One year cardiac follow up of young world cup football team compared to nonathletes
|
|
|
- Brent Simon
- 5 years ago
- Views:
Transcription
1 The Egyptian Heart Journal (2) 63, 3 22 Egyptian Society of Cardiology The Egyptian Heart Journal ORIGINAL ARTICLE One year cardiac follow up of young world cup football team compared to nonathletes Yasser Sadek Nassar *, Maha Saber, Ayman Farhan, A. Moussa, Ahmed Elsherif Critical Care Medicine Department, Cairo University, Egypt Received 2 January 2; accepted 26 February 2 Available online 24 October 2 KEYWORDS Athletes; Cardiac; Clinical; ECG; ECHO; Football; Training; Sudden death Abstract Introduction: Sudden cardiac death among professional young athletes has become a significant concern mainly attributed to structural heart changes and ECG abnormalities. Objectives: We aimed primarily to compare echocardiographic and electrocardiographic changes in young professional athletes versus a group of sedentary lifestyled nonathletic individuals of the same age group. Secondly, we aimed to follow up echocardiographic and electrocardiographic changes in young professional athletes after one year. Methods: We conducted the study from May 28 to May 29 by clinical examination, transthoraxic echocardiography and 2 lead ECG. Our study group was the national football team candidates for the youth world cup occurring in Cairo 29. This study group was compared to a group of randomly picked nonathletic third year medical students after exclusion of anyone with a known medical illness. The study group was classified into representing athletes at the beginning of the study and I representing athletes after one year follow up. Results: The Study group comprised 34 males, mean age 8.82 ±.56 years while the Control group comprised 28 males, age mean 9.64 ± 2.3 years. There was not a significant difference between the two groups regarding number, age, height or weight (P >.5). vs : Clinical parameters showed significantly lower Systolic Blood Pressure SBP (athletes 7.79 ± 6.536, ± 7.43, P =.8) and Heart Rate HR (athletes ± 5.44, ± 6.33, P =.). ECG parameters showed a significantly longer RR interval (athletes.88 ±.65,.76 ±.78, P =.), while Corrected QTc interval was not significantly different (athletes.4 ±.29,.42 ±.22, P >.5). Echo parameters showed a significant increase in Ejection fraction EF (athletes 6.94 ± 3.84 vs * Corresponding author. address: ysnassar@hotmail.com (Y.S. Nassar) ª 2 Egyptian Society of Cardiology. Production and hosting by Elsevier B.V. All rights reserved. Peer review under responsibility of Egyptian Society of Cardiology. doi:.6/j.ehj Production and hosting by Elsevier
2 4 Y.S. Nassar et al ± 3.63, P =.5) and Left atrial dimension LA (athletes 3.28 ±.392 vs 2.58 ±.32, P =.5). On the other hand Septal wall in diastole SWD, Right ventricle dimension RV, Left ventricular end systolic dimension LVESD, Left Ventricular End Diastolic Dimension LVEDD, Aortic Root AO, and Posterior wall in diastole PWD were not significantly different (P >.5). I vs : QTc became significantly longer (athletes.43 ±.28 vs.42 ±.22, P =.5). SWD was significantly thicker (athletes.2 ±.23 vs.7 ±.7, P =.4). SBP, HR remained significantly lower and RR, EF, LA remained significantly greater (P <.5), while RV, LVESD, LVEDD, AO, PWD remained not significantly different both at the beginning and also after year (P >.5). vs athletes II: ECG parameters showed a significant increase in QTc (.4 ±.29 vs.43 ±.28, P =.5) and RR interval (.8 ±.67 vs.88 ±.65, P =.46). Echo parameters showed a significant increase in SWD (.2 ±.232 vs.93 ±.24, P <.), LA (3.62 ±.423 vs 3.28 ±.392, P =.), RV (2.37 ±.565 vs 2.9 ±.234, P =.), PWD (. ±.2 vs.9 ±.2, P =.8), and a significant decrease in LVESD (3.9 ±.679 vs 3.48 ±.9, P =.6). Other parameters were not statistically significant (P >.5). Conclusions: Professional football playing in young males results in significant changes compared to their of sedentary nonathletic medical students of similar age. Clinical parameters showed a significant decrease in systolic blood pressure SBP and heart rate HR, ECG parameters showed significant increase in RR interval and QTc interval, and Echocardiographic parameters showed a significant increase in Left atrium diameter LA, Septal wall in diastole SWD, and ejection fraction EF. One year of professional football playing in young males causes a continuing significant increase in ECG parameters QTc, RR interval, and echocardiographic parameters SWD, LA, Right ventricle dimension RV, Posterior wall in diastole PWD and decrease in Left ventricular end systolic diameter LVESD compared to themselves one year earlier. The international concern of Sudden cardiac death among professional young athletes may be attributed to Structural heart changes and ECG abnormalities acquired with professional training. ª 2 Egyptian Society of Cardiology. Production and hosting by Elsevier B.V. All rights reserved.. Introduction Regular physical activity has several beneficial effects on health and is linked with reduced cardiovascular and all-cause mortality. However, in certain circumstances, an acute bout of exertion may cause dangerous health effects and, in extreme cases, sudden death (the so called paradox of exercise ). Competitive athletics has been defined as participation in an organized team or individual sport that requires regular competition against others as a central component, that places a high premium on excellence and achievement and requires some form of systematic training. Although rare, the sudden death of a young athlete is a dramatic event with a devastating impact on his family, sports community, and medical staff. It was the case of professional soccer player Marc-Vivien Foe from Cameroon (28 years old), who died suddenly while playing in the Confederations Cup, due to a hypertrophic cardiomyopathy, or, more recently, of the Spanish soccer player Antonio Puerta (22 years old) who had a syncope on the field, with spontaneous recovery and a new collapse in the locker room due to a fatal cardiac arrest. 2 Dealing with exercise-related sudden death (ESD), we usually refer to an unexpected and witnessed sudden cardiac arrest occurring within hour from an exercise bout in an apparently healthy person. Following this definition, ESD is rare, with an incidence of / to /3 per year in males. This explains why, still today, experts discuss on the usefulness of a routine medical pre-participation screening in preventing ESD. 3 It is largely demonstrated that cardiovascular diseases play the dominant role in ESD, accounting for 8 85% of cases. Usually, the fatal cardiac arrest occurs either during or immediately after strenuous exercise, suggesting that autonomic nervous system changes related to effort may trigger malignant arrhythmias in subjects with cardiac disease. This aspect is indirectly confirmed by the fact that ESD is more frequent during official events in respect to training sessions, probably because of the greater psychological involvement.aim of the work:. Compare echocardiographic and electrocardiographic changes in young professional athletes versus a group of sedentary life styled nonathletic individuals of the same age group. 2. Follow up echocardiographic and electrocardiographic changes in those young professional athletes group after one year. 3. Providing limitation criteria for eligibility of competition and suitable sports for athletes at risk for SCD. 2. Patients and methods This study was conducted in Critical Care Medicine Department Cairo University in the period from May 28 to May
3 One year cardiac follow up of young world cup football team compared to nonathletes 5 29.Our study group was picked up from the national football team candidates for the youth world cup occurring in Cairo 29. This study group was compared to a group of randomly picked nonathletic third year medical students after exclusion of anyone with a known medical illness. The study group was classified into: [I] representing athletes at the beginning of the study and [I] I representing athletes after one year follow up. 2.. Patients 2... Inclusion Criteria. Study group: Athletes, males, age between 7 and 22 years. Practicing football in a professional manner. The study group was examined in the beginning of the study (athletes I) and one year later (athletes II). 2. Control group: Nonathletic, males, age between 7 and 22 years. The study group was compared to a group of randomly picked nonathletic third year medical students Exclusion Criteria Known congenital heart disease. Implantable cardioverter defibrilator or pacemaker implantation. Hypertension. Any chronic disease as liver, kidney, autoimmune,..., etc Methods All individuals in both groups were subjected to Thorough history taking: Chest pain, syncopal attacks, palpitation, high blood pressure and family history of sudden cardiac death. () General and clinical examination:. Weight: using a standard weight calculating machine to all subjects. 2. Height: Was measured by a standard against the wall measure. 3. Arm span to height ratio and other examinations to exclude Marfan syndrome (ratio more than.5 is significant) criteria. General Clinical Examination including:. Blood pressure SPB and DBP 2. Cardiac Auscultation 3. Abdominal examination (2) Electrocardiogram ECG: 2-lead ECG was done to all subjects to evaluate the cardiovascular condition. Variables of comparison were: RR interval: from the R to the next R. PR interval: from the beginning of the P to the beginning of the QRS. QT interval: from the beginning of the QRS to the end of T wave. QT interval in second Corrected QTðQTcÞ ¼pffiffiffiffi : R Rinterval in second (3) Echocardiography: Transthoracic echocardiography was done to every candidate in both groups at the beginning and to the study group after one year follow up. The following variables were measured: Left ventricular end diastole (LVEDD cm) Left ventricular end systole (LVESD) Left atrial dimensions (LA cm). Ejection fraction (EF more than 5%). Interventricular septum (IVS.6. cm) in diastole. Posterior wall thickness (PWd.6. cm) in diastole. Right ventricle dimention (RV cm). Aortic root (AO cm) Statistical methods Data were coded and entered using the statistical package SPSS (Self-Propelled Semi-Submersible) version 5. Data were summarized using mean and standard deviation for quantitative variables & percent for quantitative variables, compare between groups was done using chi-square for qualitative variables and independent samples T-test for normal distributed quantitative variables while quantitative variables not normally distributed were compared using non-parametrical Mann-Whitney test and Wilcoxon signed rank test. P-value <.5 was considered statistically significant. 3. Results We conducted the study from May 28 to May 29 in the critical care medicine department, Cairo University. The athletes study group comprised 34 males picked from members of the football youth teams at Al Ahly football club. This study group was classified into:. : represented the athletes at the beginning of the study. 2. I: represented the athletes one year later in follow up.
4 6 Y.S. Nassar et al. The group comprised 28 males randomly picked nonathletic third year medical students after exclusion of anyone with a known medical illness. Our results will be discussed under the following items: (A) Baseline and clinical parameters (B) Electrocardiographic parameters. (C) Echocardiographic parameters. (A) Baseline and clinical data: HR I P value:.. The mean age for athletes was 8.82 ±.566 years while it was 9.64 ± 2.33 years in the group. There was no significant statistical difference between the two groups regarding the age (P >.5). 2. The mean height Ht in athletes was 76.5 ± cm while it was 77.4 ± cm in the group without significant statistical difference between the two groups (P >.5). 3. The mean weight Wt of athletes was ± kg while in the group it was ± kg with no significant statistical difference between the two groups regarding the weight (P >.5). 4. Body Surface Area BSA in athletes was.87 ±. while it was.9 ±.8 in group without significant statistical difference between the two groups (P >.5). 5. Systolic blood pressure SBP was significantly lower in athletes compared to (7.79 ± mmhg vs ± 7.43 mmhg, P =.8), respectively. 6. Diastolic blood pressure DBP showed no significant statistical difference between the two groups (74.4 vs 76.79, P =.32). 7. The mean Heart Rate HR in (athletes I) (68.88 ± 5.44) was significantly lower than (77.43 ± 6.33, P =.) (Table ). While there was no such difference between athletes II (72.97 ± 2.537) and group (77.43 ± 6.33, P =.9), as well as between (athletes I) (68.88 ± 5.44) and athletes II (72.97 ± 2.537) (P =.) (Fig. ). (B) Electrocardiographic data: RR interval: () vs : RR interval was significantly longer ( vs , P.)in athletes I vs, respectively (Table 3). Table Baseline and clinical data. Athletes (34 pts) Control (28 pts) P-value Age 8.82 ± ± Ht 76.5 ± ± Wt ± ± BSA.87 ±..9 ± SBP 7.79 ± ± DBP 74.4 ± ± HR ± ± Figure (2) Athlete II vs : RR interval was not significantly longer (.8 ±.67 vs.76 ±.78, P:.53) in athletes II vs, respectively (Table 4). (3) vs athletes II: RR interval was significantly longer ( vs.8+.67, P.46) in athletes I vs athletes II, respectively (Fig. 2, Table 2). PR interval: Mean heart rate in study versus groups. () vs : PR interval showed no significant statistical difference (49.3 ±.82 vs ± 27.67) (P =.76) in athletes I vs, respectively (Table 3). (2) Athlete II vs : PR interval showed no significant statistical difference (43.59 ± vs ± RR Figure I.76 Mean RR interval in study versus groups. Table 2 The comparison between athletes I at the beginning of study and athletes II after year of professional sport activity. (34 pts) I (34 pts) P-value ECG parameters HR ± ± RR.88 ±.65.8 ± PR 49.3 ± ± QRS.5 ± ± QTc.4 ± ±.28.5 Echo parameters SWd.93 ±.24.2 ±.232. PWd.9 ±.6 ±.2.8 EF 6.94 ± ± LVEDd 4.79 ± ±.987 LVESd 3.48 ± ± LA 3.28 ± ±.423. AO 2.79 ± ± RV 2.9 ± ±.565.
5 One year cardiac follow up of young world cup football team compared to nonathletes 7 (P =.55), in athletes II vs, respectively (Table 4). (3) vs athletes II: PR interval showed no significant statistical difference (49.3 ±.82 vs ± , P =.237) in vs athletes II, respectively (Fig. 3, Table 2). The QRS: () vs : The QRS showed no significant statistical difference (.5 ± 3.66 vs.52 ± P =.465) in athletes I vs, respectively (Table 3). (2) Athlete II vs : The QRS showed no significant statistical difference (2.74 ± 6.56 vs.25 ± 5.867, P =.25) in athletes II vs, respectively (Table 4). (3) vs athletes II: The QRS showed no significant statistical difference (.5 ± 3.66 vs 2.74 ± 6.56, P =.277) in athletes I vs athletes II, respectively (Fig. 4, Table 2). PR QRs Figure Figure 4 QTc: I I Mean PR interval in study versus groups. Control Mean QRS interval in study versus groups. Table 3 The comparison between athletes I and. (34 pts) Control P-value ECG parameters HR ± ± RR.88 ± ±.78. PR 49.3 ± ± QRS.5 ± ± QTc.4 ± ± Echo parameters SWd.93 ±.24.7 ±.79. PWd.9 ±.6.7 ±.225. EF 6.94 ± ± LVEDd 4.79 ± ± LVESd 3.48 ± ± LA 3.28 ± ±.32.5 AO 2.79 ± ±.44.8 RV 2.9 ± ± Table 4 The comparison between athletes II after year and. I (34 pts) Control P-value ECG parameters HR ± ± RR.8 ± ± PR ± ± QRS 2.74 ± ± QTc.43 ± ± Echo parameters SWd.2 ± ±.79.2 PWd ±.2.7 ± EF 6.48 ± ± LVEDd 4.79 ± 4.69 ± LVESd 3.9 ± ±.9.42 LA 3.62 ± ±.32. AO 2.7 ± ±.44.6 RV 2.37 ± ± () vs : Corrected QTc interval was not significantly different (.4 ±.29 vs.42 ±.22, P >.5) in athletes I vs, respectively (Table 3). (2) I vs : QTc became significantly longer (.43 ±.28 vs.42 ±.22, P =.5) in athletes II vs, respectively (Table 4). (3) vs athletes II: Showed a significant increase in QTc (.4 ±.29 vs.43 ±.28, P =.5) in athletes I vs athletes II, respectively (Fig. 5, Table 2). (C) Echocardiographic data: The septal wall in diastole (SWd): () vs : The septal wall in diastole (SWd) was significantly lower (.93 ±.24 vs.7 ±.79 P =.) in athletes I vs, respectively (Table 3). (2) I vs : SWd was significantly higher (.2 ±.232 vs.7 ±.79, P =.2) in athletes II vs, respectively. (3) vs athletes II: SWd showed a significant increase in (.93 ±.24 vs.2 ±.232, P <.) in athletes I vs athletes II, respectively (Fig. 6). QTc The posterior wall in diastole (PWd): Figure I Control Mean QTc interval in study versus groups.
6 8 Y.S. Nassar et al. SWd Figure 6 () vs : The posterior wall in diastole (PWd) was significantly lower (.9 ±.6 vs.7 ±.225, p =.) in athletes I vs, respectively. (2) I vs : PWd showed no significant statistical difference ( ±.2 vs.7 ±.225, P =.22) in athletes II vs, respectively. (3) vs athletes II: PWd showed a significant increase (.9 ±.6 vs ±.2, P:.8) in athletes I vs athletes II, respectively (Fig. 7, Table 2). Ejection Fraction: I Control Mean SWd in study versus groups. () vs : Ejection fraction EF showed a significant increase (6.94 ± 3.84 vs 54.4 ± 3.63, P =.5) in athletes I vs, respectively (Table 3). (2) I vs : EF remained significantly greater (6.48 ±.53 vs 54.4 ± 3.6, P =.4) in athletes II vs, respectively (Table 4). (3) vs athletes II: EF was not significantly different (6.94 ± 3.8 vs 6.48 ±.53, P =.85) in athletes I vs athletes II, respectively (Fig. 8, Table 2). The left ventricular end diastole (LVEDd): () vs : LVEDd showed no significant statistical difference (4.79 ±.57 vs , P =.46) in athletes I vs, respectively (Table 3). (2) I vs : LVEDd showed no significant statistical difference (4.79 ± vs 4.69 ±.635, P:.638) in athletes II vs, respectively (Table 4). (3) vs athletes II: LVEDd showed no significant statistical difference (4.79 ±.57 vs 4.79 ±, P:.987) in athletes I vs athletes II, respectively (Fig. 9, Table 2). The left ventricular end systole (LVESd): () vs : The left ventricular end systole LVESd showed no significant statistical difference (3.48 ±.9 vs 3.48 ±.9, P =.483) in athletes I vs, respectively (Table 3). (2) I vs : LVESd showed no significant statistical difference (3.9 ±.679 vs 3.48 ±.9, P:.42) in athletes II vs, respectively (Table 4). (3) vs athletes II: LVESd show significant decrease (3.48 ±.9 vs 3.9 ±.679, P =.6) in athletes I vs athletes II, respectively (Fig., Table 2). The left atrium LA: () vs : LA show a significant increase (3.28 ±.392 vs 2.58 ±.32, P =.5) in athletes I vs, respectively (Table 3). (2) I vs : LA show a significant increase (3.62 ±.423 vs 2.58 ±.32, P =.) in athletes II vs, respectively (Table 4). (3) vs athletes II: LA showed a significant increase (3.28 ±.392 vs, 3.62 ±.423 P:.) in athletes I vs athletes II, respectively (Fig., Table 2). The aortic root AO: () vs : The aortic root AO showed no significant statistical difference (2.79 ±.329 vs 2.63 ±.44, P =.8) in athletes I vs, respectively (Table 3). PWd LVEDd I I Figure 7 Mean PWd in study versus groups. Figure 9 Mean LVEDd in study versus groups. EF I 54.4 LVESd I 3.42 Figure 8 Mean ejection fraction in study versus groups. Figure Mean LVESd in study versus groups.
7 One year cardiac follow up of young world cup football team compared to nonathletes 9 LA AO Figure Figure 2 (2) I vs : AO showed no significant statistical difference (2.7 ±.56 vs 2.63 ±.44, P =.6) in athletes II vs, respectively (Table 4). (3) vs athletes II: AO showed no significant statistical difference (2.79 ±.329 vs 2.7 ±.56, P:.228) in athletes I vs athletes II, respectively (Fig. 2, Table 2). The right ventricle diameter RV: () vs : The right ventricle RV showed no significant statistical difference (2.9 ±.237 vs 2.27 ±.492, P =.73) in athletes I vs, respectively (Table 3). (2) I vs : RV showed no significant statistical difference (2.37 ±.565 vs 2.27 ±.492, P =.43) in athletes II vs, respectively (Table 4). (3) vs athletes II: RV was significantly increased (2.9 ±.237 vs 2.37 ±.565, P =.) in athletes I vs athletes II, respectively (Fig. 3, Table 2). 4. Discussion I 2.58 Compared to s, in our study the heart rate in athletes was lower with RR interval longer significantly than in (HR ± 5.44 with RR.88 ±.65 vs HR ± 6.33 with RR.76 ±.78, P.) in athletes I vs, respectively. HR and RR interval was not significantly chan Mean LA in study versus groups. 2.7 I 2.63 Mean AO in study versus groups. Although regular physical activity has several beneficial effects on health and is linked with reduced cardiovascular and allcause mortality, in certain circumstances, an acute bout of exertion may cause dangerous health effects and, in extreme cases, sudden death. We aimed primarily to compare echocardiographic and electrocardiographic changes in young proffessional athletes versus a group of sedentary lifestyled nonathletic individuals of the same age group. Secondly, we aimed to follow up echocardiographic and electrocardiographic changes in young proffessional athletes after one year, and finally to recognize silent cardiovascular abnormalities to provide limitation criteria for eligibility of competition for athletes at risk of sudden cardiac death (SCD). This study was conducted in Critical Care Medicine Department Cairo University in the period from may 28 to may 29. Our study group was picked up from the national football team candidates for the youth world cup occurring in Cairo 29.Our group was randomly picked nonathletic third year medical students. 4.. Regarding clinical parameters In our athletes, systolic blood pressure (SBP) was 7.79 ± mmhg while in group, it was ± 7.43 mmhg. SBP was significantly lower in athletes I vs (P =.8). While diastolic blood pressure (DBP) showed no significant statistical difference in athletes I vs, respectively (74.4 vs 76.79, P >.5). This comes in agreement with Eric Abergel et al. 4 who showed in a study done on 286 cyclists and 52 matched sedentary volunteers that Systolic blood pressure (2 ± 9 mm Hg vs. 26 ± 3 mmhg, P <.5) and diastolic blood pressure (68 ± 9 mmhg vs. 77 ± mm Hg, P <.5) were lower in athletes than in s, as was heart rate. In a study done by Hernelahti et al. 5 on 264 male orienteering runners among men aged years concluded that longterm vigorous endurance training is associated with a low prevalence of hypertension. Some of the effect can be explained by a lower body mass, but exercise seems to induce a lower rate of hypertension by other mechanisms than by decreasing body weight Regarding ECG parameters RV I Figure 3 Shows mean RV in study versus groups.
8 2 Y.S. Nassar et al. ged (HR 68.2 with RR.8 ±.67 vs HR 78.9 with RR.76 ±.78, P.53) in athletes II vs, respectively. Compared to themselves after one year of professional training, HR was lower with RR longer significantly (HR 68.2 with RR.88 ±.65 vs HR 74. with RR.8 ±.67, P =.46) in athletes I vs athletes II, respectively. This comes in agreement with Martinelli 6 who found that athletes at rest had lower heart rates in a study done on two groups cyclists and sedentary group showed (HR 65.6 ±.49 with RR.9 vs HR 7.9 ±.75 with RR.85, P <.5) in athletes vs, respectively. Similarly, in a study done by Piraye Kervancioglu and Savas Hatipoglu 7 on 4 male football players and 25 sedentary males showed (HR 6.48 ± 6.7 with RR. vs HR 73.2 ± 3.44 with RR.82, P <.5) in athletes vs, respectively. Similarly, this comes in agreement with the study done by Langdeau et al. 8 who made the study on athletes and 5 and found that athletes had significantly longer RR intervals (HR 54.5 with RR.68.5 ± 2.6 vs HR 63.8 with RR ± 2.8, P <.5) in athletes vs, respectively. The cause of bradycardia in athletic subjects is uncertain. Most evidence suggests that the sinoatrial node and atrioventricular nodes are suppressed by an increase in vagal tone, which can be abolished by atropine or stopping training. In athletes the resting bradycardia seems to be much more related to changes in intrinsic mechanisms than to modifications in autonomic. 9 Compared to s, in our study QTc interval was not significantly different (.4 ±.29 vs.42 ±.22, P >.5) in athletes I vs, respectively. QTc became significantly longer (.43 ±.28 vs.42 ±.22, P =.5) in athletes II vs, respectively. Compared to themselves after one year of professional training, QTc showed a significant increase (.4 ±.29 vs.43 ±.28, P =.5) in athletes I vs athletes II, respectively. This comes in agreement with Sharma et al. who showed that athletes have a significantly longer QTc than nonathletes (P <.5) in a study done to more than athletes (39 ± 27 vs 379 ± 29, P <.5) in athletes vs, respectively, but in disagreement with J-B Langdeau et al. 7 who did his study on athletes vs 5 (45.8 ± 9.4 vs 46.4 ± 2., P >.5) in athletes vs, respectively. Compared to s, in our study PR interval showed no significant statistical difference (49.3 ±.82 vs ± 27.67, P =.76) in athletes I vs, respectively PR interval showed no significant statistical difference (43.59 ± vs ± 27.67, P =.55) in athletes II vs, respectively. Compared to themselves after one year of professional training, PR interval showed a non-significant increase (49.3 ±.82 vs ± ms (P =.237) in athletes I vs athletes II, respectively. This comes in disagreement with S Sharma, 22 who showed in a study done on junior athletes in the same age and sex of our study group that PR interval is more prolonged in athletes than nonathletes (53 ± 2 vs 4 ± 8, P <.5) in athletes vs, respectively. Compared to s, in our study the QRS showed no significant statistical difference (.5 ± 3.66 vs.52 ± 5.867, P =.465) in athletes I vs, respectively. QRS showed no significant statistical difference (2.74 ± 6.56 vs.25 ± 5.867, P =.25) in athletes II vs, respectively. Compared to themselves after one year of professional training, QRS showed no significant statistical difference (.5 ± 3.66 vs 2.74 ± 6.56, P =.277) in athletes I vs athletes II, respectively. This comes in disagreement with S Sharma, 22 who showed in a study done on junior athletes in the same age and sex of our study group that the QRS duration was more prolonged in athletes than nonathletes (92 vs 89 ms, P <.), respectively. This difference between our study and that of S Sharma may be due to the smaller number of our study group (5 patients) in comparison to this study that comprised junior athletes. Tanji said that in young endurance athletes, the electrocardiogram may show several abnormalities such as an increase in QRS voltage, that can make it difficult to convince oneself that there is no hypertensive cardiac involvement. In some cases, an echocardiogram with a Doppler evaluation of diastolic function can help in evaluating young athletes with abnormal electrocardiograms for structural heart disease Regarding Echo parameters Compared to s, in our study the septal wall in diastole (SWd) was not significantly different (.93 ±.24 vs.7 ±.79, P >.5) in athletes I vs, respectively. SWd was significantly thicker (.2 ±.232 vs.7 ±.79, P =.2) in athletes II vs, respectively. Compared to themselves after one year of professional training, SWd Showed a significant increase (.93 ±.24 vs.2 ±.232, P <.) in athletes I vs athletes II, respectively. This comes in agreement with Piraye Kervancioglu who showed that football players were shown to have significantly higher values than the group for SWd (.98 ±.3 vs.85 ±.9, P <.5) in a study on a total of 4 male football players. 7 Compared to Controls, in our study the posterior wall in diastole (PWd) was not significantly different (.9 ±.6 vs , P >.5) in athletes I vs, respectively. PWd showed no significant statistical difference ( ±.2 vs.7 ±.225, P =.22) in athletes II vs, respectively. Compared to themselves after one year of professional training, PWd showed significant increase (.9 ±.6 vs ±.2, p.8) in athletes I vs athletes II, respectively. This came in disagreement with Piraye Kervancioglu who showed that there was no significant difference between the PWd of the football players and group (.85 ±.9 vs.8 ±.8, P =.9). 7 Compared to s, in our study Ejection fraction EF showed a significant increase (6.94 ± 3.84 vs 54.4 ± 3.63, P.5) in athletes I vs, respectively. EF remained significantly greater (6.48 ±.53 vs 54.4 ± 3.6, P =.4) in athletes II vs, respectively. Compared to themselves after one year of professional training, EF was not significantly different (6.94 ± 3.8 vs 6.48 ±.53, P =.85) in athletes I vs athletes II, respectively. This comes in agreement with Piraye Kervancioglu who showed that football players were shown to have significantly higher values than the group for EF (69.42 ± 4.5 vs ± 4.54, P <.5). 7 Compared to Controls, in our study LVEDd showed no significant statistical difference (4.79 ±.57 vs 4.69 ±.635,
9 One year cardiac follow up of young world cup football team compared to nonathletes 2 P =.46) in athletes I vs, respectively. LVEDd showed no significant statistical difference (4.79 ± vs 4.69 ±.635, P =.638) in athletes II vs, respectively. Compared to themselves after one year of professional training, LVEDd showed no significant statistical difference (4.79 ±.57 vs 4.79 ±, P =.987) in athletes I vs athletes II, respectively. This came in disagreement with Piraye Kervancioglu who showed that there was a significantly higher values in LVEDd in football players than (5.37 ±.38 vs 4.63 ±.32, P >.5) which accounts in a large part for the elevated left ventricular mass LVM in athletes. 7 Compared to s, in our study the left ventricular end systole diameter LVESd showed no significant statistical difference (3.48 ±.9 vs 3.48 ±.9, P =.483) in athletes I vs, respectively. LVESd showed no significant statistical difference (3.9 ±.679 vs 3.48 ±.9, P =.42) in athletes II vs, respectively. Compared to themselves after one year of professional training, LVESd showed a significant decrease (3.48 ±.9 vs 3.9 ±.679, P =.6) in athletes I vs athletes II, respectively. This comes in disagreement with Eric Abergel who showed in a study done on 286 cyclists and 52 matched sedentary volunteers (39.7 ± 4. vs 3.4 ± 4. P <.5) in athletes vs, respectively. 4 Compared to s, in our study the LA show a significant increase (3.28 ±.392 vs 2.58 ±.32, P =.5) in athletes I vs, respectively. LA showed a significant increase (3.62 ±.423 vs 2.58 ±.32, P =.) in athletes II vs, respectively. Compared to themselves after one year of professional training, LA showed a significant increase (3.28 ±.392 vs 3.62 ±.423 P =.) in athletes I vs athletes II, respectively. This comes in agreement with S Sharma 22 who showed a significant LA enlargement in athletes vs in a study on athletes vs 3 where 4% of athletes had LA enlargement vs.2% in P <.5. Compared to s, in our study the right ventricle RV showed no significant statistical difference (2.9 ±.237 vs 2.27 ±.492, P =.73) in athletes I vs, respectively. RV showed no significant statistical difference (2.37 ±.565 vs 2.27 ±.492, P =.43) in athletes II vs, respectively. Compared to themselves after one year of professional training, RV was significantly increased (2.9 ±.237 vs 2.37 ±.565, P =.) in athletes I vs athletes II, respectively. This comes in agreement with Gu nther Schneider who showed that endurance athletes have increased RV dimensions in a study done on 2 male endurance athletes and 2 pairmatched untrained subjects (P <.5). 2 On the other hand, this comes in disagreement with a study done by M.K. Erol and Sule Karakelleoglu, 3 the study population consisted of 36 elite highly-trained male athletes and 6 age-matched healthy sedentary s. All right ventricular systolic and diastolic echocardiographic parameters were similar in athletes with and without left ventricular hypertrophy (P >.5). The results of this study indicate that right ventricular systolic and diastolic functions do not deteriorate in the athlete s heart despite significant chamber dilatation. They suggest that these changes are a normal physiologic adaptation to prolonged training. Turpeinen 4 also showed that exercise training causes a number of well known physiological changes in the heart: an increase in LVEDD and left ventricular wall thicknesses (IVS and LVPW), stroke volume is increased and heart rate is decreased during resting conditions. 5. Conclusions Professional football playing in young males results in significant cardiovascular changes compared to their of sedentary nonathletic medical students of similar age. Compared to s, clinical parameters in athletes showed a significant decrease in systolic blood pressure SBP and heart rate HR, ECG parameters showed significant prolongation in RR interval and QTc interval, and Echocardiographic parameters showed a significant increase in Left atrium diameter LA, Septal wall in diastole SWD, and ejection fraction EF. Compared to themselves after one year of professional football playing by young males, ECG parameters showed a continuing significant prolongation in QTc, RR interval, and Echocardiographic parameters Septal wall in diastole SWD, Left atrium diameter LA, Right ventricle dimension RV, Posterior wall in diastole PWD and decrease in Left ventricular end systolic diameter LVESD compared to themselves one year earlier. The international concern of Sudden cardiac death among professional young athletes may be attributed to Structural heart changes and ECG abnormalities acquired with professional training. References. Maron BJ, Mitten MJ, Green Burnett C. Criminal consequences of commotio cordis. Am J Cardiol 22;89: Maron BJ, McKenna WJ, Danielson GK, et al. American College of Cardiology/European Society of Cardiology clinical expert consensus document on hypertrophic cardiomyopathy: a report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents and the European Society of Cardiology Committee for Practice Guidelines. J Am Coll Cardiol 23;42: Massimiliano Bianco, et al. 836 Journal of Cardiovascular Medicine 28;9(8). Screening for coronary artery anomalies in 36 elite competitive athletes. 4. Abergel Eric, Chatellier Gilles, Hagege Albert A. Clinical research: exercise, diet, and the heart serial left ventricular adaptations in world-class professional cyclists Implications for disease screening and follow-up. J Am Colloid Cardiol 24;44:44 9,.6/ j.jacc Hernelahti, Miika; Kujala, Urho M.; Kaprio, Jaakko; Karjalainen, Jouko; Sarna, Seppo. Hypertension in master endurance athletes. J Hypertension 998;6(): Martinelli FS, Chacon-Mikahil MPT, Martins LEB, et al. Heart rate variability in athletes and nonathletes at rest and during headup tilt. Braz J Med Biol Res, Piraye Kervancioglu, Savas Hatipoglu E. Cardiol J 27;4(): Langdeau J-B, Blier L, Turcotte H, et al. Boulet. Electrocardiographic findings in athletes. The prevalence of LVH and conduction defects. Can J Cardiol 2;7(6): Hedelin R, Bjerle P, Henriksson-Larsen K. Heart rate variability in athletes: relationship with central and peripheral performance. Med Sci Sports Exer 2;33: Sharma S, Maron BJ, Whyte G, et al. Physiologic limits of left ventricular hypertrophy in elite junior athletes. Relevance to
10 22 Y.S. Nassar et al. differential diagnosis of athlete s heart and hypertrophic cardiomyopathy. J Am Coll Cardiol 22;4: Tanji JL. Exercise and the hypertensive athlete. Clin Sports Med 992;(2): Gu nther Schneider et al.. Athlete s heart: Right and left ventricular mass and function in male endurance athletes and untrained individuals determined by magnetic resonance imaging. J Am College Cardiol 22;4(): Erol MK, Sule Karakelleoglu. Department of Cardiology, Medical School Hospital, Ataturk University, 255 Erzurum. Assessment of right heart function in the athlete s heart. Heart Vessels 6(5): Turpeinen AK, Kuikka JT, Vanninen E, et al. Athletic heart: a metabolic, anatomical, and functional study. Med Sci Sports Exer 996;28:33 4.
Historical Notes: Clinical Exercise Testing in the Athlete. An Efficient Heart. Structural Changes, Cont. Coronary Arteries
 Clinical Exercise Testing in the Athlete The athlete s heart Sudden cardiac death in athletes Screening athletes for cardiovascular disease Historical Notes: Giovanni Lancisi (father of cardiology), 17
Clinical Exercise Testing in the Athlete The athlete s heart Sudden cardiac death in athletes Screening athletes for cardiovascular disease Historical Notes: Giovanni Lancisi (father of cardiology), 17
Key wards: PR Interval, QT interval, bradycardia.
 bü z ÇtÄ TÜà väx : A Pilot Study Eman Abdo Elaziz Ahmed 1 and Amal Mahmoud Saied 2 Abstract Background: Sudden deaths of young competitive athletes are tragic events that continue to have a considerable
bü z ÇtÄ TÜà väx : A Pilot Study Eman Abdo Elaziz Ahmed 1 and Amal Mahmoud Saied 2 Abstract Background: Sudden deaths of young competitive athletes are tragic events that continue to have a considerable
Athlete s Heart vs. Cardiomyopathy
 Athlete s Heart vs. Cardiomyopathy Linda D. Gillam, MD, MPH, FASE Chair, Department of Cardiovascular Medicine Medical Director, Cardiovascular Service Line Former Team Cardiologist to the New York Jets
Athlete s Heart vs. Cardiomyopathy Linda D. Gillam, MD, MPH, FASE Chair, Department of Cardiovascular Medicine Medical Director, Cardiovascular Service Line Former Team Cardiologist to the New York Jets
EVALUATION OF THE ATHLETE. Karen Stout, MD Professor, Medicine and Pediatrics University of Washington
 EVALUATION OF THE 12 ATHLETE Karen Stout, MD Professor, Medicine and Pediatrics University of Washington NO DISCLOSURES OUTLINE Why evaluate athletes? What s the problem? What evaluation should be done?
EVALUATION OF THE 12 ATHLETE Karen Stout, MD Professor, Medicine and Pediatrics University of Washington NO DISCLOSURES OUTLINE Why evaluate athletes? What s the problem? What evaluation should be done?
Cardiac hypertrophy and how it may break an athlete s heart e the Cypriot case
 Eur J Echocardiography (2005) 6, 301e307 Cardiac hypertrophy and how it may break an athlete s heart e the Cypriot case C.E. Chee a,1, C.P. Anastassiades a,1, A.G. Antonopoulos b, A.A. Petsas b, L.C. Anastassiades
Eur J Echocardiography (2005) 6, 301e307 Cardiac hypertrophy and how it may break an athlete s heart e the Cypriot case C.E. Chee a,1, C.P. Anastassiades a,1, A.G. Antonopoulos b, A.A. Petsas b, L.C. Anastassiades
SABIHA GATI AND SANJAY SHARMA
 9 The athlete s heart SABIHA GATI AND SANJAY SHARMA Pasieka/Science Photo Library In this article, the authors highlight the spectrum, magnitude and determinants of the athlete s heart and provide a practical
9 The athlete s heart SABIHA GATI AND SANJAY SHARMA Pasieka/Science Photo Library In this article, the authors highlight the spectrum, magnitude and determinants of the athlete s heart and provide a practical
Athlete s Heart vs. Cardiomyopathy
 Athlete s Heart vs. Cardiomyopathy Linda D. Gillam, MD, MPH, FASE Chair, Department of Cardiovascular Medicine Medical Director, Cardiovascular Service Line Former Team Cardiologist to the New York Jets
Athlete s Heart vs. Cardiomyopathy Linda D. Gillam, MD, MPH, FASE Chair, Department of Cardiovascular Medicine Medical Director, Cardiovascular Service Line Former Team Cardiologist to the New York Jets
The Heart of a Cyclist Insights from Sports Cardiology. Michel Accad, MD February 21, 2018 UCSF Mini Medical School
 The Heart of a Cyclist Insights from Sports Cardiology Michel Accad, MD February 21, 2018 UCSF Mini Medical School Lecture outline: WARNING: Not a lecture about how to boost your performance! Preliminary
The Heart of a Cyclist Insights from Sports Cardiology Michel Accad, MD February 21, 2018 UCSF Mini Medical School Lecture outline: WARNING: Not a lecture about how to boost your performance! Preliminary
DEPARTMENT NAME PRE-PARTICIPATION SCREENING THE SPORTS PHYSICAL
 PRE-PARTICIPATION SCREENING THE SPORTS PHYSICAL Michele Krenek, MSN, RN, FNP-C TCHAPP Conference, Houston, TX April 4, 2019 PRE-PARTICIPATION SPORTS SCREENING According to the AHA the definition of the
PRE-PARTICIPATION SCREENING THE SPORTS PHYSICAL Michele Krenek, MSN, RN, FNP-C TCHAPP Conference, Houston, TX April 4, 2019 PRE-PARTICIPATION SPORTS SCREENING According to the AHA the definition of the
Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations
 Sports Cardiology Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations Domenico Corrado, MD, PhD Inherited Arrhytmogenic Cardiomyopathy Unit Department of Cardiac, Thoracic and
Sports Cardiology Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations Domenico Corrado, MD, PhD Inherited Arrhytmogenic Cardiomyopathy Unit Department of Cardiac, Thoracic and
Interpretation and Consequences of Repolarisation Changes in Athletes
 Interpretation and Consequences of Repolarisation Changes in Athletes Professor Sanjay Sharma E-mail sasharma@sgul.ac.uk @SSharmacardio Disclosures: None Athlete s ECG Vagotonia Sinus bradycardia Sinus
Interpretation and Consequences of Repolarisation Changes in Athletes Professor Sanjay Sharma E-mail sasharma@sgul.ac.uk @SSharmacardio Disclosures: None Athlete s ECG Vagotonia Sinus bradycardia Sinus
HEART CONDITIONS IN SPORT
 HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
Cardiac hypertrophy : differentiating disease from athlete
 Cardiac hypertrophy : differentiating disease from athlete Ario Soeryo Kuncoro, MD, Cardiologist Echocardiography Division, National Cardiovascular Centre Harapan Kita-Jakarta Departement of Cardiology
Cardiac hypertrophy : differentiating disease from athlete Ario Soeryo Kuncoro, MD, Cardiologist Echocardiography Division, National Cardiovascular Centre Harapan Kita-Jakarta Departement of Cardiology
Cardiac Conditions in Sport & Exercise. Cardiac Conditions in Sport. USA - Sudden Cardiac Death (SCD) Dr Anita Green. Sudden Cardiac Death
 Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
EKG screening in athletics
 Use of PPE EKG screening in athletics Stefan Montgomery MD, ATC 4/27/18 The overall role of the preparticipation physical evaluation (PPE) is to evaluate the health of the athlete to optimize safe sports
Use of PPE EKG screening in athletics Stefan Montgomery MD, ATC 4/27/18 The overall role of the preparticipation physical evaluation (PPE) is to evaluate the health of the athlete to optimize safe sports
CLINICAL RESEARCH ON CARDIOVASCULAR ALTERATION ON 86 S PROFESSIONAL ATHLETES IN IRAN
 CLINICAL RESEARCH ON CARDIOVASCULAR ALTERATION ON 86 S PROFESSIONAL ATHLETES IN IRAN Lotfali Pourkazemi 1 * and Roghieh Razeghi Jadid 2 1 Sports Medicine Federation of Iran 2 Department of Herbal Sciences,
CLINICAL RESEARCH ON CARDIOVASCULAR ALTERATION ON 86 S PROFESSIONAL ATHLETES IN IRAN Lotfali Pourkazemi 1 * and Roghieh Razeghi Jadid 2 1 Sports Medicine Federation of Iran 2 Department of Herbal Sciences,
Introduction. Abbreviations and Definitions
 Abbreviations and Definitions HCM DCM LVH ARVC LAD LV LA RV RA IVSd LVPWd LVDd EDV SV EF LA Size LVNC LBBB RBBB RWT Hypertrophic Cardiomyopathy Dilated Cardiomyopathy Left Ventricular Hypertrophy Arrhythmogenic
Abbreviations and Definitions HCM DCM LVH ARVC LAD LV LA RV RA IVSd LVPWd LVDd EDV SV EF LA Size LVNC LBBB RBBB RWT Hypertrophic Cardiomyopathy Dilated Cardiomyopathy Left Ventricular Hypertrophy Arrhythmogenic
Echo Evaluation of the Heart of an Athlete
 Echo Evaluation of the Heart of an Athlete 18 th SA Heart Congress, 2017 Johannesburg, South Africa November 9-12, 2017 Naser Ammash. MD Professor of Medicine Practice Chair, Cardiovascular Department
Echo Evaluation of the Heart of an Athlete 18 th SA Heart Congress, 2017 Johannesburg, South Africa November 9-12, 2017 Naser Ammash. MD Professor of Medicine Practice Chair, Cardiovascular Department
Index. cardiacep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A AEDs. See Automated external defibrillators (AEDs) AF. See Atrial fibrillation (AF) Age as factor in SD in marathon runners, 45 Antiarrhythmic
Note: Page numbers of article titles are in boldface type. A AEDs. See Automated external defibrillators (AEDs) AF. See Atrial fibrillation (AF) Age as factor in SD in marathon runners, 45 Antiarrhythmic
CARDIAC BENEFICIAL EFFECTS AND ADAPTATIONS IN ATHLETES
 ARISTOTLE UNIVERSITY OF THESSALONIKI, GREECE SPORTS MEDICINE LABORATORY DIRECTOR: PROF. A. DELIGIANNIS CARDIAC BENEFICIAL EFFECTS AND ADAPTATIONS IN ATHLETES ASTERIOS DELIGIANNIS CARDIOLOGIST PROFESSOR
ARISTOTLE UNIVERSITY OF THESSALONIKI, GREECE SPORTS MEDICINE LABORATORY DIRECTOR: PROF. A. DELIGIANNIS CARDIAC BENEFICIAL EFFECTS AND ADAPTATIONS IN ATHLETES ASTERIOS DELIGIANNIS CARDIOLOGIST PROFESSOR
Normal ECG And ECHO Findings in Athletes
 Normal ECG And ECHO Findings in Athletes Dr.Yahya Kiwan Consultant Interventional Cardiologist Head Of Departement Of Cardiology Canadian Specialist Hospital Sinus Bradycardia The normal heartbeat is initiated
Normal ECG And ECHO Findings in Athletes Dr.Yahya Kiwan Consultant Interventional Cardiologist Head Of Departement Of Cardiology Canadian Specialist Hospital Sinus Bradycardia The normal heartbeat is initiated
The Athlete s Heart. Critical Role of Echo. Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University
 The Athlete s Heart Critical Role of Echo Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. Disclosures Grant support (to institution)
The Athlete s Heart Critical Role of Echo Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. Disclosures Grant support (to institution)
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Pre-participation Screening for the Prevention of sudden Cardiac Death in Young Athletes. Thomas W. Allen, DO, MPH
 Pre-participation Screening for the Prevention of sudden Cardiac Death in Young Athletes Thomas W. Allen, DO, MPH Cardiovascular disorders are the leading cause of sudden death in young athletes accounting
Pre-participation Screening for the Prevention of sudden Cardiac Death in Young Athletes Thomas W. Allen, DO, MPH Cardiovascular disorders are the leading cause of sudden death in young athletes accounting
Risk Factors for Sudden cardiac Death
 Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
THE CARDIOVASCULAR SYSTEM
 THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
How to Read an Athlete s ECG. Sanjay Sharma BSc (Hons), MD, FRCP, FESC
 How to Read an Athlete s ECG Sanjay Sharma BSc (Hons), MD, FRCP, FESC Athlete s EKG Vagotonia Sinus bradycardia Sinus arrhythmia First degree AVB ST-elevation Tall T waves Increased chamber size Left ventricular
How to Read an Athlete s ECG Sanjay Sharma BSc (Hons), MD, FRCP, FESC Athlete s EKG Vagotonia Sinus bradycardia Sinus arrhythmia First degree AVB ST-elevation Tall T waves Increased chamber size Left ventricular
Sudden Cardiac Death in Youth Athletes. Dublin City Schools Athletic Health Care
 Sudden Cardiac Death in Youth Athletes Dublin City Schools Athletic Health Care Sudden Cardiac Death What is sudden cardiac death in the young athlete? Sudden cardiac death is the result of an unexpected
Sudden Cardiac Death in Youth Athletes Dublin City Schools Athletic Health Care Sudden Cardiac Death What is sudden cardiac death in the young athlete? Sudden cardiac death is the result of an unexpected
Cardiovascular Impacts of long-term endurance exercise: Implications of athlete s heart
 Cardiovascular Impacts of long-term endurance exercise: Implications of athlete s heart Dr. Gary Mak 麥耀光心臟科專科醫生 IPP of HK Associa4on of Sports Medicine and Sports Science Director of Pro-Cardio Heart Disease
