A validation study of a new nasogastric polyfunctional catheter
|
|
|
- Reginald Gibson
- 6 years ago
- Views:
Transcription
1 Intensive Care Med DOI 1.17/s ORIGINAL D. Chiumello E. Gallazzi A. Marino V. Berto C. Mietto B. Cesana L. Gattinoni A validation study of a new nasogastric polyfunctional catheter Received: 4 August 1 Accepted: 4 November 1 Ó Copyright jointly held by Springer and ESICM 11 D. Chiumello and L. Gattinoni participated in the development of Nutrivent, but do not have any patent or financial agreement, and received only an honorarium as members of the advisory board. D. Chiumello ()) V. Berto C. Mietto L. Gattinoni Dipartimento di Anestesia, Rianimazione (Intensiva e Subintensiva) e Terapia del Dolore, Fondazione IRCCS Ca Granda, Ospedale Maggiore Policlinico, Via Francesco Sforza 35, 1 Milan, Italy chiumello@libero.it Tel.:? Fax:? E. Gallazzi A. Marino Dipartimento di Anestesiologia, Terapia Intensiva e Scienze Dermatologiche, Università degli Studi di Milano, Milan, Italy B. Cesana Unità di Statistica Medica e Biometria, Dipartimento di Scienze Biomediche e Biotecnologie, Università degli Studi di Brescia, Brescia, Italy Abstract Purpose: Pleural and abdominal pressure are clinically estimated by measuring the esophageal and bladder or intragastric pressure (IGP), respectively. A new nasogastric polyfunctional catheter is now commercially available, equipped with two balloons in the lower and distal part; this catheter allows simultaneous esophageal pressure (Pes) and IGP measurements and can be also used to feed the patient. We compared the Pes and IGP measured using this new device with those obtained with a standard balloon catheter taken as gold standard. Methods: Twenty-four intubated patients requiring ventilator support (mean age 64.3 ± 16.8 years, body mass index 5.3 ± 3. kg/m, and PaO /FiO 8.8 ± 13.4 mmhg) were enrolled. Esophageal pressure and IGP were measured with the new nasogastric polyfunctional catheter (Nutrivent, Sidam, Italy) and with a standard balloon catheter (Smart Cath Viasys, USA). The Smart Cath was first inserted in the stomach and then retracted to the esophagus to measure IGP and Pes, respectively. In each patient two paired measurements were averaged. Results: In the Bland Altman analysis, the bias and agreement bands for Pes, DPes (computed as the difference of esophageal pressure between endinspiration and expiration), and IGP were -.5 (-.65 to?.15),. (-.9 to?.9), and -.45 (-.85 to? 1.95) cmh O, respectively. No side effects or complications were recorded. Conclusions: The new polyfunctional catheter showed a clinically acceptable validity in recording esophageal and intragastric pressure. This device should help physicians to better individualize the clinical patient management. Keywords Nasogastric catheter Esophageal pressure Intragastric pressure ARDS Introduction Acute lung injury (ALI)/acute respiratory distress syndrome (ARDS) is a syndrome which, despite recent therapeutic advances, still results in high mortality [1, ]. Although mechanical ventilation is a life-saving support, it may induce several types of lung injuries collectively named as ventilator-induced lung injury (VILI) [3]. The lung inflation depends on transpulmonary pressure (airway pressure minus pleural pressure), which in turn depends on the characteristics of the chest wall and the lung [4, 5]. In addition, an abnormal increase in the intra-
2 abdominal pressure, defined as intra-abdominal hypertension, is frequently reported (from 18 to 81%) in critically ill patients [6, 7]. The absence of a customized lung protective strategy based on the transpulmonary pressure could lead to an under- or over-application of positive end-expiratory pressure (PEEP) as well as misinterpretation of the airway pressure [8]. The esophageal pressure measured in the lower third of the esophagus is an adequate surrogate of the pleural pressure, because the esophagus behaves as a passive structure [9 11]. The intra-abdominal pressure can be estimated by measuring the bladder or the intragastric pressure [1]. There is currently no nasogastric catheter available which allows a continuous and simultaneous monitoring of the esophageal and intragastric pressure while also providing the possibility of feeding the patient. The aim of this study was to evaluate the accuracy of the esophageal and intragastric pressures measured with a new nasogastric polyfunctional catheter compared to those obtained by a standard balloon catheter. Materials and methods Subjects Twenty-four intubated, mechanically ventilated, sedated patients, with or without paralysis, admitted to our intensive care unit (ICU) from January to June 1 were enrolled. Baseline characteristics were mean age 64.3 ± 16.8 years, body mass index 5.3 ± 3. kg/m, new simplified acute physiology (SAP) II score 39.3 ± 1., PEEP 6.3 ± 4.5 cmh O, PaO /FiO 8.8 ± 13.3, and tidal volume 49 ± 116 ml. Inclusion criterion was the presence of mechanical ventilation in patients who required a catheter. Exclusion criteria were patients younger than 16 years, documented barotrauma, high grade of esophageal varices, a recent history of esophageal or gastric surgery, and severe coagulopathy. The study was approved by the institutional review board of our hospital, and informed consent was obtained according to the Italian national regulations. lower and in the distal portion of the tube (Fig. 1). The intragastric position of the distal catheter was confirmed by aspiration of gastric juice, auscultation of air insufflations into the stomach, and by a rise in intra-abdominal pressure following external manual epigastric pressure. The balloon position in the lower third of the esophagus was confirmed in patients with paralysis by concordant positive changes in airway, esophageal and intragastric pressures during an inspiratory occlusion [13], and in patients able to perform an inspiratory effort by performing the Baydur test [14]. For an optimal reading of the pressures, the balloon should be inflated with an adequate volume of air so as to transmit the pressure without artifacts. Previous in vitro evaluation showed that the optimal volume both for the esophageal and gastric balloons was 4 ml of air. The Smart Cath consists of a tube 13 cm long with an external diameter of 3 mm and a thin-walled balloon (1 cm long) located in the distal part. To measure the intragastric pressure, the catheter was first positioned in the stomach at a depth of cm and then inflated with a volume of ml of air. Subsequently, to measure the esophageal pressure, the catheter was retracted until it reached the upper third of the esophagus at a depth of 3 35 cm from the mouth. The Smart Cath does not allow one to aspirate the liquid from the stomach or to feed the patient. Pressure signals were measured by pressure transducers (Bentley Trantec; Bentley Laboratories, Irvine, USA) and recorded on a personal computer for subsequent analysis (Colligo, Elekton, Milan, Italy). Two-min recording sections were performed. In each patient two paired measurements were averaged for the analysis. The two catheters were positioned at the same time in the patients and the measurements were obtained at the same time. Protocol Patients were in the supine position on mechanical ventilation with pre-study ventilator settings. The esophageal Measurement Esophageal and intragastric pressure were simultaneously recorded by using the new nasogastric polyfunctional catheter (Nutrivent, Sidam, Mirandola, Italy) and by a standard balloon catheter (Smart Cath, Viasys, Palm Springs, USA). The Nutrivent consists of a polyurethane tube (11-cm long with an external diameter of 4.7 mm) with multiple small holes and two thin-walled polyethylene balloons (1-cm long and 15-mm diameter) incorporated in the Fig. 1 a Schematic drawing showing the technical characteristics of the Nutrivent
