Pediatric Chiari malformation type I: Long term outcomes following small bone window posterior fossa decompression with autologous fascia duraplasty
|
|
|
- Lucas Gibson
- 5 years ago
- Views:
Transcription
1 5652 Pediatric Chiari malformation type I: Long term outcomes following small bone window posterior fossa decompression with autologous fascia duraplasty HAI LIU *, CHENLONG YANG *, JUN YANG and YULUN XU Department of Neurosurgery, China National Clinical Research Center for Neurological Diseases, Beijing Tiantan Hospital, Capital Medical University, Beijing , P.R. China Received February 28, 2016; Accepted March 3, 2017 DOI: /etm Abstract. Chiari malformation type I (CM I) is a common hindbrain disorder that is associated with deformity and elongation of the cerebellar tonsils. Although CM I occurs in both pediatric and adult patients, its prevalence, clinical features and management in the pediatric population are not well defined. The current study evaluated a consecutive case series of 92 children (38 females and 54 males) who were diagnosed with congenital CM I. All patients underwent small bone window posterior fossa decompression with autologous fascia duraplasty. Clinical and radiological features were analyzed and long term follow up data were recorded. Risk factors associated with clinical outcomes were investigated using comprehensive statistical methods. Out of the 92 children, 11 (12.0%) were asymptomatic. Associated ventricular dilation was observed in 24 children (26.1%) and concomitant syringomyelia was observed in 72 children (78.3%). A total of 44 children (47.8%) showed scoliosis on plain films. Follow up data (mean duration, 88.6 months) were available for all patients. Syringomyelia was absent or markedly reduced in 56 patients (77.8%). Symptoms were alleviated in 66 patients, remained unchanged in 12 patients and progressed in 3 patients. Statistical analysis indicated that the cerebellar tonsillar descent (CTD) grade, basilar invagination and platybasia influenced the clinical outcome (P<0.05). In conclusion, early recognition and surgical treatment of CM I in pediatric patients can lead to good outcomes. The Correspondence to: Professor Yulun Xu, Department of Neurosurgery, China National Clinical Research Center for Neurological Diseases, Beijing Tiantan Hospital, Capital Medical University, 6 Tiantan Xili, Beijing , P.R. China E mail: xuhuxi@sina.com * Contributed equally Key words: Chiari malformation type I, cerebellar tonsil herniation, pediatrics, scoliosis, small bone window, posterior fossa decompression current results suggested that small bone window posterior fossa decompression with autologous fascia duraplasty was an effective safe treatment option with a low complication rate. High CTD grade, basilar invagination and platybasia were indicated to be predictors of poor clinical prognosis. Introduction Chiari malformation (CM) is a hindbrain disorder that is associated with deformity and elongation of the cerebellar tonsils. It is specifically characterized by the descent of the cerebellar tonsils >5 mm below the foramen magnum into the spinal canal (1,2). CM can be divided into four types, among which CM type I (CM I) is the most common. Although CM I occurs in pediatric and adult patients, the prevalence of CM I is not well defined (2). CM I often becomes clinically apparent when the patient is aged Thus, in the past, CM I had been diagnosed primarily during adolescence or adulthood (2,3). With the advent of magnetic resonance imaging (MRI), however, the number of pediatric patients diagnosed with CM I is increasing (4). Previous studies have described the clinical features of CM I in pediatric populations (2,5,6). CM I is usually associated with ventricular dilation, syringomyelia and scoliosis, but the relevant pathogenesis is not clearly understood. Moreover, the incidence of these conditions co presenting with CM I has varied considerably in previous studies (7 10). Management of CM I and concomitant syringomyelia and scoliosis in children remains controversial. Some authors have recommended syringoperitoneal shunting for treating syringomyelia (11,12). The treatment of scoliosis consists of serial observation, bracing and/or corrective spinal surgery. It is yet to be established whether aggressive surgical treatment is necessary, and the ideal therapeutic option is undetermined (13). It is widely accepted, however, that posterior fossa decompression should be included in the treatment protocol for CM I as it can lead to both clinical and radiological improvement (8,14,15). The use of specific surgical procedures and related issues, however, remain controversial; these include the use of craniectomy, the size of the bone window, whether the arachnoid should be opened and whether a cerebellar tonsil should be manipulated (14,15).
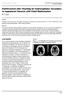
2 LIU et al: PEDIATRIC CM-I: LONG-TERM OUTCOMES FOLLOWING POSTERIOR FOSSA DECOMPRESSION 5653 The current study evaluated a consecutive case series of 92 children who were diagnosed with CM I. Their clinical manifestations, concomitant ventricular dilation, syringomyelia, basilar invagination, platybasia and scoliosis were analyzed. The study also evaluated the surgical outcomes of small bone window posterior fossa decompression (SPFD) with autologous fascia duraplasty (AFD) in the treatment of pediatric CM I. Patients and methods Patient recruitment. A search of medical records was conducted to identify pediatric patients (aged 0 18 years at their initial presentation to the neurosurgery clinic) with CM I who had been operated on in the Department of Neurosurgery at Beijing Tiantan Hospital, Capital Medical University (Beijing, China). The cohort included 92 children (female:male ratio, 1.00:1.42; mean age ± standard deviation, 10.0±4.5) with congenital CM I who were treated with SPFD + AFD between January 2001 and January CM I was diagnosed according to the following criteria (1): i) Herniation of tonsils 5 mm was below the plane of the foramen magnum; or ii) tonsillar herniation of 3 5 mm accompanied by other CM I features, such as syringomyelia. Exclusion criteria were as follows: i) Occipitocervical instability; ii) congenital spinal bifida; iii) diastematomyelia; iv) concurrent intraspinal tumors or myelitis; v) acquired CM I as a complication of cerebrospinal fluid (CSF) diversion procedures or chronic CSF leakage; and vi) incomplete data. The study protocol was approved by the Institutional Review Board and Ethics Committee of Beijing Tiantan Hospital, Capital Medical University. Clinical presentation. Subjective clinical symptoms and physical examinations were documented. Symptoms recorded included headache, foramen magnum nerve compression symptoms (occipitocervical headaches, neck or shoulder pain), sensory disturbance, motor dysfunction (weakness or muscle atrophy), lower cranial nerve dysfunction (dysphagia, hoarseness or coughing), cerebellar syndrome (truncal and appendicular ataxia) and scoliosis. Some patients also had bradycardia. Following the exclusion of endocrine dysfunction and organic heart disease by comprehensive evaluations, including laboratory, electrophysiological and radiological examinations, these symptoms were suspected to be associated with CM I or with concomitant syringomyelia. Imaging. Preoperative plain radiographs and perioperative MRI scans of the cervical spine were available for all patients. The descending distance between the inferior pole of the cerebellar tonsil and the level of the foramen magnum was measured on sagittal T1 weighted images in a picture archiving and communication system workstation (OsiriX software; version 6.0; Pixmeo SARL, Bernex, Switzerland). The degree of cerebellar descent was classified into three groups according to the cerebellar tonsillar descent (CTD) grading system (16): Grade I, the tonsil descends over the foramen magnum but does not reach the C1 arch; Grade II, the tonsil descends to the C1 arch level; and Grade III, the tonsil descends below the C1 arch. The location of the syringomyelia was determined on sagittal MRI images, and its size was determined by measuring the longitudinal and transverse diameters. The data for concomitant scoliosis were collected from standing posteroanterior radiographs (Fig. 1), and coronal curvature measurements were performed according to the Cobb method (17). Scoliosis was defined as a Cobb's angle of 10. Curve severity was defined as follows: mild, ; moderate, ; severe, 41. In cases of S shaped scoliosis, the major curve was selected for analysis and the minor curves were considered compensatory. Other associated abnormalities were also recorded, such as ventricular dilation, platybasia and basilar invagination. Ventricular dilation was defined by an Evans' index of >0.30 (18). Surgical approach. Surgery was performed on all children with a combined strategy that included SPFD and AFD. After patients were positioned left laterally, a posterior midline skin incision was made from 1 cm below the inion to the spinous process of C4. An autologous graft (2x2 cm) was resected from the fascia and reserved. The SPFD procedure, which included a small bone window suboccipital craniectomy (diameter, cm) and C 1 laminectomy (1.5 cm), was performed. The thick constraining dural band found at the occipitocervical junction was resected. When the dura mater was opened, the surgeon aimed to keep the arachnoid intact. The dura mater was subsequently grafted with the autologous graft to enlarge the cisterna magna. Six children presented with progressive hydrocephalus and severe intracranial hypertension, and an emergency ventriculoperitoneal shunt was implanted in these cases (Fig. 2). Follow up. Follow up data for all children were available in their records. The data had been obtained during individual office visits or telephone interviews, with a mean follow up time of 88.6 months (standard deviation, 46.2; range, months). Clinical outcomes were qualitatively categorized as follows: i) Improved, the patients experienced partial or complete relief of their chief complaints; or ii) not improved, no notable change in their chief complaints, or deterioration of their clinical status. Furthermore, the clinical outcomes were quantitatively evaluated according to the Chicago Chiari Outcome Scale (CCOS; Table I) (19). Statistical analysis. SPSS 22.0 software (IBM SPSS, Armonk, NY, USA) was used for statistical analyses. Chi squared test, continuity correction test or Fisher's exact probability test were used to screen the potential risk factors, including age at onset, age at diagnosis, sex, duration of symptoms, CTD grades, concomitant syringomyelia, hydrocephalus, basilar invagination, platybasia and scoliosis. Logistic regression analysis was performed to identify the risk factors for clinical outcomes (binary classification qualitative data). Furthermore, to verify the association between potential risk factors and clinical outcomes, CCOS scores (continuous variables) were compared using one way analysis of variance (ANOVA) with a Bonferroni post hoc test test for multi group comparisons and Mann Whitney U test for two group comparison. P 0.05 was considered to indicate a statistically significant significance.
