Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications
|
|
|
- Abigayle Hensley
- 6 years ago
- Views:
Transcription
1 clinical article J Neurosurg 122: , 2015 Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications Takeshi Funaki, MD, 1 Jun C. Takahashi, MD, PhD, 1 Yasushi Takagi, MD, PhD, 1 Takayuki Kikuchi, MD, PhD, 1 Kazumichi Yoshida, MD, PhD, 1 Takafumi Mitsuhara, MD, PhD, 1 Hiroharu Kataoka, MD, PhD, 2 Tomohisa Okada, MD, PhD, 3 Yasutaka Fushimi, MD, PhD, 3 and Susumu Miyamoto, MD, PhD 1 Departments of 1 Neurosurgery and 3 Diagnostic Imaging and Nuclear Medicine, Kyoto University Graduate School of Medicine, Kyoto; and 2 Department of Neurosurgery, National Cerebral and Cardiovascular Center, Osaka, Japan Object Unstable moyamoya disease, reasonably defined as cases exhibiting either rapid disease progression or repeated ischemic stroke, represents a challenge in the treatment of moyamoya disease. Despite its overall efficacy, direct bypass for such unstable disease remains controversial in terms of safety. This study aims to reveal factors associated with unstable disease and to assess its impact on postoperative silent or symptomatic ischemic lesions. Methods This retrospective cohort study included both pediatric and adult patients with moyamoya disease who had undergone 140 consecutive direct bypass procedures at Kyoto University Hospital. Unstable moyamoya disease was defined as either the rapid progression of a steno-occlusive lesion or repeat ischemic stroke, either occurring within 6 months of surgery. The extent of progression was determined through a comparison of the findings between 2 different MR angiography sessions performed before surgery. The clinical variables of the stable and unstable disease groups were compared, and the association between unstable disease and postoperative diffusion-weighted imaging (DWI) detected lesion was assessed through univariate and multivariate analyses with generalized estimating equations. Results Of 134 direct bypass procedures performed after patients had undergone at least 2 sessions of MR angiography, 24 (17.9%) were classified as cases of unstable disease. Age younger than 3 years (p = 0.029), underlying disease causing moyamoya syndrome (p = 0.049), and radiographic evidence of infarction (p = 0.030) were identified as factors associated with unstable disease. Postoperative DWI-defined lesions were detected after 13 of 140 procedures (9.3%), although only 4 lesions (2.9%) could be classified as a permanent complication. The incidence of postoperative DWI-detected lesions in the unstable group was notable at 33.3% (8 of 24). Univariate analysis revealed that unstable disease (p < 0.001), underlying disease (p = 0.028), and recent stroke (p = 0.012) were factors associated with DWI-detected lesions. Unstable disease remained statistically significant after adjustment for covariates in both the primary and sensitivity analyses (primary analysis: OR 6.62 [95% CI ]; sensitivity analysis: OR 5.36 [95% CI ]). Conclusions Unstable moyamoya disease, more prevalent in younger patients and those with underlying disease, is a possible risk factor for perioperative ischemic complications. Recognition of unstable moyamoya disease may contribute to an improved surgical result through focused perioperative management based on appropriate surgical risk stratification. Key Words moyamoya disease; rapid progression; cerebral revascularization; intraoperative complication; vascular disorders A major characteristic of moyamoya disease is the chronic progression of stenosis in the terminal portion of the internal carotid artery (ICA). 24 The rate of this progression varies by patient. Angiographic progression can occur in one-half of pediatric patients and one-quarter of adult patients, 19,21 while angiographic findings in the remaining patients are stable for years. Some patients demonstrate extremely rapid progression from disease onset, resulting in poor outcome. 4,17,18 Fujiwara et al. and Kim et al. reported similar cases in which rapid an- Abbreviations ACA = anterior cerebral artery; DWI = diffusion-weighted imaging; GEE = generalized estimating equation; ICA = internal carotid artery; MCA = middle cerebral artery; MRA = MR angiography; mrs = modified Rankin Scale; PCA = posterior cerebral artery; STA = superficial temporal artery; TIA = transient ischemic attack. submitted January 31, accepted October 21, include when citing Published online November 28, 2014; DOI: / JNS Disclosure The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. 400 AANS, 2015
2 Unstable moyamoya disease giographic progression resulted in fatal outcome. 4,18 Kim et al. reported that younger patients were more likely to suffer from an aggressive clinical course, of whom a substantial number experienced repeat stroke. 17 While the impact of such unstable disease on clinical outcome is receiving more focused attention, few studies have attempted to clearly define this condition. Accurate risk stratification in moyamoya disease requires objective definition of disease instability. According to the articles mentioned above, 4,17,18 disease progression and repeat stroke are considered essential factors reflecting instability of moyamoya disease. The concept of unstable moyamoya disease defined as either rapid disease progression or repeat stroke seems reasonable, considering that unstable angina pectoris, the concept representing instability of angina pectoris, is also characterized as an exacerbating or recurrent symptom with rapid progression of stenosis in the coronary artery. 1,23,27 Treatment of unstable moyamoya disease is challenging because patients with the disease commonly develop stroke during the perioperative period or even while awaiting surgery. 7,17 Direct bypass, such as superficial temporal artery to middle cerebral artery (STA-MCA) bypass, has the advantage of contributing to increased cerebral blood flow soon after surgery. 10 The safety and efficacy of direct bypass for unstable disease are, however, controversial. 7,17 This retrospective cohort study had 2 objectives: to detect clinical factors associated with unstable moyamoya disease and to determine whether the presence of such instability is associated with postoperative silent or symptomatic ischemic lesions detected on diffusion-weighted imaging (DWI). Methods This study was approved by the ethics committee of the Kyoto University Graduate School of Medicine. Selection Criteria A total of 88 pediatric and adult patients with moyamoya disease underwent 148 revascularization surgeries at Kyoto University Hospital between 2009 and The inclusion criteria for the present study were as follows: diagnosis of moyamoya disease or moyamoya syndrome; patients who underwent direct revascularization at Kyoto University Hospital in 2009 or thereafter; and patients who underwent routine postoperative DWI no longer than 14 days after surgery. Diagnoses were made according to the criteria proposed by the Research Committee on Moyamoya Disease in Japan. 24 Moyamoya syndrome is defined as a secondary moyamoya phenomenon caused by an underlying disease such as an autoimmune disease, meningitis, brain tumor, hyperthyroidism, Down syndrome, neurofibromatosis Type 1, or a history of head irradiation. 24 The present study also included unilateral disease in which only 1 side of the ICA was involved. Direct bypass was defined as a direct anastomotic procedure including STA-MCA, STA anterior cerebral artery (ACA), and occipital artery posterior cerebral artery (PCA) bypasses. Of the 148 consecutive revascularization procedures, 3 were excluded because they involved only indirect bypass in the ACA territory. Although postoperative MRI with DWI was mandatory in our treatment protocol, postoperative DWI was not performed after 5 procedures (these cases were excluded from the study) because a postoperative MRI scan was performed but no DWI was acquired (4 procedures), and because no MRI was performed since the patient sought early discharge (1 procedure). None of these 5 patients presented with a new neurological deficit after surgery. Consequently, 140 procedures conducted in 86 patients were included in the present study (Fig. 1). Variables Unstable moyamoya disease, a primary variable of interest, was defined as a condition with evidence of either rapid stenosis progression or repeated stroke. Rapid stenosis progression was defined as progression of a steno-occlusive lesion in an ICA, ACA, MCA, or PCA that had occurred within 6 months (Fig. 2). Whether the progression had occurred was determined using an MR angiography (MRA) scoring system, 8 and the scores were compared between 2 different sessions performed before surgery. Almost all patients referred to our institution had already undergone MRA, the results of which could be used as control imaging. If only 1 imaging session had been performed before surgery, or if the interval between the 2 sessions was less than 2 weeks, the data were eliminated from further analysis. Decreased antegrade flow due to bypass in the ipsilateral MCA territory was not regarded as stenosis progression. Repeat stroke was defined as newly developed symptomatic infarctions confirmed on DWI and occurring at least twice during an interval not exceeding 6 months. The other variables possibly affecting surgical outcome were identified from previous literature: age younger than 3 years, 16 female sex, 15 presence of underlying disease causing moyamoya syndrome, 6,22 transient ischemic attacks (TIAs) occurring at a frequency exceeding 3 times per month, 16 radiographic evidence of preexisting infarc- Fig. 1. Flowchart for patient inclusion. 401
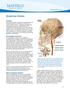
3 T. Funaki et al. Fig. 2. Serial MRA images obtained in a 1-year-old boy representing rapid disease progression. A: Image obtained 2 months before referral to our hospital, revealing moderate stenosis in the terminal portion of the ICA and M 1 segment of the MCA bilaterally. B: Image obtained at admission to our hospital, revealing signal decrease in the right MCA compared with that obtained 2 months previously, suggesting rapid disease progression in the right MCA. The patient subsequently underwent direct bypass for the right MCA territory. C: Image obtained 2 months after surgery, revealing an invisible signal in the left MCA, suggesting rapid disease progression in the left MCA. tion, 9,16,25 recent stroke occurring no more than 6 weeks before surgery or evidence of recent stroke on preoperative DWI, 9,16 advanced stage moyamoya (Suzuki Stages IV, V, and VI) in the ICA, 11 and disease involvement in the PCA. 11 Unilateral disease was defined as unilateral stenosis or occlusion of the terminal portion of the ICA with the formation of moyamoya vessels accompanied by no lesion or a subtle lesion around the contralateral terminal portion of the ICA. Severe hemodynamic compromise was defined as a defect in the cerebral blood flow both at rest and after acetazolamide challenge revealed on SPECT. Administration of antiplatelet agents was also recorded. Surgery All patients underwent MRI, SPECT, and angiography before surgery. Surgical revascularization was indicated for patients with cerebral ischemic manifestation. Patients presenting with other symptoms, such as epilepsy and intracranial hemorrhage, were also considered candidates for surgical revascularization as long as hemodynamic compromise existed. All patients underwent direct bypass, STA-MCA anastomosis, or combined bypass comprising STA-MCA anastomosis and encephalo-myo-synangiosis as a first-line treatment. 13 After completing 2 sessions of revascularization for the MCA territories, some patients required additional revascularization surgeries for the ACA and PCA territories. Our surgical procedures and treatment protocol are described in previous literature. 5,12,13 Antiplatelet agents, if administered, were discontinued for 3 days before surgery and 2 days after surgery. During general anesthesia, PaCO 2 and end-tidal CO 2 were closely monitored, and the level of PaCO 2 was strictly maintained between 37 and 40 mm Hg. Outcome All silent and symptomatic ischemic lesions, a primary outcome in this study, were diagnosed by neuroradiologists based on the results of DWI performed no longer than 14 days after surgery. A symptomatic lesion was defined as one causing a decline in the modified Rankin Scale (mrs) score. Such lesions were classified into either of 2 categories: cortical infarction or subcortical infarction. The patency of the bypass was also assessed using MRA performed in the same imaging session. Statistical Analysis Since more than half of the patients underwent multiple procedures, postoperative outcomes for such patients might not be statistically independent. In consideration of these dependencies, we used the generalized estimating equation (GEE) approach for the demographic descriptions of stable and unstable moyamoya disease as well as univariate and multivariate logistic regression analyses. 2 All p values and confidence intervals were calculated with robust standard error estimates from the GEE approach with the independent working correlation structure. Because of rare outcome events, we selected preoperative variables only with p values < 0.05 as covariates adjusted for the multivariate GEE logistic analysis. In light of its clinical importance, radiographic evidence of infarction was incorporated into the multivariate analysis regardless of its p value. As mentioned in Results, assessment of disease progression was not possible for 6 procedures; hence, these procedures were excluded from the primary analysis. We also conducted a sensitivity analysis that included the 6 procedures, all of which were assumed to be those of unstable disease (Fig. 1), considering the possibility that such patients might undergo only 1 MRA session because of rapid progression. We fit the same GEE logistic regression for both the primary and sensitivity analyses. Two-sided values of p < 0.05 and 95% confidence intervals of odds ratios that do not include 1 were considered significant. All analyses were performed using JMP (version 9) software and Windows SAS (version 9.3, SAS Institute Inc.). 402
4 Unstable moyamoya disease Results Characteristics of Unstable Disease Demographics of the 86 patients are summarized in Table 1. Among the 140 procedures performed in these patients, 6 procedures could not be assessed for disease progression for the following reasons: 2 MRI sessions were performed before surgery, but the interval was less than 2 weeks (3 procedures); only 1 MRI session was performed before surgery because the patient had suffered a minor stroke during admission to the neurological department at our hospital and was promptly referred to a neurosurgeon (1 procedure); and the surgeon did not require a second MRI before surgery because a baseline MRI had been performed shortly before referral (2 procedures). Postoperative DWI revealed neither silent nor symptomatic lesions in these 6 cases. Baseline characteristics of the 134 included and 6 excluded cases were compared, and no variable significantly differed between the 2 groups except for the prevalence of recent stroke (9% in the included group and 50% in the excluded group, p = 0.017). Of the 134 procedures included in the primary analysis, 24 (17.9%) were classified as unstable disease (Table 2): 16 as rapid progression, 6 as repeat stroke, and 2 as both. Disease progression at an interval exceeding 6 months had occurred before 5 procedures, all of which were classified in the stable group. Table 3 summarizes baseline characteristics of the stable and unstable groups. Compared with the stable group, the unstable group included more patients younger than 3 years (p = 0.029), more completed stroke as an initial manifestation (p < 0.001), more evidence of infarction (p = 0.030), and more underlying disease causing moyamoya syndrome (p = 0.049). The median interval between the 2 MRA sessions was 90.5 days (range days) for the stable group and 81.5 days (range days) for the unstable group. TABLE 1. Demographic and clinical characteristics of 86 patients included in the study Variable Value* Median age (yrs, IQR) 18.5 ( ) Female 56 (65.1) Initial manifestation TIA 51 (59.3) Completed stroke 18 (20.9) Intracranial hemorrhage 11 (12.8) Epilepsy 3 (3.5) Asymptomatic 3 (3.5) Underlying disease 7 (8.1) No. of procedures 1 37 (43.0) 2 44 (51.2) 3 5 (5.8) IQR = interquartile range. * Values are presented as the number of patients (%) unless noted otherwise. TABLE 2. Details of classification of 134 procedures as stable or unstable disease Variable No. of Procedures Stable disease (110 procedures) Neither progression nor repeated stroke 105 Progression over >6 mos 5 Unstable disease (24 procedures) Rapid progression w/in 6 mos 16 Repeated stroke w/in 6 mos 6 Both rapid progression & repeated stroke 2 Overall Outcome Postoperative DWI-defined lesions were detected after 13 (9.3%) of 140 procedures (Fig. 3). Six lesions were clinically silent, while 7 caused transient or permanent symptoms. A permanent ischemic complication occurred in 4 procedures (2.9%). These symptomatic lesions, all of which occurred in the unstable disease group, represented a cortical infarction remotely located from the anastomosis site, while the remaining 9 lesions included cortical and subcortical infarctions (Fig. 3). Lesions on the side contralateral to the surgery were detected on DWI in 3 procedures. The patency of all bypasses was confirmed using MRA. For patients who suffered a permanent ischemic complication, at the time of discharge 1 patient had an mrs score of 1, and 3 patients had an mrs score of 2. At the time of last follow-up, 2 of these patients had an mrs score of 1, and 2 patients had an mrs score of 2. Association Between Unstable Disease and Postoperative DWI-Detected Lesions The incidence of postoperative DWI-detected lesions in the unstable disease group was 33.3% (8 of 24 procedures), which was significantly higher than that in the stable disease group (5/110 procedures [4.5%], p < 0.001). Infarction causing permanent morbidity was seen after 4 procedures (16.7%) in the unstable disease group, while no permanent morbidity was observed in the stable disease group. No stroke occurred after the 14th postoperative day in either group. For the univariate analysis, unstable disease (p < 0.001), underlying disease (p = 0.028), and recent stroke (p = 0.012) were identified as preoperative variables associated with postoperative DWI-detected lesions (Table 4). The primary analysis revealed that unstable disease was a statistically significant factor independently associated with DWI-detected lesions (OR 6.62 [95% CI ]; Table 5). Unstable disease remains statistically significant in the sensitivity analysis (OR 5.36 [95% CI ]). Discussion The results of the present study suggest that age younger than 3 years and underlying disease causing moyamoya syndrome are associated with unstable moyamoya disease. Our results indicate that, despite the relatively low overall ischemic complication rate (2.9%), unstable disease is an 403
5 T. Funaki et al. TABLE 3. Demographic descriptions of stable and unstable moyamoya disease* Variable Stable (110 procedures) Unstable (24 procedures) p Value Age in yrs Mean ± SD 21.3 ± ± Median (range) 17.5 (0 52) 7.5 (1 51) Age <3 yrs 3 (2.7) 4 (16.7) Female 77 (70.0) 13 (54.2) Mean systolic BP in mm Hg ± ± Mean diastolic BP in mm Hg 73.2 ± ± Initial manifestation Completed stroke 16 (14.5) 13 (54.2) <0.001 TIA 74 (67.3) 4 (16.7) <0.001 Intracranial hemorrhage 13 (11.8) 3 (12.5) Other 7 (6.4) 4 (16.7) Underlying disease 7 (6.4) 5 (20.8) Frequency of TIA >3 times/mo 8 (7.3) 3 (12.5) Radiographic evidence of infarction 66 (60) 20 (83.3) Recent stroke 5 (4.5) 7 (29.2) <0.001 Unilateral disease 11 (10.0) 3 (12.5) Suzuki stage I 5 (4.5) 1 (4.2) II 32 (29.1) 8 (33.3) III 59 (53.6) 14 (58.3) IV 14 (12.7) 1 (4.2) V 0 0 Suzuki Stage IV 14 (12.7) 1 (4.2) PCA involvement 32 (29.1) 10 (41.7) Severe hemodynamic compromise 72 (66.7) 18 (75.0) Antiplatelet agent administration 92 (83.6) 21 (87.5) Median MRI interval in days (range) 90.5 (14 352) 81.5 (27 175) BP = blood pressure. * Values are number of procedures (%) unless indicated otherwise. Mean values are presented as the mean ± SD. The p values were calculated with robust standard errors derived from the GEE approach with the independent working correlation structure. Data were unavailable for 2 procedures. independent risk factor for perioperative DWI-detected lesions. The incidence of disease progression in moyamoya disease, which is receiving more attention especially regarding cases of unilateral disease, is not particularly rare. Disease progression occurs in 54% of pediatric patients over a mean period of 5.4 years and in 23.8% of adult patients over a mean period of 6.1 years. 19,21 A more recent study estimated the 3-year cumulative incidence of disease progression as 19% in children and adolescents with unilateral disease. 28 Younger age, 26,28 female sex, 19 contralateral angiographic abnormality, 20,26 and underlying cause of moyamoya syndrome 21 have been considered risk factors for contralateral progression of unilateral disease. The results of our study, which found younger age and underlying disease as risk factors for unstable disease, are in line with these reports. The mean time to progression estimated in the previous studies ranged from 14.3 to 34 months. 14,19,20 Our results may add important information to those of previous studies, because more rapid disease progression was observed in a substantial number of patients. Several factors, such as age younger than 3 years, 16 female sex, 15 presence of underlying disease, 6,22 frequent TIAs, 16 radiographic evidence of preexisting infarction, 9,16,25 recent episode of stroke, 9,16 advanced angiographic stage, 11 and disease involvement in the PCA, 11 are believed to increase ischemic complications after bypass surgery for moyamoya disease. Although young age and preexisting infarction were generally considered major risk factors for surgical outcome in moyamoya disease, some controversy remains in the literature regarding what constitutes a risk factor. Our univariate result, indicating that underlying disease and recent stroke are significant, partly coincides with the literature. In addition, our multivariate results suggest that unstable disease is another independent risk factor for perioperative ischemic complications. On the other hand, our results did not reveal a statistically significant impact of preexisting infarction on outcome, 404
6 Unstable moyamoya disease Fig. 3. Lesions detected on postoperative DWI. A: Silent lesions. B: Lesions causing transient symptoms. C: Lesions causing permanent symptoms. which contradicts findings of some previous reports. 9,16,25 A possible explanation for this contradiction is that unstable disease, including infarct as defined, acted as an intervening variable in multivariate analysis, which might diminish the true effect of infarct on outcome. A relatively high odds ratio was observed for preexisting infarct, and a study with a larger sample size may have detected its statistically significant impact on perioperative ischemic complication. Another reason we did not find a significant effect from TABLE 4. Univariate analyses of putative factors and postoperative DWI-detected lesions Variable OR (95% CI) p Value Unstable moyamoya 10.5 ( ) <0.001 Preop factors Age (yrs) 0.99 ( ) Age <3 yrs 4.22 ( ) Female 0.53 ( ) Systolic BP 1.02 ( ) Diastolic BP 1.02 ( ) Underlying disease 6.28 ( ) Frequency of TIAs >3 times/mo 2.26 ( ) Radiographic evidence of infarction 7.62 ( ) Recent stroke 6.28 ( ) Unilateral disease 0.69 ( ) Suzuki Stage IV 2.10 ( ) PCA involvement 0.97 ( ) Severe hemodynamic compromise* 6.31 ( ) Antiplatelet agent administration 2.38 ( ) * Data were unavailable for 2 procedures. preexisting infarct might be a difference in surgical procedures. The prestigious study by Kim et al., concluding that age younger than 3 years and preexisting infarct were risk factors for surgical ischemic complication, addressed indirect bypass. 16 On the other hand, Guzman et al., analyzing the outcomes of 450 direct bypasses, found no association between age and perioperative ischemia. 6 One possible mechanism of infarction developing after bypass surgery in the unstable disease group could be hemodynamic shift after direct bypass. Hayashi et al. discussed the mechanism of postoperative focal hypoperfusion detected by SPECT. 7 They speculated that the reversed MCA flow induced by the bypass graft could conflict with the original MCA flow, resulting in relative hypoperfusion in the remote territory of the MCA. Such a hemodynamic shift may be more prevalent in unstable disease. In unstable disease, leptomeningeal collateral flow may fail to develop sufficiently because of rapid disease progression. As a result, the bypass flow may conflict more strongly with the original antegrade flow supplying the MCA territory. Our finding that all symptomatic lesions occurring in unstable disease represent a cortical infarction remotely located from the anastomosis site may support this speculation. Our study has several limitations. First, the study excluded from the primary analysis 6 procedures before which only 1 session of MRA had been performed. The impact of possible bias caused by this exclusion may be minimal, however, because the sensitivity analysis also revealed statistical significance of unstable disease. Second, the retrospective study design meant that the interval between the 2 MRA sessions and the modality of MRA varied among patients. This might have caused a selection bias regarding the classification of unstable disease. Third, the result of 405
7 T. Funaki et al. TABLE 5. Estimated ORs and 95% CIs for primary and sensitivity multivariate analyses Primary Analysis Sensitivity Analysis Variable OR (95% CI) p Value OR (95% CI) p Value Unstable moyamoya 6.62 ( ) ( ) Underlying disease 2.98 ( ) ( ) Radiographic evidence of infarction 3.75 ( ) ( ) Recent stroke 1.88 ( ) ( ) the multivariate analysis has a relatively large confidence interval, which is attributable to the small number of cases. Larger prospective studies are therefore necessary to confirm the significant impact of unstable moyamoya disease on perioperative ischemic complications. These studies might also reveal the statistical significance of other variables such as preexisting infarct. Considering the devastating nature of unstable moyamoya disease reported to date, 4,17,18 early surgical revascularization might be recommended. Kim et al. similarly stressed the importance of early surgical intervention for aggressive moyamoya disease observed in children. 17 On the other hand, our finding, which detected the unstable state as an independent surgical risk factor, shed light on the need for preoperative diagnosis and specific perioperative management of unstable moyamoya disease. In terms of the diagnosis, performing MRA immediately before surgery might be useful, as the disease progression could be detected through a comparison with previous findings. In terms of treatment, perioperative management should be focused more on preventing ischemic complications. Although intentional lowering of blood pressure is considered for patients with hyperperfusion complications, 3 those with unstable disease should instead be maintained in a normotensive or slightly hypertensive state. Strict control of blood CO 2 level during surgery, in which PaCO 2 is maintained between 37 and 40 mm Hg at our institution, should also be undertaken. More aggressive use of antiplatelet agents could be adopted as a possible option for unstable disease. Although we adopted direct bypass as the first choice for treating moyamoya disease, tentative indirect bypass followed by elective direct bypass may be considered for unstable disease. This strategy can be indicated especially when acute hemorrhagic infarction after direct bypass as well as hemodynamic shift is concerned. The efficacy of these possible methods of management of unstable disease should be tested in future studies. Conclusions Unstable moyamoya disease, reasonably defined as cases of rapid progression or repeated stroke, represents a clinically challenging condition. It is more prevalent in patients younger than 3 years and those with underlying disease causing moyamoya syndrome. Unstable moyamoya disease is a possible risk factor associated with perioperative ischemic complication. The concept of unstable moyamoya disease may contribute to further improvement in the surgical results of moyamoya disease as a result of focused perioperative management arising from appropriate surgical risk stratification. Acknowledgments We are grateful to Dr. Tosiya Sato, Professor of the Department of Biostatics, Kyoto University School of Public Health, for providing advice on statistics and performing the GEE analyses. We also appreciate the efforts of Dr. Noritaka Sano, Ms. Yuko Tanaka, and Ms. Yuka Aramaki in collecting patient records. References 1. Austen WG, Edwards JE, Frye RL, Gensini GG, Gott VL, Griffith LS, et al: A reporting system on patients evaluated for coronary artery disease. Report of the Ad Hoc Committee for Grading of Coronary Artery Disease, Council on Cardiovascular Surgery, American Heart Association. Circulation 51 (4 Suppl):5 40, Diggle P, Heagerty PJ, Liang KY, Zeger SL: Analysis of Longitudinal Data, ed 2. Oxford, UK: Oxford University Press, Fujimura M, Inoue T, Shimizu H, Saito A, Mugikura S, Tominaga T: Efficacy of prophylactic blood pressure lowering according to a standardized postoperative management protocol to prevent symptomatic cerebral hyperperfusion after direct revascularization surgery for moyamoya disease. Cerebrovasc Dis 33: , Fujiwara F, Yamada H, Hayashi S, Tamaki N: [A case of adult moyamoya disease showing fulminant clinical course associated with progression from unilateral to bilateral involvement.] No Shinkei Geka 25:79 84, 1997 (Jpn) 5. Funaki T, Takahashi JC, Takagi Y, Yoshida K, Araki Y, Kikuchi T, et al: Impact of posterior cerebral artery involvement on long-term clinical and social outcome of pediatric moyamoya disease. J Neurosurg Pediatr 12: , Guzman R, Lee M, Achrol A, Bell-Stephens T, Kelly M, Do HM, et al: Clinical outcome after 450 revascularization procedures for moyamoya disease. Clinical article. J Neurosurg 111: , Hayashi T, Shirane R, Fujimura M, Tominaga T: Postoperative neurological deterioration in pediatric moyamoya disease: watershed shift and hyperperfusion. J Neurosurg Pediatr 6:73 81, Houkin K, Nakayama N, Kuroda S, Nonaka T, Shonai T, Yoshimoto T: Novel magnetic resonance angiography stage grading for moyamoya disease. Cerebrovasc Dis 20: , Hyun SJ, Kim JS, Hong SC: Prognostic factors associated with perioperative ischemic complications in adult-onset moyamoya disease. Acta Neurochir (Wien) 152: , Ishikawa T, Houkin K, Kamiyama H, Abe H: Effects of surgical revascularization on outcome of patients with pediatric moyamoya disease. Stroke 28: , Jung YJ, Ahn JS, Kwon H, Kwun BD: Ischemic complications occurring in the contralateral hemisphere after surgical treatment of adults with moyamoya disease. J Korean Neurosurg Soc 50: , Karasawa J, Kikuchi H, Furuse S, Kawamura J, Sakaki T: Treatment of moyamoya disease with STA-MCA anastomosis. J Neurosurg 49: ,
8 Unstable moyamoya disease 13. Karasawa J, Kikuchi H, Furuse S, Sakaki T, Yoshida Y: A surgical treatment of moyamoya disease encephalo-myo synangiosis. Neurol Med Chir (Tokyo) 17:29 37, Kelly ME, Bell-Stephens TE, Marks MP, Do HM, Steinberg GK: Progression of unilateral moyamoya disease: a clinical series. Cerebrovasc Dis 22: , Khan N, Achrol AS, Guzman R, Burns TC, Dodd R, Bell- Stephens T, et al: Sex differences in clinical presentation and treatment outcomes in Moyamoya disease. Neurosurgery 71: , Kim SH, Choi JU, Yang KH, Kim TG, Kim DS: Risk factors for postoperative ischemic complications in patients with moyamoya disease. J Neurosurg 103 (5 Suppl): , Kim SK, Seol HJ, Cho BK, Hwang YS, Lee DS, Wang KC: Moyamoya disease among young patients: its aggressive clinical course and the role of active surgical treatment. Neurosurgery 54: , Kim TW, Seo BR, Kim JH, Kim YO: Rapid progression of unilateral moyamoya disease. J Korean Neurosurg Soc 49:65 67, Kuroda S, Ishikawa T, Houkin K, Nanba R, Hokari M, Iwasaki Y: Incidence and clinical features of disease progression in adult moyamoya disease. Stroke 36: , Lee SC, Jeon JS, Kim JE, Chung YS, Ahn JH, Cho WS, et al: Contralateral progression and its risk factor in surgically treated unilateral adult moyamoya disease with a review of pertinent literature. Acta Neurochir (Wien) 156: , Lin N, Baird L, Koss M, Kopecky KE, Gone E, Ullrich NJ, et al: Discovery of asymptomatic moyamoya arteriopathy in pediatric syndromic populations: radiographic and clinical progression. Neurosurg Focus 31(6):E6, Mallory GW, Bower RS, Nwojo ME, Taussky P, Wetjen NM, Varzoni TC, et al: Surgical outcomes and predictors of stroke in a North American white and African American moyamoya population. Neurosurgery 73: , Moise A, Théroux P, Taeymans Y, Descoings B, Lespérance J, Waters DD, et al: Unstable angina and progression of coronary atherosclerosis. N Engl J Med 309: , Research Committee on the Pathology and Treatment of Spontaneous Occlusion of the Circle of Willis: Guidelines for diagnosis and treatment of moyamoya disease (spontaneous occlusion of the circle of Willis). Neurol Med Chir (Tokyo) 52: , Sato K, Shirane R, Yoshimoto T: Perioperative factors related to the development of ischemic complications in patients with moyamoya disease. Childs Nerv Syst 13:68 72, Smith ER, Scott RM: Progression of disease in unilateral moyamoya syndrome. Neurosurg Focus 24(2):E17, Yeghiazarians Y, Braunstein JB, Askari A, Stone PH: Unstable angina pectoris. N Engl J Med 342: , Yeon JY, Shin HJ, Kong DS, Seol HJ, Kim JS, Hong SC, et al: The prediction of contralateral progression in children and adolescents with unilateral moyamoya disease. Stroke 42: , 2011 Author Contributions Conception and design: Funaki. Acquisition of data: Funaki. Analysis and interpretation of data: Funaki, Okada, Fushimi. Drafting the article: Funaki. Critically revising the article: Takahashi, Takagi, Mitsuhara, Miyamoto. Reviewed submitted version of manuscript: Takahashi, Takagi, Kikuchi, Yoshida, Mitsuhara, Kataoka, Okada, Fushimi, Miyamoto. Approved the final version of the manuscript on behalf of all authors: Funaki. Statistical analysis: Funaki. Study supervision: Takahashi, Takagi, Kikuchi, Yoshida, Kataoka, Miyamoto. Correspondence Takeshi Funaki, Department of Neurosurgery, Kyoto University Graduate School of Medicine, 54 Kawahara-cho, Shogoin, Sakyo-ku, Kyoto , Japan. tfunaki@kuhp.kyoto-u. ac.jp. 407
Moyamoya disease (MMD) is a rare steno-occlusive
 CLINICAL ARTICLE J Neurosurg 126:1573 1577, 2017 Low flow velocity in the middle cerebral artery predicting infarction after bypass surgery in adult moyamoya disease *Hoyeon Cho, MD, 1 Kyung Il Jo, MD,
CLINICAL ARTICLE J Neurosurg 126:1573 1577, 2017 Low flow velocity in the middle cerebral artery predicting infarction after bypass surgery in adult moyamoya disease *Hoyeon Cho, MD, 1 Kyung Il Jo, MD,
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Neurosurg Focus 5 (5):Article 4, 1998
 Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
 Impact of posterior cerebral artery Titleclinical and social outcome of pedi Dissertation_ 全文 ) Author(s) Funaki, Takeshi Citation Kyoto University ( 京都大学 ) Issue Date 2015-01-23 URL http://dx.doi.org/10.14989/doctor.r
Impact of posterior cerebral artery Titleclinical and social outcome of pedi Dissertation_ 全文 ) Author(s) Funaki, Takeshi Citation Kyoto University ( 京都大学 ) Issue Date 2015-01-23 URL http://dx.doi.org/10.14989/doctor.r
MOYA Moya disease is a rare idiopathic
 Research Papers Moya Moya Cases Treated with Encephaloduroarteriosynangiosis Parimal Tripathi, Varsha Tripathi, Ronak J. Naik and Jaimin M. Patel From Gujarat Cancer & Research Institute, Ahmedabad; Sterling
Research Papers Moya Moya Cases Treated with Encephaloduroarteriosynangiosis Parimal Tripathi, Varsha Tripathi, Ronak J. Naik and Jaimin M. Patel From Gujarat Cancer & Research Institute, Ahmedabad; Sterling
Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study
 REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 194 198, 2015 doi: 10.2176/nmc.ra.2014-0305 Online February 20, 2015 Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study Satoshi Kuroda;
REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 194 198, 2015 doi: 10.2176/nmc.ra.2014-0305 Online February 20, 2015 Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study Satoshi Kuroda;
Title. CitationWorld Neurosurgery, 80(5): Issue Date Doc URL. Rights. Rights(URL)
 Title Effective Surgical Revascularization Improves Cerebr Moyamoya Disease Kawabori, Masahito; Kuroda, Satoshi; Nakayama, Naoki Author(s) Nagara CitationWorld Neurosurgery, 80(5): 612-619 Issue Date 2013-11
Title Effective Surgical Revascularization Improves Cerebr Moyamoya Disease Kawabori, Masahito; Kuroda, Satoshi; Nakayama, Naoki Author(s) Nagara CitationWorld Neurosurgery, 80(5): 612-619 Issue Date 2013-11
Clinicoepidemiological Features of Asymptomatic Moyamoya Disease in Adult Patients
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2014.16.3.241 Original Article Clinicoepidemiological Features of Asymptomatic
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2014.16.3.241 Original Article Clinicoepidemiological Features of Asymptomatic
Tohoku J. Exp. Med., 2015, 236, Current Management of Moyamoya Disease 45
 Tohoku J. Exp. Med., 2015, 236, 45-53 Current Management of Moyamoya Disease 45 Invited Review Current Status of Revascularization Surgery for Moyamoya Disease: Special Consideration for Its Internal Carotid-External
Tohoku J. Exp. Med., 2015, 236, 45-53 Current Management of Moyamoya Disease 45 Invited Review Current Status of Revascularization Surgery for Moyamoya Disease: Special Consideration for Its Internal Carotid-External
Moyamoya disease is a progressive cerebrovascular. Pial synangiosis in patients with moyamoya younger than 2 years of age.
 J Neurosurg Pediatrics 13:420 425, 2014 AANS, 2014 Pial synangiosis in patients with moyamoya younger than 2 years of age Clinical article Eric M. Jackson, M.D., Ning Lin, M.D., Sunil Manjila, M.D., R.
J Neurosurg Pediatrics 13:420 425, 2014 AANS, 2014 Pial synangiosis in patients with moyamoya younger than 2 years of age Clinical article Eric M. Jackson, M.D., Ning Lin, M.D., Sunil Manjila, M.D., R.
Occlusive cerebrovascular disease. A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats
 FPⅧ-1 A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats Ahmed Said Mansour 1, Kuniyasu Niizuma 2, Sherif Rashad 2, Hidenori Endo 2, Toshiki Endo 3, Kenichi
FPⅧ-1 A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats Ahmed Said Mansour 1, Kuniyasu Niizuma 2, Sherif Rashad 2, Hidenori Endo 2, Toshiki Endo 3, Kenichi
Title in Children. Issue Date Copyright 2011 S. Karger AG, Base.
 NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Features and Long-Term Fol in Children. Hayashi, Kentaro; Horie, Nobutaka; Citation Pediatric Neurosurgery, 47(1), pp.1 Issue Date 2011-09 URL
NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Features and Long-Term Fol in Children. Hayashi, Kentaro; Horie, Nobutaka; Citation Pediatric Neurosurgery, 47(1), pp.1 Issue Date 2011-09 URL
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
Case Report. Fumihiro MATANO 1, Yasuo MURAI 2, Asami KUBOTA 1, Takayuki MIZUNARI 1, Shiro KOBAYASHI 1, Akio MORITA 2
 DOI: 10.5137/1019-5149.JTN.19271-16.1 Received: 17.10.2016 / Accepted: 19.01.2017 Published Online: 07.02.2017 Case Report The Ivy Sign on Fluid Attenuated Inversion Recovery Images Related to Single-Photon
DOI: 10.5137/1019-5149.JTN.19271-16.1 Received: 17.10.2016 / Accepted: 19.01.2017 Published Online: 07.02.2017 Case Report The Ivy Sign on Fluid Attenuated Inversion Recovery Images Related to Single-Photon
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
Angiographic features of hemorrhagic moyamoya disease with high recurrence risk: a supplementary analysis of the Japan Adult Moyamoya Trial
 CLINICAL ARTICLE J Neurosurg 128:777 784, 2018 Angiographic features of hemorrhagic moyamoya disease with high recurrence risk: a supplementary analysis of the Japan Adult Moyamoya Trial Takeshi Funaki,
CLINICAL ARTICLE J Neurosurg 128:777 784, 2018 Angiographic features of hemorrhagic moyamoya disease with high recurrence risk: a supplementary analysis of the Japan Adult Moyamoya Trial Takeshi Funaki,
Young So, MD; Ho-Young Lee, MD; Seung-Ki Kim, MD; Jae Sung Lee, PhD; Kyu-Chang Wang, MD; Byung-Kyu Cho, MD; Eunjoo Kang, PhD; Dong Soo Lee, MD
 Prediction of the Clinical Outcome of Pediatric Moyamoya Disease With Postoperative Basal/Acetazolamide Stress Brain Perfusion SPECT After Revascularization Surgery Young So, MD; Ho-Young Lee, MD; Seung-Ki
Prediction of the Clinical Outcome of Pediatric Moyamoya Disease With Postoperative Basal/Acetazolamide Stress Brain Perfusion SPECT After Revascularization Surgery Young So, MD; Ho-Young Lee, MD; Seung-Ki
Moyamoya disease (MMD), an idiopathic disease. Direct versus indirect revascularization in the treatment of moyamoya disease
 CLINICAL ARTICLE J Neurosurg 129:480 489, 2018 Direct versus indirect revascularization in the treatment of moyamoya disease *Seong-eun Park, BSc, Ju-seong Kim, MD, Eun Kyung Park, MD, Kyu-Won Shim, MD,
CLINICAL ARTICLE J Neurosurg 129:480 489, 2018 Direct versus indirect revascularization in the treatment of moyamoya disease *Seong-eun Park, BSc, Ju-seong Kim, MD, Eun Kyung Park, MD, Kyu-Won Shim, MD,
Moyamoya disease. Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease.
 FPⅢ- Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease Tomohide Hayashi Departments of Neurosurgery, University of Toyama Background - is a unique cerebrovascular
FPⅢ- Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease Tomohide Hayashi Departments of Neurosurgery, University of Toyama Background - is a unique cerebrovascular
Moyamoya disease is an unusual form of chronic, occlusive
 Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease
 Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Moyamoya Disease in China Its Clinical Features and Outcomes
 Moyamoya Disease in China Its Clinical Features and Outcomes Lian Duan, MD, PhD; Xiang-Yang Bao, MM; Wei-Zhong Yang, BS; Wan-Chao Shi, MD; De-Sheng Li, MD; Zheng-Shan Zhang, MM; Rui Zong, MM; Cong Han,
Moyamoya Disease in China Its Clinical Features and Outcomes Lian Duan, MD, PhD; Xiang-Yang Bao, MM; Wei-Zhong Yang, BS; Wan-Chao Shi, MD; De-Sheng Li, MD; Zheng-Shan Zhang, MM; Rui Zong, MM; Cong Han,
Title. Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉. Citation 脳卒中の外科, 37(5): Issue Date Doc URL.
 Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
Case Report INTRODUCTION
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Department of Neurosurgery, Showa University School of Medicine; and 2 Tokyo Midtown Medical Center, Tokyo, Japan
 CLINICAL ARTICLE Detection rates and sites of unruptured intracranial aneurysms according to sex and age: an analysis of MR angiography based brain examinations of 4070 healthy Japanese adults Yohichi
CLINICAL ARTICLE Detection rates and sites of unruptured intracranial aneurysms according to sex and age: an analysis of MR angiography based brain examinations of 4070 healthy Japanese adults Yohichi
Moyamoya disease is characterized by chronic progressive
 clinical article J Neurosurg 124:1766 1772, 2016 Periventricular anastomosis in moyamoya disease: detecting fragile collateral vessels with MR angiography Takeshi Funaki, MD, PhD, 1 Jun C. Takahashi, MD,
clinical article J Neurosurg 124:1766 1772, 2016 Periventricular anastomosis in moyamoya disease: detecting fragile collateral vessels with MR angiography Takeshi Funaki, MD, PhD, 1 Jun C. Takahashi, MD,
Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
 Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Moyamoya disease in the midwestern United States
 Neurosurg Focus 5 (5):Article 1, 1998 Moyamoya disease in the midwestern United States Nicholas M. Wetjen, B.S., P. Charles Garell, M.D., Nicholas V. Stence, and Christopher M. Loftus, M.D. Division of
Neurosurg Focus 5 (5):Article 1, 1998 Moyamoya disease in the midwestern United States Nicholas M. Wetjen, B.S., P. Charles Garell, M.D., Nicholas V. Stence, and Christopher M. Loftus, M.D. Division of
Department of Neurosurgery, Hallym University College of Medicine, Chuncheon, Korea; 2
 Original Article doi: 10.2176/nmc.oa.2017-0198 Neurol Med Chir (Tokyo) 58, 116 123, 2018 Association of Hyperthyroidism and Thyroid Autoantibodies with Moyamoya Disease and Its Stroke Event: A Population-based
Original Article doi: 10.2176/nmc.oa.2017-0198 Neurol Med Chir (Tokyo) 58, 116 123, 2018 Association of Hyperthyroidism and Thyroid Autoantibodies with Moyamoya Disease and Its Stroke Event: A Population-based
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
Overview Blood supply of the brain What is moyamoya disease? > 1
 Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
CT perfusion in Moyamoya disease
 CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
Moyamoya disease (MMD) is a progressive stenoocclusive
 J Neurosurg 121:432 440, 2014 AANS, 2014 The frequency of postoperative stroke in moyamoya disease following combined revascularization: a single-university series and systematic review Clinical article
J Neurosurg 121:432 440, 2014 AANS, 2014 The frequency of postoperative stroke in moyamoya disease following combined revascularization: a single-university series and systematic review Clinical article
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Thirteen-year Experience of 44 Patients with Adult Hemorrhagic Moyamoya Disease from a Single Institution: Clinical Analysis by Management Modality
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.191 Clinical Article Thirteen-year Experience of 44 Patients with Adult
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.191 Clinical Article Thirteen-year Experience of 44 Patients with Adult
Moyamoya disease (MMD) is a chronic, progressive cerebrovascular. Clinical and Angiographic Features and Stroke Types in Adult Moyamoya Disease
 ORIGINAL RESEARCH BRAIN Clinical and Angiographic Features and Stroke Types in Adult Moyamoya Disease D.-K. Jang, K.-S. Lee, H.K. Rha, P.-W. Huh, J.-H. Yang, I.S. Park, J.-G. Ahn, J.H. Sung, and Y.-M.
ORIGINAL RESEARCH BRAIN Clinical and Angiographic Features and Stroke Types in Adult Moyamoya Disease D.-K. Jang, K.-S. Lee, H.K. Rha, P.-W. Huh, J.-H. Yang, I.S. Park, J.-G. Ahn, J.H. Sung, and Y.-M.
MMD is a rare cerebrovascular disease first described by
 ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
Clinical Study Circle of Willis Variants: Fetal PCA
 Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
In patients with moyamoya the clinical significance of. Preoperative transdural collateral vessels in moyamoya as radiographic biomarkers of disease
 CLINICAL ARTICLE J Neurosurg Pediatr 19:289 295, 2017 Preoperative transdural collateral vessels in moyamoya as radiographic biomarkers of disease Armide Storey, BS, 1 R. Michael Scott, MD, 1 Richard Robertson,
CLINICAL ARTICLE J Neurosurg Pediatr 19:289 295, 2017 Preoperative transdural collateral vessels in moyamoya as radiographic biomarkers of disease Armide Storey, BS, 1 R. Michael Scott, MD, 1 Richard Robertson,
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk
 Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
collaterals offset ischemia
 Imaging of Intracranial Stenosis objectives & next steps collaterals offset ischemia systematic evaluation of collaterals hemodynamic impact, not % stenosis develop fractional flow measures collateral
Imaging of Intracranial Stenosis objectives & next steps collaterals offset ischemia systematic evaluation of collaterals hemodynamic impact, not % stenosis develop fractional flow measures collateral
In cerebral infarction, the prognostic value of angiographic
 Nonrelevant Cerebral Atherosclerosis is a Strong Prognostic Factor in Acute Cerebral Infarction Jinkwon Kim, MD; Tae-Jin Song, MD; Dongbeom Song, MD; Hye Sun Lee, MS; Chung Mo Nam, PhD; Hyo Suk Nam, MD,
Nonrelevant Cerebral Atherosclerosis is a Strong Prognostic Factor in Acute Cerebral Infarction Jinkwon Kim, MD; Tae-Jin Song, MD; Dongbeom Song, MD; Hye Sun Lee, MS; Chung Mo Nam, PhD; Hyo Suk Nam, MD,
Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain
 Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain Christopher Payne Currently, no medical treatment exists to prevent the progression of moyamoya disease, and neurosurgical treatment
Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain Christopher Payne Currently, no medical treatment exists to prevent the progression of moyamoya disease, and neurosurgical treatment
Vertebrobasilar Insufficiency
 Equilibrium Res Vol. (3) Vertebrobasilar Insufficiency Toshiaki Yamanaka Department of Otolaryngology-Head and Neck Surgery, Nara Medical University School of Medicine Vertebrobasilar insufficiency (VBI)
Equilibrium Res Vol. (3) Vertebrobasilar Insufficiency Toshiaki Yamanaka Department of Otolaryngology-Head and Neck Surgery, Nara Medical University School of Medicine Vertebrobasilar insufficiency (VBI)
Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease
 Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Although moyamoya disease, a rare cerebrovascular occlusive
 Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Clinical implications of the cortical hyperintensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease
 clinical article J Neurosurg 126:1 7, 2017 Clinical implications of the cortical hyperintensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease Eika Hamano,
clinical article J Neurosurg 126:1 7, 2017 Clinical implications of the cortical hyperintensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease Eika Hamano,
The learning curve associated with intracranial angioplasty and stenting: analysis from a single center
 Original Article Page 1 of 7 The learning curve associated with intracranial angioplasty and stenting: analysis from a single center Peiquan Zhou, Guang Zhang, Zhiyong Ji, Shancai Xu, Huaizhang Shi Department
Original Article Page 1 of 7 The learning curve associated with intracranial angioplasty and stenting: analysis from a single center Peiquan Zhou, Guang Zhang, Zhiyong Ji, Shancai Xu, Huaizhang Shi Department
This quiz is being published on behalf of the Education Committee of the SNACC.
 Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Asymptomatic Carotid Stenosis To Do or Not To Do
 Asymptomatic Carotid Stenosis To Do or Not To Do October 22, 2016 Neurosciences: Updates and Controversies Andrew C. MacDougall, MD Advocate Medical Group Advocate Lutheran General Hospital Principle
Asymptomatic Carotid Stenosis To Do or Not To Do October 22, 2016 Neurosciences: Updates and Controversies Andrew C. MacDougall, MD Advocate Medical Group Advocate Lutheran General Hospital Principle
Moyamoya Disease: Comparison of Assessment with 3.0T MR Angiography and MR Imaging versus Conventional
 Moyamoya Disease: Comparison of Assessment with 3.0T MR Angiography and MR Imaging versus Conventional Angiography Poster No.: C-2771 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: Q.
Moyamoya Disease: Comparison of Assessment with 3.0T MR Angiography and MR Imaging versus Conventional Angiography Poster No.: C-2771 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: Q.
Emergently? Michigan Institute for Neurological Disorders. Garden City Hospital, Garden City, Michigan
 Why Should TIA be Treated Emergently? Anne M. Pawlak, D.O. F.A.C.N. Michigan Institute for Neurological Disorders Director Neurology Residency Program, Garden City Hospital, Garden City, Michigan According
Why Should TIA be Treated Emergently? Anne M. Pawlak, D.O. F.A.C.N. Michigan Institute for Neurological Disorders Director Neurology Residency Program, Garden City Hospital, Garden City, Michigan According
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Transcranial Doppler (Basic Step) Dae-il Chang, M.D., Sung Sang Yoon, M.D. Department of Neurology, College of Medicine, Kyunghee university
 Transcranial Doppler (Basic Step) Dae-il Chang, M.D., Sung Sang Yoon, M.D. Department of Neurology, College of Medicine, Kyunghee university Principles of Doppler Ultrasonography Major target Speed & direction
Transcranial Doppler (Basic Step) Dae-il Chang, M.D., Sung Sang Yoon, M.D. Department of Neurology, College of Medicine, Kyunghee university Principles of Doppler Ultrasonography Major target Speed & direction
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion
 Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
010050,Inner Mongolia, China
 Possible factors influencing postoperative temporary neurologic deterioration following standard superficial temporal artery-middle cerebral artery (STA-MCA) bypass surgery: diameter of STA and MCA (M4)
Possible factors influencing postoperative temporary neurologic deterioration following standard superficial temporal artery-middle cerebral artery (STA-MCA) bypass surgery: diameter of STA and MCA (M4)
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Moyamoya disease presenting as acute onset cortical blindness: a case report
 Romanian Neurosurgery Volume XXX Number 1 2016 January-March Article Moyamoya disease presenting as acute onset cortical blindness: a case report Dudi Maniram, Bansal Rajeev, Srivastava Trilochan, Sardana
Romanian Neurosurgery Volume XXX Number 1 2016 January-March Article Moyamoya disease presenting as acute onset cortical blindness: a case report Dudi Maniram, Bansal Rajeev, Srivastava Trilochan, Sardana
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
THE incidence of stroke after noncardiac surgery
 Lack of Association between Carotid Artery Stenosis and Stroke or Myocardial Injury after Noncardiac Surgery in High-risk Patients ABSTRACT Background: Whether carotid artery stenosis predicts stroke after
Lack of Association between Carotid Artery Stenosis and Stroke or Myocardial Injury after Noncardiac Surgery in High-risk Patients ABSTRACT Background: Whether carotid artery stenosis predicts stroke after
Summary of some of the landmark articles:
 Summary of some of the landmark articles: The significance of unruptured intracranial saccular aneurysms: Weibers et al Mayo clinic. 1987 1. 131 patients with 161 aneurysms were followed up at until death,
Summary of some of the landmark articles: The significance of unruptured intracranial saccular aneurysms: Weibers et al Mayo clinic. 1987 1. 131 patients with 161 aneurysms were followed up at until death,
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents
 Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Neuroscience. Journal. Moyamoya disease a review and case illustration. P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016
 Neuroscience P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016 Journal Moyamoya disease a review and case illustration pg. 5 Choroid Plexus Papilloma in adults pg. 8 As physician co-leaders of Palmetto
Neuroscience P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016 Journal Moyamoya disease a review and case illustration pg. 5 Choroid Plexus Papilloma in adults pg. 8 As physician co-leaders of Palmetto
Moyamoya syndrome associated with cocaine abuse Case report
 Neurosurg Focus 5 (5):Article 7, 1998 Moyamoya syndrome associated with cocaine abuse Case report Marc S. Schwartz, M.D., and R. Michael Scott, M.D. Division of Neurosurgery, Albany Medical College, Albany,
Neurosurg Focus 5 (5):Article 7, 1998 Moyamoya syndrome associated with cocaine abuse Case report Marc S. Schwartz, M.D., and R. Michael Scott, M.D. Division of Neurosurgery, Albany Medical College, Albany,
A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty
 DOI: 10.5797/jnet.cr.2017-0043 A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty Jun Niimi, Kenta Tasaka, Fumio Nemoto, Takuya
DOI: 10.5797/jnet.cr.2017-0043 A Patient with Stenosis of the Cervical Internal Carotid Artery in Whom Hyperperfusion Syndrome Occurred after Staged Angioplasty Jun Niimi, Kenta Tasaka, Fumio Nemoto, Takuya
Treatment Considerations for Carotid Artery Stenosis. Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery
 Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY
 Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
A CASE OF RECURRENT ALTERNATING TRANSIENT HEMIPARESIS Dr. Shunmuga Arumugasamy.S DNB Resident Railway Hospital, Perambur.
 A CASE OF RECURRENT ALTERNATING TRANSIENT HEMIPARESIS Dr. Shunmuga Arumugasamy.S DNB Resident Railway Hospital, Perambur. 6 year old school going child. Apparently normal till 3 yrs when she developed
A CASE OF RECURRENT ALTERNATING TRANSIENT HEMIPARESIS Dr. Shunmuga Arumugasamy.S DNB Resident Railway Hospital, Perambur. 6 year old school going child. Apparently normal till 3 yrs when she developed
Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal
 Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal anterior cerebral artery aneurysm Acta Neurochirurgica Kampei Shimizu, Shoichi Tani, Hirotoshi Imamura,
Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal anterior cerebral artery aneurysm Acta Neurochirurgica Kampei Shimizu, Shoichi Tani, Hirotoshi Imamura,
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms
 J Neurosurg 57:622-628, 1982 Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms MAMORU TANEDA, M.D. Department of Neurosurgery, Hanwa Memorial Hospital, Osaka,
J Neurosurg 57:622-628, 1982 Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms MAMORU TANEDA, M.D. Department of Neurosurgery, Hanwa Memorial Hospital, Osaka,
ACUTE STROKE IMAGING
 ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for
 Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Since the introduction of extracranial-intracranial (ECIC)
 ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Ischemic Stroke in Critically Ill Patients with Malignancy
 Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease
 272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
framework for flow Objectives Acute Stroke Treatment Collaterals in Acute Ischemic Stroke framework & basis for flow
 Acute Stroke Treatment Collaterals in Acute Ischemic Stroke Objectives role of collaterals in acute ischemic stroke collateral therapeutic strategies David S Liebeskind, MD Professor of Neurology & Director
Acute Stroke Treatment Collaterals in Acute Ischemic Stroke Objectives role of collaterals in acute ischemic stroke collateral therapeutic strategies David S Liebeskind, MD Professor of Neurology & Director
Improvement of Cerebral Arterial Stenosis Associated With Basedow's Disease
 Neurol Med Chir (Tokyo) 45, 578 582, 2005 Improvement of Cerebral Arterial Stenosis Associated With Basedow's Disease Case Report Shiro YAMASHITA, Takashi TAMIYA, AtsushiSHINDO, KeisukeMIYAKE, Takehiro
Neurol Med Chir (Tokyo) 45, 578 582, 2005 Improvement of Cerebral Arterial Stenosis Associated With Basedow's Disease Case Report Shiro YAMASHITA, Takashi TAMIYA, AtsushiSHINDO, KeisukeMIYAKE, Takehiro
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging
 AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
Recent Advances in Neurology Difficult Cases
 Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
TCD in Subclavian Steal Syndrome
 ISSN 2005-7881 Journal of Neurosonology 2(Suppl. 1):25-30, 2010 TCD in Subclavian Steal Syndrome Soon-Tae Lee, M.D., Ph.D. Department of Neurology, Seoul National University Hospital, Seoul, South Korea
ISSN 2005-7881 Journal of Neurosonology 2(Suppl. 1):25-30, 2010 TCD in Subclavian Steal Syndrome Soon-Tae Lee, M.D., Ph.D. Department of Neurology, Seoul National University Hospital, Seoul, South Korea
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Guidelines for Ultrasound Surveillance
 Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Hyperperfusion syndrome after MCA embolectomy a rare complication?
 ISSN 1507-6164 DOI: 10.12659/AJCR.889672 Received: 2013.08.13 Accepted: 2013.09.11 Published: 2013.11.29 Hyperperfusion syndrome after MCA embolectomy a rare complication? Authors Contribution: Study Design
ISSN 1507-6164 DOI: 10.12659/AJCR.889672 Received: 2013.08.13 Accepted: 2013.09.11 Published: 2013.11.29 Hyperperfusion syndrome after MCA embolectomy a rare complication? Authors Contribution: Study Design
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
TABLES. Table 1 Terminal vessel aneurysms. Table. Aneurysm location. Bypass flow** Symptoms Strategy Bypass recipient. Age/ Sex.
 Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
WHI Form Report of Cardiovascular Outcome Ver (For items 1-11, each question specifies mark one or mark all that apply.
 WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
