and the Beginnings of Direct Arrhythmia Surgery Will C. Sealy, M.D.
|
|
|
- Sydney Leonard
- 6 years ago
- Views:
Transcription
1 The Wolff -ParkinsonWhite Syndrome and the Beginnings of Direct Arrhythmia Surgery Will C. Sealy, M.D. ABSTRACT The bundle of Kent, one of the two pathways involved in the reentry tachycardia of the Wolff- Parkinson-White syndrome, was identified and then interrupted fifteen years ago. This marked the beginning of direct arrhythmia surgery. The patient was a 31-year-old man with a right free wall pathway and persistent tachycardia refractory to medical treatment. In the present report, the historical landmarks in the description of the morphology of the conduction system are reviewed. Current methods of interrupting the Kent bundle, based on experience with more than 200 surgical patients, are discussed. Included is the newer method of simplifying the surgical procedure with cryothermia. Speculation about the future of direct arrhythmia surgery is given in the concluding remarks. Fifteen years ago, a 31-year-old fisherman with the Wolff-Parkinson-White (WPW) syndrome went to Duke Hospital to seek help for an almost continuous tachycardia refractory to all medications. Electrophysiological studies pointed to a right free wall Kent bundle as the cause of the reentry tachycardia. It was decided that operative intervention was the only way to correct the problem. The surgical strategy was to try to find the bundle of Kent by epicardial mapping and then divide it. If that failed, the His bundle would be divided. The Kent bundle was found and interrupted [l], and the man was cured. This operation marked the beginning of direct arrhythmia surgery. Some of my thoughts and experiences that evolved directly from this event are related here. In an article by Wiggers [2], I found a quotation from Barthold G. Nieburh: He who calls departed ages back again in being, /Enjoys a bliss like that of creating. This is a pleasant reason for reading history. It is much better than the one most frequently used that threatens dreadful consequences if we do not learn how to avoid them by studying history. I now will review some of the events that led to our understanding of the conduction system. Historical Background Walter Holbrook Gaskell [3] of Cambridge, England, is credited with proving in the early 1880s that conduction *Professor Emeritus of Thoracic Surgety, Duke University School of Medicine, Durham, NC. From 202 Selkirk Dr, Durham, NC Accepted for publication Feb 20, 1984 of impulses from the atrium to the ventricle was by myocardium and not by nerves. Gaskell s experiments were done on the turtle s heart and could be called experimental surgical studies. In one such study, the atrioventricular (AV) junction was divided in stages with pacing of the atrium at each stage. As the connecting myocardial strand became thinner from staged division, the paced atrial beats were conducted to the ventricle in a ratio of 2 to 1 at first and then 3 to 1. Does this not suggest the possible application of this observation to the AV node and bundle in enhanced AV node conduction? Gaskell was the pupil and later colleague of the founder of the Cambridge school of physiology, Robert Foster [4]. Wilhelm His, Jr. [5], son of one of the great anatomists and embryologists of all time, is eponymously credited with showing that in mammals, AV conduction is by a small myocardial band. Appropriately, the discovery came from the younger His s observations of the chick embryo, observations proving that AV conduction takes place well before cardiac innervation develops. Later, with a series of what I know from experience to be frustrating experiments, His produced heart block in one rabbit after twenty-three tries. A few months ahead of His, Stanley Kent [6], who provided the eponym for the Kent bundle, found that AV conduction was myogenic in mammals. He believed that the normal connections were multiple, which we now know is incorrect. However, in patients with the WPW syndrome, anomalous pathways of AV conduction have been found on the right lateral wall, as Kent [7] noted. His incorrect observations did point the way to the discovery of the anomalous pathways; perhaps he deserves the eponym. On the other hand, in the story of the anatomy of the conduction system, there are examples of unused but deserved eponyms. The AV node is rarely called Tawara s node. During his five years in Aschoff s laboratory in Germany, this Japanese pathologist described the AV node and detailed the ventricular conduction system [8]. Tawara, in the idiom of today, put it all together. The sinoatrial node was the last structure in the conduction system to be found. It seldom is called the node of Keith and Flack [9], the names of its discoverers. Arthur Keith was a distinguished English anatomist of the first half of the twentieth century. Martin Flack, who later became a fine cardiologist, was a medical student and country neighbor of Keith. This brief discussion has not included contemporary anatomists, such as the late Raymond Truex, Maurice Lev, Robert Anderson, Anton Becker, Wallace McA1- pine, and Thomas James. These men identified the 176