3 5654 Table I. Chicago Chiari outcome scale. Score Characteristic Pain Worse Unchanged and refractory Improved or controlled Resolved to medication with medication Non pain Worse Unchanged or improved Improved and unimpaired Resolved but impaired Functionality Unable to attend Moderate impairment Mild impairment Fully functional (<50% attendance) (>50% attendance) Complication Persistent complication, Persistent complication, Transient complication Uncomplicated course poorly controlled well controlled Figure 1. Plain radiographs of 3 pediatric patients with scoliosis. (A) Right thoracic curve and ventriculoperitoneal shunt. Cobb's angle is 32. (B) Left thoracic curve, with a Cobb's angle of 40. (C) Right thoracic curve, with a Cobb s angle of 47. R, right hand side of the patient. Figure 2. Preoperative sagittal MRI scans of a female patient. (A) T1 weighted and (B) T2 weighted MRI scans indicate tonsillar herniation and a cervicothoracic syringomyelia. This patient's scoliosis is presented in Fig. 1A. (C) On admission, a head computed tomography scan indicated hydrocephalus. (D) An emergency ventriculoperitoneal shunt was implanted. MRI, magnetic resonance imaging. Results Patient population and clinical characteristics. Over the 14 year span of this study, 98 pediatric patients were diagnosed with CM I and underwent SPFD + AFD. Six patients were lost to follow up and excluded. This case series consisted of 38 females and 54 males, with a female:male ratio of 1.00:1.42. The average age at the time of surgery was 10.0±4.5 years (range, 1 18 years). In total, 11 (12.0%) children were asymptomatic. In the symptomatic group (n=81), the duration of symptoms preceding the initial diagnosis ranged from 2 weeks to 4 years (mean, 16.8 months). A total of 59 children presented with headache (72.8% of all symptomatic children), 17 with foramen magnum nerve compression symptoms (21.0%), 29 with sensory disturbance (35.8%), 36 with motor dysfunction (44.4%), 7 with lower cranial nerve dysfunction (8.6%) and 16 with cerebellar syndrome (19.8%). In addition, the results of electrocardiography, which is performed routinely upon
4 LIU et al: PEDIATRIC CM-I: LONG-TERM OUTCOMES FOLLOWING POSTERIOR FOSSA DECOMPRESSION 5655 Table II. Characteristics of coexisting scoliosis. Characteristic Number Percentage (%) Sex Male Female Curve type C shaped thoracic scoliosis S shaped thoracic scoliosis S shaped thoracolumbar scoliosis Curve orientation Convex to the left Convex to the right Severity Mild (10 25 ) Moderate (26 40 ) Severe (>41 ) Total Figure 3. Sagittal T1 weighted MRI scans of a male patient. (A) A preoperative MRI scan indicates tonsillar herniation. During the follow up period, the patient's symptoms were unchanged. (B) A follow up MRI scan indicates suboccipital hydrops. MRI, magnetic resonance imaging. admission, indicated that 4 patients had atrioventricular block (3 patients with second degree and 1 patient with third degree block), with no relevant underlying disease detected. None of the children complained of bowel or bladder dysfunction. Preoperative MRI. The distance of tonsillar herniation ranged from 6.0 to 18.4 mm (mean, 11.2±3.2 mm). On the preoperative MRI, platybasia was observed in 5 children (5.4%) and basilar invagination in 12 children (13.0%). Associated ventricular dilation was observed in 24 children (26.1%). Concomitant syringomyelia was observed in 72 children (78.3%): Cervical syringomyelia (n=4; 5.6% of concomitant syringomyelia cases), cervicothoracic syringomyelia (n=67; 93.0%) and holocord syringomyelia (n=1; 1.4%). Scoliosis evaluation. A total of 44 children (47.8%; 19 females and 25 males) showed scoliosis on plain films: 35 children had C shaped thoracic scoliosis in a single curve; 8 children had S shaped thoracic scoliosis with two adjacent curves; and 1 child had S shaped thoracolumbar scoliosis. According to the severity classification, 26 children were diagnosed with mild scoliosis, 12 with moderate scoliosis and 6 with severe scoliosis. Further analysis indicated that all children with scoliosis had concomitant syringomyelia. In total, 36 (81.8%) of the children with scoliosis also had a unilateral sensory disturbance and/or motor disturbance or unilateral muscle atrophy. These data are summarized in Table II. Complications and follow up. There were no deaths in this series. Central nervous system infection occurred postoperatively in four children. Antibiotics were prescribed and the infections were effectively treated. Suboccipital hydrops was noted in two children (Fig. 3). During the follow up period, Figure 4. Sagittal MRI scans of a female patient. Preoperative sagittal (A) T1 weighted and (B) T2 weighted MRI scans reveal tonsillar herniation and cervicothoracic syringomyelia. The patient's scoliosis is presented in Fig. 1B. (C and D) Immediately postoperative MRI scans indicate reconstruction of the cisterna magna and an upward shift of the tonsils, but no marked change in the syringomyelia. (E and F) Follow up MRI scans at 6 months after small bone window posterior fossa decompression with autologous fascia duraplasty indicate a marked reduction of the syringomyelia. MRI, magnetic resonance imaging; T1WI, T1 weighted image; T2WI, T2 weighted image. symptoms were alleviated in 66 patients (81.5% of all the symptomatic children), remained unchanged in 12 patients (14.8%) and progressed in 3 patients (3.7%). Preoperatively, 72 patients had concomitant syringomyelia. According to follow up MRI scans, syringomyelia was absent or markedly reduced in 56 of these patients (77.8%; Fig. 4). Analysis of these results using Chi squared tests indicated that CTD grades and the incidence of basilar invagination (Fig. 5) and platybasia were associated with clinical outcomes (P<0.05); the statistical data are summarized in Table III. Logistic regression analysis indicated that a high CTD grade [P=0.016; odds ratio (OR)=3.675; 95% confidence interval (CI), ], basilar invagination (P=0.008; OR=3.489; 95% CI, ) or platybasia (P=0.002; OR=3.981;
5 5656 Table III. Results of Chi squared tests. Chi square Characteristic value P value Age at onset (<10 vs. >10 years) Age at diagnosis (<10 vs. >10 years) Sex (male vs. female) Duration (<16.8 vs. >16.8 months) CTD (Grade I III) Syringomyelia (present vs. absent) a a Hydrocephalus (present vs. absent) a a Basilar invagination (present vs. absent) a a Platybasia (present vs. absent) b Scoliosis (present vs. absent) a Continuity correction. b Fisher's exact probability. CTD, cerebellar tonsillar descent. Figure 5. Sagittal MRI scans of a male patient. Preoperative sagittal (A) T1 weighted and (B) T2 weighted MRI scans reveal tonsillar herniation, basilar invagination and cervical syringomyelia. The patient's scoliosis is presented in Fig. 1C. (C and D) MRI scans at 28 months after small bone window posterior fossa decompression with autologous fascia duraplasty show an upward shift of the tonsils and slight reduction of syringomyelia. 95% CI, ) significantly increased the likelihood of poor clinical outcomes. A comparison of CCOS scores by ANOVA also indicated that CTD grade, and basilar invagination and platybasia by Mann Whitney U tests are predictors of poor clinical prognosis (P<0.05; Table IV). Discussion CM I is a craniocervical junction disorder characterized by a cerebellar tonsil descending below the foramen magnum into the spinal canal. This was first described by Hans Chiari in 1891 (1). The incidence of CM I has been reported to be % in the general population (20). A previous study reported a slight female predominance (female/male ratio 1.3:1.0) (20), although this is inconsistent with the findings in the current study (female/male ratio 1.00:1.52). CM I is generally considered a congenital neurological condition, although in recent years its acquired form has been identified as a complication of CSF diversion procedures or chronic CSF leakage (21,22). CM I is thought to be a multifactorial condition, although the pathogenesis is still undetermined. A well accepted hypothesis is that the hindbrain tissues are dislocated into the spinal canal because of an overcrowded posterior cranial fossa, due to underdevelopment of the mesodermal occipital somite (23). Previous morphometric results have supported this postulation. The posterior fossa volume in CM I patients was reported to be smaller compared with the control group, although the difference was not statistically significant (23,24). In addition, some familial cases suggest a genetic component (25). The incidence of syringomyelia in CM I patients has ranged widely in previous reports, from 30 to 70% (20). The exact prevalence of syringomyelia in pediatric patients remains unclear. In the current study, a high syringomyelia occurrence rate (78.3%) was observed in CM I patients. There are several hypotheses concerning the development of syringomyelia in the CM I context, including the water hammer mechanism proposed by Gardner (26) and the pressure dissociation mechanism proposed by Williams (27). However, most authors agree that partial obstruction in the foramen magnum area, which blocks the normal circulation of CSF, is the pacing factor in the development of syringomyelia (28). Diagnosis of CM I depends on MRI (29). For a long time, the diagnostic criteria have been under debate. Barkovich et al (30) proposed that 3 mm below the foramen magnum was the lowest extent of tonsillar descent in normal patients, and defined CM I as >3 mm of tonsillar descent. Others have proposed that 5 mm of tonsillar ectopia should be adopted as the cutoff for diagnosing CM I (2). In addition, Mikulis et al (31) reported that age affects the normal position of cerebellar tonsils and proposed age based diagnostic criteria. These were as follows: In patients aged 0 9, the cutoff distance for tonsillar descent should be 6 mm; in patients aged 10 29, it should be 5 mm; in patients aged years it should be 4 mm; and at >79 years of age, it should be 3 mm (31). Considering the fact that patients with lesser degrees of tonsillar ectopia (3 5 mm) may also develop classic neurological symptoms and syringomyelia that are amenable to neurosurgical intervention, the current study adopted the more flexible comprehensive diagnostic criteria proposed by Tubbs et al (1). Patients with CM I can be asymptomatic or can present with a variety of signs and symptoms ranging from headache to severe myelopathy and brain stem compression (29). With the increasing availability of diagnostic MRI, more asymptomatic patients are being identified (4). In the adult population, 15 30% of CM I patients are asymptomatic (20). In the current study, 11 (12.0%) asymptomatic children were identified. Innate bias, however, is inevitable in an in hospital cohort. Sleep apnea and feeding problems are reported to be more common in pediatric patients, although other clinical manifestations appear to be similar in different age groups (6). As previously reported, the
6 LIU et al: PEDIATRIC CM-I: LONG-TERM OUTCOMES FOLLOWING POSTERIOR FOSSA DECOMPRESSION 5657 Table IV. Results of statistical analyses. Basilar invagination Platybasia CTD (Grade I III) (present vs. absent) (present vs. absent) Clinical CCOS assessment F value P value Z value P value Z value P value Composite CCOS score Pain subscore Non pain subscore Functionality subscore Complications subscore CTD, cerebellar tonsil descent; CCOS, Chicago Chiari outcome scale. most common presenting symptom of CM I is headache (4), which is consistent with the current findings. In infants and children who are unable to communicate verbally, headaches may manifest as crying and irritability. Other common symptoms include non radicular pain in the shoulder, back and extremities, motor and sensory disturbances, clumsiness, ataxia and lower cranial nerve dysfunction (29). In the current cohort, two patients with atrioventricular block were also identified. There is no effective non surgical strategy for treating patients with CM I (12). Posterior fossa decompression, with or without dural opening, and with or without arachnoid opening or dissection, is most commonly used for the surgical treatment of CM I and can change its clinical course (13,32). However, the size of the bone window required for posterior fossa decompression is still under debate (33,34). Furthermore, it has not yet been established whether a difference exists in the operative techniques used for pediatric and adult patients. Large bone window posterior fossa decompression effectively enlarges the posterior cranial fossa and therefore relieves symptoms (35). However, there may be a higher incidence of complications, such as CSF leak, pseudocysts, meningitis and hydrocephalus (35). Furthermore, excessive removal of the squamous part of the occipital bone could lead to downward and backward displacement of the cerebellum and brain stem, leading to long term complications. According to a previous study, small bone window craniectomy is enough to achieve favorable clinical outcomes, and the incidence of complications is reduced (35). The procedure described in the aforementioned study relieves the compression of the occipitocervical bones and preserves enough bone to support the cerebellum and brain stem. In the current study, all patients underwent a small bone window approach, with which high rates of clinical (81.5%) and radiological (77.8%) improvement were achieved. Whether it is necessary to open the arachnoid space is another focus of controversy. Some authors assert that CSF related complications, such as CSF leak or meningitis, are directly associated with opening the arachnoid (36). A previous study has indicated that the incidence of CSF leaks is not higher in the arachnoid opening group, provided that watertight duraplasty is performed (37). Furthermore, reconstruction of the cisterna magna and tonsillar manipulation could contribute to a better prognosis (37). It is the current authors opinion that arachnoid opening is unnecessary in most patients; SPFD and duraplasty without arachnoid incision is sufficient to relieve compression and alleviate clinical symptoms. It should be noted that the incidence of CSF related complications was low in the pediatric cohort of the current study. The prevalence of scoliosis in the general pediatric population is 2 4%, while in children with CM I the prevalence of scoliosis is >4 fold increase (9,38). Progressive scoliosis is a relatively common manifestation of CM I when there is coexistent syringomyelia (38). In the current study, the incidence of scoliosis was markedly higher (47.8%) in CM I patients compared with the reported prevalence in the general pediatric population. Nokes et al (39) identified 3 patients with CM I and scoliosis, but without syringomyelia. In the current cohort, all scoliotic children had coexistent syringomyelia. Considering the relatively mild severity of pediatric scoliosis, spinal orthopedic surgery was not recommended for the majority of these patients. It was considered that brace treatment could effectively reverse scoliotic progression. Eule et al (40) conducted a 20 year review of surgical and nonsurgical treatment in a pediatric cohort with CM I associated with syringomyelia and scoliosis. It was found that early decompression of CM I helped stabilize or alleviate the associated scoliosis, avoiding the requirement for orthopedic spinal surgery. The current study had several limitations. Preoperatively, the scoliosis evaluations were based only on standing posteroanterior radiographs. The absence of side bending radiographs limited a three dimensional assessment. During the follow up period, only MRI scans were performed. Plain radiography was not performed in all of the patients. Therefore, the present study did not track the progression of scoliosis. Furthermore, for ethical reasons, there were no control groups undergoing large bone window posterior fossa decompression or arachnoid opening in the current study. In conclusion, early recognition and surgical treatment of pediatric CM I leads to good outcomes in the majority of patients. SPFD with duraplasty was demonstrated to be an effective, safe treatment option with a low complication rate. High CTD grade, basilar invagination and platybasia were indicated to be predictors of poor clinical prognosis.
