(Received for Publication: August 18, 2016) Key words Interventional bronchoscopy, computed tomography, cross-sectional area, pulmonary vessels
|
|
|
- Malcolm Chase
- 5 years ago
- Views:
Transcription
1 77 Original Article J. St. Marianna Univ. Vol. 7, pp , 2016 Changes in the Cross-sectional Area of Pulmonary Small Vessels Assessed via Chest Computed Tomography after Interventional Bronchoscopy in Patients with Airway Obstruction Due to a Malignant Disease Hiromi Muraoka 1, Hiroki Nishine 1, Takeo Inoue 1, Teruomi Miyazawa 1, and Masamichi Mineshita 1 (Received for Publication: August 18, 2016) Abstract Background: Pulmonary perfusion scintigraphy is a useful method to assess improvements in airflow limitation. However, the number of institutions equipped with pulmonary perfusion scintigraphy equipment is limited. Computed tomography (CT) scans are quick to perform and can be performed in severe cases. Recently, it has been reported that the percentage of the cross-sectional area of pulmonary small vessels (%CSA<5) can be measured by analyzing CT images that correlate with the radionuclide uptake rate shown by pulmonary perfusion scintigraphy. Methods: We retrospectively reviewed CT scans of 14 patients with unilateral bronchial obstruction due to malignant disease to measure the %CSA<5 before and after interventional bronchoscopy using the semi-automatic image-processing program (ImageJ). In 5 cases, we examined the correlation between the %CSA<5 and the radionuclide uptake rate visualized by pulmonary perfusion scintigraphy. Results: The %CSA<5 in the obstructed side of the lung after treatment displayed significant improvements after intervention (p = 0.04). Among the 5 cases that underwent pulmonary perfusion scintigraphy before and after the treatment, the radionuclide uptake rate of the obstructed side improved in all patients, whereas the %CSA<5 improved in 4 of the 5 patients. Conclusion: Measurement of the %CSA<5 might be useful to assess the outcome of interventional bronchoscopy. Key words Interventional bronchoscopy, computed tomography, cross-sectional area, pulmonary vessels Introduction Severe airway obstruction due to malignant disease can cause symptoms such as dyspnoea, wheezing, and failure to expectorate mucus, and is often associated with complicated atelectasis and lung abscess. Patients suffering from airway obstruction can receive significant relief from life-threatening symptoms via interventional bronchoscopy, and performing interventional bronchoscopy at the exact location of the obstruction can provide the greatest functional benefit to patients 1 10). It is essential to improve obstructions, usually using chemotherapy and radiation as the first choice of treatment 11,12). However, if the airway obstruction is predominantly due to extrinsic compression by tumour or metastatic lymph nodes, interventional bronchoscopy should be considered. In physiological assessments, we have noted distinct flow-volume curve patterns specific to the type of obstruction 10). Although flow-volume curves are widely used and easy to generate in daily clinical set Division of Respiratory Disease, Department of Internal Medicine, St. Marianna University School of Medicine 47
2 78 Muraoka H Nishine H et al tings, they cannot discriminate between the left and right lungs. Furthermore, in patients with bronchial obstructions, pulmonary function tests may not show significant changes after intervention 13). Hauck et al. reported that the normalization of blood flow via interventional bronchoscopy in patients with bronchial obstruction showed improvements for ventilation in the obstructed side of the lung 14). Pulmonary perfusion scintigraphy requires approximately 30 minutes to perform, and it is difficult for patients with airway obstructions to remain in a supine position for long periods of time. Furthermore, there are few institutions that are equipped with the necessary equipment to perform pulmonary perfusion scintigraphy. On the other hand, the time required for CT imaging is very short, making it suitable even in severe cases. Recently, it was reported that the cross-sectional area (CSA) measured by analyzing CT images correlates with the radionuclide uptake rates shown by pulmonary perfusion scintigraphy 15). In this study, we retrospectively investigated the changes in CSA in patients with unilateral bronchial obstruction due to a malignant disease to evaluate the effects of interventional bronchoscopy. Material and Methods Subjects We retrospectively reviewed CT scans of patients who were referred to our institution between April 2008 and March This study was approved by our institutional review board, waiving the need for informed consent (approval number 3126). We selected CT scans of adult patients who met all the following criteria: patients with unilateral bronchial obstruction due to a malignant disease who underwent interventional bronchoscopy, and patients with CT scans performed within 7 days before and after the interventional procedures. We excluded cases with abnormal parenchymal lesions or unclear CT images that prevented analysis using the software. We examined correlations between CSA and the radionuclide uptake rate shown by pulmonary perfusion scintigraphy. Computed Tomography (CT) CT examinations were performed using a 16-, 64-, or 80-detector CT scanner (Aquilion 16, Aquilion 64, and Aquilion Prime, Nasu, Japan, Toshiba Medical Systems). CT was performed during a breath-hold at a deep inspiration with the patient in the supine position. The MDCT parameters were as follows: 120 kv and ma; collimation, 0.5 mm; gantry rotation time, 0.5 s; and a beam pitch of All images were reconstructed using a standard reconstruction algorithm with a slice thickness of 1 mm 15). CT Measurement of Pulmonary Small Vessels CT measurements of pulmonary CSA have been described in previous literature 17,18). In brief, the following procedures were performed. For measurements of pulmonary CSA, all CT images (1-mm slice thickness) at 1-cm intervals were selected from