Propranolol Blocks Ventricular Refractory Period Changes With Orthostatic Stress in Humans
|
|
|
- Eugene Hunt
- 5 years ago
- Views:
Transcription
1 1488 JACC Vol. 12, No.6 Propranolol Blocks Ventricular Refractory Period Changes With Orthostatic Stress in Humans JAMES B. MARTINS, MD, MICHAEL G. KIENZLE, MD, FACC, MICHAEL L. McCUE, RN, LUIS CONSTANTIN, MD Iowa City, Iowa The purpose of this study was to test the hypothesis that orthostatic stress shortens the right ventricular effective refractory period by reflex activation of beta-adrenergic receptors. Twelve patients undergoing electrophysiologic testing for standard clinical indications were studied. After a full electrophysiologic study, patients underwent graded lower body negative pressure before and after administration of either propranolol (0.2 mg/kg intravenously) in Group I or atropine (0.035 mg/kg intravenously) in Group II. Before the addition of drugs, lower body negative pressure produced decreases in systolic blood pressure and significant increases in sinus rate. The effective refractory period shortened from 214 ± 8 (mean ± SEM) to 206 ± 7 ms at -40 cm H 2 0 and to 197 ± 4 ms at -60 cm H 2 0 lower body negative pressure. After propranolol, Group I patients had no change in right ventricular effective refractory period despite similar changes in sinus rate and systolic blood pressure. In Group II patients, atropine did not alter effective refractory period responses to lower body negative pressure. Thus, reflex adjustments to orthostatic stress result in shortening of right ventricular effective refractory period mediated by way of beta-adrenergic mechanisms. These findings constitute the first evidence that sympathetic influences mobilized by the body can directly modulate ventricular electrophysiologic changes. (J Am Coil CardioI1988;I2: ) Autonomic influences play an important role in ventricular arrhythmogenesis, particularly after myocardial infarction. Parasympathetic influences are believed to protect against arrhythmias and beta-adrenergic influences are thought to be arrhythmogenic in experimental animals (1-3) and in humans (4--7). The electrophysiologic mechanisms for these effects are not known, but they may be direct, acting on the tissue responsible for tachycardia (2), or indirect (3) by reduction of heart rate. It is well known that beta-adrenergic influences shorten From the Cardiovascular Division, Department of Internal Medicine and the Cardiovascular Center. University of Iowa and Veterans Administration Medical Center, Iowa City, Iowa. This study was supported in part by funds from the Veterans Administration Medical Research Fund, Iowa City, and by Ischemic Specialized Center of Research Grant HL32295 from the National Heart, Lung. and Blood Institute, National Institutes of Health, Bethesda, Maryland. This work was done during Dr. Martins' tenure as an Established Investigator of the American Heart Association, Dallas, Texas. Dr. Kienzle is supported by Grant RR59, General Clinical Research Center, Bethesda, Maryland. Manuscript received February I, 1988; revised manuscript received June 22, 1988, accepted July I, Address for reprints: James B. Martins, MD, Cardiovascular Division, Department of Internal Medicine. University of Iowa Hospitals and Clinics, Iowa City. Iowa l988 by the American College of Cardiology the ventricular effective refractory period in animals (8,9) and humans (7). Human studies like the latter have involved infusions of arbitrary doses of isoproterenol, which might have questionable physiologic significance. Even though propranolol prolongs baseline ventricular effective refractory period in anesthetized animals (1,8,9), it does not substantially affect that in humans at rest (10), perhaps because there is only a small amount of background sympathetic input to the ventricle in a patient undergoing clinical electrophysiologic testing of the ventricle. We reasoned that the beta-blocking effects of propranolol would be demonstrable in patients if background sympathetic influences were augmented by an autonomic reflex. We therefore studied the effects of lower body negative pressure on the right ventricular effective refractory period in patients because lower body negative pressure is an extremely well studied physiologic stimulus (II), that increases both circulating catecholamines (11,12) and sympathetic neural firing (13) in humans. We tested the hypotheses that lower body negative pressure would shorten right ventricular effective refractory period and that this shortening would be mainly due to sympathetic influences that could be blockeq b'y propranolol /88/$3.50
2 lacc Vol. 12, No, 6 MARTINS ET AL 1489 Table 1. Clinical Features of 12 Patients Patient Age (yr) No. & Gender Cardiac Disease Indication For EPS Results of EPS Group I I 71F None Syncope (VT-NS) Negative 2 36M Myocardial infarction Palpitation (VT-NS) Negative 3 33F Mitral prolapse Syncope (VT-NS) Negative 4 24F None (VT-Sus) VT Sus 5 69M None Syncope (SVT) SVT (AVNR) 6 67M None Presyncope (VT-NS) VT-NS Group II 7 23M None Syncope (unknown) SVT (AVNR) 8 37M Aortic regurgitation Syncope (VT-NS) VT-NS 9 49F None Cardiac arrest (VT-NS) VT-NS 10 39M None Syncope (seizure) Negative II 50M Cardiomyopathy Syncope (VT-NS) Negative 12 33F None Syncope (unknown) Negative AVNR = atrioventricular node reentry; EPS = electrophysiologic study; F = female; M = male; NS = nonsustained; Sus = sustained; SVT = supraventricular tachycardia; VT = ventricular tachycardia. Methods Study patients (Table 1). Twelve patients presenting with symptoms of syncope or palpitation or known arrhythmias were studied. The patients were invited to participate in the study after its goals were explained, and each gave written informed consent for the research protocol approved by the Human Use Committee of the University of Iowa. Electrophysiologic testing. All patients