Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome
|
|
|
- Madeline Daniel
- 5 years ago
- Views:
Transcription
1 Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome L. Stojanovich 1, M. Kontic 2, D. Smiljanic 3, A. Djokovic 1, B. Stamenkovic 4 D. Marisavljevic 1,5 1 Internal Medicine, Bezanijska Kosa, University Medical Centre, Belgrade, Serbia; 2 Clinic for Pulmonology, Clinical Center of Serbia, University in Belgrade, Serbia; 3 Department of Neurology, Clinical-Hospital Centre (KBC) Zemun, Belgrade, Serbia; 4 Rheumatology Clinic, Institute Niska Banja, Medical Faculty, University of Nis; 5 Faculty of Medicine, University of Belgrade, Belgrade, Serbia. Abstract Objectives The aim of this study was to investigate the association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipd syndrome (APS), as well as their connection with type and level of antiphospholipid antibodies. Methods Our prospective study comprises 333 patients: 218 with primary and 115 with secondary APS. Antiphospholipid antibody (apl) analysis included detection of acl(igg/igm), ß 2 GPI(IgG/IgM) and LA and served to evaluate associations with distinct neurological manifestations. Results The presence of acl IgG was more common (p=0.001) in SAPS and LA in PAPS patients (p=0.002). High ß 2 GPI IgM levels (>100PLU/ml) were more common in epilepsy (p= ) in PAPS, and in transient ischaemic attack (p=0.029) in SAPS. High ß 2 GPI IgG levels (>100PLU/ml) were more common in epilepsy (p=0.035) in SAPS. Chorea, migraine and epilepsy occurred more often in SAPS and headache and depression in PAPS. We found statistical significance considering the presence of acl IgG and acute ischaemic encephalopathy in SAPS, acl IgM and epilepsy in SAPS, acl IgM and migraine in PAPS, ß 2 GPI IgG and chorea in SAPS and ß 2 GPI IgM and TIA and epilepsy in PAPS. LA was linked to depression, transient global amnaesia and migraine in PAPS. Patients with non-stable angina pectoris were more likely to develop TIA in both PAPS and SAPS, epilepsy and transient global amnaesia in PAPS and acute ischaemic encephalopathy in SAPS. Patients with valve vegetations were more prone to epilepsy and depression. Conclusion Certain apl type and levels are associated with distinct neurological non-thrombotic manifestation, suggesting their predictive role. There is strong link between some non-thrombotic neurological and cardiac manifestations in APS patients, suggesting the complexity and evolutionary nature of APS. Key words antiphospholipid antibodies, non-thrombotic neurological manifestations, cardiac manifestations Clinical and Experimental Rheumatology 2013; 31:
2 Ljudmila Stojanovich, MD, PhD Milica Kontic, MD, PhD Dusica Smiljanic, MD Aleksandra Djokovic, MD Bojana Stamenkovic, MD, PhD Dragomir Marisavljevic, MD, PhD Please address correspondence to: Milica Kontic MD, Pulmology Clinic, Medical Faculty, University in Belgrade, Visegradska 26, Belgrade 11000, Serbia. Received on February 16, 2013; accepted in revised form on April 8, Copyright Clinical and Experimental Rheumatology Funding: this work was supported by research grant numbers and TR for , from the Ministry of Science of the Republic of Serbia. Competing interests: none declared. Introduction Antiphospholipid syndrome (APS) or Huges syndrome represents a systemic autoimmune disorder characterised by arterial and/or venous thrombosis, multiple and recurrent foetal losses, often accompanied by a thrombocytopenia and elevated levels of antiphospholipid antibodies (apl), such as lupus anticoagulant (LA), anticardiolipin antibodies (acl) and anti- GPI antibodies (1-3). This syndrome is considered primary (PAPS) if unassociated with any other connective tissue disease or secondary (SAPS) if it appears in association with other autoimmune disorders, mainly systemic lupus erythematosus (SLE) (4-13). Neurological manifestations in APS are common, including stroke, transient ischaemic attack (TIA), epilepsy, dementia, cognitive deficits, headaches, dementia, behavioural abnormalities, psychiatric disorders, seizures, chorea, multiple sclerosis-like, myelopathy, transverse myelitis and ocular symptoms, and may be associated with this syndrome in both the primary and secondary forms (4). Many of these manifestations are interrelated and may occur simultaneously in the same patient. Neurological disorders may result from vascular thrombotic events or without thrombotic events by direct injury to neuronal tissue (7). This spectrum of neurological disorders in patients with antiphospholipid antibodies is sometimes referred as the neuropsychiatric APS. The aim of this study was to observe and investigate the association between non-thrombotic neurological and cardiac manifestations, in our prospective study of APS patients. Differences between patients with primary APS and APS associated to other autoimmune diseases were also analysed. This study presents the first results from our national cohort. Materials and methods Our study includes a total of 333 antiphospholipid syndrome patients; 218 were primary APS patients (166 female and 52 male, mean age 45.8±13.7 years), 108 had APS associated with SLE (100 female and 8 male, mean age 46.9±15.8 years) and 7 patients had APS associated with Sjögren s syndrome (6 female and 1 male, mean age 50.1±15.9 years). Among these groups there were 14 patients with catastrophic APS (CAPS), who are in an international registry of patients with catastrophic APS (CAPS Registry), created in 2000 by the European Forum on Antiphospholipid Antibodies (14, 15). Our study is prospective. Patients with APS were included consecutively from 2000 until now. We investigated the association between non-thrombotic neurological and cardiac manifestations and we also followed other patients pathological features pulmonary, haematology and other and plan to report these results soon. All patients with SLE met the American College of Rheumatology (ACR) classification criteria (16). Disease activity was assessed at the time of enrolment in the study using of the SLEDAI score (17). Patients included in the study met the 1997 revised Sapporo criteria for APS (3). The study fulfills the ethical guidelines of the most recent declaration of Helsinki (Edinburgh, 2000) and has received approval from the local ethical committee. All patients were examined by council of rheumatologist, neurologist, neuroophthalmologist, psychiatrist, pulmonologist, cardiologist, radiologist and haematologist. Diagnosis of neurological manifestations was established by clinical findings, followed by: electroencephalography (EEG), nuclear magnetic resonance (NMR) of endocranium and in some cases of medulla, visual, somatosensory and acoustic evoked potentials, electromyoneurography imaging and neuropsychological testing. Cognitive and memory function were compared to the performance of 50 control patients who were comparable in age but showed no signs or symptoms of systemic disease. The diagnosis of non-stable angina pectoris was established according to the presence of chest pain, with or without ST segment and T wave ECG alterations and absence of elevated I troponin levels. In the setting of high troponin I levels with chest pain presence and/or ECG changes such as ST segment elevation or denivelation, we diagnosed 757
