SCAI Expert Consensus Statement for Renal Artery Stenting Appropriate Use
|
|
|
- Poppy Newman
- 6 years ago
- Views:
Transcription
1 Catheterization and Cardiovascular Interventions 00:00 00 (2014) Core Curriculum SCAI Expert Consensus Statement for Renal Artery Stenting Appropriate Use Sahil A. Parikh, 1 * MD, FACC, FSCAI, Mehdi H. Shishehbor, DO, MPH, FACC, FSCAI, Bruce H. Gray, DO, FSCAI, Christopher J. White, MD, FACC, FSCAI, and Michael R. Jaff, DO, FACC, FSCAI The pathophysiology of atherosclerotic renal artery stenosis (RAS) includes activation of the renin-angiotensin-aldosterone axis with resultant renovascular hypertension. Renal artery stenting has emerged as the primary revascularization strategy in most patients with hemodynamically significant atherosclerotic RAS. Despite the frequency with which hemodynamically significant RAS is observed and high rates of technical success of renal artery stenting, there remains considerable debate among experts regarding the role of medical therapy versus revascularization for renovascular hypertension. Modern, prospective, multicenter registries continue to demonstrate improvement in systolic and diastolic blood pressure with excellent safety profiles in patients with RAS. Modern randomized, controlled clinical trials of optimal medical therapy versus renal stenting particularly designed to demonstrate preservation in renal function after renal artery stenting have demonstrated limited benefit. However, these trials frequently excluded patients that may benefit from renal artery stenting. This document was developed to guide physicians in the modern practical application of renal stenting, to highlight the current limitations in the peer-reviewed literature, to suggest best-practices in the performance of renal stenting and to identify opportunities to advance the field. VC 2014 Wiley Periodicals, Inc. Key words: renovascular hypertension; renal artery stenosis; stent INTRODUCTION The pathophysiology of renovascular hypertension because of stenosis of the renal arteries has been understood for over 50 years. Impairment of renal arterial blood flow results in activation of the renin-angiotensinaldosterone axis with sequelae that include: vasoconstriction, sodium and water retention, aldosterone secretion, sympathetic nervous system activation, vascular 1 SAP University Hospitals Case Medical Center, Harrington Heart and Vascular Institute and Case Western Reserve University School of Medicine, Cleveland, Ohio 2 MRJ Massachusetts General Hospital, Boston, Massachusetts 3 BHG University of South Carolina School of Medicine/ Greenville, Greenville, South Carolina 4 MHS Cleveland Clinic, Cleveland, Ohio 5 CJW The University of Queensland and the John Ochsner Heart & Vascular Institute, Ochsner Medical Center, New Orleans, Louisiana Relationships with Industry: SAP: Consultant: Abbott Vascular, Boston Scientific, Medtronic MRJ: Non-compensated advisor: Abbott Vascular; Boston Scientific; Cordis Corporation; Covidien Vascular; Medtronic Vascular. Board Member, VIVA Physicians, a 501 c 3 not-for-profit education and research consortium Conflict of interest: Nothing to report. *Correspondence to: Sahil A Parikh, MD, FACC, FSCAI; University Hospitals Case Medical Center, Euclid Avenue, Cleveland, OH sahil.parikh@uhhospitals.org Received 17 May 2014; Revision accepted 25 May 2014 DOI: /ccd Published online 00 Month 2014 in Wiley Online Library (wileyonlinelibrary.com) VC 2014 Wiley Periodicals, Inc.
2 2 Parikh et al. Fig. 1. The Pathophysiology and Effects of RAS (Adapted from Ref. [1]) : RAS initiates a cascade of maladaptive responses that upregulate renin production with subsequent activation of the renin-angiotensin-aldosterone axis. ACE, Angiotensin Converting Enzyme; LV, Left Ventricular. remodeling, and resultant hypertension (Fig. 1) [1]. The majority (>90%) of cases of renal artery stenosis (RAS) result from atherosclerosis. Despite the frequency with which hemodynamically significant RAS is found, particularly among patients with coronary artery disease, there remains considerable debate among experts regarding the role of medical therapy versus revascularization for renovascular hypertension. Renal artery stent revascularization (renal artery stenting) has emerged as the primary revascularization strategy in most patients with hemodynamically significant atherosclerotic RAS [2]. Stent placement, with or without predilation with percutaneous transluminal angioplasty, has become the preferred endovascular technique [3]. Modern, prospective, multicenter registries continue to demonstrate improvement in systolic and diastolic blood pressure (SBP, DBP) with excellent safety profiles. However, because of their nonrandomized design, there has not been widespread acceptance of the benefits of renal artery stenting [4]. Modern randomized clinical trials of optimal medical therapy (OMT) versus renal stenting, particularly designed to demonstrate preservation in renal function have been plagued by serious methodological flaws in study design and execution [5]. The recently published CORAL trial, a prospective multicenter randomized controlled clinical trial which took a decade to complete likely excluded patients who may have gained benefit from renal artery stenting [6]. This document was developed to guide physicians in the modern practical application of renal stenting, to highlight the current limitations in the peer-reviewed literature, and to identify opportunities to advance the field. ANATOMIC CONSIDERATIONS (DIAGNOSTIC TESTING) TABLE I. Common Causes of Renal Artery Stenosis Atherosclerotic renal artery stenosis Fibromuscular dysplasia Nephroangiosclerosis (Hypertensive injury) Diabetic nephropathy (small vessels) Renal thromboembolic disease Atheroembolic renal disease Aortorenal dissection Renal artery vasculitis Trauma Neurofibromatosis Thromboangiitis obliterans Scleroderma Extrinsic compression TABLE II. Clinical Clues Suggestive of Renal Artery Stenosis Onset of hypertension at <30 years of age or severe hypertension at >55 years of age Accelerated, resistant, or malignant hypertension Unexplained atrophic kidney or size discrepancy >1.5 cm between kidneys Sudden, unexplained pulmonary edema Unexplained renal dysfunction, including individuals starting renal replacement therapy Development of new azotemia or worsening renal function after administration of an ACE inhibitor or ARB agent Multivessel coronary artery disease or peripheral artery disease Unexplained congestive heart failure or refractory angina Adapted from Ref. [10] The majority of RAS cases are because of atherosclerosis (Table I). Typical lesions involve the aortoostial junction or proximal segment of the renal artery. RAS because of fibromuscular dysplasia, vasculitis, or trauma are infrequently encountered, and are not covered in this manuscript. The diagnosis of hemodynamically significant RAS is critical to determining optimal therapy. A physical examination provides few specific clues to the presence of RAS except for the rare systolic/diastolic abdominal bruit radiating to the flank region. However, in patients with peripheral artery disease (PAD) or multi-vessel coronary artery disease (CAD), there is an increased association with hemodynamically significant RAS. In patients with significant CAD, the coexistent incidence of RAS observed at coronary angiography is approximately 20%, with the incidence rising in patients with higher burdens of extracoronary atherosclerosis [7,8]. In patients in whom there is a high clinical suspicion for RAS (Table II), and who are considered potential candidates for revascularization, a diagnostic evaluation for RAS should be undertaken [9]. A concise review of the diagnostic modalities can be found in the recently updated multisocietal guidelines [10]. Renal artery duplex ultrasonography (RADUS), which utilizes no radiation, is highly sensitive and specific, inexpensive, and can be repeated without risk or discomfort to the patient, remains an important diagnostic
3 Consensus Statement for Renal Arterial Intervention 3 TABLE III. Assessing Significance of Renal Artery Stenosis Angiographic stenosis severity a Physiologic testing Significance <50% None Mild 50 70% None Indeterminate 50 70% with Resting mean pressure Significant gradient b >10 mm Hg 50 70% with Systolic hyperemic pressure Significant gradient >20 mm Hg 50 70% with Renal Pd/Pa 0.8 c Significant 70% None Significant a Visual estimation. b Translesional gradient measured with a nonobstructive catheter, ie 4 french or with an in pressure wire (Pd/Pa). c Hyperemia may be induced with intrarenal bolus of papaverine 30 mg or dopamine at 50 mg/kg [11,13,14]. tool. RADUS may identify a stenosis severity greater than 60%. Axial imaging techniques, including computerized tomographic angiography (CTA) and magnetic resonance arteriography (MRA), are also highly sensitive and specific, but are more costly. CTA requires exposure to iodinated contrast and additional radiation. MRA requires noniodinated contrast and does not expose patients to external beam radiation, but may overestimate disease severity. In patients with renal dysfunction, CTA carries a risk of contrast-induced nephropathy while gadolinium-enhanced MRA has been associated with nephrogenic systemic fibrosis. Invasive diagnostic angiography may be considered for patients with inconclusive noninvasive testing and a high clinical suspicion of RAS. Invasive angiography is also appropriate for patients at high risk for RAS and who require invasive angiography for other indications, specifically if there is an indication for intervention and probable benefit from revascularization [9]. Renal angiography is the gold standard for the invasive assessment of hemodynamically significant RAS. Angiographic stenosis severity can be simply categorized as: mild (<50%), moderate (50 70%), and severe (>70%). However, such assessments may not accurately define hemodynamically significant stenosis [10], and only hemodynamically significant RAS should be considered for renal stenting. Angiographic stenoses >70% are considered to be severe lesions and hemodynamically significant. Moderate angiographic stenoses between 50% and 70% may or may not be hemodynamically significant, and should have further confirmation of their hemodynamic severity prior to intervention. Expert consensus and experimental evidence have determined that hemodynamic severity is present when there exists a resting translesional mean pressure gradient of > 10 mm Hg, a hyperemic peak TABLE IV. Clinical Scenarios in Which Treatment of Significant RAS a May be Considered Appropriate Care May Be Appropriate Care Rarely Appropriate Care Cardiac Disturbance Syndromes (Flash Pulmonary Edema or acute coronary syndrome (ACS)) with severe hypertension Resistant HTN (Uncontrolled hypertension with failure of maximally tolerated doses of at least three antihypertensive agents, one of which is a diuretic, or intolerance to medications) Ischemic nephropathy with chronic kidney disease (CKD) with egfr < 45 cc/min and global renal ischemia (unilateral significant RAS with a solitary kidney or bilateral significant RAS) without other explanation Unilateral RAS with CKD (egfr < 45 cc/min) Unilateral RAS with prior episodes of congestive heart failure (Stage C) Anatomically challenging or high risk lesion (early bifurcation, small vessel, severe concentric calcification, and severe aortic atheroma or mural thrombus) Unilateral, Solitary, or Bilateral RAS with controlled BP and normal renal function. Unilateral, solitary, or bilateral RAS with kidney size <7 cm in pole-to-pole length Unilateral, Solitary, or Bilateral RAS with chronic end stage renal disease on hemodialysis > 3 months. Unilateral, Solitary, or Bilateral renal artery chronic total occlusion a Significant RAS is an angiographically moderate lesion (50 70%) with physiologic confirmation of severity or a > 70% stenosis (see Table III). systolic pressure gradient of > 20 mm Hg or renal fractional flow reserve (FFR) 0.8 [11 14]. Angiographic stenoses <50% are mild, are not considered hemodynamically significant, and rarely warrant consideration for revascularization (Table III). The technical aspects of these measurements are discussed in Table III and the Technical Considerations section below. CLINICAL CONSIDERATIONS (CLINICAL SCENARIOS) Once the diagnosis of hemodynamically significant RAS is confirmed, the goals of revascularization may include: improvement in blood pressure control, prevention of progressive ischemic nephropathy, and improvement in heart failure, chronic angina, or sudden pulmonary edema (cardiac disturbance syndromes) [15]. For the purposes of this manuscript, we have enumerated the clinical scenarios in which endovascular treatment of RAS represents Appropriate Care, May Be Appropriate Care, or is Rarely Appropriate Care (Table IV). In all scenarios, only hemodynamically significant RAS is considered for endovascular therapy as previously defined. Comparisons to the multisocietal guidelines are highlighted in Fig. 2.