2 177 Sealy: WPW Syndrome and Direct Arrhythmia Surgery guideposts that have made direct arrhythmia surgery possible. The physiologists and cardiologists who made great contributions to the field of arrhythmia surgery are too numerous to include here. Four, however, must be mentioned: Dr. Willem Einthoven, Sir Thomas Lewis, Dr. Frank Wilson, and Dr. Dirk Durrer. Dr. Einthoven s application of the string galvanometer for recording the heart s electrical activity on the body surface marked the beginning of clinical cardiac electrophysiology [ 101. Sir Thomas Lewis ranks next to Einthoven for both his experimental and clinical contributions [ll]. Dr. Frank Wilson of Ann Arbor was the person most responsible for the wide clinical application of electrocardiography. Dr. Wilson and his colleagues [12], including Dr. John Alexander, did an early map, published in 1928, of the epicardial activation sequences of the ventricle in human beings. The last person, Dr. Dirk Durrer of Amsterdam, is the father of modern clinical electrophysiology [13]. It was his teaching that guided us in our efforts to cure the fisherman with the fast pulse. In the second decade of this century, Dr. Paul Dudley White, a great clinical cardiologist and teacher of cardiologists, collected a series of unusual electrocardiograms. These tracings were from young patients whose condition was normal except for paroxysmal tachycardia and preexcitation of the ventricles. On a trip to England, he found that Dr. Parkinson, an English physician, had a group of similar patients. Dr. Wolff, a fellow of Dr. White s, combined their data and reported their observations [14]. No one could explain the peculiar ECGs in these patients until Drs. Wolferth and Wood [15] published their observations on a young man with paroxysmal tachycardia and electrocardiographic changes similar to those noted by Dr. White. Dr. Wood and his colleagues came to the conclusion that the abnormalities were due to conduction from the atrium to the ventricle by a pathway other than the AV node-his bundle. The patient died. Having based their hypothesis on what Kent thought was normal AV conduction in human beings on the right free wall, Dr. Wood and colleagues [16] directed their anatomical studies to the right lateral free wall and thus found the anomalous pathway. Had Kent not published what are now considered to Se incorrect observations, Wood and colleagues might never have found the right free wall pathway. Had the fisherman s anomalous pathway been anyplace other than the right free wall, I would not likely have found it at operation. Clinical Considerations The Pathways The anomalous pathways are congenital, and thud WPW syndrome is a congenital heart disease. The path& is almost always just a strand or two of working myocardium. This strand, 1 to 2 mm in diameter, is the remnant of the sheet of myocardium that, in the embryo, once connected the atrium and ventricle as a broad sheet. The pathways can be multiple. Because of this mode of development, it is not surprising that pathways can be found anywhere on the right or left annulus fibrosus except where the left atrium is attached to the aortic annulus. There is still a scarcity of information on the morphology of the Kent bundle, not only because it is an uncommon anomaly but because the job of finding a strand a millimeter in diameter in the coronary sulcus fat is formidable. As my experience increased, I assumed that the pathways could be anywhere on the annulus fibrosus and based this assumption on embryology, the 18 reported examples I could find in the literature, and my surgical experience to that time. Subsequent clinical observations confirmed the assumption. I classified the pathways into right and left free wall, posterior septal, and anterior septal. Peculiar to each type of pathway are surgical problems as well as characteristic ECGs. The most common arrhythmia caused by a Kent bundle is a reentry arrhythmia involving the Kent and His bundles and creating a narrow QRS tachycardia. A less common arrhythmia, usually occurring in combination with reentry tachycardia, is a malignant ventricular arrhythmia. It is found in about 25% of patients referred for operation. The malignant arrhythmia is due to a Kent bundle with a short effective refractory period that permits 1:l conduction of the impulses of an atrial tachycardia to the ventricle. The reentry tachycardia is usually triggered by an extra beat, most frequently in the atrium, which finds the Kent pathway nonexcitable because of its long effective refractory period. This is the functional status of 75% of my surgical patients. During the time it takes for the impulse to pass through the AV node and His bundle, the Kent bundle becomes excitable. The impulse then reenters the atrium and initiates the circusmovement tachycardia. Rarely, the atrial reentry is by the His bundle and AV node, and thus ventricular entry is over the Kent bundle. This type produces a wide QRS tachycardia. However, such a tachycardia frequently points to the presence of a second Kent bundle, the two bundles composing the circuit. The characteristics of the pathways may differ. Some conduct only retrograde but can be associated with a reentry tachycardia that can be difficult to control. Others have only antegrade function and can cause a malignant arrhythmia but seldom are associated with a reentry tachycardia. Some behave as if composed of AV nodal tissue. Considerations before Operation The first manifestation of WPW syndrome may be in infancy. Babies with anomalous pathways may be troubled with recurrent tachycardias. Although most such arrhythmias can be controlled with digitalis, the drug can have a lethal effect on adults with WPW syndrome. Some children in the series had had incessant junctional reentry tachycardia from infancy and required operation. It is not unusual for patients to have their first
3 178 The Annals of Thoracic Surgery Vol38 No 2 August 1984 symptoms when they are 40 to 60 years old. Perhaps this is because extra beats tend to be more common at that age. The additive effect of the tachycardia on other cardiac problems, such as Ebstein s anomaly, cardiomyopathy, and valvular and coronary artery disease, make the episodes of tachycardia more frequent and less tolerable, and may make interruption of the pathway necessary. Without a doubt, the patient whose pathway has the potential to cause a malignant ventricular arrhythmia is a candidate for operation. This group of patients is selected by two methods: a history of episodes of malignant ventricular tachycardia and the finding at electrophysiological study that on induced atrial fibrillation, a rapid ventricular rate ensues. It is difficult to distinguish the young person at the right time. Sometimes the malignant arrhythmia is the first symptom of the disorder. In my opinion, any young patient known to have preexcitation on an ECG should at least undergo induced atrial fibrillation through an esophageal electrode to determine whether a malignant ventricular arrhythmia is likely to develop. Another factor that helps distinguish those patients who are candidates for operation is age. A young person who requires daily medication should undergo an operation. A lifetime of medication is too great a burden and too great a potential risk to impose on a young patient. An older patient in whom the tachycardia cannot be controlled also should have an operation. The selection process includes a careful preoperative physiological study. Sometimes a short PR interval is caused by an AV connection bypassing the AV node; or, preexcitation from a His bundle can cause a connection to go directly to the ventricle and bypass the bundle branches. Occasionally, it is discovered that the tachycardia is not caused by the Kent bundle at all, even though preexcitation is present. When done carefully, such a study can identify multiple pathways in almost every instance; they were found in nearly 20% of my patients. Electrophysiological studies in patients with reentry supraventricular arrhythmias but no preexcitation may detect an unsuspected Kent bundle with only retrograde function. The incidence of this was about 15% in the series. In fact, 30 to 40% of reentry supraventricular tachycardias are due to Kent bundles that can conduct only retrograde. A careful cardiac evaluation of patients with WPW syndrome is needed to exclude other heart problems. Three of the patients in the series who died had an unrecognized cardiomyopathy, severe idiopathic hypertrophic subvalvular aortic stenosis. Ebstein s deformity was present in about 15% of the 200 patients in my series. Division of the Kent bundle should be done with a guide to identify it at operation, for the bundle is neither visible nor palpable. This is accomplished by a procedure called mapping, an electrophysiological study performed in the operating room. It should be noted, however, that in more than 90% of patients, the preoperative study localizes the pathway well enough to act as a guide in case the pathway is obtunded by manipulation at operation. Surgical Technique In planning the surgical strategy, observations during operation are of help in defining the surgical anatomy, even though the Kent bundle is not visible. In left free wall pathways, for example, such observations led to the following conclusions. I decided that pathways in the free wall were external to the annulus fibrosus. Their course could be close to the annulus or out in the coronary sulcus fat at varying distances from the annulus fibrosus to points just beneath the epicardium. Since the coronary sinus has atrial muscle in its wall, this structure could be the atrial origin of a pathway. A drawing of the interruption of a left free wall pathway demonstrates how these suppositions were put into practice (Figure). The His bundle and AV node must always be considered in planning and performing the operation for tachycardia due to a Kent bundle. The His bundle is one of the two arms of the reentry circuit, and its division will cure the tachycardia. However, if the reason for operation is to repair a potentially malignant arrhythmia, then interruption of only the Kent bundle will suffice. His bundles and Kent bundles can be close together. In posterior pathways, both may have to be interrupted owing to the inability to separate them. On the other hand, an anterior septal Kent bundle and the His bundle have been judged by mapping to be within 2 to 3 mm of each other. By careful placement of the incision, the Kent bundle alone can be interrupted and the His bundle spared. Also, the His bundle is well protected by the membranous ventricular septum. The relationship of the Kent bundle to the His bundle and the multiple courses the Kent bundle can follow in the posterior septal area are complex. Mapping is difficult because of the relationship of the Kent bundles to the two atria, the coronary sinus, the ventricular and atrial septa, and the right fibrous trigone, which is composed, in part, of the membranous ventricular septum. The His bundle penetrates the right fibrous trigone. To give some perspective on the boundaries of this area, I have likened it to a three-sided pyramid toppled on its side. The right fibrous trigone is its apex; the epicardium of the crux and a part of the coronary sinus make up the base; and the right atrium, the left atrium, and the combination of the septum and the posterior process of the left ventricle constitute the three sides. This arrangement prevents accurate epicardial mapping because the right atrium overlaps the left ventricle. Two other structural arrangements make mapping difficult: the superior position of the left annulus fibrosus over the right and the obliquity of the atrial septum from its insertion in the right fibrous trigone to the crux. These relationships have led me to believe that a patient whose surface map shows earliest activation of the ventricle just to the left of the crux or over the interventricular groove should have an extensive dissection not
4 179 Sealy: WPW Syndrome and Direct Arrhythmia Surgery / The approach to a left free wall pathway. (Upper left) A left atriotomy similar to that used for a mitral valve replacement is done. The suture marks the site of the connection of the pathway to the atrium, as determined by mapping at operation. A long incision including a2- most all of the free wall is made. (A) The fat in the coronary sulcus is separated from the atrium and ventricle. (B) Extent of the dissection. (C) The vey superficial fibers of the ventricle are separated from the external surface of the annulus. These steps take care of all possible routes the Kent bundle may take from the atrium to the ventricle. only of the pyramidal septal space but a right and left atriotomy as well. The latter can be avoided in some patients by substituting cryothermic ablation. When the early ventricular activation site is found to the right of the crux, then only a right atriotomy and posterior septal dissection are needed. Last, the His and Kent bundles may be adjacent to each other. Problems with interruption have occurred more frequently with pathways here in the posterior septal area than anywhere else. The possibility of interrupting the Kent bundle without an atriotomy and even without cardiopulmonary bypass has now been realized by my approach recently to three right free wall pathways and by the external approach of Guiraudon* to left free wall pathways. The cryoprobe is used for this purpose. Guiradon G: Personal communication, At operation to control the reentry tachycardia in WPW syndrome, the surgeon has the option to interrupt conduction over the His bundle. Early in my experience, I used this method occasionally because I was not able to find the Kent bundle. Recently, I have elected to interrupt the His bundle only in patients with associated severe cardiomyopathies in whom the Kent bundle was on the left side or in the posterior septal area. The results of operation involving the arrhythmia associated with WPW are excellent. In my experience with more than 200 patients, only patients with serious associated diseases, including idiopathic hypertrophic subvalvular aortic stenosis, Ebstein s anomaly, and ischemic heart disease, have died. With our current knowledge, success in identifying the pathway and then interrupting it should be nearly 100%. Are there methods that promise to reduce the complexity of the procedure? A cardiac catheter electrode attached to a direct-current defibrillator and introduced through the venous system can now be used to interrupt the His bundle [17,18]. When control of the extent of the burn caused by this method can be obtained so as to avoid injury to the coronary arteries, then the technique might be more widely used in the ablation of Kent bundles. Closing Remarks In closing, I will raise some points about the future of direct arrhythmia surgery. The surgical approaches to
5 180 The Annals of Thoracic Surgery Vol38 No 2 August 1984 reentry ventricular tachycardia are now well established. Direct operation on the AV node is possible. This node is relatively large, and conduction through it is slow. By means that are not known, the node filters excessive numbers of impulses from the atrium, thereby protecting the ventricle from a fast, intolerable rate. Sometimes these two peculiar mechanisms malfunction. Would a graded division of the AV node or nodal approaches increase this capacity of the node for filtering the excess impulses resulting from a tachycardia? The AV node is sometimes found to be divided into two physiologically different pathways. In 1 patient with AV nodal tachycardia, partial division of the AV node served to interrupt a reentry circuit using these two physiologically distinct conduction pathways, and thus cured the tachycardia [19]. In disorders that arise because the sinoatrial node fails in its function as the heart s pacemaker, would elimination of this node allow a lower atrial pacemaker to become dominant? If so, would it be reliable? Animal studies have shown that the pacemaker is in the region of the coronary sinus. More experimental studies are required, for it appears that a large volume of atrium needs to be in continuity with the substitute pacemaker for the pacemaker to assume dominance [20]. This may explain the problems with