3 acute myocardial infarction (STEMI or NSTEMI). All enrolled patients underwent a transthoracic echocardiogram. Laboratory tests Lupus anticoagulant (LA) was based on the initial use of phospholipid-depleted or platelet-depleted coagulation tests, such as kaolin clotting time (KCT), dilute Russell s venom viper time (DRV- VT), the tissue thromboplastin inhibition test and diluted activated partial thromboplastin time. The LA tests were not performed while the patients were receiving anticoagulant therapy. Anticardiolipin (acl: IgG/IgM) and antiβ 2 glycoprotein I ( GPI: IgG/IgM) antibodies were measured by an enzymelinked immunosorbent assay (ELISA, Binding Site) and expressed in GPL or phospholipids (MPL) units (GPL-U and MPL-U). We also followed the revised laboratory criteria for antiphospholipid syndrome (19): Lupus anticoagulant present in plasma, on two or more occasions at least 12 weeks apart, detected according to the guidelines of the International Society on Thrombosis and Haemostasis Anticardiolipin antibody of IgG or IgM isotype, or both, in serum or plasma, present in medium or high titers (i.e. >40 GPL or MPL, or > 99th percentile) on two or more occasions, at least 12 weeks apart, measured by a standardised ELISA Anti- -gycoprotein 1 antibody of IgG or IgM isotype, or both, in serum or plasma (in titers > 99th percentile), present on two or more occasions, at least 12 weeks apart, measured by a standardised ELISA Antinuclear antibodies (ANA) were determined by indirect immunofluorescence on mouse liver and HEp-2 cell substrate. Anti-double-stranded DNA (anti-dsdna) antibodies were determined by ELISA, Binding Site. Table I. Distribution of apl in the patients with primary and APS associated to other autoimmune diseases. Statistics Results are presented as the mean SD, except for frequencies, which are expressed as percentages. Comparisons between groups were made by means of Mann-Whitney U-tests for continuous variables, and by chi-square analysis for categorical variables. For 2 by 2 tables Yates Correction for Continuity was used if necessary. Two-sided probability values <0.05 (2-tailed) were considered significant. All statistical analysis was performed with using SPSS version 16.0 statistical package. Results Distribution of apl in the patients with primary and APS associated to other autoimmune diseases is presented in Table I. It reveals that the presence of acl IgG antibodies was significantly more common (p=0.001) in patients with SAPS and the presence of LA was significantly more common (p=0.002) in patients with primary antiphospholipid syndrome (PAPS). There was no statistically significant association between the presences of other apl antibodies in either primary or secondary APS. PAPS n=218 SAPS n=115 p-value n (%) n (%) acl IgG 78 (35.8%) 62 (53.9%) acl IgM 118 (54.1%) 75 (65.2%) GPI IgG 76 (34.9%) 52 (45.2%) GPI IgM 75 (34.4%) 54 (46.6%) LA 122 (51.4%) 52 (45.2%) PAPS: primary antiphospholipid syndrome; SAPS: secondary antiphospholipid syndrome; acl: anticardiolipin antibodies; GPI: anti- glycoprotein I antibodies; LA: lupus anticoagulant; apl: antiphospholipid antibodies. Table II. Comparison of frequency of non-thrombotic neurological manifestations between patients with primary and APS aassociated to other autoimmune diseases. PAPS/ n=218 SAPS/ n=115 p-value n (%) n (%) Transient ischaemic attack 47 (21.6%) 31 (27%) Chorea 0 (0%) 9 (7.8%) Hemiballismus 0 (0%) 0 (0%) / Cerebellar ataxia 0 (0%) 0 (0%) / Epilepsy 11 (5%) 22 (19.1%) Migraine 61 (28%) 40 (34.8%) Transient global amnaesia 3 (1.4%) 2 (1.7%) Acute ischaemic encephalopathy 3 (1.4%) 5 (4.3%) Transverse myelopathy 0 (0%) 0 (0%) / Guillain-Barre syndrome 0 (0%) 0 (0%) / Anterior spinal artery syndrome 0 (0%) 1 (0.9%) Cephalea 52 (24%) 16 (13.9%) Vertigo 18 (8.3%) 4 (3.5%) Depression 8 (3.7%) 0 (0%) PAPS: primary antiphospholipid syndrome; SAPS: secondary antiphospholipid syndrome. According to gender, no association between gender and non-thrombotic neurological manifestations in PAPS or SAPS was noticed. The next step in our study was to compare the frequency of non-thrombotic neurological manifestations between patients with primary and secondary APS. Our study revealed that chorea (p<0.001), migraine (p=0.026) and epilepsy (p=0.001) occurred more often in patients with SAPS and headache (p=0.031) and depression (p=0.037) were more often in PAPS patients. Other non-thrombotic neurological manifestations occurred in both groups of patients without any statistically significant correlation (Table II). Furthermore, we analysed association between presence of apl antibodies with non-thrombotic neurological manifestations in both PAPS and SAPS group. Our study revealed statistical signifi- 758
4 Table III. Association between non-thrombotic neurological and cardiac manifestations in PAPS group. PAPS patients Transient ischaemic attack (n) Epilepsy (n) Transient global amnaesia (n) Depression (n) not present p not present p not present p not present p present present present present Non-stable not present angina pectoris present Valve vegetations not present present PAPS: primary antiphospholipid syndrome; n: number of patients. Table IV. Association between nonthrombotic neurological and cardiac manifestations in SAPS group. SAPS patients Transient ischaemic attack (n) Acute ischaemic encephalopathy (n) Vertigo (n) not present present p not present present p not present present p Non-stable angina not present pectoris (n) present SAPS: secondary antiphospholipid syndrome; n: number of patients. cance considering the presence of acl IgG and acute ischaemic encephalopathy (p=0.035) in SAPS group, acl IgM and epilepsy (p=0.030) in SAPS group, acl IgM and migraine (p=0.016) in PAPS, GPI IgG and chorea (p=0.041) in SAPS, GPI IgM and transient ischaemic attack (p=0.018) and epilepsy (p=0.036) in PAPS and the presence of LA and depression (p=0.012), transient global amnaesia (p=0.049) and migraine (p=0.036) in PAPS group. We also analysed the association between non-thrombotic neurological manifestations and non-thrombotic cardiac manifestations in both PAPS and SAPS group (Table III and IV). Patients who had unstable angina pectoris were more likely to develop transient ischaemic attack in both PAPS (p=0.002) and SAPS group (p=0.004), epilepsy (p=0.006) and transient global amnaesia (p=0.002) in PAPS and acute ischaemic encephalopathy (p=0.000) in SAPS. Patients with valve vegetations were more prone to epilepsy (p=0.001) and depression (p=0.002) in PAPS. Finally, no association between age, smoking habits or disease duration and non-thrombotic neurological manifestations in the PAPS or SAPS group was found. Discussion We present the first results from our prospective study with APS patients, which started in 2000, and performed at the University Medical Centre, Bezanijska Kosa, Belgrade, in collaboration with other clinical centres in Serbia. Besides frequent clinical manifestations of antiphospholipid syndrome, we followed less common, unusual and rare manifestations, according to Ruiz- Irastorza et al. (14). This is our first, national study which investigates the influence of antiphospholipid antibody type and level on non-thrombotic neurological manifestations, as well as the association between non-thrombotic neurological and cardiac manifestations in both PAPS and SAPS group of patients. We observed many non-thrombotic neurological manifestations, both in primary and in APS associated to other autoimmune diseases patients, and determined that some of them occurred significantly more often than others in both groups of APS patients: chorea, migraine and epilepsy occurred more often in patients with SAPS, and headache and depression were more often in PAPS patients. Migraine and transient ischaemic attack were the most common clinical findings in both groups, with total prevalence of 30.3% and 23.4% patients, respectively. The frequency of the most often neurological manifestations in our study group was comparable to data reported in previous studies (4, 7, 19). Our study revealed statistical significant difference between patients with primary and APS associated to other autoimmune diseases with respect to the presence of specific apl. acl IgG antibodies were statistically more frequent in patients with antiphospholipid syndrome associated to other autoimmune diseases and the presence of LA was significantly more common in patients with primary antiphospholipid syndrome (PAPS). This study also indicates that presence of certain types and levels of apl are associated with increased probability of some nonthrombotic neurological manifestations. We found statistical significance considering the presence of acl IgG and acute ischaemic encephalopathy in SAPS group, between presence of acl IgM and epilepsy in SAPS and acl IgM and migraine in PAPS group. There was a strong association between the presence of GPI IgG and chorea in SAPS, between GPI IgM and transient ischaemic attack and epilepsy in PAPS and between LA and depression, transient global amnaesia and migraine in PAPS. In this study we analysed the association between non-thrombotic neurological manifestations and cardiac manifestations in both the PAPS and SAPS group and found that patients with unstable angina pectoris were more likely to develop transient ischaemic attack in both the PAPS and SAPS group, epilepsy and transient global amnaesia in PAPS and acute ischaemic encephalopathy in SAPS. Patients with valve vegetations were more prone to epilepsy 759
5 and depression in PAPS. Krause et al. have shown a significant association between valvular heart disease and cerebrovascular manifestations not only stroke and TIAs, but also migraine and epilepsy (20). Our study confirmed that the presence of cardiac manifestations may be a risk factor for several types of CNS involvement in APS (21-40). Finally, we were looking for an association between gender, age and disease duration and neurological manifestations in both the PAPS and SAPS group, which has rarely been done in previous studies. Our study showed that gender, age, smoking habits and disease duration were not associated with nonthrombotic neurological manifestations in both PAPS and SAPS patients. In this study we did not track genetic markers responsible for thrombosis, but this will be part of our next study. In conclusion, we found that there is strong link between some non-thrombotic neurological and cardiac manifestations in APS patients, suggesting the complexity and evolutionary nature of APS. Acknowledgements We thank all the patients who participated in this study and our colleagues from many clinics in Serbia. References 1. PETRI M: Epidemiology of the antiphospholipid antibody syndrome. J Autoimmun 2000; 15: HUGHES GR: The antiphospholipid syndrome: ten years on. Lancet 1993; 342: WILSON WA, GHARAVI AE, KOIKE T et al.: International consensus statement on preliminary classification criteria for definite antiphospholipid syndrome: report of an international workshop. Arthritis Rheum 1999; 42: ARNSON Y, SHOENFELD Y, ALON E, AMI- TAL H: The antiphospholipid syndrome as a neurological disease. Semin Arthritis Rheum 2010; 40: BERTOLACCINI ML, KHAMASHTA MA, HUGHES GR: Diagnosis of antiphospholipid syndrome. Nat Clin Pract Rheumatol 2005; 1: ROTTEM M, KRAUSE I, FRASER A et al.: Autoimmune hemolytic anaemia in the antiphospholipid syndrome. Lupus 2006; 15: MAYER M, CEROVEC M, RADOS M, CIKES N: Antiphospholipid syndrome and central nervous system. Clin Neurol Neurosurg 2010; 112: STOJANOVICH L, ZADMAN-GODDARD G, PAVLOVICH S, SIKANOCH N: Psychiatric manifestations in systemic lupus erythematosus. Autoimmun Rev 2007; 6: CERVERA R, PIETTE JC, FONT J et al.: Antiphospholipid syndrome: clinical and immunologic manifestations and patterns of disease expression in a cohort of 1,000 patients. Arthritis Rheum 2002; 46: ERKAN D, ASHERSON RA, ESPINOSA G et al.: Long term outcome of catastrophic antiphospholipid syndrome survivors. Ann Rheum Dis 2003; 62: STOJANOVICH L, MILOVANOVICH B, de LUKA SR et al.: Cardiovascular autonomic dysfunction in systemic lupus, rheumatoid arthritis, primary Sjögren syndrome and other autoimmune diseases. Lupus 2007; 16: ASHERSON RA, CERVERA R: Antiphospholipid antibodies and infections. Ann Rheum Dis 2003; 62: CUADRADO MJ, KHAMASHTA MA, BALLES- TEROS A, GODFREY T, SIMON MJ, HUGHES GR: Can neurologic manifestations of Hughes (antiphospholipid) syndrome be distinguished from multiple sclerosis? Analysis of 27 patients and review of the literature. Medicine (Baltimore) 2000; 79: KAUL M: Catastrophic antiphospholipid syndrome (CAPS): update from the CAPS Registry. Cervera R; CAPS Registry Project Group. Lupus 2010; 19: STOJANOVICH L: The catastrophic antiphospholipid syndrome in Serbia: diagnostic and management problems. Clin Rev Allergy Immunol 2009; 36: TAN EM, COHEN AS, FRIES JF et al.: The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 1982; 25: PETRI M, BUYON J, SKOVRON ML et al.: Reliability of SELENA, SLEDAI and flare as clinical trial outcome measures. Arthritis Rheum 1998; 41: ZOGHBI WA, ENRIQUEZ-SARANO M, FOS- TER E et al.: Recommendations for evaluation of the severity of native valvular regurgitation with two-dimensional and Doppler echocardiography. J Am Soc Echocardiogr 2003; 16: RUIZ-IRASTORZA G, CROWTHER M, BRANCH W, KHAMASHTA MA: Antiphospholipid syndrome. Lancet 2010; 376: KRAUSE I, LEV S, FRASER A et al.: Close association between valvar heart disease and central nervous system manifestations in the antiphospholipid syndrome. Ann Rheum Dis 2005; 64: SHOENFELD Y, LEV S, BLATT I et al.: Features associated with epilepsy in the antiphospholipid syndrome. J Rheumatol 2004; 31: LEVINE SR, DEEGAN MJ, FUTRELL N, WELCH KM: Cerebrovascular and neurologic disease associated with antiphospholipid antibodies: 48 cases. Neurology 1990; 40: HUGHES GR: Migraine, memory loss, and multiple sclerosis. Neurological features of the antiphospholipid (Hughes ) syndrome. Postgrad Med J 2003; 79: CIMAZ R, MERONI PL, SHOENFELD Y: Epilepsy as part of systemic lupus erythematosus and systemic antiphospholipid syndrome (Hughes syndrome). Lupus 2006; 15: ZANDMAN-GODDARD G, CHAPMAN J, SHOENFELD Y: Autoantibodies involved in neuropsychiatric SLE and antiphospholipid syndrome. Semin Arthritis Rheum 2007; 36: AMITAL H, LANGEVITZ P, LEVY Y et al.: Valvular deposition of antiphospholipid antibodies in the antiphospholipid syndrome: a clue to the origin of the disease. Clin Exp Rheumatol 1999; 17: BIDOT CJ, HORSTMAN LL, JY W et al.: Clinical and neuroimaging correlates of antiphospholipid antibodies in multiple sclerosis: a preliminary study. BMC Neurol 2007; 7: TOURBAH A, CLAPIN A, GOUT O et al.: Systemic autoimmune features and multiple sclerosis: a 5-year follow-up study. Arch Neurol 1998; 55: ROLDAN JF, BREY RL: Neurologic manifestations of the antiphospholipid syndrome. Curr Rheumatol Rep 2007; 9: TEKTONIDOU MG, VARSOU N, KOTOULAS G, ANTONIOU A, MOUTSOPOULOS HM: Cognitive deficits in patients with antiphospholipid syndrome: association with clinical, laboratory, and brain magnetic resonance imaging findings. Arch Intern Med 2006; 166: SANNA G, D CRUZ D, CUADRADO MJ: Cerebral manifestations in the antiphospholipid (Hughes) syndrome. Rheum Dis Clin North Am 2006; 32: LEVINE S, JOSEPH R, D ANDREA G, WELCH KM: Migraine and the lupus anticoagulant. Case reports and review of the literature. Cephalalgia 1987; 7: SANNA G, BERTOLACCINI ML, CUADRADO MJ, KHAMASHTA MA, HUGHES GR: Central nervous system involvement in the antiphospholipid (Hughes) syndrome. Rheumatology (Oxford) 2003; 42: STOJANOVICH L, KONTIC M, DJOKOVIC A, ILIJEVSKI N, STANISAVLJEVIC N, MARISAV- LJEVIC D: Pulmonary events in antiphospholipid syndrome: influence of antiphospholipid antibody type and levels. Scand J Rheumatol 2012 May; 41: NARSHI CB, GILES IP, RAHMAN A: The endothelium: an interface between autoimmunity and atherosclerosis in systemic lupus erythematosus? Lupus 2011; 20: JARPA E, BABUL M, CALDERÓN J et al.: Common mental disorders and psychological distress in systemic lupus erythematosus are not associated with disease activity. Lupus 2011; 20: GOVONI M, BOMBARDIERI S, BORTOLUZZI A et al.; Italian Society of Rheumatology: Factors and comorbidities associated with first neuropsychiatric event in systemic lupus erythematosus: does a risk profile exist? A large multicentre retrospective cross-sectional study on 959 Italian patients. Rheumatology (Oxford) 2012; 51: KALASHNIKOVA LA, NASONOV EL, STO- JANOVICH L et al.: Sneddon s Syndrome and the primary antiphospholipid syndrome. Cerebrovasc Dis 1994; 4: HERNÁNDEZ-MOLINA G, ESPERICUETA- ARRIOLA G, CABRAL AR: The role of lupus anticoagulant and triple marker positivity as risk factors for rethrombosis in patients with primary antiphospholipid syndrome. Clin Exp Rheumatol 2013; 31: STOJANOVICH L, KONTIC M, DJOKOVIC A et al.: Association between systemic non-criteria APS manifestations and antibody type and level: results from the Serbian national cohort study. Clin Exp Rheumatol 2013; 31:
Antiphospholipid syndrome (APS) or Huges Syndrome
 Non-thrombotic Neurological and Cardiac Manifestations: In a Cohort of Serbian Patients with Primary and Secodary Antihosholiid Syndrome Ljudmila Stojanovich, Aleksandra Djokovic, Milica Kontic, Dusica
Non-thrombotic Neurological and Cardiac Manifestations: In a Cohort of Serbian Patients with Primary and Secodary Antihosholiid Syndrome Ljudmila Stojanovich, Aleksandra Djokovic, Milica Kontic, Dusica
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome
 Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome
 ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
Situaciones estresantes en el lupus
 Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Mortality in the Catastrophic Antiphospholipid Syndrome
 ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
T he antiphospholipid syndrome (APS) is a thrombophilic
 1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
Current View of the Treatment of Antiphospholipid Syndrome
 GROUPE HOSPITALIER PITIE SALPETRIERE Current View of the Treatment of Antiphospholipid Syndrome Pr Zahir AMOURA Department of Internal Medicine French National Reference center for SLE and APS Hôpital
GROUPE HOSPITALIER PITIE SALPETRIERE Current View of the Treatment of Antiphospholipid Syndrome Pr Zahir AMOURA Department of Internal Medicine French National Reference center for SLE and APS Hôpital
Key words: antiphospholipid syndrome, trombosis, pathogenesis
 26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
Central nervous system involvement in the antiphospholipid (Hughes) syndrome
 Rheumatology 2003;42:200 213 doi:10.1093/rheumatology/keg080, available online at www.rheumatology.oupjournals.org Review Central nervous system involvement in the antiphospholipid (Hughes) syndrome G.
Rheumatology 2003;42:200 213 doi:10.1093/rheumatology/keg080, available online at www.rheumatology.oupjournals.org Review Central nervous system involvement in the antiphospholipid (Hughes) syndrome G.
Prevalence of antiphospholipid auto antibodies in patients with thrombosis
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
Daniel Egan, MD April 13, 2012
 Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
ORIGINAL PAPERS. Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F. Abstract
 ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
ORIGINAL INVESTIGATION. Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings
 ORIGINAL INVESTIGATION Cognitive Deficits in Patients With Antiphospholipid Syndrome Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings Maria G. Tektonidou, MD; Natassa
ORIGINAL INVESTIGATION Cognitive Deficits in Patients With Antiphospholipid Syndrome Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings Maria G. Tektonidou, MD; Natassa
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
AN INTERESTING CASE OF RESPIRATORY DISTRESS. Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai
 AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
Systemic lupus erythematosus in 50 year olds
 Postgrad Med J (1992) 68, 440-444 The Fellowship of Postgraduate Medicine, 1992 Systemic lupus erythematosus in 50 year olds I. Domenech, 0. Aydintug, R. Cervera, M. Khamashta, A. Jedryka-Goral, J.L. Vianna
Postgrad Med J (1992) 68, 440-444 The Fellowship of Postgraduate Medicine, 1992 Systemic lupus erythematosus in 50 year olds I. Domenech, 0. Aydintug, R. Cervera, M. Khamashta, A. Jedryka-Goral, J.L. Vianna
The Antiphospholipid Syndrome
 The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
Keywords: apl, Hughes syndrome, pregnancy loss, prothrombin, thrombosis. Introduction
 Journal of Thrombosis and Haemostasis, 10: 2512 2518 DOI: 10.1111/jth.12014 ORIGINAL ARTICLE Clinical accuracy for diagnosis of antiphospholipid syndrome in systemic lupus erythematosus: evaluation of
Journal of Thrombosis and Haemostasis, 10: 2512 2518 DOI: 10.1111/jth.12014 ORIGINAL ARTICLE Clinical accuracy for diagnosis of antiphospholipid syndrome in systemic lupus erythematosus: evaluation of
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies
 Original Article Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies Col K Narayanan *, Col V Marwaha +, Col K Shanmuganandan #, Gp Capt S Shankar
Original Article Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies Col K Narayanan *, Col V Marwaha +, Col K Shanmuganandan #, Gp Capt S Shankar
A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid Antibody
 Journal of Rheumatic Diseases Vol. 22, No. 2, April, 2015 http://dx.doi.org/10.4078/jrd.2015.22.2.106 Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid
Journal of Rheumatic Diseases Vol. 22, No. 2, April, 2015 http://dx.doi.org/10.4078/jrd.2015.22.2.106 Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid
A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating Prophylaxis after Deep Vein Thrombosis- Pulmonary Embolism
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
Rituximab. B Cell Inhibition in APS. Methods. B Cell Inhibition in APS. Disclosure 11/6/2011
 Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Mohammadreza Tabatabaei IBTO COAG LAB
 Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus
 Original papers Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus Martyna Tomczyk-Socha 1, B E, Hanna Sikorska-Szaflik 2, B E, Marek Frankowski 3, B D, Karolina
Original papers Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus Martyna Tomczyk-Socha 1, B E, Hanna Sikorska-Szaflik 2, B E, Marek Frankowski 3, B D, Karolina
Neurological involvement in antiphospholipid antibodies syndrome (APS)
 European Review for Medical and Pharmacological Sciences Neurological involvement in antiphospholipid antibodies syndrome (APS) A. AMOROSO, A.P. MITTERHOFER, G.M. FERRI, S. GALLUZZO, M. VADACCA, A. AFELTRA
European Review for Medical and Pharmacological Sciences Neurological involvement in antiphospholipid antibodies syndrome (APS) A. AMOROSO, A.P. MITTERHOFER, G.M. FERRI, S. GALLUZZO, M. VADACCA, A. AFELTRA
ANTIPHOSPHOLIPID ANTIBODIES IN 57 CHILDREN AND ADOLESCENTS WITH SYSTEMIC LUPUS ERYTHEMATOSUS
 REV. HOSP. CLÍN. FAC. MED. S. PAULO 58(3):157-162, 2003 ANTIPHOSPHOLIPID ANTIBODIES IN 57 CHILDREN AND ADOLESCENTS WITH SYSTEMIC LUPUS ERYTHEMATOSUS Lúcia Maria de Arruda Campos, Maria Helena B. Kiss,
REV. HOSP. CLÍN. FAC. MED. S. PAULO 58(3):157-162, 2003 ANTIPHOSPHOLIPID ANTIBODIES IN 57 CHILDREN AND ADOLESCENTS WITH SYSTEMIC LUPUS ERYTHEMATOSUS Lúcia Maria de Arruda Campos, Maria Helena B. Kiss,
Available Online at CODEN: IJRSFP (USA) Vol. 9, Issue, 3(L), pp , March, 2018.
 ISSN: 0976-3031 Available Online at http://www.recentscientific.com CODEN: IJRSFP (USA) International Journal of Recent Scientific Research Vol. 9, Issue, 3(L), pp. 25504-25508, March, 2018 Research Article
ISSN: 0976-3031 Available Online at http://www.recentscientific.com CODEN: IJRSFP (USA) International Journal of Recent Scientific Research Vol. 9, Issue, 3(L), pp. 25504-25508, March, 2018 Research Article
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Thrombophilia. Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS
 Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Antiphospholipid Syndrome
 Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study
 Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience
 Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist
 Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Review Article. Catastrophic Antiphospholipid Syndrome. Introduction. Etiopathogenesis. Man-Chi Leung and Woon-Leung Ng
 Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome
 Original Article Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome Paula Gonçalves Perches¹, Daniela Pezzutti Domingues¹, Andréia Latanza Gomes², Augusta
Original Article Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome Paula Gonçalves Perches¹, Daniela Pezzutti Domingues¹, Andréia Latanza Gomes², Augusta
A ntiphospholipid antibodies (apl) are a group of
 1106 EXTENDED REPORT Anticardiolipin, anti-b 2 -glycoprotein I and antiprothrombin antibodies in black South African patients with infectious disease S Loizou, S Singh, E Wypkema, R A Asherson... See end
1106 EXTENDED REPORT Anticardiolipin, anti-b 2 -glycoprotein I and antiprothrombin antibodies in black South African patients with infectious disease S Loizou, S Singh, E Wypkema, R A Asherson... See end
Antiphospholipid Syndrome and Vascular Ischemic (Occlusive) Diseases: An Overview
 Yonsei Med J 48(6):901-926, 2007 DOI 10.3349/ymj.2007.48.6.901 Antiphospholipid Syndrome and Vascular Ischemic (Occlusive) Diseases: An Overview Penka A. Atanassova Department of Neurology, Medical University,
Yonsei Med J 48(6):901-926, 2007 DOI 10.3349/ymj.2007.48.6.901 Antiphospholipid Syndrome and Vascular Ischemic (Occlusive) Diseases: An Overview Penka A. Atanassova Department of Neurology, Medical University,
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience
 Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
Disclosures. Sneddon Syndrome: Untangling the Web. Case Presentation. MRI head w/ and w/o contrast. Further Workup. Further Workup 10/26/2017
 Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Central Nervous System (CNS) and Lupus: Learn from the Experts. Betty Diamond, M.D. Feinstein Institute for Medical Research
