imedpub Journals Predictors of Mortality in Patients with Isomerism Introduction Abstract 2016 Vol.2 No.
|
|
|
- Jessica Mason
- 5 years ago
- Views:
Transcription
1 Research Article imedpub Journals Journal of Pediatric Care DOI: / X Predictors of Mortality in Patients with Isomerism Rohit S Loomba 1, Peter C Frommelt 1 and Robert H Anderson 2 1 Division of Cardiology, Children s Hospital of Wisconsin, Milwaukee, WI 53211, USA 2 Institute of Genetics, Newcastle University, Newcastle Upon Tyne, UK Corresponding author: Rohit S Loomba, Division of Cardiology, Children s Hospital of Wisconsin, Milwaukee, WI 53211, USA, Tel: ; loomba.rohit@gmail.com Rec date: Aug 02, ; Acc date: Aug 23, ; Pub date: Aug 30, Copyright: Rohit S Loomba, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Citation: Loomba RS, Frommelt PC, Anderson RH. Predictors of Mortality in Patients With Isomerism. J Pediatr Care., 2:15. Abstract Background: The so-called heterotaxy, or isomerism, is associated with increased morbidity and mortality. Previous studies have identified various risk factors associated with increased mortality in those with isomerism. The aim of this study was to identify such risk factors in our single center experience. Methods: Retrospective review of patients cared for at the Children s Hospital of Wisconsin was carried out to identify patients with isomerism who received care between January 1998 and December Clinical and surgical data were collected for all these patients. Univariate analysis was conducted to compare characteristics between those who died during this period and those who remained alive. Logistic regression was then conducted to identify independent risk factors for mortality. Results: We included a total of 83 patients in our analysis. Of these patients, 17 (20%) died during the period of follow-up. The only independent risk factor found to be associated with mortality after logistic regression was the need for extracorporeal membrane oxygenation. Univariate analysis had also identified increased duration of ventilatory support after initial cardiac palliation as associated with mortality, but we did not include this feature in the logistic regression due to the low number of patients. Conclusion: The need for extracorporeal membrane oxygenation is associated with increased mortality in those with isomerism. No cardiac malformations were identified as independent risk factors of mortality. A larger multicenter effort is required to better identify risk factors associated with mortality in patients with isomerism. Keywords: Mortality; Isomerism; Patients; Diagnosis; Pneumonia Introduction The so-called heterotaxy is characterized by isomerism of the thoracic organs and random arrangement of the abdominal organs [1-4]. For this reason, among others, it is better referred to simply as isomerism [1]. Isomerism can be further segregated into the subsets of left or right on the basis of the morphology of the atrial appendages, which is the most constant feature of isomerism, and the only example of isomerism found within the heart. Delineation between the subsets of left and right isomerism allows for inferences to be made regarding associated cardiac and extracardiac malformations, as well as organ dysfunction. Thus, these features can be appropriately screened, potentially permitting earlier detection and appropriate intervention. Isomerism is associated with congenital malformations in nearly all organ systems, many of which can now be detected on fetal evaluation [5,6]. The number of organ systems affected in a single patient can be variable. The effects on the organs systems, furthermore, go beyond simply being anatomic, entailing additional functional abnormalities. For instance, any splenic anatomy, including a normal appearing, normally located, solitary spleen may be associated with splenic dysfunction [7]. This is associated with increased prevalence of thrombocytosis and bacteremia [8-11]. Abnormalities in the development of the cardiac conduction system predispose to arrhythmias [12-14]. Bronchopulmonary isomerism may also have functional implications. These anatomic and functional abnormalities potentially decrease survival in those with isomerism, such that those with congenital malformations of the heart in the setting of isomerism have lower survival than those with the same congenital cardiac malformations but without isomerism. Although there has been improvement in survival associated with isomerism in the recent era, differences are still present. We set forth, therefore, to determine the risk factors for mortality in those with isomerism. Copyright imedpub This article is available from: 1
2 Methods Patients with isomerism cared for at Children s Hospital of Wisconsin from January 1998 to January 2014 were retrospectively identified. Data regarding their cardiac and non-cardiac anatomy, cardiac surgical palliations, and other findings associated with isomerism were collected by chart review. Cardiac anatomy was analyzed by use of echocardiography, although findings were confirmed with catheterization studies, computed tomography, and magnetic resonance imaging when available, using the principle of sequential segmental analysis [15]. Bronchial morphology was determined using chest radiographs, computed tomography, and magnetic resonance imaging [16,17]. Intestinal malrotation was assessed by review of upper gastrointestinal studies. Splenic status was analyzed most often by abdominal ultrasonography, but some patients also had computed tomographic or magnetic resonance imaging from which splenic anatomy could also be noted. As it had not been a routine feature during our study period for the surgeons to document the morphology of the atrial appendages at the time of surgery, and because of the presumed difficulty associated with imaging the appendages, specific data relating to their morphology was not available. Instead, we used an aggregate of all the collected features to segregate the entire cohort into the subsets or right or left isomerism. Data regarding surgical palliation was obtained from the operative notes. This included the precise procedure, the times required for cardiopulmonary bypass and aortic cross-clamping, and any operative complications. We also noted whether or not patients were extubated in the operating room. The total postoperative length of mechanical ventilation, as well as need for reintubation in the postoperative period, was also collected, along with total length of stay associated with surgical palliation. Continuous data is presented as mean or standard deviation, while descriptive data is presented as actual number and percentage. Continuous variables were analyzed using Student s t-test, the Mann-Whitney-U test, or analysis of variance where appropriate. Descriptive data were analyzed using chi-square analysis or Fisher s exact test. Chisquare analysis was used to compare features between those dying and those who were still alive. Variables with a p-value of less than 0.2 were then entered as independent variables into a logistic regression, with mortality as the dependent variable. Continuous variables were not entered into the regression, as the study was grossly underpowered for this purpose. Statistical analysis was done using SPSS version 20.0 (Chicago, IL). A p-value of less than 0.05 was considered statistically significant. Results We included a total of 83 patients retrospectively identified for inclusion in this analysis. Of these, 17 (20%) died during the period of follow-up. Median age of death was 3 months, with a range of 1 day to 23 years. Median follow-up was 5.3 years, with a range from 0.3 years to 33.6 years, in those who remained alive during the study period, and was a median of 0.5 years, with a range from 0.1 years to 22.6 years, in those who died during the study period. Characteristics were then compared between those who remained alive and those who had died during this period. In univariate analysis, those who died were more likely to have a common atrioventricular junction (odds ratio 3.658, 95% confidence interval to ), to have required extracorporeal membrane oxygenation (odds ratio , 95% confidence interval to ), and to have experienced an episode of bacteremia (odds ratio 5.630, 95% confidence interval to ). Prenatal diagnosis, genetic mutation, pulmonary atresia, anomalous pulmonary venous connections requiring surgical intervention, left as opposed to right isomerism, intestinal malrotation, surgery for intestinal malrotation, abdominal arrangement, splenic anatomy, presence of arrhythmia, need for pacemaker placement, repair status at last follow-up, or sinupulmonary symptoms were not associated with mortality. Surgical characteristics were not associated with mortality other than the number of days of mechanical ventilatory support after initial cardiac palliation, the number of days the chest remained open after initial cardiac palliation, and the length of hospitalization associated with the initial cardiac palliation. Those who died required a median of 21 days of postoperative mechanical ventilatory support after initial cardiac palliation, in comparison to 1.5 days in those who did not die (p=0.030). Those who died underwent delayed sternal closure at a median of 3 days after initial cardiac palliation, compared to zero days in those who did not die (p=0.023). Prolonged hospitalization duration was also associated with mortality, as those who died had a median duration of 125 days after initial cardiac palliation compared to 22 days in those who survived (p=0.006). In addition, length of hospitalization after the second cardiac palliatiative procedure was also prolonged in those who died, with a median of 70.5 days compared to 14 days in those who survived (p=0.024) is shown in Tables 1 and 2. Table 1: Comparison of cardiac and clinical characteristics between those with isomerism who died and remained alive during follow-up. Alive (n=66) Deceased (n=17) P-value Odds ratio and 95% confidence interval Age at death 6.3 months (1 day to 22.6 years) 2 This article is available from:
3 Prenatal diagnosis 43 (72) 10 (71) (0.273 to 3.585) Identified genetic mutation 10 (47) 3 (63) (0.341 to ) Common atrioventricular junction 37 (56) 14 (82) (0.959 to ) Double outlet right ventricle 23 (35) 7 (41) (0.440 to 3.895) Double inlet left ventricle 1 (2) 0 (0) Bilateral superior caval veins 33 (50) 8 (47) (0.306 to 2.585) Interruption of the inferior caval vein 23 (35) 3 (18) (0.104 to 1.539) Discordant atrioventricular connections 10 (15) 4 (24) (0.466 to 6.368) Discordant ventriculoarterial connections 13 (20) 4 (24) (0.351 to 4.486) Pulmonary atresia 19 (29) 6 (35) (0.437 to 4.170) Pulmonary veins requiring intervention 21 (32) 8 (47) (0.644 to 5.632) Intestinal malrotation 26 (39) 8 (53) (0.592 to 5.060) Surgery for intestinal malrotation 24 (80) 8 (80) (0.167 to 5.985) Age at malrotation surgery (days) 7.0 (1.0 to 140.0) 21.0 (3.0 to 57.0) Inferred isomerism sidedness 42 (64) 11 (65) Right 24 (36) 6 (35) Left Bronchial morphology 12 (20) 1 (7) Right 48 (80) 13 (93) Left Abdominal arrangement 20 (31) 4 (31) Left sided stomach, right sided liver 25 (38) 6 (46) Right sided stomach, left sided liver 20 (31) 3 (23) Midline liver Splenic anatomy 38 (59) 13 (81) 0.23 Absent 9 (14) 1 (6) Multiple 18 (27) 2 (13) Single Arrhythmia 35 (53) 6 (35) (0.160 to 1.460) Need for pacemaker 10 (15) 2 (12) (0.148 to 3.779) Need for extracorporeal membrane oxygenation 2 (3) 7 (41) < (4.064 to ) Bacteremia 9 (14) 8 (47) (1.723 to ) Underwent initial cardiac palliation 62 (94) 14 (82) (0.060 to 1.499) Age at initial cardiac palliation (days) 15.5 (0 to 871.0) 7.0 (0 to 518.0) Number of ventilatory days after initial cardiac palliation 1.5 (0 to 44.0) 21.0 (2 to 114) Number of days chest open after initial cardiac palliation Length of hospitalization for initial cardiac palliation (days) 0 (0 to 13.0) 3 (0 to 28.0) (3.0 to 225.0) (13.0 to 235.0) Underwent second cardiac palliation 48 (73) 13 (77) (0.351 to 4.231) Age at second cardiac palliation (months) 8.0 (0.5 to 123.0) 5.0 (0.5 to 138.8) Number of ventilatory days after second cardiac palliation 0 (0 to 6.0) 3.0 (2.0 to 5.0) Copyright imedpub 3
4 Number of days chest open after second cardiac palliation 0 (0 to 4) 0 (0 to 4) Length of hospitalization for second cardiac palliation 14 (4 to 225) 70.5 (0 to 235) Underwent third cardiac palliation 23 (35) 4 (24) Age at third cardiac palliation (years) 4.3 (0.5 to 10.0) 4.5 (0.5 to 9.5) Number of ventilatory days after third cardiac palliation 0 (0 to 6.0) 3.0 (3.0 to 3.0) Number of days chest open after third cardiac palliation 0 (0 to 3.0) 0 (0 to 0) Length of hospitalization for third cardiac palliation 9.0 (o to 197.0) 34.0 (6 to 41) Repair status at last follow-up 43 (65) 14 (82) Functionally univentricular 21 (32) 2 (12) Biventricular 2 (3) 1 (6) Transplant Recurrent upper respiratory infections 11 (17) 2 (12) (0.133 to 3.339) Recurrent pneumonia 3 (5) 1 (6) (0.128 to ) Chronic lung disease 6 (9) 3 (18) (0.477 to 9.633) Reactive airway disease 8 (12) 2 (12) (0.186 to 5.035) Need for home oxygen 15 (24) 4 (24) Tracheostomy 2 (3) 0 (0) Follow-up duration (years) 5.3 (0.3 to 33.6) 0.5 (0.1 to 22.6) A logistic regression was then conducted to determine those factors independently associated with death. The dependent variable for this regression was death with the following being entered as independent variables: need for extracorporeal membrane oxygenation, history of bacteremia, chronic arrhythmia, presence of an interrupted inferior caval vein, and presence of a common atrioventricular junction. Need for extracorporeal membrane oxygenation (odds ratio 9.302, 95% confidence interval to ) was the only factor that remained significant after regression analysis, and thus was identified as an independent predictor of mortality in the setting of isomerism. Table 2: Results of regression analysis. Coefficient p-value Odds ratio (95% Confidence interval) Interrupted inferior caval vein (0.095 to 2.808) Arrhythmia (0.145 to 2.084) Need for extracorporeal membrane oxygenation (1.401 to ) Bacteremia (0.861 to ) Common atrioventricular junction (0.595 to ) Discussion Isomerism, also known as heterotaxy, has been associated with increased mortality, although the precise mechanisms have yet to be entirely elucidated. Congenital malformations of the heart do not account for all of this mortality, although those with isomerism and congenital malformations of the heart are known to have an increased mortality when compared to those with similar congenital malformations in the absence of isomerism [18,19]. As several organ systems can be impacted by isomerism, we sought to determine the risk factors associated with mortality in those with isomerism. After regression analysis, the need for extracorporeal membrane oxygenation was found to be the only independent risk factor for mortality. Specific congenital malformations of the heart, history of bacteremia, repair status, splenic anatomy, nor the type of isomerism sidedness were not associated with mortality. Mortality, in the setting of isomerism, appears to be greatest in the first three years of life [20]. Particularly for those requiring functionally univentricular palliation, this period is characterized by hospitalization and hemodynamic instability as patients undergo the initial staged surgical procedures. During this period, isomerism mediates an increased need for delayed sternal closure, longer duration of mechanical 4 This article is available from:
5 ventilation, and greater risk of bacteremia, all of which can increase the risk of mortality [10,11,21,22]. The increased duration of mechanical ventilation may be secondary to underlying ciliary dyskinesia, demonstrated to be found in slightly over half of patients with congenital malformations of the heart and isomerism [21]. Increased pulmonary vascular resistance, and pulmonary hypertension, may also lead to the more adverse pulmonary phenotype found in some patients with isomerism [23]. Patients with pulmonary atresia and obstructed anomalous pulmonary venous connections are known to be at particularly high risk [24]. The increased risk of bacteremia is likely due to splenic dysfunction and alterations in B-cell populations, further compounded by the presence of invasive monitoring lines and endotracheal tubes [25,26]. Extracardiac malformations of isomerism, such as those found in the central nervous system, genitourinary system, and gastrointestinal system may also require surgical intervention. These malformations themselves, or the interventions associated with these, may also increase morbidity and mortality in the setting of isomerism. These include hydrocephalus necessitating the need for a cerebral shunt or intestinal malrotation necessitating a Ladd s procedure [27]. Previous studies investigating mortality in isomerism have served to identify risk factors. These have included obstructed pulmonary venous connection, anomalous pulmonary venous connection, functionally univentricular circulation, congenital heart block, having noncardiac anomalies, mild or greater atrioventricular valvar regurgitation, having a common atrioventricular junction, aortic coarctation, need for neonatal surgery, and right ventricular outflow tract obstruction [19,28-39]. None of these features, however, proved to be associated with mortality in our analysis. Identification of factors associated with mortality in those with isomerism, nonetheless, will allow for increased vigilance in those shown to be at high risk. As more is understood about these risk factors, and what mediates them, interventions may be available to help reduce this risk. More thorough and accurate risk assessment will also allow for more appropriate counseling. Our study is limited by a relatively small number of patients, which leaves it underpowered. The single center nature of the study has its strengths, but limits the study by reducing the numbers available for analysis. Differences in surgical management and intensive care strategies, however, can lead to different results amongst individual centers. Despite this shortcoming, there is a need for a large multicenter collaboration to identify risk factors for mortality in a larger cohort of patients with isomerism. This would also allow for identification of institution specific factors, which may also affect outcomes. Conclusion Patients with isomerism are at increased risk of mortality if they require extracorporeal membrane oxygenation. In contrast to previous reports, this study did not identify any specific cardiac malformations associated with increased mortality. There is a need for a large multicenter study to better identify risk factors for mortality in this patient population. References 1. Loomba RS, Hlavacek AM, Spicer DE, Anderson RH (2015) Isomerism or heterotaxy: which term leads to better understanding? Cardiology in the young: Jacobs JP, Anderson RH, Weinberg PM, Walters HL 3rd, Tchervenkov CI, et al. (2007) The nomenclature, definition and classification of cardiac structures in the setting of heterotaxy. Cardiology in the young. 17 Suppl 2: Uemura H, Ho SY, Devine WA, Kilpatrick LL, Anderson RH (1995) Atrial appendages and venoatrial connections in hearts from patients with visceral heterotaxy. The Annals of thoracic surgery 60: Uemura H, Ho SY, Devine WA, Anderson RH (1995) Analysis of visceral heterotaxy according to splenic status, appendage morphology, or both. The American Journal of Cardiology 76: Loomba RS, Chandrasekar S, Shah PH, Sanan P (2011) The developing role of fetal magnetic resonance imaging in the diagnosis of congenital cardiac anomalies: A systematic review. Annals of pediatric cardiology 4: Loomba R, Shah PH, Anderson RH (2015) Fetal magnetic resonance imaging of malformations associated with heterotaxy. Cureus 7: e Nagel BH, Williams H, Stewart L, Paul J, Stumper O (2005) Splenic state in surviving patients with visceral heterotaxy. Cardiology in the young 15: Loomba RS, Anderson RH (2015) Letter to the editor regarding Situs inversus with levocardia, infrahepatic interruption of the inferior vena cava, and azygos continuation: A case report. Surgical and Radiologic Anatomy : SRA. 9. Loomba R (2015) Thrombocytosis in the setting of isomerism and a functionally univentricular heart. Cureus 7: Waldman JD, Rosenthal A, Smith AL, Shurin S, Nadas AS (1977) Sepsis and congenital asplenia. The Journal of Pediatrics 90: Chiu SN, Shao PL, Wang JK, Chen HC, Lin MT, et al. (2014) Severe bacterial infection in patients with heterotaxy syndrome. The Journal of Pediatrics 164: e Smith A, Ho SY, Anderson RH, Connell MG, Arnold R, et al. (2006) The diverse cardiac morphology seen in hearts with isomerism of the atrial appendages with reference to the disposition of the specialized conduction system. Cardiology in the Young 16: Loomba RS, Willes RJ, Kovach JR, Anderson RH (2015) Chronic arrhythmias in the setting of heterotaxy: Differences between right and left Isomerism. Congenital heart disease. 14. Loomba RS, Aggarwal S, Gupta N, Buelow M, Alla V, et al. (2015) Arrhythmias in adult congenital patients with bodily isomerism. Pediatric Cardiology. 15. Anderson RH, Becker AE, Freedom RM, Macartney FJ, Quero- Jimenez M, et al. (1984) Sequential segmental analysis of congenital heart disease. Pediatric Cardiology 5: Copyright imedpub 5
6 16. Loomba RS, Pelech AN, Shah PH, Anderson RH (2015) Determining bronchial morphology for the purposes of segregating so-called heterotaxy. Cardiology in the Young: Partridge JB, Scott O, Deverall PB, Macartney FJ (1975) Visualization and measurement of the main bronchi by tomography as an objective indicator of thoracic situs in congenital heart disease. Circulation 51: Aeba R, Katogi T, Takeuchi S, Kawada S (1997) Long-term followup of surgical patients with single-ventricle physiology: Prognostic anatomical determinants. Cardiovascular surgery 5: Stamm C, Friehs I, Mayer JE, Jr., Zurakowski D, Triedman JK, et al. (2001) Long-term results of the lateral tunnel fontan operation. The Journal of Thoracic and Cardiovascular Surgery 121: Loomba RS, Nijhawan K, Anderson R () Impact of era, type of isomerism, and ventricular morphology on survival in heterotaxy: Implications for Therapeutic Management. World Journal for Pediatric & Congenital Heart Surgery 7: Nakhleh N, Francis R, Giese RA, Tian X, Li Y, et al. (2012) High prevalence of respiratory ciliary dysfunction in congenital heart disease patients with heterotaxy. Circulation 125: Harden B, Tian X, Giese R, Nakhleh N, Kureshi S, et al. (2014) Increased postoperative respiratory complications in heterotaxy congenital heart disease patients with respiratory ciliary dysfunction. The Journal of Thoracic and Cardiovascular Surgery 147: e Loomba R (2015) Comment on pulmonary hypertension in a patient with congenital heart defects and heterotaxy syndrome. Ochsner Journal 15: Sinzobahamvya N, Arenz C, Reckers J, Photiadis J, Murin P, et al. (2009) Poor outcome for patients with totally anomalous pulmonary venous connection and functionally single ventricle. Cardiology in the young 19: Nagelkerken L, Henfling M, Van Breda Vriesman P (1985) Accessory cell function of thoracic duct non-lymphoid cells, dendritic cells, and splenic adherent cells in the Brown-Norway rat. Cellular Immunology 93: Chiu SN, Shao PL, Wang JK, Hsu HW, Lin MT, et al. (2015) Low immunoglobulin-m memory, B-cell percentage in patients with heterotaxy syndrome correlates with the risk of severe bacterial infection. Pediatric research. 27. Kothari SS (2014) Non-cardiac issues in patients with heterotaxy syndrome. Annals of Pediatric Cardiology 7: Cheung YF, Cheng VY, Chau AK, Chiu CS, Yung TC, et al. (2002) Outcome of infants with right atrial isomerism: Is prognosis better with normal pulmonary venous drainage? Heart 87: Cohen MS, Schultz AH, Tian ZY, Donaghue DD, Weinberg PM, et al. (2006) Heterotaxy syndrome with functional single ventricle: Does prenatal diagnosis improve survival? The Annals of Thoracic Surgery 82: Escobar-Diaz MC, Friedman K, Salem Y, Marx GR, Kalish BT, et al. (2014) Perinatal and infant outcomes of prenatal diagnosis of heterotaxy syndrome (asplenia and polysplenia). The American Journal of Cardiology 114: Foerster SR, Gauvreau K, McElhinney DB, Geva T (2008) Importance of totally anomalous pulmonary venous connection and postoperative pulmonary vein stenosis in outcomes of heterotaxy syndrome. Pediatric Cardiology 29: Gilljam T, McCrindle BW, Smallhorn JF, Williams WG, Freedom RM (2000) Outcomes of left atrial isomerism over a 28-year period at a single institution. Journal of the American College of Cardiology 36: Hashmi A, Abu-Sulaiman R, McCrindle BW, Smallhorn JF, Williams WG, et al. (1998) Management and outcomes of right atrial isomerism: a 26-year experience. Journal of the American College of Cardiology 31: Kim SJ, Kim WH, Lim HG, Lee CH, Lee JY (2006) Improving results of the Fontan procedure in patients with heterotaxy syndrome. The Annals of Thoracic Surgery 82: Ota N, Fujimoto Y, Hirose K, Tosaka Y, Nakata T, et al. (2010) Improving results of atrioventricular valve repair in challenging patients with heterotaxy syndrome. Cardiology in the Young 20: Sebastian VA, Brenes J, Murthy R, Veeram Reddy S, Dimas VV, et al. (2014) Management and outcomes of heterotaxy syndrome associated with pulmonary atresia or pulmonary stenosis. The Annals of Thoracic Surgery 98: Serraf A, Bensari N, Houyel L, Capderou A, Roussin R, et al. (2010) Surgical management of congenital heart defects associated with heterotaxy syndrome. European Journal of Cardio-Thoracic Surgery: Official Journal of the European Association for Cardio-Thoracic Surgery 38: Song J, Kang IS, Huh J, Lee OJ, Kim G, et al. (2013) Interstage mortality for functional single ventricle with heterotaxy syndrome: A retrospective study of the clinical experience of a single tertiary center. Journal of Cardiothoracic Surgery 8: Taketazu M, Lougheed J, Yoo SJ, Lim JS, Hornberger LK (2006) Spectrum of cardiovascular disease, accuracy of diagnosis, and outcome in fetal heterotaxy syndrome. The American Journal of Cardiology 97: This article is available from:
All You Need to Know About Situs and Looping Disorders: Embryology, Anatomy, and Echocardiography
 All You Need to Know About Situs and Looping Disorders: Embryology, Anatomy, and Echocardiography Helena Gardiner Co-Director of Fetal Cardiology, The Fetal Center, University of Texas at Houston Situs
All You Need to Know About Situs and Looping Disorders: Embryology, Anatomy, and Echocardiography Helena Gardiner Co-Director of Fetal Cardiology, The Fetal Center, University of Texas at Houston Situs
Fetal Heterotaxy with Tricuspid Atresia, Pulmonary Atresia, and Isomerism of the Right Atrial Appendages at 22 Weeks
 THIEME Case Report 97 Fetal Heterotaxy with Tricuspid Atresia, Pulmonary Atresia, and Isomerism of the Right Atrial Appendages at 22 Weeks Julia E. Solomon, MD 1 John H. Stock, MD 2 Randy R. Richardson,
THIEME Case Report 97 Fetal Heterotaxy with Tricuspid Atresia, Pulmonary Atresia, and Isomerism of the Right Atrial Appendages at 22 Weeks Julia E. Solomon, MD 1 John H. Stock, MD 2 Randy R. Richardson,
Congenital Heart Disease. Disharmonious Patterns of Heterotaxy and Isomerism How Often Are the Classic Patterns Breached?
 Congenital Heart Disease Disharmonious Patterns of Heterotaxy and Isomerism How Often Are the Classic Patterns Breached? Deane Yim, MBchB; Hazumu Nagata, MD; Christopher Z. Lam, MD; Lars Grosse-Wortmann,
Congenital Heart Disease Disharmonious Patterns of Heterotaxy and Isomerism How Often Are the Classic Patterns Breached? Deane Yim, MBchB; Hazumu Nagata, MD; Christopher Z. Lam, MD; Lars Grosse-Wortmann,
This is the left, right?
 This is the left, right? Poster No.: C-1214 Congress: ECR 2013 Type: Educational Exhibit Authors: L.-L. Huang, L. Mitchell, S. Andronikou, F. Suleman, Z. I. Lockhat; Pretoria/ZA Keywords: Congenital, Diagnostic
This is the left, right? Poster No.: C-1214 Congress: ECR 2013 Type: Educational Exhibit Authors: L.-L. Huang, L. Mitchell, S. Andronikou, F. Suleman, Z. I. Lockhat; Pretoria/ZA Keywords: Congenital, Diagnostic
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum
 Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Segmental approach to normal and abnormal situs arrangement - Echocardiography -
 Segmental approach to normal and abnormal situs arrangement - Echocardiography - Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London No disclosures
Segmental approach to normal and abnormal situs arrangement - Echocardiography - Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London No disclosures
CASE OF HETEROTAXY SYNDROME WITH POLYSPLENIA AND INTESTINAL MALROTATION
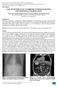 CASE OF HETEROTAXY SYNDROME WITH POLYSPLENIA AND INTESTINAL MALROTATION *Sagar H S, Basanta Manjari Swain, Jayashree Mohanty and Sasmita Parida Department of Radio diagnosis, S.C.B. Medical College, Cuttack
CASE OF HETEROTAXY SYNDROME WITH POLYSPLENIA AND INTESTINAL MALROTATION *Sagar H S, Basanta Manjari Swain, Jayashree Mohanty and Sasmita Parida Department of Radio diagnosis, S.C.B. Medical College, Cuttack
Visceral heterotaxy syndromes are characterized by. Improving Outcomes of the Surgical Management of Right Atrial Isomerism
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
LONG TERM OUTCOMES OF PALLIATIVE CONGENITAL HEART DISEASE
 LONG TERM OUTCOMES OF PALLIATIVE CONGENITAL HEART DISEASE S Bruce Greenberg, MD, FACR, FNASCI Professor of Radiology and Pediatrics Arkansas Children's Hospital University of Arkansas for Medical Sciences
LONG TERM OUTCOMES OF PALLIATIVE CONGENITAL HEART DISEASE S Bruce Greenberg, MD, FACR, FNASCI Professor of Radiology and Pediatrics Arkansas Children's Hospital University of Arkansas for Medical Sciences
Situs inversus. Dr praveena pulmonology- final year post graduate
 Situs inversus Dr praveena pulmonology- final year post graduate Definiton History Types Cause Clinical features Diagnosis Treatment Definition The term situs inversus is a short form of the latin phrase
Situs inversus Dr praveena pulmonology- final year post graduate Definiton History Types Cause Clinical features Diagnosis Treatment Definition The term situs inversus is a short form of the latin phrase
What do we know about Heterotaxy Syndrome? - An illustrated guide.
 What do we know about Heterotaxy Syndrome? - An illustrated guide. Poster No.: C-2369 Congress: ECR 2015 Type: Educational Exhibit Authors: M. C. Ageitos Casais, A. X. Martínez de Alegría Alonso, 1 1 2
What do we know about Heterotaxy Syndrome? - An illustrated guide. Poster No.: C-2369 Congress: ECR 2015 Type: Educational Exhibit Authors: M. C. Ageitos Casais, A. X. Martínez de Alegría Alonso, 1 1 2
Heterotaxy Syndrome. Introduction. Definitions. Soo-Jin Kim, MD
 REVIEW DOI 0.4070/kcj.0.4.5.7 Print ISSN 738-550 / On-line ISSN 738-5555 Copyright 0 The Korean Society of Cardiology Open Access Heterotaxy Syndrome Soo-Jin Kim, MD Division of Pediatric Cardiology, Department
REVIEW DOI 0.4070/kcj.0.4.5.7 Print ISSN 738-550 / On-line ISSN 738-5555 Copyright 0 The Korean Society of Cardiology Open Access Heterotaxy Syndrome Soo-Jin Kim, MD Division of Pediatric Cardiology, Department
J Somerville and V Grech. The chest x-ray in congenital heart disease 2. Images Paediatr Cardiol Jan-Mar; 12(1): 1 8.
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2010 PMCID: PMC3228330 The chest x-ray in congenital heart disease 2 J Somerville and V Grech Paediatric Department, Mater Dei Hospital, Malta Corresponding
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2010 PMCID: PMC3228330 The chest x-ray in congenital heart disease 2 J Somerville and V Grech Paediatric Department, Mater Dei Hospital, Malta Corresponding
Case Report Computed Tomography Angiography Successfully Used to Diagnose Postoperative Systemic-Pulmonary Artery Shunt Narrowing
 Case Reports in Cardiology Volume 2011, Article ID 802643, 4 pages doi:10.1155/2011/802643 Case Report Computed Tomography Angiography Successfully Used to Diagnose Postoperative Systemic-Pulmonary Artery
Case Reports in Cardiology Volume 2011, Article ID 802643, 4 pages doi:10.1155/2011/802643 Case Report Computed Tomography Angiography Successfully Used to Diagnose Postoperative Systemic-Pulmonary Artery
Splenic state in surviving patients with visceral heterotaxy
 Cardiol Young 2005; 15: 469 473 Cambridge University Press ISSN 1047-9511 Original Article Splenic state in surviving patients with visceral heterotaxy Bert H. P. Nagel, 1 Helen Williams, 2 Louise Stewart,
Cardiol Young 2005; 15: 469 473 Cambridge University Press ISSN 1047-9511 Original Article Splenic state in surviving patients with visceral heterotaxy Bert H. P. Nagel, 1 Helen Williams, 2 Louise Stewart,
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT
 LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
PULMONARY VENOLOBAR SYNDROME. Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital.
 PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
Anatomy of Atrioventricular Septal Defect (AVSD)
 Surgical challenges in atrio-ventricular septal defect in grown-up congenital heart disease Anatomy of Atrioventricular Septal Defect (AVSD) S. Yen Ho Professor of Cardiac Morphology Royal Brompton and
Surgical challenges in atrio-ventricular septal defect in grown-up congenital heart disease Anatomy of Atrioventricular Septal Defect (AVSD) S. Yen Ho Professor of Cardiac Morphology Royal Brompton and
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
A Classic Case Of Polysplenia Syndrome With A Pancreatic Mass And SOLs In Liver
 ISPUB.COM The Internet Journal of Radiology Volume 13 Number 2 A Classic Case Of Polysplenia Syndrome With A Pancreatic Mass And SOLs In Liver V Gupta, N Agarwal Citation V Gupta, N Agarwal. A Classic
ISPUB.COM The Internet Journal of Radiology Volume 13 Number 2 A Classic Case Of Polysplenia Syndrome With A Pancreatic Mass And SOLs In Liver V Gupta, N Agarwal Citation V Gupta, N Agarwal. A Classic
Systematic approach to Fetal Echocardiography. Objectives. Introduction 11/2/2015
 Systematic approach to Fetal Echocardiography. Pediatric Echocardiography Conference, JCMCH November 7, 2015 Rajani Anand Objectives Fetal cardiology pre-test Introduction Embryology and Physiology of
Systematic approach to Fetal Echocardiography. Pediatric Echocardiography Conference, JCMCH November 7, 2015 Rajani Anand Objectives Fetal cardiology pre-test Introduction Embryology and Physiology of
Functional SV with TAPVD: Contemporary Management of Right Atrial Isomerism
 Functional SV with TAPVD: Contemporary Management of Right Atrial Isomerism Yun TJ, Van Arsdell GS Asan Medical Center The Hospital for Sick Children in Toronto Functional SV, TAPVD and RAI FSV TAPVD RAI
Functional SV with TAPVD: Contemporary Management of Right Atrial Isomerism Yun TJ, Van Arsdell GS Asan Medical Center The Hospital for Sick Children in Toronto Functional SV, TAPVD and RAI FSV TAPVD RAI
Congenital Heart Disease: a Pictorial Illustration of Putting Segmental Approach into Practice
 pissn 2384-1095 eissn 2384-1109 imri 2015;19:205-211 http://dx.doi.org/10.13104/imri.2015.19.4.205 Congenital Heart Disease: a Pictorial Illustration of Putting Segmental Approach into Practice Tse Hang
pissn 2384-1095 eissn 2384-1109 imri 2015;19:205-211 http://dx.doi.org/10.13104/imri.2015.19.4.205 Congenital Heart Disease: a Pictorial Illustration of Putting Segmental Approach into Practice Tse Hang
The nomenclature, definition and classification of cardiac structures in the setting of heterotaxy
 Cardiol Young 2007; 17(Suppl. 2): 1 28 r Cambridge University Press ISSN 1047-9511 doi: 10.1017/S1047951107001138 Original Article The nomenclature, definition and classification of cardiac structures
Cardiol Young 2007; 17(Suppl. 2): 1 28 r Cambridge University Press ISSN 1047-9511 doi: 10.1017/S1047951107001138 Original Article The nomenclature, definition and classification of cardiac structures
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
9/8/2009 < 1 1,2 3,4 5,6 7,8 9,10 11,12 13,14 15,16 17,18 > 18. Tetralogy of Fallot. Complex Congenital Heart Disease.
 Current Indications for Pediatric CTA S Bruce Greenberg Professor of Radiology Arkansas Children s Hospital University of Arkansas for Medical Sciences greenbergsbruce@uams.edu 45 40 35 30 25 20 15 10
Current Indications for Pediatric CTA S Bruce Greenberg Professor of Radiology Arkansas Children s Hospital University of Arkansas for Medical Sciences greenbergsbruce@uams.edu 45 40 35 30 25 20 15 10
A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution
 Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
Right atrial isomerism in children older than 3 years
 DOI 10.1186/s40064-016-3007-6 RESEARCH Open Access Right atrial isomerism in children older than 3 years Sun Yan, Wang Jianpeng, Quan Xin, Zhang Minghui, Zhang Li and Wang Hao * Abstract Background: There
DOI 10.1186/s40064-016-3007-6 RESEARCH Open Access Right atrial isomerism in children older than 3 years Sun Yan, Wang Jianpeng, Quan Xin, Zhang Minghui, Zhang Li and Wang Hao * Abstract Background: There
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions
 Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Cardiac Catheterization Cases Primary Cardiac Diagnoses Facility 12 month period from to PRIMARY DIAGNOSES (one per patient)
 PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
Heart and Soul Evaluation of the Fetal Heart
 Heart and Soul Evaluation of the Fetal Heart Ivana M. Vettraino, M.D., M.B.A. Clinical Associate Professor, Michigan State University College of Human Medicine Objectives Review the embryology of the formation
Heart and Soul Evaluation of the Fetal Heart Ivana M. Vettraino, M.D., M.B.A. Clinical Associate Professor, Michigan State University College of Human Medicine Objectives Review the embryology of the formation
Management of a Patient after the Bidirectional Glenn
 Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course
 Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
Comparing levocardia and dextrocardia in fetuses with heterotaxy syndrome: prenatal features, clinical significance and outcomes
 Wang et al. BMC Pregnancy and Childbirth (217) 17:393 DOI 1.1186/s12884-17-1579-y RESEARCH ARTICLE Open Access Comparing levocardia and dextrocardia in fetuses with heterotaxy syndrome: prenatal features,
Wang et al. BMC Pregnancy and Childbirth (217) 17:393 DOI 1.1186/s12884-17-1579-y RESEARCH ARTICLE Open Access Comparing levocardia and dextrocardia in fetuses with heterotaxy syndrome: prenatal features,
Cardiopulmonary Syndromes: Conditions With Concomitant Cardiac and Pulmonary Abnormalities
 Cardiopulmonary Syndromes: Conditions With Concomitant Cardiac and Pulmonary Abnormalities Carlos S. Restrepo M.D. Professor of Radiology The University of Texas HSC at San Antonio Cardiopulmonary Syndromes
Cardiopulmonary Syndromes: Conditions With Concomitant Cardiac and Pulmonary Abnormalities Carlos S. Restrepo M.D. Professor of Radiology The University of Texas HSC at San Antonio Cardiopulmonary Syndromes
Accuracy of the Fetal Echocardiogram in Double-outlet Right Ventricle
 Blackwell Publishing IncMalden, USACHDCongenital Heart Disease 2006 The Authors; Journal compilation 2006 Blackwell Publishing, Inc.? 200723237Original ArticleFetal Echocardiogram in Double-outlet Right
Blackwell Publishing IncMalden, USACHDCongenital Heart Disease 2006 The Authors; Journal compilation 2006 Blackwell Publishing, Inc.? 200723237Original ArticleFetal Echocardiogram in Double-outlet Right
Children with Single Ventricle Physiology: The Possibilities
 Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Abnormalities of the spleen in relation to
 122 Department of Pediatric Cardiology, Children's Hospital of Pennsylvania, USA C Anderson R H Anderson J R Zuberbuhler Department of Pathology, Children's Hospital of Pennsylvania, USA W A Devine D E
122 Department of Pediatric Cardiology, Children's Hospital of Pennsylvania, USA C Anderson R H Anderson J R Zuberbuhler Department of Pathology, Children's Hospital of Pennsylvania, USA W A Devine D E
Pulmonary Vein Stenosis
 Pulmonary Vein Stenosis Yun, Tae-Jin Asan Medical Center, University of Ulsan Pulmonary Vein Stenosis Etiology: Acquired vs. Congenital Classification Indications for intervention : For individual vein
Pulmonary Vein Stenosis Yun, Tae-Jin Asan Medical Center, University of Ulsan Pulmonary Vein Stenosis Etiology: Acquired vs. Congenital Classification Indications for intervention : For individual vein
Recent technical advances and increasing experience
 Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
DR. DO NGUYEN TIN CHILDREN HOSPITAL 1
 DR. DO NGUYEN TIN CHILDREN HOSPITAL 1 BACKGROUND Congenital extrahepatic porto-systemic shunt (CEPS), known as Abernethy malformation, is a rare malformation. Intestinal and/or splenic venous blood bypasses
DR. DO NGUYEN TIN CHILDREN HOSPITAL 1 BACKGROUND Congenital extrahepatic porto-systemic shunt (CEPS), known as Abernethy malformation, is a rare malformation. Intestinal and/or splenic venous blood bypasses
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
FUNCTIONALLY SINGLE VENTRICLE
 MORPHOLOGICAL DETERMINANTS VI TRAN EuroEcho, Budapest, 7 th December 2011 DECLARATION OF CONFLICT OF INTEREST: I have nothing to declare What is the functionally single ventricle? The heart that is incapable
MORPHOLOGICAL DETERMINANTS VI TRAN EuroEcho, Budapest, 7 th December 2011 DECLARATION OF CONFLICT OF INTEREST: I have nothing to declare What is the functionally single ventricle? The heart that is incapable
Common Defects With Expected Adult Survival:
 Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Preoperative Echocardiographic Assessment of Uni-ventricular Repair
 Preoperative Echocardiographic Assessment of Uni-ventricular Repair Salem Deraz, MD Pediatric Cardiologist, Aswan Heart Centre Magdi Yacoub Heart Foundation Uni-ventricular repair A single or series of
Preoperative Echocardiographic Assessment of Uni-ventricular Repair Salem Deraz, MD Pediatric Cardiologist, Aswan Heart Centre Magdi Yacoub Heart Foundation Uni-ventricular repair A single or series of
Regional Prenatal Congenital Heart Disease Detection and Practices Jenny Ecord, APRN Ward Family Heart Center Wichita
 Regional Prenatal Congenital Heart Disease Detection and Practices Jenny Ecord, APRN Ward Family Heart Center Wichita The Children's Mercy Hospital, 2014. 05/14 Objectives Review current local and regional
Regional Prenatal Congenital Heart Disease Detection and Practices Jenny Ecord, APRN Ward Family Heart Center Wichita The Children's Mercy Hospital, 2014. 05/14 Objectives Review current local and regional
F etal dextrocardia is a condition in which the major axis
 1590 CONGENITAL HEART DISEASE Fetal dextrocardia: diagnosis and outcome in two tertiary centres A Bernasconi, A Azancot, J M Simpson, A Jones, G K Sharland... See end of article for authors affiliations...
1590 CONGENITAL HEART DISEASE Fetal dextrocardia: diagnosis and outcome in two tertiary centres A Bernasconi, A Azancot, J M Simpson, A Jones, G K Sharland... See end of article for authors affiliations...
Regional Prenatal Congenital Heart Disease Detection and Practices Lori Erickson MSN, RN, CPNP-PC Ward Family Heart Center
 Regional Prenatal Congenital Heart Disease Detection and Practices Lori Erickson MSN, RN, CPNP-PC Ward Family Heart Center The Children's Mercy Hospital, 2014. 05/14 Objectives Evaluate our regional prenatal
Regional Prenatal Congenital Heart Disease Detection and Practices Lori Erickson MSN, RN, CPNP-PC Ward Family Heart Center The Children's Mercy Hospital, 2014. 05/14 Objectives Evaluate our regional prenatal
Anomalous Systemic Venous Connection Systemic venous anomaly
 World Database for Pediatric and Congenital Heart Surgery Appendix B: Diagnosis (International Paediatric and Congenital Cardiac Codes (IPCCC) and definitions) Anomalous Systemic Venous Connection Systemic
World Database for Pediatric and Congenital Heart Surgery Appendix B: Diagnosis (International Paediatric and Congenital Cardiac Codes (IPCCC) and definitions) Anomalous Systemic Venous Connection Systemic
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Adult Congenital Heart Disease Certification Examination Blueprint
 Adult Congenital Heart Disease Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Adult Congenital Heart Disease Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Outline. Congenital Heart Disease. Special Considerations for Special Populations: Congenital Heart Disease
 Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Devendra V. Kulkarni, Rahul G. Hegde, Ankit Balani, and Anagha R. Joshi. 2. Case Report. 1. Introduction
 Case Reports in Radiology, Article ID 614647, 4 pages http://dx.doi.org/10.1155/2014/614647 Case Report A Rare Case of Pulmonary Atresia with Ventricular Septal Defect with a Right Sided Aortic Arch and
Case Reports in Radiology, Article ID 614647, 4 pages http://dx.doi.org/10.1155/2014/614647 Case Report A Rare Case of Pulmonary Atresia with Ventricular Septal Defect with a Right Sided Aortic Arch and
Advanced Congenital Cardiac Morphology. Sunday, Oct. 22, to Thursday, Oct. 26, Learn more: chop.cloud-cme.com
 Advanced Congenital Cardiac Morphology Sunday, Oct. 22, to Thursday, Oct. 26, 2017 Ruth and Tristram Colket, Jr. Translational Research Building Learn more: chop.cloud-cme.com 1 Course Information Course
Advanced Congenital Cardiac Morphology Sunday, Oct. 22, to Thursday, Oct. 26, 2017 Ruth and Tristram Colket, Jr. Translational Research Building Learn more: chop.cloud-cme.com 1 Course Information Course
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
3/14/2011 MANAGEMENT OF NEWBORNS CARDIAC INTENSIVE CARE CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 WITH HEART DEFECTS
 CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
Curricular Components for Cardiology EPA
 Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Congenital Heart Disease Systematic Interpretation of CT Suhny Abbara, MD
 Congenital Heart Disease Systematic Interpretation of CT Suhny Abbara, MD Chief, Cardiothoracic Imaging Division Professor of Radiology UT Southwestern Medical Center, Dallas, TX Suhny.Abbara@UTSouthwestern.edu
Congenital Heart Disease Systematic Interpretation of CT Suhny Abbara, MD Chief, Cardiothoracic Imaging Division Professor of Radiology UT Southwestern Medical Center, Dallas, TX Suhny.Abbara@UTSouthwestern.edu
Two Cases Report of Scimitar Syndrome: The Classical one with Subaortic Membrane and the Scimitar Variant
 Bahrain Medical Bulletin, Vol.22, No.1, March 2000 Two Cases Report of Scimitar Syndrome: The Classical one with Subaortic Membrane and the Scimitar Variant F Hakim, MD* A Madani, MD* A Abu Haweleh, MD,MRCP*
Bahrain Medical Bulletin, Vol.22, No.1, March 2000 Two Cases Report of Scimitar Syndrome: The Classical one with Subaortic Membrane and the Scimitar Variant F Hakim, MD* A Madani, MD* A Abu Haweleh, MD,MRCP*
Since first successfully performed by Jatene et al, the
 Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
The Double Switch Using Bidirectional Glenn and Hemi-Mustard. Frank Hanley
 The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients
 The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
Down Syndrome Medical Interest Group Friday, 12 June Cardiac Surgery in patients with Down Syndrome
 Down Syndrome Medical Interest Group Friday, 12 June 2015 Cardiac Surgery in patients with Down Syndrome Mr. Attilio Lotto, FRCS CTh Congenital Cardiac Surgeon Cardiac surgery in patients with Down syndrome
Down Syndrome Medical Interest Group Friday, 12 June 2015 Cardiac Surgery in patients with Down Syndrome Mr. Attilio Lotto, FRCS CTh Congenital Cardiac Surgeon Cardiac surgery in patients with Down syndrome
Chest radiographic findings in children with asplenia syndrome
 Asian Biomedicine Vol. 4 No. 4 August 2010; 585-594 Original article Chest radiographic findings in children with asplenia syndrome Panruethai Trinavarat a, Kullana Tantiprawan a, Apichai Khongphatthanayothin
Asian Biomedicine Vol. 4 No. 4 August 2010; 585-594 Original article Chest radiographic findings in children with asplenia syndrome Panruethai Trinavarat a, Kullana Tantiprawan a, Apichai Khongphatthanayothin
I worldwide [ 11. The overall number of transplantations
 Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
An Approach to Cardiac Malposition and the Heterotaxy Syndrome Using 99mTc Sulfur Colloid Imaging
 An Approach to Cardiac Malposition and the Heterotaxy Syndrome Using 99mTc Sulfur Colloid Imaging P. M. FITZER A diagnostic approach to cardiac malposition and the heterotaxy syndrome is outlined. The
An Approach to Cardiac Malposition and the Heterotaxy Syndrome Using 99mTc Sulfur Colloid Imaging P. M. FITZER A diagnostic approach to cardiac malposition and the heterotaxy syndrome is outlined. The
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Hybrid Procedure of Bilateral Pulmonary Artery Banding and Bilateral Ductal Stenting in an Infant With Aortic Atresia and Interrupted Aortic Arch
 Catheterization and Cardiovascular Interventions 84:1157 1162 (2014) Hybrid Procedure of Bilateral Pulmonary Artery Banding and Bilateral Ductal Stenting in an Infant With Aortic Atresia and Interrupted
Catheterization and Cardiovascular Interventions 84:1157 1162 (2014) Hybrid Procedure of Bilateral Pulmonary Artery Banding and Bilateral Ductal Stenting in an Infant With Aortic Atresia and Interrupted
Cardiopulmonary exercise test among children with congenital heart diseases: a multicenter study
 Cardiopulmonary exercise test among children with congenital heart diseases: a multicenter study Pascal AMEDRO, MD, PhD, Arthur Gavotto, MD, Sophie GUILLAUMONT, MD, Stefan MATECKI, MD, PhD Pediatric and
Cardiopulmonary exercise test among children with congenital heart diseases: a multicenter study Pascal AMEDRO, MD, PhD, Arthur Gavotto, MD, Sophie GUILLAUMONT, MD, Stefan MATECKI, MD, PhD Pediatric and
What Can the Database Tell Us About Reoperation?
 AATS/STS Congenital Heart Disease Postgraduate Symposium May 5, 2013 What Can the Database Tell Us About Reoperation? Jeffrey P. Jacobs, M.D. All Children s Hospital Johns Hopkins Medicine The Congenital
AATS/STS Congenital Heart Disease Postgraduate Symposium May 5, 2013 What Can the Database Tell Us About Reoperation? Jeffrey P. Jacobs, M.D. All Children s Hospital Johns Hopkins Medicine The Congenital
Assessing Cardiac Anatomy With Digital Subtraction Angiography
 485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
September 26, 2012 Philip Stockwell, MD Lifespan CVI Assistant Professor of Medicine (Clinical)
 September 26, 2012 Philip Stockwell, MD Lifespan CVI Assistant Professor of Medicine (Clinical) Advances in cardiac surgery have created a new population of adult patients with repaired congenital heart
September 26, 2012 Philip Stockwell, MD Lifespan CVI Assistant Professor of Medicine (Clinical) Advances in cardiac surgery have created a new population of adult patients with repaired congenital heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
Case Report Sinus Venosus Atrial Septal Defect as a Cause of Palpitations and Dyspnea in an Adult: A Diagnostic Imaging Challenge
 Case Reports in Medicine Volume 2015, Article ID 128462, 4 pages http://dx.doi.org/10.1155/2015/128462 Case Report Sinus Venosus Atrial Septal Defect as a Cause of Palpitations and Dyspnea in an Adult:
Case Reports in Medicine Volume 2015, Article ID 128462, 4 pages http://dx.doi.org/10.1155/2015/128462 Case Report Sinus Venosus Atrial Septal Defect as a Cause of Palpitations and Dyspnea in an Adult:
RESULTS OF 102 CASES OF COMPLETE REPAIR OF CONGENITAL HEART DEFECTS IN PATIENTS WEIGHING 700 TO 2500 GRAMS
 RESULTS OF 102 CASES OF COMPLETE REPAIR OF CONGENITAL HEART DEFECTS IN PATIENTS WEIGHING 700 TO 2500 GRAMS V. Mohan Reddy, MD a Doff B. McElhinney, MD a Theresa Sagrado, BA a Andrew J. Parry, MD a David
RESULTS OF 102 CASES OF COMPLETE REPAIR OF CONGENITAL HEART DEFECTS IN PATIENTS WEIGHING 700 TO 2500 GRAMS V. Mohan Reddy, MD a Doff B. McElhinney, MD a Theresa Sagrado, BA a Andrew J. Parry, MD a David
Summary. HVRA s Cardio Vascular Genetic Detailed L2 Obstetrical Ultrasound. CPT 76811, 76825, _ 90% CHD detection. _ 90% DS detection.
 What is the role of fetal echocardiography (2D 76825, cardiovascular color flow mapping 93325) as performed in conjunction with detailed fetal anatomy scan (CPT 76811) now that AIUM requires limited outflow
What is the role of fetal echocardiography (2D 76825, cardiovascular color flow mapping 93325) as performed in conjunction with detailed fetal anatomy scan (CPT 76811) now that AIUM requires limited outflow
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radiofrequency valvotomy in pulmonary atresia Introduction This overview has been prepared
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radiofrequency valvotomy in pulmonary atresia Introduction This overview has been prepared
Surgical Management Of Congenital Heart Disease II: Single Ventricle And Hypoplastic Left Heart Syndrome Aortic Arch Anomalies Septal Defects And...
 Surgical Management Of Congenital Heart Disease II: Single Ventricle And Hypoplastic Left Heart Syndrome Aortic Arch Anomalies Septal Defects And... Of Thoracic Arteries And Veins A Video Manual By Viktor
Surgical Management Of Congenital Heart Disease II: Single Ventricle And Hypoplastic Left Heart Syndrome Aortic Arch Anomalies Septal Defects And... Of Thoracic Arteries And Veins A Video Manual By Viktor
CYANOTIC CONGENITAL HEART DISEASES. PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU
 CYANOTIC CONGENITAL HEART DISEASES PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU DEFINITION Congenital heart diseases are defined as structural and functional problems of the heart that are
CYANOTIC CONGENITAL HEART DISEASES PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU DEFINITION Congenital heart diseases are defined as structural and functional problems of the heart that are
Bidirectional cavopulmonary shunting (BCPS) has
 Development of Pulmonary Arteriovenous Fistulas After Bidirectional Cavopulmonary Shunt Soo Jin Kim, MD, Eun Jung Bae, MD, Do Jun Cho, MD, In Seung Park, MD, Yang Min Kim, MD, Woong-Han Kim, MD, and Seong
Development of Pulmonary Arteriovenous Fistulas After Bidirectional Cavopulmonary Shunt Soo Jin Kim, MD, Eun Jung Bae, MD, Do Jun Cho, MD, In Seung Park, MD, Yang Min Kim, MD, Woong-Han Kim, MD, and Seong
Site of Interstage Care, Resource Utilization, and Interstage Mortality: A Report from the NPC-QIC Registry
 Schidlow et al 1 Site of Interstage Care, Resource Utilization, and Interstage Mortality: A Report from the NPC-QIC Registry David Schidlow Kimberlee Gauvreau Mehul Patel Karen Uzark David W. Brown For
Schidlow et al 1 Site of Interstage Care, Resource Utilization, and Interstage Mortality: A Report from the NPC-QIC Registry David Schidlow Kimberlee Gauvreau Mehul Patel Karen Uzark David W. Brown For
Heart and Lungs. LUNG Coronal section demonstrates relationship of pulmonary parenchyma to heart and chest wall.
 Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Major Infection After Pediatric Cardiac Surgery: External Validation of Risk Estimation Model
 Major Infection After Pediatric Cardiac Surgery: External Validation of Risk Estimation Model Andrzej Kansy, MD, PhD, Jeffrey P. Jacobs, MD, PhD, Andrzej Pastuszko, MD, PhD, Małgorzata Mirkowicz-Małek,
Major Infection After Pediatric Cardiac Surgery: External Validation of Risk Estimation Model Andrzej Kansy, MD, PhD, Jeffrey P. Jacobs, MD, PhD, Andrzej Pastuszko, MD, PhD, Małgorzata Mirkowicz-Małek,
COMPREHENSIVE EVALUATION OF FETAL HEART R. GOWDAMARAJAN MD
 COMPREHENSIVE EVALUATION OF FETAL HEART R. GOWDAMARAJAN MD Disclosure No Relevant Financial Relationships with Commercial Interests Fetal Echo: How to do it? Timing of Study -optimally between 22-24 weeks
COMPREHENSIVE EVALUATION OF FETAL HEART R. GOWDAMARAJAN MD Disclosure No Relevant Financial Relationships with Commercial Interests Fetal Echo: How to do it? Timing of Study -optimally between 22-24 weeks
Glenn and Fontan Caths:
 Glenn and Fontan Caths: Pre-operative evaluation and Trouble-shooting Cavo-Pulmonary Shunts Daniel H. Gruenstein, M.D. Director, Pediatric Interventional Cardiology University of Minnesota Children s Hospital,
Glenn and Fontan Caths: Pre-operative evaluation and Trouble-shooting Cavo-Pulmonary Shunts Daniel H. Gruenstein, M.D. Director, Pediatric Interventional Cardiology University of Minnesota Children s Hospital,
Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION
 Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION Carpentier classification Chauvaud S, Carpentier A. Multimedia Manual of Cardiothoracic Surgery 2007
Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION Carpentier classification Chauvaud S, Carpentier A. Multimedia Manual of Cardiothoracic Surgery 2007
The management of patients born with multiple left heart
 Predictors of Outcome of Biventricular Repair in Infants With Multiple Left Heart Obstructive Lesions Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Tal Geva, MD Background Decisions regarding surgical
Predictors of Outcome of Biventricular Repair in Infants With Multiple Left Heart Obstructive Lesions Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Tal Geva, MD Background Decisions regarding surgical
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy
 Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
Tricuspid Atresia and Single Ventricle
 chapter Definition CONGENITA HEAT DISEASE Tricuspid Atresia and Single Ventricle uc Mertens, Donald J. Hagler, and Marc Gewillig n Univentricular AV connections are hearts in which both atria are joined
chapter Definition CONGENITA HEAT DISEASE Tricuspid Atresia and Single Ventricle uc Mertens, Donald J. Hagler, and Marc Gewillig n Univentricular AV connections are hearts in which both atria are joined
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT
 ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