pacemakers after extensive atrial operations when the sinoatrial node is preserved but the surrounding right atrium is partially destroyed or excluded. The fisherman with the fast pulse started me on an interesting trip. There are many miles left to travel. I am thankful to have been in at the start. References 1. Sealy WC, Hattler BG Jr, Blumenschein SD, Cobb FR Surgical treatment of Wolff-Parkinson-White syndrome. Ann Thorac Surg 8:1, Wiggers CJ: Some significant advances in cardiac physiology during the nineteenth century. Bull Hist Med 34:1, Gaskell WH: On the innervation of the heart, with especial reference to the heart of the tortoise. J Physiol 4:43, Geison GL: Michael Foster and the Cambridge School of Physiology. Princeton, NJ, Princeton University Press, His W Jr: Activity of the embryonic human heart and the significance for the understanding of the heart movement in the adult. J Hist Med Allied Sci 4:289, Kent AFS: Researches on the structure and function of the mammalian heart. J Physiol 14233, Kent AFS: A conduction path between the right auricle and the external wall of the right ventricle in the heart of the mammal. J Physiol 4857, Aschoff KAL: A discussion on some aspects of heart-block. Br Med J 2:1103, Keith A, Flack MW The auriculo-ventricular bundle of the human heart. Lancet 2:359, Shapiro E: Willem Einthoven s fortuitous invention. Am J Cardiol40:987, Callahan JA, Keys JD, Keys TA: Sir Thomas Lewis. Mayo Clin Proc 56749, Barker PS, MacLeod AG, Wilson FN, Alexander J: The excitatory process observed in the exposed human heart. Am Heart J 5:720, Durrer D, Roos JP: Epicardial excitation of the ventricles in a patient with Wolff-Parkinson-White syndrome (type 9): temporary ablation at surgery. Circulation 3535, Wolff L, Parkinson J, White PD Bundle branch block with short P-R interval in healthy young people prone to paroxysmal tachycardia. Am Heart J 5:685, Wolferth CC, Wood FC: The mechanism of production of short P-R intervals and prolonged QRS complexes in patients with presumably undamaged hearts: hypothesis of an accessory pathway of auriculo-ventricular conduction (bundle of Kent). Am Heart J 8:297, Wood FC, Wolferth CC, Geckeler GD: Histologic demonstration of accessory muscular connections between auricle and ventricle in a case of short P-R interval and prolonged QRS complex. Am Heart J 25:454, Gonzalez R, Scheinman M, Margotten W, Rubinstein M: Closed chest electro-catheter technique for His bundle ablation in dogs. Am J Physiol 241:283, Gallagher JJ, Svenson RH, Kasell J, et al: Catheter technique for closed chest ablation of atrioventricular conduction system. New Engl J Med 306:194, Pritchett EL, Anderson RW, Benditt DG, et al: Re-entry within the atrioventricular node: surgical cure with preservation of atrioventricular conduction. Circulation 60:440, Sealy WC, Seaber AV: Cardiac rhythm following exclusion of the sinoatrial node and most of the right atrium from the remainder of the heart. J Thorac Cardiovasc Surg 77:436, 1979
Anatomical Problems with Identification and Interruption of Posterior Septa1 Kent Bundles
 Anatomical Problems with Identification and Interruption of Posterior Septa1 Kent Bundles Will C. Sealy, M.D., and Eileen M. Mikat, Ph.D. ABSTRACT To gain insight into the cause of the complex anatomical
Anatomical Problems with Identification and Interruption of Posterior Septa1 Kent Bundles Will C. Sealy, M.D., and Eileen M. Mikat, Ph.D. ABSTRACT To gain insight into the cause of the complex anatomical
It appears too early for definitive assessment. of the long-term effectiveness of these various approaches, and further investigation
 arrhythmias were not associated with coronary artery disease. The pathophysiological concepts elaborated from this clinical setting were later extended to ventricular tachycardia that complicated myocardial
arrhythmias were not associated with coronary artery disease. The pathophysiological concepts elaborated from this clinical setting were later extended to ventricular tachycardia that complicated myocardial
Kent Bundles in the Anterior Septal Space Will C. Sealy, M.D.
 Kent Bundles in the Anterior Septal Space Will C. Sealy, M.D. ABSTRACT Kent bundles in the anterior septal area of the heart occupy a region of complex morphology. In this study, the anatomical characteristics
Kent Bundles in the Anterior Septal Space Will C. Sealy, M.D. ABSTRACT Kent bundles in the anterior septal area of the heart occupy a region of complex morphology. In this study, the anatomical characteristics
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Circulation: Arrhythmia and Electrophysiology CHALLENGE OF THE WEEK
 A 14-year-old girl with Wolff-Parkinson-White syndrome and recurrent paroxysmal palpitations due to atrioventricular reentry tachycardia had undergone two prior failed left lateral accessory pathway ablations
A 14-year-old girl with Wolff-Parkinson-White syndrome and recurrent paroxysmal palpitations due to atrioventricular reentry tachycardia had undergone two prior failed left lateral accessory pathway ablations
Wolff-Parkinson-White Syndrome
 Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師
 Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
'Dual atrioventricular nodal pathways' in patients with Wolff-Parkinson-White syndrome*
