The Sensitivity of High-Resolution CT in Detecting Idiopathic Pulmonary Fibrosis Proved by Open Lung Biopsy*
|
|
|
- Holly Wheeler
- 6 years ago
- Views:
Transcription
1 The Sensitivity of High-Resolution CT in Detecting Idiopathic Pulmonary Fibrosis Proved by Open Lung Biopsy* A Prospective Study jonathan B. Orens, MD; Ella A. Kazerooni, MD, FCCP; Fernando]. Martinez, MD, FCCP; Jeffrey L. Curtis, MD; Barry H. Gross, MD, FCCP; Andrew Flint, MD, FCCP; and Joseph P. Lynch III, MD, FCCP Objectives: To assess the sensitivity of high-resolution chest computed tomography (HRCT) in detecting idiopathic pulmonary fibrosis proved by biopsy specimen. To determine the degree of physiologic and pathologic abnormalities in patients with idiopathic pulmonary fibrosis who have a false-negative HRCT. Design: Prospective 2-year study. Setting: Tertiary care university hospital. Patients: All patients with dyspnea and suspected interstitial lung disease referred to the University of Michigan for enrollment in the Idiopathic Pulmonary Fibrosis Specialized Center of Research (SCOR) protocol were included; 25 underwent open lung biopsy and formed the final study group. Measurements: All patients underwent physiologic (pulmonary function, gas exchange, and exercise testing), radiologic (chest x-ray film and HRCT), and pathologic assessments (bronchoscopic and open lung biopsy). The results of HRCT were prospectively compared with results of standard pulmonary function tests, cardiopulmonary exercise testing, and open lung biopsy. Results: Of 25 patients who had both HRCT and open lung biopsy, 3 patients (12%) had HRCTs that demonstrated no evidence of interstitial lung disease. These three patients had less severe disease based on clinical, radiographic, and physiologic (CRP) scores, gas exchange abnormalities, and pathologic scoring of open lung biopsy specimens, compared with those with an abnormal HRCT. Conclusion: We conclude that in the evaluation of patients with dyspnea and abnormal results of pulmonary function studies, a normal HRCT does not exclude early and clinically significant interstitial lung disease. In our patient population, physiologic testing was more sensitive than HRCT in detecting mild abnormalities in patients with idiopathic pulmonary fibrosis proved by biopsy specimen. (CHEST 1995; 108:109-15) CPET=cardiopulmonary exercise testing; CRP=clinical, radiographic, and physiologic; HRCT=high-resolution computed tomography; PFT=pulmonary function test; SCOR=Specialized Center of Research Key words: high-resolution computed tomography; idiopathic pulmonary fibrosis; pulmonary function tests; sensitivity The evaluation of patients with dyspnea is a complex diagnostic challenge. Dyspnea may arise from pulmonary, cardiac, muscular, or neuropsychiatric abnormalities. However, most dyspneic patients, regardless of the treatment setting, have pulmonary disease. 1 Therefore, excluding the presence of pulmonary parenchymal abnormalities is a critical *From the Departments of Internal Medicine (Drs. Orens, Martinez, Curtis, and Lynch), Radiology (Drs. Kazerooni and Gross), and Pathology (Dr. Flint), The University of Michigan School of Medicine, Ann Arbor. Supported in part by National Institutes of Health NHLBI grant P50HL46487, NIH/ NCRR 3 MOl RR S3, and by funds from the Clinical Research Center of the University of Michigan grant M01RR Manuscript received September 6, 1994; revision accepted November 23. part of the diagnostic workup. Many techniques have been used to accomplish this goal, including radiologic and nuclear imaging studies, pulmonary function testing (PFTs), cardiopulmonary exercise testing (CPET), and various biopsy techniques. Advances in imaging technologies have raised questions about the critical diagnostic pathway for dyspneic patients. Recently, a new method for performing CT scanning of the lung parenchyma, high-resolution CT (HRCT), has been shown to more clearly delineate the anatomy of the lungs when compared with conventional CT. 2 Specifically, because HRCT can image to the anatomic level of the secondary pulmonary lobule, the necessity of performing a biopsy to establish the diagnosis of interstitial lung disease has been questioned.3 If HRCT is to replace open lung biopsy, the CHEST / 108 / 1 / JULY,
2 false-negative rate of HRCT must be established. To test adequately the sensitivity of HRCT, it is essential to evaluate a homogeneous population of patients with a diagnosis confirmed by open lung biopsy specimen. We chose to address this issue in patients with idiopathic pulmonary fibrosis because open lung biopsy specimens are still considered the standard for establishing the diagnosis of this important disease. 4 5 Given the morbidity and high cost of open lung biopsy, it is essential to establish whether open lung biopsy specimens are still necessary to confirm this disease. Because the anatomic abnormalities of idiopathic pulmonary fibrosis are progressive, beginning with microscopic inflammation that precedes fibrosis, we hypothesized that some patients may have microscopic disease undetectable by HRCT. Accordingly, we prospectively evaluated dyspneic patients with suspected interstitial lung disease using plain chest radiographs, PFTs, CPET, HRCT, and when indicated, trans bronchial and open lung biopsy, to establish the cause of their complaint. To establish the sensitivity of HRCT in detecting.idiopathic pulmonary fibrosis, results of HRCT were compared with open lung biopsy specimens in 25 patients with confirmed idiopathic pulmonary fibrosis. Additionally, the severity of the disease in each patient was graded by an assessment of the degree of abnormalities of physiologic test results and pathologic findings. Patient Recruitment METHODS Patients were entered into the study protocol in a prospective fashion between January 1, 1992 and December 31, The FIGURE l. Representative HRCT scan of case 1 reveals normal lung parenchyma. There is no evidence of ground-glass opacification, thickening of septal lines, or cystic changes. initial study group included all patients referred to the University of Michigan for enrollment in the Idiopathic Pulmonary Fibrosis Specialized Center of Research (SCOR) protocol (n = 65). Patients were eligible if there was a clinical suspicion of idiopathic pulmonary fibrosis based on symptoms, physiologic abnormalities, or radiographic findings, and neither previous biopsy nor therapy. Patients were excluded if during the enrollment workup they were found to have a disease other than idiopathic pulmonary fibrosis (n=23). Specifically, excluded patients had the following entities: collagen vascular disease, pneumoconiosis, sarcoidosis, cancer, lymphoma, eosinophilic granuloma, and lymphangioleiomyomatosis. Additionally, patients were excluded if they had medically unstable conditions, or were unwilling to undergo, open or video-assisted thoracoscopic lung biopsy (n=17). HRCT Protocol All HRCTs were performed with 1.0- or 1.5-mm-thick sections taken at 1-cm intervals throughout the entire thorax and were reconstructed using a bone algorithm. No intravenous contrast was administered. The scans were performed using a CT scanner (General Electric HiLite Advantage CT/ T scanner, GE Medical Systems, Milwaukee). For scoring, HRCT scans of patients with Table 1-CRP Scoring Results Normal Abnormal Parameter HRCT HRCT p Value Subjective score 10.7 ± ± 1.3 NS* Radiographic score 1.3 ± ±0.3 Physiologic score 10.5± ± 1.5 NS FVC 64.7± ±3.7 NS FEV ± ±4.2 NS Thoracic gas volume 59.3± ± DCO/ VA 110.7± ± Resting P(A-a)02 3.9± ± Exercise score 8.3± ±2.0 NS Total CRP 24.6± ± *NS=not significant. 110 Clinical Investigations
3 Table 2-Pathologic Scoring Results Parameter Normal HRCT Inflammatory/ exudative changes Alveolar wall Cell infiltrate (total 3.8 ± 0.3 extent) Cell infiltrate (average l.l ± 0.1 severity) Bronchiolar metaplasia 0.0±0.0 Hyperplasia 0.0 ± 0.0 Alveolar space Cellularity (total 2.1 ±0.6 extent) Cellularity (average 1.1 ± 0.1 severity) Fibrotic/ reparative changes Alveolar wall Interstitial young 0.0±0.0 connective tissue Interstitial fibrosis (% 2.0±0.3 alveolar wall) Honeycombing 0.2±0.1 alone (%) Smooth muscle (% ) 0.0±0.0 low power Vessel myointimal 0.7±0.2 changes (extent) Vessel myointimal 0.6±0.1 changes (severity) Abnormal HRCT 4.4± ± ± ± ± ± ± ± ± ± ± ±0.2 p Value idiopathic pulmonary fibrosis (proved by open lung biopsy specimens after HRCT obtained) (n=25) were coded and mixed with HRCT scans of patients (n=27) with a variety of alternative diagnoses (including pulmonary hypertension, sarcoidosis, lymphoma/ cancer, eosinophilic granuloma, pulmonary fibrosis associated with collagen vascular disease, and suspected but not biopsy specimen-proved idiopathic pulmonary fibrosis). Two experienced thoracic radiologists (B.H.G. and E.A.K.) independently evaluated all HRCTs for evidence of interstitial lung disease. At the time of CT interpretation, the two radiologists were not aware of the patient's history, physiologic assessment, or lung biopsy results. Scans were graded as either abnormal or normal for interstitial lung disease based on previously published criteria 6 The criteria for a positive interpretation included one or more of the following: irregular interlobular septal thickening, intralobular interstitial thickening or irregular interfaces, visible intralobular bronchioles, honeycombing, traction bronchiectasis, or ground-glass opacity. All HRCTs in the 25 patients with idiopathic pulmonary fibrosis were obtained 1 to 4 weeks before open lung biopsy. Physiologic Assessment The physiologic assessment was performed before open lung biopsy and initiation of therapy. Pulmonary function tests, including spirometry, lung volumes, and DCO, were performed on the same day but before CPET. All spirometric studies were performed on a calibrated pneumotachograph (Medical Graphics Co, St. Paul, Minn), and values were expressed as a percent of the predicted values published by Morris et ap Lung volumes were measured in a whole-body plethysmograph, using the technique of Dubois et al; 8 data were expressed as a percent of the predicted values published by Goldman and Becklake. 9 Diffusion capacity was measured using the technique of Ogilvie et al 10 and was expressed as a percent of the predicted values published by Crapo and Morris. 11 CPETs were performed on an electronically braked, calibrated cycle ergometer. Work load was increased by 20 W /min until maximal symptom-limited exercise was achieved. Expired gases and ventilation were measured using a calibrated metabolic cart (2001 System, Medical Graphics Co, St. Paul, Minn, or Collins CPXII, Warren E. Collins, Inc, Braintree, Mass). Arterial blood gas values were obtained at rest and every 2 min of exercise via an indwelling radial artery catheter. P(A-a)Oz was calculated for each sample by the alveolar gas equation, using the measured R value during the same time-point of exercise. Oxygen saturation was measured by co-oximetry of the blood gas sample. Twelvelead electrocardiograms and noninvasive measurements of blood pressure were recorded every minute of exercise. The values of Jones et ajl 2 were used to predict maximal exercise oxygen consumption (Voz). CRP Scoring System Overall clinical severity was assessed for each patient using a previously developed composite clinical, radiographic, and physiologic (CRP) score for idiopathic pulmonary fibrosis. 13 The total CRP score ranges from 0 to 100 points (100 being the most severe disease) based on seven variables that include the following: level of dyspnea, 0 to 20 points; chest radiograph, 0 to 10 points; spirometry (FVC, 0 to 12 points; FEY[, 0 to 3 points); lung volume, 0 to 10 points; diffusion capacity (corrected for alveolar volume), 0 to 5 points; resting P(A-a)Oz, 0 to 10 points; Oz saturation corrected for maximal achieved Vozmax, 0 to 30 points. Biopsy Technique All patients underwent bronchoscopy with bronchoalveolar lavage and transbronchial biopsies before open lung biopsy. Patients were referred for open lung biopsy when the results of transbronchial biopsy did not reveal a clear-cut alternative diagnosis. Open lung biopsy was performed by formal thoracotomy (n=7) or video-assisted thoracoscopy (n= 18). Similar-sized biopsy specimens were obtained by either technique. Biopsy specimens were obtained from all three lobes on the right side or from the upper and lower lobe on the left with exclusion of the lingula. Pathologic Scoring To correlate the severity of disease with the presence or absence of abnormalities on HRCT, all open lung biopsy specimens were reviewed by a specialist in lung pathology (A. F.). The pathologist was not aware of the radiographic scoring for individual patients at the time of pathologic scoring. Each specimen was processed in routine fashion. 14 Four histologic sections were prepared from each paraffin block. Individual slides were stained with hematoxylin-eosin, pentachrome stain (which demonstrates differential staining of elastic tissue, collagenized connective tissue, and mucopolysaccharide-rich stroma), Prussian blue (iron stain), and a trichrome stain (which demonstrates differential staining of collagenized connective tissue and smooth muscle). The alveolar septa, alveolar spaces, airways, and blood vessels were evaluated semiquantitatively (on a scale of 0 to 5) for cellular infiltrates (extent and severity), granulation tissue (absence or presence, and degree), honeycombing, interstitial fibrosis, interstitial young connective tissue, vessel myointimal changes, airway (terminal and respiratory bronchioles) mural inflammation and fibrosis, and luminal granulation tissue. These scores were tabulated separately and incorporated into inflammatory, fibrotic, and total pathology scores. Statistical Analysis All data were compiled into a total CRP score and a total CHEST/108/1/JULY,
4 pathologic score, 13 which were compared with the results of chest radiographs and HRCTs. Comparisons between patients with a normal HRCT vs those with an abnormal HRCT were performed with a two-tailed Student's t test; a p value of <0.05 was considered statistically significant. Patient Characteristics RESULTS The study group consisted of 25 patients with abnormal open lung biopsy specimens compatible with idiopathic pulmonary fibrosis. An approximately equal number of men (n=12) and women (n=13) were present. The mean age for the total group was 55.7 years (range, 28 to 74 years). There was a significant difference between the ages of the group with normal HRCTs (see below) (41.3 years; range, 38 to 43 years) and the group with abnormal HRCTs (56.9 years; range, 28 to 74 years; p=). Radiologic Imaging An abnormal HRCT compatible with interstitial lung disease was found in 22 of the 25 patients with biopsy specimen-proven idiopathic pulmonary fibrosis (88.0%). Importantly, three patients had HRCT scans that were not indicative of interstitial lung disease (Fig 1). Clinical features of these three patients are summarized in the Appendix. Plain chest radiographs were normal in all three patients with normal HRCTs, as well as in one patient with an abnormal HRCT. Thus, 3 of the 25 patients (12.0%) had HRCTs and 4 of the 25 patients (16%) had chest radiographs that did not reveal evidence of interstitial lung disease, when there was open lung biopsy evidence of idiopathic pulmonary fibrosis. The two radiologists agreed on the interpretation of the chest radiographs and HRCTs in all cases. Physiologic Assessment Patients with a normal HRCT had a similar perceived level of breathlessness (subjective score) compared with those whose scans were abnormal (Table 1). Neither the overall physiologic score nor spirometry (FEV 1 and FVC) differed significantly between those patients with a normal HRCT and those with an abnormal HRCT (Table 1). Additionally, total lung capacity (TLC) as a percent of predicted did not differ between the two groups (68.6 ± 9.5% for those with an abnormal HRCT vs 77.0 ± 3.6% for those with a normal HRCT, p=0.48). However, there was a significant difference between the two groups of patients in measurements that reflect abnormalities of gas exchange. Thus, DCO as a percent of predicted (46.1 ± 2.3% for those with an abnormal HRCT vs 65.7 ± 3.8% for those with a normal HRCT; p=0.01), DCO/ VA as a percent of predicted (Table 1), and resting P(A-a)Oz (Table 1) were all more abnormal in patients with an abnormal HRCT compared with those with a normal HRCT. During CPET, there was no significant difference between the two groups in exercise score (Table 1), in maximal achieved Vo2 as a percent of predicted (64.03 ± 4.26% for those with an abnormal HRCT vs 67.5 ± 2.0% for those with a normal HRCT; p=0.47), or in maximal achieved work rate (100.0 ± 0.0 W for those with an abnormal HRCT vs ± 3.9 W for those with a normal HRCT; p=0.33). However, despite this similarity in achieved Voz, there was a significant difference in 02 saturation at maximal exercise (87.6± 1.1% for those with an abnormal HRCT vs 96.3± 1.1 % for those with a normal HRCT; p=0.005). This result also indicates less severe abnormalities of gas exchange. Importantly, the total CRP score was lower (less abnormal) for the group with a normal HRCT (Table 1). Pathologic Scoring Similar pathologic features were evident in the lung biopsy samples from the three patients with HRCT not suggesting idiopathic pulmonary fibrosis. Figure 1 shows thin alveolar septa that were delicate in most areas of the parenchyma. A usually subtle alveolar wall infiltrate of lymphocytes and rare histiocytes was present in many areas. Small numbers of intra-alveolar macrophages were evident as was focal alveolar wall fibrosis. The airways appeared normal. Pneumocyte hyperplasia and alveolar wall metaplasia were only rarely observed. Extensive fibrosis or honeycomb formation was not identified. These mild features were confirmed by the low scores for all pathologic criteria shown in Table 2. In contrast, those patients with HRCT indicating interstitial lung disease showed significantly worse pathologic changes in all areas independently scored (Table 2). DISCUSSION Three salient findings emerge from our study. First, as previously documented for normal plain chest radiographs, 15 a normal HRCT does not exclude clinically significant idiopathic pulmonary fibrosis in symptomatic patients. Second, in our group of patients, physiologic studies were more sensitive than HRCT in detecting idiopathic pulmonary fibrosis. Third, patients with an HRCT that did not indicate idiopathic pulmonary fibrosis had milder disease, as demonstrated by the results of pathologic and CRP scoring. Although our study shows that HRCT is, in fact, a good tool for detecting idiopathic pulmonary fibrosis with a sensitivity of 88%, it is not sensitive enough to detect all cases, particularly when mild disease exists. With the powerful imaging capabilities of 112 Clir.ical Investigations
5 HRCT, many clinicians have come to rely on this test to exclude such diseases as idiopathic pulmonary fibrosis when evaluating patients with dyspnea. However, previous studies have not documented a falsenegative rate for HRCT in detecting idiopathic pulmonary fibrosis. The findings from our study suggest that reliance on HRCT alone is not appropriate. Additional studies in patients with interstitial lung disease because other confirmed etiologies are needed. Despite the less-than-perfect sensitivity of HRCT, we believe it is a highly useful part of the workup of the dyspneic patient with decreased DCO. Numerous radiologic studies have documented a high correlation between pathologic findings and radiologic changes with HRCT.l 6 17 HRCT complements physiologic assessment by pointing toward likely specific etiologies. HRCT can reliably detect macroscopic emphysema, an alternative cause of altered gas exchange, even in patients without evidence of airflow obstruction.l 8 In patients with focal abnormalities, HRCT is very helpful in selecting sites for biopsy. HRCT is also superior to plain radiographs or conventional CT scanning in following potential changes during therapy of idiopathic pulmonary fibrosis, including resolution, stabilization, or deterioration It is important to recognize that PFT results were abnormal in every patient with idiopathic pulmonary fibrosis proved by biopsy specimen, including those in whom HRCT failed to detect the abnormality. The most common PFT abnormality was a reduced DCO. Thus, our study supports previous reports that have shown that abnormal pulmonary function (particularly a low DCO) in symptomatic patients requires further assessment, including lung biopsy.l 5 21 However, physiologic tests, although highly sensitive, are nonspecific and cannot be relied on solely to establish a firm diagnosis in interstitial lung disease. All patients in this study were referred to our tertiary care center, which has a widely recognized interest in interstitial lung disease. Moreover, all patients were symptomatic and had physiologic abnormalities. Hence, our data should not be extrapolated to the treatment of asymptomatic patients. Although our study documented only three cases in which HRCT failed to detect idiopathic pulmonary fibrosis, such patients are perhaps the most important to identify, as they may be the single group with the most likely chance of responding to therapy. Idiopathic pulmonary fibrosis has been postulated to progress from an early inflammatory stage, which may respond to therapy, to fibrosis, which is seldom reversible This hypothesis is supported by the observation that patients with idiopathic pulmonary fibrosis with predominantly ground-glass opacification (the radiologic correlate of early disease-alveolitis) on initial HRCT rather than reticular patterns (the radiologic correlate of late disease-fibrosis) have improved response to therapy and better survivaj Determining whether patients with initially milder, radiologically inapparent disease have a better response to therapy will require further studies with long-term follow-up. It is highly unlikely that the cases not detected by HRCT were due to technical inadequacy of imaging. In our study, the HRCT was performed with 1.0- to 1.5-mm sections at 1-cm intervals throughout the entire chest. This procedure differs from that of some centers, where thin sections are obtained at only three or four levels throughout the chest. Since idiopathic pulmonary fibrosis may cause patchy abnormalities with normal-appearing lung adjacent to highly distorted parenchyma, the latter protocol may miss areas of diseased lung. Furthermore, in our study, two highly experienced CT radiologists agreed on the interpretation of the scans in all cases; thus, there was no interobserver variability. To establish a standard to compare prospectively individual patients with idiopathic pulmonary fibrosis, we used previously published scoring methods for pathologic and physiologic assessments (CRP and pathologic score).l 3.l 4 Such a standardized scoring system is necessary for assessing a disease such as idiopathic pulmonary fibrosis, which is relatively rare and which has a heterogeneous clinical course. Data from our study support previous findings of studies using the CRP score, in that individual components of the CRP may not be significantly abnormal until added together into a total composite score. Furthermore, this total score correlates closely with the degree of anatomic abnormalities found at open lung biopsy.l 3 Based on the results of this study, we conclude that in the evaluation of patients with dyspnea, abnormal pulmonary function, and suspected interstitial lung disease, a normal HRCT does not exclude the presence of idiopathic pulmonary fibrosis. Physiologic testing, including standard PFT and CPET, should be pursued early in the evaluation of patients with unexplained dyspnea, even if imaging procedures are normal. If the clinical suspicion for interstitial lung disease is high, a normal HRCT should not exclude further evaluation with definition of etiology by lung biopsy specimen. ACKNOWLEDGMENTS: The authors wish to acknowledge Janet Hampton, RN, who coordinated patient evaluations and collected data for this study. We also wish to acknowledge M. Anthony Schork, PhD, and Molly Young for their assistance with statistical analysis. CASE 1 APPENDIX A 38-year-old black woman was evaluated at an outside hospital for chronic dyspnea and cough. She CHEST / 108/1 I JULY,
6 FIGURE 2. Open lung biopsy specimen. Small numbers of macrophages lie within alveolar spaces. Rare alveolar septae are thickened by collagen deposits (arrows) (hematoxylin-eosin, original magnification Xl65). had been exposed to toluene diisocyanate (TDI) during a brief period at her work place and had been treated for TDI-induced asthma. Subsequent pulmonary function studies revealed an FVC of 1.97 L (51 % of predicted), FEY 1 of L (57% of predicted), TLC of 2.76 (51% of predicted), and DCO of ml/ min/ mm Hg (52% of predicted), supporting a restrictive ventilatory defect with abnormal gas exchange. Medical history was unremarkable. The patient was a nonsmoker with no other chemical exposures. Results of physical examination were normal. A CPET confirmed an aerobic limitation (Vozmax=68% of predicted), normal anaerobic threshold, and a reduced ventilatory reserve (16% [normal >30%]). Pressure-volume curves demonstrated marked reductions in lung compliance at all lung volumes. HRCT was interpreted as normal by two thoracic CT radiology specialists (Fig 1). Transbronchial bronchoscopic lung biopsies were normal. A representative sample from the open lung biopsy is shown in Figure 2. She was placed on a regimen of oral prednisone at 60 mg/ d for 3 months that was subsequently tapered to 10 mg/ d of prednisone. Her pulmonary function and symptoms have stabilized after 6 months of therapy. CASE 2 A 43-year-old white woman presented with a 1-year history of progressive dyspnea. She had been hospitalized 1 year earlier with chest pain and breathlessness at which time myocardial infarction was ruled out. Cardiac catheterization revealed normal coronary arteries, ventricular function, and pulmonary artery pressure. Ventilation perfusion lung 114 scanning was low probability for pulmonary embolism, and lower extremity venous Doppler studies were negative for venous thrombosis. Over the ensuing year, she noted progressive dyspnea limiting her ability to perform moderate degrees of exercise. Medical history was notable for a partial thyroidectomy at age 16 years, a total abdominal hysterectomy and oophorectomy at age 24 years, and a cholecystectomy at age 36 years. She was a nonsmoker without significant occupational exposure. Physical examination revealed well-healed surgical scars. Chest radiograph was normal. PFTs included a FVC of 2.81 L (78% of predicted), FEY 1 of 2.18 L (78% of predicted), TLC of 4.01 L (75% of predicted), and DCO of (57% of predicted) confirming a mild restrictive ventilatory defect. CPET confirmed ventilatory limitation with abnormal widening of the P(A-a)Oz. HRCT was not indicative of interstitial lung disease. Bronchoscopic transbronchial biopsy specimens were normal. Open lung biopsy identified findings suggestive of idiopathic pulmonary fibrosis. Three months treatment with 1 mg/ kg/ d of prednisone resulted in no clinical or physiologic benefit. Subsequent therapy with cyclophosphamide (2 mg/ kg/ d) resulted in stabilization of symptoms and pulmonary function. CASE 3 A 43-year-old black woman with Madan's syndrome was referred with breathlessness for 1 year. She denied fever, chills, night sweats, sputum production, or cough. Medical history was notable for thyroidectomy for hyperthyroidism and pericarditis with surgical drainage of a pericardia! effusion at age 40 years. She was a nonsmoker and had no significant occupational exposure. Physical examination was notable only for marfanoid features. Chest radiograph was normal. PFTs demonstrated a FVC of 3.32 L (78% of predicted), FEY 1 of 2.71 L (82% of predicted), TLC of 5.26 L (82%), and a DCO of ml/ min/ mm Hg (68% of predicted). CPET confirmed aerobic limitation with a Vozmax of 1.16 L (63.7%) and reduced ventilatory reserve (6.1%; normal > 30%). HRCT did not reveal evidence of interstitial lung disease. Bronchoscopy with transbronchial biopsy specimens showed patchy interstitial fibrosis confirmed by trichrome staining. Open lung biopsy specimens identified findings suggestive of idiopathic pulmonary fibrosis. Prednisone (1 mg/ kg/ d) was given for 3 months with stability in physiologic parameters but no significant improvement. A subsequent trial of cyclophosphamide (2 mg/ kg/ d) was discontinued due to severe side effects. She has not been receiving immunosuppressive therapy for 8 months with no evidence of deterioration. Clinical Investigations
7 REFERENCES Martinez FJ, Stanopoulos I, Acero R, et al. Graded comprehensive cardiopulmonary exercise testing in the evaluation of dyspnea unexplained by routine evaluation. Chest 1994; 105: Webb WR. High resolution lung computed tomography: normal anatomic and pathologic findings. Radio! Clin North Am 1991; 29: Tung KT, Wells AU, Rubens MB, et al. Accuracy of the typical computed tomographic appearance of fibrosing alveolitis. Thorax 1993; 48: Panos RJ, King TE Jr. Idiopathic pulmonary fibrosis. In: Lynch JP III, DeRemee R, eds. Immunologically mediated pulmonary disease. Philadelphia: JB Lippincott; 1991: Lynch JP III, Chavis AD. Chronic interstitial lung disorders. In: Victor L, ed. Clinical pulmonary medicine. Boston: Little Brown; 1992: Webb WR. High-resolution computed tomography of the lung: normal and abnormal anatomy. Semin Roentgenol 1991; 26: ll Morris J, Koski A, Johnson L. Spirometric standards for healthy nonsmoking adults. Am Rev Respir Dis 1971; 103: Dubois A, Bothelho S, Bedell G, et al. A rapid plethysmographic method for measuring thoracic gas volume: a comparison with a nitrogen washout method for measuring functional residual capacity in normal subjects. J Clin Invest 1956; 35: Goldman H, Becklake M. Respiratory function tests: normal values at median altitudes and the prediction of normal results. Am Rev Tuberc 1959; 79: Ogilvie C, Forster R, Blakemore W, et al. A standard breathholding technique for the clinical measurement of the diffusing capacity of the lung for carbon monoxide. J Clin Invest 1957; 36: Crapo R, Morris A. Standardized single breath normal values for carbon monoxide diffusing capacity. Am Rev Respir Dis 1981; 123: Jones NL, Makrides L, Hitchcock C, et al. Normal standards for an incremental progressive cycle ergometer test. Am Rev Respir Dis 1985; 131: Watters LC, King TE, Schwarz Ml, et al. A clinical, radiographic and physiologic scoring system for the longitudinal assessment of patients with idiopathic pulmonary fibrosis. Am Rev Respir Dis 1986; 133: Cherniack RM, Colby TV, Flint A, et al. Quantitative assessment of lung pathology in idiopathic pulmonary fibrosis. Am Rev Respir Dis 1991; 144: Epler GR, McCloud TC, Gaensler EA, et al. Normal chest roentgenograms in chronic diffuse infiltrative lung disease. N Eng! J Med 1978; 298: Mathieson JR, Mayo JR, Staples CA, et al. Chronic diffuse infiltrative lung disease: comparison of diagnostic accuracy of CT and chest radiography. Radiology 1989; l7l:ll Padley SPG, Hansell DM, Flower CDR, et al. Comparative accuracy of high resolution computed tomography and chest radiography in the diagnosis of chronic diffuse infiltrative lung disease. Clin Radiol1991; 44: Sanders C, Nath PH, Bailey WC. Detection of emphysema with computed tomography: correlation with pulmonary function tests and chest radiography. Invest Radiol1988; 23: Veda! S, Welsh EV, Miller RR, et al. Desquamative interstitial pneumonia: computed tomographic findings before and after treatment with corticosteroids. Chest 1988; 93: Akira M, Sakatani M, Veda E. Idiopathic pulmonary fibrosis: progression of honeycombing at thin-section CT. Radiology 1993; 189: Wright PE, Sheller JR. What is the meaning of an isolated reduction in single breath diffusing capacity for carbon monoxide? Respir Care 1988; 33: Carrington C, Gaensler E, Coutu R, et al. Natural history and treated course of usual and desquamative interstitial pneumonia. N Eng] J Med 1978; 298: Lee JS, lm J, Ahn JM, et al. Fibrosing alveolitis: prognostic implications of ground glass attenuation at high-resolution CT. Radiology 1992; 184: Wells AU, Rubens MB, dubois RM, et al. Serial CT in fibrosing alveoli tis: prognostic significance of the initial pattern. AJR 1993; 16l:ll59-65 CHEST/108/1 /JULY,
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT in Diffuse Interstitial Lung Disease Steps in High Resolution CT Diagnosis. Where are the lymphatics? Anatomic distribution
 Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Serial computed tomographic evaluation in desquamative interstitial pneumonia
 Thorax 1997;52:333 337 333 Serial computed tomographic evaluation in desquamative interstitial pneumonia Masanori Akira, Satoru Yamamoto, Hideki Hara, Mitsunori Sakatani, Einosuke Ueda Abstract a better
Thorax 1997;52:333 337 333 Serial computed tomographic evaluation in desquamative interstitial pneumonia Masanori Akira, Satoru Yamamoto, Hideki Hara, Mitsunori Sakatani, Einosuke Ueda Abstract a better
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
ARTICLE IN PRESS. Ahuva Grubstein a, Daniele Bendayan b, Ithak Schactman c, Maya Cohen a, David Shitrit b, Mordechai R. Kramer b,
 Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
The crazy-paving pattern: A radiological-pathological correlated and illustrated overview
 The crazy-paving pattern: A radiological-pathological correlated and illustrated overview Poster No.: C-0827 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: W. F. M. De Wever, J. Coolen,
The crazy-paving pattern: A radiological-pathological correlated and illustrated overview Poster No.: C-0827 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: W. F. M. De Wever, J. Coolen,
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis
 Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Part I Study Questions
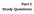 Part I Study Questions 1. A 59-year-old man with a history of pulmonary embolism diagnosed 2 years ago and treated with warfarin for 6 months is evaluated for progressive dyspnea and bilateral lower extremity
Part I Study Questions 1. A 59-year-old man with a history of pulmonary embolism diagnosed 2 years ago and treated with warfarin for 6 months is evaluated for progressive dyspnea and bilateral lower extremity
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after smoking cessation
 Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
Cryptogenic Organizing Pneumonia: Serial High-Resolution CT Findings in 22 Patients
 Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients
 Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation
 Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Nitrofurantoin-Induced Lung Toxicity
 Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review.
 Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Ventilatory Mechanics in Patients with Cardio-Pulmonary Diseases. Part III. On Pulmonary Fibrosis
 Ventilatory Mechanics in Patients with Cardio-Pulmonary Diseases Part III. On Pulmonary Fibrosis Kazuaki SERA, M.D. Pulmonary function studies have been undertaken on the pulmonary fibrosis as diagnosed
Ventilatory Mechanics in Patients with Cardio-Pulmonary Diseases Part III. On Pulmonary Fibrosis Kazuaki SERA, M.D. Pulmonary function studies have been undertaken on the pulmonary fibrosis as diagnosed
Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis
 Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Pediatric High-Resolution Chest CT
 Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Case 1: Question. 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule
 HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES
 ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
Restrictive lung diseases
 Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
CASE OF THE MONTH. Lung Disease in Rheumatoid Arthritis
 CASE OF THE MONTH Lung Disease in Rheumatoid Arthritis 61 year old male Maōri Height: 174 cm Weight: 104.6kg BMI: 34.55 Problems 1. Rheumatoid related interstitial lung disease with UIP pattern 2. Secondary
CASE OF THE MONTH Lung Disease in Rheumatoid Arthritis 61 year old male Maōri Height: 174 cm Weight: 104.6kg BMI: 34.55 Problems 1. Rheumatoid related interstitial lung disease with UIP pattern 2. Secondary
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS
 USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
Bronkhorst colloquium Interstitiële longziekten. Katrien Grünberg, klinisch patholoog
 Bronkhorst colloquium 2013-2014 Interstitiële longziekten De pathologie achter de CT Katrien Grünberg, klinisch patholoog K.grunberg@vumc.nl Preparing: introduction and 3 cases The introduction on microscopic
Bronkhorst colloquium 2013-2014 Interstitiële longziekten De pathologie achter de CT Katrien Grünberg, klinisch patholoog K.grunberg@vumc.nl Preparing: introduction and 3 cases The introduction on microscopic
Radiologic Approach to Smoking Related Interstitial Lung Disease
 Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Imaging Small Airways Diseases: Not Just Air trapping. Eric J. Stern MD University of Washington
 Imaging Small Airways Diseases: Not Just Air trapping Eric J. Stern MD University of Washington What we are discussing SAD classification SAD imaging with MDCT emphasis What is a small airway? Airway with
Imaging Small Airways Diseases: Not Just Air trapping Eric J. Stern MD University of Washington What we are discussing SAD classification SAD imaging with MDCT emphasis What is a small airway? Airway with
Manish Powari Regional Training Day 10/12/2014
 Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
Vascular Lung Diseases
 Vascular Lung Diseases SESSION SPECIFIC OBJECTIVES List the major types of vascular lung disease Recognize and describe the pathology of vascular lung disease: Pulmonary embolism, thrombosis, hypertension,
Vascular Lung Diseases SESSION SPECIFIC OBJECTIVES List the major types of vascular lung disease Recognize and describe the pathology of vascular lung disease: Pulmonary embolism, thrombosis, hypertension,
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines
 Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
BUILD-3: A Randomized, Controlled Trial of Bosentan in
 BUILD-3: A Randomized, Controlled Trial of Bosentan in Idiopathic Pulmonary Fibrosis Talmadge E. King, Jr., MD; Kevin K. Brown, MD; Ganesh Raghu, MD; Roland M. du Bois, MD; David Lynch, MD; Fernando Martinez,
BUILD-3: A Randomized, Controlled Trial of Bosentan in Idiopathic Pulmonary Fibrosis Talmadge E. King, Jr., MD; Kevin K. Brown, MD; Ganesh Raghu, MD; Roland M. du Bois, MD; David Lynch, MD; Fernando Martinez,
Atopic Pulmonary Disease: Findings on Thoracic Imaging
 July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
Hypersensitivity Pneumonitis: Spectrum of High-Resolution CT and Pathologic Findings
 CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Clinical significance of respiratory bronchiolitis on open lung biopsy and its relationship to smoking related interstitial lung disease
 Thorax 1999;54:1009 1014 1009 James Moon, Ronald M du Bois, Thomas V Colby, David M Hansell, Andrew G Nicholson Interstitial Lung Disease Unit J Moon R M du Bois Department of Radiology D M Hansell Department
Thorax 1999;54:1009 1014 1009 James Moon, Ronald M du Bois, Thomas V Colby, David M Hansell, Andrew G Nicholson Interstitial Lung Disease Unit J Moon R M du Bois Department of Radiology D M Hansell Department
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
Careful histopathological evaluation has shown the traditionally clinical diagnosis of
 Demystifying Idiopathic Interstitial Pneumonia Harold R. Collard, MD; Talmadge E. King, Jr, MD REVIEW ARTICLE Careful histopathological evaluation has shown the traditionally clinical diagnosis of idiopathic
Demystifying Idiopathic Interstitial Pneumonia Harold R. Collard, MD; Talmadge E. King, Jr, MD REVIEW ARTICLE Careful histopathological evaluation has shown the traditionally clinical diagnosis of idiopathic
pulmonary and critical care pearls
 pulmonary and critical care pearls A 12-Year-Old Girl With Dyspnea and a Normal Chest Radiographic Finding* Kristin B. Highland, MD; and Patrick A. Flume, MD, FCCP (CHEST 2001; 120:1372 1376) A 12-year-old
pulmonary and critical care pearls A 12-Year-Old Girl With Dyspnea and a Normal Chest Radiographic Finding* Kristin B. Highland, MD; and Patrick A. Flume, MD, FCCP (CHEST 2001; 120:1372 1376) A 12-year-old
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
Advances in imaging. N.L. Müller
 Eur Respir J 2001; 18: 867 871 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 SERIES 0THORACIC IMAGING 0 Edited by P.A. Gevenois, A. Bankier
Eur Respir J 2001; 18: 867 871 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 SERIES 0THORACIC IMAGING 0 Edited by P.A. Gevenois, A. Bankier
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings
 Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited
 Insights Imaging (2017) 8:483 489 DOI 10.1007/s13244-017-0565-2 PICTORIAL REVIEW Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited Daniel B. Green 1 & Alan C. Legasto 1 & Ian
Insights Imaging (2017) 8:483 489 DOI 10.1007/s13244-017-0565-2 PICTORIAL REVIEW Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited Daniel B. Green 1 & Alan C. Legasto 1 & Ian
Airways Disease MDT - 6th May 2014
 Airways Disease MDT - 6th May 2014 The inaugural AD-MDT was held on 6/5/14. The AIM of the meeting is to develop the skills and knowledge to be able to run an AD-MDT - the time frame from the start to
Airways Disease MDT - 6th May 2014 The inaugural AD-MDT was held on 6/5/14. The AIM of the meeting is to develop the skills and knowledge to be able to run an AD-MDT - the time frame from the start to
PATTERN OF INTERSTITIAL LUNG DISEASE AS SEEN BY HIGH RESOLUTION COMPUTERISED TOMOGRAPHY
 September 2012 East African Medical Journal 285 East African Medical Journal Vol. 89 No. 9 September 2012 PATTERN OF INTERSTITIAL LUNG DISEASE DETECTED BY HIGH RESOLUTION COMPUTERISED TOMOGRAPHY C. K Onyambu,
September 2012 East African Medical Journal 285 East African Medical Journal Vol. 89 No. 9 September 2012 PATTERN OF INTERSTITIAL LUNG DISEASE DETECTED BY HIGH RESOLUTION COMPUTERISED TOMOGRAPHY C. K Onyambu,
The role of Pulmonary function Testing In Interstitial lung disease in infants. [ ipft in child ]
![The role of Pulmonary function Testing In Interstitial lung disease in infants. [ ipft in child ] The role of Pulmonary function Testing In Interstitial lung disease in infants. [ ipft in child ]](/thumbs/77/74805557.jpg) The role of Pulmonary function Testing In Interstitial lung disease in infants [ ipft in child ] Introduction Managing infants with diffuse lung disease (DLD) suspected to have interstitial lung disease
The role of Pulmonary function Testing In Interstitial lung disease in infants [ ipft in child ] Introduction Managing infants with diffuse lung disease (DLD) suspected to have interstitial lung disease
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Replacement of air with fluid, inflammatory. cells or cellular debris. Parenchymal, Interstitial (Restrictive) and Vascular Diseases.
 Parenchymal, Interstitial (Restrictive) and Vascular Diseases Alain C. Borczuk, M.D. Dept of Pathology Replacement of air with fluid, inflammatory cells Pulmonary Edema Pneumonia Hemorrhage Diffuse alveolar
Parenchymal, Interstitial (Restrictive) and Vascular Diseases Alain C. Borczuk, M.D. Dept of Pathology Replacement of air with fluid, inflammatory cells Pulmonary Edema Pneumonia Hemorrhage Diffuse alveolar
Sarcoidosis Registry Proforma
 Patient Demographics Patient Data Has a patient consent form been completed? 1.1 Title Mr 1.2 1.3 Forename(s) PlainText Surname PlainText 1.4 Gender Male 1.5 1.6 1.7 1.8 1.9 Mrs Ms Miss Dr Other
Patient Demographics Patient Data Has a patient consent form been completed? 1.1 Title Mr 1.2 1.3 Forename(s) PlainText Surname PlainText 1.4 Gender Male 1.5 1.6 1.7 1.8 1.9 Mrs Ms Miss Dr Other
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
The radiological differential diagnosis of the UIP pattern
 5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker. Michael B. Gotway, MD
 August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
Combined Pulmonary Fibrosis and Emphysema - A Case Series
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 1 Ver. III (January. 2017), PP 15-19 www.iosrjournals.org Combined Pulmonary Fibrosis and Emphysema
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 1 Ver. III (January. 2017), PP 15-19 www.iosrjournals.org Combined Pulmonary Fibrosis and Emphysema
A case of a patient with IPF treated with nintedanib. Prof. Kreuter and Prof. Heussel
 A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Evaluating dyspnea: A practical approach -- When to consider cardiopulmonary exercise testing.
 Evaluating dyspnea: A practical approach -- When to consider cardiopulmonary exercise testing. ABSTRACT: Shortness of breath is a common complaint associated with a number of conditions. Although the results
Evaluating dyspnea: A practical approach -- When to consider cardiopulmonary exercise testing. ABSTRACT: Shortness of breath is a common complaint associated with a number of conditions. Although the results
In medicine, the term overlap is very common, to the extent that there is even a
 Case Report Payam Mehrian (MD) 1 Ali Cheraghvandi (MD) 2 Atousa Droudnia (PhD) 3 Firouzeh Talischi (MD) 4 Saeid Fallah Tafti (MD) *5 Shahram Kahkouee (MD) 6 Hamidreza Jamaati (MD) 7 1. Pediatric Respiratory
Case Report Payam Mehrian (MD) 1 Ali Cheraghvandi (MD) 2 Atousa Droudnia (PhD) 3 Firouzeh Talischi (MD) 4 Saeid Fallah Tafti (MD) *5 Shahram Kahkouee (MD) 6 Hamidreza Jamaati (MD) 7 1. Pediatric Respiratory
STUDY OF PULMONARY ARTERIAL HYPERTENSION IN RESPIRATORY DISORDERS
 STUDY OF PULMONARY ARTERIAL HYPERTENSION IN RESPIRATORY DISORDERS *Hegde R.R., Bharambe R.S., Phadtare J.M. and Ramraje N.N. Department of Pulmonary Medicine, Grant Government Medical College, Mumbai-8
STUDY OF PULMONARY ARTERIAL HYPERTENSION IN RESPIRATORY DISORDERS *Hegde R.R., Bharambe R.S., Phadtare J.M. and Ramraje N.N. Department of Pulmonary Medicine, Grant Government Medical College, Mumbai-8
COMPREHENSIVE RESPIROMETRY
 INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Lung-Volume Reduction Surgery ARCHIVED
 Lung-Volume Reduction Surgery ARCHIVED Policy Number: Original Effective Date: MM.06.008 04/15/2005 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST 03/22/2013 Section: Surgery Place(s) of
Lung-Volume Reduction Surgery ARCHIVED Policy Number: Original Effective Date: MM.06.008 04/15/2005 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST 03/22/2013 Section: Surgery Place(s) of
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Utility of Lung Clearance Index (LCI) as a Noninvasive Marker of Deployment Lung Disease. Silpa Krefft, M.D., M.P.H. September 20, 2016
 Utility of Lung Clearance Index (LCI) as a Noninvasive Marker of Deployment Lung Disease Silpa Krefft, M.D., M.P.H. September 20, 2016 Disclosures Mountain and Plains Education and Research Center: Pilot
Utility of Lung Clearance Index (LCI) as a Noninvasive Marker of Deployment Lung Disease Silpa Krefft, M.D., M.P.H. September 20, 2016 Disclosures Mountain and Plains Education and Research Center: Pilot
Radiologic findings of drug-induced lung disease
 Radiologic findings of drug-induced lung disease Poster No.: P-0115 Congress: ESTI 2015 Type: Educational Poster Authors: A. I. C. Santos, A. F. Roque, R. Mamede, L. Oliveira, T. Saldanha; Lisbon/PT Keywords:
Radiologic findings of drug-induced lung disease Poster No.: P-0115 Congress: ESTI 2015 Type: Educational Poster Authors: A. I. C. Santos, A. F. Roque, R. Mamede, L. Oliveira, T. Saldanha; Lisbon/PT Keywords:
