia infarcts in 7 (23%) and cerebral atrophy in 11 (37%). ilent brain infarcts (cerebral ischaemic lesions without any focal neurological features) were found in 14 (47%) patients. Treatment and evolution towards dementia Anticoagulation was used in 14/25 (56%) patients, steroids in 12/25 (48%), aspirin in 6/25 (24%) and dypiridamole in 5/25 (20%). Treatment was not reported for five cases. In the 19 (63%) patients who presented AP manifestations previous to the diagnosis of dementia, anticoagulation had been used in 7 (37%) patients, steroids in 6 (32%), aspirin in 5 (26%) and dypiridamole in 4 (21%). The mean time of evolution from the initial AP manifestations to the diagnosis of dementia in these 19 patients was 3.5 yr (range, 1 10 yr). Discussion The relationship between dementia and AP has been proposed in several studies. Mosek et al. [6] studied 87 patients diagnosed as having dementia and compared them with 69 elderly healthy controls. They found higher levels of apl in patients with dementia than in controls. Juby et al. [27] analysed the prevalence of acl in 218 elderly patients. They disclosed that 34 patients suffered from dementia and a significant association between acl and both vascular dementia and Alzheimer s disease was noted. Recently, Chapman et al. [4] studied 23 patients with primary AP and found that 13 (56%) fulfilled criteria for dementia using the Hachinski Ischemia core (HI). Patients with dementia were older, had more CT scan abnormalities and more electroencephalography changes than those without dementia. However, the Euro-Phospholipid consortium, in their cohort of 1000 AP patients, described the presence of vascular dementia in only 25 (2.5%) cases [2]. It is possible that the higher prevalence of dementia in the Chapman et al. series [4] could be merely due to the small and probably highly selected group of patients studied, but it could also be due to the exclusion of LE patients as it is know that in AP associated with LE the incidence of neurological manifestations is higher than in primary AP [28]. The presence of apl in patients with cognitive problems seems to be more than an epiphenomenon, as it has been demonstrated in experimental studies. hrot et al. [29] performed an elegant study with BALB/c mice using a staircase test and a T maze alternation test as cognitive assessment tools. Mice immunized with anti-2- glycoprotein I antibodies developed a higher degree of behavioural and cognitive abnormalities than those that had not been immunized. One-third of the patients from our series had neddon s syndrome. France` s et al. [30] described a specific subset of patients with this syndrome having apl who presented more thrombocytopenia, mitral regurgitation and irregular livedo reticularis than
4 98 J. A. Go mez-puerta et al. patients without apl. There is controversy concerning whether patients with neddon s syndrome without apl could be a special group of transient seronegative AP patients. In the present study, almost one-third of patients had valve disease. It is well known that a high proportion of cerebral infarcts have a cardiac embolic origin and that patients with apl have higher prevalence of valvular abnormalities [31]. Thickening of the valve leaflets is the most common lesion detected by echocardiography in both LE and primary AP patients. The mitral valve is involved most commonly, followed by the aortic valve [32]. Epilepsy is a common neurological manifestation in AP [2]. Recent studies by hoenfeld et al. [33] have confirmed a link between this manifestation and cerebrovascular involvement, heart valve lesions and livedo reticularis. In the present series, 13% of the patients with dementia presented seizures, thus reinforcing the role of focal brain ischaemic lesions in the pathogenesis of AP-related epilepsy. Patients with dementia exhibit a wide variety of cerebral lesions on CT or MRI studies. Cortical and subcortical infarcts are the more frequent findings. Other ischaemic lesions such as lacunar and periventricular infarcts are not uncommon. Cerebral atrophy and white matter lesions (leukoaraiosis), similar to the lesions found in Binswanger s disease, are often seen, specially in elderly AP patients [15]. In LE, these findings have been shown to be in close association with the presence of AP, but other factors, e.g. hypertension, could also contribute to their presence [34]. The continuous improvement and development of new CN imaging techniques [i.e. positron emission tomography (PET) or singlephoton emission computed tomography (PECT)] will allow to us differentiate the distinct perfusion patterns on these cerebral disorders. Kao et al. [35] studied 22 patients with primary AP with only mild neuropsychiatric manifestations (headache, depression, personality disorders, memory loss and cognitive function deficits) and normal brain MRI. They found that 16 (73%) of the patients had abnormal PECT findings, mainly diffuse