Ocular blood flow evaluation in injured and healthy fellow eyes
|
|
|
- Milton Warner
- 5 years ago
- Views:
Transcription
1 European Journal of Ophthalmology / Vol. 15 no. 1, 2005 / pp Ocular blood flow evaluation in injured and healthy fellow eyes E. MARTINI, M. GUIDUCCI, L. CAMPI, G.M. CAVALLINI Department of Neurosciences, Head-Neck and Rehabilitation, Ophthalmology Unit, University of Modena and Reggio Emila, Modena - Italy PURPOSE. To assess if injured eyes develop ocular blood flow disturbances that may contribute to development of traumatic glaucoma. METHODS. Twenty-five eyes of 25 patients hospitalized from January 1997 to July 1999 for blunt (15) or penetrating (10) eye injury and elevated intraocular pressure (IOP) (>23 mm Hg) were controlled at least 24 months after the trauma and underwent visual field examination, pulsatile ocular blood flow (pobf), and color Doppler imaging (CDI) analysis of ophthalmic artery, central retinal artery, nasal and temporal short posterior ciliary arteries. Uninjured healthy eye was used as control. RESULTS. IOP was significantly higher in injured eyes (15.1±3.3 vs 13.0±2.7 mmhg; p<0.01), but only 2 eyes (8%) were under medical treatment. pobf values were significantly lower in injured eyes: 11.25±6.56 µl/sec in the trauma eyes and 15.40±7.29 in fellow eyes (p=0.002). Resistivity index of all investigated retrobulbar vessels was very significantly higher in injured eyes than in fellow eyes (p<0.0001). There is no significant correlation between IOP and ocular blood flow disturbance. CONCLUSIONS. Long-term follow-up (mean 39±12 months) of injured eyes shows, besides a slight but significant increase of IOP, a very significant impairment of ocular blood supply to injured eyes compared to healthy fellow eyes with reduction of pulsatile ocular blood flow and marked increase of resistance to flow in all retrobulbar vessels. These anomalies may be considered an independent risk factor to develop traumatic glaucoma. (Eur J Ophthalmol 2005; 15: 48-55) KEY WORDS. Ocular trauma, Ocular blood flow, Color Doppler imaging, Resistivity index Accepted: July 12, 2004 INTRODUCTION Ocular trauma, either blunt or penetrating, is often associated with abnormalities of intraocular pressure (IOP): there may be hypotony due to reduction of aqueous production (after ciliary body contusion or inflammation) or excessive aqueous drainage (internally through a cyclodialysis cleft or externally through a break of ocular wall) but more often there is a raise in IOP that may lead to post-traumatic glaucoma. The raise in IOP may be early or late and may have several of the following mechanisms, most of which are related to impaired trabecular drainage: Intraocular and trabecular inflammation (that is generally transient) (1) Angular recession and trabecular damage and scarring (2, 3) Hyphema with blockade of trabecular meshwork by red cells (4, 5) Ghost cells coming from vitreous hemorrhage may pass in the anterior chamber and cause trabecular impairment and elevated IOP (6) Iris and/or ciliary body dialysis (7) Lenticular alterations: cataract or lens subluxation /048-08$15.00/0 Wichtig Editore, 2005
2 Martini et al may cause an alteration of aqueous humor dynamics with pupillary block and/or angle closure (8) In cases of penetrating trauma there may be also a direct injury and subsequent scarring of angle or trabecular structures. Periocular tissue scarring with elevation of episcleral veins pressure. These causes illustrate why after ocular trauma there often are IOP disturbances and there may be a traumatic glaucoma, which often has a poor response to therapy and prognosis (9, 10). In recent years there has been growing evidence that vascular factors are important in the pathogenesis and the progression of glaucomatous damage not only in so called low tension glaucoma but also in primary open angle glaucoma (11-14). Noninvasive methods to evaluate ocular blood flow are available that give information on blood supply to the orbit and ocular districts: pulsatile ocular blood flow (pobf) system by Langham measures the variations in IOP induced by blood systolic pulse and derives the pulse volume and from it the blood flow (mainly to the choroid) (15, 16). Color Doppler imaging (CDI) uses Doppler effect to measure the velocity of blood cells (peak systolic velocity = PSV and the end diastolic velocity = EDV) and the resistance to flow (Pourcelot Resistivity index: RI = PSV EDV/ PSV) in different retrobulbar vessels that are strongly correlated to blood flow (17, 18); other instruments utilize scanning laser Doppler flowmetry. Many instruments are therefore available to assess and quantify the state of intraocular circulation (19, 20). Secondary glaucomas are considered to be mainly or exclusively determined by elevated IOP, but the exact mechanism of glaucomatous damage is not clear even when IOP is strongly elevated and vascular factors may play a role in these secondary glaucomas as well. We decided to assess the state of ocular blood flow in traumatized eyes (that had in their clinical history an elevated IOP in the early post-traumatic course) using as a control the fellow not traumatized eye. The aim of the study was to identify or exclude the presence of permanent ocular hemodynamics alterations in traumatized eyes (a long time after trauma) that could be influential on the development of traumatic glaucoma in addition to and/or independently from IOP (21, 22). METHODS We selected from medical records the patients hospitalized at our institution between January 1, 1997, and July 31, 1999, with a diagnosis of ocular trauma (either blunt or penetrating, Tab. I) and an elevated IOP ( 23 mmhg) during the early post-trauma phase and at least 2 years follow-up; we excluded chemical burns (chemical injuries often have corneal dense leukomas and therefore difficulties in assessing IOP) and selected only mechanical traumatisms; the fellow eye had to be healthy, without any disease other than cataract (inclusion and exclusion criteria are listed in Tab. II). Twenty-five patients responded to inclusion criteria: from the medical records we extracted demographic data, date and type of trauma, maximum IOP recorded in the post-trauma period, surgical or laser treatment when performed; the patients were then summoned and underwent a complete ocular examination (refraction, anterior segment examination, IOP measurement by Goldmann tonometry, fundus examination), visual field (HFA II, Humphrey- Zeiss, San Leandro, CA, Program Central 30-2 SITA fast), ocular blood flow assessment by means of pobf Langham system (OBF Labs UK Ltd, Malmesbury, UK), and CDI (ATL Apogee 800 Plus; ATL Co., Bothell, WA) evaluating peak systolic velocity, end diastolic velocity, and Pourcelot RI of ophthalmic artery, central retina artery, nasal and temporal posterior ciliary arteries. OBF measures were obtained with a slit lamp mounted unit and the patient in sitting position after topical oxybuprocaine eyedrop instillation, while recording arterial pressure; the instrument measures IOP and automatically records and selects five complete pulse cycles and derives pulse amplitude (mmhg), pulse volume (µl), and pulsatile blood flow (µl/sec) (23). CDI measures were obtained with the patient in supine position while recording arterial pressure, using a 7.5 MHz flat probe. The eyes are closed and a coupling gel is applied to the eyelids. The vessels investigated are as follows (24). Ophthalmic artery (OA) is localized where it runs parallel to the optic nerve, about 40 mm from the anterior ocular surface, before the crossing of the optic nerve itself. It has a typical wave profile, similar to the internal carotid with an evident dicrotic notch. Central retinal artery (CRA) is localized in the ante- 49
3 Ocular blood flow after ocular trauma rior part of the optic nerve shadow, just posterior to the globe wall; often the central retinal vein is visible at the same location. The wave profile is flat and rounded as compared to the OA wave. Short posterior ciliary arteries (SPCA, nasal and temporal) are located just posterior to the globe wall at the side of the optic nerve shadow. The SPCA are often difficult to localize as they are small vessels at the inferior resolution limit of CDI. The wave profile is round (without dicrotic notch) but more evident than CRA, probably because more than one single artery contributes to the wave. The instrument calculates PSV, EDV, and Pourcelot RI (RI = PSV EDV/PSV). The parameters evaluated were maximum recorded IOP, IOP at the time of visit, visual field mean deviation (MD) and pattern standard deviation (PSD), OBF pulsatile flow (µl/sec), and CDI values (PSV, EDV, RI) for all four arteries examined (24-27). All parameters were matched with the healthy fellow eye data. A subgroup analysis and comparison of blunt and penetrating injured eyes was performed. The statistical analysis was performed by means of two-tailed t-test and correlation between different variables with Pearson test. A p value less than 0.05 was the significance limit. TABLE I - CAUSES AND MECHANISMS OF INJURY Injury mechanism Number No. (%) Scleral and/or corneal wound 6 (24) Intraocular foreign body 4 (16) Bottle cork 6 (24) Elastic rope 1 (4) Airbag 1 (4) Domestic accident (fall) 1 (4) Working accident (blunt) 6 (24) TABLE II - INCLUSION AND EXCLUSION CRITERIA Inclusion criteria Exclusion criteria IOP 23 mmhg Chemical or electric injury Blunt or penetrating injury Severe corneal leukoma Visual acuity 0.3 Visual acuity < 0.3 Follow-up 24 months Severe structural damage to the eye or orbit Healthy fellow eye Fellow eye with vascular ocular disease IOP = Intraocular pressure RESULTS Demographics The 25 patients included 19 men (76%) and 6 women (24%), the mean age was 52±16 years, the side of injury was the right in 12 cases (48%) and the left in 13 cases (52%). The trauma was blunt in 15 cases (60%) and penetrating in 10 cases (40%). The mechanisms and causes of trauma are listed in Table II. Thirteen patients (52%) underwent surgery either to repair the primary injury or for subsequent complications; three patients underwent Argon laser trabeculoplasty to reduce elevated IOP. All procedures performed are listed in Table III. Three patients in the blunt trauma group underwent surgery: two cataract extraction and one anterior chamber washing. In the penetrating injury group four patients underwent wound repair and subsequent cataract extraction, two patients underwent wound repair and simultaneous vitrectomy with foreign body extraction. The maximum IOP recorded after trauma ranged from 23 to 50 mmhg (mean 28±7 mmhg). The time elapsed from trauma to the study visit ranged from 24 to 53 months with a mean of 39±12 months. Intraocular pressure At the time of visit only 2 patients (8%) were still treated to reduce IOP and one of them was treated in both eyes; the remaining 23 (92%) had IOP under 21 mmhg without any therapy. Mean IOP at the visit recording was 15.1±3.3 mmhg in the injured eye and 13.0±2.7 in the fellow eye and the difference proved to be significant (p<0.01). The subgroup analysis comparing blunt trauma and penetrating trauma (Tab. IV) and operated and nonoperated eyes (Tab. V) showed no statistically significant difference between subgroups (p>0.05). TABLE III - SURGICAL AND LASER PROCEDURES PERFORMED ON THE 25 INJURED EYES AFTER THE TRAUMA Procedure Patients (%) Foreign body extraction 3 (12) Argon laser trabeculoplasty 3 (12) Corneo-scleral suture 8 (32) Anterior chamber washing 1 (4) Cataract 6 (24) 50
4 Martini et al Visual field The mean visual field MD was 4.39±4.13 db in the trauma eyes and 1.87±1.43 in the fellow eyes: the difference was statistically significant (p<0.05). The mean visual field PSD was 3.49±3.77 in the trauma group and 1.84±0.61 in the fellow eyes: the difference was not statistically significant (p=0.085). In a subgroup analysis comparing blunt and penetrating trauma (Tab. IV) or operated and nonoperated eyes (Tab. V) penetrated and operated eyes had worse results than blunt trauma and nonoperated eyes, but the difference was not statistically significant (p always greater than 0.05). pobf The pobf estimate gave a mean of 11.25±6.56 µl/sec in the trauma eyes and 15.40±7.29 in fellow eyes: the TABLE IV - COMPARISON BETWEEN BLUNT AND PENETRATING INJURIES Characteristics Blunt trauma (n=15) Penetrating trauma (n=10) p Max IOP (mmhg) 29.36± ± Follow-up (months) 39.53± ± Visual acuity 00.83± ± IOP (mmhg) 15.29± ± pobf (µl/sec) 13.61± ± MD (db) -3.81± ± PSD (db) 02.41± ± OA-PSV (cm/sec) 39.38± ± OA-EDV (cm/sec) 10.90± ± OA-RI 00.73± ± CRA-PSV (cm/sec) 16.16± ± CRA-EDV (cm/sec) 04.99± ± CRA-RI 00.71± ± NSPCA-PSV (cm/sec) 21.49± ± NSPCA-EDV (cm/sec) 05.54± ± NSPCA-RI 00.74± ± TSPCA-PSV (cm/sec) 28.57± ± TSPCA-EDV (cm/sec) 07.17± ± TSPCA-RI 00.74± ± Values are mean±sd. No differences were significant IOP = Intraocular pressure; pobf = Pulsatile ocular blood flow; MD = Mean deviation; PSD = Pattern standard deviation; OA = Ophthalmic artery; PSV = Peak systolic velocity; EDV = End diastolic velocity; RI = Resistivity index; CRA = Central retinal artery; NSPCA = Nasal short posterior ciliary arteries; TSPCA = Temporal short posterior ciliary arteries TABLE V - COMPARISON BETWEEN OPERATED AND NONOPERATED EYES Characteristics Operated eyes Nonoperated eyes p IOP (mmhg) 15.10± ± pobf (ml/sec) 09.74± ± MD (db) -4.74± ± PSD (db) 04.28± ± OA-RI 00.76± ± CRA-RI 00.73± ± NSPCA-RI 00.75± ± TSPCA-RI 00.75± ± Values are mean±sd. No differences were significant IOP = Intraocular pressure; pobf = Pulsatile ocular blood flow; MD = Mean deviation; PSD = Pattern standard deviation; OA = Ophthalmic artery; RI = Resistivity index; CRA = Central retinal artery; NSPCA = Nasal short posterior ciliary arteries; TSPCA = Temporal short posterior ciliary arteries 51
5 Ocular blood flow after ocular trauma TABLE VI - DATA OF CDI EVALUATION OF RETROBULBAR VESSELS IN INJURED AND FELLOW HEALTHY EYES Vessel Injured eye, Fellow eye, Difference mean±sd mean±sd (t-test), p OA PSV 44.42± ± EDV 11.48± ± RI 0.74± ± x10-6 CRA PSV 17.10± ± EDV 4.96± ± RI 0.71± ± NPSCA PSV 21.15± ± EDV 5.52± ± RI 0.74± ± x10-7 TPSCA PSV 24.58± ± EDV 6.75± ± RI 0.73± ± x10-7 For each vessel systolic and diastolic velocities (PSV and EDV) and resistivity index (RI) were calculated. The statistical significance of the difference between injured and healthy eyes is shown in the last column (significance limit = p<0.05) CDI = Color Doppler Imaging; OA = Ophthalmic Artery; PSV = Peak Systolic Velocity; EDV = End Diastolic Velocity; CRA = Central Retinal Artery; NSPCA = Nasal Short Posterior Ciliary Arteries; TSPCA = Temporal Short Posterior Ciliary Arteries difference resulted highly significant (p=0.002). In a subgroup analysis comparing blunt and penetrating trauma (Tab. IV) or operated and nonoperated eyes (Tab. V) penetrated and operated eyes had worse results than blunt trauma and nonoperated eyes, but the difference was not statistically significant (p always greater than 0.05). CDI CDI results are described in Table VI. OA: PSV was 44.42±28.02 cm/sec in trauma eyes and 37.64±22.42 cm/sec in fellow eyes (p<0.05); EDV was 11.48±7.63 cm/sec in trauma eyes and 12.97±8.08 cm/sec in fellow eyes (p>0.05). OA RI was 0.74±0.07 in trauma eyes and 0.66±0.06 in fellow eyes (p=3.32x10-6 p<0.0001). Central retinal artery (CRA): PSV was 17.10±6.45 cm/sec in trauma eyes and 16.68±8.13 cm/sec in fellow eyes (p>0.05); EDV was 4.96±2.71 cm/sec in trauma eyes and 6.41±3.35 cm/sec in fellow eyes (p=0.0507); RI was 0.71±0.09 in trauma eyes and 0.62±0.07 in fellow eyes (p<0.0005). Nasal SPCA (NSPCA): PSV was 21.15±11.63 cm/sec in trauma eyes and 17.04±8.20 cm/sec in fellow eyes (p>0.05); EDV was 5.52±3.30 cm/sec in trauma eyes and 6.79±3.60 cm/sec in fellow eyes (p>0.05); RI was 0.74±0.06 in trauma eyes and 0.61±0.07 in fellow eyes (p=3.87x10-7 p< ). Temporal SPCA (TSPCA): PSV was 24.58±16.54 cm/sec in trauma eyes and 25.21±17.54 cm/sec in fellow eyes (p>0.05); EDV was 6.75±4.34 cm/sec in trauma eyes and 9.90±7.63 cm/sec in fellow eyes (p>0.05); RI was 0.73±0.07 in trauma eyes and 0.62±0.06 in fellow eyes (p=1.03x10-7 p<0.0001). The subgroup analysis dividing and comparing penetrating from blunt injuries gave for all studied variables results not statistically different between the two groups (Tab. IV). Further analysis comparing the eyes that were operated with those not operated confirmed the significant difference in CDI RI between traumatized and fellow eyes in both subgroups (operated and nonoperated), while the difference between operated and nonoperated eyes was not significant (Tab. V) even if penetrated or operated eyes had higher RI than blunt trauma or nonoperated eyes. Using the Pearson s test we studied the correlations between IOP and ocular blood flow parameters and between OBF and CDI measures. The results are summarized in Tables VII and VIII. Considering the relationship between the IOP and the flow measures (Tab. VII) we note that the pobf value shows a slight (R= 0.15) inverse correlation with IOP in the injured eyes that is not present in healthy 52
6 Martini et al eyes (R=0.08); the CDI RI of ophthalmic, nasal, and temporal short posterior ciliary arteries in injured eyes have no correlation with IOP, while in healthy eyes there is a slight to fair positive correlation between IOP and RI in the same arteries.there are no clear correlations between pobf and CDI values (Tab. VIII). TABLE VII - CORRELATION (R value Pearson s test) BET- WEEN INTRAOCULAR PRESSURE AND DIFFERENT OCULAR BLOOD FLOW PARAMETERS IN IN- JURED AND HEALTHY EYES Ocular blood flow Intraocular pressure parameters Injured eye Fellow eye pobf OA-PSV OA-EDV OA-RI CRA-PSV CRA-EDV CRA-RI NPSCA-PSV NPSCA-EDV NPSCA-RI TPSCA-PSV TPSCA-EDV TPSCA-RI pobf= Pulsatile ocular blood flow; OA = Ophthalmic artery; PSV = Peak systolic velocity; EDV = End diastolic velocity; RI = Resistivity index; CRA = Central retinal artery; NSPCA = Nasal short posterior ciliary arteries; TSPCA = Temporal short posterior ciliary arteries TABLE VIII - CORRELATION (R value Pearson s test) BET- WEEN PULSATILE OCULAR BLOOD FLOW (pobf) VALUE AND DIFFERENT CDI PARAMETERS CDI POBF parameters Injured Fellow eye eye OA-PSV OA-EDV OA-RI CRA-PSV CRA-EDV CRA-RI NPSCA-PSV NPSCA-EDV NPSCA-RI TPSCA-PSV TPSCA-EDV TPSCA-RI OA = Ophthalmic artery; PSV = Peak systolic velocity; EDV = End diastolic velocity; RI = Resistivity index; CRA = Central retinal artery; NSPCA = Nasal short posterior ciliary arteries; TSPCA = Temporal short posterior ciliary arteries DISCUSSION In an attempt to draw some conclusion from the collected data we underline four points. The relevant result of our study is the very significant difference in ocular blood flow measures between injured and fellow healthy eyes: more than 2 years after the trauma, the pobf is significantly reduced in injured eyes while the CDI RI of all retrobulbar vessels is strongly increased, pointing out an increase in overall resistance to blood flow in injured eyes. The systolic velocity is significantly higher in injured than in normal eyes, while all other parameters are not significantly different between the two groups. The increase of ophthalmic artery systolic velocity in injured eyes may be explained with a relative stenosis due to scarring or increase of orbital tissues rigidity. The IOP of injured eyes is higher than in normal eyes, even if most injured eyes have IOP within the normal range without therapy (only 8% of eyes received IOP lowering drugs). The strong increase in resistance to blood flow in injured eyes does not seem to correlate with the increased IOP, but is an independent phenomenon. Harris et al (28-30) found that RI of CRA and SPCA is correlated with IOP, while OA RI is not. Our results are only partially in agreement as in normal eyes we found that SPCA and OA RI seem to be correlated with IOP in healthy eyes and this correlation is lost in injured eyes. There are no significant differences between blunt and penetrating injuries (Tab. IV): CDI values were almost identical. OA RI is higher in penetrating than in blunt injuries; similarly, pobf values are lower in penetrating injuries but the differences are not significant, perhaps due to the small numbers, and it would therefore be interesting to extend the observation to more numerous groups. Similarly, comparing operated and nonoperated eyes we found that perfusion parameters (pobf and CDI RI of all retrobulbar arteries) were worse in operated eyes but again the difference did not attain statistical significance (Tab. V). The correlations between the data obtained by two different technologies to assess the ocular perfusion dynamics give results that are not easily interpreted (Tab. VIII). The pobf is lower and the RI of retrobulbar vessels is higher in injured eyes but the two variables do not correlate each other, and 53