 Br Heart 7 1980; 43: 7-13 'Dual atrioventricular nodal pathways' in patients with Wolff-Parkinson-White syndrome* EDWARD L C PRITCHETT, ERIC N PRYSTOWSKY, DAVID G BENDITT, JOHN J GALLAGHER From the Division
Br Heart 7 1980; 43: 7-13 'Dual atrioventricular nodal pathways' in patients with Wolff-Parkinson-White syndrome* EDWARD L C PRITCHETT, ERIC N PRYSTOWSKY, DAVID G BENDITT, JOHN J GALLAGHER From the Division
Electrophysiology and Cathether Ablation: Historical Evolution. Saverio Iacopino, MD, FACC, FESC
 Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B. Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D.
 Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Ventricular Anatomy for the Electrophysiologist (Part I)
 SPECIAL REVIEW Ventricular Anatomy for the Electrophysiologist (Part I) ABSTRACT Anatomy of the conduction system for electrophysiologists is reviewed in two parts. This first part details the historical
SPECIAL REVIEW Ventricular Anatomy for the Electrophysiologist (Part I) ABSTRACT Anatomy of the conduction system for electrophysiologists is reviewed in two parts. This first part details the historical
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Declaration of conflict of interest NONE
 Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
FURTHER STUDIES OF THE CONDUCTING SYSTEM OF THE BIRD'S HEART
 FURTHER STUDIES OF THE CONDUCTING SYSTEM OF THE BIRD'S HEART By FRANCIS DAVIES, M.D. (LONDON) Anatomy Department, University College, London INTRODUCTION T1HE histological investigation of the conducting
FURTHER STUDIES OF THE CONDUCTING SYSTEM OF THE BIRD'S HEART By FRANCIS DAVIES, M.D. (LONDON) Anatomy Department, University College, London INTRODUCTION T1HE histological investigation of the conducting
The radial procedure was developed as an outgrowth
 The Radial Procedure for Atrial Fibrillation Takashi Nitta, MD The radial procedure was developed as an outgrowth of an alternative to the maze procedure. The atrial incisions are designed to radiate from
The Radial Procedure for Atrial Fibrillation Takashi Nitta, MD The radial procedure was developed as an outgrowth of an alternative to the maze procedure. The atrial incisions are designed to radiate from
Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing
 Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
2. right heart = pulmonary pump takes blood to lungs to pick up oxygen and get rid of carbon dioxide
 A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
ARTICLE. Supraventricular Tachycardia in Infancy. Catherine D. DeAngelis, MD. In most infants, SVT is due to an accessory atrioventricular
 Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
human anatomy 2016 lecture thirteen Dr meethak ali ahmed neurosurgeon
 Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Human Anatomy and Physiology II Laboratory Cardiovascular Physiology
 Human Anatomy and Physiology II Laboratory Cardiovascular Physiology 1 This lab involves two exercises: 1) Conduction System of the Heart and Electrocardiography and 2) Human Cardiovascular Physiology:
Human Anatomy and Physiology II Laboratory Cardiovascular Physiology 1 This lab involves two exercises: 1) Conduction System of the Heart and Electrocardiography and 2) Human Cardiovascular Physiology:
ORIGINAL ARTICLE. ANATOMICAL VARIATIONS OF NODAL ARTERIES IN HUMAN HEARTS. Anjali S Sabnis, Nazmeen N Silotry
 ANATOMICAL VARIATIONS OF NODAL ARTERIES IN HUMAN HEARTS. Anjali S Sabnis, Nazmeen N Silotry 1. Associate Professor, Department of Anatomy, K. J. Somaiya Medical College, Sion, Mumbai, 2. Associate Professor,
ANATOMICAL VARIATIONS OF NODAL ARTERIES IN HUMAN HEARTS. Anjali S Sabnis, Nazmeen N Silotry 1. Associate Professor, Department of Anatomy, K. J. Somaiya Medical College, Sion, Mumbai, 2. Associate Professor,
CAn Official Journalofthe cflmerican Heart cassociation, Inc.
 C*i r i *VOL 71 MARCH CAn Official Journalofthe cflmerican Heart cassociation, Inc. FEATURES NO 3 1985 The status of surgery for cardiac arrhythmias JAMES L. Cox, M.D. Downloaded from http://ahajournals.org
C*i r i *VOL 71 MARCH CAn Official Journalofthe cflmerican Heart cassociation, Inc. FEATURES NO 3 1985 The status of surgery for cardiac arrhythmias JAMES L. Cox, M.D. Downloaded from http://ahajournals.org
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow
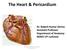 The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
Junctional Tissues of Human Heart
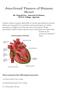 1 Junctional Tissues of Human Heart Mr. Rupajit Das, Associate Professor, M.B.B. College, Agartala Cardiac muscle consists essentially of certain specialised structures which are responsible for initiation
1 Junctional Tissues of Human Heart Mr. Rupajit Das, Associate Professor, M.B.B. College, Agartala Cardiac muscle consists essentially of certain specialised structures which are responsible for initiation
Advances in Ablation Therapy for Ventricular Tachycardia
 Advances in Ablation Therapy for Ventricular Tachycardia Nitish Badhwar, MD, FACC, FHRS Director, Cardiac Electrophysiology Training Program University of California, San Francisco For those of you who
Advances in Ablation Therapy for Ventricular Tachycardia Nitish Badhwar, MD, FACC, FHRS Director, Cardiac Electrophysiology Training Program University of California, San Francisco For those of you who
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
VENTRICULAR TACHYCARDIA IN THE ABSENCE OF STRUCTURAL HEART DISEASE
 VENTRICULAR TACHYCARDIA IN THE ABSENCE OF STRUCTURAL HEART DISEASE Dimosthenis Avramidis, MD. Consultant Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital
VENTRICULAR TACHYCARDIA IN THE ABSENCE OF STRUCTURAL HEART DISEASE Dimosthenis Avramidis, MD. Consultant Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page 5062-5066 Comparison of the Accuracy of Three Algorithms in Predicting Accessory Pathways among Adult Wolff-Parkinson-White (WPW)
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page 5062-5066 Comparison of the Accuracy of Three Algorithms in Predicting Accessory Pathways among Adult Wolff-Parkinson-White (WPW)
WPW Syndrome Complicated by Another Cardiac Disorder
 Hiroshima J. Med. Sci. Vol.40, No.1, 4 7-51, March, 1991 HIJM 40-8 47 WPW Syndrome Complicated by Another Cardiac Disorder Taijiro SUEDA, Yuichiro MATSUURA, Hiroshi ISHIHARA, Yoshiharu HAMANAKA, Hiroo
Hiroshima J. Med. Sci. Vol.40, No.1, 4 7-51, March, 1991 HIJM 40-8 47 WPW Syndrome Complicated by Another Cardiac Disorder Taijiro SUEDA, Yuichiro MATSUURA, Hiroshi ISHIHARA, Yoshiharu HAMANAKA, Hiroo
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
Dr David Begley Papworth Hospital, Cambridge HRUK Certificate of Accreditation Course: Core Heart Rhythm Congress 2011
 Dr David Begley Papworth Hospital, Cambridge HRUK Certificate of Accreditation Course: Core Heart Rhythm Congress 2011 The AV node is the soul of the heart, and whoever understands its anatomy and electrophysiology
Dr David Begley Papworth Hospital, Cambridge HRUK Certificate of Accreditation Course: Core Heart Rhythm Congress 2011 The AV node is the soul of the heart, and whoever understands its anatomy and electrophysiology
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
The Heart. The Heart A muscular double pump. The Pulmonary and Systemic Circuits
 C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
and fibrillation in pre-excitation (Wolff-Parkinson-
 British Heart Journal, 973, 35, 8ii-8i6. Factors regulating ventricular rates during atrial flutter and fibrillation in pre-excitation (Wolff-Parkinson- White) syndrome Agustin Castellanos, Jr., Robert
British Heart Journal, 973, 35, 8ii-8i6. Factors regulating ventricular rates during atrial flutter and fibrillation in pre-excitation (Wolff-Parkinson- White) syndrome Agustin Castellanos, Jr., Robert
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Circulation. Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body
 Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
THE HEART. A. The Pericardium - a double sac of serous membrane surrounding the heart
 THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Atrial fibrillation (AF) is associated with increased morbidity
 Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
This presentation will deal with the basics of ECG description as well as the physiological basics of
 Snímka 1 Electrocardiography basics This presentation will deal with the basics of ECG description as well as the physiological basics of Snímka 2 Lecture overview 1. Cardiac conduction system functional
Snímka 1 Electrocardiography basics This presentation will deal with the basics of ECG description as well as the physiological basics of Snímka 2 Lecture overview 1. Cardiac conduction system functional
Ch 19: Cardiovascular System - The Heart -
 Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Electrophysiological recognition of an atrio-ventricular mahaim fibre pathway
 Interventional Cardiology Electrophysiological recognition of an atrio-ventricular mahaim fibre pathway Mahaim fibres are cardiac accessory bundles which can cause dangerous tachyarrhythmias. Despite their
Interventional Cardiology Electrophysiological recognition of an atrio-ventricular mahaim fibre pathway Mahaim fibres are cardiac accessory bundles which can cause dangerous tachyarrhythmias. Despite their
the Cardiovascular System I
 the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia
 www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
AV Node Dependent SVT:Substrates, Mechanisms, and Recognition
 AV Node Dependent SVT:Substrates, Mechanisms, and Recognition Ching-Tai Tai Taipei Veterans General Hospital National Yang-Ming University AV Node Reentry Anatomy Physiology Anatomic-Physiologic Relation
AV Node Dependent SVT:Substrates, Mechanisms, and Recognition Ching-Tai Tai Taipei Veterans General Hospital National Yang-Ming University AV Node Reentry Anatomy Physiology Anatomic-Physiologic Relation
Fast Facts: Cardiac Arrhythmias
 Fast Facts Fast Facts: Cardiac Arrhythmias Gerry Kaye, Steve Furniss and Robert Lemery Fast Facts Fast Facts: Cardiac Arrhythmias Gerry Kaye MBChB MD FRCP FRACP Consultant Cardiologist and Associate Professor
Fast Facts Fast Facts: Cardiac Arrhythmias Gerry Kaye, Steve Furniss and Robert Lemery Fast Facts Fast Facts: Cardiac Arrhythmias Gerry Kaye MBChB MD FRCP FRACP Consultant Cardiologist and Associate Professor
AV Nodal Reentrant Tachycardia with Mahaim Fiber Conduction
 AV Nodal Reentrant Tachycardia with Mahaim Fiber Conduction Chikayoshi KOMATSU, M.D., Katsuro ITO, M.D., Takanari ISHINAGA, M.D., Yasutaka TOKUHISA, M.D., Takashi TANOIRI, M.D., Hiroshi MAKINO, M.D., Jun
AV Nodal Reentrant Tachycardia with Mahaim Fiber Conduction Chikayoshi KOMATSU, M.D., Katsuro ITO, M.D., Takanari ISHINAGA, M.D., Yasutaka TOKUHISA, M.D., Takashi TANOIRI, M.D., Hiroshi MAKINO, M.D., Jun