Cardiovascular Impacts of long-term endurance exercise: Implications of athlete s heart Dr. Gary Mak 麥耀光心臟科專科醫生 IPP of HK Associa4on of Sports Medicine and Sports Science Director of Pro-Cardio Heart Disease
I have nothing to disclose. Research support from: Cardiac Risk in The Young
 I have nothing to disclose. Research support from: Cardiac Risk in The Young Pre-participation screening of Young Athletes: Current Perspective Professor Sanjay Sharma Disclosures: None SCD in Young Athletes
I have nothing to disclose. Research support from: Cardiac Risk in The Young Pre-participation screening of Young Athletes: Current Perspective Professor Sanjay Sharma Disclosures: None SCD in Young Athletes
Aerobic Training Induced Structural Changes of the Heart
 TURKISH JOURNAL OF SPORT AND EXERCISE 2012; 14(3): 1 5 Aerobic Training Induced Structural Changes of the Heart Asim CENGIZ The School of Kinesiology and Nutritional Science. California State University,
TURKISH JOURNAL OF SPORT AND EXERCISE 2012; 14(3): 1 5 Aerobic Training Induced Structural Changes of the Heart Asim CENGIZ The School of Kinesiology and Nutritional Science. California State University,
Abnormal ECG patterns and significance in a group of mountaineers
 Original Article Abnormal ECG patterns and significance in a group of mountaineers Wg Cdr V Vasdev*, Wg Cdr DS Chadha +, Gp Capt P Kharbanda #, Lt Col SK Datta**, Air Cmde RK Ganjoo AVSM VSM ++ ABSTRACT
Original Article Abnormal ECG patterns and significance in a group of mountaineers Wg Cdr V Vasdev*, Wg Cdr DS Chadha +, Gp Capt P Kharbanda #, Lt Col SK Datta**, Air Cmde RK Ganjoo AVSM VSM ++ ABSTRACT
Congestive Heart Failure or Heart Failure
 Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
The Athlete s Heart. Role of Echo. Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University
 The Athlete s Heart Role of Echo Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. Disclosures Grant support (to institution) for Core
The Athlete s Heart Role of Echo Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. Disclosures Grant support (to institution) for Core
François Carré Hôpital Pontchaillou -INSERM UMR1099-Université Rennes 1
 Normal electrocardiogram variants in Athletes François Carré Hôpital Pontchaillou -INSERM UMR1099-Université Rennes 1 Disclosures No disclosure of interest concerning this lecture The cardiovascular sport
Normal electrocardiogram variants in Athletes François Carré Hôpital Pontchaillou -INSERM UMR1099-Université Rennes 1 Disclosures No disclosure of interest concerning this lecture The cardiovascular sport
Nancy Goldman Cutler, MD Beaumont Children s Hospital Royal Oak, Mi
 Nancy Goldman Cutler, MD Beaumont Children s Hospital Royal Oak, Mi Identify increased LV wall thickness (WT) Understand increased WT in athletes Understand hypertrophic cardiomyopathy (HCM) Enhance understanding
Nancy Goldman Cutler, MD Beaumont Children s Hospital Royal Oak, Mi Identify increased LV wall thickness (WT) Understand increased WT in athletes Understand hypertrophic cardiomyopathy (HCM) Enhance understanding
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Diastolic filling in hypertrophied hearts of elite runners: an Echo-Doppler study
 European Review for Medical and Pharmacological Sciences 2001; 5: 65-69 Diastolic filling in hypertrophied hearts of elite runners: an Echo-Doppler study A. PALAZZUOLI, L. PUCCETTI, F. BRUNI, A.L. PASQUI,
European Review for Medical and Pharmacological Sciences 2001; 5: 65-69 Diastolic filling in hypertrophied hearts of elite runners: an Echo-Doppler study A. PALAZZUOLI, L. PUCCETTI, F. BRUNI, A.L. PASQUI,
Apical Hypertrophic Cardiomyopathy With Hemodynamically Unstable Ventricular Arrhythmia Atypical Presentation
 Cronicon OPEN ACCESS Hemant Chaturvedi* Department of Cardiology, Non-Invasive Cardiology, Eternal Heart Care Center & research Institute, Rajasthan, India Received: September 15, 2015; Published: October
Cronicon OPEN ACCESS Hemant Chaturvedi* Department of Cardiology, Non-Invasive Cardiology, Eternal Heart Care Center & research Institute, Rajasthan, India Received: September 15, 2015; Published: October
Dr Navin Chandra Clinical Research Fellow in Cardiology St George s University of London
 Dr Navin Chandra Clinical Research Fellow in Cardiology St George s University of London Cardiac Adaptation in Athletes Athletic training for prolonged periods may result in physiological adaptations of
Dr Navin Chandra Clinical Research Fellow in Cardiology St George s University of London Cardiac Adaptation in Athletes Athletic training for prolonged periods may result in physiological adaptations of
EVALUATION OF ELECTROCARDIOGRAPHIC FINDINGS IN ATHLETES
 EVALUATION OF ELECTROCARDIOGRAPHIC FINDINGS IN ATHLETES UNIT OF INHERITED CV DISEASES HEART CENTER OF THE YOUNG AND ATHLETES A DPT OF CARDIOLOGY UNIVERSITY OF ATHENS EVALUATION OF ELECTROCARDIOGRAPHIC
EVALUATION OF ELECTROCARDIOGRAPHIC FINDINGS IN ATHLETES UNIT OF INHERITED CV DISEASES HEART CENTER OF THE YOUNG AND ATHLETES A DPT OF CARDIOLOGY UNIVERSITY OF ATHENS EVALUATION OF ELECTROCARDIOGRAPHIC
Sudden Death in Athletes: What is the role of ECG Screening?
 Sudden Death in Athletes: What is the role of ECG Screening? Byron K. Lee MD Professor of Medicine Director of EP Laboratory leeb@medicine.ucsf.edu Division of Cardiology Cardiac Electrophysiology Arrhythmias,
Sudden Death in Athletes: What is the role of ECG Screening? Byron K. Lee MD Professor of Medicine Director of EP Laboratory leeb@medicine.ucsf.edu Division of Cardiology Cardiac Electrophysiology Arrhythmias,
Electrocardiographic abnormalities in patients with pulmonary sarcoidosis (RCD code: III)
 Journal of Rare Cardiovascular Diseases 2017; 3 (3): 81 85 www.jrcd.eu ORIGINAL PAPER Diseases of the heart Electrocardiographic abnormalities in patients with pulmonary sarcoidosis (RCD code: III) Justyna
Journal of Rare Cardiovascular Diseases 2017; 3 (3): 81 85 www.jrcd.eu ORIGINAL PAPER Diseases of the heart Electrocardiographic abnormalities in patients with pulmonary sarcoidosis (RCD code: III) Justyna
PRELIMINARY STUDIES OF LEFT VENTRICULAR WALL THICKNESS AND MASS OF NORMOTENSIVE AND HYPERTENSIVE SUBJECTS USING M-MODE ECHOCARDIOGRAPHY
 Malaysian Journal of Medical Sciences, Vol. 9, No. 1, January 22 (28-33) ORIGINAL ARTICLE PRELIMINARY STUDIES OF LEFT VENTRICULAR WALL THICKNESS AND MASS OF NORMOTENSIVE AND HYPERTENSIVE SUBJECTS USING
Malaysian Journal of Medical Sciences, Vol. 9, No. 1, January 22 (28-33) ORIGINAL ARTICLE PRELIMINARY STUDIES OF LEFT VENTRICULAR WALL THICKNESS AND MASS OF NORMOTENSIVE AND HYPERTENSIVE SUBJECTS USING
Long-term athletic training is associated with cardiac
 Remodeling of Left Ventricular Hypertrophy in Elite Athletes After Long-Term Deconditioning Antonio Pelliccia, MD; Barry J. Maron, MD; Rosanna De Luca, MD; Fernando M. Di Paolo, MD; Antonio Spataro, MD;
Remodeling of Left Ventricular Hypertrophy in Elite Athletes After Long-Term Deconditioning Antonio Pelliccia, MD; Barry J. Maron, MD; Rosanna De Luca, MD; Fernando M. Di Paolo, MD; Antonio Spataro, MD;
R egular intensive physical exercise is associated with an
 495 CARDIOVASCULAR MEDICINE Physiological upper limits of ventricular cavity size in highly trained adolescent athletes J Makan, S Sharma, S Firoozi, G Whyte, P G Jackson, W J McKenna... See end of article
495 CARDIOVASCULAR MEDICINE Physiological upper limits of ventricular cavity size in highly trained adolescent athletes J Makan, S Sharma, S Firoozi, G Whyte, P G Jackson, W J McKenna... See end of article
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
Right ventricular adaptation in endurance athletes. António Freitas. No conflict of interest
 The role of echocardiography in sports cardiology Right ventricular adaptation in endurance athletes. António Freitas Cardiology Department - Fernando Fonseca Hospital Lisbon Sports Medicine Centre - Lisbon
The role of echocardiography in sports cardiology Right ventricular adaptation in endurance athletes. António Freitas Cardiology Department - Fernando Fonseca Hospital Lisbon Sports Medicine Centre - Lisbon
the Young Athlete David B. Gremmels, MD Pediatric Cardiologist Children s Hospitals and Clinics of MN
 Cardiovascular Risk Assessment in the Young Athlete David B. Gremmels, MD Pediatric Cardiologist Children s Heart Clinic Children s Hospitals and Clinics of MN No disclosure or financial relationships
Cardiovascular Risk Assessment in the Young Athlete David B. Gremmels, MD Pediatric Cardiologist Children s Heart Clinic Children s Hospitals and Clinics of MN No disclosure or financial relationships
SUDDEN CARDIAC DEATH IN ATHLETES
 SUDDEN CARDIAC DEATH IN ATHLETES Alix Dufresne, MD, FACP, FACC, FESC Cardiology Division Chief, Interfaith Medical Center Director Cardiology Clinic, Kingsbrook Jewish Center PURPOSE AND OBJECTIVES PURPOSE
SUDDEN CARDIAC DEATH IN ATHLETES Alix Dufresne, MD, FACP, FACC, FESC Cardiology Division Chief, Interfaith Medical Center Director Cardiology Clinic, Kingsbrook Jewish Center PURPOSE AND OBJECTIVES PURPOSE
at least 4 8 hours per week
 ECG IN ATHLETS An athlete is defined as an individual who engages in regular exercise or training for sport or general fitness, typically with a premium on performance, and often engaged in individual
ECG IN ATHLETS An athlete is defined as an individual who engages in regular exercise or training for sport or general fitness, typically with a premium on performance, and often engaged in individual
La valutazione dell atleta: è una strategia salva-vita e costo-efficace?
