Two mechanical techniques have emerged from animal
|
|
|
- Joseph Howard
- 5 years ago
- Views:
Transcription
1 CPR Techniques That Combine Chest and Abdominal Compression and Decompression Hemodynamic Insights From a Spreadsheet Model Charles F. Babbs, MD, PhD Background This study was done to elucidate mechanisms by which newer cardiopulmonary resuscitation (CPR) techniques, including interposed abdominal compression (IAC), active compression-decompression (ACD), and Lifestick CPR, augment systemic perfusion pressure and forward flow and to compare the 3 techniques in the same test system. Methods and Results Mathematical models describing hemodynamics of the adult human circulation during cardiac arrest and CPR were created and exercised by use of spreadsheet software. Assumptions of the models are limited to normal human anatomy and physiology, the definition of compliance (volume change/pressure change), and Ohm s law (flow pressure/resistance). Standard CPR generates 1.3 L/min forward and 25 mm Hg systemic perfusion pressure. In otherwise identical models, IAC-CPR generates 2.4 L/min and 45 mm Hg; ACD-CPR, 1.6 L/min and 30 mm Hg; and Lifestick CPR, which combines IAC and ACD, 3.1 L/min and 58 mm Hg. Augmented CPR techniques work by enhanced priming of either chest or abdominal pump mechanisms. Conclusions Adjunctive maneuvers, combined with conventional chest compression, can produce substantial hemodynamic benefit in CPR by credible physiological mechanisms. (Circulation. 1999;100; ) Key Words: blood flow cardiopulmonary resuscitation computers heart arrest Lifestick mechanics Two mechanical techniques have emerged from animal and clinical studies as potentially effective means of augmenting perfusion during external cardiopulmonary resuscitation (CPR). The first is the addition of interposed abdominal compression (IAC) to otherwise standard CPR. 1 3 The second is CPR with active compression and decompression (ACD) of the chest. 4 6 Reviews of these techniques are found in References 7 and 8. During IAC-CPR, positive pressure is applied to the abdomen in counterpoint to the rhythm of chest compression, so that the abdomen is being compressed when chest pressure is relaxed. During ACD- CPR, positive and negative pressures are applied alternately to the chest by means of a plunger that forms a seal with the anterior chest wall. Both methods improve hemodynamics in animal studies of electrically induced ventricular fibrillation. 9,10 Both improve CO 2 excretion as a measure of effective systemic perfusion in human resuscitation. 4,11,12 Three randomized clinical trials of IAC-CPR compared with standard CPR 2,11,13 have found statistically significant benefit, and 1 early trial found no difference. 14 Four randomized clinical trials of ACD-CPR have found improved outcome, 5,6,15,16 and 4 other trials have found no difference Most recently, Lifestick CPR 21 has become the subject of active research. The Lifestick is a 2-handled device that is able to apply IAC and ACD-CPR simultaneously by alternately compressing and decompressing the chest and the abdomen through adhesive pads. These 3 CPR adjuncts are illustrated in Figure 1. Using a mathematical model of CPR hemodynamics, the nomenclature for which is given in Table 1, the author has explored the possibility that IAC, ACD-CPR, and Lifestick CPR work by similar mechanisms. The hypothesis is that improved filling of the thoracic aorta and right heart can be accomplished either by positive pressure in the abdomen or by negative pressure in the chest and conversely, that improved filling of the abdominal aorta can be achieved either by positive pressure in the chest or by negative pressure in the abdomen. Improved pump filling, in turn, leads to higher stroke output, systemic perfusion pressure, and systemic blood flow. The approach to the present research was to create and test a mathematical model of CPR hemodynamics based on fundamental principles of cardiovascular physiology. Such a model is independent of the many confounding factors present in laboratory studies and in clinical trials. These include varying patient populations, downtime, drug therapy, central venous pressure, peripheral vascular resistance, underlying disease, chest configuration, and body size, as well as varying rescuer size, skill, strength, consistency, prior Received April 20, 1999; revision received June 29, 1999; accepted July 9, From Indiana University School of Medicine and the Department of Basic Medical Sciences, Purdue University, West Lafayette, Ind. Correspondence to Charles F. Babbs, MD, PhD, Basic Medical Sciences, 1246 Lynn Hall, Purdue University, West Lafayette, IN babbs@vet.purdue.edu 1999 American Heart Association, Inc. Circulation is available at
2 Babbs Newer CPR Techniques 2147 TABLE 1. Nomenclature Figure 1. Schematics of 3 modified CPR techniques. training, and bias. Mathematical models also allow exact control of the dominant hemodynamic mechanism of CPR (thoracic pump in large subjects versus cardiac pump in small subjects). 22 This approach facilitates quantitative comparison of various resuscitation techniques in exactly the same test system. Methods Anatomic Parameters To capture the essence of CPR hemodynamics, one may solve the family of differential equations describing pressures and flows in the simplified fluidic system shown in Figure 2. The human circulation is represented by 7 compliant chambers connected by resistances through which blood may flow. The compliances correspond to the thoracic aorta, abdominal aorta, lumped superior vena cava and right heart, lumped abdominal and lower extremity veins, carotid arteries, and jugular veins. In addition, the chest compartment contains a pump representing the pulmonary vascular and left heart compliances between the pulmonic valve and the aortic valve. This pump may be configured to function either as a heartlike cardiac pump, in which applied pressure squeezes blood from the heart itself through the aortic valve, or as a global thoracic pressure pump, in which applied pressure squeezes blood from the pulmonary vascular bed through the left heart and into the periphery Conductance pathways with nonzero resistances, R, connect the elastic compartments. R h,r ht, and R s are large and represent resistances of the systemic vascular beds of the head, heart, and trunk and legs. R c, R a,r j, and R v are small and represent in-line resistances of the great vessels. R i and R o are the small input and output resistances of the chest pump in series with the aortic and pulmonic valves. Niemann s valves between the chest and jugular veins at the level of the thoracic inlet are actual but little-known anatomic structures that function to block headward transmission of large positive pressure pulses in the chest during cough and also during CPR. 26 Symbol Definition (and Units) Subscripts AA Abdominal aorta Ao Thoracic aorta a Aorta at level of diaphragm C, car Carotid h Head J, jug Jugular IVC Inferior vena cava RH Right heart and superior vena cava ht Heart i Input to pump o Output from pump P Pump s Systemic circulation below diaphragm v Portal and systemic veins at level of diaphragm Variables C Compliance, L/mm Hg or ml/mm Hg E Pump ejection valve (1 open, 0 closed) F Pump filling valve (1 open, 0 closed) i Flow or current between compartments, L/s or L/min N Niemann s valve (1 open, 0 closed) P Instantaneous pressure in a compartment, mm Hg P Pressure increment, mm Hg, during time t R Resistance, mm Hg/(L/s) t Time during a cycle of CPR, s t Time increment, s Tpfactor Thoracic pump factor (0 1) Angular frequency for sine function, radians/s Physiological Parameters Parameters describing a textbook normal 70-kg man 27 (Table 2) are used to specify values of the compliances and resistances shown in Figure 2. The normal 30-fold ratio of venous to arterial compliance characterizes a circulation in the absence of fluid loading or congestive heart failure. The distribution of vascular conductances (1/resistance) into cranial, thoracic, and caudal components reflects textbook distributions of cardiac output to various body regions. Solving for Pressures in the System The relationships among the pressures in the various vascular compartments are determined by the definition of compliance and by Ohm s law. The definition of compliance is C V/ P, where C is compliance and P is the incremental change in pressure within a compartment as volume V is introduced. Ohm s law, which relates flow to pressure and resistance, is i (1/R)(P 1 P 2 ), where P 1 P 2 is the instantaneous change in pressure across resistance R as flow i occurs. In Figure 2, currents i c (carotid), i a (aortic), i s (systemic), i v (venous), i j (jugular), i i (pump input), and i o (pump output) are shown for clarity, with positive directions specified by arrows. Extrathoracic Components Applying these basic concepts with reference to Figure 2 provides a set of governing finite-difference equations that can be used to describe hemodynamics. These equations can be integrated numerically to describe instantaneous pressure versus time waveforms in each of the 7 compartments. Beginning, for example, with the abdominal aorta,