approximately 1 cm below the apex to approximately 1 cm above the base of the lung. Measurements were performed for the upper, middle and lower regions of the affected lung. CT images were divided into upper, middle and lower zones. The upper zone was defined as CT sections located above the aortic arch, the middle zone located below the carina, and the lower zone located below the inferior pulmonary vein. These CT images were analyzed using a semiautomatic imageprocessing program, ImageJ version 1.49v (imagej.nih.gov). CSA measurements were conducted as follows: first, the lung field was segmented using a threshold technique with all pixels between 500 and 1024 HU on each CT image (Fig. 1A). Next, the segmented images were converted into binary images with a window level of 720 HU. Using the Analyze Particles function of ImageJ, which can count and measure objects into binary images, the number of vessels of a specified size, and the CSA of each size range on every CT slice were determined. Simultaneously, vessels that ran oblique or parallel to the slice were excluded using the Circularity function of ImageJ, where circularity was calculated as 4π [area / (perimeter) 2 ] of the structure of interest. Circularity values can range from 0 (straight line) to 1.0 (circle), and a range of circularity from 0.9 to 1.0 was used so that only vessels that ran essentially perpendicular to the plane of the CT slice, based on their shape in the image, were analyzed. We measured the CSA of vessels less than 5 mm 2 (CSA<5), which showed the highest correlation with pulmonary blood flow 15). Measurements were performed for the upper, middle and lower zones of the affected lung. The areas of all vessels with a CSA<5 were calculated and summed in each image slice and expressed as a percentage of the area in the measured field of the affected-side lung (%CSA<5) 48
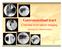
3 Changes in cross-sectional area of pulmonary vessels after interventional bronchoscopy 79 Figure 1. Measurement of the cross-sectional area of pulmonary small vessels using ImageJ software A) CT image shows the lung field segmented within threshold values from 500 to 1024 HU. B) CT image segments in A with a window level of 720 HU. C) Binary image converted from B. D) Mask image was obtained for a particle analysis after setting the vessel size parameters to within 0 5 mm 2 and circularity levels to within (circularity was calculated as 4π [area / (perimeter) 2 ], and values range from 0 [straight line] to 1.0 [circle]). for each image. Pulmonary Perfusion Scintigraphy Six static views with anterior, posterior, and right-to-left lateral, oblique posterior, and anterior projections were acquired immediately after an IV injection of MBq of 99mTc-MAA using gamma cameras. Using anteroposterior and posteroanterior projections, regions of interest were manually drawn around the right and left lungs. Lung counts were averaged for anterior and posterior projections. We determined right, left and total lung counts and then calculated the percentage of the affected side relative to the whole lung (%MAA affected/w). Statistical Analysis All statistical analyses were performed using SPSS Statistics version 19 (SPSS Inc., Chicago, IL, USA). The %CSA<5 of the affected side was statistically analyzed. P values were considered significant at less than Significant differences in %CSA<5 and %MAA affected/w before and after interventional bronchoscopy were evaluated using Wilcoxon signed-rank tests. Results Of the 30 cases considered for assessment, 3 cases were excluded because interventional bronchoscopy was undertaken at the healthy lung side, and 13 cases were excluded due to a change in lung lesions after bronchoscopy, making them unsuitable for image analysis. The characteristics of the remaining 14 cases included in this study are shown in Table 1. Symptoms and pulmonary function test (PFT) results significantly improved for all patients (Table 2). There was no statistical correlation between PFTs and %CSA<5 in the 9 cases in which PFTs could be performed. The %CSA<5 of the obstructed side of the lung displayed significant improvements after intervention (p = 0.04) (Fig. 2). In addition, of the 5 cases that underwent pulmonary perfusion scintigraphy and CT within 7 days before and after treatment, improvements in %CSA<5 were seen in 4 cases, while the %MAA im Sex, n (%) Table 1. Patient Characteristics Female 6 (42.9) Male 8 (57.1) Median age (range) 59.93(40-72) Disease, n (%) Lung Cancer 9 (64.3) Oesophageal Cancer 2 (14.3) Cervical Cancer 1 (7.1) Malignant lymphoma 1 (7.1) Malignant melanoma 1 (7.1) Affected side, n (%) Right 6 (42.9) Left 8 (57.1) Treatment, n (%) Stenting 14 (100) Ballooning 3 (21.4) Argon plasma coagulation 2 (14.3) 49
4 80 Muraoka H Nishine H et al Table 2. Changes in Pulmonary Function Test Results and Modified Medical Research Council Scale Scores Before treatment After treatment PFTs (n = 9) FVC(l) 2.12± ±0.78* (FVC/predicted FVC,%) 70.2± ±20.86* FEV1(l) 1.02± ±0.57* (FEV1/predicted FEV1, %) 41.9± ±16.15* FEV1/FVC% 70.94± ±11.35 PEF 2.39± ±1.41* MMRC (n = 13) 3±1.26 1±0.93* Definition of abbreviation: FVC = forced vital capacity, FEV1 = forced expiratory volume in one second, PEF = peak expiratory flow, MMRC = Modified Medical Research Council Scale. one second, PEF = peak expiratory flow, MMRC = Modified Medical Research Council Scale. Mean values(±sd) are given for FVC, FVC/predicated FVC, FEV1, FEV1/predicated FEV1, FEV1/FVC%, Mean values(±sd) PEF and are given MMRC. for FVC, FVC/predicated FVC, FEV1, FEV1/predicated FEV1, * p < 0.04 after treatment vs. before treatment. FEV /FVC%, PEF and MMRC. %CSA< Figure 2. Before P=0.04 After Changes in the %CSA<5 before and after treatment Each line represents the change in %CSA<5 before and after treatment. proved after treatment in all cases (Table 3). In a 72-year-old female patient with lung cancer, CT showed an extrinsic compression of the left main bronchus at the location of metastatic lymph nodes (Fig. 3A). We performed balloon dilation