7 Ocular blood flow after ocular trauma they correlate differently between the two eyes and the different arteries: both methods show an impairment of ocular perfusion but the eyes that have more reduced OBF are not those with higher RI (as one could expect). We believe that the two methods are hardly comparable each other, as they measure different variables at different anatomic levels, with very different technologies (31, 32). We conclude from collected data that ocular trauma causes a significant and longstanding impairment of ocular circulation that is apparently independent from IOP elevation and may act as an independent risk factor in the development of post-traumatic glaucoma. We do not know if this impairment is functional (increased vasoconstriction/vasospasm) or structural (increase in ocular wall rigidity, scarring of periocular tissues). We hope to have more information on this point repeating the pobf and CDI measures after administration of drugs with vasodilator effect. Reprint requests to: Prof. Gian Maria Cavallini Struttura Complessa di Oftalmologia Università di Modena e Reggio Emilia Azienda Ospedaliera Policlinico di Modena Via del Pozzo Modena, Italy cavallini.gianmaria@unimo.it REFERENCES 1. Herchler J, Cobo M. Trauma and elevated intraocular pressure. In: Ritch R., Shields MB, Krupin T, eds. The Glaucomas. St. Louis: CV Mosby; 1989: Jones WL. Posttraumatic glaucoma. J Am Optom Assoc 1987; 58: Salmon JF, Mermoud A, Ivey A, Swanevelder SA, Hoffman M. The detection of post-traumatic angle recession by gonioscopy in a population-based glaucoma survey. Ophthalmology 1994; 101: Endo S, Ishida N, Yamaguchi T. Tear in the trabecular meshwork caused by an airsoft gun. Am J Ophthalmol 2001; 131: Anid G, Powell RG, Elkington AR. Postural response of intraocular pressure following traumatic hyphaema. Br J Ophthalmol 1985; 69: Stein JD, Jaeger EA, Jeffers JB. Air bags and ocular injuries. Trans Am Ophthalmol Soc 1999; 97: 59-82; discussion Campbell DG. Ghost cell glaucoma following trauma. Ophthalmology 1981; 88: Patte M, Bonicel P, Bacin F. Treatment of post-traumatic cyclodialysis using direct cyclopexy. J Fr Ophtalmol 2001; 24: Inatani M, Tanihara H, Honjo M, Kido N, Honda Y. Secondary glaucoma associated with crystalline lens subluxation. J Cataract Refract Surg 2000; 26: Alajbegovic R, Karcic S, Al Hasan N, Alajbegovic-Halimic J. War injury of the eye and post-traumatic glaucoma. Med Arch 1994; 48: Gasser P. Why study vascular factor in glaucoma? Int Ophthalmol ; 22: Prunte C, Orgul S, Flammer J. Abnormalities of microcirculation in glaucoma: facts and hints. Curr Opin Ophthalmol 1998; 9: Bonomi L, Marchini G, Marraffa M, Bernardi P, Morbio R, Varotto A. Vascular risk factor for primary open angle glaucoma: the Egna-Neumarkt Study. Ophthalmology 2000; 107: Flammer J, Orgul S. Optic nerve blood-flow abnormalities in glaucoma. Prog Retin Eye Res 1998; 17: Gherghel D, Chiselita D. Open angle glaucoma. Identification of vascular risk factors. Oftalmologia 2000; 50: Giovagnorio F, Quaranta L, Bucci MG. Color Doppler assessment of normal ocular blood flow. J Ultrasound Med 1993; 12: Schmidt KG. Basic principles of the pobf system. In: Pillunat LE, Harris A, Anderson DR, Greve EL, eds. Current Concept on Ocular Blood Flow in Glaucoma. The Hague, The Netherlands: Kugler Publication; 1999: Baxter GM, Williamson TH. Color Doppler imaging of the eye: normal ranges, reproducibility, and observer variation. J Ultrasound Med 1995; 14: Liu CJ, Chou YH, Chou JC, Chiou HJ, Chiang SC, Liu JH. Retrobulbar haemodynamic changes studies by color Doppler imaging in glaucoma. Eye 1997; 11: Galassi F, Sodi A, Rossi MG, Ucci F, De Saint Pierre F. Ocular haemodynamics in some subgroups of normal pressure glaucoma. Acta Ophthalmol Scand 1997; 224 (Suppl): S Rankin SJA, Walman BE, Buckley AR, Drance SM. Color Doppler imaging and spectral analysis of the optic nerve vasculature in glaucoma. Am J Ophthalmol 1994; 11:
8 Martini et al 22. Flammer J, Haefliger IO, Orgul S, Resink T. Vascular dysregulation: a principal risk factor for glaucomatous damage? J Glaucoma 1999; 8: Quaranta L, Manni G, Donato F, Bucci MG. The effect of increased intraocular pressure on pulsatile ocular blood flow in low tension glaucoma. Surv Ophthalmol 1994; 38 (Suppl): S Rankin SJ, Walman BE, Buckley AR, Drance SM. Color Doppler imaging and spectral analysis of the optic nerve vasculature in glaucoma. Am J Ophthalmol 1995; 119: Aburn NS, Sergott RC. Color Doppler imaging of the ocular and orbital blood vessels. Curr Opin Ophthalmol 1993; 4: Aburn NS, Sergott RC. Orbital colour Doppler imaging. Eye 1993; 7: Gio M, Balcet U, De Laage P, Mesquita A. Blood flow velocity measurements in the optic nerve of glaucomatous patients by elaboration of a constant to evaluate the evolutive risk. J Cardiovasc Surg 1997; 38: Kagemann L, Harris A, Chung HS, Costa VP, Garzozi HJ. Basic and limitation of color Doppler imaging. In: Pillunat LE, Harris A, Anderson DR, Greve EL, eds. Current concept on ocular blood flow in glaucoma. The Hague, The Netherlands: Kugler Publication; 1999: Chung HS, Harris A, Evans DW, Kagemann L, Garzozi HJ, Martin B. Vascular aspect in the pathophysiology of glaucomatous optic neuropathy. Surv Ophthalmol 1999; 43 (Suppl): S Harris A, Sergott RC, Spaeth GL, Katz JL, Shoemaker BA, Martin BJ. Color Doppler analysis of ocular vessel blood velocity in normal-tension glaucoma. Am J Ophthalmol 1994; 118: Migdal C. Comparison of pulsatile ocular blood flow and color Doppler imaging. In: Pillunat LE, Harris A, Anderson DR, Greve EL, eds. Current concept on ocular blood flow in glaucoma. The Hague, The Netherlands: Kugler Publication; 1999: Kaiser HJ, Schoetzau A, Stumpfig D, Flammer J. Bloodflow velocities of the extraocular vessels in patients with high-tension and normal-tension primary open-angle glaucoma. Am J Ophthalmol 1997; 123:
Role of ocular Doppler ultrasonography in primary open angle glaucoma
 Role of ocular Doppler ultrasonography in primary open angle glaucoma Poster No.: C-0650 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Alconchel 1, L. Pablo 2, P. Seral Moral 2, J. Remírez 2,
Role of ocular Doppler ultrasonography in primary open angle glaucoma Poster No.: C-0650 Congress: ECR 2012 Type: Scientific Exhibit Authors: A. Alconchel 1, L. Pablo 2, P. Seral Moral 2, J. Remírez 2,
Evolution of the Definition of Primary Open-Angle Glaucoma
 OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
Bottle-cork injury to the eye: a review of 13 cases
 European Journal of Ophthalmology / Vol. 13 no. 3, 2003 / pp. 287-291 Bottle-cork injury to the eye: a review of 13 cases G.M. CAVALLINI, N. LUGLI, L. CAMPI, L. PAGLIANI, P. SACCAROLA Department of Neuropsychosensorial
European Journal of Ophthalmology / Vol. 13 no. 3, 2003 / pp. 287-291 Bottle-cork injury to the eye: a review of 13 cases G.M. CAVALLINI, N. LUGLI, L. CAMPI, L. PAGLIANI, P. SACCAROLA Department of Neuropsychosensorial
CLINICAL SCIENCES. Ocular Hemodynamics and Glaucoma Prognosis
 Ocular Hemodynamics and Glaucoma Prognosis A Color Doppler Imaging Study CLINICAL SCIENCES Fernando Galassi, MD; Andrea Sodi, MD; Francesca Ucci, MD; Giulia Renieri, MD; Benedetta Pieri, MD; Michela Baccini,
Ocular Hemodynamics and Glaucoma Prognosis A Color Doppler Imaging Study CLINICAL SCIENCES Fernando Galassi, MD; Andrea Sodi, MD; Francesca Ucci, MD; Giulia Renieri, MD; Benedetta Pieri, MD; Michela Baccini,
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
This policy is applicable to Commercial Products only. For BlueCHiP for Medicare, see related policy section.
 Medical Coverage Policy Ophthalmologic Techniques that Evaluate the Posterior Segment for Glaucoma EFFECTIVE DATE: 01 01 2017 POLICY LAST UPDATED: 09 18 2018 OVERVIEW Several techniques have been developed
Medical Coverage Policy Ophthalmologic Techniques that Evaluate the Posterior Segment for Glaucoma EFFECTIVE DATE: 01 01 2017 POLICY LAST UPDATED: 09 18 2018 OVERVIEW Several techniques have been developed
EVect of acute intraocular pressure changes on. between short posterior ciliary artery haemodynamics
 Br J Ophthalmol 1999;3:333 33 Department of Ophthalmology and Visual Science, Vanderbilt University, Nashville, TN, USA KMJoos B E Steinwand Bascom Palmer Eye Institute, University of Miami, Miami, FL,
Br J Ophthalmol 1999;3:333 33 Department of Ophthalmology and Visual Science, Vanderbilt University, Nashville, TN, USA KMJoos B E Steinwand Bascom Palmer Eye Institute, University of Miami, Miami, FL,
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation
 Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Use of Orbital Color Doppler Imaging for Detecting Internal Carotid Artery Stenosis in Patients with Amaurosis Fugax
 Use of Orbital Color Doppler Imaging for Detecting Internal Carotid Artery Stenosis in Patients with Amaurosis Fugax Sayuri Fujioka Osaka Medical Center for Cancer and Cardiovascular Diseases, Osaka, Japan
Use of Orbital Color Doppler Imaging for Detecting Internal Carotid Artery Stenosis in Patients with Amaurosis Fugax Sayuri Fujioka Osaka Medical Center for Cancer and Cardiovascular Diseases, Osaka, Japan
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
GLAUCOMA ASSOCIATED WITH OCULAR TRAUMA
 Glaucoma Associated With Ocular Trauma Chapter 11 GLAUCOMA ASSOCIATED WITH OCULAR TRAUMA NEIL T. CHOPLIN, MD * INTRODUCTION GLAUCOMA OCCURRING EARLY FOLLOWING OCULAR TRAUMA Inflammation Alterations in
Glaucoma Associated With Ocular Trauma Chapter 11 GLAUCOMA ASSOCIATED WITH OCULAR TRAUMA NEIL T. CHOPLIN, MD * INTRODUCTION GLAUCOMA OCCURRING EARLY FOLLOWING OCULAR TRAUMA Inflammation Alterations in
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
5/18/2014. Fundamentals of Gonioscopy Workshop Aaron McNulty, OD, FAAO Walt Whitley, OD, MBA, FAAO
 1 Fundamentals of Gonioscopy Workshop Aaron McNulty, OD, FAAO Walt Whitley, OD, MBA, FAAO 2 3 4 5 6 Optometry s Meeting 2014 The Most Valuable Glaucoma Tool Glaucoma Diagnosis Gonioscopy Central corneal
1 Fundamentals of Gonioscopy Workshop Aaron McNulty, OD, FAAO Walt Whitley, OD, MBA, FAAO 2 3 4 5 6 Optometry s Meeting 2014 The Most Valuable Glaucoma Tool Glaucoma Diagnosis Gonioscopy Central corneal
Corporate Medical Policy
 Corporate Medical Policy Glaucoma, Evaluation by Ophthalmologic Techniques File Name: Origination: Last CAP Review: Next CAP Review: Last Review: glaucoma_evaluation_by_ophthalmologic_techniques 3/2001
Corporate Medical Policy Glaucoma, Evaluation by Ophthalmologic Techniques File Name: Origination: Last CAP Review: Next CAP Review: Last Review: glaucoma_evaluation_by_ophthalmologic_techniques 3/2001
Glaucoma Following Penetrating Ocular Trauma: A Cohort Study of the United States Eye Injury Registry
 Glaucoma Following Penetrating Ocular Trauma: A Cohort Study of the United States Eye Injury Registry CHRISTOPHER A. GIRKIN, MD, MPSH, GERALD MCGWIN, JR, PHD, ROBERT MORRIS, MD, AND FERENC KUHN, MD, PHD
Glaucoma Following Penetrating Ocular Trauma: A Cohort Study of the United States Eye Injury Registry CHRISTOPHER A. GIRKIN, MD, MPSH, GERALD MCGWIN, JR, PHD, ROBERT MORRIS, MD, AND FERENC KUHN, MD, PHD
non-perforating injury
 Brit. J. Ophthal. (I 972) 56, 418 Anterior chamber angle tears after non-perforating injury DAVID MOONEY Croydon Eye Unit, Croydon, Surrey Recession of the anterior chamber angle is a common finding after
Brit. J. Ophthal. (I 972) 56, 418 Anterior chamber angle tears after non-perforating injury DAVID MOONEY Croydon Eye Unit, Croydon, Surrey Recession of the anterior chamber angle is a common finding after
Angle recession and secondary glaucoma
 Brit. j. Ophthal. (I973) 57, 6o8 Angle recession and secondary glaucoma D. MOONEY Kent County Ophthalmic and Aural Hospital, Maidstone In a previous article (Mooney, I972), the incidence and extent of
Brit. j. Ophthal. (I973) 57, 6o8 Angle recession and secondary glaucoma D. MOONEY Kent County Ophthalmic and Aural Hospital, Maidstone In a previous article (Mooney, I972), the incidence and extent of
Orbital Doppler Evaluation of Blood Flow Velocities in Optic Neuritis
 Orbital Doppler Evaluation of Blood Flow Velocities in Optic Neuritis Mehdi Karami, MD 1 Mohsen Janghorbani, PhD 2 Alireza Dehghani, MD 3 Maryam Riahinejad, MD 4 Abstract Purpose: To evaluate orbital blood
Orbital Doppler Evaluation of Blood Flow Velocities in Optic Neuritis Mehdi Karami, MD 1 Mohsen Janghorbani, PhD 2 Alireza Dehghani, MD 3 Maryam Riahinejad, MD 4 Abstract Purpose: To evaluate orbital blood
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Medicina (Kaunas) 2013;49(7):310-4
 310 Clinical Investigation :310-4 The Effect of Nebulized Dorzolamide/Timolol Fixed Combination Mist versus Drops on Retrobulbar Blood Flow and Intraocular Pressure in Glaucoma Patients Ingrida Janulevičienė
310 Clinical Investigation :310-4 The Effect of Nebulized Dorzolamide/Timolol Fixed Combination Mist versus Drops on Retrobulbar Blood Flow and Intraocular Pressure in Glaucoma Patients Ingrida Janulevičienė
UC SF. g h. Eye Trauma. Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California
 UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
UC SF Eye Trauma sf g h Martha Neighbor, MD Emergency Services San Francisco General Hospital University of California Goals Recognize vision threatening eye emergencies Treat them when we can Know when
RADIOLOGY HEAD & NECK IMAGING. Iranian Journal of. Hadi Rokni Yazdi 1*, Safoura Faraji 2, Farokhlegha Ahmadi 3, Reza Shahmirzae 4
 HEAD & NECK IMAGING Iran J Radiol. 2012;9(1):12-16. DOI: 10.5812/iranjradiol.6730 Iranian Journal of RADIOLOGY RADIOLOGYwww.iranjradiol.com Color Doppler Indices of Orbital Arterial Flow in End-Stage Renal
HEAD & NECK IMAGING Iran J Radiol. 2012;9(1):12-16. DOI: 10.5812/iranjradiol.6730 Iranian Journal of RADIOLOGY RADIOLOGYwww.iranjradiol.com Color Doppler Indices of Orbital Arterial Flow in End-Stage Renal
Choroidal Blood Flow Change in Eyes with High Myopia
 pissn: 1011-892 eissn: 2092-9382 Korean J Ophthalmol 2015;29(5):309-31 http://dx.doi.org/10.331/kjo.2015.29.5.309 Choroidal Blood Flow Change in Eyes with High Myopia Original Article Young Seong Yang,
pissn: 1011-892 eissn: 2092-9382 Korean J Ophthalmol 2015;29(5):309-31 http://dx.doi.org/10.331/kjo.2015.29.5.309 Choroidal Blood Flow Change in Eyes with High Myopia Original Article Young Seong Yang,
Comparison of Intraocular Pressure Fluctuations Measured by Goldmann Applanation Tonometer and Pulsatile Ocular Blood Flow Analyser
 International journal of Biomedical science ORIGINAL ARTICLE Comparison of Intraocular Pressure Fluctuations Measured by Goldmann Applanation Tonometer and Pulsatile Ocular Blood Flow Analyser Ingrida
International journal of Biomedical science ORIGINAL ARTICLE Comparison of Intraocular Pressure Fluctuations Measured by Goldmann Applanation Tonometer and Pulsatile Ocular Blood Flow Analyser Ingrida
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
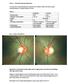 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Ocular and Periocular Trauma. Tina Rutar, MD. Assistant Professor of Ophthalmology and Pediatrics. Director, Visual Center for the Child
 Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Ocular and Periocular Trauma Tina Rutar, MD Assistant Professor of Ophthalmology and Pediatrics Director, Visual Center for the Child University of California, San Francisco Phone: 415-353-2560 Fax: 415-353-2468
Relation & Association of Mean Ocular Perfusion Pressure in Primary Open Angle Glaucoma
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. XII (May. 2017), PP 54-58 www.iosrjournals.org Relation & Association of Mean Ocular
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. XII (May. 2017), PP 54-58 www.iosrjournals.org Relation & Association of Mean Ocular
Injury. Contusion Lamellar Laceration Laceration Rupture. Penetrating IOFB. Perforating
 Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
3/16/2018. Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim. Prof. of Ophthalmology Al-Azhar University
 Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
T he pathogenic concepts of glaucoma, defined as a
 731 CLINICAL SCIENCE Colour Doppler imaging and fluorescein filling defects of the optic disc in normal tension glaucoma N Plange, A Remky, O Arend... See end of article for authors affiliations... Correspondence
731 CLINICAL SCIENCE Colour Doppler imaging and fluorescein filling defects of the optic disc in normal tension glaucoma N Plange, A Remky, O Arend... See end of article for authors affiliations... Correspondence
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
Understanding Angle Closure
 Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Eye Trauma. Lid Laceration. Orbital Fracture
 Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
Eye Trauma Lid Laceration The presence of a lid laceration, however insignificant, mandates careful exploration of the wound and examination of the globe. 1. Superficial lacerations parallel to the lid
_ Assessment of the anterior chamber. Review of anatomy of the angle
 Assessment of the anterior chamber Dr Simon Barnard PhD BSc FCOptom FAAO DCLP Department of Optometry & Visual Science City University London, UK Review of anatomy of the angle Figure 1. Anatomical section
Assessment of the anterior chamber Dr Simon Barnard PhD BSc FCOptom FAAO DCLP Department of Optometry & Visual Science City University London, UK Review of anatomy of the angle Figure 1. Anatomical section
Clinical Study Evaluation of Hemodynamic Parameters as Predictors of Glaucoma Progression
 Journal of Ophthalmology Volume 2011, Article ID 164320, 9 pages doi:10.1155/2011/164320 Clinical Study Evaluation of Hemodynamic Parameters as Predictors of Glaucoma Progression Ingrida Janulevičiene,
Journal of Ophthalmology Volume 2011, Article ID 164320, 9 pages doi:10.1155/2011/164320 Clinical Study Evaluation of Hemodynamic Parameters as Predictors of Glaucoma Progression Ingrida Janulevičiene,
@HUHEYE in Haiti 2018
 @HUHEYE in Haiti 2018 Eye Evaluation and Common Eye Diseases Leslie S. Jones, MD Associate Professor and Interim Chair Residency Program Director Glaucoma Services Director Department of Ophthalmology
@HUHEYE in Haiti 2018 Eye Evaluation and Common Eye Diseases Leslie S. Jones, MD Associate Professor and Interim Chair Residency Program Director Glaucoma Services Director Department of Ophthalmology
Carotid Abnormalities Coils, Kinks and Tortuosity David Lorelli M.D., RVT, FACS Michigan Vascular Association Conference Saturday, October 20, 2012
 Carotid Abnormalities Coils, Kinks and Tortuosity David Lorelli M.D., RVT, FACS Michigan Vascular Association Conference Saturday, October 20, 2012 Page 1 Table of Contents Carotid Anatomy Carotid Duplex
Carotid Abnormalities Coils, Kinks and Tortuosity David Lorelli M.D., RVT, FACS Michigan Vascular Association Conference Saturday, October 20, 2012 Page 1 Table of Contents Carotid Anatomy Carotid Duplex
Corporate Medical Policy
 Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
 European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
Diabetic Retinopathy and its Impact on Ocular Heamodynamics during Local Anesthesia Comparing Peribulbar and Subtenon in Phacoemulsification
 Med. J. Cairo Univ., Vol. 84, No. 2, December: 169-173, 2016 www.medicaljournalofcairouniversity.net Diabetic Retinopathy and its Impact on Ocular Heamodynamics during Local Anesthesia Comparing Peribulbar
Med. J. Cairo Univ., Vol. 84, No. 2, December: 169-173, 2016 www.medicaljournalofcairouniversity.net Diabetic Retinopathy and its Impact on Ocular Heamodynamics during Local Anesthesia Comparing Peribulbar
Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three cases
 Int Ophthalmol (2014) 34:913 917 DOI 10.1007/s10792-013-9862-z CASE REPORT Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three
Int Ophthalmol (2014) 34:913 917 DOI 10.1007/s10792-013-9862-z CASE REPORT Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three
Megalocornea is a non-progressive, uniformly
 Case Report 191 Anterior Megalophthalmos Chien-Kuang Tsai, MD; Ing-Chou Lai, MD; Hsi-Kung Kuo, MD; Mei-Chung Teng, MD; Po-Chiung Fang, MD We describe a 36-year-old female who suffered from presenile cataract
Case Report 191 Anterior Megalophthalmos Chien-Kuang Tsai, MD; Ing-Chou Lai, MD; Hsi-Kung Kuo, MD; Mei-Chung Teng, MD; Po-Chiung Fang, MD We describe a 36-year-old female who suffered from presenile cataract
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
NIH Public Access Author Manuscript Br J Ophthalmol. Author manuscript; available in PMC 2014 November 01.
 NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2014 November ; 98(11): 1551 1554. doi:10.1136/bjophthalmol-2013-304393. Optic Nerve Head Morphology in Glaucoma
NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2014 November ; 98(11): 1551 1554. doi:10.1136/bjophthalmol-2013-304393. Optic Nerve Head Morphology in Glaucoma
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs
 The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015
 Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
Gonioscopy and 3-Mirror Retinal Evaluation Workshop Edeline Lu, O.D., FAAO Benedicte Gonzalez, O.D., MPH, FAAO Tina Zheng, O.D.
 Gonioscopy and 3-Mirror Retinal Evaluation Workshop Edeline Lu, O.D., FAAO Benedicte Gonzalez, O.D., MPH, FAAO Tina Zheng, O.D., FAAO Please silence all mobile devices and remove items from chairs so others
Gonioscopy and 3-Mirror Retinal Evaluation Workshop Edeline Lu, O.D., FAAO Benedicte Gonzalez, O.D., MPH, FAAO Tina Zheng, O.D., FAAO Please silence all mobile devices and remove items from chairs so others
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
LEUKAEMIA*t INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC. pattemn * Received for pubiication November io, i967.
 Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3%
 The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Trabeculectomy - A Short Term Follow-up
 Trabeculectomy - A Short Term Follow-up Pages with reference to book, From 193 To 196 K.S. Hasan, G. Rabbani, S. Hashmani, M.M. Hasan ( Department of Ophthalmology Civil Hospital and Dow Medical College.
Trabeculectomy - A Short Term Follow-up Pages with reference to book, From 193 To 196 K.S. Hasan, G. Rabbani, S. Hashmani, M.M. Hasan ( Department of Ophthalmology Civil Hospital and Dow Medical College.
Sinus trabeculectomy. Preliminary results of IOO operations
 Brit. J. Ophthal. (I 972) 56, 833 Sinus trabeculectomy Preliminary results of IOO operations A. P. NESTEROV, N. V. FEDEROVA, AND Y. E. BATMANOV Department of Ophthalmology, Kazan Medical Institute, Kazan,
Brit. J. Ophthal. (I 972) 56, 833 Sinus trabeculectomy Preliminary results of IOO operations A. P. NESTEROV, N. V. FEDEROVA, AND Y. E. BATMANOV Department of Ophthalmology, Kazan Medical Institute, Kazan,
2/26/2017. Sameh Galal. M.D, FRCS Glasgow. Lecturer of Ophthalmology Research Institute of Ophthalmology
 Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Populations Interventions Comparators Outcomes Individuals: Who are being evaluated for angleclosure
 Protocol Optical Coherence Tomography of the Anterior Eye Segment (90318) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization No Review Dates: 07/11, 07/12, 07/13, 05/14,
Protocol Optical Coherence Tomography of the Anterior Eye Segment (90318) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization No Review Dates: 07/11, 07/12, 07/13, 05/14,
Downloaded from:
 Philippin, H; Shah, P; Burton, M (2012) The next step: Detailed assessment of an adult glaucoma patient. Community eye health / International Centre for Eye Health, 25 (79-80). pp. 50-53. ISSN 0953-6833
Philippin, H; Shah, P; Burton, M (2012) The next step: Detailed assessment of an adult glaucoma patient. Community eye health / International Centre for Eye Health, 25 (79-80). pp. 50-53. ISSN 0953-6833
Neuronal Activity Influences Hemodynamics in the Paraoptic Short Posterior Ciliary Arteries: A Comparison between Healthy and Glaucomatous Subjects
 Neuronal Activity Influences Hemodynamics in the Paraoptic Short Posterior Ciliary Arteries: A Comparison between Healthy and Glaucomatous Subjects Oliver Zeitz, Jeannette Mayer, Doreen Hufnagel, Ralf
Neuronal Activity Influences Hemodynamics in the Paraoptic Short Posterior Ciliary Arteries: A Comparison between Healthy and Glaucomatous Subjects Oliver Zeitz, Jeannette Mayer, Doreen Hufnagel, Ralf
2/5/2018. Trauma. Subdivided into two main categories: Closed globe Open Globe
 1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
1 2 3 4 5 Ocular Trauma Guide for Eye Care Office Staff Winter Thaw 2018 Aaron Yatskevich OD Definition A broad term used to describe a physical or chemical wound to the eye or eye socket. Ocular trauma
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
NERVE FIBER LAYER THICKNESS IN NORMALS AND GLAUCOMA PATIENTS
 Nerve fiber layer thickness in normals and glaucoma patients 403 NERVE FIBER LAYER THICKNESS IN NORMALS AND GLAUCOMA PATIENTS HIROTAKA SUZUMURA, KAYOKO HARASAWA, AKIKO KOBAYASHI and NARIYOSHI ENDO Department
Nerve fiber layer thickness in normals and glaucoma patients 403 NERVE FIBER LAYER THICKNESS IN NORMALS AND GLAUCOMA PATIENTS HIROTAKA SUZUMURA, KAYOKO HARASAWA, AKIKO KOBAYASHI and NARIYOSHI ENDO Department
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
5/2/2016 EYE EMERGENCIES. Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates. Anatomy. Tools
 EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
Complete Visual Rehabilitation in a Patient with No Light Perception after Surgical Management of a Penetrating Open-Globe Injury: A Case Report
 Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
INTRODUCTION S. HERDENER, D. HAFIZOVIC, M. PACHE, S. LAUTEBACH, J. FUNK. University Eye Hospital, Freiburg - Germany
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
TRAUMA, TRAUMA A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 10/24/2018 JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE
 TRAUMA, TRAUMA JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE OCT 26, 2018 A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 1 GROSS PICTURES LET S START WITH EYELIDS Lacerations
TRAUMA, TRAUMA JAMES LEE, M.D., ASSISTANT PROFESSOR TECHNICIAN CONFERENCE OCT 26, 2018 A YOUNG PARENT WOULD HAVE HEARD THE TITLE AND IMMEDIATELY THOUGHT 1 GROSS PICTURES LET S START WITH EYELIDS Lacerations
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA
 EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
A LITTLE ANATOMY. three layers of eye: 1. outer: corneosclera. 2. middle - uvea. anterior - iris,ciliary body. posterior - choroid
 GLAUCOMA A LITTLE ANATOMY three layers of eye: 1. outer: corneosclera 2. middle - uvea anterior - iris,ciliary body posterior - choroid connection at the pars plana between post and ant uvea 3. retina
GLAUCOMA A LITTLE ANATOMY three layers of eye: 1. outer: corneosclera 2. middle - uvea anterior - iris,ciliary body posterior - choroid connection at the pars plana between post and ant uvea 3. retina
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
MEASUREMENT OF OCULAR BLOOD FLOW VELOCITY USING COLOUR DOPPLER IMAGING IN LOW TENSION GLAUCOMA
 MEASUREMENT OF OCULAR BLOOD FLOW VELOCITY USING COLOUR DOPPLER IMAGING IN LOW TENSION GLAUCOMA ZAHIDA BUTT l, GRAHAM McKILLOP 2, COLM O'BRIEN l, PAUL ALLAN 2 and PETER ASPINALL 1 Edinburgh SUMMARY The
MEASUREMENT OF OCULAR BLOOD FLOW VELOCITY USING COLOUR DOPPLER IMAGING IN LOW TENSION GLAUCOMA ZAHIDA BUTT l, GRAHAM McKILLOP 2, COLM O'BRIEN l, PAUL ALLAN 2 and PETER ASPINALL 1 Edinburgh SUMMARY The
Ocular and periocular trauma
 Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Closed globe injuries, ocular and social consequences
 Closed globe injuries, ocular and social consequences Trauma is the set of local and general disorders that arise from the action of a violent foreign agent. Eye trauma is a pathology commonly found in
Closed globe injuries, ocular and social consequences Trauma is the set of local and general disorders that arise from the action of a violent foreign agent. Eye trauma is a pathology commonly found in
Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev S.K., Dr. Med. Sc., Prof.; Lazar Yu.M., Cand. Med. Sc.; Tatarina Yu.A., Junior Research Fellow
 Changes in corneoscleral rigidity and corneal thickness at various target intraocular pressures in patients with stabilized primary open-angle glaucoma Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev
Changes in corneoscleral rigidity and corneal thickness at various target intraocular pressures in patients with stabilized primary open-angle glaucoma Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev
Program= Loma Linda University Program
 OPHTHALMOLOGY: PROGRAM REPORT (Main Table) Reporting Period: Total Experience of Residents Completing rams in 2008-2009 ram=2400521023 - Loma Linda University ram [PART 1 ] rams in the Nation: 115 Residents
OPHTHALMOLOGY: PROGRAM REPORT (Main Table) Reporting Period: Total Experience of Residents Completing rams in 2008-2009 ram=2400521023 - Loma Linda University ram [PART 1 ] rams in the Nation: 115 Residents
TARGET: NORMAL TENSION GLAUCOMA
 Our official partner Alcon TARGET: NORMAL TENSION GLAUCOMA 14:30-18:00 Tuesday, September 4, 2012 Moscow Hotel: «Novotel Moscow Centre» Novoslobodskaya st. 3 CONFERENCE PROGRAM WELCOME DEAR COLLEAGUES
Our official partner Alcon TARGET: NORMAL TENSION GLAUCOMA 14:30-18:00 Tuesday, September 4, 2012 Moscow Hotel: «Novotel Moscow Centre» Novoslobodskaya st. 3 CONFERENCE PROGRAM WELCOME DEAR COLLEAGUES
EFFECT OF SYSTEMIC ADMINISTRATION OF HMG
 EFFECT OF SYSTEMIC ADMINISTRATION OF HMG Co A REDUCTASE INHIBITOR ATORVASTATIN ON CENTRAL RETINAL ARTERY FLOW DYNAMICS, INTRA OCULAR PRESSURE AND VISUAL FIELD CHANGES IN PRIMARY OPEN ANGLE GLAUCOMA AND
EFFECT OF SYSTEMIC ADMINISTRATION OF HMG Co A REDUCTASE INHIBITOR ATORVASTATIN ON CENTRAL RETINAL ARTERY FLOW DYNAMICS, INTRA OCULAR PRESSURE AND VISUAL FIELD CHANGES IN PRIMARY OPEN ANGLE GLAUCOMA AND
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Dr. D. Y. Patil Medical College, Pimpri, Pune
 Dr. D. Y. Patil Medical College, Pimpri, Pune - 411 018 Period : 04/July/16 to 22/September/16 Semester : 7 th Semester Department : Ophthalmology Lecture Lesson Plan Sr No Date Topic Learning objectives
Dr. D. Y. Patil Medical College, Pimpri, Pune - 411 018 Period : 04/July/16 to 22/September/16 Semester : 7 th Semester Department : Ophthalmology Lecture Lesson Plan Sr No Date Topic Learning objectives
C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma
 접수번호 : 2008-099 Korean Journal of Ophthalmology 2009;23:193-197 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.193 C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma Jaewan
접수번호 : 2008-099 Korean Journal of Ophthalmology 2009;23:193-197 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.193 C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma Jaewan
Routine OCT and UBM of the anterior segment
 Reprinted from No. 160 december 2012 Volume 17 Routine OCT and UBM of the anterior segment Michel Puech ISSN : 1274-5243 R e p r i n t e d w i t h t h e s u p p o r t o f t h e L a b o r a t o r y Q u
Reprinted from No. 160 december 2012 Volume 17 Routine OCT and UBM of the anterior segment Michel Puech ISSN : 1274-5243 R e p r i n t e d w i t h t h e s u p p o r t o f t h e L a b o r a t o r y Q u
CORRELATIONS BETWEEN SECONDARY GLAUCOM AND OCULAR HIPERTONY AFTER BLUNT TRAUMA
 Bulletin of the Transilvania University of Braşov Special Issue Series VI: Medical Sciences Vol. 10 (59) No. 2-2017 CORRELATIONS BETWEEN SECONDARY GLAUCOM AND OCULAR HIPERTONY AFTER BLUNT TRAUMA A.L. STUPARIU
Bulletin of the Transilvania University of Braşov Special Issue Series VI: Medical Sciences Vol. 10 (59) No. 2-2017 CORRELATIONS BETWEEN SECONDARY GLAUCOM AND OCULAR HIPERTONY AFTER BLUNT TRAUMA A.L. STUPARIU
OCULAR DISORDERS REPORT BOSTON TERRIER
 OCULAR DISORDERS REPORT BOSTON TERRIER 1991-1999 2000-2009 2010-2012 TOTAL DOGS EXAMINED 2723 6803 2004 Diagnostic Name # % # % # % GLOBE 0.110 microphthalmia 1 0.0% 1 0.0% 0 EYELIDS 20.140 ectopic cilia
OCULAR DISORDERS REPORT BOSTON TERRIER 1991-1999 2000-2009 2010-2012 TOTAL DOGS EXAMINED 2723 6803 2004 Diagnostic Name # % # % # % GLOBE 0.110 microphthalmia 1 0.0% 1 0.0% 0 EYELIDS 20.140 ectopic cilia
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Ultrasound Evaluation of the Posterior Segment of the Eye A Ready Reckoner
 180 Kerala Journal of Ophthalmology Vol. XX, No. 2 OPHTHALMIC INSTRUMENTATION Ultrasound Evaluation of the Posterior Segment of the Eye A Ready Reckoner Dr. Mahesh G. MS DO DNB FRCSEd., Dr. A. Giridhar
180 Kerala Journal of Ophthalmology Vol. XX, No. 2 OPHTHALMIC INSTRUMENTATION Ultrasound Evaluation of the Posterior Segment of the Eye A Ready Reckoner Dr. Mahesh G. MS DO DNB FRCSEd., Dr. A. Giridhar
CASE PRESENTATION. DR.Sravani 1 st yr PG Dept of Ophthalmology
 CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
Correlation between presence of primary irisand cilliary body cysts and intraocular pressure
 European Review for Medical and Pharmacological Sciences 2017; 21: 3985-3989 Correlation between presence of primary irisand cilliary body cysts and intraocular pressure R. ZHU, L. CHENG, D.-M. WANG Institute
European Review for Medical and Pharmacological Sciences 2017; 21: 3985-3989 Correlation between presence of primary irisand cilliary body cysts and intraocular pressure R. ZHU, L. CHENG, D.-M. WANG Institute
02/03/2014. Average Length: 23mm (Infant ~16mm) Approximately the size of a quarter Volume: ~5mL
 Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
Identify the anatomy of the eye. Explain the basic physiology of the parts of the eye. Briefly discuss various surgeries related to different parts of the anatomy. Average Length: 23mm (Infant ~16mm) Approximately