7 5658 References 1. Tubbs RS, Lyerly MJ, Loukas M, Shoja MM and Oakes WJ: The pediatric Chiari I malformation: A review. Childs Nerv Syst 23: , Aitken LA, Lindan CE, Sidney S, Gupta N, Barkovich AJ, Sorel M and Wu YW: Chiari type I malformation in a pediatric population. Pediatr Neurol 40: , Dones J, De Jesús O, Colen CB, Toledo MM and Delgado M: Clinical outcomes in patients with Chiari I malformation: A review of 27 cases. Surg Neurol 60: , Poretti A, Ashmawy R, Garzon Muvdi T, Jallo GI, Huisman TA and Raybaud C: Chiari type 1 deformity in children: Pathogenetic, clinical, neuroimaging, and management aspects. Neuropediatrics 47: , Albert GW, Menezes AH, Hansen DR, Greenlee JD and Weinstein SL: Chiari malformation Type I in children younger than age 6 years: Presentation and surgical outcome. J Neurosurg Pediatr 5: , Amin R, Sayal P, Sayal A, Massicote C, Pham R, Al Saleh S, Drake J and Narang I: The association between sleep disordered breathing and magnetic resonance imaging findings in a pediatric cohort with Chiari 1 malformation. Can Respir J 22: 31 36, Tubbs RS, Doyle S, Conklin M and Oakes WJ: Scoliosis in a child with Chiari I malformation and the absence of syringomyelia: Case report and a review of the literature. Childs Nerv Syst 22: , Ono A, Suetsuna F, Ueyama K, Yokoyama T, Aburakawa S, Numasawa T, Wada K and Toh S: Surgical outcomes in adult patients with syringomyelia associated with Chiari malformation type I: The relationship between scoliosis and neurological findings. J Neurosurg Spine 6: , Krieger MD, Falkinstein Y, Bowen IE, Tolo VT and McComb JG: Scoliosis and Chiari malformation type I in children. J Neurosurg Pediatr 7: 25 29, Strahle J, Smith BW, Martinez M, Bapuraj JR, Muraszko KM, Garton HJ and Maher CO: The association between Chiari malformation type I, spinal syrinx, and scoliosis. J Neurosurg Pediatr 15: , Isik N, Elmaci I, Isik N, Cerci SA, Basaran R, Gura M and Kalelioglu M: Long term results and complications of the syringopleural shunting for treatment of syringomyelia: A clinical study. Br J Neurosurg 27: 91 99, Morina D, Petridis AK, Fritzsche FS, Ntoulias G and Scholz M: Syringomyelia regression after shunting of a trapped fourth ventricle. Clin Pract 3: e1, Whitson WJ, Lane JR, Bauer DF and Durham SR: A prospective natural history study of nonoperatively managed Chiari I malformation: Does follow up MRI surveillance alter surgical decision making. J Neurosurg Pediatr 16: , Guyotat J, Bret P, Jouanneau E, Ricci AC and Lapras C: Syringomyelia associated with type I Chiari malformation. A 21 year retrospective study on 75 cases treated by foramen magnum decompression with a special emphasis on the value of tonsils resection. Acta Neurochir (Wien) 140: , Beecher JS, Liu Y, Qi X and Bolognese PA: Minimally invasive subpial tonsillectomy for Chiari I decompression. Acta Neurochir (Wien) 158: , Yilmaz A, Kanat A, Musluman AM, Colak I, Terzi Y, Kayacı S and Aydin Y: When is duraplasty required in the surgical treatment of Chiari malformation type I based on tonsillar descending grading scale? World Neurosurg 75: , Morrissy RT, Goldsmith GS, Hall EC, Kehl D and Cowie GH: Measurement of the Cobb angle on radiographs of patients who have scoliosis. Evaluation of intrinsic error. J Bone Joint Surg Am 72: , Ambarki K, Israelsson H, Wåhlin A, Birgander R, Eklund A and Malm J: Brain ventricular size in healthy elderly: Comparison between Evans index and volume measurement. Neurosurgery 67: 94 99, Yarbrough CK, Greenberg JK, Smyth MD, Leonard JR, Park TS and Limbrick DD Jr: External validation of the Chicago Chiari outcome scale. J Neurosurg Pediatr 13: , Arnautovic A, Splavski B, Boop FA and Arnautovic KI: Pediatric and adult Chiari malformation Type I surgical series : A review of demographics, operative treatment, and outcomes. J Neurosurg Pediatr 15: , Atkinson JL, Weinshenker BG, Miller GM, Piepgras DG and Mokri B: Acquired Chiari I malformation secondary to spontaneous spinal cerebrospinal fluid leakage and chronic intracranial hypotension syndrome in seven cases. J Neurosurg 88: , Riffaud L, Moughty C, Henaux PL, Haegelen C and Morandi X: Acquired Chiari I malformation and syringomyelia after valveless lumboperitoneal shunt in infancy. Pediatr Neurosurg 44: , Urbizu A, Poca MA, Vidal X, Rovira A, Sahuquillo J and Macaya A: MRI based morphometric analysis of posterior cranial fossa in the diagnosis of chiari malformation type I. J Neuroimaging 24: , Furtado SV, Reddy K and Hegde AS: Posterior fossa morphometry in symptomatic pediatric and adult Chiari I malformation. J Clin Neurosci 16: , Shimojima K, Okamoto N, Tamasaki A, Sangu N, Shimada S and Yamamoto T: An association of 19p13.2 microdeletions with Malan syndrome and Chiari malformation. Am J Med Genet A 167A: , Gardner WJ: Hydrodynamic mechanism of syringomyelia: Its relationship to myelocele. J Neurol Neurosurg Psychiatry 28: , Williams B: On the pathogenesis of syringomyelia: A review. J R Soc Med 73: , Koyanagi I and Houkin K: Pathogenesis of syringomyelia associated with Chiari type 1 malformation: Review of evidences and proposal of a new hypothesis. Neurosurg Rev 33: , McVige JW and Leonardo J: Neuroimaging and the clinical manifestations of Chiari malformation type I (CMI). Curr Pain Headache Rep 19: 18, Barkovich AJ, Wippold FJ, Sherman JL and Citrin CM: Significance of cerebellar tonsillar position on MR. AJNR Am J Neuroradiol 7: , Mikulis DJ, Diaz O, Egglin TK and Sanchez R: Variance of the position of the cerebellar tonsils with age: Preliminary report. Radiology 183: , Chotai S and Medhkour A: Surgical outcomes after posterior fossa decompression with and without duraplasty in Chiari malformation I. Clin Neurol Neurosurg 125: , Menezes AH: Current opinions for treatment of symptomatic hindbrain herniation or Chiari type I malformation. World Neurosurg 75: , Abd El Barr M and Groff MW: Less is more: Limiting the size of posterior fossa decompressions in Chiari I malformations. World Neurosurg 81: , Bao C, Yang F, Liu L, Wang B, Li D, Gu Y, Zhang S and Chen L: Surgical treatment of Chiari I malformation complicated with syringomyelia. Exp Ther Med 5: , Navarro R, Olavarria G, Seshadri R, Gonzales Portillo G, McLone DG and Tomita T: Surgical results of posterior fossa decompression for patients with Chiari I malformation. Childs Nerv Syst 20: , Alfieri A and Pinna G: Long term results after posterior fossa decompression in syringomyelia with adult Chiari Type I malformation. J Neurosurg Spine 17: , Godzik J, Dardas A, Kelly MP, Holekamp TF, Lenke LG, Smyth MD, Park TS, Leonard JR and Limbrick DD: Comparison of spinal deformity in children with Chiari I malformation with and without syringomyelia: Matched cohort study. Eur Spine J 25: , Nokes SR, Murtagh FR, Jones JD III, Downing M, Arrington JA, Turetsky D and Silbiger ML: Childhood scoliosis: MR imaging. Radiology 164: , Eule JM, Erickson MA, O'Brien MF and Handler M: Chiari I malformation associated with syringomyelia and scoliosis: A twenty year review of surgical and nonsurgical treatment in a pediatric population. Spine (Phila Pa 1976) 27: , 2002.
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
A case report on result of posterior fossa decompression on syringomyelia in a case of chiary type I malformation
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article A case report on result of posterior fossa decompression on syringomyelia in a case of chiary type I malformation Asheesh Kumar Gupta,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article A case report on result of posterior fossa decompression on syringomyelia in a case of chiary type I malformation Asheesh Kumar Gupta,
Role of MRI in Selection of Patients for Surgery and Assessing the Post Operative Outcome in Chiari 1 Malformation
 DOI: 10.7860/IJARS/2017/13599:2222 Radiology Section Original Article Role of MRI in Selection of Patients for Surgery and Assessing the Post Operative Outcome in Chiari 1 Malformation Rajesh Kumar V,
DOI: 10.7860/IJARS/2017/13599:2222 Radiology Section Original Article Role of MRI in Selection of Patients for Surgery and Assessing the Post Operative Outcome in Chiari 1 Malformation Rajesh Kumar V,
OUTCOME OF SUBOCCIPITAL DECOMPRESSION WITH AND WITHOUT DURAPLASTY IN ADULTS WITH CHIARI I MALFORMATION
 OUTCOME OF SUBOCCIPITAL DECOMPRESSION WITH AND WITHOUT DURAPLASTY IN ADULTS WITH CHIARI I MALFORMATION Mushtaq 1, Zia ur Rehman 1, M Mukhtar Khan 2 ABSTRACT Objectives: To investigate outcome for ACM1
OUTCOME OF SUBOCCIPITAL DECOMPRESSION WITH AND WITHOUT DURAPLASTY IN ADULTS WITH CHIARI I MALFORMATION Mushtaq 1, Zia ur Rehman 1, M Mukhtar Khan 2 ABSTRACT Objectives: To investigate outcome for ACM1
Suboccipital decompression for Chiari malformation associated scoliosis: risk factors and time course of deformity progression
 J Neurosurg Pediatrics 1:456 460, 2008 Suboccipital decompression for Chiari malformation associated scoliosis: risk factors and time course of deformity progression FRANK J. ATTENELLO, M.S., MATTHEW J.
J Neurosurg Pediatrics 1:456 460, 2008 Suboccipital decompression for Chiari malformation associated scoliosis: risk factors and time course of deformity progression FRANK J. ATTENELLO, M.S., MATTHEW J.
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Pediatric and adult Chiari malformation Type I surgical series : a review of demographics, operative treatment, and outcomes
 PEDIATRICS literature review Pediatric and adult Chiari malformation Type I surgical series 1965 2013: a review of demographics, operative treatment, and outcomes aska arnautovic, bsc, 1 bruno splavski,
PEDIATRICS literature review Pediatric and adult Chiari malformation Type I surgical series 1965 2013: a review of demographics, operative treatment, and outcomes aska arnautovic, bsc, 1 bruno splavski,
Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic Type 1 Chiari Patients and Healthy Controls
 The University of Akron IdeaExchange@UAkron Honors Research Projects The Dr. Gary B. and Pamela S. Williams Honors College Spring 2015 Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic
The University of Akron IdeaExchange@UAkron Honors Research Projects The Dr. Gary B. and Pamela S. Williams Honors College Spring 2015 Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic
Chiari malformation Type I (CM-I) in children is
 PEDIATRICS clinical article J Neurosurg Pediatr 16:159 166, 2015 A prospective natural history study of nonoperatively managed Chiari I malformation: does follow-up MRI surveillance alter surgical decision
PEDIATRICS clinical article J Neurosurg Pediatr 16:159 166, 2015 A prospective natural history study of nonoperatively managed Chiari I malformation: does follow-up MRI surveillance alter surgical decision
Chiari bridges review Chiari Treatments & Potential Pitfalls
 Chiari bridges review Chiari Treatments & Potential Pitfalls Once diagnosed, you will usually be referred to a specialist (not a Chiari Specialist, but an everyday, run-of-the-mill neurologist or neurosurgeon).
Chiari bridges review Chiari Treatments & Potential Pitfalls Once diagnosed, you will usually be referred to a specialist (not a Chiari Specialist, but an everyday, run-of-the-mill neurologist or neurosurgeon).
Idiopathic cervical syringomyelia can be associated. Pediatric Chiari malformation Type 0: a 12-year institutional experience.
 J Neurosurg J Neurosurg Pediatrics Pediatrics 8:000 000, 8:1 5, 2011 Pediatric Chiari malformation Type 0: a 12-year institutional experience Clinical article Joshua J. Chern, M.D., Ph.D., Amber J. Gordon,
J Neurosurg J Neurosurg Pediatrics Pediatrics 8:000 000, 8:1 5, 2011 Pediatric Chiari malformation Type 0: a 12-year institutional experience Clinical article Joshua J. Chern, M.D., Ph.D., Amber J. Gordon,
Chiari malformations. A fact sheet for patients and carers
 A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
Chiari FAQ's. 1. What is a Chiari Malformation?
 Chiari FAQ's These FAQ's are for informational purposes only and in no way represent an attempt to provide medical advice. This information may or may not apply to your case and anyone with a question
Chiari FAQ's These FAQ's are for informational purposes only and in no way represent an attempt to provide medical advice. This information may or may not apply to your case and anyone with a question
Chiari 1 malformations: an Indian hospital experience
 O r i g i n a l A r t i c l e Singapore Med J 2008; 49 (12) : 1029 Chiari 1 malformations: an Indian hospital experience Ramnarayan R, Praharaj M S, Jayakumar P N Department of Neurosurgery, The National
O r i g i n a l A r t i c l e Singapore Med J 2008; 49 (12) : 1029 Chiari 1 malformations: an Indian hospital experience Ramnarayan R, Praharaj M S, Jayakumar P N Department of Neurosurgery, The National
Decompression of the spinal subarachnoid space as a solution for syringomyelia without Chiari malformation
 (2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
(2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
The Role of Cine Flow Magnetic Resonance Imaging in Patients with Chiari 0 Malformation
 DOI: 10.5137/1019-5149.JTN.19049-16.2 Received: 11.11.2016 / Accepted: 14.12.2016 Published Online: 16.01.2017 Original Investigation The Role of Cine Flow Magnetic Resonance Imaging in Patients with Chiari
DOI: 10.5137/1019-5149.JTN.19049-16.2 Received: 11.11.2016 / Accepted: 14.12.2016 Published Online: 16.01.2017 Original Investigation The Role of Cine Flow Magnetic Resonance Imaging in Patients with Chiari
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Minimally invasive subpial tonsillectomy for Chiari I decompression
 Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
The MRI in Arnold-Chiari Syndrome I and Idiopathic Syringomyelia
 The MRI in Arnold-Chiari Syndrome I and Idiopathic Syringomyelia Author: Miguel B. Royo Salvador, MD, PhD Introduction Magnetic resonance imaging (MRI) is a crucial diagnostic tool for men, women, and
The MRI in Arnold-Chiari Syndrome I and Idiopathic Syringomyelia Author: Miguel B. Royo Salvador, MD, PhD Introduction Magnetic resonance imaging (MRI) is a crucial diagnostic tool for men, women, and
DIANE MUELLER, N.D., R.N., C-F.N.P., AND JOHN J. ORO, M.D.
 Neurosurg Focus 18 (2):ECP2, 2005 Prospective analysis of self-perceived quality of life before and after posterior fossa decompression in 112 patients with Chiari malformation with or without syringomyelia
Neurosurg Focus 18 (2):ECP2, 2005 Prospective analysis of self-perceived quality of life before and after posterior fossa decompression in 112 patients with Chiari malformation with or without syringomyelia
Djamila Kafoufi Al Galaa Military Hospital Cairo
 Djamila Kafoufi Al Galaa Military Hospital Cairo Herniation cerebellar tonsils below the foramen magnum, Hans Chiari 4 types Chiari I less than 5mm,HDC rare,syringomyelia often present. Chiari II,protrusion
Djamila Kafoufi Al Galaa Military Hospital Cairo Herniation cerebellar tonsils below the foramen magnum, Hans Chiari 4 types Chiari I less than 5mm,HDC rare,syringomyelia often present. Chiari II,protrusion
Outcome of Two Surgical Options Used in Treatment of Chiari Type-One Malformation
 ISPUB.COM The Internet Journal of Neurosurgery Volume 11 Number 1 Outcome of Two Surgical Options Used in Treatment of Chiari Type-One Malformation M G Ammar Citation M G Ammar. Outcome of Two Surgical
ISPUB.COM The Internet Journal of Neurosurgery Volume 11 Number 1 Outcome of Two Surgical Options Used in Treatment of Chiari Type-One Malformation M G Ammar Citation M G Ammar. Outcome of Two Surgical
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
The Chiari malformation I (CM I) is a disorder that has been
 DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
Developments in the treatment of Chiari type 1 malformations over the past decade
 Original Study Developments in the treatment of Chiari type 1 malformations over the past decade Peter G. Passias 1, Alexandra Pyne 1, Samantha R. Horn 1, Gregory W. Poorman 1, Muhammad B. Janjua 1, Dennis
Original Study Developments in the treatment of Chiari type 1 malformations over the past decade Peter G. Passias 1, Alexandra Pyne 1, Samantha R. Horn 1, Gregory W. Poorman 1, Muhammad B. Janjua 1, Dennis
Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms.
 RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
Persistent/Recurrent Syringomyelia after Chiari Decompression Natural History and Management Strategies: A Systematic Review
 116 Systematic Review Persistent/Recurrent Syringomyelia after Chiari Decompression Natural History and Management Strategies: A Systematic Review James M. Schuster 1 Fangyi Zhang 2,3 Daniel C. Norvell
116 Systematic Review Persistent/Recurrent Syringomyelia after Chiari Decompression Natural History and Management Strategies: A Systematic Review James M. Schuster 1 Fangyi Zhang 2,3 Daniel C. Norvell
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
NEUROSURGERY WORKING GROUP
 NEUROSURGERY WORKING GROUP OUTCOMES Primary Outcome Protect neurocognitive development by optimizing CSF dynamics throughout the life span. Optimize metrics for the management of CSF anomalies to protect/optimize
NEUROSURGERY WORKING GROUP OUTCOMES Primary Outcome Protect neurocognitive development by optimizing CSF dynamics throughout the life span. Optimize metrics for the management of CSF anomalies to protect/optimize
Brain Imaging. Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress
 Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Significance of Cerebellar Tonsillar Position on MR
 795 Significance of Cerebellar Tonsillar Position on MR A. J. Barkovich 1. 3 F. J. Wippold 2. 3 J. L. Sherman 3. 4 C. M. Citrin 4. 5 It has been noted that a low degree of ectopia of the cerebellar tonsils
795 Significance of Cerebellar Tonsillar Position on MR A. J. Barkovich 1. 3 F. J. Wippold 2. 3 J. L. Sherman 3. 4 C. M. Citrin 4. 5 It has been noted that a low degree of ectopia of the cerebellar tonsils
Chiari malformation Type I (CM-I) is often associated. The association between Chiari malformation Type I, spinal syrinx, and scoliosis PEDIATRICS
 PEDIATRICS clinical article J Neurosurg Pediatr 15:607 611, 2015 The association between Chiari malformation Type I, spinal syrinx, and scoliosis Jennifer Strahle, MD, 1 Brandon W. Smith, MD, MS, 1 Melaine
PEDIATRICS clinical article J Neurosurg Pediatr 15:607 611, 2015 The association between Chiari malformation Type I, spinal syrinx, and scoliosis Jennifer Strahle, MD, 1 Brandon W. Smith, MD, MS, 1 Melaine
Chiari I Malformation Associated with Syringomyelia and Scoliosis
 Chiari I Malformation Associated with Syringomyelia and Scoliosis A Twenty-Year Review of Surgical and Nonsurgical Treatment in a Pediatric Population James M. Eule, MD,* Mark A. Erickson, MD, Michael
Chiari I Malformation Associated with Syringomyelia and Scoliosis A Twenty-Year Review of Surgical and Nonsurgical Treatment in a Pediatric Population James M. Eule, MD,* Mark A. Erickson, MD, Michael
May have excessive movement in the unfused segment to compensate. Flexion extension better preserved than lateral bend or rotation
 IV CONGENITAL SPINE KLIPPEL FLAIL SYNDROME Prevalence 0.60% Mainly around upper 3 vertebrae [75%] Commonest: C2 3 Lower Cervical spine fusion may be associated with syndromes: Fetal alcohol syndrome Goldenhar
IV CONGENITAL SPINE KLIPPEL FLAIL SYNDROME Prevalence 0.60% Mainly around upper 3 vertebrae [75%] Commonest: C2 3 Lower Cervical spine fusion may be associated with syndromes: Fetal alcohol syndrome Goldenhar
Cranio-cervical decompression. Information for patients Neurosurgery
 Cranio-cervical decompression Information for patients Neurosurgery page 2 of 12 What is a cranio-cervical decompression? A cranio-cervical decompression is an operation involving the back of the head
Cranio-cervical decompression Information for patients Neurosurgery page 2 of 12 What is a cranio-cervical decompression? A cranio-cervical decompression is an operation involving the back of the head
IIH, previously known as pseudotumor cerebri, is a syndrome
 ORIGINAL RESEARCH A.H. Aiken J.A. Hoots A.M. Saindane P.A. Hudgins Incidence of Cerebellar Tonsillar Ectopia in Idiopathic Intracranial Hypertension: A Mimic of the Chiari I Malformation BACKGROUND AND
ORIGINAL RESEARCH A.H. Aiken J.A. Hoots A.M. Saindane P.A. Hudgins Incidence of Cerebellar Tonsillar Ectopia in Idiopathic Intracranial Hypertension: A Mimic of the Chiari I Malformation BACKGROUND AND
Chiari malformations (CMs) are well-known structural
 J Neurosurg 126:600 605, 2017 Editorial Evoked potentials and Chiari malformation Type 1 P. David Adelson, MD Barrow Neurological Institute at Phoenix Children s Hospital, Phoenix, Arizona Chiari malformations
J Neurosurg 126:600 605, 2017 Editorial Evoked potentials and Chiari malformation Type 1 P. David Adelson, MD Barrow Neurological Institute at Phoenix Children s Hospital, Phoenix, Arizona Chiari malformations
A review of the disagreements in the prevalence and treatment of the tethered cord syndromes with chiari 1 malformations
 SNI: Spine OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article A review of the disagreements
SNI: Spine OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article A review of the disagreements
International Journal of Pharma and Bio Sciences
 Original Research Article Anatomy and Allied sciences International Journal of Pharma and Bio Sciences ISSN 0975-6299 SCREENING FOR ANOMALIES IN OCCIPITO-CERVICAL JUNCTION USING CRANIOMETRY IN COMPUTED
Original Research Article Anatomy and Allied sciences International Journal of Pharma and Bio Sciences ISSN 0975-6299 SCREENING FOR ANOMALIES IN OCCIPITO-CERVICAL JUNCTION USING CRANIOMETRY IN COMPUTED
Arnold Chiari Malformation - A hospital based autopsy study
 Rapotra Megha et al / International Journal of Biomedical Research 2017; 8(05): 250-254. 250 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: https://dx.doi.org/10.7439/ijbr
Rapotra Megha et al / International Journal of Biomedical Research 2017; 8(05): 250-254. 250 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: https://dx.doi.org/10.7439/ijbr
Skull base growth in children with Chiari malformation Type I
 See the corresponding editorial in this issue, pp 187. J Neurosurg (3 Suppl Pediatrics) 107:188 192, 2007 Skull base growth in children with Chiari malformation Type I SPYROS SGOUROS, M.D., F.R.C.S.(SN),
See the corresponding editorial in this issue, pp 187. J Neurosurg (3 Suppl Pediatrics) 107:188 192, 2007 Skull base growth in children with Chiari malformation Type I SPYROS SGOUROS, M.D., F.R.C.S.(SN),
While some patients with SIH recover without intervention
 ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Primary Outcomes. Outcomes
 Neurosurgery Jeffrey Blount, MD, Chair Robin Bowman, MD Michael Partington, MD Brandon Roque, MD Elias Rizk, MD Mark Dias, MD, FAAP, FAANS Betsy Hopson, MS Outcomes Primary Outcomes Protect neurocognitive
Neurosurgery Jeffrey Blount, MD, Chair Robin Bowman, MD Michael Partington, MD Brandon Roque, MD Elias Rizk, MD Mark Dias, MD, FAAP, FAANS Betsy Hopson, MS Outcomes Primary Outcomes Protect neurocognitive
Spontaneous Intracranial Hypotension Diagnosis and Treatment
 Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Is there a relationship between the extent of tonsillar ectopia and the severity of the clinical Chiari syndrome? Linear Regression Analysis
 Is there a relationship between the extent of tonsillar ectopia and the severity of the clinical Chiari syndrome? Dan Heffez MD; John Broderick MD; Michael Connor DO; Michael Mitchell MD; Joanna Galezowska;
Is there a relationship between the extent of tonsillar ectopia and the severity of the clinical Chiari syndrome? Dan Heffez MD; John Broderick MD; Michael Connor DO; Michael Mitchell MD; Joanna Galezowska;
ISSN X (Print) Original Research Article. DOI: /sjams
 DOI: 10.21276/sjams Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2017; 5(8E):3349-3365 Scholars Academic and Scientific Publisher (An International Publisher for Academic
DOI: 10.21276/sjams Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2017; 5(8E):3349-3365 Scholars Academic and Scientific Publisher (An International Publisher for Academic
Application of three-dimensional angiography in elderly patients with meningioma
 Application of three-dimensional angiography in elderly patients with meningioma Poster No.: C-0123 Congress: ECR 2012 Type: Scientific Paper Authors: X. Han, J. Chen, K. Shi; Haikou/CN Keywords: Neuroradiology
Application of three-dimensional angiography in elderly patients with meningioma Poster No.: C-0123 Congress: ECR 2012 Type: Scientific Paper Authors: X. Han, J. Chen, K. Shi; Haikou/CN Keywords: Neuroradiology
S YRINGOMYELIA and syringobulbia are
 Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Spinal Imaging. Bearbeitet von Herwig Imhof. 1. Auflage Taschenbuch. 312 S. Paperback ISBN Format (B x L): 12,5 x 19 cm
 Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Presented by : Shashwat Mishra
 Presented by : Shashwat Mishra Named after Hans Chiari (1851 1916). Professor of Pathology in Prague, Czechoslovakia, Paper entitled Concerning alterations in the cerebellum resulting from cerebral hydrocephalus
Presented by : Shashwat Mishra Named after Hans Chiari (1851 1916). Professor of Pathology in Prague, Czechoslovakia, Paper entitled Concerning alterations in the cerebellum resulting from cerebral hydrocephalus
Fifteen-minute consultation: incidental findings on brain and spine imaging
 BEST PRACTICE Editor s choice Scan to access more free content Department of Neurosurgery, Birmingham Children s Hospital, Birmingham, UK Correspondence to Chirag Patel, Department of Neurosurgery, Birmingham
BEST PRACTICE Editor s choice Scan to access more free content Department of Neurosurgery, Birmingham Children s Hospital, Birmingham, UK Correspondence to Chirag Patel, Department of Neurosurgery, Birmingham
KEY WORDS algorithm; predictive model analysis; postsurgical improvement; outcome; Chiari Type I malformation; congenital; syringomyelia
 CLINICAL ARTICLE J Neurosurg Spine 28:23 32, 2018 A points-based algorithm for prognosticating clinical outcome of Chiari malformation Type I with syringomyelia: results from a predictive model analysis
CLINICAL ARTICLE J Neurosurg Spine 28:23 32, 2018 A points-based algorithm for prognosticating clinical outcome of Chiari malformation Type I with syringomyelia: results from a predictive model analysis
Craniovertebral Junction Realignment for the Treatment of Basilar Invagination With Syringomyelia: Preliminary Report of 12 Cases
 Neurol Med Chir (Tokyo) 45, 512 518, 2005 Craniovertebral Junction Realignment for the Treatment of Basilar Invagination With Syringomyelia: Preliminary Report of 12 Cases Atul GOEL and Praveen SHARMA
Neurol Med Chir (Tokyo) 45, 512 518, 2005 Craniovertebral Junction Realignment for the Treatment of Basilar Invagination With Syringomyelia: Preliminary Report of 12 Cases Atul GOEL and Praveen SHARMA
The "Keyhole": A Sign of
 473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
Evaluation of Apparent Diffusion Coefficients in the Cerebellar Tonsils and Bulbus in Chiari Type I Malformations: Comparison Before and After Surgery
 DOI: 10.5137/1019-5149.JTN.20326-17.1 Received: 12.03.2017 / Accepted: 07.05.2017 Published Online: 05.06.2017 Original Investigation Evaluation of Apparent Diffusion Coefficients in the Cerebellar Tonsils
DOI: 10.5137/1019-5149.JTN.20326-17.1 Received: 12.03.2017 / Accepted: 07.05.2017 Published Online: 05.06.2017 Original Investigation Evaluation of Apparent Diffusion Coefficients in the Cerebellar Tonsils
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2
 Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2 Abstract Cranio-cervical junction abnormalities are a rare combination of congenital or acquired
Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2 Abstract Cranio-cervical junction abnormalities are a rare combination of congenital or acquired
Idiopathic scoliosis Scoliosis Deformities I 06
 What is Idiopathic scoliosis? 80-90% of all scolioses are idiopathic, the rest are neuromuscular or congenital scolioses with manifest primary diseases responsible for the scoliotic pathogenesis. This
What is Idiopathic scoliosis? 80-90% of all scolioses are idiopathic, the rest are neuromuscular or congenital scolioses with manifest primary diseases responsible for the scoliotic pathogenesis. This
Microsurgery of Arnold-Chiari malformation in adults with and without hydromyelia
 Microsurgery of Arnold-Chiari malformation in adults with and without hydromyelia ALBERT L. RHOTON, JR., M.D. Division of Neurological Surgery, University of Florida Health Center, Gainesville, Florida
Microsurgery of Arnold-Chiari malformation in adults with and without hydromyelia ALBERT L. RHOTON, JR., M.D. Division of Neurological Surgery, University of Florida Health Center, Gainesville, Florida
Signal Intensity Of Cerebrospinal Fluid On MR Images Indicates The Severity Of Degenerative Lumbar Spinal Canal Stenosis
 ISPUB.COM The Internet Journal of Spine Surgery Volume 1 Number 2 Signal Intensity Of Cerebrospinal Fluid On MR Images Indicates The Severity Of Degenerative Lumbar Spinal Canal Stenosis T Sakamaki, H
ISPUB.COM The Internet Journal of Spine Surgery Volume 1 Number 2 Signal Intensity Of Cerebrospinal Fluid On MR Images Indicates The Severity Of Degenerative Lumbar Spinal Canal Stenosis T Sakamaki, H
Author's response to reviews
 Author's response to reviews Title: Scoliotic posture as the initial symptom in adolescents with lumbar disc herniation: its curve pattern and natural history after lumbar discectomy Authors: Zezhang Zhu
Author's response to reviews Title: Scoliotic posture as the initial symptom in adolescents with lumbar disc herniation: its curve pattern and natural history after lumbar discectomy Authors: Zezhang Zhu
Multimodal Evaluation Of Cerebrospinal Fluid (csf ) Dynamics Following Extradural Decompression For Chiari I Malformation
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2015 Multimodal Evaluation Of Cerebrospinal Fluid (csf ) Dynamics
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2015 Multimodal Evaluation Of Cerebrospinal Fluid (csf ) Dynamics
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Moderators: Dr Manmohan Singh Dr Pankaj Singh Presentor : Dr Kanwaljeet Garg
 Moderators: Dr Manmohan Singh Dr Pankaj Singh Presentor : Dr Kanwaljeet Garg History! Hans Chiari (1851 1916) was born in Vienna, Austria! He was Professor of pathology at Prague, Czechoslovakia! His initial
Moderators: Dr Manmohan Singh Dr Pankaj Singh Presentor : Dr Kanwaljeet Garg History! Hans Chiari (1851 1916) was born in Vienna, Austria! He was Professor of pathology at Prague, Czechoslovakia! His initial
Normal Value of Skull Base Angle. Using the Modified Magnetic Resonance Imaging Technique in Thai Population
 Open Access Journal of Oral Health and Craniofacial Science Research Article Normal Value of Skull Base Angle ISSN 2573-6191 Using the Modified Magnetic Resonance Imaging Technique in Thai Population Siriporn
Open Access Journal of Oral Health and Craniofacial Science Research Article Normal Value of Skull Base Angle ISSN 2573-6191 Using the Modified Magnetic Resonance Imaging Technique in Thai Population Siriporn
Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management
 THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Disclosures None. Common Neurosurgical Problems Seen in Office Encounters. Macrocephaly Low Back Pain Sacral Dimple Concussion Chiari Malformation
 Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
NMH happens when there is an abnormal reflex interaction between the heart and the brain, although both are structurally normal.
 Neurally mediated hypotension: is also known as: the fainting reflex, neurocardiogenic syncope, vasodepressor syncope, the vaso-vagal reflex, and autonomic dysfunction. (Hypotension= low blood pressure,
Neurally mediated hypotension: is also known as: the fainting reflex, neurocardiogenic syncope, vasodepressor syncope, the vaso-vagal reflex, and autonomic dysfunction. (Hypotension= low blood pressure,
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Abstract !"# $% &%'(% )* ( % +$$ '% % % Presentation Notes
 Presenter Name: John Oro, MD Topic: Chiari & Syringomyelia 101 A Brief Look at Neuroanatomy The brain is enclosed and protected by a rounded skull made of rigid bone. The bottom of the skull contains multiple
Presenter Name: John Oro, MD Topic: Chiari & Syringomyelia 101 A Brief Look at Neuroanatomy The brain is enclosed and protected by a rounded skull made of rigid bone. The bottom of the skull contains multiple
Static and dynamic cervical MRI: two useful exams in cervical myelopathy
 Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Chiari malformation Type I (CM-I) is typically defined
 PEDIATRICS clinical article J Neurosurg Pediatr 16:150 158, 2015 Outcomes after suboccipital decompression without dural opening in children with Chiari malformation Type I Benjamin C. Kennedy, MD, 1 Kathleen
PEDIATRICS clinical article J Neurosurg Pediatr 16:150 158, 2015 Outcomes after suboccipital decompression without dural opening in children with Chiari malformation Type I Benjamin C. Kennedy, MD, 1 Kathleen
Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage
 DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
Surgical treatment of Chiari I malformation: indications and approaches
 Neurosurg Focus 11 (1):Article 2, 2001, Click here to return to Table of Contents Surgical treatment of Chiari I malformation: indications and approaches TORD D. ALDEN, M.D., JEFFREY G. OJEMANN, M.D.,
Neurosurg Focus 11 (1):Article 2, 2001, Click here to return to Table of Contents Surgical treatment of Chiari I malformation: indications and approaches TORD D. ALDEN, M.D., JEFFREY G. OJEMANN, M.D.,
Parkinsonism after Shunting for Hydrocephalus Secondary to Aqueductal Stenosis with Chiari Malformation
 ISPUB.COM The Internet Journal of Neurosurgery Volume 6 Number 2 Parkinsonism after Shunting for Hydrocephalus Secondary to Aqueductal Stenosis with Chiari M Turgut Citation M Turgut. Parkinsonism after
ISPUB.COM The Internet Journal of Neurosurgery Volume 6 Number 2 Parkinsonism after Shunting for Hydrocephalus Secondary to Aqueductal Stenosis with Chiari M Turgut Citation M Turgut. Parkinsonism after
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Abstract Objective: Multiple surgical strategies exist for the management of the symptomatic Chiari II malformation. To date, no comprehensive
 Childs Nerv Syst (2004) 20:375 381 DOI 10.1007/s00381-004-0969-4 R E V I E W P A P E R R. Shane Tubbs Treatment and management of the Chiari II W. Jerry Oakes malformation: an evidence-based review of
Childs Nerv Syst (2004) 20:375 381 DOI 10.1007/s00381-004-0969-4 R E V I E W P A P E R R. Shane Tubbs Treatment and management of the Chiari II W. Jerry Oakes malformation: an evidence-based review of
Basilar Invagination: cranio-cervical kyphosis rather than prolapse from the upper cervical spine
 Botelho RV, Melo Diniz J. J Neurol Neuromedicine (2017) 2(3): 15-19 www.jneurology.com Neuromedicine www.jneurology.com Mini Review Open Access Basilar Invagination: cranio-cervical kyphosis rather than
Botelho RV, Melo Diniz J. J Neurol Neuromedicine (2017) 2(3): 15-19 www.jneurology.com Neuromedicine www.jneurology.com Mini Review Open Access Basilar Invagination: cranio-cervical kyphosis rather than
Estimation of CSF Flow Resistance in the Upper Cervical Spine
 NRJ Digital - The Neuroradiology Journal 3: 49-53, 2013 www.centauro.it Estimation of CSF Flow Resistance in the Upper Cervical Spine K-A. MARDAL 1, G. RUTKOWSKA 1, S. LINGE 1.2, V. HAUGHTON 3 1 Center
NRJ Digital - The Neuroradiology Journal 3: 49-53, 2013 www.centauro.it Estimation of CSF Flow Resistance in the Upper Cervical Spine K-A. MARDAL 1, G. RUTKOWSKA 1, S. LINGE 1.2, V. HAUGHTON 3 1 Center
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Slitlike syrinx cavities: a persistent central canal
 J Neurosurg (Spine 2) 97:161 165, 2002 Slitlike syrinx cavities: a persistent central canal LANGSTON T. HOLLY, M.D., AND ULRICH BATZDORF, M.D. Division of Neurosurgery, University of California at Los
J Neurosurg (Spine 2) 97:161 165, 2002 Slitlike syrinx cavities: a persistent central canal LANGSTON T. HOLLY, M.D., AND ULRICH BATZDORF, M.D. Division of Neurosurgery, University of California at Los
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CNS Embryology 5th Menstrual Week (Dorsal View)
 Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Scoliosis is considered to be the most common skeletal
 clinical article J Neurosurg Pediatr 19:96 101, 2017 Posterior-only surgical correction of dystrophic scoliosis in 31 patients with neurofibromatosis Type 1 using the multiple anchor point method Ang Deng,
clinical article J Neurosurg Pediatr 19:96 101, 2017 Posterior-only surgical correction of dystrophic scoliosis in 31 patients with neurofibromatosis Type 1 using the multiple anchor point method Ang Deng,
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Cerebrospinal Fluid Velocity Amplitudes within the Cerebral Aqueduct in Healthy
 Page 1 of 30 1 Cerebrospinal Fluid Velocity Amplitudes within the Cerebral Aqueduct in Healthy Children and Patients with Chiari I Malformation This is the author manuscript accepted for publication and
Page 1 of 30 1 Cerebrospinal Fluid Velocity Amplitudes within the Cerebral Aqueduct in Healthy Children and Patients with Chiari I Malformation This is the author manuscript accepted for publication and
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
QF-78. S. Tanaka 1, T.Yokoyama 1, K.Takeuchi 1, K.Wada 2, T. Tanaka 2, S.Abrakawa 2, G.Kumagai 2, T.Asari 2, A.Ono 2, Y.
 QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
Chiari Drop Attacks: Surgical Decompression and the Role of Tilt Table Testing
 Original Paper Pediatr Neurosurg 2009;45:384 389 DOI: 10.1159/000260909 Received: April 15, 2009 Accepted after revision: August 4, 2009 Published online: November 26, 2009 Chiari Drop Attacks: Surgical
Original Paper Pediatr Neurosurg 2009;45:384 389 DOI: 10.1159/000260909 Received: April 15, 2009 Accepted after revision: August 4, 2009 Published online: November 26, 2009 Chiari Drop Attacks: Surgical
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