at the left main bronchus and placed a silicone Y stent from the trachea to both main bronchi (Fig. 3B). After the procedure, the airway obstruction was eliminated, and the %CSA<5 of the affected side improved from 1.528% to 1.885% (Fig. 3C and D, respectively). The %MAA of the affected side also improved from 13% to 59.4% (Fig. 3E and F, respectively). Discussion In this study, the cross-sectional area of pulmonary small vessels improved after interventional bronchoscopy in cases of unilateral bronchial obstruction. CT is non-invasive and can be performed in many hospitals, and it is applicable in severe cases. Thus, CT analysis appears to be useful in evaluating the effectiveness of treatment in cases where PFTs or quantitative pulmonary perfusion scintigraphy could not be performed. Furthermore, evaluation of the %CSA <5 via CT was effective to asess treatment effects in emergent cases. This is the first report to demonstrate improvements in the %CSA<5 after removing airflow limitations. Matsuoka reported that the %CSA<5 was found to have a negative correlation with the extent of emphysema, degree of airflow limitation, and severity of pulmonary hypertension 15 17). Further, Karayama reported that the %CSA<5 significantly decreased after chemotherapy and mentioned that this result was indicative of the potential vascular toxicity induced by 50
5 Changes in cross-sectional area of pulmonary vessels after interventional bronchoscopy 81 Table 3. Results of 5 Cases that Underwent Both CT and Pulmonary Perfusion Scintigraphy No. Disease Affected Pre-%MAA Post-%MAA Pre-%CSA<5 Post-%CSA<5 (%) side affected/w (%) affected/w (%) (%) 1 Cervical Ca right Lung Ca left Oesophageal Ca left Lung Ca left Lung Ca left Definition of abbreviations: Ca = cancer, Pre-%MAA affected/w = the percentage of the affected side relative to the whole lung before treatment, Post-%MAA affected/w = the percentage of the affected side relative to the whole lung after treatment, Pre-%CSA<5 = the percentage of the cross-sectional area of pulmonary vessels less than 5 mm 2 before treatment, Post-%CSA<5 = the percentage of the cross-sectional area of pulmonary vessels less than 5 mm 2 after treatment %MAA significantly improved after treatment (p=0.04). %CSA<5 did not improve significantly after treatment (p=0.138). chemotherapy 18). In this study, the %CSA<5 improvement in the affected side of the lung was observed after the dilation of a unilateral bronchial obstruction via interventional bronchoscopy. A possible mechanism for this improvement is the amelioration of the hypoxic pulmonary vasoconstriction (HPV) caused by airway obstruction. HPV is a fundamental physiological process whereby ventilation/perfusion matching is optimized through the constriction of the pulmonary circulation supplying poorly ventilated lung units 19). Airway obstruction caused by malignant diseases may cause HPV, leading to decreases in blood flow perfusion. After interventional bronchoscopy, the improvement of hypoxic conditions in the affected lung may relieve HPV. The %CSA improvement observed in this study is considered to be indicative of increases in lung perfusion due to the elimination of HPV. Case 2 in Table 3 did not show a correlation between %CSA<5 and %MAA. For this case, the left bronchus was obstructed on CT, but intraoperative endoscope revealed a stenosis in the right bronchus confirming bilateral airway obstruction. Therefore, there was no reduction in %MAA prior to treatment. Thus, %CSA<5 cannot be used in cases of bilateral airway obstruction that cannot be found before treatment. In this study, there was no statistical correlation between PFTs and %CSA<5 in the 9 cases in which PFTs could be performed. Possible reasons for the results are as follows: small numbers of cases and the exclusion of cases that improved clinically without performing PFTs because of the patient undergoing intubation before treatment. We acknowledge that this study had some limitations. First, there were some situations in which the evaluation of %CSA<5 via CT could not be performed due to lung field abnormalities, such as atelectasis and pneumonia. Second, ventilation scintigraphy was not performed in this study. Thus, we could not accurately evaluate improvements in ventilation after the treatment. Third, this method cannot be used in cases of bilateral airway obstruction that cannot be found before treatment. Fourth, the correlation between %CSA<5 and %MAA could not be evaluated statistically because there are only 5 cases of CT and pulmonary perfusion scintigraphy before and after treatment. In conclusion, the %CSA<5 of the affected lungs significantly improved after the removal of airflow limitations, and the %CSA<5 assessed via CT might be a useful measure to evaluate improvements in pulmonary blood flow after treatment. References 1) Seijo LM, Sterman DH. Interventional pulmonology. N Engl J Med 2001; 344: ) Dumon JF. A dedicated tracheobronchial stent. Chest 1990; 97: ) Herth F, Becker HD, LoCicero J 3rd, Thurer R, Ernst A. Successful bronchoscopic placement of tracheobronchial stents without fluoroscopy. Chest 2001; 119: ) Saad CP, Murthy S, Krizmanich G, Mehta AC. 51
