Mitral valve hemodynamics after repair of acute posterior leaflet prolapse: Quadrangular resection versus triangular resection versus neochordoplasty
|
|
|
- Irene Mary Knight
- 5 years ago
- Views:
Transcription
1 Mitral valve hemodynamics after repair of acute posterior leaflet prolapse: Quadrangular resection versus triangular resection versus neochordoplasty Muralidhar Padala, MS, a Scott N. Powell, BS, a Laura R. Croft, BS, a Vinod H. Thourani, MD, b Ajit P. Yoganathan, PhD, a and David H. Adams, MD c Objective: Leaflet prolapse resulting from acute chordal rupture is one presentation of fibroelastic deficiency that is associated with minimal leaflet changes in the prolapsing segment. Minimizing resection and preserving leaflet tissue may be an optimal surgical strategy. We examined the importance of the leaflet preservation concept by comparing resective and nonresective surgical procedures in practice today. Methods: Eight porcine mitral valves were evaluated in an in vitro heart simulator before surgical manipulation. Mitral regurgitation was created in these valves by transecting the posterior marginal chordae resulting in severe P2 prolapse. After confirmation of mitral regurgiation via regurgitant flow measurement (ml/beat), regurgitation was corrected by three repairs: neochordoplasty with polytetrafluoroethylene sutures (Gore-Tex; W. L. Gore & Associates, Inc, Flagstaff, Ariz), triangular resection, and quadrangular resection with annular compression. Postrepair valve hemodynamics were quantified under pulsatile conditions of 120 mm Hg peak transmitral pressure and 5 L/min cardiac output at 70 beats/min. Furthermore, hemodynamic, geometric, and echocardiographic indices were measured. Results: Transecting the marginal chordae resulted in severe P2 prolapse and significant mitral regurgiation ( ml/beat). Regurgitant volume was significantly reduced after any of the three surgical approaches (quadrangular, ml/beat; triangular, ml/beat; neochordal, ml/beat). In comparison with the baseline normal valves, leaflet coaptation length and posterior leaflet mobility were significantly reduced in the quadrangular resection group, whereas they were partially restored in the triangular resection and fully preserved in the neochordoplasty group. Conclusions: Although the three repair procedures are hemodynamically comparable, valve function and leaflet kinematics were significantly better after a nonresection or limited resective correction of leaflet prolapse in this experimental model of acute chordal rupture with otherwise normal leaflet geometry. From the Wallace H. Coulter Department of Biomedical Engineering, Georgia Institute of Technology, a the Division of Cardiothoracic Surgery, Emory University School of Medicine, b Atlanta, Ga; and the Department of Cardiothoracic Surgery, c Mt Sinai School of Medicine, New York, NY. Read at the Eighty-eighth Annual Meeting of The American Association for Thoracic Surgery, San Diego, Calif, May 10 14, Received for publication May 13, 2008; revisions received Dec 9, 2008; accepted for publication Jan 13, Address for reprints: Ajit P. Yoganathan, PhD, The Wallace H. Coulter Distinguished Faculty Chair in Biomedical Engineering and Regents Professor, Associate Chair for Research, Wallace H. Coulter School of Biomedical Engineering, Georgia Institute of Technology and Emory University, Room 2119 U. A. Whitaker Building, 313 Ferst Dr, Atlanta, GA ( ajit.yoganathan@bme.gatech.edu). J Thorac Cardiovasc Surg 2009;138: /$36.00 Copyright Ó 2009 by The American Association for Thoracic Surgery doi: /j.jtcvs Surgical strategies addressing mitral regurgitation resulting from chordal rupture often involve partial leaflet resection with or without annular plication and annuloplasty. In the chronic setting, leaflet distension and myxoid changes may occur in the prolapsing segment and various resective techniques have been described with excellent results. 1 However, in patients with leaflet prolapse resulting from acute chordal rupture, distension of leaflets is minimal early in the course of mitral valve regurgitation, 2,3 and leaflet resection may not be as effective a strategy. Under such acute conditions, resective techniques may limit residual leaflet mobility and the leaflet surface available for opposing leaflet coaptation. We used an in vitro model of acute chordal rupture to compare mitral valve function and hemodynamics after valve repair with common repair techniques including neochordoplasty (no resection), triangular resection, and quadrangular resection with annular plication. RESEARCH DESIGN AND METHODS Specimen Selection Porcine hearts were obtained from a local abattoir and transported to the laboratory in ice cold phosphate-buffered saline solution. Eight hearts (n ¼ 8) with mitral valves of identical sizes (size 30 annuloplasty ring sizers; Edwards LifeSciences, Irvine, Calif) were identified for use in this study. Valves of the same annular size, anterior and posterior leaflet areas, and heights were selected for this study. Mitral valves with intact annular and subvalvular structures (including the papillary muscles) were extracted from these hearts and stored in cold saline for later use. A 1-cm section of atrial tissue above the mitral annulus was left uncut, and this tissue was used to suture the valve onto a silicone annulus to mount into the left heart simulator. In Vitro Left Heart Simulator The in vitro experimental left heart simulator used in this study is a wellestablished setup that was reported previously. 4,5 In brief, the simulator (Figure 1, A) is a computer-controlled, pressure-driven, compressible The Journal of Thoracic and Cardiovascular Surgery c Volume 138, Number 2 309
2 Abbreviations and acronyms a ¼ posterior excursion angle b ¼ anterior excursion angle D a ¼ distance from coaptation to anterior annulus D p ¼ distance from coaptation to posterior annulus eptfe ¼ expanded polytetrafluoroethylene bladder system that can generate the physiologic pulsatile flow and pressure flow conditions of the left heart. The simulator has a left atrium, a left ventricle, and a mitral annular plate sandwiched between them. The mitral annulus plate has a D-shaped ring made of silicone that is rigid and is covered in a water-proofing polyester (Darlexx; Darlington Fabrics Corp, Shawnut Mills, Mass). The mitral annulus was sutured onto the silicone ring with 3-0 silk sutures in a mattress fashion and the papillary muscles were mounted onto two adjustable-geared fixtures in the left ventricular chamber. After the valve was mounted, the simulator was filled with 0.9% saline solution (vol/vol) and run at adult hemodynamic conditions of 120 mm Hg peak transmitral pressure and 5-L/min cardiac output at 70 beats/min (Figure 1, B and C). The left ventricular, left atrial, and transmitral pressure curves were monitored and recorded with a differential pressure transducer (DP9-40; Validyne Engineering, Northridge, Calif), and the flow data were monitored with an electromagnetic flow probe (600; Braemar Inc, King, NC). The acquisition, signal conditioning, and analysis were performed with DAQCard 1200 (National Instruments, Austin, Tex) and a custom data processing program (DAQ-ANAL 2.0). Experimental Protocol Each mitral valve was studied under the experimental conditions in the order listed herein: 1. Control/baseline. The annulus was maintained at its normal size, and the papillary muscles were fixed in their normal positions, ie, with the papillary muscle tips perpendicular to the mitral annular plane and in the plane passing through leaflet coaptation, such that the commissural chordae from the same papillary muscle are parallel to each other. The valve was studied under adult hemodynamic conditions of 120 mm Hg peak transmitral pressure and 5-L/min cardiac output at 70 beats/min. The regurgitant volume and stroke volume were volumetrically measured, and leaflet coaptation length and indices that elucidate leaflet mobility were recorded with 2-dimensional echocardiograph (Figure 2, A). 2. Posterior leaflet prolapse. After acquisition of the baseline data, the two marginal chordae on the free edge of the posterior leaflet were transected, which resulted in severe segmental prolapse of the P2 cusp. The simulator was again run under the identical hemodynamic conditions described previously, and the hemodynamic and echocardiographic measurements were obtained. P2 prolapse was validated by reconstructing the 3-dimensional geometry of the mitral valve from the echocardiographic images and superimposed with only the reverse color Doppler data, showing the regurgitation jet as shown in Figure 2, B. The regurgitation and stroke volumes were also quantified with the flow probe. 3. Neochordoplasty. In this procedure, the transected marginal chordae tendineae were replaced with loops of 5-0 expanded polytetrafluoroethylene sutures (eptfe; Gore-Tex, W. L. Gore & Associates, Inc, Flagstaff, Ariz), 6 as shown in Figure 3, A. The ventricular chamber was filled with saline to close the mitral valve, lengths of the neochordae were adjusted, and the neochordae were tied onto a Teflon pledget on the tip of the papillary muscle. The valve was then tested under pulsatile hemodynamic flow conditions as listed in the previous sections, and relevant hemodynamic and echocardiographic end points were measured. FIGURE 1. A, Schematic of the in vitro left heart simulator with a native porcine mitral valve. B, Atrial view of the mitral valve showing the anterior and the posterior leaflets. C, Ventricular view of the valve showing the chordae tendineae and the papillary muscles. 310 The Journal of Thoracic and Cardiovascular Surgery c August 2009
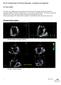
3 FIGURE 2. A, The top left image is a 2-dimensional echocardiograph that shows the prolapsing P2 scallop of the posterior leaflet resulting from chordal transection, and the bottom left image is a 3-dimensional reconstruction of the prolapsing leaflet as seen from the left atrium. The 3-dimensional reconstruction clearly shows the leaflet prolapse and the loss of leaflet coaptation. B, The 3-dimensional eccentric regurgitation jet recorded by 3-dimensional echocardiography from the top view and isometric views. A regurgitation jet directed toward the anterior annulus can be clearly seen with the posterior leaflet prolapse. 4. Limited triangular resection. After acquisition of the data in step 3, the neochordae were removed and a triangular resection was performed on the free edge of the P2 scallop (Figure 3, B). The total height of the posterior leaflet from the free edge to the annulus was measured, and a triangular segment that had a height of one third (total leaflet height) and a base width equal to the length between the two ruptured marginal chordae was resected as reported in an earlier study by Gazoni and associates. 7 The posterior leaflet was reconstructed by carefully approximating the free edges of the triangular resection with interrupted 3-0 silk sutures (Ethicon Inc, Somerville, NJ), such that minimal tension was induced on the residual leaflet segments. After reconstruction of the leaflet, the valve was again tested under the pulsatile hemodynamic conditions that were previously used. 5. Quadrangular resection with annular compression. Quadrangular resection was performed on the same valve by resecting a rectangular section of the P2 segment and compressing the annulus at this region, 8 as shown in Figure 3, C. The dimensions of the resected segment were chosen such that the breadth of the rectangle equaled the distance between the two ruptured marginal chordae and the length extended from the free edge to the mitral annulus. The section of the annulus in the resected region was then plicated and approximated with 3 or 4 compression sutures. The free edges after resection were carefully approximated with interrupted knots with 3-0 silk sutures in a similar fashion to that used in the triangular resection group. The valve was then tested under pulsatile hemodynamic conditions. Measurement Techniques and Data Acquisition Regurgitation volume. Regurgitant volume through the valve was calculated from the recorded transmitral flow curve. The flow curve was averaged over 15 cardiac cycles and the area under the negative part of the flow curve was integrated to obtain the net regurgitation volume. Echocardiographic measurements. Three-dimensional echocardiographic measurements were obtained with a 3-dimensional matrixarray ultrasound sector transducer (X7 Matrix Probe; ie33 System, Philips Medical Systems, Andover, Mass) at 18 MHz. The transducer was adjusted to provide optimal imaging with the highest possible frame rate at a sampling depth of 12 cm. An apical long-axis view cutting across both the leaflets anteroposteriorly at the midpoint of the major axis of the annulus was used for the measurements. Echocardiographic and color Doppler images were obtained to assess the forward and the leakage flow through the cleft and the coaptation regions. Peak systolic leaflet coaptation length, posterior leaflet angle, 9 and distance of the coaptation plane from the posterior annulus were measured. Statistical Analysis All data are reported as mean 1 standard deviation. The data were tested for normality by an Anderson Darling test (MINITAB 15 software). Different experimental condition groups were compared with paired t tests. The Journal of Thoracic and Cardiovascular Surgery c Volume 138, Number 2 311
4 FIGURE 3. A, Sequential steps to replace the ruptured posterior chordae tendineae with loops of 5-0 eptfe sutures. B, Sequential steps to perform triangular resection and approximation of the resected region. C, Protocol to perform quadrangular resection and annular plication with a compression stitch. RESULTS Mitral Regurgitation Volumes All the valves had good competence under control/baseline conditions with trivial regurgitation. Transecting the two posterior marginal chordae resulted in segmental P2 scallop prolapse causing severe mitral regurgitation ( ml/beat). The three repairs significantly reduced the regurgitation from the prolapse condition, to ml/beat (P ¼.007) with neochordoplasty, ml/ beat (P ¼.008) with limited triangular resection, and ml/beat (P ¼.007) with quadrangular resection and annular compression (Figure 4, A). Leaflet Coaptation Length Leaflet coaptation length was used as a measure of valve competence that was quantified under all the experimental conditions by 2-dimensional echocardiography. Under control conditions, an average coaptation length of mm was measured, whereas under prolapse conditions there was no coaptation along the A2 P2. Neochordoplasty was the only repair that restored coaptation length to the control/baseline levels ( mm; P ¼.2), whereas both limited triangular resection and quadrangular resection decreased the coaptation length significantly to mm (P ¼.01) and mm (P ¼.0001), respectively (Figure 4, B). Postrepair Leaflet Mobility and Kinematics Posterior leaflet mobility after each surgical repair was assessed by simple echocardiographic measurements: (1) perpendicular distances from the leaflet coaptation zone to the posterior (D p ) and anterior (D a ) annuli in the septal lateral plane, (2) peak systolic excursion angles of the posterior (a) and anterior (b) leaflets, and (3) depth of leaflet coaptation FIGURE 4. A, Variation in regurgitation volume per heart beat for the control, prolapse, and the three repair procedures. B, Variation in peak systolic leaflet coaptation length between the different experimental conditions. 312 The Journal of Thoracic and Cardiovascular Surgery c August 2009
5 FIGURE 5. Geometric endpoints measured from 2-dimensional echocardiographs to quantify leaflet mobility. from the mitral annular plane (Figure 5 and Table 1). The distance of the coaptation zone from the anterior and posterior annuli were nearly equal in the control case (D p ¼ mm, D a ¼ mm), showing that the leaflet coaptation was centrally positioned from the anterior and posterior annuli in normal valves. A similar coaptation geometry was observed after neochordoplasty (D p ¼ mm; P ¼.09; D a ¼ mm; P ¼.35) as in the control group. However, both limited triangular resection (D p ¼ mm; P ¼.03; D a ¼ mm; P ¼.04) and quadrangular resection (D p ¼ mm; P ¼.006; D a ¼ mm; P ¼.01) restricted posterior leaflet mobility, resulting in displacement of the coaptation zone posteriorly. Additionally, we quantified the peak systolic leaflet angles made by the posterior and anterior leaflets with the mitral annulus as a measure of systolic leaflet mobility. The posterior leaflet angles in the neochordoplasty group (a ¼ ; P ¼.77) and limited triangular resection (a ¼ ; P ¼.25) were comparable with the angles in the control (a ¼ ) but significantly higher in the quadrangular resection group (a ¼ ; P ¼.01), as shown in Figure 5 and Table 1. The anterior leaflet angles were consistent among the four conditions, indicating that the anterior leaflet has a threshold beyond which it cannot move to coapt with the posterior leaflet owing to the limited extension of the anterior chordae tendineae. DISCUSSION In this study, we report a model that simulates the clinical setting of leaflet prolapse resulting from acute chordal rupture, as seen in some cases of endocarditis or fibroelastic deficiency. Two-dimensional and 3-dimensional echocardiographic images obtained from our in vitro model clearly illustrate the segmental P2 prolapse and the anteriorly directed eccentric regurgitation jet (Figure 2, A and B) after experimental chordal rupture. Following current trends in mitral valve repair, 10 three commonly used repair procedures for mitral valve prolapse were selected for this study. Quadrangular resection with annular compression is a standard repair procedure that is associated with good long-term durability 11 but nonphysiologic mobility of the posterior leaflet after surgery, often resulting in a monocusp valve. Carpentier and associates 8 proposed quadrangular resection to correct leaflet prolapse in patients primarily with ruptured chordae and excess tissue, wherein removal of the excessive leaflet tissue is useful to reconstruct a normal leaflet segment. Over the years, this technique has evolved into standard practice for correcting posterior leaflet prolapse irrespective of the valve disease, and our study puts additional emphasis on the importance of selecting the appropriate subset of patients with prolapse and distended tissue in whom to use this procedure. Carpentier (as reported by Fornes and associates 3 ) was the first to recognize that fibroelastic deficient valves may have minimal leaflet distention with acute chordal rupture. Our study shows that in these acutely prolapsing valves, quadrangular resection significantly reduces the posterior leaflet height, thus decreasing the systolic leaflet coaptation length. Mobility of the reconstructed posterior leaflet is often limited owing to rearrangement of the anatomic positions of the chordae tendineae after resection, with the secondary chordae from the P1 and P3 scallops moving toward the center of the posterior leaflet. Such nonphysiologic valve closure could potentially affect long-term repair durability, and our in vitro observations support this potential issue if quadrangular resection is adopted indiscriminately. Limited triangular resection of the prolapsing posterior leaflet with conservative tissue resection has been reported as a good alternative procedure that significantly reduces the size of the resection and further eliminates the need for annular plication or compression. 7,12 Our findings in nondistended leaflets also suggest improved valve function, in terms of leaflet coaptation and mobility, compared with quadrangular resection. Although the outcomes of triangular resection were better than those with quadrangular resection, a 2-mm reduction in coaptation length and a 2- to 3-mm posterior displacement of the leaflet coaptation was measured in comparison with the control group. Whether these minor TABLE 1. Variation in the echocardiographic measures for posterior and anterior leaflet mobility obtained by 2-dimensional echocardiography Control Neochordoplasty Triangular resection Quadrangular resection Posterior leaflet angle (a) in degrees *,y Anterior leaflet angle (b) in degrees *,ystatistical difference compared with the control and other repair groups, respectively. The Journal of Thoracic and Cardiovascular Surgery c Volume 138, Number 2 313
6 differences between triangular resection and controls are clinically significant is not apparent on the basis of our study. Several groups are now reporting nonresective strategies to preserve leaflet tissue and restore good leaflet coaptation and mobility. 6,13,14 This study confirms that replacing the ruptured chordae with artificial eptfe sutures would restore physiologic function of the valve without disturbing the native leaflet structure. Replacing the ruptured chordae with a single eptfe loop not only eliminated regurgitation as efficiently as the standard resection procedures but also restored leaflet coaptation length to physiologic levels, with excellent mobility of the posterior leaflet. Neochordoplasty, as performed in this study, seemed to have a benefit over leaflet resection in acute leaflet prolapse without leaflet distention. In this study, two pairs of neochordae equally distributed between the two papillary muscles were used. From each pair of chordae from the same papillary muscle head, one pair supported the free edge of the prolapsing segment and the other supported the segment 1 cm laterally away from the free edge. Such a chordal distribution was effective in our studies, but it remains unclear whether there is an optimal positioning of neochordae, other than to avoid crossing native chordae. We did not use resection with correction of leaflet prolapse by chordal transfer. This represents another alternative surgical strategy that may be beneficial in the setting of minimal leaflet distention. Limitations Any clinical implications of this model must be stated circumspectly. First, this study is an acute case of leaflet prolapse resulting from isolated chordal rupture without any annular or leaflet pathologic change(s). Clearly, we used mitral valves with normal function and tissue properties, which did not take into account any pre-existing patient diseases (eg, bacterial endocarditis) that may affect the choice of mitral valve repair. In the chronic state, myxoid changes in the leaflet tissue and leaflet distention are typically observed and resection procedures have been successfully used in repairing such valves. In this study, the neochordal length was determined with the valve closed, but ideally such an exact measurement is impossible in the clinical setting owing to ventricular motion and movement of the papillary muscles caused by contraction. One other limitation is the use of the same valve preparation for all experimental groups, which dictated the order of repair procedures. In summary, this study emphasizes the importance of leaflet preservation in repairing leaflet prolapse in otherwise normal leaflet segments. It suggests that either nonresective resuspension of the leaflet margin or limited triangular resection is preferable to quadrangular resection. We thank Holifield farms of Covington, Georgia, for generously donating the porcine hearts that were used in this study. References 1. Carpentier A. Cardiac valve surgery the French correction. J Thorac Cardiovasc Surg. 1983;86: Anyanwu AC, Adams DH. Etiologic classification of degenerative mitral valve disease: Barlow s disease and fibroelastic deficiency. Semin Thorac Cardiovasc Surg. 2007;19: Fornes P, Heudes D, Fuzellier JF, Tixier D, Bruneval P, Carpentier A. Correlation between clinical and histologic patterns of degenerative mitral valve insufficiency: a histomorphometric study of 130 excised segments. Cardiovasc Pathol. 1999;8: He S, Fontaine AA, Schwammenthal E, Yoganathan AP, Levine RA. Integrated mechanism for functional mitral regurgitation: leaflet restriction versus coapting force: in vitro studies. Circulation. 1997;96: Jimenez JH, Liou SW, Padala M, He Z, Sacks M, Gorman RC, et al. A saddleshaped annulus reduces systolic strain on the central region of the mitral valve anterior leaflet. J Thorac Cardiovasc Surg. 2007;134: Seeburger J, Kuntze T, Mohr FW. Gore-Tex chordoplasty in degenerative mitral valve repair. Semin Thorac Cardiovasc Surg. 2007;19: Gazoni LM, Fedoruk LM, Kern JA, Dent JM, Reece TB, Tribble CG, et al. A simplified approach to degenerative disease: triangular resections of the mitral valve. Ann Thorac Surg. 2007;(83): ; discussion Carpentier A, Deloche A, Dauptain J, Soyer R, Blondeau P, Piwnica A, et al. A new reconstructive operation for correction of mitral and tricuspid insufficiency. J Thorac Cardiovasc Surg. 1971;61: Magne J, Pibarot P, Dagenais F, Hachicha Z, Dumesnil JG, Sénéchal M. Preoperative posterior leaflet angle accurately predicts outcome after restrictive mitral valve annuloplasty for ischemic mitral regurgitation. Circulation. 2007;115: Filsoufi F, Carpentier A. Principles of reconstructive surgery in degenerative mitral valve disease. Semin Thorac Cardiovasc Surg. 2007;19: Gillinov AM. Durability of mitral valve repair for degenerative disease. J Thorac Cardiovasc Surg. 1998;116: Da Col U, Di Bella I, Bardelli G, Koukoulis G, Ramoni E, Ragni T. Triangular resection and folding of the posterior leaflet for mitral valve repair. J Card Surg. 2006;21: Salvador L, Mirone S, Bianchini R, Regesta T, Patelli F, Minniti G, et al. A 20- year experience with mitral valve repair with artificial chordae in 608 patients. J Thorac Cardiovasc Surg. 2008;135: Tabata M, Ghanta RK, Shekar PS, Cohn LH. Early and midterm outcomes of folding valvuloplasty without leaflet resection for myxomatous mitral valve disease. Ann Thorac Surg. 2008;86: Dreyfus GD, Corbi P, Rubin S, Aubert S. Posterior leaflet preservation in mitral valve prolapse: a new approach to mitral repair. J Heart Valve Dis. 2006;15: Perier P, Hohenberger W, Lakew F, Batz G, Urbanski P, Zacher M, et al. Toward a new paradigm for the reconstruction of posterior leaflet prolapse: midterm results of the respect rather than resect approach. Ann Thorac Surg. 2008;86: Flameng W, Meuris B, Herijgers P, Herregods MC. Durability of mitral repair in Barlow disease versus fibroelastic deficiency. J Thorac Cardiovasc Surg. 2008; 135: Discussion Dr Gus J. Vlahakes (Boston, Mass). This study comes from two institutions that have considerable experience with both clinical mitral valve reconstruction surgery and fluid dynamics with respect to the mitral valve and a long history of work in this area. I have a couple of questions that have to do in part with the model and how the model is set up and, second, with potential interpretation. In the single-frame picture you show of the echocardiogram, the valve apparatus appears to be slightly apically tethered; in other words, the coaptation surface seems to be displaced a little bit further into what would be the ventricle. When you set the apparatus up, how do you determine the initial position of the papillary muscles? Dr Padala. In 1997 we published a paper in Circulation with Dr Bob Levine in which we looked at echocardiograms to find the relationship between the mitral annular plane and the papillary muscle tips in normal subjects. We used those measurements to set the 314 The Journal of Thoracic and Cardiovascular Surgery c August 2009
7 mitral line from the papillary muscle to their normal positions in the simulator as used in that study. Dr Vlahakes. Second, in the porcine valve, what is the nature of the anatomy of the posterior leaflet? Does it have partial clefts or a scallop?type design that you might see in humans, or is it a continuous sheet of tissue? Dr Padala. It is a continuous sheet of tissue, but you can see that the P2 is definitely much larger than the P1 and the P3. The anatomy is comparable with that seen in humans. Dr Vlahakes. One area that I think is potentially missing from the analysis, which may explain some of your findings, is the intervention on the annulus. When you said you introduced some annular compression, exactly what did you mean? Did you change the annular size? Did you change the relationship between the annulus subtending the anterior leaflet versus the posterior leaflet? I think this might potentially have had considerable influence on your ultimate findings. Dr Padala. We performed annular plication using a compression stitch, keeping the annular size constant. Dr Alain F. Carpentier (Paris, France). I think this study is very interesting because it does carry on a message that I would like to point out, which is the fact that leaflet tissue should not be resected if there is no excess tissue. There is a misunderstanding in this regard not in this study, but usually which is to believe that leaflet resection should be always done. That is my first comment. My second comment is that there is an alternative to neochordal replacement, that is, chordal transposition. Particularly from the basal chordae, you can transfer them to the margin, which is an easier technique and a more elegant technique using living material. Have you tried this technique? Dr Padala. Yes. The next study that we are embarking on now is to combine neochordoplasty and chordal translocation and see whether there is a difference between the two. If there is no difference I am not a surgeon, but surgical chordal translocation may be an easier procedure. Dr Craig R. Smith (New York, NY). Just so I understand what you actually did, in 8 valves, you did the three repair techniques sequentially in the same valve. Am I right? Dr Padala. Yes. Dr Smith. That would seem to me to introduce a bias in favor of the first repair technique. Dr Padala. It does not really bias toward the first procedure because of the sequence in which we chose the repair procedures. In the first one we did neochordoplasty. In the second one, when we did the triangular resection, the part of the posterior leaflet that had neochordae was removed and encompassed the triangular resection. Dr Smith. I understand that. It all sounds very neat. It is just hard for me to imagine that it is always quite so neat. Dr Padala. Okay. Dr Smith. My second question has to do with Dr Vlahakes question about the annular compression technique. I am still not clear exactly how that was done. I think many of us would argue that the posterior leaflet looks restricted and coaptation appears limited when you get through doing the reconstruction with a quadrangular resection or a triangular resection. It is frequently not until you put in the ring that coaptation improves. I think it might depend importantly on exactly what you did in that step. Dr Padala. For the annular compression, when I removed the P2 part of the leaflet, the annulus, which was present at that particular segment, was just plicated outward and sutured onto the silicone annulus that we used in this model. Dr Smith. I would argue that that is the least effective way to preserve coaptation across the whole length of the posterior leaflet. Dr Marc R. Moon (St. Louis, Mo). It always seemed important to me to decrease the stress on the posterior leaflet because that is probably what makes the chorda rupture in the first place. The neochordal technique would not relieve that stress. I suspect you would leave them with the same stress?loaded posterior leaflet. How do you feel about that in regard to the need for the annuloplasty, and did you consider doing this without an annuloplasty? Dr Padala. In this particular study, the silicone annulus that we have made into an annuloplasty ring is actually the annulus. We have not implanted any annuloplasty rings that are commercially available. I guess there are other ways of reducing stress on the chordae and also on the posterior leaflet by probably choosing a different type or shape of annuloplasty ring, but I really cannot comment on that right now because I have not studied that. Dr Adams. If I can make one final comment about the study, this was not a study trying to differentiate or condemn posterior leaflet resection, which, frankly, has the longest, most credible results in terms of durability, whether you look at freedom from reoperation or recurrence of mitral regurgitation. I think the emphasis is on the specific subgroup in which you have minimal leaflet distention. And, as Dr Carpentier said, there is a misunderstanding that all leaflets should be resected. What we hoped to show in this first study was that that is not the case in the setting of an otherwise normal segment that has acute prolapse. Craig, I think your points about annuloplasty are well taken. When you start to take out more tissue, clearly the annuloplasty does several things. One of them is stabilizing the repair and removing tension, but it also improves the coaptation lengths. I think you are absolutely right. I am not sure that was going to affect this particular study very much because the resections were very limited. The Journal of Thoracic and Cardiovascular Surgery c Volume 138, Number 2 315
Posterior leaflet prolapse is the most common lesion seen
 Techniques for Repairing Posterior Leaflet Prolapse of the Mitral Valve Robin Varghese, MD, MS, and David H. Adams, MD Posterior leaflet prolapse is the most common lesion seen in degenerative mitral valve
Techniques for Repairing Posterior Leaflet Prolapse of the Mitral Valve Robin Varghese, MD, MS, and David H. Adams, MD Posterior leaflet prolapse is the most common lesion seen in degenerative mitral valve
Chordae replacement versus leaflet resection in minimally invasive mitral valve repair
 Perspective Chordae replacement versus leaflet resection in minimally invasive mitral valve repair Tomas Holubec, Simon H. Sündermann, Stephan Jacobs, Volkmar Falk Division of Cardiovascular Surgery, University
Perspective Chordae replacement versus leaflet resection in minimally invasive mitral valve repair Tomas Holubec, Simon H. Sündermann, Stephan Jacobs, Volkmar Falk Division of Cardiovascular Surgery, University
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Surgical Repair of the Mitral Valve Presenter: Graham McCrystal Cardiothoracic Surgeon Christchurch Public Hospital
 Mitral Valve Surgical intervention Graham McCrystal Chairs: Rajesh Nair & Gerard Wilkins Surgical Repair of the Mitral Valve Presenter: Graham McCrystal Cardiothoracic Surgeon Christchurch Public Hospital
Mitral Valve Surgical intervention Graham McCrystal Chairs: Rajesh Nair & Gerard Wilkins Surgical Repair of the Mitral Valve Presenter: Graham McCrystal Cardiothoracic Surgeon Christchurch Public Hospital
Despite advances in our understanding of the pathophysiology
 Suture Relocation of the Posterior Papillary Muscle in Ischemic Mitral Regurgitation Benjamin B. Peeler MD,* and Irving L. Kron MD,*, *Department of Cardiovascular Surgery, University of Virginia, Charlottesville,
Suture Relocation of the Posterior Papillary Muscle in Ischemic Mitral Regurgitation Benjamin B. Peeler MD,* and Irving L. Kron MD,*, *Department of Cardiovascular Surgery, University of Virginia, Charlottesville,
The Edge-to-Edge Technique f For Barlow's Disease
 The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
Basic Principles of Degenerative Mitral Valve Repair Technical Aspects and Results. Manuel Antunes Coimbra-Portugal
 Basic Principles of Degenerative Mitral Valve Repair Technical Aspects and Results Manuel Antunes Coimbra-Portugal Repair for Degenerative Disease Adams D H et al. Eur Heart J 2010;31:1958-1966 Published
Basic Principles of Degenerative Mitral Valve Repair Technical Aspects and Results Manuel Antunes Coimbra-Portugal Repair for Degenerative Disease Adams D H et al. Eur Heart J 2010;31:1958-1966 Published
Valve Analysis and Pathoanatomy: THE MITRAL VALVE
 : THE MITRAL VALVE Marc R. Moon, M.D. John M. Shoenberg Chair in CV Disease Chief, Cardiac Surgery Washington University School of Medicine, St. Louis, MO Secretary, American Association for Thoracic Surgery
: THE MITRAL VALVE Marc R. Moon, M.D. John M. Shoenberg Chair in CV Disease Chief, Cardiac Surgery Washington University School of Medicine, St. Louis, MO Secretary, American Association for Thoracic Surgery
THE FOLDING LEAFLET. Rafael García Fuster. Cardiac Surgery Department University General Hospital of Valencia
 THE FOLDING LEAFLET Rafael García Fuster Cardiac Surgery Department University General Hospital of Valencia School of Medicine Catholic University of Valencia San Vicente Mártir SPAIN Carpentier s principles
THE FOLDING LEAFLET Rafael García Fuster Cardiac Surgery Department University General Hospital of Valencia School of Medicine Catholic University of Valencia San Vicente Mártir SPAIN Carpentier s principles
Really Less-Invasive Trans-apical Beating Heart Mitral Valve Repair: Which Patients?