hypoperfusion lesions in cerebral cortex. It is not only those patients with evident cerebral lesions and cognitive impairment who deserve special attention, but also those patients with an asymptomatic course or subtle decline in cerebral functions having cerebral ischaemic lesions on MRI (silent brain infarcts). Vermeer et al. [36] followed 1077 elderly patients without dementia over 5 yr, with periodical MRI evaluation. Two hundred and seventeen (21%) patients had silent brain infarcts at baseline, with a global cognitive function significantly worse than in those patients without brain infarcts. During the follow-up, 30 (3%) of these patients developed dementia. Erkan et al. [5], in a 10-yr follow-up study of 66 patients with primary AP, found that 3 patients (<30 yr old) developed dementia, independently of the presence of CVA. In the present series, previous history of CVA and/or TIA was present in only 11 and 2 patients, respectively; however, silent brain infarcts were present in 14 (47%) patients. everal strategies have been suggested for the treatment of dementia. The management of atherogenic risk factors (i.e. diabetes, hypertension, hyperlipidaemia) is crucial. However, there is still no evidence that aspirin alone is effective in treating patients with a diagnosis of dementia. In dementia associated with AP, anticoagulant treatment is required, with special care in possible everyday situations with the risk of bleeding. Furthermore, the compliance of demented patients is usually poor, which requires special thought and attention. On the other hand, prevention of dementia should be of paramount importance in those patients with a diagnosis of AP. Unfortunately, it is difficult from the present study to recommend any therapeutic strategy because patients were previously treated with a variety of medications. However, it is worth noting that the majority of patients were not on anticoagulants when the first manifestations of dementia appeared. Therefore, this reinforces the need for active antithrombotic prophylaxis once the diagnosis of AP is made. In conclusion, dementia can be present in patients with AP in multiple scenarios, such as primary AP, neddon s syndrome or with white matter lesions similar to Binswanger s disease. Due to the high disability impact and prognostic consequences, we consider that an echocardiographic and cerebral CT or MRI evaluation should be recommended in all patients with AP. Also, it is important to rule out an AP in young subjects with no explicable cause of dementia, and therefore apl should be tested in these patients in order to prevent disease progression and enable adequate treatment to begin. Rheumatology The authors have declared no conflicts of interest. References Key messages An echocardiographic and cerebral CT or MRI evaluation are recommended in all patients with AP. Ruling out AP should be recommended in the clinical approach to dementia. 1. Roman GC. Vascular dementia: distinguishing characteristics, treatment, and prevention. J Am Geriatr oc 2003;51: Cervera R, Piette JC, Font J et al. Antiphospholipid syndrome: clinical and immunologic manifestations and patterns of disease expression in a cohort of 1,000 patients. Arthritis Rheum 2002;46: Chapman J, Rand JH, Brey RL et al. Non-stroke neurological syndromes associated with antiphospholipid antibodies: evaluation of clinical and experimental studies. Lupus 2003;12: Chapman J, Abu-Katash M, Inzelberg R et al. Prevalence and clinical features of dementia associated with the antiphospholipid syndrome and circulating anticoagulants. J Neurol ci 2002; : Erkan D, Yazici Y, obel R, Lockshin MD. Primary antiphospholipid syndrome: functional outcome after 10 years. J Rheumatol 2000;27: Mosek A, Yust I, Treves TA, Vardinon N, Korczyn AD, Chapman J. Dementia and antiphospholipid antibodies. Dement Geriatr Cogn Disord 2000;11: astre-garriga J, Montalban X. AP and the brain. Lupus 2003; 12: American Psychiatric Association. Diagnostic and tatistical Manual of Mental Disorders, 4th edition (DM-IV), Washington, Tan EM, Cohen A, Fries JF et al. The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 1982;25: Hochberg MC. Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 1997;40: Wilson WA, Gharavi AE, Koike T et al. International consensus statement on preliminary classification criteria for definite antiphospholipid syndrome: report of an international workshop. Arthritis Rheum 1999;42: Asherson RA, Mercey D, Philips G et al. Recurrent stroke and multiinfarct dementia in systemic lupus erythematosus: association with antiphospholipid antibodies. Ann Rheum Dis 1987;46: Coull B, Bourdette DN, Goodnight H Jr, Briley DP, Hart R. Multiple cerebral infarctions and dementia associated with anticardiolipin antibodies. troke 1987;18: Montalbán J, Fernández J, Arderiu A et al. Demencia multiinfártica asociada a anticuerpos antifosfolı pido. Presentacio n de dos casos. Med Clin (Barc) 1989;93:424 6.