6 82 Muraoka H Nishine H et al A C E Figure year-old woman with bronchial stenosis A) 3D image of the bronchial stenosis before stenting. B) 3D image of the bronchial stenosis after stenting. C) Pulmonary perfusion scintigraphy before stenting; a decrease in left pulmonary perfusion is evident. D) Pulmonary perfusion scintigraphy after stenting. The CSA<5 measurements of pulmonary vessels are shown in CT image E) before treatment and F) after treatment. F) Plots of the increases compared with values in E. Self-expandable metallic airway stents and flexible bronchoscopy: long-term outcomes analysis. Chest 2003; 124: ) Miyazawa T, Arita K. Airway stenting in Japan. Respirology 1998; 3: ) Miyazawa T1, Yamakido M, Ikeda S, Furukawa K, Takiguchi Y, Tada H, Shirakusa T. Implantation of Ultraflex nitinol stents in malignant tracheobronchial stenoses. Chest 2000; 118: ) Ernst A, Feller-Kopman D, Becker HD, Mehta AC. Central airway obstruction. Am J Respir Crit Care Med 2003; 169: B D F 8) Ryu YJ, Kim H, Yu CM, Choi JC, Kwon YS, Kwon OJ. Use of silicone stents for the management of post-tuberculosis tracheobronchial stenosis. Eur Respir J 2006; 28: ) Oki M, Saka H. Double Y-stenting for tracheobronchial stenosis. Eur Respir J 2012; 40: ) Miyazawa T, Miyazu Y, Iwamoto Y, Ishida A, Kanoh K, Sumiyoshi H, Doi M, Kurimoto N. Stenting at the Flow-limiting segment in tracheobronchial stenosis due to lung cancer. Am J Respir Crit Care Med 2004; 169: ) Dumon JF. A dedicated tracheobronchial stent. Chest 1990; 97: ) Herth F, Becker HD, LoCicero J 3rd, Thurer R, Ernst A. Successful bronchoscopic placement of tracheobronchial stents without fluoroscopy. Chest 2001; 119: ) Ploy-Song-Sang Y, Martin RR, Ross WR, Loudon RG, Macklem PT. Breath sounds and regional ventilation. Am Rev Respir Dis 1977; 116: ) Hauck RW, Römer W, Schulz C, Lembeck RM, Schömig A, Schwaiger M. Ventilation perfusion scintigraphy and lung function testing to assess metal stent efficacy. J Nucl Med 1997; 38: ) Matsuoka S, Yamashiro T, Matsushita S, Fujikawa A, Yagihashi K, Kurihara Y, Nakajima Y. Relationship between quantitative CT of pulmonary small vessels and pulmonary perfusion. AJR Am J Roentgenol 2014; 202: ) Matsuoka S, Washko GR, Dransfield MT, Yamashiro T, San Jose Estepar R, Diaz A, Silverman EK, Patz S, Hatabu H. Quantitative CT measurement of cross-sectional area of small pulmonary vessel in COPD: correlations with emphysema and airflow limitation. Acad Radiol 2010; 17: ) Matsuoka S, Washko GR, Yamashiro T, Estepar RS, Diaz A, Silverman EK, Hoffman E, Fessler HE, Criner GJ, Marchetti N, Scharf SM, Martinez FJ, Reilly JJ, Hatabu H; National Emphysema Treatment Trial Research Group. Pulmonary hypertension and computed tomography measurement of small pulmonary vessels in severe emphysema. Am J Respir Crit Care Med 2010; 181: ) Karayama M, Inui N, Kusagaya H, Suzuki S, Inoue Y, Enomoto N, Fujisawa T, Nakamura Y, Suda T. Changes in cross-sectional area of pul 52
7 Changes in cross-sectional area of pulmonary vessels after interventional bronchoscopy 83 monary vessels on chest computed tomography after chemotherapy in patients with advanced non-squamous non-small-cell lung cancer. Cancer Chemother Pharmacol 2016; 77: ) Sylvester JT, Shimoda LA, Aaronson PI, Ward JP. Hypoxic pulmonary vasoconstriction. Physiol Rev 2012; 92:
Since central airway stenosis is often a lifethreatening. Double Y-stenting for tracheobronchial stenosis. Masahide Oki and Hideo Saka
 Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Therapeutic bronchoscopy for malignant airway stenoses: Choice of modality and survival
 Original Article Free full text available from www.cancerjournal.net Therapeutic bronchoscopy for malignant airway stenoses: Choice of modality and survival ABSTRACT Background: There are no data regarding
Original Article Free full text available from www.cancerjournal.net Therapeutic bronchoscopy for malignant airway stenoses: Choice of modality and survival ABSTRACT Background: There are no data regarding
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Stenting at the Flow-limiting Segment in Tracheobronchial Stenosis due to Lung Cancer
 Stenting at the Flow-limiting Segment in Tracheobronchial Stenosis due to Lung Cancer Teruomi Miyazawa, Yuka Miyazu, Yasuo Iwamoto, Atsuko Ishida, Koji Kanoh, Hidetaka Sumiyoshi, Masao Doi, and Noriaki
Stenting at the Flow-limiting Segment in Tracheobronchial Stenosis due to Lung Cancer Teruomi Miyazawa, Yuka Miyazu, Yasuo Iwamoto, Atsuko Ishida, Koji Kanoh, Hidetaka Sumiyoshi, Masao Doi, and Noriaki
New Horizons in the Imaging of the Lung
 New Horizons in the Imaging of the Lung Postprocessing. How to do it and when do we need it? Peter M.A. van Ooijen, MSc, PhD Principal Investigator, Radiology, UMCG Discipline Leader Medical Imaging Informatics
New Horizons in the Imaging of the Lung Postprocessing. How to do it and when do we need it? Peter M.A. van Ooijen, MSc, PhD Principal Investigator, Radiology, UMCG Discipline Leader Medical Imaging Informatics
DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA
 Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
HRCT Versus Volume Rendering (Three Colors, Three Densities Lung Images) in Diagnosis of Small Airway Disease: A Comparative Study
 Med. J. Cairo Univ., Vol. 84, No. 1, March: 359-364, 2016 www.medicaljournalofcairouniversity.net HRCT Versus Volume Rendering (Three Colors, Three Densities Lung Images) in Diagnosis of Small Airway Disease:
Med. J. Cairo Univ., Vol. 84, No. 1, March: 359-364, 2016 www.medicaljournalofcairouniversity.net HRCT Versus Volume Rendering (Three Colors, Three Densities Lung Images) in Diagnosis of Small Airway Disease:
Quantitative CT Measurement of Cross-sectional Area of Small Pulmonary Vessel in COPD:
 Quantitative CT Measurement of Cross-sectional Area of Small Pulmonary Vessel in COPD: Correlations with Emphysema and Airflow Limitation Shin Matsuoka, MD, PhD, George R. Washko, MD, Mark T. Dransfield,
Quantitative CT Measurement of Cross-sectional Area of Small Pulmonary Vessel in COPD: Correlations with Emphysema and Airflow Limitation Shin Matsuoka, MD, PhD, George R. Washko, MD, Mark T. Dransfield,
4/24/2017. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis Endoscopic & Surgical Management
 Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Ventilation / Perfusion Imaging for Pulmonary Embolic Disease
 Ventilation / Perfusion Imaging for Pulmonary Embolic Disease 1. Purpose This guideline must be read in conjunction with the BNMS Generic Guidelines. The purpose of this guideline is to assist specialists
Ventilation / Perfusion Imaging for Pulmonary Embolic Disease 1. Purpose This guideline must be read in conjunction with the BNMS Generic Guidelines. The purpose of this guideline is to assist specialists
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
SPIRATION VALVE SYSTEM Patient Selection for the Treatment of Emphysema Based on Clinical Literature.
 SPIRATION VALVE SYSTEM Patient Selection for the Treatment of Emphysema Based on Clinical Literature. SPIRATION VALVE SYSTEM The Spiration Valve System is a device placed in the lung airway to treat severely
SPIRATION VALVE SYSTEM Patient Selection for the Treatment of Emphysema Based on Clinical Literature. SPIRATION VALVE SYSTEM The Spiration Valve System is a device placed in the lung airway to treat severely
Quantitative CT in Chronic Obstructive Pulmonary Disease: Inspiratory and Expiratory Assessment
 Cardiopulmonary Imaging Original Research kira et al. CT of Chronic Obstructive Pulmonary Disease Cardiopulmonary Imaging Original Research Masanori kira 1 Kazushige Toyokawa 1 Yoshikazu Inoue 2 Toru rai
Cardiopulmonary Imaging Original Research kira et al. CT of Chronic Obstructive Pulmonary Disease Cardiopulmonary Imaging Original Research Masanori kira 1 Kazushige Toyokawa 1 Yoshikazu Inoue 2 Toru rai
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
Scientific Exhibit. Authors: D. Takenaka, Y. Ohno, Y. Onishi, K. Matsumoto, T.
 The feasibility of biphasic contrast-media-injection-protocol for chest imaging on 320-slice volume MDCT: Direct comparison of biphasic and bolus contrast-media injection protocols on 320-slice volume
The feasibility of biphasic contrast-media-injection-protocol for chest imaging on 320-slice volume MDCT: Direct comparison of biphasic and bolus contrast-media injection protocols on 320-slice volume
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
of the right B 10 fourth, r = 0.476, p < ; B 10
 Yamashiro et al. CT of Chronic Obstructive Pulmonary Disease Cardiopulmonary Imaging Original Research Tsuneo Yamashiro 1,2 Shin Matsuoka 3 Raúl San José Estépar 4 Mark T. Dransfield 5 Alejandro Diaz 6,7
Yamashiro et al. CT of Chronic Obstructive Pulmonary Disease Cardiopulmonary Imaging Original Research Tsuneo Yamashiro 1,2 Shin Matsuoka 3 Raúl San José Estépar 4 Mark T. Dransfield 5 Alejandro Diaz 6,7
Metallic stent and flexible bronchoscopy without fluoroscopy for acute respiratory failure
 Eur Respir J 2008; 31: 1019 1023 DOI: 10.1183/09031936.00099507 CopyrightßERS Journals Ltd 2008 Metallic stent and flexible bronchoscopy without fluoroscopy for acute respiratory failure S-M. Lin*,#, T-Y.
Eur Respir J 2008; 31: 1019 1023 DOI: 10.1183/09031936.00099507 CopyrightßERS Journals Ltd 2008 Metallic stent and flexible bronchoscopy without fluoroscopy for acute respiratory failure S-M. Lin*,#, T-Y.
Rigid Bronchoscopic Intervention in Patients with Respiratory Failure Caused by Malignant Central Airway Obstruction
 ORIGINAL ARTICLE Rigid Bronchoscopic Intervention in Patients with Respiratory Failure Caused by Malignant Central Airway Obstruction Kyeongman Jeon, MD, Hojoong Kim, MD, Chang-Min Yu, MD, Won-Jung Koh,
ORIGINAL ARTICLE Rigid Bronchoscopic Intervention in Patients with Respiratory Failure Caused by Malignant Central Airway Obstruction Kyeongman Jeon, MD, Hojoong Kim, MD, Chang-Min Yu, MD, Won-Jung Koh,
Cardiopulmonary Imaging Original Research
 Cardiopulmonary Imaging Original Research Yamashiro et al. CT of Chronic Obstructive Pulmonary Disease Downloaded from www.ajronline.org by 37.44.197.226 on 12/3/17 from IP address 37.44.197.226. Copyright
Cardiopulmonary Imaging Original Research Yamashiro et al. CT of Chronic Obstructive Pulmonary Disease Downloaded from www.ajronline.org by 37.44.197.226 on 12/3/17 from IP address 37.44.197.226. Copyright
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions
 Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions Original Effective Date: 8/25/14 Policy Number: MCP-206 Revision Date(s): Review
Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions Original Effective Date: 8/25/14 Policy Number: MCP-206 Revision Date(s): Review
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
Imaging Emphysema 3-Helium MR Imaging
 Imaging Emphysema 3-Helium MR Imaging Edwin J.R. van Beek MD PhD MEd FRCR Professor of Radiology and Medicine Carver College of Medicine, University of Iowa, USA. Permanent Visiting Professor of Radiology,
Imaging Emphysema 3-Helium MR Imaging Edwin J.R. van Beek MD PhD MEd FRCR Professor of Radiology and Medicine Carver College of Medicine, University of Iowa, USA. Permanent Visiting Professor of Radiology,
Airway stenting in excessive central airway collapse
 Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II)
Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II)
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
Comparison of CT findings between MDR-TB and XDR-TB
 Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
Quantitative assessment of cross-sectional area of. small pulmonary vessels in patients with COPD. using inspiratory and expiratory MDCT
 Quantitative assessment of cross-sectional area of small pulmonary vessels in patients with COPD using inspiratory and expiratory MDCT ( 慢性閉塞性肺疾患における吸気呼気 CT を用いた 肺末梢血管面積の定量的評価 ) 千葉大学大学院医学薬学府環境健康科学専攻 (
Quantitative assessment of cross-sectional area of small pulmonary vessels in patients with COPD using inspiratory and expiratory MDCT ( 慢性閉塞性肺疾患における吸気呼気 CT を用いた 肺末梢血管面積の定量的評価 ) 千葉大学大学院医学薬学府環境健康科学専攻 (
Lung Perfusion Analysis New Pathways in Lung Imaging. Case Study Brochure PLA 309 Hospital
 Lung Perfusion Analysis New Pathways in Lung Imaging Case Study Brochure PLA 309 Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2012 all rights reserved. Design and specifications
Lung Perfusion Analysis New Pathways in Lung Imaging Case Study Brochure PLA 309 Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2012 all rights reserved. Design and specifications
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Are metallic stents really safe? A long-term analysis in lung transplant recipients
 Eur Respir J 2009; 34: 1417 1422 DOI: 10.1183/09031936.00041909 CopyrightßERS Journals Ltd 2009 Are metallic stents really safe? A long-term analysis in lung transplant recipients J. Gottlieb*, T. Fuehner*,
Eur Respir J 2009; 34: 1417 1422 DOI: 10.1183/09031936.00041909 CopyrightßERS Journals Ltd 2009 Are metallic stents really safe? A long-term analysis in lung transplant recipients J. Gottlieb*, T. Fuehner*,
Temporary placement of metallic stent could lead to long-term benefits for benign tracheobronchial stenosis
 Original Article on Airway Obstruction Temporary placement of metallic stent could lead to long-term benefits for benign tracheobronchial stenosis Guo-Wu Zhou*, Hai-Dong Huang*, Qin-Ying Sun*, Ye Xiong*,
Original Article on Airway Obstruction Temporary placement of metallic stent could lead to long-term benefits for benign tracheobronchial stenosis Guo-Wu Zhou*, Hai-Dong Huang*, Qin-Ying Sun*, Ye Xiong*,
Wheeze. Dr Jo Harrison
 Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Improvement of Image Quality with ß-Blocker Premedication on ECG-Gated 16-MDCT Coronary Angiography
 16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
Airway stenosis: CT evaluation of endoscopic treatment
 Airway stenosis: CT evaluation of endoscopic treatment Poster No.: C-0334 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Maggialetti, M. Ficco, A. A. A. Stabile Ianora, M. Moschetta, A. Scardapane,
Airway stenosis: CT evaluation of endoscopic treatment Poster No.: C-0334 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Maggialetti, M. Ficco, A. A. A. Stabile Ianora, M. Moschetta, A. Scardapane,
Three Cuts Method for Identification of COPD
 ORIGINAL REPORT Three Cuts Method for Identification of COPD Mohammad-Parsa Hosseini 1,2, Hamid Soltanian-Zadeh 2,3, and Shahram Akhlaghpoor 4 1 Department of Electrical & Computer Engineering, Wayne State
ORIGINAL REPORT Three Cuts Method for Identification of COPD Mohammad-Parsa Hosseini 1,2, Hamid Soltanian-Zadeh 2,3, and Shahram Akhlaghpoor 4 1 Department of Electrical & Computer Engineering, Wayne State
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
 European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
Metallic Stent and Flexible Bronchoscopy without Fluoroscopy for
 ERJ Express. Published on January 9, 2008 as doi: 10.1183/09031936.00099507 Metallic Stent and Flexible Bronchoscopy without Fluoroscopy for Acute Respiratory Failure Shu-Min Lin, MD*,Ting-Yu Lin, MD*,
ERJ Express. Published on January 9, 2008 as doi: 10.1183/09031936.00099507 Metallic Stent and Flexible Bronchoscopy without Fluoroscopy for Acute Respiratory Failure Shu-Min Lin, MD*,Ting-Yu Lin, MD*,
Factors leading to tracheobronchial self-expandable metallic stent fracture
 GENERAL THORACIC SURGERY Factors leading to tracheobronchial self-expandable metallic stent fracture Fu-Tsai Chung, MD,* Shu-Min Lin, MD,* Hao-Cheng Chen, MD, Chun-Liang Chou, MD, Chih-Teng Yu, MD, Chien-
GENERAL THORACIC SURGERY Factors leading to tracheobronchial self-expandable metallic stent fracture Fu-Tsai Chung, MD,* Shu-Min Lin, MD,* Hao-Cheng Chen, MD, Chun-Liang Chou, MD, Chih-Teng Yu, MD, Chien-
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas
 Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas Poster No.: C-487 Congress: ECR 212 Type: Scientific Exhibit Authors: S. Akhlaghpoor,
Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas Poster No.: C-487 Congress: ECR 212 Type: Scientific Exhibit Authors: S. Akhlaghpoor,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times
 Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Introduction to Chest Radiography
 Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
E. Senéterre*, F. Paganin**, J.M. Bruel*, F.B. Michel**, J. Bousquet**
 Eur Respir J, 1994, 7, 596 6 DOI: 1.1183/931936.94.73596 Printed in UK - all rights reserved Copyright ERS Journals Ltd European Respiratory Journal ISSN 93-1936 TECHNICAL NOTE Measurement of the internal
Eur Respir J, 1994, 7, 596 6 DOI: 1.1183/931936.94.73596 Printed in UK - all rights reserved Copyright ERS Journals Ltd European Respiratory Journal ISSN 93-1936 TECHNICAL NOTE Measurement of the internal
Numerical analysis of airflow alteration in central airways following tracheobronchial stent placement
 Ho et al. Experimental Hematology & Oncology 2012, 1:23 Experimental Hematology & Oncology SHORT REPORT Open Access Numerical analysis of airflow alteration in central airways following tracheobronchial
Ho et al. Experimental Hematology & Oncology 2012, 1:23 Experimental Hematology & Oncology SHORT REPORT Open Access Numerical analysis of airflow alteration in central airways following tracheobronchial
Quantitative Assessment of Air Trapping in Chronic Obstructive Pulmonary Disease Using Inspiratory and Expiratory Volumetric MDCT
 Chest Imaging Original Research Matsuoka et al. MDCT of Air Trapping in COPD Chest Imaging Original Research Shin Matsuoka 12 Yasuyuki Kurihara 1 Kunihiro Yagihashi 1 Makoto Hoshino 3 Naoto Watanabe 3
Chest Imaging Original Research Matsuoka et al. MDCT of Air Trapping in COPD Chest Imaging Original Research Shin Matsuoka 12 Yasuyuki Kurihara 1 Kunihiro Yagihashi 1 Makoto Hoshino 3 Naoto Watanabe 3
A Retrospective Study of Rigid Bronchoscopy in 58 Paediatric Cases with Acute Respiratory Distress
 International Journal of Scientific and Research Publications, Volume 4, Issue 12, December 2014 1 A Retrospective Study of Rigid Bronchoscopy in 58 Paediatric Cases with Acute Respiratory Distress Dr.
International Journal of Scientific and Research Publications, Volume 4, Issue 12, December 2014 1 A Retrospective Study of Rigid Bronchoscopy in 58 Paediatric Cases with Acute Respiratory Distress Dr.
ENDOBRONCHIAL ABLATIVE THERAPIES. Christopher Cortes, MD, FPCCP
 ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
Pediatric chest HRCT using the idose 4 Hybrid Iterative Reconstruction Algorithm: Which idose level to choose?