 La valutazione dell atleta: è una strategia salva-vita e costo-efficace? Primo trattato di Medicina Wilson and Jungner s criteria In the 1960s the World Health Organization adopted the Wilson and Jungner
La valutazione dell atleta: è una strategia salva-vita e costo-efficace? Primo trattato di Medicina Wilson and Jungner s criteria In the 1960s the World Health Organization adopted the Wilson and Jungner
Appendix II: ECHOCARDIOGRAPHY ANALYSIS
 Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Cardiac Dysrhythmias and Sports
 Sudden unexpected death during athletic participation is the overriding consideration in advising individuals with dysrhythmias about participation in sports. The incidence of sudden death is 1 to 2 per
Sudden unexpected death during athletic participation is the overriding consideration in advising individuals with dysrhythmias about participation in sports. The incidence of sudden death is 1 to 2 per
Hereditary Cardiovascular Conditions. genetic testing for undiagnosed diseases
 Hereditary Cardiovascular Conditions genetic testing for undiagnosed diseases What is Hypertrophic Cardiomyopathy (HCM)? normal heart heart with hcm Extra or thick heart muscle Typically in the left ventricle
Hereditary Cardiovascular Conditions genetic testing for undiagnosed diseases What is Hypertrophic Cardiomyopathy (HCM)? normal heart heart with hcm Extra or thick heart muscle Typically in the left ventricle
Systolic Anterior Motion of Mitral Valve Subchordal Apparatus: A Rare Echocardiographic Pattern in Non- Obstructive Hypertrophic Cardiomyopathy
 Case Report Cardiol Res. 2017;8(5):258-264 Systolic Anterior Motion of Mitral Valve Subchordal Apparatus: A Rare Echocardiographic Pattern in Non- Obstructive Hypertrophic Cardiomyopathy Jezreel L. Taquiso
Case Report Cardiol Res. 2017;8(5):258-264 Systolic Anterior Motion of Mitral Valve Subchordal Apparatus: A Rare Echocardiographic Pattern in Non- Obstructive Hypertrophic Cardiomyopathy Jezreel L. Taquiso
Jonathan Kim MD, FACC
 Jonathan Kim MD, FACC Assistant Professor, Division of Cardiology, Emory University Adjunct Assistant Professor, School of Applied Physiology, Georgia Tech Team Cardiologist, Sports Medicine, Emory University
Jonathan Kim MD, FACC Assistant Professor, Division of Cardiology, Emory University Adjunct Assistant Professor, School of Applied Physiology, Georgia Tech Team Cardiologist, Sports Medicine, Emory University
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction
 Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Endurance Exercise and Cardiovascular Health
 Endurance Exercise and Cardiovascular Health Professor Sanjay Sharma St George s University of London St George s Hospital NHS Trust sasharma@sgul.ac.uk @SSharmacardio Conflicts/Disclosures: None Objectives
Endurance Exercise and Cardiovascular Health Professor Sanjay Sharma St George s University of London St George s Hospital NHS Trust sasharma@sgul.ac.uk @SSharmacardio Conflicts/Disclosures: None Objectives
Athletes with cardiac disease; dead and buried or chance for resurrection?
 Athletes with cardiac disease; dead and buried or chance for resurrection? EuroPRevent 2011 Geneva F. Carré University Rennes 1-Pontchaillou Hospital Inserm U642, Rennes - F-35000 Risk of physical activity
Athletes with cardiac disease; dead and buried or chance for resurrection? EuroPRevent 2011 Geneva F. Carré University Rennes 1-Pontchaillou Hospital Inserm U642, Rennes - F-35000 Risk of physical activity
Screening of Children and Adolescents at Risk of Sudden Cardiac Arrest: What Is the Utility of Non-Invasive Imaging?
 Screening of Children and Adolescents at Risk of Sudden Cardiac Arrest: What Is the Utility of Non-Invasive Imaging? Beth F. Printz, M.D., Ph.D. Medical Director, Non-Invasive Imaging Rady Children s Hospital,
Screening of Children and Adolescents at Risk of Sudden Cardiac Arrest: What Is the Utility of Non-Invasive Imaging? Beth F. Printz, M.D., Ph.D. Medical Director, Non-Invasive Imaging Rady Children s Hospital,
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
27-year-old professionnal rugby player: asymptomatic
 27-year-old professionnal rugby player: asymptomatic Benefits and limits of cardiac MRI in the young athlete with a suspected heart disease. Philippe PAULE Service de Cardiologie, HIA Clermont Tonnerre,
27-year-old professionnal rugby player: asymptomatic Benefits and limits of cardiac MRI in the young athlete with a suspected heart disease. Philippe PAULE Service de Cardiologie, HIA Clermont Tonnerre,
I n 490 BC, Pheidippides, the renowned Athenean
 710 REVIEW Risk of competitive sport in young athletes with heart disease S Firoozi, S Sharma, W J McKenna... The majority of sudden deaths in young athletes occur in the context of underlying inherited
710 REVIEW Risk of competitive sport in young athletes with heart disease S Firoozi, S Sharma, W J McKenna... The majority of sudden deaths in young athletes occur in the context of underlying inherited
Pre-Participation Athletic Cardiac Screening
 Pre-Participation Athletic Cardiac Screening Kimberly A Krabill, MD Pediatric and Fetal Cardiologist Northwest Congenital Heart Care, Division of MedNax Cardiology Update for Primary Care Symposium July
Pre-Participation Athletic Cardiac Screening Kimberly A Krabill, MD Pediatric and Fetal Cardiologist Northwest Congenital Heart Care, Division of MedNax Cardiology Update for Primary Care Symposium July
A new consensus document on electrocardiographic interpretation in athletes: does it help to prevent sudden cardiac death in athletes?
 Neth Heart J (2018) 26:127 132 https://doi.org/10.1007/s12471-018-1076-6 POINT OF VIEW A new consensus document on electrocardiographic interpretation in athletes: does it help to prevent sudden cardiac
Neth Heart J (2018) 26:127 132 https://doi.org/10.1007/s12471-018-1076-6 POINT OF VIEW A new consensus document on electrocardiographic interpretation in athletes: does it help to prevent sudden cardiac
Hypertrophic Cardiomyopathy
 019-CardioCase:019-CardioCase 4/16/07 1:39 PM Page 19 Hypertrophic Cardiomyopathy Abdullah Alshehri, MD; and Andrew Ignaszewski, MD, FRCPC CardioCase presentation Presley s check-up Presley, 37, discovered
019-CardioCase:019-CardioCase 4/16/07 1:39 PM Page 19 Hypertrophic Cardiomyopathy Abdullah Alshehri, MD; and Andrew Ignaszewski, MD, FRCPC CardioCase presentation Presley s check-up Presley, 37, discovered
Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy
 Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy Evan Adelstein, MD, FHRS John Gorcsan III, MD Samir Saba, MD, FHRS
Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy Evan Adelstein, MD, FHRS John Gorcsan III, MD Samir Saba, MD, FHRS
Current ECG interpretation guidelines in the screening of athletes
 REVIEW ARTICLE 7 How to differentiate physiological adaptation to intensive physical exercise from pathologies Current ECG interpretation guidelines in the screening of athletes Gemma Parry-Williams, Sanjay
REVIEW ARTICLE 7 How to differentiate physiological adaptation to intensive physical exercise from pathologies Current ECG interpretation guidelines in the screening of athletes Gemma Parry-Williams, Sanjay
Training adaptation of the heart according to the static-dynamic components of sports and seasonal changes in the athletes heart
 Training adaptation of the heart according to the static-dynamic components of sports and seasonal changes in the athletes heart Abstract of the PhD Thesis Eszter Csajági MD Doctoral School of Sport Sciences
Training adaptation of the heart according to the static-dynamic components of sports and seasonal changes in the athletes heart Abstract of the PhD Thesis Eszter Csajági MD Doctoral School of Sport Sciences
Cardiomyopathy. Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement
 Cardiomyopathy Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement Nebraska Home Office Life Underwriters Association March 20, 2018 1 Cardiomyopathy A myocardial disorder in which
Cardiomyopathy Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement Nebraska Home Office Life Underwriters Association March 20, 2018 1 Cardiomyopathy A myocardial disorder in which
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital
 LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Novel echocardiographic modalities: 3D echo, speckle tracking and strain rate imaging. Potential roles in sports cardiology. Stefano Caselli, MD, PhD
 Novel echocardiographic modalities: 3D echo, speckle tracking and strain rate imaging. Potential roles in sports cardiology. Stefano Caselli, MD, PhD Ospedale San Pietro Fatebenefratelli Rome, Italy Differential
Novel echocardiographic modalities: 3D echo, speckle tracking and strain rate imaging. Potential roles in sports cardiology. Stefano Caselli, MD, PhD Ospedale San Pietro Fatebenefratelli Rome, Italy Differential
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
April 22, 2017 Abraham Rothman, MD
 April 22, 2017 Abraham Rothman, MD University of Nevada School of Medicine } Definitions } Adults } Children } Heart beats } Children and adolescents who want to participate in intensive exercise. } Just
April 22, 2017 Abraham Rothman, MD University of Nevada School of Medicine } Definitions } Adults } Children } Heart beats } Children and adolescents who want to participate in intensive exercise. } Just
DOI: /
 The Egyptian Journal of Hospital Medicine (Apr. 2015) Vol. 59, Page 167-171 Optimization of Coronary Sinus Lead Position in Cardiac Resynchronization Therapy guided by Three Dimensional Echocardiography
The Egyptian Journal of Hospital Medicine (Apr. 2015) Vol. 59, Page 167-171 Optimization of Coronary Sinus Lead Position in Cardiac Resynchronization Therapy guided by Three Dimensional Echocardiography
Inspiratory Right Ventricular Outflow Obstruction in a Patient with Hypertrophic Cardiomyopathy
 Case Reports Inspiratory Right Ventricular Outflow Obstruction in a Patient with Hypertrophic Cardiomyopathy Kazufumi TSUCHIHASHI, M.D., Akihito TSUCHIDA, M.D., Nobuichi HIKITA, M.D., Shuji YONEKURA, M.D.,
Case Reports Inspiratory Right Ventricular Outflow Obstruction in a Patient with Hypertrophic Cardiomyopathy Kazufumi TSUCHIHASHI, M.D., Akihito TSUCHIDA, M.D., Nobuichi HIKITA, M.D., Shuji YONEKURA, M.D.,
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
6/19/2018. Background Athlete s heart. Ultimate question. Applying the International Criteria for ECG
 Applying the International Criteria for ECG Interpretation in Athletes to a preparticipation screening program DAVE SIEBERT, MD, CAQSM ASSISTANT PROFESSOR DEPARTMENT OF FAMILY MEDICINE UNIVERSITY OF WASHINGTON
Applying the International Criteria for ECG Interpretation in Athletes to a preparticipation screening program DAVE SIEBERT, MD, CAQSM ASSISTANT PROFESSOR DEPARTMENT OF FAMILY MEDICINE UNIVERSITY OF WASHINGTON
C. Quarta, L. Obici, S. Longhi, S. Perlini, A. Milandri, F. Del Corso, F. Perfetto, F. Cappelli, G. Merlini, C. Rapezzi
 Hereditary transthyretin-related amyloidosis with exclusively cardiac phenotype: disease profile and differential diagnosis with hypertrophic cardiomyopathy and senile systemic amyloidosis C. Quarta, L.
Hereditary transthyretin-related amyloidosis with exclusively cardiac phenotype: disease profile and differential diagnosis with hypertrophic cardiomyopathy and senile systemic amyloidosis C. Quarta, L.
Atrial Fibrillaton. Key: RA: right atrium RV: right ventricle PA: pulmonic artery LA: left atrium LV: left ventricle AO: aorta
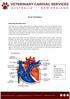 Atrial Fibrillaton How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Atrial Fibrillaton How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Evaluation of Left Ventricular Hypertrophy in U.S. Air Force Aviators
 Evaluation of Left Ventricular Hypertrophy in U.S. Air Force Aviators Daniel LaMar, MD, MPH Maj, USAF, MC, FS USAF School of Aerospace Medicine WPAFB, OH RAM 2013 Distribution A: Approved for public release;
Evaluation of Left Ventricular Hypertrophy in U.S. Air Force Aviators Daniel LaMar, MD, MPH Maj, USAF, MC, FS USAF School of Aerospace Medicine WPAFB, OH RAM 2013 Distribution A: Approved for public release;
Endurance sports and sudden cardiac death
 Symposium: Endurance training and ventricular arrhythmias Endurance sports and sudden cardiac death DOMENICO CORRADO, MD, PhD Department of Cardiac, Thoracic and Vascular Sciences University of Padova,
Symposium: Endurance training and ventricular arrhythmias Endurance sports and sudden cardiac death DOMENICO CORRADO, MD, PhD Department of Cardiac, Thoracic and Vascular Sciences University of Padova,
Cardiac Evaluation of the Adolescent. Indications for ordering an ECG 3/18/2010. Cardiac Evaluation of the Adolescent W.
 Cardiac Evaluation of the Adolescent W. Reid Thompson, M.D. The Helen B. Taussig Children s Heart Center Johns Hopkins University School of Medicine Goals for talk By the end of the session you should
Cardiac Evaluation of the Adolescent W. Reid Thompson, M.D. The Helen B. Taussig Children s Heart Center Johns Hopkins University School of Medicine Goals for talk By the end of the session you should
Echocardiographic Evaluation of the Cardiomyopathies. Stephanie Coulter, MD, FACC, FASE April, 2016
 Echocardiographic Evaluation of the Cardiomyopathies Stephanie Coulter, MD, FACC, FASE April, 2016 Cardiomyopathies (CMP) primary disease intrinsic to cardiac muscle Dilated CMP Hypertrophic CMP Infiltrative
Echocardiographic Evaluation of the Cardiomyopathies Stephanie Coulter, MD, FACC, FASE April, 2016 Cardiomyopathies (CMP) primary disease intrinsic to cardiac muscle Dilated CMP Hypertrophic CMP Infiltrative
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
THE HEART THE CIRCULATORY SYSTEM
 THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
The athlete s heart: Different training responses in African and Caucasian male elite football players
 The athlete s heart: Different training responses in African and Caucasian male elite football players Gard Filip Gjerdalen Oslo University Hospital, Aker. Bjørknes College Co-writers: Hisdal J, Solberg
The athlete s heart: Different training responses in African and Caucasian male elite football players Gard Filip Gjerdalen Oslo University Hospital, Aker. Bjørknes College Co-writers: Hisdal J, Solberg
Slide 1. Slide 2. Slide 3. Sudden Cardiac Death In Athletes. Epidemiology. Epidemiology. Shaun McMurtry, MD Primary Care Sports Medicine
 Slide 1 Sudden Cardiac Death In Athletes Shaun McMurtry, MD Primary Care Sports Medicine Slide 2 Epidemiology College and Professional Athletes 500,000 participants each year Competitive Athletics Estimated
Slide 1 Sudden Cardiac Death In Athletes Shaun McMurtry, MD Primary Care Sports Medicine Slide 2 Epidemiology College and Professional Athletes 500,000 participants each year Competitive Athletics Estimated
Syncope Update Dr Matthew Lovell, Consultant in Cardiology
 Syncope Update Dr Matthew Lovell, Consultant in Cardiology Definition of Syncope Syncope is defined as TLOC due to cerebral hypoperfusion Characterized by a rapid onset, short duration, and spontaneous
Syncope Update Dr Matthew Lovell, Consultant in Cardiology Definition of Syncope Syncope is defined as TLOC due to cerebral hypoperfusion Characterized by a rapid onset, short duration, and spontaneous
Left ventricular non-compaction: the New Cardiomyopathy on the Block
 Left ventricular non-compaction: the New Cardiomyopathy on the Block Aamir Jeewa MB BCh, FAAP, FRCPC Section Head, Cardiomyopathy & Heart Function Program The Hospital for Sick Children Assistant Professor
Left ventricular non-compaction: the New Cardiomyopathy on the Block Aamir Jeewa MB BCh, FAAP, FRCPC Section Head, Cardiomyopathy & Heart Function Program The Hospital for Sick Children Assistant Professor
CARDIOVASCULAR RISK FACTORS & TARGET ORGAN DAMAGE IN GREEK HYPERTENSIVES
 CARDIOVASCULAR RISK FACTORS & TARGET ORGAN DAMAGE IN GREEK HYPERTENSIVES C. Liakos, 1 G. Vyssoulis, 1 E. Karpanou, 2 S-M. Kyvelou, 1 V. Tzamou, 1 A. Michaelides, 1 A. Triantafyllou, 1 P. Spanos, 1 C. Stefanadis
CARDIOVASCULAR RISK FACTORS & TARGET ORGAN DAMAGE IN GREEK HYPERTENSIVES C. Liakos, 1 G. Vyssoulis, 1 E. Karpanou, 2 S-M. Kyvelou, 1 V. Tzamou, 1 A. Michaelides, 1 A. Triantafyllou, 1 P. Spanos, 1 C. Stefanadis
Managing Hypertrophic Cardiomyopathy with Imaging. Gisela C. Mueller University of Michigan Department of Radiology
 Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation
 Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation Ömer Aktug 1, MD; Guido Dohmen 2, MD; Kathrin Brehmer 1, MD; Verena Deserno 1 ; Ralf Herpertz 1 ; Rüdiger
Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation Ömer Aktug 1, MD; Guido Dohmen 2, MD; Kathrin Brehmer 1, MD; Verena Deserno 1 ; Ralf Herpertz 1 ; Rüdiger
Dr. Dermot Phelan MB BCh BAO PhD European Society of Cardiology 2012
 Relative Apical Sparing of Longitudinal Strain Using 2- Dimensional Speckle-Tracking Echocardiography is Both Sensitive and Specific for the Diagnosis of Cardiac Amyloidosis. Dr. Dermot Phelan MB BCh BAO
Relative Apical Sparing of Longitudinal Strain Using 2- Dimensional Speckle-Tracking Echocardiography is Both Sensitive and Specific for the Diagnosis of Cardiac Amyloidosis. Dr. Dermot Phelan MB BCh BAO
Title: Left atrium size in former elite athletes
 Title: Left atrium size in former elite athletes Short title: exercise and left atrium Authors: Fabian Sanchis-Gomar, MD, PhD, a Nuria Garatachea, PhD, a,b Pilar Catalán, MD, c Marta López, MD, d Alejandro
Title: Left atrium size in former elite athletes Short title: exercise and left atrium Authors: Fabian Sanchis-Gomar, MD, PhD, a Nuria Garatachea, PhD, a,b Pilar Catalán, MD, c Marta López, MD, d Alejandro
Restrictive Cardiomyopathy
 ESC Congress 2011, Paris Imaging Unusual Causes of Cardiomyopathy Restrictive Cardiomyopathy Kazuaki Tanabe, MD, PhD Professor of Medicine Chair, Division of Cardiology Izumo, Japan I Have No Disclosures
ESC Congress 2011, Paris Imaging Unusual Causes of Cardiomyopathy Restrictive Cardiomyopathy Kazuaki Tanabe, MD, PhD Professor of Medicine Chair, Division of Cardiology Izumo, Japan I Have No Disclosures