3 pressure was measured during an end-inspiratory and an end-expiratory occlusion of the airway (Pes EIO and Pes EEO ). The variation of esophageal pressure during tidal inflation (DPes) was computed as Pes EIO minus Pes EEO. The intragastric pressure was measured only during an end-expiratory occlusion of the airway (IGP EEO ). Statistical analysis Data are presented as mean ± standard deviation (SD). In addition, 95% confidence intervals (CI) were reported when necessary. Esophageal and intragastric pressures measured with the new nasogastric polyfunctional catheter and the standard balloon catheter were compared according to Bland Altman analysis [15] together with the Passing and Bablok non-parametric regression [16] and concordance correlation coefficient [17]. Statistical analysis was performed with SAS(c) 9.1. Results Esophageal pressure The mean Pes EEO and DPes were 1.8 ± 3.1 and 3. ± 1.4 cmh O, respectively, for the new nasogastric polyfunctional catheter and 1.9 ±.8 and 3.3 ± 1.5 cmh O for the standard balloon catheter. The regression equations, calculated according to the Passing and Bablok method, had an intercept of (95% CI to.9) and a slope of (95% CI ) for the Pes EEO and an intercept of -.15 (95% CI -.65 to.471) and a slope of 1. (95% CI ) for DPes. In the Bland Altman analysis, the bias and agreement bands (between brackets) for Pes EEO (Fig. a) and DPes (computed as the difference of esophageal pressure between end-inspiration and expiration, Fig. b) were -.5 (-.65 to?.15) and. (-.9 to?.9) cmh O, respectively. There was no evidence of an increase of bias at the extremes of the pressure range (p =.1936 and.3593, respectively). The concordance correlation coefficient (CCC) was.91 (95% CI.8.96) for the Pes EEO and.95 (95% CI.9.98) for DPes; these values translate into a within-sample variability of about 3% and % of the total variability, respectively. Intragastric pressure The mean IGP EEO was 9.7 ±.7 and 1. ±.7 cmh O for the new nasogastric polyfunctional catheter and standard balloon catheter, respectively. The regression equation calculated according to the Passing and Bablok method, considering the IGP EEO between the two methods, had an intercept of (95% CI to 1.75) and a slope of.9841 (95% CI ). The Bland Altman analysis showed a bias of -.45 (-.85 to 1.95) cmh O (Fig. c). The CCC was.89 (95% CI.75.95); this value translates into a withinsample variability of about 33% of the total variability. The new nasogastric polyfunctional catheter was successfully inserted in all the subjects, and it was left in some patients after the study depending on their clinical requirements. No side effects or complications were recorded. Discussion The primary finding of this study is that the new nasogastric polyfunctional catheter is able to record both the esophageal and intragastric pressure similarly to a standard balloon catheter. The respiratory system includes the lung and the chest wall, and consequently the mechanical behavior depends on the mechanical properties of these two components [4]. The distending force of the lung is not the airway pressure, which is commonly used in clinical practice, but the transpulmonary pressure [8]. The measurement of esophageal pressure, obtained by an esophageal balloon, has been used as an estimate of pleural pressure since Buytendijk [18] pioneered the technique. The most widely used method employs an aircontaining balloon sealed over a catheter, which transmits balloon pressure to manometers or, more recently, to monitoring transducers [1, 11]. When simultaneously recorded in spontaneous breathing subjects, the esophageal pressure changed at the same rate as the pleural pressure, but it was consistently more positive [18, 19]. In an experimental study, the esophageal pressure only reflected the pleural pressure measured in the middle regions, whereas it overestimated the pleural pressure in the non-dependent lung regions and underestimated it in the dependent lung regions []. In the present study the new nasogastric polyfunctional catheter showed a good clinical agreement compared to a standard balloon catheter in estimating either the absolute or the changes of esophageal pressure in mechanically ventilated patients. The level of agreement was slightly lower when recording the absolute esophageal pressure compared with the variations of esophageal pressure during the tidal inflation. This was probably due to the difference in location of the balloon of the new nasogastric polyfunctional catheter in the esophagus compared with the standard balloon catheter. To minimize the pressure artifacts due to the catheter itself, we employed a balloon 1-cm long with a very thin
4 Difference between Pes EEO new nasogastric polyfunctional catheter and Pes EEO Difference between deltapes new nasogastric polyfunctional catheter and deltapes Difference between IGP EEO new nasogastric polyfunctional catheter and IGP EEO a mean of Pes EEO new nasogastric polyfunctional catheter and Pes EEO b c mean of deltapes new nasogastric polyfunctional catheter and deltapes mean of IGP EEO new nasogastric polyfunctional catheter and IGP EEO wall, inflated with a minimum amount of air volume, to not increase the pressure inside the balloon, and positioned in the lower part of the esophagus [9 11]. b Fig. a Bland Altman analysis of the esophageal pressure measured with the new nasogastric polyfunctional catheter and the standard balloon catheter. The x-axis shows the mean of the two measurements and the y-axis the difference between the esophageal pressure measured with the new nasogastric polyfunctional catheter and the standard balloon catheter. b Bland Altman analysis of the delta esophageal pressure measured with the new nasogastric polyfunctional catheter and the standard balloon catheter. The x-axis shows the mean of the two measurements and the y-axis the difference between the delta esophageal pressure measured with the new nasogastric polyfunctional catheter and the standard balloon catheter. c Bland Altman analysis of the intragastric pressure measured with the new nasogastric polyfunctional catheter and the standard balloon catheter. The x-axis shows the mean of the two measurements and the y-axis the difference between the intragastric pressure measured with the new nasogastric polyfunctional catheter and the standard balloon catheter Several techniques have been proposed for the measurement of intra-abdominal pressure [1]. The bladder technique was originally described by Kron et al. [1] in which the bladder was infused with 5 1 ml of saline via the patients Foley catheter and the pressure was recorded by a pressure transducer at the symphysis pubis. The bladder technique, due to its simplicity, low cost, and excellent correlation with direct measurement of intraabdominal pressure, still remains the most common technique. However, it is time consuming, it requires instillation of saline into the bladder, it is intermittent and, moreover, gives a trend of intra-abdominal pressure depending on the interval between separate measurements [1]. Previous studies showed that the intra-abdominal pressure can be also accurately measured by the intragastric pressure []. In our experimental setting, the bias in recording the intragastric pressure was clinically acceptable. Even though the width of the agreement bands may be considered numerically high, the agreement was judged to be acceptable because the variations of a few units are not relevant. Thus, the intragastric pressure can be considered an alternative in patients without bladder catheter, in cases of bladder trauma, pelvic hematomas or fractures, and in all the clinical situations in which a continuous monitoring of intra-abdominal pressure is advisable. Conclusions Because the majority of patients admitted to ICU require a nasogastric catheter for nutrition during mechanical ventilation, the new nasogastric polyfunctional catheter can be a good alternative allowing the possibility to continuously monitor esophageal and intragastric pressure. The knowledge of esophageal and intragastric pressures should help in tailoring a more physiologic mechanical ventilation.
5 References 1. Detsky ME, Stewart TE (1) Longterm outcomes of patients after acute respiratory distress syndrome: hard work for nothing? Minerva Anestesiol 76: Phua J, Badia JR, Adhikari NK, Friedrich JO, Fowler RA, Singh JM, Scales DC, Stather DR, Li A, Jones A, Gattas DJ, Hallett D, Tomlinson G, Stewart TE, Ferguson ND (9) Has mortality from acute respiratory distress syndrome decreased over time? A systematic review. Am J Respir Crit Care Med 179: 7 3. Slutsky AS (1999) Lung injury caused by mechanical ventilation. Chest 116:9S 15S 4. Gattinoni L, Chiumello D, Carlesso E, Valenza F (4) Bench-to-bedside review: chest wall elastance in acute lung injury/acute respiratory distress syndrome patients. Crit Care 8: Talmor D, Sarge T, Malhotra A, O Donnell CR, Ritz R, Lisbon A, Novack V, Loring SH (8) Mechanical ventilation guided by esophageal pressure in acute lung injury. N Engl J Med 359: Malbrain ML, Chiumello D, Pelosi P, Wilmer A, Brienza N, Malcangi V, Bihari D, Innes R, Cohen J, Singer P, Japiassu A, Kurtop E, De Keulenaer BL, Daelemans R, Del Turco M, Cosimini P, Ranieri M, Jacquet L, Laterre PF, Gattinoni L (4) Prevalence of intra-abdominal hypertension in critically ill patients: a multicentre epidemiological study. Intensive Care Med 3: Malbrain ML, Chiumello D, Pelosi P, Bihari D, Innes R, Ranieri VM, Del Turco M, Wilmer A, Brienza N, Malcangi V, Cohen J, Japiassu A, De Keulenaer BL, Daelemans R, Jacquet L, Laterre PF, Frank G, de Souza P, Cesana B, Gattinoni L (5) Incidence and prognosis of intraabdominal hypertension in a mixed population of critically ill patients: a multiple-center epidemiological study. Crit Care Med 33: Chiumello D, Carlesso E, Cadringher P, Caironi P, Valenza F, Polli F, Tallarini F, Cozzi P, Cressoni M, Colombo A, Marini JJ, Gattinoni L (8) Lung stress and strain during mechanical ventilation for acute respiratory distress syndrome. Am J Respir Crit Care Med 178: Higgs BD, Behrakis PK, Bevan DR, Milic-Emili J (1983) Measurement of pleural pressure with esophageal balloon in anesthetized humans. Anesthesiology 59: Milic-Emili J, Mead J, Turner JM (1964) Topography of esophageal pressure as a function of posture in man. J Appl Physiol 19: Milic-Emili J, Mead J, Turner JM, Glauser EM (1964) Improved technique for estimating pleural pressure from esophageal balloons. J Appl Physiol 19: Malbrain ML (4) Different techniques to measure intra-abdominal pressure (IAP): time for a critical reappraisal. Intensive Care Med 3: Chiumello D, Cressoni M, Racagni M, Landi L, Li Bassi G, Polli F, Carlesso E, Gattinoni L (6) Effects of thoracopelvic supports during prone position in patients with acute lung injury/acute respiratory distress syndrome: a physiological study. Crit Care 1:R Baydur A, Behrakis PK, Zin WA, Jaeger M, Milic-Emili J (198) A simple method for assessing the validity of the esophageal balloon technique. Am Rev Respir Dis 16: Bland JM, Altman DG (199) Measuring agreement in method comparison studies. Stat Methods Med Res 8: Passing H, Bablok W (1983) A new biometrical procedure for testing the equality of measurements from two different analytical methods. Application of linear regression procedures for method comparison studies in clinical chemistry, Part I. J Clin Chem Clin Biochem 1: Lin L, Hedavat AS, Yang M () Statistical methods in assessing agreement: models, issues and tools. J Am Stat Assoc 97: Buytendijk HJ (1949) Oesophagusdruk en longelasticiteit. Electrische Drukkerij I. Oppenheim NV, Groningen 19. Mead J, McIlroy MB, Selverstone NJ, Kriete BC (1955) Measurement of intraesophageal pressure. J Appl Physiol 7: Pelosi P, Goldner M, McKibben A, Adams A, Eccher G, Caironi P, Losappio S, Gattinoni L, Marini JJ (1) Recruitment and derecruitment during acute respiratory failure: an experimental study. Am J Respir Crit Care Med 164: Kron IL, Harman PK, Nolan SP (1984) The measurement of intra-abdominal pressure as a criterion for abdominal reexploration. Ann Surg 199:8 3. Malbrain ML, Cheatham ML, Kirkpatrick A, Sugrue M, Parr M, De Waele J, Balogh Z, Leppäniemi A, Olvera C, Ivatury R, D Amours S, Wendon J, Hillman K, Johansson K, Kolkman K, Wilmer A (6) Results from the International Conference of Experts on Intra-abdominal Hypertension and Abdominal Compartment Syndrome. I. Definitions. Intensive Care Med 3:17 173
Transpulmonary pressure measurement
 White Paper Transpulmonary pressure measurement Benefit of measuring transpulmonary pressure in mechanically ventilated patients Dr. Jean-Michel Arnal, Senior Intensivist, Hopital Sainte Musse, Toulon,
White Paper Transpulmonary pressure measurement Benefit of measuring transpulmonary pressure in mechanically ventilated patients Dr. Jean-Michel Arnal, Senior Intensivist, Hopital Sainte Musse, Toulon,
The occlusion tests and end expiratory esophageal pressure: measurements and comparison in controlled and assisted ventilation
 DOI 10.1186/s13613-016-0112-1 RESEARCH Open Access The occlusion tests and end expiratory esophageal pressure: measurements and comparison in controlled and assisted ventilation Davide Chiumello 1,2*,
DOI 10.1186/s13613-016-0112-1 RESEARCH Open Access The occlusion tests and end expiratory esophageal pressure: measurements and comparison in controlled and assisted ventilation Davide Chiumello 1,2*,
The Correlation Between Esophageal and Abdominal Pressures in. Mechanically Ventilated Patients Undergoing Laparoscopic Surgery
 The Correlation Between Esophageal and Abdominal Pressures in Mechanically Ventilated Patients Undergoing Laparoscopic Surgery Anees Sindi, MBChB 1*, Tom Piraino, RRT 2 *, Waleed Alhazzani, MD 2, Marcel
The Correlation Between Esophageal and Abdominal Pressures in Mechanically Ventilated Patients Undergoing Laparoscopic Surgery Anees Sindi, MBChB 1*, Tom Piraino, RRT 2 *, Waleed Alhazzani, MD 2, Marcel
The Correlation Between Esophageal and Abdominal Pressures in Mechanically Ventilated Patients Undergoing Laparoscopic Surgery
 The Correlation Between Esophageal and Abdominal Pressures in Mechanically Ventilated Patients Undergoing Laparoscopic Surgery Anees Sindi MBChB, Tom Piraino RRT, Waleed Alhazzani MD, Marcel Tunks MD,
The Correlation Between Esophageal and Abdominal Pressures in Mechanically Ventilated Patients Undergoing Laparoscopic Surgery Anees Sindi MBChB, Tom Piraino RRT, Waleed Alhazzani MD, Marcel Tunks MD,
Measurement of compartment pressure of the rectus sheath during intra-abdominal hypertension in rats
 Intensive Care Med (2006) 32:1644 1648 DOI 10.1007/s00134-006-0366-4 TECHNICAL NOTE Christoph Meier René Schramm Joerg H. Holstein Burkhardt Seifert Otmar Trentz Michael D. Menger Measurement of compartment
Intensive Care Med (2006) 32:1644 1648 DOI 10.1007/s00134-006-0366-4 TECHNICAL NOTE Christoph Meier René Schramm Joerg H. Holstein Burkhardt Seifert Otmar Trentz Michael D. Menger Measurement of compartment
How ARDS should be treated in 2017
 How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
Use of Cardiac Cycle Locating to Minimize the Influence of Cardiac Artifacts on Esophageal Pressure Measurement During Dynamic Occlusion Test
 Use of Cardiac Cycle Locating to Minimize the Influence of Cardiac Artifacts on Esophageal Pressure Measurement During Dynamic Occlusion Test Xuan He MSc, Xiu-Mei Sun MSc, Guang-Qiang Chen MD, Yan-Lin
Use of Cardiac Cycle Locating to Minimize the Influence of Cardiac Artifacts on Esophageal Pressure Measurement During Dynamic Occlusion Test Xuan He MSc, Xiu-Mei Sun MSc, Guang-Qiang Chen MD, Yan-Lin
Refresher Course MYTHS AND REALITY ABOUT LUNG MECHANICS 5 RC 2. European Society of Anaesthesiologists FIGURE 1 STATIC MEASUREMENTS
 European Society of Anaesthesiologists Refresher Course S AND ABOUT LUNG MECHANICS 5 RC 2 Anders LARSSON Gentofte University Hospital Copenhagen University Hellerup, Denmark Saturday May 31, 2003 Euroanaesthesia
European Society of Anaesthesiologists Refresher Course S AND ABOUT LUNG MECHANICS 5 RC 2 Anders LARSSON Gentofte University Hospital Copenhagen University Hellerup, Denmark Saturday May 31, 2003 Euroanaesthesia
In vivo calibration of esophageal pressure in the mechanically ventilated patient makes measurements reliable
 Mojoli et al. Critical Care (216) 2:98 DOI.1186/s134-16-1278- RESEARCH In vivo calibration of esophageal pressure in the mechanically ventilated patient makes measurements reliable Francesco Mojoli 1,2*,
Mojoli et al. Critical Care (216) 2:98 DOI.1186/s134-16-1278- RESEARCH In vivo calibration of esophageal pressure in the mechanically ventilated patient makes measurements reliable Francesco Mojoli 1,2*,
Interpretation of the transpulmonary pressure in the critically ill patient
 Review Article Page 1 of 12 Interpretation of the transpulmonary pressure in the critically ill patient Michele Umbrello 1, Davide Chiumello 1,2 1 UOC Anestesia e Rianimazione, Ospedale San Paolo ASST
Review Article Page 1 of 12 Interpretation of the transpulmonary pressure in the critically ill patient Michele Umbrello 1, Davide Chiumello 1,2 1 UOC Anestesia e Rianimazione, Ospedale San Paolo ASST
Institute of Anesthesia and Critical Care, University of Milan, Policlinico IRCCS Hospital, Milan, Italy
 Critical Care October 2004 Vol 8 No 5 Gattinoni et al. Review Bench-to-bedside review: Chest wall elastance in acute lung injury/acute respiratory distress syndrome patients Luciano Gattinoni, Davide Chiumello,
Critical Care October 2004 Vol 8 No 5 Gattinoni et al. Review Bench-to-bedside review: Chest wall elastance in acute lung injury/acute respiratory distress syndrome patients Luciano Gattinoni, Davide Chiumello,
Protective ventilation for ALL patients
 Protective ventilation for ALL patients PAOLO PELOSI, MD, FERS Department of Surgical Sciences and Integrated Diagnostics (DISC), San Martino Policlinico Hospital IRCCS for Oncology, University of Genoa,
Protective ventilation for ALL patients PAOLO PELOSI, MD, FERS Department of Surgical Sciences and Integrated Diagnostics (DISC), San Martino Policlinico Hospital IRCCS for Oncology, University of Genoa,
A necessary evil? Intra-abdominal hypertension complicating burn patient resuscitation
 McBeth et al. Journal of Trauma Management & Outcomes 2014, 8:12 RESEARCH Open Access A necessary evil? Intra-abdominal hypertension complicating burn patient resuscitation Paul B McBeth 1, Kim Sass 1,
McBeth et al. Journal of Trauma Management & Outcomes 2014, 8:12 RESEARCH Open Access A necessary evil? Intra-abdominal hypertension complicating burn patient resuscitation Paul B McBeth 1, Kim Sass 1,
Should we titrate positive end-expiratory pressure based on an end-expiratory transpulmonary pressure?
 Perspective Page 1 of 8 Should we titrate positive end-expiratory pressure based on an end-expiratory transpulmonary pressure? John J. Marini Department of Pulmonary and Critical Care Medicine, University
Perspective Page 1 of 8 Should we titrate positive end-expiratory pressure based on an end-expiratory transpulmonary pressure? John J. Marini Department of Pulmonary and Critical Care Medicine, University
Esophageal and transpulmonary pressure in the clinical setting: meaning, usefulness and perspectives
 Intensive Care Med (2016) 42:1360 1373 DOI 10.1007/s00134-016-4400-x REVIEW Esophageal and transpulmonary pressure in the clinical setting: meaning, usefulness and perspectives Tommaso Mauri1, Takeshi
Intensive Care Med (2016) 42:1360 1373 DOI 10.1007/s00134-016-4400-x REVIEW Esophageal and transpulmonary pressure in the clinical setting: meaning, usefulness and perspectives Tommaso Mauri1, Takeshi
Comparison of automated and static pulse respiratory mechanics during supported ventilation
 Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
journal of medicine The new england Lung Recruitment in Patients with the Acute Respiratory Distress Syndrome Abstract
 The new england journal of medicine established in 1812 april 27, 2006 vol. 354 no. 17 Lung Recruitment in Patients with the Acute Respiratory Distress Syndrome Luciano Gattinoni, M.D., F.R.C.P., Pietro
The new england journal of medicine established in 1812 april 27, 2006 vol. 354 no. 17 Lung Recruitment in Patients with the Acute Respiratory Distress Syndrome Luciano Gattinoni, M.D., F.R.C.P., Pietro
Michael Moller 1*, Ulrik K Kjerkegaard 2, Jens Rolighed Larsen 3,4, Hanne Birke-Sorensen 1,5, Lars B Stolle 1,5. Abstract
 RESEARCH Open Access Temporal differences in the development of organ dysfunction based on two different approaches to induce experimental intraabdominal hypertension in swine Michael Moller 1*, Ulrik
RESEARCH Open Access Temporal differences in the development of organ dysfunction based on two different approaches to induce experimental intraabdominal hypertension in swine Michael Moller 1*, Ulrik
Lung inhomogeneities, inflation and [ 18 F]2-fluoro-2-deoxy-D-glucose uptake rate in acute respiratory distress syndrome
![Lung inhomogeneities, inflation and [ 18 F]2-fluoro-2-deoxy-D-glucose uptake rate in acute respiratory distress syndrome Lung inhomogeneities, inflation and [ 18 F]2-fluoro-2-deoxy-D-glucose uptake rate in acute respiratory distress syndrome](/thumbs/88/116222124.jpg) ORIGINAL ARTICLE ACUTE LUNG INJURY AND CRITICAL CARE Lung inhomogeneities, inflation and [ 18 F]2-fluoro-2-deoxy-D-glucose uptake rate in acute respiratory distress syndrome Massimo Cressoni 1, Davide
ORIGINAL ARTICLE ACUTE LUNG INJURY AND CRITICAL CARE Lung inhomogeneities, inflation and [ 18 F]2-fluoro-2-deoxy-D-glucose uptake rate in acute respiratory distress syndrome Massimo Cressoni 1, Davide
ARDS Management Protocol
 ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
Sitting and Supine Esophageal Pressures in Overweight and Obese Subjects Authors
 Sitting and Supine Esophageal Pressures in Overweight and Obese Subjects Authors The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Sitting and Supine Esophageal Pressures in Overweight and Obese Subjects Authors The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Evaluation of the Effects of Elevated Intraabdominal. on the Respiratory Mechanics in Mechanically Ventilated Patients
 Macedonian Journal of Medical Sciences. http://dx.doi.org/10.3889/mjms.1857-5773.2013.0306 Clinical Science Maced J Med Sci electronic publication ahead of print, published on September 05, 2013 as http://dx.doi.org/10.3889/mjms.1857-5773.2013.0306
Macedonian Journal of Medical Sciences. http://dx.doi.org/10.3889/mjms.1857-5773.2013.0306 Clinical Science Maced J Med Sci electronic publication ahead of print, published on September 05, 2013 as http://dx.doi.org/10.3889/mjms.1857-5773.2013.0306
Name and title of the investigators responsible for conducting the research: Dr Anna Lavizzari, Dr Mariarosa Colnaghi
 Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
PEEP nuove indicazioni, stesse problematiche
 PEEP nuove indicazioni, stesse problematiche Franco Valenza Department of Pathophysiology and Transplantation Fondazione IRCCS Ca' Granda - Ospedale Maggiore Policlinico Ossigenazione Clearance CO 2 Kats,
PEEP nuove indicazioni, stesse problematiche Franco Valenza Department of Pathophysiology and Transplantation Fondazione IRCCS Ca' Granda - Ospedale Maggiore Policlinico Ossigenazione Clearance CO 2 Kats,
SIGH IN SUPINE AND PRONE POSITION DURING ACUTE RESPIRATORY DISTRESS SYNDROME
 AJRCCM Articles in Press. Published on December 18, 2002 as doi:10.1164/rccm.200203-198oc SIGH IN SUPINE AND PRONE POSITION DURING ACUTE RESPIRATORY DISTRESS SYNDROME Paolo Pelosi *, Nicola Bottino, Davide
AJRCCM Articles in Press. Published on December 18, 2002 as doi:10.1164/rccm.200203-198oc SIGH IN SUPINE AND PRONE POSITION DURING ACUTE RESPIRATORY DISTRESS SYNDROME Paolo Pelosi *, Nicola Bottino, Davide
Study of intra-abdominal hypertension prevalence and awareness level among experienced ICU medical staff
 Zhang et al. Military Medical Research (2016) 3:27 DOI 10.1186/s40779-016-0097-y RESEARCH Open Access Study of intra-abdominal hypertension prevalence and awareness level among experienced ICU medical
Zhang et al. Military Medical Research (2016) 3:27 DOI 10.1186/s40779-016-0097-y RESEARCH Open Access Study of intra-abdominal hypertension prevalence and awareness level among experienced ICU medical
Comparison of patient spirometry and ventilator spirometry
 GE Healthcare Comparison of patient spirometry and ventilator spirometry Test results are based on the Master s thesis, Comparison between patient spirometry and ventilator spirometry by Saana Jenu, 2011
GE Healthcare Comparison of patient spirometry and ventilator spirometry Test results are based on the Master s thesis, Comparison between patient spirometry and ventilator spirometry by Saana Jenu, 2011
Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation response to PEEP: a systematic review and meta-analysis
 Guo et al. BMC Anesthesiology (2018) 18:172 https://doi.org/10.1186/s12871-018-0631-4 RESEARCH ARTICLE Open Access Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation
Guo et al. BMC Anesthesiology (2018) 18:172 https://doi.org/10.1186/s12871-018-0631-4 RESEARCH ARTICLE Open Access Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation
Part 2 of park s Ventilator and ARDS slides for syllabus
 Part 2 of park s Ventilator and ARDS slides for syllabus Early Neuromuscular Blockade Question 4 The early use of cis-atracurium in severe ARDS is: A. Contraindicated in patients with diabetes B. Associated
Part 2 of park s Ventilator and ARDS slides for syllabus Early Neuromuscular Blockade Question 4 The early use of cis-atracurium in severe ARDS is: A. Contraindicated in patients with diabetes B. Associated
Effects of patient positioning on respiratory mechanics in mechanically ventilated ICU patients
 Review Article Page 1 of 9 Effects of patient positioning on respiratory mechanics in mechanically ventilated ICU patients Mehdi Mezidi 1,2, Claude Guérin 1,2,3 1 Service de réanimation médicale, Hôpital
Review Article Page 1 of 9 Effects of patient positioning on respiratory mechanics in mechanically ventilated ICU patients Mehdi Mezidi 1,2, Claude Guérin 1,2,3 1 Service de réanimation médicale, Hôpital
INTRA-ABDOMINAL PRESSURE MONITORING
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Physiological Relevance of a Minimal Model in Healthy Pigs Lung
 Physiological Relevance of a Minimal Model in Healthy Pigs Lung Yeong Shiong Chiew*, Thomas Desaive** Bernard Lambermont**, Nathalie Janssen**, Geoffrey M Shaw***, Christoph Schranz****, Knut Möller****,
Physiological Relevance of a Minimal Model in Healthy Pigs Lung Yeong Shiong Chiew*, Thomas Desaive** Bernard Lambermont**, Nathalie Janssen**, Geoffrey M Shaw***, Christoph Schranz****, Knut Möller****,
Ventilator ECMO Interactions
 Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Open Access RESEARCH. Mezidi et al. Ann. Intensive Care (2018) 8:86
 https://doi.org/10.1186/s13613-018-0434-2 RESEARCH Open Access Effects of positive end expiratory pressure in supine and prone position on lung and chest wall mechanics in acute respiratory distress syndrome
https://doi.org/10.1186/s13613-018-0434-2 RESEARCH Open Access Effects of positive end expiratory pressure in supine and prone position on lung and chest wall mechanics in acute respiratory distress syndrome
Principles of Mechanical Ventilation
 47 Principles of Mechanical Ventilation Jonathan E. Sevransky, MD, MHS Objectives Understand the indications for treatment with mechanical ventilation Describe ventilator strategies that will minimize
47 Principles of Mechanical Ventilation Jonathan E. Sevransky, MD, MHS Objectives Understand the indications for treatment with mechanical ventilation Describe ventilator strategies that will minimize
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Ventilatory Management of ARDS. Alexei Ortiz Milan; MD, MSc
 Ventilatory Management of ARDS Alexei Ortiz Milan; MD, MSc 2017 Outline Ventilatory management of ARDS Protected Ventilatory Strategy Use of NMB Selection of PEEP Driving pressure Lung Recruitment Prone
Ventilatory Management of ARDS Alexei Ortiz Milan; MD, MSc 2017 Outline Ventilatory management of ARDS Protected Ventilatory Strategy Use of NMB Selection of PEEP Driving pressure Lung Recruitment Prone
Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS
 Zee and Gommers Critical Care (2019) 23:73 https://doi.org/10.1186/s13054-019-2365-1 REVIEW Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS Philip van der
Zee and Gommers Critical Care (2019) 23:73 https://doi.org/10.1186/s13054-019-2365-1 REVIEW Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS Philip van der
MINERVA ANESTESIOLOGICA. Friday night ventilation A safety starting tool kit for mechanically ventilated patients
 MINERVA ANESTESIOLOGICA EDIZIONI MINERVA MEDICA This provisional PDF corresponds to the article as it appeared upon acceptance. A copyedited and fully formatted version will be made available soon. The
MINERVA ANESTESIOLOGICA EDIZIONI MINERVA MEDICA This provisional PDF corresponds to the article as it appeared upon acceptance. A copyedited and fully formatted version will be made available soon. The
ARDS Assisted ventilation and prone position. ICU Fellowship Training Radboudumc
 ARDS Assisted ventilation and prone position ICU Fellowship Training Radboudumc Fig. 1 Physiological mechanisms controlling respiratory drive and clinical consequences of inappropriate respiratory drive
ARDS Assisted ventilation and prone position ICU Fellowship Training Radboudumc Fig. 1 Physiological mechanisms controlling respiratory drive and clinical consequences of inappropriate respiratory drive
The baby lung became an adult
 Intensive Care Med (2016) 42:663 673 DOI 10.1007/s00134-015-4200-8 REVIEW Luciano Gattinoni John J. Marini Antonio Pesenti Michael Quintel Jordi Mancebo Laurent Brochard The baby lung became an adult Received:
Intensive Care Med (2016) 42:663 673 DOI 10.1007/s00134-015-4200-8 REVIEW Luciano Gattinoni John J. Marini Antonio Pesenti Michael Quintel Jordi Mancebo Laurent Brochard The baby lung became an adult Received:
Volume 16 - Issue 3, Cover Story
 Volume 16 - Issue 3, 2016 - Cover Story Update on Intra-Abdominal Hypertension Prof. Manu Malbrain, MD, PhD ******@***uzbrussel.be ICU Director - Intensive Care Unit, University Hospital Brussels (UZB)
Volume 16 - Issue 3, 2016 - Cover Story Update on Intra-Abdominal Hypertension Prof. Manu Malbrain, MD, PhD ******@***uzbrussel.be ICU Director - Intensive Care Unit, University Hospital Brussels (UZB)
ARF. 8 8 (PaO 2 / FIO 2 ) NPPV NPPV ( P = 0.37) NPPV NPPV. (PaO 2 / FIO 2 > 200 PaO 2 / FIO 2 NPPV > 100) (P = 0.02) NPPV ( NPPV P = 0.
 Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Patient-ventilator interaction and inspiratory effort during pressure support ventilation in patients with different pathologies
 Eur Respir J, 1997; 1: 177 183 DOI: 1.1183/931936.97.11177 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 Patient-ventilator interaction and
Eur Respir J, 1997; 1: 177 183 DOI: 1.1183/931936.97.11177 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 Patient-ventilator interaction and
PAOLO PELOSI, LAURA MARIA CHIERICHETTI, PAOLO SEVERGNINI
 MANAGEMENT OF WEANING EUROANESTHESIA 2005 Vienna, Austria 28-31 May 2005 12RC11 PAOLO PELOSI, LAURA MARIA CHIERICHETTI, PAOLO SEVERGNINI Dipartimento Ambiente, Salute e Sicurezza, Universita degli Studi
MANAGEMENT OF WEANING EUROANESTHESIA 2005 Vienna, Austria 28-31 May 2005 12RC11 PAOLO PELOSI, LAURA MARIA CHIERICHETTI, PAOLO SEVERGNINI Dipartimento Ambiente, Salute e Sicurezza, Universita degli Studi
INTRA-ABDOMINAL HYPERTENSION AND SECONDARY ABDOMINAL COMPARTMENT SYNDROME IN MEDICAL PATIENTS COMPLICATION WITH A HIGH MORTALITY
 Trakia Journal of Sciences, Vol. 12, Suppl. 1, pp 202-207, 2014 Copyright 2014 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) INTRA-ABDOMINAL
Trakia Journal of Sciences, Vol. 12, Suppl. 1, pp 202-207, 2014 Copyright 2014 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) INTRA-ABDOMINAL
Tracking lung recruitment and regional tidal volume at the bedside. Antonio Pesenti
 Tracking lung recruitment and regional tidal volume at the bedside Antonio Pesenti Conflicts of Interest Maquet: Received research support and consultation fees Drager: Received research support and consultation
Tracking lung recruitment and regional tidal volume at the bedside Antonio Pesenti Conflicts of Interest Maquet: Received research support and consultation fees Drager: Received research support and consultation
Impairment of Lung and Chest Wall Mechanics in Patients with Acute Respiratory Distress Syndrome Role of Abdominal Distension
 Impairment of Lung and Chest Wall Mechanics in Patients with Acute Respiratory Distress Syndrome Role of Abdominal Distension V. MARCO RANIERI, NICOLA BRIENZA, SERGIO SANTOSTASI, FILOMENA PUNTILLO, LUCIANA
Impairment of Lung and Chest Wall Mechanics in Patients with Acute Respiratory Distress Syndrome Role of Abdominal Distension V. MARCO RANIERI, NICOLA BRIENZA, SERGIO SANTOSTASI, FILOMENA PUNTILLO, LUCIANA
Role of PoCT in Goal-Directed Therapy in Critical Care Settings
 Role of PoCT in Goal-Directed Therapy in Critical Care Settings Alessandro Protti Fondazione IRCCS Ca Granda Ospedale Maggiore Policlinico Milan, Italy Sponsored by Instrumentation Laboratory Contents
Role of PoCT in Goal-Directed Therapy in Critical Care Settings Alessandro Protti Fondazione IRCCS Ca Granda Ospedale Maggiore Policlinico Milan, Italy Sponsored by Instrumentation Laboratory Contents
Journal Club American Journal of Respiratory and Critical Care Medicine. Zhang Junyi
 Journal Club 2018 American Journal of Respiratory and Critical Care Medicine Zhang Junyi 2018.11.23 Background Mechanical Ventilation A life-saving technique used worldwide 15 million patients annually
Journal Club 2018 American Journal of Respiratory and Critical Care Medicine Zhang Junyi 2018.11.23 Background Mechanical Ventilation A life-saving technique used worldwide 15 million patients annually
Measuring End Expiratory Lung Volume after cardiac surgery
 (Acta Anaesth. Belg., 2012, 63, 115-120) Measuring End Expiratory Lung Volume after cardiac surgery G. MICHIELS (*), V. MARCHAL (**), D. LEDOUX (*) and P. DAMAS (*) Abstract. Background : The aim of this
(Acta Anaesth. Belg., 2012, 63, 115-120) Measuring End Expiratory Lung Volume after cardiac surgery G. MICHIELS (*), V. MARCHAL (**), D. LEDOUX (*) and P. DAMAS (*) Abstract. Background : The aim of this
Troubleshooting of Nursing Practice for Mechanically Ventilated Patients
 Troubleshooting of Nursing Practice for Mechanically Ventilated Patients *1 Dr. Hanan Mohammed Mohammed, 2 Dr. Abeer El-Said Hassan 1 Assistant Professor of Medical-Surgical Nursing Department, Faculty
Troubleshooting of Nursing Practice for Mechanically Ventilated Patients *1 Dr. Hanan Mohammed Mohammed, 2 Dr. Abeer El-Said Hassan 1 Assistant Professor of Medical-Surgical Nursing Department, Faculty
The new ARDS definitions: what does it mean?
 The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Intra-abdominal Pressure as a Criterion for Abdominal Re-exploration INTRODUCTION
 Intra-abdominal Pressure as a Criterion for Abdominal Re-exploration Mohammed Moustafa, Mohammed Mokhtar, Gamal Saleh & Ahmed Moustafa Department of General Surgery Benha University Hospitals, Egypt ABSTRACT
Intra-abdominal Pressure as a Criterion for Abdominal Re-exploration Mohammed Moustafa, Mohammed Mokhtar, Gamal Saleh & Ahmed Moustafa Department of General Surgery Benha University Hospitals, Egypt ABSTRACT
Lung and chest wall mechanics in normal anaesthetized subjects and in patients with COPD at different PEEP levels
 Eur Respir J 1997; 1: 2545 2552 DOI: 1.1183/931936.97.1112545 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 Lung and chest wall mechanics
Eur Respir J 1997; 1: 2545 2552 DOI: 1.1183/931936.97.1112545 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 Lung and chest wall mechanics
Prone Position in ARDS
 Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services Department of Anesthesia & Perioperative Care University of California, San Francisco, San Francisco General Hospital Case
Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services Department of Anesthesia & Perioperative Care University of California, San Francisco, San Francisco General Hospital Case
Sub-category: Intensive Care for Respiratory Distress
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Sniff nasal inspiratory pressure in patients with chronic obstructive pulmonary disease
 Eur Respir J 1997; 1: 1292 1296 DOI: 1.1183/931936.97.161292 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 Sniff nasal inspiratory pressure
Eur Respir J 1997; 1: 1292 1296 DOI: 1.1183/931936.97.161292 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 Sniff nasal inspiratory pressure
Prone Position in ARDS
 Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services San Francisco General Hospital University of California, San Francisco, Case Study A 39 yo F admitted to SFGH TICU s/p hanging,
Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services San Francisco General Hospital University of California, San Francisco, Case Study A 39 yo F admitted to SFGH TICU s/p hanging,
Noninvasive respiratory support:why is it working?
 Noninvasive respiratory support:why is it working? Paolo Pelosi Department of Surgical Sciences and Integrated Diagnostics (DISC) IRCCS San Martino IST University of Genoa, Genoa, Italy ppelosi@hotmail.com
Noninvasive respiratory support:why is it working? Paolo Pelosi Department of Surgical Sciences and Integrated Diagnostics (DISC) IRCCS San Martino IST University of Genoa, Genoa, Italy ppelosi@hotmail.com
PRACTICE GUIDELINES: INTRA-ABDOMINAL HYPERTENSION/ABDOMINAL COMPARTMENT SYNDROME
 PRACTICE GUIDELINES: INTRA-ABDOMINAL HYPERTENSION/ABDOMINAL COMPARTMENT SYNDROME OBJECTIVE: Provide guidelines describing the appropriate monitoring for adult and pediatric patients who are at risk for
PRACTICE GUIDELINES: INTRA-ABDOMINAL HYPERTENSION/ABDOMINAL COMPARTMENT SYNDROME OBJECTIVE: Provide guidelines describing the appropriate monitoring for adult and pediatric patients who are at risk for
Cardiorespiratory Physiotherapy Tutoring Services 2017
 VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013
 ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
Keywords: Non-invasive mechanical ventilation, Respiratory Failure, Respiratory muscles, Hypercapnia, Breathing pattern.
 Monaldi Arch Chest Dis 2004; 61: 2, 81-85 ORIGINAL ARTICLE Inspiratory muscle workload due to dynamic intrinsic PEEP in stable COPD patients: effects of two different settings of non-invasive pressure-support
Monaldi Arch Chest Dis 2004; 61: 2, 81-85 ORIGINAL ARTICLE Inspiratory muscle workload due to dynamic intrinsic PEEP in stable COPD patients: effects of two different settings of non-invasive pressure-support
Proportional Assist Ventilation (PAV) (NAVA) Younes ARRD 1992;145:114. Ventilator output :Triggering, Cycling Control of flow, rise time and pressure
 Conflict of Interest Disclosure Robert M Kacmarek Unconventional Techniques Using Your ICU Ventilator!" 5-5-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston,
Conflict of Interest Disclosure Robert M Kacmarek Unconventional Techniques Using Your ICU Ventilator!" 5-5-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston,
Acute transfusion-related abdominal injury in trauma patients: a case report
 Michel et al. Journal of Medical Case Reports (2016) 10:294 DOI 10.1186/s13256-016-1075-4 CASE REPORT Open Access Acute transfusion-related abdominal injury in trauma patients: a case report P. Michel
Michel et al. Journal of Medical Case Reports (2016) 10:294 DOI 10.1186/s13256-016-1075-4 CASE REPORT Open Access Acute transfusion-related abdominal injury in trauma patients: a case report P. Michel
Online Supplementary Appendix
 Online Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lehman * LH, Saeed * M, Talmor D, Mark RG, and Malhotra
Online Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lehman * LH, Saeed * M, Talmor D, Mark RG, and Malhotra
Simulation of Late Inspiratory Rise in Airway Pressure During Pressure Support Ventilation
 Simulation of Late Inspiratory Rise in Airway Pressure During Pressure Support Ventilation Chun-Hsiang Yu MD, Po-Lan Su MD, Wei-Chieh Lin MD PhD, Sheng-Hsiang Lin PhD, and Chang-Wen Chen MD MSc BACKGROUND:
Simulation of Late Inspiratory Rise in Airway Pressure During Pressure Support Ventilation Chun-Hsiang Yu MD, Po-Lan Su MD, Wei-Chieh Lin MD PhD, Sheng-Hsiang Lin PhD, and Chang-Wen Chen MD MSc BACKGROUND:
Monitoring Respiratory Drive and Respiratory Muscle Unloading during Mechanical Ventilation
 Monitoring Respiratory Drive and Respiratory Muscle Unloading during Mechanical Ventilation J. Beck and C. Sinderby z Introduction Since Galen's description 2000 years ago that the lungs could be inflated
Monitoring Respiratory Drive and Respiratory Muscle Unloading during Mechanical Ventilation J. Beck and C. Sinderby z Introduction Since Galen's description 2000 years ago that the lungs could be inflated
Lung elastic recoil during breathing at increased lung volume
 Lung elastic recoil during breathing at increased lung volume JOSEPH R. RODARTE, 1 GASSAN NOREDIN, 1 CHARLES MILLER, 1 VITO BRUSASCO, 2 AND RICCARDO PELLEGRINO 3 (With the Technical Assistance of Todd
Lung elastic recoil during breathing at increased lung volume JOSEPH R. RODARTE, 1 GASSAN NOREDIN, 1 CHARLES MILLER, 1 VITO BRUSASCO, 2 AND RICCARDO PELLEGRINO 3 (With the Technical Assistance of Todd
Lung elastic recoil during breathing at increased lung volume
 Lung elastic recoil during breathing at increased lung volume JOSEPH R. RODARTE, 1 GASSAN NOREDIN, 1 CHARLES MILLER, 1 VITO BRUSASCO, 2 AND RICCARDO PELLEGRINO 3 (With the Technical Assistance of Todd
Lung elastic recoil during breathing at increased lung volume JOSEPH R. RODARTE, 1 GASSAN NOREDIN, 1 CHARLES MILLER, 1 VITO BRUSASCO, 2 AND RICCARDO PELLEGRINO 3 (With the Technical Assistance of Todd
11 th Annual Congress Turkish Thoracic Society. Mechanical Ventilation in Acute Hypoxemic Respiratory Failure
 11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
The respiratory pressure abdominal volume curve in a porcine model
 Regli et al. Intensive Care Medicine Experimental (2017) 5:11 DOI 10.1186/s40635-017-0124-7 Intensive Care Medicine Experimental RESEARCH Open Access The respiratory pressure abdominal volume curve in
Regli et al. Intensive Care Medicine Experimental (2017) 5:11 DOI 10.1186/s40635-017-0124-7 Intensive Care Medicine Experimental RESEARCH Open Access The respiratory pressure abdominal volume curve in
Driving Pressure and Hospital Mortality in Patients Without ARDS: A Cohort Study
 Accepted Manuscript Driving Pressure and Hospital Mortality in Patients Without ARDS: A Cohort Study Marcello F.S. Schmidt, MD, Andre C.K. B. Amaral, MD, Eddy Fan, MD, PhD, Gordon D. Rubenfeld, MD, MSc
Accepted Manuscript Driving Pressure and Hospital Mortality in Patients Without ARDS: A Cohort Study Marcello F.S. Schmidt, MD, Andre C.K. B. Amaral, MD, Eddy Fan, MD, PhD, Gordon D. Rubenfeld, MD, MSc
Capnography Connections Guide
 Capnography Connections Guide Patient Monitoring Contents I Section 1: Capnography Introduction...1 I Section 2: Capnography & PCA...3 I Section 3: Capnography & Critical Care...7 I Section 4: Capnography
Capnography Connections Guide Patient Monitoring Contents I Section 1: Capnography Introduction...1 I Section 2: Capnography & PCA...3 I Section 3: Capnography & Critical Care...7 I Section 4: Capnography
Assessment of patient-ventilator breath contribution during neurally adjusted ventilatory assist in patients with acute respiratory failure
 Liu et al. Critical Care (2015) 19:43 DOI 10.1186/s13054-015-0775-2 RESEARCH Open Access Assessment of patient-ventilator breath contribution during neurally adjusted ventilatory assist in patients with
Liu et al. Critical Care (2015) 19:43 DOI 10.1186/s13054-015-0775-2 RESEARCH Open Access Assessment of patient-ventilator breath contribution during neurally adjusted ventilatory assist in patients with
Frankfurt, January
 Frankfurt, January 12-13 2018 Frankfurt, January 12-13 2018 SMART ORGANIZING AND SCIENTIFIC COMMITTEE M. Antonelli, G. Bellani, A. Braschi, G. Conti, L. Gattinoni, A. Pesenti, M. Quintel, F. Raimondi,
Frankfurt, January 12-13 2018 Frankfurt, January 12-13 2018 SMART ORGANIZING AND SCIENTIFIC COMMITTEE M. Antonelli, G. Bellani, A. Braschi, G. Conti, L. Gattinoni, A. Pesenti, M. Quintel, F. Raimondi,
Respiratory failure requiring mechanical ventilation
 Current Issues in Mechanical Ventilation for Respiratory Failure* Neil R. MacIntyre, MD The morbidity and mortality associated with respiratory failure is, to a certain extent, iatrogenic. Mechanical ventilation,
Current Issues in Mechanical Ventilation for Respiratory Failure* Neil R. MacIntyre, MD The morbidity and mortality associated with respiratory failure is, to a certain extent, iatrogenic. Mechanical ventilation,
Computed tomography in adult respiratory distress syndrome: what has it taught us?
 Eur Respir J, 1996, 9, 155 162 DOI: 1.1183/931936.96.95155 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 SERIES 'CLINICAL PHYSIOLOGY IN RESPIRATORY
Eur Respir J, 1996, 9, 155 162 DOI: 1.1183/931936.96.95155 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 SERIES 'CLINICAL PHYSIOLOGY IN RESPIRATORY
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
The Influence of Altered Pulmonarv
 The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
C-H. Hamnegård*, S. Wragg**, G. Mills +, D. Kyroussis +, J. Road +, G. Daskos +, B. Bake ++, J. Moxham**, M. Green +
 Eur Respir J, 1995, 8, 153 1536 DOI: 1.1183/931936.95.89153 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 93-1936 The effect of lung volume on transdiaphragmatic
Eur Respir J, 1995, 8, 153 1536 DOI: 1.1183/931936.95.89153 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 93-1936 The effect of lung volume on transdiaphragmatic
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Regional distribution of transpulmonary pressure
 Review Article Page 1 of 8 Regional distribution of transpulmonary pressure Pedro Leme Silva 1, Marcelo Gama de Abreu 2 1 Laboratory of Pulmonary Investigation, Carlos Chagas Filho Institute of Biophysics,
Review Article Page 1 of 8 Regional distribution of transpulmonary pressure Pedro Leme Silva 1, Marcelo Gama de Abreu 2 1 Laboratory of Pulmonary Investigation, Carlos Chagas Filho Institute of Biophysics,
Difficult Ventilation in ARDS Patients
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
The Esophageal Pressure-Guided Ventilation 2 (EPVent2) trial protocol: a multicentre, randomised clinical trial of mechanical ventilation
 The Esophageal Pressure-Guided Ventilation 2 (EPVent2) trial protocol: a multicentre, randomised clinical trial of mechanical ventilation guided by transpulmonary pressure The Harvard community has made
The Esophageal Pressure-Guided Ventilation 2 (EPVent2) trial protocol: a multicentre, randomised clinical trial of mechanical ventilation guided by transpulmonary pressure The Harvard community has made
Respiratory Mechanics
 Respiratory Mechanics Critical Care Medicine Specialty Board Tutorial Dr Arthur Chun-Wing LAU Associate Consultant Intensive Care Unit, Pamela Youde Nethersole Eastern Hospital, Hong Kong 17 th June 2014
Respiratory Mechanics Critical Care Medicine Specialty Board Tutorial Dr Arthur Chun-Wing LAU Associate Consultant Intensive Care Unit, Pamela Youde Nethersole Eastern Hospital, Hong Kong 17 th June 2014
Intra-abdominal hypertension in patients with sellar region tumors
 RESEARCH Open Access Intra-abdominal hypertension in patients with sellar region tumors Konstantin A Popugaev *, Ivan A Savin, Andrew U Lubnin, Alexander S Goriachev, Boris A Kadashev, Pavel L Kalinin,
RESEARCH Open Access Intra-abdominal hypertension in patients with sellar region tumors Konstantin A Popugaev *, Ivan A Savin, Andrew U Lubnin, Alexander S Goriachev, Boris A Kadashev, Pavel L Kalinin,
Weaning and extubation in PICU An evidence-based approach
 Weaning and extubation in PICU An evidence-based approach Suchada Sritippayawan, MD. Div. Pulmonology & Crit Care Dept. Pediatrics Faculty of Medicine Chulalongkorn University Kanokporn Udomittipong, MD.
Weaning and extubation in PICU An evidence-based approach Suchada Sritippayawan, MD. Div. Pulmonology & Crit Care Dept. Pediatrics Faculty of Medicine Chulalongkorn University Kanokporn Udomittipong, MD.
Research Article Pressure Measurement Techniques for Abdominal Hypertension: Conclusions from an Experimental Model
 Critical Care Research and Practice Volume 2015, Article ID 278139, 5 pages http://dx.doi.org/10.1155/2015/278139 Research Article Pressure Measurement Techniques for Abdominal Hypertension: Conclusions
Critical Care Research and Practice Volume 2015, Article ID 278139, 5 pages http://dx.doi.org/10.1155/2015/278139 Research Article Pressure Measurement Techniques for Abdominal Hypertension: Conclusions
Alma Mater University of Bologna. Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy
 Alma Mater University of Bologna Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy Conflict of Interest I have affiliations with, special interests, or have conducted business with the
Alma Mater University of Bologna Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy Conflict of Interest I have affiliations with, special interests, or have conducted business with the
Instellen van beademingsparameters bij de obese pa3ent. MDO Nynke Postma
 Instellen van beademingsparameters bij de obese pa3ent MDO 19-1- 2015 Nynke Postma 1. Altered respiratory mechanics in obese pa@ents 2. Transpulmonary pressure 3. Titra@ng PEEP 4. Titra@ng @dal volume
Instellen van beademingsparameters bij de obese pa3ent MDO 19-1- 2015 Nynke Postma 1. Altered respiratory mechanics in obese pa@ents 2. Transpulmonary pressure 3. Titra@ng PEEP 4. Titra@ng @dal volume
Interesting Case Series. Pulmonary Injury Secondary to Feeding Tube Misplacement
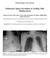 Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Septic shock-3 vs 2: an analysis of the ALBIOS study
 Vasques et al. Critical Care (2018) 22:237 https://doi.org/10.1186/s13054-018-2169-8 RESEARCH Open Access Septic shock-3 vs 2: an analysis of the ALBIOS study Francesco Vasques 1, Eleonora Duscio 1, Federica
Vasques et al. Critical Care (2018) 22:237 https://doi.org/10.1186/s13054-018-2169-8 RESEARCH Open Access Septic shock-3 vs 2: an analysis of the ALBIOS study Francesco Vasques 1, Eleonora Duscio 1, Federica
Does proning patients with refractory hypoxaemia improve mortality?
 Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