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract
 191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
2013 Health Press Ltd.
 Fast Facts Fast Facts: Cardiac Arrhythmias Second edition Gerry Kaye MBChB MD FRCP FRACP Consultant Cardiologist and Associate Professor of Cardiology Department of Cardiology Princess Alexandra Hospital
Fast Facts Fast Facts: Cardiac Arrhythmias Second edition Gerry Kaye MBChB MD FRCP FRACP Consultant Cardiologist and Associate Professor of Cardiology Department of Cardiology Princess Alexandra Hospital
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
The HEART. What is it???? Pericardium. Heart Facts. This muscle never stops working It works when you are asleep
 This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
Concise Review for Primary-Care Physicians
 Concise Review for Primary-Care Physicians Narrow QRS Complex Tachycardias STEPHEN J. PIEPER, M.D., AND MARSHALL S. STANTON, M.D. Regular narrow QRS complex tachycardias are a common problem encountered
Concise Review for Primary-Care Physicians Narrow QRS Complex Tachycardias STEPHEN J. PIEPER, M.D., AND MARSHALL S. STANTON, M.D. Regular narrow QRS complex tachycardias are a common problem encountered
SPLITTING OF HEART SOUNDS FROM VENTRICULAR
 Brit. Heart J., 1965, 27, 691. SPLITTING OF HEART SOUNDS FROM VENTRICULAR ASYNCHRONY IN BUNDLE-BRANCH BLOCK, VENTRICULAR ECTOPIC BEATS, AND ARTIFICIAL PACING* BY EDGAR HABER AND AUBREY LEATHAM From the
Brit. Heart J., 1965, 27, 691. SPLITTING OF HEART SOUNDS FROM VENTRICULAR ASYNCHRONY IN BUNDLE-BRANCH BLOCK, VENTRICULAR ECTOPIC BEATS, AND ARTIFICIAL PACING* BY EDGAR HABER AND AUBREY LEATHAM From the
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway
 Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
Introduction to Anatomy. Dr. Maher Hadidi. Bayan Yanes. April/9 th /2013
 Introduction to Anatomy Dr. Maher Hadidi Bayan Yanes 27 April/9 th /2013 KEY POINTS: 1) Right side of the heart 2) Papillary muscles 3) Left side of the heart 4) Comparison between right and left sides
Introduction to Anatomy Dr. Maher Hadidi Bayan Yanes 27 April/9 th /2013 KEY POINTS: 1) Right side of the heart 2) Papillary muscles 3) Left side of the heart 4) Comparison between right and left sides
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
Lab 2. The Intrinsic Cardiac Conduction System. 1/23/2016 MDufilho 1
 Lab 2 he Intrinsic Cardiac Conduction System 1/23/2016 MDufilho 1 Figure 18.13 Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava ight atrium 1
Lab 2 he Intrinsic Cardiac Conduction System 1/23/2016 MDufilho 1 Figure 18.13 Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava ight atrium 1
Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block
 185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
Conduction Problems / Arrhythmias. Conduction
 Conduction Problems / Arrhythmias Conduction Wolf-Parkinson White Syndrome (WPW) and Lown-Ganong-Levine (LGL): Atrial impulses bypass the AV node through an accessory pathway or bypass tract (bundle of
Conduction Problems / Arrhythmias Conduction Wolf-Parkinson White Syndrome (WPW) and Lown-Ganong-Levine (LGL): Atrial impulses bypass the AV node through an accessory pathway or bypass tract (bundle of
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
ICD-9-CM Expert. for Payers Volumes 1, 2 & 3. International Classification of Diseases 9th Revision Clinical Modification.
 ICD-9-CM Expert for Payers Volumes 1, 2 & 3 International Classification of Diseases 9th Revision Clinical Modification Sixth Edition Edited by: Anita C. Hart, RHIA, S, S-P Catherine A. Hopkins Beth Ford,
ICD-9-CM Expert for Payers Volumes 1, 2 & 3 International Classification of Diseases 9th Revision Clinical Modification Sixth Edition Edited by: Anita C. Hart, RHIA, S, S-P Catherine A. Hopkins Beth Ford,
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
THE VESSELS OF THE HEART
 1 THE VESSELS OF THE HEART The vessels of the heart include the coronary arteries, which supply the heart and the veins and lymph vessels, which drain the heart. THE CORONARY ARTERIES These are the blood
1 THE VESSELS OF THE HEART The vessels of the heart include the coronary arteries, which supply the heart and the veins and lymph vessels, which drain the heart. THE CORONARY ARTERIES These are the blood
Collin County Community College. ! BIOL Anatomy & Physiology! WEEK 5. The Heart
 Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Mapping and Ablation of Challenging Outflow Tract VTs: Pulmonary Artery, LVOT, Epicardial
 Mapping and Ablation of Challenging Outflow Tract VTs: Pulmonary Artery, LVOT, Epicardial Samuel J. Asirvatham, MD Mayo Clinic Rochester California Heart Rhythm Symposium San Francisco, CA September 8,
Mapping and Ablation of Challenging Outflow Tract VTs: Pulmonary Artery, LVOT, Epicardial Samuel J. Asirvatham, MD Mayo Clinic Rochester California Heart Rhythm Symposium San Francisco, CA September 8,
Cardiology Flash Cards
 Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Lab Activity 23. Cardiac Anatomy. Portland Community College BI 232
 Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
CV Anatomy Quiz. Dr Ella Kim Dr Pip Green
 CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
Arrival of excitation at right ventricular apical endocardium in Wolff-Parkinson-White syndrome type A, with and without right bundle-branch block'
 British Heart Journal, 973, 35, 594-600. Arrival of excitation at right ventricular apical endocardium in Wolff-Parkinson-White syndrome type A, with and without right bundle-branch block' Cesar A. Castillo,
British Heart Journal, 973, 35, 594-600. Arrival of excitation at right ventricular apical endocardium in Wolff-Parkinson-White syndrome type A, with and without right bundle-branch block' Cesar A. Castillo,
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
Electrocardiogram and Heart Sounds
 Electrocardiogram and Heart Sounds Five physiologic properties of cardiac muscle Automaticity: SA node is the primary pacemaker of the heart, but any cells in the conduction system can initiate their
Electrocardiogram and Heart Sounds Five physiologic properties of cardiac muscle Automaticity: SA node is the primary pacemaker of the heart, but any cells in the conduction system can initiate their
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