underwent electrophysiologic testing in the postabsorptive and non sedated state and were not receiving cardioactive medications. Two quadripolar catheters were placed in the femoral veins by the Seldinger technique under local lidocaine anesthesia (l to 2 ml of 1% solution). The extrastimulus protocol for the clinical electrophysiologic study was performed as previously reported from this laboratory (7,14). The study protocol followed completion of the clinical study. A quadripolar catheter was placed in the right ventricular apex and thresholds were recorded to the nearest 0.1 rna. Pacing was performed at four times threshold to decrease the variability of refractory period measurements occurring at two times threshold, owing to the varying shape of the strength-interval relation in normal and abnormal ventricular myocardium (15). The current for pacing set at the beginning of the study was maintained throughout all subsequent testing including threshold determinations. Preliminary extrastimulus testing was performed to assure stable pacing without artificial repetitive responses. The catheter was then fixed to the skin and sterile drape with a plastic adhesive sheet that prevented catheter movement. The sterile drape was folded so that it lay immediately above the patient, exposing the lateral aspects of the patient's legs and hips. The patient was placed in a lower body negative pressure chamber, which was advanced to the level just below the iliac crest. A seal was formed by applying adhesive tape circumferentially around the patient's abdomen. The folded sterile sheet containing the catheters exiting from the pressure chamber was placed under the seal. Lower body negative pressure. After satisfactory seal resulting in a range of lower body negative pressure from -20 to -60 cm H 2 0, repeat threshold testing was performed at the right ventricular apex at a basic cycle length of 450 ms (lasting approximately 20 to 30 s). Then a premature stimulus (followed by a train delay) was administered to the same electrodes at a coupling interval approximately 30 to 50 ms longer than the estimated effective refractory period. After capture occurred, the premature stimulus interval was shortened in decrements of 5 ms after each eight basic stimuli until failure to capture occurred. After this sequence, the premature interval was prolonged by 10 ms and the procedure of decrementing the premature interval was repeated. The effective refractory period was defined as the longest premature interval for which the premature stimulus did not evoke a response. The data reported herein are those that were reproducible, defined as obtaining the same value of refractoriness on two separate trials. In addition, threshold measurements were unchanged, defined as varying :so. 1 rna throughout the course of testing with lower body negative pressure; threshold is not altered by sympathetic influences (8). Protocols. The sequence of study was as follows: control period; lower body negative pressure at three levels, -20, -40 and -60 cm H 2 0; and recovery 5 min after cessation of lower body negative pressure. During each period, the spontaneous heart rate was measured for 60 s while blood pressure was measured by the inflatable cuff technique. Then ventricular pacing was begun to measure the effective refractory period. These measurements were performed after 1 min at each level of lower body negative pressure.
3 1490 MARTINS ET AL. JACC Vol. 12, No.6 Table 2. Systolic Arterial Pressure Responses (mm Hg) LBNPO LBNP -20 LBNP -40 LBNP -60 Recovery Group I (n = 6) Baseline 119 ± ± ± ± 3* 119 ± 9 Propranolol 114 ± ± ± ± ± 4 Group II (n = 6) Baseline 118 ± ± ± ± ± 14 Atropine 127 ± ± 7* 106 ± 3* Not done 128 ± 5 *p < 0.05 vs. LBNP 0 for baseline or drug. LBNP = lower body negative pressure (cm H 2 O). After completion of measurements at each level, the next level of lower body negative pressure was applied without interruption. The time at each level of lower body negative pressure averaged 5 min. The patients were classified into two groups. The first group of six patients received propranolol at a dose of 0.2 mg/kg. Repeat testing with lower body negative pressure was performed 20 min after administration of propranolol. In Group II, atropine (0.035 mg/kg intravenously) was administered by bolus injection and lower body negative pressure was repeated at levels of -20 and -40 cm H 2 0. At lower body negative pressure of -60 cm H 2 0, control of heart rate during ventricular pacing was inadequate. Data analysis. Data are expressed as mean ± SEM and were analyzed with an analysis of variance employing Dunnett's test for multiple comparisons (16). Paired Student's t tests were employed to compare variables before and after drug administration. Unpaired t tests were used to compare the two groups. A p value <0.05 was considered significant. Results Clinical features (Table 1). Our patients' ages ranged from 23 to 71 years; patients in Group I tended to be older, but this difference was not significant (p > 0.25). Moreover, the magnitude of baseline reflex responses (Tables 2 to 4) did not differ between the groups. Four patients had heart disease and all had clinical indications for electrophysiologic study. Six patients had no abnormalities at the electrophysiologic study, whereas three had nonsustained ventricular tachycardia, two had atrioventricular (A V) node reentrant tachycardia and one had sustained ventricular tachycardia induced. Arterial pressure responses (Table 2). In Group I, systolic arterial pressure decreased reversibly at a lower body negative pressure of -60 cm H 2 0, whereas in Group II, a similar magnitude of change did not result in a significant decrease. After propranolol administration in Group I, systolic blood pressure did not decrease significantly during lower body negative pressure. In Group II, systolic blood pressure decreased at lower body negative pressures of - 20 and -40 cm H 2 0 after atropine. Heart rate responses (Table 3). In Group I, sinus node rate increased at a lower body negative pressure of -60 cm H 2 0. After propranolol administration, spontaneous heart rate slowed significantly compared with that before the drug was given. The sinus rate was not significantly altered by lower body negative pressure after propranolol. In Group II, sinus rate increased at all levels of lower body negative pressure. After atropine, baseline heart rate increased, but it did not increase further with lower body negative pressure. At a lower body negative pressure of -60 cm H 2 0, spontaneous heart rate exceeded that during ventricular pacing; therefore data after atropine were not recorded. Effective refractory period responses (Fig. 1, Table 4). Before propranolol or atropine, the effective refractory period shortened in both groups during lower body negative pressures of -40 and -60 cm H 2 0. Twenty minutes after intravenous administration of propranolol, the effective refractory period was not significantly altered. Lower body negative pressure produced no change in effective refractory period at any negative pressure level after propranolol Table 3. Heart Rate Responses (beats/min) LBNPO LBNP -20 Group I (n = 6) Baseline 90 ± 6 86 ± 6 Propranolol 70 ± 3t 66 ± 4 Group II (n = 6) Baseline 76 ± 4 87 ± 3* Atropine 117 ± 5t 121 ± 6 LBNP -40 LBNP -60 Recovery 96 ± ± 7* 89 ± 9 74 ± 3 77 ± 3 69 ± 5 87 ± 4* 104 ± 8* 77 ± ± 7 Not done 107 ± 5 *p < 0.05 vs. LBNP 0; tp < 0.05 vs. recovery baseline. LBNP = lower body negative pressure Jcrri H 2 0).
4 JACC Vol. 12, No.6 MARTINS ET AL Table 4. Right Ventricular Effective Refractory Period Responses (ms) LBNP 0 LBNP -20 LBNP -40 LBNP -60 Recovery Group I (n = 6) Baseline 214 ± ± ± 7* 197 ± 4* 215 ± 6 Propranolol 218 ± ± ± ± ± 6 Group II (n = 6) Baseline 209 ± ± ± 4* 196 ± 3* 210 ± 8 Atropine 199 ± ± ± 2* Not done 201 ± 2 *p < 0.05 vs. LBNP. LBNP = lower body negative pressure (cm H 2 O). administration. At no time did the configuration of the surface electrocardiogram (ECG) or intracardiac electrogram change during pacing and at no time did the late diastolic threshold vary by >0.1 rna. In Group II after atropine administration, the effective refractory period did not shorten significantly (p = 0.0. Lower body negative pressure still shortened the effective refractory period at -40 cm H 2 0 after administration of atropine; this shortening expressed as percent of lower body negative pressure 0 (3.5 ± 1.1%) was not different from that occurring before atropine was given (4.5 ± 0.8%, p > 0.2). Discussion This study demonstrates two new observations. First, orthostatic stress (lower body negative pressure) shortens right ventricular effective refractory period through activation of beta-adrenergic receptors. Second, parasympathetic influences are not involved in controlling effective refractory Figure 1. Right ventricular effective refractory period (ERP) responses (in ms) at various levels of lower body negative pressure (LBNP) before and after propranolol administered intravenously. Before propranolol, there were graded decreases in effective refractory period. After propranolol, effective refractory period did not change. u II) '" 230! 210 IL a: '" 190 r o BEFORE PROPRANOLOL AFTER PROPRANOLOL SE,. * peo.os ws. LBNP-O I o -20 LBNP (cmh,o) I > period responses to orthostatic stress. These studies clearly demonstrate a physiologic role for the sympathetic nervous system in direct modulation of the duration of the ventricular refractory period. Comparison with previous studies. Lower body negative pressure in the present study was solely performed during electrophysiologic testing with the use of single extrastimuli to measure the ventricular effective refractory period. Because all measurements and extrastimulus testing were performed in 4 to 5 min at each level of lower body negative pressure, near syncope did not occur, although others (17) observed it commonly when lower body negative pressure at levels of -40 and -60 mm Hg continued for >5 min. This lack of presyncope during lower body negative pressure in our study may have been due to our use of pacing at a cycle length of 450 ms, which reversed the bradycardia and hypotension occurring in the prior study (17). In our study, lower body negative pressure produced reversible shortening of the right ventricular effective refractory period measured at a constant pacing rate. Others (18) have measured the right ventricular effective refractory period during tilt and found that it also shortened to a similar degree. Although there are differences between these two interventions in that tilt stimulates the vestibular system and produces differential stimulation of carotid and aortic baroreceptors (11,19), these apparently do not influence the ventricular effective refractory period responses. In addition, our study demonstrated that shortening of the effective refractory period was blocked entirely by intravenous propranolol in a dose that slowed baseline sinus rate. We did not demonstrate the significant alteration in ventricular effective refractory period with intravenous atropine as previously reported by others (10). This lack of effect might have been due to the small number of patients in Group II, but a similar number of patients (five) was studied previously (10). More likely, because our patients underwent lower body negative pressure before the administration of atropine, this procedure may have conditioned them to have less parasympathetic influence at rest to the ventricle. We also did not observe atropine to potentiate the response to lower body negative pressure (greater shortening of effective refractory period); we did not see a blockade of the restrain-
5 1492 MARTINS ET AL. JACC Vol. 12, No.6 December 1988: ing influence of the parasympathetic nerves on sympathetic function with atropine. This result may be due to the ventricular effects of parasympathetic influences produced by baroreflexes, which are small as compared with sympathetic influences as manifested by previous animal experiments (9). This disparity in magnitude of parasympathetic and sympathetic effects is especially prominent when there is coincident parasympathetic withdrawal and sympathetic activation during lower body negative pressure. Possible limitations of this study. We considered other possibilities to explain our results with propranolol in Group I. It could be argued that propranolol prevented lower body negative pressure from being an effective stress because of the blunted (nonsignificant) responses of the systolic blood pressure to lower body negative pressure. However, at a lower body negative pressure of -60 cm H 2 0, a similar level of systolic arterial pressure was produced before and after propranolol, indicating that the stimulus of the lower body negative pressure was very similar before and after propranolol. A second possible concern was that the lack of effective refractory period response after propranolol reflected effects of the repeated application of lower body negative pressure and not drug effect (11). This possibility is unlikely because responses of the effective refractory period were preserved after atropine. The third possibility was that the stimulus of lower body negative pressure was altered because propranolol decreased left ventricular contractility and the sensitivity of cardiac afferents (20). However, effects on effective refractory period occurred at -40 and -60 cm H 2 0 (corresponding to -29 and -44 mm Hg) when the arterial and cardiac baroreflexes are activated by lower body negative pressure (20--22). Propranolol does not desensitize the arterial baroreflex (20); thus, it is unlikely that the effects of propranolol on cardiac sensory receptors accounted for its effect on the ventricular effective refractory period. Therefore, we conclude that propranolol prevented right ventricular effective refractory period shortening during lower body negative pressure because of blockade of beta-receptors, which prevented expression of augmented sympathetic neural and humoral influence. With the use of catheter techniques, any change in the position of the heart, such as that which might occur with lower body negative pressure, may alter the recording and pacing sites. In this study, we carefully performed the following procedures to document that results of lower body negative pressure were accurately reflecting ventricular electrophysiologic changes. First, threshold changes were measured with each intervention and found not to alter over the course of each study. Second, the effective refractory period returned to control level and lower body negative pressure. Third, the surface ECG and intracardiac electrograms did not change during ventricular pacing in any of the patients studied. Thus, the positional changes of the heart in the chest occurring with lower body negative pressure did not change the catheter position to another site which might have altered our data. Increases in sympathetic neural influence to the ventricles may produce dispersion of ventricular refractoriness and may predispose to ventricular fibrillation (23). Changes in the right ventricular effective refractory period do not necessarily demonstrate dispersion because lower body negative pressure also increases circulating epinephrine (11,12). We did not measure dispersion of refractory periods; however, we did not observe any QT interval or T wave changes consistent with altered sympathetic neural input to the heart. Clinical implications. Recent observations in patients have suggested that parasympathetic influences do modulate ventricular refractoriness (10) and interrupt ventricular tachycardia (24,25). The present study documents the modulating effect of physiologically activated sympathetic influences on duration of ventricular refractory period, but we did not investigate such influences on spontaneous or inducible arrhythmias in our patients. However, in a preliminary series of patients with repetitive monomorphic ventricular tachycardia from our laboratory (26), lower body Regative pressure appeared to be similar to infusion of isoproterenol in facilitation of tachycardia. Specifically, both interventions shortened right ventricular refractoriness and tachycardia cycle length and facilitated induction of ventricular tachycardia during extrastimulus testing. At this time, we do not know whether lower body negative pressure will facilitate induction of clinically occurring ventricular tachycardias associated with prior myocardial infarction. Because nearly all such ventricular tachycardias are induced with premature stimulation alone and because at least short-term administration of a beta-blocking agent is not effective in preventing tachycardia induction, the frequency of facilitation of such induction may not be common. However, reentry is the likely mechanism of these inducible ventricular tachycardias, and shortening of refractoriness in tissue critical to the circuit may facilitate tachycardia induction on occasion (7). Further work is needed to assess whether physiologic augmentation of sympathetic influences by lower body negative pressure during extrastimulus testing will be useful in predicting efficacy of adrenergic blockade, as has been demonstrated with isoproterenol (7). Because of the physiologic activation of sympathetic influences, lower body negative pressure may be a better means than infused isoproterenol of testing responses of arrhythmias to betaadrenergic blocking drugs. We thank Rosanne Hopson for assistance in data collection and Linda Bang for expert secretarial assistance. We also thank Allyn L. Mark, MD for continued encouragement and advice.
6 JACC Vol. 12, No.6 December 1988: MARTINS ET AL References I. Gang ES, Bigger JT, Uhl EW. Effects of timolol and propranolol on inducible sustained ventricular tachyarrhythmias in dogs with subacute myocardial infarction. Am J Cardiol 1984;53: Martins JB. Autonomic control of ventricular tachycardia: sympathetic neural influences on spontaneous tachycardia 24 hours after coronary occlusion. Circulation 1985;72: Patterson E, Scherlag BJ, Lazzara R. Mechanism of prevention of sudden death by nadolol: differential actions on arrhythmia triggers and substrate after myocardial infarction in the dog. J Am Coli Cardiol 1986;8: Beta-BHA Study Group. The Beta Blocker Heart Attack Trial. JAMA 1981 ;246: MIAMI Group Trial Research. Metoprolol in acute myocardial infarction: mortality. Am J CardioI1985;56:15G-22G. 6. Mason JW, Winkle RA. Electrode-catheter arrhythmia induction in the selection and assessment of antiarrhythmic drug therapy for recurrent ventricular tachycardia. Circulation 1978;58: Olshansky B, Martins JB. Usefulness of isoproterenol facilitation of ventricular tachycardia induction during extrastimulus testing in predicting effective chronic therapy with beta-adrenergic blockade. Am J Cardiol 1987;59: Martins JB, Zipes DP. Effects of sympathetic and vagal nerves on recovery properties of the endocardium and epicardium of the canine left ventricle. Circ Res 1980;46: Martins JB. Carotid sinus baroreflex influence on electrophysiology of the canine atrioventricular node and ventricle. Am J Cardiol 1984;54:431--{'. 10. Prystowsky EN, Jackman WM, Rinkenberger RL, Heger 11, Zipes DP. Effect of autonomic blockade on ventricular refractoriness and atrioventricular nodal conduction in humans. Circ Res 1981 ;49: Woldhuis RA, Bergman SA, Nicogossian AE. Physiological effects of locally applied reduced pressure in man. Physiol Rev 1974;54: Mohanty PK, Sowers JR, Beck F, et al. Catecholamine, renin, aldosterone, and arginine vasopressin responses to lower body negative pressure and tilt in normal man: effect of bromocriptine. J Cardiovasc Pharmacol 1985;7:104(}"' SundlofG, Wallin BG. Effect of lower body negative pressure on human muscle nerve sympathetic activity. J Physiol 1978;278: Olshansky B, Mazuz M, Martins JB. Significance of inducible tachycardia in patients with syncope of unknown origin: a long term follow-up. J Am Coli Cardiol 1985;5: Michelson EL, Spear JF, Moore EN. Strength-interval relations in a chronic canine model of myocardial infarction. Circulation 1981 ;63: Steel RGD, Torrie JH. Principles and Procedures of Statistics. New York: McGraw-Hill, Stevens PM, Lamb LE. Effects of lower body negative pressure on the cardiovascular system. Am J CardioI1965;16: Hermiller JB, Walker SS, Binkley PF, et al. The electrophysiologic effects of upright posture. Am Heart J 1984;108: I 25(} Eckberg DL. Parasympathetic cardiovascular control in human disease: a critical review of methods and results. Am J PhysioI1980;239:H581-H Ferguson OW, Thames MD, Mark AL. Effects of propranolol on reflex vascular responses to orthostatic stress in humans: role of ventricular baroreceptors. Circulation 1983;67: Zoller RP, Mark AL, Abboud FM, Schmid PG, Heistad DO. Role of low pressure baroreceptors in reflex vasoconstrictor responses in man. J Clin Invest 1972;51:2% Johnson JM, Rowell LB, Niederberger M, Eisman MM. Human splanchnic and forearm vasoconstrictor responses to reductions of right atrial and aortic pressures. Circ Res 1974;34: Han 11, Alon PGD, Moe GK. Adrenergic effects on ventricular vulnerability. Circ Res 1964;14: Waxman MB, Wald RW. Termination of ventricular tachycardia by an increase in cardiac vagal drive. Circulation 1977;56: Hess OS, Hanlon T, Scheinman M, Budge R, Desai J. Termination of ventricular tachycardia by carotid sinus massage. Circulation 1982;65: Kienzle MG, Martins JB, Constantin L, McCue ML. Autonomic influence in repetitive monomorphic ventricular tachycardia: effects of sympathetic activation (abstrj. Circulation 1986;74(suppllI):II-127.
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Bernard Belhassen, MD; Roman Fish, MD; Sami Viskin, MD; Aharon Glick, MD; Michael Glikson, MD; Michael Eldar, MD
 www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
Use of Electrophysiologic Testing in Patients With Nonsustained Ventricular Tachycardia Prognostic and Therapeutic Implications
 JACC Vol. 14, No. I July 1 8 1 5 5-61 155 ELECTROPHYSIOLOGIC STUDIES Use of Electrophysiologic Testing in Patients With Nonsustained Ventricular Tachycardia Prognostic and Therapeutic Implications RICHARD
JACC Vol. 14, No. I July 1 8 1 5 5-61 155 ELECTROPHYSIOLOGIC STUDIES Use of Electrophysiologic Testing in Patients With Nonsustained Ventricular Tachycardia Prognostic and Therapeutic Implications RICHARD
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Atrial fibrillation (AF) is the most common sustained
 Effect of Atrial Fibrillation and an Irregular Ventricular Response on Sympathetic Nerve Activity in Human Subjects Stephen L. Wasmund, PhD; Jian-Ming Li, MD, PhD; Richard L. Page, MD; Jose A. Joglar,
Effect of Atrial Fibrillation and an Irregular Ventricular Response on Sympathetic Nerve Activity in Human Subjects Stephen L. Wasmund, PhD; Jian-Ming Li, MD, PhD; Richard L. Page, MD; Jose A. Joglar,
The autonomic nervous system is known to play an
 Effects of Continuous Enhanced Vagal Tone on Dual Atrioventricular Node and Accessory Pathways Chuen-Wang Chiou, MD; Shih-Ann Chen, MD; Ming-Ho Kung, MD; Mau-Song Chang, MD; Eric N. Prystowsky, MD Background
Effects of Continuous Enhanced Vagal Tone on Dual Atrioventricular Node and Accessory Pathways Chuen-Wang Chiou, MD; Shih-Ann Chen, MD; Ming-Ho Kung, MD; Mau-Song Chang, MD; Eric N. Prystowsky, MD Background
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular Nodal Reentrant Tachycardia
 645 Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular dal Reentrant Tachycardia S. ADAM STRICKBERGER, M.D., EMILE DAOUD, M.D., MARK
645 Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular dal Reentrant Tachycardia S. ADAM STRICKBERGER, M.D., EMILE DAOUD, M.D., MARK
Differentiating Junctional Tachycardia and Atrioventricular Node Re-Entry Tachycardia Based on Response to Atrial Extrastimulus Pacing
 Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
An Approach to the Patient with Syncope. Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva
 An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
Ventricular ectopic activity after premature atrial beats
 British Heart Journal, 1977, 39, 1033-1037 Ventricular ectopic activity after premature atrial beats in acute myocardial infarction1 R. J. MYERBURG, R. J. SUNG, G. GERSTENBLITH, STEPHEN M. MALLON, AND
British Heart Journal, 1977, 39, 1033-1037 Ventricular ectopic activity after premature atrial beats in acute myocardial infarction1 R. J. MYERBURG, R. J. SUNG, G. GERSTENBLITH, STEPHEN M. MALLON, AND
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
CLINICAL INVESTIGATIONS. Methods
 CLINICAL INVESTIGATIONS Jpn Circ J 2001; 65: 702 706 Correlation Between the Effective Refractory Period and Activation-Recovery Interval Calculated From the Intracardiac Unipolar Electrogram of Humans
CLINICAL INVESTIGATIONS Jpn Circ J 2001; 65: 702 706 Correlation Between the Effective Refractory Period and Activation-Recovery Interval Calculated From the Intracardiac Unipolar Electrogram of Humans
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia
 www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
Reversion of ventricular tachycardia by pacemaker stimulation
 British Heart Journal, 1971, 33, 922-927. Reversion of ventricular tachycardia by pacemaker stimulation M. A. Bennett and B. L. Pentecost From the General Hospital, Birmingham 4 Reversion of ventricular
British Heart Journal, 1971, 33, 922-927. Reversion of ventricular tachycardia by pacemaker stimulation M. A. Bennett and B. L. Pentecost From the General Hospital, Birmingham 4 Reversion of ventricular
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
were inserted into the right femoral vein and positioned system and intracardiac recordings were displayed
 CASE REPORTS Termination of Ventricular Tachycardia by Carotid Sinus Massage DAVID S. HESS, M.D., TIMOTHY HANLON, M.D., MELVIN SCHEINMAN, M.D., ROGER BUDGE, M.D., AND JAWAHAR DESAI, M.D. SUMMARY Intracardiac
CASE REPORTS Termination of Ventricular Tachycardia by Carotid Sinus Massage DAVID S. HESS, M.D., TIMOTHY HANLON, M.D., MELVIN SCHEINMAN, M.D., ROGER BUDGE, M.D., AND JAWAHAR DESAI, M.D. SUMMARY Intracardiac
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
V. TACHYCARDIAS Rapid rhythm abnormalities
 V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Medicine. Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract
 Medicine CLINICAL CASE REPORT Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract A Case Report Li Yue-Chun, MD, Lin Jia-Feng,
Medicine CLINICAL CASE REPORT Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract A Case Report Li Yue-Chun, MD, Lin Jia-Feng,
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways
 Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Mechanism of Ventricular Tachycardia Termination by Pacing at Left Ventricular Sites in Patients with Coronary Artery Disease
 Journal of Interventional Cardiac Electrophysiology 6, 35 41, 2002 C 2002 Kluwer Academic Publishers. Manufactured in The Netherlands. Mechanism of Ventricular Tachycardia Termination by Pacing at Left
Journal of Interventional Cardiac Electrophysiology 6, 35 41, 2002 C 2002 Kluwer Academic Publishers. Manufactured in The Netherlands. Mechanism of Ventricular Tachycardia Termination by Pacing at Left
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
Idiopathic Long QT Syndrome With Early Afterdepolarization Induced by Epinephrine
 CASE REPORTS Circ J 2004; 68: 587 591 Idiopathic Long QT Syndrome With Early Afterdepolarization Induced by Epinephrine A Case Report Norifumi Urao, MD; Hirokazu Shiraishi, MD; Kazuya Ishibashi, MD; Masayuki
CASE REPORTS Circ J 2004; 68: 587 591 Idiopathic Long QT Syndrome With Early Afterdepolarization Induced by Epinephrine A Case Report Norifumi Urao, MD; Hirokazu Shiraishi, MD; Kazuya Ishibashi, MD; Masayuki
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract
 191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες. Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο
 Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο Όλες οι κοιλιακές αρρσθμίες δεν είναι ίδιες Υπάρτοσν διαθορές ζηον πληθυσμό, ηον μηχανισμό
Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο Όλες οι κοιλιακές αρρσθμίες δεν είναι ίδιες Υπάρτοσν διαθορές ζηον πληθυσμό, ηον μηχανισμό
Unusual Tachycardia Association In A patient Without Structural Heart Disease
 www.ipej.org 233 Case Report Unusual Tachycardia Association In A patient Without Structural Heart Disease Eduardo Arana-Rueda, Alonso Pedrote, Lorena Garcia-Riesco, Manuel Frutos-Lopez, Juan A. Sanchez-Brotons
www.ipej.org 233 Case Report Unusual Tachycardia Association In A patient Without Structural Heart Disease Eduardo Arana-Rueda, Alonso Pedrote, Lorena Garcia-Riesco, Manuel Frutos-Lopez, Juan A. Sanchez-Brotons
Title. CitationJournal of Electrocardiology, 43(5): Issue Date Doc URL. Type. File Information.
 Title Pleomorphic ventricular tachycardia originating from Author(s)Yokoshiki, Hisashi; Mitsuyama, Hirofumi; Watanabe, M CitationJournal of Electrocardiology, 43(5): 452-458 Issue Date 2010-09 Doc URL
Title Pleomorphic ventricular tachycardia originating from Author(s)Yokoshiki, Hisashi; Mitsuyama, Hirofumi; Watanabe, M CitationJournal of Electrocardiology, 43(5): 452-458 Issue Date 2010-09 Doc URL
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block
 185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
Journal of the American College of Cardiology Vol. 36, No. 2, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
Utility of Atrial and Ventricular Cycle Length Variability in Determining the Mechanism of Paroxysmal Supraventricular Tachycardia
 698 Utility of Atrial and Ventricular Cycle Length Variability in Determining the Mechanism of Paroxysmal Supraventricular Tachycardia THOMAS C. CRAWFORD, M.D., SIDDHARTH MUKERJI, M.D., ERIC GOOD, D.O.,
698 Utility of Atrial and Ventricular Cycle Length Variability in Determining the Mechanism of Paroxysmal Supraventricular Tachycardia THOMAS C. CRAWFORD, M.D., SIDDHARTH MUKERJI, M.D., ERIC GOOD, D.O.,
Effect of an increase in coronary perfusion on transmural. ventricular repolarization
 Effect of an increase in coronary perfusion on transmural ventricular repolarization Yan-Zhou Zhang 1, MD, PhD, Ben He 1, MD, Le-Xin Wang 2, MD, PhD. From: 1 Department of Cardiology, Renji Hospital, Medical
Effect of an increase in coronary perfusion on transmural ventricular repolarization Yan-Zhou Zhang 1, MD, PhD, Ben He 1, MD, Le-Xin Wang 2, MD, PhD. From: 1 Department of Cardiology, Renji Hospital, Medical
Tachycardia-induced heart failure - Does it exist?
 Tachycardia-induced heart failure - Does it exist? PD Dr Etienne Delacrétaz Clinique Cecil et Hôpital de Fribourg SSC Cardiology meeting 2015 Zürich Rapid atrial fibrillation is a common cause of heart
Tachycardia-induced heart failure - Does it exist? PD Dr Etienne Delacrétaz Clinique Cecil et Hôpital de Fribourg SSC Cardiology meeting 2015 Zürich Rapid atrial fibrillation is a common cause of heart
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
COMPLEX CASE STUDY INNOVATIVE COLLECTIONS. Case presentation
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation
 J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
Effect of an Increase in Coronary Perfusion on Transmural Ventricular Repolarization
 Physiol. Res. 56: 285-290, 2007 Effect of an Increase in Coronary Perfusion on Transmural Ventricular Repolarization Y.-Z. ZHANG 1, B. HE 1, L.-X. WANG 2 1 Department of Cardiology, Renji Hospital, Medical
Physiol. Res. 56: 285-290, 2007 Effect of an Increase in Coronary Perfusion on Transmural Ventricular Repolarization Y.-Z. ZHANG 1, B. HE 1, L.-X. WANG 2 1 Department of Cardiology, Renji Hospital, Medical
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway
 Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Case 1 Left Atrial Tachycardia
 Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Electrical Storm in Coronary Artery Disease. Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic July 2016
 Electrical Storm in Coronary Artery Disease Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic July 2016 48 yrs. Old diabetic with ACS 48 yrs. Old diabetic with ACS
Electrical Storm in Coronary Artery Disease Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic July 2016 48 yrs. Old diabetic with ACS 48 yrs. Old diabetic with ACS
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Repetitive ventricular response
 BrHeartJ7 1981; 46: 152-8 Repetitive ventricular response Prevalence and prognostic significance GERALD V NACCARELLI, ERIC N PRYSTOWSKY, WARREN M JACKMAN, JAMES J HEGER, ROBERT L RINKENBERGER, DOUGLAS
BrHeartJ7 1981; 46: 152-8 Repetitive ventricular response Prevalence and prognostic significance GERALD V NACCARELLI, ERIC N PRYSTOWSKY, WARREN M JACKMAN, JAMES J HEGER, ROBERT L RINKENBERGER, DOUGLAS
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
Journal of the American College of Cardiology Vol. 37, No. 2, by the American College of Cardiology ISSN /01/$20.
 Journal of the American College of Cardiology Vol. 37, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)01133-5 Coronary
Journal of the American College of Cardiology Vol. 37, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)01133-5 Coronary
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
Journal of the American College of Cardiology Vol. 36, No. 1, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 1, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00699-9 Increased
Journal of the American College of Cardiology Vol. 36, No. 1, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00699-9 Increased
Ventricular arrhythmias in acute coronary syndromes. Dimitrios Manolatos, MD, PhD, FESC Electrophysiology Lab Evaggelismos General Hospital
 Ventricular arrhythmias in acute coronary syndromes Dimitrios Manolatos, MD, PhD, FESC Electrophysiology Lab Evaggelismos General Hospital introduction myocardial ischaemia and infarction leads to severe
Ventricular arrhythmias in acute coronary syndromes Dimitrios Manolatos, MD, PhD, FESC Electrophysiology Lab Evaggelismos General Hospital introduction myocardial ischaemia and infarction leads to severe
Results of Catheter Ablation of Ventricular Tachycardia Using Direct Current Shocks
 Results of Catheter Ablation of Ventricular Tachycardia Using Direct Current Shocks FRED MORADY, MELVIN M. SCHEINMAN, JERRY C. GRIFFIN, JOHN M. HERRE, and WILLIAM H. KOU From the Divisions of Cardiology,
Results of Catheter Ablation of Ventricular Tachycardia Using Direct Current Shocks FRED MORADY, MELVIN M. SCHEINMAN, JERRY C. GRIFFIN, JOHN M. HERRE, and WILLIAM H. KOU From the Divisions of Cardiology,
Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing
 Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Effects of intravenous amiodarone on ventricular refractoriness, intraventricular conduction, and ventricular tachycardia induction
 Europace (2000) 2, 207 215 doi:10.1053/eupc.2000.0099, available online at http://www.idealibrary.com on Effects of intravenous amiodarone on ventricular refractoriness, intraventricular conduction, and
Europace (2000) 2, 207 215 doi:10.1053/eupc.2000.0099, available online at http://www.idealibrary.com on Effects of intravenous amiodarone on ventricular refractoriness, intraventricular conduction, and
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Catheter Ablation of VT Without Structural Heart Disease 성균관의대 온영근
 Catheter Ablation of VT Without Structural Heart Disease 성균관의대 온영근 Idiopathic Monomorphic Ventricular Tachycardia Adenosine-sensitive Verapamil-sensitive Propranolol-sensitive Mech (Triggered activity)
Catheter Ablation of VT Without Structural Heart Disease 성균관의대 온영근 Idiopathic Monomorphic Ventricular Tachycardia Adenosine-sensitive Verapamil-sensitive Propranolol-sensitive Mech (Triggered activity)
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013
 Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Patient Examination. Objectives for Presentation RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS 9/8/2016
 RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
Tachycardias II. Štěpán Havránek
 Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY
 PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
Syncope: Evaluation of the Weak and Dizzy
 Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Risk Factors for Sudden cardiac Death
 Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
Syncope: Evaluation of the Weak and Dizzy
 Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
VENTRICULAR TACHYCARDIA WITH HEMODYNAMIC INSTABILITY REFRACTORY TO CARDIOVERSION: A CASE REPORT
 VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
Where are the normal pacemaker and the backup pacemakers of the heart located?
 CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
What is Closed Loop Stimulation?
 May 1998 49 What is Closed Loop Stimulation? M. SCHALDACH Department of Biomedical Engineering, University Erlangen-Nuremberg, Erlangen, Germany Summary Improving the patient s quality-of-life has become
May 1998 49 What is Closed Loop Stimulation? M. SCHALDACH Department of Biomedical Engineering, University Erlangen-Nuremberg, Erlangen, Germany Summary Improving the patient s quality-of-life has become
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12
 A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
SHOCK THE PATIENT. Disclosures. Goals of the Talk. Tachyarrhythmias- Unstable 11/7/2017
 Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Journal of the American College of Cardiology Vol. 33, No. 3, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 3, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00614-7 A Technique
Journal of the American College of Cardiology Vol. 33, No. 3, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00614-7 A Technique
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
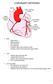 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B. Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D.
 Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Reflex Vascular Responses to Left. Ventricular Baroreceptors in Dogs. Ventricular Outflow Obstruction and Activation of. formn 15 January 1973.
 Reflex Vascular Responses to Left Ventricular Outflow Obstruction and Activation of Ventricular Baroreceptors in Dogs ALLYN L. MARK, FRANCOIS M. ABBOUD, PHILLIP G. SCHMID, and DONALD D. HISTAD with the
Reflex Vascular Responses to Left Ventricular Outflow Obstruction and Activation of Ventricular Baroreceptors in Dogs ALLYN L. MARK, FRANCOIS M. ABBOUD, PHILLIP G. SCHMID, and DONALD D. HISTAD with the