 Central Nervous System (CNS) and Lupus: Learn from the Experts Betty Diamond, M.D. Feinstein Institute for Medical Research Stages in SLE Pathogenesis Crow MK, Arth Res & Tx. 2009 ACR Criteria for the
Central Nervous System (CNS) and Lupus: Learn from the Experts Betty Diamond, M.D. Feinstein Institute for Medical Research Stages in SLE Pathogenesis Crow MK, Arth Res & Tx. 2009 ACR Criteria for the
Research Article Seizures in Primary Antiphospholipid Syndrome: The Relevance of Smoking to Stroke
 Hindawi Publishing Corporation Clinical and Developmental Immunology Volume 2012, Article ID 981519, 7 pages doi:10.1155/2012/981519 Research Article Seizures in Primary Antiphospholipid Syndrome: The
Hindawi Publishing Corporation Clinical and Developmental Immunology Volume 2012, Article ID 981519, 7 pages doi:10.1155/2012/981519 Research Article Seizures in Primary Antiphospholipid Syndrome: The
Thrombotic Risk Factors In Primary Antiphospholipid Syndrome A 5-Year Prospective Study
 Thrombotic Risk Factors In Primary Antiphospholipid Syndrome A 5-Year Prospective Study Maurizio Turiel, MD; Piercarlo Sarzi-Puttini, MD; Rossana Peretti, MD; Edoardo Rossi, MD; Fabiola Atzeni, MD; Wendy
Thrombotic Risk Factors In Primary Antiphospholipid Syndrome A 5-Year Prospective Study Maurizio Turiel, MD; Piercarlo Sarzi-Puttini, MD; Rossana Peretti, MD; Edoardo Rossi, MD; Fabiola Atzeni, MD; Wendy
Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus
 J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
å ORIGINAL ARTICLE å Distribution and Clinical Significance of Lupus Anticoagulant and Anticardiolipin Antibody in 349 Patients with
 å ORIGINAL ARTICLE å Distribution and Clinical Significance of Lupus Anticoagulant and Anticardiolipin Antibody in 349 Patients with Systemic Lupus Erythematosus Chiho Ninomiya, Osamu Taniguchi, Toshihiko
å ORIGINAL ARTICLE å Distribution and Clinical Significance of Lupus Anticoagulant and Anticardiolipin Antibody in 349 Patients with Systemic Lupus Erythematosus Chiho Ninomiya, Osamu Taniguchi, Toshihiko
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Sang Hyuk Park, 1,2 Seongsoo Jang, 3 Chan-Jeoung Park, 3 and Hyun-Sook Chi Introduction
 BioMed Research International Volume 2016, Article ID 2641526, 6 pages http://dx.doi.org/10.1155/2016/2641526 Research Article Clinical Application of Revised Laboratory Classification Criteria for Antiphospholipid
BioMed Research International Volume 2016, Article ID 2641526, 6 pages http://dx.doi.org/10.1155/2016/2641526 Research Article Clinical Application of Revised Laboratory Classification Criteria for Antiphospholipid
Serum lipids and anti-oxidized LDL antibodies in primary antiphospholipid syndrome
 Serum lipids and anti-oxidized LDL antibodies in primary antiphospholipid syndrome M. Bećarević 1, S. Andrejević 2, P. Miljić 3, B. Bonači-Nikolić 2, N. Majkić-Singh 1 1 Institute for Medical Biochemistry,
Serum lipids and anti-oxidized LDL antibodies in primary antiphospholipid syndrome M. Bećarević 1, S. Andrejević 2, P. Miljić 3, B. Bonači-Nikolić 2, N. Majkić-Singh 1 1 Institute for Medical Biochemistry,
Livedo reticularis is a marker for predicting multi-system thrombosis in antiphospholipid syndrome
 Livedo reticularis is a marker for predicting multi-system thrombosis in antiphospholipid syndrome E. Toubi 1, I. Krause 2,3, A. Fraser 3, S. Lev 3, L. Stojanovich 4, J. Rovensky 5, M. Blank 2, Y. Shoenfeld
Livedo reticularis is a marker for predicting multi-system thrombosis in antiphospholipid syndrome E. Toubi 1, I. Krause 2,3, A. Fraser 3, S. Lev 3, L. Stojanovich 4, J. Rovensky 5, M. Blank 2, Y. Shoenfeld
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Case Report Catastrophic Antiphospholipid Syndrome
 Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
CASE REPORT. Malgorzata Biernacka-Zielinska, Joanna Lipinska, Joanna Szymanska-Kaluza, Jerzy Stanczyk and Elzbieta Smolewska *
 Biernacka-Zielinska et al. Journal of Medical Case Reports 2013, 7:221 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Recurrent arterial and venous thrombosis in a 16- year-old boy in the course
Biernacka-Zielinska et al. Journal of Medical Case Reports 2013, 7:221 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Recurrent arterial and venous thrombosis in a 16- year-old boy in the course
Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu VK*; Singh H
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Testing strategies for diagnosing lupus anticoagulant: decision analysis Segal J B, Lehmann H P, Petri M, Mueller L, Kickler T S
 Testing strategies for diagnosing lupus anticoagulant: decision analysis Segal J B, Lehmann H P, Petri M, Mueller L, Kickler T S Record Status This is a critical abstract of an economic evaluation that
Testing strategies for diagnosing lupus anticoagulant: decision analysis Segal J B, Lehmann H P, Petri M, Mueller L, Kickler T S Record Status This is a critical abstract of an economic evaluation that
Antiphospholipid Antibody in Serum of Guillain-Barre Syndrome Patients
 Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 181-79 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ Antiphospholipid Antibody in Serum of Guillain-Barre Syndrome Patients
Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 181-79 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ Antiphospholipid Antibody in Serum of Guillain-Barre Syndrome Patients
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
February 2016, Volume: 8, Issue: 2, Pages: , DOI:
 Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Lupus Anticoagulants (LA), Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update. Antiphospholipid. Antiphospholipid
 , Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
, Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
Systemic Lupus Erythematosus
 Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Antiphospholipid Antibody Testing: Which Are Most Useful for Diagnosis?
 Rheum Dis Clin N Am 32 (2006) 455 463 Antiphospholipid Antibody Testing: Which Are Most Useful for Diagnosis? Maria Laura Bertolaccini, MD, PhD*, Graham R.V. Hughes, MD, FRCP Lupus Research Unit, The Rayne
Rheum Dis Clin N Am 32 (2006) 455 463 Antiphospholipid Antibody Testing: Which Are Most Useful for Diagnosis? Maria Laura Bertolaccini, MD, PhD*, Graham R.V. Hughes, MD, FRCP Lupus Research Unit, The Rayne
Lupus as a risk factor for cardiovascular disease
 Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Antiphospholipid antibodies
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
Lymphocytopenia is associated with anti-beta-2 glycoprotein-1 in patients with systemic lupus erythematosus
 ARTIGO ORIGINAL Lymphocytopenia is associated with anti-beta-2 glycoprotein-1 in patients with systemic lupus erythematosus Skare T 1, Borba EA 1, Utiyama SR 2, Nisihara R 3 ACTA REUMATOL PORT. 2016;41:220-225
ARTIGO ORIGINAL Lymphocytopenia is associated with anti-beta-2 glycoprotein-1 in patients with systemic lupus erythematosus Skare T 1, Borba EA 1, Utiyama SR 2, Nisihara R 3 ACTA REUMATOL PORT. 2016;41:220-225
PURPOSE SCIENTIFIC QUESTIONS. How the prevalence of the nine different apl varies among the different age groups of patients with SLE?