3 2148 Circulation November 23, 1999 Figure 2. Model of human circulatory system. Variables are defined in Table 1. (1) P AA P abd 1 C a s t AA P abd t C AA 1 P R Ao P AA 1 P a R AA P IVC s. Here, P abd represents the change in external pressure applied to vessels in the abdominal compartment during IAC and Lifestick CPR. For standard CPR, P abd is assumed to be zero. The next term represents the increase in abdominal aortic pressure caused by net inflow of blood during the small time interval t. Substitution for currents i a and i s by use of Ohm s law completes the expression. Similarly, the pressure changes in other extrathoracic vascular compartments are given by Equations 2 through 4, as follows. (2) P IVC P abd 1 C s v t IVC TABLE 2., P abd t C IVC 1 P R AA P IVC 1 P s R IVC P RH v Nominal Normal Values of Model Parameters Parameter Symbol Value Compliances, L/mm Hg Thoracic aortic Cao Chest pump Cp Right heart and superior vena cava Crh Abdominal aorta Caa Inferior vena cava Civc Carotid artery Ccar Jugular veins Cjug Resistances, mm Hg/(L/sec) Pump output (aortic valve) Ro 10 Pump input (tricuspid valve) Ri 10 Carotid arteries Rc 60 Head arm resistance Rh 4470 Jugular veins Rj 30 Aorta Ra 25 Subphrenic vena cava Rv 25 Subphrenic organs Rs 1704 Coronary vessels Rht Peak applied pressures, mm Hg Chest compression Pmaxch 60 Chest decompression Pmaxacd 20 Abdominal compression Pmaxiac 110 Abdominal decompression Pmaxaad 30 (3) P car 1 C car c h t and t C car 1 R c P Ao P car 1 R h P car P jug (4) P jug 1 C jug h j t t C jug 1 P R car P jug N 1 P h R jug P RH j where N 1 normally and N 0 during cough or intrathoracic pressure pulses (when P RH P jug ). Thoracic Components Corresponding expressions for the 3 thoracic components of the model are as follows. (5) P Ao P chest 1 C o c a ht t Ao,, P chest t C Ao E 1 P R P P Ao 1 P o R Ao P car c 1 P R Ao P AA 1 P a R Ao P RH ht, where E 1 during ejection (aortic valve open) and E 0 otherwise. (6) P RH P chest 1 C j v ht i t RH P chest t C RH N 1 P R jug P RH 1 P j R IVC P RH v 1 P R Ao P RH F 1 P ht R RH P P i, where F 1 during the filling phase (pulmonic valve open) and F 0 otherwise, and N 0 during CPR-induced intrathoracic pressure pulses (Niemann s valve closed) and N 1 otherwise. Finally, (7) P P P chest 1 C P i o t P chest t C P F 1 R i P RH P P E 1 R o P P P Ao Numerical Methods Integration Standard spreadsheet programs, such as Microsoft Excel, are ideal for implementing numerical integration of Equations 1 through 7 to obtain pressures in all 7 compartments as a function of time. To simulate a resuscitation, one can create a spreadsheet in which pressures in each compartment at any point in time are computed from the pressures at the preceding time point and the corresponding P s that is, (8) P(t t) P(t) P(t). One begins with a uniform pressure of 10 mm Hg in all compartments of the arrested circulation and applies phased external pressure pulses to the chest and abdominal compartments, as desired. The incremental changes in compartment pressure computed from Equations 1 through 7 are used to construct a marching solution for successive small increments of time, t, typically to second. Use of a time increment that is too coarse results in unstable oscillations of computed pressures. Decreasing the value of t, however, can always return stability. In the models used for the.
4 Babbs Newer CPR Techniques 2149 Figure 3. Driving pressure waveforms for phased chest and abdominal compression and decompression. Pchest is positive chest compression; Pacd, active chest decompression; Pabd, positive abdominal compression; and Paad, active abdominal decompression. present research, each row of the spreadsheet represents a time point. Pressures for row n 1 are computed from values in row n by use of Equation 8 and compartmental P values from Equations 1 through 7. At a minimum, 15 columns are needed to represent time from the onset of CPR, absolute pressures P 1 through P 7 in the 7 compartments of the model, and incremental pressures P 1 through P 7. For convenience, it is useful also to include columns for systemic perfusion pressure; the applied pressure waveform; the sine function, sin( t); P chest ; and P abd. Applied Pressures for Chest and Abdominal Compression P chest and P abd represent driving intrathoracic and intraabdominal pressures applied to outer surfaces of blood vessels in the chest and abdomen of the model. Although any arbitrary function or waveform can be used to represent the imposed chest and abdominal pressures in external CPR, the present studies used half-sinusoidal functions, defined as follows and sketched in Figure 3. To represent chest compression, (9) P chest (t) max 0, sin t P maxchest. If IAC-CPR is being simulated, then (10) P abd (t) max 0, sin t P maxabd, and if active compression-decompression CPR is being simulated, (11) P acd (t) min 0, sin t P maxacd. In simulations of abdominal decompression during 4-phase Lifestick CPR, (12) P aad (t) min 0, sin t P maxaad. Thoracic Versus Cardiac Chest Pump Mechanisms To explore the influence of the thoracic pump versus the cardiac pump mechanisms that can impel blood during cardiac arrest and chest compression, a factor 0 Tpfactor 1 is introduced, and a pressure equal to the product of P chest and Tpfactor is applied to the thoracic aorta and superior vena cava to create a continuum of hybrid pump mechanisms ranging from pure cardiac pump (Tpfactor 0) to pure thoracic pump (Tpfactor 1). When Tpfactor 1, all intrathoracic structures, including the great veins and thoracic aorta, experience a uniform global intrathoracic pressure rise, as originally conceived by Rudikoff and coworkers. 28 When Tpfactor 0, only the pump compliance, C P, is pressurized, as if the heart alone, and not the great vessels, were compressed between the sternum and the spine, as originally conceived by Kouwenhoven et al. 29 Intermediate values of the thoracic pump factor allow models approximating the present understanding, 25,30,31 in which for small animals and children, blood is impelled in external CPR predominantly by the cardiac pump mechanism (for example, Tpfactor 0.25), whereas in larger animals and adult humans, blood is impelled predominantly by the thoracic pump mechanism (for example, Tpfactor 0.75). Test Cases and Validation The spreadsheet code was validated by solution of 12 simple test cases for very small or very large values of the resistances and compliances and by establishment of a model of the normal adult circulation using Tpfactor 0. This model had an aortic blood pressure of 120/82 mm Hg and a cardiac output of 4.9 L/min for a heart rate of 80 bpm, closely approximating the textbook normal values of 120/80 mm Hg and 5.0 L/min. Results Alternative CPR Methods in Adult Human Models Figure 4a, 4b, and 4c illustrates 5-channel pressure records after 20 cycles of CPR for the normal human circulatory model as shown in Table 2 during a simulation of continuous standard CPR, IAC-CPR, or ACD-CPR, respectively. In Figure 4, the peak positive abdominal pressure for IAC-CPR is 110 mm Hg, and the maximal negative intrathoracic pressure for ACD-CPR is 20 mm Hg, approximating published values for the 2 techniques. 1,2,32 35 In this model, the thoracic pump factor is 0.75 to simulate an adult patient in whom the thoracic pump mechanism is dominant but there is some degree of selective cardiac compression. 25 The parameters in Table 2 were used for this and all subsequent simulations, unless explicitly stated otherwise. Figure 4a illustrates steady-state pressures generated by standard CPR.
5 2150 Circulation November 23, 1999 Figure 4. Detailed pressures of known CPR modalities in a mathematical model. Steady-state pressures after 20 compression cycles are shown. Thoracic pump factor is Peak applied pressures as in Table 2. Compression rate is 90/min. a, Standard CPR; b, IAC- CPR; c, ACD-CPR; and d, 4-phase Lifestick CPR. SPP P Ao P RH is mean systemic perfusion pressure in mm Hg. Flow is forward flow in L/min. See Table 1 for abbreviations. IAC-CPR Comparison of the pressure waveforms in Figure 4a and 4b shows the mechanism of 110 mm Hg interposed abdominal compression CPR. The abdominal venous pressure pulse induces increased right heart filling pressure during IAC and consequent faster pump emptying during chest compression compared with standard CPR. Faster pump filling is caused by larger pressure gradients across the input valve from times 0.54 to 0.67 second of the cycle. Faster pump emptying is caused by the Starling characteristic of the pump associated with greater filling and, in turn, larger pressure gradients across the aortic valve during ejection. With the addition of IAC, cardiac output increases from 1.3 to 2.4 L/min, and mean systemic perfusion pressure (SPP R Ao R RH ) increases from 25 to 45 mm Hg compared with standard CPR. The abdominal aortic pressure waveform (crosses in figure) leads the thoracic aortic pressure waveform (squares) during the onset and peak of IAC, indicating retrograde flow in the aorta. This action is similar to that of an intra-aortic balloon pump. ACD-CPR Figure 4c shows steady-state pressure waveforms for 20 mm Hg ACD-CPR. Reduced pump pressure (pulmonary vascular pressure) during diastole promotes faster pump filling from 0.45 to 0.60 second into the cycle. Cardiac output is increased from 1.3 to 1.6 L/min, and mean systemic perfusion pressure is increased from 25 to 30 mm Hg compared with standard CPR. The ACD-induced decrease in central venous pressure offsets the ACD-induced decrease in thoracic aortic pressure, so that augmented perfusion pressure is maintained.
6 Babbs Newer CPR Techniques 2151 Figure 5. Mean systemic perfusion pressure (SPP) generated by standard and augmented CPR techniques in models with varying mechanisms of blood flow. Effects of chest compression vary according to the thoracic pump factor, ranging from 0 (no compression of the thoracic aorta and superior vena cava) to 1.0 (same pressure applied to the thoracic aorta and superior vena cava as is applied to the heart). The effects on systemic perfusion pressure of IAC and ACD are similar to those reported for studies in experimental animals and in human patients. 1,32,36 39 Compared with standard CPR, 110 mm Hg IAC produced an 85% increase in total flow. In the same model, 20 mm Hg ACD produced a 23% increase in total flow. The present results in an independent mathematical model confirm that the positive findings in animal studies and most clinical studies are valid and are based on the fundamental anatomy and physiology of the circulatory system. Four-Phase Lifestick CPR Although less well studied, Lifestick CPR is a recently developed technique to combine the effects of IAC and ACD. The sticky, self-adhesive compression pads of the Lifestick permit active compression and decompression of both the chest and the abdomen. Accurate simulation of Lifestick CPR is difficult, because actual values of negative intra-abdominal pressure have not yet been reported. If one estimates maximal decompression-phase pressure in the abdomen to be 30 mm Hg, the results in Figure 4d are obtained. With this possible 4-phase technique, mean systemic perfusion pressure is 58 mm Hg. Total forward flow is 3.1 L/min 2.5 times that of standard CPR. Study of the pressure waveforms in Figure 4d reveals that in 4-phase CPR, negative inferior vena cava pressure draws blood out of the chest from 0 to 0.3 second into the cycle, widening the systemic perfusion pressure. Positive inferior vena cava pressure from 0.33 to 0.67 second promotes excellent pump filling. Influence of Chest Pump Mechanisms Systemic perfusion pressures obtained by chest and abdominal compression are dependent on the degree to which blood is impelled by cardiac compression versus global intrathoracic pressure fluctuation. In Figure 5, mean systemic perfusion pressure is plotted as a function of the thoracic pump factor for 4 possible CPR techniques: standard, IAC, ACD, and 4-phase Lifestick CPR. Maximal compression or decompression pressures are those listed in Table 2. Although perfusion pressures for the augmented CPR techniques are always better than those for standard CPR, the ratios of experimental to standard perfusion pressures vary with the thoracic pump factor. The relative benefit of IAC-CPR compared with standard CPR, evident in Figure 5, appears to be greater in a pure thoracic pump model than in a pure cardiac pump model. Conversely, the relative benefit of ACD-CPR appears to be greater in a pure cardiac pump model. The apparent benefit of ACD-CPR is especially model-dependent and may be greater in small-animal models, such as beagles, which permit more cardiac compression, than in larger-animal models, including humans. This effect might well explain the generally more dramatic and favorable results with ACD in animal models compared with the overall mixed results observed in humans. 8 Discussion Mathematical models provide a good way to synthesize knowledge about complex systems in new and interesting ways and to explore assumptions about how the systems operate. The present mathematical model provides an independent test confirming the efficacy of adjunctive diastolicphase maneuvers to augment perfusion during CPR. It offers a convenient and low-cost way to compare various CPR adjuncts in exactly the same test system, eliminating the need to extrapolate published results from one animal or clinical model to another. The results confirm that compression and decompression of either the chest or the abdomen can move blood in cardiac arrest. Importantly, the positive effects of IAC-CPR, ACD-CPR, and 4-phase Lifestick CPR can be predicted from fundamental principles of cardiovascular physiology the definition of compliance and Ohm s law. Analysis of pressure waveforms suggests that these techniques function primarily by pump priming. In IAC-CPR, the chest pump is primed by positive pressure in the abdomen during thoracic recoil. In ACD-CPR, the chest pump is primed by negative diastolic pressure in the chest that draws blood centrally from extra-thoracic veins. In 4-phase Lifestick CPR, these effects are combined so that negative thoracic and positive abdominal pressures prime the chest pump. In turn, positive thoracic and negative abdominal pressures prime the abdominal pump. Conclusions The present mathematical model, based on fundamental aspects of cardiovascular physiology, provides a recapitulation and synthesis of abundant experimental and clinical evidence suggesting that adjunctive compression and decompression of the chest and abdomen can improve current standard CPR. Systemic perfusion pressure achievable with IAC alone is approximately double that of standard CPR. Systemic perfusion pressure achievable with full 4-phase CPR might possibly exceed 3-fold that of current standard CPR. Improved perfusion during IAC-CPR may not necessarily lead to better long-term survival, especially when the underlying rhythm is asystole or electromechanical dissociation. 13 For the fraction of cardiac arrest victims who can be saved, however, these techniques, performed by trained healthcare providers, are valid and practical alternatives to standard CPR and have a rational place in resuscitation protocols of the 21st century.
7 2152 Circulation November 23, 1999 References 1. Ralston SH, Babbs CF, Niebauer MJ. Cardiopulmonary resuscitation with interposed abdominal compression in dogs. Anesth Analg. 1982;61: Sack JB, Kesselbrenner MB, Bregman D. Survival from in-hospital cardiac arrest with interposed abdominal counterpulsation during cardiopulmonary resuscitation. JAMA. 1992;267: Sack JB, Kesselbrenner MB. Hemodynamics, survival benefits, and complications of interposed abdominal compression during cardiopulmonary resuscitation. Acad Emerg Med. 1994;1: Cohen TJ, Tucker KJ, Lurie KG, Redberg RF, Dutton JP, Dwyer KA, Schwab TM, Chin MC, Gelb AM, Scheinman MM, Cardiopulmonary Resuscitation Working Group. Active compression-decompression: a new method of cardiopulmonary resuscitation. JAMA. 1992;267: Lurie KG, Shultz JJ, Callaham ML, Schwab TM, Gisch T, Rector T, Frascone RJ, Long L. Evaluation of active compression-decompression CPR in victims of out-of-hospital cardiac arrest. JAMA. 1994;271: Plaisance P, Adnet F, Vicaut E, Hennequin B, Magne P, Prudhomme C, Lambert Y, Cantineau JP, Leopold C, Ferracci C, Gizzi M, Payen D. Benefit of active compression-decompression cardiopulmonary resuscitation as a prehospital advanced cardiac life support: a randomized multicenter study. Circulation. 1997;95: Babbs CF, Tacker WA. Cardiopulmonary resuscitation with interposed abdominal compression. Circulation. 1986;74(suppl IV):IV37 IV Wik L, Mauer D, Robertson C. The first European pre-hospital active compression-decompression (ACD) cardiopulmonary resuscitation workshop: a report and a review of ACD-CPR. Resuscitation. 1995;30: Einagle V, Bertrand F, Wise RA, Roussos C, Madger S. Interposed abdominal compressions and carotid blood flow during cardiopulmonary resuscitation: support for a thoracoabdominal unit. Chest. 1988;93: Lindner KH, Ahnefeld FW, Bowdler IM. Cardiopulmonary resuscitation with interposed abdominal compression after asphyxial or fibrillatory cardiac arrest in pigs. Anesthesiology. 1990;72: Ward KR, Sullivan RJ, Zelenak RR, Summer WR. A comparison of interposed abdominal compression CPR and standard CPR by monitoring end-tidal PCO2. Ann Emerg Med. 1989;18: Orliaguet GA, Carli PA, Rozenberg A, Janniere D, Sauval P, Delpech P. End-tidal carbon dioxide during out-of-hospital cardiac arrest resuscitation: comparison of active compression-decompression and standard CPR. Ann Emerg Med. 1995;25: Sack JB, Kesselbrenner MB, Jarrad A. Interposed abdominal compression CPR and resuscitation outcome during asystole and electromechanical dissociation. Circulation. 1992;86: Mateer JR, Steuven HA, Thompson BM, Aprahamian C, Darin J. Prehospital IAC-CPR versus standard CPR: paramedic resuscitation of cardiac arrests. Am J Emerg Med. 1985;3: Cohen TJ, Goldner BG, Maccaro PC, Ardito AP, Trazzera S, Cohen MB, Dibs SR. A comparison of active compression-decompression cardiopulmonary resuscitation with standard cardiopulmonary resuscitation for cardiac arrests occurring in the hospital. N Engl J Med. 1993;329: Tucker KJ, Galli F, Savitt MA, Kahsai D, Bresnahan L, Redberg RF. Active compression-decompression resuscitation: effect on resuscitation success after in-hospital cardiac arrest. J Am Coll Cardiol. 1994;24: Luiz T, Ellinger K, Denz C. Active compression-decompression cardiopulmonary resuscitation does not improve survival in patients with prehospital cardiac arrest in a physician-manned emergency medical system. J Cardiothorac Vasc Anesth. 1996;10: Schwab TM, Callaham ML, Madsen CD, Utecht TA. A randomized clinical trial of active compression-decompression CPR vs. standard CPR in out-of-hospital cardiac arrest in two cities. JAMA. 1995;273: Stiell IG, Hebert PC, Wells GA, Laupacis A, Vandemheen K, Dreyer JF, Eisenhauer MA, Gibson J, Higginson LA, Kirby AS, Mahon JL, Maloney JP, Weitzman BN. The Ontario trial of active compressiondecompression cardiopulmonary resuscitation for in-hospital and prehospital cardiac arrest. JAMA. 1996;275: Mauer D, Schneider T, Dick W, Withelm A, Elich D, Mauer M. Active compression-decompression resuscitation: a prospective, randomized study in a two-tiered EMS system with physicians in the field. Resuscitation. 1996;33: Tang W, Weil MH, Schock RB, Sato Y, Lucas J, Sun S, Bisera J. Phased chest and abdominal compression-decompression: a new option for cardiopulmonary resuscitation. Circulation. 1997;95: Babbs CF, Tacker WA, Paris RL, Murphy RJ, Davis RW. Cardiopulmonary resuscitation with simultaneous compression and ventilation at high airway pressure in 4 animal models. Crit Care Med. 1982;10: Babbs CF. New versus old theories of blood flow during cardiopulmonary resuscitation. Crit Care Med. 1980;8: Weisfeldt ML, Chandra N. Physiology of cardiopulmonary resuscitation. Annu Rev Med. 1981;32: Chandra NC. Mechanisms of blood flow during CPR. Ann Emerg Med. 1993;22: Niemann JT, Ung S, Rosborough JP, Suzuki J, Criley JM. Preferential brachiocephalic flow during CPR a hemodynamic explanation. Circulation. 64(IV). 1981;64(suppl IV):IV Hamilton WF, Dow P, eds. Handbook of Physiology, Volume 2, Section 2: Circulation. Washington DC: American Physiological Society; Rudikoff MT, Maughan WL, Effron M, Freund P, Weisfeldt ML. Mechanisms of blood flow during cardiopulmonary resuscitation. Circulation. 1980;61: Kouwenhoven WB, Jude JR, Knickerbocker GG. Closed-chest cardiac massage. JAMA. 1960;173: Paradis NA, Martin GB, Goetting MG, Rosenberg JM, Rivers EP, Appleton TJ, Nowak RM. Simultaneous aortic, jugular bulb, and right atrial pressures during cardiopulmonary resuscitation in humans: insights into mechanisms. Circulation. 1989;80: Halperin HR, Tsitlik JE, Guerci AD, Mellits ED, Levin HR, Shi AY, Chandra N, Weisfeldt ML. Determinants of blood flow to vital organs during cardiopulmonary resuscitation in dogs. Circulation. 1986;73: Voorhees WD, Niebauer MJ, Babbs CF. Improved oxygen delivery during cardiopulmonary resuscitation with interposed abdominal compressions. Ann Emerg Med. 1983;12: Wik L, Naess PA, Ilebekk A, Nicolaysen G, Steen PA. Effects of various degrees of compression and active decompression on haemodynamics, end-tidal CO 2, and ventilation during cardiopulmonary resuscitation of pigs. Resuscitation. 1996;31: Sunde K, Wik L, Naess PA, Ilebekk A, Nicolaysen G, Steen PA. Effect of different compression-decompression cycles on haemodynamics during ACD-CPR in pigs. Resuscitation. 1998;36: Chang MW, Coffeen P, Lurie KG, Shultz J, Bache RJ, White CW. Active compression-decompression CPR improves vital organ perfusion in a dog model of ventricular fibrillation. Chest. 1994;106: Berryman CR, Phillips GM. Interposed abdominal compression-cpr in human subjects. Ann Emerg Med. 1984;13: Shultz JJ, Coffeen P, Sweeney M, Detloff B, Kehler C, Pineda E, Yakshe P, Adler SW, Chang M, Lurie KG. Evaluation of standard and active compression-decompression CPR in an acute human model of ventricular fibrillation. Circulation. 1994;89: Guly UM, Robertson CE. Active decompression improves the haemodynamic state during cardiopulmonary resuscitation. Br Heart J. 1995; 73: Malzer R, Zeiner A, Binder M, Domanovits H, Knappitsch G, Sterz F, Laggner AN. Hemodynamic effects of active compressiondecompression after prolonged CPR. Resuscitation. 1996;31:
Purdue e-pubs. Purdue University. Charles F. Babbs Purdue University, Weldon School of Biomedical Engineering Faculty Publications
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2000 Efficacy of interposed abdominal compressioncardiopulmonary resuscitation
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2000 Efficacy of interposed abdominal compressioncardiopulmonary resuscitation
A dose-response curve for the negative bias pressure of an intrathoracic pressure regulator during CPR
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 10-2005 A dose-response curve for the negative bias pressure of an intrathoracic
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 10-2005 A dose-response curve for the negative bias pressure of an intrathoracic
Preclinical Studies of Abdominal Counterpulsation in CPR
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1984 Preclinical Studies of Abdominal Counterpulsation in CPR Charles
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1984 Preclinical Studies of Abdominal Counterpulsation in CPR Charles
Relative effectiveness of interposed abdominal compression CPR: sensitivity analysis and recommended compression rates
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2005 elative effectiveness of interposed abdominal compression P: sensitivity
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2005 elative effectiveness of interposed abdominal compression P: sensitivity
Mechanical devices for cardiopulmonary resuscitation Jane G. Wigginton, Adam H. Miller, Fernando L. Benitez and Paul E. Pepe
 Mechanical devices for cardiopulmonary resuscitation Jane G. Wigginton, Adam H. Miller, Fernando L. Benitez and Paul E. Pepe Purpose of the review For over 40 years, manual chest compressions have been
Mechanical devices for cardiopulmonary resuscitation Jane G. Wigginton, Adam H. Miller, Fernando L. Benitez and Paul E. Pepe Purpose of the review For over 40 years, manual chest compressions have been
Methods for Calculating Coronary Perfusion Pressure During CPR
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 9-2009 Methods for Calculating Coronary Perfusion Pressure During CPR
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 9-2009 Methods for Calculating Coronary Perfusion Pressure During CPR
A new cardiopulmonary resuscitation method using only rhythmic abdominal compression A preliminary report B
 American Journal of Emergency Medicine (2007) 25, 786 790 www.elsevier.com/locate/ajem Original Contribution A new cardiopulmonary resuscitation method using only rhythmic abdominal compression A preliminary
American Journal of Emergency Medicine (2007) 25, 786 790 www.elsevier.com/locate/ajem Original Contribution A new cardiopulmonary resuscitation method using only rhythmic abdominal compression A preliminary
Therapeutic hypothermia Transcutaneous pacing Sodium bicarbonate Rx Calcium, Magnesium Fluids and Pressors Antiarrhythmic Rx Epi/Vasopressin O 2
 Resuscitation Arsenal Therapeutic hypothermia Transcutaneous pacing Sodium bicarbonate Rx Calcium, Magnesium Fluids and Pressors Antiarrhythmic Rx Epi/Vasopressin O 2 /intubation Shock CPR ` 1994-96 Standing
Resuscitation Arsenal Therapeutic hypothermia Transcutaneous pacing Sodium bicarbonate Rx Calcium, Magnesium Fluids and Pressors Antiarrhythmic Rx Epi/Vasopressin O 2 /intubation Shock CPR ` 1994-96 Standing
Theoretically Optimal Duty Cycles for Chest and Abdominal Compression during External Cardiopulmonary Resuscitation
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1995 Theoretically Optimal Duty Cycles for Chest and Abdominal Compression
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1995 Theoretically Optimal Duty Cycles for Chest and Abdominal Compression
DEVICE DURING STANDARD ACTIVE DECOMPRESSION
 USE OF AN IMPEDANCE THRESHOLD DEVICE DURING STANDARD AND/OR ACTIVE COMPRESSION DECOMPRESSION ITD Bibliography 1. Aufderheide TP, Pirrallo RG, et al. Clinical evaluation of an inspiratory impedance threshold
USE OF AN IMPEDANCE THRESHOLD DEVICE DURING STANDARD AND/OR ACTIVE COMPRESSION DECOMPRESSION ITD Bibliography 1. Aufderheide TP, Pirrallo RG, et al. Clinical evaluation of an inspiratory impedance threshold
CIRCULATORY ADJUNCTS. Newer Methods of Cardiopulmonary Resuscitation. Charles F. Babbs, MD, PhD
 EMERGENCY CARDIOVASCULAR CARE 0733 8651/02 $15.00.00 CIRCULATORY ADJUNCTS Newer Methods of Cardiopulmonary Resuscitation Charles F. Babbs, MD, PhD Conventional cardiopulmonary resuscitation what has come
EMERGENCY CARDIOVASCULAR CARE 0733 8651/02 $15.00.00 CIRCULATORY ADJUNCTS Newer Methods of Cardiopulmonary Resuscitation Charles F. Babbs, MD, PhD Conventional cardiopulmonary resuscitation what has come
haemodynamic state during cardiopulmonary
 372 Br HeartJ_ 1995;73372-376 TECHNIQUE Department of Accident and Emergency Medicine, Royal Infirmary of Edinburgh, Edinburgh U M Guly C E Robertson Correspondence to Miss U M Guly, Department of Accident
372 Br HeartJ_ 1995;73372-376 TECHNIQUE Department of Accident and Emergency Medicine, Royal Infirmary of Edinburgh, Edinburgh U M Guly C E Robertson Correspondence to Miss U M Guly, Department of Accident
WORKSHEET for Evidence-Based Review of Science for Veterinary CPR
 RECOVER 2011 1 of 9 WORKSHEET for Evidence-Based Review of Science for Veterinary CPR 1. Basic Demographics Worksheet author(s) Jennifer Hess Date Submitted for review: August 14, 2011 Mailing address:
RECOVER 2011 1 of 9 WORKSHEET for Evidence-Based Review of Science for Veterinary CPR 1. Basic Demographics Worksheet author(s) Jennifer Hess Date Submitted for review: August 14, 2011 Mailing address:
Myocardial Perfusion Pressure: A Predictor of 24Hour Survival During Prolonged Cardiac Arrest in Dogs
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1988 Myocardial Perfusion Pressure: A Predictor of 24Hour Survival During
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1988 Myocardial Perfusion Pressure: A Predictor of 24Hour Survival During
Interposed abdominal compression as an adjunct to cardiopulmonary resuscitation
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1994 Interposed abdominal compression as an adjunct to cardiopulmonary
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1994 Interposed abdominal compression as an adjunct to cardiopulmonary
The potential value of increasing negative intrathoracic
 Optimizing Standard Cardiopulmonary Resuscitation With an Inspiratory Impedance Threshold Valve* Keith G. Lurie, MD; Katherine A. Mulligan, BA; Scott McKnite, BS; Barry Detloff, BA; Paul Lindstrom, BS;
Optimizing Standard Cardiopulmonary Resuscitation With an Inspiratory Impedance Threshold Valve* Keith G. Lurie, MD; Katherine A. Mulligan, BA; Scott McKnite, BS; Barry Detloff, BA; Paul Lindstrom, BS;
Effect of thoracic venting on arterial pressure, and flow during external cardiopulmonary resuscitation in animals
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1981 Effect of thoracic venting on arterial pressure, and flow during
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1981 Effect of thoracic venting on arterial pressure, and flow during
Abdominal Binding and Counterpulsation in Cardiopulmonary Resuscitation
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1986 Abdominal Binding and Counterpulsation in Cardiopulmonary Resuscitation
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1986 Abdominal Binding and Counterpulsation in Cardiopulmonary Resuscitation
The Case for Inteposed Abdominal Compression CPR in Hospital Settings
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2013 The Case for Inteposed Abdominal Compression CPR in Hospital Settings
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2013 The Case for Inteposed Abdominal Compression CPR in Hospital Settings
More Than A Heartbeat
 More Than A Heartbeat Improve Perfusion During CPR Today, only a small number of out of hospital cardiac arrest victims survive. A focus on high-quality CPR and adoption of new techniques and technologies
More Than A Heartbeat Improve Perfusion During CPR Today, only a small number of out of hospital cardiac arrest victims survive. A focus on high-quality CPR and adoption of new techniques and technologies
Improved Oxygen Delivery During Cardiopulmonary Resuscitation with Interposed Abdominal Compressions
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1983 Improved Oxygen Delivery During Cardiopulmonary Resuscitation with
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1983 Improved Oxygen Delivery During Cardiopulmonary Resuscitation with
Keywords active compression decompression, cardiopulmonary resuscitation, inspiratory impedance threshold device
 Combination of active compression decompression cardiopulmonary resuscitation and the inspiratory impedance threshold device: state of the art Ralph J. Frascone, a,c Dawn Bitz c and Keith Lurie b,d Purpose
Combination of active compression decompression cardiopulmonary resuscitation and the inspiratory impedance threshold device: state of the art Ralph J. Frascone, a,c Dawn Bitz c and Keith Lurie b,d Purpose
Design of near-optimal waveforms for chest and abdominal compression and decompression in CPR using computer-simulated evolution
 urdue University urdue e-ubs Weldon School of Biomedical Engineering Faculty ublications Weldon School of Biomedical Engineering 26 Design of near-optimal waveforms for chest and abdominal compression
urdue University urdue e-ubs Weldon School of Biomedical Engineering Faculty ublications Weldon School of Biomedical Engineering 26 Design of near-optimal waveforms for chest and abdominal compression
Effects of an impedance threshold valve upon hemodynamics in standard CPR: studies in a refined computational model
 urdue University urdue e-ubs Weldon School of Biomedical Engineering Faculty ublications Weldon School of Biomedical Engineering 3-2005 Effects of an impedance threshold valve upon hemodynamics in standard
urdue University urdue e-ubs Weldon School of Biomedical Engineering Faculty ublications Weldon School of Biomedical Engineering 3-2005 Effects of an impedance threshold valve upon hemodynamics in standard
The Cardiac Cycle Clive M. Baumgarten, Ph.D.
 The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
CRITICAL THINKING QUESTIONS AND ANSWERS AND CYCLE 2 LAB EXAM TEMPLATE. There are two main mechanisms that work in conjunction to return the blood
 CRITICAL THINKING QUESTIONS AND ANSWERS AND CYCLE 2 LAB EXAM TEMPLATE There are two main mechanisms that work in conjunction to return the blood THE CARDIAC PUMP 1) The forward pull(vis a fronte) This
CRITICAL THINKING QUESTIONS AND ANSWERS AND CYCLE 2 LAB EXAM TEMPLATE There are two main mechanisms that work in conjunction to return the blood THE CARDIAC PUMP 1) The forward pull(vis a fronte) This
Visualization of Cardiac Valve Motion in Man During External Chest Compression Using Two-dimensional Echocardiography
 Visualization of Cardiac Valve Motion in Man During External Chest Compression Using Two-dimensional Echocardiography Implications Regarding the Mechanism of Blood Flow JEFFREY A. WERNER, M.D., H. LEON
Visualization of Cardiac Valve Motion in Man During External Chest Compression Using Two-dimensional Echocardiography Implications Regarding the Mechanism of Blood Flow JEFFREY A. WERNER, M.D., H. LEON
Interposed Abdominal Compression CPR: A Comprehensive Evidence Based Review
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2003 Interposed Abdominal Compression CPR: A Comprehensive Evidence
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 2003 Interposed Abdominal Compression CPR: A Comprehensive Evidence
The principal target of mechanical resuscitation measures
 Phased Chest and Abdominal Compression-Decompression Versus Conventional Cardiopulmonary Resuscitation in Out-of-Hospital Cardiac Arrest Hans-Richard Arntz, MD; Rahul Agrawal, MD; Hans Richter, MD; Stefan
Phased Chest and Abdominal Compression-Decompression Versus Conventional Cardiopulmonary Resuscitation in Out-of-Hospital Cardiac Arrest Hans-Richard Arntz, MD; Rahul Agrawal, MD; Hans Richter, MD; Stefan
Mechanism of closed chest cardiopulmonary resuscitation investigated by transoesophageal echocardiography
 Journal of Accident and Emergency Medicine 1994 11, 139-143 Correspondence: C. Robertson, Consultant, Department of Accident and Emergency Medicine, Royal Infirmary, Lauriston Place, Edinburgh EH3 9YW,
Journal of Accident and Emergency Medicine 1994 11, 139-143 Correspondence: C. Robertson, Consultant, Department of Accident and Emergency Medicine, Royal Infirmary, Lauriston Place, Edinburgh EH3 9YW,
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
BME 5742 Bio-Systems Modeling and Control. Lecture 41 Heart & Blood Circulation Heart Function Basics
 BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
A New Technique for Repeated Measurement of Cardiac Output During Cardiopulmonary Resuscitation
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1980 A New Technique for Repeated Measurement of Cardiac Output During
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1980 A New Technique for Repeated Measurement of Cardiac Output During
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Morphological Variations Of The Internal Jugular Venous Valve
 ISPUB.COM The Internet Journal of Human Anatomy Volume 2 Number 1 Morphological Variations Of The Internal Jugular Venous Valve S Furukawa, A Takaya, T Nakagawa, I Sakaguchi, K Nishi Citation S Furukawa,
ISPUB.COM The Internet Journal of Human Anatomy Volume 2 Number 1 Morphological Variations Of The Internal Jugular Venous Valve S Furukawa, A Takaya, T Nakagawa, I Sakaguchi, K Nishi Citation S Furukawa,
MORE HEARTBEAT THAN A. Enhanced CPR. Better neurologic outcomes. Steve Dunn, Ph.D., Professor, University of Wisconsin Oshkosh
 MORE THAN A HEARTBEAT Enhanced CPR. Better neurologic outcomes. Steve Dunn, Ph.D., Professor, University of Wisconsin Oshkosh Thanks to the ResQPOD and a dedicated EMS team, Steve survived sudden cardiac
MORE THAN A HEARTBEAT Enhanced CPR. Better neurologic outcomes. Steve Dunn, Ph.D., Professor, University of Wisconsin Oshkosh Thanks to the ResQPOD and a dedicated EMS team, Steve survived sudden cardiac
Interposed abdominal compression cardiopulmonary resuscitation: Are we missing the mark in clinical trials?
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1993 Interposed abdominal compression cardiopulmonary resuscitation:
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1993 Interposed abdominal compression cardiopulmonary resuscitation:
Endotracheal Versus Intravenous Epinephrine During Electromechanical Dissociation with CPR in Dogs
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1985 Endotracheal Versus Intravenous Epinephrine During Electromechanical
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1985 Endotracheal Versus Intravenous Epinephrine During Electromechanical
QUIZ 1. Tuesday, March 2, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Ali Movahedi, Seyed Reza Mirhafez, PhD, Hamidreza Behnam-Voshani, Hamidreza Reihani, MD, Ali Kavosi, Gordon A. Ferns, DSc, MD, and Javad Malekzadeh
 ORIGINAL CONTRIBUTION A Comparison of the Effect of Interposed Abdominal Compression Cardiopulmonary Resuscitation and Standard Cardiopulmonary Resuscitation Methods on End-tidal CO 2 and the Return of
ORIGINAL CONTRIBUTION A Comparison of the Effect of Interposed Abdominal Compression Cardiopulmonary Resuscitation and Standard Cardiopulmonary Resuscitation Methods on End-tidal CO 2 and the Return of
Science and Technology of Head Up CPR
 Science and Technology of Head Up CPR Keith Lurie MD Professor of Emergency Medicine and Internal Medicine University of Minnesota Minneapolis, Minnesota USA April 4, 2018 Minneapolis, Minnesota 2 Disclosures
Science and Technology of Head Up CPR Keith Lurie MD Professor of Emergency Medicine and Internal Medicine University of Minnesota Minneapolis, Minnesota USA April 4, 2018 Minneapolis, Minnesota 2 Disclosures
Cardiac output during cardiopulmonary resuscitation at various compression rates and durations
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1981 Cardiac output during cardiopulmonary resuscitation at various
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1981 Cardiac output during cardiopulmonary resuscitation at various
Changes in Expired End-Tidal Carbon Dioxide During Cardiopulmonary Resuscitation in Dogs: A Prognostic Guide for Resuscitation Efforts
 1184 JACC Vol. 13, No. 5 Changes in Expired End-Tidal Carbon Dioxide During Cardiopulmonary Resuscitation in Dogs: A Prognostic Guide for Resuscitation Efforts KARL B. KERN, MD, FACC, ARTHUR B. SANDERS,
1184 JACC Vol. 13, No. 5 Changes in Expired End-Tidal Carbon Dioxide During Cardiopulmonary Resuscitation in Dogs: A Prognostic Guide for Resuscitation Efforts KARL B. KERN, MD, FACC, ARTHUR B. SANDERS,
MASSACHUSETTS INSTITUTE OF TECHNOLOGY
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Blood flows away from the heart in arteries, to the capillaries and back to the heart in the veins
 Cardiovascular System Summary Notes The cardiovascular system includes: The heart, a muscular pump The blood, a fluid connective tissue The blood vessels, arteries, veins and capillaries Blood flows away
Cardiovascular System Summary Notes The cardiovascular system includes: The heart, a muscular pump The blood, a fluid connective tissue The blood vessels, arteries, veins and capillaries Blood flows away
AS Level OCR Cardiovascular System
 AS Level OCR Cardiovascular System Learning Objectives The link between the Cardiac Cycle and the Conduction system of the heart. The relationship between Stroke volume, Heart rate and Cardiac Output.
AS Level OCR Cardiovascular System Learning Objectives The link between the Cardiac Cycle and the Conduction system of the heart. The relationship between Stroke volume, Heart rate and Cardiac Output.
Gastric Insufflation during IAC-CPR and Standard CPR in a Canine Model
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1985 Gastric Insufflation during IAC-CPR and Standard CPR in a Canine
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1985 Gastric Insufflation during IAC-CPR and Standard CPR in a Canine
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
² C Y E N G R E M E ssignac Cardiac Arrest Resuscitation Device uob
 E M E R G E N C Y Boussignac Cardiac Arrest Resuscitation Device ² What is b-card? b-card Boussignac Cardiac Arrest Resuscitation Device has been designed specifically for the treatment of cardiac arrest.
E M E R G E N C Y Boussignac Cardiac Arrest Resuscitation Device ² What is b-card? b-card Boussignac Cardiac Arrest Resuscitation Device has been designed specifically for the treatment of cardiac arrest.
The Arterial and Venous Systems Roland Pittman, Ph.D.
 The Arterial and Venous Systems Roland Pittman, Ph.D. OBJECTIVES: 1. State the primary characteristics of the arterial and venous systems. 2. Describe the elastic properties of arteries in terms of pressure,
The Arterial and Venous Systems Roland Pittman, Ph.D. OBJECTIVES: 1. State the primary characteristics of the arterial and venous systems. 2. Describe the elastic properties of arteries in terms of pressure,
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Clinical Investigation
 1692 Clinical Investigation Interposed Abdominal Compression Cardiopulmonary Resuscitation and Resuscitation Outcome During Asystole and Electromechanical Dissociation Jeffrey B. Sack, MD; Michael B. Kesselbrenner,
1692 Clinical Investigation Interposed Abdominal Compression Cardiopulmonary Resuscitation and Resuscitation Outcome During Asystole and Electromechanical Dissociation Jeffrey B. Sack, MD; Michael B. Kesselbrenner,
Chapter 2 The Human Cardiovascular System
 Chapter 2 The Human Cardiovascular System 2.1 Introduction Before delving into the computational methods of CHD, this chapter provides a preliminary understanding of the circulatory system from a physiological
Chapter 2 The Human Cardiovascular System 2.1 Introduction Before delving into the computational methods of CHD, this chapter provides a preliminary understanding of the circulatory system from a physiological
Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900.
 1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations. Eric M. Graham, MD
 Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations Eric M. Graham, MD Background Heart & lungs work to meet oxygen demands Imbalance between supply
Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations Eric M. Graham, MD Background Heart & lungs work to meet oxygen demands Imbalance between supply
Haemodynamic outcomes during piston-based mechanical CPR with or without active decompression in a porcine model of cardiac arrest
 Steinberg et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine (2018) 26:31 https://doi.org/10.1186/s13049-018-0496-z ORIGINAL RESEARCH Haemodynamic outcomes during piston-based
Steinberg et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine (2018) 26:31 https://doi.org/10.1186/s13049-018-0496-z ORIGINAL RESEARCH Haemodynamic outcomes during piston-based
CHAPTER 4 Basic Physiological Principles
 4-1 CHAPTER 4 Basic Physiological Principles Now that we have a working anatomical knowledge of the heart and circulatory system, we will next develop a functional and quantitative knowledge of the cardiovascular
4-1 CHAPTER 4 Basic Physiological Principles Now that we have a working anatomical knowledge of the heart and circulatory system, we will next develop a functional and quantitative knowledge of the cardiovascular
SIKLUS JANTUNG. Rahmatina B. Herman
 SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
Design of near-optimal waveforms for chest and abdominal compression and decompression in CPR using computer-simulated evolution
 urdue University urdue e-ubs Weldon School of Biomedical Engineering Faculty ublications Weldon School of Biomedical Engineering 2-5-25 Design of near-optimal waveforms for chest and abdominal compression
urdue University urdue e-ubs Weldon School of Biomedical Engineering Faculty ublications Weldon School of Biomedical Engineering 2-5-25 Design of near-optimal waveforms for chest and abdominal compression
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
THE VESSELS OF BLOOD CIRCULATION
 THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Use of the Trendelenburg Position in the Porcine Model Improves Carotid Flow During Cardiopulmonary
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Use of the Trendelenburg Position in the Porcine Model Improves Carotid Flow During Cardiopulmonary
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital,
 Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital, Disclosure Statement of Financial Interest I, Georgios Bompotis DO NOT have a financial interest/arrangement
Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital, Disclosure Statement of Financial Interest I, Georgios Bompotis DO NOT have a financial interest/arrangement
Joseph S. Redding's Contributions to Cardiac Resuscitation
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1985 Joseph S. Redding's Contributions to Cardiac Resuscitation Sandra
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1985 Joseph S. Redding's Contributions to Cardiac Resuscitation Sandra
END-TIDAL CARBON DIOXIDE AND OUTCOME OF OUT-OF-HOSPITAL CARDIAC ARREST END-TIDAL CARBON DIOXIDE AND OUTCOME OF OUT-OF-HOSPITAL CARDIAC ARREST
 END-TIDAL CARBON DIOXIDE AND OUTCOME OF OUT-OF-HOSPITAL CARDIAC ARREST END-TIDAL CARBON DIOXIDE AND OUTCOME OF OUT-OF-HOSPITAL CARDIAC ARREST ROBERT L. LEVINE, M.D., MARVIN A. WAYNE, M.D., AND CHARLES
END-TIDAL CARBON DIOXIDE AND OUTCOME OF OUT-OF-HOSPITAL CARDIAC ARREST END-TIDAL CARBON DIOXIDE AND OUTCOME OF OUT-OF-HOSPITAL CARDIAC ARREST ROBERT L. LEVINE, M.D., MARVIN A. WAYNE, M.D., AND CHARLES
This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors
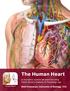 1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Chapter 14. The Cardiovascular System
 Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
Feasibility of Leadless Cardiac Pacing Using Injectable. Magnetic Microparticles
 Supplementary Information for Feasibility of Leadless Cardiac Pacing Using Injectable Magnetic Microparticles Menahem Y. Rotenberg, Hovav Gabay, Yoram Etzion and Smadar Cohen. Correspondence to: scohen@bgu.ac.il,
Supplementary Information for Feasibility of Leadless Cardiac Pacing Using Injectable Magnetic Microparticles Menahem Y. Rotenberg, Hovav Gabay, Yoram Etzion and Smadar Cohen. Correspondence to: scohen@bgu.ac.il,
2.02 Understand the functions and disorders of the circulatory system
 2.02 Understand the functions and disorders of the circulatory system 2.02 Understand the functions and disorders of the circulatory system Essential questions: What are the functions of blood? What are
2.02 Understand the functions and disorders of the circulatory system 2.02 Understand the functions and disorders of the circulatory system Essential questions: What are the functions of blood? What are
THE HEART OBJECTIVES: LOCATION OF THE HEART IN THE THORACIC CAVITY CARDIOVASCULAR SYSTEM
 BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
The Cardiovascular System
 The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
MECHANICAL CHEST COMPRESSION DEVICES. Erica Simon, DO, MHA Military EMS & Disaster Medicine Fellow SAUSHEC
 MECHANICAL CHEST COMPRESSION DEVICES Erica Simon, DO, MHA Military EMS & Disaster Medicine Fellow SAUSHEC Disclaimer The view(s) expressed herein are those of the author and do not reflect the official
MECHANICAL CHEST COMPRESSION DEVICES Erica Simon, DO, MHA Military EMS & Disaster Medicine Fellow SAUSHEC Disclaimer The view(s) expressed herein are those of the author and do not reflect the official
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
ANZCOR Guideline 11.1 Introduction to Advanced Life Support
 ANZCOR Guideline 11.1 Introduction to Advanced Life Support Who does this guideline apply to? Summary This guideline applies to adults who require advanced life support. Who is the audience for this guideline?
ANZCOR Guideline 11.1 Introduction to Advanced Life Support Who does this guideline apply to? Summary This guideline applies to adults who require advanced life support. Who is the audience for this guideline?
But unfortunately, the first sign of cardiovascular disease is often the last. Chest-Compression-Only Resuscitation Gordon A.
 THE UNIVERSITY OF ARIZONA Sarver Heart Center 1 THE UNIVERSITY OF ARIZONA Sarver Heart Center 2 But unfortunately, the first sign of cardiovascular disease is often the last 3 4 1 5 6 7 8 2 Risk of Cardiac
THE UNIVERSITY OF ARIZONA Sarver Heart Center 1 THE UNIVERSITY OF ARIZONA Sarver Heart Center 2 But unfortunately, the first sign of cardiovascular disease is often the last 3 4 1 5 6 7 8 2 Risk of Cardiac
THE HEART. Unit 3: Transportation and Respiration
 THE HEART Unit 3: Transportation and Respiration The Circulatory System Also called the Cardiovascular System Circulates blood in the body Transports nutrients, oxygen, carbon dioxide, hormones, and blood
THE HEART Unit 3: Transportation and Respiration The Circulatory System Also called the Cardiovascular System Circulates blood in the body Transports nutrients, oxygen, carbon dioxide, hormones, and blood
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
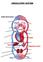 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
Use of an Inspiratory Impedance Valve Improves Neurologically Intact Survival in a Porcine Model of Ventricular Fibrillation
 Use of an Inspiratory Impedance Valve Improves Neurologically Intact Survival in a Porcine Model of Ventricular Fibrillation Keith G. Lurie, MD; Todd Zielinski, MS; Scott McKnite, BS; Tom Aufderheide,
Use of an Inspiratory Impedance Valve Improves Neurologically Intact Survival in a Porcine Model of Ventricular Fibrillation Keith G. Lurie, MD; Todd Zielinski, MS; Scott McKnite, BS; Tom Aufderheide,
CHF and Pulmonary Edema. Rod Hetherington
 CHF and Pulmonary Edema Rod Hetherington Objectives Given a lecture and group discussion, the paramedic will be able to: Identify and name the key anatomical structures of the heart and vessels Describe
CHF and Pulmonary Edema Rod Hetherington Objectives Given a lecture and group discussion, the paramedic will be able to: Identify and name the key anatomical structures of the heart and vessels Describe
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Importance of the Duration of Inadequate Coronary Perfusion Pressure on Resuscitation From Cardiac Arrest
 JACC Vol. 6. No. I July 1985: 113-8 113 Importance of the Duration of Inadequate Coronary Perfusion Pressure on Resuscitation From Cardiac Arrest ARTHUR B. SANDERS, MD, KARL B. KERN, MD, MATTHEW ATLAS,
JACC Vol. 6. No. I July 1985: 113-8 113 Importance of the Duration of Inadequate Coronary Perfusion Pressure on Resuscitation From Cardiac Arrest ARTHUR B. SANDERS, MD, KARL B. KERN, MD, MATTHEW ATLAS,
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
External cardiac compression may be harmful in some. some scenarios of pulseless electrical activity.
 External cardiac compression may be harmful in some scenarios of pulseless electrical activity. Item Type Article Authors Hogan, T S Citation External cardiac compression may be harmful in some scenarios
External cardiac compression may be harmful in some scenarios of pulseless electrical activity. Item Type Article Authors Hogan, T S Citation External cardiac compression may be harmful in some scenarios
WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR
 RECOVER 2011 1 of 6 WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR 1. Basic Demographics Worksheet author(s) Kate Hopper Mailing address: Dept Vet Surgical & Radiological Sciences Room
RECOVER 2011 1 of 6 WORKSHEET for Evidence-Based Review of Science for Veterinary CPCR 1. Basic Demographics Worksheet author(s) Kate Hopper Mailing address: Dept Vet Surgical & Radiological Sciences Room
Heart. Structure Physiology of blood pressure and heartbeat
 Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Lab 16. The Cardiovascular System Heart and Blood Vessels. Laboratory Objectives
 Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
ADVANCED ASSESSMENT Cardiovascular System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Cardiovascular System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Cardiovascular System AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Cardiovascular System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Cardiovascular System AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Lecture 10. Circulatory systems; flow dynamics, flow regulation in response to environmental and internal conditions.
 Lecture 10 Circulatory systems; flow dynamics, flow regulation in response to environmental and internal conditions Professor Simchon Influence of P O2 on Hemoglobin Saturation Hemoglobin saturation plotted
Lecture 10 Circulatory systems; flow dynamics, flow regulation in response to environmental and internal conditions Professor Simchon Influence of P O2 on Hemoglobin Saturation Hemoglobin saturation plotted
