Role of the AV Interval in DDD Pacing: Insights into Programming with Respect to Ventricular Function when AV Nodal Conduction is Intact
|
|
|
- Amie Page
- 5 years ago
- Views:
Transcription
1 Role of the AV Interval in DDD Pacing: Insights into Programming with Respect to Ventricular Function when AV Nodal Conduction is Intact Paul A. Levine, MD, FHRS, FACC Vice President, Medical Services, St. Jude Medical CRMD Clinical Professor of Medicine, Loma Linda University School of Medicine Introduction : The original indication for permanent pacing was complete heart block. The original pacing mode was asynchronous ventricular (VOO) pacing and the results were spectacular but the number of patients who would benefit from these early pacemakers was very limited. Since this early experience, the indications have grown as have the available pacing modes, the complexity and versatility of these devices and a recognition that when programmed inappropriately, these device may contribute to congestive heart failure and other adverse consequences. In the late 1970 s to early 1980 s, the medical profession first began to appreciate the adverse consequences associated with the loss of AV synchrony (pacemaker syndrome). In the early 1990 s, the first reports started to appear that patients with intact AV nodal conduction and a normal ventricular activation pattern might do better with AAI pacing as compared to DDD pacing although the results were mixed. Coincident with this growing recognition that AAI might be better than DDD were early studies suggesting that patients with refractory congestive heart failure, if associated with a left bundle branch block, might benefit from dual chamber pacing even in the absence of second or third degree AV block or sinus node dysfunction. Two underlying electrophysiologic states correctable by cardiac pacing and thus able to positively impact the management of congestive heart failure were identified in CHF patients. One was first degree AV block even though implantation of a DDD pacemaker to control the AV delay would force an abnormal ventricular activation sequence. This suggested that AV delay in some patients may be as if not more important than a normal ventricular activation sequence. The second was the disordered ventricular activation sequence resulting in mechanical dyssynchrony. This second mechanism could be addressed by stimulating a site other than the RV apex or simultaneously stimulating both the septal and postero-lateral walls of the left ventricle to improve mechanical dyssynchrony associated with the abnormal ventricular activation pattern. Dual site stimulation was first called biventricular pacing and is now known as cardiac resynchronization therapy. The role of CRT is being discussed in other articles in this symposium. The purpose of this paper is to address the
2 current status of dual chamber pacing with respect to its impact on ventricular function and programming the AV delay in patients who need a pacemaker for standard indications. The DAVID study 1 was a prospective randomized trial comparing single and dual chamber pacing in a group of patients being implanted with an ICD. Over the previous decade since the introduction of dual chamber ICDs, these had become the favored selection based on two presumptions. The first is that the atrial channel would provide improved arrhythmia discrimination. The second was based on the pacemaker literature with respect to pacemaker syndrome and the demonstration that dual chamber pacing was superior to single chamber ventricular pacing. There was data suggesting that one had to be very careful in programming the SVT discriminators to gain a benefit from the atrial channel with respect to improved specificity for recognition of ventricular tachyarrhythmias. If care was not taken, the results could be worse, not better than a single chamber ICD. The DAVID investigators wanted to evaluate the second presumption that DDD pacing in an ICD was superior to VVI pacing. The entry criteria required that the patients needed an ICD but did not require pacing support. One group was randomized to VVI pacing at a base rate of 40 bpm to provide back-up protection but otherwise allow the intrinsic rhythm to dominate. The second group was programmed to the DDD mode at a base rate of 60 bpm with AV delay programming left to the decision of each investigator. A majority left the paced and sensed AV delays at the shipped setting (170/150 ms) which resulted in ventricular pacing usurping control of the normal conduction system. The primary endpoint was hospitalization for new onset or worsening congestive heart failure and/or mortality. While the investigators were blinded as to the results, the Data Safety Monitoring Board reviewed the data on a regular basis and terminated the study prematurely because of a statistically significant increase in the primary endpoint in the DDD group rather than the VVI group. On review, the investigators concluded that the forced ventricular pacing in the DDD group causing a left bundle branch block contributed to the increased incidence of congestive heart failure. The incidence of ventricular pacing in the DDD group was 70% while it was only 4% in the VVI group. Based on the DAVID trial, the investigators in a number of other prospective studies (MOST 2, MADIT II 3, Midas 6 4 ) focusing on other issues 1 The DAVID Trial Investigators, Dual-chamber pacing or ventricular backup pacing in patients with an implantable defibrillator. JAMA 2002; 288: Shukla HH, Hellkamp AS, James EA, Flaker GC, Lee KL, Sweeney MO, Lamas GA, Heart failure hospitalization is more common in pacemaker patients with sinus node dysfunction and a prolonged paced QRS duration, Heart Rhythm 2005; 2: O Keefe JH, Jones PG, Thompson RC, Bateman TM, McGhie AI, Ramza BM, Steinhaus DM, Effect of chronic right ventricular apical pacing on left ventricular function, American J Cardiology 2005; 95: Freudenberger RS, Wilson AC, Lawrence-Nelson J, Hare JM, Kostis JB, Permanent pacing is a risk factor for the development of heart failure, American J Cardiology 2005; 95:
3 but comparing VVI to DDD re-examined their data and corroborated the findings of DAVID. An increased incidence of ventricular pacing when AV nodal conduction was otherwise intact was associated with an increased incidence of congestive heart failure and atrial fibrillation. This seems contradictory to the experience with CRT where a short AV delay is intentionally programmed but the setting is different patients with CRT start with a bundle branch block and severe CHF where as the above studies focused on patients with normal ventricular function and a narrow QRS complex. Over the past couple of years, based on these results, physicians have been programming very long AV delays or implementing algorithms to achieve functional AAI pacing even at the expense of a marked first degree AV block. Where AV nodal conduction and the ventricular activation sequence is normal, this is prudent and appropriate with an growing literature to support this approach. However, blindly programming a long AV delay may, for selected patients, be as counterproductive as programming a short AV delay in the presence of intact AV nodal conduction. Clinical vs Device Measurement of AV Delay: Many physicians do not appreciate that there is a difference between the pacemaker s definition of a PR interval and the clinician s definition. The standard clinical measurement of the PR interval starts with the onset of the P wave to the onset of the QRS complex as recorded on a standard surface electrocardiogram. The pacemaker starts its measurements with the intrinsic deflection of the atrial depolarization and ends its measurement with the intrinsic deflection of the ventricular depolarization (Figure 1a, 1b). It is the exception that the pacemaker detects with the atrial or ventricular depolarization at the leading edge of the respective P wave or QRS complex. In addition, when atrial pacing is involved, there may be a delay (latency) between the atrial stimulus and the onset of the atrial depolarization. There may also be an intra- and interatrial conduction delay (Figure1B). Thus, the AR interval is likely to be significantly longer than the PR interval and these differences must be taken into account during the evaluation of the patient and programming of the pacemaker.
4 Figure 1A Figure 1B Figure 1A: Surface ECG and simultaneous atrial bipolar electrogram during atrial sensed ventricular sensing. The intrinsic deflection of the P wave occurs well-after the onset of the P wave. The PR interval according to the pacemaker is 211 ms. Figure 1B: Surface ECG and simultaneous ventricular bipolar electrogram during atrial pacing ventricular sensing. The R according the pacemaker occurs towards the end of the conducted QRS complex. The AR interval as measured from the atrial stimulus to the intrinsic deflection of the QRS complex was 305 ms. The PR interval associated with this complex was 180 ms. This is what should be taken into account when deciding whether the AV delay should be extended sufficiently to allow for intact conduction or adjusted to totally control the AV interval even if there was ventricular pacing.
5 First degree AV block: In the excitement following DAVID and the retrospective analyses of MOST, MADIT II and other studies, a presumption has developed that if the ventricular activation sequence is basically normal as indicated by a narrow QRS, single chamber atrial pacing should take precedence over AV pacing short of second or third degree AV block. However, first degree AV block may be associated with exercise intolerance and shortness of breath as the native P wave coincides with the ST-T wave of the preceding conducted QRS complex even with a normal ventricular activation sequence (Figure 2). Figure 2: Rhythm strip from a Holter monitor. The patient had first degree AV block and with mild activities, a significant increase in his sinus rate and dyspnea on exertion that was out of proportion to the level of activity. Ventricular function was normal as assessed with Doppler echocardiography. These symptoms resolved with an increase in exercise tolerance following implantation of a dual chamber pacemaker despite ventricular pacing with its associated abnormal ventricular activation sequence. The upward directed arrows identify two of the sinus P waves in the ST-T wave segment driving the next QRS complex. In the original Guidelines for pacemaker implantation, first degree AV block was considered a Class III indication meaning that there was a general consensus that pacing was not required. There are a number of studies over the past decade that have demonstrated the adverse hemodynamic effects of first degree AV block, even when the resultant ventricular activation pattern was normal 5,6,7,8. In the studies by Vardas 7 and Schwaab 8, there was improvement in acute cardiac function with DDD pacing and its associated abnormal ventricular activation sequence compared to AAI pacing with the first degree AV block. In a study by Iliev 9, an AR interval > 270 ms 5 Barold SS, Indications for permanent cardiac pacing in first degree AV block: Class I, II or III? PACE 1996; 19: Kim YH, O Nunain S, Trouto T, et al, Pseudo-pacemaker syndrome following inadvertent fast pathway ablation for atrioventricular nodal reentrant tachycardia, J Cardiovasc Electrophysiol 1993; 4: Vardas PE, et al, AAIR vs DDDR pacing in patients with impaired sinus node chronotropy. An echocardiographic and cardiopulmonary study, PACE 1997; 20: Schwaab B, et al., AAIR vs DDDR pacing in the bradycardia tachycardia syndrome. A prospective randomized double-blind crossover trial, PACE 2001; 24: Iliev H, et al, Preserving normal ventricular activation versus atrioventricular delay optimization during pacing. The role of intrinsic atrioventricular conduction and pacing rate, PACE 2000; 23:
6 was associated with better cardiac performance associated with AV interval optimization as compared to normal ventricular activation. The ACC/AHA/HRS guidelines to indications for pacemaker implantation have elevated first degree AV block to a Class II indication when there are significant symptoms associated with this rhythm. The symptom complex associated with first degree AV block has been called pseudo-pacemaker syndrome. At increased sinus rates, the sinus P wave coincides with the ST-T wave of the previously conducted QRS complex causing the atrium to contract against a closed mitral and tricuspid valve limiting the atrial contribution to ventricular filling and by causing the atrium to contract against a closed mitral and tricuspid valve, contributing to pulmonary and systemic vascular congestion, effectively congestive heart failure with a mechanically normal heart. The normal physiology of native AV conduction is to progressively shorten the PR interval as the rate increases in response to a physiologic stress. This is the positive dromotropic effect of catecholamines 11,12. There is an entity termed the AAIR Pacemaker Syndrome, which is similar to symptomatic first degree AV block. With exercise and an increase in the atrial paced rate due to rate modulation, the AR interval fails to appropriately shorten causing the paced P wave to coincide with the ST-T wave associated with the previously conducted QRS complex 13. Indeed, in patients with sick sinus syndrome, the failure to appropriately shorten the AR interval with progressive increases in rate is not uncommon 14.This was one reason for the introduction of progressive shortening of the paced or sensed AV delay as the atrial rate increased. 15 Others have also shown that simply programming a long AV delay may be counterproductive, even in patients with intact AV nodal conduction 16,17. Allowing the AAI pacing mode to persist as the atrial rate 10 Gregoratos G, Abrams J, Epstein AE, et al, ACC/AHA/NASPE 2002 Guideline update for implantation of cardiac pacemakers and antiarrhytnmia devices, A report of the ACC/AHA Task Force on Practice Guidelines, Circulation 2002; 106: Luceri RM, Brownstein SL, Vardeman L, Goldstein S, PR interval behavior during exercise, implications for physiologic pacemakers, PACE 1990; 13: Barbieri D, Percoco GF, Toselli T, et al, AV delay and exercise stress tests: Behavior in normal subjects, PACE 1990; 13: Den Dulk K, Lindemans FW, Brugada P, Smeets JLRM, Wellens HJJ, Pacemaker Syndrome with AAI Rate variable pacing: Importance of atrioventricular conduction properties, medications and pacemaker programmability, PACE 1988; 11: Mabo P, Pouillot C, Kermarrec A, et al, Lack of physiologic adaptation of the atrioventricular interval to heart rate in patients chronically paced in the AAIR mode, PACE 1991; 14: Ritter P, Vai F, Bonnet JL, et al, Rate adaptive atrioventricular delay improves cardiopulmonary performance in patients with a dual chamber pacemaker for complete heart block, Eur J Cardiac Pacing and Electrophysiol 1991; 11: Pieterse MGC, Den Dulk K, van Gelder BM, van Mechelen R, Wellens HJJ, Programming a long paced atrioventricular interval may be risky in DDDR pacing, PACE 1994; 17: Kindermann M, Frohlig G, Doerr T, Schieffer H, Optimizing the AV delay in DDD pacemaker patients with preserved AV conduction, Heartweb, 1996; 2: Article ( htm)
7 increases may be associated with symptoms as originally described by Den Dulk and others due to the failure to appropriately shorten the AR interval during either physiologic or device-based increases in the atrial rate. This becomes even more common in the elderly patients who may be on beta-adrenergic blocking or calcium channel blocking drugs for the treatment of hypertension, ischemic heart disease and other conditions. A recent study used Doppler echocardiography to assess the myocardial performance index (MPI) in patients with sinus node dysfunction and intact AV nodal conduction 18. MPI had been previously used to optimize paced and sensed AV delays in the setting of AV block. The investigators used a phonocardiogram to identify the first heart sound defining the end of diastole and ventricular filling. The MPI is a ratio of the sum of the isovolumic contraction and isovolumic relaxation periods divided by the left ventricular ejection time. A low number identifies a better left ventricular function. They measured the MPI in the AAI mode was compared to the MPI in the DDD mode after the AV delay was adjusted to provide an optimal AV delay in the resting supine state. The ratio of the MPI in the AAI mode to that measured at the optimal AV delay in the DDD mode was defined as relative MPI or rmpi. The investigators also measured a relative atrioventricular interval (ravi), which was defined as the ratio of the AR interval measured during AAI pacing to the optimal AV delay measured during DDD pacing. The native PR interval in this group of patients was 161 ms ± 31 ms and the intrinsic QRS duration was 92 ±12 ms. The mean optimal AV delay in the DDD mode was 139 ± 22 ms which, interestingly, is very close to the mean AV delay being used in CRT systems. The atrial stimulus to R wave interval (AR) correlated with the rmpi. With atrial pacing, the AR interval commonly increased quite markedly. This is due to the site of stimulation and subsequent inter- and intraatrial conduction. When the ravi was > 1.73 meaning that the AR interval was significantly longer than the PR interval, DDD pacing was superior to AAI pacing. This is consistent with prior studies in patients with first degree AV block who have been shown to benefit from an optimal AV delay despite ventricular pacing with the abnormal ventricular activation sequence. When the ravi was < 1.5, AAI pacing tended to be superior. The investigators noted that there was no way to assess this simply from the surface ECG and indeed, in virtually all the patients in this study, the PR interval associated with the native rhythm was normal. 18 Kato M, Dote K, Sasaki S, Goto K, Takemoto H, Habara S, Hasegawa D, Matsuda O, Determination of the optimal atrioventricular interval in sick sinus syndrome during DDD pacing, PACE 2005; 28:
8 The major limitation of the study by Kato and the other studies cited is that they were acute without long term follow-up. In addition they assessed cardiac function in a single physiologic state supine at rest except for the Vardas paper which was at rest and exercise. Discussion: While David and the retrospective analysis of MADIT II, MOST and other studies have significantly impacted the practice of medicine with respect to programming AV delay, they have also caused the pendulum to swing too far towards blindly programming a long AV delay when AV nodal conduction is intact but compromised. Vardas, Schwaab and Iliev have shown that in the presence of first degree AV block as measured from the surface ECG, there may be an acute improvement in cardiac function by carefully programming the AV delay despite forcing an abnormal ventricular activation sequence. Kato and associates have demonstrated that even with a normal PR interval, there may be a significant difference between even the normal PR interval and the AR interval. In that setting, a careful assessment of the AV delay may also demonstrate improved cardiac function with AV pacing despite the disordered ventricular activation sequence. The goal of therapy is to improve cardiac function, not worsen it. These studies demonstrate that cardiac physiology is complex and while we now appreciate that forcing ventricular pacing when it is not needed may contribute to congestive heart failure, blindly eliminating all ventricular pacing in patients who have a primary indication for pacing, particularly sinus node dysfunction, may provide a false sense of reassurance that we are providing optimal therapy for these patients. It is important to carefully evaluate each patient. Those patients with normal baseline ventricular function may be able to initially compensate for any inadequacies associated with the pacing prescription making it difficult to prove a long term adverse consequence.
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Effect of Ventricular Pacing on Myocardial Function. Inha University Hospital Sung-Hee Shin
 Effect of Ventricular Pacing on Myocardial Function Inha University Hospital Sung-Hee Shin Contents 1. The effect of right ventricular apical pacing 2. Strategies for physiologically optimal ventricular
Effect of Ventricular Pacing on Myocardial Function Inha University Hospital Sung-Hee Shin Contents 1. The effect of right ventricular apical pacing 2. Strategies for physiologically optimal ventricular
Pacing Codes and Modes Concepts
 Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
How to prevent unecessary right ventricular pacing
 How to prevent unecessary right ventricular pacing Jens Cosedis Nielsen, MD, PhD, DMSci Dept of Cardiology, Aarhus University Hospital, Skejby, Denmark June 27, 2011, Europace Madrid Conflicts of interest
How to prevent unecessary right ventricular pacing Jens Cosedis Nielsen, MD, PhD, DMSci Dept of Cardiology, Aarhus University Hospital, Skejby, Denmark June 27, 2011, Europace Madrid Conflicts of interest
Reduction of Mitral Regurgitation by Endocardial Right Ventricular Bifocal Pacing in Cases of Dilated Cardiomyopathy
 June 2000 233 Reduction of Mitral Regurgitation by Endocardial Right Ventricular Bifocal Pacing in Cases of Dilated Cardiomyopathy J. C. PACHON M., R. N. ALBORNOZ, E. I. PACHON M., V. M. GIMENES, J. PACHON
June 2000 233 Reduction of Mitral Regurgitation by Endocardial Right Ventricular Bifocal Pacing in Cases of Dilated Cardiomyopathy J. C. PACHON M., R. N. ALBORNOZ, E. I. PACHON M., V. M. GIMENES, J. PACHON
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
How to Approach the Patient with CRT and Recurrent Heart Failure
 How to Approach the Patient with CRT and Recurrent Heart Failure Byron K. Lee MD Associate Professor of Medicine Electrophysiology and Arrhythmia Section UCSF Update in Electrocardiography and Arrhythmias
How to Approach the Patient with CRT and Recurrent Heart Failure Byron K. Lee MD Associate Professor of Medicine Electrophysiology and Arrhythmia Section UCSF Update in Electrocardiography and Arrhythmias
Friedman, Rott, Wokhlu, Asirvatham, Hayes 201. Figure 65.7 Shortening of the AV interval during pacing.
 Friedman, Rott, Wokhlu, Asirvatham, Hayes 201 Figure.7 Shortening of the AV interval during pacing. 202 A Case-Based Approach to Pacemakers, ICDs, and Cardiac Resynchronization Figure.8 is obtained from
Friedman, Rott, Wokhlu, Asirvatham, Hayes 201 Figure.7 Shortening of the AV interval during pacing. 202 A Case-Based Approach to Pacemakers, ICDs, and Cardiac Resynchronization Figure.8 is obtained from
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Upgrade to Resynchronization Therapy. Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic May 2016
 Upgrade to Resynchronization Therapy Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic May 2016 Event Free Survival (%) CRT Cardiac resynchronization therapy (CRT)
Upgrade to Resynchronization Therapy Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic May 2016 Event Free Survival (%) CRT Cardiac resynchronization therapy (CRT)
DON T FORGET TO OPTIMISE DEVICE PROGRAMMING
 CRT:NON-RESPONDERS OR NON-PROGRESSORS? DON T FORGET TO OPTIMISE DEVICE PROGRAMMING Prof. ALİ OTO,MD,FESC,FACC,FHRS Chairman,Department of Cardiology Hacettepe University Faculty of Medicine,Ankara Causes
CRT:NON-RESPONDERS OR NON-PROGRESSORS? DON T FORGET TO OPTIMISE DEVICE PROGRAMMING Prof. ALİ OTO,MD,FESC,FACC,FHRS Chairman,Department of Cardiology Hacettepe University Faculty of Medicine,Ankara Causes
The Management of Heart Failure after Biventricular Pacing
 The Management of Heart Failure after Biventricular Pacing Juan M. Aranda, Jr., MD University of Florida College of Medicine, Division of Cardiovascular Medicine, Gainesville, Florida Approximately 271,000
The Management of Heart Failure after Biventricular Pacing Juan M. Aranda, Jr., MD University of Florida College of Medicine, Division of Cardiovascular Medicine, Gainesville, Florida Approximately 271,000
Cardiac rhythm detailed monitoring by an implanted pacemaker: The iecg solution
 Cardiac rhythm detailed monitoring by an implanted pacemaker: The iecg solution Francesco Zanon, MD, FESC, FHRS Arrhythmia and Electrophysiology Unit, Cardiology Dept. Santa Maria della Misericordia General
Cardiac rhythm detailed monitoring by an implanted pacemaker: The iecg solution Francesco Zanon, MD, FESC, FHRS Arrhythmia and Electrophysiology Unit, Cardiology Dept. Santa Maria della Misericordia General
AF Today: W. For the majority of patients with atrial. are the Options? Chris Case
 AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Cardiac Resynchronisation Therapy for all Patients Requiring Ventricular Pacing
 Cardiac Resynchronisation Therapy for all Patients Requiring Ventricular Pacing Philippe Mabo University Hospital, Rennes, France ESC Congress 2010, Stockholm 29 Aug 2010 Which Patients? Candidate for
Cardiac Resynchronisation Therapy for all Patients Requiring Ventricular Pacing Philippe Mabo University Hospital, Rennes, France ESC Congress 2010, Stockholm 29 Aug 2010 Which Patients? Candidate for
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
How Do I Balance Bradycardia with Rate Control in Atrial Fibrillation?
 How Do I Balance Bradycardia with Rate Control in Atrial Fibrillation? Thang Nguyen MD FRCPC Assistant Professor Section of Cardiology Department of Internal Medicine University of Manitoba Objectives
How Do I Balance Bradycardia with Rate Control in Atrial Fibrillation? Thang Nguyen MD FRCPC Assistant Professor Section of Cardiology Department of Internal Medicine University of Manitoba Objectives
6to. Congreso Virtual de Cardiología - 6th. Virtual Congress of Cardiology
 Index > 6CVC >Arrhythmias and Electrophysiology Arrhythmias and Electrophysiology Symposium Pacemaker Mediated Tachycardia and Repetitive Non-Reentrant Ventriculo-Atrial Synchronous Rhythm: Two Sides of
Index > 6CVC >Arrhythmias and Electrophysiology Arrhythmias and Electrophysiology Symposium Pacemaker Mediated Tachycardia and Repetitive Non-Reentrant Ventriculo-Atrial Synchronous Rhythm: Two Sides of
Pediatric pacemakers & ICDs:
 Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Case Report Intermittent Right Ventricular Outflow Tract Capture due to Chronic Right Atrial Lead Dislodgement
 217 Case Report Intermittent Right Ventricular Outflow Tract Capture due to Chronic Right Atrial Lead Dislodgement Partha Prateem Choudhury, Vivek Chaturvedi, Saibal Mukhopadhyay, Jamal Yusuf Department
217 Case Report Intermittent Right Ventricular Outflow Tract Capture due to Chronic Right Atrial Lead Dislodgement Partha Prateem Choudhury, Vivek Chaturvedi, Saibal Mukhopadhyay, Jamal Yusuf Department
Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm
 April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
Programming of Bradycardic Parameters. C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany
 Programming of Bradycardic Parameters C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany Carsten.Israel@evkb.de Programming of ICD Brady Parameters Conflict of Interest Biotronik
Programming of Bradycardic Parameters C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany Carsten.Israel@evkb.de Programming of ICD Brady Parameters Conflict of Interest Biotronik
How Harmful is Conventional Right Ventricular Apical Pacing? Iatrogenic Left Bundle Branch Block: Need for Alternate Site Pacing
 HOSPITAL CHRONICLES, SUPPLEMENT 2006 HOSPITAL CHRONICLES 2006, SUPPLEMENT: 160 175 CARDIOLOGY UPDATE 2006 How Harmful is Conventional Right Ventricular Apical Pacing? Iatrogenic Left Bundle Branch Block:
HOSPITAL CHRONICLES, SUPPLEMENT 2006 HOSPITAL CHRONICLES 2006, SUPPLEMENT: 160 175 CARDIOLOGY UPDATE 2006 How Harmful is Conventional Right Ventricular Apical Pacing? Iatrogenic Left Bundle Branch Block:
Preventive Pacing in Atrial Fibrillation
 358 September 2001 Preventive Pacing in Atrial Fibrillation W. KAINZ Department of Cardiology, Hanusch Hospital, Vienna, Austria Summary Patients with paroxysmal atrial fibrillation are often highly symptomatic,
358 September 2001 Preventive Pacing in Atrial Fibrillation W. KAINZ Department of Cardiology, Hanusch Hospital, Vienna, Austria Summary Patients with paroxysmal atrial fibrillation are often highly symptomatic,
Dipartimento di Scienze Cardiovascolari Università Campus Bio-Medico di Roma Dott. Vito Calabrese
 Dipartimento di Scienze Cardiovascolari Università Campus Bio-Medico di Roma Dott. Vito Calabrese Because the primary objective was cure symptomatic bradicardya due to syncope Because this is the common
Dipartimento di Scienze Cardiovascolari Università Campus Bio-Medico di Roma Dott. Vito Calabrese Because the primary objective was cure symptomatic bradicardya due to syncope Because this is the common
Why do we need ECHO for CRT device optimization?
 Why do we need ECHO for CRT device optimization? Prof.dr.sc. J. Separovic Hanzevacki Department of Cardiovascular Diseases, University Hospital Centre Zagreb School of medicine, University of Zagreb Zagreb,
Why do we need ECHO for CRT device optimization? Prof.dr.sc. J. Separovic Hanzevacki Department of Cardiovascular Diseases, University Hospital Centre Zagreb School of medicine, University of Zagreb Zagreb,
Is This Thing Working?
 Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
Biatrial Stimulation and the Prevention of Atrial Fibrillation
 374 September 2001 Biatrial Stimulation and the Prevention of Atrial Fibrillation L. MELCZER Heart Institute, Faculty of Medicine, University of Pécs, Pécs, Hungary I. LORINCZ 1 st Internal Department,
374 September 2001 Biatrial Stimulation and the Prevention of Atrial Fibrillation L. MELCZER Heart Institute, Faculty of Medicine, University of Pécs, Pécs, Hungary I. LORINCZ 1 st Internal Department,
PRESENTER DISCLOSURE INFORMATION. There are no potential conflicts of interest regarding current presentation
 PRESENTER DISCLOSURE INFORMATION There are no potential conflicts of interest regarding current presentation Better synchrony and diastolic function for septal versus apical right ventricular permanent
PRESENTER DISCLOSURE INFORMATION There are no potential conflicts of interest regarding current presentation Better synchrony and diastolic function for septal versus apical right ventricular permanent
Wide QRS Tachycardia in a Dual Chamber Pacemaker Patient: What is the Mechanism?
 CASE REPORTS Arrhythmia 2015;16(3):173-177 doi: http://dx.doi.org/10.18501/arrhythmia.2015.029 Wide QRS Tachycardia in a Dual Chamber Pacemaker Patient: What is the Mechanism? Eun-Sun Jin, MD, PhD Cardiovascular
CASE REPORTS Arrhythmia 2015;16(3):173-177 doi: http://dx.doi.org/10.18501/arrhythmia.2015.029 Wide QRS Tachycardia in a Dual Chamber Pacemaker Patient: What is the Mechanism? Eun-Sun Jin, MD, PhD Cardiovascular
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale
 Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Treatment of AF by Pacing Therapy Is there Anything Else Beyond AVN Ablation?
 1 Treatment of AF by Pacing Therapy Is there Anything Else Beyond AVN Ablation? Chu-Pak Lau, MD Honorary Clinical Professor Queen Mary Hospital The University of Hong Kong How to Prevent AF by Pacing 1.
1 Treatment of AF by Pacing Therapy Is there Anything Else Beyond AVN Ablation? Chu-Pak Lau, MD Honorary Clinical Professor Queen Mary Hospital The University of Hong Kong How to Prevent AF by Pacing 1.
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
11/21/18. EKG Pop Quiz. Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants
 EKG Pop Quiz Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants 1 Disclosures No financial relationships to disclose. EKG #1 75 y/o woman with a dual-chamber pacemaker
EKG Pop Quiz Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants 1 Disclosures No financial relationships to disclose. EKG #1 75 y/o woman with a dual-chamber pacemaker
Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation
 J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
Document Version Publisher s PDF, also known as Version of Record (includes final page, issue and volume numbers)
 Initiation of ventricular tachycardia by interruption of pacemaker-mediated tachycardia in a patient with a dualchamber implantable cardioverter defibrillator Van Gelder, B.M.; Meijer, A.; Dekker, L.R.C.;
Initiation of ventricular tachycardia by interruption of pacemaker-mediated tachycardia in a patient with a dualchamber implantable cardioverter defibrillator Van Gelder, B.M.; Meijer, A.; Dekker, L.R.C.;
Practice Questions.
 IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
PARAD/PARAD+ : P and R Based Arrhythmia Detection
 Tech Corner PARAD/PARAD+ : P and R Based Arrhythmia Detection NOTE: PLEASE NOTE THAT THE FOLLOWING INFORMATION IS A GENERAL DESCRIPTION OF THE FUNCTION. DETAILS AND PARTICULAR CASES ARE NOT DESCRIBED IN
Tech Corner PARAD/PARAD+ : P and R Based Arrhythmia Detection NOTE: PLEASE NOTE THAT THE FOLLOWING INFORMATION IS A GENERAL DESCRIPTION OF THE FUNCTION. DETAILS AND PARTICULAR CASES ARE NOT DESCRIBED IN
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Ambulatory Monitors, Pacers, and Defibrillators
 Ambulatory Monitors, Pacers, and Defibrillators Vermont Cardiac Network 2018 Mark L. Greenberg MD Clinical Associate Professor of Medicine Geisel School of Medicine, Dartmouth Mark.L.Greenberg@Dartmouth.edu
Ambulatory Monitors, Pacers, and Defibrillators Vermont Cardiac Network 2018 Mark L. Greenberg MD Clinical Associate Professor of Medicine Geisel School of Medicine, Dartmouth Mark.L.Greenberg@Dartmouth.edu
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS
 INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS
 PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
A Square Peg in a Round Hole: CRT IN PAEDIATRICS AND CONGENITAL HEART DISEASE
 A Square Peg in a Round Hole: CRT IN PAEDIATRICS AND CONGENITAL HEART DISEASE Adele Greyling Dora Nginza Hospital, Port Elizabeth SA Heart November 2017 What are the guidelines based on? MADIT-II Size:
A Square Peg in a Round Hole: CRT IN PAEDIATRICS AND CONGENITAL HEART DISEASE Adele Greyling Dora Nginza Hospital, Port Elizabeth SA Heart November 2017 What are the guidelines based on? MADIT-II Size:
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
CRT-D or CRT-P: HOW TO CHOOSE THE RIGHT PATIENT?
 CRT-D or CRT-P: HOW TO CHOOSE THE RIGHT PATIENT? Alessandro Lipari, MD Chair and Department of Cardiology University of Study and Spedali Civili Brescia -Italy The birth of CRT in Europe, 20 years ago
CRT-D or CRT-P: HOW TO CHOOSE THE RIGHT PATIENT? Alessandro Lipari, MD Chair and Department of Cardiology University of Study and Spedali Civili Brescia -Italy The birth of CRT in Europe, 20 years ago
Long-term Preservation of Left Ventricular Function and Heart Failure Incidence with Ablate and Pace Therapy Utilizing Biventricular Pacing
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 976 981 HEART FAILURE RESEARCH ARTICLE Long-term Preservation of Left Ventricular Function and Heart Failure Incidence with Ablate and
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 976 981 HEART FAILURE RESEARCH ARTICLE Long-term Preservation of Left Ventricular Function and Heart Failure Incidence with Ablate and
Cardiac Devices CRT,ICD: Who is and is not a Candidate? Who Decides
 Cardiac Devices CRT,ICD: Who is and is not a Candidate? Who Decides Colette Seifer MB(Hons) FRCP(UK) Associate Professor, University of Manitoba, Cardiologist, Cardiac Sciences Program, St Boniface Hospital
Cardiac Devices CRT,ICD: Who is and is not a Candidate? Who Decides Colette Seifer MB(Hons) FRCP(UK) Associate Professor, University of Manitoba, Cardiologist, Cardiac Sciences Program, St Boniface Hospital
Cardiac resynchronization therapy for heart failure: state of the art
 Cardiac resynchronization therapy for heart failure: state of the art Béla Merkely MD, PhD, DSc, FESC, FACC Vice president of the European Society of Cardiology Honorary president of the Hungarian Society
Cardiac resynchronization therapy for heart failure: state of the art Béla Merkely MD, PhD, DSc, FESC, FACC Vice president of the European Society of Cardiology Honorary president of the Hungarian Society
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
Case Report Left Ventricular Dysfunction Caused by Unrecognized Surgical AV block in a Patient with a Manifest Right Free Wall Accessory Pathway
 109 Case Report Left Ventricular Dysfunction Caused by Unrecognized Surgical AV block in a Patient with a Manifest Right Free Wall Accessory Pathway Rakesh Gopinathannair, MD, MA 1, Dwayne N Campbell,
109 Case Report Left Ventricular Dysfunction Caused by Unrecognized Surgical AV block in a Patient with a Manifest Right Free Wall Accessory Pathway Rakesh Gopinathannair, MD, MA 1, Dwayne N Campbell,
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
II V 1 HRA 3 4 HB 5 6 HB 3 4 HB 1 2 CS 7 8 CS 5 6 CS 3 4 CS 1 2 ABL 3 4 ABL 1 2 RVA 3 4. T. Suga et al.
 Table 1. The distance between the positions of the catheter tip Patient Location Before elimination of After elimination of Number of the the accessory pathway the accessory pathway accessory pathway RAO
Table 1. The distance between the positions of the catheter tip Patient Location Before elimination of After elimination of Number of the the accessory pathway the accessory pathway accessory pathway RAO
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Review Article Resting Sinus Heart Rate and First Degree AV block: Modifiable Risk Predictors or Epiphenomena?
 www.ipej.org 334 Review Article Resting Sinus Heart Rate and First Degree AV block: Modifiable Risk Predictors or Epiphenomena? Rakesh Gopinathannair, MD, MA, Brian Olshansky, MD Division of Cardiovascular
www.ipej.org 334 Review Article Resting Sinus Heart Rate and First Degree AV block: Modifiable Risk Predictors or Epiphenomena? Rakesh Gopinathannair, MD, MA, Brian Olshansky, MD Division of Cardiovascular
Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators
 22 March 2002 Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators F. HINTRINGER, O. PACHINGER Division of Cardiology, Department for Internal Medicine, University
22 March 2002 Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators F. HINTRINGER, O. PACHINGER Division of Cardiology, Department for Internal Medicine, University
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II 2012 Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 ADDITIVES IN DEVICE THERAPY Key Choice / CNEA 1 Adaptive Rate
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II 2012 Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 ADDITIVES IN DEVICE THERAPY Key Choice / CNEA 1 Adaptive Rate
Cardiac Resynchronization ICD Therapy: What is New?
 Cardiac Resynchronization ICD Therapy: What is New? Emile Daoud, MD Section Chief, Cardiac Electrophysiology Professor of Medicine The Ohio State University Normal Activation, Narrow QRS Synchrony Abnormal
Cardiac Resynchronization ICD Therapy: What is New? Emile Daoud, MD Section Chief, Cardiac Electrophysiology Professor of Medicine The Ohio State University Normal Activation, Narrow QRS Synchrony Abnormal
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC
 Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact
GDT1000 SENSING ACUTE STUDY
 CAUTION: Federal law restricts this device to sale by or on the order of a physician trained or experienced in device implant and follow-up procedures. CLINICAL SUMMARY GDT1000 SENSING ACUTE STUDY Boston
CAUTION: Federal law restricts this device to sale by or on the order of a physician trained or experienced in device implant and follow-up procedures. CLINICAL SUMMARY GDT1000 SENSING ACUTE STUDY Boston
On Discovery. Pediatric Electrophysiology D CO. Electrophysiology. University of Texas Health Science Center at San Antonio, Texas
 Pediatric Electrophysiology David M Bush, MD, PhD ssistant Professor of Pediatrics Children s Heart Network Center San ntonio On Discovery What is wanted is not the will to believe, but the will to find
Pediatric Electrophysiology David M Bush, MD, PhD ssistant Professor of Pediatrics Children s Heart Network Center San ntonio On Discovery What is wanted is not the will to believe, but the will to find
a lecture series by SWESEMJR
 Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Teaching Rounds in Cardiac Electrophysiology
 Teaching Rounds in Cardiac Electrophysiology Sustained Multiple Railroad Tracks on Implantable Cardiac Defibrillator Interval Plots Mechanisms and Management Alex Y. Tan, MD; Kenneth A. Ellenbogen, MD;
Teaching Rounds in Cardiac Electrophysiology Sustained Multiple Railroad Tracks on Implantable Cardiac Defibrillator Interval Plots Mechanisms and Management Alex Y. Tan, MD; Kenneth A. Ellenbogen, MD;
Device Interrogation- Pacemakers, ICD and Loop Recorders. Dulce Obias-Manno, RN, MHSA, CCDS,CEPS, FHRS Device Clinic Coordinator, MHVI
 Device Interrogation- Pacemakers, ICD and Loop Recorders Dulce Obias-Manno, RN, MHSA, CCDS,CEPS, FHRS Device Clinic Coordinator, MHVI Disclosures Consultant: Medtronic Speaker s Bureau: St. Jude Medical
Device Interrogation- Pacemakers, ICD and Loop Recorders Dulce Obias-Manno, RN, MHSA, CCDS,CEPS, FHRS Device Clinic Coordinator, MHVI Disclosures Consultant: Medtronic Speaker s Bureau: St. Jude Medical
The effects of right ventricular apical pacing on ventricular function and dyssynchrony: implications for therapy
 1 1 The effects of right ventricular apical pacing on ventricular function and dyssynchrony: implications for therapy Laurens F. Tops Martin J. Schalij Jeroen J. Bax Department of Cardiology, Leiden University
1 1 The effects of right ventricular apical pacing on ventricular function and dyssynchrony: implications for therapy Laurens F. Tops Martin J. Schalij Jeroen J. Bax Department of Cardiology, Leiden University
Cardiac Telemetry Self Study: Part One Cardiovascular Review 2017 THINGS TO REMEMBER
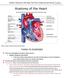 Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
Please review the above anatomy of the heart. THINGS TO REMEMBER There are 3 electrolytes that affect cardiac function o Sodium, Potassium, and Calcium When any of these electrolytes are out of the normal
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
Carlo Budano. Closed loop physiological stimulation: from the pacemaker patient to the patient with an ICD
 Closed loop physiological stimulation: from the pacemaker patient to the patient with an ICD Carlo Budano Dipartimento Cardiovascolare Città della Salute e della Scienza di Torino Physiological rate regulation
Closed loop physiological stimulation: from the pacemaker patient to the patient with an ICD Carlo Budano Dipartimento Cardiovascolare Città della Salute e della Scienza di Torino Physiological rate regulation
CLINICAL SUMMARY COGENT-4 FIELD FOLLOWING STUDY
 CAUTION: Federal law (USA) restricts this device to sale by or on the order of a physician trained or experienced in device implant and follow-up procedures. CLINICAL SUMMARY COGENT-4 FIELD FOLLOWING STUDY
CAUTION: Federal law (USA) restricts this device to sale by or on the order of a physician trained or experienced in device implant and follow-up procedures. CLINICAL SUMMARY COGENT-4 FIELD FOLLOWING STUDY
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS
 NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
Objectives of the Heart
 Objectives of the Heart Electrical activity of the heart Action potential EKG Cardiac cycle Heart sounds Heart Rate The heart s beat separated into 2 phases Relaxed phase diastole (filling of the chambers)
Objectives of the Heart Electrical activity of the heart Action potential EKG Cardiac cycle Heart sounds Heart Rate The heart s beat separated into 2 phases Relaxed phase diastole (filling of the chambers)
Case 1 Left Atrial Tachycardia
 Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Heart Failure Overview. Dr Chris K Y Wong
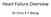 Heart Failure Overview Dr Chris K Y Wong Heart Failure: A Growing, Global Health Issue Heart Failure 23 Million Afflicted Global Impact Worldwide ~23 million peopleworldwide afflicted with CHF 1 Exceeds
Heart Failure Overview Dr Chris K Y Wong Heart Failure: A Growing, Global Health Issue Heart Failure 23 Million Afflicted Global Impact Worldwide ~23 million peopleworldwide afflicted with CHF 1 Exceeds
Bi-Ventricular pacing after the most recent studies
 Seminars of the Hellenic Working Groups February 18th-20 20,, 2010, Thessaloniki, Greece Bi-Ventricular pacing after the most recent studies Maurizio Lunati MD Director EP Lab & Unit Cardiology Dpt. Niguarda
Seminars of the Hellenic Working Groups February 18th-20 20,, 2010, Thessaloniki, Greece Bi-Ventricular pacing after the most recent studies Maurizio Lunati MD Director EP Lab & Unit Cardiology Dpt. Niguarda
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Three-dimensional Wall Motion Tracking:
 Three-dimensional Wall Motion Tracking: A Novel Echocardiographic Method for the Assessment of Ventricular Volumes, Strain and Dyssynchrony Jeffrey C. Hill, BS, RDCS, FASE Jennifer L. Kane, RCS Gerard
Three-dimensional Wall Motion Tracking: A Novel Echocardiographic Method for the Assessment of Ventricular Volumes, Strain and Dyssynchrony Jeffrey C. Hill, BS, RDCS, FASE Jennifer L. Kane, RCS Gerard
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
8/8/2011. CARDIAC RESYCHRONIZATION THERAPY for Heart Failure. Case Presentation. Case Presentation
 CARDIAC RESYCHRONIZATION THERAPY for Heart Failure James Taylor, DO, FACOS Cardiothoracic and Vascular surgery San Angelo Community Medical Center San Angelo, TX Case Presentation 64 year old female with
CARDIAC RESYCHRONIZATION THERAPY for Heart Failure James Taylor, DO, FACOS Cardiothoracic and Vascular surgery San Angelo Community Medical Center San Angelo, TX Case Presentation 64 year old female with
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
Atrial paralysis due to progression of cardiac disease in a patient with Emery-Dreifuss muscular dystrophy
 CASE REPORT Cardiology Journal 2011, Vol. 18, No. 2, pp. 189 193 Copyright 2011 Via Medica ISSN 1897 5593 Atrial paralysis due to progression of cardiac disease in a patient with Emery-Dreifuss muscular
CASE REPORT Cardiology Journal 2011, Vol. 18, No. 2, pp. 189 193 Copyright 2011 Via Medica ISSN 1897 5593 Atrial paralysis due to progression of cardiac disease in a patient with Emery-Dreifuss muscular
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]](/thumbs/96/126998162.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
Name of Policy: Bi-Ventricular Pacemakers (Cardiac Resynchronization Therapy) for the Treatment of Heart Failure
 Name of Policy: Bi-Ventricular Pacemakers (Cardiac Resynchronization Therapy) for the Treatment of Heart Failure Policy #: 055 Latest Review Date: April 2014 Category: Surgery Policy Grade: A Background/Definitions:
Name of Policy: Bi-Ventricular Pacemakers (Cardiac Resynchronization Therapy) for the Treatment of Heart Failure Policy #: 055 Latest Review Date: April 2014 Category: Surgery Policy Grade: A Background/Definitions:
Tehran Arrhythmia Center
 Tehran Arrhythmia Center The Worst Scenario A 4 year old kid High heart rates first noted by parents at 20 months of age. Family physician detected rates as high as 220 bpm at that age. He was visited,
Tehran Arrhythmia Center The Worst Scenario A 4 year old kid High heart rates first noted by parents at 20 months of age. Family physician detected rates as high as 220 bpm at that age. He was visited,