 Project plan The prevalence of IgG, IgM, and IgA antibodies against cardiolipin, β2-glycoprotein I and domain I of β2-glycoprotein I in a large cohort of patients with Systemic Lupus Erythematosus and
Project plan The prevalence of IgG, IgM, and IgA antibodies against cardiolipin, β2-glycoprotein I and domain I of β2-glycoprotein I in a large cohort of patients with Systemic Lupus Erythematosus and
SLE and the Antiphospholipid Syndrome
 SLE and the Antiphospholipid Syndrome Susan Y. Ritter MD, PhD Associate Physician Division of Rheumatology, Immunology and Allergy Department of Medicine Brigham and Women s Hospital Instructor in Medicine
SLE and the Antiphospholipid Syndrome Susan Y. Ritter MD, PhD Associate Physician Division of Rheumatology, Immunology and Allergy Department of Medicine Brigham and Women s Hospital Instructor in Medicine
Images in Cardiovascular Medicine
 Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
Clinical consequences of antiphospholipid antibodies
 Clinical consequences of antiphospholipid antibodies R.H.W.M. Derksen 1*, P.G. de Groot 2,3 1 Department of Rheumatology and Clinical Immunology, Room F02.127, 2 Thrombosis and Haemostasis Laboratory,
Clinical consequences of antiphospholipid antibodies R.H.W.M. Derksen 1*, P.G. de Groot 2,3 1 Department of Rheumatology and Clinical Immunology, Room F02.127, 2 Thrombosis and Haemostasis Laboratory,
INTRODUCTION: Systemic lupus erythematosus (SLE) is the most common multisystemic autoimmune connective tissue disease
 THE SYSTEMIC IRAQI POSTGRADUATE LUPUS ERYTHEMATOSUS MEDICAL JOURNAL Cardiovascular Autonomic Nervous System Dysfunction in Iraqi Systemic Lupus Erythematosus Patients Ziad Shafeek Al-Rawi*, Nizar Abdul
THE SYSTEMIC IRAQI POSTGRADUATE LUPUS ERYTHEMATOSUS MEDICAL JOURNAL Cardiovascular Autonomic Nervous System Dysfunction in Iraqi Systemic Lupus Erythematosus Patients Ziad Shafeek Al-Rawi*, Nizar Abdul
Antiphospholipid Syndrome ( APS)
 Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
The meaning of MSCT angiography in early detection of visceral arterial lesions in patients with antiphospholipid syndrome
 The meaning of MSCT angiography in early detection of visceral arterial lesions in patients with antiphospholipid syndrome Authors: Jovica Saponjski, Ljudmila Stojanovich, Jelena Petrovic, Dusan Saponjski*
The meaning of MSCT angiography in early detection of visceral arterial lesions in patients with antiphospholipid syndrome Authors: Jovica Saponjski, Ljudmila Stojanovich, Jelena Petrovic, Dusan Saponjski*
The antiphospholipid syndrome: a large elephant with many parts or an elusive chameleon disguised by many colours?
 Autoimmun Highlights (2010) 1:5 14 DOI 10.1007/s13317-010-0003-7 REVIEW ARTICLE The antiphospholipid syndrome: a large elephant with many parts or an elusive chameleon disguised by many colours? Emmanuel
Autoimmun Highlights (2010) 1:5 14 DOI 10.1007/s13317-010-0003-7 REVIEW ARTICLE The antiphospholipid syndrome: a large elephant with many parts or an elusive chameleon disguised by many colours? Emmanuel
PSYCHIATRIC MANIFESTATIONS IN PEDIATRIC SLE PATIENTS AT SIRIRAJ HOSPITAL BANGKOK, THAILAND
 PSYCHIATRIC MANIFESTATIONS IN PEDIATRIC SLE PATIENTS AT SIRIRAJ HOSPITAL BANGKOK, THAILAND Sasitorn Chantaratin, Prae Wongtangman, Sudrat Sirisakpanit and Vitharon Boon-yasidhi Division of Child and Adolescent
PSYCHIATRIC MANIFESTATIONS IN PEDIATRIC SLE PATIENTS AT SIRIRAJ HOSPITAL BANGKOK, THAILAND Sasitorn Chantaratin, Prae Wongtangman, Sudrat Sirisakpanit and Vitharon Boon-yasidhi Division of Child and Adolescent
Review Article Rheumatic Fever Associated with Antiphospholipid Syndrome: Systematic Review
 Immunology Research, Article ID 614591, 6 pages http://dx.doi.org/10.1155/2014/614591 Review Article Rheumatic Fever Associated with Antiphospholipid Syndrome: Systematic Review Felipe da Silva 1 and Jozélio
Immunology Research, Article ID 614591, 6 pages http://dx.doi.org/10.1155/2014/614591 Review Article Rheumatic Fever Associated with Antiphospholipid Syndrome: Systematic Review Felipe da Silva 1 and Jozélio
ANTICARDIOLIPIN ANTIBODIES IN PATIENTS WITH SYSTEMIC LUPUS ERYTHEMATOSUS
 382 ANTICARDIOLIPIN ANTIBODIES IN PATIENTS WITH SYSTEMIC LUPUS ERYTHEMATOSUS GUNNAR STURFELT, OLA NIVED, RENEE NORBERG, RIGMOR THORSTENSSON, and KATARINA KROOK We studied a group of 59 unselected patients
382 ANTICARDIOLIPIN ANTIBODIES IN PATIENTS WITH SYSTEMIC LUPUS ERYTHEMATOSUS GUNNAR STURFELT, OLA NIVED, RENEE NORBERG, RIGMOR THORSTENSSON, and KATARINA KROOK We studied a group of 59 unselected patients
Catastrophic antiphospholipid syndrome: how to diagnose a rare but highly fatal disease
 502919TAB5610.1177/1759720X13502919Therapeutic Advances in Musculoskeletal DiseaseCL Aguiar and D Erkan 2013502919 Therapeutic Advances in Musculoskeletal Disease Review Catastrophic antiphospholipid syndrome:
502919TAB5610.1177/1759720X13502919Therapeutic Advances in Musculoskeletal DiseaseCL Aguiar and D Erkan 2013502919 Therapeutic Advances in Musculoskeletal Disease Review Catastrophic antiphospholipid syndrome:
World Journal of Pharmaceutical Research
 World Journal of Pharmaceutical research Al-Aubaidy et al. Volume 3, Issue 2, XXX-XXX. Research Article ISSN 2277 7105 RESPONSE OF ANTI-CARDIOLIPIN ANTIBODIES TO VARIOUS TREATMENT MODALITIES IN GUILLAIN
World Journal of Pharmaceutical research Al-Aubaidy et al. Volume 3, Issue 2, XXX-XXX. Research Article ISSN 2277 7105 RESPONSE OF ANTI-CARDIOLIPIN ANTIBODIES TO VARIOUS TREATMENT MODALITIES IN GUILLAIN
Case Report Antiphospholipid Syndrome: Multiple Manifestations in a Single Patient A High Suspicion Is Still Needed
 Hindawi Case Reports in Medicine Volume 2017, Article ID 5797041, 4 pages https://doi.org/10.1155/2017/5797041 Case Report Antiphospholipid Syndrome: Multiple Manifestations in a Single Patient A High
Hindawi Case Reports in Medicine Volume 2017, Article ID 5797041, 4 pages https://doi.org/10.1155/2017/5797041 Case Report Antiphospholipid Syndrome: Multiple Manifestations in a Single Patient A High
Antiphospholipid antibodies in patients with venous thrombosis at Kenyatta National Hospital
 Research article Department of Human Pathology, School of Medicine, University of Nairobi, P. O. Box 19676 00202, Nairobi, Kenya Corresponding author: Dr KA Barasa, Department of Human Pathology, School
Research article Department of Human Pathology, School of Medicine, University of Nairobi, P. O. Box 19676 00202, Nairobi, Kenya Corresponding author: Dr KA Barasa, Department of Human Pathology, School
Late onset systemic lupus erythematosus in southern Chinese. Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p.
 Title Late onset systemic lupus erythematosus in southern Chinese Author(s) Ho, CTK; Mok, CC; Lau, CS; Wong, RWS Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p. 437-440 Issued Date 1998
Title Late onset systemic lupus erythematosus in southern Chinese Author(s) Ho, CTK; Mok, CC; Lau, CS; Wong, RWS Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p. 437-440 Issued Date 1998
Antiphospholipid antibodies are a heterogeneous family
 Seasonal Distribution of Antiphospholipid Antibodies Thanh-Ha Luong, MD; Jacob H. Rand, MD; Xiao-Xuan Wu, MD; James H. Godbold, PhD; Mayra Gascon-Lema, MS; Stanley Tuhrim, MD Background and Purpose The
Seasonal Distribution of Antiphospholipid Antibodies Thanh-Ha Luong, MD; Jacob H. Rand, MD; Xiao-Xuan Wu, MD; James H. Godbold, PhD; Mayra Gascon-Lema, MS; Stanley Tuhrim, MD Background and Purpose The
PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE
 Autoimmune Disorders in Gynecology/Obstetrics PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE Abstract The spectrum
Autoimmune Disorders in Gynecology/Obstetrics PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE Abstract The spectrum
Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study.
 1. Title Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study. 2. Background Systemic Lupus Erythematosus (SLE) is a chronic, autoimmune and
1. Title Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study. 2. Background Systemic Lupus Erythematosus (SLE) is a chronic, autoimmune and
ANTI-PHOSPHATIDYLSERINE ANTIBODIES IN ACUTE MYOCARDIAL INFARCTION
 American Journal of Immunology 9 (4): 96-100, 2013 ISSN: 1553-619X 2013 Science Publication doi:10.3844/ajisp.2013.96.100 Published Online 9 (4) 2013 (http://www.thescipub.com/aji.toc) ANTI-PHOSPHATIDYLSERINE
American Journal of Immunology 9 (4): 96-100, 2013 ISSN: 1553-619X 2013 Science Publication doi:10.3844/ajisp.2013.96.100 Published Online 9 (4) 2013 (http://www.thescipub.com/aji.toc) ANTI-PHOSPHATIDYLSERINE
Phospholipid Screen IgG/IgM ELISA Kit
 Phospholipid Screen IgG/IgM ELISA Kit Catalog Number KA1109 96 assays Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle
Phospholipid Screen IgG/IgM ELISA Kit Catalog Number KA1109 96 assays Version: 03 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle
Original Article. Abstract
 Original Article Diagnostic accuracy of antinuclear antibodies and anti-double stranded DNA antibodies in patients of systemic lupus erythematosus presenting with dermatological features Attiya Tareen*,
Original Article Diagnostic accuracy of antinuclear antibodies and anti-double stranded DNA antibodies in patients of systemic lupus erythematosus presenting with dermatological features Attiya Tareen*,
Neurological manifestations of antiphospholipid syndrome
 DOI: 10.1111/j.1365-2362.2010.02263.x REVIEW Neurological manifestations of antiphospholipid syndrome Carlos E. M. Rodrigues *, Jozélio F. Carvalho * and Yehuda Shoenfeld,1 * University of São Paulo, São
DOI: 10.1111/j.1365-2362.2010.02263.x REVIEW Neurological manifestations of antiphospholipid syndrome Carlos E. M. Rodrigues *, Jozélio F. Carvalho * and Yehuda Shoenfeld,1 * University of São Paulo, São
Supplemental Figures and Legends
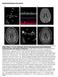 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Conflict of Interest. Systemic Lupus Erythematosus and the Antiphospholipid Syndrome Bonnie L. Bermas, MD Brigham and Women s Hospital.
 Systemic Lupus Erythematosus and the Antiphospholipid Syndrome Bonnie L. Bermas, MD Brigham and Women s Hospital Conflict of Interest Disclosures: None Overview Diagnostic Classification Criteria of SLE
Systemic Lupus Erythematosus and the Antiphospholipid Syndrome Bonnie L. Bermas, MD Brigham and Women s Hospital Conflict of Interest Disclosures: None Overview Diagnostic Classification Criteria of SLE
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care AF symptoms Tachycardia
 Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Antiphospholipid. Syndrome. Ricard Cervera Margarita Rodríguez-Mahou
 Antiphospholipid Syndrome Ricard Cervera Margarita Rodríguez-Mahou Antiphospholipid Syndrome Ricard Cervera Department of Autoimmune Diseases Barcelona Hospital Margarita Rodríguez-Mahou Autoimmunity
Antiphospholipid Syndrome Ricard Cervera Margarita Rodríguez-Mahou Antiphospholipid Syndrome Ricard Cervera Department of Autoimmune Diseases Barcelona Hospital Margarita Rodríguez-Mahou Autoimmunity
TECHNICAL SERIES. Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss. ...Setting trends TULIP DIAGNOSTICS (P) LTD.
 For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
The Power of the ANA. April 2018 Emily Littlejohn, DO MPH
 Emergent Rheumatologic Diseases and Disorders for Primary Care. The Power of the ANA April 2018 Emily Littlejohn, DO MPH Question 1: the ANA test is: A) A screening test with high specificity to diagnose
Emergent Rheumatologic Diseases and Disorders for Primary Care. The Power of the ANA April 2018 Emily Littlejohn, DO MPH Question 1: the ANA test is: A) A screening test with high specificity to diagnose
Catastrophic antiphospholipid syndrome: first signs in the neonatal period
 DOI 10.1007/s00431-011-1548-9 SHORT REPORT Catastrophic antiphospholipid syndrome: first signs in the neonatal period Marta Cabral & Clara Abadesso & Marta Conde & Helena Almeida & Helena Carreiro Received:
DOI 10.1007/s00431-011-1548-9 SHORT REPORT Catastrophic antiphospholipid syndrome: first signs in the neonatal period Marta Cabral & Clara Abadesso & Marta Conde & Helena Almeida & Helena Carreiro Received:
