Tohoku J. Exp. Med., 2015, 236, Current Management of Moyamoya Disease 45
|
|
|
- Austen Rodgers
- 5 years ago
- Views:
Transcription
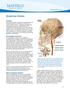
1 Tohoku J. Exp. Med., 2015, 236, Current Management of Moyamoya Disease 45 Invited Review Current Status of Revascularization Surgery for Moyamoya Disease: Special Consideration for Its Internal Carotid-External Carotid (IC-EC) Conversion as the Physiological Reorganization System Miki Fujimura 1 and Teiji Tominaga 1 1 Department of Neurosurgery, Tohoku University Graduate School of Medicine, Sendai, Miyagi, Japan Moyamoya disease is a chronic cerebrovascular disease with unknown etiology, which is characterized by bilateral steno-occlusive changes at the terminal portion of the internal carotid artery and an abnormal vascular network formation at the base of the brain. Moyamoya disease is known to have unique and dynamic nature to convert the vascular supply for the brain from internal carotid (IC) system to the external carotid (EC) system, as indicated by Suzuki s angiographic staging established in Insufficiency of this IC-EC conversion system may result in cerebral ischemia, as well as in intracranial hemorrhage from inadequate collateral vascular network, both of which represent the clinical presentation of moyamoya disease. Therefore, surgical revascularization by extracranial-intracranial bypass is the preferred procedure for moyamoya disease to complement IC-EC conversion and thus to avoid cerebral infarction and/or intracranial hemorrhage. Long-term outcome of revascularization surgery for moyamoya disease is favorable, but rapid increase in cerebral blood flow on the affected hemisphere could temporarily cause unfavorable phenomenon such as cerebral hyperperfusion syndrome. We would review the current status of revascularization surgery for moyamoya disease based on its basic pathology, and sought to discuss the significance of measuring cerebral blood flow in the acute stage and intensive perioperative management. Keywords: cerebral blood flow; extracranial-intracranial bypass; moyamoya disease; perioperative management; single-photon emission computed tomography Tohoku J. Exp. Med., 2015 May, 236 (1), Tohoku University Medical Press Introduction Moyamoya disease is a chronic, occlusive cerebrovascular disease with unknown etiology characterized by a unique and dynamic nature to convert the vascular supply for the cerebral hemisphere from internal carotid (IC) system to the external carotid (EC) system, so called IC-EC conversion disease (Suzuki and Takaku 1969; Fujimura and Tominaga 2012b). In most of the literature, the characteristic of moyamoya disease is represented by its typical angiographic finding at the transitional state of IC-EC conversion, when steno-occlusive change at the terminal portion of the internal carotid artery (ICA) and an abnormal vascular network at the base of the brain are evident (Fig. 1). Extracranial-intracranial bypass, such as superficial temporal artery-middle cerebral artery (STA-MCA) anastomosis, is generally employed as the standard surgical treatment for moyamoya disease to complement IC-EC conversion and thus prevent cerebral ischemic attacks (Fukui 1997; Houkin et al. 1997). Recently, the extracranial-intracranial bypass was also shown to reduce the risk of rebleeding in hemorrhagic-onset patients with moyamoya disease by the Japan Adult Moyamoya (JAM) trial: a multicenter randomized control trial to compare the incidence of re-bleeding rate between surgical and non-surgical groups of hemorrhagic-onset moyamoya disease (Miyamoto et al. 2014). Long-term outcome of the extracranial-intracranial bypass for moyamoya disease is favorable, but cerebral ischemia and hyperperfusion syndrome are potential complications of this procedure, which could lead to neurological deterioration in the acute stage (Fujimura et al. 2007; Kim et al. 2008; Ohue et al. 2008). We sought to review the current status of revascularization surgery for moyamoya disease based on its basic pathology, and sought to discuss the significance of measuring cerebral blood flow Received April 13, 2015; revised and accepted April 23, Published online May 13, 2015; doi: /tjem Correspondence: Miki Fujimura, M.D., Ph.D., Department of Neurosurgery, Tohoku University Graduate School of Medicine, 1-1 Seiryo-machi, Aoba-ku, Sendai, Miyagi , Japan. fujimur@nsg.med.tohoku.ac.jp Dr. Miki Fujimura is a recipient of the 2014 Gold Prize, Tohoku University School of Medicine. 45
2 46 M. Fujimura and T. Tominaga Fig. 1. Representative finding of the catheter angiography of moyamoya disease. Bilateral carotid angiogram demonstrates steno-occlusive changes at the terminal ICA associated with the abnormal vascular network formation at the base of the brain. (CBF) in the acute stage and intensive perioperative management after revascularization surgery. Diagnosis of moyamoya disease Diagnostic criteria It had been required that steno-occlusive change at ICA should be evident bilaterally for the definitive diagnosis of moyamoya disease (Research Committee on the Pathology and Treatment of Spontaneous Occlusion of the Circle of Willis; Health Labour Sciences Research Grant for Research on Measures for Intractable Diseases 2012). In light of the increasing number of the patients with unilateral involvement (Hayashi et al. 2014) as well as the evidence that substantial number of unilateral cases could progress to the bilateral presentation (Kuroda et al. 2005), diagnostic criteria of the definitive moyamoya disease was revised to include patients, demonstrating both bilateral and unilateral involvement of terminal ICA stenosis associated with abnormal vascular network at the base of the brain with unknown etiology, as stated by the Research Committee of Moyamoya Disease of the Japanese Ministry of Health, Labour, and Welfare in Diagnostic criteria also state that definitive diagnosis of moyamoya disease requires catheter angiography in unilateral cases while bilateral cases could be promptly diagnosed by either catheter angiography or magnetic resonance (MR) imaging/angiography. Modern supportive diagnostic tools Definitive diagnosis of moyamoya disease is not always easy, especially in patients with early stage of Suzuki s angiographic grading (Suzuki and Takaku 1969), when abnormal vascular network is not yet evident. To resolve this critical issue, it is essential to understand the diagnostic value of high resolution MR imaging focusing on vascular wall anatomy of moyamoya disease. Kaku and colleagues (2012) recently proposed the constrictive remodeling theory that outer diameter narrowing of the affected intracranial vessels was the early characteristic change of moyamoya disease as demonstrated by three-dimensional (3D) constructive interference in steady-state (CIISS) MR image. Yuan et al. (2015) also reported that the vascular wall thinning and the arterial outer diameter narrowing shown by high resolution MR imaging could be the early morphological changes characteristic to moyamoya disease. Taken together, the high resolution MR imaging including 3D-CISS could provide the supportive information for the accurate diagnosis of moyamoya disease especially in the early angiographic stage. Alternatively, genetic analysis as described in the next paragraph would also provide supportive information for the diagnosis of moyamoya disease. Etiology of moyamoya disease Genetics: significance of RNF213 susceptibility gene The etiology of moyamoya disease remains unknown, while recent findings suggest the importance of genetic factors (Ikeda et al. 1999; Inoue et al. 2000; Yamauchi et al. 2000; Sakurai et al. 2004). A more recent genome-wide association study identified the ring finger protein (RNF) 213 gene (RNF213) in the 17q25-ter region as a susceptibility gene for moyamoya disease among East Asian population (Kamada et al. 2011), although the exact function of RNF213 is undetermined. We previously reported that a single-nucleotide polymorphism (SNP) of c.14576g>a in RNF213 was detected in 95% of familial moyamoya diseases and 79% of sporadic cases among Japanese patients (Kamada et al. 2011). Although the mechanism underlying SNP of RNF213 in moyamoya disease patients is undetermined, recent in vivo experiment using the RNF213- deficient mice may give clue to address this important question. We reported that the target disruption of RNF213 did not develop moyamoya disease in the RNF213-deficient mice (Sonobe et al. 2014), but post-ischemic angiogenesis was significantly enhanced in mice lacking RNF213 after chronic hind-limb ischemia (Ito et al. 2015), suggesting the potential role of the RNF213 abnormality in the development of abnormal vascular networks in chronic ischemia. Further investigation with RNF213-deficient mice under variety of additional insults such as chronic brain ischemia and/or immune-adjuvants administration may provide new insight to clarify the etiology of moyamoya disease. Environmental factors underlying moyamoya disease As indicated by the basic research using genetic engineered mice of RNF213, moyamoya disease susceptibility gene, genetic abnormality is important but not the exclusive factor to develop moyamoya disease. Environmental factors as the secondary insults in addition to the genetic abnormality might be important to develop moyamoya disease, because RNF213 polymorphism characteristic to moyamoya disease is also evident in 1.4% of the normal
3 Current Management of Moyamoya Disease 47 control population (Kamada et al. 2011). Regarding the candidate of the secondary insults, infection, autoimmunity, other inflammatory conditions, and cranial irradiation are implicated in the etiology of moyamoya disease (Research Committee on the Pathology and Treatment of Spontaneous Occlusion of the Circle of Willis; Health Labour Sciences Research Grant for Research on Measures for Intractable Diseases 2012). Among them, autoimmune response could be the strongest candidate as the secondary insult to develop moyamoya disease, in light of the high prevalence of Graves disease; autoimmune hyperthyroidism among East Asia patients with moyamoya disease (Kim et al. 2010). Alternatively, RNF213 polymorphism could directly affect autoimmunity and thus contribute to the development of moyamoya disease, because RNF213 is predominantly expressed in white blood cells and spleen (Kamada et al. 2011). Revascularization surgery for moyamoya disease Concept of revascularization surgery Due to the insufficiency of IC-EC conversion at the transitional stage, such as at stage 3 and stage 4 of Suzuki s angiographic staging (Suzuki and Takaku 1969), substantial number of patients manifest as ischemic symptom and/or intracranial hemorrhage, while some patients may alternatively achieve favorable IC-EC conversion without undergoing surgical intervention, as often seen in asymptomatic adult patients. While considering the pathological condition of each patient, it is essential to go back to Suzuki s angiographic staging and to consider the patients angiographic and hemodynamic status. Concept of revascularization surgery for moyamoya disease includes both microsurgical reconstruction by STA- MCA anastomosis and the consolidation for future vasculogenesis by indirect pial synangiosis such as encephalo-myosynangiosis and encephalo-duro-arterio-synangiosis (Fujimura and Tominaga 2012b). Both concepts may attempt to convert the vascular supply for the brain from IC system to the EC system, which again match the physiological nature of moyamoya disease. Thus the concept of revascularization surgery for moyamoya disease is based on the idea to complement the intrinsic compensatory nature of moyamoya disease, rather than to eradicate the intrinsic nature of this entity (Fujimura and Tominaga 2012b). Alternatively, rapid increase in CBF provided by direct extracranial-intracranial bypass could provide temporary impact to the affected brain, because IC-EC conversion is usually attempted during lengthy time period in the natural course of moyamoya disease. Guideline recommendation Surgical revascularization prevents cerebral ischemic attack by improving CBF. Direct revascularization surgery such as STA-MCA anastomosis is established as an effective procedure for the moyamoya disease patients with ischemic symptoms, providing long-term favorable outcomes. In fact, the Japanese Stroke Guideline recommends direct revascularization surgery for the patients with moyamoya disease manifesting as cerebral ischemic symptoms (Recommendation grade B) (Research Committee on the Pathology and Treatment of Spontaneous Occlusion of the Circle of Willis; Health Labour Sciences Research Grant for Research on Measures for Intractable Diseases 2012). Intraoperative views are shown in Fig. 2. Regarding hem- Fig. 2. Intra-operative view of STA-MCA anastomosis. Surgical view before (A), during (B), and after right STA-MCA anastomosis (C, D). Arrows in C and D indicate the site of the anastomosis. Indocyanine green video-angiography demonstrated apparently patent bypass with favorable distribution of bypass flow.
4 48 M. Fujimura and T. Tominaga orrhagic-onset patients, revascularization could be considered but adequate scientific evidence had been lacking (Recommendation grade C1). Nevertheless, recent evidence by JAM trial strongly encourages direct revascularization surgery for reducing the risk for re-bleeding in adult moyamoya disease patients presenting with intracranial hemorrhage (Miyamoto et al. 2014), although the statistical significance was marginal. Sub-group analysis of the JAM trial is currently undertaken to further clarify the patient population among hemorrhagic-onset moyamoya disease in which revascularization surgery exerts particular benefit by preventing re-bleeding. Finally, revascularization surgery for asymptomatic moyamoya disease patients is not recommended due to the uncertainty of the natural history of this patient population (Kuroda et al. 2007). To answer this important question, asymptomatic moyamoya registry (AMORE) study; multicenter observational study is currently undertaken in Japan to clarify the natural history of asymptomatic moyamoya disease (Kuroda et al. 2015). Surgical complications Cerebral ischemia such as peri-operative cerebral infarction Revascularization surgery for moyamoya disease is based on the physiological concept as indicated by IC-EC conversion theory, but it includes potential issue of the rapid CBF increase in the chronic ischemic brain, which may underlay the surgical complications of this procedure (Fig. 3). Surgical complications of moyamoya disease include both neurological and non-neurological complications, and neurological complications include peri-operative cerebral infarction and cerebral hyperperfusion syndrome (Table 1). Regarding the perioperative cerebral infarction, following distinct pathologies are reported as the possible mechanisms underlying peri-operative ischemia. Firstly, Hayashi et al. (2010) proposed watershed shift phenomenon as an intrinsic hemodynamic ischemia at the adjacent cortex to the STA-MCA bypass for child-onset moyamoya disease. Retrograde blood supply from STA-MCA bypass may interfere with the anterograde blood flow from proximal MCA, and thus result in the temporary decrease in CBF at the cortex supplied by the adjacent branch of MCA. The watershed shift phenomenon could lead to subsequent cerebral infarction among pediatric moyamoya disease (Hayashi et al. 2010). Besides hemodynamic ischemia due to watershed shift phenomenon, thrombo-embolic complication originated from the anastomosed site (Fujimura et al. 2008) and the mechanical compression by swollen temporal muscle flap could also cause cerebral ischemia in the acute stage (Fujimura et al. 2009a). Based on these observations, we believe that proper perioperative hydration, hemoglobin concentration maintenance, and routine use of anti-platelet agent are essential to avoid ischemic complications (Fujimura et al. 2012a). It is important to differentiate these distinct pathologies by CBF measurement and MR imaging/angiography in the acute stage for the accurate diagnosis and prompt perioperative management (Fig. 3). The management of each pathological condition is summarized in Table 1. Cerebral hyperperfusion syndrome Because the pial artery network is markedly affected in moyamoya disease patients (Kim et al. 2008; Nakagawa et al. 2009), the STA-MCA bypass may temporarily lead to Fig. 3. Background of moyamoya disease and the peri-operative pathologies after STA-MCA anastomosis. The scheme also shows the potential risk factors responsible for the peri-operative pathologies, such as focal cerebral hyperperfusion and local vasogenic edema.
5 Current Management of Moyamoya Disease 49 Table 1. Surgical complications of the revascularization surgery for moyamoya disease. Complication Classification Procedure Management Neurological complications Ischemic complication (Cerebral infarction, TIA) Cerebral hyperperfusion syndrome Others Watershed shift phenomenon Thrombo-embolism from anastomosis Cortical compression by muscle pedicle Focal neurological deterioration Delayed intracranial hemorrhage Seizure Chronic subdural hematoma Vasogenic edema without hyperperfusion Indirect bypass Hydration, Antiplatelet, Edaravone Antiplatelet, Edaravone Revision of indirect bypass BP lowering, Minocycline BP lowering Anti-epileptic agent Drainage BP lowering, Minocycline, Edaravone Others Aesthetic complication etc. Systemic complication Skin necrosis Delayed wound healing CSF collection/leakage Cardiopulmonary complication Activation of autoimmune diseases (Thyrotoxicosis etc.) Skin graft patch, Dressing Dressing Spinal drainage Water balance correction etc. Anti-thyroid therapy etc. TIA, transient ischemic attack; BP, blood pressure; CSF, cerebrospinal fluid. heterogeneous hemodynamic condition even within the hemisphere operated on. Rapid focal increase in CBF at the site of the anastomosis could result in focal hyperemia associated with vasogenic edema and/or hemorrhagic conversion in moyamoya disease (Fujimura et al. 2011). Now it is well known that cerebral hyperperfusion syndrome is one of the most serious complications of revascularization surgery for moyamoya disease, especially in adult patients (Fujimura et al. 2009b; Uchino et al. 2012). It had been believed for a long time that cerebral hyperperfusion was extremely rare after low flow bypass such as STA-MCA anastomosis, and the cause of the focal neurological deterioration after revascularization surgery for moyamoya disease had been exclusively attributed to cerebral ischemia. To counteract with this stereotype, we routinely measured CBF by N-isopropyl-p-[ 123 I] iodoamphetamine single-photon emission computed tomography ( 123 I-IMP SPECT) in the acute stage of 257 consecutive surgical revascularization surgeries for moyamoya disease from 2004 operated by the single surgeon (M.F.), and found that that the incidence of symptomatic hyperperfusion, including mild focal neurological sign, was as high as 38.2% after STA-MCA anastomosis for adult-onset moyamoya disease in the initial series (Fujimura et al. 2007). Furthermore, the incidence of cerebral hyperperfusion syndrome after STA-MCA anastomosis was significantly higher in moyamoya disease patients than the patients with atherosclerotic occlusive cerebrovascular diseases (Fujimura et al. 2011). Focal cerebral hyperperfusion can cause temporary focal neurological deficit such as aphasia, hemiparesis, and dysarthria in a blood pressure dependent manner (Fujimura et al. 2007, 2009b, 2011). Although clinical manifestation is similar to that of transient ischemic attack, blood pressure dependent deterioration of the focal neurological sign convinced the diagnosis of symptomatic focal hyperperfusion. Because the symptoms due to hyperperfusion become evident between 2 to 6 days after surgery in most cases (Fujimura et al. 2011), we recommend routine CBF study within 48 hours after surgery (Fujimura et al. 2008). Prognosis of the focal neurological deficit is favorable in most cases, but focal hyperperfusion could also lead to delayed intracerebral hemorrhage and/or subarachnoid hemorrhage (Fujimura et al. 2009c, 2011). The incidence of delayed symptomatic hemorrhage due to hypeprerfusion is reported to be 3.3% (Fujimura et al. 2011), which could potentially result in permanent neurological deficit and/or mortality. Finally, the risk factors for hyperperfusion syndrome in moyamoya disease were reported as follows (Table 2); adult-onset (Fujimura et al. 2009b; Uchino et al. 2012), increased preoperative cerebral blood volume (Uchino et al. 2012), hemorrhagic-onset (Fujimura et al. 2009b), operation on the dominant (left) hemisphere (Hwang et al. 2013; Fujimura et al. 2014) and smaller diameter of the recipient artery (Fujimura et al. 2014). We also reported the predictive value of intraoperative brain surface monitoring by infrared thermography for postoperative hypeperfusion syndrome (Nakagawa et al. 2009). More recently, the predictive value of intraoperative indocyanine green video angiography findings for post-operative hyperperfusion was reported from different institutes (Horie et al. 2014; Uchino et al. 2014). Representative findings of cerebral hyperperfusion are shown in Fig. 4. Vasogenic edema without cerebral hyperperfusion Besides cerebral ischemia and hyperperfusion, we recently reported local vasogenic edema without cerebral hyperperfusion in two cases of adult-onset moyamoya disease undergoing STA-MCA bypass (Sakata et al. 2015). Both patients exhibited apparent vasogenic edema at the site of the anastomosis, which prolonged over one month after revascularization surgery. Repeated CBF analysis failed to detect any evidence of either hyperperfusion or
6 50 M. Fujimura and T. Tominaga Table 2. Risk factors for cerebral hyperperfusion syndrome (CHS) in moyamoya disease. Risk factors for CHS References Patients age Adult-onset Higher age Fujimura et al. 2009b Uchino et al Pre-operative hemodynamics Increased CBV Uchino et al Onset-type Hemorrhagic-onset Fujimura et al. 2009b Operation side Dominant hemisphere Left hemisphere Hwang et al Fujimura et al Vascular anatomy Smaller diameter of the recipient artery Fujimura et al Intraoperative findings Local temperature increase by infra-red thermography Restricted distribution by ICG video-angiography Nakagawa et al Horie et al. 2014, Uchino et al CHS, cerebral hyperperfusion syndrome; CBV, cerebral blood volume; CVR, cerebrovascular reactivity; ICG, indocyanine green. Fig. 4. Representative case of adult-onset moyamoya disease manifesting as focal cerebral hyperperfusion. N-isopropyl-p-[ 123 I] iodoamphetamine single-photon emission computed tomography before (A) and one day (B), and seven days (C) after right STA-MCA anastomosis demonstrating marked increase in CBF near the site of the anastomosis (arrow in B) compared to pre-operative status (A). Focal hyperperfusion was ameliorated 7 days after surgery (C). hypoperfusion. No neurological deterioration was found in these patients by intensive blood pressure control and minocycline administration, while increased vascular permeability as demonstrated by vasogenic edema formation might suggest the potential risk for hemorrhagic conversion (Sakata et al. 2015). Further evaluation is warranted to clarify the peri-operative pathologies after revascularization surgery for moyamoya disease to reduce the potential risk for surgical complications. Establishment of peri-operative management protocol Concept of the peri-operative care for moyamoya disease is to afford favorable IC-EC conversion without causing deleterious impact to the affected brain. The excessive blood pressure lowering may increase the risk for perioperative infarction at the remote area from STA-MCA bypass, but we found that prophylactic mild blood pressure lowering reduced the risk for hyperperfusion syndrome without increasing the incidence of ischemic complication, as long as adequate antiplatelet administration is attempted (Fujimura et al. 2012a). We have shown that prophylactic blood pressure control between 110 to 130 mmhg of the systolic blood pressure in the awake state significantly reduced the incidence of hyperperfusion syndrome after STA-MCA bypass in patients with moyamoya disease below that of the patients treated under normotensive conditions (Fujimura et al. 2012a). To further ameliorate the reperfusion injury to the affected brain, we additionally introduced minocycline hydrochloride, a neuro-protective antibiotic, to block the deleterious inflammatory cascade caused by the activation of matrix metalloproteinase-9 (MMP-9), which was implicated in moyamoya disease (Fujimura et al. 2009d; Kang et al. 2010), to prevent both hyperperfusion syndrome and cerebral infarction at the remote area. By the prophylactic blood pressure control combined with minocycline hydrochloride administration, the incidence of cerebral hyperperfusion syndrome as characterized by focal neurological deterioration was markedly reduced without increasing the ischemic complication (Fujimura et al. 2014). Our current protocol for peri-operative management of moyamoya disease is summarized in Fig. 5. The CBF analysis in the acute stage facilitated safer and more elegant perioperative management after direct/ indirect revascularization surgery for moyamoya disease, but the following limitation should be noted. Firstly, the hyperperfusion phenomenon shown by CBF analysis, either symptomatic or asymptomatic, could not be exclusively prevented even by current peri-operative management protocol. We observed delayed intracranial hemorrhage in 7 patients (6.9%) among 102 consecutive direct/indirect
7 Current Management of Moyamoya Disease 51 Fig. 5. Our peri-operative management strategy after STA-MCA anastomosis for moyamoya disease. The strategy attempts to avoid surgical complications including cerebral ischemia and hyperperfusion. Red arrow indicates the deleterious effect of blood pressure lowering to increase the potential risk for cerebral ischemia at remote area, including contralateral hemisphere and/or posterior circulation. revascularization surgeries even after the introduction of minocycline hydrochloride, although most of them remained asymptomatic (Fujimura et al. 2015). It is essential to develop perioperative management of moyamoya disease based on the pharmacological strategies, by targeting molecular pathway underlying the early perioperative pathology after revascularization surgery. Conclusion Concept of revascularization surgery for moyamoya disease includes both microsurgical reconstruction by direct extracranial-intracranial bypass and the consolidation for the future vasculogenesis by indirect pial synangiosis. The direct/indirect revascularization surgery is a safe and effective treatment for moyamoya disease, while peri-operative cerebral infarction and cerebral hyperperfusion syndrome are potential complications of this procedure. Routine CBF measurement in the early postoperative period under strict blood pressure control between 110 to 130 mmhg (systolic) combined with the use of neuro-protective antibiotics minocycline hydrochloride facilitated safer and more elegant peri-operative management for moyamoya disease. Conflict of Interest The authors declare no conflict of interest. References Fujimura, M., Inoue, T., Shimizu, H., Saito, A., Mugikura, S. & Tominaga, T. (2012a) Efficacy of prophylactic blood pressure lowering according to a standardized postoperative management protocol to prevent symptomatic cerebral hyperperfusion after direct revascularization surgery for moyamoya disease. Cerebrovasc. Dis., 33, Fujimura, M., Kaneta, T., Mugikura, S., Shimizu, H. & Tominaga, T. (2007) Temporary neurologic deterioration due to cerebral hyperperfusion after superficial temporal artery-middle cerebral artery anastomosis in patients with adult-onset moyamoya disease. Surg. Neurol., 67, Fujimura, M., Kaneta, T., Shimizu, H. & Tominaga, T. (2009a) Cerebral ischemia owing to compression of the brain by swollen temporal muscle used for encephalo-myo-synangiosis in moyamoya disease. Neurosurg. Rev., 32, Fujimura, M., Kaneta, T. & Tominaga, T. (2008) Efficacy of superficial temporal artery-middle cerebral artery anastomosis with routine postoperative cerebral blood flow measurement during the acute stage in childhood moyamoya disease. Childs Nerv. Syst., 24, Fujimura, M., Mugikura, S., Kaneta, T., Shimizu, H. & Tominaga, T. (2009b) Incidence and risk factors for symptomatic cerebral hyperperfusion after superficial temporal artery-middle cerebral artery anastomosis in patients with moyamoya disease. Surg. Neurol., 71, Fujimura, M., Niizuma, K., Endo, H., Sato, K., Inoue, T. & Tominaga, T. (2015) Blood pressure lowering and minocycline administration as secure and effective psooperative management after revascularization surgery for moyamoya disease. Surg. Cereb. Stroke, 43, (in Japanese).
8 52 M. Fujimura and T. Tominaga Fujimura, M., Niizuma, K., Inoue, T., Sato, K., Endo, H., Shimizu, H. & Tominaga, T. (2014) Minocycline prevents focal neurological deterioration due to cerebral hyperperfusion after extracranial-intracranial bypass for moyamoya disease. Neurosurgery, 74, Fujimura, M., Shimizu, H., Inoue, T., Mugikura, S., Saito, A. & Tominaga, T. (2011) Significance of focal cerebral hyperperfusion as a cause of transient neurologic deterioration after EC-IC bypass for moyamoya disease: comparative study with non-moyamoya patients using 123 I-IMP SPECT. Neurosurgery, 68, Fujimura, M., Shimizu, H., Mugikura, S. & Tominaga, T. (2009c) Delayed intracerebral hemorrhage after superficial temporal artery-middle cerebral artery anastomosis in a patient with moyamoya disease: possible involvement of cerebral hyperperfusion and increased vascular permeability. Surg. Neurol., 71, Fujimura, M. & Tominaga, T. (2012b) Lessons learned from moyamoya disease: outcome of direct/indirect revascularization surgery for 150 affected hemispheres. Neurol. Med. Chir. (Tokyo), 52, Fujimura, M., Watanabe, M., Narisawa, A., Shimizu, H. & Tominaga, T. (2009d) Increased expression of serum matrix metalloproteinase-9 in patients with moyamoya disease. Surg. Neurol., 72, Fukui, M. (1997) Guidelines for the diagnosis and treatment of spontaneous occlusion of the circle of Willis ( moyamoya disease). Research Committee on Spontaneous Occlusion of the Circle of Willis (Moyamoya Disease) of the Ministry of Health and Welfare, Japan. Clin. Neurol. Neurosurg., 99 Suppl 2, S Hayashi, K., Horie, N., Izumo, T. & Nagata, I. (2014) A nationwide survey on unilateral moyamoya disease in Japan. Clin. Neurol. Neurosurg., 124, 1-5. Hayashi, T., Shirane, R., Fujimura, M. & Tominaga, T. (2010) Postoperative neurological deterioration in pediatric moyamoya disease: watershed shift and hyperperfusion. J. Neurosurg. Pediatr., 6, Horie, N., Fukuda, Y., Izumo, T., Hayashi, K., Suyama, K. & Nagata, I. (2014) Indocyanine green videoangiography for assessment of postoperative hyperperfusion in moyamoya disease. Acta Neurochir. (Wien), 156, Houkin, K., Ishikawa, T., Yoshimoto, T. & Abe, H. (1997) Direct and indirect revascularization for moyamoya disease surgical techniques and peri-operative complications. Clin. Neurol. Neurosurg., 99 Suppl 2, S Hwang, J.W., Yang, H.M., Lee, H., Lee, H.K., Jeon, Y.T., Kim, J.E., Lim, Y.J. & Park, H.P. (2013) Predictive factors of symptomatic cerebral hyperperfusion after superficial temporal artery-middle cerebral artery anastomosis in adult patients with moyamoya disease. Br. J. Anaesth., 110, Ikeda, H., Sasaki, T., Yoshimoto, T., Fukui, M. & Arinami, T. (1999) Mapping of a familial moyamoya disease gene to chromosome 3p24.2-p26. Am. J. Hum. Genet., 64, Inoue, T.K., Ikezaki, K., Sasazuki, T., Matsushima, T. & Fukui, M. (2000) Linkage analysis of moyamoya disease on chromosome 6. J. Child Neurol., 15, Ito, A., Fujimura, M., Niizuma, K., Kanoke, A., Sakata, H., Morita- Fujimura, Y., Kikuchi, A., Kure, S. & Tominaga, T. (2015) Enhanced post-ischemic angiogenesis in mice lacking RNF213; a susceptibility gene for moyamoya disease. Brain Res., 1594, Kaku, Y., Morioka, M., Ohmori, Y., Kawano, T., Kai, Y., Fukuoka, H., Hirai, T., Yamashita, Y. & Kuratsu, J. (2012) Outer-diameter narrowing of the internal carotid and middle cerebral arteries in moyamoya disease detected on 3D constructive interference in steady-state MR image: is arterial constrictive remodeling a major pathogenesis? Acta Neurochir. (Wien), 154, Kamada, F., Aoki, Y., Narisawa, A., Abe, Y., Komatsuzaki, S., Kikuchi, A., Kanno, J., Niihori, T., Ono, M., Ishii, N., Owada, Y., Fujimura, M., Mashimo, Y., Suzuki, Y., Hata, A., Tsuchiya, S., Tominaga, T., Matsubara, Y. & Kure, S. (2011) A genomewide association study identifies RNF213 as the first Moyamoya disease gene. J. Hum. Genet., 56, Kang, H.S., Kim, J.H., Phi, J.H., Kim, Y.Y., Kim, J.E., Wang, K.C., Cho, B.K. & Kim, S.K. (2010) Plasma matrix metalloproteinases, cytokines and angiogenic factors in moyamoya disease. J. Neurol. Neurosurg. Psychiatry, 81, Kim, J.E., Oh, C.W., Kwon, O.K., Park, S.Q., Kim, S.E. & Kim, Y.K. (2008) Transient hyperperfusion after superficial temporal artery/middle cerebral artery bypass surgery as a possible cause of postoperative transient neurological deterioration. Cerebrovasc. Dis., 25, Kim, S.J., Heo, K.G., Shin, H.Y., Bang, O.Y., Kim, G.M., Chung, C.S., Kim, K.H., Jeon, P., Kim, J.S., Hong, S.C. & Lee, K.H. (2010) Association of thyroid autoantibodies with moyamoyatype cerebrovascular disease: a prospective study. Stroke, 41, Kuroda, S.; AMORE Study Group (2015) Asymptomatic moyamoya disease: literature review and ongoing AMORE study. Neurol. Med. Chir. (Tokyo), 55, Kuroda, S., Hashimoto, N., Yoshimoto, T. & Iwasaki, Y.; Research Committee on Moyamoya Disease in Japan (2007) Radiological findings, clinical course, and outcome in asymptomatic moyamoya disease: results of multicenter survey in Japan. Stroke, 38, Kuroda, S., Ishikawa, T., Houkin, K., Nanba, R., Hokari, M. & Iwasaki, Y. (2005) Incidence and clinical features of disease progression in adult moyamoya disease. Stroke, 36, Miyamoto, S., Yoshimoto, T., Hashimoto, N., Okada, Y., Tsuji, I., Tominaga, T., Nakagawara, J. & Takahashi, J.C.; JAM Trial Investigators (2014) Effects of extracranial-intracranial bypass for patients with hemorrhagic moyamoya disease: results of the Japan Adult Moyamoya Trial. Stroke, 45, Nakagawa, A., Fujimura, M., Arafune, T., Sakuma, I. & Tominaga, T. (2009) Clinical implications of intraoperative infrared brain surface monitoring during superficial temporal artery-middle cerebral artery anastomosis in patients with moyamoya disease. J. Neurosurg., 111, Ohue, S., Kumon, Y., Kohno, K., Watanabe, H., Iwata, S. & Ohnishi, T. (2008) Postoperative temporary neurological deficits in adults with moyamoya disease. Surg. Neurol., 69, Research Committee on the Pathology and Treatment of Spontaneous Occlusion of the Circle of Willis; Health Labour Sciences Research Grant for Research on Measures for Intractable Diseases (2012) Guidelines for diagnosis and treatment of moyamoya disease (spontaneous occlusion of the circle of willis). Neurol. Med. Chir. (Tokyo), 52, Sakata, H., Fujimura, M., Mugikura, S., Sato, K. & Tominaga, T. (2015) Local vasogenic edema without cerebral hyperperfusion after direct revascularization surgery for moyamoya disease. J. Stroke Cerebrovasc. Dis., [in press]. Sakurai, K., Horiuchi, Y., Ikeda, H., Ikezaki, K., Yoshimoto, T., Fukui, M. & Arinami, T. (2004) A novel susceptibility locus for moyamoya disease on chromosome 8q23. J. Hum. Genet., 49, Sonobe, S., Fujimura, M., Niizuma, K., Nishijima, Y., Ito, A., Shimizu, H., Kikuchi, A., Arai-Ichinoi, N., Kure, S. & Tominaga, T. (2014) Temporal profile of the vascular anatomy evaluated by 9.4-T magnetic resonance angiography and histopathological analysis in mice lacking RNF213: a susceptibility gene for moyamoya disease. Brain Res., 1552, Suzuki, J. & Takaku, A. (1969) Cerebrovascular moyamoya disease. Disease showing abnormal net-like vessels in base of
9 Current Management of Moyamoya Disease 53 brain. Arch. Neurol., 20, Uchino, H., Kazumata, K., Ito, M., Nakayama, N., Kuroda, S. & Houkin, K. (2014) Intraoperative assessment of cortical perfusion by indocyanine green videoangiography in surgical revascularization for moyamoya disease. Acta Neurochir. (Wien), 156, Uchino, H., Kuroda, S., Hirata, K., Shiga, T., Houkin, K. & Tamaki, N. (2012) Predictors and clinical features of postoperative hyperperfusion after surgical revascularization for moyamoya disease: a serial single photon emission CT/positron emission tomography study. Stroke, 43, Yamauchi, T., Tada, M., Houkin, K., Tanaka, T., Nakamura, Y., Kuroda, S., Abe, H., Inoue, T., Ikezaki, K., Matsushima, T. & Fukui, M. (2000) Linkage of familial moyamoya disease (spontaneous occlusion of the circle of Willis) to chromosome 17q25. Stroke, 31, Yuan, M., Liu, Z.Q., Wang, Z.Q., Li, B., Xu, L.J. & Xiao, X.L. (2015) High-resolution MR imaging of the arterial wall in moyamoya disease. Neurosci. Lett., 584,
Title in Children. Issue Date Copyright 2011 S. Karger AG, Base.
 NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Features and Long-Term Fol in Children. Hayashi, Kentaro; Horie, Nobutaka; Citation Pediatric Neurosurgery, 47(1), pp.1 Issue Date 2011-09 URL
NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Features and Long-Term Fol in Children. Hayashi, Kentaro; Horie, Nobutaka; Citation Pediatric Neurosurgery, 47(1), pp.1 Issue Date 2011-09 URL
Neurosurg Focus 5 (5):Article 4, 1998
 Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Case Report. Fumihiro MATANO 1, Yasuo MURAI 2, Asami KUBOTA 1, Takayuki MIZUNARI 1, Shiro KOBAYASHI 1, Akio MORITA 2
 DOI: 10.5137/1019-5149.JTN.19271-16.1 Received: 17.10.2016 / Accepted: 19.01.2017 Published Online: 07.02.2017 Case Report The Ivy Sign on Fluid Attenuated Inversion Recovery Images Related to Single-Photon
DOI: 10.5137/1019-5149.JTN.19271-16.1 Received: 17.10.2016 / Accepted: 19.01.2017 Published Online: 07.02.2017 Case Report The Ivy Sign on Fluid Attenuated Inversion Recovery Images Related to Single-Photon
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
Title. CitationWorld Neurosurgery, 80(5): Issue Date Doc URL. Rights. Rights(URL)
 Title Effective Surgical Revascularization Improves Cerebr Moyamoya Disease Kawabori, Masahito; Kuroda, Satoshi; Nakayama, Naoki Author(s) Nagara CitationWorld Neurosurgery, 80(5): 612-619 Issue Date 2013-11
Title Effective Surgical Revascularization Improves Cerebr Moyamoya Disease Kawabori, Masahito; Kuroda, Satoshi; Nakayama, Naoki Author(s) Nagara CitationWorld Neurosurgery, 80(5): 612-619 Issue Date 2013-11
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Occlusive cerebrovascular disease. A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats
 FPⅧ-1 A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats Ahmed Said Mansour 1, Kuniyasu Niizuma 2, Sherif Rashad 2, Hidenori Endo 2, Toshiki Endo 3, Kenichi
FPⅧ-1 A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats Ahmed Said Mansour 1, Kuniyasu Niizuma 2, Sherif Rashad 2, Hidenori Endo 2, Toshiki Endo 3, Kenichi
MOYA Moya disease is a rare idiopathic
 Research Papers Moya Moya Cases Treated with Encephaloduroarteriosynangiosis Parimal Tripathi, Varsha Tripathi, Ronak J. Naik and Jaimin M. Patel From Gujarat Cancer & Research Institute, Ahmedabad; Sterling
Research Papers Moya Moya Cases Treated with Encephaloduroarteriosynangiosis Parimal Tripathi, Varsha Tripathi, Ronak J. Naik and Jaimin M. Patel From Gujarat Cancer & Research Institute, Ahmedabad; Sterling
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study
 REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 194 198, 2015 doi: 10.2176/nmc.ra.2014-0305 Online February 20, 2015 Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study Satoshi Kuroda;
REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 194 198, 2015 doi: 10.2176/nmc.ra.2014-0305 Online February 20, 2015 Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study Satoshi Kuroda;
Moyamoya disease (MMD) is a rare steno-occlusive
 CLINICAL ARTICLE J Neurosurg 126:1573 1577, 2017 Low flow velocity in the middle cerebral artery predicting infarction after bypass surgery in adult moyamoya disease *Hoyeon Cho, MD, 1 Kyung Il Jo, MD,
CLINICAL ARTICLE J Neurosurg 126:1573 1577, 2017 Low flow velocity in the middle cerebral artery predicting infarction after bypass surgery in adult moyamoya disease *Hoyeon Cho, MD, 1 Kyung Il Jo, MD,
Moyamoya disease is an unusual form of chronic, occlusive
 Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Clinicoepidemiological Features of Asymptomatic Moyamoya Disease in Adult Patients
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2014.16.3.241 Original Article Clinicoepidemiological Features of Asymptomatic
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2014.16.3.241 Original Article Clinicoepidemiological Features of Asymptomatic
010050,Inner Mongolia, China
 Possible factors influencing postoperative temporary neurologic deterioration following standard superficial temporal artery-middle cerebral artery (STA-MCA) bypass surgery: diameter of STA and MCA (M4)
Possible factors influencing postoperative temporary neurologic deterioration following standard superficial temporal artery-middle cerebral artery (STA-MCA) bypass surgery: diameter of STA and MCA (M4)
Moyamoya disease presenting as acute onset cortical blindness: a case report
 Romanian Neurosurgery Volume XXX Number 1 2016 January-March Article Moyamoya disease presenting as acute onset cortical blindness: a case report Dudi Maniram, Bansal Rajeev, Srivastava Trilochan, Sardana
Romanian Neurosurgery Volume XXX Number 1 2016 January-March Article Moyamoya disease presenting as acute onset cortical blindness: a case report Dudi Maniram, Bansal Rajeev, Srivastava Trilochan, Sardana
Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain
 Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain Christopher Payne Currently, no medical treatment exists to prevent the progression of moyamoya disease, and neurosurgical treatment
Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain Christopher Payne Currently, no medical treatment exists to prevent the progression of moyamoya disease, and neurosurgical treatment
Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications
 clinical article J Neurosurg 122:400 407, 2015 Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications Takeshi Funaki, MD, 1 Jun C. Takahashi, MD, PhD, 1 Yasushi
clinical article J Neurosurg 122:400 407, 2015 Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications Takeshi Funaki, MD, 1 Jun C. Takahashi, MD, PhD, 1 Yasushi
A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty
 DOI: 10.5797/jnet.cr.2017-0043 A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty Jun Niimi, Kenta Tasaka, Fumio Nemoto, Takuya
DOI: 10.5797/jnet.cr.2017-0043 A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty Jun Niimi, Kenta Tasaka, Fumio Nemoto, Takuya
Thirteen-year Experience of 44 Patients with Adult Hemorrhagic Moyamoya Disease from a Single Institution: Clinical Analysis by Management Modality
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.191 Clinical Article Thirteen-year Experience of 44 Patients with Adult
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.191 Clinical Article Thirteen-year Experience of 44 Patients with Adult
Moyamoya disease in the midwestern United States
 Neurosurg Focus 5 (5):Article 1, 1998 Moyamoya disease in the midwestern United States Nicholas M. Wetjen, B.S., P. Charles Garell, M.D., Nicholas V. Stence, and Christopher M. Loftus, M.D. Division of
Neurosurg Focus 5 (5):Article 1, 1998 Moyamoya disease in the midwestern United States Nicholas M. Wetjen, B.S., P. Charles Garell, M.D., Nicholas V. Stence, and Christopher M. Loftus, M.D. Division of
Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease
 272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
Although moyamoya disease, a rare cerebrovascular occlusive
 Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Moyamoya disease (MMD) is a progressive stenoocclusive
 J Neurosurg 121:432 440, 2014 AANS, 2014 The frequency of postoperative stroke in moyamoya disease following combined revascularization: a single-university series and systematic review Clinical article
J Neurosurg 121:432 440, 2014 AANS, 2014 The frequency of postoperative stroke in moyamoya disease following combined revascularization: a single-university series and systematic review Clinical article
Overview Blood supply of the brain What is moyamoya disease? > 1
 Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Title. Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉. Citation 脳卒中の外科, 37(5): Issue Date Doc URL.
 Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
Moyamoya disease. Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease.
 FPⅢ- Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease Tomohide Hayashi Departments of Neurosurgery, University of Toyama Background - is a unique cerebrovascular
FPⅢ- Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease Tomohide Hayashi Departments of Neurosurgery, University of Toyama Background - is a unique cerebrovascular
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
Moyamoya Disease in China Its Clinical Features and Outcomes
 Moyamoya Disease in China Its Clinical Features and Outcomes Lian Duan, MD, PhD; Xiang-Yang Bao, MM; Wei-Zhong Yang, BS; Wan-Chao Shi, MD; De-Sheng Li, MD; Zheng-Shan Zhang, MM; Rui Zong, MM; Cong Han,
Moyamoya Disease in China Its Clinical Features and Outcomes Lian Duan, MD, PhD; Xiang-Yang Bao, MM; Wei-Zhong Yang, BS; Wan-Chao Shi, MD; De-Sheng Li, MD; Zheng-Shan Zhang, MM; Rui Zong, MM; Cong Han,
Clinical implications of the cortical hyperintensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease
 clinical article J Neurosurg 126:1 7, 2017 Clinical implications of the cortical hyperintensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease Eika Hamano,
clinical article J Neurosurg 126:1 7, 2017 Clinical implications of the cortical hyperintensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease Eika Hamano,
This quiz is being published on behalf of the Education Committee of the SNACC.
 Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Moyamoya disease (MMD), an idiopathic disease. Direct versus indirect revascularization in the treatment of moyamoya disease
 CLINICAL ARTICLE J Neurosurg 129:480 489, 2018 Direct versus indirect revascularization in the treatment of moyamoya disease *Seong-eun Park, BSc, Ju-seong Kim, MD, Eun Kyung Park, MD, Kyu-Won Shim, MD,
CLINICAL ARTICLE J Neurosurg 129:480 489, 2018 Direct versus indirect revascularization in the treatment of moyamoya disease *Seong-eun Park, BSc, Ju-seong Kim, MD, Eun Kyung Park, MD, Kyu-Won Shim, MD,
Angiographic features of hemorrhagic moyamoya disease with high recurrence risk: a supplementary analysis of the Japan Adult Moyamoya Trial
 CLINICAL ARTICLE J Neurosurg 128:777 784, 2018 Angiographic features of hemorrhagic moyamoya disease with high recurrence risk: a supplementary analysis of the Japan Adult Moyamoya Trial Takeshi Funaki,
CLINICAL ARTICLE J Neurosurg 128:777 784, 2018 Angiographic features of hemorrhagic moyamoya disease with high recurrence risk: a supplementary analysis of the Japan Adult Moyamoya Trial Takeshi Funaki,
Moyamoya disease (MMD) is a chronic, progressive cerebrovascular. Clinical and Angiographic Features and Stroke Types in Adult Moyamoya Disease
 ORIGINAL RESEARCH BRAIN Clinical and Angiographic Features and Stroke Types in Adult Moyamoya Disease D.-K. Jang, K.-S. Lee, H.K. Rha, P.-W. Huh, J.-H. Yang, I.S. Park, J.-G. Ahn, J.H. Sung, and Y.-M.
ORIGINAL RESEARCH BRAIN Clinical and Angiographic Features and Stroke Types in Adult Moyamoya Disease D.-K. Jang, K.-S. Lee, H.K. Rha, P.-W. Huh, J.-H. Yang, I.S. Park, J.-G. Ahn, J.H. Sung, and Y.-M.
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease
 Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Moyamoya. Moyamoya Disease Double Trouble. Epidemiology 1/16/2015
 Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Moyamoya disease (MMD) is a chronic, progressive. Topical Reviews Section Editors: Guiseppe Lanzino, MD, and Michael Tymianski, MD, PhD
 Topical Reviews Section Editors: Guiseppe Lanzino, MD, and Michael Tymianski, MD, PhD Neurosurgical Advances in the Treatment of Moyamoya Disease Paritosh Pandey, MD; Gary K. Steinberg, MD, PhD Background
Topical Reviews Section Editors: Guiseppe Lanzino, MD, and Michael Tymianski, MD, PhD Neurosurgical Advances in the Treatment of Moyamoya Disease Paritosh Pandey, MD; Gary K. Steinberg, MD, PhD Background
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
positron emission tomography PET
 020-8505 19-1 1-3) positron emission tomography PET PET PET single photon emission computed tomography SPECT acetazolamide 4-10) magnetic resonance imaging MRI MRI 11,12) MRI perfusion weighted imaging
020-8505 19-1 1-3) positron emission tomography PET PET PET single photon emission computed tomography SPECT acetazolamide 4-10) magnetic resonance imaging MRI MRI 11,12) MRI perfusion weighted imaging
The Importance of Middle Cerebral Artery Stenosis In Patients With A Lacunar Infarction In The Carotid Artery Territory
 The Importance of Middle Cerebral Artery Stenosis In Patients With A Lacunar Infarction In The Carotid Artery Territory Oh Young Bang, M.D., Jeong Hoon Cho, M.D., Ji Hoe Heo, M.D., Dong Ik Kim, M.D.* Department
The Importance of Middle Cerebral Artery Stenosis In Patients With A Lacunar Infarction In The Carotid Artery Territory Oh Young Bang, M.D., Jeong Hoon Cho, M.D., Ji Hoe Heo, M.D., Dong Ik Kim, M.D.* Department
Intraoperative EC-IC Bypass Blood Flow Assessment With Indocyanine Green Angiography in Moyamoya and Non-Moyamoya Ischemic Stroke
 Intraoperative EC-IC Bypass Blood Flow Assessment With Indocyanine Green Angiography in Moyamoya and Non-Moyamoya Ischemic Stroke Takayuki Awano 1, Kaoru Sakatani 1,2, Noriaki Yokose 1, Yuko Kondo 1, Takahiro
Intraoperative EC-IC Bypass Blood Flow Assessment With Indocyanine Green Angiography in Moyamoya and Non-Moyamoya Ischemic Stroke Takayuki Awano 1, Kaoru Sakatani 1,2, Noriaki Yokose 1, Yuko Kondo 1, Takahiro
Moyamoya disease is a progressive cerebrovascular. Pial synangiosis in patients with moyamoya younger than 2 years of age.
 J Neurosurg Pediatrics 13:420 425, 2014 AANS, 2014 Pial synangiosis in patients with moyamoya younger than 2 years of age Clinical article Eric M. Jackson, M.D., Ning Lin, M.D., Sunil Manjila, M.D., R.
J Neurosurg Pediatrics 13:420 425, 2014 AANS, 2014 Pial synangiosis in patients with moyamoya younger than 2 years of age Clinical article Eric M. Jackson, M.D., Ning Lin, M.D., Sunil Manjila, M.D., R.
MMD is a rare cerebrovascular disease first described by
 ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
Imaging of Moya Moya Disease
 Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Moyamoya disease (MMD) is a chronic, progressive. Topical Reviews Section Editors: Guiseppe Lanzino, MD, and Michael Tymianski, MD, PhD
 Topical Reviews Section Editors: Guiseppe Lanzino, MD, and Michael Tymianski, MD, PhD Neurosurgical Advances in the Treatment of Moyamoya Disease Paritosh Pandey, MD; Gary K. Steinberg, MD, PhD Downloaded
Topical Reviews Section Editors: Guiseppe Lanzino, MD, and Michael Tymianski, MD, PhD Neurosurgical Advances in the Treatment of Moyamoya Disease Paritosh Pandey, MD; Gary K. Steinberg, MD, PhD Downloaded
Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis
 Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis Craig D. McClain, MD, MPH Boston Children s Hospital and Harvard Medical School Case Presentation 14 year old male with bilateral
Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis Craig D. McClain, MD, MPH Boston Children s Hospital and Harvard Medical School Case Presentation 14 year old male with bilateral
 Impact of posterior cerebral artery Titleclinical and social outcome of pedi Dissertation_ 全文 ) Author(s) Funaki, Takeshi Citation Kyoto University ( 京都大学 ) Issue Date 2015-01-23 URL http://dx.doi.org/10.14989/doctor.r
Impact of posterior cerebral artery Titleclinical and social outcome of pedi Dissertation_ 全文 ) Author(s) Funaki, Takeshi Citation Kyoto University ( 京都大学 ) Issue Date 2015-01-23 URL http://dx.doi.org/10.14989/doctor.r
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for
 Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Moyamoya disease (MMD) is a rare idiopathic disorder
 Moyamoya: An Update for the Practicing Neurologist Distinguishing between definite MMD, probable MMD, and MMS may not have significant practical implications. By Timothy G. White, MD; Julia R. Schneider,
Moyamoya: An Update for the Practicing Neurologist Distinguishing between definite MMD, probable MMD, and MMS may not have significant practical implications. By Timothy G. White, MD; Julia R. Schneider,
Association of HLA-DR and -DQ Genes with Familial Moyamoya Disease in Koreans
 www.jkns.or.kr 10.3340/jkns.2009.46.6.558 J Korean Neurosurg Soc 46 : 558-563, 2009 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2009 The Korean Neurosurgical Society Laboratory Investigation
www.jkns.or.kr 10.3340/jkns.2009.46.6.558 J Korean Neurosurg Soc 46 : 558-563, 2009 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2009 The Korean Neurosurgical Society Laboratory Investigation
Neuroscience. Journal. Moyamoya disease a review and case illustration. P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016
 Neuroscience P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016 Journal Moyamoya disease a review and case illustration pg. 5 Choroid Plexus Papilloma in adults pg. 8 As physician co-leaders of Palmetto
Neuroscience P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016 Journal Moyamoya disease a review and case illustration pg. 5 Choroid Plexus Papilloma in adults pg. 8 As physician co-leaders of Palmetto
Young So, MD; Ho-Young Lee, MD; Seung-Ki Kim, MD; Jae Sung Lee, PhD; Kyu-Chang Wang, MD; Byung-Kyu Cho, MD; Eunjoo Kang, PhD; Dong Soo Lee, MD
 Prediction of the Clinical Outcome of Pediatric Moyamoya Disease With Postoperative Basal/Acetazolamide Stress Brain Perfusion SPECT After Revascularization Surgery Young So, MD; Ho-Young Lee, MD; Seung-Ki
Prediction of the Clinical Outcome of Pediatric Moyamoya Disease With Postoperative Basal/Acetazolamide Stress Brain Perfusion SPECT After Revascularization Surgery Young So, MD; Ho-Young Lee, MD; Seung-Ki
Moyamoya syndrome associated with cocaine abuse Case report
 Neurosurg Focus 5 (5):Article 7, 1998 Moyamoya syndrome associated with cocaine abuse Case report Marc S. Schwartz, M.D., and R. Michael Scott, M.D. Division of Neurosurgery, Albany Medical College, Albany,
Neurosurg Focus 5 (5):Article 7, 1998 Moyamoya syndrome associated with cocaine abuse Case report Marc S. Schwartz, M.D., and R. Michael Scott, M.D. Division of Neurosurgery, Albany Medical College, Albany,
Since the introduction of extracranial-intracranial (ECIC)
 ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
Case Report INTRODUCTION
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Department of Neurosurgery, Hallym University College of Medicine, Chuncheon, Korea; 2
 Original Article doi: 10.2176/nmc.oa.2017-0198 Neurol Med Chir (Tokyo) 58, 116 123, 2018 Association of Hyperthyroidism and Thyroid Autoantibodies with Moyamoya Disease and Its Stroke Event: A Population-based
Original Article doi: 10.2176/nmc.oa.2017-0198 Neurol Med Chir (Tokyo) 58, 116 123, 2018 Association of Hyperthyroidism and Thyroid Autoantibodies with Moyamoya Disease and Its Stroke Event: A Population-based
Original Article Ischemic and hemorrhagic moyamoya disease in adults: CT findings
 Int J Clin Exp Med 2015;8(11):21351-21357 www.ijcem.com /ISSN:1940-5901/IJCEM0009621 Original Article Ischemic and hemorrhagic moyamoya disease in adults: CT findings Anming Xie 1*, Li Luo 2*, Yaojun Ding
Int J Clin Exp Med 2015;8(11):21351-21357 www.ijcem.com /ISSN:1940-5901/IJCEM0009621 Original Article Ischemic and hemorrhagic moyamoya disease in adults: CT findings Anming Xie 1*, Li Luo 2*, Yaojun Ding
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Improvement of Cerebral Arterial Stenosis Associated With Basedow's Disease
 Neurol Med Chir (Tokyo) 45, 578 582, 2005 Improvement of Cerebral Arterial Stenosis Associated With Basedow's Disease Case Report Shiro YAMASHITA, Takashi TAMIYA, AtsushiSHINDO, KeisukeMIYAKE, Takehiro
Neurol Med Chir (Tokyo) 45, 578 582, 2005 Improvement of Cerebral Arterial Stenosis Associated With Basedow's Disease Case Report Shiro YAMASHITA, Takashi TAMIYA, AtsushiSHINDO, KeisukeMIYAKE, Takehiro
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion
 Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Spontaneous cervicocephalic arterial dissection with headache and neck pain as the only symptom
 J Headache Pain (2012) 13:247 253 DOI 10.1007/s10194-012-0420-2 BRIEF REPORT Spontaneous cervicocephalic arterial dissection with headache and neck pain as the only symptom Hajime Maruyama Harumitsu Nagoya
J Headache Pain (2012) 13:247 253 DOI 10.1007/s10194-012-0420-2 BRIEF REPORT Spontaneous cervicocephalic arterial dissection with headache and neck pain as the only symptom Hajime Maruyama Harumitsu Nagoya
Epidemiology, diagnosis and treatment of moyamoya disease (Review)
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 17: 1977-1984, 2019 Epidemiology, diagnosis and treatment of moyamoya disease (Review) HUI ZHANG, LIJIAN ZHENG and LEI FENG Department of Neurosurgery, The First People's
EXPERIMENTAL AND THERAPEUTIC MEDICINE 17: 1977-1984, 2019 Epidemiology, diagnosis and treatment of moyamoya disease (Review) HUI ZHANG, LIJIAN ZHENG and LEI FENG Department of Neurosurgery, The First People's
Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging
 AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D.
 J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents
 Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Moyamoya disease is an idiopathic cerebrovascular disorder
 ORIGINAL RESEARCH N. Mori S. Mugikura S. Higano T. Kaneta M. Fujimura A. Umetsu T. Murata S. Takahashi The Leptomeningeal Ivy Sign on Fluid- Attenuated Inversion Recovery MR Imaging in Moyamoya Disease:
ORIGINAL RESEARCH N. Mori S. Mugikura S. Higano T. Kaneta M. Fujimura A. Umetsu T. Murata S. Takahashi The Leptomeningeal Ivy Sign on Fluid- Attenuated Inversion Recovery MR Imaging in Moyamoya Disease:
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
Chapter 43 Monitoring of Filter Patency During Carotid Artery Stenting Using Near-Infrared Spectroscopy with High Time-Resolution
 Chapter 43 Monitoring of Filter Patency During Carotid Artery Stenting Using Near-Infrared Spectroscopy with High Time-Resolution Takahiro Igarashi, Kaoru Sakatani, Tadashi Shibuya, Teruyasu Hirayama,
Chapter 43 Monitoring of Filter Patency During Carotid Artery Stenting Using Near-Infrared Spectroscopy with High Time-Resolution Takahiro Igarashi, Kaoru Sakatani, Tadashi Shibuya, Teruyasu Hirayama,
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Effect of Surgery on the Long-Term Functional Outcome of Moyamoya Disease: A Meta-Analysis
 DOI: 10.5137/1019-5149.JTN.22598-18.3 Received: 14.01.2018 / Accepted: 06.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Effect of Surgery on the Long-Term Functional
DOI: 10.5137/1019-5149.JTN.22598-18.3 Received: 14.01.2018 / Accepted: 06.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Effect of Surgery on the Long-Term Functional
CT perfusion in Moyamoya disease
 CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
Intracranial vascular anastomosis using the microanastomotic system
 J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms
 J Neurosurg 57:622-628, 1982 Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms MAMORU TANEDA, M.D. Department of Neurosurgery, Hanwa Memorial Hospital, Osaka,
J Neurosurg 57:622-628, 1982 Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms MAMORU TANEDA, M.D. Department of Neurosurgery, Hanwa Memorial Hospital, Osaka,
Moyamoya Disease: Comparison of Assessment with 3.0T MR Angiography and MR Imaging versus Conventional
 Moyamoya Disease: Comparison of Assessment with 3.0T MR Angiography and MR Imaging versus Conventional Angiography Poster No.: C-2771 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: Q.
Moyamoya Disease: Comparison of Assessment with 3.0T MR Angiography and MR Imaging versus Conventional Angiography Poster No.: C-2771 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: Q.
TABLES. Table 1 Terminal vessel aneurysms. Table. Aneurysm location. Bypass flow** Symptoms Strategy Bypass recipient. Age/ Sex.
 Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Moyamoya Disease: Epidemiology, Clinical Features, and Diagnosis
 Journal of Stroke 2016;18(1):2-11 http://dx.doi.org/10.5853/jos.2015.01627 Special Review Moyamoya Disease: Epidemiology, Clinical Features, and Diagnosis Jong S. Kim Stroke Center and Department of Neurology,
Journal of Stroke 2016;18(1):2-11 http://dx.doi.org/10.5853/jos.2015.01627 Special Review Moyamoya Disease: Epidemiology, Clinical Features, and Diagnosis Jong S. Kim Stroke Center and Department of Neurology,
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: , 2018
 3570 Clinical and angiographic outcomes after combined direct and indirect bypass in adult patients with moyamoya disease: A retrospective study of 76 procedures JINBING ZHAO, HONGYI LIU, YUANJIE ZOU,
3570 Clinical and angiographic outcomes after combined direct and indirect bypass in adult patients with moyamoya disease: A retrospective study of 76 procedures JINBING ZHAO, HONGYI LIU, YUANJIE ZOU,
Chronic middle cerebral artery (MCA) occlusion as a cause
 ORIGINAL RESEARCH M. Tanaka E. Shimosegawa K. Kajimoto Y. Kimura H. Kato N. Oku M. Hori K. Kitagawa J. Hatazawa Chronic Middle Cerebral Artery Occlusion: A Hemodynamic and Metabolic Study with Positron-Emission
ORIGINAL RESEARCH M. Tanaka E. Shimosegawa K. Kajimoto Y. Kimura H. Kato N. Oku M. Hori K. Kitagawa J. Hatazawa Chronic Middle Cerebral Artery Occlusion: A Hemodynamic and Metabolic Study with Positron-Emission
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal
 Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal anterior cerebral artery aneurysm Acta Neurochirurgica Kampei Shimizu, Shoichi Tani, Hirotoshi Imamura,
Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal anterior cerebral artery aneurysm Acta Neurochirurgica Kampei Shimizu, Shoichi Tani, Hirotoshi Imamura,
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
 Case Reports in Vascular Medicine Volume 2013, Article ID 207602, 4 pages http://dx.doi.org/10.1155/2013/207602 Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
Case Reports in Vascular Medicine Volume 2013, Article ID 207602, 4 pages http://dx.doi.org/10.1155/2013/207602 Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
Cerebral hyperperfusion syndrome after carotid angioplasty
 case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
Bilateral Carotid and Vertebral Rete Mirabile Presenting with Subarachnoid Hemorrhage Caused by the Rupture of Spinal Artery Aneurysm
 Tohoku J. Exp. Med., 2013, 230, 205-209 Carotid and Vertebral Rete Mirabile Presenting with SAH 205 Bilateral Carotid and Vertebral Rete Mirabile Presenting with Subarachnoid Hemorrhage Caused by the Rupture
Tohoku J. Exp. Med., 2013, 230, 205-209 Carotid and Vertebral Rete Mirabile Presenting with SAH 205 Bilateral Carotid and Vertebral Rete Mirabile Presenting with Subarachnoid Hemorrhage Caused by the Rupture
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Neuro Quiz 29 Transcranial Doppler Monitoring
 Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D Neuro Quiz 29 Transcranial Doppler Monitoring This
Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D Neuro Quiz 29 Transcranial Doppler Monitoring This
Clinicoradiological Profile of Childhood Moyamoya Disease: Indian Study of 30 Children with Literature Review
 Original article Clinicoradiological Profile 10.5005/jp-journals-10066-0020 of Childhood Moyamoya Disease Clinicoradiological Profile of Childhood Moyamoya Disease: Indian Study of 30 Children with Literature
Original article Clinicoradiological Profile 10.5005/jp-journals-10066-0020 of Childhood Moyamoya Disease Clinicoradiological Profile of Childhood Moyamoya Disease: Indian Study of 30 Children with Literature
Hemodynamics in the Anterior Part of the Circle of Willis in Patients with Intracranial Aneurysms : A Study by Cerebral Angiography
 Tohoku J. exp. Med., 1980, 132, 69-73 Hemodynamics in the Anterior Part of the Circle of Willis in Patients with Intracranial Aneurysms : A Study by Cerebral Angiography RYUNGCHAN KWAK, HIROSHI NIIZUMA
Tohoku J. exp. Med., 1980, 132, 69-73 Hemodynamics in the Anterior Part of the Circle of Willis in Patients with Intracranial Aneurysms : A Study by Cerebral Angiography RYUNGCHAN KWAK, HIROSHI NIIZUMA
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY
 Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Recent Advances in Neurology Difficult Cases
 Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
 Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