4 4 Parikh et al. Fig. 2. Review of Multi-Societal Guidelines Recommendations Adapted from [10]: Multisocietal Guideline Indications for renal artery revascularization. RAS, renal artery stenosis; CRI, chronic renal insufficiency; LOE, level of evidence. A recent meta-analysis of six randomized controlled trials (RCTs), that evaluated the safety and efficacy of renal stenting to either treat hypertension or to delay progression of renal ischemia, showed no improvement in renal function (as measured by serum creatinine or reciprocal of the serum creatinine) or clinical outcomes with stenting, compared to OMT [16]. Despite these findings, many experts agree that the RCTs conducted to date had major flaws in design, patient selection, lesion severity, and sample size, thus limiting their clinical applicability [17,18]. For example, in AS- TRAL, the largest of these trials, only 40% of patients had a stenosis between 50% and 70%, and the highrisk patients felt most likely to benefit from renal stenting (i.e. recurrent flash pulmonary edema) were excluded [17 19]. In the recently concluded Cardiovascular Outcomes in Renal Atherosclerotic Lesions (CORAL) Trial, patients with RAS and hypertension with SBP of greater than 155 mm Hg or higher while taking two or more antihypertensive drugs with angiographic RAS of at least 60% with evidence of a translesional gradient greater than 20 mm Hg or angiographic severity of greater than 80% (but less than 100% stenosis) were randomized to OMT versus renal artery stenting [6]. The primary endpoint was a composite of cardiovascular or renal death, stroke, myocardial infarction, hospitalization for congestive heart failure (CHF), progressive renal insufficiency, or the need for permanent renal replacement therapy. In 947 patients enrolled in the trial, there was no statistically significant difference observed in the primary endpoint (35.1% stent group vs 35.8% medical therapy group) with both groups demonstrating nearly a 15 mm Hg reduction in blood pressure over the course of the study. CORAL confirms that first line therapy for patients with RAS and hypertension is OMT. However, CORAL did not evaluate those who failed OMT, and many patients were not eligible for inclusion in the trial. Therefore, there are many patients commonly found in clinical practice whose management remains uncertain, and it is for those that this document is designed. It is clear that anatomic findings of RAS in isolation do not necessarily result in any clinical syndrome, including renovascular hypertension chronic kidney disease. However, when considering renal artery stenting, and given the limitations of RCTs to date, we encourage clinicians to use the steps outlined in this document in conjunction with the recent multisocietal guidelines to guide their management strategy. Renal Artery Stenting Represents Appropriate Care The strongest evidence supporting renal artery stenting for RAS is in patients with the presence of a cardiac disturbance syndrome or flash pulmonary edema [10,20]. We agree with the multisocietal guidelines which provide a Class I recommendation (Level of Evidence (LOE) B) in this subset of patients, in which a variety of physiologic mechanisms play a role [10]. Patients with severe bilateral RAS or stenosis to a solitary functioning kidney may lack adequate renal sodium handling capacity to generate pressure
5 natriuresis to autoregulate BP, or they may demonstrate inappropriate peripheral vasoconstriction resulting in abrupt increases in afterload and resultant myocardial ischemia or heart failure. Each of these mechanisms, when managed with renal artery stenting, have resulted in clinical improvement in case series where such patients are carefully selected [21 23]. It must be noted that in CORAL, 20% of patients randomized to stent and 16% randomized to medical therapy had global renal ischemia, and there was no statistical difference in hospitalization for heart failure [6]. Patients with accelerated or resistant hypertension (failure of 3 maximally tolerated medications including the use of a diuretic), global renal ischemia (bilateral RAS or severe RAS in a solitary functioning kidney), or hypertension with medication intolerance also generally benefit from renal artery stenting after a trial of OMT [10,20]. Multiple, relatively small, prospective, and retrospective series have shown benefit from renal artery stenting minimizing recurrent symptoms and end organ injury. The multisocietal guidelines provide a Class II a (LOE B) recommendation in this subset of patients, though we feel more strongly that renal artery stenting in these patients is generally appropriate, particularly in light of more recent data that use the same definition of accelerated or resistant hypertension. De Bruyne and colleagues demonstrated a threshold severity for renal vein renin release determined by a ratio of translesional to aortic pressure (Pd/ Pa) of < 0.9 [13]. Patients with the highest baseline systolic blood pressures will have the greatest decrease in systolic pressure. There has been no correlation between blood pressure improvement after renal stenting and the variables of age, sex, race, severity of stenosis, number of vessels treated, baseline diastolic pressure, or baseline serum creatinine [24]. In a pooled analysis of 901 patients enrolled in five prospective investigational device exemption trials, systolic blood pressure >150 mm Hg (OR ¼ 4.09, CI ¼ , P < ) was positively associated with BP response following renal artery stent revascularization [25]. Multiple, prospective, multicenter nonrandomized trials have consistently demonstrated a significant improvement in blood pressure control following renal stenting in medically refractory patients [4]. For patients with progressive deterioration in renal function and global renal ischemia without another etiology for chronic kidney disease, clinical case series have demonstrated a significant reduction in the rate of loss of renal function in patients undergoing renal stenting [26 28]. Therefore, we agree with the multisocietal guidelines that patients with global renal ischemia and declining renal function may benefit from Consensus Statement for Renal Arterial Intervention 5 renal stenting and that such therapy represents appropriate care. Renal Stenting May Represent Appropriate Care There are a number of common clinical scenarios in which renal stenting for RAS remain controversial and where the data are inconclusive. In our opinion these scenarios often pose the greatest challenge to clinicians, and therefore require an individualized patient approach, particularly given the lack of conclusive evidence. The data for preservation of renal parenchymal function in patients at high risk for progressive ischemic nephropathy, particularly those with chronic kidney disease, suggests that revascularization may stabilize renal function [29 32]. However, as noted previously, generalizable results from RCTs designed to answer this question are limited [17,18]. Based on observational studies it appears that higher risk patients, such as those with global renal ischemia and egfr <45 cc/min, including individuals with a solitary functioning kidney, may gain the greatest benefit from renal stenting [10]. The multisocietal guidelines offer a Class II b (LOE C) recommendation for revascularization in such patients, and as such, we agree that renal stenting may be appropriate in carefully selected patients. Recent data suggest that RAS induces secretion of paracrine effectors that activate myocardial hypertrophic response genes and may have deleterious longterm impact upon the clinical course of heart failure. It remains speculative if renal artery stenting may reverse this cascade [33]. Renal stenting of patients with hemodynamically significant unilateral RAS with prior episodes of congestive heart failure (Stage C) without a primary cardiac etiology for such may represent appropriate care in selected patients. In patients with challenging or anatomically difficult or high-risk renal lesions (i.e. early bifurcation, small (< 3.0 cm) diameter vessels, in vessels with severe concentric calcification, in patients with diffuse aortic atherosclerosis or mural thrombus, and those in which RAS is seen in conjunction with a renal artery aneurysm or juxtarenal abdominal aortic aneurysm), the risk-to-benefit ratio will depend on individual patient circumstances and individual operator skill, making these cases indeterminate for appropriate use. Renal Stenting Rarely Represents Appropriate Care While there are scenarios in which revascularization for RAS remains controversial, it is clear that hemodynamically mild to moderate stenoses (e.g. peak to peak translesional gradient < 20 mm Hg, mean translesional
6 6 Parikh et al. gradient <10 mm Hg or renal FFR >0.8) do not merit revascularization. Given the inaccuracy of invasive angiography in determining the physiologic significance of moderate RAS, it would be rarely appropriate for an intervention to be performed on an angiographically moderate 50% to 70% diameter stenosis without hemodynamic confirmation of the severity of the lesion [11 14,34]. Patients with long standing ischemic nephropathy, such as those requiring chronic hemodialysis for greater than three months or in those with marked renal atrophy (< 7 cm pole to pole), are not likely to benefit from revascularization [35,36]. Similarly, chronic total occlusions of renal arteries do not warrant revascularization. TECHNICAL CONSIDERATIONS (PERFORMANCE OF RENAL STENTING) Preparation for Angiography Renal angiography is justified when there is an appropriate clinical indication for renal artery revascularization and, in most clinical scenarios, the presence of RAS has been confirmed by a noninvasive evaluation or when noninvasive imaging is nondiagnostic, confirmed by arteriography. Performance of renal angiography in a patient without an indication for revascularization is not advised, as this practice may lead to inappropriate revascularization and unwarranted complications. Prior to the procedure, all noninvasive studies should be reviewed for the presence of aortic atherosclerosis, accessory renal arteries, location of the RAS, angulation of the renal arteries, the presence of fibromuscular dysplasia, and pole-to-pole kidney size. Additional information that may alter the procedural approach include the presence of an abdominal aortic aneurysm with or without mural thrombus, aortic calcification, and iliac artery atherosclerotic disease. This information will influence the choice of access (radial, brachial, or femoral) for both diagnostic angiography and revascularization. Performance of Renal Angiography The classic approach of performing abdominal aortography, followed by selective renal angiography, is safe and effective. The use of the radial artery for vascular access may be considered to reduce the risk of periprocedural access site complications. However, when performing renal stenting to preserve renal function in patients with chronic kidney disease, every attempt should be made to minimize iodinated contrast load. In these cases, one may perform limited abdominal aortography with dilute contrast or carbon dioxide (CO 2 ) with a focus towards accessing the renal arteries. Alternatively, when appropriate, one can directly perform selective renal arteriography using aortic and renal artery calcification as a guide. We strongly recommend digital subtraction angiography and contrast-sparing techniques, particularly when performing renal stenting for the preservation of kidney function. Selective renal angiography should be performed with visualization of the entire kidney. Lack of perfusion to a particular segment may indicate the presence of an infarcted segment, an accessory renal artery, or renal mass or cyst. The differentiation of each may be complemented by data obtained on preprocedure noninvasive imaging. Translesional Pressure Gradient Assessment Translesional pressure gradients should be routinely assessed as a component of the invasive evaluation of moderate (50 70%) RAS. Several investigators have demonstrated that a hyperemic systolic gradient of approximately 20 mm Hg induced by the administration of intrarenal papaverine (30 mg intra-arterial bolus) or dopamine (50mg/kg intra-arterial bolus) represents the greatest single predictor of blood pressure reduction after renal stenting [11,14]. It must be noted that adenosine is a vasoconstrictor in the renal artery and will not induce renal hyperemia. The most important reason for performing hemodynamic assessment is to discriminate hemodynamically significant stenoses from insignificant moderate angiographic stenoses. In general, the translesional pressure gradient (Pd/Pa ratio) <0.8, a resting mean gradient of 10 mm Hg, or a 20 mm Hg hyperemic systolic gradient are considered significant [11,12,14]. Intravascular Ultrasound Assessment Intravascular ultrasound (IVUS) may provide information regarding minimal luminal area, plaque burden, reference vessel diameter, presence of calcification, and postintervention characteristics like stent apposition. However, IVUS has not been demonstrated to improve outcomes in patients undergoing renal stenting, and therefore cannot be recommended for routine use [14]. At the operator s discretion, IVUS may be used to improve anatomic assessment of individual lesions and to facilitate stenting with the optimal stent diameter. Renal Artery Stenting Technique We recommend the use of a guide catheter with a curve and caliber appropriate to the intervention to be performed. Operators should minimize trauma, or scraping of the peri-renal aorta, by either using the no-touch technique or a telescoping technique with a 4F diagnostic catheter [37,38]. Currently, there are three 0.014" platform FDA approved balloon expandable
7 stents available for renal artery stenting (Express SD, Boston Scientific, Natick, MA, USA; Formula, Cook Incorporated, Bloomington, IN, USA; Herculink Elite, Abbott Vascular, Santa Clara, CA, USA). Radial artery access has increasingly been used to reduce access site related bleeding and to improve patient comfort. Access from the radial artery often affords excellent alignment of the renal ostium using a multipurpose guiding catheter. Occasionally, a 110 or 125 cm length guide is needed to reach the renal artery, which necessitates a longer shaft length for balloons and stents. Left arm access may reduce the distance to the renal ostia when catheter length is a concern. Under-sizing renal stents leads to increased restenosis, and over-sizing stents leads to increased procedural complications [39]. Appropriate stent sizing usually can be obtained from a preprocedural CTA/MRA, semi-quantitative angiography and when needed by IVUS. Care should be taken not to use the ectatic poststenotic dilated segment of the renal artery as the reference vessel diameter. The goal is to safely reduce the RAS to 30% angiographic stenosis and abolish the translesional pressure gradient to zero. Some patients will experience discomfort during balloon inflation which may signify impending vascular rupture because of stretching of the adventitia. When pain occurs, the balloon should be immediately deflated. This may limit the maximum size or complete expansion of the stent. The evidence supporting the use of embolic protection devices (EPD) and glycoprotein IIb/IIIa inhibitors are preliminary and unconfirmed [2]. In a two-by-two factorial design, the efficacy of the Angioguard EPD (Cordis Corporation, New Brunswick, NJ, USA) and abciximab (Janssen Biotech, Philadelphia, USA)) during renal stenting were evaluated in 100 patients [40]. No significant advantages were seen with the use of either alone, however, there was a benefit when EPD and abciximab were used in combination. While the study is of interest, there has been no confirmatory evidence supporting the routine use of EPDs or glycoprotein IIb/IIIa inhibitors. The initial CORAL trial mandated the use of EPD for all randomized to stent therapy, however, soon after trial initiation, this requirement was removed [6]. There is agreement by experts that selective use of EPDs may be appropriate in patients with favorable anatomy who are at increased risk for renal dysfunction from potential atheromatous embolization [i.e. patients with significant baseline impairment of renal function (egfr <45 ml/min)]. Complications Renal artery stenting is a safe procedure with a major complication rate of 2%. The most common complications are related to femoral access (hematoma, Consensus Statement for Renal Arterial Intervention 7 pseudoaneurysm, arteriovenous fistula, or localized deep venous thrombosis). Less common complications including retroperitoneal hemorrhage, renal artery perforation, arterial and aortic dissection, atheromatous embolization, renal infarction, and death have all been reported. In general, radial artery access, conservative balloon sizing for predilatation or direct stenting, sizing the stent 1:1 to the reference vessel diameter, and attention to patient complaints of peri-procedural pain will minimize serious complications. Follow-up There are no standard guidelines for routine followup after renal artery stenting. In general, most operators use RADUS for follow-up assessment [41]. The recent appropriate use (AU) guidelines for peripheral vascular ultrasound suggest a baseline RADUS onemonth following renal stenting. Following the onemonth assessment, annual RADUS in asymptomatic patients is appropriate [42]. The recurrence of uncontrolled hypertension or progressive deterioration in renal function without other explanation is an appropriate indication for repeat RADUS to evaluate for the presence of renal artery in-stent restenosis [43]. CONCLUSION Rigorously conducted clinical trials are critical to our understanding of the optimal treatment of our complex RAS patients. The CORAL trial and others have added to our understanding of the pathophysiology of RAS and the role of renal artery stenting [6]. However, as is commonly found in multicenter randomized trials, variable inclusion and exclusion criteria, outdated technology and technique, and an enrollment bias may limit the generalizability of results. Planning novel, clinically relevant trial designs requires an appreciation for the unanswered questions in the field and the likelihood of enrollment over a reasonable time frame. Our May Represent Appropriate Care category of renal stenting offers an opportunity to shed light on these patient characteristics, and given the absence of currently available data, clinical equipoise certainly exists. Enrolling patients with ischemic nephropathy, unilateral RAS and hypertension, and/or congestive heart failure with hemodynamically significant RAS using core lab adjudicated metrics (i.e. angiography, translesional pressure gradients with and without hyperemia, novel intravascular imaging techniques) would be challenging, but the outcomes may impact patient care. Improving technology for hemodynamic and imaging assessment of RAS will hopefully yield significant
8 8 Parikh et al. improvements in safety and efficacy of renal stenting. Smaller studies continue to explore the role of adjunctive pharmacology and EPD in renal artery revascularization. Nonetheless, given the paucity of scientifically valid data guiding our clinical decision making, the practitioner is required to use individual patient characteristics and best medical evidence (as referenced herein) to yield optimal and appropriate patient outcomes. REFERENCES 1. Garovic VD, Textor SC. Renovascular hypertension and ischemic nephropathy. Circulation, 2005;112: White CJ, Olin JW. Diagnosis and management of atherosclerotic renal artery stenosis: Improving patient selection and outcomes. Nat Clin Pract Cardiovasc Med 2009;6: Dorros G, Prince C, Mathiak L. Stenting of a renal artery stenosis achieves better relief of the obstructive lesion than balloon angioplasty. Cathet Cardiovasc Diagn 1993;29: Jaff MR, Bates M, Sullivan T, et al. Significant reduction in systolic blood pressure following renal artery stenting in patients with uncontrolled hypertension: Results from the HERCULES trial. Catheter Cardiovasc Interv 2012;80: George JC, White CJ. Renal artery stenting: Lessons from AS- TRAL (Angioplasty and Stenting for Renal Artery Lesions). JACC Cardiovasc Interv 2010;3: Cooper CJ, Murphy TP, Cutlip DE, et al. Stenting and medical therapy for atherosclerotic renal-artery stenosis. N Engl J Med 2014;370: Rihal CS, Textor SC, Breen JF, et al. Incidental renal artery stenosis among a prospective cohort of hypertensive patients undergoing coronary angiography. Mayo Clin Proc 2002;77: Olin JW, Melia M, Young JR, et al. Prevalence of atherosclerotic renal artery stenosis in patients with atherosclerosis elsewhere. Am J Med 1990;88:46N 51N. 9. White CJ, Jaff MR, Haskal ZJ, et al. Indications for renal arteriography at the time of coronary arteriography: A science advisory from the American Heart Association Committee on Diagnostic and Interventional Cardiac Catheterization, Council on Clinical Cardiology, and the Councils on Cardiovascular Radiology and Intervention and on Kidney in Cardiovascular Disease. Circulation 2006;114: Hirsch AT, Haskal ZJ, Hertzer NR, et al. ACC/AHA 2005 Practice Guidelines for the management of patients with peripheral arterial disease (lower extremity, renal, mesenteric, and abdominal aortic): A collaborative report from the American Association for Vascular Surgery/Society for Vascular Surgery, Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, Society of Interventional Radiology, and the ACC/AHA Task Force on Practice Guidelines (Writing Committee to Develop Guidelines for the Management of Patients With Peripheral Arterial Disease): Endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation; National Heart, Lung, and Blood Institute; Society for Vascular Nursing; TransAtlantic Inter-Society Consensus; and Vascular Disease Foundation. Circulation 2006;113:e Mangiacapra F, Trana C, Sarno G, et al. Translesional pressure gradients to predict blood pressure response after renal artery stenting in patients with renovascular hypertension. Circ Cardiovasc Interv 2010;3: Mitchell JA, Subramanian R, White CJ, et al. Predicting blood pressure improvement in hypertensive patients after renal artery stent placement: Renal fractional flow reserve. Catheter Cardiovasc Interv 2007; 69: De Bruyne B, Manoharan G, Pijls NH, et al. Assessment of renal artery stenosis severity by pressure gradient measurements. J Am Coll Cardiol 2006; 48: Leesar MA, Varma J, Shapira A, et al. Prediction of hypertension improvement after stenting of renal artery stenosis: Comparative accuracy of translesional pressure gradients, intravascular ultrasound, and angiography. J Am Coll Cardiol 2009;53: Rundback JH, Sacks D, Kent KC, et al. Guidelines for the reporting of renal artery revascularization in clinical trials. American Heart Association. Circulation 2002;106: Kumbhani DJ, Bavry AA, Harvey JE, et al. Clinical outcomes after percutaneous revascularization versus medical management in patients with significant renal artery stenosis: A meta-analysis of randomized controlled trials. Am Heart J 2011;161: e White CJ. Kiss my astral: One seriously flawed study of renal stenting after another. Catheter Cardiovasc Interv 2010;75: Weinberg MD, Olin JW. Stenting for atherosclerotic renal artery stenosis: One poorly designed trial after another. Cleve Clin J Med 2010;77: Wheatley K, Ives N, Gray R, et al. Revascularization versus medical therapy for renal-artery stenosis. N Engl J Med 2009; 361: Messerli FH, Bangalore S, Makani H, et al. Flash pulmonary oedema and bilateral renal artery stenosis: The Pickering syndrome. Eur Heart J 2011;32: Gray BH, Olin JW, Childs MB, et al. Clinical benefit of renal artery angioplasty with stenting for the control of recurrent and refractory congestive heart failure. Vasc Med 2002;7: Bloch MJ, Trost DW, Pickering TG, et al. Prevention of recurrent pulmonary edema in patients with bilateral renovascular disease through renal artery stent placement. Am J Hypertens 1999;12(1 Pt 1): Khosla S, White CJ, Collins TJ, et al. Effects of renal artery stent implantation in patients with renovascular hypertension presenting with unstable angina or congestive heart failure. Am J Cardiol 1997;80: Burket MW, Cooper CJ, Kennedy DJ, et al. Renal artery angioplasty and stent placement:predictors of a favorable outcome. Am Heart J 2000;139(1 Pt 1): Weinberg I, et al. Blood pressure response to renal artery stenting in 901 patients from five prospective multicenter FDAapproved trials. Catheter Cardiovasc Interv, 2014;83: Harden PN, MacLeod MJ, Rodger RS, et al. Effect of renal artery stenting on progression of renovascular renal failure. Lancet 1997;349: Kashyap VS, Sepulveda RN, Bena JF, et al. The management of renal artery atherosclerosis for renal salvage: Does stenting help? J Vasc Surg 2007; 45: ;discussion Muray S, Martin M, Amoedo ML, et al. Rapid decline in renal function reflects reversibility and predicts the outcome after angioplasty in renal artery stenosis. Am J Kidney Dis 2002; 39: Isles CG, Robertson S, Hill D. Management of renovascular disease: A review of renal artery stenting in ten studies. QJM 1999; 92: Watson PS, Hadjipetrou P, Cox SV, et al. Effect of renal artery stenting on renal function and size in patients with atherosclerotic renovascular disease. Circulation 2000; 102: Rocha-Singh KJ, Ahuja RK, Sung CH, et al. Long-term renal function preservation after renal artery stenting in patients with
9 Consensus Statement for Renal Arterial Intervention 9 progressive ischemic nephropathy. Catheter Cardiovasc Interv 2002; 57: Zeller T, Frank U, Muller C, et al. Predictors of improved renal function after percutaneous stent-supported angioplasty of severe atherosclerotic ostial renal artery stenosis. Circulation 2003; 108: Tian J, Haller S, Periyasamy S, et al. Renal ischemia regulates marinobufagenin release in humans. Hypertension 2010; 56: Subramanian R, White CJ, Rosenfield K, et al. Renal fractional flow reserve: A hemodynamic evaluation of moderate renal artery stenoses. Catheter Cardiovasc Interv 2005; 64: Shanley PF. The pathology of chronic renal ischemia. Semin Nephrol 1996; 16: Lerman LO, Textor SC, Grande JP. Mechanisms of tissue injury in renal artery stenosis: Ischemia and beyond. Prog Cardiovasc Dis 2009; 52: Patel RA, White CJ. Tips and tricks in renal artery angioplasty and stenting: Angiography, stent placement, embolic protection, complications, and contrast induced nephropathy. Minerva Cardioangiol 2010; 58: Feldman RL, Wargovich TJ, Bittl JA. No-touch technique for reducing aortic wall trauma during renal artery stenting. Catheter Cardiovasc Interv 1999;46: Lederman RJ, Mendelsohn FO, Santos R, et al. Primary renal artery stenting: Characteristics and outcomes after 363 procedures. Am Heart J 2001; 142: Cooper CJ, Haller ST, Colyer W, et al. Embolic protection and platelet inhibition during renal artery stenting. Circulation 2008; 117: Chi YW, White CJ, Thornton S, et al. Ultrasound velocity criteria for renal in-stent restenosis. J Vasc Surg, 2009;50: Mohler, ER, 3rd, Gornik HL, Gerhard-Herman M, et al., ACCF/ ACR/AIUM/ASE/ASN/ICAVL/SCAI/SCCT/SIR/SVM/SVS 2012 Appropriate Use Criteria for Peripheral Vascular Ultrasound and Physiological Testing Part I: Arterial Ultrasound and Physiological Testing: A Report of the American College of Cardiology Foundation Appropriate Use Criteria Task Force, American College of Radiology, American Institute of Ultrasound in Medicine, American Society of Echocardiography, American Society of Nephrology, Intersocietal Commission for the Accreditation of Vascular Laboratories, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, Society for Interventional Radiology, Society for Vascular Medicine, and Society for Vascular Surgery. J Am Coll Cardiol 2012;60: Davies MG, Saad WA, Bismuth JX, et al. Outcomes of endoluminal reintervention for restenosis after percutaneous renal angioplasty and stenting. J Vasc Surg 2009;49:
10 10 Parikh et al. Author Relationships with Industry and Other Entities (Comprehensive) Appropriate Use for Renal Artery Stenting: An Expert Consensus Statement from SCAI Ownership/ Partnership/ Personal Principal Research Institutional, Organizational or Other Financial Benefit Committee Member Advisory Board/ Board Member Consultant Speaker s Bureau Expert Witness Bruce Gray, DO None None None None None None None Michael Jaff, DO Abbott Vascular* None PQ Bypass None VIVA Physicians, a 501 None American Genomics Astra Zeneca Biomet Biologicals Boston Scientific* Cordis* Covidien* Ekos Corporation Medtronic* Micell, Inc. Primacea c 3 not-for-profit education and research organization Board member Sahil Parikh, MD None Abbott Vascular Abbott Vascular None Abbott Vascular None Boston Scientific Boston Boston Scientific Medtronic Scientific Medtronic Abiomed Medtronic Atrium Medical Astra Zeneca TriReme Medical Mehdi Shishehbor, DO None None None None None None None Christopher White, MD None None None None None None None This table represents all healthcare relationships of committee members with industry and other entities that were reported by authors, including those not deemed to be relevant to this document, at the time this document was under development. The table does not necessarily reflect relationships with industry at the time of publication. A person is deemed to have a significant interest in a business if the interest represents ownership of 5% of the voting stock or share of the business entity, or ownership of $ of the fair market value of the business entity; or if funds received by the person from the business entity exceed 5% of the person s gross income for the previous year. Relationships that exist with no financial benefit are also included for the purpose of transparency. Relationships in this table are modest unless otherwise noted. Please refer to for definitions of disclosure categories or additional information about the ACCF Disclosure Policy for Writing Committees. *No financial benefit. Significant relationship. Institutional relationship; person enrolls patients in trial per institutional requirement but has no direct relationship with the trial or trial sponsor. Therefore, this relationship was not deemed relevant to this document.
Renal Artery Stenting
 Renal Artery Stenting J.P. Reilly, MD, FSCAI Ochsner Medical Center Speaker s bureau: Astra Zeneca and Lilly/Diachi Sankyo Prevalence of RAS is high in cath population. Renal artery intervention can help
Renal Artery Stenting J.P. Reilly, MD, FSCAI Ochsner Medical Center Speaker s bureau: Astra Zeneca and Lilly/Diachi Sankyo Prevalence of RAS is high in cath population. Renal artery intervention can help
Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis
 Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea Etiology Fibromuscular
Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea Etiology Fibromuscular
Life After CORAL: What Did CORAL Prove? David Paul Slovut, MD, PhD Co-director TAVR, Dir of Advanced Intervention
 Life After CORAL: What Did CORAL Prove? David Paul Slovut, MD, PhD Co-director TAVR, Dir of Advanced Intervention No Relationships to Disclose The Need for Modern Renal Trials Increased rate of RAS diagnosis
Life After CORAL: What Did CORAL Prove? David Paul Slovut, MD, PhD Co-director TAVR, Dir of Advanced Intervention No Relationships to Disclose The Need for Modern Renal Trials Increased rate of RAS diagnosis
CORAL Trial Aftermath: What Do We Do Now? Renal Revascularization in Perspective
 CORAL Trial Aftermath: What Do We Do Now? Renal Revascularization in Perspective Michael R. Jaff, DO Massachusetts General Hospital Boston, Massachusetts, USA Michael R. Jaff, DO Conflicts of Interest
CORAL Trial Aftermath: What Do We Do Now? Renal Revascularization in Perspective Michael R. Jaff, DO Massachusetts General Hospital Boston, Massachusetts, USA Michael R. Jaff, DO Conflicts of Interest
Renal Artery Stenosis: Insights from the CORAL Trial
 Renal Artery Stenosis: Insights from the CORAL Trial Christopher J. Cooper, M.D., FACC, FACP Dean and Senior Vice President University of Toledo, College of Medicine President, Ohio Chapter ACC State of
Renal Artery Stenosis: Insights from the CORAL Trial Christopher J. Cooper, M.D., FACC, FACP Dean and Senior Vice President University of Toledo, College of Medicine President, Ohio Chapter ACC State of
Appropriate Patient Identification For Renal Artery Intervention Remains Challenging
 Renal Intervention Herbert D. Aronow, MD, MPH, FACC, FSCAI, FSVM Director, Interventional Cardiology, Cardiovascular Institute Director, Cardiac Cath Labs, Rhode Island &The Miriam Hospitals None Disclosures
Renal Intervention Herbert D. Aronow, MD, MPH, FACC, FSCAI, FSVM Director, Interventional Cardiology, Cardiovascular Institute Director, Cardiac Cath Labs, Rhode Island &The Miriam Hospitals None Disclosures
Coral Trials: A personal experience that challenges its results in patients with uncontrolled blood pressure.
 Coral Trials: A personal experience that challenges its results in patients with uncontrolled blood pressure.. Dr. Javier Ruiz Aburto, FACS, FICS Assistant Professor Ponce School of Medicine Puerto Rico
Coral Trials: A personal experience that challenges its results in patients with uncontrolled blood pressure.. Dr. Javier Ruiz Aburto, FACS, FICS Assistant Professor Ponce School of Medicine Puerto Rico
Renal Intervention. Douglas E. Drachman, MD, FSCAI Division of Cardiology Vascular Medicine Section December 9, 2014
 Renal Intervention Douglas E. Drachman, MD, FSCAI Division of Cardiology Vascular Medicine Section December 9, 2014 Disclosure Information Douglas E. Drachman, MD, FACC Abbott Vascular, Inc.: Advisory
Renal Intervention Douglas E. Drachman, MD, FSCAI Division of Cardiology Vascular Medicine Section December 9, 2014 Disclosure Information Douglas E. Drachman, MD, FACC Abbott Vascular, Inc.: Advisory
PCI for Renal Artery stenosis
 PCI for Renal Artery stenosis Why should we treat Renal Artery Stenosis? Natural History of RAS RAS is progressive disease Study Follow-up (months) Pts Progression N (%) Total occlusion Wollenweber Meaney
PCI for Renal Artery stenosis Why should we treat Renal Artery Stenosis? Natural History of RAS RAS is progressive disease Study Follow-up (months) Pts Progression N (%) Total occlusion Wollenweber Meaney
Effective Health Care
 Number 5 Effective Health Care Comparative Effectiveness of Management Strategies for Renal Artery Stenosis Executive Summary Background Renal artery stenosis (RAS) is defined as the narrowing of the lumen
Number 5 Effective Health Care Comparative Effectiveness of Management Strategies for Renal Artery Stenosis Executive Summary Background Renal artery stenosis (RAS) is defined as the narrowing of the lumen
Renal artery stenosis (RAS) is a relatively common
 The Importance of Appropriate Renal Artery Stenting Considerations for diagnosis and treatment of patients with renal artery stenosis. By Massoud A. Leesar, MD, FACC, FSCAI Renal artery stenosis (RAS)
The Importance of Appropriate Renal Artery Stenting Considerations for diagnosis and treatment of patients with renal artery stenosis. By Massoud A. Leesar, MD, FACC, FSCAI Renal artery stenosis (RAS)
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Duplex Ultrasound of the Renal Arteries. Duplex Ultrasound. In the Beginning
 Duplex Ultrasound of the Renal Arteries DIMENSIONS IN HEART AND VASCULAR CARE 2013 PENN STATE HEART AND VASCULAR INSTITUTE ROBERT G. ATNIP MD PROFESSOR OF SURGERY AND RADIOLOGY Duplex Ultrasound Developed
Duplex Ultrasound of the Renal Arteries DIMENSIONS IN HEART AND VASCULAR CARE 2013 PENN STATE HEART AND VASCULAR INSTITUTE ROBERT G. ATNIP MD PROFESSOR OF SURGERY AND RADIOLOGY Duplex Ultrasound Developed
Renal artery stenosis
 Renal artery stenosis Dr. Alexander Woywodt Consultant Renal Physician, Royal Preston Hospital Preston, 31.10.2007 Menu anatomy of the renal arteries diseases of the large renal arteries atherosclerotic
Renal artery stenosis Dr. Alexander Woywodt Consultant Renal Physician, Royal Preston Hospital Preston, 31.10.2007 Menu anatomy of the renal arteries diseases of the large renal arteries atherosclerotic
A Closer Look: Renal Artery Stenosis. Renal artery stenosis (RAS) is defined as a TOPICS FROM CHEP. Shawn s stenosis
 TOPICS FROM CHEP A Closer Look: Renal Artery Stenosis On behalf of the Canadian Hypertension Education Program (CHEP), Dr. Tobe gives an overview of renal artery stenosis, including the prevalence, screening
TOPICS FROM CHEP A Closer Look: Renal Artery Stenosis On behalf of the Canadian Hypertension Education Program (CHEP), Dr. Tobe gives an overview of renal artery stenosis, including the prevalence, screening
Disclosure of Potential Conflicts. Renal Artery Stenosis. RAS Epidemiology. Road Map. Background. ASDIN 7th Annual Scientific Meeting
 Renal Artery Stenosis Disclosure of Potential Conflicts Cytopherx, Inc. R4 Vascular, Inc. Bard Peripheral Vascular Spectranetics, Inc. Alexander S. Yevzlin, MD Associate Professor of Medicine (CHS) ASDIN
Renal Artery Stenosis Disclosure of Potential Conflicts Cytopherx, Inc. R4 Vascular, Inc. Bard Peripheral Vascular Spectranetics, Inc. Alexander S. Yevzlin, MD Associate Professor of Medicine (CHS) ASDIN
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Renal Artery Disease. None > 65,000,000. Learning objectives: Renal Artery Disease
 Renal Artery Disease Robert D. McBane, M.D. Division of Cardiology Mayo Clinic Rochester Financial Disclosure Information Renal Artery Disease Robert McBane, MD None To appreciate: Learning objectives:
Renal Artery Disease Robert D. McBane, M.D. Division of Cardiology Mayo Clinic Rochester Financial Disclosure Information Renal Artery Disease Robert McBane, MD None To appreciate: Learning objectives:
Interventional Cardiology
 nal Review Interventional Cardiology Selecting patients likely to benefit from renal artery stenting Patients with refractory hypertension, progressive ischemic nephropathy and cardiac destabilization
nal Review Interventional Cardiology Selecting patients likely to benefit from renal artery stenting Patients with refractory hypertension, progressive ischemic nephropathy and cardiac destabilization
Masahiko Fujihara, MD
 Verify the efficacy of renal artery stenting to define the predictive factors by physiological assessment with pressure wire gradient VERDICT study Masahiko Fujihara, MD Kishiwada Tokushukai Hospital Osaka,
Verify the efficacy of renal artery stenting to define the predictive factors by physiological assessment with pressure wire gradient VERDICT study Masahiko Fujihara, MD Kishiwada Tokushukai Hospital Osaka,
Peripheral Arterial Disease: Who has it and what to do about it?
 Peripheral Arterial Disease: Who has it and what to do about it? Seth Krauss, M.D. Alaska Annual Nurse Practitioner Conference September 16, 2011 Scope of the Problem Incidence: 20%
Peripheral Arterial Disease: Who has it and what to do about it? Seth Krauss, M.D. Alaska Annual Nurse Practitioner Conference September 16, 2011 Scope of the Problem Incidence: 20%
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Fibromuscular Dysplasia (FMD) of the renal arteries Angiographic features and therapeutic options
 Fibromuscular Dysplasia (FMD) of the renal arteries Angiographic features and therapeutic options Poster No.: C-0630 Congress: ECR 2012 Type: Educational Exhibit Authors: K. I. Ringe, B. Meyer, F. Wacker,
Fibromuscular Dysplasia (FMD) of the renal arteries Angiographic features and therapeutic options Poster No.: C-0630 Congress: ECR 2012 Type: Educational Exhibit Authors: K. I. Ringe, B. Meyer, F. Wacker,
Michael Meuse, M.D. Vascular and Interventional Radiology
 Michael Meuse, M.D. Vascular and Interventional Radiology Which patient would likely benefit from renal artery revascularization? Patient A- 60 y/o male with 20 year hx of htn; on 2 drug therapy for 10
Michael Meuse, M.D. Vascular and Interventional Radiology Which patient would likely benefit from renal artery revascularization? Patient A- 60 y/o male with 20 year hx of htn; on 2 drug therapy for 10
ACCF/ACR/AIUM/ASE/ASN/ICAVL/SCAI/SCCT/SIR/SVM/SVS 2012 Appropriate Use Criteria. Indications A _ appropriate; I _ inappropriate; U _ uncertain
 National Imaging Associates, Inc. Clinical guidelines ABDOMINAL, PELVIS, SCROTAL, RETROPERITONEAL ORGANS DUPLEX SCAN (US) CPT Codes: 93975 Bilateral or Complete 93976 - Unilateral or Limited Guideline
National Imaging Associates, Inc. Clinical guidelines ABDOMINAL, PELVIS, SCROTAL, RETROPERITONEAL ORGANS DUPLEX SCAN (US) CPT Codes: 93975 Bilateral or Complete 93976 - Unilateral or Limited Guideline
Evaluation of the Safety and Effectiveness of Renal Artery Stenting After Unsuccessful Balloon Angioplasty The ASPIRE-2 Study
 Journal of the American College of Cardiology Vol. 46, No. 5, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.073
Journal of the American College of Cardiology Vol. 46, No. 5, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.11.073
NOT FOR PUBLICATION, QUOTATION, OR CITATION RESOLUTION NO. 22
 BE IT RESOLVED, Sponsored By: RESOLUTION NO. 22 that the American College of Radiology adopt the ACR SIR Practice Parameter for the Performance of Angiography, Angioplasty, and Stenting for the Diagnosis
BE IT RESOLVED, Sponsored By: RESOLUTION NO. 22 that the American College of Radiology adopt the ACR SIR Practice Parameter for the Performance of Angiography, Angioplasty, and Stenting for the Diagnosis
Atherosclerotic Renovascular Hypertension : Lessons from Recent Clinical Studies
 Review ISSN 1738-5997 (Print) ISSN 2092-9935 (Online) Electrolyte Blood Press 8:87-91, 2010 doi: 10.5049/EBP.2010.8.2.87 Atherosclerotic Renovascular Hypertension : Lessons from Recent Clinical Studies
Review ISSN 1738-5997 (Print) ISSN 2092-9935 (Online) Electrolyte Blood Press 8:87-91, 2010 doi: 10.5049/EBP.2010.8.2.87 Atherosclerotic Renovascular Hypertension : Lessons from Recent Clinical Studies
VCU Pauley Heart Center: A 2009 US News Top 50 Heart and Heart Surgery Hospital
 VCU Pauley Heart Center: A 2009 US News Top 50 Heart and Heart Surgery Hospital Complex PCI: Multivessel Disease George W. Vetrovec, MD. Kimmerling Chair of Cardiology VCU Pauley Heart Center Virginia
VCU Pauley Heart Center: A 2009 US News Top 50 Heart and Heart Surgery Hospital Complex PCI: Multivessel Disease George W. Vetrovec, MD. Kimmerling Chair of Cardiology VCU Pauley Heart Center Virginia
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Diagnosis of Renal Artery Stenosis (RAS)
 May 2001 Diagnosis of Renal Artery Stenosis (RAS) Kurt Fink, Harvard Medical School, Year III Epidemiology Hypertension -Affects 60 million Americans Essential HTN >95% of cases Secondary HTN 1-5% of cases
May 2001 Diagnosis of Renal Artery Stenosis (RAS) Kurt Fink, Harvard Medical School, Year III Epidemiology Hypertension -Affects 60 million Americans Essential HTN >95% of cases Secondary HTN 1-5% of cases
Endovascular treatment of transplant renal artery stenosis based on hemodynamic assessment using a pressure wire: a case report
 Kadoya et al. BMC Cardiovascular Disorders (2018) 18:172 https://doi.org/10.1186/s12872-018-0909-y CASE REPORT Open Access Endovascular treatment of transplant renal artery stenosis based on hemodynamic
Kadoya et al. BMC Cardiovascular Disorders (2018) 18:172 https://doi.org/10.1186/s12872-018-0909-y CASE REPORT Open Access Endovascular treatment of transplant renal artery stenosis based on hemodynamic
Anatomy is Destiny, But Physiology is Here Today
 Published on Journal of Invasive Cardiology (http://www.invasivecardiology.com) September, 2010 [1] Anatomy is Destiny, But Physiology is Here Today Thu, 9/9/10-10:54am 0 Comments Section: Commentary Issue
Published on Journal of Invasive Cardiology (http://www.invasivecardiology.com) September, 2010 [1] Anatomy is Destiny, But Physiology is Here Today Thu, 9/9/10-10:54am 0 Comments Section: Commentary Issue
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Fractional Flow Reserve: Basics, FAME 1, FAME 2. William F. Fearon, MD Associate Professor Stanford University Medical Center
 Fractional Flow Reserve: Basics, FAME 1, FAME 2 William F. Fearon, MD Associate Professor Stanford University Medical Center Conflict of Interest Advisory Board for HeartFlow Research grant from St. Jude
Fractional Flow Reserve: Basics, FAME 1, FAME 2 William F. Fearon, MD Associate Professor Stanford University Medical Center Conflict of Interest Advisory Board for HeartFlow Research grant from St. Jude
Renal Artery Stenting With Embolic Protection
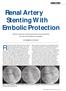 Renal Artery Stenting With Embolic Protection Embolic protection during renal stenting may be beneficial, but new device designs are necessary. BY RAJESH M. DAVE, MD Renal artery stenosis (RAS) is the
Renal Artery Stenting With Embolic Protection Embolic protection during renal stenting may be beneficial, but new device designs are necessary. BY RAJESH M. DAVE, MD Renal artery stenosis (RAS) is the
The Centers for Medicare & Medicaid Services
 Percutaneous Renal Revascularization and Medicare Coverage The Society of Interventional Radiology s position on the current CMS coverage of renal interventions. BY DAVID SACKS, MD, AND TIMOTHY P. MURPHY,
Percutaneous Renal Revascularization and Medicare Coverage The Society of Interventional Radiology s position on the current CMS coverage of renal interventions. BY DAVID SACKS, MD, AND TIMOTHY P. MURPHY,
IN.PACT AV Access IDE Study Full Baseline Data. Robert Lookstein, MD MHCDL New York, NY On Behalf of the IN.PACT AV ACCESS Investigators
 IN.PACT AV Access IDE Study Full Baseline Data Robert Lookstein, MD MHCDL New York, NY On Behalf of the IN.PACT AV ACCESS Investigators Disclosures Speaker name: Robert Lookstein, MD... I have the following
IN.PACT AV Access IDE Study Full Baseline Data Robert Lookstein, MD MHCDL New York, NY On Behalf of the IN.PACT AV ACCESS Investigators Disclosures Speaker name: Robert Lookstein, MD... I have the following
RAS Epidemiology. Renal Artery Stenosis. Pathophysiology of RAS. Disclosure of Potential Conflicts. Background Pathophysiology of RAS.
 Renal Artery Stenosis RAS Epidemiology Common Disease Incidence General Population 0.1% Hypertensive Population 4% HTN & Suspected CAD 10-20% Malignant HTN 20-30% Malignant HTN and CKD 30-40% Alexander
Renal Artery Stenosis RAS Epidemiology Common Disease Incidence General Population 0.1% Hypertensive Population 4% HTN & Suspected CAD 10-20% Malignant HTN 20-30% Malignant HTN and CKD 30-40% Alexander
RAPID Phase III Perspectives from the Medical Device Industry
 RAPID Phase III Perspectives from the Medical Device Industry Megan M. Brandt Vice President, Quality and Regulatory Affairs Cardiovascular Systems, Inc. St. Paul, MN PAD and Critical Limb Ischemia: Disease
RAPID Phase III Perspectives from the Medical Device Industry Megan M. Brandt Vice President, Quality and Regulatory Affairs Cardiovascular Systems, Inc. St. Paul, MN PAD and Critical Limb Ischemia: Disease
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
Prospective, randomized controlled study of paclitaxel-coated versus plain balloon angioplasty for the treatment of failing dialysis access
 Prospective, randomized controlled study of paclitaxel-coated versus plain balloon angioplasty for the treatment of failing dialysis access Disclosure Speaker name:... I have the following potential conflicts
Prospective, randomized controlled study of paclitaxel-coated versus plain balloon angioplasty for the treatment of failing dialysis access Disclosure Speaker name:... I have the following potential conflicts
US of Renovascular Hypertension. Jonathan R. Dillman, MD, MSc Associate Professor Director, Thoracoabdominal Imaging
 US of Renovascular Hypertension Jonathan R. Dillman, MD, MSc Associate Professor Director, Thoracoabdominal Imaging Disclosures Nothing Relevant Unrelated grant funding Siemens US Toshiba US Objectives
US of Renovascular Hypertension Jonathan R. Dillman, MD, MSc Associate Professor Director, Thoracoabdominal Imaging Disclosures Nothing Relevant Unrelated grant funding Siemens US Toshiba US Objectives
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Treatment Options for Angina
 Treatment Options for Angina Interventional Cardiology Perspective Michael A. Robertson, M.D. 10/30/10 Prevalence of CAD in USA 15 million Americans with CAD 2 million diagnostic catheterizations 1 million
Treatment Options for Angina Interventional Cardiology Perspective Michael A. Robertson, M.D. 10/30/10 Prevalence of CAD in USA 15 million Americans with CAD 2 million diagnostic catheterizations 1 million
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
A Novel Simple Technique Using Hyperemia to Enhance Pressure Gradient Measurement of the Lower Extremity During Peripheral Intervention
 A Novel Simple Technique Using Hyperemia to Enhance Pressure Gradient Measurement of the Lower Extremity During Peripheral Intervention Issam Koleilat, MD; Bruce Gray, MD From Greenville Health System,
A Novel Simple Technique Using Hyperemia to Enhance Pressure Gradient Measurement of the Lower Extremity During Peripheral Intervention Issam Koleilat, MD; Bruce Gray, MD From Greenville Health System,
Outcomes Of DCB Use In Real World Registries: 2 Year Results From The INPACT Global Registry
 Outcomes Of DCB Use In Real World Registries: 2 Year Results From The INPACT Global Registry Marianne Brodmann, MD Head of the Clinical Division of Angiology Department of Internal Medicine Medical University
Outcomes Of DCB Use In Real World Registries: 2 Year Results From The INPACT Global Registry Marianne Brodmann, MD Head of the Clinical Division of Angiology Department of Internal Medicine Medical University
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Left Main Intervention: Will it become standard of care?
 Left Main Intervention: Will it become standard of care? David Cox, MD FSCAI, FACC Director, Interventional Cardiology Research Associate Director, Cardiac Cath Lab Lehigh Valley Health Network Allentown,
Left Main Intervention: Will it become standard of care? David Cox, MD FSCAI, FACC Director, Interventional Cardiology Research Associate Director, Cardiac Cath Lab Lehigh Valley Health Network Allentown,
DCB use in fem-pop lesions of patients with CLI (RCC 4-5): subgroup analysis of IN.PACT Global 12-month outcomes
 DCB use in fem-pop lesions of patients with CLI (RCC 4-5): subgroup analysis of IN.PACT Global 12-month outcomes Carlos Mena, MD FACC FSCAI Associate Professor of Medicine - Cardiology Director Cardiac
DCB use in fem-pop lesions of patients with CLI (RCC 4-5): subgroup analysis of IN.PACT Global 12-month outcomes Carlos Mena, MD FACC FSCAI Associate Professor of Medicine - Cardiology Director Cardiac
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E39-E41 A Case With Successful Retrograde Stent Delivery via AC Branch for Tortuous Right Coronary Artery Yoshiki Uehara, MD, PhD, Mitsuyuki Shimizu, MD, PhD,
Case Report J INVASIVE CARDIOL 2013;25(2):E39-E41 A Case With Successful Retrograde Stent Delivery via AC Branch for Tortuous Right Coronary Artery Yoshiki Uehara, MD, PhD, Mitsuyuki Shimizu, MD, PhD,
VIRTUS: Trial Design and Primary Endpoint Results
 VIRTUS: Trial Design and Primary Endpoint Results Mahmood K. Razavi, MD St. Joseph Cardiac and Vascular Center Orange, CA, USA IMPORTANT INFORMATION: These materials are intended to describe common clinical
VIRTUS: Trial Design and Primary Endpoint Results Mahmood K. Razavi, MD St. Joseph Cardiac and Vascular Center Orange, CA, USA IMPORTANT INFORMATION: These materials are intended to describe common clinical
Renal Artery Stenosis With Severe Hypertension: A Case Report
 CASE REPORT Renal Artery Stenosis With Severe Hypertension: A Case Report Suwaid MA ABSTRACT Background: Renal artery stenosis (RAS) is found in 77% of hypertensive patients and is responsible for 1-2%
CASE REPORT Renal Artery Stenosis With Severe Hypertension: A Case Report Suwaid MA ABSTRACT Background: Renal artery stenosis (RAS) is found in 77% of hypertensive patients and is responsible for 1-2%
Patterns of Vessel Calcification and Clinical Relevance
 Patterns of Vessel Calcification and Clinical Relevance Michael R. Jaff, DO Paul and Phyllis Fireman Endowed Chair in Vascular Medicine Massachusetts General Hospital Professor of Medicine Harvard Medical
Patterns of Vessel Calcification and Clinical Relevance Michael R. Jaff, DO Paul and Phyllis Fireman Endowed Chair in Vascular Medicine Massachusetts General Hospital Professor of Medicine Harvard Medical
Coronary Artery Manifestations of Fibromuscular Dysplasia: Infrequent and Easily Missed
 Coronary Artery Manifestations of Fibromuscular Dysplasia: Infrequent and Easily Missed Jeffrey W Olin, D.O., F.A.C.C., F.A.H.A. Professor of Medicine (Cardiology) Director of Vascular Medicine & Vascular
Coronary Artery Manifestations of Fibromuscular Dysplasia: Infrequent and Easily Missed Jeffrey W Olin, D.O., F.A.C.C., F.A.H.A. Professor of Medicine (Cardiology) Director of Vascular Medicine & Vascular
MEET /06/2013 SESSION : RENAL AND VISCERAL
 MEET 2003 11/06/2013 SESSION : RENAL AND VISCERAL AFTER 35 YEARS, WHAT ARE THE INDICATIONS AND RESULTS OF PTRA IN PATIENTS WITH RI OR RVH? THOMAS SOS, MD NYPH CORNELL New York, NY THOMAS SOS, MD NYPH CORNELL
MEET 2003 11/06/2013 SESSION : RENAL AND VISCERAL AFTER 35 YEARS, WHAT ARE THE INDICATIONS AND RESULTS OF PTRA IN PATIENTS WITH RI OR RVH? THOMAS SOS, MD NYPH CORNELL New York, NY THOMAS SOS, MD NYPH CORNELL
Intervention for Deep Venous Thrombosis and Pulmonary Embolus
 Intervention for Deep Venous Thrombosis and Pulmonary Embolus Michael R. Jaff, DO Paul and Phyllis Fireman Endowed Chair in Vascular Medicine Massachusetts General Hospital Professor of Medicine Harvard
Intervention for Deep Venous Thrombosis and Pulmonary Embolus Michael R. Jaff, DO Paul and Phyllis Fireman Endowed Chair in Vascular Medicine Massachusetts General Hospital Professor of Medicine Harvard
Diagnosis and management of atherosclerotic renal artery stenosis: improving patient selection and outcomes
 Diagnosis and management of atherosclerotic renal artery stenosis: improving patient selection and outcomes Christopher J White* and Jeffrey W Olin SuMMarY Renal artery stenosis (RAS) is common among patients
Diagnosis and management of atherosclerotic renal artery stenosis: improving patient selection and outcomes Christopher J White* and Jeffrey W Olin SuMMarY Renal artery stenosis (RAS) is common among patients
Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report
 Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report The Leipzig Interventional Course, January 24 27, 2017 El Samman K., Šedivý P., Šnajdrová A., Přindišová
Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report The Leipzig Interventional Course, January 24 27, 2017 El Samman K., Šedivý P., Šnajdrová A., Přindišová
Treatment of renal artery in-stent restenosis with sirolimus-eluting stents
 Treatment of renal artery in-stent restenosis with sirolimus-eluting stents Vascular Medicine 15(1) 3 7 The Author(s) 2009 Reprints and permission: http://www. sagepub.co.uk/journalspermission.nav DOI:
Treatment of renal artery in-stent restenosis with sirolimus-eluting stents Vascular Medicine 15(1) 3 7 The Author(s) 2009 Reprints and permission: http://www. sagepub.co.uk/journalspermission.nav DOI:
Incidence and Prevalence of Atherosclerotic Renal Artery Stenosis (RAS) in Patients with Coronary Artery Disease (CAD)
 Incidence and Prevalence of Atherosclerotic Renal Artery Stenosis (RAS) in Patients with Coronary Artery Disease (CAD) AHMW Islam, S Munwar, S Talukder, AQM Reza Dept. of Invasive & Interventional Cardiology,
Incidence and Prevalence of Atherosclerotic Renal Artery Stenosis (RAS) in Patients with Coronary Artery Disease (CAD) AHMW Islam, S Munwar, S Talukder, AQM Reza Dept. of Invasive & Interventional Cardiology,
Larry Diaz, MD, FSCAI Mehdi H. Shishehbor, DO, FSCAI
 PAD Diagnosis Larry Diaz, MD, FSCAI Metro Health / University of Michigan Health, Wyoming, MI Mehdi H. Shishehbor, DO, FSCAI University Hospitals Harrington Heart & Vascular Institute, Cleveland, OH PAD:
PAD Diagnosis Larry Diaz, MD, FSCAI Metro Health / University of Michigan Health, Wyoming, MI Mehdi H. Shishehbor, DO, FSCAI University Hospitals Harrington Heart & Vascular Institute, Cleveland, OH PAD:
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
KEY WORDS: Bilateral Renal Artery Stenosis, Cardiac Catherization, Incidental Findings, Associated Co- morbidity
 BILATERAL RENAL ARTERY STENOSIS - AN INCIDENTAL FINDING DURING CARDIAC CATHETERIZATION Review of 15 Cases of BRAS Stenting at Queen Alia Heart Institute in Jordan Hatem Hamdan Salaheen Abbadi 1 ABSTRACT:
BILATERAL RENAL ARTERY STENOSIS - AN INCIDENTAL FINDING DURING CARDIAC CATHETERIZATION Review of 15 Cases of BRAS Stenting at Queen Alia Heart Institute in Jordan Hatem Hamdan Salaheen Abbadi 1 ABSTRACT:
Controversies in the management of the renal artery stenosis
 REVIEW ARTICLE Cardiology Journal 2013, Vol. 20, No. 1, pp. 11 16 10.5603/CJ.2013.0003 Copyright 2013 Via Medica ISSN 1897 5593 Controversies in the management of the renal artery stenosis Khalil Kanjwal
REVIEW ARTICLE Cardiology Journal 2013, Vol. 20, No. 1, pp. 11 16 10.5603/CJ.2013.0003 Copyright 2013 Via Medica ISSN 1897 5593 Controversies in the management of the renal artery stenosis Khalil Kanjwal
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Contrast Induced Nephropathy
 Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
Premier Health Plan considers Intravascular Ultrasound (IVUS) for Coronary Vessels medically necessary for the following indications:
 Premier Health Plan POLICY AND PROCEDURE MANUAL MP.091.PH - Intravascular Ultrasound for Coronary Vessels This policy applies to the following lines of business: Premier Commercial Premier Employee Premier
Premier Health Plan POLICY AND PROCEDURE MANUAL MP.091.PH - Intravascular Ultrasound for Coronary Vessels This policy applies to the following lines of business: Premier Commercial Premier Employee Premier
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
2019 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule
 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
Assessment of recurrent mesenteric ischemia after stenting with a pressure wire
 524852VMJ0010.1177/1358863X14524852Vascular MedicineMargiotta and Gray research-article2014 Case Report Assessment of recurrent mesenteric ischemia after stenting with a pressure wire Vascular Medicine
524852VMJ0010.1177/1358863X14524852Vascular MedicineMargiotta and Gray research-article2014 Case Report Assessment of recurrent mesenteric ischemia after stenting with a pressure wire Vascular Medicine
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
FFR Incorporating & Expanding it s use in Clinical Practice
 FFR Incorporating & Expanding it s use in Clinical Practice Suleiman Kharabsheh, MD Consultant Invasive Cardiology Assistant professor, Alfaisal Univ. KFHI - KFSHRC Concept of FFR Maximum flow down a vessel
FFR Incorporating & Expanding it s use in Clinical Practice Suleiman Kharabsheh, MD Consultant Invasive Cardiology Assistant professor, Alfaisal Univ. KFHI - KFSHRC Concept of FFR Maximum flow down a vessel
The Utility of Atherectomy and the Jetstream Atherectomy System
 The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
How to manage TAVI related vascular complications. Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI
 How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
PCIs on Intermediate Lesions NCDR Cath-PCI Registry
 Practical Application Of Coronary Physiology in The Cath Lab Talal T Attar, MD, MBA, FACC PCIs on Intermediate Lesions NCDR Cath-PCI Registry Fraction of stenoses 50-70% treated with PCI without further
Practical Application Of Coronary Physiology in The Cath Lab Talal T Attar, MD, MBA, FACC PCIs on Intermediate Lesions NCDR Cath-PCI Registry Fraction of stenoses 50-70% treated with PCI without further
Renal Artery Stenting
 Renal Artery Stenting We are unable to predict patients who will benefit from RAS MEET 2008 Thomas Ischinger MD FACC FESC Heart Center Bogenhausen Munich, Germany Disclosure Statement of Financial Interest
Renal Artery Stenting We are unable to predict patients who will benefit from RAS MEET 2008 Thomas Ischinger MD FACC FESC Heart Center Bogenhausen Munich, Germany Disclosure Statement of Financial Interest
Secondary Hypertension: A Real World Approach
 Secondary Hypertension: A Real World Approach Evan Brittain, MD December 7, 2012 Kingston, Jamaica Disclosures None Real World Causes Renovascular Hypertension Endocrine Obstructive Sleep Apnea Pseudosecondary
Secondary Hypertension: A Real World Approach Evan Brittain, MD December 7, 2012 Kingston, Jamaica Disclosures None Real World Causes Renovascular Hypertension Endocrine Obstructive Sleep Apnea Pseudosecondary
Coronary angiography and PCI
 Coronary arteries Coronary angiography and PCI Samo Granda, Franjo Naji Department of Cardiology Clinical department of internal medicine University clinical centre Maribor Coronary arteries Atherosclerosis
Coronary arteries Coronary angiography and PCI Samo Granda, Franjo Naji Department of Cardiology Clinical department of internal medicine University clinical centre Maribor Coronary arteries Atherosclerosis
Renal PEI: critical appraisal
 Renal PEI: critical appraisal On Topaz M.D., F.A.C.C.,F.S.V.M. Professor of Medicine & Pathology Director, Interventional Cardiology McGuire Veterans Medical Center Virginia Commonwealth University Richmond,
Renal PEI: critical appraisal On Topaz M.D., F.A.C.C.,F.S.V.M. Professor of Medicine & Pathology Director, Interventional Cardiology McGuire Veterans Medical Center Virginia Commonwealth University Richmond,
Minimally Invasive Treatment Options for Renal Artery FMD
 Minimally Invasive Treatment Options for Renal Artery FMD FMDSA Meeting 2016 Alan H. Matsumoto, M.D., FSIR, FACR, FAHA Professor and Chair Department of Radiology & Medical Imaging University of Virginia
Minimally Invasive Treatment Options for Renal Artery FMD FMDSA Meeting 2016 Alan H. Matsumoto, M.D., FSIR, FACR, FAHA Professor and Chair Department of Radiology & Medical Imaging University of Virginia
(EU), FACC (USA), FSCAI (USA)
 How to reduce vascular complications of TAVI Paul TL Chiam MBBS (S pore), MMed, MRCP (UK), FAMS FRCP (Edin), FESC (EU), FACC (USA), FSCAI (USA) Cardiologist Mount Elizabeth Hospital Singapore Definition
How to reduce vascular complications of TAVI Paul TL Chiam MBBS (S pore), MMed, MRCP (UK), FAMS FRCP (Edin), FESC (EU), FACC (USA), FSCAI (USA) Cardiologist Mount Elizabeth Hospital Singapore Definition
DETECT-PAD Computerized and patient specific model to determine pressure gradients in borderline iliac artery stenosis with MRA/ CTA
 DETECT-PAD Computerized and patient specific model to determine pressure gradients in borderline iliac artery stenosis with MRA/ CTA Jean-Paul P.M. de Vries Head Department of Surgery University Medical
DETECT-PAD Computerized and patient specific model to determine pressure gradients in borderline iliac artery stenosis with MRA/ CTA Jean-Paul P.M. de Vries Head Department of Surgery University Medical
Left Main Intervention: Where are we in 2015?
 Left Main Intervention: Where are we in 2015? David A. Cox, MD FSCAI Director, Cardiology Research Associate Director, Cardiac Cath Lab Lehigh Valley Health Network Allentown, PA Fall Fellows Course Laa
Left Main Intervention: Where are we in 2015? David A. Cox, MD FSCAI Director, Cardiology Research Associate Director, Cardiac Cath Lab Lehigh Valley Health Network Allentown, PA Fall Fellows Course Laa
Instantaneous Wave-Free Ratio
 Instantaneous Wave-Free Ratio Alejandro Aquino MD Interventional Cardiology Fellow Washington University in St. Louis Barnes-Jewish Hospital Instantaneous Wave-Free Ratio Alejandro Aquino MD Disclosure
Instantaneous Wave-Free Ratio Alejandro Aquino MD Interventional Cardiology Fellow Washington University in St. Louis Barnes-Jewish Hospital Instantaneous Wave-Free Ratio Alejandro Aquino MD Disclosure
FRACTIONAL FLOW RESERVE: STANDARD OF CARE
 FRACTIONAL FLOW RESERVE: FROM INVESTIGATIONAL TOOL TO STANDARD OF CARE TCT ASIA Seoul, Korea, april 26 th, 2012 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands FRACTIONAL FLOW
FRACTIONAL FLOW RESERVE: FROM INVESTIGATIONAL TOOL TO STANDARD OF CARE TCT ASIA Seoul, Korea, april 26 th, 2012 Nico H. J. Pijls, MD, PhD Catharina Hospital, Eindhoven, The Netherlands FRACTIONAL FLOW
FFR and intravascular imaging, which of which?
 FFR and intravascular imaging, which of which? Ayman Khairy MD, PhD, FESC Associate professor of Cardiovascular Medicine Vice Director of Assiut University Hospitals Assiut, Egypt Diagnostic assessment
FFR and intravascular imaging, which of which? Ayman Khairy MD, PhD, FESC Associate professor of Cardiovascular Medicine Vice Director of Assiut University Hospitals Assiut, Egypt Diagnostic assessment
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
9/7/2018. Disclosures. CV and Limb Events in PAD. Challenges to Revascularization. Challenges. Answering the Challenge
 Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Case yr old lady; type 2 Diabetes 10 yrs; PVD; hypertension
 Does this patient have flash pulmonary oedema? Philip A Kalra Professor of Nephrology, Salford Royal Hospital and University of Manchester, UK 73 yr old lady; type 2 Diabetes 1 yrs; PVD; hypertension Acute
Does this patient have flash pulmonary oedema? Philip A Kalra Professor of Nephrology, Salford Royal Hospital and University of Manchester, UK 73 yr old lady; type 2 Diabetes 1 yrs; PVD; hypertension Acute
The results of EVT for Chronic Aortic Occlusion - a multicenter retrospective study - Taku Kato, MD Rakuwakai Otowa Hospital, Kyoto, Japan
 The results of EVT for Chronic Aortic Occlusion - a multicenter retrospective study - Taku Kato, MD Rakuwakai Otowa Hospital, Kyoto, Japan COI disclosure Disclosure Speaker name: Taku Kato... I have the
The results of EVT for Chronic Aortic Occlusion - a multicenter retrospective study - Taku Kato, MD Rakuwakai Otowa Hospital, Kyoto, Japan COI disclosure Disclosure Speaker name: Taku Kato... I have the
REBEL. Platinum Chromium Coronary Stent System. Patient Information Guide
 REBEL Patient Information Guide REBEL PATIENT INFORMATION GUIDE You have recently had a REBEL bare metal stent implanted in the coronary arteries of your heart. The following information is important for
REBEL Patient Information Guide REBEL PATIENT INFORMATION GUIDE You have recently had a REBEL bare metal stent implanted in the coronary arteries of your heart. The following information is important for
Imaging for Peripheral Vascular Disease
 Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Do stents deserve the bad press? Mark A. Tulli MD, FACC
 Do stents deserve the bad press? Mark A. Tulli MD, FACC Disclosures: None Introduction Stents don t help people. Stents are bad for patients. Heart Treatment Overused WSJ Study Finds Doctors Often Too
Do stents deserve the bad press? Mark A. Tulli MD, FACC Disclosures: None Introduction Stents don t help people. Stents are bad for patients. Heart Treatment Overused WSJ Study Finds Doctors Often Too
The major issues in approaching patients with renal artery stenosis
 Renovascular Hypertension and Ischemic Nephropathy Marc A. Pohl The major issues in approaching patients with renal artery stenosis relate to the role of renal artery stenosis in the management of hypertension,
Renovascular Hypertension and Ischemic Nephropathy Marc A. Pohl The major issues in approaching patients with renal artery stenosis relate to the role of renal artery stenosis in the management of hypertension,
Ostial Stents and Distal Embolic Protection During Renal Stenting
 Ostial Stents and Distal Embolic Protection During Renal Stenting John R. Laird, MD Professor of Medicine Director of the Vascular Center UC Davis Medical Center Limitations of Current Techniques of Renal
Ostial Stents and Distal Embolic Protection During Renal Stenting John R. Laird, MD Professor of Medicine Director of the Vascular Center UC Davis Medical Center Limitations of Current Techniques of Renal
