Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation response to PEEP: a systematic review and meta-analysis
|
|
|
- Scarlett Hall
- 5 years ago
- Views:
Transcription
1 Guo et al. BMC Anesthesiology (2018) 18:172 RESEARCH ARTICLE Open Access Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation response to PEEP: a systematic review and meta-analysis Lanqi Guo, Jianfeng Xie, Yingzi Huang, Chun Pan, Yi Yang, Haibo Qiu and Ling Liu * Abstract Background: Mortality in patients with acute respiratory distress syndrome (ARDS) remains high. These patients require mechanical ventilation strategies that include high positive end-expiratory pressure (PEEP). It remains controversial whether high PEEP can improve outcomes for ARDS patients, especially patients who show improvement in oxygenation in response to PEEP. In this meta-analysis, we aimed to evaluate the effects of high PEEP on ARDS patients. Methods: We electronically searched randomized controlled trials (RCTs) reported in the MEDLINE, CENTRAL, EMBASE, CINAHL and Web of Science databases from January 1990 to December Meta-analyses of the effects of PEEP on survival in adults with ARDS were conducted using the methods recommended by the Cochrane Collaboration. Results: A total of 3612 patients from nine randomized controlled trials (RCTs) were included. There were 1794 and 1818 patients in the high and low PEEP groups, respectively. Hospital mortality showed no significant difference between the high and low PEEP groups (RR = 0.92; 95% CI, 0.79 to 1.07; P = 0.26). Similar results were found for 28-d mortality (RR = 0. 88; 95% CI, 0.72 to 1.07; P = 0.19) and ICU mortality (RR = 0.83; 95% CI, 0.65 to 1.07; P = 0.15). The risk of clinically objectified barotrauma was not significantly different between the high and low PEEP groups (RR = 1.24; 95% CI, 0.74 to 2.09, P =0. 41). In the subgroup of ARDS patients who responded to increased PEEP by improved oxygenation (from 6 RCTs), high PEEP significantly reduced hospital mortality (RR = 0.83; 95% CI 0.69 to 0.98; P = 0.03), ICU mortality (RR = 0.74; 95% CI, 0.56 to 0.98; P = 0.04),but the 28-d mortality was not decreased(rr = 0.83; 95% CI, 0.67 to 1.01; P = 0.07). For ARDS patients in the low PEEP group who received a PEEP level lower than 10 cmh 2 O (from 6 RCTs), ICU mortality was lower in the high PEEP group than the low PEEP group (RR = 0.65; 95% CI, 0.45 to 0.94; P =0.02). Conclusions: For ARDS patients who responded to increased PEEP by improved oxygenation, high PEEP could reduce hospital mortality, ICU mortality and 28-d mortality. High PEEP does not increase the risk of clinically objectified barotrauma. Keywords: ARDS, PEEP, Mortality, Barotrauma, Meta * Correspondence: liulingdoctor@126.com Department of Critical Care Medicine, Zhongda Hospital, School of Medicine, Southeast University, Nanjing, Jiangsu, China The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Guo et al. BMC Anesthesiology (2018) 18:172 Page 2 of 11 Background Acute respiratory distress syndrome (ARDS) is a common clinical syndrome that has significant morbidity and mortality [1]. In patients with acute respiratory distress syndrome, mechanical ventilation with a lower tidal volume could decrease mortality [2]. Numerous approaches had been adopted to improve lung-protective ventilation strategies, but the mortality of ARDS remains high. Three large RCTs were performed to assess if higher PEEP could improve outcomes in patients with ARDS [3 5]. All of the trials failed to find that higher PEEP could improve the survival of ARDS patients. However, higher PEEP showed benefits in severe ARDS patients in subgroup analysis. High PEEP can improve the PaO 2 /FiO 2 compared with low PEEP. PEEP is an easily implemented intervention that is primarily used to prevent atelectasis and to correct hypoxemia caused by alveolar hypoventilation. Borges et al. showed that recruitment manoeuvres with PEEP and subsequent maintenance of a high level of PEEP reversed the collapse of alveoli and improved oxygenation [6]. Putensen s study showed better outcomes with routine use of low tidal volume but not high PEEP ventilation in unselected patients with ARDS [7]. Recently, the Alveolar Recruitment for ARDS Trial found that in patients with moderate to severe ARDS, a strategy of lung recruitment and titrated PEEP compared with low PEEP decreased 28-day all-cause mortality [8]. A meta-analysis showed that higher PEEP could improve survival in ARDS patients with a PaO 2 /FiO 2 less than 200 mmhg [9]. These findings indicated that higher PEEP needed to be used in patients who potentially benefit from it. PEEP is a double-edged sword when it is used in ARDS patients. PEEP could open the collapsed alveoli in the dependent lung and may induce hyperinflation in the nondependent lung. Therefore, higher PEEP could improve outcomes based on lung recruitablity in ARDS patients [2]. According to the findings from Goligher s study [10], patients who responded to increased PEEP by improved oxygenation, defined as positive oxygenation response to PEEP, might benefit more from higher PEEP. Thus, we speculated that PEEP could have different effects on clinical outcomes according to the nature of the clinical response to PEEP itself. Therefore, we conducted this meta-analysis to establish whether higher PEEP could improve survival among specific subgroups of ARDS patients who show improvement in oxygenation as a response to increased PEEP. Methods Eligibility criteria and information sources We electronically searched randomized controlled trials (RCTs) published in the MEDLINE, EMBASE, CINAHL and Web of Science databases from January 1990 to December Additional files 1, 2, 3, 4, 5, 6, 7, 8, and 9 and supplementary appendices of the relevant articles were also reviewed. Search and study selection To avoid bias, two investigators assessed the appropriateness of retrieved studies by considering the titles, abstracts and citations independently. The following keywords were used: ALI or acute lung injury, or ARDS, or acute respiratory distress syndrome, or ARF, or acute respiratory failure, and PEEP, or positive end-expiratory pressure, mortality, ICU mortality and barotrauma. The reviewers evaluated the studies based on the inclusion and exclusion criteria, and they worked out any differences by consensus. The study subjects were limited to human. Because a meta-analysis has as its research material previously published data, this research required no ethical approval or patient consent. We only included randomized controlled clinical trials that compared high PEEP with low PEEP in acute respiratory failure, acute lung injury or acute respiratory distress syndrome, whether to ventilate with low tidal volume, that provided the numbers of patients with high PEEP and low PEEP, and that reported patient mortality. We excluded retrospective studies and studies in which previously published data were re-analysed. We also excluded studies involving children and infants. Data items Clinically objectified barotrauma was defined as the presence of pneumothorax on chest radiograph or chest tube insertion for any new pneumothorax, pneumomediastinum, subcutaneous emphysema, or pneumatocele after random assignment. The hospital mortality, ICU mortality and 28-day mortality and the incidence of clinically objectified barotrauma were extracted. Quality assessment Two reviewers independently assessed the quality of RCTs, extracted data, and cross-checked the results. Any disagreements were resolved by a third party. The quality evaluation criteria were assessed by the 5-point scale Jadad scale [5]. The total score was 1 5 (1 2: low-quality research; 3 5: high-quality research). This instrument grades (a) the use of randomization, (b) the use of blinding, (c) the handling of withdrawals and dropouts, (d) the comparability of baselines between groups, and (e) the similarity to other treatment interventions and the accuracy of intervention. The other method to assess the quality of RCTs was assessing the randomization method according to the criteria from the Cochrane Collaboration (Fig. 1).
3 Guo et al. BMC Anesthesiology (2018) 18:172 Page 3 of 11 Fig. 1 Cochrane risk of bias assessment for mortality outcome Sub-group analysis According to Goligher s study[10], we defined positive oxygenation response to PEEP as ΔPaO 2 /FiO 2 >0 mmhg when compared mean PaO 2 /FiO 2 at baseline (lower PEEP) and after PEEP increased to a higher PEEP level in the high PEEP group. However, in the low PEEP group, oxygenation response to PEEP was unavailable because the baseline PEEP did not increase to a high level during the study period. We analysed the sub-groups according to whether patients in the high PEEP group had positive oxygenation response to PEEP to determine whether high PEEP could improve outcomes in patients who respond to increased PEEP by improved oxygenation. In addition, the PEEP value in the low PEEP group and the severity of ARDS also affected whether high PEEP reduced mortality. Therefore, we also performed sub-group analysis to determine whether PEEP greater than 10 cmh 2 Ointhelow PEEP group or baseline PaO 2 /FiO 2 equal to or less than 150 mmhg could have some effect on mortality between the high and low PEEP groups. random-effects model was applied with I 2 statistics greater than 50%. For other I 2 values, a fixed-effects model was selected. Funnel plot were used to analyse publication bias. Results Study selection Our initial electronic and manual search identified 8124 studies. Ultimately, nine RCTs fulfilled the inclusion criteria and were included in the cumulative meta-analysis (Fig. 2). The characteristics of the included studies are Summary measures The meta-analysis was performed according to the Cochrane Collaboration guidelines. All statistical analyses were performed with Review Manager, version 5.3 (the Nordic Cochrane Centre, Copenhagen, Denmark), the Cochrane Collaboration s software for preparing and maintaining Cochrane systematic reviews. The pooled-effects estimates for binary variables are expressed as risk ratios with 95% CIs, whereas continuous variables are expressed as weighted mean differences with 95% CIs. Synthesis of results We tested the difference in the estimated value of the treatment effect between the experimental and control groups with a 2-sided z-test. Statistical significance was defined as P < We predefined heterogeneity as low, moderate, and high with I 2 statistics greater than 25, 50, and 75%, respectively [11]. A meta-analysis with a Fig. 2 Study flow diagram
4 Guo et al. BMC Anesthesiology (2018) 18:172 Page 4 of 11 Table 1 Characteristics of the included patients Trial Jadad score Inclusion criteria method of PEEP selection Number of Patients (HP/LP) Amato/1998 [12] 3 Lung injury score 2.5 HP a :LIP c + 2 cmh2o LP b :FiO2-PEEP Age (HP/LP) PEEP (cmh 2 O) (HP/LP) Gender (HP vs. LP) [male/female] PaO 2 /FIO 2 (mmhg) (HP/LP) 29/ 24 36/ ± 0.4/9.3 ± /134 Ranieri/1999 [13] 3 PaO 2 :FIO mmhg HP a :LIP c + 2 cm H2O LP b :FiO 2 -PEEP 18/19 51/ ± 2.7/6.5 ± 1.7 7/11 vs. 10/19 149/142 Brower/2004 [3] 4 PaO 2 :FIO mmhg HP a :FiO 2 -PEEP (ARDSnet) LP b :FiO2-PEEP (PEEP more than 12 cmh2o) 276/273 54/ ± 3.5/8.9 ± /128 vs.157/ /165 Villar/2006 [14] 3 PaO2:FIO2 200 mmhg HP a :LIP c + 2 cmh2o LP b :FiO 2 -PEEP 50/45 48/ ± 2.8/9.0 ± /27 vs.27/18 111/109 Meade/2008 [5] 4 PaO 2 :FIO mmhg FiO 2 -PEEP 475/ / ± 3.9/10.1 ± /193 vs. 307/ /144.6 Mercat/2008 [15] 4 PaO 2 :FIO mmhg HP a :Pplat LP b : FiO 2 -PEEP 385/382 60/ ± 3.2/7.1 ± /125 vs. 256/ /143 Talmor/2008 [16] 3 PaO2:FIO2 200 mmhg HP a :Transpulmonary pressure LP b :FiO2-PEEP 30/ / ± 6.0/10 ± /11 vs. 17/14 91/107 Huh/2009 [17] 3 PaO2:FIO2 200 mmhg HP a :saturation decrease more than 2% and drop of static compliance LP b :FiO2-PEEP 30/27 55/62 18/12 vs. 17/10 115/110 ART/2017 [8] 3 PaO2:FIO2 200 mmhg HP a : Maximum alveolar recruitment by compliance + 2 cmh2o LP b : FiO 2 -PEEP 501/ / ± 3.8/13.0 ± /188 vs. 318/ /117.2 a HP High PEEP group, b LP Low PEEP group, c LIP lower inflection point
5 Guo et al. BMC Anesthesiology (2018) 18:172 Page 5 of 11 Fig. 3 Effect of high PEEP on hospital mortality in ARDS patients with or without positive oxygenation response to PEEP shown in Table 1. A total of 3612 patients, including 1794 patients in the high PEEP group and 1818 patients in the low PEEP group, were included in our meta-analysis. Effect of high PEEP on hospital mortality in ARDS patients There was no difference in hospital mortality between the high PEEP and low PEEP groups (RR = 0.92; 95% CI, 0.79 to 1.07; P = 0.26) (Fig. 3). In ARDS with positive oxygenation response to PEEP (from 4 RCTs), hospital mortality was lower in the high PEEP group than the low PEEP group (RR = 0.83; 95% CI, 0.69 to 0.98; P = 0.03) (Fig. 3). However, hospital mortality was comparable between groups in patients without positive oxygenation response to PEEP (RR = 1.08; 95% CI, 0.98 to 1.18; P = 0.1) (Fig. 3). For ARDS patients in the low PEEP group who received a PEEP level lower than 10 cmh 2 O (from 4 RCTs), hospital mortality was no different in the high and low PEEP groups (RR = 0.83; 95% CI, 0.64 to 1.08; P = 0.16) (Fig. 4). There was no significant difference in Fig. 4 Effect of high PEEP on hospital mortality while the PEEP level of patients in low PEEP group was different
6 Guo et al. BMC Anesthesiology (2018) 18:172 Page 6 of 11 Fig. 5 Effect of high PEEP on hospital mortality of moderate and severe ARDS patients between high and low PEEP groups hospital mortality between high and low PEEP groups (RR = 1.0; 95% CI, 0.84 to 1.19; P = 0.97) for ARDS patients in the low PEEP group who received a PEEP level equal or higher than 10 cmh 2 O(Fig.4). For ARDS patients with baseline PaO 2 /FiO mmhg (from 5 RCTs), there was no significant difference in hospital mortality between high and low PEEP groups (RR = 0.88; 95% CI, 0.74 to 1.05; P =0.15)(Fig.5). Effect of high PEEP on 28-day mortality in ARDS patients Twenty-eight-day mortality was reported in seven RCTs and was similar in the high and low PEEP groups (RR = 0.88; 95% CI,0.72 to 1.07; P = 0.19) (Fig. 6). In ARDS patients with positive oxygenation response to PEEP (5 RCTs), 28-day mortality was lower in the high PEEP group than the low PEEP group (RR = 0.83; 95% CI, 0.67 to 1.01; P = 0.07) (Fig. 6). Fig. 6 Effect of high PEEP on 28-day mortality in ARDS patients
7 Guo et al. BMC Anesthesiology (2018) 18:172 Page 7 of 11 Fig. 7 Effect of high PEEP on 28-day mortality while the PEEP level of patients in low PEEP group was different There was no difference in 28-day mortality between the high and low PEEP groups, regardless of the PEEP level used in the low PEEP group (For PEEP less than 10 cmh 2 O, RR = 0.80; 95% CI, 0.60 to 1.07; P = 0.14) (For PEEP equal and more than10 cmh 2 O, RR = 0.93; 95% CI, 0.70 to 1.24; P = 0.64) (Fig. 7). Effect of high PEEP on ICU mortality in ARDS patients ICU mortality was reported in five RCTs. A high PEEP strategy did not decrease the ICU mortality compared to the low PEEP strategy (RR = 0.83; 95% CI, 0.65 to 1.07; P = 0.15) (Fig. 8). In ARDS with positive oxygenation response to PEEP (4 RCTs), ICU mortality was lower in the high PEEP group than the low PEEP group (RR = 0.74; 95% CI, 0.56 to 0.98; P = 0.04) (Fig. 8). However, ICU mortality was not different between the high and low PEEP groups among ARDS patients without a positive oxygenation response to PEEP. For ARDS patients in the low PEEP group who received a PEEP level lower than 10 cmh 2 O (from 3 RCTs), ICU mortality was lower in the high PEEP group Fig. 8 Effect of high PEEP on ICU mortality in ARDS patients
8 Guo et al. BMC Anesthesiology (2018) 18:172 Page 8 of 11 Fig. 9 Effect of high PEEP on ICU mortality while the PEEP level of patients in low PEEP group was different than the low PEEP group (RR = 0.65; 95% CI, 0.45 to 0.94; P = 0.02) (Fig. 9). In contrast, there was no significant difference in ICU mortality between the high and low PEEP groups if the PEEP level was equal and more than 10 cmh 2 O in the low PEEP group (RR = 0.98; 95% CI, 0.79 to 1.23; P = 0.89) (Fig. 9). Effect of high PEEP on clinically objectified barotrauma in ARDS patients Seven RCTs reported data on clinically objectified barotrauma, including 1746 patients in the high PEEP group and 1768 patients in the low PEEP group. A meta-analysis with a random-effects model showed that the incidence of clinically objectified barotrauma in the high and low PEEP groups were 9.97% (174/1746) and 6.8% (120/1768), respectively. High PEEP did not increase the incidence of clinically objectified barotrauma (RR = 1.24; 95% CI, 0.74 to 2.09, P = 0.41) (Fig. 10). However, in ARDS patients without positive oxygenation response to PEEP, high PEEP increased the incidence of clinically objectified barotrauma (RR = 2.50; 95% CI, 1.64 to 3.79, P < ) (Fig. 10). Fig. 10 Effect of high PEEP on clinically objectified barotrauma in ARDS patients
9 Guo et al. BMC Anesthesiology (2018) 18:172 Page 9 of 11 Discussion Our meta-analysis showed that high PEEP did not improve outcomes in patients with ARDS. However, subgroup analysis showed that it may decrease hospital mortality as well as ICU and 28-d mortality in ARDS patients with clinically positive oxygenation response to PEEP. In addition, in ARDS patients without positive oxygenation response to PEEP, high PEEP increased the incidence of clinically objectified barotrauma. The results were different from Goligher s study [18], which found that recruitment manoeuvres in combination with higher PEEP could reduce mortality in ARDS patients. Evidence from previous studies showed that high PEEP does not decrease mortality in patients with ARDS [7, 8, 19, 20], which is in line with our results. However, several issues must be considered when interpreting this result. First, there was a large variation in the PEEP level between the different studies. For example, Huh et al. [17] set a high PEEP of 10 cmh 2 O, while the high PEEP was 16.3 cmh 2 O in Amato s study [12]. Similarly, the PEEP level varied from 6.5 to 13 cmh 2 O in the low PEEP groups among the included studies. Therefore, the different PEEP levels may have led to the different results. Subgroup results showed that the PEEP level in the low PEEP group greatly impacted the effect of PEEP on ICU mortality. Second, patient characteristics also impacted the effect of PEEP. Among these studies, the severity of ARDS in patients varied widely. For example, baseline PaO 2 /FiO 2 ranged from ± 6.3 to 165 ± 77 mmhg. Oxygenation response to PEEP was also significantly associated with the severity of ARDS. The potential lung with response to PEEP was considerably stronger in more severe ARDS patients than in less severe individuals. A previous meta-analysis showed that a high PEEP reduced mortality in patients with ARDS but not ALI [8] However, in the present study, there was no difference of hospital mortality between groups of ARDS patients with a baseline PaO 2 /FiO 2 less than 150 mmhg. The purpose of PEEP is to recruit collapsed alveoli in a gravity-dependent lung but not to induce the alveoli to overdistend in the non-dependent lung. Patients with ARDS exhibit significant dependent atelectasis due to increased lung weight resulting from interstitial and alveolar edema. Both higher PEEP and recruitment manoeuvres can reduce atelectasis and increase end-expiratory lung volume. Physically, we need higher pressure to open alveoli and only need a relative lower PEEP to keep the lung open. Therefore, it was noted that higher PEEP should follow the recruitment manoeuvres. Goligher et al. showed that combine with recruitment manoeuvres and higher PEEP could reduce mortality of patients with ARDS [18]. The results were also demonstrated in the study by Constantin et al. [21]. However, the study by Goligher et al. [10] indicated that the percentage of potentially respond to PEEP was extremely variable. Our results demonstrated the hypothesis that only patients who respond to increased PEEP by improved oxygenation benefitted more from higher PEEP. PEEP could have different effects on clinical outcomes based on the nature of the clinical response to PEEP itself. In ARDS patients with clinically positive oxygenation response to PEEP, the main effect of a high PEEP might be recruiting the collapsed lung, which may reduce ventilation-induced lung injury (VILI). In contrast, a high PEEP might result in alveolar overdistension, which induces lung injury in ARDS patients without positive oxygenation response to PEEP. These reasons could help to explain why our subgroup analysis showed that high PEEP reduced mortality in ARDS patients with clinically positive oxygenation response to PEEP. The severity of ARDS can be used to titrate PEEP. There are many methods for PEEP titration, such as oxygenation, stress index and transpulmonary pressure. Chiumello et al. found that oxygenation-guided PEEP provided PEEP levels related to oxygenation response to PEEP in the lung that progressively increased from mild to moderate and severe ARDS [19]. In assessing the oxygenation response to PEEP at 5 cmh 2 O PEEP based on the Berlin definition [6, 22], a simple Friday-night ventilation strategy can be used in patients with ARDS [23]. Therefore, while we only included studies in which the PEEP level was lower than 10 cmh 2 O in the low PEEP group, decreased ICU mortality was found in the high PEEP group. There are many methods that can be used with ARDS patients at present. To date, prolonged sessions of prone positioning has not only been shown to be efficient at significantly increasing oxygenation and decreasing driving pressure in severe ARDS in the APRONET study [24], but the PROSEVA trial also showed that prone positioning was associated with improved patient survival [25]. However, the LUNG SAFE study showed that the rate of prone positioning was low because of selection bias or the clinician s perception [26]. On the other hand, neuromuscular blockers could be used in severe ARDS, but they are controversial. Many previous studies found that the mortality of ARDS treated with neuromuscular blockers was not decreased. However, neuromuscular blockers could exert beneficial effects in patients with moderate ARDS, at least in part, by limiting expiratoryeffortsasshowninguervilly s study[27]. In our study, there were 3 RCTs that included prone position or neuromuscular blockers. Unfortunately, due to the lack of prognostic data, statistical analysis was not possible.
10 Guo et al. BMC Anesthesiology (2018) 18:172 Page 10 of 11 We did not find a significant difference in clinically objectified barotrauma between high PEEP and low PEEP groups. Lung-protective strategies were used in all of the included studies, which decreased the incidence of clinically objectified barotrauma [28, 29]. In addition, most patients in these studies had moderate or severe ARDS, which indicates that more lung area was responsive to increased PEEP. However, in ARDS patients without positive oxygenation response to PEEP, high PEEP increased the incidence of clinically objectified barotrauma. It was shown in a recent study that an exceedingly high pressure was used to recruit the lung, especially in ARDS patients without positive oxygenation response to PEEP, and mortality may increase [8]. Some limitations of our analysis should be noted. First, we were unable to obtain patient-level data despite asking for these data from the authors of the included studies. The lung oxygenation response to PEEP was evaluated based on the mean PaO 2 /FiO 2 values reported in each study but not the individual patient data. That finding means most of the patients in the study with positive oxygenation response to increased PEEP were in their respective groups. Second, the definition of positive oxygenation response to PEEP based on Goligher s study is not highly precise [10]. We also did not assess other factors that may affect the oxygenation response to PEEP. These factors may have affected the accuracy of our results. In this meta-analysis, we only included the data from the included studies. In addition, we did not used the data on SpO 2, PaCO 2 and respiratory compliance at the two different PEEP levels. We only used the PaO 2 /FiO 2 data at higher and lower PEEP levels. Therefore, we defined the groups as positive oxygenation response to PEEP if the mean PaO 2 /FiO 2 was higher in the high PEEP group than at baseline. Based on this definition, we found that patients with clinically positive oxygenation response to PEEP benefitted from high PEEP. Third, the methods of PEEP titration were different between the included studies, which may have induced bias in our study. Oxygenation response to PEEP should be considered during PEEP titration in patients with ARDS. However, no clinical trial has shown that oxygenation response to PEEP using assessment guided PEEP titration could improve the outcomes in patients with ARDS, which indicates further studies are needed. Conclusion In this study, high PEEP did not improve outcomes in patients with ARDS as a whole. However, subgroup analysis showed that high PEEP decreased hospital and ICU mortality in ARDS patients with a clinically objective positive oxygenation response to PEEP. Additional files Additional file 1: Table S1. Description of Patients, Interventions, Comparators, and Outcomes (PICO) targeted by the systematic review. (DOCX 42 kb) Additional file 2: Figure S1. Funnel plot of high PEEP effect on hospital mortality in ARDS patients. (PNG 52 kb) Additional file 3: Figure S2. funnel plot of high PEEP effect on hospital mortality while the PEEP level of patients in low PEEP group was different. (PNG 44 kb) Additional file 4: Figure S3. Funnel plot of high PEEP effect on hospital mortality of moderate and severe ARDS patients between high and low PEEP groups. (PNG 57 kb) Additional file 5: Figure S4. Funnel plot of high PEEP effect on 28-day mortality in ARDS patients. (PNG 53 kb) Additional file 6: Figure S5. Funnel plot of high PEEP effect on 28-day mortality while the PEEP level of patients in low PEEP group was different. (PNG 42 kb) Additional file 7: Figure S6. Funnel plot of high PEEP effect on ICU mortality in ARDS patients. (PNG 63 kb) Additional file 8: Figure S7. Funnel plot of high PEEP effect on ICU mortality while the PEEP level of patients in low PEEP group was different. (PNG 53 kb) Additional file 9: Figure S8. Funnel plot of high PEEP effect on clinically objectified barotrauma in ARDS patients. (PNG 46 kb) Abbreviations ALI: Acute lung injury; ARDS: Acute respiratory distress syndrome; ARF: Acute respiratory failure; ICU: Intensive care unit; PEEP: Positive end-expiratory pressure; RCT: Randomized controlled trials; VILI: Ventilation-induced lung injury Acknowledgements Not available. Funding This work was supported by the National Natural Science Foundation of China under grant No , the Jiangsu Provincial Medical Youth Talent grant No. QNRC , and the Third Level Talents of the 333 High Level Talents Training Project in the fifth phase in Jiangsu (LGY ). Availability of data and materials All data generated or analysed during this study are included in this published article. Authors contributions LQG, LL conceived the study, participated in the design, collected the data, performed statistical analyses, and drafted the manuscript. HBQ and YY participated in the design, and helped to draft the manuscript. JFX, YZH and CP helped to perform statistical analyses and to revise it critically for important intellectual content. All authors read and approved the final manuscript. Ethics approval and consent to participate Not available. Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
11 Guo et al. BMC Anesthesiology (2018) 18:172 Page 11 of 11 Received: 10 May 2018 Accepted: 29 October 2018 References 1. Esteban A, Ferguson ND, Meade MO, Frutos-Vivar F, Apezteguia C, Brochard L, VENTILA Group, et al. Evolution of mechanical ventilation in response to clinical research. Am J Respir Crit Care Med. 2008;177: Gattinoni L, Caironi P, Cressoni M, et al. Lung recruitment in patients with the acute respiratory distress syndrome. N Engl J Med. 2006;354: Brower RG, Lanken PN, Mac Intyre N, et al. Higher versus lower positive end expiratory pressures in patients with the acute respiratory distress syndrome. N Engl J Med. 2004;351: Gattinoni L, Caironi P. Refining ventilatory treatment for acute lung injury and acute respiratory distress syndrome. JAMA. 2008;299(6): Meade MO, Cook DJ, Guyatt GH, et al. Lung open ventilation study investigators. Ventilation strategy using low tidal volumes, recruitment maneuvers, and high positive end-expiratory pressure for acute lung injury and acute respiratory distress syndrome: a randomized controlled trial. JAMA. 2008;299: Borges JB, Okamoto VN, Matos GFJ, Caramez MPR, Arantes PR, Barrios F, et al. Reversibility of lung collapse and hypoxemia in early acute respiratory distress syndrome. Am J Respir Crit Care Med. 2006;174: Putensen C, Theuerkauf N, Zinserling J, et al. Meta-analysis: ventilation strategies and outcomes of the acute respiratory distress syndrome and acute lung injury. Ann Intern Med. 2009;151: Cavalcanti AB, Suzumura ÉA, Laranjeira LN, et al. Effect of lung recruitment and titrated positive end-expiratory pressure (PEEP) vs low PEEP on mortality in patients with acute respiratory distress syndrome: a randomized clinical trial. JAMA. 2017;318(14): Briel M, Meade M, Mercat A, et al. Higher vs lower positive end-expiratory pressure in patients with acute lung injury and acute respiratory distress syndrome systematic review and Meta-analysis. JAMA. 2010;303(9): Goligher EC, Kavanagh BP, Rubenfeld GD, et al. Oxygenation response to PEEP predicts mortality in ARDS: a secondary analysis of the LOVS and ExPress trials. Am J Respir Crit Care Med. 2014;190(1): Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327: Amato MSP, Barbas CSV, Medeiros DM, et al. Effect of a protectiveventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med. 1998;338: Ranieri VM, Suter PM, Tortorella C, et al. Effect of mechanical ventilation on inflammatory mediators in patients with acute respiratory distress syndrome: a randomized controlled trial. JAMA. 1999;282: Villar J, Kacmarek RM, Pérez-Méndez L, et al. A high positive end-expiratory pressure, low tidal volume ventilatory strategy improves outcome in persistent acute respiratory distress syndrome: A randomized, controlled trial*. Crit Care Med. 2006;34: Mercat A, Richard JC, Vielle B, et al. Expiratory pressure (Express) study group. Positive end-expiratory pressure setting in adults with acute lung injury and acute respiratory distress syndrome: a randomized controlled trial. JAMA. 2008;299: Talmor D, Sarge T, Malhotra A, et al. Mechanical ventilation guided by esophageal pressure in acute lung injury. N Engl J Med. 2008;359: Huh JW, Jung H, Sook Choi H, et al. Efficacy of positive end-expiratory pressure titration after the alveolar recruitment manoeuvre in patients with acute respiratory distress syndrome. Crit Care. 2009;13:R Goligher EC, Hodgson CL, Adhikari NKJ, et al. Lung recruitment maneuvers for adult patients with acute respiratory distress syndrome. A systematic review and Meta-analysis. Ann Am Thorac Soc. 2017;14(Supplement_4): S Chiumello D, Cressoni M, Carlesso E, et al. Bedside selection of positive endexpiratory pressure in mild, moderate, and severe acute respiratory distress syndrome. Crit Care Med. 2014;42(2): Dasenbrook EC, Needham DM, Brower RG, et al. Higher PEEP in patients with acute lung injury: a systematic review and Meta-analysis. Respir Care. 2011;56(5): Constantin JM, Jaber S, Futier E, et al. Respiratory effects of different recruitment maneuvers in acute respiratory distress syndrome. Critical Care. 2008;12:R Ranieri VM, Rubenfeld GD, Thompson BT, et al. Acute respiratory distress syndrome: the Berlin definition. JAMA. 2012;307: Gattinoni L, Carlesso E, Brazzi L, et al. Friday night ventilation: a safety starting tool kit for mechanically ventilated patients. Minerva Anestesiol. 2014;80(9): Guérin C, Beuret P, Constantin JM, et al. A prospective international observational prevalence study on prone positioning of ARDS patients: the APRONET (ARDS prone position network) study. Intensive Care Med. 2017; 44(1): Guérin C, Reignier J, Richard JC, et al. Prone positioning in severe acute respiratory distress syndrome. N Engl J Med. 2013;368(23): Bellani G, Laffey JG, Pham T, et al. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA. 2016;315(8): Guervilly C, Bisbal M, Forel JM, et al. Effects of neuromuscular blockers on transpulmonary pressures in moderate to severe acute respiratory distress syndrome. Intensive Care Med. 2016;43(3): Remblay LN, Slutsky AS. Ventilator-induced lung injury: from the bench to the bedside. Intensive Care Med. 2006;32(1): Tagami T, Sawabe M, Kushimoto S, et al. Quantitative diagnosis of diffuse alveolar damage using extravascular lung water. Crit Care Med. 2013;41(9):
Protective ventilation for ALL patients
 Protective ventilation for ALL patients PAOLO PELOSI, MD, FERS Department of Surgical Sciences and Integrated Diagnostics (DISC), San Martino Policlinico Hospital IRCCS for Oncology, University of Genoa,
Protective ventilation for ALL patients PAOLO PELOSI, MD, FERS Department of Surgical Sciences and Integrated Diagnostics (DISC), San Martino Policlinico Hospital IRCCS for Oncology, University of Genoa,
Should the ART trial change our practice?
 Editorial Should the ART trial change our practice? Jesús Villar 1,2,3, Fernando Suárez-Sipmann 1,4,5, Robert M. Kacmarek 6,7 1 CIBER de Enfermedades Respiratorias, Instituto de Salud Carlos III, Madrid,
Editorial Should the ART trial change our practice? Jesús Villar 1,2,3, Fernando Suárez-Sipmann 1,4,5, Robert M. Kacmarek 6,7 1 CIBER de Enfermedades Respiratorias, Instituto de Salud Carlos III, Madrid,
Analyzing Lung protective ventilation F Javier Belda MD, PhD Sº de Anestesiología y Reanimación. Hospital Clinico Universitario Valencia (Spain)
 Analyzing Lung protective ventilation F Javier Belda MD, PhD Sº de Anestesiología y Reanimación Hospital Clinico Universitario Valencia (Spain) ALI/ARDS Report of the American-European consensus conference
Analyzing Lung protective ventilation F Javier Belda MD, PhD Sº de Anestesiología y Reanimación Hospital Clinico Universitario Valencia (Spain) ALI/ARDS Report of the American-European consensus conference
Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS
 Zee and Gommers Critical Care (2019) 23:73 https://doi.org/10.1186/s13054-019-2365-1 REVIEW Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS Philip van der
Zee and Gommers Critical Care (2019) 23:73 https://doi.org/10.1186/s13054-019-2365-1 REVIEW Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS Philip van der
Sub-category: Intensive Care for Respiratory Distress
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Management of Severe ARDS: Current Canadian Practice
 Management of Severe ARDS: Current Canadian Practice Erick Duan MD FRCPC Clinical Scholar, Department of Medicine, Division of Critical Care, McMaster University Intensivist, St. Joseph's Healthcare Hamilton
Management of Severe ARDS: Current Canadian Practice Erick Duan MD FRCPC Clinical Scholar, Department of Medicine, Division of Critical Care, McMaster University Intensivist, St. Joseph's Healthcare Hamilton
Ventilatory Management of ARDS. Alexei Ortiz Milan; MD, MSc
 Ventilatory Management of ARDS Alexei Ortiz Milan; MD, MSc 2017 Outline Ventilatory management of ARDS Protected Ventilatory Strategy Use of NMB Selection of PEEP Driving pressure Lung Recruitment Prone
Ventilatory Management of ARDS Alexei Ortiz Milan; MD, MSc 2017 Outline Ventilatory management of ARDS Protected Ventilatory Strategy Use of NMB Selection of PEEP Driving pressure Lung Recruitment Prone
The new ARDS definitions: what does it mean?
 The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
Effect of peak inspiratory pressure on the development. of postoperative pulmonary complications.
 Effect of peak inspiratory pressure on the development of postoperative pulmonary complications in mechanically ventilated adult surgical patients: a systematic review protocol Chelsa Wamsley Donald Missel
Effect of peak inspiratory pressure on the development of postoperative pulmonary complications in mechanically ventilated adult surgical patients: a systematic review protocol Chelsa Wamsley Donald Missel
Higher PEEP in Patients With Acute Lung Injury: A Systematic Review and Meta-Analysis
 Original Research Higher in Patients With Acute Lung Injury: A Systematic Review and Meta-Analysis Elliott C Dasenbrook MD MHS, Dale M Needham MD PhD, Roy G Brower MD, and Eddy Fan MD BACKGROUND: Studies
Original Research Higher in Patients With Acute Lung Injury: A Systematic Review and Meta-Analysis Elliott C Dasenbrook MD MHS, Dale M Needham MD PhD, Roy G Brower MD, and Eddy Fan MD BACKGROUND: Studies
Application of Lung Protective Ventilation MUST Begin Immediately After Intubation
 Conflict of Interest Disclosure Robert M Kacmarek Managing Severe Hypoxemia!" 9-28-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts I disclose
Conflict of Interest Disclosure Robert M Kacmarek Managing Severe Hypoxemia!" 9-28-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts I disclose
Difficult Ventilation in ARDS Patients
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Driving Pressure and Hospital Mortality in Patients Without ARDS: A Cohort Study
 Accepted Manuscript Driving Pressure and Hospital Mortality in Patients Without ARDS: A Cohort Study Marcello F.S. Schmidt, MD, Andre C.K. B. Amaral, MD, Eddy Fan, MD, PhD, Gordon D. Rubenfeld, MD, MSc
Accepted Manuscript Driving Pressure and Hospital Mortality in Patients Without ARDS: A Cohort Study Marcello F.S. Schmidt, MD, Andre C.K. B. Amaral, MD, Eddy Fan, MD, PhD, Gordon D. Rubenfeld, MD, MSc
Oxygenation Failure. Increase FiO2. Titrate end-expiratory pressure. Adjust duty cycle to increase MAP. Patient Positioning. Inhaled Vasodilators
 Oxygenation Failure Increase FiO2 Titrate end-expiratory pressure Adjust duty cycle to increase MAP Patient Positioning Inhaled Vasodilators Extracorporeal Circulation ARDS Radiology Increasing Intensity
Oxygenation Failure Increase FiO2 Titrate end-expiratory pressure Adjust duty cycle to increase MAP Patient Positioning Inhaled Vasodilators Extracorporeal Circulation ARDS Radiology Increasing Intensity
ARDS Assisted ventilation and prone position. ICU Fellowship Training Radboudumc
 ARDS Assisted ventilation and prone position ICU Fellowship Training Radboudumc Fig. 1 Physiological mechanisms controlling respiratory drive and clinical consequences of inappropriate respiratory drive
ARDS Assisted ventilation and prone position ICU Fellowship Training Radboudumc Fig. 1 Physiological mechanisms controlling respiratory drive and clinical consequences of inappropriate respiratory drive
How ARDS should be treated in 2017
 How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013
 ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
APPENDIX VI HFOV Quick Guide
 APPENDIX VI HFOV Quick Guide Overall goal: Maintain PH in the target range at the minimum tidal volume. This is achieved by favoring higher frequencies over lower P (amplitude). This goal is also promoted
APPENDIX VI HFOV Quick Guide Overall goal: Maintain PH in the target range at the minimum tidal volume. This is achieved by favoring higher frequencies over lower P (amplitude). This goal is also promoted
Higher vs Lower Positive End-Expiratory Pressure in Patients With Acute Lung Injury and Acute Respiratory Distress Syndrome
 CARING FOR THE CRITICALLY ILL PATIENT vs Positive End-Expiratory Pressure in Patients With Acute Lung Injury and Acute Respiratory Distress Syndrome Systematic Review and Meta-analysis Matthias Briel,
CARING FOR THE CRITICALLY ILL PATIENT vs Positive End-Expiratory Pressure in Patients With Acute Lung Injury and Acute Respiratory Distress Syndrome Systematic Review and Meta-analysis Matthias Briel,
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Prone positioning reduces mortality from acute respiratory distress syndrome in the low tidal volume era: a meta-analysis
 Intensive Care Med (2014) 40:332 341 DOI 10.1007/s00134-013-3194-3 SYSTEMATIC REVIEW Jeremy R. Beitler Shahzad Shaefi Sydney B. Montesi Amy Devlin Stephen H. Loring Daniel Talmor Atul Malhotra Prone positioning
Intensive Care Med (2014) 40:332 341 DOI 10.1007/s00134-013-3194-3 SYSTEMATIC REVIEW Jeremy R. Beitler Shahzad Shaefi Sydney B. Montesi Amy Devlin Stephen H. Loring Daniel Talmor Atul Malhotra Prone positioning
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
ORIGINAL ARTICLE. &get_box_var; Abstract
 &get_box_var; ORIGINAL ARTICLE Oxygenation Response to Positive End-Expiratory Pressure Predicts Mortality in Acute Respiratory Distress Syndrome A Secondary Analysis of the LOVS and ExPress Trials Ewan
&get_box_var; ORIGINAL ARTICLE Oxygenation Response to Positive End-Expiratory Pressure Predicts Mortality in Acute Respiratory Distress Syndrome A Secondary Analysis of the LOVS and ExPress Trials Ewan
Ventilator ECMO Interactions
 Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
What s New About Proning?
 1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
RESPIRATORY CARE Paper in Press. Published on January 29, 2013 as DOI: /respcare.02068
 TITLE PAGE: Title: INDIVIDUALIZED POSITIVE END-EXPIRATORY PRESSURE SETTING IN PATIENTS WITH ACUTE RESPIRATORY DISTRESS SYNDROME. A RANDOMIZED CONTROLLED PILOT STUDY. Running title: INDIVIDUALIZED PEEP
TITLE PAGE: Title: INDIVIDUALIZED POSITIVE END-EXPIRATORY PRESSURE SETTING IN PATIENTS WITH ACUTE RESPIRATORY DISTRESS SYNDROME. A RANDOMIZED CONTROLLED PILOT STUDY. Running title: INDIVIDUALIZED PEEP
Acute Lung Injury/ARDS. Disclosures. Overview. Acute Respiratory Failure 5/30/2014. Research funding: NIH, UCSF CTSI, Glaxo Smith Kline
 Disclosures Acute Respiratory Failure Carolyn S. Calfee, MD MAS UCSF Critical Care Medicine and Trauma CME May 30, 2014 Research funding: NIH, UCSF CTSI, Glaxo Smith Kline Medical advisory boards: Cerus
Disclosures Acute Respiratory Failure Carolyn S. Calfee, MD MAS UCSF Critical Care Medicine and Trauma CME May 30, 2014 Research funding: NIH, UCSF CTSI, Glaxo Smith Kline Medical advisory boards: Cerus
Driving pressure: a marker of severity, a safety limit, or a goal for mechanical ventilation?
 Bugedo et al. Critical Care (2017) 21:199 DOI 10.1186/s13054-017-1779-x VIEWPOINT Driving pressure: a marker of severity, a safety limit, or a goal for mechanical ventilation? Guillermo Bugedo *, Jaime
Bugedo et al. Critical Care (2017) 21:199 DOI 10.1186/s13054-017-1779-x VIEWPOINT Driving pressure: a marker of severity, a safety limit, or a goal for mechanical ventilation? Guillermo Bugedo *, Jaime
Does proning patients with refractory hypoxaemia improve mortality?
 Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Effects of the use of neuromuscular blocking agents on acute respiratory distress syndrome outcomes: A systematic review
 Effects of the use of neuromuscular blocking agents on acute respiratory distress syndrome outcomes: A systematic review Samantha Paramore, AG-ACNP BC ABSTRACT Background and purpose: Acute respiratory
Effects of the use of neuromuscular blocking agents on acute respiratory distress syndrome outcomes: A systematic review Samantha Paramore, AG-ACNP BC ABSTRACT Background and purpose: Acute respiratory
This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness.
 Bibliography Lung recruitment This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness. Table of Contents 1 Effect of intensive
Bibliography Lung recruitment This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness. Table of Contents 1 Effect of intensive
Principles of Mechanical Ventilation
 47 Principles of Mechanical Ventilation Jonathan E. Sevransky, MD, MHS Objectives Understand the indications for treatment with mechanical ventilation Describe ventilator strategies that will minimize
47 Principles of Mechanical Ventilation Jonathan E. Sevransky, MD, MHS Objectives Understand the indications for treatment with mechanical ventilation Describe ventilator strategies that will minimize
This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness.
 Bibliography INTELLiVENT-ASV This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness. Table of Contents 1 Closed-loop ventilation
Bibliography INTELLiVENT-ASV This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness. Table of Contents 1 Closed-loop ventilation
Driving Pressure and Survival in the Acute Respiratory Distress Syndrome
 Special Article Driving Pressure and Survival in the Acute Respiratory Distress Syndrome Marcelo B.P. Amato, M.D., Maureen O. Meade, M.D., Arthur S. Slutsky, M.D., Laurent Brochard, M.D., Eduardo L.V.
Special Article Driving Pressure and Survival in the Acute Respiratory Distress Syndrome Marcelo B.P. Amato, M.D., Maureen O. Meade, M.D., Arthur S. Slutsky, M.D., Laurent Brochard, M.D., Eduardo L.V.
Seminar. Current Concepts
 Seminar Current Concepts In ARDS What I think is possible to cover in 40 minutes- Definition Management Ventilatory strategies Conventional LPV Rescue therapy Non Ventilatory strategies Definition and
Seminar Current Concepts In ARDS What I think is possible to cover in 40 minutes- Definition Management Ventilatory strategies Conventional LPV Rescue therapy Non Ventilatory strategies Definition and
Prone Position in ARDS
 Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services San Francisco General Hospital University of California, San Francisco, Case Study A 39 yo F admitted to SFGH TICU s/p hanging,
Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services San Francisco General Hospital University of California, San Francisco, Case Study A 39 yo F admitted to SFGH TICU s/p hanging,
Physiology to Improve RCTs
 Physiology to Improve RCTs Brian Kavanagh Hospital for Sick Children University of Toronto 1 Conflicts of Interest No financial conflict of interest with the subject matter of this talk Where s the Interest
Physiology to Improve RCTs Brian Kavanagh Hospital for Sick Children University of Toronto 1 Conflicts of Interest No financial conflict of interest with the subject matter of this talk Where s the Interest
Cardiorespiratory Physiotherapy Tutoring Services 2017
 VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
Transpulmonary pressure measurement
 White Paper Transpulmonary pressure measurement Benefit of measuring transpulmonary pressure in mechanically ventilated patients Dr. Jean-Michel Arnal, Senior Intensivist, Hopital Sainte Musse, Toulon,
White Paper Transpulmonary pressure measurement Benefit of measuring transpulmonary pressure in mechanically ventilated patients Dr. Jean-Michel Arnal, Senior Intensivist, Hopital Sainte Musse, Toulon,
Biomedical engineer s guide to the clinical aspects of intensive care mechanical ventilation
 https://doi.org/10.1186/s12938-018-0599-9 BioMedical Engineering OnLine REVIEW Open Access Biomedical engineer s guide to the clinical aspects of intensive care mechanical ventilation Vincent J. Major
https://doi.org/10.1186/s12938-018-0599-9 BioMedical Engineering OnLine REVIEW Open Access Biomedical engineer s guide to the clinical aspects of intensive care mechanical ventilation Vincent J. Major
APRV Ventilation Mode
 APRV Ventilation Mode Airway Pressure Release Ventilation A Type of CPAP Continuous Positive Airway Pressure (CPAP) with an intermittent release phase. Patient cycles between two levels of CPAP higher
APRV Ventilation Mode Airway Pressure Release Ventilation A Type of CPAP Continuous Positive Airway Pressure (CPAP) with an intermittent release phase. Patient cycles between two levels of CPAP higher
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
Prone position: the time of certainty*
 DOI 10.1007/s13546-013-0809-1 SESSION THÉMATIQUE MÉDECIN Prone position: the time of certainty* Décubitus ventral : le temps des certitudes C. Guérin Received: 14 August 2013; Accepted: 4 October 2013
DOI 10.1007/s13546-013-0809-1 SESSION THÉMATIQUE MÉDECIN Prone position: the time of certainty* Décubitus ventral : le temps des certitudes C. Guérin Received: 14 August 2013; Accepted: 4 October 2013
Lung Recruitment Strategies in Anesthesia
 Lung Recruitment Strategies in Anesthesia Intraoperative ventilatory management to prevent Post-operative Pulmonary Complications Kook-Hyun Lee, MD, PhD Department of Anesthesiology Seoul National University
Lung Recruitment Strategies in Anesthesia Intraoperative ventilatory management to prevent Post-operative Pulmonary Complications Kook-Hyun Lee, MD, PhD Department of Anesthesiology Seoul National University
Effects of N acetylcysteine treatment in acute respiratory distress syndrome: A meta analysis
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: 2863-2868, 2017 Effects of N acetylcysteine treatment in acute respiratory distress syndrome: A meta analysis YING ZHANG 1*, SHAOXUE DING 2*, CAIFENG LI 1, YIFENG
EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: 2863-2868, 2017 Effects of N acetylcysteine treatment in acute respiratory distress syndrome: A meta analysis YING ZHANG 1*, SHAOXUE DING 2*, CAIFENG LI 1, YIFENG
Respiratory insufficiency in bariatric patients
 Respiratory insufficiency in bariatric patients Special considerations or just more of the same? Weaning and rehabilation conference 6th November 2015 Definition of obesity Underweight BMI< 18 Normal weight
Respiratory insufficiency in bariatric patients Special considerations or just more of the same? Weaning and rehabilation conference 6th November 2015 Definition of obesity Underweight BMI< 18 Normal weight
Rescue therapies for acute respiratory distress syndrome: what to try first?
 REVIEW C URRENT OPINION Rescue therapies for acute respiratory distress syndrome: what to try first? Onnen Moerer, Tommaso Tonetti, and Michael Quintel Purpose of review Severe respiratory failure due
REVIEW C URRENT OPINION Rescue therapies for acute respiratory distress syndrome: what to try first? Onnen Moerer, Tommaso Tonetti, and Michael Quintel Purpose of review Severe respiratory failure due
Should we titrate positive end-expiratory pressure based on an end-expiratory transpulmonary pressure?
 Perspective Page 1 of 8 Should we titrate positive end-expiratory pressure based on an end-expiratory transpulmonary pressure? John J. Marini Department of Pulmonary and Critical Care Medicine, University
Perspective Page 1 of 8 Should we titrate positive end-expiratory pressure based on an end-expiratory transpulmonary pressure? John J. Marini Department of Pulmonary and Critical Care Medicine, University
11 th Annual Congress Turkish Thoracic Society. Mechanical Ventilation in Acute Hypoxemic Respiratory Failure
 11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
Clinical Study Increased Extravascular Lung Water Reduces the Efficacy of Alveolar Recruitment Maneuver in Acute Respiratory Distress Syndrome
 Critical Care Research and Practice Volume 2012, Article ID 606528, 7 pages doi:10.1155/2012/606528 Clinical Study Increased Extravascular Lung Water Reduces the Efficacy of Alveolar Recruitment Maneuver
Critical Care Research and Practice Volume 2012, Article ID 606528, 7 pages doi:10.1155/2012/606528 Clinical Study Increased Extravascular Lung Water Reduces the Efficacy of Alveolar Recruitment Maneuver
Breathing life into new therapies: Updates on treatment for severe respiratory failure. Whitney Gannon, MSN ACNP-BC
 Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
ARDS: The Evidence. Topics. New definition Breaths: Little or Big? Wet or Dry? Moving or Still? Upside down or Right side up?
 ARDS: The Evidence Todd M Bull MD Professor of Medicine Division of Pulmonary Sciences and Critical Care Division of Cardiology Director Pulmonary Vascular Disease Center Director Center for Lungs and
ARDS: The Evidence Todd M Bull MD Professor of Medicine Division of Pulmonary Sciences and Critical Care Division of Cardiology Director Pulmonary Vascular Disease Center Director Center for Lungs and
What links ventilator driving pressure with survival in the acute respiratory distress syndrome? A computational study
 Das et al. Respiratory Research (2019) 20:29 https://doi.org/10.1186/s12931-019-0990-5 RESEARCH What links ventilator driving pressure with survival in the acute respiratory distress syndrome? A computational
Das et al. Respiratory Research (2019) 20:29 https://doi.org/10.1186/s12931-019-0990-5 RESEARCH What links ventilator driving pressure with survival in the acute respiratory distress syndrome? A computational
Outline. Basic principles of lung protective ventilation. The challenging areas. Small tidal volumes Recruitment
 ARDS beyond 6/kg Gordon D. Rubenfeld, MD MSc Professor of Medicine, University of Toronto Chief, Program in Trauma, Emergency, and Critical Care Sunnybrook Health Sciences Centre Outline Basic principles
ARDS beyond 6/kg Gordon D. Rubenfeld, MD MSc Professor of Medicine, University of Toronto Chief, Program in Trauma, Emergency, and Critical Care Sunnybrook Health Sciences Centre Outline Basic principles
On the complexity of scoring acute respiratory distress syndrome: do not forget hemodynamics!
 Perspective On the complexity of scoring acute respiratory distress syndrome: do not forget hemodynamics! Xavier Repessé 1, Alix Aubry 1,2, Antoine Vieillard-Baron 1,2,3 1 Assistance Publique-Hôpitaux
Perspective On the complexity of scoring acute respiratory distress syndrome: do not forget hemodynamics! Xavier Repessé 1, Alix Aubry 1,2, Antoine Vieillard-Baron 1,2,3 1 Assistance Publique-Hôpitaux
Regional overdistension during prone positioning in a patient with acute respiratory failure who was ventilated with a low tidal volume: a case report
 Kotani et al. Journal of Intensive Care (2018) 6:18 https://doi.org/10.1186/s40560-018-0290-z CASE REPORT Regional overdistension during prone positioning in a patient with acute respiratory failure who
Kotani et al. Journal of Intensive Care (2018) 6:18 https://doi.org/10.1186/s40560-018-0290-z CASE REPORT Regional overdistension during prone positioning in a patient with acute respiratory failure who
ARDS Management Protocol
 ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
Experience with Low Flow ECCO2R device on a CRRT platform : CO2 removal
 Experience with Low Flow ECCO2R device on a CRRT platform : CO2 removal Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre
Experience with Low Flow ECCO2R device on a CRRT platform : CO2 removal Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre
Refresher Course MYTHS AND REALITY ABOUT LUNG MECHANICS 5 RC 2. European Society of Anaesthesiologists FIGURE 1 STATIC MEASUREMENTS
 European Society of Anaesthesiologists Refresher Course S AND ABOUT LUNG MECHANICS 5 RC 2 Anders LARSSON Gentofte University Hospital Copenhagen University Hellerup, Denmark Saturday May 31, 2003 Euroanaesthesia
European Society of Anaesthesiologists Refresher Course S AND ABOUT LUNG MECHANICS 5 RC 2 Anders LARSSON Gentofte University Hospital Copenhagen University Hellerup, Denmark Saturday May 31, 2003 Euroanaesthesia
Ventilation in Paediatric ARDS: extrapolate from adult studies?
 Ventilation in Paediatric ARDS: extrapolate from adult studies? ASMIC 2014 Dr Adrian Plunkett Consultant Paediatric Intensivist Birmingham Children s Hospital, UK Aims of the presentation Ventilation
Ventilation in Paediatric ARDS: extrapolate from adult studies? ASMIC 2014 Dr Adrian Plunkett Consultant Paediatric Intensivist Birmingham Children s Hospital, UK Aims of the presentation Ventilation
Author: Thomas Sisson, MD, 2009
 Author: Thomas Sisson, MD, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author: Thomas Sisson, MD, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
THE USE OF HYPERINFLATION IN THE MANAGEMENT OF INTUBATED AND VENTILATED ADULT PATIENTS RECOMMENDATIONS
 THE USE OF HYPERINFLATION IN THE MANAGEMENT OF INTUBATED AND VENTILATED ADULT PATIENTS RECOMMENDATIONS Recommendation 1 on website Hyperinflation (Ventilator or manual) might be included in the management
THE USE OF HYPERINFLATION IN THE MANAGEMENT OF INTUBATED AND VENTILATED ADULT PATIENTS RECOMMENDATIONS Recommendation 1 on website Hyperinflation (Ventilator or manual) might be included in the management
Case discussion Acute severe asthma during pregnancy. J.G. van der Hoeven
 Case discussion Acute severe asthma during pregnancy J.G. van der Hoeven Case (1) 32-year-old female - gravida 3 - para 2 Previous medical history - asthma Pregnant (33 w) Acute onset fever with wheezing
Case discussion Acute severe asthma during pregnancy J.G. van der Hoeven Case (1) 32-year-old female - gravida 3 - para 2 Previous medical history - asthma Pregnant (33 w) Acute onset fever with wheezing
SWISS SOCIETY OF NEONATOLOGY. Supercarbia in an infant with meconium aspiration syndrome
 SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
Part 2 of park s Ventilator and ARDS slides for syllabus
 Part 2 of park s Ventilator and ARDS slides for syllabus Early Neuromuscular Blockade Question 4 The early use of cis-atracurium in severe ARDS is: A. Contraindicated in patients with diabetes B. Associated
Part 2 of park s Ventilator and ARDS slides for syllabus Early Neuromuscular Blockade Question 4 The early use of cis-atracurium in severe ARDS is: A. Contraindicated in patients with diabetes B. Associated
Understanding test accuracy research: a test consequence graphic
 Whiting and Davenport Diagnostic and Prognostic Research (2018) 2:2 DOI 10.1186/s41512-017-0023-0 Diagnostic and Prognostic Research METHODOLOGY Understanding test accuracy research: a test consequence
Whiting and Davenport Diagnostic and Prognostic Research (2018) 2:2 DOI 10.1186/s41512-017-0023-0 Diagnostic and Prognostic Research METHODOLOGY Understanding test accuracy research: a test consequence
The Berlin Definition: Does it fix anything?
 The Berlin Definition: Does it fix anything? Gordon D. Rubenfeld, MD MSc Professor of Medicine, University of Toronto Chief, Program in Trauma, Emergency, and Critical Care Sunnybrook Health Sciences Centre
The Berlin Definition: Does it fix anything? Gordon D. Rubenfeld, MD MSc Professor of Medicine, University of Toronto Chief, Program in Trauma, Emergency, and Critical Care Sunnybrook Health Sciences Centre
This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness.
 Bibliography INTELLiVENT-ASV This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness. Table of Contents 1 Closed loop ventilation
Bibliography INTELLiVENT-ASV This bibliography is a literature reference for users and represents selected relevant publications, without any claim to completeness. Table of Contents 1 Closed loop ventilation
journal of medicine The new england High-Frequency Oscillation in Early Acute Respiratory Distress Syndrome A bs tr ac t
 The new england journal of medicine established in 1812 february 28, 2013 vol. 368 no. 9 High-Frequency Oscillation in Early Acute Respiratory Distress Syndrome Niall D. Ferguson, M.D., Deborah J. Cook,
The new england journal of medicine established in 1812 february 28, 2013 vol. 368 no. 9 High-Frequency Oscillation in Early Acute Respiratory Distress Syndrome Niall D. Ferguson, M.D., Deborah J. Cook,
APRV for ARDS: the complexities of a mode and how it affects even the best trials
 Editorial APRV for ARDS: the complexities of a mode and how it affects even the best trials Eduardo Mireles-Cabodevila 1,2, Siddharth Dugar 1,2, Robert L. Chatburn 1,2 1 Respiratory Institute, Cleveland
Editorial APRV for ARDS: the complexities of a mode and how it affects even the best trials Eduardo Mireles-Cabodevila 1,2, Siddharth Dugar 1,2, Robert L. Chatburn 1,2 1 Respiratory Institute, Cleveland
ARF, Mechaical Ventilation and PFTs: ACOI Board Review 2018
 ARF, Mechaical Ventilation and PFTs: ACOI Board Review 2018 Thomas F. Morley, DO, FACOI, FCCP, FAASM Professor of Medicine Chairman Department of Internal Medicine Director of the Division of Pulmonary,
ARF, Mechaical Ventilation and PFTs: ACOI Board Review 2018 Thomas F. Morley, DO, FACOI, FCCP, FAASM Professor of Medicine Chairman Department of Internal Medicine Director of the Division of Pulmonary,
How the Knowledge Proceeds in Intensive Care: the ARDS Example
 How the Knowledge Proceeds in Intensive Care: the ARDS Example 2016, Antalya Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany INDUCTION: From particular (application) to general (law/theory)
How the Knowledge Proceeds in Intensive Care: the ARDS Example 2016, Antalya Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany INDUCTION: From particular (application) to general (law/theory)
ARDS and treatment strategies
 ARDS and treatment strategies Geoff Bellingan Medical Director University College Hospital ARDS: Definitions History of predisposing condition Refractory hypoxaemia of acute onset PaO 2 /FiO 2 ratio:
ARDS and treatment strategies Geoff Bellingan Medical Director University College Hospital ARDS: Definitions History of predisposing condition Refractory hypoxaemia of acute onset PaO 2 /FiO 2 ratio:
ARDS A Brief Overview. Lucas Pitts, M.D. Assistant Professor of Medicine Pulmonary and Critical Care Medicine University of Kansas School of Medicine
 ARDS A Brief Overview Lucas Pitts, M.D. Assistant Professor of Medicine Pulmonary and Critical Care Medicine University of Kansas School of Medicine Outline Definition of ARDS Epidemiology of ARDS Pathophysiology
ARDS A Brief Overview Lucas Pitts, M.D. Assistant Professor of Medicine Pulmonary and Critical Care Medicine University of Kansas School of Medicine Outline Definition of ARDS Epidemiology of ARDS Pathophysiology
OSCAR & OSCILLATE. & the Future of High Frequency Oscillatory Ventilation (HFOV)
 & & the Future of High Frequency Oscillatory Ventilation (HFOV) www.philippelefevre.com What do we know already? Sud S et al. BMJ 2010 & Multi-centre randomised controlled trials of HFOV verses current
& & the Future of High Frequency Oscillatory Ventilation (HFOV) www.philippelefevre.com What do we know already? Sud S et al. BMJ 2010 & Multi-centre randomised controlled trials of HFOV verses current
Oxygenation improves during the first 8 h of extended-duration prone positioning in patients with respiratory failure: a retrospective study
 Miyamoto et al. Journal of Intensive Care 2014, 2:52 RESEARCH Open Access Oxygenation improves during the first 8 h of extended-duration prone positioning in patients with respiratory failure: a retrospective
Miyamoto et al. Journal of Intensive Care 2014, 2:52 RESEARCH Open Access Oxygenation improves during the first 8 h of extended-duration prone positioning in patients with respiratory failure: a retrospective
Dr. Yasser Fathi M.B.B.S, M.Sc, M.D. Anesthesia Consultant, Head of ICU King Saud Hospital, Unaizah
 BY Dr. Yasser Fathi M.B.B.S, M.Sc, M.D Anesthesia Consultant, Head of ICU King Saud Hospital, Unaizah Objectives For Discussion Respiratory Physiology Pulmonary Graphics BIPAP Graphics Trouble Shootings
BY Dr. Yasser Fathi M.B.B.S, M.Sc, M.D Anesthesia Consultant, Head of ICU King Saud Hospital, Unaizah Objectives For Discussion Respiratory Physiology Pulmonary Graphics BIPAP Graphics Trouble Shootings
ARDS: MANAGEMENT UPDATE
 ARDS: MANAGEMENT UPDATE Tanıl Kendirli, Assoc. Prof. Ankara University School of Medicine, Pediatric Critical Care Medicine The AECC Definition Timing Acute onset, within 48-72 hours Oxygenation ALI PaO2/FiO2
ARDS: MANAGEMENT UPDATE Tanıl Kendirli, Assoc. Prof. Ankara University School of Medicine, Pediatric Critical Care Medicine The AECC Definition Timing Acute onset, within 48-72 hours Oxygenation ALI PaO2/FiO2
Prone Position in ARDS
 Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services Department of Anesthesia & Perioperative Care University of California, San Francisco, San Francisco General Hospital Case
Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services Department of Anesthesia & Perioperative Care University of California, San Francisco, San Francisco General Hospital Case
Original Article Ultrasound reaeration scores to assess lung recruitment in rabbits with acute respiratory distress syndrome
 Int J Clin Exp Med 2018;11(8):7761-7769 www.ijcem.com /ISSN:1940-5901/IJCEM0077713 Original Article Ultrasound reaeration scores to assess lung recruitment in rabbits with acute respiratory distress syndrome
Int J Clin Exp Med 2018;11(8):7761-7769 www.ijcem.com /ISSN:1940-5901/IJCEM0077713 Original Article Ultrasound reaeration scores to assess lung recruitment in rabbits with acute respiratory distress syndrome
All rights, in particular the proprietary rights of use and exploitation relating to the following contribution as well as parts thereof (including
 All rights, in particular the proprietary rights of use and exploitation relating to the following contribution as well as parts thereof (including figures and tables) are the exclusive property of Springer
All rights, in particular the proprietary rights of use and exploitation relating to the following contribution as well as parts thereof (including figures and tables) are the exclusive property of Springer
Respiratory failure requiring mechanical ventilation
 Current Issues in Mechanical Ventilation for Respiratory Failure* Neil R. MacIntyre, MD The morbidity and mortality associated with respiratory failure is, to a certain extent, iatrogenic. Mechanical ventilation,
Current Issues in Mechanical Ventilation for Respiratory Failure* Neil R. MacIntyre, MD The morbidity and mortality associated with respiratory failure is, to a certain extent, iatrogenic. Mechanical ventilation,
ARF. 8 8 (PaO 2 / FIO 2 ) NPPV NPPV ( P = 0.37) NPPV NPPV. (PaO 2 / FIO 2 > 200 PaO 2 / FIO 2 NPPV > 100) (P = 0.02) NPPV ( NPPV P = 0.
 Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
ARDS & TBI - Trading Off Ventilation Targets
 ARDS & TBI - Trading Off Ventilation Targets Salvatore M. Maggiore, MD, PhD Rome, Italy smmaggiore@rm.unicatt.it Conflict of interest Principal Investigator: RINO trial o Nasal high-flow vs Venturi mask
ARDS & TBI - Trading Off Ventilation Targets Salvatore M. Maggiore, MD, PhD Rome, Italy smmaggiore@rm.unicatt.it Conflict of interest Principal Investigator: RINO trial o Nasal high-flow vs Venturi mask
Severe Hypoxemic Respiratory Failure
 CHEST Postgraduate Education Corner CONTEMPORARY REVIEWS IN CRITICAL CARE MEDICINE Severe Hypoxemic Respiratory Failure Part 1 Ventilatory Strategies Adebayo Esan, MD ; Dean R. Hess, PhD, RRT, FCCP ; Suhail
CHEST Postgraduate Education Corner CONTEMPORARY REVIEWS IN CRITICAL CARE MEDICINE Severe Hypoxemic Respiratory Failure Part 1 Ventilatory Strategies Adebayo Esan, MD ; Dean R. Hess, PhD, RRT, FCCP ; Suhail
Shan-Shan Meng, Wei Chang, Zhong-Hua Lu, Jian-Feng Xie, Hai-Bo Qiu, Yi Yang and Feng-Mei Guo *
 Meng et al. BMC Pulmonary Medicine (2019) 19:9 https://doi.org/10.1186/s12890-018-0761-y RESEARCH ARTICLE Open Access Effect of surfactant administration on outcomes of adult patients in acute respiratory
Meng et al. BMC Pulmonary Medicine (2019) 19:9 https://doi.org/10.1186/s12890-018-0761-y RESEARCH ARTICLE Open Access Effect of surfactant administration on outcomes of adult patients in acute respiratory
Weaning and extubation in PICU An evidence-based approach
 Weaning and extubation in PICU An evidence-based approach Suchada Sritippayawan, MD. Div. Pulmonology & Crit Care Dept. Pediatrics Faculty of Medicine Chulalongkorn University Kanokporn Udomittipong, MD.
Weaning and extubation in PICU An evidence-based approach Suchada Sritippayawan, MD. Div. Pulmonology & Crit Care Dept. Pediatrics Faculty of Medicine Chulalongkorn University Kanokporn Udomittipong, MD.
RESEARCH. High frequency oscillation in patients with acute lung injury andacuterespiratorydistresssyndrome(ards):systematic review and meta-analysis
 High frequency oscillation in patients with acute lung injury andacuterespiratorydistresssyndrome(ards):systematic review and meta-analysis Sachin Sud, fellow, 1 Maneesh Sud, medical student, 2 Jan O Friedrich,
High frequency oscillation in patients with acute lung injury andacuterespiratorydistresssyndrome(ards):systematic review and meta-analysis Sachin Sud, fellow, 1 Maneesh Sud, medical student, 2 Jan O Friedrich,
Acute respiratory distress syndrome
 20 Acute respiratory distress syndrome Introduction i Key points Acute respiratory distress syndrome is triggered by injury to the alveolar capillary barrier from any of a variety of causes, resulting
20 Acute respiratory distress syndrome Introduction i Key points Acute respiratory distress syndrome is triggered by injury to the alveolar capillary barrier from any of a variety of causes, resulting
Is ARDS Important to Recognize?
 Is ARDS Important to Recognize? Lorraine B. Ware MD Vanderbilt University Financial Disclosures: research funding from Boehringer Ingelheim, Global Blood Therapeutics Why diagnose ARDS? -initiate specific
Is ARDS Important to Recognize? Lorraine B. Ware MD Vanderbilt University Financial Disclosures: research funding from Boehringer Ingelheim, Global Blood Therapeutics Why diagnose ARDS? -initiate specific
ARDS and Lung Protection
 ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
Post Arrest Ventilation/Oxygenation Management
 Post Arrest Ventilation/Oxygenation Management Richard Branson MSc RRT Professor of Surgery University of Cincinnati Editor-In-Chief Respiratory Care 0 Presenter Disclosure Information Richard Branson
Post Arrest Ventilation/Oxygenation Management Richard Branson MSc RRT Professor of Surgery University of Cincinnati Editor-In-Chief Respiratory Care 0 Presenter Disclosure Information Richard Branson
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Neuromuscular Blockade in ARDS
 Neuromuscular Blockade in ARDS Maureen O. Meade, MD, FRCPC Critical care consultant, Hamilton Health Sciences Professor of Medicine, McMaster University www.oscillatetrial.com Disclosures None Possible
Neuromuscular Blockade in ARDS Maureen O. Meade, MD, FRCPC Critical care consultant, Hamilton Health Sciences Professor of Medicine, McMaster University www.oscillatetrial.com Disclosures None Possible
Mechanical Ventilation in Adults with Acute Respiratory Distress Syndrome Summary of the Experimental Evidence for the Clinical Practice Guideline
 Mechanical Ventilation in Adults with Acute Respiratory Distress Syndrome Summary of the Experimental Evidence for the Clinical Practice Guideline Lorenzo Del Sorbo 1, Ewan C. Goligher 1, Daniel F. McAuley
Mechanical Ventilation in Adults with Acute Respiratory Distress Syndrome Summary of the Experimental Evidence for the Clinical Practice Guideline Lorenzo Del Sorbo 1, Ewan C. Goligher 1, Daniel F. McAuley
Incidence of dyssynchronous spontaneous Breathing Effort, breath-stacking and reverse triggering in early ARDS. - The BEARDS project -
 Incidence of dyssynchronous spontaneous Breathing Effort, breath-stacking and reverse triggering in early ARDS - The BEARDS project - Scientific committee: Tai Pham Martin Dres Irene Telias Tommaso Mauri
Incidence of dyssynchronous spontaneous Breathing Effort, breath-stacking and reverse triggering in early ARDS - The BEARDS project - Scientific committee: Tai Pham Martin Dres Irene Telias Tommaso Mauri
Best of Pulmonary Jennifer R. Hucks, MD University of South Carolina School of Medicine
 Best of Pulmonary 2012-2013 Jennifer R. Hucks, MD University of South Carolina School of Medicine Topics ARDS- Berlin Definition Prone Positioning For ARDS Lung Protective Ventilation In Patients Without
Best of Pulmonary 2012-2013 Jennifer R. Hucks, MD University of South Carolina School of Medicine Topics ARDS- Berlin Definition Prone Positioning For ARDS Lung Protective Ventilation In Patients Without
Inhaled nitric oxide: clinical evidence for use in adults
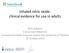 Inhaled nitric oxide: clinical evidence for use in adults Neill Adhikari Critical Care Medicine Sunnybrook Health Sciences Centre and University of Toronto 31 October 2014 Conflict of interest Ikaria provided
Inhaled nitric oxide: clinical evidence for use in adults Neill Adhikari Critical Care Medicine Sunnybrook Health Sciences Centre and University of Toronto 31 October 2014 Conflict of interest Ikaria provided
