Limitations of the Outback LTD re-entry device in femoropopliteal chronic total occlusions
|
|
|
- Colleen Armstrong
- 5 years ago
- Views:
Transcription
1 From the Society for Clinical Vascular Surgery Limitations of the Outback LTD re-entry device in femoropopliteal chronic total occlusions Susanna H. Shin, MD, Donald Baril, MD, Rabih Chaer, MD, Robert Rhee, MD, Michel Makaroun, MD, and Luke Marone, MD, Pittsburgh, Pa Objective: Subintimal recanalization for the treatment of femoropopliteal chronic total occlusions (CTO) occasionally requires re-entry devices to access the true lumen distally, but limited information is available on factors predicting the success or failure of these devices. We evaluated the Outback LTD re-entry device (LuMend, Redwood City, Calif; acquired by Cordis Corp, Miami Lakes, Fla). Methods: A retrospective review of patients with femoropopliteal CTO from August 2006 to August 2009 was performed. Age, gender, occlusion length, site of re-entry, and the angle of the aortic bifurcation were recorded. Procedural angiograms were used to assign a calcification score (none, mild, moderate, severe) at the re-entry site. Univariate and multivariate logistic regression analyses were used to identify factors predicting failure of re-entry into the true lumen. Results: Of 249 CTOs treated, the re-entry device was used 52 times (20.9%): 47 superficial femoral artery (SFA) occlusions and 5 combined SFA and popliteal artery occlusions (33 TransAtlantic InterSociety Consensus II type C and 18 type D lesions). Of 48 procedures with available angiograms for review, the target re-entry site was at the adductor canal in 30 (62.5%), the above-knee popliteal artery in 13 (27.1%), behind the knee joint in 4 (8.3%), and the mid-sfa in 2 (4.2%). Patients (54% men) were a mean age of 73.1 years. Re-entry was successful in 34 attempts (64.5%). Causes of failure included inability to re-enter the true lumen in 11 (61.1%), difficulty tracking the device over a wire in 3 (16.7%), acute angle of aortic bifurcation in 2 (11.1%), mechanical failure of the device in 1 (5.6%), and difficulty tracking the device through the lesion in 1 (5.6%). Moderate or severe calcification at the site of re-entry was the only significant predictor of failure (odds ratio, 6.3; 95% confidence interval, ; P.01). An aortic bifurcation angle >40 did trend toward predicting success (odds ratio, 0.23; 95% confidence interval, ; P.054). Conclusions: Although the Outback re-entry device can be successful in extending the applicability of endovascular management to difficult femoropopliteal occlusions, it is not uniformly successful in current clinical practice. Significant calcification at the proposed re-entry site is a strong predictor of failure. (J Vasc Surg 2011;53: ) Subintimal angioplasty with recanalization of chronic total occlusions (CTOs) is the accepted first-line therapy for TransAtlantic InterSociety Consensus (TASC) II B and C lesions in the femoropopliteal location. Subintimal angioplasty, first described by Bolia et al, 1 is performed by creating entry into the subintimal plane using hydrophilic wires and crossing catheters and then establishing re-entry into the true lumen with similar wire and catheter techniques. The primary limitation of this technique is true lumen re-entry distal to the occluded segment, with reported failure rates of 16.5% to 26%. In addition, conventional re-entry techniques may be possible but only distal to the vessel reconstitution point, leading to the sacrifice of significant collateral vessels. 2,3 These difficulties with re-entry have prompted the introduction of re-entry devices such as the Pioneer catheter From the Division of Vascular Surgery, University of Pittsburgh Medical Center. Competition of interest: none. Presented at the Thirty-eighth Annual Symposium of the Society of Clinical Vascular Surgery, Scottsdale, Ariz, April 8-11, Reprint requests: Susanna Shin, MD, UPP Vascular Surgery, UPMC Presbyterian, 200 Lothrop St, A-1017, Pittsburgh, Pa ( shins@upmc.edu). The editors and reviewers of this article have no relevant financial relationships to disclose per the JVS policy that requires reviewers to decline review of any manuscript for which they may have a competition of interest /$36.00 Copyright 2011 by the Society for Vascular Surgery. doi: /j.jvs (Medtronic Inc, Minneapolis, Minn) and the Outback LTD catheter (LuMend, Redwood City, Calif [acquired by Cordis Corp, Miami Lakes, Fla]). The Pioneer catheter uses intravascular ultrasound to guide a retractable curved nitinol needle into the true lumen. The Outback catheter uses 2-dimensional fluoroscopy to guide a retractable curved nitinol needle into the true lumen. Previous studies have shown variable success of 50% to 100% with these re-entry devices in the treatment of infrainguinal CTOs. 2-7 Previous reports indicate the primary limitation of these devices is heavy calcification at the proposed site of true lumen re-entry; however, these were small series that included various vascular beds. 2,6,7 In this study, we examined the success and the predictors of failure of using the Outback LTD device in CTOs of the femoropopliteal segment that have failed conventional re-entry techniques. METHODS Institutional Review Board approval was obtained for human research for this study from the University of Pittsburgh Medical Center. All procedures described in this series were performed by or under the supervision of attending vascular surgeons at the University of Pittsburgh Medical Center. Patient selection. A retrospective review of a prospectively maintained database identified 249 patients with femoropopliteal CTOs treated endoluminally with subinti-
2 JOURNAL OF VASCULAR SURGERY Volume 53, Number 5 Shin et al 1261 Fig 1. Calcification scoring system. mal angioplasty, with and selective stenting, by our group from August 1, 2006, to August 31, Some patients in whom subintimal recanalization was attempted but unsuccessful were not included in this database and were lost to analysis in this study. This cohort included patients with prohibitive surgical risk undergoing intervention for critical limb ischemia (CLI) as well as patients being offered endovascular therapy as a primary modality in the treatment of CLI or intermittent claudication. From this series, we identified 52 procedures in which the Outback LTD reentry catheter was used. Data collected included basic demographic data (age, gender) and details about the lesion, including location, length of occlusion, distal reconstitution site, and the 2007 TASC II classification. Technique. All interventions were performed using fixed imaging in a dedicated angiography suite or hybrid operating room under conscious sedation with local 1% lidocaine anesthesia. Our preferred method of subintimal recanalization was through percutaneous access from a contralateral retrograde common femoral artery puncture. Deviation from this approach occurred when the anatomy was not amenable, and in such cases, an antegrade ipsilateral approach was used or puncture of a femoral-femoral bypass graft was performed. All interventions were performed with systemic heparinization and the support of a 6F or 7F sheath ( up and over technique with contralateral approach). Initial subintimal recanalization was performed with a inch hydrophilic wire and a 4F or 5F hydrophilic catheter. If entry into the subintimal space was achieved using this technique but re-entry into the true lumen was not possible using multiple conventional re-entry maneuvers, then the attending vascular surgeon considered using the Outback LTD re-entry catheter (Fig 1). The crossing catheter was left in the subintimal space and the inch hydrophilic wire was exchanged for a inch Spartacore guidewire (Guidant, Temecula, Calif). The Outback catheter was then placed over the Spartacore wire. Using fluoroscopy and road map imaging, the Outback catheter was oriented with the needle positioned toward the lumen distal to the occlusion. This involves imaging at two separate angles. Initially, the catheter was located parallel to the vessel with the radiopaque marker oriented as an L toward the lumen. The image intensifier was then rotated 90 orthogonally and the radiopaque marker was simultaneously oriented as a T over the center of the flow lumen. The needle was then deployed and the guidewire advanced through the needle. The Outback catheter was removed and angioplasty was performed, with self-expanding stents placed when residual stenosis was 30% or flow-limiting dissection was identified. All re-entry attempts made with the Outback LTD catheter were performed at the most proximal vessel reconstitution point in an attempt to preserve chronic collateral perfusion. Procedural details (wires, catheters and sheaths used, success of device, site of re-entry, reason for failure) were recorded from the procedure dictation. Anatomic details were assessed based on review of the procedural angiogram. The aortic bifurcation angle (ABA) was measured from the aortogram (abdominal and pelvic) using a built-in tool on the imaging software at our institution that allows the accurate measure of angles. The ABA was measured in the anterior-posterior view of the aortogram. An aortic bifurcation angle 40 was considered acute. Calcification at the region of the site of re-entry was considered because it might represent an obstacle to re-entry. Calcification at other sites of the artery was not considered in the analysis. The degree of calcification at the site of re-entry was estimated by a single observer using angiographic images based on the presence of calcification on no side, one side, both sides of the artery, or circumferentially (Table I and
3 1262 Shin et al JOURNAL OF VASCULAR SURGERY May 2011 Table I. Calcification scoring system Score None Mild Moderate Severe Angiographic findings No calcification visible Calcification visible only on one side of the vessel Calcification visible on both (lumen) sides of the vessel with lucent center Calcification visible on both center (lumen) sides of the vessel without lucent Fig 2). The aortic bifurcation angle and calcification for each patient was measured or estimated before categorization as success or failure of the Outback device. Statistics. Statistical analysis was performed by an independent statistician using SAS 9.2 software (SAS Institute Inc, Cary, NC). Continuous variables were compared using the t test, and categoric variables were compared using the 2 or Fisher exact test. Logistic regression was used to model the association of variables with treatment failure. Odds ratios (ORs) are presented with 95% confidence intervals (CIs). Statistical significance was defined with a value of P.05. RESULTS Infrainguinal recanalizations. From August 1, 2006, to August 31, 2009, 249 infrainguinal CTOs were treated with endoluminal techniques. Of these, 249 femoropopliteal lesions, 37.8% were TASC II C lesions and the rest were D lesions. Patients (52.4% men) were a mean age of 72.2 years. Outback catheter. The Outback re-entry catheter was used in 52 limbs in 50 patients after traditional wire and catheter techniques failed to allow re-entry into the true lumen. A total of 47 superficial femoral artery (SFA) occlusions and 5 combined SFA and popliteal artery occlusions were treated (33 were TASC II C and 18 were TASC II D lesions). The mean patient age was 73.1 years, and 54.0% were men. The mean lesion length was 17.6 cm. True lumen re-entry with the Outback catheter was successful in 34 limbs (64.5%; Table II). The site of re-entry (attempted or successful) was most commonly the adductor canal (61.7%). Other sites included the above-knee popliteal artery (25.5%), directly behind the knee joint (8.5%), and the mid-sfa (4.3%). The mean ABA was 42.8 (range, ). Overall, 29 ABAs (63.0%) were not acute. An ABA 40 trended toward being significant as a negative predictor of failure (protective factor) of the device (OR, 0.23; 95% CI, ; P.054). Outback catheter failures. Moderate or severe calcification at the site of re-entry was the only significant predictor of failure (OR, 6.3; 95% CI, ; P.01). The most common reason for failure was inability to re-enter the true lumen, accounting for 11 failures (61.1%). In this subgroup as well, moderate or severe calcification at the attempted site of re-entry was a significant predictor of failure (OR, 7.5; 95% CI, ; P.03). Additional reasons for failure included 3 cases (16.7%) of difficulty Fig 2. When Outback LTD re-entry catheter was considered for use, the crossing catheter was left in the subintimal space and the inch hydrophilic wire was exchanged for a inch Spartacore guidewire (Guidant, Temecula, Calif) and placed over the Spartacore wire. Using fluoroscopy and road map imaging, the Outback catheter is oriented with the needle positioned toward the lumen distal to the occlusion. This involves imaging at 2 separate angles. Initially, the catheter is located parallel to the vessel with the radiopaque marker oriented as an L toward the lumen. The image intensifier is then rotated 90 degrees orthogonally and the radiopaque marker is simultaneously oriented as a T over the center of the flow lumen. The needle is then deployed and the guidewire advanced through the needle. The Outback catheter is then removed and angioplasty performed with self-expanding stents placed when residual stenosis was 30% or flow-limiting dissection was identified.
4 JOURNAL OF VASCULAR SURGERY Volume 53, Number 5 Shin et al 1263 Table II. Characteristics of patients and lesions treated with Outback LTD re-entry catheter Variable Successful Failure P (n 34) (n 18) Age, mean y Male, No. (%) 16 (47.1) 11 (61.1).39 TASC II C, No. (%) 21 (63.6) 11 (61.1).99 TASC II D, No. (%) 12 (36.3) 7 (38.9) Lesion length, mean mm Calcification, No. (%) None/mild 29 (85.3) 10 (55.6).04 Moderate/severe 5 (14.7) 8 (44.4) Aortic bifurcation angle TASC, TransAtlantic InterSociety Consensus. tracking the catheter over a wire related to wire friction and tortuosity, 2 cases of acute angle of aortic bifurcation (11.1%) that resulted in failure of device delivery to the re-entry site, 1 mechanical failure (5.6%), and 1 case of difficulty tracking the catheter through the lesion (5.6%). The mean ABA in the entire failure subgroup was 39.8 (range, ). Ten patients in the failure cohort (58.8%) did have an acute ABA. One technical malfunction occurred with the needle device, and the needle would not deploy. Complications. In three cases, the Outback catheter created an arteriovenous fistula, but no intervention was performed and no adverse sequelae resulted from this complication. No distal embolization occurred as a result of the intervention. This was documented with a completion angiogram at the conclusion of the case, which is standard protocol for these procedures. No bleeding related to Outback LTD needle puncture was identified. One extravascular revascularization occurred; in this case, the subintimal crossing inadvertently entered the subsartorial space by rupturing the adventitia, and successful true lumen re-entry was established with the Outback LTD. This was not recognized at the time of the original procedure. A substantial subsartorial pseudoaneurysm was identified 1 week after the initial procedure and was treated successfully with placement of a Viabahn stent graft (W L Gore and Assoc, Flagstaff, Ariz), thus creating a percutaneous extravascular bypass. 8 DISCUSSION Endovascular therapy is regarded as the first-line procedural treatment for patients with symptomatic TASC II A, B, and C femoropopliteal lesions. In addition, these techniques are increasingly applied in the treatment of patients of high surgical risk with TASC II D lesions and CLI. During the last decade, periprocedural failure rates have been diminished with the use of nitinol stent technology, 9 and new developments in the area of debulking and drug elution may improve long-term outcomes. The Outback LTD was developed to overcome procedural failures and improve treatment success after subintimal passage through a CTO. This series describes the use of the Outback LTD re-entry catheter in the treatment of femoropopliteal CTOs where re-entry could not be established with conventional wire and catheter techniques. Approximately one-fifth of infrainguinal subintimal recanalizations fail because of failure to re-enter the true lumen distal to the CTO. 2,3 In our series, a re-entry device was required in 20.9% of femoropopliteal CTO cases. Technologic advances such as the Outback LTD re-entry device have been designed specifically to overcome this well-known limitation. Previous reports have cited variable success rates with currently available re-entry devices. At our institution using a single device in an isolated vascular territory, we report an overall success rate of 64.5%. The use of a re-entry device can substantially increase the overall technical success rates in the treatment of CTOs. Only four complications occurred as a result of the Outback LTD catheter, three were arteriovenous fistulas that were not clinically significant and resulted in no adverse sequelae. One resulted in extravascular revascularization of the femoropopliteal lesion and has been reported independently. 8 Similar to other reports, failure to achieve successful endoluminal therapy was most often due to failure of the device to re-enter the true lumen. 2,4-7 The current review has identified heavy calcification at the proposed re-entry site as the primary reason for device failure. In the series from Hausegger et al, 6 two failures (20%) to re-enter the true lumen were attributed to heavy calcification of the artery. Specifically, the investigators described a heavily calcified occlusion that impaired the free rotation of the Outback catheter. In addition, the needle could not be deployed in one of those cases due to the heavy calcification. Similarly, calcification was described as a major factor in the five failures (21%) reported by Setacci et al. 2 The degree of calcification at the site of re-entry was judged by the amount of calcium visible on the procedural angiogram. Specifically, we observed whether calcium was lining the vessel on no side, one side or both sides, or filling the lumen. In the failure cohort of our series, moderate or severe calcification at the re-entry site specifically made success less likely. In one case in our series, the heavily calcified occlusion made it impossible to track the catheter through the subintimal plane adjacent to the calcification even after predilation with balloon angioplasty. In other cases with heavy calcification, the catheter could be directed and oriented appropriately; however, the needle could not penetrate the calcium to achieve re-entry. This is not unexpected, because the needle is a 23-gauge nitinol construct and is easily deflected when deployed in a region with significant calcification. This deflection can inadvertently rotate the device thus changing orientation and resulting in unsuccessful true lumen re-entry. Two failures of subintimal recanalization occurred as a result of an acutely angled aortic bifurcation (37 and 28 ). Angiographic review of these cases revealed significant acute aortic bifurcation with calcification extending into the common iliac arteries, which did not allow for splaying
5 1264 Shin et al JOURNAL OF VASCULAR SURGERY May 2011 of the aortic bifurcation, notwithstanding the use of a stiff inch wire. In these cases, the Outback LTD catheter could not be delivered over the aortic bifurcation despite the use of a larger 7F sheath. This failure to advance over the bifurcation is the result of the stiff nose cone that houses the nitinol re-entry needle. Although not a statistically significant limitation in our review, this technical consideration should be considered before attempted reentry with the Outback LTD catheter. Additional failures of the Outback catheter to aid in re-entry occurred as a technical problem with the actual device. In three cases, difficulty tracking the catheter over the wire related to friction was problematic. In these cases, the catheter tracked easily over the wire initially and reentry was achieved with the aid of the catheter. However, once the wire was advanced into the true lumen at the re-entry point, the catheter became adherent to the wire, and the wire and catheter had to be removed together, thus losing access to the true lumen. The conclusion in these cases was that friction of the wire on the inner hydrophilic catheter coating had resulted in the wire binding to the catheter. One technical malfunction occurred with the needle device and the needle would not deploy. Although no significant learning curve was identified when the success rates of the various device users within the vascular division were examined, this may be another possible contributing factor to failure of re-entry using the Outback LTD catheter. Four of the 50 cases using the Outback LTD catheter represented the lone application of the device by the attending surgeon. In three of these cases, the surgeon was not successful re-entering the true lumen distal to the occlusion. Only three (42.9%) of the seven surgeons using this device were successful on their initial use. The Outback LTD catheter is not a difficult device to use, but it is intuitive that repeated use would increase comfort level and success rate with the device. The primary limitations of this study are inherent to those of retrospective design and small sample size. In addition, the series included operators with various levels of experience with the device. The small sample size coupled with large number of operators may have concealed a significant learning curve. Another limitation brought on by the retrospective design was our method of grading the calcification at the re-entry site using procedural angiograms. Plain angiography is inferior to computed tomography angiography as a modality of imaging to grade calcification. In our practice, however, computed tomography angiography is not routinely used before intervention because it adds expense, radiation exposure, and contrast toxicity. CONCLUSIONS Although the Outback LTD re-entry catheter can be successful in extending the applicability of endovascular management to difficult femoropopliteal occlusions, when conventional methods of lumen re-entry fail, it is not uniformly successful in current clinical practice. However, the Outback LTD catheter is safe in the femoropopliteal location. Significant calcification at the proposed re-entry site is a strong predictor of device failure. AUTHOR CONTRIBUTIONS Conception and design: SS, DB, RC, MM, RR, LM Analysis and interpretation: SS, LM Data collection: SS, DB Writing the article: SS, LM Critical revision of the article: SS, DB, RC, MM, RR, LM Final approval of the article: SS, DB, RC, MM, RR, LM Statistical analysis: SS Obtained funding: Not applicable Overall responsibility: SS REFERENCES 1. Bolia A, Miles KA, Brennan J, Bell PR. Percutaneous transluminal angioplasty of occlusions of the femoral and popliteal arteries by subintimal dissection. Cardiovasc Intervent Radiol 1990;13: Setacci C, Chisci E, de Donato G, Setacci F, Iacoponi F, Galzerano G. Subintimal angioplasty with the aid of a re-entry device for TASC C and D lesions of the SFA. Eur J Vasc Endovasc Surg 2009;38: Jacobs DL, Motaganahalli RL, Cox DE, Wittgen CM, Peterson GJ. True lumen re-entry devices facilitate subintimal angioplasty and stenting of total chronic occlusions: Initial report. J Vasc Surg 2006;43: Al-Ameri H, Shin V, Mayeda GS, Burstein S, Matthews RV, Kloner RA, et al. Peripheral chronic total occlusions treated with subintimal angioplasty and a true lumen re-entry device. J Invasive Cardiol 2009;21: Husmann M, Federer J, Keo HH, Schmidli J, Kickuth R, Baumgartner I, et al. Bailout revascularization of chronic femoral artery occlusions with the new outback catheter following failed conventional endovascular intervention. J Endovasc Ther 2009;16: Hausegger KA, Georgieva B, Portugaller H, Tauss J, Stark G. The outback catheter: a new device for true lumen re-entry after dissection during recanalization of arterial occlusions. Cardiovasc Intervent Radiol 2004;27: Wiesinger B, Steinkamp H, Konig C, Tepe G, Duda SH. Technical report and preliminary clinical data of a novel catheter for luminal re-entry after subintimal dissection. Invest Radiol 2005;40: Wagner JK, Chaer RA, Rhee RY, Marone LK. True lumen re-entry after extravascular recanalization of a superficial femoral artery chronic total occlusion. J Vasc Surg. 2010;52: Schillinger M, Sabeti S, Loewe C, Dick P, Amighi J, Mlekusch W, et al. Balloon angioplasty versus implantation of nitinol stents in the superficial femoral artery. N Engl J Med 2006;354: Submitted Jul 11, 2010; accepted Oct 29, 2010.
Below-the-knee (BTK) targeted re-entry using the Outback catheter in subintimal angioplasty: Success rate and complications
 Below-the-knee (BTK) targeted re-entry using the Outback catheter in subintimal angioplasty: Success rate and complications Poster No.: C-0734 Congress: ECR 2016 Type: Scientific Exhibit Authors: S. M.
Below-the-knee (BTK) targeted re-entry using the Outback catheter in subintimal angioplasty: Success rate and complications Poster No.: C-0734 Congress: ECR 2016 Type: Scientific Exhibit Authors: S. M.
Case Report pissn / eissn J Korean Soc Radiol 2016;74(1):
 Case Report pissn 1738-2637 / eissn 2288-2928 http://dx.doi.org/10.3348/jksr.2016.74.1.37 Target Balloon-Assisted Antegrade and Retrograde Approach for Recanalization of Thrombosed Fem-Pop Bypass Graft
Case Report pissn 1738-2637 / eissn 2288-2928 http://dx.doi.org/10.3348/jksr.2016.74.1.37 Target Balloon-Assisted Antegrade and Retrograde Approach for Recanalization of Thrombosed Fem-Pop Bypass Graft
True lumen re-entry devices facilitate subintimal angioplasty and stenting of total chronic occlusions: Initial report
 TECHNICAL NOTE True lumen re-entry devices facilitate subintimal angioplasty and stenting of total chronic occlusions: Initial report Donald L. Jacobs, MD, Raghunandan L. Motaganahalli, MD, Daniel E. Cox,
TECHNICAL NOTE True lumen re-entry devices facilitate subintimal angioplasty and stenting of total chronic occlusions: Initial report Donald L. Jacobs, MD, Raghunandan L. Motaganahalli, MD, Daniel E. Cox,
Bailout revascularization of chronic femoral artery occlusions with the new outback catheter following failed conventional endovascular intervention
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2009 Bailout revascularization of chronic femoral artery occlusions with the
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2009 Bailout revascularization of chronic femoral artery occlusions with the
Lessons for Successful Subintimal Angioplasty in SFA CTO
 Lessons for Successful Subintimal Angioplasty in SFA CTO John R. Laird Professor of Medicine Medical Director of the Vascular Center UC Davis Medical Center CTOs in the Periphery Presence of Total Occlusion
Lessons for Successful Subintimal Angioplasty in SFA CTO John R. Laird Professor of Medicine Medical Director of the Vascular Center UC Davis Medical Center CTOs in the Periphery Presence of Total Occlusion
Annals of Vascular Diseases Advance Published Date: June 2, Horie K, et al.
 2016 Annals of Vascular Diseases doi:10.3400/avd.cr.16-00007 Case Report Recanalization of a Heavily Calcified Chronic Total Occlusion in a Femoropopliteal Artery Using a Wingman Crossing Catheter Kazunori
2016 Annals of Vascular Diseases doi:10.3400/avd.cr.16-00007 Case Report Recanalization of a Heavily Calcified Chronic Total Occlusion in a Femoropopliteal Artery Using a Wingman Crossing Catheter Kazunori
Copyright HMP Communications
 Ocelot With Wildcat in a Complicated Superficial Femoral Artery Chronic Total Occlusion Soundos K. Moualla, MD, FACC, FSCAI; Richard R. Heuser, MD, FACC, FACP, FESC, FSCAI From Phoenix Heart Center, Phoenix,
Ocelot With Wildcat in a Complicated Superficial Femoral Artery Chronic Total Occlusion Soundos K. Moualla, MD, FACC, FSCAI; Richard R. Heuser, MD, FACC, FACP, FESC, FSCAI From Phoenix Heart Center, Phoenix,
Re-entry into the true lumen from the subintimal space
 VASCULAR AND ENDOVASCULAR TECHNIQUES Peter F. Lawrence, MD, Section Editor Re-entry into the true lumen from the subintimal space Peter A. Schneider, MD, Michael T. Caps, MD, MPH, and Nicolas Nelken, MD,
VASCULAR AND ENDOVASCULAR TECHNIQUES Peter F. Lawrence, MD, Section Editor Re-entry into the true lumen from the subintimal space Peter A. Schneider, MD, Michael T. Caps, MD, MPH, and Nicolas Nelken, MD,
Chronic Total Occlusion (CTO) Technologies
 to receive our latest news and key activities. Chronic Total Occlusion (CTO) Technologies Re-open vital channels LinkedIn page Follow us on CORDIS EMEA OUTBACK LTD Re-Entry Catheter True Lumen Re-Entry
to receive our latest news and key activities. Chronic Total Occlusion (CTO) Technologies Re-open vital channels LinkedIn page Follow us on CORDIS EMEA OUTBACK LTD Re-Entry Catheter True Lumen Re-Entry
Endovascular Repair of Combined Occluded Femoral and Popliteal Arteries
 MEET 2013 Endovascular Repair of Combined Occluded Femoral and Popliteal Arteries ALI AMIN MD, FACS,FACC, RVT CHIEF OF ENDOVASCULAR INTERVENTIONS READING HOSPITAL AND MEDICAL CENTER READING, PA USA Chronic
MEET 2013 Endovascular Repair of Combined Occluded Femoral and Popliteal Arteries ALI AMIN MD, FACS,FACC, RVT CHIEF OF ENDOVASCULAR INTERVENTIONS READING HOSPITAL AND MEDICAL CENTER READING, PA USA Chronic
Endovascular intervention for patients with femoro-popliteal and aorto-iliac TASC D lesions
 Endovascular intervention for patients with femoro-popliteal and aorto-iliac TASC D lesions Poster No.: C-2012 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Thomee, W. C. Liong, D. R. Warakaulle;
Endovascular intervention for patients with femoro-popliteal and aorto-iliac TASC D lesions Poster No.: C-2012 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Thomee, W. C. Liong, D. R. Warakaulle;
Interventional Cardiology
 r l Interventional Cardiology Intravascular ultrasound findings after knuckle wire technique for superficial femoral artery occlusion Aim: We assessed the wire behavior by using intravascular ultrasound
r l Interventional Cardiology Intravascular ultrasound findings after knuckle wire technique for superficial femoral artery occlusion Aim: We assessed the wire behavior by using intravascular ultrasound
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Utility of Image-Guided Atherectomy for Optimal Treatment of Ambiguous Lesions by Angiography
 Utility of Image-Guided Atherectomy for Optimal Treatment of Ambiguous Lesions by Angiography Jon C. George, MD; Vincent Varghese, DO From the Deborah Heart and Lung Center, Browns Mills, New Jersey. ABSTRACT:
Utility of Image-Guided Atherectomy for Optimal Treatment of Ambiguous Lesions by Angiography Jon C. George, MD; Vincent Varghese, DO From the Deborah Heart and Lung Center, Browns Mills, New Jersey. ABSTRACT:
Chronic Total Occlusion (CTO) Technologies. Re-open vital channels
 Chronic Total Occlusion (CTO) Technologies Re-open vital channels OUTBACK LTD Re-Entry Catheter True Lumen Re-Entry Technology Get back into the true lumen with ease and precision There are a number of
Chronic Total Occlusion (CTO) Technologies Re-open vital channels OUTBACK LTD Re-Entry Catheter True Lumen Re-Entry Technology Get back into the true lumen with ease and precision There are a number of
Endovascular Approach to CTOs: Crossing methods and Devices
 Endovascular Approach to CTOs: Crossing methods and Devices Anish J. Thomas, MD FACC FSCAI Interventional Cardiology Vascular/Endovascular Medicine SSM Heart Institute St. Louis, MO Disclosure Consultant:
Endovascular Approach to CTOs: Crossing methods and Devices Anish J. Thomas, MD FACC FSCAI Interventional Cardiology Vascular/Endovascular Medicine SSM Heart Institute St. Louis, MO Disclosure Consultant:
Endovascular Treatment of Aortoiliac Occlusive Disease: What s in My Toolbox in Jade S. Hiramoto, MD, MAS UCSF Vascular Symposium April 20, 2018
 Endovascular Treatment of Aortoiliac Occlusive Disease: What s in My Toolbox in 2018 Jade S. Hiramoto, MD, MAS UCSF Vascular Symposium April 20, 2018 Disclosures Research support and royalties, Cook Inc.
Endovascular Treatment of Aortoiliac Occlusive Disease: What s in My Toolbox in 2018 Jade S. Hiramoto, MD, MAS UCSF Vascular Symposium April 20, 2018 Disclosures Research support and royalties, Cook Inc.
Can t See the Forest for the Trees: Transcollateral Crossing of Chronic Total Occlusions
 Can t See the Forest for the Trees: Transcollateral Crossing of Chronic Total Occlusions Vinayak Subramanian, BS 1 ; George L. Adams, MD, MHS 2 From 1 Department of Biomedical Engineering, North Carolina
Can t See the Forest for the Trees: Transcollateral Crossing of Chronic Total Occlusions Vinayak Subramanian, BS 1 ; George L. Adams, MD, MHS 2 From 1 Department of Biomedical Engineering, North Carolina
Access strategy for chronic total occlusions (CTOs) is crucial
 Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
Step by step Hybrid procedures in peripheral obstructive disease. Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery
 Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Chronic total occlusions (CTOs) are frequently
 Specialty Crossing Devices: Understanding the Learning Curve Technical pearls and new devices for crossing peripheral CTOs. y Usman Javed, MD, and John R. Laird, MD (Courtesy of ard Peripheral Vascular,
Specialty Crossing Devices: Understanding the Learning Curve Technical pearls and new devices for crossing peripheral CTOs. y Usman Javed, MD, and John R. Laird, MD (Courtesy of ard Peripheral Vascular,
Disclosures. Tips and Tricks for Tibial Intervention. Tibial intervention overview
 Tips and Tricks for Tibial Intervention Donald L. Jacobs, MD C Rollins Hanlon Endowed Professor and Chair Chair of Surgery Saint Louis University SSM-STL Saint Louis University Hospital Disclosures Abbott
Tips and Tricks for Tibial Intervention Donald L. Jacobs, MD C Rollins Hanlon Endowed Professor and Chair Chair of Surgery Saint Louis University SSM-STL Saint Louis University Hospital Disclosures Abbott
Current Status and Limitations in the Treatment of Femoropopliteal In-Stent Restenosis
 Current Status and Limitations in the Treatment of Femoropopliteal In-Stent Restenosis Osamu Iida, MD From the Kansai Rosai Hospital Cardiovascular Center, Amagasaki City, Japan. ABSTRACT: Approximately
Current Status and Limitations in the Treatment of Femoropopliteal In-Stent Restenosis Osamu Iida, MD From the Kansai Rosai Hospital Cardiovascular Center, Amagasaki City, Japan. ABSTRACT: Approximately
Turbo-Power. Laser atherectomy catheter. The standard. for ISR
 Turbo-Power Laser atherectomy catheter The standard for ISR Vaporize the ISR challenge In-stent restenosis (ISR) Chance of recurring 7 115,000 + /year (U.S.) 1-6 Repeated narrowing of the arteries after
Turbo-Power Laser atherectomy catheter The standard for ISR Vaporize the ISR challenge In-stent restenosis (ISR) Chance of recurring 7 115,000 + /year (U.S.) 1-6 Repeated narrowing of the arteries after
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
There are multiple endovascular options for treatment
 Peripheral Rotablator Atherectomy: The Below-the-Knee Approach to Address Calcium Head On Peripheral Rotablator s front-cutting, diamond-tipped burr provides stable rotation in calcified lesions. BY SONYA
Peripheral Rotablator Atherectomy: The Below-the-Knee Approach to Address Calcium Head On Peripheral Rotablator s front-cutting, diamond-tipped burr provides stable rotation in calcified lesions. BY SONYA
Hybrid Procedures for Peripheral Obstructive Disease - Step by Step -
 Hybrid Procedures for Peripheral Obstructive Disease - Step by Step - Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name:..holger Staab... I have
Hybrid Procedures for Peripheral Obstructive Disease - Step by Step - Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name:..holger Staab... I have
Page 2 of 9
 OUTBACK LTD re-entry catheter in subintimal superficial femoral artery CTO revascularization: Preliminary data about procedure time, radioscopy time and precision in targeting the expected re-entry site
OUTBACK LTD re-entry catheter in subintimal superficial femoral artery CTO revascularization: Preliminary data about procedure time, radioscopy time and precision in targeting the expected re-entry site
9/7/2018. Disclosures. CV and Limb Events in PAD. Challenges to Revascularization. Challenges. Answering the Challenge
 Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
Peripheral Arterial Disease: A Practical Approach
 Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Plaque Excision Infrainguinal PAD An update on this nonstenting alternative, with intermediate-term results of the ongoing TALON Registry.
 Plaque Excision Treatment of Infrainguinal PAD An update on this nonstenting alternative, with intermediate-term results of the ongoing TALON Registry. BY ROGER GAMMON, MD Despite surgical options and
Plaque Excision Treatment of Infrainguinal PAD An update on this nonstenting alternative, with intermediate-term results of the ongoing TALON Registry. BY ROGER GAMMON, MD Despite surgical options and
Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases
 Original paper Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases Sakir Arslan, Isa Oner Yuksel, Erkan Koklu, Goksel
Original paper Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases Sakir Arslan, Isa Oner Yuksel, Erkan Koklu, Goksel
Challenging of contrast agent-free endovascular treatment using 3D imaging
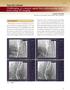 AC17-0010 Challenging of contrast agent-free endovascular treatment using 3D imaging Amane Kozuki Department of Cardiology, Osaka Saiseikai Nakatsu Hospital Introduction With advances in devices and techniques,
AC17-0010 Challenging of contrast agent-free endovascular treatment using 3D imaging Amane Kozuki Department of Cardiology, Osaka Saiseikai Nakatsu Hospital Introduction With advances in devices and techniques,
Outcomes of endovascular treatment for patients with TASC II D femoropopliteal occlusive disease: a single center study
 BMC Cardiovascular Disorders This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Outcomes of endovascular
BMC Cardiovascular Disorders This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Outcomes of endovascular
Pocket Reference Guide For (CTO) Technologies
 to receive our latest news and key activities. Pocket Reference Guide For (CTO) Technologies LinkedIn page Follow us on CORDIS EMEA Table of Contents Essential prescribing information for both FRONTRUNNER
to receive our latest news and key activities. Pocket Reference Guide For (CTO) Technologies LinkedIn page Follow us on CORDIS EMEA Table of Contents Essential prescribing information for both FRONTRUNNER
Appropriate Device Selection for Endovascular Procedures
 Appropriate Device Selection for Endovascular Procedures Thomas M. Shimshak, MD Florida Hospital Heartland Medical Center Sebring, Florida Disclosures Speaker s Bureau: Abbott Vascular Boston Scientific
Appropriate Device Selection for Endovascular Procedures Thomas M. Shimshak, MD Florida Hospital Heartland Medical Center Sebring, Florida Disclosures Speaker s Bureau: Abbott Vascular Boston Scientific
Retrograde dorsalis pedis and posterior tibial artery access after failed antegrade angioplasty
 Retrograde dorsalis pedis and posterior tibial artery access after failed antegrade angioplasty Poster No.: C-2067 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit Interventional
Retrograde dorsalis pedis and posterior tibial artery access after failed antegrade angioplasty Poster No.: C-2067 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit Interventional
The femoropopliteal (FP) artery refers to the composite
 The Role of Atherectomy in the Femoropopliteal Artery With the growing number of tools for femoropopliteal artery intervention, what is the role of atherectomy in the endovascular treatment of femoropopliteal
The Role of Atherectomy in the Femoropopliteal Artery With the growing number of tools for femoropopliteal artery intervention, what is the role of atherectomy in the endovascular treatment of femoropopliteal
PATIENT SPECIFIC STRATEGIES IN CRITICAL LIMB ISCHEMIA. Dr. Manar Trab Consultant Vascular Surgeon European Vascular Clinic DMCC Dubai, UAE
 PATIENT SPECIFIC STRATEGIES IN CRITICAL LIMB ISCHEMIA Dr. Manar Trab Consultant Vascular Surgeon European Vascular Clinic DMCC Dubai, UAE Disclosure Speaker name: DR. Manar Trab I have the following potential
PATIENT SPECIFIC STRATEGIES IN CRITICAL LIMB ISCHEMIA Dr. Manar Trab Consultant Vascular Surgeon European Vascular Clinic DMCC Dubai, UAE Disclosure Speaker name: DR. Manar Trab I have the following potential
UC SF. Introduction: Retrograde Access. Pedal Access: When to Do It How Does it Fare. Introduction: Retrograde Access. Introduction: Retrograde Access
 Introduction: Retrograde Access Pedal Access: When to Do It How Does it Fare Wide spread application of endovascular techniques to infrageniculate arterial occlusive disease Technical failure rate of crossing
Introduction: Retrograde Access Pedal Access: When to Do It How Does it Fare Wide spread application of endovascular techniques to infrageniculate arterial occlusive disease Technical failure rate of crossing
Clinical Data Update for Drug Coated Balloons (DCB) Seung-Whan Lee, MD, PhD
 Clinical Data Update for Drug Coated Balloons (DCB) Seung-Whan Lee, MD, PhD Asan Medical Center, Heart Institute, University of Ulsan College of Medicine, Werk et al. Circulation Cardiovasc Intervent 2012
Clinical Data Update for Drug Coated Balloons (DCB) Seung-Whan Lee, MD, PhD Asan Medical Center, Heart Institute, University of Ulsan College of Medicine, Werk et al. Circulation Cardiovasc Intervent 2012
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease
 Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
The Crack and Pave technique for highly resistant calcified lesions. Manuela Matschuck MD University Hospital Leipzig Department Angiology
 The Crack and Pave technique for highly resistant calcified lesions Manuela Matschuck MD University Hospital Leipzig Department Angiology Disclosure Speaker name: Dr. med. Manuela Matschuck I have the
The Crack and Pave technique for highly resistant calcified lesions Manuela Matschuck MD University Hospital Leipzig Department Angiology Disclosure Speaker name: Dr. med. Manuela Matschuck I have the
For Personal Use. Copyright HMP 2013 J INVASIVE CARDIOL 2013;25(5):E96-E100
 Case Report and Brief Review Transcollateral Approach for Percutaneous Revascularization of Complex Superficial Femoral Artery Chronic Total Occlusion Zaheed Tai, DO ABSTRACT: Chronic total occlusions
Case Report and Brief Review Transcollateral Approach for Percutaneous Revascularization of Complex Superficial Femoral Artery Chronic Total Occlusion Zaheed Tai, DO ABSTRACT: Chronic total occlusions
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
2009 BUYER S GUIDE BY JOHN H. RUNDBACK, MD, AND LUIS RODRIGUEZ, JR, MD
 Interventional Strategies for Atherosclerotic Disease A review of the limitations and therapeutic options available for treating this challenging segment. BY JOHN H. RUNDBACK, MD, AND LUIS RODRIGUEZ, JR,
Interventional Strategies for Atherosclerotic Disease A review of the limitations and therapeutic options available for treating this challenging segment. BY JOHN H. RUNDBACK, MD, AND LUIS RODRIGUEZ, JR,
ENDOVASCULAR TREATMENT OF SFA
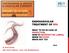 ENDOVASCULAR TREATMENT OF SFA WHAT TO DO IN CASE OF DISSECTION, HOW TO REENTER THE LUMEN, WHEN TO STENT, WHEN NOT TO? E.DUCASSE MD PHD FEBVS, CHU DE BORDEAUX 2018 ENDOVASCULAR TTT OF SFA NOWDAYS PTA first
ENDOVASCULAR TREATMENT OF SFA WHAT TO DO IN CASE OF DISSECTION, HOW TO REENTER THE LUMEN, WHEN TO STENT, WHEN NOT TO? E.DUCASSE MD PHD FEBVS, CHU DE BORDEAUX 2018 ENDOVASCULAR TTT OF SFA NOWDAYS PTA first
Superficial Femoral Artery Intervention: The gift that keeps on giving! Wm. Britton Eaves,MD WKHSC Bossier City, LA
 : The gift that keeps on giving! Wm. Britton Eaves,MD WKHSC Bossier City, LA Peripheral arterial disease (PAD) of the superficial femoral artery (SFA) is the most common cause of intermittent claudication
: The gift that keeps on giving! Wm. Britton Eaves,MD WKHSC Bossier City, LA Peripheral arterial disease (PAD) of the superficial femoral artery (SFA) is the most common cause of intermittent claudication
Robert W. Fincher, DO The Ritz-Carlton, Dove Mountain Marana, Arizona February 7th, 2015
 Robert W. Fincher, DO The Ritz-Carlton, Dove Mountain Marana, Arizona February 7th, 2015 Disclosure I have nothing to disclose Randomized Controlled Studies In SFA Technology: What s The Best Tool For
Robert W. Fincher, DO The Ritz-Carlton, Dove Mountain Marana, Arizona February 7th, 2015 Disclosure I have nothing to disclose Randomized Controlled Studies In SFA Technology: What s The Best Tool For
Advance Publication Journal of Atherosclerosis and Thrombosis. Accepted for publication: March 23, Published online: May 17, 2017
 Original Article Advance Publication J Atheroscler Thromb, 2017; 24: 000-000. http://doi.org/10.5551/jat.40048 Comparison of the OUTBACK Elite Reentry Catheter and the Bi-directional Approach after Failed
Original Article Advance Publication J Atheroscler Thromb, 2017; 24: 000-000. http://doi.org/10.5551/jat.40048 Comparison of the OUTBACK Elite Reentry Catheter and the Bi-directional Approach after Failed
Novel distal popliteal artery puncture technique in supine position for chronic femoropopliteal arterial occlusion; frontal popliteal puncture
 Novel distal popliteal artery puncture technique in supine position for chronic femoropopliteal arterial occlusion; frontal popliteal puncture Miyazaki Medical Association Hospital Cardiovascular Center
Novel distal popliteal artery puncture technique in supine position for chronic femoropopliteal arterial occlusion; frontal popliteal puncture Miyazaki Medical Association Hospital Cardiovascular Center
CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION
 CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION ARMANDO MANSILHA MD, PhD, FEBVS UNIVERSITY HOSPITAL - PORTO Disclosure of Interest Speaker name: ARMANDO MANSILHA I have the following potential conflicts
CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION ARMANDO MANSILHA MD, PhD, FEBVS UNIVERSITY HOSPITAL - PORTO Disclosure of Interest Speaker name: ARMANDO MANSILHA I have the following potential conflicts
The Utility of Atherectomy and the Jetstream Atherectomy System
 The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E39-E41 A Case With Successful Retrograde Stent Delivery via AC Branch for Tortuous Right Coronary Artery Yoshiki Uehara, MD, PhD, Mitsuyuki Shimizu, MD, PhD,
Case Report J INVASIVE CARDIOL 2013;25(2):E39-E41 A Case With Successful Retrograde Stent Delivery via AC Branch for Tortuous Right Coronary Artery Yoshiki Uehara, MD, PhD, Mitsuyuki Shimizu, MD, PhD,
FLEXIBLE, BALOON EXPANDABLE
 EARLY RESULTS OF A CLINICAL TRIAL OF FLEXIBLE, BALOON EXPANDABLE COVERED STENT GRAFT IN ILIAC OCCLUSIVE DISEASE Chris LeCroy Coastal Vascular and Interventional Pensacola, Florida Clinical Trial WL GORE
EARLY RESULTS OF A CLINICAL TRIAL OF FLEXIBLE, BALOON EXPANDABLE COVERED STENT GRAFT IN ILIAC OCCLUSIVE DISEASE Chris LeCroy Coastal Vascular and Interventional Pensacola, Florida Clinical Trial WL GORE
Atherectomy with thrombectomy of. Rotarex S : The Leipzig experience
 Atherectomy with thrombectomy of femoropopliteal occlusions with Rotarex S : The Leipzig experience Dr. Bruno Freitas, Prof., MD Department of Interventional Angiology, Universität Leipzig, Germany Santa
Atherectomy with thrombectomy of femoropopliteal occlusions with Rotarex S : The Leipzig experience Dr. Bruno Freitas, Prof., MD Department of Interventional Angiology, Universität Leipzig, Germany Santa
TurboHawk. Plaque Excision System
 TurboHawk Plaque Excision System Twelve-month Patency in Diabetics DIABETICS VS. NON-DIABETICS 12-month Primary Patency (%) Diabetic patients show a more positive response to directional atherectomy than
TurboHawk Plaque Excision System Twelve-month Patency in Diabetics DIABETICS VS. NON-DIABETICS 12-month Primary Patency (%) Diabetic patients show a more positive response to directional atherectomy than
Antegrade techniques for CTO recanalization. Dr. George Karavolias, MD, PhD, FESC, FACC Interventional Cardiologist
 Antegrade techniques for CTO recanalization Dr. George Karavolias, MD, PhD, FESC, FACC Interventional Cardiologist can CTOs be reliably opened by PCI? Meta-Analysis of 18,061 Patients Patel V, J Am Coll
Antegrade techniques for CTO recanalization Dr. George Karavolias, MD, PhD, FESC, FACC Interventional Cardiologist can CTOs be reliably opened by PCI? Meta-Analysis of 18,061 Patients Patel V, J Am Coll
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Access (Antegrade, Retrograde, Pedal)
 Access (Antegrade, Retrograde, Pedal) ARCH St. Louis Craig M. Walker, MD, FACC, FACP Clinical Professor of Medicine Tulane University School of Medicine New Orleans, LA Clinical Professor of Medicine LSU
Access (Antegrade, Retrograde, Pedal) ARCH St. Louis Craig M. Walker, MD, FACC, FACP Clinical Professor of Medicine Tulane University School of Medicine New Orleans, LA Clinical Professor of Medicine LSU
Hydrodynamic boost: a novel re-entry technique in subintimal angioplasty of below-the-knee vessels
 DOI 10.1007/s00330-015-4078-4 VASCULAR-INTERVENTIONAL Hydrodynamic boost: a novel re-entry technique in subintimal angioplasty of below-the-knee vessels Roberto Ferraresi 1 & Meneme Hamade 2 & Vito Gallicchio
DOI 10.1007/s00330-015-4078-4 VASCULAR-INTERVENTIONAL Hydrodynamic boost: a novel re-entry technique in subintimal angioplasty of below-the-knee vessels Roberto Ferraresi 1 & Meneme Hamade 2 & Vito Gallicchio
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
THE NEW ARMENIAN MEDICAL JOURNAL
 THE NEW ARMENIAN MEDICAL JOURNAL Vol.10 (2016), Nо 1, p. 57-62 Clinical Research SHORT-TERM OUTCOMES OF ENDOVASCULAR INTERVENTION OF INFRAINGUINAL ARTERIES IN PATIENTS WITH CRITICAL LIMB ISCHEMIA Sultanyan
THE NEW ARMENIAN MEDICAL JOURNAL Vol.10 (2016), Nо 1, p. 57-62 Clinical Research SHORT-TERM OUTCOMES OF ENDOVASCULAR INTERVENTION OF INFRAINGUINAL ARTERIES IN PATIENTS WITH CRITICAL LIMB ISCHEMIA Sultanyan
Accurate Vessel Sizing Drives Clinical Results. IVUS In the Periphery
 Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Patterns of femoropopliteal recurrence after routine and selective stenting endoluminal therapy
 From the Society for Clinical Vascular Surgery Patterns of femoropopliteal recurrence after routine and selective stenting endoluminal therapy Misaki M. Kiguchi, MD, MBA, a Luke K. Marone, MD, a Rabih
From the Society for Clinical Vascular Surgery Patterns of femoropopliteal recurrence after routine and selective stenting endoluminal therapy Misaki M. Kiguchi, MD, MBA, a Luke K. Marone, MD, a Rabih
Access More Patients. Customize Each Seal.
 Access More. Customize Each Seal. The Least Invasive Path Towards Proven Patency ULTRA LOW PROFILE TO EASE ADVANCEMENT The flexible, ultra-low 12F ID Ovation ix delivery system enables you to navigate
Access More. Customize Each Seal. The Least Invasive Path Towards Proven Patency ULTRA LOW PROFILE TO EASE ADVANCEMENT The flexible, ultra-low 12F ID Ovation ix delivery system enables you to navigate
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Update on Tack Optimized Balloon Angioplasty (TOBA) Below the Knee. Marianne Brodmann, MD Medical University Graz Graz, Austria
 Update on Tack Optimized Balloon Angioplasty (TOBA) Below the Knee Marianne Brodmann, MD Medical University Graz Graz, Austria Critical Limb Ischemia Infrapopliteal arterial disease is a leading source
Update on Tack Optimized Balloon Angioplasty (TOBA) Below the Knee Marianne Brodmann, MD Medical University Graz Graz, Austria Critical Limb Ischemia Infrapopliteal arterial disease is a leading source
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division
 John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
DIFFICULT ACCESS REMAINS A CONTRAINDICATION FOR EVAR APOSTOLOS K. TASSIOPOULOS, MD, FACS PROFESSOR AND CHIEF DIVISION OF VASCULAR SURGERY
 DIFFICULT ACCESS REMAINS A CONTRAINDICATION FOR EVAR APOSTOLOS K. TASSIOPOULOS, MD, FACS PROFESSOR AND CHIEF DIVISION OF VASCULAR SURGERY Disclosures Speaker Bureau: - Medtronic - Cook Medical - Bolton
DIFFICULT ACCESS REMAINS A CONTRAINDICATION FOR EVAR APOSTOLOS K. TASSIOPOULOS, MD, FACS PROFESSOR AND CHIEF DIVISION OF VASCULAR SURGERY Disclosures Speaker Bureau: - Medtronic - Cook Medical - Bolton
New Modalities and Advanced Techniques: The Role of Crossing Devices and Atherectomy
 New Modalities and Advanced Techniques: The Role of Crossing Devices and Atherectomy Satish Gadi, MD FACC FSCAI Interventional Cardiologist, Cardiovascular Institute of the South (CIS) Baton Rouge Clinical
New Modalities and Advanced Techniques: The Role of Crossing Devices and Atherectomy Satish Gadi, MD FACC FSCAI Interventional Cardiologist, Cardiovascular Institute of the South (CIS) Baton Rouge Clinical
Straub Endovascular System &
 Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
Christian Wissgott MD, PhD Assistant Director, Radiology Westküstenkliniken Heide
 2-Year Results Of The Tack Optimized Balloon Angioplasty (TOBA) Trial For Fem- Pop Lesions Demonstrates Safety and Efficacy Of The Tack Endovascular System In Repairing Focal Post-PTA Dissections Christian
2-Year Results Of The Tack Optimized Balloon Angioplasty (TOBA) Trial For Fem- Pop Lesions Demonstrates Safety and Efficacy Of The Tack Endovascular System In Repairing Focal Post-PTA Dissections Christian
Is combination therapy with directional atherectomy followed by DCB the answer to challenges in treating SFA disease?
 Is combination therapy with directional atherectomy followed by DCB the answer to challenges in treating SFA disease? The REALITY trial G. Torsello Münster Disclosure Speaker name: G. Torsello... I have
Is combination therapy with directional atherectomy followed by DCB the answer to challenges in treating SFA disease? The REALITY trial G. Torsello Münster Disclosure Speaker name: G. Torsello... I have
The essentials for BTK procedures: wires, balloons, what else
 A comprehensive approach to diabetic patient Tx The essentials for BTK procedures: wires, balloons, what else Dai-Do Do Clinical and Interventional Angiology Cardiovascular Department Disclosure Speaker
A comprehensive approach to diabetic patient Tx The essentials for BTK procedures: wires, balloons, what else Dai-Do Do Clinical and Interventional Angiology Cardiovascular Department Disclosure Speaker
Ping-Pong Guide Catheter Technique for Retrograde Intervention of a Chronic Total Occlusion Through an Ipsilateral Collateral
 Catheterization and Cardiovascular Interventions 78:395 399 (2011) Case Reports Ping-Pong Guide Catheter Technique for Retrograde Intervention of a Chronic Total Occlusion Through an Ipsilateral Collateral
Catheterization and Cardiovascular Interventions 78:395 399 (2011) Case Reports Ping-Pong Guide Catheter Technique for Retrograde Intervention of a Chronic Total Occlusion Through an Ipsilateral Collateral
Recanalization Techniques: Sharp Needle Recanalization. Recanalization Techniques: Sharp Needle Recanalization
 Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Angiographic dissection pattern and patency outcomes of post balloon angioplasty for SFA lesions -a retrospective multi center analysis-
 Angiographic dissection pattern and patency outcomes of post balloon angioplasty for SFA lesions -a retrospective multi center analysis- Masahiko Fujihara Kishiwada Tokushukai Hospital, Osaka, Japan Disclosure
Angiographic dissection pattern and patency outcomes of post balloon angioplasty for SFA lesions -a retrospective multi center analysis- Masahiko Fujihara Kishiwada Tokushukai Hospital, Osaka, Japan Disclosure
Future Algorithm for Lower Extremity Revascularization: Where Does Vessel Prep Fit?
 Future Algorithm for Lower Extremity Revascularization: Where Does Vessel Prep Fit? John R. Laird Adventist Heart and Vascular Institute St. Helena, CA Disclosure Speaker name: John R. Laird... I have
Future Algorithm for Lower Extremity Revascularization: Where Does Vessel Prep Fit? John R. Laird Adventist Heart and Vascular Institute St. Helena, CA Disclosure Speaker name: John R. Laird... I have
PCI for Chronic Total Occlusions
 PCI for Chronic Total Occlusions Chronic Total Occlusions Why not Medical Treatment? Medical Treatment CTO in 891 pts over 24 years High 10% Mortality Low 2 % 1 year 10 years Puma JA, et al. JACC 1994;23:390A
PCI for Chronic Total Occlusions Chronic Total Occlusions Why not Medical Treatment? Medical Treatment CTO in 891 pts over 24 years High 10% Mortality Low 2 % 1 year 10 years Puma JA, et al. JACC 1994;23:390A
Hydrodynamic boost: a novel re-entry technique in distal BTK vessel: when and how to do it
 Hydrodynamic boost: a novel re-entry technique in distal BTK vessel: when and how to do it Roberto Ferraresi Peripheral Interventional Unit Bergamo Italy Disclosure Roberto Ferraresi, MD I have the following
Hydrodynamic boost: a novel re-entry technique in distal BTK vessel: when and how to do it Roberto Ferraresi Peripheral Interventional Unit Bergamo Italy Disclosure Roberto Ferraresi, MD I have the following
Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts
 Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts Disclosure Speaker name: Matthew T. Menard... x I do not have
Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts Disclosure Speaker name: Matthew T. Menard... x I do not have
Guidewire Selection. Making the Most Out of My Guidewire: LINC 2016: Leipzig Interventional Course Leipzig, Germany January 26-29, 2016
 Making the Most Out of My Guidewire: Guidewire Selection LINC 2016: Leipzig Interventional Course Leipzig, Germany January 26-29, 2016 Brian DeRubertis, MD, FACS Associate Professor of Surgery Division
Making the Most Out of My Guidewire: Guidewire Selection LINC 2016: Leipzig Interventional Course Leipzig, Germany January 26-29, 2016 Brian DeRubertis, MD, FACS Associate Professor of Surgery Division
Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System
 Volume 1, Issue 1 Case Report Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System Robert F. Riley * and Bill Lombardi University of Washington Medical Center, Division
Volume 1, Issue 1 Case Report Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System Robert F. Riley * and Bill Lombardi University of Washington Medical Center, Division
IVUS Guided Case Review Case Performed by Frank R. Arko III, MD Charlotte, NC
 IVUS Guided Case Review Case Performed by Frank R. Arko III, MD Charlotte, NC The opinions and clinical experiences presented herein are for informational purposes only. Dr. Arko is a paid consultant for
IVUS Guided Case Review Case Performed by Frank R. Arko III, MD Charlotte, NC The opinions and clinical experiences presented herein are for informational purposes only. Dr. Arko is a paid consultant for
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Is a Stent or Scaffold Necessary in The SFA?
 1 2 3 Is a Stent or Scaffold Necessary in The SFA? Stents were developed to optimize acute results after angioplasty Specifically, stents are universally accepted to manage flow limiting dissections and
1 2 3 Is a Stent or Scaffold Necessary in The SFA? Stents were developed to optimize acute results after angioplasty Specifically, stents are universally accepted to manage flow limiting dissections and
Lower Extremity Endovascular Revascularization Codes
 Lower Extremity Endovascular Update: AAPC National Long Beach, CA April 4, 2011 Presented by: David Zielske, MD, CIRCC, CPC H, CCC, CCS, RCC Lower Extremity Endovascular Revascularization Codes 37220 37235
Lower Extremity Endovascular Update: AAPC National Long Beach, CA April 4, 2011 Presented by: David Zielske, MD, CIRCC, CPC H, CCC, CCS, RCC Lower Extremity Endovascular Revascularization Codes 37220 37235
I am no good at debates!
 Disclosure Statement of Financial Interest Imaging Strategy for Claudication: Ultrasound Alone is Not Adequate to Select Patients for Endovascular Intervention Within the past 12 months, I or my spouse/partner
Disclosure Statement of Financial Interest Imaging Strategy for Claudication: Ultrasound Alone is Not Adequate to Select Patients for Endovascular Intervention Within the past 12 months, I or my spouse/partner
MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES
 MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES PUSHING BOUNDARIES Terumo Interventional Systems is committed to your success with innovative procedural solutions and ongoing support for your most challenging
MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES PUSHING BOUNDARIES Terumo Interventional Systems is committed to your success with innovative procedural solutions and ongoing support for your most challenging
CPT Code Details
 CPT Code 93572 Details Code Descriptor Intravascular Doppler velocity and/or pressure derived coronary flow reserve measurement (coronary vessel or graft) during coronary angiography including pharmacologically
CPT Code 93572 Details Code Descriptor Intravascular Doppler velocity and/or pressure derived coronary flow reserve measurement (coronary vessel or graft) during coronary angiography including pharmacologically
Endovascular treatment (EVT) has markedly advanced,
 Ann Vasc Dis Vol. 6, No. 3; 2013; pp 573 577 Online August 12, 2013 2013 Annals of Vascular Diseases doi:10.3400/avd.oa.13-00055 Original Article A Review of Surgically Treated Patients with Obstruction
Ann Vasc Dis Vol. 6, No. 3; 2013; pp 573 577 Online August 12, 2013 2013 Annals of Vascular Diseases doi:10.3400/avd.oa.13-00055 Original Article A Review of Surgically Treated Patients with Obstruction
Efficacy of DEB in Calcification and Subintimal Angioplasty
 Efficacy of DEB in Calcification and Subintimal Angioplasty Seung-Woon Rha, MD, PhD, FACC, FAHA, FSCAI, FESC, FAPSIC Div of Cardiovascular Intervention and Research Cardiovascular Center, Korea University
Efficacy of DEB in Calcification and Subintimal Angioplasty Seung-Woon Rha, MD, PhD, FACC, FAHA, FSCAI, FESC, FAPSIC Div of Cardiovascular Intervention and Research Cardiovascular Center, Korea University
The incidence of peripheral artery disease (PAD)
 Pharmacologic Options for Treating Restenosis The role of cilostazol in the treatment of patients with infrainguinal lesions. By Osamu Iida, MD, and Yoshimitsu Soga, MD The incidence of peripheral artery
Pharmacologic Options for Treating Restenosis The role of cilostazol in the treatment of patients with infrainguinal lesions. By Osamu Iida, MD, and Yoshimitsu Soga, MD The incidence of peripheral artery
How to manage TAVI related vascular complications. Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI
 How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
CTO: Technique and Tools
 CTO: Technique and Tools S. Hinan Ahmed, MD Associate Professor: Cardiology and Cardiothoracic Surgery Program Director: Interventional Fellowship Program Associate Editor: Cath Cardiov Interventions UT
CTO: Technique and Tools S. Hinan Ahmed, MD Associate Professor: Cardiology and Cardiothoracic Surgery Program Director: Interventional Fellowship Program Associate Editor: Cath Cardiov Interventions UT
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue
 Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Which Stent Is Best for Various Femoropopliteal Anatomy? 2018 Pacific Northwest Endovascular Conference June 15-26, 2018 Seattle, WA
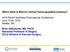 Which Stent Is Best for Various Femoropopliteal Anatomy? 2018 Pacific Northwest Endovascular Conference June 15-26, 2018 Seattle, WA Brian DeRubertis, MD, FACS Associate Professor of Surgery UCLA Division
Which Stent Is Best for Various Femoropopliteal Anatomy? 2018 Pacific Northwest Endovascular Conference June 15-26, 2018 Seattle, WA Brian DeRubertis, MD, FACS Associate Professor of Surgery UCLA Division