5 Dementia and antiphospholipid syndrome Asherson RA, Khamashta MA, Gil A et al. Cerebrovascular disease and antiphospholipid antibodies in systemic lupus erythematosus, lupus-like disease, and the primary antiphospholipid syndrome. Am J Med 1989;86: Westerman EM, Miles JM, Backnova M, undst W. Neuropathologic findings in multi-infarct dementia associated with anticardiolipin antibody. Arthritis Rheum 1992;35: Charles PD, Fenichel GM. neddon and antiphospholipid antibody syndromes causing bilateral thalamic infarction. Pediatr Neurol 1994;10: Kurita A, Hasunuma T, Mochio, himada T, Isogai Y, Kurahashi T. A young case with multi-infarct dementia associated with lupus anticoagulant. Intern Med 1994;33: Robin C, Gonnaud PM, Durieu I et al. Progressive lupus dementia. 2 cases with or without antiphospholipid antibodies. Rev Neurol (Paris) 1995;151: erra-mestres J. Antiphospholipid antibodies and Binswanger s disease. Neurology 1996;46: van Horn G, Arnett FC, Dimachkie MM. Reversible dementia and chorea in a young woman with the lupus anticoagulant. Neurology 1996;46: Tomimoto H, Akiguchi I, Ohtani R, Yagi H, Ogura, Wakita H. Effects of an antithrombin drug in patients with subacute exacerbations of Binswanger disease. Intern Med 2000;39: Rich MW. neddon syndrome and dementia. Mayo Clin Proc 1999;74: Fukui T, Kawamura M, Hasegawa Y, Kato T, Kaga E. Multiple cognitive impairments associated with systemic lupus erythematosus and antiphospholipid antibody syndrome: a form of progressive vascular dementia? Eur Neurol 2000;43: Hilker R, Thiel A, Geisen C, Rudolf J. Cerebral blood flow and glucose metabolism in multi-infarct-dementia related to primary antiphospholipid antibody syndrome. Lupus 2000;9: Rodríguez Campello A, Roquer J, Munteis E, Gomis M, Pou A. neddon syndrome presenting with dementia. Neurología 2002;17: Juby A, David JA, Genge T, McElhaney J. Anticardiolipin antibodies in two elderly subpopulations. Lupus 1995;4: oltész P, Veres K, Lakos G, Kiss E, Muszbek L, zegedi G. Evaluation of clinical and laboratory features of antiphospholipid syndrome: a retrospective study of 637 patients. Lupus 2003;12: hrot, Katzav A, Korczyn AD et al. Behavioral and cognitive deficits occur only after prolonged exposure of mice to antiphospholipid antibodies. Lupus 2002;11: Francès C, Papo T, Wechsler B, Laporte JL, Biousse V, Piette JC. neddon syndrome with or without antiphospholipid antibodies. A comparative study in 46 patients. Medicine 1999;78: Khamashta MA, Cervera R, Asherson RA et al. Association of antibodies against phospholipids with heart valve disease in systemic lupus erythematosus. Lancet 1990;335: Cervera R. Recent advances in antiphospholipid antibody-related valvulopathies. J Autoimmun 2000;15: hoenfeld Y, Lev, Blatt I et al. Features associated with epilepsy in the antiphospholipid syndrome. J Rheumatol 2004;31: Csépa ny T, Bereczki D, Kollar J, ikula J, Kiss E, Csiba L. MRI findings in central nervous system systemic lupus erythematosus are associated with immunoserological parameters and hypertension. J Neurol 2003;250: Kao CH, Lan JL, Hsieh JF et al. Evaluation of regional cerebral blood flow with 99mTc-HMPAO in primary antiphospholipid antibody syndrome. J Nucl Med 1999;40: Vermeer E, Prins ND, den Heijer T, Hofman A, Koudstaal PJ, Breteler MM. ilent brain infarcts and the risk of dementia and cognitive decline. N Engl J Med 2003;348:
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Disclosures. Sneddon Syndrome: Untangling the Web. Case Presentation. MRI head w/ and w/o contrast. Further Workup. Further Workup 10/26/2017
 Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Mortality in the Catastrophic Antiphospholipid Syndrome
 ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome
 ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Vague Neurological Conditions
 Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Situaciones estresantes en el lupus
 Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
CEREBRO VASCULAR ACCIDENTS
 CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
Introduction, use of imaging and current guidelines. John O Brien Professor of Old Age Psychiatry University of Cambridge
 Introduction, use of imaging and current guidelines John O Brien Professor of Old Age Psychiatry University of Cambridge Why do we undertake brain imaging in AD and other dementias? Exclude other causes
Introduction, use of imaging and current guidelines John O Brien Professor of Old Age Psychiatry University of Cambridge Why do we undertake brain imaging in AD and other dementias? Exclude other causes
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
ORIGINAL INVESTIGATION. Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings
 ORIGINAL INVESTIGATION Cognitive Deficits in Patients With Antiphospholipid Syndrome Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings Maria G. Tektonidou, MD; Natassa
ORIGINAL INVESTIGATION Cognitive Deficits in Patients With Antiphospholipid Syndrome Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings Maria G. Tektonidou, MD; Natassa
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
The Antiphospholipid Syndrome
 The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Prevalence of antiphospholipid auto antibodies in patients with thrombosis
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome
 Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neurological involvement in antiphospholipid antibodies syndrome (APS)
 European Review for Medical and Pharmacological Sciences Neurological involvement in antiphospholipid antibodies syndrome (APS) A. AMOROSO, A.P. MITTERHOFER, G.M. FERRI, S. GALLUZZO, M. VADACCA, A. AFELTRA
European Review for Medical and Pharmacological Sciences Neurological involvement in antiphospholipid antibodies syndrome (APS) A. AMOROSO, A.P. MITTERHOFER, G.M. FERRI, S. GALLUZZO, M. VADACCA, A. AFELTRA
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
A pictorial review of neurological complications of systemic lupus erythematosus and antiphospholipid syndrome
 A pictorial review of neurological complications of systemic lupus erythematosus and antiphospholipid syndrome Poster No.: C-2780 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: E. Tavernaraki,
A pictorial review of neurological complications of systemic lupus erythematosus and antiphospholipid syndrome Poster No.: C-2780 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: E. Tavernaraki,
Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care AF symptoms Tachycardia
 Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Central nervous system involvement in the antiphospholipid (Hughes) syndrome
 Rheumatology 2003;42:200 213 doi:10.1093/rheumatology/keg080, available online at www.rheumatology.oupjournals.org Review Central nervous system involvement in the antiphospholipid (Hughes) syndrome G.
Rheumatology 2003;42:200 213 doi:10.1093/rheumatology/keg080, available online at www.rheumatology.oupjournals.org Review Central nervous system involvement in the antiphospholipid (Hughes) syndrome G.
Cerebral small vessel disease
 Cerebral small vessel disease What is it? What are the clinical syndromes? How do we diagnose it? What is the pathophysiology? New insights from genetics? Possible therapies? Small Vessel disease Changes
Cerebral small vessel disease What is it? What are the clinical syndromes? How do we diagnose it? What is the pathophysiology? New insights from genetics? Possible therapies? Small Vessel disease Changes
FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK
 07 June, 2018 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK Document Filetype: PDF 365.11 KB 0 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK I recently had a MRI last week with
07 June, 2018 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK Document Filetype: PDF 365.11 KB 0 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK I recently had a MRI last week with
Patient with Musculo-skeletal Complaints - Summary
 Patient with Musculo-skeletal Complaints - Summary 1. Soft Tissue Rheumatism or Arthritis 2. Arthritis Monoarticular Polyarticular - :- (Asymmetrical) (Symetrical) :- -Crystals, Gout - Infective acute
Patient with Musculo-skeletal Complaints - Summary 1. Soft Tissue Rheumatism or Arthritis 2. Arthritis Monoarticular Polyarticular - :- (Asymmetrical) (Symetrical) :- -Crystals, Gout - Infective acute
GERIATRICS CASE PRESENTATION
 GERIATRICS CASE PRESENTATION CASE 79 year old Patient X was admitted to hospital with SOB. He had a hx of sarcoidosis and asbestosis. Home oxygen requirement is 3-3.5litre. He was admitted, given ceftriaxone
GERIATRICS CASE PRESENTATION CASE 79 year old Patient X was admitted to hospital with SOB. He had a hx of sarcoidosis and asbestosis. Home oxygen requirement is 3-3.5litre. He was admitted, given ceftriaxone
Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study
 Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Daniel Egan, MD April 13, 2012
 Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
The Epidemiology of Stroke and Vascular Risk Factors in Cognitive Aging
 The Epidemiology of Stroke and Vascular Risk Factors in Cognitive Aging REBECCA F. GOTTESMAN, MD PHD ASSOCIATE PROFESSOR OF NEUROLOGY AND EPIDEMIOLOGY JOHNS HOPKINS UNIVERSITY OCTOBER 20, 2014 Outline
The Epidemiology of Stroke and Vascular Risk Factors in Cognitive Aging REBECCA F. GOTTESMAN, MD PHD ASSOCIATE PROFESSOR OF NEUROLOGY AND EPIDEMIOLOGY JOHNS HOPKINS UNIVERSITY OCTOBER 20, 2014 Outline
Supplemental Figures and Legends
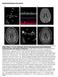 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Vascular Dementia. Laura Pedelty, PhD MD The University of Illinois at Chicago and Jesse Brown VA Medical Center
 Vascular Dementia Laura Pedelty, PhD MD The University of Illinois at Chicago and Jesse Brown VA Medical Center none Disclosures Objectives To review the definition of Vascular Cognitive Impairment (VCI);
Vascular Dementia Laura Pedelty, PhD MD The University of Illinois at Chicago and Jesse Brown VA Medical Center none Disclosures Objectives To review the definition of Vascular Cognitive Impairment (VCI);
Patent Foramen Ovale and Cryptogenic Stroke: Do We Finally Have Closure? Christopher Streib, MD, MS
 Patent Foramen Ovale and Cryptogenic Stroke: Do We Finally Have Closure? Christopher Streib, MD, MS 11-8-18 Outline 1. Background 2. Anatomy of patent foramen ovale (PFO) 3. Relationship between PFO and
Patent Foramen Ovale and Cryptogenic Stroke: Do We Finally Have Closure? Christopher Streib, MD, MS 11-8-18 Outline 1. Background 2. Anatomy of patent foramen ovale (PFO) 3. Relationship between PFO and
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kang D-H, Kim Y-J, Kim S-H, et al. Early surgery versus conventional
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kang D-H, Kim Y-J, Kim S-H, et al. Early surgery versus conventional
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Hypertensive Haemorrhagic Stroke. Dr Philip Lam Thuon Mine
 Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Antiphospholipid antibodies
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
ORIGINAL PAPERS. Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F. Abstract
 ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case Report and Review of the Literature
 Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Thrombophilia. Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS
 Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase <48h)
 Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Patient with vertigo, dizziness and depression
 Clinical Case - Test Yourself Neuro/Head and Neck Radiology Patient with vertigo, dizziness and depression Michael Mantatzis, Paraskevi Argyropoulou, Panos Prassopoulos Radiology Department, Democritus
Clinical Case - Test Yourself Neuro/Head and Neck Radiology Patient with vertigo, dizziness and depression Michael Mantatzis, Paraskevi Argyropoulou, Panos Prassopoulos Radiology Department, Democritus
PRESERVE: How intensively should we treat blood pressure in established cerebral small vessel disease? Guide to assessing MRI scans
 PRESERVE: How intensively should we treat blood pressure in established cerebral small vessel disease? Guide to assessing MRI scans Inclusion Criteria Clinical syndrome Patients must have clinical evidence
PRESERVE: How intensively should we treat blood pressure in established cerebral small vessel disease? Guide to assessing MRI scans Inclusion Criteria Clinical syndrome Patients must have clinical evidence
Patrick R Wood, MD Fellow, Rheumatology University of Colorado
 Patrick R Wood, MD Fellow, Rheumatology University of Colorado Discuss an unusual case of CNS calcification encountered on an academic VA rheumatology service Summarize bilateral striatopallidodentate
Patrick R Wood, MD Fellow, Rheumatology University of Colorado Discuss an unusual case of CNS calcification encountered on an academic VA rheumatology service Summarize bilateral striatopallidodentate
Clinical Research on Treating Senile Dementia by Combining Acupuncture with Acupoint-Injection
 Clinical Research on Treating Senile Dementia by Combining Acupuncture with Acupoint-Injection Yemeng Chen, M.D. Acupuncture Department, Huashan Hospital Shanghai Medical University, Shanghai 20040, P.
Clinical Research on Treating Senile Dementia by Combining Acupuncture with Acupoint-Injection Yemeng Chen, M.D. Acupuncture Department, Huashan Hospital Shanghai Medical University, Shanghai 20040, P.
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome
 Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome L. Stojanovich 1, M. Kontic 2, D. Smiljanic 3, A. Djokovic 1, B. Stamenkovic 4 D. Marisavljevic
Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome L. Stojanovich 1, M. Kontic 2, D. Smiljanic 3, A. Djokovic 1, B. Stamenkovic 4 D. Marisavljevic
PFO Management update
 PFO Management update May 12, 2017 Peter Casterella, MD Swedish Heart and Vascular 1 PFO Update 2017: Objectives Review recently released late outcomes of RESPECT trial and subsequent FDA approval of PFO
PFO Management update May 12, 2017 Peter Casterella, MD Swedish Heart and Vascular 1 PFO Update 2017: Objectives Review recently released late outcomes of RESPECT trial and subsequent FDA approval of PFO
Dianette (cyproterone acetate 2mg/ethinylestradiol 35 mcg): Strengthening of warnings, new contraindications, and updated indication
 Dianette (cyproterone acetate 2mg/ethinylestradiol 35 mcg): Strengthening of warnings, new contraindications, and updated indication Dear Healthcare Professional, In agreement with the European Medicines
Dianette (cyproterone acetate 2mg/ethinylestradiol 35 mcg): Strengthening of warnings, new contraindications, and updated indication Dear Healthcare Professional, In agreement with the European Medicines
Rituximab. B Cell Inhibition in APS. Methods. B Cell Inhibition in APS. Disclosure 11/6/2011
 Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
ATTENDING PHYSICIAN'S STATEMENT STROKE / BRAIN ANEURYSM SURGERY OR CEREBRAL SHUNT INSERTION / CAROTID ARTERY SURGERY
 ATTENDING PHYSICIAN'S STATEMENT STROKE / BRAIN ANEURYSM SURGERY OR CEREBRAL SHUNT INSERTION / CAROTID ARTERY SURGERY A) Patient s Particulars Name of Patient Gender NRIC/FIN or Passport No. Date of Birth
ATTENDING PHYSICIAN'S STATEMENT STROKE / BRAIN ANEURYSM SURGERY OR CEREBRAL SHUNT INSERTION / CAROTID ARTERY SURGERY A) Patient s Particulars Name of Patient Gender NRIC/FIN or Passport No. Date of Birth
Alliance A Symptomatic brain radionecrosis after receiving radiosurgery for
 RANDOMIZED PHASE II STUDY: CORTICOSTEROIDS + BEVACIZUMAB VS. CORTICOSTEROIDS + PLACEBO (BEST) FOR RADIONECROSIS AFTER RADIOSURGERY FOR BRAIN METASTASES Pre-registration Eligibility Criteria Required Initial
RANDOMIZED PHASE II STUDY: CORTICOSTEROIDS + BEVACIZUMAB VS. CORTICOSTEROIDS + PLACEBO (BEST) FOR RADIONECROSIS AFTER RADIOSURGERY FOR BRAIN METASTASES Pre-registration Eligibility Criteria Required Initial
1 MS Lesions in T2-Weighted Images
 1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2
 Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2 C. Jongen J. van der Grond L.J. Kappelle G.J. Biessels M.A. Viergever J.P.W. Pluim On behalf of the Utrecht Diabetic Encephalopathy
Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2 C. Jongen J. van der Grond L.J. Kappelle G.J. Biessels M.A. Viergever J.P.W. Pluim On behalf of the Utrecht Diabetic Encephalopathy
Primary Care practice clinics within the Edmonton Southside Primary Care Network.
 INR Monitoring and Warfarin Dose Adjustment Last Review: November 2016 Intervention(s) and/or Procedure: Registered Nurses (RNs) adjust warfarin dosage according to individual patient International Normalized
INR Monitoring and Warfarin Dose Adjustment Last Review: November 2016 Intervention(s) and/or Procedure: Registered Nurses (RNs) adjust warfarin dosage according to individual patient International Normalized
An Introduc+on to Stroke
 An Introduc+on to Stroke Elizabeth Huntoon MS, MD Assistant Professor Department of Physical Medicine and Rehabilita>on Vanderbilt University School of Medicine Defini+on Sudden focal neurologic deficit
An Introduc+on to Stroke Elizabeth Huntoon MS, MD Assistant Professor Department of Physical Medicine and Rehabilita>on Vanderbilt University School of Medicine Defini+on Sudden focal neurologic deficit
Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus
 J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents
 Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating Prophylaxis after Deep Vein Thrombosis- Pulmonary Embolism
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre
 Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre Today Introduction to CT Introduction to MRI Introduction to nuclear medicine Imaging the dementias The Brain ~ 1.5
Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre Today Introduction to CT Introduction to MRI Introduction to nuclear medicine Imaging the dementias The Brain ~ 1.5
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist
 Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia
 86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
Molecular Imaging and the Brain
 Molecular imaging technologies are playing an important role in neuroimaging, a branch of medical imaging, by providing a window into the living brain. Where CT and conventional MR imaging provide important
Molecular imaging technologies are playing an important role in neuroimaging, a branch of medical imaging, by providing a window into the living brain. Where CT and conventional MR imaging provide important
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
Anticoagulants and Head Injuries. Asaad Shujaa,MD,FRCPC,FAAEM Assistant Professor,weill Corneal Medicne Senior Consultant,HMC Qatar
 Anticoagulants and Head Injuries Asaad Shujaa,MD,FRCPC,FAAEM Assistant Professor,weill Corneal Medicne Senior Consultant,HMC Qatar Common Anticoagulants and Indications Coumadin (warfarin) indicated for
Anticoagulants and Head Injuries Asaad Shujaa,MD,FRCPC,FAAEM Assistant Professor,weill Corneal Medicne Senior Consultant,HMC Qatar Common Anticoagulants and Indications Coumadin (warfarin) indicated for
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Critical Review Form Therapy
 Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Arterial Ischemic Stroke with Protein S Deficiency in Pakistan
 Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
MRI and differential diagnosis in patients suspected of having MS
 Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience
 Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Stroke in the ED. Dr. William Whiteley. Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian
 Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
A Neuropsychiatric, Neuroradiological, and Neuropsychological Profile of a Cohort of Patients with Vascular Dementia
 A Neuropsychiatric, Neuroradiological, and Neuropsychological Profile of a Cohort of Patients with Vascular Dementia Moises Gaviria, MD University of Illinois at Chicago Advocate Christ Medical Center
A Neuropsychiatric, Neuroradiological, and Neuropsychological Profile of a Cohort of Patients with Vascular Dementia Moises Gaviria, MD University of Illinois at Chicago Advocate Christ Medical Center
PFO closure group total no. PFO closure group no. of males
 Suppl Table. Characteristics of the five trials included in this meta-analysis. Trial name Device used for Definition of medical Primary Endpoint group total no. group no. of males group age (yrs) group
Suppl Table. Characteristics of the five trials included in this meta-analysis. Trial name Device used for Definition of medical Primary Endpoint group total no. group no. of males group age (yrs) group
UNDERWRITING GUIDELINES. Individual Insurance
 UNDERWRITING GUIDELINES Individual Insurance TABLE OF CONTENTS About this guide... 4 Medical conditions Asthma...5 Auricular fibrillation...5 Autism...5 Bariatric surgery...5 Barrett s esophagus...5 Cancer