 Really Less-Invasive Trans-apical Beating Heart Mitral Valve Repair: Which Patients? David H. Adams, MD Cardiac Surgeon-in-Chief Mount Sinai Health System Marie Josée and Henry R. Kravis Professor and
Really Less-Invasive Trans-apical Beating Heart Mitral Valve Repair: Which Patients? David H. Adams, MD Cardiac Surgeon-in-Chief Mount Sinai Health System Marie Josée and Henry R. Kravis Professor and
Technical aspects of robotic posterior mitral valve leaflet repair
 rt of Operative Techniques Technical aspects of robotic posterior mitral valve leaflet repair Hoda Javadikasgari, Rakesh M. Suri, Tomislav Mihaljevic, Stephanie Mick,. Marc Gillinov Department of Thoracic
rt of Operative Techniques Technical aspects of robotic posterior mitral valve leaflet repair Hoda Javadikasgari, Rakesh M. Suri, Tomislav Mihaljevic, Stephanie Mick,. Marc Gillinov Department of Thoracic
Χειρουργική Αντιμετώπιση της Ανεπάρκειας της Μιτροειδούς Βαλβίδας
 Χειρουργική Αντιμετώπιση της Ανεπάρκειας της Μιτροειδούς Βαλβίδας Dr Χρήστος ΑΛΕΞΙΟΥ MD, PhD, FRCS(Glasgow), FRCS(CTh), CCST(UK) Consultant Cardiothoracic Surgeon Normal Mitral Valve Function Mitral Regurgitation
Χειρουργική Αντιμετώπιση της Ανεπάρκειας της Μιτροειδούς Βαλβίδας Dr Χρήστος ΑΛΕΞΙΟΥ MD, PhD, FRCS(Glasgow), FRCS(CTh), CCST(UK) Consultant Cardiothoracic Surgeon Normal Mitral Valve Function Mitral Regurgitation
The Key Questions in Mitral Valve Interventions. Where Are We in 2018?
 The Key Questions in Mitral Valve Interventions Where Are We in 2018? Gilles D. DREYFUS, MD, FRCS, FESC Professor of Cardiothoracic Surgery 30 GIORNATE CARDIOLOGICHE TORINESI - OCT 2018 Are guidelines
The Key Questions in Mitral Valve Interventions Where Are We in 2018? Gilles D. DREYFUS, MD, FRCS, FESC Professor of Cardiothoracic Surgery 30 GIORNATE CARDIOLOGICHE TORINESI - OCT 2018 Are guidelines
Effect of anterior strut chordal transection on the force distribution on the marginal chordae of the mitral valve
 Acquired Cardiovascular Disease Padala et al Effect of anterior strut chordal transection on the force distribution on the marginal chordae of the mitral valve Muralidhar Padala, PhD, a Lazarina Gyoneva,
Acquired Cardiovascular Disease Padala et al Effect of anterior strut chordal transection on the force distribution on the marginal chordae of the mitral valve Muralidhar Padala, PhD, a Lazarina Gyoneva,
Mitral Valve Repair for Functional Mitral Regurgitation- Description of A New Technique and Classification System
 Case Report Mitral Valve Repair for Functional Mitral Regurgitation- Description of A New Technique and Classification System Antonio Chiricolo 1*, Leonard Y Lee 2 1 Department of Anesthesiology, Rutgers
Case Report Mitral Valve Repair for Functional Mitral Regurgitation- Description of A New Technique and Classification System Antonio Chiricolo 1*, Leonard Y Lee 2 1 Department of Anesthesiology, Rutgers
The clinical problem of atrioventricular valve regurgitation
 Mitral Regurgitation in Congenital Heart Defects: Surgical Techniques for Reconstruction Richard G. Ohye Mitral valve regurgitation (MR) is an important source of morbidity and mortality worldwide. While
Mitral Regurgitation in Congenital Heart Defects: Surgical Techniques for Reconstruction Richard G. Ohye Mitral valve regurgitation (MR) is an important source of morbidity and mortality worldwide. While
Echocardiographic Evaluation of Primary Mitral Regurgitation
 Echocardiographic Evaluation of Primary Mitral Regurgitation Roberto M Lang, MD 0-10 o ME 4CH Med A2 P2 50-70 o Commissural P3 P1 A2 80-100 o ME 2CH P3 A2 A1 A1 125-135 o - ME Long axis P2 A2 P3 A3 P2
Echocardiographic Evaluation of Primary Mitral Regurgitation Roberto M Lang, MD 0-10 o ME 4CH Med A2 P2 50-70 o Commissural P3 P1 A2 80-100 o ME 2CH P3 A2 A1 A1 125-135 o - ME Long axis P2 A2 P3 A3 P2
8/31/2016. Mitraclip in Matthew Johnson, MD
 Mitraclip in 2016 Matthew Johnson, MD 1 Abnormal Valve Function Valve Stenosis Obstruction to valve flow during that phase of the cardiac cycle when the valve is normally open. Hemodynamic hallmark - pressure
Mitraclip in 2016 Matthew Johnson, MD 1 Abnormal Valve Function Valve Stenosis Obstruction to valve flow during that phase of the cardiac cycle when the valve is normally open. Hemodynamic hallmark - pressure
Tricuspid leaflet repair: innovative solutions
 Perspective Tricuspid leaflet repair: innovative solutions Jack H. Boyd 1, J. James B. Edelman 2, David H. Scoville 1, Y. Joseph Woo 1 1 Department of Cardiothoracic Surgery, Stanford University School
Perspective Tricuspid leaflet repair: innovative solutions Jack H. Boyd 1, J. James B. Edelman 2, David H. Scoville 1, Y. Joseph Woo 1 1 Department of Cardiothoracic Surgery, Stanford University School
There is increasing acceptance of the value of reconstructing
 Fleur de Lys Repair of Posterior Mitral Valve Leaflet Richard A. Hopkins, MD There is increasing acceptance of the value of reconstructing mitral valves and retaining the various components of the mitral
Fleur de Lys Repair of Posterior Mitral Valve Leaflet Richard A. Hopkins, MD There is increasing acceptance of the value of reconstructing mitral valves and retaining the various components of the mitral
Degenerative mitral valve disease is the leading cause of
 Recurrence of Mitral Valve Regurgitation After Mitral Valve Repair in Degenerative Valve Disease Willem Flameng, MD, PhD; Paul Herijgers, MD, PhD; Kris Bogaerts, MSc Background Durability assessment of
Recurrence of Mitral Valve Regurgitation After Mitral Valve Repair in Degenerative Valve Disease Willem Flameng, MD, PhD; Paul Herijgers, MD, PhD; Kris Bogaerts, MSc Background Durability assessment of
Choosing the Right Treatment for Primary Mitral Regurgitation ΓΡΗΓΟΡΙΟΣ ΠΑΤΤΑΚΟΣ, MD, MS Καρδιοχειρουργός Β Κ/Χ Κλινικής Αναπλ. Διευθ.
 Choosing the Right Treatment for Primary Mitral Regurgitation ΓΡΗΓΟΡΙΟΣ ΠΑΤΤΑΚΟΣ, MD, MS Καρδιοχειρουργός Β Κ/Χ Κλινικής Αναπλ. Διευθ. Διαδερμικών Βαλβίδων Δ.Θ.Κ.Α. «ΥΓΕΙΑ» Mitral Regurgitation Very common
Choosing the Right Treatment for Primary Mitral Regurgitation ΓΡΗΓΟΡΙΟΣ ΠΑΤΤΑΚΟΣ, MD, MS Καρδιοχειρουργός Β Κ/Χ Κλινικής Αναπλ. Διευθ. Διαδερμικών Βαλβίδων Δ.Θ.Κ.Α. «ΥΓΕΙΑ» Mitral Regurgitation Very common
Disclosure Statement of Financial Interest Saibal Kar, MD, FACC
 MitraClip Therapy Saibal Kar, MD, FACC, FAHA, FSCAI Director of Interventional Cardiac Research Program Director, Interventional Cardiology Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA
MitraClip Therapy Saibal Kar, MD, FACC, FAHA, FSCAI Director of Interventional Cardiac Research Program Director, Interventional Cardiology Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA
Atrioventricular valve repair: The limits of operability
 Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Ischemic mitral regurgitation (IMR) is an insufficiency of
 Repair Techniques for Ischemic Mitral Regurgitation Damien J. LaPar, MD, MSc, and Irving L. Kron, MD Ischemic mitral regurgitation (IMR) is an insufficiency of the mitral valve (MV) secondary to myocardial
Repair Techniques for Ischemic Mitral Regurgitation Damien J. LaPar, MD, MSc, and Irving L. Kron, MD Ischemic mitral regurgitation (IMR) is an insufficiency of the mitral valve (MV) secondary to myocardial
Historical perspective R1 黃維立
 Degenerative mitral valve disease refers to a spectrum of conditions in which morphologic changes in the connective tissue of the mitral valve cause structural lesions that prevent normal function of the
Degenerative mitral valve disease refers to a spectrum of conditions in which morphologic changes in the connective tissue of the mitral valve cause structural lesions that prevent normal function of the
MEMO 4D Reshaping Mitral Repair
 MEMO 4D Reshaping Mitral Repair Designed to Best Support Your Technique MEMO 4D Reshaping Mitral Repair Innovation Starts at the Core Designed to Best Support Your Technique ReChord: Chordal Guide System
MEMO 4D Reshaping Mitral Repair Designed to Best Support Your Technique MEMO 4D Reshaping Mitral Repair Innovation Starts at the Core Designed to Best Support Your Technique ReChord: Chordal Guide System
Valve Repair for Mitral Regurgitation Caused by Isolated Prolapse of the Posterior Leaflet
 Valve Repair for Mitral Regurgitation Caused by Isolated Prolapse of the Posterior Leaflet Patrick Perier, MD, J/2rgen Stumpf, MD, Christian GStz, MD, Fitsoum Lakew, MD, Andr6 Schneider, MD, Bernd Clausnizer,
Valve Repair for Mitral Regurgitation Caused by Isolated Prolapse of the Posterior Leaflet Patrick Perier, MD, J/2rgen Stumpf, MD, Christian GStz, MD, Fitsoum Lakew, MD, Andr6 Schneider, MD, Bernd Clausnizer,
Overview of Surgical Approach to Mitral Valve Disease : Why Repair? Steven F. Bolling, MD Cardiac Surgery University of Michigan
 Overview of Surgical Approach to Mitral Valve Disease : Why Repair? Steven F. Bolling, MD Cardiac Surgery University of Michigan Degenerative MR is not Functional MR 2o - Functional MR : Ventricular Problem!!
Overview of Surgical Approach to Mitral Valve Disease : Why Repair? Steven F. Bolling, MD Cardiac Surgery University of Michigan Degenerative MR is not Functional MR 2o - Functional MR : Ventricular Problem!!
Rheumatic fever and rheumatic heart disease still remain a. The Rheumatic Mitral Valve and Repair Techniques in Children. Afksendiyos Kalangos
 The Rheumatic Mitral Valve and Repair Techniques in Children Afksendiyos Kalangos The mitral valve is the most commonly affected valve in acute and chronic rheumatic heart disease in the first and second
The Rheumatic Mitral Valve and Repair Techniques in Children Afksendiyos Kalangos The mitral valve is the most commonly affected valve in acute and chronic rheumatic heart disease in the first and second
Treatment of Ruptured or Elon ated Anterior Mitral Valve Chordae bv Parti 3 Transposition of the Posterior Leaflet: Experience with 29 Patients
 Treatment of Ruptured or Elon ated Anterior Mitral Valve Chordae bv Parti 3 Transposition of the Posterior Leaflet: Experience with 29 Patients Arrigo Lessana, M.D., Mauro Romano, M.D., Genevieve Lutfalla,
Treatment of Ruptured or Elon ated Anterior Mitral Valve Chordae bv Parti 3 Transposition of the Posterior Leaflet: Experience with 29 Patients Arrigo Lessana, M.D., Mauro Romano, M.D., Genevieve Lutfalla,
Cases of mitral valve causing mitral regurgitation: the MV prolapse spectrum CASE
 Cases of mitral valve causing mitral regurgitation: the MV prolapse spectrum Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA CASE Mr. M; 50 Year male presents to internist for
Cases of mitral valve causing mitral regurgitation: the MV prolapse spectrum Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA CASE Mr. M; 50 Year male presents to internist for
Myxomatous degeneration of the mitral valve is the
 CARDIOVASCULAR Midterm Results of the Edge-to-Edge Technique for Complex Mitral Valve Repair Derek R. Brinster, MD, Daniel Unic, MD, Michael N. D Ambra, MD, Nadia Nathan, MD, and Lawrence H. Cohn, MD Division
CARDIOVASCULAR Midterm Results of the Edge-to-Edge Technique for Complex Mitral Valve Repair Derek R. Brinster, MD, Daniel Unic, MD, Michael N. D Ambra, MD, Nadia Nathan, MD, and Lawrence H. Cohn, MD Division
Long term outcomes of posterior leaflet folding valvuloplasty for mitral valve regurgitation
 Featured Article Long term outcomes of posterior leaflet folding valvuloplasty for mitral valve regurgitation Igor Gosev 1, Maroun Yammine 1, Marzia Leacche 1, Siobhan McGurk 1, Vladimir Ivkovic 1, Michael
Featured Article Long term outcomes of posterior leaflet folding valvuloplasty for mitral valve regurgitation Igor Gosev 1, Maroun Yammine 1, Marzia Leacche 1, Siobhan McGurk 1, Vladimir Ivkovic 1, Michael
Professor and Chief, Division of Cardiac Surgery Chief Medical Officer, Harpoon Medical. The Houston Aortic Symposium February 23-25, 2017
 James S. Gammie, MD Professor and Chief, Division of Cardiac Surgery Chief Medical Officer, Harpoon Medical The Houston Aortic Symposium February 2-25, 2017 Disclosure Statement of Financial Interest Within
James S. Gammie, MD Professor and Chief, Division of Cardiac Surgery Chief Medical Officer, Harpoon Medical The Houston Aortic Symposium February 2-25, 2017 Disclosure Statement of Financial Interest Within
Minimally invasive valve sparing mitral valve repair the loop technique how we do it
 Art of Operative Techniques Minimally invasive valve sparing mitral valve repair the loop technique how we do it Stephan Jacobs, Simon H. Sündermann Division of Cardiovascular Surgery, University Hospital
Art of Operative Techniques Minimally invasive valve sparing mitral valve repair the loop technique how we do it Stephan Jacobs, Simon H. Sündermann Division of Cardiovascular Surgery, University Hospital
MEMO 3D. The true reflection of the mitral annulus. Natural physiological 3D motion
 MEMO 3D TM The true reflection of the mitral annulus Natural physiological 3D motion Imagine... if there was one annuloplasty ring that provided an optimal solution across the entire spectrum of mitral
MEMO 3D TM The true reflection of the mitral annulus Natural physiological 3D motion Imagine... if there was one annuloplasty ring that provided an optimal solution across the entire spectrum of mitral
Regurgitant Lesions. Bicol Hospital, Legazpi City, Philippines July Gregg S. Pressman MD, FACC, FASE Einstein Medical Center Philadelphia, USA
 Regurgitant Lesions Bicol Hospital, Legazpi City, Philippines July 2016 Gregg S. Pressman MD, FACC, FASE Einstein Medical Center Philadelphia, USA Aortic Insufficiency Valve anatomy and function LVOT and
Regurgitant Lesions Bicol Hospital, Legazpi City, Philippines July 2016 Gregg S. Pressman MD, FACC, FASE Einstein Medical Center Philadelphia, USA Aortic Insufficiency Valve anatomy and function LVOT and
Mitral valve repair is the gold standard to treat mitral regurgitation.
 Papillary muscle repositioning for repair of anterior leaflet prolapse caused by chordal elongation Gilles D. Dreyfus, MD, PhD, FRCS, Olivio Souza Neto, MD, and Stéphane Aubert, MD, MSc Objective: Anterior
Papillary muscle repositioning for repair of anterior leaflet prolapse caused by chordal elongation Gilles D. Dreyfus, MD, PhD, FRCS, Olivio Souza Neto, MD, and Stéphane Aubert, MD, MSc Objective: Anterior
Percutaneous Mitral Valve Repair
 Indiana Chapter of ACC November 15 th,2008 Percutaneous Mitral Valve Repair James B Hermiller, MD, FACC The Care Group, LLC St Vincent Hospital Indianapolis, IN Mechanisms of Mitral Regurgitation Mitral
Indiana Chapter of ACC November 15 th,2008 Percutaneous Mitral Valve Repair James B Hermiller, MD, FACC The Care Group, LLC St Vincent Hospital Indianapolis, IN Mechanisms of Mitral Regurgitation Mitral
Surgical repair techniques for IMR: future percutaneous options?
 Surgical repair techniques for IMR: can this teach us about future percutaneous options? Genk - Belgium Prof. Dr. R. Dion KULeu Disclosure slide Robert A. Dion I disclose the following financial relationships:
Surgical repair techniques for IMR: can this teach us about future percutaneous options? Genk - Belgium Prof. Dr. R. Dion KULeu Disclosure slide Robert A. Dion I disclose the following financial relationships:
Long-Term Assessment of Mitral Valve Reconstruction With Resection of the Leaflets: Triangular and Quadrangular Resection
 Long-Term Assessment of Mitral Valve Reconstruction With Resection of the Leaflets: Triangular and Quadrangular Resection Yoshimasa Sakamoto, MD, Kazuhiro Hashimoto, MD, Hiroshi Okuyama, MD, Shinichi Ishii,
Long-Term Assessment of Mitral Valve Reconstruction With Resection of the Leaflets: Triangular and Quadrangular Resection Yoshimasa Sakamoto, MD, Kazuhiro Hashimoto, MD, Hiroshi Okuyama, MD, Shinichi Ishii,
The correlation between the coaptation height of mitral valve and mitral regurgitation after mitral valve repair
 Wei et al. Journal of Cardiothoracic Surgery (2017) 12:120 DOI 10.1186/s13019-017-0687-0 RESEARCH ARTICLE Open Access The correlation between the coaptation height of mitral valve and mitral regurgitation
Wei et al. Journal of Cardiothoracic Surgery (2017) 12:120 DOI 10.1186/s13019-017-0687-0 RESEARCH ARTICLE Open Access The correlation between the coaptation height of mitral valve and mitral regurgitation
ISCHEMIC/FUNCTIONAL MR
 ISCHEMIC/FUNCTIONAL MR Mitral valve annuloplasty and papillary muscle relocation oriented by 3-dimensional transesophageal echocardiography for severe functional mitral regurgitation Khalil Fattouch, MD,
ISCHEMIC/FUNCTIONAL MR Mitral valve annuloplasty and papillary muscle relocation oriented by 3-dimensional transesophageal echocardiography for severe functional mitral regurgitation Khalil Fattouch, MD,
A near 100% repair rate for mitral valve prolapse is achievable in a reference center: Implications for future guidelines
 A near 100% repair rate for mitral valve prolapse is achievable in a reference center: Implications for future guidelines Javier G. Castillo, MD, Anelechi C. Anyanwu, MD, Valentin Fuster, MD, PhD, and
A near 100% repair rate for mitral valve prolapse is achievable in a reference center: Implications for future guidelines Javier G. Castillo, MD, Anelechi C. Anyanwu, MD, Valentin Fuster, MD, PhD, and
Management of Incomplete Initial Repair in the Treatment of Degenerative Mitral Insufficiency An Institutional Protocol and Mid-Term Outcomes
 CLINICAL STUDY Management of Incomplete Initial Repair in the Treatment of Degenerative Mitral Insufficiency An Institutional Protocol and Mid-Term Outcomes Wenrui Ma, 1 MD, Wei Shi, 1 MD, Wei Zhang, 1
CLINICAL STUDY Management of Incomplete Initial Repair in the Treatment of Degenerative Mitral Insufficiency An Institutional Protocol and Mid-Term Outcomes Wenrui Ma, 1 MD, Wei Shi, 1 MD, Wei Zhang, 1
Recurrent mitral regurgitation after repair: Should the mitral valve be re-repaired?
 Surgery for Acquired Cardiovascular Disease Recurrent mitral regurgitation after repair: Should the mitral valve be re-repaired? Rakesh M. Suri, MD, DPhil, Hartzell V. Schaff, MD, Joseph A. Dearani, MD,
Surgery for Acquired Cardiovascular Disease Recurrent mitral regurgitation after repair: Should the mitral valve be re-repaired? Rakesh M. Suri, MD, DPhil, Hartzell V. Schaff, MD, Joseph A. Dearani, MD,
Aortic valve repair: Techniques and Pitfalls. Allan Stewart, MD Columbia University Medical Center New York, NY
 Aortic valve repair: Techniques and Pitfalls Allan Stewart, MD Columbia University Medical Center New York, NY Take Away Points 1. Valve anatomy is essential to assess repair 2. Unique Decisions with Aneurysm/AI
Aortic valve repair: Techniques and Pitfalls Allan Stewart, MD Columbia University Medical Center New York, NY Take Away Points 1. Valve anatomy is essential to assess repair 2. Unique Decisions with Aneurysm/AI
Percutaneous mitral annuloplasty. Francesco Maisano MD, FESC San Raffaele Hospital Milano, Italy
 Percutaneous mitral annuloplasty Francesco Maisano MD, FESC San Raffaele Hospital Milano, Italy Disclosure Consultant for Abbott, Medtronic, St Jude, Edwards, ValtechCardio Founder of 4Tech Surgical techniques
Percutaneous mitral annuloplasty Francesco Maisano MD, FESC San Raffaele Hospital Milano, Italy Disclosure Consultant for Abbott, Medtronic, St Jude, Edwards, ValtechCardio Founder of 4Tech Surgical techniques
3D Printing & Echocardiography
 ASE SOTA Feb 19, 2018 3D Printing & Echocardiography Stephen H. Little, MD John S. Dunn Chair in Cardiovascular Research and Education, Associate professor, Weill Cornell Medicine Disclosures Personal
ASE SOTA Feb 19, 2018 3D Printing & Echocardiography Stephen H. Little, MD John S. Dunn Chair in Cardiovascular Research and Education, Associate professor, Weill Cornell Medicine Disclosures Personal
Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention
 Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention John N. Hamaty D.O. FACC, FACOI November 17 th 2017 I have no financial disclosures Primary Mitral
Degenerative Mitral Regurgitation: Etiology and Natural History of Disease and Triggers for Intervention John N. Hamaty D.O. FACC, FACOI November 17 th 2017 I have no financial disclosures Primary Mitral
MEMO 3D RECHORD. Ready to repair. Guiding standards in Mitral valve repair
 MEMO 3D RECHORD TM Ready to repair Guiding standards in Mitral valve repair CARDIAC SURGERY SOLUTIONS A 45-year long history of innovative records in cardiac surgery LivaNova s relentless commitment to
MEMO 3D RECHORD TM Ready to repair Guiding standards in Mitral valve repair CARDIAC SURGERY SOLUTIONS A 45-year long history of innovative records in cardiac surgery LivaNova s relentless commitment to
Late secondary TR after left sided heart disease correction: is it predictibale and preventable
 Late secondary TR after left sided heart disease correction: is it predictibale and preventable Gilles D. Dreyfus Professor of Cardiothoracic surgery Nath J, et al. JACC 2004 PREDICT Incidence of secondary
Late secondary TR after left sided heart disease correction: is it predictibale and preventable Gilles D. Dreyfus Professor of Cardiothoracic surgery Nath J, et al. JACC 2004 PREDICT Incidence of secondary
Degenerative mitral valve disease is now the most common
 Triangular Resection for Repair of Mitral Regurgitation Due to Degenerative Disease Rakesh M. Suri, MD, DPhil, FRCS(C), and Thomas A. Orszulak, MD, FACC Degenerative mitral valve disease is now the most
Triangular Resection for Repair of Mitral Regurgitation Due to Degenerative Disease Rakesh M. Suri, MD, DPhil, FRCS(C), and Thomas A. Orszulak, MD, FACC Degenerative mitral valve disease is now the most
Transoesophageal Echocardiographic Evaluation of the Mitral Valve
 10.5005/jp-journals-10027-1018 REVIEW ARTICLE IJPUT Transoesophageal Echocardiographic Evaluation of the Mitral Valve Gary Lau, Ravi Hebballi ABSTRACT Transoesophageal echocardiography allows the precise
10.5005/jp-journals-10027-1018 REVIEW ARTICLE IJPUT Transoesophageal Echocardiographic Evaluation of the Mitral Valve Gary Lau, Ravi Hebballi ABSTRACT Transoesophageal echocardiography allows the precise
Part II: Fundamentals of 3D Echocardiography: Acquisition and Application
 Part II: Fundamentals of 3D Echocardiography: Acquisition and Application Dr. Bruce Bollen 3D matrix array TEE probes provide options for both 2D and 3D imaging. Indeed, their utility in obtaining multiple
Part II: Fundamentals of 3D Echocardiography: Acquisition and Application Dr. Bruce Bollen 3D matrix array TEE probes provide options for both 2D and 3D imaging. Indeed, their utility in obtaining multiple
MITRAL REGURGITATION ECHO PARAMETERS TOOL
 Comprehensive assessment of qualitative and quantitative parameters, along with the use of standardized nomenclature when reporting echocardiographic findings, helps to better define a patient s MR and
Comprehensive assessment of qualitative and quantitative parameters, along with the use of standardized nomenclature when reporting echocardiographic findings, helps to better define a patient s MR and
Transcatheter Mitral Valve Replacement How Close Are We?
 Transcatheter Mitral Valve Replacement How Close Are We? Gregory Pavlides, MD, PhD, FACC, FESC Professor of Medicine Miscia Chair of Interventional Cardiology Director, Cardiac Catheterization Laboratories,
Transcatheter Mitral Valve Replacement How Close Are We? Gregory Pavlides, MD, PhD, FACC, FESC Professor of Medicine Miscia Chair of Interventional Cardiology Director, Cardiac Catheterization Laboratories,
Cardiac ultrasound protocols
 Cardiac ultrasound protocols IDEXX Telemedicine Consultants Two-dimensional and M-mode imaging planes Right parasternal long axis four chamber Obtained from the right side Displays the relative proportions
Cardiac ultrasound protocols IDEXX Telemedicine Consultants Two-dimensional and M-mode imaging planes Right parasternal long axis four chamber Obtained from the right side Displays the relative proportions
Annular Stabilization Techniques in the Context of Aortic Valve Repair
 Annular Stabilization Techniques in the Context of Aortic Valve Repair Prashanth Vallabhajosyula, MD MS University of Pennsylvania, Philadelphia, Pennsylvania 2 nd North American Aortic Valve Repair Symposium
Annular Stabilization Techniques in the Context of Aortic Valve Repair Prashanth Vallabhajosyula, MD MS University of Pennsylvania, Philadelphia, Pennsylvania 2 nd North American Aortic Valve Repair Symposium
MitraClip in the ICCU: Which Patient will Benefit?
 MitraClip in the ICCU: Which Patient will Benefit? DAVID MEERKIN STRUCTURAL A ND CONGENITAL HEART DISEASE UNIT SHAARE ZEDEK MEDICAL CENTER JERUSALEM Conflict of Interest No relevant disclosures Complex
MitraClip in the ICCU: Which Patient will Benefit? DAVID MEERKIN STRUCTURAL A ND CONGENITAL HEART DISEASE UNIT SHAARE ZEDEK MEDICAL CENTER JERUSALEM Conflict of Interest No relevant disclosures Complex
ready to repair product brochure PERFORMANCE INNOVATION DESIGN mitral solutions
 ready to repair PERFORMANCE INNOVATION DESIGN mitral solutions product brochure a 45-year long history of innovative records in cardiac surgery Carbofilm Sorin Group's relentless commitment to providing
ready to repair PERFORMANCE INNOVATION DESIGN mitral solutions product brochure a 45-year long history of innovative records in cardiac surgery Carbofilm Sorin Group's relentless commitment to providing
DEVELOPMENT OF A CRYO-ANCHORING AND RADIOFREQUENCY ABLATION CATHETER FOR PERCUTANEOUS TREATMENT OF MITRAL VALVE PROLAPSE. Steven Michael Boronyak
 DEVELOPMENT OF A CRYO-ANCHORING AND RADIOFREQUENCY ABLATION CATHETER FOR PERCUTANEOUS TREATMENT OF MITRAL VALVE PROLAPSE By Steven Michael Boronyak Dissertation Submitted to the Faculty of the Graduate
DEVELOPMENT OF A CRYO-ANCHORING AND RADIOFREQUENCY ABLATION CATHETER FOR PERCUTANEOUS TREATMENT OF MITRAL VALVE PROLAPSE By Steven Michael Boronyak Dissertation Submitted to the Faculty of the Graduate
Eva Maria Delmo Walter Takeshi Komoda Roland Hetzer
 Surgical repair of the congenitally malformed mitral valve leaflets in infants and children Eva Maria Delmo Walter Takeshi Komoda Roland Hetzer Deutsches Herzzentrum Berlin Germany Background and Objective
Surgical repair of the congenitally malformed mitral valve leaflets in infants and children Eva Maria Delmo Walter Takeshi Komoda Roland Hetzer Deutsches Herzzentrum Berlin Germany Background and Objective
Outline. EuroScore II. Society of Thoracic Surgeons Score. EuroScore II
 SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
Comparison of outcomes of minimally invasive mitral valve surgery for posterior, anterior and bileaflet prolapse
 European Journal of Cardio-thoracic Surgery 36 (2009) 532 538 www.elsevier.com/locate/ejcts Comparison of outcomes of minimally invasive mitral valve surgery for posterior, anterior and bileaflet prolapse
European Journal of Cardio-thoracic Surgery 36 (2009) 532 538 www.elsevier.com/locate/ejcts Comparison of outcomes of minimally invasive mitral valve surgery for posterior, anterior and bileaflet prolapse
A new era in cardiac valve surgery has begun...
 THE CENTER FOR VALVE SURGERY A new era in cardiac valve surgery has begun... Good Help to Those in Need Rawn Salenger, MD, FACS, Director, The Center for Valve Surgery Edward F. Lundy, MD, PhD, Chief of
THE CENTER FOR VALVE SURGERY A new era in cardiac valve surgery has begun... Good Help to Those in Need Rawn Salenger, MD, FACS, Director, The Center for Valve Surgery Edward F. Lundy, MD, PhD, Chief of
Bulging Subaortic Septum: An Important Risk Factor for Systolic Anterior Motion After Mitral Valve Repair
 Bulging Subaortic Septum: An Important Risk Factor for Systolic Anterior Motion After Mitral Valve Repair Sameh M. Said, MD, Hartzell V. Schaff, MD, Rakesh M. Suri, MD, DPhil, Kevin L. Greason, MD, Joseph
Bulging Subaortic Septum: An Important Risk Factor for Systolic Anterior Motion After Mitral Valve Repair Sameh M. Said, MD, Hartzell V. Schaff, MD, Rakesh M. Suri, MD, DPhil, Kevin L. Greason, MD, Joseph
3D Printing & Echocardiography
 Echo Hawaii Jan 18, 2018 3D Printing & Echocardiography Stephen H. Little, MD John S. Dunn Chair in Cardiovascular Research and Education, Associate professor, Weill Cornell Medicine Rapid Prototyping
Echo Hawaii Jan 18, 2018 3D Printing & Echocardiography Stephen H. Little, MD John S. Dunn Chair in Cardiovascular Research and Education, Associate professor, Weill Cornell Medicine Rapid Prototyping
Surgery For Ebstein Anomaly
 Surgery For Ebstein Anomaly Christian Pizarro, MD Chief, Pediatric Cardiothoracic Surgery Director, Nemours Cardiac Center Alfred I. dupont Hospital for Children Professor of Surgery and Pediatrics Sidney
Surgery For Ebstein Anomaly Christian Pizarro, MD Chief, Pediatric Cardiothoracic Surgery Director, Nemours Cardiac Center Alfred I. dupont Hospital for Children Professor of Surgery and Pediatrics Sidney
Basic principles of Rheumatic mitral valve Repair
 Basic principles of Rheumatic mitral valve Repair Prof. Gebrine El Khoury, MD DEPARTMENT OF CARDIOVASCULAR AND THORACIC SURGERY ST. LUC HOSPITAL - BRUSSELS, BELGIUM 1 Rheumatic MV disease MV repair confers
Basic principles of Rheumatic mitral valve Repair Prof. Gebrine El Khoury, MD DEPARTMENT OF CARDIOVASCULAR AND THORACIC SURGERY ST. LUC HOSPITAL - BRUSSELS, BELGIUM 1 Rheumatic MV disease MV repair confers
When should we intervene surgically in pediatric patient with MR?
 When should we intervene surgically in pediatric patient with MR? DR.SAUD A. BAHAIDARAH CONSULTANT, PEDIATRIC CARDIOLOGY ASSISTANT PROFESSOR OF PEDIATRICS HEAD OF CARDIOLOGY AND CARDIAC SURGERY UNIT KAUH
When should we intervene surgically in pediatric patient with MR? DR.SAUD A. BAHAIDARAH CONSULTANT, PEDIATRIC CARDIOLOGY ASSISTANT PROFESSOR OF PEDIATRICS HEAD OF CARDIOLOGY AND CARDIAC SURGERY UNIT KAUH
Indications and Late Results of Aortic Valve Repair
 Indications and Late Results of Aortic Valve Repair Prof. Gebrine El Khoury Department of Cardiovascular and Thoracic Surgery Cliniques St. Luc Brussels, Belgium Aortic Valve Repair Question # 1 Can the
Indications and Late Results of Aortic Valve Repair Prof. Gebrine El Khoury Department of Cardiovascular and Thoracic Surgery Cliniques St. Luc Brussels, Belgium Aortic Valve Repair Question # 1 Can the
ΔΙΑΔΕΡΜΙΚΗ ΑΝΤΙΜΕΤΩΠΙΣΗ ΔΟΜΙΚΩΝ ΠΑΘΗΣΕΩΝ: Ο ΡΟΛΟΣ ΤΗΣ ΑΠΕΙΚΟΝΙΣΗΣ ΣΤΟ ΑΙΜΟΔΥΝΑΜΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΣΤΗΝ ΤΟΠΟΘΕΤΗΣΗ MITRACLIP
 ΔΙΑΔΕΡΜΙΚΗ ΑΝΤΙΜΕΤΩΠΙΣΗ ΔΟΜΙΚΩΝ ΠΑΘΗΣΕΩΝ: Ο ΡΟΛΟΣ ΤΗΣ ΑΠΕΙΚΟΝΙΣΗΣ ΣΤΟ ΑΙΜΟΔΥΝΑΜΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΣΤΗΝ ΤΟΠΟΘΕΤΗΣΗ MITRACLIP ΒΛΑΣΗΣ ΝΙΝΙΟΣ MD MRCP ΚΛΙΝΙΚΗ ΑΓΙΟΣ ΛΟΥΚΑΣ ΘΕΣΣΑΛΟΝΙΚΗ CONFLICT OF INTEREST PROCTOR
ΔΙΑΔΕΡΜΙΚΗ ΑΝΤΙΜΕΤΩΠΙΣΗ ΔΟΜΙΚΩΝ ΠΑΘΗΣΕΩΝ: Ο ΡΟΛΟΣ ΤΗΣ ΑΠΕΙΚΟΝΙΣΗΣ ΣΤΟ ΑΙΜΟΔΥΝΑΜΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΣΤΗΝ ΤΟΠΟΘΕΤΗΣΗ MITRACLIP ΒΛΑΣΗΣ ΝΙΝΙΟΣ MD MRCP ΚΛΙΝΙΚΗ ΑΓΙΟΣ ΛΟΥΚΑΣ ΘΕΣΣΑΛΟΝΙΚΗ CONFLICT OF INTEREST PROCTOR
Percutaneous mitral valve repair/replacement. Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein
 Percutaneous mitral valve repair/replacement Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein Mitral Valve anatomy Difference between AoV and MV Aortic Valve Mitral Valve Transcatheter Mitral
Percutaneous mitral valve repair/replacement Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein Mitral Valve anatomy Difference between AoV and MV Aortic Valve Mitral Valve Transcatheter Mitral
The need for right ventricular outflow tract reconstruction
 Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Repair of Mitral Valve Prolapse with a Novel Leaflet Plication Clip in an Animal Model
 Repair of Mitral Valve Prolapse with a Novel Leaflet Plication Clip in an Animal Model Eric N. Feins 1, Haruo Yamauchi 1, Gerald R. Marx 2, Franz P. Freudenthal 3, Hua Liu 1, Pedro J. del Nido 1, Nikolay
Repair of Mitral Valve Prolapse with a Novel Leaflet Plication Clip in an Animal Model Eric N. Feins 1, Haruo Yamauchi 1, Gerald R. Marx 2, Franz P. Freudenthal 3, Hua Liu 1, Pedro J. del Nido 1, Nikolay
Ο ΡΟΛΟΣ ΤΩΝ ΚΟΛΠΩΝ ΣΤΗ ΛΕΙΤΟΥΡΓΙΚΗ ΑΝΕΠΑΡΚΕΙΑ ΤΩΝ ΚΟΛΠΟΚΟΙΛΙΑΚΩΝ ΒΑΛΒΙΔΩΝ
 Ο ΡΟΛΟΣ ΤΩΝ ΚΟΛΠΩΝ ΣΤΗ ΛΕΙΤΟΥΡΓΙΚΗ ΑΝΕΠΑΡΚΕΙΑ ΤΩΝ ΚΟΛΠΟΚΟΙΛΙΑΚΩΝ ΒΑΛΒΙΔΩΝ Ανδρέας Κατσαρός Καρδιολόγος Επιµ. Α Καρδιοχειρ/κών Τµηµάτων Γ.Ν.Α. Ιπποκράτειο ΚΑΜΙΑ ΣΥΓΚΡΟΥΣΗ ΣΥΜΦΕΡΟΝΤΩΝ ΑΝΑΦΟΡΙΚΑ ΜΕ ΤΗΝ ΠΑΡΟΥΣΙΑΣΗ
Ο ΡΟΛΟΣ ΤΩΝ ΚΟΛΠΩΝ ΣΤΗ ΛΕΙΤΟΥΡΓΙΚΗ ΑΝΕΠΑΡΚΕΙΑ ΤΩΝ ΚΟΛΠΟΚΟΙΛΙΑΚΩΝ ΒΑΛΒΙΔΩΝ Ανδρέας Κατσαρός Καρδιολόγος Επιµ. Α Καρδιοχειρ/κών Τµηµάτων Γ.Ν.Α. Ιπποκράτειο ΚΑΜΙΑ ΣΥΓΚΡΟΥΣΗ ΣΥΜΦΕΡΟΝΤΩΝ ΑΝΑΦΟΡΙΚΑ ΜΕ ΤΗΝ ΠΑΡΟΥΣΙΑΣΗ
Correction of anterior mitral prolapse: The parachute technique
 Correction of anterior mitral prolapse: The parachute technique Konstantinos Zannis, MD, a Laurens Mitchell-Heggs, MD, a Valentina Di Nitto, MD, a Matthias E. W. Kirsch, MD, PhD, b Milena Noghin, MD, a
Correction of anterior mitral prolapse: The parachute technique Konstantinos Zannis, MD, a Laurens Mitchell-Heggs, MD, a Valentina Di Nitto, MD, a Matthias E. W. Kirsch, MD, PhD, b Milena Noghin, MD, a
CHAPTER 34 LEFT VENTRICULAR FLOW 34-1
 CHAPTER 34 LEFT VENTRICULAR FLOW 34-1 CHAPTER 34 LEFT VENTRICULAR FLOW In Chapter 05 we studied the relationship of anterior leaflet shape to left ventricular pressure and flow from mid-diastole through
CHAPTER 34 LEFT VENTRICULAR FLOW 34-1 CHAPTER 34 LEFT VENTRICULAR FLOW In Chapter 05 we studied the relationship of anterior leaflet shape to left ventricular pressure and flow from mid-diastole through
Quality Outcomes Mitral Valve Repair
 Quality Outcomes Mitral Valve Repair Moving Beyond Reoperation Rakesh M. Suri, D.Phil. Professor of Surgery 2015 MFMER 3431548-1 Disclosure Mayo Clinic Division of Cardiovascular Surgery Research funding
Quality Outcomes Mitral Valve Repair Moving Beyond Reoperation Rakesh M. Suri, D.Phil. Professor of Surgery 2015 MFMER 3431548-1 Disclosure Mayo Clinic Division of Cardiovascular Surgery Research funding
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis
 JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20135 holds various files of this Leiden University dissertation. Author: Braun, Jerry Title: Surgical treatment of functional mitral regurgitation Issue
Cover Page The handle http://hdl.handle.net/1887/20135 holds various files of this Leiden University dissertation. Author: Braun, Jerry Title: Surgical treatment of functional mitral regurgitation Issue
What is Ebstein Anomaly?
 Echocardiograpnhic Evaluation of : Definition, Detection and Determinants of Outcome P. W. O Leary, M.D. Division of Pediatric Cardiology Mayo Clinic No Conflicts to Disclose What is? Failure of the TV
Echocardiograpnhic Evaluation of : Definition, Detection and Determinants of Outcome P. W. O Leary, M.D. Division of Pediatric Cardiology Mayo Clinic No Conflicts to Disclose What is? Failure of the TV
MITRAL VALVE FORCE BALANCE: A QUANTITATIVE ASSESSMENT OF ANNULAR AND SUBVALVULAR FORCES
 MITRAL VALVE FORCE BALANCE: A QUANTITATIVE ASSESSMENT OF ANNULAR AND SUBVALVULAR FORCES A Dissertation Presented to The Academic Faculty by Andrew W. Siefert In Partial Fulfillment of the Requirements
MITRAL VALVE FORCE BALANCE: A QUANTITATIVE ASSESSMENT OF ANNULAR AND SUBVALVULAR FORCES A Dissertation Presented to The Academic Faculty by Andrew W. Siefert In Partial Fulfillment of the Requirements
Accepted Manuscript. A Bad Trade: Mitral Regurgitation for Mitral Stenosis and Atrial Fibrillation
 Accepted Manuscript A Bad Trade: Mitral Regurgitation for Mitral Stenosis and Atrial Fibrillation Marc Gillinov, MD, Per Wierup, MD, PhD, Stephanie Mick, MD PII: S0022-5223(18)32281-5 DOI: 10.1016/j.jtcvs.2018.08.036
Accepted Manuscript A Bad Trade: Mitral Regurgitation for Mitral Stenosis and Atrial Fibrillation Marc Gillinov, MD, Per Wierup, MD, PhD, Stephanie Mick, MD PII: S0022-5223(18)32281-5 DOI: 10.1016/j.jtcvs.2018.08.036
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgery for Valvular Heart Disease. Very Long-Term Survival and Durability of Mitral Valve Repair for Mitral Valve Prolapse
 Surgery for Valvular Heart Disease Very Long-Term Survival and Durability of Mitral Valve Repair for Mitral Valve Prolapse Dania Mohty, MD; Thomas A. Orszulak, MD; Hartzell V. Schaff, MD; Jean-Francois
Surgery for Valvular Heart Disease Very Long-Term Survival and Durability of Mitral Valve Repair for Mitral Valve Prolapse Dania Mohty, MD; Thomas A. Orszulak, MD; Hartzell V. Schaff, MD; Jean-Francois
Surgical Mininvasive Approach for Mitral Repair Prof. Mauro Rinaldi
 Surgical Mininvasive Approach for Mitral Repair Prof. Mauro Rinaldi SC Cardiochirurgia U Universita degli Studi di Torino PORT-ACCESS TECNIQUE Reduce surgical trauma Minimize disruption of the chest wall
Surgical Mininvasive Approach for Mitral Repair Prof. Mauro Rinaldi SC Cardiochirurgia U Universita degli Studi di Torino PORT-ACCESS TECNIQUE Reduce surgical trauma Minimize disruption of the chest wall
Evolution of the concept and practice of mitral valve repair
 Keynote Lecture Series Evolution of the concept and practice of mitral valve repair Lawrence H. Cohn 1, Vakhtang Tchantchaleishvili 1,2, Taufiek K. Rajab 1 1 Brigham and Women s Hospital, Harvard Medical
Keynote Lecture Series Evolution of the concept and practice of mitral valve repair Lawrence H. Cohn 1, Vakhtang Tchantchaleishvili 1,2, Taufiek K. Rajab 1 1 Brigham and Women s Hospital, Harvard Medical
CLIP ΜΙΤΡΟΕΙ ΟΥΣ: ΠΟΥ ΒΡΙΣΚΟΜΑΣΤΕ;
 CLIP ΜΙΤΡΟΕΙ ΟΥΣ: ΠΟΥ ΒΡΙΣΚΟΜΑΣΤΕ; Επιµορφωτικά Σεµινάρια Ειδικευοµένων Καρδιολογίας 7 Απριλίου 2012 M Chrissoheris MD FACC THV Department HYGEIA Hospital Degenerative MR (DMR) Usually refers to an anatomic
CLIP ΜΙΤΡΟΕΙ ΟΥΣ: ΠΟΥ ΒΡΙΣΚΟΜΑΣΤΕ; Επιµορφωτικά Σεµινάρια Ειδικευοµένων Καρδιολογίας 7 Απριλίου 2012 M Chrissoheris MD FACC THV Department HYGEIA Hospital Degenerative MR (DMR) Usually refers to an anatomic
New Technique for Aortic Valve Functional Annulus Reshaping Using a Handmade Prosthetic Ring
 New Technique for Aortic Valve Functional Annulus Reshaping Using a Handmade Prosthetic Ring Khalil Fattouch, MD, PhD, Roberta Sampognaro, MD, Giuseppe Speziale, MD, and Giovanni Ruvolo, MD Department
New Technique for Aortic Valve Functional Annulus Reshaping Using a Handmade Prosthetic Ring Khalil Fattouch, MD, PhD, Roberta Sampognaro, MD, Giuseppe Speziale, MD, and Giovanni Ruvolo, MD Department
Introduction. Aortic Valve. Outflow Tract and Aortic Valve Annulus
 Chapter 1: Surgical anatomy of the aortic and mitral valves Jordan RH Hoffman MD, David A. Fullerton MD, FACC University of Colorado School of Medicine, Department of Surgery, Division of Cardiothoracic
Chapter 1: Surgical anatomy of the aortic and mitral valves Jordan RH Hoffman MD, David A. Fullerton MD, FACC University of Colorado School of Medicine, Department of Surgery, Division of Cardiothoracic
Quantitation of Mitral Valve Tenting in Ischemic Mitral Regurgitation by Transthoracic Real-Time Three-Dimensional Echocardiography
 Journal of the American College of Cardiology Vol. 45, No. 5, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.048
Journal of the American College of Cardiology Vol. 45, No. 5, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.048
Imaging to select patients for Transcatheter TV
 Imaging to select patients for Transcatheter TV Jeroen J Bax Dept of Cardiology Leiden Univ Medical Center The Netherlands San Diego, february 2018 Research grants: Medtronic, Biotronik, Boston Scientific,
Imaging to select patients for Transcatheter TV Jeroen J Bax Dept of Cardiology Leiden Univ Medical Center The Netherlands San Diego, february 2018 Research grants: Medtronic, Biotronik, Boston Scientific,
Aortic valve repair is a technique that is gaining popularity
 Aortic Valve Repair in Children, Including Pericardial Patch Reconstruction Aditya K. Kaza, MD,* and John A. Hawkins, MD Aortic valve repair is a technique that is gaining popularity in children because
Aortic Valve Repair in Children, Including Pericardial Patch Reconstruction Aditya K. Kaza, MD,* and John A. Hawkins, MD Aortic valve repair is a technique that is gaining popularity in children because
Chordal replacement with polytetrafluoroethylene sutures for mitral valve repair: A 25-year experience
 Chordal replacement with polytetrafluoroethylene sutures for mitral valve repair: A 25-year experience Tirone E. David, MD, Susan Armstrong, MSc, and Joan Ivanov, PhD Objective: The study objective was
Chordal replacement with polytetrafluoroethylene sutures for mitral valve repair: A 25-year experience Tirone E. David, MD, Susan Armstrong, MSc, and Joan Ivanov, PhD Objective: The study objective was
The Tricuspid Valve: The Not So Forgotten Valve. Manuel J Antunes Cardiothoracic Surgery Coimbra, Portugal
 The Tricuspid Valve: The Not So Forgotten Valve Manuel J Antunes Cardiothoracic Surgery Coimbra, Portugal No Conflicts of Interest to declare with regards to this subject 2 INCIDENCE OF TRICUSPID REGURGITATION
The Tricuspid Valve: The Not So Forgotten Valve Manuel J Antunes Cardiothoracic Surgery Coimbra, Portugal No Conflicts of Interest to declare with regards to this subject 2 INCIDENCE OF TRICUSPID REGURGITATION
Mitral valve infective endocarditis (IE) is the most
 Mitral Valve Replacement for Infective Endocarditis With Annular Abscess: Annular Reconstruction Gregory J. Bittle, MD, Murtaza Y. Dawood, MD, and James S. Gammie, MD Mitral valve infective endocarditis
Mitral Valve Replacement for Infective Endocarditis With Annular Abscess: Annular Reconstruction Gregory J. Bittle, MD, Murtaza Y. Dawood, MD, and James S. Gammie, MD Mitral valve infective endocarditis
Surgical mitral valve repair (MVR) is the gold
 Transcatheter Chordal Repair for Degenerative Mitral Regurgitation Current and future directions of therapeutic options for patients with degenerative MR. BY ANDREA COLLI, MD, PhD; ALESSANDRO FIOCCO, MD;
Transcatheter Chordal Repair for Degenerative Mitral Regurgitation Current and future directions of therapeutic options for patients with degenerative MR. BY ANDREA COLLI, MD, PhD; ALESSANDRO FIOCCO, MD;