 Journal of Physics: Conference Series PAPER OPEN ACCESS Pediatric chest HRCT using the idose 4 Hybrid Iterative Reconstruction Algorithm: Which idose level to choose? To cite this article: M Smarda et
Journal of Physics: Conference Series PAPER OPEN ACCESS Pediatric chest HRCT using the idose 4 Hybrid Iterative Reconstruction Algorithm: Which idose level to choose? To cite this article: M Smarda et
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Metallic Stent Placement for the Management of Tracheal Carina Strictures and Fistulas: Technical and Clinical Outcomes
 Vascular and Interventional Radiology Original Research Kim et al. Outcomes of Tracheal Stent Placement Vascular and Interventional Radiology Original Research Jinoo Kim 1 Ji Hoon Shin 2 Jin-Hyoung Kim
Vascular and Interventional Radiology Original Research Kim et al. Outcomes of Tracheal Stent Placement Vascular and Interventional Radiology Original Research Jinoo Kim 1 Ji Hoon Shin 2 Jin-Hyoung Kim
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012
 Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Tracheobronchial stents are useful in the management
 Do Expandable Metallic Airway Stents Have a Role in the Management of Patients With Benign Tracheobronchial Disease? Brendan P. Madden, MD, FRCP, Tuck-Kay Loke, MRCP, and Abhijat C. Sheth, FRCS Department
Do Expandable Metallic Airway Stents Have a Role in the Management of Patients With Benign Tracheobronchial Disease? Brendan P. Madden, MD, FRCP, Tuck-Kay Loke, MRCP, and Abhijat C. Sheth, FRCS Department
Airway stent placement for malignant tracheobronchial strictures in patients with an endotracheal tube
 Airway stent placement for malignant tracheobronchial strictures in patients with an endotracheal tube Poster No.: C-1121 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit M. J. Kim,
Airway stent placement for malignant tracheobronchial strictures in patients with an endotracheal tube Poster No.: C-1121 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit M. J. Kim,
Sang Min Lee, M.D., Jin Hur, M.D., Tae Hoon Kim, M.D., Sang Jin Kim, M.D., Hyung Jung Kim, M.D. 2
 Quantitative Assessment of Lung Volumes using Multidetector Row Computed Tomography (MDCT) in Patients with Chronic Obstructive Pulmonary Disease (COPD) 1 Sang Min Lee, M.D., Jin Hur, M.D., Tae Hoon Kim,
Quantitative Assessment of Lung Volumes using Multidetector Row Computed Tomography (MDCT) in Patients with Chronic Obstructive Pulmonary Disease (COPD) 1 Sang Min Lee, M.D., Jin Hur, M.D., Tae Hoon Kim,
Preoperative assessment for lung resection. RA Dyer
 Preoperative assessment for lung resection RA Dyer 2016 The ideal assessment of operative risk would identify every patient who could safely tolerate surgery. This ideal is probably unattainable... Mittman,
Preoperative assessment for lung resection RA Dyer 2016 The ideal assessment of operative risk would identify every patient who could safely tolerate surgery. This ideal is probably unattainable... Mittman,
Gastrointestinal tract
 Gastrointestinal tract Colloidal liver-spleen imaging Presented by: Jehad Felemban Introduction: To obtain better anatomic display of liver and spleen architecture, we use (CT Ultrasound). (Radionuclide
Gastrointestinal tract Colloidal liver-spleen imaging Presented by: Jehad Felemban Introduction: To obtain better anatomic display of liver and spleen architecture, we use (CT Ultrasound). (Radionuclide
Diagnosis of old anterior myocardial infarction in
 Br Heart J 1981; 45: 522-26 Diagnosis of old anterior myocardial infarction in emphysema with poor R wave progression in anterior chest leads GRAHAM J HART, PETER A BARRETT, PETER F BARNABY, ELIZABETH
Br Heart J 1981; 45: 522-26 Diagnosis of old anterior myocardial infarction in emphysema with poor R wave progression in anterior chest leads GRAHAM J HART, PETER A BARRETT, PETER F BARNABY, ELIZABETH
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
FOCAL STENOSIS IN RIGHT UPPER LOBE BRONCHUS IN A RECURRENTLY WHEEZING CHILD SEQUENTIALLY STUDIED BY MULTIDETECTOR-ROW SPIRAL COMPUTED TOMOGRAPHY
 FOCAL STENOSIS IN RIGHT UPPER LOBE BRONCHUS IN A RECURRENTLY WHEEZING CHILD SEQUENTIALLY STUDIED BY MULTIDETECTOR-ROW SPIRAL COMPUTED TOMOGRAPHY AND SCINTIGRAPHY I-Chen Chen, 1 Jiunn-Ren Wu, 2,3 Chia-Ying
FOCAL STENOSIS IN RIGHT UPPER LOBE BRONCHUS IN A RECURRENTLY WHEEZING CHILD SEQUENTIALLY STUDIED BY MULTIDETECTOR-ROW SPIRAL COMPUTED TOMOGRAPHY AND SCINTIGRAPHY I-Chen Chen, 1 Jiunn-Ren Wu, 2,3 Chia-Ying
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
The Role of an Interventional Pulmonologist in Management of Complications of Thoracic Malignancies
 Canadian Association of General Practitioners in Oncology 2015 The Role of an Interventional Pulmonologist in Management of Complications of Thoracic Malignancies Kayvan Amjadi MD, FRCPC Director, Interventional
Canadian Association of General Practitioners in Oncology 2015 The Role of an Interventional Pulmonologist in Management of Complications of Thoracic Malignancies Kayvan Amjadi MD, FRCPC Director, Interventional
Cardiac Imaging Tests
 Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
SPIRATION. VALVE SYSTEM For the Treatment of Emphysema or Air Leaks.