UNDERWRITING GUIDELINES Individual Insurance TABLE OF CONTENTS About this guide... 4 Medical conditions Asthma...5 Auricular fibrillation...5 Autism...5 Bariatric surgery...5 Barrett s esophagus...5 Cancer
HYPERTENSIVE ENCEPHALOPATHY
 HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
Neuroimaging for dementia diagnosis. Guidance from the London Dementia Clinical Network
 Neuroimaging for dementia diagnosis Guidance from the London Dementia Clinical Network Authors Dr Stephen Orleans-Foli Consultant Psychiatrist, West London Mental Health NHS Trust Dr Jeremy Isaacs Consultant
Neuroimaging for dementia diagnosis Guidance from the London Dementia Clinical Network Authors Dr Stephen Orleans-Foli Consultant Psychiatrist, West London Mental Health NHS Trust Dr Jeremy Isaacs Consultant
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Review Article. Catastrophic Antiphospholipid Syndrome. Introduction. Etiopathogenesis. Man-Chi Leung and Woon-Leung Ng
 Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
T he antiphospholipid syndrome (APS) is a thrombophilic
 1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
Embolic Protection Devices for Transcatheter Aortic Valve Replacement
 Embolic Protection Devices for Transcatheter Aortic Valve Replacement James M. McCabe, MD Medical Director, Cardiac Cath Lab University of Washington Seattle, WA Disclosures Proctoring and honoraria for
Embolic Protection Devices for Transcatheter Aortic Valve Replacement James M. McCabe, MD Medical Director, Cardiac Cath Lab University of Washington Seattle, WA Disclosures Proctoring and honoraria for
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 positive options for antiphospholipid syndrome aps self help and treatment
DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 positive options for antiphospholipid syndrome aps self help and treatment
62 yo F, RHD Epilepsy onset: 44 yo Seizure type: 1) Dyscognitive seizure 2) Somatosensory aura (abnormal feeling at both feet) Seizures disappeared
 62 yo F, RHD Epilepsy onset: 44 yo Seizure type: 1) Dyscognitive seizure 2) Somatosensory aura (abnormal feeling at both feet) Seizures disappeared since age 56 years Seizure period: 12 years (44 56 yrs)
62 yo F, RHD Epilepsy onset: 44 yo Seizure type: 1) Dyscognitive seizure 2) Somatosensory aura (abnormal feeling at both feet) Seizures disappeared since age 56 years Seizure period: 12 years (44 56 yrs)
HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM
 REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS. 1. Cardiovascular Disease
 THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS 1. Cardiovascular Disease Cardiovascular disease is considered to have developed if there was a definite manifestation
THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS 1. Cardiovascular Disease Cardiovascular disease is considered to have developed if there was a definite manifestation
The Importance of Middle Cerebral Artery Stenosis In Patients With A Lacunar Infarction In The Carotid Artery Territory
 The Importance of Middle Cerebral Artery Stenosis In Patients With A Lacunar Infarction In The Carotid Artery Territory Oh Young Bang, M.D., Jeong Hoon Cho, M.D., Ji Hoe Heo, M.D., Dong Ik Kim, M.D.* Department
The Importance of Middle Cerebral Artery Stenosis In Patients With A Lacunar Infarction In The Carotid Artery Territory Oh Young Bang, M.D., Jeong Hoon Cho, M.D., Ji Hoe Heo, M.D., Dong Ik Kim, M.D.* Department
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI
 Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
UNIVERSA MEDICINA. A 55 year old man with progressive neurologic deficits
 UNIVERSA MEDICINA May-August, 2009 Vol.28 - No.2 A 55 year old man with progressive neurologic deficits Sendjaja Muljadi* a, and Hardy Senjaya** ABSTRACT At least 50 percent of the decline in functional
UNIVERSA MEDICINA May-August, 2009 Vol.28 - No.2 A 55 year old man with progressive neurologic deficits Sendjaja Muljadi* a, and Hardy Senjaya** ABSTRACT At least 50 percent of the decline in functional
DEBATE: PFO MANAGEMENT TO CLOSE OR NOT TO CLOSE. Matthew Starr, MD Stroke Attending
 DEBATE: PFO MANAGEMENT TO CLOSE OR NOT TO CLOSE Matthew Starr, MD Stroke Attending DISCLOSURES None DEBATE Should PFO be closed? * * Sometimes yes THE CASE AGAINST PFO CLOSURE 1. Did the PFO cause the
DEBATE: PFO MANAGEMENT TO CLOSE OR NOT TO CLOSE Matthew Starr, MD Stroke Attending DISCLOSURES None DEBATE Should PFO be closed? * * Sometimes yes THE CASE AGAINST PFO CLOSURE 1. Did the PFO cause the