 SPIRATION VALVE SYSTEM For the Treatment of Emphysema or Air Leaks. 0000 ENGINEERED FOR AIRWAY MANAGEMENT Inspired by aerodynamics, the Spiration Valve redirects air away from diseased or damaged lung
SPIRATION VALVE SYSTEM For the Treatment of Emphysema or Air Leaks. 0000 ENGINEERED FOR AIRWAY MANAGEMENT Inspired by aerodynamics, the Spiration Valve redirects air away from diseased or damaged lung
Novatech Products for Interventional Pulmonology
 Novatech Products for Novatech and Boston Medical Products Bringing you the finest products for Novatech is a manufacturer of top-quality medical products used successfully worldwide in the growing specialty
Novatech Products for Novatech and Boston Medical Products Bringing you the finest products for Novatech is a manufacturer of top-quality medical products used successfully worldwide in the growing specialty
Chest radiograph of an. asymptomatic man. Case report. Case history
 Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Image Guided Stereotactic Radiotherapy of the Lung
 Image Guided Stereotactic Radiotherapy of the Lung Jamie Marie Harris, MS DABR Avera McKennan Radiation Oncology September 25, 2015 Stereotactic Body Radiotherapy - Clinical Dose/Fractionation - Normal
Image Guided Stereotactic Radiotherapy of the Lung Jamie Marie Harris, MS DABR Avera McKennan Radiation Oncology September 25, 2015 Stereotactic Body Radiotherapy - Clinical Dose/Fractionation - Normal
RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION. Tilman Koelsch, MD National Jewish Health - Department of Radiology
 Pr N op ot er fo ty r R of ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures No relevant financial
Pr N op ot er fo ty r R of ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures No relevant financial
Pediatric Isolated Trachea Rupture Treated with a Conservative Approach İ Akdulum 1, M Öztürk 2, N Dağ 1, A Sığırcı 1 ABSTRACT
 Pediatric Isolated Trachea Rupture Treated with a Conservative Approach İ Akdulum 1, M Öztürk 2, N Dağ 1, A Sığırcı 1 ABSTRACT Tracheobronchial rupture as a result of blunt thoracic trauma is extremely
Pediatric Isolated Trachea Rupture Treated with a Conservative Approach İ Akdulum 1, M Öztürk 2, N Dağ 1, A Sığırcı 1 ABSTRACT Tracheobronchial rupture as a result of blunt thoracic trauma is extremely
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Postmortem Computed Tomography Finding of Lungs in Sudden Infant Death.
 Postmortem Computed Tomography Finding of Lungs in Sudden Infant Death. Poster No.: C-1147 Congress: ECR 2013 Type: Educational Exhibit Authors: Y. Kawasumi, A. Usui, Y. Hosokai, M. Sato, A. Nakajima,
Postmortem Computed Tomography Finding of Lungs in Sudden Infant Death. Poster No.: C-1147 Congress: ECR 2013 Type: Educational Exhibit Authors: Y. Kawasumi, A. Usui, Y. Hosokai, M. Sato, A. Nakajima,
RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION. Tilman Koelsch, MD National Jewish Health - Department of Radiology
 Pr N op ot e fo rty rr o f ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures None Goals Identify
Pr N op ot e fo rty rr o f ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures None Goals Identify
Endoscopic management of critical neoplastic central airway obstruction
 Original Article Page 1 of 8 Endoscopic management of critical neoplastic central airway obstruction Alfonso Fiorelli 1, Roberto Cascone 1, Davide Di Natale 1, Annalisa Carlucci 1, Gaetana Messina 1, Emanuele
Original Article Page 1 of 8 Endoscopic management of critical neoplastic central airway obstruction Alfonso Fiorelli 1, Roberto Cascone 1, Davide Di Natale 1, Annalisa Carlucci 1, Gaetana Messina 1, Emanuele
Airway Foreign Body in Children
 Joseph E. Dohar, M.D., M.S. Dr. Dohar Financial Disclosures Alcon consultant Incusmed consultant Otonomy consultant OrbiMed consultant Learning Objectives Identify clinical situations that may require
Joseph E. Dohar, M.D., M.S. Dr. Dohar Financial Disclosures Alcon consultant Incusmed consultant Otonomy consultant OrbiMed consultant Learning Objectives Identify clinical situations that may require
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Radiologic characterization of emphysema's pattern of distribution - a subjective approach
 Radiologic characterization of emphysema's pattern of distribution - a subjective approach Poster No.: C-0866 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Praia, C. Maciel, J. Pereira, J. Albuquerque,
Radiologic characterization of emphysema's pattern of distribution - a subjective approach Poster No.: C-0866 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Praia, C. Maciel, J. Pereira, J. Albuquerque,
Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis
 Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of endobronchial nitinol coils to improve lung function in emphysema
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of endobronchial nitinol coils to improve lung function in emphysema
Pulmonary Function Testing. Ramez Sunna MD, FCCP
 Pulmonary Function Testing Ramez Sunna MD, FCCP Lecture Overview General Introduction Indications and Uses Technical aspects Interpretation Patterns of Abnormalities When to perform a PFT 1. Evaluation
Pulmonary Function Testing Ramez Sunna MD, FCCP Lecture Overview General Introduction Indications and Uses Technical aspects Interpretation Patterns of Abnormalities When to perform a PFT 1. Evaluation
Methods of nuclear medicine
 Methods of nuclear medicine Per Wollmer Dept. of Translational Medicine Lund University Gamma camera Positron camera Both frequently combined with CT Ventilation/perfusion scanning Perfusion: Albumin macroaggregates
Methods of nuclear medicine Per Wollmer Dept. of Translational Medicine Lund University Gamma camera Positron camera Both frequently combined with CT Ventilation/perfusion scanning Perfusion: Albumin macroaggregates
National COPD Audit Programme
 National COPD Audit Programme Planning for every breath National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Primary care audit (Wales) 2015 17 Data analysis and methodology Section 2:
National COPD Audit Programme Planning for every breath National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Primary care audit (Wales) 2015 17 Data analysis and methodology Section 2:
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Virtual Bronchoscopic Navigation Improves the Diagnostic Yield of Radial-Endobronchial Ultrasound for Peripheral Pulmonary Lesions with Involved Bronchi on CT Fumihiro Asano 1, Naofumi
ORIGINAL ARTICLE Virtual Bronchoscopic Navigation Improves the Diagnostic Yield of Radial-Endobronchial Ultrasound for Peripheral Pulmonary Lesions with Involved Bronchi on CT Fumihiro Asano 1, Naofumi
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiratory distress in patients with central airway obstruction
 Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
